Label: AMOXICILLIN capsule
-
Contains inactivated NDC Code(s)
NDC Code(s): 10544-619-21, 10544-619-30, 10544-619-42 - Packager: Blenheim Pharmacal, Inc.
- This is a repackaged label.
- Source NDC Code(s): 0143-9939
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: None
- Marketing Status: Abbreviated New Drug Application
Drug Label Information
Updated October 18, 2010
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
Formulations of amoxicillin capsules contain amoxicillin, a semisynthetic antibiotic, an analog of ampicillin, with a broad spectrum of bactericidal activity against many gram-positive and gram-negative microorganisms. Chemically it is (2 S, 5 R, 6 R)-6-[(R)-(-)-2-amino-2-(p-hydroxyphenyl) acetamido]-3,3-dimethyl-7-oxo-4-thia-1-azabicyclo [3.2.0] heptane-2-carboxylic acid trihydrate. It may be represented structurally as:
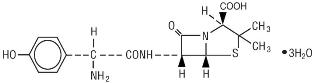
Structural Formula
The amoxicillin molecular formula is C16H19N3O5S•3H2O, and the molecular weight is 419.45.
Each amoxicillin capsule USP, for oral administration, contains either 250 mg or 500 mg of amoxicillin as the trihydrate. In addition, the capsules also contain the following inactive ingredients: croscarmellose sodium, gelatin, magnesium stearate, titanium dioxide, and yellow iron oxide. Additionally, the 250 mg capsules contain black iron oxide and red iron oxide. The 250 mg capsule with caramel cap and ivory body is imprinted with West-ward 938, while the 500 mg capsule with ivory cap and ivory body is imprinted with West-ward 939.
-
CLINICAL PHARMACOLOGY
Amoxicillin is stable in the presence of gastric acid and is rapidly absorbed after oral administration. Amoxicillin diffuses readily into most body tissues and fluids, with the exception of brain and spinal fluid, except when meninges are inflamed. The half-life of amoxicillin is 61.3 minutes. Most of the amoxicillin is excreted unchanged in the urine; its excretion can be delayed by concurrent administration of probenecid. In blood serum, amoxicillin is approximately 20% protein-bound.
Orally administered doses of 250 mg and 500 mg amoxicillin capsules result in average peak blood levels 1 to 2 hours after administration in the range of 3.5 mcg/mL to 5 mcg/mL and 5.5 mcg/mL to 7.5 mcg/mL, respectively.
Microbiology:
Amoxicillin is similar to ampicillin in its bactericidal action against susceptible organisms during the stage of active multiplication. It acts through the inhibition of biosynthesis of cell wall mucopeptide. Amoxicillin has been shown to be active against most strains of the following microorganisms, both in vitro and in clinical infections as described in the INDICATIONS AND USAGE section.
Aerobic Gram-Positive Microorganisms:
Enterococcus faecalis
Staphylococcus spp.* (β-lactamase–negative strains only)
Streptococcus pneumoniae
Streptococcus spp. (α- and β-hemolytic strains only)
* Staphylococci which are susceptible to amoxicillin but resistant to methicillin/oxacillin should be considered as resistant to amoxicillin.Aerobic Gram-Negative Microorganisms:
Escherichia coli (β-lactamase–negative strains only)
Haemophilus influenzae (β-lactamase–negative strains only)
Neisseria gonorrhoeae (β-lactamase–negative strains only)
Proteus mirabilis (β-lactamase–negative strains only)Helicobacter:
Helicobacter pyloriSusceptibility Tests:
Dilution Techniques: Quantitative methods are used to determine antimicrobial minimum inhibitory concentrations (MICs). These MICs provide estimates of the susceptibility of bacteria to antimi-crobial compounds. The MICs should be determined using a standardized procedure. Standardized procedures are based on a dilution method1 (broth or agar) or equivalent with standardized inoculum concentrations and standardized concentrations of ampicillin powder. Ampicillin is sometimes used to predict susceptibility of S. pneumoniae to amoxicillin; however, some intermediate strains have been shown to be susceptible to amoxicillin. Therefore, S. pneumoniae susceptibility should be tested using amoxicillin powder.
