Label: KETEK- telithromycin tablet, film coated
-
Contains inactivated NDC Code(s)
NDC Code(s): 54868-5171-0 - Packager: Physicians Total Care, Inc.
- This is a repackaged label.
- Source NDC Code(s): 0088-2225
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: None
- Marketing Status: New Drug Application
Drug Label Information
Updated May 2, 2012
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Medication Guide: HTML
- Official Label (Printer Friendly)
-
BOXED WARNING
(What is this?)
Ketek is contraindicated in patients with myasthenia gravis. There have been reports of fatal and life-threatening respiratory failure in patients with myasthenia gravis associated with the use of Ketek. (See CONTRAINDICATIONS.)
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
KETEK® tablets contain telithromycin, a semisynthetic antibacterial in the ketolide class for oral administration. Chemically, telithromycin is designated as Erythromycin, 3-de[(2,6-dideoxy-3-C-methyl-3-O-methyl-α-L-ribo-hexopyranosyl)oxy]-11,12-dideoxy-6-O-methyl-3-oxo-12,11-[oxycarbonyl[[4-[4-(3-pyridinyl)-1H-imidazol-1-yl]butyl]imino]]-.
Telithromycin, a ketolide, differs chemically from the macrolide group of antibacterials by the lack of α-L-cladinose at position 3 of the erythronolide A ring, resulting in a 3-keto function. It is further characterized by a C11-12 carbamate substituted by an imidazolyl and pyridyl ring through a butyl chain. Its empirical formula is C43H65N5O10 and its molecular weight is 812.03. Telithromycin is a white to off-white crystalline powder. The following represents the chemical structure of telithromycin.
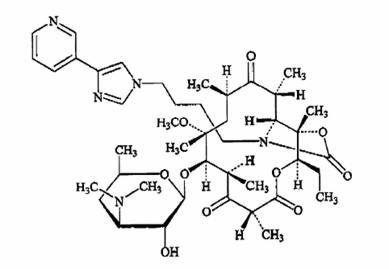
KETEK tablets are available as light-orange, oval, film-coated tablets, each containing 400 mg or 300 mg of telithromycin, and the following inactive ingredients: croscarmellose sodium, hypromellose, magnesium stearate, microcrystalline cellulose, polyethylene glycol, povidone, red ferric oxide, talc, titanium dioxide, and yellow ferric oxide.
-
CLINICAL PHARMACOLOGY
Pharmacokinetics
Absorption
Following oral administration, telithromycin reached maximal concentration at about 1 hour (0.5 – 4 hours).
It has an absolute bioavailability of 57% in both young and elderly subjects.
The rate and extent of absorption are unaffected by food intake, thus KETEK tablets can be given without regard to food.
In healthy adult subjects, peak plasma telithromycin concentrations of approximately 2 µg/mL are attained at a median of 1 hour after an 800-mg oral dose.
Steady-state plasma concentrations are reached within 2 to 3 days of once daily dosing with telithromycin 800 mg.
Following oral dosing, the mean terminal elimination half-life of telithromycin is 10 hours.
The pharmacokinetics of telithromycin after administration of single and multiple (7 days) once daily 800-mg doses to healthy adult subjects are shown in Table 1.
Table 1 Mean (SD) Parameter Single dose (n=18) Multiple dose (n=18) SD=Standard deviation Cmax=Maximum plasma concentration Tmax=Time to Cmax AUC=Area under concentration vs. time curve t1/2=Terminal plasma half-life C24h=Plasma concentration at 24 hours post-dose - *
- Median (min–max) values
Cmax (µg/mL) 1.9 (0.80) 2.27 (0.71) Tmax (h)* 1.0 (0.5–4.0) 1.0 (0.5–3.0) AUC(0–24) (µg∙h/mL) 8.25 (2.6) 12.5 (5.4) Terminal t1/2 (h) 7.16 (1.3) 9.81 (1.9) C24h (µg/mL) 0.03 (0.013) 0.07 (0.051) In a patient population, mean peak and trough plasma concentrations were 2.9 µg/mL (±1.55), (n=219) and 0.2 µg/mL (±0.22), (n=204), respectively, after 3 to 5 days of KETEK 800 mg once daily.
Distribution
Total in vitro protein binding is approximately 60% to 70% and is primarily due to human serum albumin.
Protein binding is not modified in elderly subjects and in patients with hepatic impairment.
The volume of distribution of telithromycin after intravenous infusion is 2.9 L/kg.
Telithromycin concentrations in bronchial mucosa, epithelial lining fluid, and alveolar macrophages after 800 mg once daily dosing for 5 days in patients are displayed in Table 2.
Table 2 Hours
post-doseMean concentration (µg/mL) Tissue/Plasma Ratio Tissue or
fluidPlasma - *
- Units in mg/kg
Bronchial mucosa 2 3.88* 1.86 2.11 12 1.41* 0.23 6.33 24 0.78* 0.08 12.11 Epithelial lining fluid 2 14.89 1.86 8.57 12 3.27 0.23 13.8 24 0.84 0.08 14.41 Alveolar macrophages 2 65 1.07 55 8 100 0.605 180 24 41 0.073 540 Telithromycin concentration in white blood cells exceeds the concentration in plasma and is eliminated more slowly from white blood cells than from plasma. Mean white blood cell concentrations of telithromycin peaked at 72.1 µg/mL at 6 hours, and remained at 14.1 µg/mL 24 hours after 5 days of repeated dosing of 600 mg once daily. After 10 days, repeated dosing of 600 mg once daily, white blood cell concentrations remained at 8.9 µg/mL 48 hours after the last dose.
Metabolism
In total, metabolism accounts for approximately 70% of the dose. In plasma, the main circulating compound after administration of an 800-mg radio-labeled dose was parent compound, representing 56.7% of the total radioactivity. The main metabolite represented 12.6% of the AUC of telithromycin. Three other plasma metabolites were quantified, each representing 3% or less of the AUC of telithromycin.
It is estimated that approximately 50% of its metabolism is mediated by CYP 450 3A4 and the remaining 50% is CYP 450-independent.
Elimination
The systemically available telithromycin is eliminated by multiple pathways as follows: 7% of the dose is excreted unchanged in feces by biliary and/or intestinal secretion; 13% of the dose is excreted unchanged in urine by renal excretion; and 37% of the dose is metabolized by the liver.
Special populations
Gender
There was no significant difference between males and females in mean AUC, Cmax, and elimination half-life in two studies; one in 18 healthy young volunteers (18 to 40 years of age) and the other in 14 healthy elderly volunteers (65 to 92 years of age), given single and multiple once daily doses of 800 mg of KETEK.
Hepatic insufficiency
In a single-dose study (800 mg) in 12 patients and a multiple-dose study (800 mg) in 13 patients with mild to severe hepatic insufficiency (Child Pugh Class A, B and C), the Cmax, AUC and t1/2 of telithromycin were similar to those obtained in age- and sex-matched healthy subjects. In both studies, an increase in renal elimination was observed in hepatically impaired patients indicating that this pathway may compensate for some of the decrease in metabolic clearance. No dosage adjustment is recommended due to hepatic impairment.
