Label: heparin sodium- Heparin Sodium injection, solution
-
Contains inactivated NDC Code(s)
NDC Code(s): 0009-0268-01, 0009-0268-02, 0009-0268-12, 0009-0291-01, view more0009-0317-02, 0009-0317-10, 0009-0317-11
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: None
Drug Label Information
Updated April 13, 2006
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
- N/A - Section Title Not Found In Database
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
Heparin is a heterogenous group of straight-chain anionic mucopolysaccharides, called glycosaminoglycans having anticoagulant properties. Although others may be present, the main sugars occurring in heparin are: (1) α-L-iduronic acid 2-sulfate, (2) 2-deoxy-2-sulfamino-α-D-glucose 6-sulfate, (3) β-D-glucuronic acid, (4) 2-acetamido-2-deoxy-α-D-glucose, and (5) α-L-iduronic acid. These sugars are present in decreasing amounts, usually in the order (2) > (1) > (4) > (3) > (5), and are joined by glycosidic linkages, forming polymers of varying sizes. Heparin is strongly acidic because of its content of covalently linked sulfate and carboxylic acid groups. In heparin sodium, the acidic protons of the sulfate units are partially replaced by sodium ions.
Structure of Heparin Sodium (representative subunits):
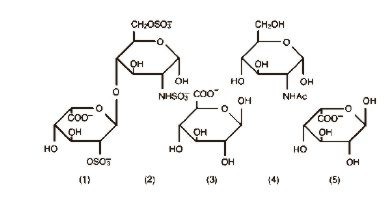
Heparin Sodium Injection, USP is a sterile solution of heparin sodium derived from bovine lung tissue, standardized for anticoagulant activity. It is to be administered by intravenous or deep subcutaneous routes. The potency is determined by a biological assay using a USP reference standard based on units of heparin activity per milligram. Heparin is pyrogen-free.
Each mL of the 1,000 and 5,000 USP Units per mL preparations contains: heparin sodium 1,000 or 5,000 USP Units; 9 mg sodium chloride; 9.45 mg benzyl alcohol added as preservative. Each mL of the 10,000 USP Units per mL preparations contains: heparin sodium 10,000 USP Units; 9.45 mg benzyl alcohol added as preservative.
When necessary, the pH of Heparin Sodium Injection, USP was adjusted with hydrochloric acid and/or sodium hydroxide. The pH range is 5.0–7.5.
-
CLINICAL PHARMACOLOGY
Heparin inhibits reactions that lead to the clotting of blood and the formation of fibrin clots both in vitro and in vivo. Heparin acts at multiple sites in the normal coagulation system. Small amounts of heparin in combination with antithrombin III (heparin cofactor) can inhibit thrombosis by inactivating activated Factor X and inhibiting the conversion of prothrombin to thrombin. Once active thrombosis has developed, larger amounts of heparin can inhibit further coagulation by inactivating thrombin and preventing the conversion of fibrinogen to fibrin. Heparin also prevents the formation of a stable fibrin clot by inhibiting the activation of the fibrin stabilizing factor.
Bleeding time is usually unaffected by heparin. Clotting time is prolonged by full therapeutic doses of heparin; in most cases, it is not measurably affected by low doses of heparin.
Patients over 60 years of age, following similar doses of heparin, may have higher plasma levels of heparin and longer activated partial thromboplastin times (APTTs) compared with patients under 60 years of age.
Peak plasma levels of heparin are achieved 2–4 hours following subcutaneous administration, although there are considerable individual variations. Loglinear plots of heparin plasma concentrations with time for a wide range of dose levels are linear which suggests the absence of zero order processes. Liver and the reticulo-endothelial system are the site of biotransformation. The biphasic elimination curve, a rapidly declining alpha phase (t½=10 minutes) and after the age of 40 a slower beta phase, indicates uptake in organs. The absence of a relationship between anticoagulant half-life and concentration half-life may reflect factors such as protein binding of heparin.
