VALTURNA- aliskiren hemifumarate and valsartan tablet, film coated
Novartis Pharmaceuticals Corporation
----------
HIGHLIGHTS OF PRESCRIBING INFORMATION
These highlights do not include all the information needed to use VALTURNA safely and effectively. See full prescribing information for VALTURNA.
Valturna (aliskiren and valsartan, USP) tablets, for oral use Initial U.S. Approval: 2009 RECENT MAJOR CHANGESINDICATIONS AND USAGEValturna is a combination of aliskiren, a renin inhibitor, and valsartan, an angiotensin II receptor blocker (ARB), indicated for the treatment of hypertension, to lower blood pressure.
Lowering blood pressure reduces the risk of fatal and nonfatal cardiovascular events, primarily strokes and myocardial infarctions. DOSAGE AND ADMINISTRATION
DOSAGE FORMS AND STRENGTHSTablets (mg aliskiren/mg valsartan): 150/160, 300/320. (3) CONTRAINDICATIONSDo not use in patients with diabetes (4) WARNINGS AND PRECAUTIONS
ADVERSE REACTIONSThe most common adverse events (incidence ≥1.5% and more common than with placebo) are: Fatigue and nasopharyngitis. (6.1) To report SUSPECTED ADVERSE REACTIONS, contact Novartis Pharmaceuticals Corporation at 1-888-669-6682 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch. DRUG INTERACTIONS
USE IN SPECIFIC POPULATIONSNursing Mothers: Nursing or drug should be discontinued. (8.3) See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling. Revised: 04/2012 |
FULL PRESCRIBING INFORMATION
WARNING: FETAL TOXICITY
- When pregnancy is detected, discontinue Valturna as soon as possible. (5.1)
- Drugs that act directly on the renin-angiotensin system can cause injury and death to the developing fetus. (5.1)
1 INDICATIONS AND USAGE
Valturna is indicated for the treatment of hypertension, to lower blood pressure. Lowering blood pressure reduces the risk of fatal and nonfatal cardiovascular events, primarily strokes and myocardial infarctions. These benefits have been seen in controlled trials of antihypertensive drugs from a wide variety of pharmacologic classes including the ARB class to which the valsartan component of this drug principally belongs. There are no controlled trials demonstrating risk reduction with Valturna.
Control of high blood pressure should be part of comprehensive cardiovascular risk management, including, as appropriate, lipid control, diabetes management, antithrombotic therapy, smoking cessation, exercise, and limited sodium intake. Many patients will require more than one drug to achieve blood pressure goals. For specific advice on goals and management, see published guidelines, such as those of the National High Blood Pressure Education Program’s Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC).
Numerous antihypertensive drugs, from a variety of pharmacologic classes and with different mechanisms of action, have been shown in randomized controlled trials to reduce cardiovascular morbidity and mortality, and it can be concluded that it is blood pressure reduction, and not some other pharmacologic property of the drugs, that is largely responsible for those benefits. The largest and most consistent cardiovascular outcome benefit has been a reduction in the risk of stroke, but reductions in myocardial infarction and cardiovascular mortality also have been seen regularly.
Elevated systolic or diastolic pressure causes increased cardiovascular risk, and the absolute risk increase per mmHg is greater at higher blood pressures, so that even modest reductions of severe hypertension can provide substantial benefit. Relative risk reduction from blood pressure reduction is similar across populations with varying absolute risk, so the absolute benefit is greater in patients who are at higher risk independent of their hypertension (for example, patients with diabetes or hyperlipidemia), and such patients would be expected to benefit from more aggressive treatment to a lower blood pressure goal.
Some antihypertensive drugs have smaller blood pressure effects (as monotherapy) in black patients, and many antihypertensive drugs have additional approved indications and effects (e.g., on angina, heart failure, or diabetic kidney disease). These considerations may guide selection of therapy.
Add-on Therapy
A patient whose blood pressure is not adequately controlled with aliskiren alone or valsartan (or another angiotensin receptor blocker) alone may be switched to combination therapy with Valturna.
Replacement Therapy
Valturna may be substituted for the titrated components.
Initial Therapy
Valturna may be used as initial therapy in patients who are likely to need multiple drugs to achieve their blood pressure goals.
The choice of Valturna as initial therapy should be based on an assessment of potential benefits and risks.
Patients with Stage 2 hypertension are at a relatively high risk for cardiovascular events (such as strokes, heart attacks, and heart failure), kidney failure, and vision problems, so prompt treatment is clinically relevant. The decision to use a combination as initial therapy should be individualized and should be shaped by considerations such as baseline blood pressure, the target goal, and the incremental likelihood of achieving goal with a combination compared to monotherapy. Individual blood pressure goals may vary based upon the patient’s risk.
Data from the high-dose multifactorial study [See Clinical Studies (14)] provide estimates of the probability of reaching a target blood pressure with Valturna compared to aliskiren or valsartan monotherapy. The figures below provide estimates of the likelihood of achieving systolic or diastolic blood pressure control with Valturna 300/320 mg, based upon baseline systolic or diastolic blood pressure. The curve of each treatment group was estimated by logistic regression modeling. The estimated likelihood at the right tail of each curve is less reliable because of a small number of subjects with high baseline blood pressures.
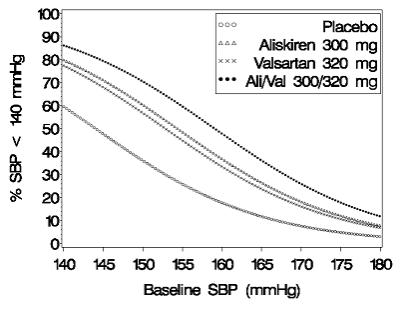
Figure 1: Probability of Achieving Systolic Blood Pressure (SBP) <140 mmHg in Patients at Endpoint
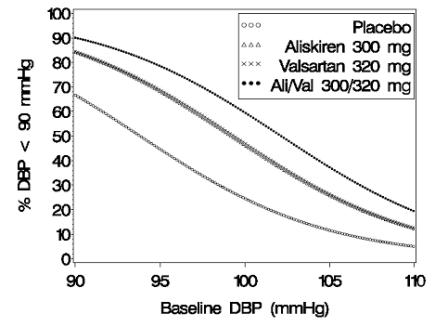
Figure 2: Probability of Achieving Diastolic Blood Pressure (DBP) <90 mmHg in Patients at Endpoint

Figure 3: Probability of Achieving Systolic Blood Pressure (SBP) <130 mmHg in Patients at Endpoint
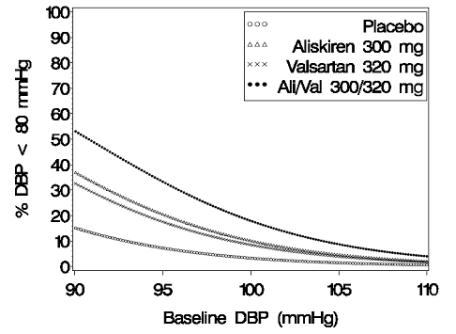
Figure 4: Probability of Achieving Diastolic Blood Pressure (DBP) <80 mmHg in Patients at Endpoint
At all levels of baseline blood pressure, the probability of achieving any given diastolic or systolic goal is greater with the combination than for either monotherapy. For example, the mean baseline SBP/DBP for patients participating in this multifactorial study was 154/100 mmHg. A patient with a baseline blood pressure of 154/100 mmHg has about a 51% likelihood of achieving a goal of <140 mmHg (systolic) and 46% likelihood of achieving <90 mmHg (diastolic) on aliskiren alone, and the likelihood of achieving these goals on valsartan alone is about 47% (systolic) and 47% (diastolic). The likelihood of achieving these goals on Valturna rises to about 62% (systolic) and 60% (diastolic). The likelihood of achieving these goals on placebo is about 28% (systolic) and 25% (diastolic) [See Dosage and Administration (2) and Clinical Studies (14)].
