Medication Guide
EXUBERA® (eg-ZU-ber-uh)
(insulin human [rDNA origin]) Inhalation Powder
Carefully read the Instructions for Use at the end of this Medication Guide, so you will be sure to get the right amount of your insulin.
Read this Medication Guide that comes with EXUBERA before you start using it, and each time you get a refill. There may be new information. This Medication Guide does not take the place of talking with your healthcare provider about your medical condition or treatment.
What is the most important information I should know about EXUBERA?
- EXUBERA is a prescription medicine that contains an insulin powder that you breathe in (inhale) through your mouth using the EXUBERA® Inhaler. It is used to treat adults with diabetes. It helps to control high blood sugar.
- Do not use EXUBERA if you smoke, start smoking, or if you quit smoking less than 6 months ago. Smoking can increase the amount of EXUBERA you get and may cause your blood sugar to get dangerously low. If you smoke, or you quit smoking less than 6 months ago, you will need a different treatment for your diabetes.
-
EXUBERA may lower your lung function, so:
- •
- You need to have lung tests before you start EXUBERA, and after you start EXUBERA, you may need to have lung tests again later as directed by your healthcare provider.
- •
- EXUBERA is not recommended for people that have chronic lung disease (such as asthma or chronic obstructive pulmonary disease or emphysema).
- •
- Also, EXUBERA should not be used at all by people with unstable or poorly controlled lung disease.
- The dose of EXUBERA is different from other insulin. Make sure you take the exact dose of EXUBERA that your healthcare provider prescribes.
- EXUBERA comes in 1 mg dose or in 3 mg dose "blisters", which are small foil dose packets. "Blister" is a standard term for the shape and type of foil dose packet that holds the insulin powder. Each individual dose of EXUBERA is enclosed in one of these small foil "blister" packets. For the rest of this Medication Guide, these small foil "blister" dose packets will just be called blisters. These blisters come packaged together in a larger foil overwrap package.
- Make sure you get the right dose from your pharmacy. Do not use three 1 mg blisters in place of one 3 mg blister because you may get too much insulin. If you use 3 mg blisters as a part of your usual dosing and you cannot get the 3 mg blisters for some time, call your healthcare provider for advice. If you need to take the insulin before you have spoken to your healthcare provider, use two 1 mg blisters as a temporary replacement for one 3 mg blister. Then, check your blood sugar levels and continue to call your healthcare provider for advice.
What is EXUBERA?
- EXUBERA is a prescription medicine that contains an insulin powder that you breathe in (inhale) through your mouth using the EXUBERA® Inhaler. It is used to treat adults with diabetes. It helps to control high blood sugar.
- For adults with type 2 diabetes, EXUBERA may be used by itself, or with diabetes pills, or with a longer-acting insulin.
- For adults with type 1 diabetes, EXUBERA is always used with treatment that includes a longer-acting insulin.
- EXUBERA contains a short- or rapid-acting form of insulin. It should NOT be taken at the same time as other short- or rapid-acting insulins. It is not a longer-acting insulin.
- EXUBERA inhaled insulin starts working faster than regular injected insulin. It works as long as regular injected insulin. When used as your mealtime insulin, EXUBERA should be used within 10 minutes before your meal.
- The insulin in EXUBERA is a man-made insulin that is the same as the insulin made by the human body.
What is Diabetes?
- Diabetes is a disease that affects the amount of insulin and sugar in your body. Your body needs insulin to turn sugar (glucose) into energy. With diabetes, your body may not make enough insulin. If this is the case, you need to take more insulin. Taking insulin will help to keep you from having too much sugar in your blood.
- Treatment with insulin helps to keep your diabetes under control. The way you live helps, as well. Watch your diet. Check your blood sugar levels. Exercise. Plan to be active. These good habits work with your insulin to help you control your diabetes.
- Ask your healthcare provider for more information about diabetes.
Who should NOT use EXUBERA?
Do not use EXUBERA if you:
- smoke or stopped smoking less than 6 months ago. If you start smoking or resume smoking, stop using EXUBERA right away. See your healthcare provider right away for a different treatment.
- have an unstable or poorly controlled lung disease (such as unstable or poorly controlled asthma, chronic obstructive pulmonary disease or emphysema).
