BIDIL- hydralazine hydrochloride and isosorbide dinitrate tablet, film coated
Arbor Pharmaceuticals
----------
BiDil®
(isosorbide dinitrate and hydralazine hydrochloride)
Tablets
DESCRIPTION
BiDil is a fixed-dose combination of isosorbide dinitrate, a vasodilator with effects on both arteries and veins, and hydralazine hydrochloride, a predominantly arterial vasodilator.
Isosorbide dinitrate is described chemically as 1,4:3,6-dianhydro-d-glucitol-2,5-dinitrate and its structural formula is:
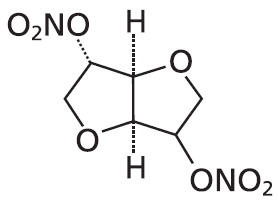
Isosorbide dinitrate is a white to off-white, crystalline powder with the empirical formula C6H8N2O8 and a molecular weight of 236.14. It is freely soluble in organic solvents such as alcohol, chloroform and ether, but is only sparingly soluble in water.
Hydralazine hydrochloride is described chemically as 1-hydrazinophthalazine monohydrochloride, and its structural formula is:
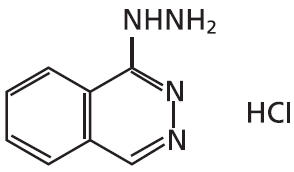
Hydralazine HCl is a white to off-white, crystalline powder with the empirical formula C8H8N4•HCl and a molecular weight of 196.64. It is soluble in water, slightly soluble in alcohol, and very slightly soluble in ether.
Each BiDil Tablet for oral administration contains 20 mg of isosorbide dinitrate and 37.5 mg of hydralazine hydrochloride.
The inactive ingredients in BiDil tablets include: anhydrous lactose, microcrystalline cellulose, sodium starch glycolate, colloidal silicon dioxide, magnesium stearate, hypromellose, FD&C Yellow No.6 aluminum lake, polyethylene glycol, titanium dioxide, polysorbate 80.
CLINICAL PHARMACOLOGY
Mechanism of Action
The mechanism of action underlying the beneficial effects of BiDil in the treatment of heart failure has not been established.
Isosorbide dinitrate is a vasodilator affecting both arteries and veins. Its dilator properties result from the release of nitric oxide and the subsequent activation of guanylyl cyclase, and ultimate relaxation of vascular smooth muscle.
Several well-controlled clinical trials have used exercise testing to assess the anti-anginal efficacy of chronically-delivered nitrates. In the large majority of these trials, active agents were no more effective than placebo after 24 hours (or less) of continuous therapy. Attempts to overcome nitrate tolerance by dose escalation, even to doses far in excess of those used acutely, have consistently failed. Only after nitrates have been absent from the body for several hours has response to nitrates been restored.
Hydralazine is a selective dilator of arterial smooth muscle. Animal data suggests that hydralazine may also mitigate tolerance to nitrates.
Pharmacokinetics
Hydralazine
Absorption and Distribution
About 2/3 of a 50-mg dose of 14C-hydralazine HCl given in gelatin capsules was absorbed in hypertensive subjects. In patients with heart failure, mean absolute bioavailability of a single oral dose of hydralazine 75 mg varies from 10 to 26%, with the higher percentages in slow acetylators (See Metabolism and Elimination). Administration of doses escalating from 75 mg to 1000 mg tid to congestive heart failure patients resulted in an up to 9-fold increase in the dose normalized AUC, indicating non-linear kinetics of hydralazine, probably reflecting saturable first pass metabolism.
After intravenous administration of hydralazine in a dose of 0.3 mg/kg, the steady-state volume of distribution in patients with congestive heart failure was 2.2 L/kg.
Metabolism and Elimination
Metabolism is the main route for the elimination of hydralazine. Negligible amounts of unchanged hydralazine are excreted in urine. Hydralazine is metabolized by acetylation, ring oxidation and conjugation with endogenous compounds including pyruvic acid. Acetylation occurs predominantly during the first pass after oral administration which explains the dependence of the absolute bioavailability on the acetylator phenotype. About 50% of patients are fast acetylators and have lower exposure.
