Label: FLUTICASONE PROPIONATE ointment
- NDC Code(s): 51672-4095-1, 51672-4095-2, 51672-4095-3, 51672-4095-5
- Packager: Taro Pharmaceuticals U.S.A., Inc.
- Category: HUMAN PRESCRIPTION DRUG LABEL
Drug Label Information
Updated February 4, 2020
If you are a healthcare professional or from the pharmaceutical industry please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use FLUTICASONE PROPIONATE OINTMENT safely and effectively. See full prescribing information for FLUTICASONE PROPIONATE OINTMENT.
FLUTICASONE PROPIONATE ointment, for topical use
Initial U.S. Approval: 1990INDICATIONS AND USAGE
Fluticasone propionate ointment is a corticosteroid indicated for the relief of the inflammatory and pruritic manifestations of corticosteroid-responsive dermatoses in adult patients. (1)
DOSAGE AND ADMINISTRATION
- Apply a thin film to affected skin areas twice daily. (2)
DOSAGE FORMS AND STRENGTHS
Ointment, 0.005%, supplied in 5 g physician samples, 15 g, 30 g and 60 g tubes. (3)
CONTRAINDICATIONS
Fluticasone propionate ointment is contraindicated in those patients with a history of serious hypersensitivity to any of the components in the preparation. (4)
WARNINGS AND PRECAUTIONS
- Hypothalamic-Pituitary-Adrenal (HPA) Axis Suppression: Reversible HPA axis suppression and resulting clinical glucocorticoid insufficiency can occur during or after withdrawal of treatment. Risk factors include use over large surface area, prolonged use, use under occlusion, altered skin barrier, liver failure, and young age. Modify use if HPA axis suppression is suspected. (5.1)
ADVERSE REACTIONS
The most common adverse reactions (<1%) were pruritus, burning, hypertrichosis, increased erythema, urticaria, irritation, and lightheadedness. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Taro Pharmaceuticals U.S.A., Inc., at 1-866-923-4914 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 1/2020
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Hypothalamic-Pituitary-Adrenal (HPA) Axis Suppression and Other Adverse Endocrine Effects
5.2 Local Adverse Reactions
5.3 Allergic Contact Dermatitis
5.4 Skin Infections
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.3 Nursing Mothers
8.4 Pediatric Use
8.5 Geriatric Use
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
16 HOW SUPPLIED/STORAGE AND HANDLING
17 PATIENT COUNSELING INFORMATION
- *
- Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
- 2 DOSAGE AND ADMINISTRATION
- 3 DOSAGE FORMS AND STRENGTHS
- 4 CONTRAINDICATIONS
-
5 WARNINGS AND PRECAUTIONS
5.1 Hypothalamic-Pituitary-Adrenal (HPA) Axis Suppression and Other Adverse Endocrine Effects
Topical corticosteroids, including fluticasone propionate ointment, can produce reversible HPA axis suppression with the potential for clinical glucocorticoid insufficiency. Factors that predispose to HPA axis suppression include large treatment surface areas, prolonged use, use under occlusion, altered skin barrier, liver failure, and young age. Cushing's syndrome, hyperglycemia, and unmasking of latent diabetes mellitus can also result from systemic absorption of topical corticosteroids.
If HPA axis suppression is suspected, gradually withdraw the drug, reduce the frequency of application, or substitute with a less potent corticosteroid. An ACTH stimulation test may be helpful in evaluating patients for HPA axis suppression.
Pediatric patients may be at greater risk of HPA axis suppression due to their higher skin surface area to body mass ratios [see Use in Specific Populations (8.4)].
HPA axis suppression may occur during or after withdrawal of treatment. If HPA axis suppression is suspected, gradually withdraw the drug, reduce the frequency of application, or substitute with a less potent corticosteroid. Evaluation of HPA axis suppression may be done by using the cosyntropin stimulation test.
5.2 Local Adverse Reactions
Fluticasone propionate ointment may cause local adverse reactions, including skin atrophy [see Adverse Reactions (6.1, 6.2)]. The risk is greater with use under occlusion.