Renal insufficiency
In a multiple-dose study, 36 subjects with varying degrees of renal impairment received 400 mg, 600 mg, or 800 mg KETEK once daily for 5 days. There was a 1.4-fold increase in Cmax,ss, and a 1.9-fold increase in AUC (0–24)ss at 800 mg multiple doses in the severely renally impaired group (CLCR < 30 mL/min) compared to healthy volunteers. Renal excretion may serve as a compensatory elimination pathway for telithromycin in situations where metabolic clearance is impaired. Patients with severe renal impairment are prone to conditions that may impair their metabolic clearance. Therefore, in the presence of severe renal impairment (CLCR < 30 mL/min), a reduced dosage of KETEK is recommended. (See DOSAGE AND ADMINISTRATION)
In a single-dose study in patients with end-stage renal failure on hemodialysis (n=10), the mean Cmax and AUC values were similar to normal healthy subjects when KETEK was administered 2 hours post-dialysis. However, the effect of dialysis on removing telithromycin from the body has not been studied.
Multiple insufficiency
The effects of co-administration of ketoconazole in 12 subjects (age ≥ 60 years), with impaired renal function were studied (CLCR= 24 to 80 mL/min). In this study, when severe renal insufficiency (CLCR < 30 mL/min, n=2) and concomitant impairment of CYP 3A4 metabolism pathway were present, telithromycin exposure (AUC (0–24)) was increased by approximately 4- to 5-fold compared with the exposure in healthy subjects with normal renal function receiving telithromycin alone. In the presence of severe renal impairment (CLCR < 30 mL/min), with coexisting hepatic impairment, a reduced dosage of KETEK is recommended. (See PRECAUTIONS, General and DOSAGE AND ADMINISTRATION)
Geriatric
Pharmacokinetic data show that there is an increase of 1.4-fold in exposure (AUC) in 20 patients ≥ 65 years of age with community acquired pneumonia in a Phase III study, and a 2.0-fold increase in exposure (AUC) in 14 subjects ≥ 65 years of age as compared with subjects less than 65 years of age in a Phase I study. No dosage adjustment is required based on age alone.
Drug-drug interactions
In vitro interactions
In vitro studies using a model compound have shown that telithromycin may act as an inhibitor for the hepatic uptake transporters OATP1B1 and OATP1B3. Although the clinical relevance of this finding is unknown, it is possible that concomitant administration of telithromycin with drugs that are substrates of OATP family members could result in increased plasma concentrations of the co-administered drug.
In vivo interactions
Studies were performed to evaluate the effect of CYP 3A4 inhibitors on telithromycin and the effect of telithromycin on drugs that are substrates of CYP 3A4 and CYP 2D6. In addition, drug interaction studies were conducted with several other concomitantly prescribed drugs.
CYP 3A4 inhibitors
Itraconazole
A multiple-dose interaction study with itraconazole showed that Cmax of telithromycin was increased by 22% and AUC by 54%.
CYP 3A4 substrates
Cisapride
Steady-state peak plasma concentrations of cisapride (an agent with the potential to increase QT interval) were increased by 95% when co-administered with repeated doses of telithromycin, resulting in significant increases in QTc. (See CONTRAINDICATIONS)
Simvastatin
When simvastatin was co-administered with telithromycin, there was a 5.3-fold increase in simvastatin Cmax, an 8.9-fold increase in simvastatin AUC, a 15-fold increase in the simvastatin active metabolite Cmax, and a 12-fold increase in the simvastatin active metabolite AUC. (See PRECAUTIONS)
In another study, when simvastatin and telithromycin were administered 12 hours apart, there was a 3.4-fold increase in simvastatin Cmax, a 4.0-fold increase in simvastatin AUC, a 3.2-fold increase in the active metabolite Cmax, and a 4.3-fold increase in the active metabolite AUC. (See PRECAUTIONS)
Midazolam
Concomitant administration of telithromycin with intravenous or oral midazolam resulted in 2- and 6-fold increases, respectively, in the AUC of midazolam due to inhibition of CYP 3A4-dependent metabolism of midazolam. (See PRECAUTIONS)
CYP 2D6 substrates
Paroxetine
There was no pharmacokinetic effect on paroxetine when telithromycin was co-administered.
Metoprolol
When metoprolol was co-administered with telithromycin, there was an increase of approximately 38% on the Cmax and AUC of metoprolol, however, there was no effect on the elimination half-life of metoprolol. Telithromycin exposure is not modified with concomitant single-dose administration of metoprolol. (See PRECAUTIONS, Drug interactions)
Other drug interactions
Digoxin
The plasma peak and trough levels of digoxin were increased by 73% and 21%, respectively, in healthy volunteers when co-administered with telithromycin. However, trough plasma concentrations of digoxin (when equilibrium between plasma and tissue concentrations has been achieved) ranged from 0.74 to 2.17 ng/mL. There were no significant changes in ECG parameters and no signs of digoxin toxicity. (See PRECAUTIONS)
Theophylline
When theophylline was co-administered with repeated doses of telithromycin, there was an increase of approximately 16% and 17% on the steady-state Cmax and AUC of theophylline. Co-administration of theophylline may worsen gastrointestinal side effects such as nausea and vomiting, especially in female patients. It is recommended that telithromycin should be taken with theophylline 1 hour apart to decrease the likelihood of gastrointestinal side effects.
Sotalol
Telithromycin has been shown to decrease the Cmax and AUC of sotalol by 34% and 20%, respectively, due to decreased absorption.
Warfarin
When co-administered with telithromycin in healthy subjects, there were no pharmacodynamic or pharmacokinetic effects on racemic warfarin.
Oral contraceptives
When oral contraceptives containing ethinyl estradiol and levonorgestrel were co-administered with telithromycin, the steady-state AUC of ethinyl estradiol did not change and the steady-state AUC of levonorgestrel was increased by 50%. The pharmacokinetic/pharmacodynamic study showed that telithromycin did not interfere with the antiovulatory effect of oral contraceptives containing ethinyl estradiol and levonorgestrel.
Ranitidine, antacid
There was no clinically relevant pharmacokinetic interaction of ranitidine or antacids containing aluminum and magnesium hydroxide on telithromycin.
Rifampin
During concomitant administration of rifampin and KETEK in repeated doses, Cmax and AUC of telithromycin were decreased by 79%, and 86%, respectively. (See PRECAUTIONS, Drug Interactions)
Microbiology
Telithromycin belongs to the ketolide class of antibacterials and is structurally related to the macrolide family of antibiotics. Telithromycin concentrates in phagocytes where it exhibits activity against intracellular respiratory pathogens. In vitro, telithromycin has been shown to demonstrate concentration-dependent bactericidal activity against isolates of Streptococcus pneumoniae (including multi-drug resistant isolates [MDRSP1]).
- 1
- MDRSP=Multi-drug resistant Streptococcus pneumoniae includes isolates known as PRSP (penicillin-resistant Streptococcus pneumoniae), and are isolates resistant to two or more of the following antimicrobials: penicillin, 2nd generation cephalosporins (e.g., cefuroxime), macrolides, tetracyclines, and trimethoprim/sulfamethoxazole.
Mechanism of action
Telithromycin blocks protein synthesis by binding to domains II and V of 23S rRNA of the 50S ribosomal subunit. By binding at domain II, telithromycin retains activity against gram-positive cocci (e.g., Streptococcus pneumoniae) in the presence of resistance mediated by methylases (erm genes) that alter the domain V binding site of telithromycin. Telithromycin may also inhibit the assembly of nascent ribosomal units.
