Label: OXAZEPAM capsule
- NDC Code(s): 71610-639-30, 71610-639-53, 71610-639-60
- Packager: Aphena Pharma Solutions - Tennessee, LLC
- This is a repackaged label.
- Source NDC Code(s): 52817-291
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: CIV
- Marketing Status: Abbreviated New Drug Application
Drug Label Information
Updated March 10, 2022
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Medication Guide: HTML
- Official Label (Printer Friendly)
- SPL UNCLASSIFIED SECTION
-
BOXED WARNING
(What is this?)
WARNING: RISKS FROM CONCOMITANT USE WITH OPIOIDS; ABUSE, MISUSE, AND ADDICTION; AND DEPENDENCE AND WITHDRAWAL REACTIONS
• Concomitant use of benzodiazepines and opioids may result in profound sedation, respiratory depression, coma, and death
Reserve concomitant prescribing of these drugs in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Follow patients for signs and symptoms of respiratory depression and sedation (see WARNINGS and PRECAUTIONS).
• The use of benzodiazepines, including Oxazepam, exposes users to risks of abuse, misuse, and addiction, which can lead to overdose or death. Abuse and misuse of benzodiazepines commonly involve concomitant use of other medications, alcohol, and/or illicit substances, which is associated with an increased frequency of serious adverse outcomes. Before prescribing Oxazepam and throughout treatment, assess each patient’s risk for abuse, misuse, and addiction (see WARNINGS).
• The continued use of benzodiazepines, including Oxazepam, may lead to clinically significant physical dependence. The risks of dependence and withdrawal increase with longer treatment duration and higher daily dose. Abrupt discontinuation or rapid dosage reduction of Oxazepam after continued use may precipitate acute withdrawal reactions, which can be life-threatening. To reduce the risk of withdrawal reactions, use a gradual taper to discontinue Oxazepam or reduce the dosage (see DOSAGE AND ADMINISTRATION and WARNINGS).
-
DESCRIPTION
Oxazepam, USP is the first of a chemical series of compounds known as the 3- hydroxybenzodiazepinones. A therapeutic agent providing versatility and flexibility in control of common emotional disturbances, this product exerts prompt action in a wide variety of disorders associated with anxiety, tension, agitation, and irritability, and anxiety associated with depression. In tolerance and toxicity studies on several animal species, this product reveals significantly greater safety factors than related compounds (chlordiazepoxide and diazepam) and manifests a wide separation of effective doses and doses inducing side effects.
Oxazepam, is 7-chloro-1,3-dihydro-3-hydroxy-5-phenyl-2H-1,4-benzodiazepin-2-one and has the following structural formula:
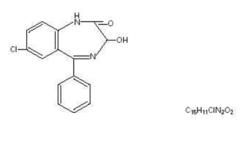 MW 286.72
MW 286.72Oxazepam is a white-crystalline powder.
Each capsule for oral administration contain 10 mg, 15 mg or 30 mg of oxazepam.
Inactive ingredients: croscarmellose sodium, D&C yellow #10, FD&C blue #1, FD&C blue # 2, FD&C red # 40, ferric oxide black, gelatin, lactose monohydrate, magnesium stearate, microcrystalline cellulose, n-butyl alcohol, propylene glycol, sda-3a alcohol, shellac, sodium lauryl sulfate, titanium dioxide and other inert ingredients.
The 15 mg capsule also contains: FD&C yellow # 6.
The 30 mg capsule also contains: D&C red # 28.
-
CLINICAL PHARMACOLOGY
Pharmacokinetic testing in 12 volunteers demonstrated that a single 30 mg dose of a capsule, tablet or suspension will result in equivalent extent of absorption.
For the capsule and tablet, peak plasma levels averaged 450 mg/mL and were observed to occur about 3 hours after dosing. The mean elimination half-life for oxazepam was approximately 8.2 hours (range 5.7 to 10.9 hours).
This product has a single, major inactive metabolite in man, a glucuronide excreted in the urine.
Age (<80 years old) does not appear to have a clinically significant effect on oxazepam kinetics. A statistically significant increase in elimination half-life in the very elderly (> 80 years of age) as compared to younger subjects has been reported, due to a 30% increase in volume of distribution, as well as a 50% reduction in unbound clearance of oxazepam in the very elderly (see PRECAUTIONS, Geriatric Use).
