Label: THERATRAMADOL-60- tramadol hydrochloride, gaba kit
-
Contains inactivated NDC Code(s)
NDC Code(s): 52959-688-60, 68405-380-26 - Packager: Physician Therapeutics LLC
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: None
- Marketing Status: unapproved drug other
DISCLAIMER: This drug has not been found by FDA to be safe and effective, and this labeling has not been approved by FDA. For further information about unapproved drugs, click here.
Drug Label Information
Updated August 1, 2011
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
-
DESCRIPTION
DESCRIPTION
Tramadol hydrochloride tablets is a centrally acting analgesic. The chemical name for tramadol hydrochloride is (±)cis-2-[(dimethylamino)methyl]-1-(3methoxyphenyl) cyclohexanol hydrochloride. Its structural formula is:
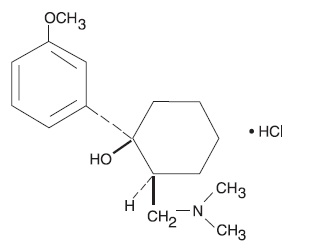
The molecular formula of tramadol hydrochloride is C16H25NO2•HCl and its molecular weight is 299.8.
Tramadol hydrochloride is a white, bitter, crystalline and odorless powder. It is readily soluble in water and ethanol and has a pKa of 9.41. The n-octanol/water log partition coefficient (logP) is 1.35 at pH 7.
Each tramadol hydrochloride tablet intended for oral administration contains 50 mg of tramadol hydrochloride. In addition, it also contains the following inactive ingredients: hypromellose, lactose monohydrate, magnesium stearate, microcrystalline cellulose, polyethylene glycol, polysorbate 80, pregelatinized starch, sodium starch glycolate, and titanium dioxide. -
CLINICAL PHARMACOLOGY
CLINICAL PHARMACOLOGY
PHARMACODYNAMICS
Tramadol Hydrochloride contains tramadol, a centrally acting synthetic opioid analgesic. Although its mode of action is not completely understood, from animal tests, at least two complementary mechanisms appear applicable: binding of parent and M1 metabolite to μ-opioid receptors and weak inhibition of re-uptake of norepinephrine and serotonin.
Opioid activity is due to both low affinity binding of the parent compound and higher affinity binding of the O-demethylated metabolite M1 to μ-opioid receptors. In animal models, M1 is up to 6 times more potent than tramadol in producing analgesia and 200 times more potent in μ-opioid binding. Tramadol-induced analgesia is only partially antagonized by the opiate antagonist naloxone in several animal tests. The relative contribution of both tramadol and M1 to human analgesia is dependent upon the plasma concentrations of each compound (see CLINICAL PHARMACOLOGY, Pharmacokinetics).
Tramadol has been shown to inhibit reuptake of norepinephrine and serotonin in vitro, as have some other opioid analgesics. These mechanisms may contribute independently to the overall analgesic profile of tramadol hydrochloride. Analgesia in humans begins approximately within one hour after administration and reaches a peak in approximately two to three hours.
Apart from analgesia, tramadol hydrochloride administration may produce a constellation of symptoms (including dizziness, somnolence, nausea, constipation, sweating and pruritus) similar to that of other opioids. In contrast to morphine, tramadol has not been shown to cause histamine release. At therapeutic doses, tramadol hydrochloride has no effect on heart rate, left-ventricular function or cardiac index. Orthostatic hypotension has been observed. -
PHARMACOKINETICS
PHARMACOKINETICS
The analgesic activity of tramadol hydrochloride is due to both parent drug and the M1 metabolite (see CLINICAL PHARMACOLOGY, Pharmacodynamics). Tramadol is administered as a racemate and both the [-] and [+] forms of both tramadol and M1 are detected in the circulation. Linear pharmacokinetics have been observed following multiple doses of 50 and 100 mg to steady-state.
Absorption
The mean absolute bioavailability of a 100 mg oral dose is approximately 75%. The mean peak plasma concentration of racemic tramadol and M1 occurs at two and three hours, respectively, after administration in healthy adults. In general, both enantiomers of tramadol and M1 follow a parallel time course in the body following single and multiple doses although small differences (∼ 10%) exist in the absolute amount of each enantiomer present.
Steady-state plasma concentrations of both tramadol and M1 are achieved within two days with four times per day dosing. There is no evidence of self-induction (see Figure 1 and Table 1 below).
Figure 1: Mean Tramadol and M1 Plasma Concentration Profiles after a Single 100 mg Oral Dose and after Twenty-Nine 100 mg Oral Doses of Tramadol HCl given four times per year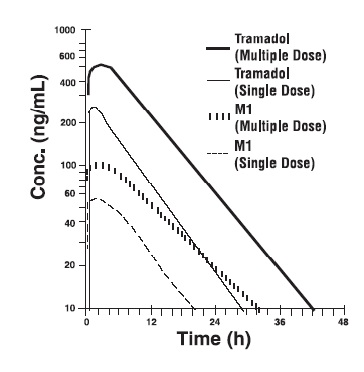 a SD = Single dose, MD = Multiple dose, p.o.= Oral administration, i.v.= Intravenous administration, q.i.d. = Four times daily
a SD = Single dose, MD = Multiple dose, p.o.= Oral administration, i.v.= Intravenous administration, q.i.d. = Four times dailyTable 1 Mean (%CV) Pharmacokinetic Parameters for Racemic Tramadol and M1 Metabolite Population/
Dosage RegimenaParent Drug/
MetabolitePeakConc.
(ng/mL)Time to
Peak (hrs)Clearence/Fb
(mL/min/Kg)t1/2 (hrs) Healthy Adults,
100 mg qid, MD p.o.Tramadol
M1592 (30)
110 (29)2.3 (61)
2.4 (46)5.90 (25)
c6.7 (15)
7.0 (14)Healthy Adults,
100 mg SD p.o.Tramadol
M1308 (25)
55.0 (36)1.6 (63)
3.0 (51)8.50 (31)
c5.6 (20)
6.7 (16)Geriatric, (Greater than 75 yrs)
50 mg SD p.o.Tramadol
M1208 (31)
d2.1 (19)
d6.89 (25)
c7.0 (23)
dHepatic Impaired,
50 mg SD p.o.Tramadol
M1217 (11)
19.4 (12)1.9 (16)
9.8 (20)4.23 (56)
c13.3 (11)
18.5 (15)Renal Impaired,
CLcr10-30 mL/min
100 mg SD i.vTramadol
M1c
cc
c4.23 (54)
c10.6 (31)
11.5 (40)Renal Impaired,
CLcrLess than 5mL/min
100 mg SD i.vTramadol
M1c
cc
c3.73 (17)
c11.0 (29)
16.9 (18)
b F represents the oral bioavailability of tramadol
c Not applicable
d Not measured
Food Effects
Oral administration of tramadol hydrochloride with food does not significantly affect its rate or extent of absorption, therefore, tramadol hydrochloride can be administered without regard to food.
Distribution
The volume of distribution of tramadol was 2.6 and 2.9 liters/kg in male and female subjects, respectively, following a 100 mg intravenous dose. The binding of tramadol to human plasma proteins is approximately 20% and binding also appears to be independent of concentration up to 10 μg/mL. Saturation of plasma protein binding occurs only at concentrations outside the clinically relevant range.
