Label: DILTIAZEM HCI injection
- NDC Code(s): 51662-1335-1, 51662-1335-2
- Packager: HF Acquisition Co LLC, DBA HealthFirst
- This is a repackaged label.
- Source NDC Code(s): 0641-6013
- Category: HUMAN PRESCRIPTION DRUG LABEL
Drug Label Information
Updated January 19, 2023
If you are a healthcare professional or from the pharmaceutical industry please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
-
DESCRIPTION
Diltiazem hydrochloride is a calcium ion influx inhibitor (slow channel blocker or calcium channel antagonist). Chemically, diltiazem hydrochloride is (+)-5-[2-(Dimethylamino)ethyl]-cis-2,3-dihydro-3-hydroxy-2-(p-methoxyphenyl)-1,5-benzothiazepin-4(5H)-one acetate(ester) monohydrochloride. The structural formula is:
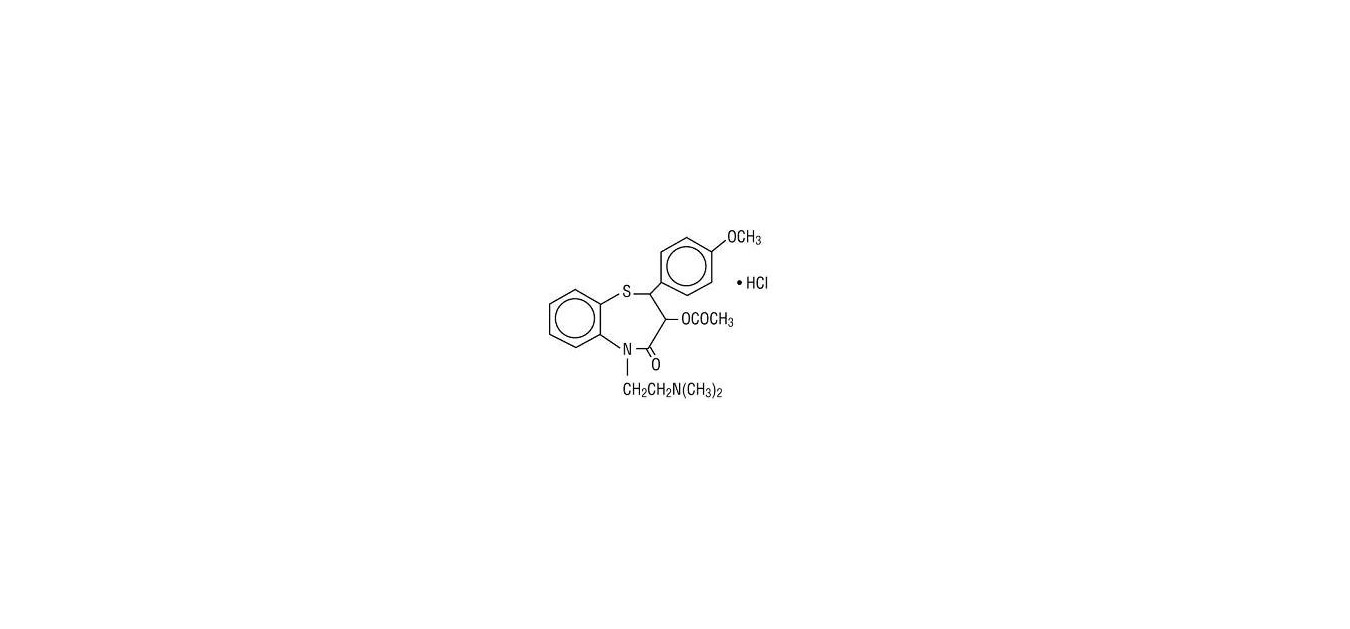
C22H26N2O4S• HCl MW: 450.98
Diltiazem hydrochloride is a white to off-white crystalline powder with a bitter taste. It is soluble in water, methanol, and chloroform.
Diltiazem hydrochloride injection is a clear, colorless, sterile, nonpyrogenic solution. It has a pH range of 3.7 to 4.1.
Diltiazem hydrochloride injection is for direct intravenous bolus injection and continuous intravenous infusion.
Each mL contains: 5 mg Diltiazem Hydrochloride, USP, 0.75 mg Citric Acid Anhydrous, USP, 0.65 mg Sodium Citrate Dihydrate USP, 50 mg Sorbitol NF, and Water for Injection, USP q.s. Sodium Hydroxide or Hydrochloric Acid is used to adjust pH.
-
CLINICAL PHARMACOLOGY
Mechanisms of Action
Diltiazem inhibits the influx of calcium (Ca 2+) ions during membrane depolarization of cardiac and vascular smooth muscle. The therapeutic benefits of diltiazem in supraventricular tachycardias are related to its ability to slow AV nodal conduction time and prolong AV nodal refractoriness. Diltiazem exhibits frequency (use) dependent effects on AV nodal conduction such that it may selectively reduce the heart rate during tachycardias involving the AV node with little or no effect on normal AV nodal conduction at normal heart rates.