The MIC values should be interpreted according to the following criteria:
For Gram-Positive Aerobes:
Enterococcus MIC (mca /mL) Interpretation ≤ 8 Susceptible (S) ≥ 16 Resistant (R) Staphylococcusa MIC (mca /mL) Interpretation ≤ 0.25 Susceptible (S) ≥ 0.5 Resistant (R) Streptococcus (except S. pneumoniae) MIC (mca /mL) Interpretation ≤ 0.25 Susceptible (S) 0.5 to 4 Intermediate (I) ≥ 8 Resistant (R) S. pneumoniaeb from non-meningitis sources. (Amoxicillin powder should be used to determine susceptibility.) MIC (mca /mL) Interpretation ≤ 2 Susceptible (S) 4 Intermediate (I) ≥ 8 Resistant (R) NOTE: These interpretive criteria are based on the recommended doses for respiratory tract infections.
For Gram-Negative Aerobes:
Enterobacteriaceae MIC (mca /mL) Interpretation ≤ 8 Susceptible (S) 16 Intermediate (I) ≥ 32 Resistant (R) H. influenzaec a. Staphylococci which are susceptible to amoxicillin but resistant to methicillin/oxacillin should be considered as resistant to amoxicillin.
b. These interpretive standards are applicable only to broth microdilution susceptibility tests using cation-adjusted Mueller-Hinton broth with 2-5% lysed horse blood. c. These interpretive standards are applicable only to broth microdilution test with H. influenzae using Haemophilus Test Medium (HTM).1 MIC (mcg/mL) Interpretation ≤ 1 Susceptible (S) 2 Intermediate (I) ≥ 4 Resistant (R) A report of “Susceptible” indicates that the pathogen is likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable. A report of “Intermediate” indicates that the result should be considered equivocal, and, if the microorganism is not fully susceptible to alternative, clinically feasible drugs, the test should be repeated. This category implies possible clinical applicability in body sites where the drug is physiologically concentrated or in situations where high dosage of drug can be used. This category also provides a buffer zone, which prevents small uncontrolled technical factors from causing major discrepancies in interpretation. A report of “Resistant” indicates that the pathogen is not likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable; other therapy should be selected.
Standardized susceptibility test procedures require the use of laboratory control microorganisms to control the technical aspects of the laboratory procedures.
Standard ampicillin powder should provide the following MIC values:
Microorganism MIC (mcg /mL) E. coli ATCC 25922 2 to 8 E. faecalis ATCC 29212 0.5 to 2 H. influenzae ATCC 49247d 2 to 8 S. aureus ATCC 29213 0.25 to 1 Using amoxicillin to determine susceptibility:
d. This quality control range is applicable to only H. influenzae ATCC 49247 tested by a broth microdilution procedure using HTM. 1
e. This quality control range is applicable to only S. pneumoniae ATCC 49619 tested by the broth microdilution procedure using cation-adjusted Mueller-Hinton broth with 2-5% lysed horse blood. Microorganism MIC Range (mcg /mL) S. pneumoniae ATCC 49619e 0.03 to 0.12 Diffusion Techniques: Quantitative methods that require measurement of zone diameters also provide reproducible estimates of the susceptibility of bacteria to antimicrobial compounds. One such standardized procedure2 requires the use of standardized inoculum concentrations. This procedure uses paper disks impregnated with 10 mcg ampicillin to test the susceptibility of microorganisms, except S. pneumoniae, to amoxicillin. Interpretation involves correlation of the diameter obtained in the disk test with the MIC for ampicillin.
Reports from the laboratory providing results of the standard single-disk susceptibility test with a 10 mcg ampicillin disk should be interpreted according to the following criteria:
For gram-positive aerobes:
Enterococcus Zone Diameter (mm) Interpretation ≥ 17 Susceptible (S) ≤ 16 Resistant (R) Staphylococcusf Zone Diameter (mm) Interpretation ≥ 29 Susceptible (S) ≤ 28 Resistant (R) β-hemolytic streptococci Zone Diameter (mm) Interpretation ≥ 26 Susceptible (S) 19 to 25 Intermediate (I) ≤ 18 Resistant (R) NOTE: For streptococci (other than β-hemolytic streptococci and S. pneumoniae), an ampicillin MIC should be determined.
S. pneumoniae
S. pneumoniae should be tested using a 1 mcg oxacillin disk. Isolates with oxacillin zone sizes of ≥ 20 mm are susceptible to amoxicillin. An amoxicillin MIC should be determined on isolates of S. pneumoniae with oxacillin zone sizes of ≤ 19 mm.For gram-negative aerobes:
Enterobacteriaceae Zone Diameter (mm) Interpretation ≥17 Susceptible (S) 14 to 16 Intermediate (I) ≤13 Resistant (R) H. influenzaeg f. Staphylococci which are susceptible to amoxicillin but resistant to methicillin/oxacillin should be considered as resistant to amoxicillin.
g. These interpretive standards are applicable only to disk diffusion susceptibility tests with H. influenzae using Haemophilus Test Medium (HTM).2 Zone Diameter (mm) Interpretation ≥ 22 Susceptible (S) 19 to 21 Intermediate fl) ≤18 Resistant (R) Interpretation should be as stated above for results using dilution techniques.