-
ANIMAL PHARMACOLOGY AND TOXICOLOGY
In mice, oxazepam exerts an anticonvulsant (anti-pentylenetetrazol) activity at 50-percent-effective doses of about 0.6 mg/kg orally. (Such anticonvulsant activity of benzodiazepines correlates with their tranquilizing properties.) To produce ataxia (rotabar test) and sedation (abolition of spontaneous motor activity), the 50-percent-effective doses of this product are greater than 5 mg/kg orally. Thus, about ten times the therapeutic (anticonvulsant) dose must be given before ataxia ensues, indicating a wide separation of effective doses and doses inducing side effects.
In evaluation of antianxiety activity of compounds, conflict behavioral tests in rats differentiate continuous response for food in the presence of anxiety-provoking stress (shock) from drug-induced motor incoordination. This product shows significant separation of doses required to relieve anxiety and doses producing sedation or ataxia. Ataxia-producing doses exceed those of related CNS-acting drugs.
Acute oral LD50 in mice is greater than 5000 mg/kg, compared to 800 mg/kg for a related compound (chlordiazepoxide).
Subacute toxicity studies in dogs for four weeks at 480 mg/kg daily showed no specific changes; at 960 mg/kg, two out of eight died with evidence of circulatory collapse. This wide margin of safety is significant compared to chlordiazepoxide HCl, which showed nonspecific changes in six dogs at 80 mg/kg. On chlordiazepoxide, two out of six died with evidence of circulatory collapse at 127 mg/kg, and six out of six died at 200 mg/kg daily. Chronic toxicity studies of oxazepam in dogs at 120 mg/kg/day for 52 weeks produced no toxic manifestation.
Fatty metamorphosis of the liver has been noted in six-week toxicity studies in rats given this product at 0.5% of the diet. Such accumulations of fat are considered reversible, as there is no liver necrosis or fibrosis. Breeding studies in rats through two successive litters did not produce fetal abnormality.
Oxazepam has not been adequately evaluated for mutagenic activity.
In a carcinogenicity study, oxazepam was administered with diet to rats for two years. Male rats receiving 30 times the maximum human dose showed a statistical increase, when compared to controls, in benign thyroid follicular cell tumors, testicular interstitial cell adenomas, and prostatic adenomas. An earlier published study reported that mice fed dietary dosages of 35 or 100 times the human daily dose of oxazepam for 9 months developed a dose-related increase in liver adenomas.1 In an independent analysis of some of the microscopic slides from this mouse study, several of these tumors were classified as liver carcinomas. At this time, there is no evidence that clinical use of oxazepam is associated with tumors.
-
INDICATIONS
Oxazepam is indicated for the management of anxiety disorders or for the short-term relief of the symptoms of anxiety. Anxiety or tension associated with the stress of everyday life usually does not require treatment with an anxiolytic.
Anxiety associated with depression is also responsive to oxazepam therapy.
This product has been found particularly useful in the management of anxiety, tension, agitation, and irritability in older patients.
Alcoholics with acute tremulousness, inebriation, or with anxiety, associated with alcohol withdrawal are responsive to therapy.
The effectiveness of oxazepam in long-term use, that is, more than 4 months, has not been assessed by systematic clinical studies. The physician should periodically reassess the usefulness of the drug for the individual patient.
- CONTRAINDICATIONS
-
WARNINGS
Risks from Concomitant Use with Opioids: Concomitant use of benzodiazepines, including oxazepam, and opioids may result in profound sedation, respiratory depression, coma, and death. Because of these risks, reserve concomitant prescribing of these drugs in patients for whom alternative treatment options are inadequate.
Observational studies have demonstrated that concomitant use of opioid analgesics and benzodiazepines increases the risk of drug-related mortality compared to use of opioids alone. If a decision is made to prescribe oxazepam concomitantly with opioids, prescribe the lowest effective dosages and minimum durations of concomitant use, and follow patients closely for signs and symptoms of respiratory depression and sedation. In patients already receiving an opioid analgesic, prescribe a lower initial dose of oxazepam than indicated in the absence of an opioid and titrate based on clinical response. If an opioid is initiated in a patient already taking oxazepam, prescribe a lower initial dose of the opioid and titrate based upon clinical response.
