DETAILED PATIENT LABELING
Norgestimate and Ethinyl Estradiol Tablets USP, 0.25 mg/0.035 mg
PLEASE NOTE: This labeling is revised from time to time as important new medical information becomes available. Therefore, please review this labeling carefully.
This product (like all oral contraceptives) does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
Norgestimate and Ethinyl Estradiol Tablets USP Regimen
Each blue tablet contains 0.25 mg norgestimate USP and 0.035 mg ethinyl estradiol USP. Each light green tablet contains inert ingredients.
INTRODUCTION
Any woman who considers using oral contraceptives (the birth control pill or the pill) should understand the benefits and risks of using this form of birth control. This patient labeling will give you much of the information you will need to make this decision and will also help you determine if you are at risk of developing any of the serious side effects of the pill. It will tell you how to use the pill properly so that it will be as effective as possible. However, this labeling is not a replacement for a careful discussion between you and your healthcare professional. You should discuss the information provided in this labeling with him or her, both when you first start taking the pill and during your revisits. You should also follow your healthcare professional’s advice with regard to regular check-ups while you are on the pill.
EFFECTIVENESS OF ORAL CONTRACEPTIVES FOR CONTRACEPTION
Oral contraceptives or "birth control pills" or "the pill" are used to prevent pregnancy and are more effective than most other non-surgical methods of birth control. When they are taken correctly without missing any pills, the chance of becoming pregnant is approximately 1% per year (1 pregnancy per 100 women per year of use). Typical failure rates, including women who do not always take the pill correctly, are approximately 5% per year (5 pregnancies per 100 women per year of use). The chance of becoming pregnant increases with each missed pill during a menstrual cycle.
In comparison, typical failure rates for other non-surgical methods of birth control during the first year of use are as follows:
| Implant: <1% | Male sterilization: <1% |
| Injection: <1% | Cervical Cap with spermicides: 20 to 40% |
| IUD: 1 to 2% | Condom alone (male): 14% |
| Diaphragm with spermicides: 20% | Condom alone (female): 21% |
| Spermicides alone: 26% | Periodic abstinence: 25% |
| Vaginal sponge: 20 to 40% | Withdrawal: 19% |
| Female sterilization: <1% | No methods: 85% |
WHO SHOULD NOT TAKE ORAL CONTRACEPTIVES
Cigarette smoking increases the risk of serious cardiovascular side effects from oral contraceptive use. This risk increases with age and with heavy smoking (15 or more cigarettes per day) and is quite marked in women over 35 years of age. Women who use oral contraceptives are strongly advised not to smoke.
Some women should not use the pill. For example, you should not take the pill if you have any of the following conditions:
- A history of heart attack or stroke
- Blood clots in the legs (thrombophlebitis), lungs (pulmonary embolism), or eyes
- A history of blood clots in the deep veins of your legs
- Chest pain (angina pectoris)
- Known or suspected breast cancer or cancer of the lining of the uterus, cervix or vagina
- Unexplained vaginal bleeding (until a diagnosis is reached by your healthcare professional)
- Yellowing of the whites of the eyes or of the skin (jaundice) during pregnancy or during previous use of the pill
- Liver tumor (benign or cancerous) or active liver disease
- Known or suspected pregnancy
- Valvular heart disease with complications
- Severe hypertension
- Diabetes with vascular involvement
- Headaches with focal neurological symptoms
- Major surgery with prolonged immobilization
- Hypersensitivity to any component of this product
Tell your healthcare professional if you have had any of these conditions. Your healthcare professional can recommend a safer method of birth control.
OTHER CONSIDERATIONS BEFORE TAKING ORAL CONTRACEPTIVES
Tell your healthcare professional if you have or have had:
- Breast nodules, fibrocystic disease of the breast, an abnormal breast x-ray or mammogram
- Diabetes
- Elevated cholesterol or triglycerides
- High blood pressure
- Migraine or other headaches or epilepsy
- Mental depression
- Gallbladder, liver, heart or kidney disease
- History of scanty or irregular menstrual periods
Women with any of these conditions should be checked often by their healthcare professional if they choose to use oral contraceptives.
Also, be sure to inform your healthcare professional if you smoke or are on any medications.