As with standard dilution techniques, disk diffusion susceptibility test procedures require the use of laboratory control microorganisms. The 10 mcg ampicillin disk should provide the following zone diameters in these laboratory test quality control strains:
Microorqanism Zone Diameter (mm) E. coli ATCC 25922 16 to 22 H. influenzae ATCC 49247h 13 to 21 S. aureus ATCC 25923 27 to 35 Using 1 mcg oxacillin disk:
h. This quality control range is applicable to only H. influenzae ATCC 49247 tested by a disk diffusion procedure using HTM.2
i. This quality control range is applicable to only S. pneumoniae ATCC 49619 tested by a disk diffusion procedure using Mueller-Hinton agar supplemented with 5% sheep blood and incubated in 5% CO2. Microorganism Zone Diameter (mm) S. pneumoniae ATCC 49619i 8 to 12 Susceptibility testing for Helicobacter pylori:
In vitro susceptibility testing methods and diagnostic products currently available for determining minimum inhibitory concentrations (MICs) and zone sizes have not been standardized, validated, or approved for testing H. pylori microorganisms.
Culture and susceptibility testing should be obtained in patients who fail triple therapy. If clarithromycin resistance is found, a non-clarithromycin-containing regimen should be used.
-
INDICATIONS AND USAGE
To reduce the development of drug-resistant bacteria and maintain the effectiveness of amoxicillin and other antibacterial drugs, amoxicillin should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Amoxicillin is indicated in the treatment of infections due to susceptible (ONLY β-lactamase–negative) strains of the designated microorganisms in the conditions listed below:
Infections of the ear, nose, and throat –due to Streptococcus spp. (α- and β-hemolytic strains only), Streptococcus pneumoniae, Staphylococcus spp., or H. influenzae.
Infections of the genitourinary tract – due to E. coli, P. mirabilis, or E. faecalis.
Infections of the skin and skin structure – due to Streptococcus spp. (α- and β-hemolytic strains only), Staphylococcus spp., or E. coli.
Infections of the lower respiratory tract due to Streptococcus spp. (α- and β-hemolytic strains only), S. pneumoniae, Staphylococcus spp., or H. influenzae.Gonorrhea, acute uncomplicated (ano-genital and urethral infections) due to N. gonorrhoeae (males and females).
H. pylori eradication to reduce the risk of duodenal ulcer recurrence
Triple therapy: Amoxicillin /clarithromycin/lansoprazole
Amoxicillin, in combination with clarithromycin plus lansoprazole as triple therapy, is indicated for the treatment of patients with H. pylori infection and duodenal ulcer disease (active or 1-year history of a duodenal ulcer) to eradicate H. pylori. Eradication of H. pylori has been shown to reduce the risk of duodenal ulcer recurrence. (See CLINICAL STUDIES and DOSAGE AND ADMINISTRATION.)Dual therapy: Amoxicillin/lansoprazole
Amoxicillin, in combination with lansoprazole delayed-release capsules as dual therapy, is indicated for the treatment of patients with H. pylori infection and duodenal ulcer disease (active or 1-year history of a duodenal ulcer) who are either allergic or intolerant to clarithromycin or in whom resistance to clarithromycin is known or suspected. (See the clarithromycin package insert, MICROBIOLOGY.) Eradication of H. pylori has been shown to reduce the risk of duodenal ulcer recurrence. (See CLINICAL STUDIES and DOSAGE AND ADMINISTRATION.)Indicated surgical procedures should be performed.