Metabolism
Tramadol is extensively metabolized after oral administration by a number of pathways, including CYP2D6 and CYP3A4, as well as by conjugation of parent and metabolites. Approximately 30% of the dose is excreted in the urine as unchanged drug, whereas 60% of the dose is excreted as metabolites. The remainder is excreted either as unidentified or as unextractable metabolites. The major metabolic pathways appear to be N- and O-demethylation and glucuronidation or sulfation in the liver. One metabolite (O-desmethyltramadol, denoted M1) is pharmacologically active in animal models. Formation of M1 is dependent on CYP2D6 and as such is subject to inhibition, which may affect the therapeutic response (see PRECAUTIONS, Drug Interaction).
Approximately 7% of the population has reduced activity of the CYP2D6 isoenzyme of cytochrome P-450. These individuals are "poor metabolizers" of debrisoquine, dextromethorphan, tricyclic antidepressants, among other drugs. Based on a population PK analysis of Phase I studies in healthy subjects, concentrations of tramadol were approximately 20% higher in "poor metabolizers" versus "extensive metabolizers", while M1 concentrations were 40% lower. Concomitant therapy with inhibitors of CYP2D6 such as fluoxetine, paroxetine and quinidine could result in significant drug interactions. In vitro drug interaction studies in human liver microsomes indicate that inhibitors of CYP2D6 such as fluoxetine and its metabolite norfluoxetine, amitriptyline and quinidine inhibit the metabolism of tramadol to various degrees, suggesting that concomitant administration of these compounds could result in increases in tramadol concentrations and decreased concentrations of M1. The full pharmacological impact of these alterations in terms of either efficacy or safety is unknown. Concomitant use of SEROTONIN re-uptake INHIBITORS and MAO INHIBITORS may enhance the risk of adverse events, including seizure (see WARNINGS) and serotonin syndrome.
Elimination
Tramadol is eliminated primarily through metabolism by the liver and the metabolites are eliminated primarily by the kidneys. The mean terminal plasma elimination half-lives of racemic tramadol and racemic M1 are 6.3 ± 1.4 and 7.4 ± 1.4 hours, respectively. The plasma elimination half-life of racemic tramadol increased from approximately six hours to seven hours upon multiple dosing.
Special Populations
Renal
Impaired renal function results in a decreased rate and extent of excretion of tramadol and its active metabolite, M1. In patients with creatinine clearances of less than 30 mL/min, adjustment of the dosing regimen is recommended (see DOSAGE AND ADMINISTRATION). The total amount of tramadol and M1 removed during a 4-hour dialysis period is less than 7% of the administered dose.
Hepatic
Metabolism of tramadol and M1 is reduced in patients with advanced cirrhosis of the liver, resulting in both a larger area under the concentration time curve for tramadol and longer tramadol and M1 elimination half-lives (13 hrs. for tramadol and 19 hrs. for M1). In cirrhotic patients, adjustment of the dosing regimen is recommended (see DOSAGE AND ADMINISTRATION).
Geriatric
Healthy elderly subjects aged 65 to 75 years have plasma tramadol concentrations and elimination half-lives comparable to those observed in healthy subjects less than 65 years of age. In subjects over 75 years, maximum serum concentrations are elevated (208 vs. 162 ng/mL) and the elimination half-life is prolonged (7 vs. 6 hours) compared to subjects 65 to 75 years of age. Adjustment of the daily dose is recommended for patients older than 75 years (see DOSAGE AND ADMINISTRATION).
Gender
The absolute bioavailability of tramadol was 73% in males and 79% in females. The plasma clearance was 6.4 mL/min/kg in males and 5.7 mL/min/kg in females following a 100 mg IV dose of tramadol. Following a single oral dose, and after adjusting for body weight, females had a 12% higher peak tramadol concentration and a 35% higher area under the concentration-time curve compared to males. The clinical significance of this difference is unknown.
-
CLINICAL STUDIES
CLINICAL STUDIES
Tramadol hydrochloride has been given in single oral doses of 50, 75 and 100 mg to patients with pain following surgical procedures and pain following oral surgery (extraction of impacted molars).
In single-dose models of pain following oral surgery, pain relief was demonstrated in some patients at doses of 50 mg and 75 mg. A dose of 100 mg tramadol hydrochloride tended to provide analgesia superior to codeine sulfate 60 mg, but it was not as effective as the combination of aspirin 650 mg with codeine phosphate 60 mg.
Tramadol hydrochloride has been studied in three long-term controlled trials involving a total of 820 patients, with 530 patients receiving tramadol hydrochloride. Patients with a variety of chronic painful conditions were studied in double-blind trials of one to three months duration. Average daily doses of approximately 250 mg of tramadol hydrochloride in divided doses were generally comparable to five doses of acetaminophen 300 mg with codeine phosphate 30 mg (TYLENOL® with Codeine #3) daily, five doses of aspirin 325 mg with codeine phosphate 30 mg daily, or two to three doses of acetaminophen 500 mg with oxycodone hydrochloride 5 mg (TYLOX® ) daily.
Titration Trials
In a randomized, blinded clinical study with 129 to 132 patients per group, a 10-day titration to a daily tramadol hydrochloride dose of 200 mg (50 mg four times per day), attained in 50 mg increments every 3 days, was found to result in fewer discontinuations due to dizziness or vertigo than titration over only 4 days or no titration. In a second study with 54 to 59 patients per group, patients who had nausea or vomiting when titrated over 4 days were randomized to re-initiate tramadol hydrochloride therapy using slower titration rates.
A 16-day titration schedule, starting with 25 mg qAM and using additional doses in 25 mg increments every third day to 100 mg/day (25 mg four times per day), followed by 50 mg increments in the total daily dose every third day to 200 mg/day (50 mg four times per day), resulted in fewer discontinuations due to nausea or vomiting and fewer discontinuations due to any cause than did a 10-day titration schedule.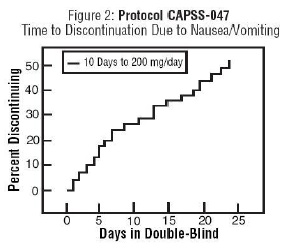
- INDICATIONS & USAGE
-
CONTRAINDICATIONS
CONTRAINDICATIONS
Tramadol hydrochloride should not be administered to patients who have previously demonstrated hypersensitivity to tramadol, any other component of this product or opioids. Tramadol hydrochloride is contraindicated in any situation where opioids are contraindicated, including acute intoxication with any of the following: alcohol, hypnotics, narcotics, centrally acting analgesics, opioids or psychotropic drugs. Tramadol hydrochloride may worsen central nervous system and respiratory depression in these patients. -
WARNINGS
WARNINGS
Seizure Risk
Seizures have been reported in patients receiving Tramadol hydrochloride within the recommended dosage range. Spontaneous post-marketing reports indicate that seizure risk is increased with doses of tramadol hydrochloride above the recommended range.
Concomitant use of tramadol hydrochloride increases the seizure risk in patients taking:
- Selective serotonin re-uptake inhibitors (SSRI antidepressants or anorectics),
- Tricyclic antidepressants (TCAs), and other tricyclic compounds (e.g., cyclobenzaprine , promethazine, etc.), or
-Other opioids.