RISKS OF TAKING ORAL CONTRACEPTIVES
1. Risk of Developing Blood Clots
Blood clots and blockage of blood vessels are one of the most serious side effects of taking oral contraceptives and can cause death or serious disability. In particular, a clot in the legs can cause thrombophlebitis and a clot that travels to the lungs can cause a sudden blocking of the vessel carrying blood to the lungs. Rarely, clots occur in the blood vessels of the eye and may cause blindness, double vision, or impaired vision.
If you take oral contraceptives and need elective surgery, need to stay in bed for a prolonged illness or injury or have recently delivered a baby, you may be at risk of developing blood clots. You should consult your healthcare professional about stopping oral contraceptives four weeks before surgery and not taking oral contraceptives for two weeks after surgery or during bed rest. You should also not take oral contraceptives soon after delivery of a baby. It is advisable to wait for at least four weeks after delivery if you are not breast feeding. If you are breast feeding, you should wait until you have weaned your child before using the pill. (See also the section on Breast Feeding in General Precautions.)
The risk of circulatory disease in oral contraceptive users may be higher in users of high- dose pills and may be greater with longer duration of oral contraceptive use. In addition, some of these increased risks may continue for a number of years after stopping oral contraceptives. The risk of abnormal blood clotting increases with age in both users and nonusers of oral contraceptives, but the increased risk from the oral contraceptive appears to be present at all ages. For women aged 20 to 44 it is estimated that about 1 in 2,000 using oral contraceptives will be hospitalized each year because of abnormal clotting. Among nonusers in the same age group, about 1 in 20,000 would be hospitalized each year. For oral contraceptive users in general, it has been estimated that in women between the ages of 15 and 34 the risk of death due to a circulatory disorder is about 1 in 12,000 per year, whereas for nonusers the rate is about 1 in 50,000 per year. In the age group 35 to 44, the risk is estimated to be about 1 in 2,500 per year for oral contraceptive users and about 1 in 10,000 per year for nonusers.
2. Heart Attacks and Strokes
Oral contraceptives may increase the tendency to develop strokes (stoppage or rupture of blood vessels in the brain) and angina pectoris and heart attacks (blockage of blood vessels in the heart). Any of these conditions can cause death or serious disability.
Smoking greatly increases the possibility of suffering heart attacks and strokes. Furthermore, smoking and the use of oral contraceptives greatly increase the chances of developing and dying of heart disease.
3. Gallbladder Disease
Oral contraceptive users probably have a greater risk than nonusers of having gallbladder disease, although this risk may be related to pills containing high doses of estrogens.
4. Liver Tumors
In rare cases, oral contraceptives can cause benign but dangerous liver tumors. These benign liver tumors can rupture and cause fatal internal bleeding. In addition, some studies report an increased risk of developing liver cancer. However, liver cancers are rare.
5. Cancer of the Reproductive Organs and Breasts
Various studies give conflicting reports on the relationship between breast cancer and oral contraceptive use. Oral contraceptive use may slightly increase your chance of having breast cancer diagnosed, particularly after using hormonal contraceptives at a younger age. After you stop using hormonal contraceptives, the chances of having breast cancer diagnosed begin to go back down. You should have regular breast examinations by a healthcare professional and examine your own breasts monthly. Tell your healthcare professional if you have a family history of breast cancer or if you have had breast nodules or an abnormal mammogram. Women who currently have or have had breast cancer should not use oral contraceptives because breast cancer is usually a hormone-sensitive tumor.
Some studies have found an increase in the incidence of cancer of the cervix in women who use oral contraceptives. However, this finding may be related to factors other than the use of oral contraceptives. There is insufficient evidence to rule out the possibility that the pill may cause such cancers.
ESTIMATED RISK OF DEATH FROM A BIRTH CONTROL METHOD OR PREGNANCY
All methods of birth control and pregnancy are associated with a risk of developing certain diseases which may lead to disability or death. An estimate of the number of deaths associated with different methods of birth control and pregnancy has been calculated and is shown in the following table.