- are allergic to insulin or any of the inactive ingredients in EXUBERA. See the end of this leaflet for a list of ingredients in EXUBERA.
Children and teenagers should not use EXUBERA, because it has not been tested enough in children and teenagers under 18 years of age.
What should I tell my healthcare provider before starting EXUBERA?
Tell your healthcare provider about all your health and medical conditions, including if you:
- have any lung disease or have breathing problems.
- are using any inhaled medications
- have liver or kidney problems. Your dose may need to be adjusted.
- are pregnant or plan to become pregnant. EXUBERA has not been tested enough in pregnant females. It is very important to maintain control of your blood sugar levels during pregnancy. Your healthcare provider will decide which insulin is best for you during your pregnancy.
- are breast-feeding or plan to breast-feed. Many medicines, including insulin, pass into breast milk, and could affect your baby. Talk to your healthcare provider about the best way to feed your baby.
- are smoking or have recently stopped smoking.
- are taking any medicines or supplements. This includes: 1) medicines you get with a prescription, 2) those you get without a prescription and 3) herbal supplements and vitamins. Ask your healthcare provider for advice if you take other medicines. See "What can affect how much insulin I need?".
How should I take EXUBERA?
See the end of this Medication Guide for the Instructions for Use for using EXUBERA blisters with the EXUBERA® Inhaler. Make sure your healthcare provider teaches you the right way to use EXUBERA blisters with the EXUBERA® Inhaler and make sure you understand everything.
- Follow the medicine instructions that your healthcare provider gives you. Do not make any changes with your insulin unless you have talked to your healthcare provider. Your insulin needs may change because of 1) illness 2) stress, 3) other medicines or 4) changes in diet or activity level. Talk to your healthcare provider about how to adjust your insulin dose.
- Do not change any of your other diabetes medicines without talking to your healthcare provider. This includes insulin that you now inject. It also includes any diabetes medicines you may now take by mouth. Your healthcare provider may need to adjust the doses of your other diabetes medicines.
- Follow your healthcare provider's instructions for testing your blood sugar. Ask what to do if it is high or low. Low blood sugar (hypoglycemia) is the most common side effect of EXUBERA and all insulin.
- Never use three 1 mg blisters for one 3 mg blister because you may get too much insulin. If your 3 mg blisters become temporarily unavailable, use only two 1 mg blisters instead and check your blood sugar levels. Call your healthcare provider to get a new supply of 3 mg blisters as soon as possible. See "What is the most important information I should know about EXUBERA?"
- Do not open the individual EXUBERA blisters. The EXUBERA® Inhaler is designed to open the blister after you put the unopened blister in the Inhaler. You don't need to open the blister yourself.
- Never swallow the contents of the EXUBERA blister. You should only breathe in EXUBERA using the EXUBERA® Inhaler. Do not try to breathe in the EXUBERA insulin powder without using the EXUBERA® Inhaler.
- After a blister has been used, throw it away. Do not try to re-use a blister.
- You should take EXUBERA within 10 minutes before a meal.
- You need to have lung tests before you start EXUBERA, and after you start EXUBERA, you may need to have lung tests again as directed by your healthcare provider.
- If you are having problems with your EXUBERA® Inhaler or it breaks and you need a replacement, call 1-800-EXUBERA. Then, call your healthcare provider for treatment instructions until you receive your replacement Inhaler.
What can affect how much insulin I need?
Talk to your healthcare provider if you have any questions about how much insulin you need. Many things can affect how much insulin you need, including:
- Illness: Illness may change how much insulin you need. It is a good idea to think ahead and make a "sick day" plan with your healthcare provider. Do this in advance, so you will be ready when this happens. Be sure to test your blood sugar more often. Be sure to call your healthcare provider if you are sick.
- Medicines: Many medicines can affect your insulin needs. Other medicines can change the way insulin works. This includes prescription and non-prescription medicines, vitamins, and herbal supplements. You may need a different dose of insulin when you are taking certain other medicines. Know all the medicines you take. Keep a list. Show this list to all your healthcare providers and pharmacists anytime you get a new medicine or refill. Your healthcare provider will tell you if your insulin dose needs to be changed.
- Meals. The amount of food you eat can affect your insulin needs. You may need a different dose of insulin if you: 1) eat less food 2) skip meals, or 3) eat more food than usual. Talk to your healthcare provider if you change your diet. This will help you know how to adjust your EXUBERA and other insulin doses.
