Label: METOPROLOL SUCCINATE- metoprolol succinate tablet, film coated, extended release
-
Contains inactivated NDC Code(s)
NDC Code(s): 58177-358-04, 58177-358-09, 58177-368-04, 58177-368-09, view more58177-368-11, 58177-368-12 - Packager: Ethex Corporation
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: None
- Marketing Status: Abbreviated New Drug Application
Drug Label Information
Updated November 1, 2009
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
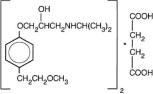
Metoprolol succinate is a beta1-selective (cardioselective) adrenoceptor blocking agent, for oral administration, available as extended-release tablets. Metoprolol succinate extended-release tablets have been formulated to provide a controlled and predictable release of metoprolol for once daily oral administration. The tablets comprise a multiple unit system containing metoprolol succinate in a multitude of controlled-release pellets. Each pellet acts as a separate drug delivery unit and is designed to deliver metoprolol continuously over the dosage interval. The tablets contain 95 and 190 mg of metoprolol succinate equivalent to 100 and 200 mg of metoprolol tartrate, USP, respectively. Its chemical name is (±) 1-(isopropylamino)-3-[p-(2-methoxyethyl) phenoxy]-2-propanol succinate (2:1) (salt). Its structural formula is:
Metoprolol succinate is a white crystalline powder with a molecular weight of 652.8. It is freely soluble in water; soluble in methanol; sparingly soluble in ethanol; slightly soluble in dichloromethane and 2-propanol; practically insoluble in ethyl-acetate, acetone, diethylether and heptane. Inactive ingredients: calcium stearate, carboxymethylcellulose sodium, carnauba wax, croscarmellose sodium, glyceryl behenate, hydrogenated vegetable oil, hypromellose, maltodextrin, methacrylic acid copolymer, microcrystalline cellulose, polydextrose, polyethylene glycol, povidone, sodium stearyl fumarate, titanium dioxide, triacetin, triethyl citrate, vinyl acetate copolymer.
Does not comply with the dissolution test of the USP monograph for metoprolol succinate extended-release tablets.
-
CLINICAL PHARMACOLOGY
General
Metoprolol is a beta1-selective (cardioselective) adrenergic receptor blocking agent. This preferential effect is not absolute, however, and at higher plasma concentrations, metoprolol also inhibits beta2-adrenoreceptors, chiefly located in the bronchial and vascular musculature. Metoprolol has no intrinsic sympathomimetic activity, and membrane-stabilizing activity is detectable only at plasma concentrations much greater than required for beta-blockade. Animal and human experiments indicate that metoprolol slows the sinus rate and decreases AV nodal conduction.
Clinical pharmacology studies have confirmed the beta-blocking activity of metoprolol in man, as shown by (1) reduction in heart rate and cardiac output at rest and upon exercise, (2) reduction of systolic blood pressure upon exercise, (3) inhibition of isoproterenol-induced tachycardia, and (4) reduction of reflex orthostatic tachycardia.
The relative beta1-selectivity of metoprolol has been confirmed by the following: (1) In normal subjects, metoprolol is unable to reverse the beta2-mediated vasodilating effects of epinephrine. This contrasts with the effect of nonselective beta-blockers, which completely reverse the vasodilating effects of epinephrine. (2) In asthmatic patients, metoprolol reduces FEV1 and FVC significantly less than a nonselective beta-blocker, propranolol, at equivalent beta1-receptor blocking doses.
In five controlled studies in normal healthy subjects, the same daily doses of metoprolol succinate extended-release tablets and immediate-release metoprolol were compared in terms of the extent and duration of beta 1-blockade produced. Both formulations were given in a dose range equivalent to 100 to 400 mg of immediate release metoprolol per day. In these studies, metoprolol succinate extended-release tablets were administered once a day and immediate-release metoprolol was administered once to four times a day. A sixth controlled study compared the beta1- blocking effects of a 50 mg daily dose of the two formulations. In each study, beta1-blockade was expressed as the percent change from baseline in exercise heart rate following standardized submaximal exercise tolerance tests at steady state. Metoprolol succinate extended-release tablets administered once a day, and immediate-release metoprolol administered once to four times a day, provided comparable total beta1-blockade over 24 hours (area under the beta1-blockade versus time curve) in the dose range 100 to 400 mg. At a dosage of 50 mg once daily, metoprolol succinate extended-release tablets produced significantly higher total beta1-blockade over 24 hours than immediate-release metoprolol. For metoprolol succinate extended-release tablets, the percent reduction in exercise heart rate was relatively stable throughout the entire dosage interval and the level of beta1-blockade increased with increasing doses from 50 to 300 mg daily. The effects at peak/trough (i.e., at 24 hours post-dosing) were 14/9, 16/10, 24/14, 27/22 and 27/20% reduction in exercise heart rate for doses of 50, 100, 200, 300 and 400 mg metoprolol succinate extended-release tablets once a day, respectively. In contrast to metoprolol succinate extended-release tablets, immediate-release metoprolol given at a dose of 50 to 100 mg once a day produced a significantly larger peak effect on exercise tachycardia, but the effect was not evident at 24 hours. To match the peak to trough ratio obtained with metoprolol succinate extended-release tablets over the dosing range of 200 to 400 mg, a t.i.d. to q.i.d. divided dosing regimen was required for immediate-release metoprolol. A controlled crossover study in heart failure patients compared the plasma concentrations and beta1-blocking effects of 50 mg immediate-release metoprolol administered t.i.d., 100 mg and 200 mg metoprolol succinate extended-release tablets once daily. A 50 mg dose of immediate-release metoprolol t.i.d. produced a peak plasma level of metoprolol similar to the peak level observed with 200 mg of metoprolol succinate extended-release tablets. A 200 mg dose of metoprolol succinate extended-release tablets produced a larger effect on suppression of exercise-induced and Holter-monitored heart rate over 24 hours compared to 50 mg t.i.d. of immediate-release metoprolol.
