Label: TOPICORT- desoximetasone spray
-
NDC Code(s):
51672-5281-0,
51672-5281-3,
51672-5281-4,
51672-5281-6, view more51672-5281-7
- Packager: Taro Pharmaceuticals U.S.A., Inc.
- Category: HUMAN PRESCRIPTION DRUG LABEL
Drug Label Information
Updated September 14, 2021
If you are a healthcare professional or from the pharmaceutical industry please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
-
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use TOPICORT® topical spray safely and effectively. See full prescribing information for TOPICORT® topical spray.
TOPICORT® (desoximetasone) topical spray
Initial U.S. Approval: 1977INDICATIONS AND USAGE
Topicort® Topical Spray is a corticosteroid indicated for the treatment of plaque psoriasis in patients 18 years of age or older (1).
DOSAGE AND ADMINISTRATION
- Apply a thin film to the affected skin areas twice daily. Rub in gently. (2)
- Discontinue treatment when control is achieved. (2)
- Treatment beyond 4 weeks is not recommended. (2)
- Do not use if atrophy is present at the treatment site. (2)
- Do not use with occlusive dressings, unless directed by the physician. (2)
- Avoid use on the face, axilla or groin. (2)
- Not for oral, ophthalmic, or intravaginal use. (2)
DOSAGE FORMS AND STRENGTHS
Spray, 0.25% w/w (3)
CONTRAINDICATIONS
None (4)
WARNINGS AND PRECAUTIONS
-
Effect on Endocrine System: Topicort® Topical Spray can produce reversible HPA axis suppression with the potential for glucocorticosteroid insufficiency during or after treatment. (5.1)
- Cushing's syndrome, hyperglycemia, and unmasking of latent diabetes mellitus can result from systemic absorption of topical corticosteroids. (5.1)
- Because of the potential for systemic absorption, use of topical corticosteroids may require that patients be periodically evaluated for HPA axis suppression. (5.1)
- Modify use if HPA axis suppression develops. (5.1)
- High potency corticosteroids, large treatment surface areas, prolonged use, use of occlusive dressings, altered skin barrier, liver failure and young age may predispose patients to HPA axis suppression. (5.1)
- Pediatric patients may be more susceptible to systemic toxicity when treated with topical corticosteroids. Safety and effectiveness have not been established in pediatric patients and use in pediatric patients is not recommended. (5.1, 8.4)
- Ophthalmic Adverse Reactions: Topical corticosteroid products may increase the risk of cataracts and glaucoma. If visual symptoms occur, consider referral to an ophthalmologist. (5.3).
- Flammability: Topicort Topical Spray is flammable; keep away from heat or flame. (5.6)
ADVERSE REACTIONS
The most common adverse reactions (≥ 1%) are application site dryness, application site irritation and application site pruritus. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Taro Pharmaceuticals U.S.A., Inc. at 1-866-923-4914 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling.
Revised: 9/2021
-
Table of Contents
FULL PRESCRIBING INFORMATION: CONTENTS*
1 INDICATIONS AND USAGE
2 DOSAGE AND ADMINISTRATION
3 DOSAGE FORMS AND STRENGTHS
4 CONTRAINDICATIONS
5 WARNINGS AND PRECAUTIONS
5.1 Effect on Endocrine System
5.2 Local Adverse Reactions with Topical Corticosteroids
5.3 Ophthalmic Adverse Reactions
5.4 Allergic Contact Dermatitis with Topical Corticosteroids
5.5 Concomitant Skin Infections
5.6 Flammability
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
6.2 Postmarketing Experience
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
8.2 Lactation
8.4 Pediatric Use
8.5 Geriatric Use
10 OVERDOSAGE
11 DESCRIPTION
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
12.2 Pharmacodynamics
12.3 Pharmacokinetics
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
14 CLINICAL STUDIES
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 How Supplied/Storage
16.2 Instructions for the Pharmacist
17 PATIENT COUNSELING INFORMATION
- *
- Sections or subsections omitted from the full prescribing information are not listed.