- Alcohol. Alcohol may affect the way your insulin works and affect your blood sugar levels. Beer and wine, as well as other kinds of alcohol, can cause these problems with your blood sugar levels. Talk to your healthcare provider about drinking alcohol.
- Exercise or Activity Level. Exercise or activity level may change the way your body uses insulin. Check with your healthcare provider before you start an exercise program. Do this, because your dose may need to be changed.
- Travel. If you are going to travel across time zones, talk with your healthcare provider about how to time your dosing. When you travel, wear your medical alert identification. Take extra insulin and supplies with you.
What are some of the possible side effects of EXUBERA?
1. Low blood sugar (HYPOglycemia):
As with all forms of insulin, a possible side effect of EXUBERA is low blood sugar. Low blood sugar is often called "hypoglycemia" or an "insulin reaction". It may happen when you do not have enough sugar in your blood. Common causes of low blood sugar are: 1) illness, 2) emotional or physical stress, 3) too much insulin, 4) too little food or missed meals, and 5) too much exercise or activity.
Early warning signs of low blood sugar may differ from person to person. For some people, signs may be easy to notice. For others, signs may be harder to notice, if noticed at all. That is why it is important to check your blood sugar as your healthcare provider has advised you.
Low blood sugar can happen with:
- The wrong insulin dose. This can happen when you take too much insulin.
- Not enough food intake. This can happen if a meal or snack is missed or delayed.
- Vomiting or diarrhea that decreases the amount of sugar absorbed by your body.
- Drinking alcohol.
- Medicines that affect insulin. Be sure to discuss all your medicines with your healthcare provider. Do not start any new medicines until you know how they may affect your insulin dose.
- Medical conditions that can affect your blood sugar levels or insulin. These conditions include diseases of: 1) the adrenal glands, 2) the pituitary, 3) the thyroid gland, 4) the liver, and 5) the kidneys.
- Too much blood sugar use by the body. This can happen if you exercise too much or have a fever.
Low blood sugar can be mild to severe. It can start quickly.
The following patients may have few or no warning symptoms of hypoglycemia:
- patients who have had diabetes for a long time
- patients with diabetic nerve problems (neuropathy) - for example, numbness in the feet
- patients using certain medicines for high blood pressure or heart problems.
Symptoms of low blood sugar may include:
- shaking (tremor)
- sweating
- anxiety, irritability, restlessness, trouble concentrating, personality changes, mood changes, or other abnormal behavior
- tingling in your hands, feet, lips, or tongue
- dizziness, light-headedness, or drowsiness
- nightmares or trouble sleeping
- headache
- blurred vision
- slurred speech
- fast heart beat (palpitations)
- unsteady walking (unsteady gait)
Low blood sugar is a problem:
- Driving and using machinery: If you have low blood sugar, your ability to concentrate or react may be reduced so that you may be less able to drive a vehicle or use mechanical equipment. If you do, you may risk causing injury to yourself or others.
- Effects on your heart and brain: Severe low blood sugar can be dangerous. It can cause temporary or permanent harm to your heart or brain. It may even cause unconsciousness, seizures, or death.
What to do about low blood sugar:
- Juice or food can treat low blood sugar. Mild to moderate low blood sugar can be treated by eating or drinking carbohydrates such as fruit juice, raisins, sugar candies, milk, or glucose tablets. Talk to your healthcare provider about the amount of carbohydrates you should eat to treat mild to moderate low blood sugar.
- Talk to your healthcare provider if : 1) you have low blood sugar often, or 2) it is hard for you to know if you have the symptoms of low blood sugar.
- Getting emergency help: Plan for a way to get medical help if you need it. Severe low blood sugar may require the help of another person or emergency medical personnel. A person with low blood sugar who cannot take foods or liquids with sugar by mouth will need medical help fast and treatment with: 1) a glucagon injection or 2) glucose given intravenously (IV). Without medical help right away, serious reactions or even death could occur.
2. High Blood Sugar (HYPERglycemia):
High blood sugar may occur when you have diabetes, even while you are on insulin treatment. High blood sugar is often called "hyperglycemia". It may occur when you have too much sugar in your blood. Usually, it means there is not enough insulin to break down the food you eat into energy your body can use.
