Label: methadone- methadone hydrochloride injection, solution
-
Contains inactivated NDC Code(s)
NDC Code(s): 66479-530-02 - Packager: Xanodyne Pharmaceuticals Inc.
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: CII
Drug Label Information
Updated October 6, 2007
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
- N/A - Section Title Not Found In Database
- SPL UNCLASSIFIED SECTION
-
BOXED WARNING
(What is this?)
CONDITIONS FOR DISTRIBUTION AND USE OF METHADONE PRODUCTS
FOR THE TREATMENT OF OPIOID ADDICTIONCode of Federal Regulations, Title 42, Sec 8
METHADONE PRODUCTS WHEN USED FOR THE TREATMENT OF OPIOID ADDICTION IN DETOXIFICATION OR MAINTENANCE PROGRAMS, SHALL BE DISPENSED ONLY BY OPIOID TREATMENT PROGRAMS (AND AGENCIES, PRACTITIONERS OR INSTITUTIONS BY FORMAL AGREEMENT WITH THE PROGRAM SPONSOR) CERTIFIED BY THE SUBSTANCE ABUSE AND MENTAL HEALTH SERVICES ADMINISTRATION AND APPROVED BY THE DESIGNATED STATE AUTHORITY. CERTIFIED TREATMENT PROGRAMS SHALL DISPENSE AND USE METHADONE IN ORAL FORM ONLY AND ACCORDING TO THE TREATMENT REQUIREMENTS STIPULATED IN THE FEDERAL OPIOID TREATMENT STANDARDS (42 CFR 8.12). See below for important regulatory exceptions to the general requirement for certification to provide opioid agonist treatment.
FAILURE TO ABIDE BY THE REQUIREMENTS IN THESE REGULATIONS MAY RESULT IN CRIMINAL PROSECUTION, SEIZURE OF THE DRUG SUPPLY, REVOCATION OF THE PROGRAM APPROVAL, AND INJUNCTION PRECLUDING OPERATION OF THE PROGRAM.
-
SPL UNCLASSIFIED SECTION
Regulatory Exceptions To The General Requirement For Certification To Provide Opioid Agonist Treatment:
- During inpatient care, when the patient was admitted for any condition other than concurrent opioid addiction (pursuant to 21CFR 1306.07(c)), to facilitate the treatment of the primary admitting diagnosis). For patients unable to take oral medication, parenteral methadone may be used.
- During an emergency period of no longer than 3 days while definitive care for the addiction is being sought in an appropriately licensed facility (pursuant to 21CFR 1306.07(b)).
-
DESCRIPTION
Methadone Hydrochloride Injection, USP, 10 mg/mL is an opioid analgesic.
Each milliliter of Methadone Hydrochloride Injection contains 10 mg (0.029 mmol) of methadone hydrochloride, equivalent to 8.95 mg of methadone free base.
Methadone hydrochloride is a white, crystalline material that is water-soluble.
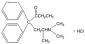
Methadone hydrochloride is chemically described as 6-(dimethylamino)-4,4-diphenyl-3-hepatanone hydrochloride. Its molecular formula is C21H27NO•HCl and it has a molecular weight of 345.91. Methadone hydrochloride has a melting point of 235° C, and a pKa of 8.25 in water at 20°C. Its octanol/water partition coefficient at pH 7.4 is 117. A solution (1:100) in water has a pH between 4.5 and 6.5.
It has the following structural formula:
Methadone Hydrochloride Injection is a sterile injectable solution containing the following inactive ingredients: chlorobutanol, 0.5%, as a preservative, and sodium chloride. The pH of the sterile injectable solution may have been adjusted during manufacturing with sodium hydroxide and/or hydrochloric acid.
-
CLINICAL PHARMACOLOGY
Mechanism of Action
Methadone hydrochloride is a μ agonist; a synthetic opioid analgesic with multiple actions qualitatively similar to those of morphine, the most prominent of which involve the central nervous system and organs composed of smooth muscle. The principal therapeutic uses for methadone are for analgesia and for detoxification or maintenance in opioid addiction. The methadone abstinence syndrome, although qualitatively similar to that of morphine, differs in that the onset is slower, the course is more prolonged, and the symptoms are less severe. Some data also indicate that methadone acts as an antagonist at the N-methyl-D-aspartate (NMDA) receptor. The contribution of NMDA receptor antagonism to methadone's efficacy is unknown. Other NMDA receptor antagonists have been shown to produce neurotoxic effects in animals.
Pharmacokinetics
Absorption:
Methadone Hydrochloride Injection is intended for parenteral (intravenous, subcutaneous and intramuscular) administration. Methadone pharmacokinetics following subcutaneous and intramuscular administration have not been systematically studied and differences among the various parenteral routes have not been well characterized. As with many drugs, absorption into the systemic circulation may vary with subcutaneous and intramuscular administration.
Distribution:
Methadone is a lipophilic drug and the steady state volume of distribution ranges between 2 -6 L/kg. In plasma, methadone is predominantly bound to α1-acid glycoprotein (85% - 90%). Methadone is secreted in saliva, breast milk, amniotic fluid and umbilical cord plasma.
Metabolism:
Methadone is primarily metabolized by N-demethylation to an inactive metabolite, 2-ethylidene-1,5-dimethyl-3,3-diphenylpyrrolidene (EDDP). Cytochrome P450 enzymes, primarily CYP3A4 and to a lesser extent CYP2D6, are responsible for conversion of methadone to EDDP and other inactive metabolites, which are excreted mainly in urine.
Excretion:
Elimination of methadone is mediated by extensive biotransformation, followed by renal and fecal excretion. After single intravenous dose administration the plasma clearance of methadone ranged between 3-10 L/h and the terminal half-life (t½) ranged between 8 - 59 hours. Methadone has been known to persist in the liver and other tissues. Slow release from the liver and other tissues may prolong the duration of methadone action despite low plasma concentrations.