- 1 INDICATIONS AND USAGE
-
2 DOSAGE AND ADMINISTRATION
Apply Topicort Topical Spray as a thin film to the affected skin areas twice daily. Rub in gently.
Do not bandage or otherwise cover or wrap the treated skin unless directed by the physician.
Discontinue treatment when control is achieved.
Treatment beyond 4 weeks is not recommended.
Do not use if atrophy is present at the treatment site.
Avoid use on the face, axilla or groin.
Topicort Topical Spray is for external use only. It is not for oral, ophthalmic, or intravaginal use.
- 3 DOSAGE FORMS AND STRENGTHS
- 4 CONTRAINDICATIONS
-
5 WARNINGS AND PRECAUTIONS
5.1 Effect on Endocrine System
Topicort Topical Spray is a topical corticosteroid that has been shown to suppress the hypothalamic-pituitary-adrenal (HPA) axis.
Systemic absorption of topical corticosteroids can produce reversible HPA axis suppression with the potential for glucocorticosteroid insufficiency. This may occur during treatment or upon withdrawal of the topical corticosteroid.
In a study including 21 evaluable subjects 18 years of age or older with moderate to severe plaque psoriasis, adrenal suppression was identified in 1 out of 12 subjects having involvement of 10 to15% of body surface area (BSA) and 2 out of 9 subjects having involvement of >15% of BSA after treatment with Topicort Topical Spray twice a day for 28 days [see Clinical Pharmacology (12.2)].
Because of the potential for systemic absorption, use of topical corticosteroids may require that patients be periodically evaluated for HPA axis suppression. Factors that predispose a patient using a topical corticosteroid to HPA axis suppression include the use of high potency steroids, larger treatment surface areas, prolonged use, use of occlusive dressings, altered skin barrier, liver failure and young age.
An ACTH stimulation test may be helpful in evaluating patients for HPA axis suppression.
If HPA axis suppression is documented, an attempt should be made to gradually withdraw the drug, to reduce the frequency of application, or to substitute a less potent steroid. Manifestations of adrenal insufficiency may require supplemental systemic corticosteroids. Recovery of HPA axis function is generally prompt and complete upon discontinuation of topical corticosteroids.
Cushing's syndrome, hyperglycemia, and unmasking of latent diabetes mellitus can also result from systemic absorption of topical corticosteroids.
Use of more than one corticosteroid-containing product at the same time may increase the total systemic corticosteroid exposure.
Pediatric patients may be more susceptible to systemic toxicity from use of topical corticosteroids. Use in patients under 18 years of age is not recommended due to numerically high rates of HPA axis suppression (the safety and effectiveness of Topicort Topical Spray have not been established in pediatric patients) [see Use in Specific Populations (8.4) and Clinical Pharmacology (12.2)].
5.2 Local Adverse Reactions with Topical Corticosteroids
Local adverse reactions may be more likely to occur with occlusive use, prolonged use or use of higher potency corticosteroids. Reactions may include atrophy, striae, telangiectasias, burning, itching, irritation, dryness, folliculitis, acneiform eruptions, hypopigmentation, perioral dermatitis, allergic contact dermatitis, secondary infection, and miliaria. Some local adverse reactions may be irreversible.
5.3 Ophthalmic Adverse Reactions
Use of topical corticosteroids, including Topicort Topical Spray, may increase the risk of posterior subcapsular cataracts and glaucoma. Cataracts and glaucoma have been reported with the postmarketing use of topical corticosteroid products [see Adverse Reactions (6.2)]. Avoid contact of Topicort Topical Spray with eyes. Topicort Topical Spray may cause eye irritation. Advise patients to report any visual symptoms and consider referral to an ophthalmologist for evaluation.
5.4 Allergic Contact Dermatitis with Topical Corticosteroids
Allergic contact dermatitis to any component of topical corticosteroids is usually diagnosed by a failure to heal rather than a clinical exacerbation. Clinical diagnosis of allergic contact dermatitis can be confirmed by patch testing.