5.3 Allergic Contact Dermatitis
Allergic contact dermatitis with topical corticosteroids is usually diagnosed by observing failure to heal rather than noting a clinical exacerbation. Such an observation can be corroborated with appropriate diagnostic patch testing. Discontinue fluticasone propionate ointment if appropriate.
-
6 ADVERSE REACTIONS
The following adverse reactions are discussed in greater detail in other sections of the labeling:
- HPA Axis Suppression and Other Adverse Endocrine Effects [see Warnings and Precautions (5.1)]
- Local Adverse Reactions [see Warnings and Precautions (5.2)]
- Concomitant Skin Infections [see Warnings and Precautions (5.3)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In controlled clinical trials, the total incidence of adverse reactions associated with the use of fluticasone propionate ointment was approximately 4%. These adverse reactions were usually mild, self-limiting, and consisted primarily of pruritus, burning, hypertrichosis, increased erythema, urticaria, irritation, and lightheadedness. Each of these events occurred individually in less than 1% of patients.
6.2 Postmarketing Experience
The following local adverse reactions have been identified during post-approval use of fluticasone propionate ointment: acneiform dermatitis, edema, rash, hypoaesthesia, pustular psoriasis, skin atrophy.
The following systemic adverse reactions have been identified during post-approval use of fluticasone propionate cream and fluticasone propionate ointment: immunosuppression/Pneumocystis jirovecii pneumonia/leukopenia/thrombocytopenia; hyperglycemia/glycosuria; Cushing syndrome; generalized body edema/blurred vision; and acute urticarial reaction (edema, urticaria, pruritus, and throat swelling).
The following local adverse reactions have also been reported with the use of topical corticosteroids: telangiectasia, striae, dryness, folliculitis, hypopigmentation, perioral dermatitis, allergic contact dermatitis, secondary infection, and miliaria.
Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category C
There are no adequate and well-controlled studies in pregnant women. Therefore, fluticasone propionate ointment should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Systemic embryofetal development studies were conducted in mice, rats and rabbits.
Subcutaneous doses of 15 μg/kg/day, 45 μg/kg/day and 150 μg/kg/day of fluticasone propionate were administered to pregnant female mice from gestation days 6 to 15. A teratogenic effect characteristic of corticosteroids (cleft palate) was noted after administration of 45 μg/kg/day and 150 μg/kg/day (less than the MRHD in adults based on body surface area comparisons) in this study. No treatment related effects on embryofetal toxicity or teratogenicity were noted at 15 μg/kg/day (less than the MRHD in adults based on body surface area comparisons).
Subcutaneous doses of 10 μg/kg/day, 30 μg/kg/day and 100 μg/kg/day of fluticasone propionate were administered to pregnant female rats in two embryofetal development studies (one study administered fluticasone propionate from gestation days 6 to 15 and the other study from gestation days 7 to 17). In the presence of maternal toxicity, fetal effects noted at 100 μg/kg/day (less than the MRHD in adults based on body surface area comparisons) included decreased fetal weights, omphalocele, cleft palate, and retarded skeletal ossification. No treatment related effects on embryofetal toxicity or teratogenicity were noted at 10 μg/kg/day (less than the MRHD in adults based on body surface area comparisons).
Subcutaneous doses of 0.08 μg/kg/day, 0.57 μg/kg/day and 4 μg/kg/day of fluticasone propionate were administered to pregnant female rabbits from gestation days 6 to 18. Fetal effects noted at 4 μg/kg/day (less than the MRHD in adults based on body surface area comparisons) included decreased fetal weights, cleft palate and retarded skeletal ossification. No treatment related effects on embryofetal toxicity or teratogenicity were noted at 0.57 μg/kg/day (less than the MRHD in adults based on body surface area comparisons).
Oral doses of 3 μg/kg/day, 30 μg/kg/day and 300 μg/kg/day fluticasone propionate were administered to pregnant female rabbits from gestation days 8 to 20. No fetal or teratogenic effects were noted at oral doses up to 300 μg/kg/day (less than the MRHD in adults based on body surface area comparisons) in this study. However, no fluticasone propionate was detected in the plasma in this study, consistent with the established low bioavailability following oral administration.