Administration of tramadol hydrochloride may enhance the seizure risk in patients taking:
-MAO inhibitors (see alsoWARNINGS, Use with MAO Inhibitors and Serotonin Re-Uptake Inhibitors),
- Neuroleptics, or
- Other drugs that reduce the seizure threshold.
Risk of convulsions may also increase in patients with epilepsy, those with a history of seizures, or in patients with a recognized risk for seizure (such as head trauma, metabolic disorders, alcohol and drug withdrawal, CNS infections). In tramadol hydrochloride overdose, naloxone administration may increase the risk of seizure.
Suicide Risk
- Do not prescribe tramadol hydrochloride for patients who are suicidal or addiction-prone.
- Prescribe tramadol hydrochloride tablets with caution for patients who are taking tranquilizers or antidepressant drug and patients who use alcohol in excess and who suffer from emotional disturbance or depression.
The judicious prescribing of tramadol is essential to the safe use of this drug. With patients who are depressed or suicidal, consideration should be given to the use of nonnarcotic analgesics.
Tramadol-related deaths have occurred in patients with previous histories of emotional disturbances or suicidal ideation or attempts as well as histories of misuse of tranquilizers, alcohol, and other CNS-active drugs (see WARNINGS, Risk of Overdosage).
Serotonin Syndrome Risk
The development of a potentially life-threatening serotonin syndrome may occur with the use of tramadol products, including tramadol hydrochloride, particularly with concomitant use of serotonergic drugs such as SSRIs, SNRIs, TCAs, MAOIs, and triptans, with drugs which impair metabolism of serotonin (including MAOIs), and with drugs which impair metabolism of tramadol (CYP2D6 and CYP3A4 inhibitors). This may occur within the recommended dose (seeCLINICAL PHARMACOLOGY, Pharmacokinetics).
Serotonin syndrome may include mental-status changes (e.g., agitation, hallucinations, coma), autonomic instability (e.g., tachycardia, labile blood pressure, hyperthermia), neuromuscular aberrations (e.g., hyperreflexia, incoordination) and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea).
Anaphylactoid Reactions
Serious and rarely fatal anaphylactoid reactions have been reported in patients receiving therapy with tramadol hydrochloride. When these events do occur it is often following the first dose. Other reported allergic reactions include pruritus, hives, bronchospasm, angioedema, toxic epidermal necrolysis and Stevens-Johnson syndrome. Patients with a history of anaphylactoid reactions to codeine and other opioids may be at increased risk and therefore should not receive tramadol hydrochloride (see CONTRAINDICATIONS).
Respiratory Depression
Administer tramadol hydrochoride cautiously in patients at risk for respiratory depression. In these patients alternative non-opioid analgesics should be considered. When large doses of tramadol hydrochloride are administered with anesthetic medications or alcohol, respiratory depression may result. Respiratory depression should be treated as an overdose. If naloxone is to be administered, use cautiously because it may precipitate seizures (see WARNINGS, Seizure Risk and OVERDOSAGE).
Interaction With Central Nervous System (CNS) Depressants
Tramadol hydrochloride should be used with caution and in reduced dosages when administered to patients receiving CNS depressants such as alcohol, opioids, anesthetic agents, narcotics, phenothiazines, tranquilizers or sedative hypnotics. Tramadol hydrochloride increases the risk of CNS and respiratory depression in these patients.
Interactions with Alcohol and Drugs of Abuse
Tramadol may be expected to have additive effects when used in conjunction with alcohol, other opioids, or illicit drugs that cause central nervous system depression.
Increased Intracranial Pressure or Head Trauma
Tramadol hydrochloride should be used with caution in patients with increased intracranial pressure or head injury. The respiratory depressant effects of opioids include carbon dioxide retention and secondary elevation of cerebrospinal fluid pressure, and may be markedly exaggerated in these patients. Additionally, pupillary changes (miosis) from tramadol may obscure the existence, extent, or course of intracranial pathology. Clinicians should also maintain a high index of suspicion for adverse drug reaction when evaluating altered mental status in these patients if they are receiving tramadol hydrochloride (see WARNINGS, Respiratory Depression).
Use in Ambulatory Patients
Tramadol hydrochloride may impair the mental and or physical abilities required for the performance of potentially hazardous tasks such as driving a car or operating machinery. The patient using this drug should be cautioned accordingly.
Use With MAO Inhibitors and Serotonin Re-uptake Inhibitors
Use tramadol hydrochloride with great caution in patients taking monoamine oxidase inhibitors. Animal studies have shown increased deaths with combined administration. Concomitant use of tramadol hydrochloride with MAO inhibitors or SSRI’s increases the risk of adverse events, including seizure and serotonin syndrome.
Misuse, Abuse and Diversion
Tramadol has mu-opioid agonist activity. Tramadol hydrochloride® can be sought by drug abusers and people with addiction disorders and may be subject to criminal diversion. The possibility of illegal or illicit use should be considered when prescribing or dispensing tramadol hydrochloride® in situations where the physician or pharmacist is concerned about an increased risk of misuse, abuse, or diversion. Misuse or abuse poses a significant risk to the abuser that could result in overdose and death (see DRUG ABUSE AND DEPENDENCE and OVERDOSAGE).
Concerns about abuse, addiction, and diversion should not prevent the proper management of pain. The development of addiction to opioid analgesics in properly managed patients with pain has been reported to be rare. However, data are not available to establish the true incidence of addiction in chronic pain patients.
Risk of Overdosage
Patients taking tramadol should be warned not to exceed the dose recommended by their physician. Tramadol products in excessive doses, either alone or in combination with other CNS depressants, including alcohol, are a cause of drug-related deaths. Patients should be cautioned about the concomitant use of tramadol products and alcohol because of potentially serious CNS additive effects of these agents. Because of its added depressant effects, tramadol should be prescribed with caution for those patients whose medical condition requires the concomitant administration of sedatives, tranquilizers, muscle relaxants, antidepressants, or other CNS depressant drugs. Patients should be advised of the additive depressant effects of these combinations.
Serious potential consequences of overdosage with tramadol hydrochloride (tramadol hydrochloride) tablets are central nervous system depression, respiratory depression and death. Some deaths have occurred as a consequence of the accidental ingestion of excessive quantities of tramadol alone or in combination with other drugs. In treating an overdose, primary attention should be given to maintaining adequate ventilation along with general supportive treatment (see OVERDOSAGE).
Withdrawal
Withdrawal symptoms may occur if tramadol hydrochloride is discontinued abruptly (see also DRUG ABUSE AND DEPENDENCE). Reported symptoms have included anxiety, sweating, insomnia, rigors, pain, nausea, tremors, diarrhea, upper respiratory symptoms, piloerection, and rarely hallucinations. Other symptoms that have been reported less frequently with tramadol hydrchloride discontinuation include panic attacks, severe anxiety, and paresthesias. Clinical experience suggests that withdrawal symptoms may be avoided by tapering tramadol hydrochloride at the time of discontinuation. -
PRECAUTIONS
PRECAUTIONS
Acute Abdominal Conditions
The administration of tramadol hydrochloride may complicate the clinical assessment of patients with acute abdominal conditions.
