Label: enlon- Edrophonium chloride injection
-
Contains inactivated NDC Code(s)
NDC Code(s): 10019-873-15, 10019-873-39 - Packager: Baxter Healthcare Corporation
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: None
Drug Label Information
Updated October 17, 2006
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
- N/A - Section Title Not Found In Database
-
DESCRIPTION
ENLON is a short and rapid-acting cholinergic drug. Chemically, edrophonium chloride is ethyl(m-hydroxyphenyl) dimethylammonium chloride and its structural formula is:
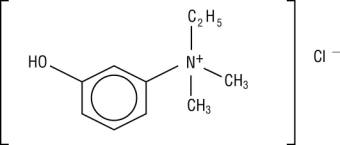
Each mL contains, in a sterile solution, 10 mg edrophonium chloride compounded with 0.45% phenol as a preservative, and 0.2% sodium sulfite as an antioxidant, buffered with sodium citrate and citric acid, and pH adjusted to approximately 5.4.
- ACTIONS
-
INDICATIONS
ENLON is recommended for the differential diagnosis of myasthenia gravis and as an adjunct in the evaluation of treatment requirements in this disease. It may also be used for evaluating emergency treatment in myasthenic crises. Because of its brief duration of action, it is not recommended for maintenance therapy in myasthenia gravis.
ENLON is also useful whenever a curare antagonist is needed to reverse the neuromuscular block produced by curare, tubocurarine, gallamine triethiodide or dimethyl-tubocurarine. It is not effective against decamethonium bromide and succinylcholine chloride. It may be used adjunctively in the treatment of respiratory depression caused by curare overdosage.
- CONTRAINDICATIONS
-
WARNINGS
Whenever anticholinesterase drugs are used for testing, a syringe containing 1 mg of atropine sulfate should be immediately available to be given in aliquots intravenously to counteract severe cholinergic reactions which may occur in the hypersensitive individual, whether he is normal or myasthenic. ENLON should be used with caution in patients with bronchial asthma or cardiac dysrhythmias. The transient bradycardia which sometimes occurs can be relieved by atropine sulfate. Isolated instances of cardiac and respiratory arrest following administration of ENLON have been reported. It is postulated that these are vagotonic effects.
Contains sodium sulfite, a sulfite that may cause allergic-type reactions including anaphylactic symptoms and life-threatening or less severe asthmatic episodes in certain susceptible people. The overall prevalence of sulfite sensitivity in the general population is unknown and probably low. Sulfite sensitivity is seen more frequently in asthmatic than in nonasthmatic people.
-
PRECAUTIONS
Patients may develop “anticholinesterase insensitivity” for brief or prolonged periods. During these periods the patients should be carefully monitored and may need respiratory assistance. Dosages of anticholinesterase drugs should be reduced or withheld until patients again become sensitive to them.
-
ADVERSE REACTIONS
Careful observation should be made for severe cholinergic reactions in the hyperreactive individual. The myasthenic patient in crisis who is being tested with ENLON should be observed for bradycardia or cardiac standstill and cholinergic reactions if an overdose is given.
The following reactions common to anticholinesterase agents may occur, although not all of these reactions have been reported with the administration of ENLON, probably because of its short duration of action and limited indications:
Eye: Increased lacrimation, pupillary constriction, spasm of accommodation, diplopia, conjunctival hyperemia. CNS: Convulsions, dysarthria, dysphonia, dysphagia. Respiratory: Increased tracheobronchial secretions, laryngospasm, bronchiolar constriction, paralysis of muscles of respiration, central respiratory paralysis. Cardiac: Arrhythmias (especially bradycardia), fall in cardiac output leading to hypotension. G.I.: Increased salivary, gastric and intestinal secretion, nausea, vomiting, increased peristalsis, diarrhea, abdominal cramps. Skeletal Muscle: Weakness, fasciculations. Miscellaneous: Increased urinary frequency and incontinence, diaphoresis. -
DOSAGE AND ADMINISTRATION
ENLON Test in the Differential Diagnosis of Myasthenia Gravis 1-8
Intravenous Dosage (Adults)
A tuberculin syringe containing 1 mL (10 mg) of ENLON is prepared with an intravenous needle, and 0.2 mL (2 mg) is injected intravenously within 15 to 30 seconds. The needle is left in situ. Only if no reaction occurs after 45 seconds is the remaining 0.8 mL (8 mg) injected. If a cholinergic reaction (muscarinic side effects, skeletal muscle fasciculations and increased muscle weakness) occurs after injection of 0.2 mL (2 mg), the test is discontinued and atropine sulfate, 0.4 mg to 0.5 mg, is administered intravenously. After one-half hour the test may be repeated.