High blood sugar can happen with:
-
The wrong insulin dose. This can happen from:
- -
- taking too little or no insulin
- -
- incorrect storage of insulin (freezing, or too much heat)
- -
- using insulin after the expiration date.
- Too much carbohydrate intake (includes starchy foods, fruits and sweet foods and drinks). This can happen if you 1) eat larger meals, 2) eat more often, or 3) increase the amount of carbohydrate in your meals.
- Medicines that affect insulin. Be sure to discuss all your medicines with your healthcare provider. Do not start any new medicines until you know how they may affect your insulin dose.
- Medical conditions that affect insulin. These medical conditions include 1) fevers, 2) infections, 3) heart attacks, and 4) stress.
High blood sugar can be a serious problem.
- High blood sugar can be mild or severe.
- When your blood sugar is extremely high, it can cause very serious problems that need treatment right away.
- These severe states can result in unconsciousness and death.
What are the symptoms of high blood sugar?
Often, high blood sugar has no symptoms at all. When high blood sugar does have symptoms, they can include:
- confusion or drowsiness
- increased thirst
- decreased appetite, nausea, or vomiting
- rapid heart rate
- increased urination and dehydration (too little fluid in your body)
- fruity smelling breath
- fast, deep breathing
- pain in the stomach area (abdominal pain)
Test your blood sugar levels to prevent problems.
- Because some patients get few symptoms of high blood sugar, it is important to check your blood sugar regularly.
- Testing your blood often for your blood sugar level will let you know if you have high blood sugar.
- If your tests are often high, tell your healthcare provider as soon as possible so your dose of medicine can be changed.
- Talk to your healthcare provider to find out what blood sugar level is too high for you. Ask about when you should call your healthcare provider for a high blood sugar level. Also ask about what blood sugar number is high enough that you should go straight to the hospital.
3. Effect on Lung Function:
EXUBERA may lower your lung function. See "What is the most important information I should know about EXUBERA?"
- You need to have lung tests before you start EXUBERA, and after you start EXUBERA, you may need to have lung tests again later as directed by your healthcare provider.
- If you notice a change in your breathing while taking EXUBERA, call your healthcare provider.
4. Serious allergic reactions:
Sometimes severe, life-threatening allergic reactions can happen with insulin. If you think you are having a severe allergic reaction, get medical help right away. Signs of insulin allergy include:
- a rash all over your body
- shortness of breath
- wheezing (trouble breathing)
- a fast pulse
- sweating
- low blood pressure
5. EXUBERA may cause a cough, dry mouth, or chest discomfort.
Tell your healthcare provider if you have any side effects that bother you.
These are not all the side effects that can happen with EXUBERA. Ask your healthcare provider or pharmacist for more information.
6. In studies of EXUBERA in people with diabetes, lung cancer occurred in a few more people who were taking EXUBERA than in people who were taking other diabetes medicines. All the people in these studies who developed lung cancer used to smoke cigarettes. There were too few cases to know if the lung cancer was related to EXUBERA.
How should I store EXUBERA?
- Store EXUBERA in a dry place at room temperature below 86° F (the same as below 30° C). Be sure to protect the small foil blisters from humid places, from steam and from water.
- Do not refrigerate or freeze EXUBERA, or expose it to excessive heat. If an EXUBERA blister freezes or is exposed to excessive heat, throw it away.
Keep EXUBERA and all medicines out of the reach of children.
General Information about EXUBERA
- Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use EXUBERA for a condition for which it was not prescribed.
- Do not give or share EXUBERA with another person, even if they have diabetes also. It may harm them.
For more information about EXUBERA:
- Talk with your healthcare provider. This Medication Guide only summarizes the most important information about EXUBERA.
- You can also ask your healthcare provider or pharmacist for information about EXUBERA that is written for healthcare professionals.
- Call 1-800-EXUBERA or go to website www.exubera.com.
What are the ingredients of EXUBERA?