- CONTRAINDICATIONS
-
WARNINGS
SERIOUS AND OCCASIONALLY FATAL HYPERSENSITIVITY (ANAPHYLACTIC) REACTIONS HAVE BEEN REPORTED IN PATIENTS ON PENICILLIN THERAPY. ALTHOUGH ANAPHYLAXIS IS MORE FREQUENT FOLLOWING PARENTERAL THERAPY, IT HAS OCCURRED IN PATIENTS ON ORAL PENICILLINS. THESE REACTIONS ARE MORE LIKELY TO OCCUR IN INDIVIDUALS WITH A HISTORY OF PENICILLIN HYPERSENSITIVITY AND/OR A HISTORY OF SENSITIVITY TO MULTIPLE ALLERGENS. THERE HAVE BEEN REPORTS OF INDIVIDUALS WITH A HISTORY OF PENICILLIN HYPERSENSITIVITY WHO HAVE EXPERIENCED SEVERE REACTIONS WHEN TREATED WITH CEPHALOSPORINS. BEFORE INITIATING THERAPY WITH AMOXICILLIN, CAREFUL INQUIRY SHOULD BE MADE CONCERNING PREVIOUS HYPERSENSITIVITY REACTIONS TO PENICILLINS, CEPHALOSPORINS, OR OTHER ALLERGENS. IF AN ALLERGIC REACTION OCCURS, AMOXICILLIN SHOULD BE DISCONTINUED AND APPROPRIATE THERAPY INSTITUTED. SERIOUS ANAPHYLACTIC REACTIONS REQUIRE IMMEDIATE EMERGENCY TREATMENT WITH EPINEPHRINE. OXYGEN, INTRAVENOUS STEROIDS, AND AIRWAY MANAGEMENT, INCLUDING INTUBATION, SHOULD ALSO BE ADMINISTERED AS INDICATED.
Pseudomembranous colitis has been reported with nearly all antibacterial agents, including amoxicillin, and may range in severity from mild to life-threatening. Therefore, it is important to consider this diagnosis in patients who present with diarrhea subsequent to the administration of antibacterial agents.
Treatment with antibacterial agents alters the normal flora of the colon and may permit overgrowth of clostridia. Studies indicate that a toxin produced by Clostridium difficile is a primary cause of “antibiotic-associated colitis.”
After the diagnosis of pseudomembranous colitis has been established, appropriate therapeutic measures should be initiated. Mild cases of pseudomembranous colitis usually respond to drug discontinuation alone. In moderate-to-severe cases, consideration should be given to management with fluids and electrolytes, protein supplementation, and treatment with an antibacterial drug clinically effective against C. difficile colitis.
-
PRECAUTIONS
General:
The possibility of superinfections with mycotic or bacterial pathogens should be kept in mind during therapy. If superinfections occur, amoxicillin should be discontinued and appropriate therapy instituted.
Prescribing amoxicillin in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
Laboratory Tests:
As with any potent drug, periodic assessment of renal, hepatic, and hematopoietic function should be made during prolonged therapy.
All patients with gonorrhea should have a serologic test for syphilis at the time of diagnosis. Patients treated with amoxicillin should have a follow-up serologic test for syphilis after 3 months.
Drug Interactions:
Probenecid decreases the renal tubular secretion of amoxicillin. Concurrent use of amoxicillin and probenecid may result in increased and prolonged blood levels of amoxicillin.
Chloramphenicol, macrolides, sulfonamides, and tetracyclines may interfere with the bactericidal effects of penicillin. This has been demonstrated in vitro; however, the clinical significance of this interaction is not well documented.
Drug/Laboratory Test Interactions:
High urine concentrations of ampicillin may result in false-positive reactions when testing for the presence of glucose in urine using Clinitest®, Benedict's Solution, or Fehling's Solution. Since this effect may also occur with amoxicillin, it is recommended that glucose tests based on enzymatic glucose oxidase reactions (such as Clinistix®) be used.
Following administration of ampicillin to pregnant women, a transient decrease in plasma concentration of total conjugated estriol, estriol-glucuronide, conjugated estrone, and estradiol has been noted. This effect may also occur with amoxicillin.
Carcinogenesis, Mutagenesis, Impairment of Fertility:
Long-term studies in animals have not been performed to evaluate carcinogenic potential. Studies to detect mutagenic potential of amoxicillin alone have not been conducted; however, the following information is available from tests on a 4:1 mixture of amoxicillin and potassium clavulanate (AUGMENTIN). AUGMENTIN was non-mutagenic in the Ames bacterial mutation assay, and the yeast gene conversion assay. AUGMENTIN was weakly positive in the mouse lymphoma assay, but the trend toward increased mutation frequencies in this assay occurred at doses that were also associated with decreased cell survival. AUGMENTIN was negative in the mouse micronucleus test, and in the dominant lethal assay in mice. Potassium clavulanate alone was tested in the Ames bacterial mutation assay and in the mouse micronucleus test, and was negative in each of these assays. In a multi-generation reproduction study in rats, no impairment of fertility or other adverse reproductive effects were seen at doses up to 500 mg/kg (approximately 3 times the human dose in mg/m2).