2 DOSAGE AND ADMINISTRATION
2.1 Dose Selection
The recommended once-daily dose of Valturna is 150/160 mg or 300/320 mg. The recommended initial once-daily dose of Valturna is 150/160 mg. Titrate as needed to a maximum of 300/320 mg.
Patients switched from monotherapy to Valturna on average experience greater blood pressure reductions with use of the combination product.
2.2 Dose Titration
The antihypertensive effect of Valturna is largely attained within 2 weeks. If blood pressure remains uncontrolled after 2 to 4 weeks of therapy, the dose may be titrated up to a maximum of 300/320 mg.
2.3 Add-on Therapy
A patient whose blood pressure is not adequately controlled with aliskiren alone or valsartan (or another angiotensin receptor blocker) alone may be switched to combination therapy with Valturna. The usual recommended starting dose is 150/160 mg once daily as needed to control blood pressure.
2.4 Replacement Therapy
For convenience, patients receiving aliskiren and valsartan from separate tablets may instead wish to receive a single tablet of Valturna containing the same component doses.
2.5 Initial Therapy
The usual recommended starting dose of Valturna is 150/160 mg once daily as needed to control blood pressure. The dose may be titrated up to a maximum of 300/320 mg once daily.
Valturna is not recommended for use as initial therapy in patients with intravascular volume depletion [see Warnings and Precautions (5.4)].
3 DOSAGE FORMS AND STRENGTHS
- 150/160 mg aliskiren/valsartan tablets: light red, standard convex ovaloid, film-coated tablets with beveled edges debossed with NVR/HDU
- 300/320 mg aliskiren/valsartan tablets: light brown, shallow convex ovaloid, film-coated tablets with beveled edges debossed with NVR/SNB
4 CONTRAINDICATIONS
Do not use in patients with diabetes [see Warnings (5.2), Clinical Trials (14.2)].
5 WARNINGS AND PRECAUTIONS
5.1 Fetal Toxicity
Pregnancy Category D
Use of drugs that act on the renin-angiotensin system during the second and third trimesters of pregnancy reduces fetal renal function and increases fetal and neonatal morbidity and death. Resulting oligohydramnios can be associated with fetal lung hypoplasia and skeletal deformations. Potential neonatal adverse effects include skull hypoplasia, anuria, hypotension, renal failure, and death. When pregnancy is detected, discontinue Valturna as soon as possible. [see Use in Specific Populations (8.1)]
5.2 Renal Impairment/Hyperkalemia/Hypotension when Valturna is used in patients with diabetes
Valturna is contraindicated in patients with diabetes because of the increased risks of renal impairment, hyperkalemia, and hypotension [see Contraindications (4) and Clinical Trials (14.2)].
Avoid use of Valturna in patients with moderate renal impairment (GFR <60 ml/min).
5.3 Head and Neck Angioedema
Aliskiren
Angioedema of the face, extremities, lips, tongue, glottis and/or larynx has been reported in patients treated with aliskiren and has necessitated hospitalization and intubation. This may occur at any time during treatment and has occurred in patients with and without a history of angioedema with ACE inhibitors or angiotensin receptor antagonists. If angioedema involves the throat, tongue, glottis or larynx, or if the patient has a history of upper respiratory surgery, airway obstruction may occur and be fatal. Patients who experience these effects, even without respiratory distress, require prolonged observation since treatment with antihistamines and corticosteroids may not be sufficient to prevent respiratory involvement. Prompt administration of subcutaneous epinephrine solution 1:1000 (0.3 to 0.5 ml) and measures to ensure a patent airway may be necessary.
Discontinue aliskiren immediately in patients who develop angioedema and do not readminister.
5.4 Hypotension
In patients with an activated renin-angiotensin-aldosterone system, such as volume- or salt-depleted patients receiving high doses of diuretics, symptomatic hypotension may occur in patients receiving renin-angiotensin-aldosterone system (RAAS) blockers. Correct these conditions prior to the administration of Valturna, or start the treatment under close medical supervision.
Initiate therapy cautiously in patients with heart failure or recent myocardial infarction and in patients undergoing surgery or dialysis. Patients with heart failure or post-myocardial infarction patients given valsartan commonly have some reduction in blood pressure, but discontinuation of therapy because of continuing symptomatic hypotension usually is not necessary when dosing instructions are followed. In controlled trials in heart failure patients, the incidence of hypotension in valsartan-treated patients was 5.5% compared to 1.8% in placebo-treated patients. In the Valsartan in Acute Myocardial Infarction Trial (VALIANT), hypotension in post-myocardial infarction patients led to permanent discontinuation of therapy in 1.4% of valsartan-treated patients and 0.8% of captopril-treated patients.
A transient hypotensive response is not a contraindication to further treatment, which usually can be continued without difficulty once the blood pressure has stabilized.
5.5 Impaired Renal Function
Monitor renal function periodically in patients treated with Valturna. Changes in renal function, including acute renal failure, can be caused by drugs that affect the renin-angiotensin system. Patients whose renal function may depend in part on the activity of the renin-angiotensin system (e.g., patients with renal artery stenosis, severe heart failure, post-myocardial infarction or volume depletion) or non-steroidal anti-inflammatory (NSAID) therapy may be at particular risk for developing acute renal failure on Valturna [see Contraindications (4), Warnings (5.2), Clinical Trials (14.2)]. Consider withholding or discontinuing therapy in patients who develop a clinically significant decrease in renal function.
5.6 Patients with Hepatic Impairment
Valsartan
As the majority of valsartan is eliminated in the bile, patients with mild-to-moderate hepatic impairment, including patients with biliary obstructive disorders, showed lower valsartan clearance (higher AUCs).
5.7 Patients with Congestive Heart Failure and Post-Myocardial Infarction
Valsartan
Some patients with heart failure have developed increases in blood urea nitrogen, serum creatinine, and potassium on valsartan. These effects are usually minor and transient, and they are more likely to occur in patients with pre-existing renal impairment. Dosage reduction and/or discontinuation of the diuretic and/or valsartan may be required. In the Valsartan Heart Failure Trial, in which 93% of patients were on concomitant ACE inhibitors, treatment was discontinued for elevations in creatinine or potassium (total of 1.0% on valsartan vs. 0.2% on placebo). In the Valsartan in Acute Myocardial Infarction Trial (VALIANT), discontinuation due to various types of renal dysfunction occurred in 1.1% of valsartan-treated patients and 0.8% of captopril-treated patients. Include assessment of renal function when evaluating patients with heart failure or post-myocardial infarction.
5.8 Serum Electrolyte Abnormalities
Monitor serum potassium periodically in patients receiving Valturna. Drugs that affect the renin-angiotensin system can cause hyperkalemia. Risk factors for the development of hyperkalemia include renal insufficiency, diabetes [see Contraindications (4), Warnings (5.2), and Clinical Trials (14.2)], NSAIDs, potassium supplements or potassium sparing diuretics.
In the short-term controlled trials of various doses of Valturna, in patients without renal insufficiency the incidence of hyperkalemia (serum potassium >5.5 mEq/L) was about 1%-2% higher in the combination treatment group compared with the monotherapies aliskiren and valsartan, or with placebo.