Diltiazem slows the ventricular rate in patients with a rapid ventricular response during atrial fibrillation or atrial flutter. Diltiazem converts paroxysmal supraventricular tachycardia (PSVT) to normal sinus rhythm by interrupting the reentry circuit in AV nodal reentrant tachycardias and reciprocating tachycardias, e.g., Wolff-Parkinson-White syndrome (WPW).
Diltiazem prolongs the sinus cycle length. It has no effect on the sinus node recovery time or on the sinoatrial conduction time in patients without SA nodal dysfunction. Diltiazem has no significant electrophysiologic effects on tissues in the heart that are fast sodium channel dependent, e.g., His-Purkinje tissue, atrial and ventricular muscle, and extranodal accessory pathways.
Like other calcium channel antagonists, because of its effect on vascular smooth muscle, diltiazem decreases total peripheral resistance resulting in a decrease in both systolic and diastolic blood pressure.
Hemodynamics
In patients with cardiovascular disease, diltiazem hydrochloride administered intravenously in single bolus doses, followed in some cases by a continuous infusion, reduced blood pressure, systemic vascular resistance, the rate-pressure product, and coronary vascular resistance and increased coronary blood flow. In a limited number of studies of patients with compromised myocardium (severe congestive heart failure, acute myocardial infarction, hypertrophic cardiomyopathy), administration of intravenous diltiazem produced no significant effect on contractility, left ventricular end diastolic pressure, or pulmonary capillary wedge pressure. The mean ejection fraction and cardiac output/index remained unchanged or increased. Maximal hemodynamic effects usually occurred within 2 to 5 minutes of an injection. However, in rare instances, worsening of congestive heart failure has been reported in patients with preexisting impaired ventricular function.
Pharmacodynamics
The prolongation of PR interval correlated significantly with plasma diltiazem concentration in normal volunteers using the Sigmoidal Emax model. Changes in heart rate, systolic blood pressure, and diastolic blood pressure did not correlate with diltiazem plasma concentrations in normal volunteers. Reduction in mean arterial pressure correlated linearly with diltiazem plasma concentration in a group of hypertensive patients.
In patients with atrial fibrillation and atrial flutter, a significant correlation was observed between the percent reduction in HR and plasma diltiazem concentration using the Sigmoidal Emax model. Based on this relationship, the mean plasma diltiazem concentration required to produce a 20% decrease in heart rate was determined to be 80 ng/mL. Mean plasma diltiazem concentrations of 130 ng/mL and 300 ng/mL were determined to produce reductions in heart rate of 30% and 40%.
Pharmacokinetics and Metabolism
Following a single intravenous injection in healthy male volunteers, diltiazem hydrochloride appears to obey linear pharmacokinetics over a dose range of 10.5 to 21 mg. The plasma elimination half-life is approximately 3.4 hours. The apparent volume of distribution of diltiazem is approximately 305 L. Diltiazem is extensively metabolized in the liver with a systemic clearance of approximately 65 L/h.
After constant rate intravenous infusion to healthy male volunteers, diltiazem exhibits nonlinear pharmacokinetics over an infusion range of 4.8 to 13.2 mg/h for 24 hours. Over this infusion range, as the dose is increased, systemic clearance decreases from 64 to 48 L/h while the plasma elimination half-life increases from 4.1 to 4.9 hours. The apparent volume of distribution remains unchanged (360 to 391 L). In patients with atrial fibrillation or atrial flutter, diltiazem systemic clearance has been found to be decreased compared to healthy volunteers. In patients administered bolus doses ranging from 2.5 mg to 38.5 mg, systemic clearance averaged 36 L/h. In patients administered continuous infusions at 10 mg/h or 15 mg/h for 24 hours, diltiazem systemic clearance averaged 42 L/h and 31 L/h, respectively.
Based on the results of pharmacokinetic studies in healthy volunteers administered different oral diltiazem hydrochloride formulations, constant rate intravenous infusions of diltiazem hydrochloride at 3, 5, 7, and 11 mg/h are predicted to produce steady-state plasma diltiazem concentrations equivalent to 120-, 180-, 240-, and 360-mg total daily oral doses of diltiazem hydrochloride tablets or diltiazem hydrochloride extended-release capsules.
After oral administration, diltiazem undergoes extensive metabolism in man by deacetylation, N-demethylation, and O-demethylation via cytochrome P-450 (oxidative metabolism) in addition to conjugation. Metabolites N-monodesmethyldiltiazem, desacetyldiltiazem, desacetyl-N-monodesmethyldiltiazem, desacetyl-O-desmethyldiltiazem, and desacetyl-N, O-desmethyldiltiazem have been identified in human urine. Following oral administration, 2% to 4% of the unchanged diltiazem appears in the urine. Drugs which induce or inhibit hepatic microsomal enzymes may alter diltiazem disposition.