Pregnancy:Teratogenic Effects:
Pregnancy Category B. Reproduction studies have been performed in mice and rats at doses up to 10 times the human dose and have revealed no evidence of impaired fertility or harm to the fetus due to amoxicillin. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
Labor and Delivery:
Oral ampicillin-class antibiotics are poorly absorbed during labor. Studies in guinea pigs showed that intravenous administration of ampicillin slightly decreased the uterine tone and frequency of contractions but moderately increased the height and duration of contractions. However, it is not known whether use of amoxicillin in humans during labor or delivery has immediate or delayed adverse effects on the fetus, prolongs the duration of labor, or increases the likelihood that forceps delivery or other obstetrical intervention or resuscitation of the newborn will be necessary.
Nursing Mothers:
Penicillins have been shown to be excreted in human milk. Amoxicillin use by nursing mothers may lead to sensitization of infants. Caution should be exercised when amoxicillin is administered to a nursing woman.
Pediatric Use:
Because of incompletely developed renal function in neonates and young infants, the elimination of amoxicillin may be delayed. Dosing of amoxicillin should be modified in pediatric patients 12 weeks or younger (≤ 3 months). (See DOSAGE AND ADMINISTRATION — Neonates and infants.)
Geriatric Use:
An analysis of clinical studies of amoxicillin was conducted to determine whether subjects aged 65 and over respond differently from younger subjects. Of the 1,811 subjects treated with capsules of amoxicillin, 85% were < 60 years old, 15% were ≥ 61 years old and 7% were ≥ 71 years old. This analysis and other reported clinical experience have not identified differences in responses between the elderly and younger patients, but a greater sensitivity of some older individuals cannot be ruled out.
This drug is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and may be useful to the monitor renal function.
Information for Patients:
Amoxicillin may be taken every 8 hours or every 12 hours, depending on the strength of the product prescribed.
Patients should be counseled that antibacterial drugs, including amoxicillin, should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When amoxicillin is prescribed to treat a bacterial infection, patients should be told that although it is common to feel better early in the course of therapy, the medication should be taken exactly as directed. Skipping doses or not completing the full course of therapy may: (1) decrease the effectiveness of the immediate treatment, and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by amoxicillin or other antibacterial drugs in the future.
-
ADVERSE REACTIONS
As with other penicillins, it may be expected that untoward reactions will be essentially limited to sensitivity phenomena. They are more likely to occur in individuals who have previously demonstrated hypersensitivity to penicillins and in those with a history of allergy, asthma, hay fever, or urticaria. The following adverse reactions have been reported as associated with the use of penicillins:
Gastrointestinal: Nausea, vomiting, diarrhea, and hemorrhagic / pseudomembranous colitis.
Onset of pseudomembranous colitis symptoms may occur during or after antibiotic treatment. (See WARNINGS.)
Hypersensitivity Reactions: Serum sickness–like reactions, erythematous maculopapular rashes, erythema multiforme, Stevens-Johnson syndrome, exfoliative dermatitis, toxic epidermal necrolysis, acute generalized exanthematous pustulosis, hypersensitivity vasculitis and urticaria have been reported.
NOTE: These hypersensitivity reactions may be controlled with antihistamines and, if necessary, systemic corticosteroids. Whenever such reactions occur, amoxicillin should be discontinued unless, in the opinion of the physician, the condition being treated is life-threatening and amenable only to amoxicillin therapy.
Liver: A moderate rise in AST (SGOT) and/or ALT (SGPT) has been noted, but the significance of this finding is unknown. Hepatic dysfunction including cholestatic jaundice, hepatic cholestasis and acute cytolytic hepatitis have been reported.
Renal: Crystalluria has also been reported (see OVERDOSAGE)
Hemic and Lymphatic Systems: Anemia, including hemolytic anemia, thrombocytopenia, thrombocytopenic purpura, eosinophilia, leukopenia, and agranulocytosis have been reported during therapy with penicillins. These reactions are usually reversible on discontinuation of therapy and are believed to be hypersensitivity phenomena.
Central Nervous System: Reversible hyperactivity, agitation, anxiety, insomnia, confusion, convulsions, behavioral changes, and/or dizziness have been reported rarely.
Miscellaneous: Tooth discoloration (brown, yellow, or gray staining) has been rarely reported. Most reports occurred in pediatric patients. Discoloration was reduced or eliminated with brushing or dental cleaning in most cases.