Pharmacokinetics in Special Populations:
Pregnancy
There are no pharmacokinetic studies of parenteral methadone in pregnancy. The disposition of oral methadone has been studied in approximately 30 pregnant patients in 2nd and 3rd trimesters. Elimination of methadone was significantly changed in pregnancy. Total body clearance of methadone was increased in pregnant patients compared to the same patients postpartum or to non-pregnant opioid-dependent women. The terminal half-life of methadone is decreased during second and third trimesters. The decrease in plasma half-life and increased clearance of methadone resulting in lower methadone trough levels during pregnancy can lead to withdrawal symptoms in some pregnant patients. The dosage may need to be increased or the dosing interval decreased in pregnant patients receiving methadone (See DOSAGE AND ADMINISTRATION).
Renal Impairment
Methadone pharmacokinetics have not been extensively evaluated in patients with renal insufficiency. Unchanged methadone and its metabolites are excreted in urine to a variable degree. Methadone is a basic (pKa=9.2) compound and the luminal pH of the urinary tract can affect its extraction from plasma. Urine acidification has been shown to increase renal elimination of methadone. Forced diuresis, peritoneal dialysis, hemodialysis, or charcoal hemoperfusion have not been established as beneficial for increasing methadone or metabolite elimination.
Drug Interactions
(see PRECAUTIONS, Drug Interactions)
Methadone undergoes hepatic N-demethylation by cytochrome P-450 isoforms, principally CYP3A4, and to a lesser extent CYP2D6. Coadministration of methadone with inducers of these enzymes may result in more rapid methadone metabolism and potentially, decreased effects of methadone. Conversely, administration with CYP3A4 or CYP2D6 inhibitors may reduce metabolism and potentiate methadone's effects. Therefore, drugs administered concomitantly with methadone should be evaluated for interaction potential (see Drug Interactions)
-
INDICATIONS AND USAGE
- For the treatment of moderate to severe pain not responsive to non-narcotic analgesics.
- For use in temporary treatment of opioid dependence in patients unable to take oral medication.
Outpatient maintenance and outpatient detoxification treatment may be provided only by opioid treatment programs (OTPs) certified by the Federal Substance Abuse and Mental Health Services Administration (SAMHSA) and registered by the Drug Enforcement Administration (DEA). This does not preclude the maintenance treatment of a patient with concurrent opioid addiction who is hospitalized for conditions other than opioid addiction and who requires temporary maintenance during the critical period of hospitalization, or of a patient whose enrollment has been verified in a program which has been certified for maintenance treatment with methadone.
-
CONTRAINDICATIONS
Methadone Hydrochloride Injection is contraindicated in patients with a known hypersensitivity to methadone hydrochloride or any other ingredient in Methadone Hydrochloride Injection. Methadone Hydrochloride Injection is contraindicated in any situation where opioids are contraindicated such as: patients with respiratory depression (in the absence of resuscitative equipment or in unmonitored settings), and in patients with acute bronchial asthma or hypercarbia.
-
WARNINGS
Cardiac Conduction Effects
Laboratory studies, both in vivo and in vitro, have demonstrated that methadone inhibits cardiac potassium channels and prolongs the QT interval. Cases of QT interval prolongation and serious arrhythmia (torsades de pointes) have been observed during treatment with methadone. These cases appear to be more commonly associated with, but not limited to, higher dose treatment (> 200 mg/day). Most cases involve patients being treated for pain with large, multiple daily doses of methadone, although cases have been reported in patients receiving doses commonly used for maintenance treatment of opioid addiction.
Methadone should be administered with particular caution to patients already at risk for development of prolonged QT interval (e.g., cardiac hypertrophy, concomitant diuretic use, hypokalemia, hypomagnesemia). Careful monitoring is recommended when using methadone in patients with a history of cardiac conduction abnormalities, those taking medications affecting cardiac conduction, and in other cases where history or physical exam suggest an increased risk of dysrhythmia. QT prolongation has also been reported in patients with no prior cardiac history who have received high doses of methadone. Patients developing QT prolongation while on methadone treatment should be evaluated for the presence of modifiable risk factors, such as concomitant medications with cardiac effects, drugs which might cause electrolyte abnormalities, and drugs which might act as inhibitors of methadone metabolism. For use of methadone to treat pain, the risk of QT prolongation and development of dysrhythmias should be weighed against the benefit of adequate pain management and the availability of alternative therapies.
Methadone treatment for analgesic therapy in patients with acute or chronic pain should only be initiated if the potential analgesic or palliative care benefit of treatment with methadone has been considered to outweigh the risk of QT prolongation that has been reported with high doses of methadone.
The use of methadone in patients already known to have a prolonged QT interval has not been systematically studied.
In using methadone an individualized benefit to risk assessment should be carried out and should include evaluation of patient presentation and complete medical history. For patients judged to be at risk, careful monitoring of cardiovascular status, including QT prolongation and dysrhythmias and those described previously should be performed.
Respiratory Depression
Respiratory depression is the chief hazard from methadone hydrochloride. Respiratory depression is a particular potential problem in elderly or debilitated patients as well as in those suffering from conditions accompanied by hypoxia or hypercapnia when even moderate therapeutic doses may dangerously decrease pulmonary ventilation.
Methadone Hydrochloride Injection should be administered with extreme caution to patients with conditions accompanied by hypoxia, hypercapnia, or decreased respiratory reserve such as; asthma, chronic obstructive pulmonary disease or cor pulmonale, severe obesity, sleep apnea syndrome, myxedema, kyphoscoliosis, CNS depression or coma. In these patients even usual therapeutic doses of methadone may decrease respiratory drive while simultaneously increasing airway resistance to the point of apnea. Alternative non-opioid analgesics should be considered, and methadone should be employed only under careful medical supervision at the lowest effective dose.