Mechanism of resistance
Staphylococcus aureus and Streptococcus pyogenes with the constitutive macrolide-lincosamide-streptogramin B (cMLSB) phenotype are resistant to telithromycin.
Mutants of Streptococcus pneumoniae derived in the laboratory by serial passage in subinhibitory concentrations of telithromycin have demonstrated resistance based on L22 riboprotein mutations (telithromycin MICs are elevated but still within the susceptible range), one of two reported mutations affecting the L4 riboprotein, and production of K-peptide. The clinical significance of these laboratory mutants is not known.
Cross resistance
Telithromycin does not induce resistance through methylase gene expression in erythromycin-inducibly resistant bacteria, a function of its 3-keto moiety. Telithromycin has not been shown to induce resistance to itself.
List of Microorganisms
Telithromycin has been shown to be active against most strains of the following microorganisms, both in vitro and in clinical settings as described in the INDICATIONS AND USAGE section.
Aerobic gram-positive microorganisms
Streptococcus pneumoniae (including multi-drug resistant isolates [MDRSP2])
Aerobic gram-negative microorganisms
Haemophilus influenzae
Moraxella catarrhalis
Other microorganisms
Chlamydophila (Chlamydia) pneumoniae
Mycoplasma pneumoniae
The following in vitro data are available, but their clinical significance is unknown.
At least 90% of the following microorganisms exhibit in vitro minimum inhibitory concentrations (MICs) less than or equal to the susceptible breakpoint for telithromycin. However, the safety and efficacy of telithromycin in treating clinical infections due to these microorganisms have not been established in adequate and well-controlled clinical trials.
Aerobic gram-positive microorganisms
Staphylococcus aureus (methicillin and erythromycin susceptible isolates only)
Streptococcus pyogenes (erythromycin susceptible isolates only)
Streptococci (Lancefield groups C and G)
Other microorganisms
Legionella pneumophila
- 2
- MDRSP=Multi-drug resistant Streptococcus pneumoniae includes isolates known as PRSP (penicillin-resistant S. pneumoniae), and are isolates resistant to two or more of the following antimicrobials: penicillin, 2nd generation cephalosporins (e.g., cefuroxime), macrolides, tetracyclines, and trimethoprim/sulfamethoxazole.
Susceptibility Test Methods
When available, the clinical microbiology laboratory should provide cumulative results of in vitro susceptibility test results for antimicrobial drugs used in local hospitals and practice areas to the physician as periodic reports that describe the susceptibility profile of nosocomial and community-acquired pathogens. These reports should aid the physician in selecting the most effective antimicrobial.
Dilution techniques
Quantitative methods are used to determine antimicrobial minimum inhibitory concentrations (MICs). These MICs provide estimates of the susceptibility of bacteria to antibacterial compounds. The MICs should be determined using a standardized procedure. Standardized procedures are based on dilution methods (broth or agar dilution)1,3 or equivalent with standardized inoculum and concentrations of telithromycin powder. The MIC values should be interpreted according to criteria provided in Table 3.
Diffusion techniques
Quantitative methods that require measurement of zone diameters also provide reproducible estimates of the susceptibility of bacteria to antibiotics. One such standardized procedure2,3 requires the use of standardized inoculum concentrations. This procedure uses paper disks impregnated with 15 µg telithromycin to test the susceptibility of microorganisms to telithromycin. Disc diffusion zone sizes should be interpreted according to criteria in Table 3.
Table 3. Susceptibility Test Result Interpretive Criteria for Telithromycin Minimal Inhibitory Concentrations
(µg/mL)Disk Diffusion
(zone diameters in mm)Pathogen S I R S I R Streptococcus
pneumoniae≤ 1 2 ≥ 4 ≥ 19 16–18 ≤ 15 Haemophilus
influenzae≤ 4 8 ≥ 16 ≥ 15 12–14 ≤ 11 A report of "Susceptible" indicates that the antimicrobial is likely to inhibit growth of the pathogen if the antibacterial compound in the blood reaches the concentrations usually achievable. A report of "Intermediate" indicates that the result should be considered equivocal, and, if the microorganism is not fully susceptible to alternative, clinically feasible drugs, the test should be repeated. This category implies possible clinical applicability in body sites where the drug is physiologically concentrated or in situations where high dosage of drug can be used. This category also provides a buffer zone that prevents small uncontrolled technical factors from causing major discrepancies in interpretation. A report of "Resistant" indicates that the antimicrobial is not likely to inhibit growth of the pathogen if the antimicrobial compound in the blood reaches the concentrations usually achievable; other therapy should be selected.
Quality control
Standardized susceptibility test procedures require the use of quality control microorganisms to determine the performance of the test procedures1,2,3. Standard telithromycin powder should provide the MIC ranges for the quality control organisms in Table 4. For the disk diffusion technique, the 15-µg telithromycin disk should provide the zone diameter ranges for the quality control organisms in Table 4.
Table 4. Acceptable Quality Control Ranges for Telithromycin QC Strain Minimum Inhibitory Concentrations
(µg/mL)Disk Diffusion
(Zone diameter in mm)ATCC = American Type Culture Collection Streptococcus pneumoniae
ATCC 496190.004–0.03 27–33 Haemophilus influenzae
ATCC 492471.0–4.0 17–23 INDICATIONS AND USAGE
KETEK tablets are indicated for the treatment of community-acquired pneumonia (of mild to moderate severity) due to Streptococcus pneumoniae, (including multi-drug resistant isolates [MDRSP3]), Haemophilus influenzae, Moraxella catarrhalis, Chlamydophila pneumoniae, or Mycoplasma pneumoniae, for patients 18 years old and above.
To reduce the development of drug-resistant bacteria and maintain the effectiveness of KETEK and other antibacterial drugs, KETEK should be used only to treat infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
- 3
- MDRSP, Multi-drug resistant Streptococcus pneumoniae includes isolates known as PRSP (penicillin-resistant Streptococcus pneumoniae), and are isolates resistant to two or more of the following antibiotics: penicillin, 2nd generation cephalosporins, e.g., cefuroxime, macrolides, tetracyclines and trimethoprim/sulfamethoxazole.
-
CONTRAINDICATIONS
KETEK is contraindicated in patients with myasthenia gravis. Exacerbations of myasthenia gravis have been reported in patients and sometimes occurred within a few hours of the first dose of telithromycin. Reports have included fatal and life-threatening acute respiratory failure with a rapid onset and progression.
KETEK is contraindicated in patients with previous history of hepatitis and/or jaundice associated with the use of KETEK tablets, or any macrolide antibiotic.
KETEK is contraindicated in patients with a history of hypersensitivity to telithromycin and/or any components of KETEK tablets, or any macrolide antibiotic.
Concomitant administration of KETEK with cisapride or pimozide is contraindicated. (See CLINICAL PHARMACOLOGY, Drug-drug Interactions and PRECAUTIONS.)
Concomitant administration of KETEK and colchicine is contraindicated in patients with renal or hepatic impairment. (See WARNINGS, Drug Interactions and PRECAUTIONS, Drug interactions.)