| Annual Number of Birth-Related or Method-Related Deaths Associated With Control of Fertility Per 100,000 Non-Sterile Women, by Fertility Control Method According to Age | ||||||
| Method of control and outcome | 15-19 | 20-24 | 25-29 | 30-34 | 35-39 | 40-44 |
| No fertility control methods* | 7.0 | 7.4 | 9.1 | 14.8 | 25.7 | 28.2 |
| Oral contraceptives | 0.3 | 0.5 | 0.9 | 1.9 | 13.8 | 31.6 |
| non-smoker** | ||||||
| Oral contraceptives | 2.2 | 3.4 | 6.6 | 13.5 | 51.1 | 117.2 |
| smoker** | ||||||
| IUD** | 0.8 | 0.8 | 1.0 | 1.0 | 1.4 | 1.4 |
| Condom* | 1.1 | 1.6 | 0.7 | 0.2 | 0.3 | 0.4 |
| Diaphragm/spermicide* | 1.9 | 1.2 | 1.2 | 1.3 | 2.2 | 2.8 |
| Periodic abstinence* | 2.5 | 1.6 | 1.6 | 1.7 | 2.9 | 3.6 |
| *Deaths are birth-related | ||||||
| **Deaths are method-related | ||||||
| Adapted from H.W.Ory, ref. #35 | ||||||
In the above table, the risk of death from any birth control method is less than the risk of childbirth, except for oral contraceptive users over the age of 35 who smoke and pill users over the age of 40 even if they do not smoke. It can be seen in the table that for women aged 15 to 39, the risk of death was highest with pregnancy (7 to 26 deaths per 100,000 women, depending on age). Among pill users who do not smoke, the risk of death was always lower than that associated with pregnancy for any age group less than 40. Over the age of 40, the risk increases to 32 deaths per 100,000 women, compared to 28 associated with pregnancy in that age group. However, for pill users who smoke and are over the age of 35, the estimated number of deaths exceeds those for other methods of birth control. If a woman is over the age of 40 and smokes, her estimated risk of death is four times higher (117/100,000 women) than the estimated risk associated with pregnancy (28/100,000 women) in that age group.
The suggestion that women over 40 who do not smoke should not take oral contraceptives is based on information from older, higher-dose pills. An Advisory Committee of the FDA discussed this issue in 1989 and recommended that the benefits of low-dose oral contraceptive use by healthy, non-smoking women over 40 years of age may outweigh the possible risks. Older women, as all women, who take oral contraceptives, should take an oral contraceptive which contains the least amount of estrogen and progestogen that is compatible with the individual patient needs.
WARNING SIGNALS
If any of these adverse effects occur while you are taking oral contraceptives, call your healthcare professional immediately:
- Sharp chest pain, coughing of blood, or sudden shortness of breath (indicating a possible clot in the lung)
- Pain in the calf (indicating a possible clot in the leg)
- Crushing chest pain or heaviness in the chest (indicating a possible heart attack)
- Sudden severe headache or vomiting, dizziness or fainting, disturbances of vision or speech, weakness, or numbness in an arm or leg (indicating a possible stroke)
- Sudden partial or complete loss of vision (indicating a possible clot in the eye)
- Breast lumps (indicating possible breast cancer or fibrocystic disease of the breast; ask your healthcare professional to show you how to examine your breasts)
- Severe pain or tenderness in the stomach area (indicating a possibly ruptured liver tumor)
- Difficulty in sleeping, weakness, lack of energy, fatigue, or change in mood (possibly indicating severe depression)
- Jaundice or a yellowing of the skin or eyeballs, accompanied frequently by fever, fatigue, loss of appetite, dark colored urine, or light colored bowel movements (indicating possible liver problems)
SIDE EFFECTS OF ORAL CONTRACEPTIVES
In addition to the risks and more serious side effects discussed above, the following may also occur:
1. Irregular Vaginal Bleeding
Irregular vaginal bleeding or spotting may occur while you are taking the pills. Irregular bleeding may vary from slight staining between menstrual periods to breakthrough bleeding which is a flow much like a regular period. Irregular bleeding occurs most often during the first few months of oral contraceptive use, but may also occur after you have been taking the pill for some time. Such bleeding may be temporary and usually does not indicate any serious problems. It is important to continue taking your pills on schedule. If the bleeding occurs in more than one cycle or lasts for more than a few days, talk to your healthcare professional.
2. Contact Lenses
If you wear contact lenses and notice a change in vision or an inability to wear your lenses, contact your healthcare professional.