Fluticasone propionate crossed the placenta following administration of a subcutaneous or an oral dose of 100 μg/kg tritiated fluticasone propionate to pregnant rats.
8.3 Nursing Mothers
Systemically administered corticosteroids appear in human milk and can suppress growth, interfere with endogenous corticosteroid production, or cause other untoward effects. It is not known whether topical administration of corticosteroids could result in sufficient systemic absorption to produce detectable quantities in human milk. Because many drugs are excreted in human milk, caution should be exercised when fluticasone propionate ointment is administered to a nursing woman.
8.4 Pediatric Use
The safety and effectiveness of fluticasone propionate ointment have not been established in pediatric patients. Use of fluticasone propionate ointment in pediatric patients is not recommended.
Because of a higher ratio of skin surface area to body mass, pediatric patients are at a greater risk than adults of systemic effects when treated with topical drugs. They are, therefore, also at greater risk of HPA axis suppression and adrenal insufficiency upon the use of topical corticosteroids [see Warnings and Precautions (5.1)].
In a trial of 35 pediatric subjects treated with fluticasone propionate ointment, 0.005% for atopic dermatitis over at least 35% of body surface area, subnormal adrenal function was observed with cosyntropin stimulation testing at the end of 3 to 4 weeks of treatment in 4 subjects who had normal testing prior to treatment. It is not known if these subjects had recovery of adrenal function because follow-up testing was not performed. The decreased responsiveness of cosyntropin testing was not correlated to age of subject, amount of fluticasone propionate ointment used, or serum levels of fluticasone propionate.
In the above trial, telangiectasia on the face was noted in one subject on the eighth day of a 4-week treatment period. Facial use was discontinued and the telangiectasia resolved.
HPA axis suppression, Cushing's syndrome, linear growth retardation, delayed weight gain, and intracranial hypertension have been reported in pediatric patients receiving topical corticosteroids.
8.5 Geriatric Use
A limited number of patients above 65 years of age (n = 203) have been treated with futicasone propionate ointment in US and non-US clinical trials. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients. However, greater sensitivity of some older individuals cannot be ruled out.
-
11 DESCRIPTION
Fluticasone Propionate Ointment USP, 0.005% contains fluticasone propionate [S-Fluoromethyl 6α, 9α-difluoro-11β-hydroxy-16α-methyl-3-oxo-17α-propionyloxyandrosta-1,4-diene-17β-carbothioate], a synthetic fluorinated corticosteroid, for topical use.
Chemically, fluticasone propionate is C25H31F3O5S. It has the following structural formula:
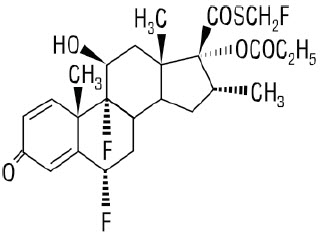
Fluticasone propionate has a molecular weight of 500.6. It is a white to off-white powder and is insoluble in water.
Each gram of Fluticasone Propionate Ointment USP, 0.005% contains fluticasone propionate 0.05 mg in a white to off-white translucent ointment base of microcrystalline wax, mineral oil, propylene glycol and sorbitan sesquioleate.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Corticosteroids play a role in cellular signaling, immune function, inflammation, and protein regulation; however, the precise mechanism of action of fluticasone propionate ointment in corticosteroid-responsive dermatoses is unknown.
12.2 Pharmacodynamics
Vasoconstrictor Assay
Studies performed with fluticasone propionate ointment indicate that it is in the medium range of potency as demonstrated in vasoconstrictor trials in healthy subjects when compared with other topical corticosteroids. However, similar blanching scores do not necessarily imply therapeutic equivalence.
12.3 Pharmacokinetics
Absorption
The extent of percutaneous absorption of topical corticosteroids is determined by many factors, including the vehicle and the integrity of the epidermal barrier. Occlusive dressing enhances penetration. Topical corticosteroids can be absorbed from normal intact skin. Inflammation and/or other disease processes in the skin increase percutaneous absorption.