-
WARNINGS
Hepatotoxicity
Acute hepatic failure and severe liver injury, in some cases fatal, have been reported in patients treated with KETEK. These hepatic reactions included fulminant hepatitis and hepatic necrosis leading to liver transplant, and were observed during or immediately after treatment. In some of these cases, liver injury progressed rapidly and occurred after administration of a few doses of KETEK. (See ADVERSE REACTIONS)
Physicians and patients should monitor for the appearance of signs or symptoms of hepatitis, such as fatigue, malaise, anorexia, nausea, jaundice, bilirubinuria, acholic stools, liver tenderness or hepatomegaly. Patients with signs or symptoms of hepatitis must be advised to discontinue KETEK and immediately seek medical evaluation, which should include liver function tests. (See ADVERSE REACTIONS, PRECAUTIONS, Information to Patients.) If clinical hepatitis or transaminase elevations combined with other systemic symptoms occur, KETEK should be permanently discontinued.
Ketek must not be re-administered to patients with a previous history of hepatitis and/or jaundice associated with the use of KETEK tablets, or any macrolide antibiotic. (See CONTRAINDICATIONS)
In addition, less severe hepatic dysfunction associated with increased liver enzymes, hepatitis and in some cases jaundice was reported with the use of KETEK. These events associated with less severe forms of liver toxicity were reversible.
QTc prolongation
Telithromycin has the potential to prolong the QTc interval of the electrocardiogram in some patients. QTc prolongation may lead to an increased risk for ventricular arrhythmias, including torsades de pointes. Thus, telithromycin should be avoided in patients with congenital prolongation of the QTc interval, and in patients with ongoing proarrhythmic conditions such as uncorrected hypokalemia or hypomagnesemia, clinically significant bradycardia, and in patients receiving Class IA (e.g., quinidine and procainamide) or Class III (e.g., dofetilide) antiarrhythmic agents.
Cases of torsades de pointes have been reported post-marketing with KETEK. In clinical trials, no cardiovascular morbidity or mortality attributable to QTc prolongation occurred with telithromycin treatment in 4780 patients in clinical trials, including 204 patients having a prolonged QTc at baseline.
Visual disturbances*
KETEK may cause visual disturbances particularly in slowing the ability to accommodate and the ability to release accommodation. Visual disturbances included blurred vision, difficulty focusing, and diplopia. Most events were mild to moderate; however, severe cases have been reported.
Loss of Consciousness*
There have been post-marketing adverse event reports of transient loss of consciousness including some cases associated with vagal syndrome.
*Because of potential visual difficulties or loss of consciousness, patients should attempt to minimize activities such as driving a motor vehicle, operating heavy machinery or engaging in other hazardous activities during treatment with KETEK. If patients experience visual disorders or loss of consciousness while taking KETEK, patients should not drive a motor vehicle, operate heavy machinery or engage in other hazardous activities.
(See PRECAUTIONS, Information for Patients)Drug Interactions
Serious adverse reactions have been reported in patients taking KETEK concomitantly with CYP 3A4 substrates. These include colchicine toxicity with colchicine; rhabdomyolysis with simvastatin, lovastatin, and atorvastatin; and hypotension with calcium channel blockers metabolized by CYP 3A4 (e.g., verapamil, amlodipine, diltiazem). (See PRECAUTIONS, Drug interactions.)
Life-threatening and fatal drug interactions have been reported in patients treated with colchicine and strong CYP 3A4 inhibitors. Telithromycin is a strong CYP 3A4 inhibitor and this interaction may occur while using both drugs at their recommended doses. If co-administration of telithromycin and colchicine is necessary in patients with normal renal and hepatic function, the dose of colchicine should be reduced. Patients should be monitored for clinical symptoms of colchicine toxicity. Concomitant administration of KETEK and colchicine is contraindicated in patients with renal or hepatic impairment. (See CONTRAINDICATIONS and PRECAUTIONS, Drug interactions.)
Pseudomembranous colitis
Clostridium difficile associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including KETEK, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibiotic use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibiotic use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibiotic treatment of C difficile, and surgical evaluation should be instituted as clinically indicated.
-
PRECAUTIONS
General
Prescribing KETEK in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
Telithromycin is principally excreted via the liver and kidney. Telithromycin may be administered without dosage adjustment in the presence of hepatic impairment. In the presence of severe renal impairment (CLCR < 30 mL/min), a reduced dosage of KETEK is recommended. (See DOSAGE AND ADMINISTRATION)
Information for patients
A Medication Guide is provided to patients when Ketek is dispensed. Patients should be instructed to read the MedGuide when Ketek is received. In addition, the complete text of the MedGuide is reprinted at the end of this document.
The following information and instructions should be communicated to the patient.
- KETEK may cause problems with vision particularly when looking quickly between objects close by and objects far away. These events include blurred vision, difficulty focusing, and objects looking doubled. Most events were mild to moderate; however, severe cases have been reported. Problems with vision were reported as having occurred after any dose during treatment, but most occurred following the first or second dose. These problems lasted several hours and in some patients came back with the next dose. (See WARNINGS and ADVERSE REACTIONS.)
Patients should be advised that avoiding quick changes in viewing between objects in the distance and objects nearby may help to decrease the effects of these visual difficulties.
- Because of potential visual difficulties, loss of consciousness, confusion or hallucinations, patients should attempt to minimize activities such as driving a motor vehicle, operating heavy machinery or engaging in other hazardous activities during treatment with KETEK.
If patients experience visual difficulties, loss of consciousness / fainting, confusion or hallucination
- patients should seek advice from their physician before taking another dose
- patients should not drive a motor vehicle, operate heavy machinery, or engage in otherwise hazardous activities.
Patients should also be advised:
-
Ketek is contraindicated in patients with myasthenia gravis.
(See CONTRAINDICATIONS) - of the possibility of liver injury, associated with KETEK, which in rare cases may be severe. Patients developing signs or symptoms of liver injury should be instructed to discontinue KETEK and seek medical attention immediately. Symptoms of liver injury may include nausea, fatigue, anorexia, jaundice, dark urine, light-colored stools, pruritus, or tender abdomen. Ketek must not be taken by patients with a previous history of hepatitis/jaundice associated with the use of KETEK or macrolide antibiotics.
(See CONTRAINDICATIONS and WARNINGS) - antibacterial drugs including KETEK should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When KETEK is prescribed to treat a bacterial infection, patients should be told that although it is common to feel better early in the course of therapy, the medication should be taken exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by KETEK or other antibacterial drugs in the future.
- KETEK has the potential to produce changes in the electrocardiogram (QTc interval prolongation) and that they should report any fainting occurring during drug treatment.
- KETEK should be avoided in patients receiving Class 1A (e.g., quinidine, procainamide) or Class III (e.g., dofetilide) antiarrhythmic agents.
- to inform their physician of any personal or family history of QTc prolongation or proarrhythmic conditions such as uncorrected hypokalemia, or clinically significant bradycardia.
- diarrhea is a common problem caused by antibiotics which usually ends when the antibiotic is discontinued. Sometimes after starting treatment with antibiotics, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as two or more months after having taken the last dose of the antibiotic. If this occurs, patients should contact their physician as soon as possible.
- simvastatin, lovastatin, or atorvastatin should be avoided in patients receiving KETEK. If KETEK is prescribed, therapy with simvastatin, lovastatin, or atorvastatin should be stopped during the course of treatment. (See CLINICAL PHARMACOLOGY, Drug-drug interactions)
- colchicine should be avoided in patients receiving KETEK. If KETEK is prescribed in patients with normal kidney and liver function, the dose is colchicine should be reduced. Concomitant treatment with KETEK and colchicine is contraindicated in patients with kidney or liver impairment. (See CONTRAINDICATIONS and WARNINGS, Drug interactions.)
