TRIMETHOPRIM- trimethoprim tablet
Watson Labs
----------
TRIMETHOPRIM
Tablets USP
Revised: April 2000
Rx Only
DESCRIPTION
Trimethoprim is a synthetic antibacterial available as 100 mg tablets for oral administration.
Trimethoprim is 2,4-Diamino-5-(3,4,5-trimethoxybenzyl)pyrimidine. It is a white to cream colored, odorless, bitter compound. The structural formula is represented below:
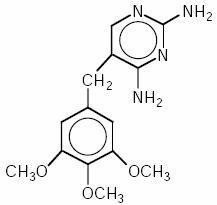
C14H18N4O3 M.W. 290.32
Trimethoprim Tablets USP, 100 mg contain the following inactive ingredients: anhydrous lactose, colloidal silicon dioxide, magnesium stearate, sodium lauryl sulfate, sodium starch glycolate and stearic acid.
CLINICAL PHARMACOLOGY
Trimethoprim is rapidly absorbed following oral administration. It exists in the blood as unbound, protein-bound and metabolized forms. Ten to twenty percent of trimethoprim is metabolized, primarily in the liver; the remainder is excreted unchanged in the urine. The principal metabolites of trimethoprim are the 1- and 3-oxides and the 3'- and 4'-hydroxy derivatives. The free form is considered to be the therapeutically active form. Approximately 44% of trimethoprim is bound to plasma proteins.
Mean peak plasma concentrations of approximately 1.0 mcg/mL occur 1 to 4 hours after oral administration of a single 100 mg dose. A single 200 mg dose will result in serum levels approximately twice as high. The half-life of trimethoprim ranges from 8 to 10 hours. However, patients with severely impaired renal function exhibit an increase in the half-life of trimethoprim, which requires either dosage regimen adjustment or not using the drug in such patients (seeDOSAGE AND ADMINISTRATION). During a 13-week study of trimethoprim administered at a daily dosage of 200 mg (50 mg q.i.d.), the mean minimum steady-state concentration of the drug was 1.1 mcg/mL. Steady-state concentrations were achieved within 2 to 3 days of chronic administration, and were maintained throughout the experimental period.
Excretion of trimethoprim is primarily by the kidneys through glomerular filtration and tubular secretion. Urine concentrations of trimethoprim are considerably higher than are the concentrations in the blood. After a single oral dose of 100 mg, urine concentrations of trimethoprim ranged from 30 to 160 mcg/mL during the 0- to 4-hour period and declined to approximately 18 to 91 mcg/mL during the 8- to 24-hour period. A 200 mg single oral dose will result in trimethoprim urine levels approximately twice as high. After oral administration, 50% to 60% of trimethoprim is excreted in the urine within 24 hours, approximately 80% of this being unmetabolized trimethoprim.
Since normal vaginal and fecal flora are the source of most pathogens causing urinary tract infections, it is relevant to consider the distribution of trimethoprim into these sites. Concentrations of trimethoprim in vaginal secretions are consistently greater than those found simultaneously in the serum, being typically 1.6 times the concentrations of simultaneously obtained serum samples. Sufficient trimethoprim is excreted in the feces to markedly reduce or eliminate trimethoprim-susceptible organisms from the fecal flora.
Trimethoprim also passes the placental barrier and is excreted in human milk.
Microbiology
Trimethoprim blocks the production of tetrahydrofolic acid from dihydrofolic acid by binding to and reversibly inhibiting the required enzyme, dihydrofolate reductase. This binding is much stronger for the bacterial enzyme than for the corresponding mammalian enzyme. Thus, trimethoprim selectively interferes with bacterial biosynthesis of nucleic acids and proteins.
In vitro serial dilution tests have shown that the spectrum of antibacterial activity of trimethoprim includes the common urinary tract pathogens with the exception of Pseudomonas aeruginosa.
The dominant non-Enterobacteriaceae fecal organisms, Bacteroides spp. and Lactobacillus spp., are not susceptible to trimethoprim concentrations obtained with the recommended dosage.
| Bacteria | Trimethoprim |
| MIC mcg/mL (Range) | |
| Escherichia coli | 0.05-1.5 |
| Proteus mirabilis | 0.5-1.5 |
| Klebsiella pneumoniae | 0.5-5.0 |
| Enterobacter species | 0.5-5.0 |
| Staphylococcus species, | 0.15-5.0 |
| coagulase-negative |
Susceptibility Tests: Dilution Techniques: Quantitative methods are used to determine antimicrobial minimal inhibitory concentrations (MICs). These MICs provide estimates of the susceptibility of bacteria to antimicrobial compounds. The MICs should be determined using a standardized procedure. Standardized procedures are based on a dilution method1 (broth or agar) or equivalent with standardized inoculum concentrations and standardized concentrations of trimethoprim powder. The MIC values should be interpreted according to the following criteria:
| MIC (mcg/mL) | Interpretation |
| ≤8 | Susceptible (S) |
| ≥16 | Resistant (R) |
A report of “Susceptible” indicates that the pathogen is likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable. A report of “Intermediate” indicates that the result should be considered equivocal, and, if the microorganism is not fully susceptible to alternative, clinically feasible drugs, the test should be repeated. This category implies possible clinical applicability in body sites where the drug is physiologically concentrated or in situations where high dosage of drug can be used. This category also provides a buffer zone which prevents small uncontrolled technical factors from causing major discrepancies in interpretation. A report of “Resistant” indicates that the pathogen is not likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable; other therapy should be selected.