-
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
In randomized, multicenter, prospective vehicle-controlled clinical trials, subjects with moderate to severe plaque psoriasis of the body applied Topicort Topical Spray or vehicle spray twice daily for 4 weeks. A total of 149 subjects applied Topicort Topical Spray.
Adverse reactions that occurred in ≥ 1% of subjects treated with Topicort Topical Spray are presented in Table 1.
Table 1. Number (%) of Subjects with Adverse Reactions Occurring in ≥ 1% Topicort Topical Spray, 0.25% b.i.d.
(N = 149)Vehicle spray b.i.d.
(N = 135)Number of Subjects with Adverse Reactions 13 (8.7%) 18 (13.3%) Application site dryness 4 (2.7%) 7 (5.2%) Application site irritation 4 (2.7%) 5 (3.7%) Application site pruritus 3 (2.0%) 5 (3.7%) Another less common adverse reaction (<1% but >0.1%) was folliculitis.
6.2 Postmarketing Experience
Because adverse reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Postmarketing reports for local adverse reactions to topical corticosteroids included atrophy, striae, telangiectasias, itching, dryness, hypopigmentation, perioral dermatitis, secondary infection, and miliaria.
Ophthalmic adverse reactions of cataracts, glaucoma, and increased intraocular pressure have been reported during use of topical corticosteroids.
-
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
There are no available data on desoximetasone use in pregnant women to evaluate for a drug-associated risk of major birth defects, miscarriage or adverse maternal or fetal outcomes. Observational studies suggest maternal use of high to super-high potency topical steroids, including Topicort Topical Spray, may be associated with an increased risk of low birthweight infants (see Data). Advise pregnant woman that Topicort Topical Spray may increase the potential risk of low birth weight infants and to use Topicort Topical Spray on the smallest area of skin and for the shortest duration possible.
Desoximetasone has been shown to cause malformations and be embryotoxic in mice, rats, and rabbits when given by subcutaneous or dermal routes of administration at doses 3 to 30 times the human dose of Topicort Topical Spray based on a body surface area comparison.
The background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Data
Human Data
Available observational studies in pregnant women did not identify a drug-associated risk of major birth defects, preterm delivery, or fetal mortality with the use of topical corticosteroids of any potency. However, when the dispensed amount of high to super-high potency topical corticosteroids exceeded 300g during the entire pregnancy, maternal use was associated with an increased risk of low birth weight in infants.
8.2 Lactation
Risk Summary
There is no information on the presence of topically administered desoximetasone in human milk, the effects on the breastfed infant, or the effects on milk production. It is not known whether topical administration of corticosteroids could result in sufficient systemic absorption to produce detectable quantities in breast milk. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for Topicort Topical Spray and any potential adverse effects on the breastfed infant from Topicort Topical Spray or from the underlying maternal condition.
Clinical Considerations
To minimize potential exposure to the breastfed infant via breast milk, use Topicort Topical Spray on the smallest area of skin and for the shortest duration possible while breastfeeding. Advise breastfeeding women not to apply Topicort Topical Spray directly to the nipple and areola to avoid direct infant exposure [see Warnings and Precautions (5.1) and Use in Specific Populations (8.4)].
8.4 Pediatric Use
The safety and effectiveness of Topicort Topical Spray have not been established in pediatric patients for the treatment of plaque psoriasis. Topicort Topical Spray is not recommended for use in patients less than 18 years of age due to the high incidence of HPA axis suppression observed [see Warnings and Precautions (5.1)].
