FULL PRESCRIBING INFORMATION
WARNING: RISK OF SERIOUS CARDIOVASCULAR AND GASTROINTESTINAL EVENTS
Cardiovascular Thrombotic Events
- Non-Steroidal Anti-inflammatory Drugs (NSAIDs), a component of VIMOVO, cause an increased risk of serious cardiovascular thrombotic events, including myocardial infarction and stroke, which can be fatal. This risk may occur early in treatment and may increase with duration of use [see Warnings and Precautions (5.1)].
- VIMOVO is contraindicated in the setting of coronary artery bypass graft (CABG) surgery [see Contraindications (4), and Warnings and Precautions (5.1)].
Gastrointestinal Bleeding, Ulceration, and Perforation
- NSAIDs, a component of VIMOVO cause an increased risk of serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients and patients with a prior history of peptic ulcer disease and/or GI bleeding are at greater risk for serious GI events [see Warnings and Precautions (5.2)].
1 INDICATIONS AND USAGE
VIMOVO, a combination of naproxen and esomeprazole magnesium, is indicated in adult and adolescent patients 12 years of age and older weighing at least 38 kg, requiring naproxen for symptomatic relief of arthritis and esomeprazole magnesium to decrease the risk for developing naproxen-associated gastric ulcers.
The naproxen component of VIMOVO is indicated for relief of signs and symptoms of:
- osteoarthritis, rheumatoid arthritis and ankylosing spondylitis in adults.
- juvenile idiopathic arthritis (JIA) in adolescent patients.
The esomeprazole magnesium component of VIMOVO is indicated to decrease the risk of developing naproxen-associated gastric ulcers.
Limitations of Use:
- Do not substitute VIMOVO with the single-ingredient products of naproxen and esomeprazole magnesium.
- VIMOVO is not recommended for initial treatment of acute pain because the absorption of naproxen is delayed compared to absorption from other naproxen-containing products.
- Controlled studies do not extend beyond 6 months [see Use in Specific Populations (8.4), Clinical Studies (14)].
2 DOSAGE AND ADMINISTRATION
2.1 Important Administration Instructions
- Use the lowest naproxen dose for the shortest duration consistent with individual patient treatment goals [see Warnings and Precautions (5.1)].
- Carefully consider the potential benefits and risks of VIMOVO and other treatment options before deciding to use VIMOVO.
- VIMOVO does not allow for administration of a lower daily dose of esomeprazole magnesium. If a total daily dose of less than 40 mg esomeprazole is more appropriate, a different treatment should be considered.
- Swallow VIMOVO tablets whole with liquid. Do not split, chew, crush or dissolve the tablet. Take VIMOVO at least 30 minutes before meals.
- Patients should be instructed that if a dose is missed, it should be taken as soon as possible. However, if the next scheduled dose is due, the patient should not take the missed dose, and should be instructed to take the next dose on time. Patients should be instructed not to take 2 doses at one time to make up for a missed dose.
- Antacids may be used while taking VIMOVO.
2.2 Recommended Dosage
The recommended dosage of VIMOVO by indication is shown in the table:
| Indication | Patient Population | Recommended Dosage |
|---|---|---|
| Rheumatoid Arthritis, Osteoarthritis, and Ankylosing Spondylitis | Adults | One VIMOVO tablet twice daily of either: 375 mg naproxen/20 mg of esomeprazole; or 500 mg naproxen/20 mg of esomeprazole |
| Juvenile Idiopathic Arthritis in Adolescent Patients 12 Years of Age and Older and Weighing at Least 38 kg | Greater than 50 kg | |
| 38 kg to less than 50 kg | One VIMOVO tablet twice daily of: 375 mg naproxen/20 mg of esomeprazole |
2.3 Use in Renal Impairment or Hepatic Impairment
Renal Impairment
Naproxen-containing products are not recommended for use in patients with moderate to severe or severe renal impairment (creatinine clearance less than 30 mL/min) [see Warnings and Precautions (5.6), Use in Specific Populations (8.7)].
Hepatic Impairment
Monitor patients with mild to moderate hepatic impairment closely and consider a possible dose reduction based on the naproxen component of VIMOVO.
VIMOVO should be avoided in patients with severe hepatic impairment [see Warnings and Precautions (5.3), Use in Specific Populations (8.6)].
3 DOSAGE FORMS AND STRENGTHS
VIMOVO is an oval, yellow, delayed-release tablets for oral administration containing either:
- 375 mg enteric-coated naproxen and 20 mg immediate-release esomeprazole tablets printed with 375/20 in black, or
- 500 mg enteric-coated naproxen and 20 mg immediate-release esomeprazole tablets printed with 500/20 in black.
4 CONTRAINDICATIONS
VIMOVO is contraindicated in the following patients:
- Known hypersensitivity (e.g., anaphylactic reactions and serious skin reactions) to naproxen, esomeprazole magnesium, substituted benzimidazoles, or to any components of the drug product, including omeprazole. Hypersensitivity reactions to esomeprazole may include anaphylaxis, anaphylactic shock, angioedema, bronchospasm, acute tubulointerstitial nephritis, and urticaria [see Warnings and Precautions (5.7, 5.8, 5.9, 5.18), Adverse Reactions (6.2)].
- History of asthma, urticaria, or allergic-type reactions after taking aspirin or other NSAIDs. Severe, sometimes fatal, anaphylactic reactions to NSAIDs have been reported in such patients [see Warnings and Precautions (5.7, 5.8)].
- In the setting of coronary artery bypass graft (CABG) surgery [see Warnings and Precautions (5.1)].
- Proton pump inhibitors (PPIs), including esomeprazole magnesium, are contraindicated in patients receiving rilpivirine-containing products [see Drug Interactions (7)].
5 WARNINGS AND PRECAUTIONS
5.1 Cardiovascular Thrombotic Events
Clinical trials of several COX-2 selective and nonselective NSAIDs of up to three years duration have shown an increased risk of serious cardiovascular (CV) thrombotic events, including myocardial infarction (MI), and stroke, which can be fatal. Based on available data, it is unclear that the risk for CV thrombotic events is similar for all NSAIDS. The relative increase in serious CV thrombotic events over baseline conferred by NSAID use appears to be similar in those with and without known CV disease or risk factors for CV disease. However, patients with known CV disease or risk factors had a higher absolute incidence of excess serious CV thrombotic events, due to their increased baseline rate. Some observational studies found that this increased risk of serious CV thrombotic events began as early as the first weeks of treatment. The increase in CV thrombotic risk has been observed most consistently at higher doses.
To minimize the potential risk for an adverse CV event in NSAID-treated patients, use the lowest effective dose for the shortest duration possible. Physicians and patients should remain alert for the development of such events, throughout the entire treatment course, even in the absence of previous CV symptoms. Patients should be informed about the symptoms of serious CV events and the steps to take if they occur.
There is no consistent evidence that concurrent use of aspirin mitigates the increased risk of serious CV thrombotic events associated with NSAID use. The concurrent use of aspirin and an NSAID, such as naproxen, increases the risk of serious gastrointestinal (GI) events [see Warnings and Precautions (5.2)].
Status Post Coronary Artery Bypass Graft (CABG) Surgery
Two large, controlled, clinical trials of a COX-2 selective NSAID for the treatment of pain in the first 10–14 days following CABG surgery found an increased incidence of myocardial infarction and stroke. NSAIDs are contraindicated in the setting of CABG [see Contraindications (4)].
Post-MI Patients
Observational studies conducted in the Danish National Registry have demonstrated that patients treated with NSAIDs in the post-MI period were at increased risk of reinfarction, CV-related death, and all-cause mortality beginning in the first week of treatment. In this same cohort, the incidence of death in the first year post-MI was 20 per 100-person years in NSAID-treated patients compared to 12 per 100 person years in non-NSAID exposed patients. Although the absolute rate of death declined somewhat after the first year post-MI, the increased relative risk of death in NSAID users persisted over at least the next four years after follow-up.
Avoid the use of VIMOVO in patients with a recent MI unless the benefits are expected to outweigh the risk of recurrent CV thrombotic events. If VIMOVO is used in patients with a recent MI, monitor patients for signs of cardiac ischemia.
5.2 Gastrointestinal Bleeding, Ulceration, and Perforation
NSAIDs, including naproxen, can cause serious gastrointestinal (GI) adverse events including inflammation, bleeding, ulceration, and perforation of the esophagus, stomach, small intestine, or large intestine, which can be fatal. These serious adverse events can occur at any time, with or without warning symptoms, in patients treated with NSAIDs. Only one in five patients who develop a serious upper GI adverse event on NSAID therapy is symptomatic. Upper GI ulcers, gross bleeding, or perforation caused by NSAIDs occurred in approximately 1% of patients treated for 3-6 months, and in about 2% to 4% of patients treated for one year. However, even short-term NSAID therapy is not without risk.