Active ingredient: human insulin
Inactive ingredients: sodium citrate (dihydrate), mannitol, glycine, and sodium hydroxide
Please read these instructions carefully before starting to use your EXUBERA® Inhaler. Keep this Medication Guide, as you may need to read it again. Make sure you understand everything. Talk to your healthcare provider if you do not understand the instructions. Always be sure you have the correct EXUBERA blisters available before using your EXUBERA® Inhaler. EXUBERA blisters must only be used with the EXUBERA® Inhaler.
| KNOW THE PARTS OF YOUR EXUBERA® INHALER | 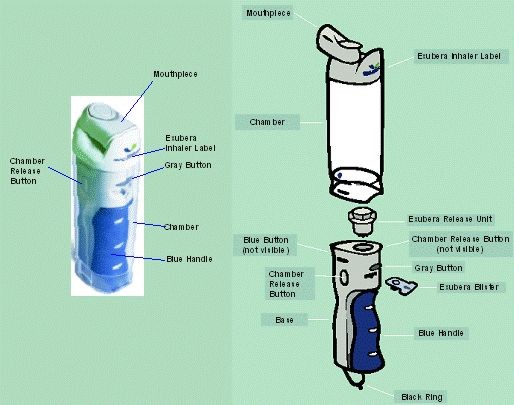 |
| HOW TO TAKE YOUR DOSE | |
|---|---|
| Step 1: Set up your EXUBERA® Inhaler | |
| Hold your EXUBERA® Inhaler in your hand. Be sure that the words "EXUBERA® Inhaler" at the top face you. |
|
| Hold the black ring at the bottom of the base and use it to pull the base out of the chamber. |
|
| You will hear a click when the EXUBERA® Inhaler is fully extended and locked into place. The bottom of the chamber MUST be above the gray button. |
|
| Step 2: Load your EXUBERA blister | |
| Hold the EXUBERA blister by the tab with printed side up and with the notch pointed towards the EXUBERA® Inhaler and insert one blister into the slot. Do not open the EXUBERA blister. |
|
| Slide one EXUBERA blister straight into the slot as far as it will go. |
|
| Step 3: Getting ready to take your dose | |
| Make sure that the mouthpiece is closed. If the mouthpiece is open, turn it around so that it is closed. |
|
| Pull out the blue handle from the bottom as far as it will go. |
|
| Squeeze the handle until it snaps shut. This will put pressure in the system. |
|
| Stand or sit up straight. |
|
| Step 4: Inhale your insulin dose | |
|
Perform the following steps in order.
Hold the EXUBERA® Inhaler upright with the blue button facing towards you. Push the blue button until it clicks and watch for the insulin cloud to fill the chamber. If a cloud does not appear right away, press the gray button, pull out the used EXUBERA blister, go back to Step 2 and repeat. If the blister is punctured or appears damaged, use a new blister. Breathe out normally. |
|
| After the cloud appears, right away turn the mouthpiece around. The mouthpiece should now be facing towards you. |
|
|
Promptly place the mouthpiece fully in the mouth, forming a seal around the mouthpiece with your lips, so that the insulin will not leak out.
Do not block the opening of the mouthpiece with your tongue or teeth. Do not blow into the mouthpiece. In one breath, slowly and deeply breathe the insulin cloud in through your mouth. |
|
|
Take the mouthpiece out of your mouth. Close your mouth and hold your breath for 5 seconds. Breathe out normally. |
|
| Step 5: After your dose | |
| Turn the mouthpiece back to its closed position. |
|
|
Press the gray button and pull out the used EXUBERA blister. If you need another blister as part of your dose, repeat steps 2, 3 and 4. The contents of only one blister should be inhaled at a time. |
|
| Step 6. After your dosing is completed | |
|
Squeeze the two chamber release buttons on the side of the base at the same time. Push the base back into the chamber to store the EXUBERA® Inhaler. After a blister has been used, throw it away. Do not try to re-use a blister. |
|
|
HOW TO TAKE CARE OF YOUR EXUBERA® INHALER It is important to follow these steps so that your EXUBERA® Inhaler stays clean and works properly. |
|
|
How to Take your EXUBERA® Inhaler apart You need to know how to take your EXUBERA® Inhaler apart for you when you need to clean your EXUBERA® Inhaler (once a week), and for when you need to change the EXUBERA® Release Unit (every two weeks). Spare EXUBERA® Release Units should be kept out of children's reach. |
|
| Hold the EXUBERA® Inhaler in your hand. Be sure that the words "EXUBERA® Inhaler" at the top face you. |
|
| Hold the black ring at the bottom of the base and use it to pull the base out of the chamber. |
|
| You will hear a click when the EXUBERA® Inhaler is fully extended and locked into place. The bottom of the chamber MUST be above the gray button. |
|
| With one hand, squeeze the two chamber release buttons on the side of the base at the same time while pulling the base all the way out of the chamber with the other hand. |