Heparin does not have fibrinolytic activity; therefore, it will not lyse existing clots.
-
INDICATIONS AND USAGE
Heparin Sodium Injection is indicated for:
Anticoagulant therapy in prophylaxis and treatment of venous thrombosis and its extension;
(In a low-dose regimen) for prevention of postoperative deep venous thrombosis and pulmonary embolism in patients undergoing major abdomino-thoracic surgery or who for other reasons are at risk of developing thromboembolic disease (see DOSAGE AND ADMINISTRATION);
Prophylaxis and treatment of pulmonary embolism;
Atrial fibrillation with embolization;
Diagnosis and treatment of acute and chronic consumption coagulopathies (disseminated intravascular coagulation);
Prevention of clotting in arterial and heart surgery;
Prophylaxis and treatment of peripheral arterial embolism;
As an anticoagulant in blood transfusions, extracorporeal circulation, and dialysis procedures and in blood samples for laboratory purposes.
-
CONTRAINDICATIONS
Heparin sodium should not be used in patients:
With severe thrombocytopenia;
In whom suitable blood coagulation tests—e.g., the whole-blood clotting time, partial thromboplastin time, etc.—cannot be performed at appropriate intervals (this contraindication refers to full-dose heparin; there is usually no need to monitor coagulation parameters in patients receiving low-dose heparin);
With an uncontrollable active bleeding state (see WARNINGS), except when this is due to disseminated intravascular coagulation.
-
WARNINGS
Heparin is not intended for intramuscular use.
Hypersensitivity
Patients with documented hypersensitivity to heparin should be given the drug only in clearly life-threatening situations.
Hemorrhage
Hemorrhage can occur at virtually any site in patients receiving heparin. An unexplained fall in hematocrit, fall in blood pressure, or any other unexplained symptom should lead to serious consideration of a hemorrhagic event.
Heparin sodium should be used with extreme caution in disease states in which there is increased danger of hemorrhage. Some of the conditions in which increased danger of hemorrhage exists are:
Cardiovascular—Subacute bacterial endocarditis. Severe hypertension.
Surgical—During and immediately following (a) spinal tap or spinal anesthesia or (b) major surgery, especially involving the brain, spinal cord, or eye.
Hematologic—Conditions associated with increased bleeding tendencies, such as hemophilia, thrombocytopenia, and some vascular purpuras.
The anticoagulant effect of heparin is enhanced by concurrent treatment with antithrombin III (human) in patients with hereditary antithrombin III deficiency. Thus in order to avoid bleeding, reduced dosage of heparin is recommended during treatment with antithrombin III (human).
Gastrointestinal—Ulcerative lesions and continuous tube drainage of the stomach or small intestine.
Other—Menstruation, liver disease with impaired hemostasis.
Coagulation Testing
When heparin sodium is administered in therapeutic amounts, its dosage should be regulated by frequent blood coagulation tests. If the coagulation test is unduly prolonged or if hemorrhage occurs, heparin sodium should be discontinued promptly (see OVERDOSAGE).
Thrombocytopenia
Thrombocytopenia has been reported to occur in patients receiving heparin with a reported incidence of 0 to 30%. Mild thrombocytopenia (count greater than 100,000/mm3) may remain stable or reverse even if heparin is continued. However, reduction in platelet count of any degree should be monitored closely. If the count falls below 100,000/mm3 or if recurrent thrombosis develops (see White Clot Syndrome, PRECAUTIONS), the heparin product should be discontinued. If continued heparin therapy is essential, administration of heparin from a different organ source can be reinstituted with caution.
-
PRECAUTIONS
1. General
a. White Clot Syndrome
It has been reported that patients on heparin may develop new thrombus formation in association with thrombocytopenia resulting from irreversible aggregation of platelets induced by heparin, the so-called "white clot syndrome." The process may lead to severe thromboembolic complications like skin necrosis, gangrene of the extremities that may lead to amputation, myocardial infarction, pulmonary embolism, stroke, and possibly death. Therefore, heparin administration should be promptly discontinued if a patient develops new thrombosis in association with a reduction in platelet count.