Risk Factors for GI Bleeding, Ulceration, and Perforation
Patients with a prior history of peptic ulcer disease and/or GI bleeding who used NSAIDs had a greater than 10-fold increased risk for developing a GI bleed compared to patients without these risk factors. Other factors that increase the risk for GI bleeding in patients treated with NSAIDs include longer duration of NSAID therapy; concomitant use of oral corticosteroids, aspirin, anticoagulants, or selective serotonin reuptake inhibitors (SSRIs); smoking; use of alcohol; older age; and poor general health status. Most postmarketing reports of fatal GI events are in elderly or debilitated patients. Additionally, patients with advanced liver disease and/or coagulopathy are at increased risk for GI bleeding.
Strategies to Minimize the GI Risks in NSAID-treated patients:
- Use the lowest effective dosage for the shortest possible duration.
- Avoid administration of more than one NSAID at a time.
- Avoid use in patients at higher risk unless benefits are expected to outweigh the increased risk of bleeding. For such as patients, as well as those with active GI bleeding, consider alternate therapies other than NSAIDs.
- Remain alert for signs and symptoms of GI ulceration and bleeding during NSAID therapy.
- If a serious GI adverse event is suspected, promptly initiate evaluation and treatment, and discontinue VIMOVO until a serious GI adverse event is ruled out.
- In the setting of concomitant use of low-dose aspirin for cardiac prophylaxis, monitor patients more closely for evidence of GI bleeding [see Drug Interactions (7)].
NSAIDs should be given with care to patients with a history of inflammatory bowel disease (ulcerative colitis, Crohn's disease) as their condition may be exacerbated.
5.3 Hepatotoxicity
Elevations of ALT or AST (three or more times the upper limit of the normal [ULN]) have been reported in approximately 1% of NSAID-treated patients in clinical trials. In addition, rare, and sometimes fatal, cases of severe hepatic injury, including jaundice and fatal fulminant hepatitis, liver necrosis, and hepatic failure have been reported.
Elevations of ALT or AST (less than three times ULN) may occur in up to 15% of patients treated with NSAIDs including naproxen.
Inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, diarrhea, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If clinical signs and symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, etc.), discontinue VIMOVO immediately, and perform a clinical evaluation of the patient.
VIMOVO should be avoided in patients with severe hepatic impairment [see Dosage and Administration (2), Use in Specific Populations (8.6), and Clinical Pharmacology (12.3)].
5.4 Hypertension
NSAIDs, including VIMOVO, can lead to new onset of hypertension or worsening of pre- existing hypertension, either of which may contribute to the increased incidence of CV events.
Patients taking angiotensin converting enzyme (ACE) inhibitors, thiazides diuretics, or loop diuretics may have impaired response to these therapies when taking NSAIDs [see Drug Interactions (7)].
Monitor blood pressure (BP) during the initiation of NSAID treatment and throughout the course of therapy.
5.5 Heart Failure and Edema
The Coxib and traditional NSAID Trialists' Collaboration meta-analysis of randomized controlled trials demonstrated an approximately two-fold increase in hospitalizations for heart failure in COX-2 selective treated patients and nonselective NSAID-treated patients compared to placebo-treated patients. In a Danish National Registry study of patients with heart failure, NSAID use increased the risk of MI, hospitalization for heart failure, and death.
Additionally, fluid retention and edema have been observed in some patients treated with NSAIDs. Use of naproxen may blunt the CV effects of several therapeutic agents used to treat these medical conditions (e.g., diuretics, ACE inhibitors, or angiotensin receptor blockers [ARBs]) [see Drug Interactions (7)].
Avoid the use of VIMOVO in patients with severe heart failure unless the benefits are expected to outweigh the risk of worsening heart failure. If VIMOVO is used in patients with severe heart failure, monitor patients for signs and symptoms of worsening heart failure.
5.6 Renal Toxicity and Hyperkalemia
Renal Toxicity
Long-term administration of NSAIDs has resulted in renal papillary necrosis and other renal injury. Renal toxicity has also been seen in patients in whom renal prostaglandins have a compensatory role in the maintenance of renal perfusion. In these patients, administration of an NSAID may cause a dose-dependent reduction in prostaglandin formation and, secondarily, in renal blood flow, which may precipitate overt renal decompensation. Patients at greatest risk of this reaction are those with impaired renal function, dehydration, hypovolemia, heart failure, liver dysfunction, those taking diuretics and ACE-inhibitors or ARBs, and the elderly.
Discontinuation of NSAID therapy was usually followed by recovery to the pretreatment state.
No information is available from controlled clinical studies regarding the use of VIMOVO in patients with advanced renal disease. The renal effects of VIMOVO may hasten the progression of renal dysfunction in patients with pre-existing renal disease.
Correct volume status in dehydrated or hypovolemic patients prior to initiating VIMOVO. Monitor renal function in patients with renal or hepatic impairment, heart failure, dehydration, or hypovolemia during use of VIMOVO [see Drug Interactions (7)]. Avoid the use of VIMOVO in patients with advanced renal disease unless the benefits are expected to outweigh the risk of worsening renal failure. If VIMOVO is used in patients with advanced renal disease, monitor patients for signs of worsening renal function.
5.7 Anaphylactic Reactions
Naproxen has been associated with anaphylactic reactions in patients with and without known hypersensitivity to naproxen and in patients with aspirin-sensitive asthma [see Contraindications (4) and Warnings and Precautions (5.8)].
Seek emergency help if an anaphylactic reaction occurs.
5.8 Exacerbation of Asthma Related to Aspirin Sensitivity
A subpopulation of patients with asthma may have aspirin-sensitive asthma which may include chronic rhinosinusitis complicated by nasal polyps; severe, potentially fatal bronchospasm; and/or intolerance to aspirin and other NSAIDs. Because cross-reactivity between aspirin and other NSAIDs has been reported in such aspirin-sensitive patients, VIMOVO is contraindicated in patients with this form of aspirin sensitivity [see Contraindications (4)]. When VIMOVO is used in patients with preexisting asthma (without known aspirin sensitivity), monitor patients for changes in the signs and symptoms of asthma.
5.9 Serious Skin Reactions
NSAIDs, including naproxen, can cause serious skin adverse events such as exfoliative dermatitis, Stevens-Johnson syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal. PPIs can cause severe cutaneous adverse reactions, SJS, TEN, and acute generalized exanthematous pustulosis (AGEP) [see Adverse Reactions (6.2)]. These serious events may occur without warning. Inform patients about the signs and symptoms of serious skin reactions, and to discontinue the use of VIMOVO at the first appearance of skin rash or any other sign of hypersensitivity. VIMOVO is contraindicated in patients with previous serious skin reactions to NSAIDs [see Contraindications (4)].
5.10 Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) has been reported in patients taking NSAIDs and PPIs such as those contained in VIMOVO. Some of these events have been fatal or life-threatening. DRESS typically, although not exclusively, presents with fever, rash, lymphadenopathy, and/or facial swelling. Other clinical manifestations may include hepatitis, nephritis, hematological abnormalities, myocarditis, or myositis. Sometimes symptoms of DRESS may resemble an acute viral infection. Eosinophilia is often present. Because this disorder is variable in its presentation, other organ systems not noted here may be involved. It is important to note that early manifestations of hypersensitivity, such as fever or lymphadenopathy, may be present even though rash is not evident. If such signs or symptoms are present, discontinue VIMOVO and evaluate the patient immediately [see also Warnings and Precautions (5.9)].
5.11 Fetal Toxicity
Premature Closure of Fetal Ductus Arteriosus:
Avoid use of NSAIDs, including VIMOVO, in pregnant women at about 30 weeks gestation and later. NSAIDs, including VIMOVO, increase the risk of premature closure of the fetal ductus arteriosus at approximately this gestational age.
Oligohydramnios/Neonatal Renal Impairment:
Use of NSAIDs, including VIMOVO, at about 20 weeks gestation or later in pregnancy may cause fetal renal dysfunction leading to oligohydramnios and, in some cases, neonatal renal impairment. These adverse outcomes are seen, on average, after days to weeks of treatment, although oligohydramnios has been infrequently reported as soon as 48 hours after NSAID initiation. Oligohydramnios is often, but not always, reversible with treatment discontinuation. Complications of prolonged oligohydramnios may, for example, include limb contractures and delayed lung maturation. In some postmarketing cases of impaired neonatal renal function, invasive procedures such as exchange transfusion or dialysis were required.