Hypothalamic-Pituitary Adrenal (HPA) Axis Suppression
The HPA axis suppression potential of Topicort Topical Spray was assessed in an open-label, sequential cohort, safety trial in 129 subjects 2 years to less than 18 years of age with moderate to severe plaque psoriasis defined as a Physician Global Assessment (PGA) score of ≥3 with involvement of at least 10% of their body surface area (excluding the face and scalp). In total, 100 pediatric subjects were evaluated for HPA axis function via cosyntropin stimulation testing at baseline and following 4 weeks of twice daily application of Topicort Topical Spray. Overall, 36% of pediatric subjects 2 years to less than 18 years of age demonstrated HPA axis suppression defined as a serum cortisol level ≤ 18 mcg/dL 30-minutes post cosyntropin stimulation. The proportion of subjects demonstrating HPA axis suppression was 35.0% in Cohort 1 (12 years to less than 18 years of age) and 43.3% in Cohort 2 (6 years to less than 12 years of age). Trial enrollment in the youngest cohort (2 years to less than 6 years of age) was discontinued early due to high incidence of HPA axis suppression observed in the two oldest cohorts (6 years to less than 18 years of age) [see Clinical Pharmacology (12.2)].
Because of a higher ratio of skin surface area to body mass, pediatric patients are at a greater risk than adults of HPA axis suppression and Cushing's syndrome when they are treated with topical corticosteroids. They are therefore at greater risk of adrenal insufficiency during and/or after withdrawal of treatment. Adverse reactions including striae have been reported with inappropriate use of topical corticosteroids in infants and children.
HPA axis suppression, Cushing's syndrome, linear growth retardation, delayed weight gain, and intracranial hypertension have been reported in children receiving topical corticosteroids. Manifestations of adrenal suppression in children include low plasma cortisol levels and absence of response to ACTH stimulation. Manifestations of intracranial hypertension include bulging fontanelles, headaches, and bilateral papilledema.
8.5 Geriatric Use
Clinical studies of Topicort Topical Spray did not include sufficient numbers of subjects aged 65 years and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
-
10 OVERDOSAGE
Topicort Topical Spray can be absorbed in sufficient amounts to produce systemic effects [see Warnings and Precautions (5.1)].
-
11 DESCRIPTION
Topicort® (desoximetasone) Topical Spray, 0.25% for dermatologic use contains desoximetasone as the active ingredient.
Desoximetasone is a corticosteroid with the chemical name of pregna-1, 4-diene-3, 20-dione, 9-fluoro-11, 21-dihydroxy-16-methyl-, (11β,16α)-.
Desoximetasone has the molecular formula of C22H29FO4 and a molecular weight of 376.47. The CAS Registry Number is 382-67-2.
The structural formula is:
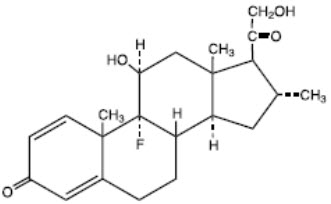
Each gram of Topicort® Topical Spray contains 2.5 mg of desoximetasone in a clear, colorless liquid with the following inactive ingredients: glyceryl oleate, isopropyl alcohol (23.4%), isopropyl myristate, L-menthol, and mineral oil. Topicort® Topical Spray is co-packaged with a manual spray pump for installation by the pharmacist prior to dispensing to patients.
-
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Corticosteroids play a role in cellular signaling, immune function, inflammation and protein regulation; however, the precise mechanism of action in psoriasis is unknown.
12.2 Pharmacodynamics
Vasoconstrictor Assay
Vasoconstrictor studies performed with Topicort Topical Spray in healthy subjects indicate that it is in the high to super-high range of potency as compared with other topical corticosteroids.
Hypothalamic-Pituitary Adrenal (HPA) Axis Suppression
The potential for hypothalamic-pituitary-adrenal (HPA) axis suppression was evaluated in two trials. Topicort Topical Spray was applied twice a day for 28 days and HPA axis suppression was defined as serum cortisol level ≤18 mcg/dL 30-min post cosyntropin stimulation.
In the first trial, out of 24 adult subjects with moderate to severe plaque psoriasis, 21 subjects had evaluable serum cortisol levels. The proportion of subjects demonstrating HPA axis suppression was 8.3% (1 out of 12) in subjects having psoriasis involvement of 10-15% of body surface area (BSA), and 22.2% (2 out of 9) in subjects having psoriasis involvement of > 15% of their BSA. In the 2 subjects with available follow-up values, suppression reversed 28 days after the end of treatment.