Following single intravenous injection of diltiazem hydrochloride, however, plasma concentrations of N-mono-desmethyldiltiazem and desacetyldiltiazem, two principal metabolites found in plasma after oral administration, are typically not detected. These metabolites are observed, however, following 24 hour constant rate intravenous infusion. Total radioactivity measurement following short IV administration in healthy volunteers suggests the presence of other unidentified metabolites which attain higher concentrations than those of diltiazem and are more slowly eliminated; half-life of total radioactivity is about 20 hours compared to 2 to 5 hours for diltiazem.
Diltiazem hydrochloride is 70% to 80% bound to plasma proteins. In vitro studies suggest alpha1-acid glycoprotein binds approximately 40% of the drug at clinically significant concentrations. Albumin appears to bind approximately 30% of the drug, while other constituents bind the remaining bound fraction. Competitive in vitro ligand binding studies have shown that diltiazem hydrochloride binding is not altered by therapeutic concentrations of digoxin, phenytoin, hydrochlorothiazide, indomethacin, phenylbutazone, propranolol, salicylic acid, tolbutamide, or warfarin.
Renal insufficiency, or even end-stage renal disease, does not appear to influence diltiazem disposition following oral administration. Liver cirrhosis was shown to reduce diltiazem’s apparent oral clearance and prolong its half-life.
-
INDICATIONS & USAGE
Diltiazem Hydrochloride Injection is indicated for the following:
Atrial Fibrillation or Atrial Flutter
Temporary control of rapid ventricular rate in atrial fibrillation or atrial flutter. It should not be used in patients with atrial fibrillation or atrial flutter associated with an accessory bypass tract such as in Wolff-Parkinson-White (WPW) syndrome or short PR syndrome.
Paroxysmal Supraventricular Tachycardia
Rapid conversion of paroxysmal supraventricular tachycardias (PSVT) to sinus rhythm. This includes AV nodal reentrant tachycardias and reciprocating tachycardias associated with an extranodal accessory pathway such as the WPW syndrome or short PR syndrome. Unless otherwise contraindicated, appropriate vagal maneuvers should be attempted prior to administration of diltiazem hydrochloride injection.
The use of diltiazem hydrochloride injection should be undertaken with caution when the patient is compromised hemodynamically or is taking other drugs that decrease any or all of the following: peripheral resistance, myocardial filling, myocardial contractility, or electrical impulse propagation in the myocardium.
For either indication and particularly when employing continuous intravenous infusion, the setting should include continuous monitoring of the ECG and frequent measurement of blood pressure. A defibrillator and emergency equipment should be readily available.
In domestic controlled trials in patients with atrial fibrillation or atrial flutter, bolus administration of diltiazem hydrochloride injection was effective in reducing heart rate by at least 20% in 95% of patients. Diltiazem hydrochloride injection rarely converts atrial fibrillation or atrial flutter to normal sinus rhythm. Following administration of one or two intravenous bolus doses of diltiazem injection, response usually occurs within 3 minutes and maximal heart rate reduction generally occurs in 2 to 7 minutes. Heart rate reduction may last from 1 to 3 hours. If hypotension occurs, it is generally short-lived, but may last from 1 to 3 hours.
A 24-hour continuous infusion of diltiazem injection in the treatment of atrial fibrillation or atrial flutter maintained at least a 20% heart rate reduction during the infusion in 83% of patients. Upon discontinuation of infusion, heart rate reduction may last from 0.5 hours to more than 10 hours (median duration 7 hours). Hypotension, if it occurs, may be similarly persistent.
In the controlled clinical trials, 3.2% of patients required some form of intervention (typically, use of intravenous fluids or the Trendelenburg position) for blood pressure support following diltiazem hydrochloride injection.
In domestic controlled trials, bolus administration of diltiazem hydrochloride injection was effective in converting PSVT to normal sinus rhythm in 88% of patients within 3 minutes of the first or second bolus dose.
Symptoms associated with the arrhythmia were improved in conjunction with decreased heart rate or conversion to normal sinus rhythm following administration of diltiazem hydrochloride injection.
-
CONTRAINDICATIONS
Diltiazem hydrochloride injection is contraindicated in:
Patients with sick sinus syndrome except in the presence of a functioning ventricular pacemaker.
Patients with second- or third-degree AV block except in the presence of a functioning ventricular pacemaker.
Patients with severe hypotension or cardiogenic shock.
Patients who have demonstrated hypersensitivity to the drug.
Intravenous diltiazem and intravenous beta-blockers should not be administered together or in close proximity (within a few hours).
Patients with atrial fibrillation or atrial flutter associated with an accessory bypass tract such as in WPW syndrome or short PR syndrome. As with other agents which slow AV nodal conduction and do not prolong the refractoriness of the accessory pathway (e.g., verapamil, digoxin), in rare instances patients in atrial fibrillation or atrial flutter associated with an accessory bypass tract may experience a potentially life-threatening increase in heart rate accompanied by hypotension when treated with diltiazem hydrochloride injection. As such, the initial use of diltiazem hydrochloride injection should be, if possible, in a setting where monitoring and resuscitation capabilities, including DC cardioversion/defibrillation, are present (see OVERDOSAGE). Once familiarity of the patient’s response is established, use in an office setting may be acceptable.