In a long-term, uncontrolled study with median treatment duration of about one year, about 4% of the patients had at least one serum potassium >5.5 mEq/L at some time during the study; about 0.8% of patients discontinued study treatment and had a high serum potassium at some point during the study. Patients with hyperkalemia were older (median age 65 vs. 55) with slightly lower mean baseline estimated creatinine clearance compared to patients without hyperkalemia. While about 25% of the hyperkalemic episodes occurred in the first two months, other initial episodes were reported throughout the study.
6 ADVERSE REACTIONS
6.1 Clinical Studies Experience
The following serious adverse reactions are discussed in greater detail in other sections of the label:
- Risk of fetal/neonatal morbidity and mortality [See Warnings and Precautions (5.1)].
- Head and neck angioedema [See Warnings and Precautions (5.3)].
- Hypotension [See Warnings and Precautions (5.4)].
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in clinical trials of another drug and may not reflect the rates observed in practice.
Valturna
Valturna has been evaluated for safety in more than 1,225 patients, including over 316 patients for over 1 year. In placebo-controlled clinical trials, discontinuation of therapy because of a clinical adverse event (including uncontrolled hypertension) occurred in 1.4% of patients treated with Valturna versus 2.7% of patients given placebo.
Adverse events in placebo-controlled trials that occurred in at least 1% of patients treated with Valturna and at a higher incidence than placebo included fatigue (2.6% vs. 1.4%), nasopharyngitis (2.6% vs. 2.2%), diarrhea (1.4% vs 0.9%), upper respiratory tract infection (1.4% vs. 1.1%), urinary tract infection (1.4% vs. 0.6%), influenza (1.1% vs 0.2%), and vertigo (1.1% vs. 0.3%).
Aliskiren
Aliskiren has been evaluated for safety in 6,460 patients, including 1,740 treated for longer than 6 months, and 1,250 for longer than 1 year. In placebo-controlled clinical trials, discontinuation of therapy because of a clinical adverse event, including uncontrolled hypertension occurred in 2.2% of patients treated with aliskiren, versus 3.5% of patients given placebo. These data do not include information from the ALTITUDE study which evaluated the use of aliskiren in combination with ARBs or ACEI [see Contraindications (4), Warnings (5.2), and Clinical Trials (14.2)].
Two cases of angioedema with respiratory symptoms were reported with aliskiren use in the clinical studies. Two other cases of periorbital edema without respiratory symptoms were reported as possible angioedema and resulted in discontinuation. The rate of these angioedema cases in the completed studies was 0.06%.
In addition, 26 other cases of edema involving the face, hands, or whole body were reported with aliskiren use, including 4 leading to discontinuation.
In the placebo-controlled studies, however, the incidence of edema involving the face, hands, or whole body was 0.4% with aliskiren compared with 0.5% with placebo. In a long-term active-controlled study with aliskiren and HCTZ arms, the incidence of edema involving the face, hands, or whole body was 0.4% in both treatment arms.
Aliskiren produces dose-related gastrointestinal (GI) adverse reactions. Diarrhea was reported by 2.3% of patients at 300 mg, compared to 1.2% in placebo patients. In women and the elderly (age ≥65) increases in diarrhea rates were evident starting at a dose of 150 mg daily, with rates for these subgroups at 150 mg similar to those seen at 300 mg for men or younger patients (all rates about 2%). Other GI symptoms included abdominal pain, dyspepsia, and gastroesophageal reflux, although increased rates for abdominal pain and dyspepsia were distinguished from placebo only at 600 mg daily. Diarrhea and other GI symptoms were typically mild and rarely led to discontinuation.
Aliskiren was associated with a slight increase in cough in the placebo-controlled studies (1.1% for any aliskiren use vs. 0.6% for placebo). In active-controlled trials with ACE inhibitor (ramipril, lisinopril) arms, the rates of cough for the aliskiren arms were about one-third to one-half the rates in the ACE inhibitor arms.
Other adverse reactions with increased rates for aliskiren compared to placebo included rash (1% vs. 0.3%), elevated uric acid (0.4% vs. 0.1%), gout (0.2% vs. 0.1%), and renal stones (0.2% vs. 0%).
Single episodes of tonic-clonic seizures with loss of consciousness were reported in two patients treated with aliskiren in the clinical trials. One patient had predisposing causes for seizures and had a negative electroencephalogram (EEG) and cerebral imaging following the seizures; for the other patient, EEG and imaging results were not reported. Aliskiren was discontinued and there was no rechallenge in either case.
No clinically meaningful changes in vital signs or in ECG (including QTc interval) were observed in patients treated with aliskiren.
Valsartan
Valsartan has been evaluated for safety in more than 4,000 hypertensive patients in clinical trials, including over 400 treated for over 6 months, and more than 160 for over 1 year.
In trials in which valsartan was compared to an ACE inhibitor with or without placebo, the incidence of dry cough was significantly greater in the ACE inhibitor group (7.9%) than in the groups who received valsartan (2.6%) or placebo (1.5%). In a 129 patient trial limited to patients who had had dry cough when they had previously received ACE inhibitors, the incidences of cough in patients who received valsartan, HCTZ, or lisinopril were 20%, 19%, and 69% respectively (p<0.001).
Other adverse reactions, not listed above, occurring in >0.2% of patients in controlled clinical trials with valsartan are:
Body as a Whole: allergic reaction, asthenia
Musculoskeletal: muscle cramps
Neurologic and Psychiatric: paresthesia
Respiratory: sinusitis, pharyngitis
Urogenital: impotence
Other reported events seen less frequently in clinical trials were: angioedema.
Adverse reactions reported for valsartan for indications other than hypertension may be found in the prescribing information for Diovan.
Clinical Laboratory Test Abnormalities
RBC count, hemoglobin and hematocrit:
Small mean decreases from baseline were seen in RBC count, hemoglobin and hematocrit in both monotherapies and combination therapy. These changes were small, but changes in hemoglobin were slightly more pronounced with the combination therapy (-0.26 g/dL) than with monotherapy regimens (-0.04 g/dL in aliskiren or -0.13 g/dL in valsartan) or placebo (+0.07 g/dL).
Blood Urea Nitrogen (BUN)/Creatinine:
In patients without renal dysfunction, elevations in BUN (>40 mg/dL) and creatinine (>2.0 mg/dL) in any treatment group were less than 1.0%. For creatinine, 0.5% (3/599) of patients on combination treatment had a creatinine level >1.5 mg/dL at the end of the study and a 30% increase from baseline compared to none in either monotherapy or placebo [see Warnings (5.2)].
6.2 Post-Marketing Experience
The following adverse reactions have been reported in aliskiren post-marketing experience. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to estimate their frequency or establish a causal relationship to drug exposure.
Hypersensitivity: angioedema requiring airway management and hospitalization
Skin: Severe cutaneous adverse reactions, including Stevens Johnson syndrome and toxic epidermal necrolysis
Peripheral edema
7 DRUG INTERACTIONS
No drug interaction studies have been conducted with Valturna and other drugs, although studies with the individual aliskiren and valsartan components are described below.
Aliskiren
Cyclosporine: Avoid co-administration of cyclosporine with aliskiren.
Itraconazole: Avoid co-administration of itraconazole with aliskiren [see Clinical Pharmacology (12.3)].
Valsartan
No clinically significant pharmacokinetic interactions were observed when valsartan was coadministered with aliskiren, amlodipine, atenolol, cimetidine, digoxin, furosemide, glyburide, hydrochlorothiazide, or indomethacin. The valsartan-atenolol combination was more antihypertensive than either component, but it did not lower the heart rate more than atenolol alone.
Warfarin: Coadministration of valsartan and warfarin did not change the pharmacokinetics of valsartan or the time-course of the anticoagulant properties of warfarin.