In another trial, the HPA axis suppression was evaluated in 106 pediatric subjects with moderate to severe plaque psoriasis. One hundred subjects had evaluable serum cortisol levels. The proportion of subjects demonstrating HPA axis suppression was 35.0% (21 out of 60) in Cohort 1 (12 years to less than 18 years of age, with a mean baseline BSA involvement of 16%), and 43.3% (13 out of 30) in Cohort 2 (6 years to less than 12 years of age, with a mean baseline BSA involvement of 19%). Trial enrollment in the youngest cohort (2 years to less than 6 years of age) was discontinued early due to high incidence of HPA axis suppression observed in the two oldest cohorts (6 years to less than 18 years of age). The overall HPA axis suppression rate was 36% in pediatric subjects 2 years to less than 18 years of age. Due to high incidence of HPA axis suppression observed from this trial, Topicort Topical Spray is not recommended for use in pediatric patients less than 18 years of age [see Use in Specific Populations (8.4)].
12.3 Pharmacokinetics
The extent of percutaneous absorption of topical corticosteroids is determined by many factors including the vehicle, the integrity of the epidermal barrier, and the use of occlusive dressings.
Topical corticosteroids can be absorbed from normal intact skin. Inflammation and/or other disease processes in the skin increase percutaneous absorption. Occlusive dressings substantially increase the percutaneous absorption of topical corticosteroids. Once absorbed through the skin, topical corticosteroids are handled through pharmacokinetic pathways similar to systemically administered corticosteroids. Corticosteroids are bound to plasma proteins in varying degrees. Corticosteroids are metabolized primarily in the liver and are then excreted by the kidneys. Some of the topical corticosteroids and their metabolites are also excreted into the bile.
Plasma concentrations of desoximetasone were measured at two single random time points in the HPA axis suppression trial in 24 adult subjects with psoriasis [see Clinical Pharmacology (12.2)]. The mean (% Coefficient of Variation) concentration of desoximetasone was 449 pg/mL (86%) at Day 14 and 678 pg/mL (135%) at Day 28. The concentration time profile following application of Topicort Topical Spray is not known.
In the pediatric HPA axis suppression trial, plasma concentrations of desoximetasone were measured in a subset of subjects in Cohorts 1 and 2 [see Clinical Pharmacology (12.2)]. High inter subject variability in plasma concentrations was observed in both cohorts. The mean (% Coefficient of Variation) maximum concentration on Day 29 was 1881 pg/mL (127%) in Cohort 1 (n=11) and 1116 pg/mL (94%) in Cohort 2 (n=8).
-
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term animal studies have not been performed to evaluate the carcinogenic potential of Topicort Topical Spray.
In a 13-week repeat-dose toxicity study in rats, topical administration of desoximetasone spray at concentrations of 0.001, 0.005 and 0.02% BID (which corresponds to dose levels of 0.01, 0.05, or 0.2 mg/kg/dose BID, respectively) resulted in a toxicity profile consistent with long-term exposure to corticosteroids, including adrenal atrophy and histopathological changes in several organ systems indicative of severe immune suppression. A no observable adverse effect level (NOAEL) could not be determined in this study. Although the clinical relevance of the findings in animals to humans is not clear, sustained glucocorticoid-related immune suppression may increase the risk of infection and possibly the risk for carcinogenesis.
Desoximetasone revealed no evidence of mutagenic or clastogenic potential based on the results of two in vitro genotoxicity tests (Ames assay and Chinese hamster ovary cell chromosome aberration assay) and one in vivo genotoxicity test (mouse bone marrow micronucleus assay).
No evidence of impairment of male or female fertility was observed at subcutaneous desoximetasone doses up to 0.1 mg/kg/day (0.6 mg/m2/day) in Sprague-Dawley rats.