Patients with ventricular tachycardia. Administration of other calcium channel blockers to patients with wide complex tachycardia (QRS ≥0.12 seconds) has resulted in hemodynamic deterioration and ventricular fibrillation. It is important that an accurate pretreatment diagnosis distinguish wide complex QRS tachycardia of superventricular origin from that of ventricular origin prior to administration of diltiazem hydrochloride injection. -
WARNINGS
Cardiac Conduction
Diltiazem prolongs AV nodal conduction and refractoriness that may rarely result in second- or third-degree AV block in sinus rhythm. Concomitant use of diltiazem with agents known to affect cardiac conduction may result in additive effects (see PRECAUTIONS, Drug Interactions). If high-degree AV block occurs in sinus rhythm, intravenous diltiazem should be discontinued and appropriate supportive measures instituted (see OVERDOSAGE).
Congestive Heart Failure
Although diltiazem has a negative inotropic effect in isolated animal tissue preparations, hemodynamic studies in humans with normal ventricular function and in patients with a compromised myocardium, such as severe CHF, acute MI, and hypertrophic cardiomyopathy, have not shown a reduction in cardiac index nor consistent negative effects on contractility (dp/dt). Administration of oral diltiazem in patients with acute myocardial infarction and pulmonary congestion documented by x-ray on admission is contraindicated. Experience with the use of diltiazem hydrochloride injection in patients with impaired ventricular function is limited. Caution should be exercised when using the drug in such patients.
Hypotension
Decreases in blood pressure associated with diltiazem hydrochloride injection therapy may occasionally result in symptomatic hypotension (3.2%). The use of intravenous diltiazem for control of ventricular response in patients with supraventricular arrhythmias should be undertaken with caution when the patient is compromised hemodynamically. In addition, caution should be used in patients taking other drugs that decrease peripheral resistance, intravascular volume, myocardial contractility or conduction.
Acute Hepatic Injury
In rare instances, significant elevations in enzymes such as alkaline phosphatase, LDH, SGOT, SGPT, and other phenomena consistent with acute hepatic injury have been noted following oral diltiazem. Therefore, the potential for acute hepatic injury exists following administration of intravenous diltiazem.
Ventricular Premature Beats (VPBs)
VPBs may be present on conversion of PSVT to sinus rhythm with diltiazem hydrochloride injection. These VPBs are transient, are typically considered to be benign, and appear to have no clinical significance. Similar ventricular complexes have been noted during cardioversion, other pharmacologic therapy, and during spontaneous conversion of PSVT to sinus rhythm.
-
PRECAUTIONS
General
Diltiazem hydrochloride is extensively metabolized by the liver and excreted by the kidneys and in bile. The drug should be used with caution in patients with impaired renal or hepatic function (see WARNINGS). High intravenous dosages (4.5 mg/kg tid) administered to dogs resulted in significant bradycardia and alterations in AV conduction. In subacute and chronic dog and rat studies designed to produce toxicity, high oral doses of diltiazem were associated with hepatic damage. In special subacute hepatic studies, oral doses of 125 mg/kg and higher in rats were associated with histological changes in the liver, which were reversible when the drug was discontinued. In dogs, oral doses of 20 mg/kg were also associated with hepatic changes; however, these changes were reversible with continued dosing.
Dermatologic events progressing to erythema multiforme and/or exfoliative dermatitis have been infrequently reported following oral diltiazem. Therefore, the potential for these dermatologic reactions exists following exposure to intravenous diltiazem. Should a dermatologic reaction persist, the drug should be discontinued.
Drug Interactions
As with all drugs, care should be exercised when treating patients with multiple medications. Diltiazem is both a substrate and an inhibitor of the cytochrome P-450 3A4 enzyme system. Other drugs that are specific substrates, inhibitors, or inducers of this enzyme system may have a significant impact on the efficacy and side effect profile of diltiazem. Patients taking other drugs that are substrates of CYP450 3A4, especially patients with renal and/or hepatic impairment, may require dosage adjustment when starting or stopping concomitantly administered diltiazem in order to maintain optimum therapeutic blood levels.
ANESTHETICS
The depression of cardiac contractility, conductivity, and automaticity as well as the vascular dilation associated with anesthetics may be potentiated by calcium channel blockers. When used concomitantly, anesthetics and calcium blockers should be titrated carefully.
BENZODIAZEPINES
Studies showed that diltiazem increased the AUC of midazolam and triazolam by 3-4 fold and Cmaxby 2-fold, compared to placebo. The elimination half-life of midazolam and triazolam also increased (1.5 to 2.5 fold) during coadministration with diltiazem. These pharmacokinectic effects seen during diltiazem coadministration can result in increased clinical effects (e.g. prolonged sedation) of both midazolam and triazolam.
BETA-BLOCKERS
Intravenous diltiazem has been administered to patients on chronic oral beta-blocker therapy. The combination of the two drugs was generally well tolerated without serious adverse effects. If intravenous diltiazem is administered to patients receiving chronic oral beta-blocker therapy, the possibility for bradycardia, AV block, and/or depression of contractility should be considered (see CONTRAINDICATIONS). Oral administration of diltiazem with propranolol in five normal volunteers resulted in increased propranolol levels in all subjects and bioavailability of propranolol was increased approximately 50%. In vitro, propranolol appears to be displaced from its binding sites by diltiazem.