- KETEK tablets can be taken with or without food.
- to inform their physician of any other medications taken concurrently with KETEK, including over-the-counter medications and dietary supplements.
Drug interactions
Telithromycin is a strong inhibitor of the cytochrome P450 3A4 system. Co-administration of KETEK tablets and a drug primarily metabolized by the cytochrome P450 3A4 enzyme system may result in increased plasma concentration of the drug co-administered with telithromycin that could increase or prolong both the therapeutic and adverse effects. Therefore, appropriate dosage adjustments may be necessary for the drug co-administered with telithromycin.
The use of KETEK is contraindicated with cisapride. (See CONTRAINDICATIONS and CLINICAL PHARMACOLOGY, Drug-drug interactions)
The use of KETEK is contraindicated with pimozide. Although there are no studies looking at the interaction between KETEK and pimozide, there is a potential risk of increased pimozide plasma levels by inhibition of CYP 3A4 pathways by KETEK as with macrolides. (See CONTRAINDICATIONS)
In a pharmacokinetic study, simvastatin levels were increased due to CYP 3A4 inhibition by telithromycin. (See CLINICAL PHARMACOLOGY, Drug-drug interactions) Similarly, an interaction may occur with lovastatin or atorvastatin but not with statins which are not metabolized by CYP3A4.
High levels of HMG-CoA reductase inhibitors increase the risk of myopathy and rhabdomyolysis. Use of simvastatin, lovastatin, or atorvastatin concomitantly with KETEK should be avoided. If KETEK is prescribed, therapy with simvastatin, lovastatin, or atorvastatin should be suspended during the course of treatment. Patients concomitantly treated with statins should be carefully monitored for signs and symptoms of myopathy and rhabdomyolysis.
Colchicine is a substrate for both CYP 3A4 and the efflux transporter, P-glycoprotein (P-gp), and a significant increase in colchicine plasma concentration is anticipated when co-administered with strong CYP 3A4 inhibitors such as telithromycin. (See CONTRAINDICATIONS and WARNINGS, Drug interactions).
Monitoring of digoxin side effects or serum levels should be considered during concomitant administration of digoxin and KETEK. (See CLINICAL PHARMACOLOGY, Drug-drug interactions.)
Hypotension, bradyarrhythmia and loss of consciousness have been observed in patients receiving concomitant treatment with calcium channel blockers that are substrates of CYP 3A4 (e.g., verapamil, amlodipine, diltiazem).
Patients should be monitored with concomitant administration of midazolam and dosage adjustment of midazolam should be considered if necessary. Precaution should be used with other benzodiazepines, which are metabolized by CYP 3A4 and undergo a high first-pass effect (e.g., triazolam). (See CLINICAL PHARMACOLOGY, Drug-drug interactions.)
Concomitant treatment of KETEK with rifampin, a CYP 3A4 inducer, should be avoided. Concomitant administration of other CYP 3A4 inducers such as phenytoin, carbamazepine, or phenobarbital is likely to result in subtherapeutic levels of telithromycin and loss of effect. (See CLINICAL PHARMACOLOGY, Other drug interactions.)
In patients treated with metoprolol for heart failure, the increased exposure to metoprolol, a CYP 2D6 substrate, may be of clinical importance. Therefore, co-administration of KETEK and metoprolol in patients with heart failure should be considered with caution. (See CLINICAL PHARMACOLOGY, Drug-drug interactions.)
Spontaneous post-marketing reports suggest that administration of KETEK and oral anticoagulants concomitantly may potentiate the effects of the oral anticoagulants. Consideration should be given to monitoring prothrombin times/INR while patients are receiving KETEK and oral anticoagulants simultaneously.
No specific drug interaction studies have been performed to evaluate the following potential drug-drug interactions with KETEK. However, these drug interactions have been observed with macrolide products.
Drugs metabolized by the cytochrome P450 system such as carbamazepine, cyclosporine, tacrolimus, sirolimus, hexobarbital, and phenytoin: elevation of serum levels of these drugs may be observed when co-administered with telithromycin. As a result, increases or prolongation of the therapeutic and/or adverse effects of the concomitant drug may be observed.
Ergot alkaloid derivatives (such as ergotamine or dihydroergotamine): acute ergot toxicity characterized by severe peripheral vasospasm and dysesthesia has been reported when macrolide antibiotics were co-administered. Without further data, the co-administration of KETEK and these drugs is not recommended.
Carcinogenesis, mutagenesis, impairment of fertility
Long-term studies in animals to determine the carcinogenic potential of KETEK have not been conducted.
Telithromycin showed no evidence of genotoxicity in four tests: gene mutation in bacterial cells, gene mutation in mammalian cells, chromosome aberration in human lymphocytes, and the micronucleus test in the mouse.
No evidence of impaired fertility in the rat was observed at doses estimated to be 0.61 times the human daily dose on a mg/m2 basis. At doses of 1.8–3.6 times the human daily dose, at which signs of parental toxicity were observed, moderate reductions in fertility indices were noted in male and female animals treated with telithromycin.
Pregnancy
Teratogenic effects
Pregnancy Category C
Telithromycin was not teratogenic in the rat or rabbit. Reproduction studies have been performed in rats and rabbits, with effect on pre-post natal development studied in the rat. At doses estimated to be 1.8 times (900 mg/m2) and 0.49 times (240 mg/m2) the daily human dose of 800 mg (492 mg/m2) in the rat and rabbit, respectively, no evidence of fetal terata was found. At doses higher than the 900 mg/m2 and 240 mg/m2 in rats and rabbits, respectively, maternal toxicity may have resulted in delayed fetal maturation. No adverse effects on prenatal and postnatal development of rat pups were observed at 1.5 times (750 mg/m2/d) the daily human dose.
There are no adequate and well-controlled studies in pregnant women. Telithromycin should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Nursing mothers
Telithromycin is excreted in breast milk of rats. Telithromycin may also be excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when KETEK is administered to a nursing mother.
Geriatric use
In all Phase III clinical trials (n=4,780), KETEK was administered to 694 patients who were 65 years and older, including 231 patients who were 75 years and older. Efficacy and safety in elderly patients ≥ 65 years were generally similar to that observed in younger patients; however, greater sensitivity of some older individuals cannot be ruled out. No dosage adjustment is required based on age alone. (See CLINICAL PHARMACOLOGY, Special populations, Geriatric and DOSAGE AND ADMINISTRATION.)
-
ADVERSE REACTIONS
In Phase III clinical trials, 4,780 patients (n=2702 in controlled trials) received daily oral doses of KETEK 800 mg once daily for 5 days or 7 to 10 days. Most adverse events were mild to moderate in severity. In the combined Phase III studies, discontinuation due to treatment-emergent adverse events occurred in 4.4% of KETEK-treated patients and 4.3% of combined comparator-treated patients. Most discontinuations in the KETEK group were due to treatment-emergent adverse events in the gastrointestinal body system, primarily diarrhea (0.9% for KETEK vs. 0.7% for comparators), nausea (0.7% for KETEK vs. 0.5% for comparators).