The relationship between plasma metoprolol levels and reduction in exercise heart rate is independent of the pharmaceutical formulation. Using an Emax model, the maximum effect is a 30% reduction in exercise heart rate, which is attributed to beta1-blockade. Beta1-blocking effects in the range of 30 to 80% of the maximal effect (approximately 8 to 23% reduction in exercise heart rate) corresponds to metoprolol plasma concentrations from 30 to 540 nmol/L. The relative beta1-selectivity of metoprolol diminishes and blockade of beta2-adrenoceptors increases at plasma concentrations above 300 nmol/L.
Although beta-adrenergic receptor blockade is useful in the treatment of angina, hypertension, and heart failure there are situations in which sympathetic stimulation is vital. In patients with severely damaged hearts, adequate ventricular function may depend on sympathetic drive. In the presence of AV block, beta-blockade may prevent the necessary facilitating effect of sympathetic activity on conduction. Beta2-adrenergic blockade results in passive bronchial constriction by interfering with endogenous adrenergic bronchodilator activity in patients subject to bronchospasm and may also interfere with exogenous bronchodilators in such patients.
In other studies, treatment with metoprolol succinate extended-release tablets produced an improvement in left ventricular ejection fraction. Metoprolol succinate extended-release tablets were also shown to delay the increase in left ventricular end-systolic and end-diastolic volumes after 6 months of treatment.
Pharmacokinetics
Adults
In man, absorption of metoprolol is rapid and complete. Plasma levels following oral administration of conventional metoprolol tablets, however, approximate 50% of levels following intravenous administration, indicating about 50% first-pass metabolism. Metoprolol crosses the blood-brain barrier and has been reported in the CSF in a concentration 78% of the simultaneous plasma concentration.
Plasma levels achieved are highly variable after oral administration. Only a small fraction of the drug (about 12%) is bound to human serum albumin. Metoprolol is a racemic mixture of R- and S-enantiomers, and is primarily metabolized by CYP2D6. When administered orally, it exhibits stereoselective metabolism that is dependent on oxidation phenotype. Elimination is mainly by biotransformation in the liver, and the plasma half-life ranges from approximately 3 to 7 hours. Less than 5% of an oral dose of metoprolol is recovered unchanged in the urine; the rest is excreted by the kidneys as metabolites that appear to have no beta-blocking activity. Following intravenous administration of metoprolol, the urinary recovery of unchanged drug is approximately 10%. The systemic availability and half-life of metoprolol in patients with renal failure do not differ to a clinically significant degree from those in normal subjects. Consequently, no reduction in dosage is usually needed in patients with chronic renal failure.
Metoprolol is metabolized predominantly by CYP2D6, an enzyme that is absent in about 8% of Caucasians (poor metabolizers) and about 2% of most other populations. CYP2D6 can be inhibited by a number of drugs. Concomitant use of inhibiting drugs in poor metabolizers will increase blood levels of metoprolol several-fold, decreasing metoprolol's cardioselectivity (see PRECAUTIONS, Drug Interactions).
In comparison to conventional metoprolol, the plasma metoprolol levels following administration of metoprolol succinate extended-release tablets are characterized by lower peaks, longer time to peak and significantly lower peak to trough variation. The peak plasma levels following once-daily administration of metoprolol succinate extended-release tablets average one-fourth to one-half the peak plasma levels obtained following a corresponding dose of conventional metoprolol, administered once daily or in divided doses. At steady state the average bioavailability of metoprolol following administration of metoprolol succinate extended-release tablets, across the dosage range of 50 to 400 mg once daily, was 77% relative to the corresponding single or divided doses of conventional metoprolol. Nevertheless, over the 24-hour dosing interval, beta1-blockade is comparable and dose-related (see CLINICAL PHARMACOLOGY). The bioavailability of metoprolol shows a dose-related, although not directly proportional, increase with dose and is not significantly affected by food following metoprolol succinate extended-release tablets administration.
Hypertension
The mechanism of the antihypertensive effects of beta-blocking agents has not been elucidated. However, several possible mechanisms have been proposed: (1) competitive antagonism of catecholamines at peripheral (especially cardiac) adrenergic neuron sites, leading to decreased cardiac output; (2) a central effect leading to reduced sympathetic outflow to the periphery; and (3) suppression of renin activity.