2. Laboratory Tests
Periodic platelet counts, hematocrits, and tests for occult blood in stool are recommended during the entire course of heparin therapy, regardless of the route of administration (see DOSAGE AND ADMINISTRATION).
3. Drug Interactions
a. Drugs Enhancing Heparin Effect
Oral anticoagulants
Heparin sodium may prolong the one-stage prothrombin time. Therefore, when heparin sodium is given with dicumarol or warfarin sodium, a period of at least 5 hours after the last intravenous dose or 24 hours after the last subcutaneous dose should elapse before blood is drawn if a valid prothrombin time is to be obtained.
Platelet inhibitors
Drugs such as acetylsalicylic acid, dextran, phenylbutazone, ibuprofen, indomethacin, dipyridamole, hydroxychloroquine and others that interfere with platelet-aggregation reactions (the main hemostatic defense of heparinized patients) may induce bleeding and should be used with caution in patients receiving heparin sodium.
b. Drugs Decreasing Heparin Effect
Digitalis, tetracyclines, nicotine, or antihistamines may partially counteract the anticoagulant action of heparin sodium. Heparin Sodium Injection should not be mixed with doxorubicin, droperidol, ciprofloxacin, or mitoxantrone, since it has been reported that these drugs are incompatible with heparin and a precipitate may form.
4. Drug/Laboratory Tests Interactions
Hyperaminotransferasemia
Significant elevations of aminotransferase (SGOT [S-AST] and SGPT [S-ALT]) levels have occurred in a high percentage of patients (and healthy subjects) who have received heparin. Since aminotransferase determinations are important in the differential diagnosis of myocardial infarction, liver disease, and pulmonary emboli, rises that might be caused by drugs (like heparin) should be interpreted with caution.
5. Carcinogenesis, Mutagenesis, Impairment of Fertility
No long-term studies in animals have been performed to evaluate carcinogenic potential of heparin. Also, no reproduction studies in animals have been performed concerning mutagenesis or impairment of fertility.
6. Pregnancy
Teratogenic Effects
Pregnancy Category C
Animal reproduction studies have not been conducted with heparin sodium. It is also not known whether heparin sodium can cause fetal harm when administered to a pregnant woman or can affect reproduction capacity. Heparin sodium should be given to a pregnant woman only if clearly needed.
9. Geriatric Use
A higher incidence of bleeding has been reported in patients over 60 years of age, especially women (see PRECAUTIONS, General). Clinical studies indicated that lower doses of heparin may be indicated in these patients (see CLINICAL PHARMACOLOGY and DOSAGE AND ADMINISTRATION).
-
ADVERSE REACTIONS
1. Hemorrhage
Hemorrhage is the chief complication that may result from heparin therapy (see WARNINGS). An overly prolonged clotting time or minor bleeding during therapy can usually be controlled by withdrawing the drug (see OVERDOSAGE). It should be appreciated that gastrointestinal or urinary tract bleeding during anticoagulant therapy may indicate the presence of an underlying occult lesion. Bleeding can occur at any site but certain specific hemorrhagic complications may be difficult to detect:
- Adrenal hemorrhage, with resultant acute adrenal insufficiency, has occurred during anticoagulant therapy. Therefore, such treatment should be discontinued in patients who develop signs and symptoms of acute adrenal hemorrhage and insufficiency. Initiation of corrective therapy should not depend on laboratory confirmation of the diagnosis, since any delay in an acute situation may result in the patient's death.
- Ovarian (corpus luteum) hemorrhage developed in a number of women of reproductive age receiving short- or long-term anticoagulant therapy. This complication if unrecognized may be fatal.
- Retroperitoneal hemorrhage.
2. Local irritation
Local irritation, erythema, mild pain, hematoma or ulceration may follow deep subcutaneous (intrafat) injection of heparin sodium. These complications are much more common after intramuscular use, and such use is not recommended.