Methadone's peak respiratory depressant effects typically occur later, and persist longer than its peak analgesic effects, in the short-term use setting. These characteristics can contribute to cases of iatrogenic overdose, particularly during treatment initiation and dose titration.
Incomplete Cross-Tolerance Between Methadone and Other Opioids
Patients tolerant to other opioids may be incompletely tolerant to methadone. Incomplete cross-tolerance is a particular concern for patients tolerant to other μ-opioid agonists when converting to methadone, making determination of dosing during opioid conversion complex. Deaths have been reported during conversion from chronic, high dose treatment with other opioid agonists. Therefore, it is critical to understand the pharmacokinetics of methadone when converting patients from other opioids (see DOSAGE AND ADMINISTRATION, Tables 1 and 2, for appropriate conversion schedules). A high degree of "opioid tolerance" does not eliminate the possibility of methadone toxicity.
Misuse, Abuse, and Diversion of Opioids
Methadone is a μ-agonist opioid with an abuse liability similar to that of morphine and is a Schedule II controlled substance. Methadone, like morphine and other opioids used for analgesia, has the potential for being abused and is subject to criminal diversion.
Methadone can be abused in a manner similar to other opioid agonists, legal or illicit. This should be considered when dispensing Methadone Hydrochloride Injection in situations where the clinician is concerned about an increased risk of misuse, abuse, or diversion.
Concerns about abuse, addiction, diversion should not prevent the proper management of pain.
Healthcare professionals should contact their State Professional Licensing Board, or State Controlled Substances Authority for information on how to prevent and detect abuse or diversion of this product.
Interactions with other CNS Depressants
Patients receiving other opioid analgesics, general anesthetics, phenothiazines, other tranquilizers, sedatives, hypnotics, or other CNS depressants (including alcohol) concomitantly with methadone may experience respiratory depression, hypotension, profound sedation, or coma (see PRECAUTIONS)
Interactions with Alcohol and Drugs of Abuse
Methadone may be expected to have additive effects when used in conjunction with alcohol, other opioids, or illicit drugs that cause central nervous system depression. Deaths associated with illicit use of methadone have frequently involved concomitant benzodiazepine abuse.
Head Injury and Increased Intracranial Pressure
The respiratory depressant effects of opioids and their capacity to elevate cerebrospinal-fluid pressure may be markedly exaggerated in the presence of head injury, other intracranial lesions or a pre-existing increase in intracranial pressure. Furthermore, opioids produce effects which may obscure the clinical course of patients with head injuries. In such patients, opioids must be used with caution, and only if it is deemed essential.
-
PRECAUTIONS
General
Methadone given on a fixed-dose schedule may have a narrow therapeutic index in certain patient populations, especially when combined with other drugs, and should be reserved for cases where the benefits of opioid analgesia outweigh the known potential risks of cardiac conduction abnormalities, respiratory depression, altered mental states and postural hypotension. Methadone Hydrochloride Injection should be used with caution in elderly and debilitated patients; patients who are known to be sensitive to central nervous system depressants, such as those with cardiovascular, pulmonary, renal, or hepatic disease; and in patients with comorbid conditions or concomitant medications which may predispose to dysrhythmia.
Selection of patients for treatment with methadone should be governed by the same principles that apply to the use of other parenteral opioids (see INDICATIONS AND USAGE). Physicians should individualize treatment in every case (see DOSAGE AND ADMINISTRATION), taking into account the high degree of interpatient variability in response to and metabolism of methadone.
Drug Interactions
In vitro results indicate that methadone undergoes hepatic N-demethylation by cytochrome P450 enzymes, principally CYP3A4, and to a lesser extent CYP2D6. Coadministration of methadone with inducers of these enzymes may result in a more rapid metabolism and potential for decreased effects of methadone, whereas administration with inhibitors may reduce metabolism and potentiate methadone's effects. Therefore, drugs administered concomitantly with methadone should be evaluated for interaction potential; clinicians are advised to evaluate individual response to drug therapy.
Opioid antagonists, mixed agonist/antagonists, and partial agonists: As with other μ-agonists, patients maintained on methadone may experience withdrawal symptoms when given these agents. Examples of such agents are naloxone, naltrexone, pentazocine, nalbuphine, butorphanol, and buprenorphine.
Anti-retroviral agents:
Nevirapine: Based on the known metabolism of methadone, nevirapine may decrease plasma concentrations of methadone by increasing its hepatic metabolism. Opioid withdrawal syndrome has been reported in patients treated with nevirapine and methadone concomitantly. Methadone-maintained patients beginning nevirapine therapy should be monitored for evidence of withdrawal and methadone dose should be adjusted accordingly.
Efavirenz: Coadministration of efavirenz in HIV-infected methadone-maintenance patients has resulted in decreased methadone plasma concentrations of methadone associated with signs of opiod withdrawal, and necessitating increases in methadone dose.
Ritonavir and Ritonavir/Lopinavir: Reduced plasma methadone levels have been observed after administration of ritonavir alone or ritonavir/lopinavir combination. Withdrawal symptoms were however, inconsistently observed. Caution is warranted when administering methadone to patients receiving ritonavir-containing regimens in addition to other drugs known to decrease methadone plasma levels.
Zidovudine: Experimental evidence suggests that methadone increases the area under the concentration-time curve (AUC) of zidovudine with possible toxic effects.
Didanosine and Stavudine: Experimental evidence suggests that methadone decreased the AUC and peak levels for didanosine and stavudine, with a more significant decrease for didanosine. Methadone disposition was not substantially altered.
Cytochrome P450 inducers: The following drug interactions were reported following coadministration of methadone with inducers of cytochrome P450 enzymes.