Advise both patients and caregivers about the risks of respiratory depression and sedation when oxazepam is used with opioids. Advise patients not to drive or operate heavy machinery until the effects of concomitant use with the opioid have been determined (see PRECAUTIONS: Drug Interactions.)
Abuse, Misuse, and Addiction: The use of benzodiazepines, including Oxazepam, exposes users to the risks of abuse, misuse, and addiction, which can lead to overdose or death. Abuse and misuse of benzodiazepines often (but not always) involve the use of doses greater than the maximum recommended dosage and commonly involve concomitant use of other medications, alcohol, and/or illicit substances, which is associated with an increased frequency of serious adverse outcomes, including respiratory depression, overdose, or death (see DRUG ABUSE AND DEPENDENCE: Abuse).
Before prescribing Oxazepam and throughout treatment, assess each patient’s risk for abuse, misuse, and addiction (e.g., using a standardized screening tool). Use of Oxazepam, particularly in patients at elevated risk, necessitates counseling about the risks and proper use of Oxazepam along with monitoring for signs and symptoms of abuse, misuse, and addiction. Prescribe the lowest effective dosage; avoid or minimize concomitant use of CNS depressants and other substances associated with abuse, misuse, and addiction (e.g., opioid analgesics, stimulants); and advise patients on the proper disposal of unused drug. If a substance use disorder is suspected, evaluate the patient and institute (or refer them for) early treatment, as appropriate.
Dependence and Withdrawal Reactions: To reduce the risk of withdrawal reactions, use a gradual taper to discontinue Oxazepam or reduce the dosage (a patient-specific plan should be used to taper the dose) (see DOSAGE AND ADMINISTRATION: Discontinuation or Dosage Reduction of Oxazepam).
Patients at an increased risk of withdrawal adverse reactions after benzodiazepine discontinuation or rapid dosage reduction include those who take higher dosages, and those who have had longer durations of use.
Acute Withdrawal Reactions
The continued use of benzodiazepines, including Oxazepam, may lead to clinically significant physical dependence. Abrupt discontinuation or rapid dosage reduction of Oxazepam after continued use or administration of flumazenil (a benzodiazepine antagonist) may precipitate acute withdrawal reactions, which can be life threatening. (e.g., seizures) (see DRUG ABUSE AND DEPENDENCE-Dependence).
Protracted Withdrawal Syndrome
In some cases, benzodiazepine users have developed a protracted withdrawal syndrome with withdrawal symptoms lasting weeks to more than 12 months (see DRUG ABUSE AND DEPENDENCE-Dependence).
As with other CNS-acting drugs, patients should be cautioned against driving automobiles or operating dangerous machinery until it is known that they do not become drowsy or dizzy on oxazepam therapy.
Patients should be warned that the effects of alcohol or other CNS-depressant drugs may be additive to those of Oxazepam, possibly requiring adjustment of dosage or elimination of such agents.
-
USE IN PREGNANCY
An increased risk of congenital malformations associated with the use of minor tranquilizers (chlordiazepoxide, diazepam, and meprobamate) during the first trimester of pregnancy has been suggested in several studies. Oxazepam, a benzodiazepine derivative, has not been studied adequately to· determine whether it, too, may be associated with an increased risk of fetal abnormality. Because use of these drugs is rarely a matter of urgency, their use during this period should almost always be avoided. The possibility that a woman of childbearing potential may be pregnant at the time of institution of therapy should be considered. Patients should be advised that if they become pregnant during therapy or intend to become pregnant they should communicate with their physician about the desirability of discontinuing the drug.
-
PRECAUTIONS
General:
Although hypotension has occurred only rarely, oxazepam should be administered with caution to patients in whom a drop in blood pressure might lead to cardiac complications. This is particularly true in the elderly patient.
Information for Patients
Advise the patient to read the FDA-approved patient labeling (Medication Guide)
Risks from Concomitant Use with Opioids
Advise both patients and caregivers about the risks of potentially fatal respiratory depression and sedation when Oxazepam is used with opioids and not to use such drugs concomitantly unless supervised by a health care provider. Advise patients not to drive or operate heavy machinery until the effects of concomitant use with the opioid have been determined (see WARNINGS: Risks from Concomitant Use with Opioids and PRECAUTIONS: Drug Interactions).