Standardized susceptibility test procedures require the use of laboratory control microorganisms to control the technical aspects of the laboratory procedures. Standard trimethoprim powder should provide the following MIC values:
| Microorganism | MIC (mcg/mL) |
| S. aureus ATCC 29213 | 1-4 |
| E. faecalis ATCC 29212 | ≤1 |
| E. coli ATCC 25922 | 0.5-2 |
| P. aeruginosa ATCC 27853 | >64 |
Diffusion Techniques: Quantitative methods that require measurement of zone diameters also provide reproducible estimates of the susceptibility of bacteria to antimicrobial compounds. One such standardized procedure2 requires the use of standardized inoculum concentrations. This procedure uses paper disks impregnated with 5 mcg trimethoprim to test the susceptibility of microorganisms to trimethoprim.
Reports from the laboratory providing results of the standard single-disk susceptibility test with a 5 mcg trimethoprim disk should be interpreted according to the following criteria:
| Zone Diameter (mm) | Interpretation |
| ≥16 | Susceptible (S) |
| 11-15 | Intermediate (I) |
| ≤10 | Resistant (R) |
Interpretation should be as stated above for results using dilution techniques. Interpretation involves correlation of the diameter obtained in the disk test with the MIC for trimethoprim.
As with standardized dilution techniques, diffusion methods require the use of laboratory control microorganisms that are used to control the technical aspects of the laboratory procedures. For the diffusion technique, the 5 mcg trimethoprim disk should provide the following zone diameters in these laboratory test quality control strains.
| Microorganism | Zone Diameter (mm) |
| E. coli ATCC 25922 | 21 - 28 mm |
| S. aureus ATCC 25923 | 19 - 26 mm |
INDICATIONS AND USAGE
For the treatment of initial episodes of uncomplicated urinary tract infections due to susceptible strains of the following organisms: Escherichia coli, Proteus mirabilis, Klebsiella pneumoniae, Enterobacter species and coagulase-negative Staphylococcus species, including S. saprophyticus.
Cultures and susceptibility tests should be performed to determine the susceptibility of the bacteria to trimethoprim. Therapy may be initiated prior to obtaining the results of these tests.
CONTRAINDICATIONS
Trimethoprim tablets are contraindicated in individuals hypersensitive to trimethoprim and in those with documented megaloblastic anemia due to folate deficiency.
WARNINGS
Serious hypersensitivity reactions have been reported rarely in patients on trimethoprim therapy. Trimethoprim has been reported rarely to interfere with hematopoiesis, especially when administered in large doses and/or for prolonged periods.
The presence of clinical signs such as sore throat, fever, pallor or purpura may be early indications of serious blood disorders (seeOVERDOSAGE: Chronic). Complete blood counts should be obtained if any of these signs are noted in a patient receiving trimethoprim and the drug discontinued if a significant reduction in the count of any formed blood element is found.
PRECAUTIONS
General
Trimethoprim should be given with caution to patients with possible folate deficiency. Folates may be administered concomitantly without interfering with the antibacterial action of trimethoprim. Trimethoprim should also be given with caution to patients with impaired renal or hepatic function (seeCLINICAL PHARMACOLOGY andDOSAGE AND ADMINISTRATION).
Drug Interactions
Trimethoprim may inhibit the hepatic metabolism of phenytoin. Trimethoprim, given at a common clinical dosage, increased the phenytoin half-life by 51% and decreased the phenytoin metabolic clearance rate by 30%. When administering these drugs concurrently, one should be alert for possible excessive phenytoin effect.
Drug/Laboratory Test Interactions
Trimethoprim can interfere with a serum methotrexate assay as determined by the Competitive Binding Protein Technique (CBPA) when a bacterial dihydrofolate reductase is used as the binding protein. No interference occurs, however, if methotrexate is measured by a radioimmunoassay (RIA).
The presence of trimethoprim may also interfere with the Jaffé alkaline picrate reaction assay for creatinine resulting in over estimations of about 10% in the range of normal values.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Long-term studies in animals to evaluate carcinogenic potential have not been conducted with trimethoprim.
Mutagenesis
Trimethoprim was demonstrated to be non-mutagenic in the Ames assay. In studies at two laboratories, no chromosomal damage was detected in cultured Chinese hamster ovary cells at concentrations approximately 500 times human plasma levels; at concentrations approximately 1000 times human plasma levels in these same cells, a low level of chromosomal damage was induced at one of the laboratories. No chromosomal abnormalities were observed in cultured human leukocytes at concentrations of trimethoprim up to 20 times human steady-state plasma levels. No chromosomal effects were detected in peripheral lymphocytes of human subjects receiving 320 mg of trimethoprim in combination with up to 1600 mg of sulfamethoxazole per day for as long as 112 weeks.