If NSAID treatment is necessary between about 20 weeks and 30 weeks gestation, limit VIMOVO use to the lowest effective dose and shortest duration possible. Consider ultrasound monitoring of amniotic fluid if VIMOVO treatment is needed in a pregnant woman. Discontinue VIMOVO if oligohydramnios occurs and follow up according to clinical practice [see Use in Specific Populations (8.1)].
5.12 Hematologic Toxicity
Anemia has occurred in NSAID-treated patients. This may be due to occult or gross blood loss, fluid retention, or an incompletely described effect on erythropoiesis. If a patient treated with VIMOVO has any signs or symptoms of anemia, monitor hemoglobin or hematocrit.
NSAIDs, including VIMOVO, may increase the risk of bleeding events. Co-morbid conditions such as coagulation disorders or concomitant use of warfarin and other anticoagulants, antiplatelet agents (e.g., aspirin), and serotonin reuptake inhibitors (SSRIs) and serotonin norepinephrine reuptake inhibitors (SNRIs) may increase the risk. Monitor these patients for signs of bleeding [see Drug Interactions (7)].
5.13 Masking of Inflammation and Fever
The pharmacological activity of VIMOVO in reducing inflammation, and possibly fever, may diminish the utility of diagnostic signs in detecting infections.
5.14 Laboratory Monitoring
Because serious GI bleeding, hepatotoxicity, and renal injury can occur without warning symptoms or signs, consider monitoring patients on long-term NSAID treatment with a CBC and chemistry profile periodically [see Warnings and Precautions (5.2, 5.3, 5.6)].
Patients with initial hemoglobin values of 10 g or less who are to receive long-term therapy should have hemoglobin values determined periodically.
5.15 Active Bleeding
When active and clinically significant bleeding from any source occurs in patients receiving VIMOVO, the treatment should be withdrawn.
5.16 Concomitant NSAID Use
VIMOVO contains naproxen as one of its active ingredients. It should not be used with other naproxen-containing products since they all circulate in the plasma as the naproxen anion.
The concomitant use of VIMOVO with any dose of a non-aspirin NSAID should be avoided due to the potential for increased risk of adverse reactions.
5.17 Presence of Gastric Malignancy
In adults, response to gastric symptoms with VIMOVO does not preclude the presence of gastric malignancy. Consider additional gastrointestinal follow-up and diagnostic testing in adult patients who experience gastric symptoms during treatment with VIMOVO or have a symptomatic relapse after completing treatment. In older patients, also consider an endoscopy.
5.18 Acute Tubulointerstitial Nephritis
Acute tubulointerstitial nephritis (TIN) has been observed in patients taking PPIs and may occur at any point during PPI therapy. Patients may present with varying signs and symptoms from symptomatic hypersensitivity reactions to non-specific symptoms of decreased renal function (e.g., malaise, nausea, anorexia). In reported case series, some patients were diagnosed on biopsy and in the absence of extra-renal manifestations (e.g., fever, rash or arthralgia).
Discontinue VIMOVO and evaluate patients with suspected acute TIN [see Contraindications (4)].
5.19 Clostridium difficile-Associated Diarrhea
Published observational studies suggest that proton pump inhibitor (PPI) therapy like VIMOVO may be associated with an increased risk of Clostridium difficile associated diarrhea, especially in hospitalized patients. This diagnosis should be considered for diarrhea that does not improve [see Adverse Reactions (6.2)].
Patients should use the lowest dose and shortest duration of PPI therapy appropriate to the condition being treated [see Dosage and Administration (2)].
5.20 Bone Fracture
Several published observational studies suggest that PPI therapy may be associated with an increased risk for osteoporosis-related fractures of the hip, wrist, or spine. The risk of fracture was increased in patients who received high-dose, defined as multiple daily doses, and long-term PPI therapy (a year or longer). Patients should use the lowest dose and shortest duration of PPI therapy appropriate to the condition being treated. Patients at risk for osteoporosis-related fractures should be managed according to the established treatment guidelines [see Dosage and Administration (2), Adverse Reactions (6.2)].
VIMOVO (a combination PPI/NSAID) is approved for use twice a day and does not allow for administration of a lower daily dose of the PPI [see Dosage and Administration (2)].
5.21 Cutaneous and Systemic Lupus Erythematosus
Cutaneous lupus erythematosus (CLE) and systemic lupus erythematosus (SLE) have been reported in patients taking PPIs, including esomeprazole. These events have occurred as both new onset and an exacerbation of existing autoimmune disease. The majority of PPI- induced lupus erythematous cases were CLE.
The most common form of CLE reported in patients treated with PPIs was subacute CLE (SCLE) and occurred within weeks to years after continuous drug therapy inpatients ranging from infants to the elderly. Generally, histological findings were observed without organ involvement.
SLE is less commonly reported than CLE in patients receiving PPIs. PPI associated SLE is usually milder than non-drug induced SLE. Onset of SLE typically occurred within days to years after initiating treatment primarily in patients ranging from young adults to the elderly. The majority of patients presented with rash; however, arthralgia and cytopenia were also reported.
Avoid administration of PPIs for longer than medically indicated. If signs or symptoms consistent with CLE or SLE are noted in patients receiving VIMOVO, discontinue drug and refer the patient to the appropriate specialist for evaluation. Most patients improve with discontinuation of the PPI alone in 4 to 12 weeks. Serological testing (e.g., ANA) may be positive and elevated serological test results may take longer to resolve than clinical manifestations.
5.22 Interaction with Clopidogrel
Avoid concomitant use of esomeprazole with clopidogrel. Clopidogrel is a prodrug. Inhibition of platelet aggregation by clopidogrel is entirely due to an active metabolite. The metabolism of clopidogrel to its active metabolite can be impaired by use with concomitant medications, such as esomeprazole, that inhibit CYP2C19 activity. Concomitant use of clopidogrel with 40 mg esomeprazole reduces the pharmacological activity of clopidogrel. When using esomeprazole, a component of VIMOVO, consider alternative anti-platelet therapy [see Drug Interactions (7), Clinical Pharmacology (12.3)].
5.23 Cyanocobalamin (Vitamin B-12) Deficiency
Daily treatment with any acid-suppressing medications over a long period of time (e.g., longer than 3 years) may lead to malabsorption of cyanocobalamin (vitamin B-12) caused by hypo-or achlorhydria. Rare reports of cyanocobalamin deficiency occurring with acid- suppressing therapy have been reported in the literature. This diagnosis should be considered if clinical symptoms consistent with cyanocobalamin deficiency are observed.
5.24 Hypomagnesemia and Mineral Metabolism
Hypomagnesemia, symptomatic and asymptomatic, has been reported rarely in patients treated with PPIs for at least three months, in most cases after a year of therapy. Serious adverse events include tetany, arrhythmias, and seizures. Hypomagnesemia may lead to hypocalcemia and/or hypokalemia and may exacerbate underlying hypocalcemia in at-risk patients. In most patients, treatment of hypomagnesemia required magnesium replacement and discontinuation of the PPI.
For patients expected to be on prolonged treatment or who take PPIs with medications such as digoxin or drugs that may cause hypomagnesemia (e.g., diuretics), health care professionals may consider monitoring magnesium levels prior to initiation of PPI treatment and periodically [see Adverse Reactions (6.2)].
Consider monitoring magnesium and calcium levels prior to initiation of VIMOVO and periodically while on treatment in patients with a preexisting risk of hypocalcemia (e.g., hypoparathyroidism). Supplement with magnesium and/or calcium, as necessary. If hypocalcemia is refractory to treatment, consider discontinuing the VIMOVO.
5.25 Concomitant Use of St. John's Wort or Rifampin with VIMOVO
Drugs that induce CYP2C19 or CYP3A4 (such as St. John's Wort or rifampin) can substantially decrease esomeprazole concentrations. Avoid concomitant use of VIMOVO with St. John's Wort or rifampin [see Drug Interactions (7)].
5.26 Interactions with Diagnostic Investigations for Neuroendocrine Tumors
Serum chromogranin A (CgA) levels increase secondary to drug-induced decreases in gastric acidity. The increased CgA level may cause false positive results in diagnostic investigations for neuroendocrine tumors. Providers should temporarily stop esomeprazole treatment at least 14 days before assessing CgA levels and consider repeating the test if initial CgA levels are high. If serial tests are performed (e.g. for monitoring), the same commercial laboratory should be used for testing, as reference ranges between tests may vary [see Drug Interactions (7), Clinical Pharmacology (12.2)].