Rifampin: In patients well-stabilized on methadone, concomitant administration of rifampin resulted in marked reduction in serum methadone levels and concurrent appearance of withdrawal symptoms.
Phenytoin: In a pharmacokinetic study with patients on methadone maintenance therapy, phenytoin administration (250 mg b.i.d initially for 1 day followed by 300 mg QD for 3-4 days) resulted in ~50% reduction in methadone exposure and concurrently withdrawal symptoms occurred. Upon discontinuation of phenytoin, the incidence of withdrawal symptoms decreased and the methadone exposure increased and was comparable to pre-phenytoin dose scenario.
Cytochrome P450 inhibitors: Since the metabolism of methadone is mediated by the CYP3A4 isozyme, coadministration of drugs that inhibit CYP3A4 activity may cause decreased clearance of methadone. The expected clinical results would be increased or prolonged opioid effects. Thus patients coadministered with inhibitors of CYP3A4 such as azole antifungal agents (e.g., ketoconazole), macrolide antibiotics (e.g., erythromycin), while receiving methadone should be carefully monitored and dosage adjustment made if warranted. Some selective serotonin reuptake inhibitors (SSRI's) (i.e., sertraline, fluvoxamine) upon coadministration may increase methadone plasma levels and result in increased opiate effects or toxicity.
Others:
Monoamine Oxidase (MAO) Inhibitors: Therapeutic doses of meperidine have precipitated severe reactions in patients concurrently receiving monoamine oxidase inhibitors or those who have received such agents within 14 days. Similar reactions thus far have not been reported with methadone; but if the use of methadone is necessary in such patients, a sensitivity test should be performed in which repeated small incremental doses are administered over the course of several hours while the patient's condition and vital signs are under careful observation.
Potentially Arrhythmogenic Agents: Extreme caution is necessary when any drug known to have the potential to prolong the QT interval is prescribed in conjunction with methadone. Pharmacodynamic interactions may occur with concomitant use of methadone and potentially arrhythmogenic agents such as class I and III antiarrhythmics, some neuroleptics and tricyclic antidepressants, and calcium channel blockers. Caution should also be exercised when prescribing concomitant drugs capable of inducing electrolyte disturbances that may prolong the QT interval (hypomagnesemia, hypokalemia). These include diuretics, laxatives, and in rare cases mineralocorticoid hormones.
Interactions with other CNS Depressants: Patients receiving other opioid analgesics, general anesthetics, phenothiazines, other tranquilizers, sedatives, hypnotics, or other CNS depressants (including alcohol) concomitantly with methadone may experience respiratory depression, hypotension, profound sedation, or coma.
Use with Mixed Agonist/Antagonist Opioid Analgesics: Agonist/antagonist analgesics (i.e., pentazocine, nalbuphine, butorphanol, or buprenorphine) should not be administered to patients who have received or are receiving a course of therapy with a pure opioid agonist, such as Methadone Hydrochloride Injection. In this situation, mixed agonist/antagonist analgesics may reduce the analgesic effect of Methadone Hydrochloride Injection and/or may precipitate withdrawal symptoms.
Anxiety
Methadone, used by tolerant patients at a constant maintenance dosage, is not a tranquilizer. Patients who are maintained on this drug will react to life problems and stresses as do other individuals. Anxiety in a patient on methadone should not be confused with narcotic abstinence and should not prompt treatment by increasing the dosage of methadone. The action of methadone in maintenance treatment is limited to the control of symptoms of opioid dependence or pain. Methadone is ineffective for relief of general anxiety.
Acute Pain
Maintenance patients on a stable dose of methadone who experience physical trauma, postoperative pain or other causes of acute pain cannot be expected to derive analgesia from their stable dose of methadone regimens. Such patients should be given analgesics, including opioids, that would be indicated in other patients experiencing similar nociceptive stimulation. Due to the opioid tolerance induced by methadone, when opioids are required for management of acute pain in methadone patients, somewhat higher and/or more frequent doses will often be required than would be the case for other, non-tolerant patients.
Risk of Relapse in Patients on Methadone Maintenance Treatment of Opioid Addiction
Abrupt opioid discontinuation can lead to development of opioid withdrawal symptoms (see PRECAUTIONS). Presentation of these symptoms has been associated with an increased risk of susceptible patients to relapse to illicit drug use and should be considered when assessing the risks and benefit of methadone use.
Tolerance and Physical Dependence
Tolerance is the need for increasing doses of opioids to maintain a defined effect such as analgesia (in the absence of disease progression or other external factors). Physical dependence is manifested by withdrawal symptoms after abrupt discontinuation of a drug or upon administration of an antagonist. Physical dependence and/or tolerance are not unusual during chronic opioid therapy.
If methadone is abruptly discontinued in a physically dependent patient, an abstinence syndrome may occur. The opioid abstinence or withdrawal syndrome is characterized by some or all of the following: restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other symptoms also may develop, including: irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate.
In general, chronically administered methadone should not be abruptly discontinued.
Special-Risk Patients
Methadone should be given with caution and the initial dose reduced in certain patients, such as the elderly and debilitated and those with severe impairment of hepatic or renal function, hypothyroidism, Addison's disease, prostatic hypertrophy, or urethral stricture. The usual precautions appropriate to the use of parenteral opioids should be observed and the possibility of respiratory depression should always be kept in mind.
Information for Patients
Methadone, like all opioids, may impair the mental and/or physical abilities required for the performance of potentially hazardous tasks such as driving or operating machinery. The patient should be cautioned accordingly.
Methadone, like other opioids, may produce orthostatic hypotension in ambulatory patients.
Alcohol and other CNS depressants may produce an additive CNS depression, when taken with methadone, and should be avoided.