Abuse, Misuse, and Addiction
Inform patients that the use of Oxazepam, even at recommended dosages, exposes users to risks of abuse, misuse, and addiction, which can lead to overdose and death, especially when used in combination with other medications (e.g., opioid analgesics), alcohol, and/or illicit substances. Inform patients about the signs and symptoms of benzodiazepine abuse, misuse, and addiction; to seek medical help if they develop these signs and/or symptoms; and on the proper disposal of unused drug (see WARNINGS: Abuse, Misuse, and Addiction and DRUG ABUSE AND DEPENDENCE).
Withdrawal Reactions
Inform patients that the continued use of Oxazepam may lead to clinically significant physical dependence and that abrupt discontinuation or rapid dosage reduction of Oxazepam may precipitate acute withdrawal reactions, which can be life-threatening. Inform patients that in some cases, patients taking benzodiazepines have developed a protracted withdrawal syndrome with withdrawal symptoms lasting weeks to more than 12 months. Instruct patients that discontinuation or dosage reduction of Oxazepam may require a slow taper (see WARNINGS: Dependence and Withdrawal Reactions and DRUG ABUSE AND DEPENDENCE).
Drug Interactions:
The concomitant use of benzodiazepines and opioids increases the risk of respiratory depression because of actions at different receptor sites in the CNS that control respiration. Benzodiazepines interact at GABAA sites and opioids interact primarily at mu receptors. When benzodiazepines and opioids are combined, the potential for benzodiazepines to significantly worsen opioid- related respiratory depression exists. Limit dosage and duration of concomitant use of benzodiazepines and opioids, and monitor patients closely for respiratory depression and sedation.
Pediatric Use:
Safety and effectiveness in pediatric patients under 6 years of age have not been established. Absolute dosage for pediatric patients 6 to 12 years of age is not established.
Geriatric Use:
Clinical studies of oxazepam were not adequate to determine whether subjects aged 65 and over respond differently than younger subjects. Age (<80 years old) does not appear to have a clinically significant effect on oxazepam kinetics [see CLINICAL PHARMACOLOGY].
Clinical circumstances, some of which may be more common in the elderly, such as hepatic or renal impairment, should be considered. Greater sensitivity of some older individuals to the effects of oxazepam (e.g., sedation, hypotension, paradoxical excitation) cannot be ruled out [see PRECAUTIONS: General; see ADVERSE REACTIONS]. In general, dose selection for oxazepam for elderly patients should be cautious, usually starting at the lower end of the dosing range (see DOSAGE AND ADMINISTRATION).
-
ADVERSE REACTIONS
The necessity for discontinuation of therapy due to undesirable effects has been rare. Transient, mild drowsiness is commonly seen in the first few days of therapy. If it persists, the dosage should be reduced. In few instances, dizziness, vertigo, headache, and rarely syncope have occurred either alone or together with drowsiness. Mild paradoxical reactions, i.e., excitement, stimulation of affect, have been reported in psychiatric patients; these reactions may be secondary to relief of anxiety and usually appear in the first two weeks of therapy.
Other side effects occurring during oxazepam therapy include rare instances of minor diffuse skin rashes-morbilliform, urticarial, and maculopapular nausea, lethargy, edema, slurred speech, tremor and altered libido. Such side effects have been infrequent and are generally controlled with reduction of dosage. A case of an extensive fixed drug eruption also has been reported.
Although rare, leukopenia and hepatic dysfunction including jaundice have been reported during therapy. Periodic blood counts and liver-function tests are advisable. Ataxia with oxazepam has been reported in rare instances and does not appear to be specifically related to dose or age.
Although the following side reactions have not as yet been reported with oxazepam, they have occurred with related compounds (chlordiazepoxide and diazepam): paradoxical excitation with severe rage reactions, hallucinations, menstrual irregularities, change in EEG pattern, blood dyscrasias including agranulocytosis, blurred vision, diplopia, incontinence, stupor, disorientation, fever, and euphoria.
Transient amnesia or memory impairment has been reported in association with the use of benzodiazepines.
-
DRUG ABUSE AND DEPENDENCE
Controlled Substance
Oxazepam is a Schedule IV controlled substance.