BUSPIRONE
In nine healthy subjects, diltiazem significantly increased the mean buspirone AUC 5.5 fold and Cmax 4.1 fold compared to placebo. The T1/2 and Tmax of buspirone were not significantly affected by diltiazem. Enhanced effects and increased toxicity of buspirone may be possible during concomitant administration with diltiazem. Subsequent dose adjustments may be necessary during coadministration, and should be based on clinical assessment.
CARBAMAZEPINE
Concomitant administration of oral diltiazem with carbamazepine has been reported to result in elevated plasma levels of carbamazepine (by 40 to 72%), resulting in toxicity in some cases. Patients receiving these drugs concurrently should be monitored for a potential drug interaction.
CIMETIDINE
A study in six healthy volunteers has shown a significant increase in peak diltiazem plasma levels (58%) and area-under-the-curve (53%) after a 1-week course of cimetidine at 1200 mg per day and a single dose of diltiazem 60 mg. Ranitidine produced smaller, nonsignificant increases. The effect may be mediated by cimetidine’s known inhibition of hepatic cytochrome P-450, the enzyme system responsible for the first-pass metabolism of diltiazem. Patients currently receiving diltiazem therapy should be carefully monitored for a change in pharmacological effect when initiating and discontinuing therapy with cimetidine. An adjustment in the diltiazem dose may be warranted.
CYCLOSPORINE
A pharmacokinetic interaction between diltiazem and cyclosporine has been observed during studies involving renal and cardiac transplant patients. In renal and cardiac transplant recipients, a reduction of cyclosporine dose ranging from 15% to 48% was necessary to maintain cyclosporine trough concentrations similar to those seen prior to the addition of diltiazem. If these agents are to be administered concurrently, cyclosporine concentrations should be monitored, especially when diltiazem therapy is initiated, adjusted or discontinued.
The effect of cyclosporine on diltiazem plasma concentrations has not been evaluated.
DIGITALIS
Intravenous diltiazem has been administered to patients receiving either intravenous or oral digitalis therapy. The combination of the two drugs was well tolerated without serious adverse effects. However, since both drugs affect AV nodal conduction, patients should be monitored for excessive slowing of the heart rate and/or AV block.
LOVASTATIN
In a ten-subject study, coadministration of diltiazem (120 mg bid, diltiazem SR) with lovastatin resulted in a 3 to 4 times increase in mean lovastatin AUC and Cmax versus lovastatin alone; no change in pravastatin AUC and Cmax was observed during diltiazem coadministration. Diltiazem plasma levels were not significantly affected by lovastatin or pravastatin.
QUINIDINE
Diltiazem significantly increases the AUC(0-∞) of quinidine by 51%, T1/2 by 36% and decreases its CLoral, by 33%. Monitoring for quinidine adverse effects may be warranted and the dose adjusted accordingly.
RIFAMPIN
Coadministration of rifampin with diltiazem lowered the diltiazem plasma concentrations to undetectable levels. Coadministration of diltiazem with rifampin or any known CYP3A4 inducer should be avoided when possible, and alternative therapy considered.
Carcinogenesis, Mutagenesis, Impairment of Fertility
A 24-month study in rats at oral dosage levels of up to 100 mg/kg/day, and a 21- month study in mice at oral dosage levels of up to 30 mg/kg/day showed no evidence of carcinogenicity. There was also no mutagenic response in vitro or in vivo in mammalian cell assays or in vitro in bacteria. No evidence of impaired fertility was observed in a study performed in male and female rats at oral dosages of up to 100 mg/kg/day.
Pregnancy
TERATOGENIC EFFECTS
Pregnancy Category C
Reproduction studies have been conducted in mice, rats and rabbits. Administration of oral doses ranging from five to ten times greater (on a mg/kg basis) than the daily recommended oral antianginal therapeutic dose has resulted in embryo and fetal lethality. These doses, in some studies, have been reported to cause skeletal abnormalities. In the perinatal/postnatal studies there was some reduction in early individual pup weights and survival rates. There was an increased incidence of stillbirths at doses of 20 times the human oral antianginal dose or greater.
There are no well-controlled studies in pregnant women; therefore, use diltiazem in pregnant women only if the potential benefit justifies the potential risk to the fetus.
Nursing Mothers
Diltiazem is excreted in human milk. One report with oral diltiazem suggests that concentrations in breast milk may approximate serum levels. If use of diltiazem is deemed essential, an alternative method of infant feeding should be instituted.
Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
Geriatric Use
Clinical studies of diltiazem did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
ATRIAL FIBRILLATION OR ATRIAL FLUTTER
In clinical studies with diltiazem hydrochloride for AF/FI, 135 of 257 patients were >65 years of age. No overall differences in safety or effectiveness were observed between these patients and younger patients, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
In subgroup analysis of double-blind and open-label trials following first-dose response, 116 patients >65 years of age had a response rate of 84%. One hundred two (102) patients <65 had a response rate of 78%. In subgroup analysis following a two-dose procedure in double-blind and open-label studies, 104 patients >65 years of age and 95 patients <65 both had a 95% response rate.