Combination therapy with clarithromycin and lansoprazole:
In clinical trials using combination therapy with amoxicillin plus clarithromycin and lansoprazole, and amoxicillin plus lansoprazole, no adverse reactions peculiar to these drug combinations were observed. Adverse reactions that have occurred have been limited to those that had been previously reported with amoxicillin, clarithromycin, or lansoprazole.Triple therapy: amoxicillin/clarithromycin/lansoprazole:
The most frequently reported adverse events for patients who received triple therapy were diarrhea (7%), headache (6%), and taste perversion (5%). No treatment-emergent adverse events were observed at significantly higher rates with triple therapy than with any dual therapy regimen.
Dual therapy: Amoxicillin/lansoprazole:
The most frequently reported adverse events for patients who received amoxicillin 3 times daily plus lansoprazole three times daily dual therapy were diarrhea (8%) and headache (7%). No treatment-emergent adverse events were observed at significantly higher rates with amoxicillin 3 times daily plus lansoprazole 3 times daily dual therapy than with lansoprazole alone.
For more information on adverse reactions with clarithromycin or lansoprazole, refer to their package inserts, ADVERSE REACTIONS.
-
OVERDOSAGE
In case of overdosage, discontinue medication, treat symptomatically, and institute supportive measures as required. If the overdosage is very recent and there is no contraindication, an attempt at emesis or other means of removal of drug from the stomach may be performed. A prospective study of 51 pediatric patients at a poison-control center suggested that overdosages of less than 250 mg/kg of amoxicillin are not associated with significant clinical symptoms and do not require gastric emptying.3
Interstitial nephritis resulting in oliguric renal failure has been reported in a small number of patients after over-dosage with amoxicillin.
Crystalluria, in some cases leading to renal failure, has also been reported after amoxicillin overdosage in adult and pediatric patients. In case of overdosage, adequate fluid intake and diuresis should be maintained to reduce the risk of amoxicillin crystalluria.
Renal impairment appears to be reversible with cessation of drug administration. High blood levels may occur more readily in patients with impaired renal function because of decreased renal clearance of amoxicillin. Amoxicillin may be removed from circulation by hemodialysis.
-
DOSAGE AND ADMINISTRATION
Amoxicillin capsules may be given without regard to meals. However, food effect studies have not been performed with the 500 mg formulation.
Neonates and infants aged ≤ 12 weeks (≤ 3 months):
Due to incompletely developed renal function affecting elimination of amoxicillin in this age group, the recommended upper dose of amoxicillin is 30 mg/kg/day divided q12h.
Adults and pediatric patients >3 months: * Dosing for infections caused by less susceptible organisms should follow the recommendations for severe infections.
† The children's dosage is intended for individuals whose weight is less than 40 kg. Children weighing 40 kg or more should be dosed according to the adult recommendations. Infection Severity* Usual Usual Dose Adult Dose for Children >3 months† Ear/nose/throat Mild/Moderate 500 mg 25 mg/kg/day every 12 hours in divided doses or every 12 hours 250 mg or every 8 hours 20 mg/kg/day in divided doses every 8 hours Severe 875 mg 45 mg/kg/day every 12 hours in divided doses or every 12 hours 500 mg or every 8 hours 40 mg/kg/day in divided doses every 8 hours Lower respiratory Mild/Moderate 875 mg 45 mg/kg/day Tract or Severe every 12 hours in divided doses or every 12 hours 500 mg every or 8 hours 40 mg/kg/day in divided doses every 8 hours Skin/Skin Mild/Moderate 500 mg 25 mg/kg/day Structure every 12 hours in divided doses or every 12 hours 250 mg every or 8 hours 20 mg/kg/day in divided doses every 8 hours Severe 875 mg 45 mg/kg/day every 12 hours in divided doses or every 12 hours 500 mg every or 8 hours 40 mg/kg/day in divided doses every 8 hours Genitourinary Mild/Moderate 500 mg 25 mg/kg/day Tract every 12 hours in divided doses or every 12 hours 250 mg every or 8 hours 20 mg/kg/day in divided doses every 8 hours Severe 875 mg 45 mg/kg/day every 12 hours in divided doses or every 12 hours 500 mg or every 8 hours 40 mg/kg/day in divided doses every 8 hours Gonorrhea 3 grams Prepubertal Acute, as children: uncomplicated single oral dose 50 mg/kg ano-genital and amoxicillin combined with 25 mg/kg probenecid urethral infections as a single dose. in males and NOTE: SINCE females PROBENECID IS CONTRAINDICATED IN CHILDREN UNDER 2 YEARS. DO NOT USE
THIS REGIMENIN THESE CASES. All patients with gonorrhea should be evaluated for syphilis. (See PRECAUTIONS - Laboratory Tests.)