CYP 450 Interactions: In vitro metabolism studies have indicated that CYP450 mediated drug interactions between valsartan and coadministered drugs are unlikely because of low extent of metabolism [see Pharmacokinetics – Valsartan (12.3)].
Transporters: The results from an in vitro study with human liver tissue indicate that valsartan is a substrate of the hepatic uptake transporter OATP1B1 and the hepatic efflux transporter MRP2. Coadministration of inhibitors of the uptake transporter (rifampin, cyclosporine) or efflux transporter (ritonavir) may increase the systemic exposure to valsartan.
As with other drugs that block angiotensin II or its effects, concomitant use of potassium sparing diuretics (e.g., spironolactone, triamterene, amiloride), potassium supplements, or salt substitutes containing potassium may lead to increases in serum potassium and in heart failure patients to increases in serum creatinine.
Aliskiren and Valsartan
Non-Steroidal Anti-Inflammatory Agents(NSAIDS) including selective Cyclooxygenase-2 inhibitors (COX-2 inhibitors): In patients who are elderly, volume-depleted (including those on diuretic therapy), or with compromised renal function, co-administration of NSAIDs, including selective COX-2 inhibitors with agents that affect the renin-angiotensin system, including aliskiren and valsartan, may result in deterioration of renal function, including possible acute renal failure. These effects are usually reversible. Monitor renal function periodically in patients receiving aliskiren, valsartan and NSAID therapy.
The antihypertensive effect may be attenuated by NSAIDS.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category D
Use of drugs that act on the renin-angiotensin system during the second and third trimesters of pregnancy reduces fetal renal function and increases fetal and neonatal morbidity and death. Resulting oligohydramnios can be associated with fetal lung hypoplasia and skeletal deformations. Potential neonatal adverse effects include skull hypoplasia, anuria, hypotension, renal failure, and death. When pregnancy is detected, discontinue Valturna as soon as possible. These adverse outcomes are usually associated with use of these drugs in the second and third trimester of pregnancy. Most epidemiologic studies examining fetal abnormalities after exposure to antihypertensive use in the first trimester have not distinguished drugs affecting the renin-angiotensin system from other antihypertensive agents. Appropriate management of maternal hypertension during pregnancy is important to optimize outcomes for both mother and fetus.
In the unusual case that there is no appropriate alternative to therapy with drugs affecting the renin-angiotensin system for a particular patient, apprise the mother of the potential risk to the fetus. Perform serial ultrasound examinations to assess the intra-amniotic environment. If oligohydramnios is observed, discontinue Valturna, unless it is considered lifesaving for the mother. Fetal testing may be appropriate, based on the week of pregnancy. Patients and physicians should be aware, however, that oligohydramnios may not appear until after the fetus has sustained irreversible injury. Closely observe infants with histories of in utero exposure to Valturna for hypotension, oliguria, and hyperkalemia. [see Use in Specific Populations (8.4)]
No reproductive toxicity studies have been conducted with the combination of aliskiren and valsartan. However, these studies have been conducted for aliskiren as well as valsartan alone [See Nonclinical Toxicology (13)].
8.3 Nursing Mothers
It is not known whether aliskiren is excreted in human milk, but aliskiren was secreted in the milk of lactating rats. It is not known whether valsartan is excreted in human milk. Valsartan was excreted into the milk of lactating rats; however, animal breast milk drug levels may not accurately reflect human breast milk levels. Because of the potential for adverse effects on the nursing infant, a decision should be made whether to discontinue nursing or discontinue the drug, taking into account the importance of the drug to the mother.
8.4 Pediatric Use
Safety and effectiveness of Valturna in pediatric patients have not been established.
Neonates with a history of in utero exposure to Valturna:
If oliguria or hypotension occurs, direct attention toward support of blood pressure and renal perfusion. Exchange transfusions or dialysis may be required as a means of reversing hypotension and/or substituting for disordered renal function.
8.5 Geriatric Use
In the short-term controlled clinical trials of Valturna, 99 (15.9%) patients treated with Valturna were ≥65 years and 14 (2.2%) were ≥75 years.
No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
10 OVERDOSAGE
Aliskiren
Limited data are available related to overdosage in humans. The most likely manifestation of overdosage would be hypotension. If symptomatic hypotension occurs, provide supportive treatment.
Aliskiren is poorly dialyzed. Therefore, hemodialysis is not adequate to treat aliskiren overexposure [see Clinical Pharmacology (12.3)].
Valsartan
Limited data are available related to overdosage in humans. The most likely effect of overdose with valsartan would be hypotension and tachycardia; bradycardia could occur from parasympathetic (vagal) stimulation. Depressed level of consciousness, circulatory collapse and shock have been reported. If symptomatic hypotension occurs, provide supportive treatment.
Valsartan is not removed from the plasma by hemodialysis.
Valsartan was without grossly observable adverse effects at single oral doses up to 2000 mg/kg in rats and up to 1000 mg/kg in marmosets, except for the salivation and diarrhea in the rat and vomiting in the marmoset at the highest dose (60 and 31 times, respectively, the maximum recommended human dose on a mg/m2 basis). (Calculations assume an oral dose of 320 mg/day and a 60-kg patient.)
11 DESCRIPTION
Valturna is a single tablet for oral administration of aliskiren (an orally active, nonpeptide, potent renin inhibitor) and valsartan (an orally active, nonpeptide, specific angiotensin II antagonist acting on the AT1 receptor subtype).
Aliskiren
Aliskiren hemifumarate is chemically described as (2S,4S,5S,7S)-N-(2-carbamoyl-2-methylpropyl)-5-amino-4-hydroxy-2,7-diisopropyl-8-[4-methoxy-3-(3-methoxypropoxy)phenyl]-octanamide hemifumarate and its structural formula is
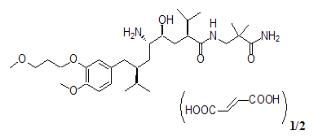
Molecular formula: C30H53N3O6 • 0.5 C4H4O4
Aliskiren hemifumarate is a white to slightly yellowish crystalline powder with a molecular weight of 609.8 (free base- 551.8). It is soluble in phosphate buffer, n-octanol, and highly soluble in water.
Valsartan
Valsartan is a white to practically white fine powder, soluble in ethanol and methanol and slightly soluble in water. Valsartan’s chemical name is N-(1-oxopentyl)-N-[[2’-(1H-tetrazol-5-yl) [1,1’-biphenyl]-4-yl]methyl]-L-valine; its structural formula is
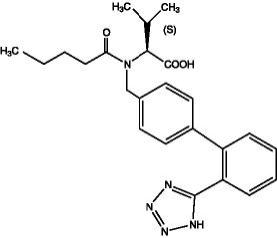
Its empirical formula is C24H29N5O3 and its molecular weight is 435.5.
Valturna tablets are formulated for oral administration to contain aliskiren hemifumarate and valsartan, USP 150/160 mg, and 300/320 mg. The inactive ingredients for all strengths of the tablets are colloidal silicon dioxide, crospovidone, hydroxypropylcellulose, indigotin blue lake, iron oxide black, iron oxide red, iron oxide yellow, magnesium stearate, microcrystalline cellulose, polyethylene glycol, talc, titanium dioxide and hypromellose.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Aliskiren
Renin is secreted by the kidney in response to decreases in blood volume and renal perfusion. Renin cleaves angiotensinogen to form the inactive decapeptide angiotensin I (Ang I). Ang I is converted to the active octapeptide angiotensin II (Ang II) by angiotensin-converting enzyme (ACE) and non-ACE pathways. Ang II is a powerful vasoconstrictor and leads to the release of catecholamines from the adrenal medulla and prejunctional nerve endings. It also promotes aldosterone secretion and sodium reabsorption. Together, these effects increase blood pressure. Ang II also inhibits renin release, thus providing a negative feedback to the system. This cycle, from renin through angiotensin to aldosterone and its associated negative feedback loop, is known as the renin-angiotensin-aldosterone system (RAAS). Aliskiren is a direct renin inhibitor, decreasing plasma renin activity (PRA) and inhibiting the conversion of angiotensinogen to Ang I. Whether aliskiren affects other RAAS components, e.g., ACE or non-ACE pathways, is not known.