PAROXYSMAL SUPRAVENTRICULAR TACHYCARDIA
Clinical studies of diltiazem hydrochloride for PSVT did not include sufficient numbers of patients aged 65 and over to determine whether they respond differently from younger patients. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Diltiazem hydrochloride is extensively metabolized by the liver and excreted by the kidneys and in bile. The risk of toxic reactions to this drug may be greater in patients with impaired renal or hepatic function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function. As with all drugs, care should be exercised when treating patients with multiple medications. (See PRECAUTIONS, General and Drug Interactions.)
-
ADVERSE REACTIONS
The following adverse reaction rates are based on the use of diltiazem hydrochloride injection in over 400 domestic clinical trial patients with atrial fibrillation/flutter or PSVT under double-blind or open-label conditions. Worldwide experience in over 1300 patients was similar.
Adverse events reported in controlled and uncontrolled clinical trials were generally mild and transient. Hypotension was the most commonly reported adverse event during clinical trials. Asymptomatic hypotension occurred in 4.3% of patients. Symptomatic hypotension occurred in 3.2% of patients. When treatment for hypotension was required, it generally consisted of administration of saline or placing the patient in the Trendelenburg position. Other events reported in at least 1% of the diltiazem-treated patients were injection site reactions (e.g., itching, burning) - 3.9%, vasodilation (flushing) - 1.7%, and arrhythmia (junctional rhythm or isorhythmic dissociation) - 1%.
In addition, the following events were reported infrequently (less than 1%):
Cardiovascular
Asystole, atrial flutter, AV block first degree, AV block second degree, bradycardia, chest pain, congestive heart failure, sinus pause, sinus node dysfunction, syncope, ventricular arrhythmia, ventricular fibrillation, ventricular tachycardia.
Dermatologic
Pruritus, sweating.
Gastrointestinal
Constipation, elevated SGOT or alkaline phosphatase, nausea, vomiting.
Nervous System
Dizziness, paresthesia.
Other
Amblyopia, asthenia, dry mouth, dyspnea, edema, headache, hyperuricemia. Although not observed in clinical trials with diltiazem hydrochloride injection, the following events associated with oral diltiazem may occur.
CARDIOVASCULAR
AV block (third degree), bundle branch block, ECG abnormality, palpitations, syncope, tachycardia, ventricular extrasystoles.
DERMATOLOGIC
Alopecia, erythema multiforme (including Stevens-Johnson syndrome, toxic epidermal necrolysis), exfoliative dermatitis, leukocytoclastic vasculitis, petechiae, photosensitivity, purpura, rash, urticaria.
GASTROINTESTINAL
Anorexia, diarrhea, dysgeusia, dyspepsia, mild elevations of SGPT and LDH, thirst, weight increase.
NERVOUS SYSTEM
Abnormal dreams, amnesia, depression, extrapyramidal symptoms, gait abnormality, hallucinations, insomnia, nervousness, personality change, somnolence, tremor.
OTHER
Allergic reactions, angioedema (including facial or periorbital edema), CPK elevation, epistaxis, eye irritation, gingival hyperplasia, hemolytic anemia, hyperglycemia, impotence, increased bleeding time, leukopenia, muscle cramps, myopathy, nasal congestion, nocturia, osteoarticular pain, polyuria, retinopathy, sexual difficulties, thrombocytopenia, tinnitus.
Events such as myocardial infarction have been observed which are not readily distinguishable from the natural history of the disease for the patient.
-
OVERDOSAGE
Overdosage experience is limited. In the event of overdosage or an exaggerated response, appropriate supportive measures should be employed. The following measures may be considered:
Bradycardia
Administer atropine (0.6 to 1 mg). If there is no response to vagal blockade administer isoproterenol cautiously.
High-Degree AV Block
Treat as for bradycardia above. Fixed high-degree AV block should be treated with cardiac pacing.
Cardiac Failure
Administer inotropic agents (isoproterenol, dopamine, or dobutamine) and diuretics.
Hypotension
Vasopressors (e.g., dopamine or levarterenol bitartrate).
The effectiveness of intravenous calcium administration to reverse the pharmacological effects of diltiazem overdose has been inconsistent. In a few reported cases, overdose with calcium channel blockers associated with hypotension and bradycardia that was initially refractory to atropine became more responsive to atropine after the patients received intravenous calcium. In some cases intravenous calcium has been administered (1 g calcium chloride or 3 g calcium gluconate) over 5 minutes, and repeated every 10 to 20 minutes as necessary. Calcium gluconate has also been administered as a continuous infusion at a rate of 2 g per hour for 10 hours. Infusions of calcium for 24 hours or more may be required. Patients should be monitored for signs of hypercalcemia.
Actual treatment and dosage should depend on the severity of the clinical situation and the judgment and experience of the treating physician.