Clinical Trials
In a double-blind study, 1092 patients with mild-to-moderate hypertension were randomized to once daily metoprolol succinate extended-release tablets (25, 100, or 400 mg), felodipine extended-release tablets, the combination, or placebo. After 9 weeks, metoprolol succinate extended-release tablets alone decreased sitting blood pressure by 6-8/4-7 mmHg (placebo-corrected change from baseline) at 24 hours post-dose. The combination of metoprolol succinate extended-release tablets with felodipine extended-release tablets has greater effects on blood pressure.
In controlled clinical studies, an immediate-release dosage form of metoprolol was an effective antihypertensive agent when used alone or as concomitant therapy with thiazide-type diuretics at dosages of 100 to 450 mg daily. Metoprolol succinate extended-release tablets, in dosages of 100 to 400 mg once daily, produces similar beta1-blockade as conventional metoprolol tablets administered two to four times daily. In addition, metoprolol succinate extended-release tablets administered at a dose of 50 mg once daily lowered blood pressure 24 hours post-dosing in placebo-controlled studies. In controlled, comparative, clinical studies, immediate-release metoprolol appeared comparable as an antihypertensive agent to propranolol, methyldopa, and thiazide-type diuretics, and affected both supine and standing blood pressure. Because of variable plasma levels attained with a given dose and lack of a consistent relationship of antihypertensive activity to drug plasma concentration, selection of proper dosage requires individual titration.
Angina Pectoris
By blocking catecholamine-induced increases in heart rate, in velocity and extent of myocardial contraction, and in blood pressure, metoprolol reduces the oxygen requirements of the heart at any given level of effort, thus making it useful in the long- term management of angina pectoris.
Clinical Trials
In controlled clinical trials, an immediate-release formulation of metoprolol has been shown to be an effective antianginal agent, reducing the number of angina attacks and increasing exercise tolerance. The dosage used in these studies ranged from 100 to 400 mg daily. Metoprolol succinate extended-release tablets, in dosages of 100 to 400 mg once daily, has been shown to possess beta-blockade similar to conventional metoprolol tablets administered two to four times daily.
Heart Failure
The precise mechanism for the beneficial effects of beta-blockers in heart failure has not been elucidated.
Clinical Trials
MERIT-HF was a double-blind, placebo-controlled study of metoprolol succinate extended-release tablets conducted in 14 countries including the U.S. It randomized 3991 patients (1990 to metoprolol succinate extended-release tablets) with ejection fraction ≤0.40 and NYHA Class II-IV heart failure attributable to ischemia, hypertension, or cardiomyopathy. The protocol excluded patients with contraindications to beta-blocker use, those expected to undergo heart surgery, and those within 28 days of myocardial infarction or unstable angina. The primary endpoints of the trial were (1) all-cause mortality plus all-cause hospitalization (time to first event) and (2) all-cause mortality. Patients were stabilized on optimal concomitant therapy for heart failure, including diuretics, ACE inhibitors, cardiac glycosides, and nitrates. At randomization, 41% of patients were NYHA Class II, 55% NYHA Class III; 65% of patients had heart failure attributed to ischemic heart disease; 44% had a history of hypertension; 25% had diabetes mellitus; 48% had a history of myocardial infarction. Among patients in the trial, 90% were on diuretics, 89% were on ACE inhibitors, 64% were on digitalis, 27% were on a lipid-lowering agent, 37% were on an oral anticoagulant, and the mean ejection fraction was 0.28. The mean duration of follow-up was one year. At the end of the study, the mean daily dose of metoprolol succinate extended-release tablets was 159 mg.
The trial was terminated early for a statistically significant reduction in all-cause mortality (34%, nominal p=0.00009). The risk of all-cause mortality plus all-cause hospitalization was reduced by 19% (p=0.00012). The trial also showed improvements in heart failure-related mortality and heart failure-related hospitalizations, and NYHA functional class.
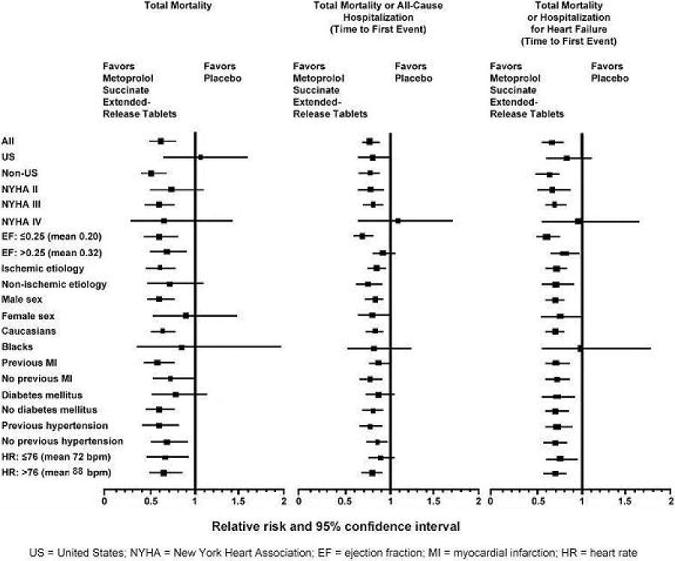
The table below shows the principal results for the overall study population. The figure below illustrates principal results for a wide variety of subgroup comparisons, including U.S. vs. non-U.S. populations (the latter of which was not pre-specified). The combined endpoints of all-cause mortality plus all-cause hospitalization and of mortality plus heart failure hospitalization showed consistent effects in the overall study population and the subgroups, including women and the U.S. population. However, in the U.S. subgroup (n=1071) and women (n=898), overall mortality and cardiovascular mortality appeared less affected. Analyses of female and U.S. patients were carried out because they each represented about 25% of the overall population. Nonetheless, subgroup analyses can be difficult to interpret and it is not known whether these represent true differences or chance effects.