All agents that inhibit the RAAS, including renin inhibitors, suppress the negative feedback loop, leading to a compensatory rise in plasma renin concentration. When this rise occurs during treatment with ACE inhibitors and ARBs, the result is increased levels of PRA. During treatment with aliskiren, however, the effect of increased renin levels is blocked, so that PRA, Ang I and Ang II are all reduced, whether aliskiren is used as monotherapy or in combination with other antihypertensive agents.
Valsartan
Ang II is formed from Ang I in a reaction catalyzed by angiotensin-converting enzyme (ACE, kininase II). Ang II is the principal pressor agent of the renin-angiotensin-aldosterone system, with effects that include vasoconstriction, stimulation of synthesis and release of aldosterone, cardiac stimulation, and renal reabsorption of sodium. Valsartan blocks the vasoconstrictor and aldosterone-secreting effects of Ang II by selectively blocking the binding of Ang II to the AT1 receptor in many tissues, such as vascular smooth muscle and the adrenal gland. Its action is therefore independent of the pathways for Ang II synthesis.
There is also an AT2 receptor found in many tissues, but AT2 is not known to be associated with cardiovascular homeostasis. Valsartan has much greater affinity (about 20,000-fold) for the AT1 receptor than for the AT2 receptor. The increased plasma levels of angiotensin following AT1 receptor blockade with valsartan may stimulate the unblocked AT2 receptor. The primary metabolite of valsartan is essentially inactive with an affinity for the AT1 receptor about one-200th that of valsartan itself.
Blockade of the renin-angiotensin-aldosterone system with ACE inhibitors, which inhibit the biosynthesis of Ang II from Ang I, is widely used in the treatment of hypertension. ACE inhibitors also inhibit the degradation of bradykinin, a reaction also catalyzed by ACE. Because valsartan does not inhibit ACE (kininase II), it does not affect the response to bradykinin. Whether this difference has clinical relevance is not yet known. Valsartan does not bind to or block other hormone receptors or ion channels known to be important in cardiovascular regulation.
Blockade of the Ang II receptor inhibits the negative regulatory feedback of Ang II on renin secretion, but the resulting increased PRA and Ang II circulating levels do not overcome the effect of valsartan on blood pressure.
Valsartan has indications other than hypertension which can be found in the Diovan® package insert.
Valturna
Since aliskiren and valsartan block the RAAS at different sites (inhibition of plasma renin activity and antagonism of the AT1 receptor), their combination provides a complementary mechanism to achieve a pharmacologic inhibition of the RAAS. Such RAAS inhibition with Valturna is associated with significant reductions in PRA, Ang I, Ang II and aldosterone.
12.2 Pharmacodynamics
Aliskiren
PRA reductions in clinical trials ranged from approximately 50% to 80%, were not dose-related and did not correlate with blood pressure reductions. The clinical implications of the differences in effect on PRA are not known.
Valsartan
Valsartan inhibits the pressor effect of angiotensin II infusions. An oral dose of 80 mg inhibits the pressor effect by about 80% at peak with approximately 30% inhibition persisting for 24 hours. No information on the effect of larger doses is available.
Removal of the negative feedback of angiotensin II causes a 2- to 3-fold rise in plasma renin and consequent rise in angiotensin II plasma concentration in hypertensive patients. Minimal decreases in plasma aldosterone were observed after administration of valsartan; very little effect on serum potassium was observed.
In multiple-dose studies in hypertensive patients with stable renal insufficiency and patients with renovascular hypertension, valsartan had no clinically significant effects on glomerular filtration rate, filtration fraction, creatinine clearance, or renal plasma flow.
In multiple-dose studies in hypertensive patients, valsartan had no notable effects on total cholesterol, fasting triglycerides, fasting serum glucose, or uric acid.
Administration of valsartan to patients with essential hypertension results in a significant reduction of sitting, supine, and standing systolic blood pressure, usually with little or no orthostatic change.
Valturna
In normotensive subjects receiving sodium supplementation, a single oral dose of 320 mg valsartan increased PRA, angiotensin I and angiotensin II, whereas 300 mg of aliskiren decreased them for 48 hours. In combination, 150 mg of aliskiren neutralized the 160 mg valsartan-induced increase in PRA, plasma angiotensin I and angiotensin II for 48 hours. The reduction in urinary aldosterone excretion with the 150/160 mg aliskiren/valsartan combination was similar to 300 mg of aliskiren and greater than that of 320 mg of valsartan and placebo.
12.3 Pharmacokinetics
Absorption and Distribution
Valturna
Following oral administration of Valturna combination tablets, the median peak plasma concentration times are within 1 hour for aliskiren and 3 hours for valsartan. The mean half-lives of aliskiren and valsartan are 34 hours and 12 hours, respectively. The rate and extent of absorption of aliskiren and valsartan from Valturna are the same as when administered as individual tablets. When taken with food, mean AUC and Cmax of aliskiren are decreased by 76% and 88%, respectively; mean AUC and Cmax of valsartan were not significantly affected. In clinical trials of Valturna, it was administered without requiring a fixed relation of administration to meals.
Valsartan
The steady state volume of distribution of valsartan after intravenous administration is 17 L indicating that valsartan does not distribute into tissues extensively. Valsartan is highly bound to serum proteins (95%), mainly serum albumin.
Metabolism and Elimination
Aliskiren
About one-fourth of the absorbed dose appears in the urine as parent drug. How much of the absorbed dose is metabolized is unknown. Based on the in vitro studies, the major enzyme responsible for aliskiren metabolism appears to be CYP 3A4. Aliskiren does not inhibit the CYP450 isoenzymes (CYP 1A2, 2C8, 2C9, 2C19, 2D6, 2E1, and 3A) or induce CYP 3A4.
Transporters: Pgp (MDR1/Mdr1a/1b) was found to be the major efflux system involved in absorption and disposition of aliskiren in preclinical studies. The potential for drug interactions at the Pgp site will likely depend on the degree of inhibition of this transporter.
Valsartan
Valsartan shows bi-exponential decay kinetics following intravenous administration with an average elimination half-life of about 6 hours. The recovery is mainly as unchanged drug, with only about 20% of dose recovered as metabolites. The primary metabolite, accounting for about 9% of dose, is valeryl 4-hydroxy valsartan. In vitro metabolism studies involving recombinant CYP450 enzymes indicated that the CYP2C9 isozyme is responsible for the formation of valeryl-4-hydroxy valsartan. It has also been shown that valsartan does not inhibit CYP450 isozymes at clinically relevant concentrations. CYP450 mediated drug interactions between valsartan and coadministered drugs are unlikely because of the low extent of metabolism.
Valsartan, when administered as an oral solution, is primarily recovered in feces (about 83% of dose) and urine (about 13% of dose). Following intravenous administration, plasma clearance of valsartan is about 2 L/h and its renal clearance is 0.62 L/h (about 30% of total clearance).
Drug interactions
Aliskiren
The effect of co-administered drugs on the pharmacokinetics of aliskiren and vice versa, were studied in several single and multiple dose studies. Pharmacokinetic measures indicating the magnitude of these interactions are presented in Figure 5 (impact of co-administered drugs on aliskiren) and Figure 6 (impact on co-administered drugs).