If a patient taking methadone experiences symptoms suggestive of an arrhythmia (such as palpitations, dizziness, lightheadedness, or syncope), that patient should seek immediate medical attention.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Data from published reports of carcinogenicity studies indicate that there was a significant increase in pituitary adenomas in female B6C2F1 mice consuming 15 mg/kg/day methadone for two years. This dose was approximately 0.6 times a human daily oral dose of 120 mg/day, on a body surface area basis. However, this finding was not seen in mice consuming 60 mg/kg/day (approximately 2.5 times a human daily oral dose of 120 mg/day). Furthermore, in a two-year study of dietary administration of methadone to Fischer 344 rats, there was no clear evidence for treatment related increase in the incidence of neoplasms, at doses as high as 28 mg/kg/day in males and 88 mg/kg/day in females (approximately 2.3 times and 7.1 times, respectively, a human daily oral dose of 120 mg/day) based on body surface area comparison.
In published reports, methadone tested negative in tests for chromosome breakage and disjunction and sex-linked recessive lethal gene mutations in germ cells of Drosophila using feeding and injection procedures. Methadone treatment of male mice increased sex chromosome and autosome univalent chromosomes and translocations in multivalent chromosomes. Methadone tested positive in the E.coli DNA repair system and Neurospora crassa and mouse lymphoma forward mutation assays.
Pregnancy
Teratogenic effects: Pregnancy Category C. There are no controlled studies of methadone use in pregnant women that can be used to establish safety. However, an expert review of published data on experiences with methadone use during pregnancy by TERIS - the Teratogen Information System -concluded that maternal use of methadone during pregnancy as part of a supervised, therapeutic regimen is unlikely to pose a substantial teratogenic risk (quantity and quality of data assessed as “limited to fair”), however, the data are insufficient to state that there is no risk (TERIS, last reviewed October, 2002). Pregnant women involved in methadone maintenance programs have been reported to have significantly improved prenatal care, improved fetal outcomes, and reduced mortality when compared to pregnant women using illicit drugs. Several factors complicate the interpretation of investigations of the children of women who took methadone during pregnancy. These include: the maternal use of illicit drugs, other maternal factors such as nutrition, infection, and psychosocial circumstances, limited information regarding dose and duration of methadone use during pregnancy, and the fact that most maternal exposure appears to occur after the first trimester of pregnancy. In addition, reported studies generally compare the benefit of methadone to the risk of untreated addiction to illicit drugs; the relevance of these findings to pain patients prescribed methadone during pregnancy is unclear.
Methadone has been detected in amniotic fluid and cord plasma at concentrations proportional to maternal plasma and in newborn urine at lower concentrations than corresponding maternal urine.
A retrospective series of 101 pregnant opiate-dependent women who underwent inpatient opiate detoxification with methadone did not demonstrate any increased risk of miscarriage in the 2nd trimester or premature delivery in the 3rd trimester.
Several studies have suggested that infants born to narcotic-addicted women treated with methadone during all or part of pregnancy have been found to have decreased fetal growth with reduced birth weight, length, and/or head circumference compared to controls. The growth deficit does not appear to persist into later childhood. However, children born to women treated with methadone during pregnancy have been shown to demonstrate mild but persistent deficits in performance on psychometric and behavioral tests.
Methadone should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Additional information on the potential risks of methadone may be derived from animal data. Methadone does not appear to be teratogenic in the rat or rabbit models. However, following large doses, methadone produced teratogenic effects in the guinea pig, hamster and mouse. One published study found that in hamster fetuses, subcutaneous methadone doses of 31 mg/kg or greater (estimated exposure was approximately 2 times a human daily oral dose of 120 mg/day on a mg/m2 basis, or equivalent to a human daily intravenous dose of 120 mg/day) on day 8 of gestation produced exencephaly and neurological effects. Some of the reported effects were observed at doses that were maternally toxic. In another study, a single subcutaneous dose of 22-24 mg/kg methadone (estimated exposure was approximately equivalent to a human daily oral dose of 120 mg/day on a mg/m2 basis; or half a human daily intravenous dose of 120 mg/day) on day 9 of gestation in mice also produced exencephaly in 11% of the embryos. However, no effects were reported in rats and rabbits at oral doses up to 40 mg/kg (estimated exposure was approximately 3 and 6 times, respectively, a human daily oral dose of 120 mg/day on a mg/m2 basis; or 1.5 and 3 times a human daily intravenous dose of 120 mg/day) during days 6-15 and 6-18, respectively.
Nonteratogenetic Effects: Babies born to mothers who have been taking opioids regularly prior to delivery may be physically dependent. Onset of withdrawal symptoms in infants is usually in the first days after birth but may be delayed for two to four weeks. Withdrawal signs in the newborn include irritability and excessive crying, tremors, hyperactive reflexes, increased respiratory rate, increased stools, sneezing, yawning, vomiting, and fever. The intensity of the syndrome does not always correlate with the duration of maternal opioid dose or maternal dose. There is no consensus on the appropriate management of infant withdrawal.
There are conflicting reports on whether the risk of sudden infant death syndrome (SIDS) is increased in infants born to women treated with methadone during pregnancy.
Abnormal fetal nonstress tests (NSTs) have been reported to occur more frequently when the test is performed 1-2 hours after a maintenance dose of methadone in late pregnancy compared to controls. Published animal studies suggest that perinatal exposure to opioids including methadone may alter neuronal development and behavior in the offspring. Perinatal methadone exposure in rats has been linked to alterations in learning ability, motor activity, thermal regulation, nociception responses and sensitivity to other drugs. Additional animal data demonstrates evidence for neurochemical changes in the brains of methadone-treated offspring, including the cholinergic, dopaminergic, noradrenergic and serotonergic systems.