Use in Renal and Hepatic Disease
Impaired renal function results in a decreased rate and extent of excretion of tramadol and its active metabolite, M1. In patients with creatinine clearances of less than 30 mL/min, dosing reduction is recommended (see DOSAGE AND ADMINISTRATION). Metabolism of tramadol and M1 is reduced in patients with advanced cirrhosis of the liver. In cirrhotic patients, dosing reduction is recommended (see DOSAGE AND ADMINISTRATION).
With the prolonged half-life in these conditions, achievement of steady-state is delayed, so that it may take several days for elevated plasma concentrations to develop. -
INFORMATION FOR PATIENTS
Information for Patients
- Patients should be informed that tramadol hydrochloride may cause seizures and/or serotonin syndrome with concomitant use of serotonergic agents (including SSRIs, SNRIs, and triptans) or drugs that significantly reduce the metabolic clearance of tramadol.
- may impair mental or physical abilities required for the performance of potentially hazardous tasks such as driving a car or operating machinery.
- Tramadol hydrochloride should not be taken with alcohol containing beverages.
- Tramadol hydrochloride should be used with caution when taking medications such as tranquilizers, hypnotics or other opiate containing analgesics.
- The patient should be instructed to inform the physician if they are pregnant, think they might become pregnant, or are trying to become pregnant (see PRECAUTIONS, Labor and Delivery).
- The patient should understand the single-dose and 24-hour dose limit and the time interval between doses, since exceeding these recommendations can result in respiratory depression, seizures and death. -
DRUG INTERACTIONS
Drug Interactions
CYP2D6 and CYP3A4 Inhibitors
Concomitant administration of CYP2D6 and/or CYP3A4 inhibitors (see CLINICAL PHARMACOLOGY, Pharmacokinetics), such as quinidine, fluoxetine, paroxetine and amitriptyline (CYP2D6 inhibitors), and ketoconazole and erythromycin (CYP3A4 inhibitors), may reduce metabolic clearance of tramadol increasing the risk for serious adverse events including seizures and serotonin syndrome.
Serotonergic Drugs
There have been postmarketing reports of serotonin syndrome with use of tramadol and SSRIs/SNRIs or MAOIs and α2-adrenergic blockers. Caution is advised when tramadol hydrochloride is coadministered with other drugs that may affect the serotonergic neurotransmitter systems, such as SSRIs, MAOIs, triptans, linezolid (an antibiotic which is a reversible non-selective MAOI), lithium, or St. John’s Wort. If concomitant treatment of tramadol hydrochloride with a drug affecting the serotonergic neurotransmitter system is clinically warranted, careful observation of the patient is advised, particularly during treatment initiation and dose increases (see WARNINGS, Serotonin Syndrome).
Triptans
Based on the mechanism of action of tramadol and the potential for serotonin syndrome, caution is advised when tramadol hydrochloride is coadministered with a triptan. If concomitant treatment of tramadol hydrochloride with a triptan is clinically warranted, careful observation of the patient is advised, particularly during treatment initiation and dose increases (see WARNINGS, Serotonin Syndrome).
Use With Carbamazepine
Patients taking carbamazepine may have a significantly reduced analgesic effect of tramadol hydrochloride. Because carbamazepine increases tramadol metabolism and because of the seizure risk associated with tramadol, concomitant administration of tramadol hydrochloride and carbamazepine is not recommended.
Use With Quinidine
Tramadol is metabolized to M1 by CYP2D6. Quinidine is a selective inhibitor of that isoenzyme, so that concomitant administration of quinidine and tramadol hydrochloride results in increased concentrations of tramadol and reduced concentrations of M1. The clinical consequences of these findings are unknown. In vitro drug interaction studies in human liver microsomes indicate that tramadol has no effect on quinidine metabolism.
Potential for Other Drugs to Affect Tramadol
In vitro drug interaction studies in human liver microsomes indicate that concomitant administration with inhibitors of CYP2D6 such as fluoxetine, paroxetine, and amitriptyline could result in some inhibition of the metabolism of tramadol. Administration of CYP3A4 inhibitors, such as ketoconazole and erythromycin, or inducers, such as rifampin and St. John’s Wort, with tramadol hydrochloride may affect the metabolism of tramadol leading to alteted tramadol exposure.
Potential for Tramadol to Affect Other Drugs
In vitro studies indicate that tramadol is unlikely to inhibit the CYP3A4-mediated metabolism of other drugs when tramadol is administered concomitantly at therapeutic doses. Tramadol does not appear to induce its own metabolism in humans, since observed maximal plasma concentrations after multiple oral doses are higher than expected based on single-dose data. Tramadol is a mild inducer of selected drug metabolism pathways measured in animals.
Use With Cimetidine
Concomitant administration of tramadol hydrochloride® with cimetidine does not result in clinically significant changes in tramadol pharmacokinetics. Therefore, no alteration of the tramadol hydrochloride dosage regimen is recommended.
Use With Digoxin and Warfarin
Post-marketing surveillance has revealed rare reports of digoxin toxicity and alteration of warfarin effect, including elevation of prothrombin times. -
CARCINOGENESIS & MUTAGENESIS & IMPAIRMENT OF FERTILITY
Carcinogenesis, Mutagenesis, Impairment of Fertility
A slight, but statistically significant, increase in two common murine tumors, pulmonary and hepatic, was observed in a mouse carcinogenicity study, particularly in aged mice. Mice were dosed orally up to 30 mg/kg (90 mg/m2 or 0.36 times the maximum daily human dosage of 246 mg/m2) for approximately two years, although the study was not done with the Maximum Tolerated Dose. This finding is not believed to suggest risk in humans. No such finding occurred in a rat carcinogenicity study (dosing orally up to 30 mg/kg, 180 mg/m2, or 0.73 times the maximum daily human dosage).
Tramadol was not mutagenic in the following assays: Ames Salmonella microsomal activation test, CHO/HPRT mammalian cell assay, mouse lymphoma assay (in the absence of metabolic activation), dominant lethal mutation tests in mice, chromosome aberration test in Chinese hamsters, and bone marrow micronucleus tests in mice and Chinese hamsters. Weakly mutagenic results occurred in the presence of metabolic activation in the mouse lymphoma assay and micronucleus test in rats. Overall, the weight of evidence from these tests indicates that tramadol does not pose a genotoxic risk to humans.
No effects on fertility were observed for tramadol at oral dose levels up to 50 mg/kg (300 mg/m2) in male rats and 75 mg/kg (450 mg/m2) in female rats. These dosages are 1.2 and 1.8 times the maximum daily human dosage of 246 mg/m2, respectively. -
PREGNANCY
Pregnancy, Teratogenic Effects: Pregnancy Category C
Tramadol has been shown to be embryotoxic and fetotoxic in mice, (120 mg/kg or 360 mg/m2), rats (Greater than or equal to 25 mg/kg or 150 mg/m2) and rabbits (Greater than or equal to 75 mg/kg or 900 mg/m2) at maternally toxic dosages, but was not teratogenic at these dose levels. These dosages on a mg/m2 basis are 1.4, Greater than or equal to 0.6, and Greater than or equal to 3.6 times the maximum daily human dosage (246 mg/m2) for mouse, rat and rabbit, respectively.