In a study of 6 healthy subjects applying 25 g of fluticasone propionate ointment 0.005% twice daily to the trunk and legs for up to 5 days under occlusion, plasma levels of fluticasone ranged from 0.08 to 0.22 ng/mL.
Distribution
The percentage of fluticasone propionate bound to human plasma proteins averaged 91%. Fluticasone propionate is weakly and reversibly bound to erythrocytes. Fluticasone propionate is not significantly bound to human transcortin.
Metabolism
No metabolites of fluticasone propionate were detected in an in vitro study of radiolabeled fluticasone propionate incubated in human skin homogenate.
Fluticasone propionate is metabolized in the liver by cytochrome P450 3A4-mediated hydrolysis of the 5-fluoromethyl carbothioate grouping. This transformation occurs in 1 metabolic step to produce the inactive 17-β-carboxylic acid metabolite, the only known metabolite detected in man. This metabolite has approximately 2,000 times less affinity than the parent drug for the glucocorticoid receptor of human lung cytosol in vitro and negligible pharmacological activity in animal studies. Other metabolites detected in vitro using cultured human hepatoma cells have not been detected in man.
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
In an oral (gavage) mouse carcinogenicity study, doses of 0.1 mg/kg/day, 0.3 mg/kg/day and 1 mg/kg/day fluticasone propionate were administered to mice for 18 months. Fluticasone propionate demonstrated no tumorigenic potential at oral doses up to 1 mg/kg/day (less than the MRHD in adults based on body surface area comparisons) in this study.
In a dermal mouse carcinogenicity study, 0.05% fluticasone propionate ointment (40 μl) was topically administered for 1, 3 or 7 days/week for 80 weeks. Fluticasone propionate demonstrated no tumorigenic potential at dermal doses up to 6.7 μg/kg/day (less than the MRHD in adults based on body surface area comparisons) in this study.
Fluticasone propionate revealed no evidence of mutagenic or clastogenic potential based on the results of five in vitro genotoxicity tests (Ames assay, E. coli fluctuation test, S. cerevisiae gene conversion test, Chinese hamster ovary cell chromosome aberration assay and human lymphocyte chromosome aberration assay) and one in vivo genotoxicity test (mouse micronucleus assay).
No evidence of impairment of fertility or effect on mating performance was observed in a fertility and general reproductive performance study conducted in male and female rats at subcutaneous doses up to 50 μg/kg/day (less than the MRHD in adults based on body surface area comparisons).
- 16 HOW SUPPLIED/STORAGE AND HANDLING
-
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Patient Information).
Advise the patient:
- Avoid contact with the eyes.
- Do not bandage the treated skin area, or cover or wrap it to cause occlusion unless directed by the healthcare provider.
- Report any signs of local adverse reaction to their healthcare provider.
- Do not use on the face, underarms, or groin areas unless directed by the healthcare provider.
- SPL UNCLASSIFIED SECTION
-
PATIENT PACKAGE INSERT
PATIENT INFORMATION
Fluticasone Propionate (floo tik' a sone proe' pee oh nate) Ointment, 0.005%This Patient Information has been approved by the U.S. Food and Drug Administration. Revised: January 2020 Important: Fluticasone propionate ointment is for use on skin only (topical). Do not get fluticasone propionate ointment near or in your eyes, mouth, or vagina.
Read this Patient Information before you start using fluticasone propionate ointment and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or your treatment.What is fluticasone propionate ointment?
Fluticasone propionate ointment is a prescription corticosteroid medicine used on the skin (topical) for the relief of inflammation and itching caused by certain skin conditions in adults.
It is not known if fluticasone propionate ointment is safe and effective in children. Fluticasone propionate ointment is not recommended for use in children.Before using fluticasone propionate ointment, tell your healthcare provider about all of your medical conditions, including if you: - have an allergy to any of the ingredients in fluticasone propionate ointment
- have a skin infection at the site to be treated. You may also need medicine to treat the skin infection.
- have adrenal gland problems
- have liver problems
- have diabetes
- have thinning skin (atrophy) at the site to be treated
- are pregnant or plan to become pregnant. It is not known if fluticasone propionate ointment will harm your unborn baby.