Clinical Pharmacology for Pregnancy: Pregnant women have significantly lower trough plasma concentrations, increased plasma methadone clearance and shorter half-life than after delivery. Dosage adjustment using higher doses or administering the daily dose in divided doses may be necessary in pregnant women treated with methadone. [See CLINICAL PHARMACOLOGY and DOSAGE AND ADMINISTRATION].
Labor and Delivery: As with all opioids, administration of methadone to the mother shortly before delivery may result in some degree of respiratory depression in the newborn, especially if higher doses are used. Methadone is not recommended for obstetric analgesia because its long duration of action increases the probability of respiratory depression in the newborn. Narcotics with mixed agonist-antagonist properties should not be used for pain control during labor in patients chronically treated with methadone because they may precipitate acute withdrawal.
Nursing mothers: Methadone is secreted into human milk. There is no information on use of parenteral methadone in breast feeding, or on the safety of the high doses of methadone typically used in chronic pain treatment. The safety of breastfeeding while taking oral methadone is also controversial. At maternal oral doses of 10-80 mg/day, methadone concentrations from 50 to 570 ug/L in milk have been reported, which, in the majority of samples, were lower than maternal serum drug concentrations at steady state. Peak methadone levels in milk occur approximately 4-5 hours after an oral dose. Based on an average milk consumption of 150 mL/kg/day, an infant would consume approximately 17.4 ug/kg/day, which is approximately 2-3% of the oral maternal dose. Methadone has been detected in very low plasma concentrations in some infants whose mothers were taking methadone. Women on high dose methadone maintenance, who are already breast feeding, should be counseled to wean breast-feeding gradually in order to prevent neonatal abstinence syndrome. Methadone-treated mothers considering nursing an opioid-naïve infant should be counseled of the presence of methadone in breast milk.
Because of the potential for serious adverse reactions in nursing infants from methadone, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
Safety and effectiveness in pediatric patients below the age of 18 years have not been established.
Geriatric Use
Clinical studies of Methadone Hydrochloride Injection did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for elderly patients should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
Renal Impairment
The use of methadone has not been extensively evaluated in patients with renal insufficiency.
-
ADVERSE REACTIONS
Initial Administration: The initial methadone dose should be carefully titrated to the individual. Induction too rapid for the patient's sensitivity is more likely to produce adverse effects.
The major hazards of methadone are respiratory depression and, to a lesser degree, systemic hypotension. Respiratory arrest, shock, cardiac arrest, and death have occurred.
The most frequently observed adverse reactions include lightheadedness, dizziness, sedation, nausea, vomiting, and sweating. These effects seem to be more prominent in ambulatory patients and in those who are not suffering severe pain. In such individuals, lower doses of methadone are advisable.
Other adverse reactions that have been reported in patients (including opioid addicts taking methadone for detoxification or maintenance) receiving methadone include the following:
Body as a Whole: asthenia (weakness), edema, headache
Cardiovascular: Arrhythmias, bigeminal rhythms, bradycardia, extrasystoles, tachycardia, Torsade de Pointes, ventricular fibrillation, ventricular tachycardia. ECG abnormalities, prolonged QT interval, T-wave inversion, cardiomyopathy, flushing, heart failure, hypotension, palpitations, phlebitis, syncope.
Digestive: Abdominal pain, anorexia, biliary tract spasm, constipation, dry mouth, glossitis
Hematologic and Lymphatic: Reversible thrombocytopenia has been described in opioid addicts with chronic hepatitis.
Metabolic and Nutritional: Hypokalemia, hypomagnesemia, weight gain
Nervous: Agitation, confusion, seizures, disorientation, dysphoria, euphoria, insomnia
Respiratory: Pulmonary edema
Skin and appendages:
Intramuscular and Subcutaneous: Local tissue reactions (pain, erythema, swelling), particularly with continuous subcutaneous infusion
Intravenous: Pruritis, urticaria, other skin rashes, and rarely, hemorrhagic urticaria
Special senses: Visual disturbances
Urogenital: Antidiuretic effect, amenorrhea, urinary retention or hesitancy, reduced libido and/or potency
-
DRUG ABUSE AND DEPENDENCE
Methadone is a μ-agonist opioid with an abuse liability similar to that of morphine and is a Schedule II controlled substance. Methadone, like morphine and other opioids used for analgesia, has the potential for being abused and is subject to criminal diversion.
Abuse
Drug addiction is characterized by a preoccupation with the procurement, hoarding, and abuse of drugs for non-medicinal purposes. Drug addiction is treatable, utilizing a multi-disciplinary approach, but relapse is common.
“Drug seeking” behavior is very common to addicts and drug abusers. Drug seeking tactics include emergency calls or visits near the end of the office hours, refusal to undergo appropriate examination, testing or referral, repeated claims of loss of prescriptions, tampering with prescriptions and reluctance to provide prior medical records or contact information for other treating physician(s). Doctor shopping (visiting multiple prescribers) to obtain additional prescriptions is common among drug abusers and people suffering from untreated addictions.
Physical Dependence and Tolerance
Abuse and addiction are separate and distinct from physical dependence and tolerance. Physicians should be aware that addiction may not be accompanied by concurrent tolerance and symptoms of physical dependence in all addicts. In addition, abuse of opioids can occur in the absence of true addiction and is characterized by misuse for non-medical purposes, often in combination with other psychoactive substances. Methadone Hydrochloride Injection, like other opioids, may be diverted for non-medical use. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests is strongly advised.
Abuse of Methadone Hydrochloride Injection poses a risk of overdose and death. This risk is increased with concurrent abuse of Methadone Hydrochloride Injection with alcohol and other substances. In addition, parenteral drug abuse is commonly associated with transmission of infectious disease such as hepatitis and HIV.