Clinical Endpoints in the MERIT-HF Study † Time to first event
‡ Comparison of treatment groups examines the number of hospitalizations (Wilcoxon test); relative risk and risk reduction are not applicable.
Clinical EndpointNumber of Patients
Relative
Risk
(95% CI)Risk Reduction
with
Metoprolol Succinate Extended-release tablets
Nominal
P-value
Placebo
n=2001Metoprolol Succinate Extended-release tablets
n=1990All-cause mortality plus all-cause hospitalization† 767 641 0.81
(0.73-0.90)19% 0.00012 All-cause mortality 217 145 0.66
(0.53-0.81)34% 0.00009 All-cause mortality plus heart failure hospitalization† 439 311 0.69
(0.60-0.80)31% 0.0000008 Cardiovascular mortality 203 128 0.62
(0.50-0.78)38% 0.000022 Sudden death 132 79 0.59
(0.45-0.78)41% 0.0002 Death due to worsening heart failure 58 30 0.51
(0.33-0.79)49% 0.0023 Hospitalizations due to worsening heart failure‡ 451 317 N/A N/A 0.0000076 Cardiovascular hospitalization‡ 773 649 N/A N/A 0.00028 Results for Subgroups in MERIT-HF
-
INDICATIONS AND USAGE
Hypertension
Metoprolol succinate extended-release tablets are indicated for the treatment of hypertension. It may be used alone or in combination with other antihypertensive agents.
Angina Pectoris
Metoprolol succinate extended-release tablets are indicated in the long-term treatment of angina pectoris.
Heart Failure
Metoprolol succinate extended-release tablets are indicated for the treatment of stable, symptomatic (NYHA Class II or III) heart failure of ischemic, hypertensive, or cardiomyopathic origin. It was studied in patients already receiving ACE inhibitors, diuretics, and, in the majority of cases, digitalis. In this population, metoprolol succinate extended-release tablets decreased the rate of mortality plus hospitalization, largely through a reduction in cardiovascular mortality and hospitalizations for heart failure.
-
CONTRAINDICATIONS
Metoprolol succinate extended-release tablets are contraindicated in severe bradycardia, heart block greater than first degree, cardiogenic shock, decompensated cardiac failure, sick sinus syndrome (unless a permanent pacemaker is in place), and in patients who are hypersensitive to any component of this product.
-
WARNINGS
Ischemic Heart Disease: Following abrupt cessation of therapy with certain beta-blocking agents, exacerbations of angina pectoris and, in some cases, myocardial infarction have occurred. When discontinuing chronically administered metoprolol succinate extended-release tablets, particularly in patients with ischemic heart disease, the dosage should be gradually reduced over a period of 1 to 2 weeks and the patient should be carefully monitored. If angina markedly worsens or acute coronary insufficiency develops, metoprolol succinate extended-release tablets administration should be reinstated promptly, at least temporarily, and other measures appropriate for the management of unstable angina should be taken. Patients should be warned against interruption or discontinuation of therapy without the physician's advice. Because coronary artery disease is common and may be unrecognized, it may be prudent not to discontinue metoprolol succinate extended-release tablets therapy abruptly even in patients treated only for hypertension.
Bronchospastic Diseases: PATIENTS WITH BRONCHOSPASTIC DISEASES SHOULD, IN GENERAL, NOT RECEIVE BETA-BLOCKERS. Because of its relative beta1-selectivity, however, metoprolol succinate extended-release tablets may be used with caution in patients with bronchospastic disease who do not respond to, or cannot tolerate, other antihypertensive treatment. Since beta1-selectivity is not absolute, a beta2-stimulating agent should be administered concomitantly, and the lowest possible dose of metoprolol succinate extended-release tablets should be used (see DOSAGE AND ADMINISTRATION).
Pheochromocytoma: If metoprolol succinate extended-release tablets are used in the setting of pheochromocytoma, it should be given in combination with an alpha blocker, and only after the alpha blocker has been initiated. Administration of beta blockers alone in the setting of pheochromocytoma has been associated with a paradoxical increase in blood pressure due to the attenuation of beta-mediated vasodilatation in skeletal muscle.
Major Surgery: The necessity or desirability of withdrawing beta-blocking therapy prior to major surgery is controversial; the impaired ability of the heart to respond to reflex adrenergic stimuli may augment the risks of general anesthesia and surgical procedures.
Metoprolol succinate extended-release tablets, like other beta-blockers, is a competitive inhibitor of beta-receptor agonists, and its effects can be reversed by administration of such agents, e.g., dobutamine or isoproterenol. However, such patients may be subject to protracted severe hypotension. Difficulty in restarting and maintaining the heart beat has also been reported with beta-blockers.