All and possibly related treatment-emergent adverse events (TEAEs) occurring in controlled clinical studies in ≥ 2.0% of all patients are included below:
Table 5 All and Possibly Related Treatment-Emergent Adverse Events Reported in Controlled Phase III Clinical Studies (Percent Incidence) Adverse Event All TEAEs Possibly-Related TEAEs KETEK
n= 2702Comparator*
n= 2139KETEK
n= 2702Comparator*
n= 2139- *
- Includes comparators from all controlled Phase III studies.
Diarrhea 10.8% 8.6% 10.0% 8.0% Nausea 7.9% 4.6% 7.0% 4.1% Headache 5.5% 5.8% 2.0% 2.5% Dizziness (excl. vertigo) 3.7% 2.7% 2.8% 1.5% Vomiting 2.9% 2.2% 2.4% 1.4% Loose Stools 2.3% 1.5% 2.1% 1.4% Dysgeusia 1.6% 3.6% 1.5% 3.6% The following events judged by investigators to be at least possibly drug related were observed infrequently (≥ 0.2% and < 2%), in KETEK-treated patients in the controlled Phase III studies.
Gastrointestinal system: abdominal distension, dyspepsia, gastrointestinal upset, flatulence, constipation, gastroenteritis, gastritis, anorexia, oral candidiasis, glossitis, stomatitis, watery stools.
Liver and biliary system: abnormal liver function tests: increased transaminases, increased liver enzymes (e.g., ALT, AST) were usually asymptomatic and reversible. ALT elevations above 3 times the upper limit of normal were observed in 1.6%, and 1.7% of patients treated with KETEK and comparators, respectively. Hepatitis, with or without jaundice, occurred in 0.07% of patients treated with KETEK, and was reversible. (See PRECAUTIONS, General.)
Nervous system: dry mouth, somnolence, insomnia, vertigo, increased sweating
Body as a whole: abdominal pain, upper abdominal pain, fatigue
Special senses: Visual adverse events most often included blurred vision, diplopia, or difficulty focusing. Most events were mild to moderate; however, severe cases have been reported. Some patients discontinued therapy due to these adverse events. Visual adverse events were reported as having occurred after any dose during treatment, but most visual adverse events (65%) occurred following the first or second dose. Visual events lasted several hours and recurred upon subsequent dosing in some patients. For patients who continued treatment, some resolved on therapy while others continued to have symptoms until they completed the full course of treatment. (See WARNINGS and PRECAUTIONS, Information for patients.)
Females and patients under 40 years old experienced a higher incidence of telithromycin-associated visual adverse events. (See CLINICAL STUDIES.)
Urogenital system: vaginal candidiasis, vaginitis, vaginosis fungal
Skin: rash
Hematologic: increased platelet count
Other possibly related clinically-relevant events occurring in <0.2% of patients treated with KETEK from the controlled Phase III studies included: anxiety, bradycardia, eczema, elevated blood bilirubin, erythema multiforme, flushing, hypotension, increased blood alkaline phosphatase, increased eosinophil count, paresthesia, pruritus, urticaria.
Post-Marketing Adverse Event Reports
In addition to adverse events reported from clinical trials, the following events have been reported from worldwide post-marketing experience with KETEK.
Allergic: face edema, rare reports of severe allergic (hypersensitivity) reactions, including angioedema and anaphylaxis
Cardiovascular: atrial arrhythmias, palpitations
Gastrointestinal system: pancreatitis
Liver and biliary system: Hepatic dysfunction has been reported.
Severe and in some cases fatal hepatotoxicity, including fulminant hepatitis, hepatic necrosis and hepatic failure have been reported in patients treated with KETEK. These hepatic reactions were observed during or immediately after treatment. In some of these cases, liver injury progressed rapidly and occurred after administration of only a few doses of KETEK. (See CONTRAINDICATIONS and WARNINGS.) Severe reactions, in some but not all cases, have been associated with serious underlying diseases or concomitant medications.
Data from post-marketing reports and clinical trials show that most cases of hepatic dysfunction were mild to moderate. (See PRECAUTIONS, General.)
Musculoskeletal: muscle cramps, rare reports of exacerbation of myasthenia gravis. (See CONTRAINDICATIONS.) arthralgia, myalgia
Nervous system: loss of consciousness, in some cases associated with vagal syndrome.
Psychiatric disorders: confusion, hallucinations (mostly visual)
Special senses: taste/smell perversion and/or loss
-
OVERDOSAGE
In the event of acute overdosage, the stomach should be emptied by gastric lavage. The patient should be carefully monitored (e.g., ECG, electrolytes) and given symptomatic and supportive treatment. Adequate hydration should be maintained. The effectiveness of hemodialysis in an overdose situation with KETEK is unknown.
-
DOSAGE AND ADMINISTRATION
The dose of KETEK tablets is 800 mg (2 tablets of 400 mg) taken orally once every 24 hours, for 7–10 days. KETEK tablets can be administered with or without food.
KETEK may be administered without dosage adjustment in the presence of hepatic impairment.
In the presence of severe renal impairment (CLCR < 30 mL/min), including patients who need dialysis, the dose should be reduced to KETEK 600 mg once daily. In patients undergoing hemodialysis, KETEK should be given after the dialysis session on dialysis days. (See CLINICAL PHARMACOLOGY, Renal insufficiency.)
In the presence of severe renal impairment (CLCR < 30 mL/min), with coexisting hepatic impairment, the dose should be reduced to KETEK 400 mg once daily. (See CLINICAL PHARMACOLOGY, Multiple insufficiency.)
-
HOW SUPPLIED
KETEK® 400 mg tablets are supplied as light-orange, oval, film-coated tablets, imprinted "H3647" on one side and "400" on the other side. These are packaged in bottles or blister cards (Ketek Pak™ and unit dose) as follows:
Ketek Pak™, 10-tablet cards (2 tablets per blister cavity) (NDC 54868-5171-0)
-
CLINICAL STUDIES
Community-acquired pneumonia (CAP)
KETEK was studied in four randomized, double-blind, controlled studies and four open-label studies for the treatment of community-acquired pneumonia. Patients with mild to moderate CAP who were considered appropriate for oral outpatient treatment were enrolled in these trials. Patients with severe pneumonia were excluded based on any one of the following: ICU admission, need for parenteral antibiotics, respiratory rate > 30/minute, hypotension, altered mental status, < 90% oxygen saturation by pulse oximetry, or white blood cell count < 4000/mm3. Total number of clinically evaluable patients in the telithromycin group included 2016 patients.
Table 6. CAP: Clinical cure rate at post-therapy follow-up (17–24 days) Patients (n) Clinical cure rate Controlled Studies KETEK Comparator KETEK Comparator - *
- This study was stopped prematurely after trovafloxacin was restricted for use in hospitalized patients with severe infection.
KETEK vs. clarithromycin 500 mg BID for 10 days 162 156 88.3% 88.5% KETEK vs. trovafloxacin* 200 mg QD for 7 to 10 days 80 86 90.0% 94.2% KETEK vs. amoxicillin 1000 mg TID for 10 days 149 152 94.6% 90.1% KETEK for 7 days vs. clarithromycin 500 mg BID for 10 days 161 146 88.8% 91.8% Clinical cure rates by pathogen from the four CAP controlled clinical trials in microbiologically evaluable patients given KETEK for 7–10 days or a comparator are displayed in Table 7.