After oral administration of hydralazine, the major circulating metabolites are hydralazine pyruvate hydrazone and methyl-triazolophthalazine. Hydralazine is the main pharmacologically active entity; hydralazine pyruvate hydrazone has only minimal hypotensive and tachycardic activity. The pharmacological activity of methyltriazolophthalazine has not been determined. The major identified metabolite of hydralazine excreted in urine is acetylhydrazinophthalazinone.
Isosorbide Dinitrate
Absorption and Distribution
Absorption of isosorbide dinitrate from tablets after oral dosing is nearly complete. The average bioavailability of isosorbide dinitrate is about 25%, but is highly variable (10%-90%) due to first-pass metabolism and increases progressively during chronic therapy. Serum concentrations reach their maximum about one hour after ingestion.
The volume of distribution of isosorbide dinitrate is 2 to 4 L/kg. About 28% of circulating isosorbide dinitrate is protein bound.
Under steady-state conditions, isosorbide dinitrate accumulates significantly in muscle (pectoral) and vein (saphenous) wall relative to simultaneous plasma concentrations.
Metabolism and Elimination
Isosorbide dinitrate undergoes extensive first-pass metabolism in the liver and is cleared at a rate of 2 to 4 L/minute with a serum half-life of about 1 hour. Isosorbide dinitrate's clearance is primarily by denitration to the 2-mononitrate (15 to 25%) and the 5-mononitrate (75 to 85%). Both metabolites have biological activity, especially the 5-mononitrate which has an overall half-life of about 5 hours. The 5-mononitrate is cleared by denitration to isosorbide, glucuronidation to the 5-mononitrate glucuronides, and by denitration/hydration to sorbitol. The 2-mononitrate appears to participate in the same metabolic pathways with a half-life of about 2 hours.
Most isosorbide dinitrate is eliminated renally as conjugated metabolites.
BiDil
Absorption and Bioavailability
Following a single 75-mg oral dose of hydralazine plus 40 mg of isosorbide dinitrate to 19 healthy adults, peak plasma concentrations of hydralazine (88 ng/mL/65 kg) and isosorbide dinitrate (76 ng/mL/65 kg) were reached in 1 hour. The half-lives were about 4 hours for hydralazine and about 2 hours for isosorbide dinitrate. Peak plasma concentrations of the two active metabolites, isosorbide-2-mononitrate and isosorbide-5-mononitrate, were 98 and 364 ng/mL/65 kg, respectively, at about 2 hours. No information is currently available regarding the effect of food on the bioavailability of hydralazine or isosorbide dinitrate from BiDil tablets.
Special Populations
Pediatric
The pharmacokinetics of hydralazine and isosorbide dinitrate, alone or in combination, have not been determined in patients below the age of 18 years.
Geriatric
The pharmacokinetics of hydralazine and isosorbide dinitrate, alone or in combination, have not been determined in patients over 65 years of age.
Renal Impairment
The effect of renal impairment on the pharmacokinetics of hydralazine has not been determined. In a study with 49 hypertensive patients on chronic therapy with hydralazine in daily doses of 25-200 mg, the daily dose of hydralazine in 19 subjects with severely impaired renal function (creatinine clearance 5-28 mL/min) and in 17 subjects with normal renal function (creatinine clearance >100 mL/min) was not different, suggesting no need for dose adjustment in patients with renal impairment. The dialyzability of hydralazine has not been determined. In three studies, renal insufficiency did not affect the pharmacokinetics of isosorbide dinitrate. Dialysis is not an effective method for removing isosorbide dinitrate or its metabolite isosorbide-5-mononitrate from the body.
Hepatic Impairment
The effect of hepatic impairment on the pharmacokinetics of hydralazine alone has not been determined. Isosorbide dinitrate concentrations increase in patients with cirrhosis. There are no studies of hepatic impairment using BiDil.
Gender
There are no studies of gender-dependent effects with hydralazine. In a single dose study with isosorbide dinitrate, no gender-dependent differences in the pharmacokinetics of isosorbide dinitrate and its mononitrate metabolites were found.
No pharmacokinetic studies in special populations were conducted with BiDil.
Pharmacokinetic Drug-Drug Interactions
Hydralazine
Administration of hydralazine can increase the exposure to a number of drugs including beta blockers.