Diabetes and Hypoglycemia: Metoprolol succinate extended-release tablets should be used with caution in diabetic patients if a beta-blocking agent is required. Beta-blockers may mask tachycardia occurring with hypoglycemia, but other manifestations such as dizziness and sweating may not be significantly affected.
Thyrotoxicosis: Beta-adrenergic blockade may mask certain clinical signs (e.g., tachycardia) of hyperthyroidism. Patients suspected of developing thyrotoxicosis should be managed carefully to avoid abrupt withdrawal of beta-blockade, which might precipitate a thyroid storm.
-
PRECAUTIONS
General
Metoprolol succinate extended-release tablets should be used with caution in patients with impaired hepatic function. In patients with pheochromocytoma, an alpha-blocking agent should be initiated prior to the use of any beta-blocking agent (see WARNINGS).
Worsening cardiac failure may occur during up-titration of metoprolol succinate extended-release tablets. If such symptoms occur, diuretics should be increased and the dose of metoprolol succinate extended-release tablets should not be advanced until clinical stability is restored (see DOSAGE AND ADMINISTRATION). It may be necessary to lower the dose of metoprolol succinate extended-release tablets or temporarily discontinue it. Such episodes do not preclude subsequent successful titration of metoprolol succinate extended-release tablets.
Information for Patients
Patients should be advised to take metoprolol succinate regularly and continuously, as directed, preferably with or immediately following meals. If a dose should be missed, the patient should take only the next scheduled dose (without doubling it). Patients should not interrupt or discontinue metoprolol succinate extended-release tablets without consulting the physician.
Patients should be advised (1) to avoid operating automobiles and machinery or engaging in other tasks requiring alertness until the patient 's response to therapy with metoprolol succinate extended-release tablets has been determined; (2) to contact the physician if any difficulty in breathing occurs; (3) to inform the physician or dentist before any type of surgery that he or she is taking metoprolol succinate extended-release tablets.
Heart failure patients should be advised to consult their physician if they experience signs or symptoms of worsening heart failure such as weight gain or increasing shortness of breath.
Laboratory Tests
Clinical laboratory findings may include elevated levels of serum transaminase, alkaline phosphatase, and lactate dehydrogenase.
Drug Interactions
Catecholamine-depleting drugs (e.g., reserpine, monoamine oxidase (MAO) inhibitors) may have an additive effect when given with beta-blocking agents. Patients treated with metoprolol succinate extended-release tablets plus a catecholamine depletor should therefore be closely observed for evidence of hypotension or marked bradycardia, which may produce vertigo, syncope, or postural hypotension.
Drugs that inhibit CYP2D6 such as quinidine, fluoxetine, paroxetine, and propafenone are likely to increase metoprolol concentration. In healthy subjects with CYP2D6 extensive metabolizer phenotype, coadministration of quinidine 100 mg and immediate release metoprolol 200 mg tripled the concentration of S-metoprolol and doubled the metoprolol elimination half-life. In four patients with cardiovascular disease, coadministration of propafenone 150 mg t.i.d. with immediate-release metoprolol 50 mg t.i.d. resulted in two- to five-fold increases in the steady-state concentration of metoprolol. These increases in plasma concentration would decrease the cardioselectivity of metoprolol.
Both digitalis glycosides and beta-blockers slow atrioventricular conduction and decrease heart rate. Concomitant use can increase the risk of bradycardia.
Beta-blockers may exacerbate the rebound hypertension which can follow the withdrawal of clonidine. If the two drugs are coadministered, the beta blocker should be withdrawn several days before the gradual withdrawal of clonidine. If replacing clonidine by beta-blocker therapy, the introduction of beta-blockers should be delayed for several days after clonidine administration has stopped.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term studies in animals have been conducted to evaluate the carcinogenic potential of metoprolol tartrate. In 2-year studies in rats at three oral dosage levels of up to 800 mg/kg/day (41 times, on a mg/m2 basis, the daily dose of 200 mg for a 60-kg patient), there was no increase in the development of spontaneously occurring benign or malignant neoplasms of any type. The only histologic changes that appeared to be drug related were an increased incidence of generally mild focal accumulation of foamy macrophages in pulmonary alveoli and a slight increase in biliary hyperplasia. In a 21-month study in Swiss albino mice at three oral dosage levels of up to 750 mg/kg/day (18 times, on a mg/m2 basis, the daily dose of 200 mg for a 60-kg patient), benign lung tumors (small adenomas) occurred more frequently in female mice receiving the highest dose than in untreated control animals. There was no increase in malignant or total (benign plus malignant) lung tumors, nor in the overall incidence of tumors or malignant tumors. This 21-month study was repeated in CD-1 mice, and no statistically or biologically significant differences were observed between treated and control mice of either sex for any type of tumor.
All genotoxicity tests performed on metoprolol tartrate (a dominant lethal study in mice, chromosome studies in somatic cells, a Salmonella/mammalian-microsome mutagenicity test, and a nucleus anomaly test in somatic interphase nuclei) and metoprolol succinate (a Salmonella/mammalian-microsome mutagenicity test) were negative.