Impairment of Fertility
No adverse effects on fertility or general reproductive performance were observed in rats given trimethoprim in oral dosages as high as 70 mg/kg/day for males and 14 mg/kg/day for females.
Pregnancy
Teratogenic Effects
Pregnancy Category C. Trimethoprim has been shown to be teratogenic in the rat when given in doses 40 times the human dose. In some rabbit studies, the overall increase in fetal loss (dead and resorbed and malformed conceptuses) was associated with doses six times the human therapeutic dose.
While there are no large, well-controlled studies on the use of trimethoprim in pregnant women, Brumfitt and Pursell,3 in a retrospective study, reported the outcome of 186 pregnancies during which the mother received either placebo or trimethoprim in combination with sulfamethoxazole. The incidence of congenital abnormalities was 4.5% (3 of 66) in those who received placebo and 3.3% (4 of 120) in those receiving trimethoprim and sulfamethoxazole. There were no abnormalities in the 10 children whose mothers received the drug during the first trimester. In a separate survey, Brumfitt and Pursell also found no congenital abnormalities in 35 children whose mothers had received trimethoprim and sulfamethoxazole at the time of conception or shortly thereafter.
Because trimethoprim may interfere with folic acid metabolism, trimethoprim should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
ADVERSE REACTIONS
The adverse effects encountered most often with trimethoprim were rash and pruritus.
Dermatologic
Rash, pruritus, and phototoxic skin eruptions. At the recommended dosage regimens of 100 mg b.i.d. or 200 mg q.d. each for 10 days, the incidence of rash is 2.9% to 6.7%. In clinical studies which employed high doses of trimethoprim, an elevated incidence of rash was noted. These rashes were maculopapular, morbilliform, pruritic, and generally mild to moderate, appearing 7 to 14 days after the initiation of therapy.
Hypersensitivity
Rare reports of exfoliative dermatitis, erythema multiforme, Stevens-Johnson syndrome, toxic epidermal necrolysis (Lyell Syndrome), and anaphylaxis have been received.
Gastrointestinal
Epigastric distress, nausea, vomiting, and glossitis. Elevation of serum transaminase and bilirubin has been noted, but the significance of this finding is unknown. Cholestatic jaundice has been rarely reported.
Hematologic
Thrombocytopenia, leukopenia, neutropenia, megaloblastic anemia, and methemoglobinemia.
Metabolic
Hyperkalemia, hyponatremia.
Neurologic
Aseptic meningitis has been rarely reported.
Miscellaneous
Fever, and increases in BUN and serum creatinine levels.
OVERDOSAGE
Acute
Signs of acute overdosage with trimethoprim may appear following ingestion of 1 gram or more of the drug and include nausea, vomiting, dizziness, headaches, mental depression, confusion and bone marrow depression (seeChronic subsection).
Treatment consists of gastric lavage and general supportive measures. Acidification of the urine will increase renal elimination of trimethoprim. Peritoneal dialysis is not effective and hemodialysis only moderately effective in eliminating the drug.
Chronic
Use of trimethoprim at high doses and/or for extended periods of time may cause bone marrow depression manifested as thrombocytopenia, leukopenia and/or megaloblastic anemia. If signs of bone marrow depression occur, trimethoprim should be discontinued and the patient should be given leucovorin; 5 to 15 mg leucovorin daily has been recommended by some investigators.
DOSAGE AND ADMINISTRATION
The usual oral adult dosage is 100 mg of trimethoprim every 12 hours or 200 mg trimethoprim (two 100 mg tablets) every 24 hours, each for 10 days. The use of trimethoprim in patients with a creatinine clearance of less than 15 mL/min is not recommended. For patients with a creatinine clearance of 15 to 30 mL/min, the dose should be 50 mg every 12 hours.
HOW SUPPLIED
Trimethoprim Tablets USP, 100 mg are scored, oval-shaped, white tablets imprinted “DAN DAN” and “5571” supplied in bottles of 100.
Dispense in a tight, light-resistant container with child-resistant closure.
Store at controlled room temperature 15°-30°C (59°-86°F) in a dry place.
REFERENCES
-
National Committee for Clinical Laboratory Standards. Methods for Dilution Antimicrobial Susceptibility Tests for Bacteria That Grow Aerobically. 3rd ed.: Approved Standard. NCCLS Document M7-A3. Vol. 13. No. 25. Villanova. Pa: NCCLS: 1993.
-
National Committee for Clinical Laboratory Standards. Performance Standards for Antimicrobial Disk Susceptibility Tests. 5th ed.: Approved Standard. NCCLS Document M2-A5. Vol. 13. No. 24. Villanova. Pa: NCCLS: 1993.
-
Brumfitt W, Pursell R. Trimethoprim-sulfamethoxazole in the treatment of bacteriuria in women. J Infect Dis. 1973;128(suppl):S657-S663.
Manufactured by:
DANBURY PHARMACAL, INC.
Danbury, CT 06810
Rev: April 2000
| TRIMETHOPRIM
trimethoprim tablet |
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
| Labeler - Watson Labs |