GENERAL PRECAUTIONS
1. Missed Periods and Use of Oral Contraceptives Before or During Early Pregnancy
There may be times when you may not menstruate regularly after you have completed taking a cycle of pills. If you have taken your pills regularly and miss one menstrual period, continue taking your pills for the next cycle but be sure to inform your healthcare professional. If you have not taken the pills daily as instructed and missed a menstrual period, or if you missed two consecutive menstrual periods, you may be pregnant. Check with your healthcare professional immediately to determine whether you are pregnant. Stop taking your pills if you are pregnant.
There is no conclusive evidence that oral contraceptive use is associated with an increase in birth defects, when taken inadvertently during early pregnancy. Previously, a few studies had reported that oral contraceptives might be associated with birth defects, but these findings have not been seen in more recent studies. Nevertheless, oral contraceptives should not be used during pregnancy. You should check with your healthcare professional about risks to your unborn child of any medication taken during pregnancy.
2. While Breast Feeding
If you are breast feeding, consult your healthcare professional before starting oral contraceptives. Some of the drug will be passed on to the child in the milk. A few adverse effects on the child have been reported, including yellowing of the skin (jaundice) and breast enlargement. In addition, combination oral contraceptives may decrease the amount and quality of your milk. If possible, do not use combination oral contraceptives while breast feeding. You should use another method of contraception since breast feeding provides only partial protection from becoming pregnant and this partial protection decreases significantly as you breast feed for longer periods of time. You should consider starting combination oral contraceptives only after you have weaned your child completely.
3. Laboratory Tests
If you are scheduled for any laboratory tests, tell your healthcare professional you are taking birth control pills. Certain blood tests may be affected by birth control pills.
4. Drug Interactions
Certain drugs may interact with birth control pills to make them less effective in preventing pregnancy or cause an increase in breakthrough bleeding. Such drugs include rifampin, drugs used for epilepsy such as barbiturates (for example, phenobarbital), topiramate (Topamax®), carbamazepine (Tegretol® is one brand of this drug), or phenytoin (Dilantin® is one brand of this drug), phenylbutazone (Butazolidin® is one brand), certain drugs used in the treatment of HIV or AIDS, and possibly certain antibiotics. Pregnancies and breakthrough bleeding have been reported by women who also used some form of the herbal supplement St. John’s Wort while using combined hormonal contraceptives.
You may need to use additional contraception when you take drugs which can make oral contraceptives less effective. Be sure to tell your healthcare professional if you are taking or start taking any medications while taking birth control pills.
5. Sexually Transmitted Diseases
Norgestimate and ethinyl estradiol tablets (like all oral contraceptives) are intended to prevent pregnancy. Oral contraceptives do not protect against transmission of HIV (AIDS) and other sexually transmitted diseases such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
HOW TO TAKE THE PILL
IMPORTANT POINTS TO REMEMBER
BEFORE YOU START TAKING YOUR PILLS:
- BE SURE TO READ THESE DIRECTIONS: Before you start taking your pills. Anytime you are not sure what to do.
- THE RIGHT WAY TO TAKE THE PILL IS TO TAKE ONE PILL EVERY DAY AT THE SAME TIME. If you miss pills you could get pregnant. This includes starting the pack late. The more pills you miss, the more likely you are to get pregnant.
- MANY WOMEN HAVE SPOTTING OR LIGHT BLEEDING, OR MAY FEEL SICK TO THEIR STOMACH DURING THE FIRST 1-3 PACKS OF PILLS. If you feel sick to your stomach or have spotting or light bleeding, do not stop taking the pill. The problem will usually go away. If it doesn't go away, check with your healthcare professional.
- MISSING PILLS CAN ALSO CAUSE SPOTTING OR LIGHT BLEEDING, even when you make up these missed pills. On the days you take 2 pills to make up for missed pills, you could also feel a little sick to your stomach.
- IF YOU HAVE VOMITING OR DIARRHEA, OR IF YOU TAKE SOME MEDICINES, including some antibiotics, your pills may not work as well. Use a back-up method (such as condoms or spermicide) until you check with your healthcare professional.
- IF YOU HAVE TROUBLE REMEMBERING TO TAKE THE PILL, talk to your healthcare professional about how to make pill-taking easier or about using another method of birth control.
- IF YOU HAVE ANY QUESTIONS OR ARE UNSURE ABOUT THE INFORMATION IN THIS LEAFLET, call your healthcare professional.