3. Hypersensitivity
Generalized hypersensitivity reactions have been reported, with chills, fever, and urticaria as the most usual manifestations, and asthma, rhinitis, lacrimation, headache, nausea and vomiting, and anaphylactoid reactions, including shock, occurring more rarely. Itching and burning, especially on the plantar site of the feet, may occur.
Thrombocytopenia has been reported to occur in patients receiving heparin with a reported incidence of 0–30%. While often mild and of no obvious clinical significance, a reduction in platelet count can be accompanied by severe thromboembolic complications such as skin necrosis, gangrene of the extremities that may lead to amputation, myocardial infarction, pulmonary embolism, stroke, and possibly death. (See WARNINGS, PRECAUTIONS.)
Certain episodes of painful, ischemic, and cyanosed limbs have in the past been attributed to allergic vasospastic reactions. Whether these are in fact identical to the thrombocytopenia associated complications remains to be determined.
4. Miscellaneous
Osteoporosis following long-term administration of high-doses of heparin, cutaneous necrosis after systemic administration, suppression of aldosterone synthesis, delayed transient alopecia, priapism, and rebound hyperlipemia on discontinuation of heparin sodium have also been reported.
Significant elevations of aminotransferase (SGOT [S-AST] and SGPT [S-ALT]) levels have occurred in a high percentage of patients (and healthy subjects) who have received heparin.
-
OVERDOSAGE
Symptoms
Bleeding is the chief sign of heparin overdosage. Nosebleeds, blood in urine or tarry stools may be noted as the first sign of bleeding. Easy bruising or petechial formations may precede frank bleeding.
Treatment
Neutralization of heparin effect. When clinical circumstances (bleeding) require reversal of heparinization, protamine sulfate (1% solution) by slow infusion will neutralize heparin sodium. No more than 50 mg should be administered, very slowly, in any 10 minute period. Each mg of protamine sulfate neutralizes approximately 100 USP heparin units. The amount of protamine required decreases over time as heparin is metabolized. Although the metabolism of heparin is complex, it may, for the purpose of choosing a protamine dose, be assumed to have a half-life of about ½ hour after intravenous injection.
Administration of protamine sulfate can cause severe hypotensive and anaphylactoid reactions. Because fatal reactions often resembling anaphylaxis have been reported, the drug should be given only when resuscitation techniques and treatment of anaphylactoid shock are readily available.
For additional information the labeling of Protamine Sulfate Injection, USP products should be consulted.
-
DOSAGE AND ADMINISTRATION
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Slight discoloration does not alter potency.
When heparin is added to an infusion solution for continuous intravenous administration, the container should be inverted at least six times to ensure adequate mixing and prevent pooling of the heparin in the solution.
Heparin sodium is not effective by oral administration and should be given by intermittent intravenous injection, intravenous infusion, or deep subcutaneous (intrafat, i.e., above the iliac crest or abdominal fat layer) injection. The intramuscular route of administration should be avoided because of the frequent occurrence of hematoma at the injection site.
The dosage of heparin sodium should be adjusted according to the patient's coagulation test results. When heparin is given by continuous intravenous infusion, the coagulation time should be determined approximately every 4 hours in the early stages of treatment. When the drug is administered intermittently by intravenous injection, coagulation tests should be performed before each injection during the early stages of treatment and at appropriate intervals thereafter. Dosage is considered adequate when the activated partial thromboplastin time (APTT) is 1.5 to 2 times normal or when the whole blood clotting time is elevated approximately 2.5 to 3 times the control value. After deep subcutaneous (intrafat) injections, tests for adequacy of dosage are best performed on samples drawn 4–6 hours after the injections.
Periodic platelet counts, hematocrits, and tests for occult blood in stool are recommended during the entire course of heparin therapy, regardless of the route of administration.