Diltiazem does not appear to be removed by peritoneal or hemodialysis. Limited data suggest that plasmapheresis or charcoal hemoperfusion may hasten diltiazem elimination following overdose.
The intravenous LD 50s in mice and rats were 60 and 38 mg/kg, respectively. The toxic dose in man is not known.
-
DOSAGE & ADMINISTRATION
Direct Intravenous Single Injections (Bolus)
The initial dose of diltiazem hydrochloride injection should be 0.25 mg/kg actual body weight as a bolus administered over 2 minutes (20 mg is a reasonable dose for the average patient). If response is inadequate, a second dose may be administered after 15 minutes. The second bolus dose of diltiazem hydrochloride injection should be 0.35 mg/kg actual body weight administered over 2 minutes (25 mg is a reasonable dose for the average patient). Subsequent intravenous bolus doses should be individualized for each patient. Patients with low body weights should be dosed on a mg/kg basis. Some patients may respond to an initial dose of 0.15 mg/kg, although duration of action may be shorter. Experience with this dose is limited.
Continuous Intravenous Infusion
For continued reduction of the heart rate (up to 24 hours) in patients with atrial fibrillation or atrial flutter, an intravenous infusion of diltiazem hydrochloride injection may be administered. Immediately following bolus administration of 20 mg (0.25 mg/kg) or 25 mg (0.35 mg/kg) diltiazem hydrochloride injection and reduction of heart rate, begin an intravenous infusion of diltiazem hydrochloride. The recommended initial infusion rate of diltiazem hydrochloride is 10 mg/h. Some patients may maintain response to an initial rate of 5 mg/h. The infusion rate may be increased in 5 mg/h increments up to 15 mg/h as needed, if further reduction in heart rate is required. The infusion may be maintained for up to 24 hours.
Diltiazem shows dose-dependent, non-linear pharmacokinetics. Duration of infusion longer than 24 hours and infusion rates greater than 15 mg/h have not been studied. Therefore, infusion duration exceeding 24 hours and infusion rates exceeding 15 mg/h are not recommended.
DILUTION
To prepare diltiazem hydrochloride injection for continuous intravenous infusion, aseptically transfer the appropriate quantity (see chart) of diltiazem hydrochloride injection to the desired volume of either Normal Saline, D5W, or D5W/0.45% NaCl. Mix thoroughly. Use within 24 hours. Keep refrigerated until use.
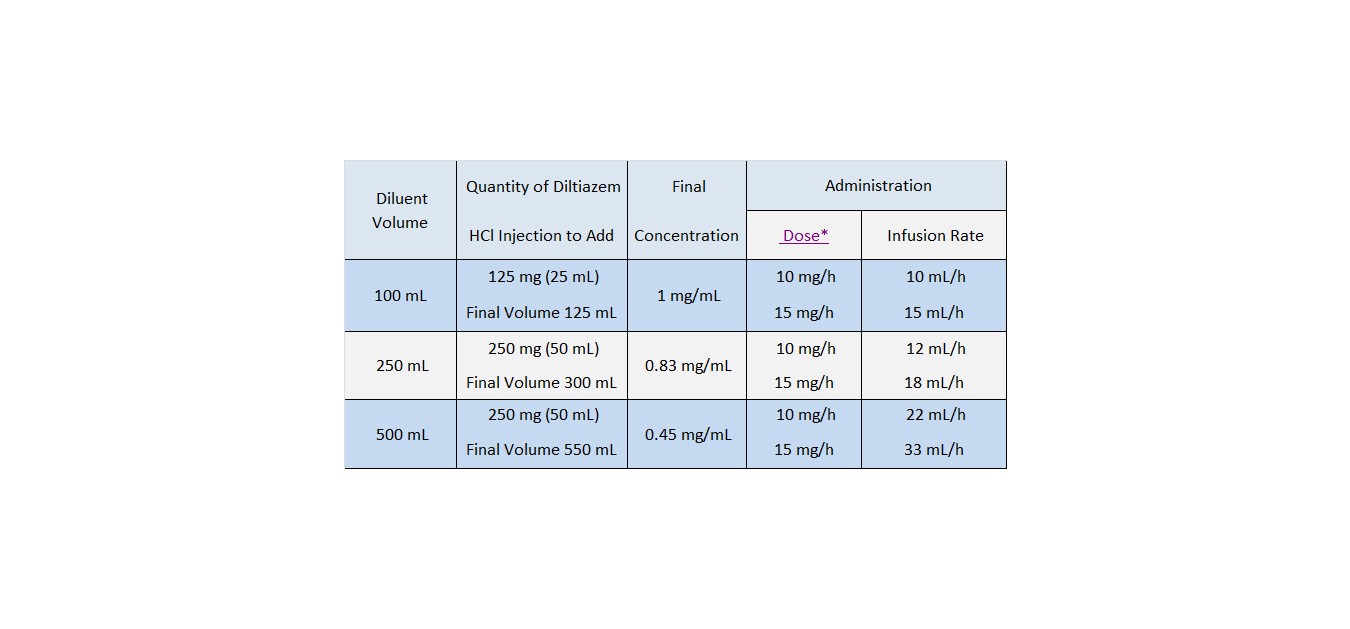
*
5 mg/h may be appropriate for some patientsCompatibility
Diltiazem hydrochloride injection was tested for compatibility with three commonly used intravenous fluids at a maximal concentration of 1 mg diltiazem hydrochloride per milliliter. Diltiazem hydrochloride injection was found to be physically compatible and chemically stable in the following parenteral solutions for at least 24 hours when stored in glass or polyvinylchloride (PVC) bags at controlled room temperature 15º-30°C (59°-86°F) or under refrigeration 2°-8°C (36°-46°F).