No evidence of impaired fertility due to metoprolol tartrate was observed in a study performed in rats at doses up to 22 times, on a mg/m2 basis, the daily dose of 200 mg in a 60-kg patient.
Pregnancy Category C
Metoprolol tartrate has been shown to increase post-implantation loss and decrease neonatal survival in rats at doses up to 22 times, on a mg/m2 basis, the daily dose of 200 mg in a 60 kg patient. Distribution studies in mice confirm exposure of the fetus when metoprolol tartrate is administered to the pregnant animal. These studies have revealed no evidence of impaired fertility or teratogenicity. There are no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
Nursing Mothers
Metoprolol is excreted in breast milk in very small quantities. An infant consuming 1 liter of breast milk daily would receive a dose of less than 1 mg of the drug. Caution should be exercised when metoprolol succinate extended-release tablets is administered to a nursing woman.
Pediatric Use
Safety and effectiveness of metoprolol succinate have not been established in patients < 6 years of age. Due to AstraZeneca's marketing exclusivity rights, this generic drug product is not labeled for pediatric use. Pediatric use information is approved for AstraZeneca's metoprolol succinate extended-release tablets.
Geriatric Use
Clinical studies of metoprolol succinate extended-release tablets in hypertension did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience in hypertensive patients has not identified differences in responses between elderly and younger patients.
Of the 1,990 patients with heart failure randomized to metoprolol succinate extended-release tablets in the MERIT-HF trial, 50% (990) were 65 years of age and older and 12% (238) were 75 years of age and older. There were no notable differences in efficacy or the rate of adverse events between older and younger patients.
In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Risk of Anaphylactic Reactions
While taking beta-blockers, patients with a history of severe anaphylactic reactions to a variety of allergens may be more reactive to repeated challenge, either accidental, diagnostic or therapeutic. Such patients may be unresponsive to the usual doses of epinephrine used to treat allergic reaction.
-
ADVERSE REACTIONS
Hypertension and Angina
Most adverse effects have been mild and transient. The following adverse reactions have been reported for immediate release metoprolol tartrate.
Central Nervous System: Tiredness and dizziness have occurred in about 10 of 100 patients. Depression has been reported in about 5 of 100 patients. Mental confusion and short- term memory loss have been reported. Headache, somnolence, nightmares, and insomnia have also been reported.
Cardiovascular: Shortness of breath and bradycardia have occurred in approximately 3 of 100 patients. Cold extremities; arterial insufficiency, usually of the Raynaud type; palpitations; congestive heart failure; peripheral edema; syncope; chest pain; and hypotension have been reported in about 1 of 100 patients (see CONTRAINDICATIONS, WARNINGS, and PRECAUTIONS).
Respiratory: Wheezing (bronchospasm) and dyspnea have been reported in about 1 of 100 patients (see WARNINGS).
Gastrointestinal: Diarrhea has occurred in about 5 of 100 patients. Nausea, dry mouth, gastric pain, constipation, flatulence, digestive tract disorders and heartburn have been reported in about 1 of 100 patients.
Hypersensitive Reactions: Pruritus or rash have occurred in about 5 of 100 patients. Worsening of psoriasis has also been reported.
Miscellaneous: Peyronie's disease has been reported in fewer than 1 of 100,000 patients. Musculoskeletal pain, blurred vision, decreased libido, and tinnitus have also been reported.
There have been rare reports of reversible alopecia, agranulocytosis, and dry eyes. Discontinuation of the drug should be considered if any such reaction is not otherwise explicable. The oculomucocutaneous syndrome associated with the beta-blocker practolol has not been reported with metoprolol.
Potential Adverse Reactions
In addition, there are a variety of adverse reactions not listed above which have been reported with other beta-adrenergic blocking agents and should be considered potential adverse reactions to metoprolol succinate.
Central Nervous System: Reversible mental depression progressing to catatonia; an acute reversible syndrome characterized by disorientation for time and place, short-term memory loss, emotional lability, slightly clouded sensorium, and decreased performance on neuropsychometrics.
Cardiovascular: Intensification of AV block (see CONTRAINDICATIONS).
Hematologic: Agranulocytosis, nonthrombocytopenic purpura, thrombocytopenic purpura.
Hypersensitive Reactions: Fever combined with aching and sore throat, laryngospasm, and respiratory distress.
Heart Failure
In the MERIT-HF study, serious adverse events and adverse events leading to discontinuation of study medication were systematically collected. In the MERIT-HF study comparing metoprolol succinate extended-release tablets in daily doses up to 200 mg (mean dose 159 mg once-daily) (n=1990) to placebo (n=2001), 10.3% of metoprolol succinate extended-release tablets patients discontinued for adverse events vs. 12.2% of placebo patients.
The table below lists adverse events in the MERIT-HF study that occurred at an incidence of equal to or greater than 1% in the metoprolol succinate extended-release tablets group and greater than placebo by more than 0.5%, regardless of the assessment of causality.