No drug-related teratogenic effects were observed in progeny of mice (up to 140 mg/kg or 420 mg/m2), rats (up to 80 mg/kg or 480 mg/m2) or rabbits (up to 300 mg/kg or 3600 mg/m2) treated with tramadol by various routes. Embryo and fetal toxicity consisted primarily of decreased fetal weights, skeletal ossification and increased supernumerary ribs at maternally toxic dose levels. Transient delays in developmental or behavioral parameters were also seen in pups from rat dams allowed to deliver. Embryo and fetal lethality were reported only in one rabbit study at 300 mg/kg (3600 mg/m2), a dose that would cause extreme maternal toxicity in the rabbit. The dosages listed for mouse, rat and rabbit are 1.7, 1.9 and 14.6 times the maximum daily human dosage (246 mg/m2), respectively. -
NONTERATOGENIC EFFECTS
Non-teratogenic Effects
Tramadol was evaluated in peri- and post-natal studies in rats. Progeny of dams receiving oral (gavage) dose levels of 50 mg/kg (300 mg/m2 or 1.2 times the maximum daily human tramadol dosage) or greater had decreased weights, and pup survival was decreased early in lactation at 80 mg/kg (480 mg/m2 or 1.9 and higher the maximum daily human dose).
There are no adequate and well-controlled studies in pregnant women. Tramadol Hydrochloride should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. Neonatal seizures, neonatal withdrawal syndrome, fetal death and still birth have been reported during post-marketing. -
LABOR & DELIVERY
Labor and Delivery
Tramadol hydrochloride should not be used in pregnant women prior to or during labor unless the potential benefits outweigh the risks. Safe use in pregnancy has not been established. Chronic use during pregnancy may lead to physical dependence and post-partum withdrawal symptoms in the newborn (see DRUG ABUSE AND DEPENDENCE). Tramadol has been shown to cross the placenta. The mean ratio of serum tramadol in the umbilical veins compared to maternal veins was 0.83 for 40 women given tramadol during labor.
The effect of tramadol hydrochloride, if any, on the later growth, development, and functional maturation of the child is unknown. -
NURSING MOTHERS
Nursing Mothers
Tramadol hydrochloride is not recommended for obstetrical preoperative medication or for post-delivery analgesia in nursing mothers because its safety in infants and newborns has not been studied. Following a single IV 100 mg dose of tramadol, the cumulative excretion in breast milk within 16 hours postdose was 100 μg of tramadol (0.1% of the maternal dose) and 27 μg of M1. - PEDIATRIC USE
-
GERIATRIC USE
Geriatric Use
In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal or cardiac function and of concomitant disease or other drug therapy. In patients over 75 years of age, daily doses in excess of 300 mg are not recommended (see CLINICAL PHARMACOLOGY and DOSAGE AND ADMINISTRATION).
A total of 455 elderly (65 years of age or older) subjects were exposed to tramadol hydrochloride in controlled clinical trials. Of those, 145 subjects were 75 years of age and older.
In studies including geriatric patients, treatment-limiting adverse events were higher in subjects over 75 years of age compared to those under 65 years of age. Specifically, 30% of those over 75 years of age had gastrointestinal treatment-limiting adverse events compared to 17% of those under 65 years of age. Constipation resulted in discontinuation of treatment in 10% of those over 75. -
ADVERSE REACTIONS
ADVERSE REACTIONS
Tramadol hydrochloride was administered to 550 patients during the double-blind or open-label extension periods in U.S. studies of chronic nonmalignant pain. Of these patients, 375 were 65 years old or older. Table 2 reports the cumulative incidence rate of adverse reactions by 7, 30 and 90 days for the most frequent reactions (5% or more by 7 days). The most frequently reported events were in the central nervous system and gastrointestinal system. Although the reactions listed in the table are felt to be probably related to tramadol hydrochloride administration, the reported rates also include some events that may have been due to underlying disease or concomitant medication. The overall incidence rates of adverse experiences in these trials were similar for tramadol hydrochloride and the active control groups, TYLENOL® with Codeine #3 (acetaminophen 300 mg with codeine phosphate 30 mg), and aspirin 325 mg with codeine phosphate 30 mg, however, the rates of withdrawals due to adverse events appeared to be higher in the tramadol hydrochloride groups.Table 2: Cumulative Incidence of Adverse Reactions for Tramadol Hydrochloride in Chronic Trials of Nonmalignant Pain (N=427)
Up to 7 Days Up to 30 Days Up to 90 Days Dizziness/Vertigo 26% 31% 33% Nausea 24% 34% 40% Constipation 24% 38% 46% Headache 18% 26% 32% Somnolence 16% 23% 25% Vomiting 9% 13% 17% Pruritus 8% 10% 11% ‘CNS Stimulation’1 7% 11% 14% Asthenia 6% 11% 12% Sweating 6% 7% 9% Dyspepsia 5% 9% 13% Dry Mouth 5% 9% 10% Diarrhea 5% 9% 10% 1 “CNS Stimulation” is a composite of nervousness, anxiety, agitation, tremor, spasticity, euphoria, emotional lability and hallucinations
Incidence 1% to less than 5% possibly causally related: the following lists adverse reactions that occurred with an incidence of 1% to less than 5% in clinical trials, and for which the possibility of a causal relationship with tramadol hydrochloride exists.
Body as a Whole: Malaise.
Cardiovascular: Vasodilation.
Central Nervous System: Anxiety, Confusion, Coordination disturbance, Euphoria,
Miosis, Nervousness, Sleep disorder.
Gastrointestinal: Abdominal pain, Anorexia, Flatulence.
Musculoskeletal: Hypertonia.
Skin: Rash.
Special Senses: Visual disturbance.
Urogenital: Menopausal symptoms, Urinary frequency, Urinary retention.
Incidence less than 1%, possibly causally related: the following lists adverse reactions that occurred with an incidence of less than 1% in clinical trials and/or reported in post-marketing experience.
Body as a Whole: Accidental injury, Allergic reaction, Anaphylaxis, Death, Suicidal tendency, Weight loss, Serotonin syndrome (mental status change, hyperreflexia, fever, shivering, tremor, agitation, diaphoresis, seizures and coma).
Cardiovascular: Orthostatic hypotension, Syncope, Tachycardia.
Central Nervous System: Abnormal gait, Amnesia, Cognitive dysfunction, Depression, Difficulty in concentration, Hallucinations, Paresthesia, Seizure (see WARNINGS). Tremor.
Respiratory: Dyspnea.
Skin: Stevens-Johnson syndrome/Toxic epidermal necrolysis, Urticaria, Vesicles.
Special Senses: Dysgeusia.
Urogenital: Dysuria, Menstrual disorder.
Other adverse experiences, causal relationship unknown: A variety of other adverse events were reported infrequently in patients taking tramadol hydrochloride during clinical trials and/or reported in post-marketing experience. A causal relationship between tramadol hydrochloride and these events has not been determined. However, the most significant events are listed below as alerting information to the physician.
Cardiovascular: Abnormal ECG, Hypertension, Hypotension, Myocardial ischemia, Palpitations, Pulmonary edema, Pulmonary embolism.