Intramuscular Dosage (Adults)
In adults with inaccessible veins, dosage for intramuscular injection is 1 mL (10 mg) of ENLON. Subjects who demonstrate hyperreactivity to this injection (cholinergic reaction), should be retested after one-half hour with 0.2 mL (2 mg) of ENLON intramuscularly to rule out false-negative reactions.
Dosage (Children)
The intravenous testing dose of ENLON in children weighing up to 75 lbs is 0.1 mL (1 mg); above this weight, the dose is 0.2 mL (2 mg). If there is no response after 45 seconds, it may be titrated up to 0.5 mL (5 mg) in children under 75 lbs, given in increments of 0.1 mL (1 mg) every 30 to 45 seconds and up to 1 mL (10 mg) in heavier children. In infants, the recommended dose is 0.05 mL (0.5 mg). Because of technical difficulty with intravenous injection in children, the intramuscular route may be used. In children weighing up to 75 lbs, 0.2 mL (2 mg) is injected intramuscularly. In children weighing more than 75 lbs, 0.5 mL (5 mg) is injected intramuscularly. All signs which would appear with the intravenous test appears with the intramuscular test except that there is a delay of two to ten minutes before a reaction is noted.
ENLON Test for Evaluation of Treatment Requirements in Myasthenia Gravis
The recommended dose is 0.1 mL to 0.2 mL (1 mg to 2 mg) of ENLON, administered intravenously one hour after oral intake of the drug being used in treatment.1-5 Response will be myasthenic in the undertreated patient, adequate in the controlled patient, and cholinergic in the overtreated patient. Responses to ENLON in myasthenic and nonmyasthenic individuals are summarized in the following chart.
- *
- Myasthenic Response- occurs in untreated myasthenics and may serve to establish diagnosis; in patients under treatment, indicates that therapy is inadequate.
- †
- Adequate Response- observed in treated patients when therapy is stabilized: a typical response in normal individuals. In addition to this response in non-myasthenics, the phenomenon of forced lid closure is often observed in psychoneurotics.
- ‡
- Cholinergic Response- seen in myasthenics who have been overtreated with anticholinesterase drugs.
Myasthenic* Adequate† Cholinergic‡ Muscle Strength (ptosis, diplopia dysphonia, dysphagia, dysarthria, respiration, limb strength) Increased No change Decreased Fasciculations (orbicularis oculi, facial muscles, limb muscles) Absent Present or absent Present or absent Side reactions (lacrimation diaphoresis, salivation, abdominal cramps, nausea, vomiting, diarrhea) Absent Minimal Severe ENLON Test in Crisis
The term crisis is applied to the myasthenic whenever severe respiratory distress with objective ventilatory inadequacy occurs and the response to medication is not predictable. This state may be secondary to a sudden increase in severity of myasthenia gravis (myasthenic crisis), or to overtreatment with anticholinesterase drugs (cholinergic crisis).
When a patient is apneic, controlled ventilation must be secured immediately in order to avoid cardiac arrest and irreversible central nervous system damage. No attempt is made to test with ENLON until respiratory exchange is adequate.