-
14 CLINICAL STUDIES
Two multi-center, randomized, double-blind, vehicle-controlled clinical trials were conducted in 239 subjects aged 18 years and older with moderate to severe plaque psoriasis of the body. In both trials, randomized subjects applied Topicort Topical Spray or vehicle spray to the affected areas twice daily for 4 weeks. Enrolled subjects had a minimum body surface area of involvement of 10%, and a Physician's Global Assessment score (PGA) of 3 (moderate) or 4 (severe).
Efficacy was assessed at Week 4 as the proportion of subjects who were considered a Clinical Success ("clear" (0) or "almost clear" (1) according to the PGA scale). Table 2 presents the efficacy results.
Table 2. Number of Subjects (%) with Clinical Success (scored as clear or almost clear) at Week 4. Parameter Trial 1 Trial 2 Topicort
N=59Vehicle
N=60Topicort
N=60Vehicle
N=60Clinical Success 18 (30.5%) 3 (5.0%) 32 (53.3%) 11 (18.3%) -
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 How Supplied/Storage
Topicort® (desoximetasone) Topical Spray, 0.25% is a clear colorless liquid supplied in white, opaque bottles with white, opaque screw caps in the following sizes:
- 30 mL (NDC 51672-5281-3)
- 50 mL (NDC 51672-5281-4)
- 100 mL (2- 50mL bottles) (NDC 51672-5281-6)
- 100 mL (NDC 51672-5281-7)
Store at controlled room temperature between 20°C to 25°C (68°F to 77°F), excursions permitted to 15°C to 30°C (59°F to 86°F). [See USP Controlled Room Temperature] Spray is flammable; avoid heat, flame or smoking when using this product.
Each unit is co-packaged with a manual spray pump for installation by the pharmacist.
16.2 Instructions for the Pharmacist
- Remove the spray pump from the wrapper
- Remove and discard the cap from the bottle
- Keeping the bottle vertical, insert the spray pump into the bottle and turn clockwise until well-fastened
- Dispense the bottle with the spray pump inserted
- Label the bottle with "discard the product 30 days after dispensing"
-
17 PATIENT COUNSELING INFORMATION
See FDA-approved patient labeling (Patient Information and Instructions for Use)
Inform patients of the following:
- Use this medication as directed by the physician. Do not use this medication for any disorder other than that for which it was prescribed.
- Topicort Topical Spray is for external use only.
- Avoid contact with eyes and use on the face, axilla or groin.
- To minimize the risk of adverse reactions:
- do not bandage or otherwise cover or wrap the treated skin so as to be occlusive.
- discontinue therapy when control is achieved. If no improvement is seen within 4 weeks, contact the physician.
- do not use other corticosteroid-containing products with Topicort Topical Spray without first consulting with the physician.
- Advise patients that Topicort Topical Spray may require periodic evaluation for HPA axis suppression. Topical corticosteroids may have other endocrine effects [see Warnings and Precautions (5.1)].
- Advise women to use Topicort Topical Spray on the smallest area of skin and for the shortest duration possible while pregnant or breastfeeding. Advise breastfeeding women not to apply Topicort Topical Spray directly to the nipple and areola to avoid direct infant exposure [see Use in Specific Populations (8.1 and 8.2)].
- Report any signs of local or systemic adverse reactions including any visual symptoms to the physician.
- This medication is flammable; avoid heat, flame, or smoking when applying this product.
- Discard this product 30 days after dispensed by pharmacist.
- SPL UNCLASSIFIED SECTION
-
INSTRUCTIONS FOR USE
Instructions for Use
TOPICORT® (Top-i-cort)
(desoximetasone) topical sprayImportant information: Topicort Topical Spray is for use on skin (topical) only. Do not get Topicort Topical Spray near or in your mouth, eyes or vagina. Read the Instructions for Use before you start using Topicort Topical Spray and each time you get a refill. There may be new information. This information does not take the place of talking with your doctor about your medical condition or your treatment.
Parts of Topicort Topical Spray bottle (See Figure A).