Central Nervous System: Migraine, Speech disorders.
Gastrointestinal: Gastrointestinal bleeding, Hepatitis, Stomatitis, Liver failure.
Laboratory Abnormalities: Creatinine increase, Elevated liver enzymes, Hemoglobin decrease, Proteinuria.
Sensory: Cataracts, Deafness, Tinnitus. -
DRUG ABUSE AND DEPENDENCE
DRUG ABUSE AND DEPENDENCE
Abuse
Tramadol has mu-opioid agonist activity. Tramadol hydrochloride tablets can be abused and may be subject to criminal diversion.
Addiction is a primary, chronic, neurobiologic disease, with genetic, psychosocial, and environmental factors influencing its development and manifestations. Drug addiction is characterized by behaviors that include one or more of the following: impaired control over drug use, compulsive use, use for non-medical purposes, and continued use despite harm or risk of harm, and craving. Drug addiction is a treatable disease, utilizing a multidisciplinary approach, but relapse is common.
“Drug-seeking” behavior is very common in addicts and drug abusers. Drug-seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing or referral, repeated “loss” of prescriptions, tampering with prescriptions and reluctance to provide prior medical records or contact information for other treating physician(s). “Doctor shopping” to obtain additional prescriptions is common among drug abusers and people suffering from untreated addiction.
Abuse and addiction are separate and distinct from physical dependence and tolerance. Physicians should be aware that addiction may not be accompanied by concurrent tolerance and symptoms of physical dependence in all addicts. In addition, abuse of ULTRAM® can occur in the absence of true addiction and is characterized by misuse for non-medical purposes, often in combination with other psychoactive substances.
Concerns about abuse and addiction should not prevent the proper management of pain. However all patients treated with opioids require careful monitoring for signs of abuse and addiction, because use of opioid analgesic products carries the risk of addiction even under appropriate medical use.
Proper assessment of the patient and periodic re-evaluation of therapy are appropriate measures that help to limit the potential abuse of this product.
Tramadol hydrochloride tablets is intended for oral use only.
Dependence
Tolerance is the need for increasing doses of drugs to maintain a defined effect such as analgesia (in the absence of disease progression or other external factors). Physical dependence is manifested by withdrawal symptoms after abrupt discontinuation of a drug or upon administration of an antagonist (see also WARNINGS, Withdrawal).
The opioid abstinence or withdrawal syndrome is characterized by some or all of the following: restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate.
Generally, tolerance and/or withdrawal are more likely to occur the longer a patient is on continuous therapy with tramadol hydrochloride tablets. -
OVERDOSAGE
OVERDOSAGE
Acute overdosage with tramadol can be manifested by respiratory depression, somnolence progressing to stupor or coma, skeletal muscle flaccidity, cold and clammy skin, constricted pupils, seizures, bradycardia, hypotension, cardiac arrest, and death. Deaths due to overdose have been reported with abuse and misuse of tramadol (see WARNINGS, Misuse, Abuse, and Diversion). Review of case reports has indicated that the risk of fatal overdose is further increased when tramadol is abused concurrently with alcohol or other CNS depressants, including other opioids.
In the treatment of tramadol overdosage, primary attention should be given to the reestablishment of a patent airway and institution of assisted or controlled ventilation. Supportive measures (including oxygen and vasopressors) should be employed in the management of circulatory shock and pulmonary edema accompanying overdose as indicated. Cardiac arrest or arrhythmias may require cardiac massage or defibrillation.
While naloxone will reverse some, but not all, symptoms caused by overdosage with tramadol, the risk of seizures is also increased with naloxone administration. In animals convulsions following the administration of toxic doses of tramadol hydrochloride tablets could be suppressed with barbiturates or benzodiazepines but were increased with naloxone. Naloxone administration did not change the lethality of an overdose in mice. Hemodialysis is not expected to be helpful in an overdose because it removes less than 7% of the administered dose in a 4-hour dialysis period. -
DOSAGE & ADMINISTRATION
DOSAGE And ADMINISTRATION
Adults (17 years of age and over)
For patients with moderate to moderately severe chronic pain not requiring rapid onset of analgesic effect, the tolerability of tramadol hydrochloride tablets can be improved by initiating therapy with the following titration regimen: tramadol hydrochloride tablets should be started at 25 mg/day qAM and titrated in 25 mg increments as separate doses every 3 days to reach 100 mg/day (25 mg q.i.d.). Thereafter the total daily dose may be increased by 50 mg as tolerated every 3 days to reach 200 mg/day (50 mg q.i.d.). After titration, tramdol hydrochloride tablets 50 to 100 mg can be administered as needed for pain relief every 4 to 6 hours not to exceed 400 mg/day.
For the subset of patients for whom rapid onset of analgesic effect is required and for whom the benefits outweigh the risk of discontinuation due to adverse events associated with higher initial doses, tramdol hydrochloride tablets 50 mg to 100 mg can be administered as needed for pain relief every four to six hours, not to exceed 400 mg per day.
Individualization of Dose
Good pain management practice dictates that the dose be individualized according to patient need using the lowest beneficial dose. Studies with tramadol in adults have shown that starting at the lowest possible dose and titrating upward will result in fewer discontinuations and increased tolerability.
- In all patients with creatinine clearance less than 30 mL/min, it is recommended that the dosing interval of tramadol hydrochloride tablets be increased to 12 hours, with a maximum daily dose of 200 mg. Since only 7% of an administered dose is removed by hemodialysis, dialysis patients can receive their regular dose on the day of dialysis.
- The recommended dose for adult patients with cirrhosis is 50 mg every 12 hours.
- In general, dose selection for an elderly patient over 65 years old should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal or cardiac function and of concomitant disease or other drug therapy. For elderly patients over 75 years old, total dose should not exceed 300 mg/day. -
HOW SUPPLIED
HOW SUPPLIED
Tramadol hydrochloride tablets 50 mg are supplied as unscored, white, round film coated tablets debossed “AN” over “627”.
They are supplied as follows:
Bottles of 100 tablets: NDC 65162-627-10
Bottles of 500 tablets: NDC 65162-627-50
Bottles of 1000 tablets: NDC 65162-627-11
Manufactured by:
Amneal Pharmaceuticals
Paterson, New Jersey 07504
Amneal Pharmaceuticals
Hauppauge, NY 11788
Distributed by:
Amneal Pharmaceuticals
Glasgow, KY 42164
Rev. 11-2009
- STORAGE AND HANDLING
-
PRINCIPAL DISPLAY PANEL
NDC 65162-627-10 traMADOL Hydrochloride Tablets AN;627 50 mg Rx only 100 TABLETS amneal PHARMACEUTICALS Each tablet contains: Tramadol Hydrochloride.............50 mg Usual Dosage: See attached labelling for complete precribing information. Store at 20°C to 25°C (68°F to 77°F). [see USP Controlled Room Temperature] Dispense in a tight container as defined in the USP. Manufactured by: Amneal Pharmaceuticals Paterson, New Jersey 07504 Distributed by:
Amneal Pharmaceuticals Glasgow, KY 42141 MF# 101 Rev. 12-2007 N3 65162-627-10 7 Lot No: Exp. Date: 3/4' Non-Vanish Area.
