FLURANDRENOLIDE- flurandrenolide lotion
Taro Pharmaceuticals U.S.A., Inc.
----------
Flurandrenolide
Lotion, USP, 0.05%
DESCRIPTION
Flurandrenolide, USP is a potent corticosteroid intended for topical use. Flurandrenolide occurs as white to off-white, fluffy, crystalline powder and is odorless. Flurandrenolide is practically insoluble in water and in ether. One g dissolves in 72 mL of alcohol and in 10 mL of chloroform. The molecular weight of flurandrenolide is 436.52.
The chemical name of flurandrenolide is Pregn-4-ene-3,20-dione, 6-fluoro-11,21-dihydroxy-16,17-[(1-methylethylidene)bis (oxy)]-, (6α, 11β, 16α)-; its empirical formula is C24H33FO6. The structure is as follows:
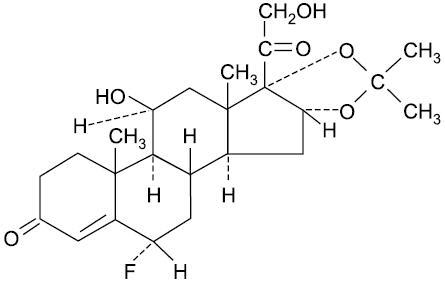
Each mL of flurandrenolide lotion contains 0.5 mg (1.145 µmol) (0.05%) flurandrenolide in an oil-in-water emulsion base composed of glycerin, cetyl alcohol, stearic acid, glyceryl monostearate, mineral oil, polyoxyl 40 stearate, menthol, benzyl alcohol, and purified water.
CLINICAL PHARMACOLOGY
Flurandrenolide lotion is primarily effective because of its anti-inflammatory, antipruritic, and vasoconstrictive actions.
The mechanism of the anti-inflammatory effect of topical corticosteroids is not completely understood. Various laboratory methods, including vasoconstrictor assays, are used to compare and predict potencies and/or clinical efficacies of the topical corticosteroids. There is some evidence to suggest that a recognizable correlation exists between vasoconstrictor potency and therapeutic efficacy in man. Corticosteroids with anti-inflammatory activity may stabilize cellular and lysosomal membranes. There is also the suggestion that the effect on the membranes of lysosomes prevents the release of proteolytic enzymes and, thus, plays a part in reducing inflammation.
Evaporation of water from the lotion vehicle produces a cooling effect, which is often desirable in the treatment of acutely inflamed or weeping lesions.
Pharmacokinetics
The extent of percutaneous absorption of topical corticosteroids is determined by many factors, including the vehicle, the integrity of the epidermal barrier, and the use of occlusive dressings.
Topical corticosteroids can be absorbed from normal intact skin. Inflammation and/or other disease processes in the skin increase percutaneous absorption.
Once absorbed through the skin, topical corticosteroids are handled through pharmacokinetic pathways similar to those of systemically administered corticosteroids. Corticosteroids are bound to plasma proteins in varying degrees. They are metabolized primarily in the liver and then excreted in the kidneys. Some of the topical corticosteroids and their metabolites are also excreted into the bile.
INDICATIONS AND USAGE
Flurandrenolide lotion is indicated for the relief of the inflammatory and pruritic manifestations of corticosteroid-responsive dermatoses.
CONTRAINDICATIONS
Topical corticosteroids are contraindicated in patients with a history of hypersensitivity to any of the components of these preparations.
PRECAUTIONS
General
Systemic absorption of topical corticosteroids has produced reversible hypothalamic-pituitary-adrenal (HPA) axis suppression, manifestations of Cushing's syndrome, hyperglycemia, and glucosuria in some patients.
Conditions that augment systemic absorption include application of the more potent steroids, use over large surface areas, prolonged use, and the addition of occlusive dressings.
Therefore, patients receiving a large dose of a potent topical steroid applied to a large surface area or under an occlusive dressing should be evaluated periodically for evidence of HPA axis suppression using urinary-free cortisol and ACTH stimulation tests. If HPA axis suppression is noted, an attempt should be made to withdraw the drug, to reduce the frequency of application, or to substitute a less potent steroid.
Recovery of HPA axis function is generally prompt and complete on discontinuation of the drug. Infrequently, signs and symptoms of steroid withdrawal may occur, so that supplemental systemic corticosteroids are required.
Pediatric patients may absorb proportionately larger amounts of topical corticosteroids and thus be more susceptible to systemic toxicity (see Pediatric Use under PRECAUTIONS).
If irritation develops, topical corticosteroids should be discontinued and appropriate therapy instituted.
In the presence of dermatologic infections, the use of an appropriate antifungal or antibacterial agent should be instituted. If a favorable response does not occur promptly, flurandrenolide lotion should be discontinued until the infection has been adequately controlled.