5.27 Concomitant Use of VIMOVO with Methotrexate
Literature suggests that concomitant use of PPIs with methotrexate (primarily at high dose; see methotrexate prescribing information) may elevate and prolong serum levels of methotrexate and/or its metabolite, possibly leading to methotrexate toxicities. In high-dose methotrexate administration a temporary withdrawal of the PPI may be considered in some patients [see Drug Interactions (7)].
5.28 Fundic Gland Polyps
PPI use is associated with an increased risk of fundic gland polyps that increases with long-term use, especially beyond one year. Most PPI users who developed fundic gland polyps were asymptomatic and fundic gland polyps were identified incidentally on endoscopy. Use the shortest duration of PPI therapy appropriate to the condition being treated.
6 ADVERSE REACTIONS
The following adverse reactions are discussed in greater detail in other sections of the labeling:
- Cardiovascular Thrombotic Events [see Warnings and Precautions (5.1)]
- GI Bleeding, Ulceration and Perforations [see Warnings and Precautions (5.2)]
- Hepatotoxicity [see Warnings and Precautions (5.3)]
- Hypertension [see Warnings and Precautions (5.4)]
- Heart Failure and Edema [see Warnings and Precautions (5.5)]
- Renal Toxicity and Hyperkalemia [see Warnings and Precautions (5.6)]
- Anaphylactic Reactions [see Warnings and Precautions (5.7)]
- Serious Skin Reactions [see Warnings and Precautions (5.9)]
- Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) [see Warnings and Precautions (5.10)]
- Fetal Toxicity [see Warnings and Precautions (5.11)]
- Hematologic Toxicity [see Warnings and Precautions (5.12)]
- Active Bleeding [see Warnings and Precautions (5.15)]
- Acute Tubulointerstitial Nephritis [see Warnings and Precautions (5.18)]
- Clostridium difficile-Associated Diarrhea [see Warnings and Precautions (5.19)]
- Bone Fracture [see Warnings and Precautions (5.20)]
- Cutaneous and Systemic Lupus Erythematosus [see Warnings and Precautions (5.21)]
- Cyanocobalamin (Vitamin B-12) Deficiency [see Warnings and Precautions (5.23)]
- Hypomagnesemia and Mineral Metabolism [see Warnings and Precautions (5.24)]
- Fundic Gland Polyps [see Warnings and Precautions (5.28)]
6.1 Clinical Trials Experience
Clinical Trials Experience with VIMOVO
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The adverse reactions reported below are specific to the clinical trials with VIMOVO.
The safety of VIMOVO was evaluated in clinical studies involving 2317 patients (aged 27 to 90 years) and ranging from 3 to 12 months. Patients received either 500 mg/20 mg of VIMOVO twice daily (n=1157), 500 mg of enteric-coated naproxen twice daily (n=426), or placebo (n=246). The average number of VIMOVO doses taken over 12 months was 696+44.
The table below lists all adverse reactions, regardless of causality, occurring in >2% of patients receiving VIMOVO and higher in the VIMOVO group than control from two clinical studies (Study 1 and Study 2). Both of these studies were randomized, multi-center, double-blind, parallel studies. The majority of patients were female (67%), white (86%). The majority of patients were 50-69 years of age (83%). Approximately one quarter were on low-dose aspirin.
| Preferred term | VIMOVO 500 mg/20 mg twice daily (n=428) % | EC-Naproxen 500 mg twice daily (n=426) % |
|---|---|---|
|
||
| Gastritis | 17 | 14 |
| Diarrhea | 6 | 5 |
| Upper respiratory tract infection | 5 | 4 |
| Flatulence | 4 | 3 |
| Headache | 3 | 1 |
| Urinary tract infection | 2 | 1 |
| Dysgeusia | 2 | 1 |
In Study 1 and Study 2, patients taking VIMOVO had fewer premature discontinuations due to adverse reactions compared to patients taking enteric-coated naproxen alone (7.9% vs. 12.5% respectively). The most common reasons for discontinuations due to adverse events in the VIMOVO treatment group were upper abdominal pain (1.2%, n=5), duodenal ulcer (0.7%, n=3) and erosive gastritis (0.7%, n=3). Among patients receiving enteric-coated naproxen, the most common reasons for discontinuations due to adverse events were duodenal ulcer 5.4% (n=23), dyspepsia 2.8% (n=12) and upper abdominal pain 1.2% (n=5). The proportion of patients discontinuing treatment due to any upper gastrointestinal adverse events (including duodenal ulcers) in patients treated with VIMOVO was 4% compared to 12% for patients taking enteric- coated naproxen.
The table below lists all adverse reactions, regardless of causality, occurring in >2% of patients and higher in the VIMOVO group than placebo from 2 clinical studies conducted in patients with osteoarthritis of the knee (Study 3 and Study 4).
| Preferred term | VIMOVO 500 mg/20 mg twice daily (n=490) % | Placebo (n=246) % |
|---|---|---|
|
||
| Diarrhea | 6 | 4 |
| Abdominal Pain Upper | 4 | 3 |
| Constipation | 4 | 1 |
| Dizziness | 3 | 2 |
| Peripheral edema | 3 | 1 |
The percentage of subjects who withdrew from the VIMOVO treatment group in these studies due to treatment-emergent adverse events was 7%. There were no preferred terms in which more than 1% of subjects withdrew from any treatment group.
The long-term safety of VIMOVO was evaluated in an open-label clinical trial of 239 patients, of which 135 patients received 500 mg/20 mg of VIMOVO for 12 months. There were no differences in frequency or types of adverse reactions seen in the long-term safety study compared to shorter-term treatment in the randomized controlled studies.
Clinical Trials Experience with Naproxen and Other NSAIDs
In patients taking naproxen in clinical trials, the most frequent reported adverse experiences in approximately 1% to 10% of patients are:
Gastrointestinal: heartburn, nausea, dyspepsia, stomatitis
Central Nervous System: drowsiness, lightheadedness, vertigo
Dermatologic: pruritus, skin eruptions, ecchymoses, sweating, purpura
Special Senses: tinnitus, visual disturbances, hearing disturbances
Cardiovascular: palpitations
General: dyspnea, thirst
In patients taking NSAIDs, the following adverse experiences have also been reported in approximately 1% to 10% of patients.
Gastrointestinal: gross bleeding/perforation, GI ulcers (gastric/duodenal), vomiting
General: abnormal renal function, anemia, elevated liver enzymes, increased bleeding time, rashes
The following are additional adverse experiences reported in <1% of patients taking naproxen during clinical trials.
Gastrointestinal: pancreatitis
Hepatobiliary: jaundice
Hemic and Lymphatic: melena, thrombocytopenia, agranulocytosis
Nervous System: inability to concentrate
Dermatologic: skin rashes
In patients taking NSAIDs, the following adverse experiences have also been reported in <1% of patients.