In healthy males administered a single oral dose of hydralazine 50 mg and propranolol 1 mg/kg, the Cmax and AUC for propranolol increased by about 143% and 77%, respectively. In healthy subjects administered a single oral dose of hydralazine 50 mg and metoprolol 100 mg, the Cmax and AUC for metoprolol increased by about 50% and 30%, respectively. In pre-eclamptic women, multiple doses of hydralazine 25 mg bid and metoprolol 50 mg bid increased the Cmax and AUC for metoprolol by 88% and 38%, respectively.
In healthy males administered single oral doses of hydralazine 25 mg and either lisinopril 20 mg or enalapril 20 mg, Cmax and AUC for lisinopril were each increased by about 30%, but enalapril concentrations were unaffected.
Intravenous co-administration of 0.2 mg/kg hydralazine HCl and 40 mg furosemide in Japanese patients with congestive heart failure resulted in a 21% increase in the clearance of furosemide.
Isosorbide Dinitrate
A single dose of 20 mg of isosorbide dinitrate was administered to healthy subjects after pretreatment with 80 mg propranolol tid for 48 hours, resulting in no impact on the pharmacokinetics of isosorbide dinitrate and isosorbide 5-mononitrate.
When single 100-mg oral doses of atenolol were administered 2 hours before isosorbide dinitrate at a 10-mg dose no differences in the pharmacokinetics of isosorbide dinitrate or its mononitrates were observed.
The vasodilating effects of coadministered isosorbide dinitrate may be additive to those of other vasodilators, especially alcohol when administered concomitantly with isosorbide dinitrate.
Pharmacodynamics
The basis for the beneficial clinical effects of BiDil is not known. In a small study of patients with chronic heart failure administered single doses of hydralazine 75 mg, isosorbide dinitrate 20 mg, and the combination, the combination elicited a statistically significant decrease in pulmonary capillary wedge pressure compared to hydralazine alone. The increase in cardiac output, renal blood flow and limb blood flow with the combination, however, was not greater than with hydralazine alone. There is no study of hemodynamic effects following multiple dosing.
Clinical Trials
BiDil or a combination of isosorbide dinitrate and hydralazine hydrochloride was studied in two placebo-controlled clinical trials in 1,692 patients with mild to severe heart failure (mostly NYHA class II and III) and one active control trial (vs. enalapril) in 804 patients.
In the multicenter trial V-HeFT I, the combination of hydralazine and isosorbide dinitrate 75 mg/40 mg qid (n=186) was compared to placebo (n=273) in men with impaired cardiac function and reduced exercise tolerance (primarily NYHA class II and III), and on therapy with digitalis glycosides and diuretics. There was no overall significant difference in mortality between the two treatment groups. There was, however, a trend favoring hydralazine and isosorbide dinitrate, which on retrospective analysis, was attributable to an effect in blacks (n=128). Survival in white patients (n=324) was similar on placebo and the combination treatment.
In a second study of mortality, V-HeFT II, the combination of hydralazine and isosorbide dinitrate 75 mg/40 mg qid was compared to enalapril in 804 men with impaired cardiac function and reduced exercise tolerance (NYHA class II and III), and on therapy with digitalis glycosides and diuretics. The combination of hydralazine and isosorbide dinitrate was inferior to enalapril overall, but retrospective analysis showed that the difference was observed in the white population (n=574); there was essentially no difference in the black population (n=215).
Based on these retrospective analyses suggesting an effect on survival in black patients, but showing little evidence of an effect in the white population, a third study was conducted among black patients with heart failure.
The A-HeFT trial evaluated BiDil vs. placebo among 1,050 self-identified black patients (over 95% NYHA class III) at 169 centers in the United States. All patients had stable symptomatic heart failure. Patients were required to have LVEF ≤ 35% or left ventricular internal diastolic dimension > 2.9 cm/m2 plus LVEF < 45%. Patients were maintained on stable background therapy and randomized to BiDil (n=518) or placebo (n=532). BiDil was initiated at 20 mg isosorbide dinitrate/37.5 mg hydralazine hydrochloride three times daily and titrated to a target dose of 40/75 mg three times daily or to the maximum tolerated dose. Patients were treated for up to 18 months.
