|
Medication Guide
Lazanda® (La-ZAN-da) CII
(fentanyl) nasal spray
|
|
IMPORTANT:
Do not use LAZANDA unless you are regularly using another opioid pain medicine around-the-clock for at least one week or longer for your cancer pain and your body is used to
these medicines (this means that you are opioid tolerant). You can ask your healthcare provider if you are opioid tolerant.
Keep LAZANDA in a safe place away from children.
Get emergency medical help right away if:
-
a child takes LAZANDA. LAZANDA can cause an overdose and death in any child who takes it
-
an adult who has not been prescribed LAZANDA takes it
-
an adult who is not already taking opioids around-the-clock takes LAZANDA
-
These are medical emergencies that can cause death.
|
|
LAZANDA is:
- A strong prescription pain medicine that contains an opioid (narcotic) that is used to manage breakthrough pain in
adults (18 years of age and older) with cancer who are already routinely taking other opioid pain medicines
around-the-clock for cancer pain. LAZANDA is started only after you have been taking other opioid pain medicines and your body has become
used to them (you are opioid tolerant). Do not use LAZANDA if you are not opioid tolerant.
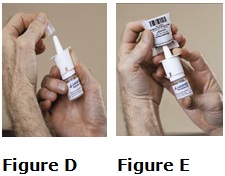
- A nasal spray. You use LAZANDA by placing the nozzle attached to the bottle in your nostril and spraying. See the Medication Guide section
“
When taking LAZANDA”
and the
“
Instructions for Use”
at the end of this Medication Guide
- An opioid pain medicine that can put you at risk for overdose and death. Even if you take your dose correctly as prescribed you are at risk for opioid addiction, abuse, and misuse that can lead to death.
|
|
Important information about LAZANDA:
-
Get emergency help right away if you take too much LAZANDA (overdose). When you first start taking LAZANDA, when your dose is changed,
or if you take too much (overdose), serious or life-threatening breathing problems that can lead to death may occur.
- Taking LAZANDA with other opioid medicines, that may make you sleepy, such as other pain medicines, anti-depressants, sleeping pills, anti-anxiety medicines,
antihistamines, or tranquilizers, or with alcohol or street drugs can cause severe drowsiness, confusion, breathing problems, coma, and death.
- Never give anyone else your LAZANDA. They could die from taking it. Store LAZANDA away from children and in a safe place to prevent stealing or abuse.
Selling or giving away LAZANDA is against the law.
- If you stop taking your around-the-clock opioid pain medicine for your cancer pain,
you must stop using LAZANDA. You may no longer be opioid tolerant.
Talk to your healthcare provider about how to treat your pain.
- LAZANDA is available only through a program called the
Transmucosal
Immediate
Release
Fentanyl (TIRF)
Risk
Evaluation
and
Mitigation Strategy (REMS) Access program.
To receive LAZANDA, you must:
- talk to your healthcare provider
- understand the benefits and risks of LAZANDA
- agree to all of the instructions
- sign the Patient-Prescriber Agreement form
- LAZANDA is only available at pharmacies that are part of the TIRF REMS Access program. Your healthcare provider will let you know the pharmacy closest
to your home where you can have your LAZANDA prescription filled.
Be very careful about taking other medicines that may make you sleepy, such as other pain medicines, anti-depressants, sleeping pills, anti-anxiety medicines, antihistamines, or tranquilizers.
Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine.
|
|
Do not take LAZANDA if:
- You are not opioid tolerant. Opioid tolerant means that you are already taking other opioid pain medicines around-the-clock for at least one week
or longer for your cancer pain, and your body is used to these medicines.
- You have severe asthma, trouble breathing, or other lung problems.
- You have a bowel blockage or have narrowing of the stomach or intestines.
- You are allergic to any of the ingredients in LAZANDA. See the end of this Medication Guide for a complete list of ingredients in LAZANDA.
- You have short-term pain that you would expect to go away in a few days, such as:
- pain after surgery
- headache or migraine
- dental pain
|
|
Before taking LAZANDA, tell your healthcare provider if you have a history of:
- troubled breathing or lung problems such as asthma, wheezing, or shortness of breath
- head injury, seizures
- slow heart rate or other heart problems
- low blood pressure
- abuse of street or prescription drugs, alcohol addiction, or mental health problems
- mental problems [including major depression, schizophrenia or hallucinations (seeing or hearing things that are not there)]
- problems urinating
- liver, kidney, thyroid problems
- pancreas or gallbladder problems
|
|
Tell your healthcare provider if you are:
-
Pregnant or planning to become pregnant. Prolonged use of LAZANDA during pregnancy can cause withdrawal symptoms in your newborn baby that could be life-threatening if not recognized and treated.
-
Breastfeeding. LAZANDA passes into breast milk and may harm your baby.
- Taking prescription over-the-counter medicines, vitamins, or herbal supplements. Taking LAZANDA with certain other medicines can cause serious side effects that could lead to death.
|
|
When taking LAZANDA:
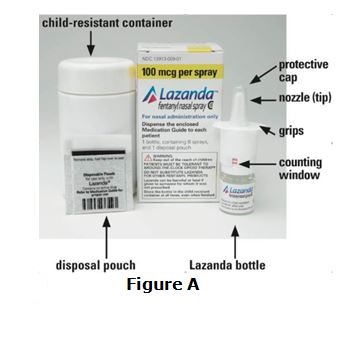
- Know that LAZANDA comes in 3 strengths. When you are first prescribed LAZANDA, your healthcare provider will start you with the lower strength medicine, and will
change the dose until you and your healthcare provider find the right dose for you.