Proper assessment of the patient, proper prescribing practices, periodic re-evaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
Infants born to mothers physically dependent on opioids may also be physically dependent and may exhibit respiratory difficulties and withdrawal symptoms (See PRECAUTIONS; Pregnancy and Labor and Delivery)
-
OVERDOSAGE
Signs and Symptoms
Serious overdosage of methadone is characterized by respiratory depression (a decrease in respiratory rate and/or tidal volume, Cheyne-Stokes respiration, cyanosis), extreme somnolence progressing to stupor or coma, maximally constricted pupils, skeletal-muscle flaccidity, cold and clammy skin, and sometimes, bradycardia and hypotension. In severe overdosage, particularly by the intravenous route, apnea, circulatory collapse, cardiac arrest, and death may occur.
Treatment
Primary attention should be given to the reestablishment of adequate respiratory exchange through provision of a patent airway and institution of assisted or controlled ventilation. If a non-tolerant person takes a large dose of methadone, effective opioid antagonists are available to counteract the potentially lethal respiratory depression. The physician must remember, however, that methadone is a long-acting depressant (36 to 48 hours), whereas the antagonists act for much shorter periods (one to three hours). The patient must, therefore, be monitored continuously for recurrence of respiratory depression and may need to be treated repeatedly with the narcotic antagonist. If the diagnosis is correct and respiratory depression is due only to overdosage of methadone, the use of other respiratory stimulants is not indicated.
Opioid antagonists should not be administered in the absence of clinically significant respiratory or cardiovascular depression. In an individual physically dependent on opioids, the administration of the usual dose of an opioid antagonist may precipitate an acute withdrawal syndrome. The severity of this syndrome will depend on the degree of physical dependence and the dose of the antagonist administered. If antagonists must be used to treat serious respiratory depression in the physically dependent patient, the antagonist should be administered with extreme care and by titration with smaller than usual doses of the antagonist.
Intravenously administered naloxone or nalmefene may be used to reverse signs of intoxication. Because of the relatively short half-life of naloxone as compared with methadone, repeated injections may be required until the status of the patient remains satisfactory. Naloxone may also be administered by continuous intravenous infusion.
Oxygen, intravenous fluids, vasopressors, and other supportive measures should be employed as indicated.
-
DOSAGE AND ADMINISTRATION
Methadone differs from many other opioid agonists in several important ways. Methadone's pharmacokinetic properties, coupled with high interpatient variability in its absorption, metabolism, and relative analgesic potency, necessitate a cautious and highly individualized approach to prescribing. Particular vigilance is necessary during treatment initiation, during conversion from one opioid to another, and during dose titration.
While methadone's duration of analgesic action (typically 4 to 8 hours) in the setting of single-dose studies approximates that of morphine, methadone's plasma elimination half-life is substantially longer than that of morphine (typically 8 to 59 hours vs. 1 to 5 hours). Methadone's peak respiratory depressant effects typically occur later, and persist longer than its peak analgesic effects. Also, with repeated dosing, methadone may be retained in the liver and then slowly released, prolonging the duration of action despite low plasma concentrations. For these reasons, steady-state plasma concentrations, and full analgesic effects, are usually not attained until 3 to 5 days of dosing. Additionally, incomplete cross-tolerance between μ-opioid agonists makes determination of dosing during opioid conversion complex.
All of these characteristics make methadone dosing complex and can contribute to cases of iatrogenic overdose, particularly during treatment initiation and dose titration. A high degree of "opioid tolerance" does not eliminate the possibility of methadone overdose, iatrogenic or otherwise. Deaths have been reported during conversion to methadone from chronic, high-dose treatment with other opioid agonists.
Treatment of Pain
Optimal methadone initiation and dose titration strategies for the treatment of pain have not been determined. Published equianalgesic conversion ratios between methadone and other opioids are imprecise, providing at best, only population averages that cannot be applied consistently to all patients. It should be noted that many commonly cited equianalgesia tables only present relative analgesic potencies of single opioid doses in non-tolerant patients, thus greatly underestimating methadone's analgesic potency, and its potential for adverse effects in repeated-dose settings. Regardless of the dose determination strategy employed, methadone is most safely initiated and titrated using small initial doses and gradual dose adjustments.
As with all opioid drugs, it is necessary to adjust the dosing regimen for each patient individually, taking into account the patient's prior analgesic treatment experience. The following dosing recommendations should only be considered as suggested approaches to what is actually a series of clinical decisions over time in the management of the pain of each individual patient. Prescribers should always follow appropriate pain management principles of careful assessment and ongoing monitoring.
In the selection of an initial dose of Methadone Hydrochloride Injection, attention should be given to the following:
- The total daily dose, potency and specific characteristics of the opioid the patient had been taking previously, if any;
- The relative potency estimate used to calculate an equianalgesic starting methadone dose, in particular, whether it is intended for use in acute or chronic methadone dosing;
- The patient's degree of opioid tolerance;
- The age, general condition and medical status of the patient;
- Concurrent medications, particularly other CNS and respiratory depressants;
- The type, severity and expected duration of the patient's pain;
- The acceptable balance between pain control and adverse side effects.
Methadone Hydrochloride Injection may be administered intravenously, subcutaneously or intramuscularly. The absorption of subcutaneous and intramuscular methadone has not been well characterized and appears to be unpredictable. Local tissue reactions may occur.
Parenteral products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
Initiation of Therapy in Opioid Non-Tolerant Patients
When parenteral methadone is used as the first analgesic in patients who are not already being treated with, and tolerant to, opioids, the usual intravenous methadone starting dose is 2.5 mg to 10 mg every 8 to 12 hours, slowly titrated to effect. More frequent administration may be required during methadone initiation in order to maintain adequate analgesia, and extreme caution is necessary to avoid overdosage, taking into account methadone's long elimination half life.