Body as a Whole: fever, infection, sepsis, anaphylactic reactions, appetite changes, death
Cardiovascular: hypertension, tachycardia, syncope, arrhythmia, hypotension, myocardial infarction
Gastrointestinal: dry mouth, glossitis, eructation
Hepatobiliary: hepatitis, liver failure
Hemic and Lymphatic: rectal bleeding, lymphadenopathy, pancytopenia
Metabolic and Nutritional: weight changes
Nervous System: anxiety, asthenia, confusion, nervousness, paresthesia, somnolence, tremor, coma, hallucinations
Respiratory: asthma, respiratory depression, pneumonia
Dermatologic: exfoliative dermatitis
Special Senses: blurred vision, conjunctivitis
Urogenital: cystitis, dysuria, oliguria/polyuria, proteinuria
Clinical Trials Experience with Esomeprazole Magnesium
Additional adverse reactions that were reported as possibly or probably related to esomeprazole magnesium with an incidence of <1% are listed below by body system:
Body as a Whole: abdomen enlarged, allergic reaction, asthenia, back pain, chest pain, substernal chest pain, facial edema, hot flushes, fatigue, fever, flu-like disorder, generalized edema, malaise, pain, rigors
Cardiovascular: flushing, hypertension, tachycardia
Endocrine: goiter
Gastrointestinal: dyspepsia, dysphagia, dysplasia GI, epigastric pain, eructation, esophageal disorder, gastroenteritis, GI hemorrhage, GI symptoms not otherwise specified, hiccup, melena, mouth disorder, pharynx disorder, rectal disorder, serum gastrin increased, tongue disorder, tongue edema, ulcerative stomatitis, vomiting
Hearing: earache, tinnitus
Hematologic: anemia, anemia hypochromic, cervical lymphadenopathy, epistaxis, leukocytosis, leukopenia, thrombocytopenia
Hepatic: bilirubinemia, hepatic function abnormal, SGOT increased, SGPT increased
Metabolic/Nutritional: glycosuria, hyperuricemia, hyponatremia, increased alkaline phosphatase, thirst, vitamin B12 deficiency, weight increase, weight decrease
Musculoskeletal: arthralgia, arthritis aggravated, arthropathy, cramps, fibromyalgia syndrome, hernia, polymyalgia rheumatica
Nervous System/Psychiatric: anorexia, apathy, appetite increased, confusion, depression aggravated, hypertonia, nervousness, hypoesthesia, impotence, insomnia, migraine, migraine aggravated, paresthesia, sleep disorder, somnolence, tremor, vertigo, visual field defect
Reproductive: dysmenorrhea, menstrual disorder, vaginitis
Respiratory: asthma aggravated, coughing, dyspnea, larynx edema, pharyngitis, rhinitis, sinusitis
Skin and Appendages: acne, angioedema, dermatitis, pruritus, pruritus ani, rash, rash erythematous, rash maculo-papular, skin inflammation, sweating increased, urticaria
Special Senses: otitis media, parosmia, taste loss
Urogenital: abnormal urine, albuminuria, cystitis, dysuria, fungal infection, hematuria, micturition frequency, moniliasis, genital moniliasis, polyuria
Visual: conjunctivitis, vision abnormal
The following potentially clinically significant laboratory changes in clinical trials, irrespective of relationship to esomeprazole magnesium, were reported in ≤ 1% of patients: increased creatinine, uric acid, total bilirubin, alkaline phosphatase, ALT, AST, hemoglobin, white blood cell count, platelets, serum gastrin, potassium, sodium, thyroxine and thyroid stimulating hormone.
Decreases were seen in hemoglobin, white blood cell count, platelets, potassium, sodium, and thyroxine.
Endoscopic findings that were reported as adverse reactions include: duodenitis, esophagitis, esophageal stricture, esophageal ulceration, esophageal varices, gastric ulcer, hernia, benign polyps or nodules, Barrett's esophagus, and mucosal discoloration.
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of VIMOVO. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
VIMOVO
Body as a Whole: gait disturbance
Gastrointestinal: abdominal distension, abdominal pain, gastroesophageal reflux, hematochezia
Injury, Poisoning and Procedural Complications: contusion, fall
Musculoskeletal and Connective Tissue: joint swelling, muscle spasms
Urogenital: renal tubular necrosis
Naproxen
Body as a Whole: angioneurotic edema, menstrual disorders
Cardiovascular: congestive heart failure, vasculitis, pulmonary edema
Gastrointestinal: inflammation, bleeding (sometimes fatal, particularly in the elderly), ulceration, and obstruction of the upper or lower gastrointestinal tract, esophagitis, stomatitis, hematemesis, colitis, exacerbation of inflammatory bowel disease (ulcerative colitis, Crohn's disease)
Hepatobiliary: hepatitis (some cases have been fatal)
Hemic and Lymphatic: eosinophilia, hemolytic anemia, aplastic anemia
Metabolic and Nutritional: hyperglycemia, hypoglycemia
Nervous System: depression, dream abnormalities, insomnia, malaise, myalgia, muscle weakness, aseptic meningitis, cognitive dysfunction, convulsions
Respiratory: eosinophilic pneumonitis
Dermatologic: alopecia, urticaria, toxic epidermal necrolysis, erythema multiforme, erythema nodosum, fixed drug eruption, lichen planus, pustular reaction, systemic lupus erythematoses, bullous reactions, including Stevens-Johnson syndrome, photosensitive dermatitis, photosensitivity reactions, including rare cases resembling porphyria cutanea tarda (pseudoporphyria) or epidermolysis bullosa. If skin fragility, blistering or other symptoms suggestive of pseudoporphyria occur, treatment should be discontinued and the patient monitored.
Special Senses: hearing impairment, corneal opacity, papillitis, retrobulbar optic neuritis, papilledema
Urogenital: glomerular nephritis, hematuria, hyperkalemia, interstitial nephritis, nephrotic syndrome, renal disease, renal failure, renal papillary necrosis, raised serum creatinine
Reproduction (female): infertility
Esomeprazole Magnesium
Blood and Lymphatic: agranulocytosis
Eye: blurred vision
Gastrointestinal: pancreatitis, microscopic colitis, fundic gland polyps
Hepatobiliary: hepatic failure, hepatitis with or without jaundice
Immune System: anaphylactic reaction/shock, systemic lupus erythematosus
Infections and Infestations: GI candidiasis, Clostridium difficile associated diarrhea
Metabolism and Nutritional Disorders: hypomagnesemia, hypocalcemia, hypokalemia [see Warnings and Precautions (5.24)], hyponatremia
Musculoskeletal and Connective Tissue: muscular weakness, myalgia, bone fracture
Nervous System: hepatic encephalopathy
Psychiatric: aggression, agitation, hallucination
Renal and Urinary: interstitial nephritis
Reproductive System and Breast: gynecomastia, erectile dysfunction
Respiratory, Thoracic, and Mediastinal: bronchospasm
Skin and Subcutaneous Tissue: alopecia, erythema multiforme, photosensitivity, SJS, TEN (some fatal), DRESS, AGEP, cutaneous lupus erythematosus
7 DRUG INTERACTIONS
See Table 3 and Table 4 for clinically significant drug interactions and interactions with diagnostics with naproxen and esomeprazole magnesium.
| Clinical Impact: | Naproxen
|
Esomeprazole Magnesium
|
|
| Intervention: | Monitor patients with concomitant use of VIMOVO with anticoagulants (e.g., warfarin), antiplatelet agents (e.g., aspirin), selective serotonin reuptake inhibitors (SSRIs), and serotonin norepinephrine reuptake inhibitors (SNRIs) for signs of bleeding [see Warnings and Precautions (5.14)]. Clopidogrel: Avoid concomitant use of clopidogrel with VIMOVO. Consider use of alternative anti-platelet therapy [see Warnings and Precautions (5.22)]. |
| Aspirin | |
| Clinical Impact: | A pharmacodynamics (PD) study has demonstrated an interaction in which lower dose naproxen (220mg/day or 220mg twice daily) interfered with the antiplatelet effect of low-dose immediate-release aspirin, with the interaction most marked during the washout period of naproxen [see Clinical Pharmacology (12.2.)]. There is reason to expect that the interaction would be present with prescription doses of naproxen or with enteric-coated low-dose aspirin; however, the peak interference with aspirin function may be later than observed in the PD study due to the longer washout period. |
| Controlled clinical studies showed that the concomitant use of NSAIDs and analgesic doses of aspirin does not produce any greater therapeutic effect than the use of NSAIDs alone. In a clinical study, the concomitant use of an NSAID and aspirin was associated with a significantly increased incidence of GI adverse reactions as compared to use of the NSAID alone [see Warnings and Precautions (5.2)]. | |
| Intervention: | Because there may be an increased risk of cardiovascular events following discontinuation of naproxen due to the interference with the antiplatelet effect of aspirin during the washout period, for patients taking low-dose aspirin for cardioprotection who require intermittent analgesics, consider use of an NSAID that does not interfere with the antiplatelet effect of aspirin, or non-NSAID analgesics where appropriate. |
| Concomitant use of VIMOVO and analgesic doses of aspirin is not generally recommended because of the increased risk of bleeding [see Warnings and Precautions (5.12)]. VIMOVO is not a substitute for low dose aspirin for cardiovascular protection. |
|
| ACE Inhibitors, Angiotensin Receptor Blockers, and Beta-Blockers | |
| Clinical Impact: |
|
| Intervention: |
|
| Diuretics | |
| Clinical Impact: | Clinical studies, as well as post-marketing observations, showed that NSAIDs reduced the natriuretic effect of loop diuretics (e.g., furosemide) and thiazide diuretics in some patients. This effect has been attributed to the NSAID inhibition of renal prostaglandin synthesis. |
| Intervention: | During concomitant use of VIMOVO with diuretics, observe patients for signs of worsening renal function, in addition to assuring diuretic efficacy including antihypertensive effects [see Warnings and Precautions (5.6)]. |
| Antiretrovirals | |
| Clinical Impact: | The effect of esomeprazole magnesium on antiretroviral drugs is variable. The clinical importance and mechanisms behind these interactions are not always known.