Abuse
Oxazepam is a benzodiazepine and a CNS depressant with a potential for abuse and addiction. Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects. Misuse is the intentional use, for therapeutic purposes, of a drug by an individual in a way other than prescribed by a health care provider or for whom it was not prescribed. Drug addiction is a cluster of behavioral, cognitive, and physiological phenomena that may include a strong desire to take the drug, difficulties in controlling drug use (e.g., continuing drug use despite harmful consequences, giving a higher priority to drug use than other activities and obligations), and possible tolerance or physical dependence. Even taking benzodiazepines as prescribed may put patients at risk for abuse and misuse of their medication. Abuse and misuse may lead to addiction.
Abuse and misuse of benzodiazepines often (but not always) involve the use of doses greater than the maximum recommended dosage and commonly involve concomitant use of other medications, alcohol, and/or illicit substances, which is associated with an increased frequency of serious adverse outcomes, including respiratory depression, overdose, or death. Benzodiazepines are often sought by individuals who abuse drugs and other substances, and by individuals with addictive disorders (see WARNINGS- Abuse, Misuse, and Addiction).
The following adverse reactions have occurred with benzodiazepine abuse and/or misuse: abdominal pain, amnesia, anorexia, anxiety, aggression, ataxia, blurred vision, confusion, depression, disinhibition, disorientation, dizziness, euphoria, impaired concentration and memory, indigestion, irritability, muscle pain, slurred speech, tremors, and vertigo.
The following severe adverse reactions have occurred with benzodiazepine abuse and/or misuse: delirium, paranoia, suicidal ideation and behavior, seizures, coma, breathing difficulty, and death. Death is more often associated with polysubstance use (especially benzodiazepines with other CNS depressants such as opioids and alcohol).
Dependence
Physical Dependence
Oxazepam may produce physical dependence from continued therapy. Physical dependence is a state that develops as a result of physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
Abrupt discontinuation or rapid dosage reduction of benzodiazepines or administration of flumazenil, a benzodiazepine antagonist, may precipitate acute withdrawal reactions, including seizures, which can be life-threatening. Patients at an increased risk of withdrawal adverse reactions after benzodiazepine discontinuation or rapid dosage reduction include those who take higher dosages (i.e., higher and/or more frequent doses) and those who have had longer durations of use (see WARNINGS-Dependence and Withdrawal Reactions).
To reduce the risk of withdrawal reactions, use a gradual taper to discontinue Oxazepam or reduce the dosage (see DOSAGE AND DMINISTRATION-Discontinuation or Dosage Reduction of Oxazepam and WARNINGS- Dependence and Withdrawal Reactions).
Acute Withdrawal Signs and Symptoms
Acute withdrawal signs and symptoms associated with benzodiazepines have included abnormal involuntary movements, anxiety, blurred vision, depersonalization, depression, derealization, dizziness, fatigue, gastrointestinal adverse reactions (e.g., nausea, vomiting, diarrhea, weight loss, decreased appetite), headache, hyperacusis, hypertension, irritability, insomnia, memory impairment, muscle pain and stiffness, panic attacks, photophobia, restlessness, tachycardia, and tremor. More severe acute withdrawal signs and symptoms, including life-threatening reactions, have included catatonia, convulsions, delirium tremens, depression, hallucinations, mania, psychosis, seizures, and suicidality.
Protracted Withdrawal Syndrome
Protracted withdrawal syndrome associated with benzodiazepines is characterized by anxiety, cognitive impairment, depression, insomnia, formication, motor symptoms (e.g., weakness, tremor, muscle twitches), paresthesia, and tinnitus that persists beyond 4 to 6 weeks after initial benzodiazepine withdrawal. Protracted withdrawal symptoms may last weeks to more than 12 months. As a result, there may be difficulty in differentiating withdrawal symptoms from potential re-emergence or continuation of symptoms for which the benzodiazepine was being used.
Tolerance
Tolerance to Oxazepam may develop from continued therapy. Tolerance is a physiological state characterized by a reduced response to a drug after repeated administration (i.e., a higher dose of a drug is required to produce the same effect that was once obtained at a lower dose). Tolerance to the therapeutic effect of Oxazepam may develop; however, little tolerance develops to the amnestic reactions and other cognitive impairments caused by benzodiazepines.
-
OVERDOSAGE
In the management of overdosage with any drug, it should be borne in mind that multiple agents may have been taken.