The randomized population was 60% male, 1% NYHA class II, 95% NYHA class III and 4% NYHA class IV, with a mean age of 57 years, and was generally treated with standard treatments for heart failure including diuretics (94%, almost all loop diuretics), beta-blockers (87%), angiotensin converting enzyme inhibitors (ACE-I; 78%), angiotensin II receptor blockers (ARBs; 28%), either ACE-I or ARB (93%), digitalis glycosides (62%) and aldosterone antagonists (39%).
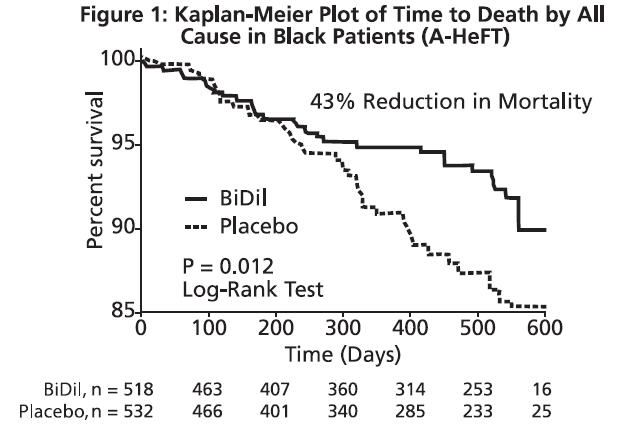
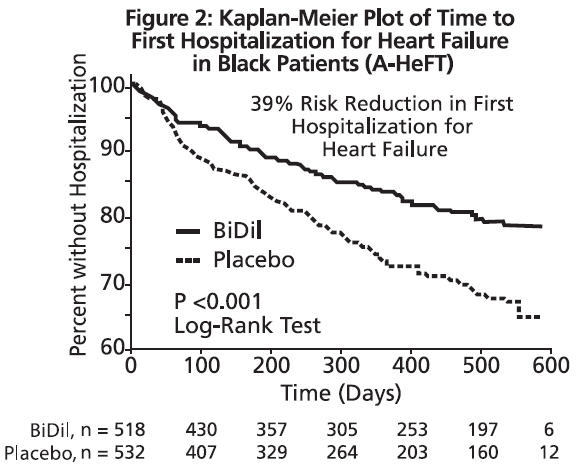
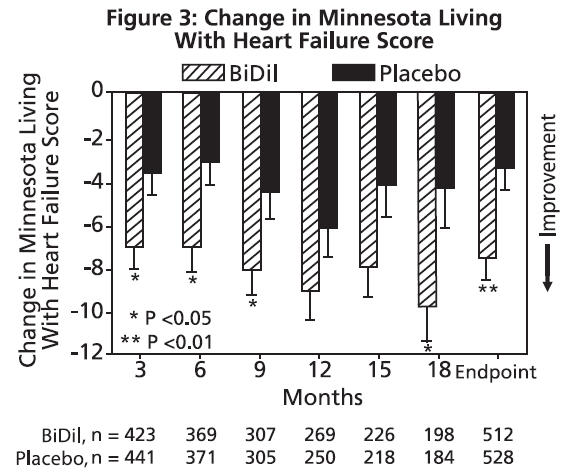
The primary end point was a composite score consisting of all-cause mortality, first hospitalization for heart failure, and responses to the Minnesota Living with Heart Failure questionnaire, with the individual components of the composite examined as separate endpoints. The trial was terminated early, at a mean follow-up of 12 months, primarily because of a statistically significant 43% reduction in all-cause mortality in the BiDil-treated group (p=0.012; see Table 1 and Figure 1). The primary endpoint was also statistically in favor of BiDil (p ≤ 0.021). The BiDil-treated group also showed a 39% reduction in the risk of a first hospitalization for heart failure (p<0.001; see Table 1 and Figure 2) and had statistically significant improvement in response to the Minnesota Living with Heart Failure questionnaire, a self-report of the patient's functional status, at most time points (see Figure 3). Patients in both treatment groups had mean baseline questionnaire scores of 51 (out of a possible 105).