|
| Intervention: | Rilpivirine-containing products: Concomitant use with VIMOVO is contraindicated [see Contraindications (4)]. Atazanavir: See prescribing information for atazanavir for dosing information. Nelfinavir: Avoid concomitant use with VIMOVO. Saquinavir: See the prescribing information for saquinavir for monitoring of potential saquinavir-related toxicities. Other antiretrovirals: See prescribing information of specific drugs. |
| Cilostazol | |
| Clinical Impact: | Increased exposure of cilostazol and one of its active metabolites (3,4-dihydro-cilostazol) when coadministered with omeprazole magnesium, the racemate of esomeprazole [see Clinical Pharmacology (12.3)]. |
| Intervention: | Consider reducing the dose of cilostazol to 50 mg twice daily. |
| Digoxin | |
| Clinical Impact: | Naproxen
|
| Intervention: | Monitor digoxin concentrations during concomitant use of VIMOVO. Dose adjustment of digoxin may be needed to maintain therapeutic drug concentrations. |
| Lithium | |
| Clinical Impact: | NSAIDs have produced elevations of plasma lithium levels and reductions in renal lithium clearance. The mean minimum lithium concentration increased 15%, and the renal clearance decreased by approximately 20%. This effect has been attributed to NSAID inhibition of renal prostaglandin synthesis. |
| Intervention: | During concomitant use of VIMOVO and lithium, monitor patients for signs of lithium toxicity. |
| Methotrexate | |
| Clinical Impact: | Naproxen
|
| Intervention: | During concomitant use of VIMOVO and methotrexate, monitor patients for methotrexate toxicity. A temporary withdrawal of VIMOVO may be considered in some patients receiving high-dose methotrexate. |
| Cyclosporine | |
| Clinical Impact: | Concomitant use of naproxen and cyclosporine may increase cyclosporine's nephrotoxicity. |
| Intervention: | During concomitant use of VIMOVO and cyclosporine, monitor patients for signs of worsening renal function. |
| Tacrolimus | |
| Clinical Impact: | Concomitant use of esomeprazole magnesium and tacrolimus may increase exposure of tacrolimus |
| Intervention: | During concomitant use of VIMOVO and tacrolimus, monitor tacrolimus whole blood concentrations. |
| NSAIDs and Salicylates | |
| Clinical Impact: | Concomitant use of naproxen with other NSAIDs or salicylates (e.g., diflunisal, salsalate) increases the risk of GI toxicity, with little or no increase in efficacy [see Warnings and Precautions (5.2)]. |
| Intervention: | The concomitant use of VIMOVO with other NSAIDs or salicylates is not recommended. |
| Pemetrexed | |
| Clinical Impact: | Concomitant use of VIMOVO and pemetrexed may increase the risk of pemetrexed-associated myelosuppression, renal, and GI toxicity (see the pemetrexed prescribing information). |
| Intervention: | During concomitant use of VIMOVO and pemetrexed, in patients with renal impairment whose creatinine clearance ranges from 45 to 79 mL/min, monitor for myelosuppression, renal and GI toxicity. |
| Drugs Dependent on Gastric pH for Absorption (e.g., iron salts, erlotinib, mycophenoloate mofetil, ketoconazole) | |
| Clinical Impact: | Esomeprazole magnesium can reduce the absorption of other drugs due to its effect on reducing intragastric acidity |
| Intervention: | Mycophenolate mofetil (MMF): Co-administration of omeprazole, of which esomeprazole magnesium is an enantiomer, in healthy subjects and in transplant patients receiving MMF has been reported to reduce the exposure to the active metabolite, mycophenolic acid (MPA), possibly due to a decrease in MMF solubility at an increased gastric pH. The clinical relevance of reduced MPA exposure on organ rejection has not been established in transplant patients receiving esomeprazole and MMF. Use VIMOVO with caution in transplant patients receiving MMF [see Clinical Pharmacology (12.3)]. See the prescribing information for other drugs dependent on gastric pH for absorption. |
| Interactions with Investigations of Neuroendocrine Tumors | |
| Clinical Impact: | Serum chromogranin A (CgA) levels increase secondary to PPI-induced decreases in gastric acidity. The increased CgA levels may cause false positive results in diagnostic investigations for neuroendocrine tumors [see Warnings and Precautions (5.26), Clinical Pharmacology (12.2)]. |
| Intervention: | Temporarily stop VIMOVO treatment at least 14 days before assessing CgA levels and consider repeating the test if initial CgA levels are high. If serial tests are performed (e.g. for monitoring), the same commercial laboratory should be used for testing, as reference ranges between tests may vary. |
| Diazepam | |
| Clinical Impact: | Increased exposure of diazepam [see Clinical Pharmacology (12.3)]. |
| Intervention: | Monitor patients for increased sedation and adjust the dose of diazepam as needed. |
| CYP2C19 or CYP3A4 Inducers | |
| Clinical Impact: | Decreased exposure of esomeprazole when used concomitantly with strong inducers [see Clinical Pharmacology (12.3)]. |
| Intervention: | St. John's Wort, rifampin: Avoid concomitant use with VIMOVO [see Warnings and Precautions (5.25)]. |
| CYP2C19 or CYP3A4 Inhibitors | |
| Clinical Impact: | Increased exposure of esomeprazole [see Clinical Pharmacology (12.3)]. |
| Intervention: | Voriconazole: Avoid concomitant use with VIMOVO. |
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
Use of NSAIDs, including VIMOVO, can cause premature closure of the fetal ductus arteriosus and fetal and renal dysfunction leading to oligohydramnios and, in some cases, neonatal renal impairment. Because of these risks, limit dose and duration of VIMOVO use between about 20 and 30 weeks of gestation and avoid VIMOVO use at about 30 weeks of gestation and later in pregnancy (see Clinical Considerations, Data).
Premature Closure of the Fetal Ductus Arteriosus
Use of NSAIDs, including VIMOVO, at about 30 weeks gestation or later in pregnancy increases the risk of premature closure of the fetal ductus arteriosus.
Oligohydramnios/Neonatal Renal Impairment
Use of NSAIDs at about 20 weeks gestation or later in pregnancy has been associated with cases of fetal renal dysfunction leading to oligohydramnios, and in some cases, neonatal renal impairment.
VIMOVO contains naproxen and esomeprazole magnesium. Esomeprazole is the S- isomer of omeprazole.
Naproxen
Data from observational studies regarding potential embryofetal risks of NSAID use in women in the first or second trimesters of pregnancy are inconclusive. In animal reproduction studies, naproxen administered during organogenesis to rats and rabbits at doses less than the maximum recommended human daily dose of 1500 mg/day showed no evidence of harm to the fetus (see Data). Based on animal data, prostaglandins have been shown to have an important role in endometrial vascular permeability, blastocyst implantation, and decidualization. In animal studies, administration of prostaglandin synthesis inhibitors such as naproxen resulted in increased pre- and post-implantation loss.
Prostaglandins also have been shown to have an important role in fetal kidney development. In published animal studies, prostaglandin synthesis inhibitors have been reported to impair kidney development when administered at clinically relevant doses.
Esomeprazole
There are no human data for esomeprazole. However, available epidemiologic data for omeprazole (esomeprazole is the S-isomer of omeprazole) fail to demonstrate an increased risk of major congenital malformations or other adverse pregnancy outcomes with first trimester omeprazole use (see Data). In animal studies with administration of oral esomeprazole magnesium in rats, changes in bone morphology were observed in offspring of rats dosed through most of pregnancy and lactation at doses equal to or greater than approximately 34 times an oral human dose of 40 mg esomeprazole or 40 mg omeprazole. When maternal administration was confined to gestation only, there were no effects on bone physeal morphology in the offspring at any age [see Data].
The estimated background risks of major birth defects and miscarriage for the indicated population are unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations
Fetal/Neonatal Adverse Reactions
Premature Closure of Fetal Ductus Arteriosus:
Avoid use of NSAIDs in women at about 30 weeks gestation and later in pregnancy, because NSAIDs, including VIMOVO, can cause premature closure of the fetal ductus arteriosus (see Data).
Oligohydramnios/Neonatal Renal Impairment
If an NSAID is necessary at about 20 weeks gestation or later in pregnancy, limit the use to the lowest effective dose and shortest duration possible. If VIMOVO treatment is needed in pregnant women, consider monitoring with ultrasound for oligohydramnios. If oligohydramnios occurs, discontinue VIMOVO and follow up according to clinical practice (see Data).