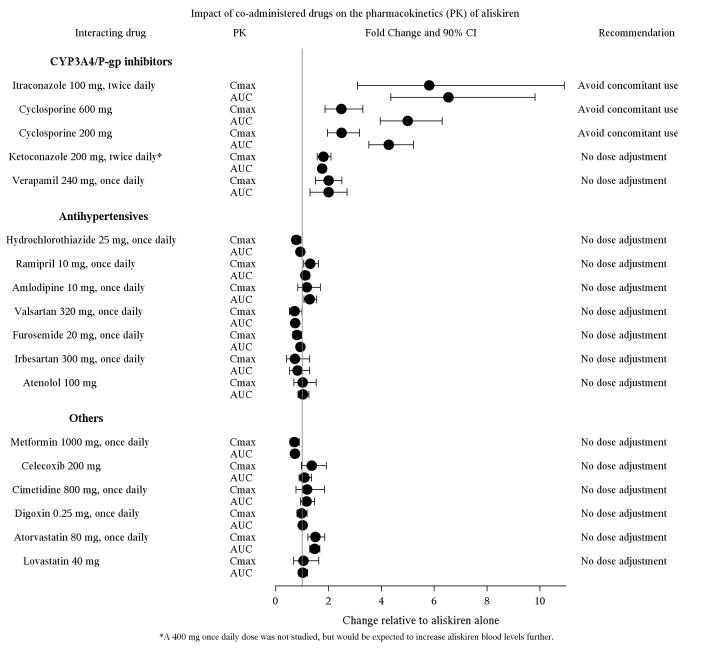
Figure 5: The impact of co-administered drugs on the pharmacokinetics of aliskiren.
Warfarin: There was no clinically significant effect of a single dose of warfarin 25 mg on the pharmacokinetics of aliskiren.

Figure 6: The impact of aliskiren on the pharmacokinetics of co-administered drugs.
Special Populations
Pediatric Patients
The pharmacokinetics of Valturna have not been investigated in patients <18 years of age.
Geriatric Patients
The pharmacokinetics of aliskiren were studied in the elderly (≥65 years). Exposure (measured by AUC) is increased in elderly patients. Adjustment of the starting dose is not required in these patients. Exposure (measured by AUC) to valsartan is higher by 70% and the half-life is longer by 35% in the elderly than in the young. No dosage adjustment is necessary.
Race
With Valturna, pharmacokinetic differences due to race have not been studied. The pharmacokinetic differences among Blacks, Caucasians, and Japanese are minimal with aliskiren therapy.
Renal Impairment
Aliskiren
The pharmacokinetics of aliskiren were evaluated in patients with varying degrees of renal impairment. Rate and extent of exposure (AUC and Cmax) of aliskiren in subjects with renal impairment did not show a consistent correlation with the severity of renal impairment. Adjustment of the starting dose is not required in these patients [see Warnings (5.2)].
The pharmacokinetics of aliskiren following administration of a single oral dose of 300 mg was evaluated in patients with End Stage Renal Disease (ESRD) undergoing hemodialysis. When compared to matched healthy subjects, changes in the rate and extent of aliskiren exposure (Cmax and AUC) in ESRD patients undergoing hemodialysis was not clinically significant.
Timing of hemodialysis did not significantly alter the pharmacokinetics of aliskiren in ESRD patients. Therefore, no dose adjustment is warranted in ESRD patients receiving hemodialysis.
Valsartan
There is no apparent correlation between renal function (measured by creatinine clearance) and exposure (measured by AUC) to valsartan in patients with different degrees of renal impairment. Consequently, dose adjustment is not required in patients with mild-to-moderate renal dysfunction. No studies have been performed in patients with severe impairment of renal function (creatinine clearance <10 mL/min). Valsartan is not removed from the plasma by hemodialysis.
Hepatic Impairment
Aliskiren
The pharmacokinetics of aliskiren were not significantly affected in patients with mild-to-severe liver disease. Consequently, adjustment of the starting dose is not required in these patients.
Valsartan
On average, patients with mild-to-moderate chronic liver disease have twice the exposure (measured by AUC values) to valsartan of healthy volunteers (matched by age, sex and weight). In general, no dosage adjustment is needed in patients with mild-to-moderate liver disease.
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Valturna
No carcinogenicity, mutagenicity or fertility studies have been conducted for Valturna alone as these studies have been conducted for each individual component. Valturna has been studied in 2- and 13-week toxicity studies and was generally well-tolerated. Findings were primarily attributable to the exaggerated pharmacological effects of each component.
Aliskiren
Carcinogenic potential was assessed in a 2-year rat study and a 6-month transgenic (rasH2) mouse study with aliskiren hemifumarate at oral doses of up to 1500 mg aliskiren/kg/day. Although there were no statistically significant increases in tumor incidence associated with exposure to aliskiren, mucosal epithelial hyperplasia (with or without erosion/ulceration) was observed in the lower gastrointestinal tract at doses of 750 or more mg/kg/day in both species, with a colonic adenoma identified in one rat and a cecal adenocarcinoma identified in another, rare tumors in the strain of rat studied. On a systemic exposure (AUC0-24hr) basis, 1500 mg/kg/day in the rat is about 4 times and in the mouse about 1.5 times the maximum recommended human dose (300 mg aliskiren/day). Mucosal hyperplasia in the cecum or colon of rats was also observed at doses of 250 mg/kg/day (the lowest tested dose) as well as at higher doses in 4- and 13-week studies.
Aliskiren hemifumarate was devoid of genotoxic potential in the Ames reverse mutation assay with S. typhimurium and E. coli, the in vitro Chinese hamster ovary cell chromosomal aberration assay, the in vitro Chinese hamster V79 cell gene mutation test and the in vivo mouse bone marrow micronucleus assay.
Fertility of male and female rats was unaffected at doses of up to 250 mg aliskiren/kg/day (8 times the maximum recommended human dose of 300 mg Tekturna/60 kg on a mg/m2 basis).
Valsartan
There was no evidence of carcinogenicity when valsartan was administered in the diet to mice and rats for up to 2 years at concentrations calculated to provide doses of up to 160 and 200 mg/kg/day, respectively. These doses in mice and rats are about 2.4 and 6 times, respectively, the MRHD of 320 mg/day on a mg/m2 basis. (Calculations based on a 60 kg patient.)
Mutagenicity assays did not reveal any valsartan-related effects at either the gene or chromosome level. These assays included bacterial mutagenicity tests with Salmonella and E. coli, a gene mutation test with Chinese hamster V79 cells, a cytogenetic test with Chinese hamster ovary cells, and a rat micronucleus test.
13.2 Animal Toxicology and/or Pharmacology
Reproductive Toxicology Studies
Aliskiren
Reproductive toxicity studies of aliskiren hemifumarate did not reveal any evidence of teratogenicity at oral doses up to 600 mg aliskiren/kg/day (20 times the maximum recommended human dose [MRHD] of 300 mg/day on a mg/m2 basis) in pregnant rats or up to 100 mg aliskiren/kg/day (seven times the MRHD on a mg/m2 basis) in pregnant rabbits. Fetal birth weight was adversely affected in rabbits at 50 mg/kg/day (3.2 times the MRHD on a mg/m2 basis). Aliskiren was present in placenta, amniotic fluid and fetuses of pregnant rabbits.