- are breastfeeding or plan to breastfeed. It is not known if fluticasone propionate ointment can pass into your breast milk and harm your baby.
How should I use fluticasone propionate ointment? - Use fluticasone propionate ointment exactly as your healthcare provider tells you to use it.
- Apply a thin film of fluticasone propionate ointment to the affected area 2 times each day. Gently rub into your skin.
- Do not bandage, cover, or wrap the treated area unless your healthcare provider tells you to.
- Do not use fluticasone propionate ointment on your face, groin, underarms (armpits), unless your healthcare provider tells you to.
- Wash your hands after applying fluticasone propionate ointment, unless your hands are being treated.
- Tell your healthcare provider if your symptoms get worse with fluticasone propionate ointment or if your symptoms do not improve after 2 weeks of treatment.
What are the possible side effects of fluticasone propionate ointment?
Fluticasone propionate ointment may cause serious side effects, including:- Fluticasone propionate ointment can pass through your skin and may cause adrenal gland problems. This is more likely to happen if you use fluticasone propionate ointment for too long, use it over a large treatment area, use it with other topical medicines that contain corticosteroids, cover the treated area, or have liver failure. Your healthcare provider may do blood tests to check your adrenal gland function during and after treatment with fluticasone propionate ointment.
- Skin problems, including skin reactions or thinning of your skin (atrophy), skin infections, and allergic reactions (allergic contact dermatitis) at the treatment site. Tell your healthcare provider if you get any skin reactions such as pain, tenderness, swelling, or healing problems.
These are not all the possible side effects of fluticasone propionate ointment. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.How should I store fluticasone propionate ointment? - Store fluticasone propionate ointment between 68°F to 77°F (20°C to 25°C).
General information about the safe and effective use of fluticasone propionate ointment.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use fluticasone propionate ointment for a condition for which it was not prescribed. Do not give fluticasone propionate ointment to other people, even if they have the same symptoms you have. It may harm them. You can ask your pharmacist or healthcare provider for information about fluticasone propionate ointment that is written for health professionals.What are the ingredients in fluticasone propionate ointment?
Active ingredient: fluticasone propionate
Inactive ingredients: microcrystalline wax, mineral oil, propylene glycol and sorbitan sesquioleate
Manufactured by: Taro Pharmaceutical Industries Ltd., Haifa Bay, Israel 2624761
Distributed by: Taro Pharmaceuticals U.S.A., Inc., Hawthorne, NY 10532 - PRINCIPAL DISPLAY PANEL - 60 g Tube Carton
-
INGREDIENTS AND APPEARANCE
FLUTICASONE PROPIONATE
fluticasone propionate ointmentProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:51672-4095 Route of Administration TOPICAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Fluticasone Propionate (UNII: O2GMZ0LF5W) (Fluticasone - UNII:CUT2W21N7U) Fluticasone Propionate 0.05 mg in 1 g Inactive Ingredients Ingredient Name Strength mineral oil (UNII: T5L8T28FGP) microcrystalline wax (UNII: XOF597Q3KY) sorbitan sesquioleate (UNII: 0W8RRI5W5A) propylene glycol (UNII: 6DC9Q167V3) Product Characteristics Color WHITE Score Shape Size Flavor Imprint Code Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:51672-4095-5 5 g in 1 TUBE; Type 0: Not a Combination Product 06/14/2005 2 NDC:51672-4095-1 1 in 1 CARTON 06/14/2005 2 15 g in 1 TUBE; Type 0: Not a Combination Product 3 NDC:51672-4095-2 1 in 1 CARTON 06/14/2005 3 30 g in 1 TUBE; Type 0: Not a Combination Product 4 NDC:51672-4095-3 1 in 1 CARTON 06/14/2005 4 60 g in 1 TUBE; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA077145 06/14/2005 Labeler - Taro Pharmaceuticals U.S.A., Inc. (145186370) Establishment Name Address ID/FEI Business Operations Taro Pharmaceutical Industries Ltd. 600072078 MANUFACTURE(51672-4095)