Adverse Events Occurring in the MERIT-HF Study at an Incidence ≥ 1% in the Metoprolol Succinate Extended-Release Tablets Group and Greater than Placebo by More Than 0.5% Metoprolol Succinate Extended-Release Tablets
N=1990
% of patientsPlacebo
N=2001
% of patientsDizziness/vertigo 1.8 1.0 Bradycardia 1.5 0.4 Accident and/or injury 1.4 0.8 Other adverse events with an incidence of >1% on metoprolol succinate extended-release tablets and as common on placebo (within 0.5%) included myocardial infarction, pneumonia, cerebrovascular disorder, chest pain, dyspnea/dyspnea aggravated, syncope, coronary artery disorder, ventricular tachycardia/arrhythmia aggravated, hypotension, diabetes mellitus/diabetes mellitus aggravated, abdominal pain, and fatigue.
Postmarketing Experience
The following adverse reactions have been reported with metoprolol succinate extended-release tablets in worldwide postmarketing use, regardless of causality:
Cardiovascular: 2nd and 3rd degree heart block, cardiogenic shock in patients with acute myocardial infarction.
Gastrointestinal: hepatitis, vomiting.
Hematologic: thrombocytopenia.
Musculoskeletal: arthralgia.
Nervous System/Psychiatric: anxiety/nervousness, hallucinations, paresthesia.
Reproductive, male: impotence.
Skin: increased sweating, photosensitivity, urticaria.
Special Sense Organs: taste disturbances.
-
OVERDOSAGE
Acute Toxicity
There have been a few reports of overdosage with metoprolol succinate extended-release tablets and no specific overdosage information was obtained with this drug, with the exception of animal toxicology data. However, since metoprolol succinate extended-release tablets (metoprolol succinate salt) contain the same active moiety, metoprolol, as conventional metoprolol tablets (metoprolol tartrate salt), the recommendations on overdosage for metoprolol conventional tablets are applicable to metoprolol succinate extended-release tablets.
Signs and Symptoms
Overdosage of metoprolol succinate extended-release tablets may lead to severe hypotension, sinus bradycardia, atrioventricular block, heart failure, cardiogenic shock, cardiac arrest, bronchospasm, impairment of consciousness/coma, nausea, vomiting, and cyanosis.
Treatment
In general, patients with acute or recent myocardial infarction or congestive heart failure may be more hemodynamically unstable than other patients and should be treated accordingly. When possible the patient should be treated under intensive care conditions. On the basis of the pharmacologic actions of metoprolol, the following general measures should be employed:
-
DOSAGE AND ADMINISTRATION
Metoprolol succinate extended-release tablets are intended for once daily administration. For treatment of hypertension and angina, when switching from immediate-release metoprolol to metoprolol succinate extended-release tablets, the same total daily dose of metoprolol succinate extended-release tablets should be used. Dosages of metoprolol succinate extended-release tablets should be individualized and titration may be needed in some patients.
Metoprolol succinate extended-release tablets are scored and can be divided; however, the whole or half tablet should be swallowed whole and not chewed or crushed.
Hypertension
The usual initial dosage is 25 to 100 mg daily in a single dose, whether used alone or added to a diuretic. The dosage may be increased at weekly (or longer) intervals until optimum blood pressure reduction is achieved. In general, the maximum effect of any given dosage level will be apparent after 1 week of therapy. Dosages above 400 mg per day have not been studied.
Due to AstraZeneca's marketing exclusivity rights, this generic drug product is not labeled for pediatric use. Dosage and administration information in pediatric patients 6 years and older is approved for AstraZeneca's metoprolol succinate extended-release tablets.
Angina Pectoris
The dosage of metoprolol succinate extended-release tablets should be individualized. The usual initial dosage is 100 mg daily, given in a single dose. The dosage may be gradually increased at weekly intervals until optimum clinical response has been obtained or there is a pronounced slowing of the heart rate. Dosages above 400 mg per day have not been studied. If treatment is to be discontinued, the dosage should be reduced gradually over a period of 1 to 2 weeks (see WARNINGS).
Heart Failure
Dosage must be individualized and closely monitored during up-titration. Prior to initiation of metoprolol succinate extended-release tablets, the dosing of diuretics, ACE inhibitors, and digitalis (if used) should be stabilized. The recommended starting dose of metoprolol succinate extended-release tablets is 25 mg once daily for two weeks in patients with NYHA Class II heart failure and 12.5 mg once daily in patients with more severe heart failure. The dose should then be doubled every two weeks to the highest dosage level tolerated by the patient or up to 200 mg of metoprolol succinate extended-release tablets. If transient worsening of heart failure occurs, it may be treated with increased doses of diuretics, and it may also be necessary to lower the dose of metoprolol succinate extended-release tablets or temporarily discontinue it. The dose of metoprolol succinate extended-release tablets should not be increased until symptoms of worsening heart failure have been stabilized. Initial difficulty with titration should not preclude later attempts to introduce metoprolol succinate extended-release tablets. If heart failure patients experience symptomatic bradycardia, the dose of metoprolol succinate extended-release tablets should be reduced.
-
HOW SUPPLIED
Metoprolol succinate extended-release tablets for oral administration are supplied as follows:
100 mg: White film-coated round tablets with a bevel edge containing 95 mg of metoprolol succinate equivalent to 100 mg of metoprolol tartrate, USP and debossed “368” on one side with a bisect on the other side.