|
| Cleaning | |
|
Chamber and mouthpiece – once a week for best functioning. Keeping the chamber and mouthpiece clean is very important to prevent medicine build-up. It is suggested that you choose one day of the week (such as Monday) and clean the chamber and mouthpiece after your last dose for that day every week. How? Take your EXUBERA® Inhaler apart. (See above) |
|
| Turn the mouthpiece to the open position. |
|
|
Dampen a clean soft cloth and use mild liquid soap to wipe the outside and inside of the chamber and mouthpiece. Do NOT put the chamber in the dishwasher. | |
| Thoroughly rinse the soap out of the chamber and mouthpiece with warm water. | |
| Allow to completely air dry. This will probably take about 4 hours. Make sure that the chamber and mouthpiece are completely dry and that no water droplets remain. Close the mouthpiece. Reattach the chamber to the base. | |
| For instructions on how to attach the chamber to the base, refer to the section "Put your EXUBERA® Inhaler together". | |
| If the washed chamber is not completely dry prior to taking your next dose, use your spare chamber. | |
| Base – clean once a week |
|
|
How? Do not put the base in water. Do not get the inside of the EXUBERA® Release Unit wet. Do not wipe the Release Unit. Do not use soap or any other cleanser. Dampen a clean soft cloth with water; do not use a paper towel. Hold the base upside down with the Release Unit facing the ground. While cleaning the top of the base be careful not to get any water into the Release Unit. Do not take the Release Unit out at this time. Keep the blue handle closed. Make sure that no water droplets remain. Wipe only the TOP and OUTSIDE surfaces of the base. Do not wipe the slot where the blister is inserted. |
|
| Put your EXUBERA® Inhaler together | |
|
Line the top of the base with the open end of the chamber. The blue dot on the bottom of the chamber must be on the same side as the blue button on the base. Squeeze the two chamber release buttons on the side of the base at the same time. Push the base back into the chamber to store. Store your EXUBERA® Inhaler in a dry place at room temperature. |
|
|
Replacing your EXUBERA® Release Unit Change the Release Unit Every 2 weeks. You should mark your calendar to remind you when you need to replace the Release Unit. You may also mark the EXUBERA® Release Unit carton in the spaces provided. Be careful when handling the Release Unit, because it has sharp edges. You should not clean the Release Unit. |
|
|
How? Take out the used EXUBERA® Release Unit While the chamber is removed from the base (see "How to take your EXUBERA® Inhaler apart"), hold the base in your hand with the gray button facing you. Turn the used Release Unit about a one-quarter turn counter–clockwise towards the unlock symbol. |
|
| Pull the used Release Unit up and out of the base and discard. |
|
|
Put in a New EXUBERA® Release Unit Remove the Release Unit from its packaging. Hold the new Release Unit so the top is facing you. You will see a blue line on it. While holding the Release Unit with one hand, turn the top counter-clockwise with the other hand as far as it will go. |
|
|
Line up the blue line on the top of the Release Unit with the unlock symbol on the top of the base. Insert the Release Unit gently into the base. Do not force - it should easily drop into place. (If the new Release Unit does not drop into place or fits tightly, remove and try again). If after several attempts you are not able to insert the Release Unit, try another Release Unit. If you are still having problems, please call 1-800-EXUBERA. |
|
| Turn the top of the Release Unit clockwise until the blue line points to the lock symbol on the top of the base. The new Release Unit is now locked in place. |
|
Replacing your EXUBERA® Inhaler and the EXUBERA® Release Unit
You should change your EXUBERA® Inhaler once a year from the date you first use the Inhaler. You can mark the date of first use on the bottom of the Inhaler base.
You should change the EXUBERA® Release Unit in your EXUBERA® Inhaler every 2 weeks. The replacement dates can be marked on the EXUBERA® Release Unit carton.
This Medication Guide has been approved by the U.S. Food and Drug Administration.