- Do not change your dose of LAZANDA unless your healthcare provider tells you to.
-
See the detailed
Patient Instructions for Use at the end of this Medication Guide for information about how to use LAZANDA.
- The beginning dose of LAZANDA is always 1 spray in one of your nostrils.
- Always use 1 dose of LAZANDA for an episode of breakthrough cancer pain exactly as your healthcare provider tells you to. As your dose is adjusted, your healthcare provider
will tell you whether your dose of LAZANDA is 1, 2, 3 or 4 sprays:
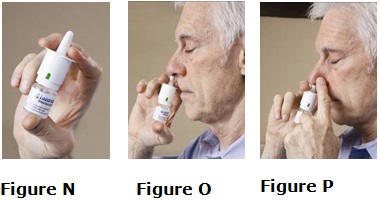
- 1 spray is given by spraying 1 time into one of your nostrils
- 2 sprays are given by spraying 1 time into each nostril for a total of 2 sprays
- 3 sprays are given by spraying alternately into each nostril as follows:
- 1 time right nostril, 1 time left nostril, 1 time right nostril for a total of 3 sprays
- 4 sprays are given by spraying 2 times into each nostril.
- Change (alternate) nostrils for each spray, for example, right, left, right, left for a total of 4 sprays.
- You must never use more than 4 sprays (2 sprays in alternating nostrils) for an episode of breakthrough pain.
- If an episode of breakthrough cancer pain continues for more than 30 minutes after you take a dose of LAZANDA, follow your healthcare provider’s instructions about taking a short-acting opioid pain medicine to manage your pain.
- Wait at least 2 hours before treating a new episode of breakthrough cancer pain with LAZANDA.
- It is important for you to keep taking your around-the-clock opioid pain medicine while using LAZANDA.
- Talk to your healthcare provider if your dose of LAZANDA does not relieve your breakthrough cancer pain. Your healthcare provider will decide if your dose of LAZANDA needs to be changed.
- Talk to your healthcare provider if you have more than 4 episodes of breakthrough cancer pain per day. The dose of your around-the-clock opioid pain medicine may need to be adjusted.
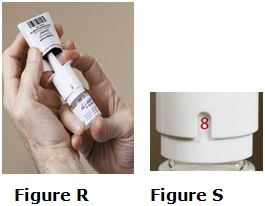
- The LAZANDA nasal spray pump provides a total of 8 full sprays. When there is a red number “8” in the counting window, you have used all the medicine in the bottle. You may still see medicine in the bottle, but there is not enough for a full dose. Do not try to take more than 8 sprays from a bottle of LAZANDA.
- If you use too much LAZANDA or overdose, you or your caregiver should call for emergency medical help or have someone take you to the nearest hospital emergency room right away.
- Do not stop taking LAZANDA without talking to your healthcare provider.
- After you stop taking, or when LAZANDA is no longer needed, see “
How should I dispose of LAZANDA when it is no longer needed?” for proper disposal of LAZANDA.
-
DO NOT Drive or operate heavy machinery, until you know how LAZANDA affects you. LAZANDA can make you sleepy, dizzy, or lightheaded.
-
DO NOT Drink alcohol or use prescription or over-the-counter medicines that contain alcohol. Using products containing alcohol during treatment with LAZANDA may cause you to overdose and die.
-
DO NOT Switch from LAZANDA to other medicines that contain fentanyl without talking to your healthcare provider. The amount of fentanyl in a dose of LAZANDA is not the same as the amount of fentanyl in other medicines that contain fentanyl. Your healthcare provider will prescribe a starting dose of LAZANDA that may be different than other fentanyl containing medicines you may have been taking.
|
|
The possible side effects of LAZANDA:
- constipation, nausea, sleepiness, vomiting, tiredness, headache, dizziness, abdominal pain, weakness, anxiety, depression, rash, trouble sleeping, low red blood cell count, swelling of the arms, hands, legs and feet . Call your healthcare provider if you have any of these symptoms and they are severe.
- Decreased blood pressure. This can make you feel dizzy or lightheaded if you get up too fast from sitting or lying down.
Get emergency medical help if you have:
- trouble breathing, shortness of breath, fast heartbeat, chest pain, swelling of your face, tongue, or throat, extreme drowsiness, light-headedness
when changing positions, feeling faint, agitation, high body temperature, trouble walking, stiff muscles, or mental changes such as confusion.
- These symptoms can be a sign that you have used too much LAZANDA or the dose is too high for you.
These symptoms may lead to serious problems or death if not treated right away. If you have any of these symptoms, do not use any more LAZANDA
until you have talked to your healthcare provider.
These are not all the possible side effects of LAZANDA. Call your doctor for medical advice about side effects.
You may report side effects to FDA at 1-800-FDA-1088. For more information go to dailymed.nlm.nih.gov
|
| This Medication Guide has been approved by the U.S. Food and Drug Administration | Revised: 12/2016 |