Information for the Patient
Patients using topical corticosteroids should receive the following information and instructions:
- This medication is to be used as directed by the physician. It is for external use only. Avoid contact with the eyes.
- Do not use flurandrenolide lotion on the face, underarms, or groin areas unless directed by your physician.
- Patients should be advised not to use this medication for any disorder other than that for which it was prescribed.
- The treated skin area should not be bandaged or otherwise covered or wrapped in order to be occlusive unless the patient is directed to do so by the physician.
- Patients should report any signs of local adverse reactions, especially under occlusive dressing.
- Parents of pediatric patients should be advised not to use tight-fitting diapers or plastic pants on a patient being treated in the diaper area, because these garments may constitute occlusive dressings.
- If no improvement is seen within 2 weeks, contact your physician.
- Do not use other corticosteroid-containing products while using flurandrenolide lotion without first consulting your physician.
Laboratory Tests
The following tests may be helpful in evaluating the HPA axis suppression:
- Urinary-free cortisol test
- ACTH stimulation test
Carcinogenesis, Mutagenesis, and Impairment of Fertility
Long-term animal studies have not been performed to evaluate the carcinogenic potential or the effect on fertility of topical corticosteroids.
Studies to determine mutagenicity with prednisolone and hydrocortisone have revealed negative results.
Usage in Pregnancy
Pregnancy Category C
Corticosteroids are generally teratogenic in laboratory animals when administered systemically at relatively low dosage levels. The more potent corticosteroids have been shown to be teratogenic after dermal application in laboratory animals. There are no adequate and well-controlled studies in pregnant women on teratogenic effects from topically applied corticosteroids. Therefore, topical corticosteroids should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. Drugs of this class should not be used extensively for pregnant patients or in large amounts or for prolonged periods of time.
Nursing Mothers
It is not known whether topical administration of corticosteroids could result in sufficient systemic absorption to produce detectable quantities in breast milk. Systemically administered corticosteroids are secreted into breast milk in quantities not likely to have a deleterious effect on the infant. Nevertheless, caution should be exercised when topical corticosteroids are administered to a nursing woman.
Pediatric Use
Pediatric patients may demonstrate greater susceptibility to topical corticosteroid-induced HPA axis suppression and Cushing's syndrome than do mature patients because of a larger skin surface area to body weight ratio.
Hypothalamic-pituitary-adrenal (HPA) axis suppression, Cushing's syndrome, and intracranial hypertension have been reported in pediatric patients receiving topical corticosteroids. Manifestations of adrenal suppression in pediatric patients include linear growth retardation, delayed weight gain, low plasma cortisol levels, and absence of response to ACTH stimulation. Manifestations of intracranial hypertension include bulging fontanelles, headaches, and bilateral papilledema.
Administration of topical corticosteroids to pediatric patients should be limited to the least amount compatible with an effective therapeutic regimen. Chronic corticosteroid therapy may interfere with the growth and development of pediatric patients.
ADVERSE REACTIONS
The following local adverse reactions are reported infrequently with topical corticosteroids but may occur more frequently with the use of occlusive dressings. These reactions are listed in an approximate decreasing order of occurrence:
- Burning
- Itching
- Irritation
- Dryness
- Folliculitis
- Hypertrichosis
- Acneform eruptions
- Hypopigmentation
- Perioral dermatitis
- Allergic contact dermatitis
The following may occur more frequently with occlusive dressings:
- Maceration of the skin
- Secondary infection
- Skin atrophy
- Striae
- Miliaria
Postmarketing Adverse Reactions
The following adverse reactions have been identified during post approval use of flurandrenolide lotion. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Skin: skin striae, hypersensitivity, skin atrophy, contact dermatitis, and skin discoloration.
OVERDOSAGE
Topically applied corticosteroids can be absorbed in sufficient amounts to produce systemic effects (see PRECAUTIONS).
DOSAGE AND ADMINISTRATION
Shake well before using. A small quantity of flurandrenolide lotion should be rubbed gently into the affected area 2 or 3 times daily.
Therapy should be discontinued when control is achieved. If no improvement is seen within 2 weeks, reassessment of the diagnosis may be necessary.
Flurandrenolide lotion should not be used with occlusive dressings unless directed by a physician. Tight-fitting diapers or plastic pants may constitute occlusive dressings.
HOW SUPPLIED
Flurandrenolide Lotion, USP, 0.05% is supplied in a plastic squeeze bottle as follows: 120 mL (NDC 51672-5298-8)
Keep out of reach of children.
| FLURANDRENOLIDE
flurandrenolide lotion |
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
| Labeler - Taro Pharmaceuticals U.S.A., Inc. (145186370) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| DPT Laboratories, Ltd. | 832224526 | MANUFACTURE(51672-5298) | |