Heparin Sodium Injection should not be mixed with doxorubicin, droperidol, ciprofloxacin, or mitoxantrone, since it has been reported that these drugs are incompatible with heparin and a precipitate may form.
Converting to Oral Anticoagulant
When an oral anticoagulant of the coumarin or similar type is to be begun in patients already receiving heparin sodium, baseline and subsequent tests of prothrombin activity must be determined at a time when heparin activity is too low to affect the prothrombin time. This is about 5 hours after the last I.V. bolus and 24 hours after the last subcutaneous dose. If continuous I.V. heparin infusion is used, prothrombin time can usually be measured at any time.
In converting from heparin to an oral anticoagulant, the dose of the oral anticoagulant should be the usual initial amount and thereafter prothrombin time should be determined at the usual intervals. To ensure continuous anticoagulation, it is advisable to continue full heparin therapy for several days after the prothrombin time has reached the therapeutic range. Heparin therapy may then be discontinued without tapering.
Therapeutic Anticoagulant Effect with Full-Dose Heparin
Although dosage must be adjusted for the individual patient according to the results of suitable laboratory tests, the following dosage schedules may be used as guidelines:
METHOD OF ADMINISTRATION FREQUENCY RECOMMENDED DOSE* - *
- Based on 150-lb. (68-kg) patient.
Deep Subcutaneous
(Intrafat) InjectionInitial Dose 5,000 units by I.V. injection, followed by
10,000–20,000 units of a concentrated solution, subcutaneouslyA different site should be used for each
injection to prevent the
development of massive
hematoma.Every 8 hours
or8,000–10,000 units of a
concentrated solution
Every 12 hours 15,000–20,000 units of
a concentrated solutionIntermittent Intravenous
InjectionInitial Dose 10,000 units, either undiluted or in 50–100 mL of 0.9% Sodium Chloride Injection, USP
Every 4 to 6
hours5,000–10,000 units, either undiluted or in 50–100 mL of 0.9% Sodium Chloride Injection, USP Continuous Intravenous
InfusionInitial Dose 5,000 units by I.V. injection Continuous 20,000–40,000 units/24 hours in 1,000 mL of 0.9% Sodium Chloride Injection, USP (or in any compatible solution) for infusion Pediatric Use
Follow recommendations of appropriate pediatric reference texts. In general, the following dosage schedule may be used as a guideline:
Initial Dose: 50 units/kg (I.V., drip)
Maintenance Dose: 100 units/kg (I.V., drip) every four hours, or
20,000 units/M2/24 hours continuouslySurgery of the Heart and Blood Vessels
Patients undergoing total body perfusion for open-heart surgery should receive an initial dose of not less than 150 units of heparin sodium per kilogram of body weight. Frequently, a dose of 300 units per kilogram is used for procedures estimated to last less than 60 minutes or 400 units per kilogram for those estimated to last longer than 60 minutes.
Low-Dose Prophylaxis of Postoperative Thromboembolism
A number of well-controlled clinical trials have demonstrated that low-dose heparin prophylaxis, given just prior to and after surgery, will reduce the incidence of postoperative deep vein thrombosis in the legs (as measured by the I-125 fibrinogen technique and venography) and of clinical pulmonary embolism. The most widely used dosage has been 5,000 units 2 hours before surgery and 5,000 units every 8 to 12 hours thereafter for 7 days or until the patient is fully ambulatory, whichever is longer. The heparin is given by deep subcutaneous (intrafat, i.e., above the iliac crest or abdominal fat layer, arm or thigh) injection with a fine (25 to 26-gauge) needle to minimize tissue trauma. A concentrated solution of heparin sodium is recommended. Such prophylaxis should be reserved for patients over the age of 40 who are undergoing major surgery. Patients with bleeding disorders and those having brain or spinal cord surgery, spinal anesthesia, eye surgery, or potentially sanguineous operations should be excluded, as should patients receiving oral anticoagulants or platelet-active drugs (see WARNINGS). The value of such prophylaxis in hip surgery has not been established. The possibility of increased bleeding during surgery or postoperatively should be borne in mind. If such bleeding occurs, discontinuance of heparin and neutralization with protamine sulfate are advisable. If clinical evidence of thromboembolism develops despite low-dose prophylaxis, full therapeutic doses of anticoagulants should be given unless contraindicated. Prior to initiating heparinization the physician should rule out bleeding disorders by appropriate history and laboratory tests, and appropriate coagulation tests should be repeated just prior to surgery. Coagulation tests values should be normal or only slightly elevated at these times.