How to apply Topicort Topical Spray:
Step 1: Remove the cap from the pump top.
Step 2: Hold the bottle in an upright position while pointing the opening of the pump top in the direction of the affected area. To spray, push down on the pump top. Apply Topicort Topical Spray to the affected area as instructed by your doctor. (See Figure B).
Step 3: Spray only enough Topicort Topical Spray to cover the affected area, for example, the elbow (See Figure C). Rub in Topicort Topical Spray gently to the affected area.
Repeat Steps 2 and 3 to apply Topicort Topical Spray to other affected areas as instructed by your doctor.
Step 4: After applying Topicort Topical Spray, place the cap back onto the pump top (See Figure D).

How should I store Topicort Topical Spray?
- Store Topicort Topical Spray at room temperature between 68˚F to 77˚F (20˚C to 25˚C).
- Throw away (discard) unused Topicort Topical Spray 30 days after it has been opened.
- Topicort Topical Spray is flammable. Keep away from heat, flames or smoke.
Keep Topicort Topical Spray and all medicines out of the reach of children.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Mfd by: Taro Pharmaceuticals Inc., Brampton, Ontario, Canada L6T 1C1
Dist. by: TaroPharma a division of Taro Pharmaceuticals U.S.A., Inc., Hawthorne, NY 10532Topicort® and TaroPharma® are registered trademarks of Taro Pharmaceuticals U.S.A., Inc. and/or its affiliates.
Revised: September 2021
PK-7265-0 110 -
PATIENT PACKAGE INSERT
PATIENT INFORMATION
TOPICORT® (Top-i-cort)
(desoximetasone) topical sprayThis Patient Information has been approved by the U.S. Food and Drug Administration.
Revised: September 2021Important information: Topicort Topical Spray is for use on skin (topical) only. Do not get Topicort Topical Spray near or in your mouth, eyes or vagina. What is Topicort Topical Spray?
Topicort Topical Spray is a prescription corticosteroid medicine used to treat plaque psoriasis of the body in people 18 years of age and older.
It is not known if Topicort Topical Spray is safe and effective in children under 18 years of age. Topicort Topical Spray is not recommended for use in children under 18 years of age.Before you use Topicort Topical Spray, tell your doctor about all of your medical conditions, including if you: - have had irritation or other skin reaction to a steroid medicine in the past.
- have a skin infection. You may need medicine to treat the skin infection before you use Topicort Topical Spray.
- have thinning of the skin (atrophy) at the treatment site
- have adrenal gland problems
- have diabetes
- liver problems
- are pregnant or plan to become pregnant. It is not known if Topicort Topical Spray will harm your unborn baby. Topicort Topical Spray may increase your chance of having a low birthweight baby. If you use Topicort Topical Spray during pregnancy, use Topicort Topical Spray on the smallest area of the skin and for the shortest time needed.
- are breastfeeding or plan to breastfeed. It is not known if Topicort Topical Spray passes into your breast milk. If you use Topicort Topical Spray and breastfeed, use Topicort Topical Spray on the smallest area of the skin and for the shortest time needed. Do not apply Topicort Topical spray directly to the nipple and areola to avoid contact with your baby.
What should I avoid while using Topicort Topical Spray?
Topicort Topical Spray is flammable. Avoid heat, flames or smoking while applying Topicort Topical Spray to your skin.How should I use Topicort Topical Spray?
See the "Instructions for Use" for detailed information about the right way to apply Topicort Topical Spray.- Use Topicort Topical Spray exactly as your doctor tells you to use it.
- Your doctor should tell you how much Topicort Topical Spray to use and where to use it.
- Apply Topicort Topical Spray to the affected skin areas 2 times a day and rub it in gently.
- Do not bandage, cover, or wrap the treated skin area, unless your doctor tells you to.
- Use Topicort Topical Spray for the shortest amount of time needed to treat your plaque psoriasis. Tell your doctor if your skin condition is not getting better after 4 weeks of using Topicort Topical Spray. You should not use Topicort Topical Spray for longer than 4 weeks.