BEFORE YOU START TAKING YOUR PILLS
1.DECIDE WHAT TIME OF DAY YOU WANT TO TAKE YOUR PILL
It is important to take it at about the same time every day.
2.LOOK AT YOUR PILL PACK
The pill pack has 21 "active" pills (with hormones) to take for 3 weeks. This is followed by 1 week of "reminder" light green pills (without hormones).
Norgestimate and Ethinyl Estradiol Tablets: There are 21 blue "active" pills, and 7 light green "reminder" pills.
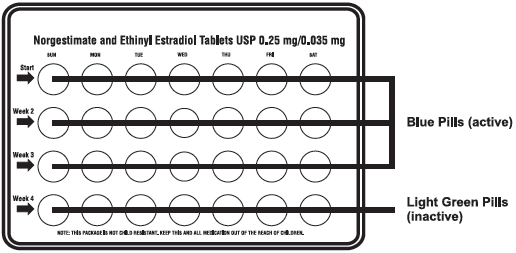
3.ALSO FIND:
A.where on the pack to start taking pills
B. in what order to take the pills.
4.BE SURE YOU HAVE READY AT ALL TIMES
ANOTHER KIND OF BIRTH CONTROL (such as condoms or spermicide) to use as a backup method in case you miss pills
AN EXTRA, FULL PILL PACK
WHEN TO START THE FIRST PACK OF PILLS
You have a choice of which day to start taking your first pack of pills. Norgestimate and ethinyl estradiol tablets are available in a blister pack which is preset for a Sunday Start. Day 1 Start is also provided. Decide with your healthcare professional which is the best day for you. Pick a time of day which will be easy to remember.
Sunday Start:
Norgestimate and Ethinyl Estradiol Tablets: Take the first blue "active" pill of the first pack on the Sunday after your period starts, even if you are still bleeding. If your period begins on Sunday, start the pack that same day.
Use another method of birth control such as condoms or spermicide as a back-up method if you have sex anytime from the Sunday you start your first pack until the next Sunday (7 days).
Day 1 Start:
Norgestimate and Ethinyl Estradiol Tablets: Take the first blue "active" pill of the first pack during the first 24 hours of your period.
1. Pick the day label strip that starts with the first day of your period (this is the day you start bleeding or spotting, even if it is almost midnight when the bleeding begins).
2. Place this day label strip on the tablet blister card over the area that has the days of the week (starting with Sunday) imprinted in the plastic.
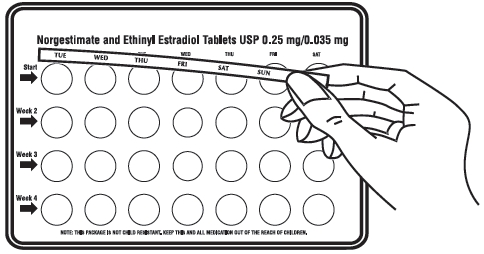
Note: If the first day of your period is a Sunday, you can skip steps # 1 and # 2
You will not need to use a back-up method of birth control, since you are starting the pill at the beginning of your period.
WHAT TO DO DURING THE MONTH
-
TAKE ONE PILL AT THE SAME TIME EVERY DAY UNTIL THE PACK IS EMPTY.
Do not skip pills even if you are spotting or bleeding between monthly periods or feel sick to your stomach (nausea).
Do not skip pills even if you do not have sex very often. -
WHEN YOU FINISH A PACK OR SWITCH YOUR BRAND OF PILLS:
Start the next pack on the day after your last “reminder” pill. Do not wait any days between packs.
WHAT TO DO IF YOU MISS PILLS
Norgestimate and Ethinyl Estradiol Tablets:
If you MISS 1 blue "active" pill:
- Take it as soon as you remember. Take the next pill at your regular time. This means you may take 2 pills in 1 day.
- You do not need to use a back-up birth control method if you have sex.
If you MISS 2 blue "active" pills in a row in WEEK 1 OR WEEK 2 of your pack:
- Take 2 pills on the day you remember and 2 pills the next day.
- Then take 1 pill a day until you finish the pack.
- You COULD BECOME PREGNANT if you have sex in the 7 days after you miss pills. You MUST use another birth control method (such as condoms or spermicide) as a back-up method for those 7 days.