-
SPL UNCLASSIFIED SECTION
Theramine (U.S. patent pending) capsules by oral administration. A specially formulated Medical Food product, consisting of a proprietary blend of amino acids and polyphenol ingredients in specific proportions, for the dietary management of the metabolic processes associated with pain disorders and inflammatory conditions. (PD) (IC). Must be administered under physician supervision.
Medical Foods
Medical Food products are often used in hospitals (e.g., for burn victims or kidney dialysis patients) and outside of a hospital setting under a physician’s care for the dietary management of diseases in patients with particular, unique or distinctive medical or metabolic needs due to their disease or condition. Congress defined "Medical Food" in the Orphan Drug Act and Amendments of 1988 as "a food which is formulated to be consumed or administered enterally [or orally] under the supervision of a physician and which is intended for the specific dietary management of a disease or condition for which distinctive nutritional requirements, based on recognized scientific principles, are established by medical evaluation." Medical Foods are complex formulated products, requiring sophisticated and exacting technology, and that are used only for a patient receiving active and ongoing medical supervision wherein the patient requires medical care on a recurring basis for, among other things, instructions on the use of the Medical Food. Theramine has been developed, manufactured, and labeled in accordance with both the statutory definition of a Medical Food and FDA’s regulatory labeling guidelines. Theramine must be used while the patient is under the ongoing care of a physician.
PAIN DISORDERS (PD) INFLAMMATORY CONDITIONS (IC)
PD and IC as a Metabolic Deficiency Disease
A critical component of the definition of a Medical Food is that the product must address the distinct nutritional requirements of a particular disease or condition. FDA scientists have proposed a physiologic definition of distinctive nutritional requirements as follows: “the dietary management of patients with specific diseases requires, in some instances, the ability to meet nutritional requirements that differ substantially from the needs of healthy persons. For example, in establishing the recommended dietary allowances for general, healthy population, the Food and Nutrition Board of the Institute of Medicine National Academy of Sciences, recognized that different or distinctive physiologic requirements may exist for certain persons with "special nutritional needs arising from metabolic disorders, chronic diseases, injuries, premature birth, other medical conditions and drug therapies. Thus, the distinctive nutritional needs associated with a disease reflects the total amount needed by a healthy person to support life or maintain homeostasis, adjusted for the distinctive changes in the nutritional needs of the patient as a result of the effects of the disease process on absorption, metabolism and excretion.” It was also proposed that in patients with certain disease states who respond to nutritional therapies, a physiologic deficiency of the nutrient is assumed to exist. For example, if a patient with a pain disorder responds to a tryptophan formulation by decreasing perceived pain, then a deficiency of tryptophan is assumed to exist. Patients with pain disorders and inflammatory conditions are known to have increased nutritional requirements for tryptophan, choline, arginine, GABA, flavonoids, and certain antioxidants. These nutritional requirements are such that they cannot be achieved by the modification of the normal diet alone, or by supplementing the diet.
Patients with pain disorders and inflammatory conditions frequently exhibit reduced plasma levels of tryptophan and GABA, and have been shown to respond to oral administration of GABA, arginine, tryptophan, or a 5-hydroxytryptophan formulation. Research has shown that tryptophan, arginine or GABA reduced diets result in a fall of circulating tryptophan, arginine, and/or GABA. Patients with pain disorders frequently exhibit activation of the degradation pathways that increases the turnover rate of GABA, arginine and/or tryptophan leading to a reduced level of production of serotonin, GABA or nitric oxide for a given precursor blood level. Research has also shown that a genetic predisposition to accelerated degradation can lead to increased precursor requirements in certain patients with pain disorders and inflammatory conditions.
Choline is required to fully potentiate acetylcholine synthesis by brain neurons. A deficiency of choline leads to reduced acetylcholine production by the neurons. Provision of tryptophan, arginine, GABA, choline and flavonoids with antioxidants, in specific proportions can restore the production of beneficial serotonin, nitric oxide, and acetylcholine, thereby reducing the perception of pain and reducing inflammation. L-Histidine is known to produce brain histamine that stimulates production of ACTH, producing cortisol to reduce inflammation. -
DESCRIPTION
PRODUCT DESCRIPTION
Primary Ingredients
Theramine consists of a proprietary formulation of Gamma Aminobutyric Acid, Choline Bitartrate, Whey Protein Hydrolysate, L-Arginine, L-Histidine, L-Glutamine, Theobromine, Griffonia See, Grape Seed, L-Serine, and Cinnamon in specific proportions. These ingredients fall into the classification of Generally Recognized as Safe (GRAS) as defined by the Food and Drug Administration (FDA) (Sections 201(s) and 409 of the Federal Food, Drug, and Cosmetic Act). A GRAS substance is distinguished from a food additive on the basis of the common knowledge about the safety of the substance for its intended use. The standard for an ingredient to achieve GRAS status requires not only technical demonstration of non-toxicity and safety, but also general recognition of safety through widespread usage and agreement of that safety by experts in the field. Many ingredients have been determined by the FDA to be GRAS, and are listed as such by regulation, in Volume 21 Code of Federal Regulations (CFR) Sections 182, 184, and 186.
Amino Acids
Amino Acids are the building blocks of protein and are GRAS listed as they have been safely ingested by humans for thousands of years. The formulations of the amino acids in Theramine are equivalent to those found in the usual human diet. Patients with pain disorders may require an increased amount of certain amino acids that cannot be obtained from normal diet alone. Tryptophan, for example, is an obligatory amino acid. The body cannot make tryptophan and must obtain tryptophan from the diet. Tryptophan is needed to produce serotonin. Serotonin is required to reduce pain. Patients with pain disorders and inflammatory conditions have altered serotonin metabolism.
Flavonoids
Flavonoids are a group of phytochemical compounds found in all vascular plants including fruits and vegetables. They are a part of a larger class of compounds known as polyphenols. Many of the therapeutic or health benefits of colored fruits and vegetables, cocoa, red wine, and green tea are directly related to their flavonoid content. The specially formulated flavonoids found in Theramine cannot be obtained from conventional foods in the necessary proportions to elicit a therapeutic response.
Other Ingredients
Theramine contains the following “inactive” or other ingredients, as fillers, excipients, and colorings: Gelatin, Silicon Dioxide, Tricalcium Phosphate, Vegetable Magnesium stearate, Cellulose, FDandC Blue#1, FDandC Red #3, Titanium Dioxide.
Physical Description
Theramine is a yellow to light brown powder. Theramine contains Gamma Aminobutyric Acid, Choline Bitartrate, Whey Protein Hydrolysate, L-Arginine, L-Histidine HCL, L-Glutamine, Theobromine, Griffonia Seed, Grape Seed, L-Serine, and Cinnamon. Each capsule consists of a proprietary blend of these ingredients in an amount of 366mg or 732mg per two (2) capsule dose. -
CLINICAL PHARMACOLOGY
CLINICAL PHARMACOLOGY
Mechanism of Action
Theramine acts by restoring and maintaining the balance of the neurotransmitters GABA, nitric oxide, serotonin, and acetylcholine that are associated with pain disorders and inflammatory conditions. Theramine stimulates the production ACTH to reduce inflammation.