NDC 58177-368-04………………….…Bottles of 100
NDC 58177-368-09………………….…Bottles of 1000
NDC 58177-368-12………………….…Bottles of 5000
NDC 58177-368-11………………….…Packages of 100 (10 x 10 cards)
200 mg: White film-coated oval tablets containing 190 mg of metoprolol succinate equivalent to 200 mg of metoprolol tartrate, USP and debossed “358” on one side with a bisect on the other side.
NDC 58177-358-04………………….…Bottles of 100
NDC 58177-358-09………………….…Bottles of 1000
Store at 25°C (77°F). Excursions permitted to 15°-30°C (59°-86°F). (See USP Controlled Room Temperature.)
Manufactured by
KV Pharmaceutical Co. for
ETHEX Corporation
St. Louis, MO 63044P5081-7
02/09 - PRINCIPAL DISPLAY PANEL
- PRINCIPAL DISPLAY PANEL
- PRINCIPAL DISPLAY PANEL
- PRINCIPAL DISPLAY PANEL
- PRINCIPAL DISPLAY PANEL
-
INGREDIENTS AND APPEARANCE
METOPROLOL SUCCINATE EXTENDED-RELEASE
metoprolol succinate tablet, film coated, extended releaseProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:58177-368 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength metoprolol succinate (UNII: TH25PD4CCB) (METOPROLOL - UNII:GEB06NHM23) metoprolol succinate 90 mg Inactive Ingredients Ingredient Name Strength CALCIUM STEARATE (UNII: 776XM7047L) CARBOXYMETHYLCELLULOSE SODIUM (UNII: K679OBS311) CARNAUBA WAX (UNII: R12CBM0EIZ) CROSCARMELLOSE SODIUM (UNII: M28OL1HH48) GLYCERYL BEHENATE (UNII: R8WTH25YS2) HYPROMELLOSE (UNII: 3NXW29V3WO) MALTODEXTRIN (UNII: 7CVR7L4A2D) METHACRYLIC ACID - METHYL METHACRYLATE COPOLYMER (1:1) (UNII: 74G4R6TH13) CELLULOSE, MICROCRYSTALLINE (UNII: OP1R32D61U) POLYDEXTROSE (UNII: VH2XOU12IE) POLYETHYLENE GLYCOL (UNII: 3WJQ0SDW1A) POVIDONE (UNII: FZ989GH94E) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) TRIACETIN (UNII: XHX3C3X673) TRIETHYL CITRATE (UNII: 8Z96QXD6UM) Product Characteristics Color white (white) Score 2 pieces Shape ROUND (ROUND) Size 10mm Flavor Imprint Code 368 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:58177-368-04 100 in 1 BOTTLE 2 NDC:58177-368-09 1000 in 1 BOTTLE 3 NDC:58177-368-12 5000 in 1 BOTTLE 4 NDC:58177-368-11 100 in 1 BLISTER PACK Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA076640 11/01/2009 METOPROLOL SUCCINATE EXTENDED-RELEASE
metoprolol succinate tablet, film coated, extended releaseProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:58177-358 Route of Administration ORAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength metoprolol succinate (UNII: TH25PD4CCB) (METOPROLOL - UNII:GEB06NHM23) metoprolol succinate 190 mg Inactive Ingredients Ingredient Name Strength CALCIUM STEARATE (UNII: 776XM7047L) CARBOXYMETHYLCELLULOSE SODIUM (UNII: K679OBS311) CARNAUBA WAX (UNII: R12CBM0EIZ) CROSCARMELLOSE SODIUM (UNII: M28OL1HH48) GLYCERYL BEHENATE (UNII: R8WTH25YS2) HYPROMELLOSE (UNII: 3NXW29V3WO) MALTODEXTRIN (UNII: 7CVR7L4A2D) METHACRYLIC ACID - METHYL METHACRYLATE COPOLYMER (1:1) (UNII: 74G4R6TH13) CELLULOSE, MICROCRYSTALLINE (UNII: OP1R32D61U) POLYDEXTROSE (UNII: VH2XOU12IE) POLYETHYLENE GLYCOL (UNII: 3WJQ0SDW1A) POVIDONE (UNII: FZ989GH94E) SODIUM STEARYL FUMARATE (UNII: 7CV7WJK4UI) TITANIUM DIOXIDE (UNII: 15FIX9V2JP) TRIACETIN (UNII: XHX3C3X673) TRIETHYL CITRATE (UNII: 8Z96QXD6UM) Product Characteristics Color white (white) Score 2 pieces Shape OVAL (OVAL) Size 9mm Flavor Imprint Code 358 Contains Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:58177-358-04 100 in 1 BOTTLE 2 NDC:58177-358-09 1000 in 1 BOTTLE Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA076640 11/01/2009 Labeler - Ethex Corporation (615424686) Registrant - KV Pharmaceutical (006291405) Establishment Name Address ID/FEI Business Operations KV Pharmaceutical (EC IV) 161097225 MANUFACTURE Establishment Name Address ID/FEI Business Operations KV Pharmaceutical (Westport) 152053658 MANUFACTURE Establishment Name Address ID/FEI Business Operations KV Pharmaceutical (EC I) 034060843 ANALYSIS Establishment Name Address ID/FEI Business Operations KV Pharmaceutical (Metro 2) 961097503 ANALYSIS