| End point | BiDil®
N=518 | Placebo N=532 | Hazard Ratio (95% CI) | Risk Reduction with BiDil | P-value |
|---|---|---|---|---|---|
| Composite score | -0.16±1.93 | -0.47± 2.04 | N/A | N/A | ≤ 0.021 |
| All-cause mortality | 6.2% | 10.2% | 0.57 (0.37, 0.89) | 43% | 0.012 |
| First hospitalization for heart failure | 16.4% | 24.4% | 0.61 (0.46, 0.80) | 39% | <0.001 |
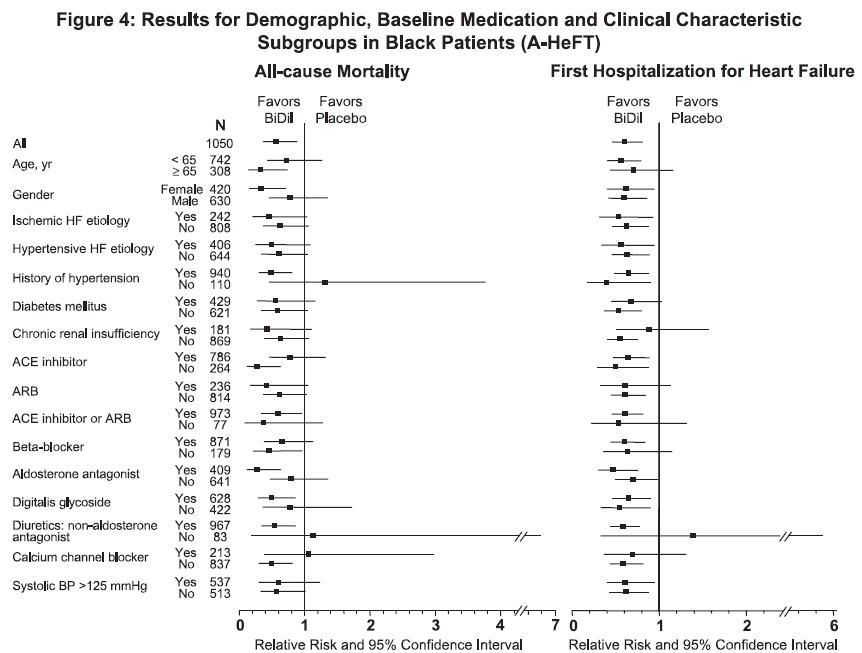
Effects on survival and hospitalization for heart failure were similar in subgroups by age, gender, baseline disease, and use of concomitant medications, as shown in Figure 4.
Patients treated with BiDil in the A-HeFT study had randomly measured blood pressures on average 3/3 mmHg lower than did patients on placebo. The contribution of the difference in blood pressure to the overall outcome difference is unknown. Whether both hydralazine and isosorbide dinitrate contribute to the overall outcome difference has not been studied in outcome trials. Isosorbide dinitrate and hydralazine have not been systematically studied for the treatment of heart failure as separate agents, and neither drug is indicated for heart failure.
INDICATIONS AND USAGE
BiDil is indicated for the treatment of heart failure as an adjunct to standard therapy in self-identified black patients to improve survival, to prolong time to hospitalization for heart failure, and to improve patient-reported functional status. There is little experience in patients with NYHA class IV heart failure. Most patients in the clinical trial supporting effectiveness (A-HeFT) received a loop diuretic, an angiotensin converting enzyme inhibitor or an angiotensin II receptor blocker, and a beta blocker, and many also received a cardiac glycoside or an aldosterone antagonist.
WARNINGS
Augmentation of the vasodilatory effects of isosorbide dinitrate by phosphodiesterase inhibitors such as sildenafil, vardenafil, or tadalafil could result in severe hypotension. The time course and dose dependence of this interaction have not been studied. Reasonable supportive care should consist of those measures used to treat a nitrate overdose with elevation of the extremities and central volume expansion.
PRECAUTIONS
General
The precautions that need to be taken when using BiDil are those appropriate to each of its components.
Treatment with hydralazine hydrochloride may produce a clinical picture simulating systemic lupus erythematosus including glomerulonephritis.
If systemic lupus erythematosus-like symptoms occur in patients treated with BiDil, discontinuation of BiDil should be considered only after a thorough benefit-to-risk assessment. Symptoms and signs of systemic lupus erythematosus usually regress when hydralazine hydrochloride is discontinued but residua have been detected many years later. Long-term treatment with steroids may be necessary. (See PRECAUTIONS. Laboratory Tests.)
Symptomatic hypotension, particularly with upright posture, may occur with even small doses of BiDil. Therefore, BiDil should be used with caution in patients who may be volume depleted or who, for whatever reason, are already hypotensive.