Symptoms
Overdosage of benzodiazepines is usually manifested by varying degrees of central nervous system depression ranging from drowsiness to coma. In mild cases, symptoms include drowsiness, mental confusion and lethargy. In more serious cases, and especially when other drugs or alcohol were ingested, symptoms may include ataxia, hypotonia, hypotension, hypnotic state, stage one (1) to three (3) coma, and very rarely, death.
Management
Induced vomiting and/or gastric lavage should be undertaken, followed by general supportive care, monitoring of vital signs, and close observation of the patient. Hypotension, though unlikely, usually may be controlled with norepinephrine bitartrate injection. The value of dialysis has not been adequately determined for oxazepam.
The benzodiazepine antagonist flumazenil may be used in hospitalized patients as an adjunct to, not as a substitute for, proper management of benzodiazepine overdose. The prescriber should be aware of a risk of seizure in association with flumazenil treatment, particularly in long-term benzodiazepine users and in cyclic antidepressant overdose. The complete flurnazenil package insert including “CONTRAINDICATIONS,” “WARNINGS,” and “PRECAUTIONS” should be consulted prior to use.
-
DOSAGE AND ADMINISTRATION
Because of the flexibility of this product and the range of emotional disturbances responsive to it, dosage should be individualized for maximum beneficial effects.
OXAZEPAM Usual Dose Mild-to-moderate anxiety, with associated tension, irritability, agitation, or related symptoms of functional origin secondary to organic 10 to 15 mg. 3 or 4 times daily Severe anxiety syndromes, agitation, or anxiety associated with depression 15 to 30 mg. 3 or 4 times daily
Older patients with anxiety, tension, irritability, and agitation Initial dosage: 10 mg, 3 times daily.
If necessary, increase cautiously to 15 mg, 3 or 4 times daily.Alcoholics with acute inebriation, tremulousness, or anxiety on withdrawal 15 to 30 mg, 3 or 4 times daily This product is not indicated in pediatric patients under 6 years of age. Absolute dosage for pediatric patients 6 to 12 years of age is not established.
Discontinuation or Dosage Reduction of Oxazepam
To reduce the risk of withdrawal reactions, use a gradual taper to discontinue Oxazepam or reduce the dosage. If a patient develops withdrawal reactions, consider pausing the taper or increasing the dosage to the previous tapered dosage level. Subsequently decrease the dosage more slowly (see WARNINGS: Dependence and Withdrawal Reactions and DRUG ABUSE AND DEPENDENCE: Dependence).
-
HOW SUPPLIED
Oxazepam capsules, USP are available as:
10 mg - Each #4 white opaque/white opaque gelatin capsule, printed FBP660 in black ink on the cap and body contains 10 mg of Oxazepam, USP. Oxazepam Capsules are supplied in bottles of 100 (NDC 52817-290-10)
15 mg - Each #4 red opaque/red opaque gelatin capsule, printed FBP661in black ink on the cap and body, contains 15 mg of Oxazepam, USP. Oxazepam Capsules are supplied in bottles of 100 (NDC 52817-291-10)
30 mg - Each #4 maroon opaque/maroon opaque gelatin capsule, printed FBP662 in black ink on the cap and body, contains 30 mg of Oxazepam, USP. Oxazepam Capsules are supplied in bottles of 100 (NDC 52817-292-10)
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. Protect from moisture.
Dispense in a tight, light-resistant container.
- REFERENCE
-
MEDICATION GUIDE
MEDICATION GUIDE
Oxazepam (ox-AZE-e-pam) Capsules, USP C-IV
What is the most important information I should know about oxazepam?
- Oxazepam is a benzodiazepine medicine. Taking benzodiazepines with opioid medicines, alcohol, or other central nervous system (CNS) depressants (including street drugs) can cause severe drowsiness, breathing problems (respiratory depression), coma and death.
Get emergency help right away if any of the following happens:
o shallow or slowed breathing
o breathing stops (which may lead to the heart stopping)
o excessive sleepiness (sedation).
Do not drive or operate heavy machinery until you know how taking oxazepam with opioids affects you.
Risk of abuse, misuse, and addiction. There is a risk of abuse, misuse, and addiction with benzodiazepines, including Oxazepam, which can lead to overdose and serious side effects including coma and death.
o Serious side effects including coma and death have happened in people who have abused or misused benzodiazepines, including Oxazepam. These serious side effects may include delirium, paranoia, suicidal thoughts or actions, seizures, and difficulty breathing. Call your healthcare provider or go to the nearest hospital emergency room right away if you get any of these serious side effects.