- Do not use Topicort Topical Spray on your face, armpits or groin.
- Do not use Topicort Topical Spray if you have thinning of your skin (atrophy) at the treatment site.
- Wash your hands after applying Topicort Topical Spray.
What are the possible side effects of Topicort Topical Spray?
Topicort Topical Spray may cause serious side effects, including:- Symptoms of a disorder where the adrenal gland does not make enough of certain hormones (adrenal insufficiency) during treatment or after stopping treatment with Topicort Topical Spray. Your doctor may do blood tests to check for adrenal gland problems.
- Cushing's syndrome, a condition that happens when your body is exposed to large amounts of the hormone cortisol. Your doctor may do tests to check for this.
- High blood sugar (hyperglycemia) or diabetes mellitus that has not been diagnosed can happen when treated with Topicort Topical Spray. Your doctor may do tests to check for this.
- Skin reactions at the treated skin site. Tell your doctor if you get any skin reactions or skin infections.
- Eye problems. Using Topicort Topical Spray may increase your chance of getting cataracts and glaucoma. Do not get Topicort Topical Spray in your eyes because it may cause eye irritation. Tell your doctor if you have blurred vision or other vision problems during treatment with Topicort Topical Spray.
These are not all of the possible side effects of Topicort Topical Spray.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088How should I store Topicort Topical Spray? - Store Topicort Topical Spray at room temperature between 68˚F to 77˚F (20˚C to 25˚C).
- Throw away (discard) unused Topicort Topical Spray after 30 days.
General information about the safe and effective use of Topicort Topical Spray.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use Topicort Topical Spray for a condition for which it was not prescribed. Do not give Topicort Topical Spray to other people, even if they have the same symptoms you have. It may harm them. You can ask your pharmacist or doctor for information about Topicort Topical Spray that is written for health professionals.What are the ingredients in Topicort Topical Spray?
Active ingredient: desoximetasone
Inactive ingredients: glyceryl oleate, isopropyl alcohol, isopropyl myristate, L-menthol, and mineral oil
Mfd. by: Taro Pharmaceuticals Inc., Brampton, Ontario, Canada L6T 1C1
Dist. by: TaroPharma a division of Taro Pharmaceuticals U.S.A., Inc., Hawthorne, NY 10532
PK-7265-0 110 - PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
TOPICORT
desoximetasone sprayProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:51672-5281 Route of Administration TOPICAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Desoximetasone (UNII: 4E07GXB7AU) (Desoximetasone - UNII:4E07GXB7AU) Desoximetasone 2.5 mg in 1 mL Inactive Ingredients Ingredient Name Strength glyceryl oleate (UNII: 4PC054V79P) isopropyl alcohol (UNII: ND2M416302) isopropyl myristate (UNII: 0RE8K4LNJS) Levomenthol (UNII: BZ1R15MTK7) mineral oil (UNII: T5L8T28FGP) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:51672-5281-0 1 in 1 CARTON 04/11/2013 1 6 mL in 1 BOTTLE; Type 0: Not a Combination Product 2 NDC:51672-5281-3 1 in 1 CARTON 04/11/2013 2 30 mL in 1 BOTTLE; Type 0: Not a Combination Product 3 NDC:51672-5281-4 1 in 1 CARTON 04/11/2013 3 50 mL in 1 BOTTLE; Type 0: Not a Combination Product 4 NDC:51672-5281-7 1 in 1 CARTON 04/11/2013 4 100 mL in 1 BOTTLE; Type 0: Not a Combination Product 5 NDC:51672-5281-6 2 in 1 CARTON 04/11/2013 5 50 mL in 1 BOTTLE; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA204141 04/11/2013 Labeler - Taro Pharmaceuticals U.S.A., Inc. (145186370) Establishment Name Address ID/FEI Business Operations Taro Pharmaceuticals Inc. 206263295 MANUFACTURE(51672-5281)