Hydralazine hydrochloride can cause tachycardia potentially leading to myocardial ischemia and anginal attacks.
Careful clinical and hemodynamic monitoring is recommended when BiDil is administered to patients with acute myocardial infarction to avoid the hazards of hypotension and tachycardia.
Hydralazine hydrochloride has been associated with peripheral neuritis, evidenced by paresthesia, numbness, and tingling, which may be related to an antipyridoxine effect. Pyridoxine should be added to BiDil therapy if such symptoms develop.
Isosorbide dinitrate therapy may aggravate angina associated with hypertrophic cardiomyopathy.
Information for Patients
Patients should be informed of possible side effects and advised to take the medication regularly and continuously as directed.
Patients should be told that headaches often accompany treatment with BiDil, especially during initiation of treatment. Headaches tend to subside even with continued dosing. Patients should be instructed to consult a physician to adjust the dose of BiDil if headache continues with repeated dosing. Treatment of emerging headache was managed with acetaminophen in some clinical trial patients.
Treatment with BiDil may be associated with lightheadedness on standing, especially after rising from a recumbent or seated position.
Patients should be cautioned that inadequate fluid intake or excessive fluid loss from perspiration, diarrhea or vomiting may lead to an excessive fall in blood pressure and cause lightheadedness or even syncope. If syncope does occur, BiDil should be discontinued, and the prescribing physician should be notified as soon as possible.
Patients should be cautioned about the increased risk of hypotension especially if they are taking antihypertensive drugs concomitantly.
Patients should be cautioned against concomitant use of BiDil with phosphodiesterase-5 inhibitor drugs used for the treatment for erectile dysfunction or pulmonary hypertension such as sildenafil citrate (Viagra®; Revatio™), vardenafil (Levitra®) or tadalafil (Cialis®). Use of BiDil may produce an extreme drop in blood pressure that may result in fainting or may provoke chest pain or a heart attack.
Laboratory Tests
If symptoms suggestive of systemic lupus erythematosus occur, such as arthralgia, fever, chest pain, prolonged malaise, or other unexplained signs or symptoms, complete blood counts and antinuclear antibody titer determinations should be performed. A positive antinuclear antibody titer requires that the physician carefully weigh the benefits and risks of continued therapy with BiDil.
Drug/Drug Interactions
Due to the hydralazine component of BiDil, monoamine-oxidase inhibitors should be used with caution in patients receiving BiDil.
Patients treated with BiDil who receive any potent parenteral antihypertensive agent should be continuously observed for several hours for excessive fall in blood pressure.
The effects of BiDil on vasodilators including alcohol may be additive.
Sildenafil: See WARNINGS.
Vardenafil: See WARNINGS.
Tadalafil: See WARNINGS.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Hydralazine Hydrochloride
An increased incidence of lung tumors (adenomas and adenocarcinomas) was observed in a lifetime study in Swiss albino mice given hydralazine hydrochloride continuously in their drinking water at a dosage of about 250 mg/kg per day (6 times the MRHD provided by BiDil on a body surface area basis). In a 2-year carcinogenicity study of rats given hydralazine hydrochloride by gavage at dose levels of 15, 30, and 60 mg/kg/day (up to 3 times the MRHD of BiDil on a body surface area basis), microscopic examination of the liver revealed a small, but statistically significant increase in benign neoplastic nodules in males (high-dosage) and females (both high and intermediate dosage groups). Benign interstitial cell tumors of the testes were also significantly increased in the high-dose group.
Hydralazine hydrochloride is mutagenic in bacterial systems, and is positive in rat and rabbit hepatocyte DNA repair studies in vitro. Additional in vivo and in vitro studies using lymphoma cells, germinal cells, fibroblasts from mice, bone marrow cells from Chinese hamsters and fibroblasts from human cell lines did not demonstrate any mutagenic or clastogenic potential for hydralazine hydrochloride.
Isosorbide Dinitrate
No long-term animal studies have been performed to evaluate the mutagenic or carcinogenic potential of isosorbide dinitrate. A modified two-litter reproduction study among rats fed isosorbide dinitrate at 25 or 100 mg/kg/day (up to 9 times the Maximum Recommended Human Dose of BiDil on a body surface area basis) revealed no evidence of altered fertility or gestation.