- You can develop an addiction even if you take Oxazepam exactly as prescribed by your healthcare provider.
o Take Oxazepam exactly as your healthcare provider prescribed.
o Do not share your Oxazepam with other people
o Keep Oxazepam in a safe place and away from children.
Physical dependence and withdrawal reactions.
o Do not suddenly stop taking Oxazepam. Stopping Oxazepam suddenly can cause serious and life-threatening side effects, including unusual movements, responses, or expressions, seizures, sudden and severe mental or nervous system changes, depression, seeing or hearing things that others do not see or hear, an extreme increase in activity or talking, losing touch with reality, and suicidal thoughts or actions. Call your healthcare provider or go to the nearest hospital emergency room right away if you get any of these symptoms.
o Some people who suddenly stop benzodiazepines have symptoms that can last for several weeks to more than 12 months, including, anxiety, trouble remembering, learning, or concentrating, depression, problems sleeping, feeling like insects are crawling under your skin, weakness, shaking, muscle twitching, burning or prickling feeling in your hands, arms, legs or feet, and ringing in your ears.
Physical dependence is not the same as drug addiction. Your healthcare provider can tell you more about the differences between physical dependence and drug addiction.
o Do not take more oxazepam than prescribed or take oxazepam for longer than prescribed.
What is oxazepam?
- Oxazepam is a prescription medicine used:
- to treat anxiety disorders
- for the short-term relief of the symptoms of anxiety or anxiety that can happen with depression
- to treat anxiety, tension, agitation and irritability in elderly people
- to relieve the symptoms of alcohol withdrawal including agitation, shakiness (tremor), and anxiety associated with acute alcohol withdrawal.
-
Oxazepam is a federal controlled substance (C-IV) because it contains oxazepam that can be abused or lead to dependence. Keep oxazepam capsules in a safe place to prevent misuse and abuse. Selling or giving away oxazepam capsules may harm others, and is against the law. Tell your healthcare provider if you have abused or been dependent on alcohol, prescription medicines or street drugs.
- It is not known if oxazepam is safe and effective in children under 6 years of age.
- It is known if oxazepam is safe and effective for use longer than 4 months.
Do not take oxazepam if you:
• are allergic to oxazepam or any of the ingredients in oxazepam capsules. See the end of this Medication Guide for a complete list of ingredients in oxazepam capsules.
Before you take oxazepam, tell your healthcare provider about all of your medical conditions, including if you:
- have or have had depression, mood problems, or suicidal thoughts or behavior
- have liver or kidney problems
- have or have had problems with fainting or low blood pressure
- are pregnant or plan to become pregnant. Oxazepam may harm your unborn baby. You and your healthcare provider should decide if you should take oxazepam while you are pregnant.
- are breastfeeding or plan to breastfeed. Oxazepam may pass into your breast milk and may harm your baby. Talk to your healthcare provider about the best way to feed your baby if you take oxazepam
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
Taking oxazepam with certain other medicines can cause side effects or affect how well oxazepam or the other medicines work Do not start or stop other medicines without talking to your healthcare provider.
How should I take oxazepam?
- See "What is the most important information I should know about oxazepam?"
- Take oxazepam exactly as your healthcare provider tells you to take it. Your healthcare provider will tell you how many oxazepam capsules to take and when to take it.
- If you take too many oxazepam capsules, call your healthcare provider or go to the nearest hospital emergency room right away.
What are the possible side effects of oxazepam?
Oxazepam may cause serious side effects, including:
-
See "What is the most important information I should know about oxazepam?"
- Low blood pressure. Oxazepam can cause low blood pressure especially in elderly people.
Oxazepam can make you sleepy or dizzy and can slow your thinking and motor skills.
o Do not drive, operate heavy machinery, or do other dangerous activities until you know how oxazepam affects you.
o Do not drink alcohol or take other drugs that may make you sleepy or dizzy while taking oxazepam without first talking to your healthcare provider. When taken with alcohol or drugs that cause sleepiness or dizziness, oxazepam may make your sleepiness or dizziness much worse.
The most common side effects of oxazepam include:
- drowsiness
- dizziness
- vertigo
- headache
These are not all the possible side effects of oxazepam. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store oxazepam?