Metabolism
The amino acids in Theramine are primarily absorbed by the stomach and small intestines. All cells metabolize the amino acids in Theramine. Circulating tryptophan, arginine and choline blood levels determine the production of serotonin, nitric oxide, and acetylcholine.
Excretion
Theramine is not an inhibitor of cytochrome P450 1A2, 2C9, 2C19, 2D6, or 3A4. These isoenzymes are principally responsible for 95% of all detoxification of drugs, with CYP3A4 being responsible for detoxification of roughly 50% of drugs. Amino acids do not appear to have an effect on drug metabolizing enzymes. - INDICATIONS & USAGE
-
CLINICAL STUDIES
CLINICAL EXPERIENCE
Administration of Theramine has demonstrated significant reduction in symptoms of pain and inflammation in patients with acute and chronic pain when used
for the dietary management of the metabolic processes associated with pain disorders and inflammatory conditions. Administration of Theramine results in
the induction and maintenance of pain relief in patients with pain disorders and inflammatory conditions. - CONTRAINDICATIONS
-
ADVERSE REACTIONS
ADVERSE REACTIONS
Ingestion of L-Tryptophan, L-Arginine, or Choline at high doses of up to 15 grams daily is generally well tolerated. The most common adverse reactions of higher
doses — from 15 to 30 grams daily — are nausea, abdominal cramps, and diarrhea. Theramine contains less than 1 gram per dose of amino acids however, some patients
may experience these symptoms at lower doses. The total combined amount of amino acids in each Theramine capsule does not exceed 300 mg. - DRUG INTERACTIONS
-
OVERDOSAGE
OVERDOSE
There is a negligible risk of overdose with Theramine as the total amount of amino acids in a one month supply (90 capsules) is less than 30 grams. Overdose symptoms may include diarrhea, weakness, and nausea.
POST-MARKETING SURVEILLANCE
Post-marketing surveillance has shown no serious adverse reactions. Reported cases of mild rash and itching may have been associated with allergies to Theramine flavonoid ingredients, including Cinnamon, Cocoa, and Grape Seed. These reactions were temporary, transient in nature and subsided within 24-hours. -
DOSAGE & ADMINISTRATION
DOSAGE AND ADMINISTRATION
Recommended Administration
For the dietary management of the metabolic processes associated with pain disorders and inflammatory conditions. Take two (2) capsules every four hours or as directed by physician. As with most amino acid formulations Theramine should be taken without food to increase the absorption of key ingredients. -
HOW SUPPLIED
How Supplied
Theramine is supplied in purple and white, size 0 capsules in bottles of 60 and 90 capsules.
Physician Supervision
Theramine is a Medical Food product available by prescription only and may be used per FDA law, and product labeling only while the patient is under ongoing physician supervision.
U.S. patent pending
Manufactured by Arizona Nutritional Supplements, Inc. Chandler AZ 85225
Distributed exclusively by Physician Therapeutics LLC, a wholly owned subsidiary of Targeted Medical Pharma Inc. Los Angeles, CA
www.ptlcentral.com NDC: 68405-008-02 NDC: 68405-008-03 - STORAGE AND HANDLING
-
PRINCIPAL DISPLAY PANEL
68405-008-02 Directions for use: Must be administered under physician supervision. For adults only. As a Medical Food, take one (1) or two (2) capsules every four hours or as directed by physician. For the dietary management of Myalgia. Contains no added sugar, starch, wheat, yeast, preservatives, artificial flavor. Storage: Keep tightly closed in a cool dry place 8-32°C (45-90°F), relative humidity, below 50%. Warning: Keep this product out of the reach of children. NDC# 68405-008-02 LOT# 007007 PHYSICIAN THERAPEUTICS THERAMINE Medical Food Rx only 60 Capsules Ingredients: Each serving (per 2 capsules) contains: Proprietary Amino Acid Formulation Whey Protein Hydrolysate (milk sourced isolate), L-Arginine (as L-Arginine HCl), L-Histidine HCI, L-Glutamine, L-Serine Gamma Amino Butyric Acid Choline Bitartrate Griffonia Seed Extract (5-HTP) Cocoa Extract (6% Theobromine) Grape Seed Extract (85% Polyphenols) Cinnamon (bark) Other Ingredients: Gelatin, Tricalcium Phosphate, Silicon Dioxide, Magnesium Stearate, Microcrystalline Cellulose, Titanium Dioxide, FDandC Red #3, FDandC Blue #1. Distributed exclusively by: Physicians Therapeutics A Division of Targeted Medical Pharma, Inc. Los Angeles, CA 90077 www.ptlcentral.com US Patent 7,582,315; 7,585,523; 7,595,067; 7,601,369. LOT 007007 EXP 08/13
- PRINCIPAL DISPLAY PANEL
- PRINCIPAL DISPLAY PANEL
- PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
THERATRAMADOL-60
tramadol hydrochloride, gaba kitProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:68405-380 Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:68405-380-26 1 in 1 KIT Quantity of Parts Part # Package Quantity Total Product Quantity Part 1 1 BOTTLE 60 Part 2 1 BOTTLE 60 Part 1 of 2 TRAMADOL HYDROCHLORIDE
tramadol hydrochloride tabletProduct Information Item Code (Source) NDC:52959-688(NDC:65162-627) Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength TRAMADOL HYDROCHLORIDE (UNII: 9N7R477WCK) (TRAMADOL - UNII:39J1LGJ30J) TRAMADOL HYDROCHLORIDE 50 mg Product Characteristics Color white (WHITE) Score no score Shape ROUND Size 9mm Flavor Imprint Code AN;627 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:52959-688-60 60 in 1 BOTTLE Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA076003 05/20/2011 Part 2 of 2 THERAMINE 60
gaba capsuleProduct Information Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength .GAMMA.-AMINOBUTYRIC ACID (UNII: 2ACZ6IPC6I) (.GAMMA.-AMINOBUTYRIC ACID - UNII:2ACZ6IPC6I) .GAMMA.-AMINOBUTYRIC ACID 100 mg Inactive Ingredients Ingredient Name Strength GELATIN (UNII: 2G86QN327L) SILICON DIOXIDE (UNII: ETJ7Z6XBU4) TRICALCIUM PHOSPHATE (UNII: K4C08XP666) MAGNESIUM STEARATE (UNII: 70097M6I30) POWDERED CELLULOSE (UNII: SMD1X3XO9M) FD&C BLUE NO. 1 (UNII: H3R47K3TBD) FD&C RED NO. 3 (UNII: PN2ZH5LOQY) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) Product Characteristics Color white (PURPLE, WHITE) Score no score Shape CAPSULE Size 20mm Flavor Imprint Code ; Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 60 in 1 BOTTLE Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date Medical Food 05/20/2011 Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date unapproved drug other 05/20/2011 Labeler - Physician Therapeutics LLC (931940964) Establishment Name Address ID/FEI Business Operations Ameal Pharmaceuticals 831227801 manufacture Establishment Name Address ID/FEI Business Operations Targeted Medical Pharma Inc. 126962740 manufacture Establishment Name Address ID/FEI Business Operations H.J. Harkins Company, Inc. 147681894 repack