Valsartan
No teratogenic effects were observed when valsartan was administered to pregnant mice and rats at oral doses up at 600 mg/kg/day and to pregnant rabbits at oral doses up to 10 mg/kg/day. However, significant decreases in fetal weight, pup birth weight, pup survival rate, and slight delays in developmental milestones were observed in studies in which parental rats were treated with valsartan at oral, maternally toxic (reduction in body weight gain and food consumption) doses of 600 mg/kg/day during organogenesis or late gestation and lactation. In rabbits, fetotoxicity (i.e., resorptions, litter loss, abortions, and low body weight) associated with maternal toxicity (mortality) was observed at doses of 5 and 10 mg/kg/day. The no observed adverse effect doses of 600, 200 and 2 mg/kg/day in mice, rats and rabbits represent 9, 6, and 0.1 times, respectively, the maximum recommended human dose on a mg/m2 basis. Calculations assume an oral dose of 320 mg/day and a 60-kg patient.
14 CLINICAL STUDIES
14.1 Valturna
Aliskiren 150 mg and 300 mg and valsartan 160 mg and 320 mg were studied alone and in combination in an 8-week, 1,797-patient, randomized, double-blind, placebo-controlled, parallel-group, 4-arm, dose-escalation study. The dosages of aliskiren and valsartan were started at 150 mg and 160 mg, respectively, and increased at four weeks to 300 mg and 320 mg, respectively. Seated trough cuff blood pressure was measured at baseline, 4, and 8 weeks. Blood pressure reductions with the combinations were statistically significantly (p<0.05) greater than the reductions with the monotherapies as shown in Table 1.
| Valsartan, mg | ||||
| Aliskiren, mg | (mmHg) | 0 | 160 | 320 |
| Mean Change | 4.6/4.1* | 10.9/8.7 | 12.8/9.7 | |
| 0 | Placebo-Subtracted Mean Change | -- | 5.6/3.9p | 8.2/5.6p |
| Mean Change | 10.7/7.5 | 15.3/10.5 | -- | |
| 150 | Placebo-Subtracted Mean Change | 5.4/2.7p | 10.0/5.7pav | -- |
| Mean Change | 13.0/9.0 | -- | 17.2/12.2 | |
| 300 | Placebo-Subtracted Mean Change | 8.4/4.9p | -- | 12.6/8.1pav |
| * The placebo change is 5.2/4.8 for Week 4 endpoint which was used for the dose groups containing aliskiren 150 mg or valsartan 160 mg. p p<0.05 vs. placebo by ANCOVA for the pairwise comparison. a p<0.05 vs. respective aliskiren monotherapy by ANCOVA for the pairwise comparison. v p<0.05 vs. respective valsartan monotherapy by ANCOVA for the pairwise comparison. |
||||
The safety and efficacy of Valturna as initial therapy were evaluated. The figures [See Indications and Usage (1)] display the probability that a patient will achieve systolic or diastolic blood pressure goal with Valturna 300/320 mg, based upon their baseline systolic or diastolic blood pressure. At all levels of baseline blood pressure, the probability of achieving any given diastolic or systolic goal is greater with the combination than for either monotherapy.
The antihypertensive effect of Valturna was attained within 2 weeks.
One active-controlled trial investigated the addition of aliskiren 300 mg plus valsartan 320 mg in hypertensive patients who did not respond adequately to HCTZ 25 mg, and showed decreases from baseline in systolic and diastolic blood pressure of approximately 22/16 mmHg compared with approximately 6/6 mmHg with continuation of HCTZ 25 mg alone.
The antihypertensive effect was similar in patients with or without diabetes, in patients ≥65 years of age and <65 years of age, and in women and men. The effects of aliskiren, valsartan, and the combination were diminished in Blacks compared to Caucasians as has been seen with ACE inhibitors, other angiotensin receptor blockers, and beta blockers.
There are no trials of the Valturna combination tablet demonstrating reductions in cardiovascular risk in patients with hypertension, but several ARBs which are the same pharmacological class as the valsartan component, have demonstrated such benefits.
14.2 Aliskiren in Patients with Diabetes treated with ARB or ACEI (ALTITUDE study)
Patients with diabetes with renal disease (defined either by the presence of albuminuria or reduced GFR) were randomized to aliskiren 300 mg daily (n=4283) or placebo (n=4296). All patients were receiving background therapy with an ARB or ACEI. The primary efficacy outcome was the time to the first event of the primary composite endpoint consisting of cardiovascular death, resuscitated sudden death, non-fatal myocardial infarction, non-fatal stroke, unplanned hospitalization for heart failure, onset of end stage renal disease, renal death, and doubling of serum creatinine concentration from baseline sustained for at least one month. After a median follow up of about 27 months, the trial was terminated early for lack of efficacy. Higher risk of renal impairment, hypotension and hyperkalemia was observed in aliskiren compared to placebo treated patients, as shown in the table below.
| Aliskiren N=4283 | Placebo N=4296 |
|||
| Serious Adverse Events* (%) | Adverse Events (%) | Serious Adverse Events* (%) | Adverse Events (%) | |
| Renal impairment † | 4.7 | 12.4 | 3.3 | 10.4 |
| Hypotension †† | 2.0 | 18.6 | 1.7 | 14.8 |
| Hyperkalemia ††† | 1.1 | 36.9 | 0.3 | 27.1 |
†renal failure, renal failure acute, renal failure chronic, renal impairment
††dizziness, dizziness postural, hypotension, orthostatic hypotension, presyncope, syncope
††† Given the variable baseline potassium levels of patients with renal insufficiency on dual RAAS therapy, the reporting of adverse event of hyperkalemia was at the discretion of the investigator.
* A Serious Adverse Event (SAE) is defined as: an event which is fatal or life-threatening, results in persistent or significant disability/incapacity, constitutes a congenital anomaly/birth defect, requires inpatient hospitalization or prolongation of existing hospitalization, or is medically significant (i.e. defined as an event that jeopardizes the patient or may require medical or surgical intervention to prevent one of the outcomes previously listed).
The risk of stroke (2.7% aliskiren vs 2.0% placebo) and death (6.9% aliskiren vs. 6.4% placebo) were also numerically higher in aliskiren treated patients.
16 HOW SUPPLIED/STORAGE AND HANDLING
Valturna is supplied as convex, beveled edged, ovaloid film-coated tablets.
All strengths are packaged in bottles and unit-dose blister packages (10 strips of 10 tablets) as described below.
| Tablet | Color | Debossed | Debossed | NDC 0078- XXXX-XX | ||
| Aliskiren/valsartan | Side 1 | Side 2 | Bottle of 30 | Bottle of 90 | Blister Packages of 100 | |
| 150 mg/160 mg | Light Red | NVR | HDU | 0572-15 | 0572-34 | 0572-35 |
| 300 mg/320 mg | Light Brown | NVR | SNB | 0574-15 | 0574-34 | 0574-35 |
Storage
Store at 25ºC (77ºF); excursions permitted to 15-30ºC (59-86ºF) in original container. [See USP Controlled Room Temperature.]
Protect from moisture.
Dispense in original container.
17 PATIENT COUNSELING INFORMATION
See FDA-approved patient labeling (Patient Information)
Healthcare professionals should instruct their patients to read the Patient Package Insert before starting Valturna and to reread each time the prescription is renewed. Patients should be instructed to inform their doctor or pharmacist if they develop any unusual symptom, or if any known symptom persists or worsens.
Pregnancy
Female patients of childbearing age should be told about the consequences of exposure to Valturna during pregnancy. Discuss treatment options with women planning to become pregnant. Patients should be asked to report pregnancies to their physicians as soon as possible.
Symptomatic Hypotension
Caution patients receiving Valturna that lightheadedness can occur, especially during the first days of therapy, and that it should be reported to the prescribing physician. Tell the patients that if syncope occurs, discontinue Valturna until the physician has been consulted.