Larger doses may be required for stubborn or severe infections.
General:
It should be recognized that in the treatment of chronic urinary tract infections, frequent bacteriological and clinical appraisals are necessary. Smaller doses than those recommended above should not be used. Even higher doses may be needed at times. In stubborn infections, therapy may be required for several weeks. It may be necessary to continue clinical and/or bacteriological follow-up for several months after cessation of therapy. Except for gonorrhea, treatment should be continued for a minimum of 48 to 72 hours beyond the time that the patient becomes asymptomatic or evidence of bacterial eradication has been obtained. It is recommended that there be at least 10 days' treatment for any infection caused by Streptococcus pyogenes to prevent the occurrence of acute rheumatic fever.
H. pylori eradication to reduce the risk of duodenal ulcer recurrence:
Triple therapy:
Amoxicillin/clarithromycin/lansoprazole
The recommended adult oral dose is 1 gram amoxicillin, 500 mg clarithromycin, and 30 mg lansoprazole, all given twice daily (q12h) for 14 days. (See INDICATIONS AND USAGE.)
Dual therapy:
Amoxicillin/lansoprazole
The recommended adult oral dose is 1 gram amoxicillin and 30 mg lansoprazole, each given three times daily (q8h) for 14 days. (See INDICATIONS AND USAGE.)
Please refer to clarithromycin and lansoprazole full prescribing information for CONTRAINDICATIONS and WARNINGS, and for information regarding dosing in elderly and renally impaired patients.
Dosing recommendations for adults with impaired renal function:
Patients with impaired renal function do not generally require a reduction in dose unless the impairment is severe. Severely impaired patients with a glomerular filtration rate of <30 mL/min. should not receive the 875-mg tablet. Patients with a glomerular filtration rate of 10 to 30 mL/min. should receive 500 mg or 250 mg every 12 hours, depending on the severity of the infection. Patients with a less than 10 mL/minute glomerular filtration rate should receive 500 mg or 250 mg every 24 hours, depending on severity of the infection.
Hemodialysis patients should receive 500 mg or 250 mg every 24 hours, depending on severity of the infection. They should receive an additional dose both during and at the end of dialysis.
There are currently no dosing recommendations for pediatric patients with impaired renal function.
-
HOW SUPPLIED
Capsules:
Amoxicillin Capsules USP, 500 mg are available as ivory cap and ivory body. The cap of the 500 mg capsule is imprinted with West-ward and the body with 939.Amoxicillin capsules USP, 250 mg, are available as caramel cap and ivory body. The cap of the 250 mg capsule is imprinted with West-ward and the body with 938.
Amoxicillin capsules USP, 250 mg are available in:
- Bottles of 100
- Bottles of 500
Amoxicillin capsules USP, 500 mg are available in:
- Bottles of 100
- Bottles of 500
Store at 20°- 25°C (68°- 77°F) [See USP Controlled Room Temperature]. Dispense in a tight container.
-
CLINICAL STUDIES
H. pylori eradication to reduce the risk of duodenal ulcer recurrence:
Randomized, double-blind clinical studies performed in the United States in patients with H. pylori and duodenal ulcer disease (defined as an active ulcer or history of an ulcer within 1 year) evaluated the efficacy of lansoprazole in combination with amoxicillin capsules and clarithromycin tablets as triple 14-day therapy, or in combination with amoxicillin capsules as dual 14-day therapy, for the eradication of H. pylori. Based on the results of these studies, the safety and efficacy of 2 different eradication regimens were established:
Triple therapy: Amoxicillin 1 gram twice daily/clarithromycin 500 mg twice daily/lansoprazole 30 mg twice daily.
Dual therapy: Amoxicillin 1 gram three times daily/lansoprazole 30 mg 3 times daily.
All treatments were for 14 days. H. pylori eradication was defined as 2 negative tests (culture and histology) at 4 to 6 weeks following the end of treatment.
Triple therapy was shown to be more effective than all possible dual therapy combinations. Dual therapy was shown to be more effective than both monotherapies.
Eradication of H. pylori has been shown to reduce the risk of duodenal ulcer recurrence.