Data
Human Data
Naproxen
When used to delay preterm labor, inhibitors of prostaglandin synthesis, including NSAIDs such naproxen, may increase the risk of neonatal complications such as necrotizing enterocolitis, patent ductus arteriosus and intracranial hemorrhage. Naproxen treatment given in late pregnancy to delay parturition has been associated with persistent pulmonary hypertension, renal dysfunction and abnormal prostaglandin E levels in preterm infants.
Premature Closure of Fetal Ductus Arteriosus:
Published literature reports that the use of NSAIDs at about 30 weeks of gestation and later in pregnancy may cause premature closure of the fetal ductus arteriosus.
Oligohydramnios/Neonatal Renal Impairment:
Published studies and postmarketing reports describe maternal NSAID use at about 20 weeks gestation or later in pregnancy associated with fetal renal dysfunction leading to oligohydramnios, and in some cases, neonatal renal impairment. These adverse outcomes are seen, on average, after days to weeks of treatment, although oligohydramnios has been infrequently reported as soon as 48 hours after NSAID initiation. In many cases, but not all, the decrease in amniotic fluid was transient and reversible with cessation of the drug. There have been a limited number of case reports of maternal NSAID use and neonatal renal dysfunction without oligohydramnios, some of which were irreversible. Some cases of neonatal renal dysfunction required treatment with invasive procedures, such as exchange transfusion or dialysis.
Methodological limitations of these postmarketing studies and reports include lack of a control group; limited information regarding dose, duration, and timing of drug exposure; and concomitant use of other medications. These limitations preclude establishing a reliable estimate of the risk of adverse fetal and neonatal outcomes with maternal NSAID use. Because the published safety data on neonatal outcomes involved mostly preterm infants, the generalizability of certain reported risks to the full-term infant exposed to NSAIDs through maternal use is uncertain.
Esomeprazole
Esomeprazole is the S-isomer of omeprazole. Four epidemiological studies compared the frequency of congenital abnormalities among infants born to women who used omeprazole during pregnancy with the frequency of abnormalities among infants of women exposed to H2-receptor antagonists or other controls.
A population-based retrospective cohort epidemiological study from the Swedish Medical Birth Registry, covering approximately 99% of pregnancies, from 1995-99, reported on 955 infants (824 exposed during the first trimester with 39 of these exposed beyond first trimester, and 131 exposed after the first trimester) whose mothers used omeprazole during pregnancy. The number of infants exposed in utero to omeprazole that had any malformation, low birth weight, low Apgar score, or hospitalization was similar to the number observed in this population. The number of infants born with ventricular septal defects and the number of stillborn infants was slightly higher in the omeprazole-exposed infants than the expected number in this population.
A population-based retrospective cohort study covering all live births in Denmark from 1996- 2009, reported on 1,800 live births whose mothers used omeprazole during the first trimester of pregnancy and 837, 317 live births whose mothers did not use any proton pump inhibitor. The overall rate of birth defects in infants born to mothers with first trimester exposure to omeprazole was 2.9% and 2.6% in infants born to mothers not exposed to any proton pump inhibitor during the first trimester.
A retrospective cohort study reported on 689 pregnant women exposed to either H2-blockers or omeprazole in the first trimester (134 exposed to omeprazole) and 1,572 pregnant women unexposed to either during the first trimester. The overall malformation rate in offspring born to mothers with first trimester exposure to omeprazole, an H2-blocker, or were unexposed was 3.6%, 5.5%, and 4.1% respectively.
A small prospective observational cohort study followed 113 women exposed to omeprazole during pregnancy (89% first trimester exposures). The reported rate of major congenital malformations was 4% in the omeprazole group, 2% in controls exposed to non-teratogens, and 2.8% in disease-paired controls. Rates of spontaneous and elective abortions, preterm deliveries, gestational age at delivery, and mean birth weight were similar among the groups.
Several studies have reported no apparent adverse short-term effects on the infant when single dose oral or intravenous omeprazole was administered to over 200 pregnant women as premedication for cesarean section under general anesthesia.
Animal Data
There are no reproduction studies in animals with VIMOVO, a combination of naproxen and esomeprazole.
Naproxen
Reproduction studies with naproxen administered during the period of organogenesis have been performed in rats at 20 mg/kg/day (0.13 times the maximum recommended human daily dose of 1500 mg/day based on body surface area comparison) rabbits at 20 mg/kg/day (0.26 times the maximum recommended human daily dose, based on body surface area comparison), and mice at 170 mg/kg/day (0.56 times the maximum recommended human daily dose based on body surface area comparison) with no evidence of harm to the fetus due to the drug.
Esomeprazole
No effects on embryo-fetal development were observed in reproduction studies with esomeprazole magnesium in rats at oral doses up to 280 mg/kg/day (about 68 times an oral human dose of 40 mg on a body surface area basis) or in rabbits at oral doses up to 86 mg/kg/day (about 42 times an oral human dose of 40 mg esomeprazole or 40 mg omeprazole on a body surface area basis) administered during organogenesis and have revealed no evidence of harm to the fetus due to esomeprazole magnesium.
A pre- and postnatal developmental toxicity study in rats with additional endpoints to evaluate bone development were performed with esomeprazole magnesium at oral doses of 14 to 280 mg/kg/day (about 3.4 to 68 times a daily human dose of 40 mg on a body surface area basis). Neonatal/early postnatal (birth to weaning) survival was decreased at doses equal to or greater than 138 mg/kg/day (about 34 times an oral human dose of 40 mg on a body surface area basis). Body weight and body weight gain were reduced and neurobehavioral or general developmental delays in the immediate post-weaning timeframe were evident at doses equal to or greater than 69 mg /kg/day (about 17 times an oral human dose of 40 mg on a body surface area basis). In addition, decreased femur length, width and thickness of cortical bone, decreased thickness of the tibial growth plate and minimal to mild bone marrow hypocellularity were noted at doses equal to or greater than 14 mg/kg/day (about 3.4 times a daily human dose of 40 mg on a body surface area basis). Physeal dysplasia in the femur was observed in offspring of rats treated with oral doses of esomeprazole magnesium at doses equal to or greater than 138 mg/kg/day (about 34 times the daily human dose of 40 mg on a body surface area basis).
Effects on maternal bone were observed in pregnant and lactating rats in the pre- and postnatal toxicity study when esomeprazole magnesium was administered at oral doses of 14 to 280 mg /kg/day (about 3.4 to 68 times an oral human dose of 40 mg on a body surface area basis). When rats were dosed from gestational day 7 through weaning on postnatal day 21, a statistically significant decrease in maternal femur weight of up to 14% (as compared to placebo treatment) was observed at doses equal to or greater than 138 mg/kg/day (about 34 times an oral human dose of 40 mg on a body surface area basis).
A pre- and postnatal development study in rats with esomeprazole strontium (using equimolar doses compared to esomeprazole magnesium study) produced similar results in dams and pups as described above. A follow up developmental toxicity study in rats with further time points to evaluate pup bone development from postnatal day 2 to adulthood was performed with esomeprazole magnesium at oral doses of 280 mg/kg/day (about 68 times an oral human dose of 40 mg on a body surface area basis) where esomeprazole administration was from either gestational day 7 or gestational day 16 until parturition. When maternal administration was confined to gestation only, there were no effects on bone physeal morphology in the offspring at any age.
8.2 Lactation
Risk Summary
Limited data from published literature report that naproxen anion has been found in the milk of lactating women at a concentration equivalent to approximately 1% of maximum naproxen concentration in plasma. Esomeprazole is the S-isomer of omeprazole and limited data from published literature suggest omeprazole may be present in human milk. There is no information on the effects of naproxen or omeprazole on the breastfed infant or on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for VIMOVO and any potential adverse effects on the breastfed infant from the drug or from the underlying maternal condition.
8.3 Females and Males of Reproductive Potential
Infertility
Females
Based on the mechanism of action, the use of prostaglandin-mediated NSAIDs, including VIMOVO, may delay or prevent rupture of ovarian follicles that may lead to reversible infertility in some women. Small studies in women treated with NSAIDs have also shown a reversible delay in ovulation. Published animal studies have shown that administration of prostaglandin synthesis inhibitors have the potential to disrupt prostaglandin-mediated follicular rupture required for ovulation. Consider withdrawal of NSAIDs, including VIMOVO, in women who have difficulties conceiving or who are undergoing investigation of infertility.
8.4 Pediatric Use
The safety and effectiveness of VIMOVO have been established in adolescent patients 12 years of age and older weighing at least 38 kg for the symptomatic relief of JIA and to decrease the risk of developing naproxen-associated gastric ulcers. Use of VIMOVO in this age group is based on extrapolation of adequate and well-controlled studies in adults and supported by a 6 month safety study including pharmacokinetic assessment of naproxen and esomeprazole magnesium in 36 adolescent patients with JIA. Based on the limited data, the plasma naproxen and plasma esomeprazole concentrations were found to be within the range to that observed to those found in healthy adults. The safety profile of VIMOVO in adolescent patients with JIA was similar to adults with RA.