Caution all patients that inadequate fluid intake, excessive perspiration, diarrhea, or vomiting can lead to an excessive fall in blood pressure, with the same consequences of lightheadedness and possible syncope.
Potassium Supplements
Tell patients receiving Valturna not to use potassium supplements or salt substitutes containing potassium without consulting the prescribing physician.
Relationship to Meals
Patients should establish a routine pattern for taking Valturna with regard to meals. High-fat meals decrease absorption substantially.
FDA-Approved Patient Labeling
Patient Information
Valturna® (val-tur-na )
(aliskiren and valsartan, USP) Tablets
Read the Patient Information that comes with Valturna before you start taking it and each time you get a refill. There may be new information. This leaflet does not take the place of talking with your doctor about your condition and treatment.
What is the most important information I should know about Valturna?
Valturna can cause harm or death to an unborn baby. Talk to your doctor about other ways to lower your blood pressure if you plan to become pregnant. If you get pregnant while taking Valturna, tell your doctor right away.
What is Valturna?
Valturna contains two prescription medicines in one tablet that work together to lower blood pressure. It contains:
- aliskiren (Tekturna), a direct renin inhibitor (DRI)
- valsartan (Diovan), an angiotensin receptor blocker (ARB)
Aliskiren (Tekturna) reduces the effect of renin, and the harmful process that narrows blood vessels. Aliskiren also helps blood vessels relax and widen so blood pressure is lower. Valsartan (Diovan) can help lower your blood pressure by blocking a potent chemical, angiotensin II, that leads to blood vessel constriction and narrowing.
Valturna may be used to lower high blood pressure in adults:
- when one medicine to lower high blood pressure is not enough
- as the first medicine to lower high blood pressure if your doctor decides that you are likely to need more than one medicine
Valturna has not been studied in children under 18 years of age.
Your doctor may prescribe other medicines for you to take along with Valturna to treat your high blood pressure.
What is high blood pressure (hypertension)?
Blood pressure is the force that pushes the blood through your blood vessels to all the organs of your body. You have high blood pressure when the force of your blood moving through your blood vessels is too great. One cause of high blood pressure is renin, a chemical in the body that starts a process that makes blood vessels narrow, leading to high blood pressure.
Valturna reduces high blood pressure. Medicines that lower your blood pressure lower your chance of having a stroke or heart attack. High blood pressure makes the heart work harder to pump blood throughout the body and causes damage to the blood vessels. If high blood pressure is not treated, it can lead to stroke, heart attack, heart failure, kidney failure, and vision problems.
Blood pressure is reduced more with Valturna than when either Tekturna or Diovan is taken by itself.
Who should not take Valturna?
-
If you get pregnant, stop taking Valturna and call your doctor right away. If you plan to become pregnant, talk to your doctor about other treatment options for your high blood pressure.
-
If you have diabetes.
- Do not take Valturna if you are allergic to any of its ingredients. See the end of this leaflet for a complete list of the ingredients in Valturna.
What should I tell my doctor before taking Valturna?
Tell your doctor about all your medical conditions, including whether you:
- have kidney problems
- have liver problems
- have ever had a reaction called angioedema, to another blood pressure medicine. Angioedema causes swelling of the face, lips, tongue, throat, arms and legs, and may cause difficulty breathing.
- are pregnant or planning to become pregnant. See What is the most important information I should know about Valturna?
- are breast-feeding. It is not known if Valturna passes into your breast milk.
Tell your doctor about all the medicines you take including prescription and nonprescription medicines, vitamins and herbal supplements. Especially tell your doctor if you are taking:
- a kind of medicine called angiotensin receptor blocker or angiotensin converting enzyme inhibitor
- water pills (also called “diuretics”)
- medicines for treating fungus or fungal infections
- cyclosporine (a medicine used to suppress the immune system)
- potassium-containing medicines, potassium supplements, or salt substitutes containing potassium
- atorvastatin
- nonsteroidal anti-inflammatory drugs (like ibuprofen or naproxen)
Your doctor or pharmacist will know what medicines are safe to take together. Know your medicines. Keep a list of your medicines and show it to your doctor or pharmacist when you get a new medicine.
How should I take Valturna?
- Take Valturna exactly as prescribed by your doctor. It is important to take Valturna every day to control your blood pressure.
- Take Valturna once each day, about the same time each day.
- Take Valturna the same way everyday, either with or without a meal.
- Your doctor may change your dose of Valturna if needed.
- If you miss a dose of Valturna, take it as soon as you remember. If it is close to your next dose, do not take the missed dose. Just take the next dose at your regular time.
- If you take too much Valturna, call your doctor or a Poison Control Center, or go to the nearest hospital emergency room.
What are the possible side effects of Valturna?
Valturna may cause serious side effects:
-
Injury or death to an unborn baby. See What is the most important information I should know about Valturna?
-
Low blood pressure (hypotension). Your blood pressure may get too low if you also take water pills, are on a low-salt diet, get dialysis treatments, have heart problems, or get sick with vomiting or diarrhea. Drinking alcohol and taking certain medicines (barbiturates or narcotics) can cause low blood pressure to get worse. Lie down if you feel faint or dizzy, and call your doctor right away.
- Angioedema. Aliskiren, a component in Valturna, can cause swelling of the face, lips, tongue, throat, arms and legs, or the whole body. Get medical help right away and tell your doctor if you get any one or more of these symptoms. Angioedema can happen at any time while you are taking Valturna.
Common side effects of Valturna include:
- Tiredness
- Sore throat
- Runny nose
- Diarrhea
- Upper respiratory tract infection
- Urinary tract infection
- Flu or flu-like symptoms
- High levels of potassium in the blood (hyperkalemia)
- Dizziness
Tell your doctor if you have any side effect that bothers you or that does not go away. These are not all of the possible side effects of Valturna. For a complete list of side effects, ask your doctor or pharmacist.
How do I store Valturna?
- Store Valturna tablets at room temperature between 59oF-86oF (15oC-30oC).
- Keep Valturna in the original prescription bottle in a dry place. Do not remove the desiccant (drying agent) from the bottle.
Keep Valturna and all medicines out of the reach of children.
General information about Valturna
Medicines are sometimes prescribed for conditions not listed in the patient information leaflet. Do not take Valturna for a condition for which it was not prescribed. Do not give Valturna to other people, even if they have the same condition or symptoms you have. It may harm them.
This leaflet summarizes the most important information about Valturna. If you have questions about Valturna talk with your doctor. You can ask your doctor or pharmacist for information that is written for healthcare professionals.
For more information about Valturna, visit www.valturna.com or call 1-877-282-5887.
What are the ingredients in Valturna?
Active ingredients: Aliskiren and valsartan
Inactive ingredients: The inactive ingredients for all strengths of the tablets are colloidal silicon dioxide, crospovidone, hydroxypropylcellulose, indigotin blue lake, iron oxide black, iron oxide red, iron oxide yellow, magnesium stearate, microcrystalline cellulose, polyethylene glycol, talc, titanium dioxide, and hypromellose
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Manufactured by:
Novartis Pharma Stein AG
Stein, Switzerland
Distributed by:
Novartis Pharmaceuticals Corporation
East Hanover, New Jersey 07936
© Novartis
T2012-86/T2012-87
April 2012/April 2012
| VALTURNA
aliskiren hemifumarate and valsartan tablet, film coated |
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
| VALTURNA
aliskiren hemifumarate and valsartan tablet, film coated |
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||
| Labeler - Novartis Pharmaceuticals Corporation (002147023) |