Blood Transfusion
Addition of 400 to 600 USP units per 100 mL of whole blood is usually employed to prevent coagulation. Usually, 7,500 USP units of heparin sodium are added to 100 mL of 0.9% Sodium Chloride Injection, USP (or 75,000 USP units per 1,000 mL of 0.9% Sodium Chloride Injection, USP) and mixed; from this sterile solution, 6 to 8 mL are added per 100 mL of whole blood.
Laboratory Samples
Addition of 70 to 150 units of heparin sodium per 10 to 20 mL sample of whole blood is usually employed to prevent coagulation of the sample. Leukocyte counts should be performed on heparinized blood within 2 hours after addition of the heparin. Heparinized blood should not be used for isoagglutinin, complement, or erythrocyte fragility tests or platelet counts.
-
HOW SUPPLIED
Heparin Sodium Injection, USP derived from beef lung is available in the following strengths and package sizes:
1,000 units per mL 10 mL vials NDC 0009-0268-01 25 × 10 mL vials NDC 0009-0268-12 30 mL vials NDC 0009-0268-02 5,000 units per mL 10 mL vials NDC 0009-0291-01 10,000 units per mL 25 × 1 mL vials NDC 0009-0317-10 4 mL vials NDC 0009-0317-02 25 × 4 mL vials NDC 0009-0317-11 Store the product at controlled room temperature 20° to 25°C (68° to 77°F) [see USP].
- SPL UNCLASSIFIED SECTION
-
INGREDIENTS AND APPEARANCE
HEPARIN SODIUM
heparin sodium injection, solutionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:0009-0268 Route of Administration INTRAVENOUS, SUBCUTANEOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Heparin Sodium (UNII: ZZ45AB24CA) (Heparin - UNII:T2410KM04A) 1000 in 1 mL Inactive Ingredients Ingredient Name Strength sodium chloride (UNII: 451W47IQ8X) 9 mg in 1 mL benzyl alcohol (UNII: LKG8494WBH) 9.45 mg in 1 mL Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:0009-0268-12 25 in 1 PACKAGE 1 NDC:0009-0268-01 10 mL in 1 VIAL 2 NDC:0009-0268-02 30 mL in 1 VIAL HEPARIN SODIUM
heparin sodium injection, solutionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:0009-0291 Route of Administration INTRAVENOUS, SUBCUTANEOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Heparin Sodium (UNII: ZZ45AB24CA) (Heparin - UNII:T2410KM04A) 5000 in 1 mL Inactive Ingredients Ingredient Name Strength sodium chloride (UNII: 451W47IQ8X) 9 mg in 1 mL benzyl alcohol (UNII: LKG8494WBH) 9.45 mg in 1 mL Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:0009-0291-01 10 mL in 1 VIAL HEPARIN SODIUM
heparin sodium injection, solutionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:0009-0317 Route of Administration INTRAVENOUS, SUBCUTANEOUS Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Heparin Sodium (UNII: ZZ45AB24CA) (Heparin - UNII:T2410KM04A) 10000 in 1 mL Inactive Ingredients Ingredient Name Strength benzyl alcohol (UNII: LKG8494WBH) 9.45 mg in 1 mL Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:0009-0317-11 25 in 1 PACKAGE 1 NDC:0009-0317-02 4 mL in 1 VIAL 2 NDC:0009-0317-10 25 in 1 PACKAGE 2 1 mL in 1 VIAL