dextrose (5%) injection
sodium chloride (0.9%) injection
dextrose (5%) and sodium chloride (0.45%) injectionPhysical Incompatibilities
Because of potential physical incompatibilities, it is recommended that diltiazem hydrochloride not be mixed with any other drugs in the same container. If possible, it is recommended that diltiazem hydrochloride not be co-infused in the same intravenous line.
Physical incompatibilities (precipitate formation or cloudiness) were observed when diltiazem hydrochloride injection was infused in the same intravenous line with the following drugs: acetazolamide, acyclovir, aminophylline, ampicillin, ampicillin sodium/sulbactam sodium, cefamandole, cefoperazone, diazepam, furosemide, hydrocortisone sodium succinate, insulin (regular: 100 units/mL), methylprednisolone sodium succinate, mezlocillin, nafcillin, phenytoin, rifampin, and sodium bicarbonate.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
Transition to Further Antiarrhythmic Therapy
Transition to other antiarrhythmic agents following administration of diltiazem hydrochloride injection is generally safe. However, reference should be made to the respective agent manufacturer’s package insert for information relative to dosage and administration.
In controlled clinical trials, therapy with antiarrhythmic agents to maintain reduced heart rate in atrial fibrillation or atrial flutter or for prophylaxis of PSVT was generally started within 3 hours after bolus administration of diltiazem hydrochloride. These antiarrhythmic agents were intravenous or oral digoxin, Class 1 antiarrthythmics (e.g., quinidine, procainamide), calcium channel blockers, and oral beta-blockers.
Experience in the use of antiarrhythmic agents following maintenance infusion of diltiazem hydrochloride injection is limited. Patients should be dosed on an individual basis and reference should be made to the respective manufacturer’s package insert for information relative to dosage and administration.
-
HOW SUPPLIED
DILTIAZEM HCI INJECTION is supplied in the following dosage forms.
NDC 51662-1335-1
DILTIAZEM HCI INJECTION 25mg/5mL (5 mg/mL) 5mL VIALNDC 51662-1335-2
DILTIAZEM HCI INJECTION 25mg/5mL (5 mg/mL) 5mL VIAL IN A POUCHHF Acquisition Co LLC, DBA HealthFirst
Mukilteo, WA 98275SINGLE-DOSE VIALS. DISCARD UNUSED PORTION.
This product, including the packaging components, is free of latex.
Store diltiazem hydrochloride injection under refrigeration 2º-8ºC (36º-46ºF). DO NOT FREEZE. May be stored at room temperature for up to 1 month. Destroy after 1 month at room temperature.
- SPL UNCLASSIFIED
- PRINCIPAL DISPLAY PANEL-VIAL LABEL
- PRINCIPAL DISPLAY PANEL-LABEL ON VIAL
- PRINCIPAL DISPLAY PANEL-SERIALIZED LABELING
- PRINCIPAL DISPLAY PANEL, NDC 51662-1335-2 POUCH LABELING
-
INGREDIENTS AND APPEARANCE
DILTIAZEM HCI
diltiazem hci injectionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:51662-1335(NDC:0641-6013) Route of Administration INTRAVENOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength DILTIAZEM HYDROCHLORIDE (UNII: OLH94387TE) (DILTIAZEM - UNII:EE92BBP03H) DILTIAZEM HYDROCHLORIDE 5 mg in 1 mL Inactive Ingredients Ingredient Name Strength ANHYDROUS CITRIC ACID (UNII: XF417D3PSL) 0.75 mg in 1 mL SODIUM HYDROXIDE (UNII: 55X04QC32I) SODIUM CITRATE (UNII: 1Q73Q2JULR) 0.65 mg in 1 mL WATER (UNII: 059QF0KO0R) HYDROCHLORIC ACID (UNII: QTT17582CB) SORBITOL (UNII: 506T60A25R) 50 mg in 1 mL Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:51662-1335-1 5 mL in 1 VIAL; Type 0: Not a Combination Product 12/21/2018 2 NDC:51662-1335-2 1 in 1 POUCH 01/19/2023 2 5 mL in 1 VIAL; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA078538 12/21/2018 Labeler - HF Acquisition Co LLC, DBA HealthFirst (045657305) Registrant - HF Acquisition Co LLC, DBA HealthFirst (045657305) Establishment Name Address ID/FEI Business Operations HF Acquisition Co LLC, DBA HealthFirst 045657305 relabel(51662-1335)