Conversion from Oral Methadone to Parenteral Methadone
Conversion from oral methadone to parenteral methadone should initially use a 2:1 dose ratio (e.g., 10 mg oral methadone to 5 mg parenteral methadone).
Switching Patients to Parenteral Methadone from other Chronic Opioids
Switching a patient from another chronically administered opioid to methadone requires caution due to the uncertainty of dose conversion ratios and incomplete cross-tolerance. Deaths have occurred in opioid tolerant patients during conversion to methadone.
Conversion ratios in many commonly used equianalgesic dosing tables do not apply in the setting of repeated methadone dosing. Although with single-dose administration the onset and duration of analgesic action, as well as the analgesic potency of methadone and morphine, are similar methadone's potency increases over time with repeated dosing. Furthermore, the conversion ratio between methadone and other opiates varies dramatically depending on baseline opiate (morphine equivalent) use as shown in the table below.
The dose conversion scheme below is derived from various consensus guidelines for converting chronic pain patients to methadone from morphine. The guidelines used to construct this table, however, were all designed for converting patients from oral morphine to oral methadone. The third column assumes a 2:1 ratio for converting from oral to intravenous methadone. Clinicians should consult published conversion guidelines to determine the equivalent morphine dose for patients converting from other opioids.
Table 1. Oral Morphine to Intravenous Methadone Conversion for Chronic Administration *The total daily methadone dose derived from the table above may then be divided to reflect the intended dosing schedule (i.e., for administration every 8 hours, divide total daily methadone dose by 3).
Total Daily Baseline Oral Estimated Daily Oral Methadone Estimated Daily Intravenous Morphine Dose Reguirement as Percent of Methadone as Percent of Total Daily Total Daily Morphine Dose Oral Morphine Dose* < 100mg 20% to 30% 10% to 15% 100 to 300 mg 10% to 20% 5% to 10% 300 to 600 mg 8% to 12% 4% to 6% 600 mg to 1000 mg 5% to 10% 3% to 5% > 1000 mg < 5% < 3% Table 2. Parenteral Morphine to Intravenous Methadone Conversion for Chronic Administration (Derived from Table 1, assuming a 3:1 oral:parenteral morphine ratio) *The total daily methadone dose derived from the table above may then be divided to reflect the intended dosing schedule (i.e., for administration every 8 hours, divide total daily methadone dose by 3).
Total Daily Baseline Parenteral Estimated Daily Parenteral Methadone Morphine Dose Requirement as Percent of Total Daily Morphine Dose* 10 mg to 30 mg 40% to 66% 30 mg to 50 mg 27% to 66% 50 mg to 100 mg 22% to 50% 100 mg to 200 mg 15% to 34% 200 mg to 500 mg 10% to 20% Note: Equianalgesic methadone dosing varies not only between patients, but also within the same patient, depending on baseline morphine (or other opioid) dose. Tables 1 and 2 have been included in order to illustrate this concept and to provide a safe starting point for opioid conversion. Methadone dosing should not be based solely on these tables. Methadone conversion and dose titration methods should always be individualized to account for the patient's prior opioid exposure, general medical condition, concomitant medication, and anticipated breakthrough medication use. The endpoint of titration is achievement of adequate pain relief, balanced against tolerability of opioid side effects. If a patient develops intolerable opioid related side effects, the methadone dose, or dosing interval, may need to be decreased.
Methadone conversion and dose titration methods should always be individualized to account for the patient's prior opioid exposure, general medical condition, concomitant medication, and anticipated breakthrough medication use. The endpoint of titration is achievement of adequate pain relief, balanced against tolerability of opioid side effects. If a patient develops intolerable opioid related side effects, the methadone dose, or dosing interval, may need to be decreased.
Dosage Adjustment During Pregnancy
Methadone clearance may be increased during pregnancy. Several small studies have demonstrated significantly lower trough methadone plasma concentrations and shorter methadone half-lives in women during their pregnancy compared to after their delivery. During pregnancy a woman's methadone dose may need to be increased, or their dosing interval decreased. Methadone should be used in pregnancy only if the potential benefit justifies the potential risk to the fetus.
Detoxification and Maintenance Treatment of Opiate Dependence
For detoxification and maintenance of opiate dependence, methadone should be administered in accordance with the treatment standards cited in 42CFR Section 8.12, including limitations on unsupervised administration. Injectable methadone products are not approved for the outpatient treatment of opioid dependence. Parenteral methadone should be used only for patients who are unable to take oral medication, such as during hospitalization. The patient's oral methadone dose should be converted to an equivalent parenteral dose using the considerations above.
-
HOW SUPPLIED
Multiple-Dose Vials: 10 mg/mL, 20 mL, NDC 66479-530-02
One vial per package
Protect from light. Store in carton until contents have been used.
Store at 25°C (77°F); excursions are permitted to 15°-30°C (59°-86°F) [See USP Controlled Room Temperature]
Manufactured by: AAIPharma Inc., Charleston, SC 29405
Marketed by: Xanodyne Pharmaceuticals Inc., Newport, KY 41071
Xanodyne®
Pharmaceuticals, inc.
©2006, Xanodyne Pharmaceuticals Inc. PC3374B Rev. 03-2006
-
INGREDIENTS AND APPEARANCE
METHADONE
methadone hydrochloride injection, solutionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:66479-530 Route of Administration INTRAVENOUS DEA Schedule CII Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength methadone hydrochloride (UNII: 229809935B) (methadone - UNII:UC6VBE7V1Z) 10 mg in 1 mL Inactive Ingredients Ingredient Name Strength chlorobutanol (UNII: HM4YQM8WRC) sodium chloride (UNII: 451W47IQ8X) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:66479-530-02 1 in 1 PACKAGE 1 20 mL in 1 VIAL Labeler - Xanodyne Pharmaceuticals Inc.