Table 7. CAP: Clinical cure rate by pathogen at post-therapy follow-up (17–24 days) Pathogen KETEK Comparator Streptococcus pneumoniae 73/78 (93.6%) 63/70 (90.0%) Haemophilus influenzae 39/47 (83.0%) 42/44 (95.5%) Moraxella catarrhalis 12/14 (85.7%) 7/9 (77.8%) Chlamydophila (Chlamydia) pneumoniae 23/25 (92.0%) 18/19 (94.7%) Mycoplasma pneumoniae 22/23 (95.7%) 20/22 (90.9%) Clinical cure rates for patients with CAP due to Streptococcus pneumoniae were determined from patients in controlled and uncontrolled trials. Of 333 evaluable patients with CAP due to Streptococcus pneumoniae, 312 (93.7%) achieved clinical success. Only patients considered appropriate for oral outpatient therapy were included in these trials. More severely ill patients were not enrolled. Blood cultures were obtained in all patients participating in the clinical trials of mild to moderate community-acquired pneumonia. In a limited number of outpatients with incidental pneumococcal bacteremia treated with KETEK, a clinical cure rate of 88% (67/76) has been observed. KETEK is not indicated for the treatment of severe community-acquired pneumonia or suspected pneumococcal bacteremia.
Clinical cure rates for patients with CAP due to multi-drug resistant Streptococcus pneumoniae (MDRSP*) were determined from patients in controlled and uncontrolled trials. Of 36 evaluable patients with CAP due to MDRSP, 33 (91.7%) achieved clinical success.
*MDRSP: Multi-drug resistant Streptococcus pneumoniae includes isolates known as PRSP (penicillin-resistant Streptococcus pneumoniae), and are isolates resistant to two or more of the following antibiotics: penicillin, 2nd generation cephalosporins, e.g., cefuroxime, macrolides, tetracyclines and trimethoprim/sulfamethoxazole.
Table 8. Clinical cure rate for 36 evaluable patients with MDRSP treated with KETEK in studies of community-acquired pneumonia Screening Susceptibility Clinical Success in Evaluable MDRSP Patients n/N* % Penicillin-resistant 20/23 86.9 2nd generation cephalosporin-resistant 20/22 90.9 Macrolide-resistant 25/28 89.3 Trimethoprim/sulfamethoxazole-resistant 24/27 88.9 Tetracycline-resistant† 11/13 84.6 Visual Adverse Events
Table 9 provides the incidence of all treatment-emergent visual adverse events in controlled Phase III studies by age and gender. The group with the highest incidence was females under the age of 40, while males over the age of 40 had rates of visual adverse events similar to comparator-treated patients.
Table 9. Incidence of All Treatment-Emergent Visual Adverse Events in Controlled Phase III Studies Gender/Age Telithromycin Comparators* - *
- Includes all comparators combined
Female
≤ 402.1%
(14/682)0.0%
(0/534)Female
> 401.0%
(7/703)0.35%
(2/574)Male
≤ 401.2%
(7/563)0.48%
(2/417)Male
> 400.27%
(2/754)0.33%
(2/614)Total 1.1%
(30/2702)0.28%
(6/2139) -
ANIMAL PHARMACOLOGY
Repeated dose toxicity studies of 1, 3, and 6 months' duration with telithromycin conducted in rat, dog and monkey showed that the liver was the principal target for toxicity with elevations of liver enzymes and histological evidence of damage. There was evidence of reversibility after cessation of treatment. Plasma exposures based on free fraction of drug at the no observed adverse effect levels ranged from 1 to 10 times the expected clinical exposure.
Phospholipidosis (intracellular phospholipid accumulation) affecting a number of organs and tissues (e.g., liver, kidney, lung, thymus, spleen, gall bladder, mesenteric lymph nodes, GI-tract) has been observed with the administration of telithromycin in rats at repeated doses of 900 mg/m2/day (1.8× the human dose) or more for 1 month, and 300 mg/m2/day (0.61× the human dose) or more for 3–6 months. Similarly, phospholipidosis has been observed in dogs with telithromycin at repeated doses of 3000 mg/m2/day (6.1× the human dose) or more for 1 month and 1000 mg/m2/day (2.0× the human dose) or more for 3 months. The significance of these findings for humans is unknown.
Pharmacology/toxicology studies showed an effect both in prolonging QTc interval in dogs in vivo and in vitro action potential duration (APD) in rabbit Purkinje fibers. These effects were observed at concentrations of free drug at least 8.8 (in dogs) times those circulating in clinical use. In vitro electrophysiological studies (hERG assays) suggested an inhibition of the rapid activating component of the delayed rectifier potassium current (IKr) as an underlying mechanism.
- SPL UNCLASSIFIED SECTION
-
REFERENCES
- National Committee for Clinical Laboratory Standards. Methods for Dilution Antimicrobial Susceptibility Tests for Bacteria That Grow Aerobically – Sixth Edition; Approved Standard, NCCLS Document M7-A6, Vol. 23, No. 2, NCCLS, Wayne, PA, January, 2003.
- National Committee for Clinical Laboratory Standards. Performance Standards for Antimicrobial Disk Susceptibility Tests - Eighth Edition; Approved Standard, NCCLS Document M2-A8, Vol. 23, No. 1, NCCLS, Wayne, PA, January, 2003.
- National Committee for Clinical Laboratory Standards. Performance Standards for Antimicrobial Susceptibility Testing: Twelfth Informational Supplement; Approved Standard, NCCLS Document M2-A8 and M7-A6, Vol. 23, No. 1, NCCLS, Wayne, PA, January, 2004.
-
Medication Guide
KETEK® (KEE tek)
(telithromycin)
TabletsRead the Medication Guide that comes with KETEK before you start taking it and each time you get a new prescription. There may be new information. Talk to your doctor if you have any questions about KETEK. This Medication Guide does not take the place of talking with your doctor about your medical condition or treatment.
What is the most important information I should know about KETEK?
Do not take KETEK if you have myasthenia gravis (a rare disease which causes muscle weakness). Worsening of myasthenia gravis symptoms including life-threatening breathing problems have happened in people with myasthenia gravis after taking KETEK, in some cases leading to death.
KETEK can cause other serious side effects, including:
- 1.
- Severe liver damage (hepatotoxicity). Severe liver damage, in some cases leading to a liver transplant or death has happened in people treated with KETEK. Severe liver damage has happened during treatment, even after a few doses, or right after treatment with KETEK has ended.
Stop taking KETEK and call your doctor right away if you have signs of liver problems. Do not take another dose of KETEK unless your doctor tells you to.
Signs of liver problems include:
- increased tiredness
- loss of appetite
- nausea
- yellowing of your skin or whites of your eyes
- dark colored urine (tea colored)
- light colored stools
- right upper belly pain
- itchy skin
Do not take KETEK if you have ever had liver problems while taking KETEK or macrolide antibiotics. Macrolide antibiotics include:
- erythromycin
- azithromycin (Zithromax®, Zmax®)
- clarithromycin (Biaxin®)
- dirithromycin (Dynabac®)
- 2.
- Vision problems. KETEK may cause you to have blurred vision, trouble focusing your eyes, and double vision. You may especially notice vision problems if you look quickly between objects close to you and objects far away from you.
- 3.
- Fainting. KETEK may cause you to faint, especially if you also have nausea, vomiting, and lightheadedness.