Dosage used at this time is most important: If the patient is cholinergic, ENLON will cause increased oropharyngeal secretions and further weakness in the muscles of respiration. If the crisis is myasthenic, the test clearly improves respiration and the patient can be treated with longer-acting intravenous anticholinesterase medication. When the test is performed, there should not be more than 0.2 mL (2 mg) ENLON in the syringe. An intravenous dose of 0.1 mL (1 mg) is given initially. The patient’s heart action is carefully observed. If, after an interval of one minute, this dose does not further impair the patient, the remaining 0.1 mL (1 mg) can be injected. If no clear improvement of respiration occurs after 0.2 mL (2 mg) dose, it is usually wisest to discontinue all anticholinesterase drug therapy and secure controlled ventilation by tracheostomy with assisted respiration.5
For Use as a Curare Antagonist
ENLON should be administered by intravenous injection in 1 mL (10 mg) doses given slowly over a period of 30 to 45 seconds so that the onset of cholinergic reaction can be detected. This dosage may be repeated whenever necessary. The maximal dose for any one patient should be 4 mL (40 mg). Because of its brief effect, ENLON should not be given prior to the administration of curare, tubocurarine, gallamine triethiodide or dimethyl-tubocurarine: it should be used at the time when its effect is needed. When given to counteract curare overdosage, the effect of each dose on the respiration should be carefully observed before it is repeated, and assisted ventilation should always be employed.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
-
DRUG INTERACTIONS
Care should be given when administering this drug to patients with symptoms of myasthenic weakness who are also on anticholinesterase drugs. Since symptoms of anticholinesterase overdose (cholinergic crisis) may mimic underdosage (myasthenic weakness), their condition may be worsened by the use of this drug. (See OVERDOSAGE section for treatment.)
-
OVERDOSAGE
With drugs of this type, muscarine-like symptoms (nausea, vomiting, diarrhea, sweating, increased bronchial and salivary secretions and bradycardia) often appear with overdosage (cholinergic crisis). An important complication that can arise is obstruction of the airway by bronchial secretions. These may be managed with suction (especially if tracheostomy has been performed) and by the use of atropine. Many experts have advocated a wide range of dosages of atropine (for ENLON, see atropine dosage below), but if there are copious secretions, up to 1.2 mg intravenously may be given initially and repeated every 20 minutes until secretions are controlled. Signs of atropine overdosage such as dry mouth, flush and tachycardia should be avoided as tenacious secretions and bronchial plugs may form. A total dose of atropine of 5 to 10 mg or even more may be required. The following steps should be taken in the management of overdosage of ENLON:
- Adequate respiratory exchange should be maintained by assuring an open airway and by the use of assisted respiration augmented by oxygen.
- Cardiac function should be monitored until complete stabilization has been achieved
- Atropine sulfate in doses of 0.4 to 0.5 mg should be administered intravenously. This may be repeated every 3 to 10 minutes. Because of the short duration of action of ENLON the total dose required will seldom exceed 2 mg.
- Pralidoxime chloride (a cholinesterase reactivator) may be given intravenously at the rate of 50 to 100 mg per minute; usually the total dose does not exceed 1000 mg. Extreme caution should be exercised in the use of pralidoxime chloride when the cholinergic symptoms are induced by double-bond phosphorous anticholinesterase drugs. 9
- If convulsions occur or shock is present, appropriate measures should be instituted.
- HOW SUPPLIED
-
REFERENCES
- Osserman KE, Kaplan LI. JAMA 1952;150:265.
- Osserman KE, Kaplan LI., Besson G. J Mt Sinai Hosp 1953;20:165.
- Osserman KE, Kaplan LI. Arch Neurol Psychiatr 1953;70:385.
- Osserman KE, Teng P. JAMA 1956;160:153.
- Osserman KE, Genkins G. Ann Ny Acad Sci 1966;135:312.
- Tether JE, Second International Symposium Proceedings, Myasthenia Gravis, 1961, p.444.
- Tether JE, in HF Conn: Current Therapy 1960, Philadelphia, WB Saunders Co, p.551.
- Tether JE, in HF Conn: Current Therapy 1965, Philadelphia, WB Saunders Co, p.556.
- Grob D. Johns RJ. JAMA 1958;166:1855.
Baxter and Enlon are trademarks of Baxter International, Inc.
-
INGREDIENTS AND APPEARANCE
ENLON
edrophonium chloride injectionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:10019-873 Route of Administration INTRAVENOUS, INTRAMUSCULAR Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength edrophonium chloride (UNII: QO611KSM5P) (edrophonium cation - UNII:70FP3JLY7N) 10 mg in 1 mL Inactive Ingredients Ingredient Name Strength phenol (UNII: 339NCG44TV) sodium sulfite (UNII: VTK01UQK3G) sodium citrate (UNII: 1Q73Q2JULR) citric acid (UNII: 2968PHW8QP) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:10019-873-15 1 in 1 PACKAGE 1 NDC:10019-873-39 15 mL in 1 VIAL Labeler - Baxter Healthcare Corporation