If you MISS 2 blue "active" pills in a row in THE 3RD WEEK:
If you are a Sunday Starter:
1. Keep taking 1 pill every day until Sunday. On Sunday, THROW OUT the rest of the pack and start a new pack of pills that same day.
If you are a Day 1 Starter:
THROW OUT the rest of the pill pack and start a new pack that same day.
2. You may not have your period this month but this is expected. However, if you miss your period 2 months in a row, call your healthcare professional because you might be pregnant.
3. You COULD BECOME PREGNANT if you have sex in the 7 days after you miss pills. You MUST use another birth control method (such as condoms or spermicide) as a back-up method for those 7 days.
If you MISS 3 OR MORE blue "active" pills in a row (during the first 3 weeks):
If you are a Sunday Starter:
1. Keep taking 1 pill every day until Sunday. On Sunday, THROW OUT the rest of the pack and start a new pack of pills that same day.
If you are a Day 1 Starter:
THROW OUT the rest of the pill pack and start a new pack that same day.
2. You may not have your period this month but this is expected. However, if you miss your period 2 months in a row, call your healthcare professional because you might be pregnant.
3. You COULD BECOME PREGNANT if you have sex in the 7 days after you miss pills. You MUST use another birth control method (such as condoms or spermicide) as a back-up method for those 7 days.
A REMINDER:
If you forget any of the 7 light green "reminder" pills in Week 4:
THROW AWAY the pills you missed.
Keep taking 1 pill each day until the pack is empty.
You do not need a back-up method.
FINALLY, IF YOU ARE STILL NOT SURE WHAT TO DO ABOUT THE PILLS YOU HAVE MISSED:
Use a BACK-UP METHOD anytime you have sex.
KEEP TAKING ONE "ACTIVE" PILL EACH DAY until you can reach your healthcare professional.
PREGNANCY DUE TO PILL FAILURE
The incidence of pill failure resulting in pregnancy is approximately 5%, including women who do not always take the pills exactly as directed. If failure does occur, the risk to the fetus is minimal.
PREGNANCY AFTER STOPPING THE PILL
There may be some delay in becoming pregnant after you stop using oral contraceptives, especially if you had irregular menstrual cycles before you used oral contraceptives. It may be advisable to postpone conception until you begin menstruating regularly once you have stopped taking the pill and desire pregnancy.
There does not appear to be any increase in birth defects in newborn babies when pregnancy occurs soon after stopping the pill.
OVERDOSAGE
Serious ill effects have not been reported following ingestion of large doses of oral contraceptives by young children. Overdosage may cause nausea and withdrawal bleeding in females. In case of overdosage, contact your healthcare professional or pharmacist.
OTHER INFORMATION
Your healthcare professional will take a medical and family history before prescribing oral contraceptives and will examine you. The physical examination may be delayed to another time if you request it and the healthcare professional believes that it is a good medical practice to postpone it. You should be reexamined at least once a year. Be sure to inform your healthcare professional if there is a family history of any of the conditions listed previously in this leaflet. Be sure to keep all appointments with your healthcare professional, because this is a time to determine if there are early signs of side effects of oral contraceptive use.
Do not use the drug for any condition other than the one for which it was prescribed. This drug has been prescribed specifically for you; do not give it to others who may want birth control pills.
HEALTH BENEFITS FROM ORAL CONTRACEPTIVES
In addition to preventing pregnancy, use of combination oral contraceptives may provide certain benefits. They are:
- menstrual cycles may become more regular
- blood flow during menstruation may be lighter and less iron may be lost. Therefore, anemia due to iron deficiency is less likely to occur
- pain or other symptoms during menstruation may be encountered less frequently
- ectopic (tubal) pregnancy may occur less frequently
- noncancerous cysts or lumps in the breast may occur less frequently
- acute pelvic inflammatory disease may occur less frequently
- oral contraceptive use may provide some protection against developing two forms of cancer: cancer of the ovaries and cancer of the lining of the uterus.
If you want more information about birth control pills, ask your healthcare professional or pharmacist. They have a more technical leaflet called the Professional Labeling, which you may wish to read. The professional labeling is also published in a book entitled Physicians' Desk Reference, available in many book stores and public libraries.
Keep out of reach of children.
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature].
Protect from light.