Pregnancy Category C
Isosorbide dinitrate has been shown to cause a dose-related increase in embryo-toxicity (excess mummified pups) in rabbits at 70 mg/kg (12 times the MRHD of BiDil on a body surface area basis). Hydralazine hydrochloride is teratogenic in mice at 66 mg/kg and possibly in rabbits at 33 mg/kg (2 and 3 times the MRHD of BiDil on a body surface area basis). There are no animal studies assessing the teratogenicity of BiDil.
A meta-analysis of randomized controlled trials comparing hydralazine hydrochloride with other antihypertensive agents for severe hypertension in pregnancy found that hydralazine hydrochloride was associated with significantly more maternal hypotension, placental abruption, caesarean sections and oliguria, with more adverse effects on fetal heart rate and with lower Apgar scores.
A combination of propranolol and hydralazine hydrochloride was administered to 13 patients with long-standing hypertension during 15 pregnancies. These pregnancies resulted in 14 live births and one unexplained stillbirth. The only neonatal complications were two cases of mild hypoglycemia. Hydralazine hydrochloride and its metabolites have been detected using a non-selective assay in maternal and umbilical plasma in patients treated with the drug during pregnancy.
Isosorbide dinitrate has been used for effective acute and sub-chronic control of hypertension in pregnant women, but there are no studies using it in a chronic regimen and assessing its effects on pregnant women and/or the fetus.
There are no studies using BiDil in pregnant women. Therefore, BiDil should be used with caution during pregnancy and only if the potential benefit justifies the potential risk to the fetus.
Nursing mothers
The possible excretion of hydralazine in breast milk has not been determined. It is also not known whether isosorbide dinitrate is excreted in human milk. No studies have been performed with BiDil. Caution should be exercised when BiDil is administered to a nursing woman.
Geriatric use
Clinical studies of BiDil did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in response between elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic and renal function, and of concomitant disease or other drug therapies.
Isosorbide dinitrate, its active metabolites, and hydralazine may be eliminated more slowly in elderly patients.
ADVERSE REACTIONS
To report SUSPECTED ADVERSE REACTIONS, contact NitroMed, Inc. at 1-888-692-4345 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
BiDil
BiDil has been evaluated for safety in 517 heart failure patients in A-HeFT. A total of 317 of these patients received BiDil for at least 6 months, and 220 received BiDil for at least 12 months. In A-HeFT, 21% of the patients discontinued BiDil for adverse experiences compared to 12% who discontinued placebo. Overall, adverse events were more common in BiDil-treated than in placebo-treated patients. Table 2 lists adverse events reported with an incidence of ≥ 2% in patients treated with BiDil in A-HeFT, and, after rounding to the nearest 1%, occurring more frequently than in the placebo group, regardless of causality. Headache and dizziness were the two most frequent adverse events and were more than twice as frequent in the BiDil group. The most common reasons for discontinuing BiDil in the A-HeFT trial were headache (7%) and dizziness (4%).
| BiDil (N=517) (% of patients) | Placebo (N=527) (% of patients) |
|
|---|---|---|
| Headache | 50 | 21 |
| Dizziness | 32 | 14 |
| Chest pain | 16 | 15 |
| Asthenia | 14 | 11 |
| Nausea | 10 | 6 |
| Bronchitis | 8 | 7 |
| Hypotension | 8 | 4 |
| Sinusitis | 4 | 2 |
| Ventricular tachycardia | 4 | 2 |
| Palpitations | 4 | 3 |
| Hyperglycemia | 4 | 3 |
| Rhinitis | 4 | 3 |
| Paresthesia | 4 | 2 |
| Vomiting | 4 | 2 |
| Amblyopia | 3 | 1 |
| Hyperlipidemia | 3 | 2 |
| Tachycardia | 2 | 1 |
The following adverse events were reported in A-HeFT in at least 1% but less than 2% of patients treated with BiDil, and also occurred in at least 0.5% more patients than in placebo-treated patients; all such events are included unless they are too non-specific to be meaningful or appear to reflect underlying disease.
Body as a Whole: Allergic reaction, malaise.
Central nervous system: Somnolence.
Gastrointestinal: Cholecystitis.
Metabolic: Hypercholesteremia.
Musculoskeletal: Arthralgia, myalgia, tendon disorder.