Do not drive, operate heavy machinery, or do other dangerous activities while taking KETEK if you have:
- vision problems
- fainting
- confusion
- seeing things that are not there (visual hallucinations)
Stop taking KETEK and call your doctor right away if you have any of these symptoms. Do not take another dose of KETEK unless your doctor tells you to.
4. Low blood pressure, slow heart rate, and fainting. Ketek may cause you to have low blood pressure, a slow heart rate, and fainting when you also take certain medicines called calcium channel blockers. Calcium channel blockers include:
- verapamil (Calan®)
- amlodipine (Norvasc®)
- diltiazem (Cardizem®)
- or other medications containing these products.
See "What are the possible side effects of KETEK?"
What is KETEK?
KETEK is an antibiotic. KETEK is used to treat adults 18 years of age and older with a lung infection called "community acquired pneumonia" that is caused by certain germs called bacteria.
- KETEK is not for other types of infections.
- KETEK does not kill viruses like the common cold.
Who should not take KETEK?
Do not take KETEK if you:
- have myasthenia gravis
- have had liver problems while taking KETEK or macrolide antibiotics.
- have ever had an allergic reaction to telithromycin in KETEK or macrolide antibiotics.
- take cisapride (Propulsid®) or pimozide (Orap®).
- take colchicine (Colcrys®) and have kidney or liver problems.
Talk to your doctor before taking KETEK if you have any of the conditions listed above.
What should I tell my doctor before taking KETEK?
Before taking KETEK, tell your doctor if you:
- have liver problems
- have a heart problem called "QTc prolongation" or have a family history of QTc prolongation
- have other heart problems
- are pregnant or plan to become pregnant. It is not known if KETEK will harm your unborn baby. Talk to your doctor if you are pregnant or plan to become pregnant.
- are breast-feeding or plan to breast-feed. It is not known if KETEK passes into your breast milk. Talk to your doctor about the best way to feed your baby if you take KETEK.
Tell your doctor about all of the medicines you take, including prescription and nonprescription medicines, vitamins, and herbal supplements. KETEK and other medicines may affect or interact with each other, sometimes causing serious side effects.
Especially tell your doctor if you take:
- colchicine (Colcrys®) while you take KETEK
- certain medicines called calcium channel blockers, such as: verapamil (Calan®), amlodipine (Norvasc®), diltiazem (Cardizem®), or other medications containing these products while you take KETEK
- cholesterol lowering medicines; you should not take these cholesterol lowering medicines while taking KETEK:
- simvastatin (Zocor®, Vytorin®)
- lovastatin (Mevacor®)
- atorvastatin (Lipitor®)
Ask your doctor if you are not sure if the medicine you take is included in the list of medicines above.
Know the medicines you take. Keep a list of your medicines with you to show your doctor or pharmacist.
Do not take other medicines with KETEK without first checking with your doctor. Your doctor will tell you if you can take other medicines while taking KETEK.
How should I take KETEK?
- Take KETEK exactly as your doctor tells you.
- Skipping doses or not taking all of an antibiotic may:
- make the treatment not work as well
- increase the chance that the bacteria will develop resistance to the antibiotic
- If you have kidney disease, your doctor may prescribe a lower dose for you.
- Take KETEK with or without food.
- Swallow KETEK tablets whole.
- If you take too much KETEK, call your doctor, or go to the nearest hospital emergency room right away.
What are the possible side effects of KETEK?
See "What is the most important information I should know about KETEK?"
KETEK may cause serious side effects, including:
- Pseudomembranous colitis (an intestine infection). Pseudomembranous colitis can happen with most antibiotics, including KETEK. Call your doctor if you get watery diarrhea, diarrhea that does not go away, or bloody stools. You may also have stomach cramps and a fever. Pseudomembranous colitis can happen up to 2 months after you have finished your antibiotic.
The most common side effects of KETEK are:
- nausea
- headache
- dizziness
- vomiting
- diarrhea
- problems with taste
Tell your doctor if you have any side effect that bothers you or that does not go away.
These are not all of the possible side effects of KETEK. For more information ask your doctor or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
You may also report side effects to sanofi-aventis U.S. at 1-800-633-1610.
How should I store KETEK?
- Store KETEK tablets at room temperature, between 59°F to 86°F (15°C to 30°C).
- Keep KETEK and all medicines out of the reach of children.
General Information about KETEK
- Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use KETEK for a condition for which it was not prescribed. Do not share KETEK with other people, even if they have the same symptoms that you have. It may harm them.
This Medication Guide summarizes the most important information about KETEK. If you would like more information, talk with your doctor. You can ask your doctor or pharmacist for information about KETEK that was written for healthcare professionals. This information is also available on the KETEK website at www.KETEK.com or call 1-800-446-6267.
What are the ingredients in KETEK?
Active Ingredient: telithromycin
Inactive Ingredients: croscarmellose sodium, hypromellose, magnesium stearate, microcrystalline cellulose, polyethylene glycol, povidone, red ferric oxide, talc, titanium dioxide, and yellow ferric oxide
Revised December 2010
This Medication Guide has been approved by the U.S. Food and Drug Administration.
sanofi-aventis U.S. LLC
Bridgewater, NJ 08807© 2010 sanofi-aventis U.S. LLC
BIAXIN® (clarithromycin) is a registered trademark of Abbott Laboratories.
ZITHROMAX® (azithromycin) is a registered trademark of Pfizer Inc.
DYNABAC® (dirithromycin) is a registered trademark of Eli Lilly and Company.
PROPULSID® (cisapride) is a registered trademark of Johnson & Johnson.
ORAP® (pimozide) is a registered trademark of Teva Pharmaceuticals USA, Inc.
LIPITOR® (atorvastatin) is a registered trademark of Pfizer Inc.
ZOCOR® (simvastatin) is a registered trademark of Merck & Co Inc.
VYTORIN® (simvastatin and ezetimibe) is a registered trademark of Merck/Schering Plough Pharmaceuticals.
MEVACOR® (lovastatin) is a registered trademark of Merck & Co Inc. - PRINCIPAL DISPLAY PANEL - 400 mg Tablets
-
INGREDIENTS AND APPEARANCE
KETEK
telithromycin tablet, film coatedProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:54868-5171(NDC:0088-2225) Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength telithromycin (UNII: KI8H7H19WL) (telithromycin - UNII:KI8H7H19WL) telithromycin 400 mg Inactive Ingredients Ingredient Name Strength croscarmellose sodium (UNII: M28OL1HH48) hypromelloses (UNII: 3NXW29V3WO) magnesium stearate (UNII: 70097M6I30) cellulose, microcrystalline (UNII: OP1R32D61U) polyethylene glycol (UNII: 3WJQ0SDW1A) povidone (UNII: FZ989GH94E) ferric oxide red (UNII: 1K09F3G675) talc (UNII: 7SEV7J4R1U) titanium dioxide (UNII: 15FIX9V2JP) ferric oxide yellow (UNII: EX438O2MRT) Product Characteristics Color ORANGE Score no score Shape OVAL Size 13mm Flavor Imprint Code H3647;400 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:54868-5171-0 1 in 1 BOX 1 10 in 1 BLISTER PACK Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA021144 10/27/2004 Labeler - Physicians Total Care, Inc. (194123980) Establishment Name Address ID/FEI Business Operations Physicians Total Care, Inc. 194123980 relabel