- Store oxazepam at room temperature between 68°F to 77°F (20°C to 25°C).
- Keep oxazepam in a tightly closed container and out of the light.
- Keep oxazepam capsules and all medicines out of the reach of children.
General information about the safe and effective use of oxazepam capsules.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use oxazepam for a condition for which it was not prescribed. Do not give oxazepam to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about oxazepam that is written for health professionals.
What are the ingredients in oxazepam?
Active ingredient: oxazepam
Inactive ingredients:
croscarmellose sodium, D&C yellow #10, FD&C blue #1, FD&C blue # 2, FD&C red # 40, ferric oxide black, gelatin, lactose monohydrate, magnesium stearate, microcrystalline cellulose, n-butyl alcohol, propylene glycol, sda-3a alcohol, shellac, sodium lauryl sulfate, titanium dioxide and other inert ingredients.
The 15 mg capsule also contains: FD&C yellow # 6.
The 30 mg also contains: D&C red # 28.
For more information, call TruPharma LLC at 1-877-541-5504
Manufactured by:
Frontida BioPharm, Inc. Philadelphia, PA 19124 USA
Distributed by:
TruPharma LLC, Tampa, FL 33609 USA
This Medication Guide has been approved by the U.S. Food and Drug Administration
Issued: 02/05/2021
Rev 04, 02/2021
-
Repackaging Information
Please reference the How Supplied section listed above for a description of individual tablets. This drug product has been received by Aphena Pharma - TN in a manufacturer or distributor packaged configuration and repackaged in full compliance with all applicable cGMP regulations. The package configurations available from Aphena are listed below:
Count 15 mg 30 71610-639-30 60 71610-639-53 90 71610-639-60 Store between 20°-25°C (68°-77°F). See USP Controlled Room Temperature. Dispense in a tight light-resistant container as defined by USP. Keep this and all drugs out of the reach of children.
Repackaged by:

Cookeville, TN 38506
20220310JK - PRINCIPAL DISPLAY PANEL - 15 mg
-
INGREDIENTS AND APPEARANCE
OXAZEPAM
oxazepam capsuleProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:71610-639(NDC:52817-291) Route of Administration ORAL DEA Schedule CIV Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength OXAZEPAM (UNII: 6GOW6DWN2A) (OXAZEPAM - UNII:6GOW6DWN2A) OXAZEPAM 15 mg Inactive Ingredients Ingredient Name Strength CROSCARMELLOSE SODIUM (UNII: M28OL1HH48) D&C YELLOW NO. 10 (UNII: 35SW5USQ3G) FD&C BLUE NO. 1 (UNII: H3R47K3TBD) FD&C BLUE NO. 2 (UNII: L06K8R7DQK) FD&C RED NO. 40 (UNII: WZB9127XOA) FERROSOFERRIC OXIDE (UNII: XM0M87F357) GELATIN (UNII: 2G86QN327L) LACTOSE MONOHYDRATE (UNII: EWQ57Q8I5X) MAGNESIUM STEARATE (UNII: 70097M6I30) MICROCRYSTALLINE CELLULOSE (UNII: OP1R32D61U) BUTYL ALCOHOL (UNII: 8PJ61P6TS3) PROPYLENE GLYCOL (UNII: 6DC9Q167V3) ALCOHOL (UNII: 3K9958V90M) SHELLAC (UNII: 46N107B71O) SODIUM LAURYL SULFATE (UNII: 368GB5141J) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) FD&C YELLOW NO. 6 (UNII: H77VEI93A8) Product Characteristics Color RED Score no score Shape CAPSULE Size 14mm Flavor Imprint Code FBP661 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:71610-639-30 30 in 1 BOTTLE; Type 0: Not a Combination Product 03/09/2022 2 NDC:71610-639-53 60 in 1 BOTTLE; Type 0: Not a Combination Product 03/09/2022 3 NDC:71610-639-60 90 in 1 BOTTLE; Type 0: Not a Combination Product 03/09/2022 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA071026 06/01/2021 Labeler - Aphena Pharma Solutions - Tennessee, LLC (128385585) Establishment Name Address ID/FEI Business Operations Aphena Pharma Solutions - Tennessee, LLC 128385585 REPACK(71610-639)