Skin: Alopecia, angioedema, sweating.
In the V-HeFT I and II studies, a total of 587 patients with heart failure were treated with the combination of isosorbide dinitrate and hydralazine hydrochloride. The type, pattern, frequency and severity of adverse experiences reported in these studies were similar to those reported in A-HeFT, and no unusual adverse experiences were reported.
Prior experience with BiDil components
The following additional adverse events have been reported with hydralazine hydrochloride or isosorbide dinitrate but not necessarily with BiDil:
Digestive: paralytic ileus.
Cardiovascular: paradoxical pressor response, crescendo angina.
Neurologic: peripheral neuritis, numbness, tingling, muscle cramps, psychotic reactions, disorientation.
Genitourinary: difficulty in urination.
Hematologic: blood dyscrasias, agranulocytosis, purpura, splenomegaly.
Hypersensitive Reactions: eosinophilia, hepatitis.
Other: nasal congestion, flushing, lacrimation, conjunctivitis.
OVERDOSAGE
There are no documented cases of overdosage with BiDil. The signs and symptoms of overdosage with BiDil are expected to be those of excessive pharmacologic effect and those that may occur with overdosage of either isosorbide dinitrate or hydralazine hydrochloride administered alone.
Signs and Symptoms
The signs and symptoms of overdosage with BiDil are expected to be those of excessive pharmacologic effect, i.e., vasodilatation, reduced cardiac output and hypotension, and signs and symptoms include headache, confusion, tachycardia and generalized skin flushing. Complications can include myocardial ischemia and subsequent myocardial infarction, cardiac arrhythmia, and profound shock. Syncope, coma and death may ensue without appropriate treatment.
Treatment
There is no specific antidote.
Support of the cardiovascular system is of primary importance. Shock should be treated with plasma expanders, vasopressors, and positive inotropic agents. The gastric contents should be evacuated, taking adequate precautions to prevent aspiration. These manipulations have to be carried out after cardiovascular status has been stabilized, since they might precipitate cardiac arrhythmias or increase the depth of shock.
In patients with renal disease or congestive heart failure, therapy resulting in central volume expansion is not without hazard. Treatment of isosorbide dinitrate overdose in these patients may be difficult, and invasive monitoring may be required.
No data are available to suggest physiological maneuvers (e.g., maneuvers to change the pH of the urine) that might accelerate elimination of the components of BiDil. Dialysis is not effective in removing circulating isosorbide dinitrate. The dialyzability of hydralazine has not been determined.
Methemoglobinemia
Nitrate ions liberated during metabolism of isosorbide dinitrate can oxidize hemoglobin into methemoglobin.
There are case reports of significant methemoglobinemia in association with moderate overdoses of organic nitrates.
Methemoglobin levels are measurable by most clinical laboratories.
Methemoglobinemia could be serious in chronic heart failure patients because of already compromised vascular bed-tissue gas exchange dynamics. Classically, methemoglobinemic blood is described as chocolate brown, without color change on exposure to air.
When methemoglobinemia is diagnosed, the treatment of choice is methylene blue, 1 to 2 mg/kg intravenously.
DOSAGE AND ADMINISTRATION
Treatment with BiDil should be initiated at a dose of one BiDil Tablet, 3 times a day. BiDil may be titrated to a maximum tolerated dose, not to exceed two BiDil Tablets, 3 times a day.
There is no adequate experience in heart failure with doses of BiDil other than those recommended and no experience with use of individual components.
Although titration of BiDil can be rapid (3-5 days), some patients may experience side effects and may take longer to reach their maximum tolerated dose. The dosage may be decreased to as little as one-half BiDil Tablet 3 times a day if intolerable side effects occur. Efforts should be made to titrate up as soon as side effects subside.
HOW SUPPLIED
BiDil Tablets contain 20 mg of isosorbide dinitrate plus 37.5 mg of hydralazine hydrochloride. They are biconvex, approximately 8 mm in diameter, scored, film-coated, orange tablets debossed "20" on one side over the score and "N" on the other side.
NDC 12948-001-01 bottle of 12.
NDC 12948-001-12 bottle of 180.
| BIDIL
hydralazine hydrochloride and isosorbide dinitrate tablet, film coated |
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
| Labeler - Arbor Pharmaceuticals (781796417) |