H. pylori Eradication Rates – Triple Therapy (amoxicillin/ clarithromycin /lansoprazole) Percent of Patients Cured [95% Confidence Interval] (Number of Patients) * This analysis was based on evaluable patients with confirmed duodenal ulcer (active or within one year) and H. pylori infection at baseline defined as at least two of three positive endoscopic tests from CLOtest®, (Delta West Ltd., Bentley, Australia), histology, and/or culture. Patients were included in the analysis if they completed the study. Additionally, if patients dropped out of the study due to an adverse event related to the study drug, they were included in the analysis as failures of therapy.
† Patients were included in the analysis if they had documented H. pylori infection at baseline as defined above and had a confirmed duodenal ulcer (active or within one year). All dropouts were included as failures of therapy. ‡ (p<0.05) versus lansoprazole/amoxicillin and lansoprazole/clarithromycin dual therapy. § (p<0.05) versus clarithromycin/amoxicillin dual therapy. Study Triple Therapy Triple Therapy Evaluable Analysis* Intent-to-Treat
Analysis†Study 1 92‡ 86‡ [80 - 97.7] [73.3 - 93.5] (n = 48) (n = 55) Study 2 86§ 83§ [75.7 - 93.6] [72 - 90.8] (n = 66) (n = 70) H. pylori Eradication Rates – Dual Therapy (amoxicillin/lansoprazole) Percent of Patients Cured [95% Confidence Interval] (Number of Patients) * This analysis was based on evaluable patients with confirmed duodenal ulcer (active or within one year) and H. pylori infection at baseline defined as at least two of three positive endoscopic tests from CLOtest®, histology, and/or culture. Patients were included in the analysis if they completed the study. Additionally, if patients dropped out of the study due to an adverse event related to the study drug, they were included in the analysis as failures of therapy. † Patients were included in the analysis if they had documented H. pylori infection at baseline as defined above and had a confirmed duodenal ulcer (active or within one year). All dropouts were included as failures of therapy. ‡ (p<0.05) versus lansoprazole alone. § (p<0.05) versus lansoprazole alone or amoxicillin alone. Study Dual Therapy Dual Therapy Evaluable Analysis* Intent-to-Treat Analysis† Study 1 77‡ 70‡ [62.5 - 87.2] [56.8 - 81.2] (n = 51) (n = 60) Study 2 66§ 61§ [51.9 - 77.5] [48.5 - 72.9] (n = 58) (n = 67) -
REFERENCES
- National Committee for Clinical Laboratory Standards. Methods for Dilution Antimicrobial Susceptibility Tests for Bacteria that Grow Aerobically - Fourth Edition; Approved Standard. NCCLS Document M7-A4, Vol. 17, No. 2. NCCLS, Wayne, PA, January 1997.
- National Committee for Clinical Laboratory Standards. Performance Standards for Antimicrobial Disk Susceptibility Tests - Sixth Edition; Approved Standard. NCCLS Document M2-A6, Vol. 17, No. 1. NCCLS, Wayne, PA, January 1997.
- Swanson-Biearman B, Dean BS, Lopez G, Krenzelok EP. The effects of penicillin and cephalosporin ingestions in children less than six years of age. Vet Hum Toxicol 1988; 30:66-67
West-ward Pharmaceutical Corp.
Eatontown, NJ 07724
DistributorManufactured by :
Hikma Pharmaceuticals
P.O. Box 182400
Amman 11118 – JordanRevised: December 2006
- PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
AMOXICILLIN
amoxicillin capsuleProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:10544-619(NDC:0143-9939) Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength AMOXICILLIN (UNII: 804826J2HU) (AMOXICILLIN - UNII:804826J2HU) AMOXICILLIN 500 mg Inactive Ingredients Ingredient Name Strength CROSCARMELLOSE SODIUM (UNII: M28OL1HH48) GELATIN (UNII: 2G86QN327L) MAGNESIUM STEARATE (UNII: 70097M6I30) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) FERRIC OXIDE YELLOW (UNII: EX438O2MRT) Product Characteristics Color white (WHITE) Score no score Shape CAPSULE (CAPSULE) Size 20mm Flavor Imprint Code Westward;939 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:10544-619-21 21 in 1 BOTTLE 2 NDC:10544-619-30 30 in 1 BOTTLE 3 NDC:10544-619-42 42 in 1 BOTTLE Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA065291 05/17/2010 Labeler - Blenheim Pharmacal, Inc. (171434587) Registrant - Blenheim Pharmacal, Inc. (171434587) Establishment Name Address ID/FEI Business Operations Blenheim Pharmacal, Inc. 171434587 repack