The safety and effectiveness of VIMOVO in pediatric patients less than 12 years of age or less than 38 kg with JIA have not been established.
Juvenile Animal Data
In a juvenile rat toxicity study, esomeprazole was administered with both magnesium and strontium salts at oral doses about 34 to 68 times a daily human dose of 40 mg based on body surface area. Increases in death were seen at the high dose, and at all doses of esomeprazole, there were decreases in body weight, body weight gain, femur weight and femur length, and decreases in overall growth [see Nonclinical Toxicology (13.2)].
8.5 Geriatric Use
Elderly patients, compared to younger patients, are at greater risk for NSAID-associated serious cardiovascular, gastrointestinal, and/or renal adverse reactions. If the anticipated benefit for the elderly patient outweighs these potential risks, start dosing at the low end of the dosing range, and monitor patients for adverse effects [see Warnings and Precautions (5.1, 5.2, 5.3, 5.6, 5.14)].
Of the total number of patients who received VIMOVO (n=1157) in clinical trials, 387 were ≥65 years of age, of which 85 patients were 75 years and over. No meaningful differences in efficacy or safety were observed between these subjects and younger subjects [see Adverse Reactions (6)].
Studies indicate that although total plasma concentration of naproxen is unchanged, the unbound plasma fraction of naproxen is increased in the elderly. Caution is advised when high doses are required and some adjustment of dosage may be required in elderly patients. As with other drugs used in the elderly, it is prudent to use the lowest effective dose [see Dosage and Administration (2), Clinical Pharmacology (12.3)].
Experience indicates that geriatric patients may be particularly sensitive to certain adverse effects of NSAIDs. Elderly or debilitated patients seem to tolerate peptic ulceration or bleeding less well when these events do occur. Most spontaneous reports of fatal GI events are in the geriatric population [see Warnings and Precautions (5.2)].
Naproxen and its metabolites are known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function. Geriatric patients may be at a greater risk for the development of a form of renal toxicity precipitated by reduced prostaglandin formation during administration of NSAIDs [see Warnings and Precautions (5.6)].
8.6 Hepatic Impairment
VIMOVO should be avoided in patients with severe hepatic impairment because naproxen may increase the risk of renal failure or bleeding and esomeprazole doses should not exceed 20 mg daily in these patients [see Dosage and Administration (2), Warnings and Precautions (5.3), Clinical Pharmacology (12.3)].
8.7 Renal Impairment
Naproxen-containing products, including VIMOVO, are not recommended for use in patients with advanced renal disease [see Dosage and Administration (2), Warnings and Precautions (5.6)].
10 OVERDOSAGE
There is no clinical data on overdosage with VIMOVO.
Overdosage of naproxen:
Symptoms following acute NSAID overdosages have been typically limited to lethargy, drowsiness, nausea, vomiting, and epigastric pain, which have been generally reversible with supportive care. Gastrointestinal bleeding has occurred. Hypertension, acute renal failure, respiratory depression, and coma have occurred but were rare [see Warnings and Precautions (5.1, 5.2, 5.4, 5.6)].
A few patients have experienced seizures, but it is not clear whether or not these were drug- related. It is not known what dose of the drug would be life threatening. The oral LD50 of the drug is 500 mg/kg in rats, 1200 mg/kg in mice, 4000 mg/kg in hamsters and greater than 1000 mg/kg in dogs. In animals 0.5 g/kg of activated charcoal was effective in reducing plasma levels of naproxen.
Manage patients with symptomatic and supportive care following an NSAID overdosage. There are no specific antidotes. Hemodialysis does not decrease the plasma concentration of naproxen because of the high degree of its protein binding. Consider emesis and/or activated charcoal (60 to 100 grams in adults, 1 to 2 grams per kg of body weight in pediatric patients) and/or osmotic cathartic in symptomatic patients seen within four hours of ingestion or in patients with a large overdosage (5 to 10 times the recommended dosage). Forced diuresis, alkalinization of urine, hemodialysis, or hemoperfusion may not be useful due to high protein binding.
Overdosage of esomeprazole:
A single oral dose of esomeprazole at 510 mg/kg (about 124 times the human dose on a body surface area basis) was lethal to rats. The major signs of acute toxicity were reduced motor activity, changes in respiratory frequency, tremor, ataxia, and intermittent clonic convulsions. The symptoms described in connection with deliberate esomeprazole overdose (limited experience of doses in excess of 240 mg/day) are transient. Single doses of 80 mg of esomeprazole were uneventful. Reports of overdosage with omeprazole in humans may also be relevant. Doses ranged up to 2,400 mg (120 times the usual recommended clinical dose).
Manifestations were variable, but included confusion, drowsiness, blurred vision, tachycardia, nausea, diaphoresis, flushing, headache, dry mouth, and other adverse reactions similar to those seen in normal clinical experience (see omeprazole package insert - Adverse Reactions). No specific antidote for esomeprazole is known. Since esomeprazole is extensively protein bound, it is not expected to be removed by dialysis. In the event of overdosage, treatment should be symptomatic and supportive.
If over-exposure occurs, call your Poison Control Center at 1-800-222-1222 for current information on the management of poisoning or overdosage.
11 DESCRIPTION
The active ingredients of VIMOVO are naproxen which is an NSAID and esomeprazole magnesium which is a Proton Pump Inhibitor (PPI).
VIMOVO (naproxen and esomeprazole magnesium) is combination of a nonsteroidal anti- inflammatory drug and a PPI available as an oval, yellow, multi-layer, delayed-release tablet combining an enteric-coated naproxen core and an immediate-release esomeprazole magnesium layer surrounding the core.
Each strength contains either 375 mg of naproxen and 20 mg of esomeprazole (equivalent to 22.3 mg esomeprazole magnesium trihydrate) or 500 mg of naproxen and 20 mg of esomeprazole (equivalent to 22.3 mg esomeprazole magnesium trihydrate) for oral administration. The inactive ingredients are carnauba wax, colloidal silicon dioxide, croscarmellose sodium, iron oxide yellow, glyceryl monostearate, hypromellose, iron oxide black, magnesium stearate, methacrylic acid copolymer dispersion, methylparaben, polysorbate 80, polydextrose, polyethylene glycol, povidone, propylene glycol, propylparaben, titanium dioxide, and triethyl citrate.
The chemical name for naproxen is (S)-6-methoxy-α-methyl-2-naphthaleneacetic acid. Naproxen has the following structure:
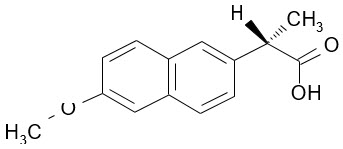
Naproxen has a molecular weight of 230.26 and a molecular formula of C14H14O3.
Naproxen is an odorless, white to off-white crystalline substance. It is lipid soluble, practically insoluble in water at low pH and freely soluble in water at high pH. The octanol/water partition coefficient of naproxen at pH 7.4 is 1.6 to 1.8.
The chemical name for esomeprazole is bis(5-methoxy-2-[(S)-[(4-methoxy-3,5-dimethyl-2- pyridinyl)methyl]sulfinyl]-1H-benzimidazole-1-yl) magnesium trihydrate. Esomeprazole is the S- isomer of omeprazole, which is a mixture of the S- and R- isomers. Its molecular formula is (C17H18N3O3S)2Mg × 3 H2O with molecular weight of 767.2 as a trihydrate and 713.1 on an anhydrous basis. The structural formula is:
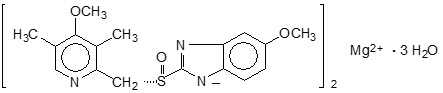
The magnesium salt is a white to slightly colored crystalline powder. It contains 3 moles of water of solvation and is slightly soluble in water.
The stability of esomeprazole magnesium is a function of pH; it rapidly degrades in acidic media, but it has acceptable stability under alkaline conditions. At pH 6.8 (buffer), the half-life of the magnesium salt is about 19 hours at 25°C and about 8 hours at 37°C.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
VIMOVO consists of an immediate-release esomeprazole magnesium layer and an enteric-coated naproxen core. As a result, esomeprazole is released first in the stomach, prior to the dissolution of naproxen in the small intestine. The enteric coating prevents naproxen release at pH levels below 5.5.
The mechanism of action of the naproxen anion, like that of other NSAIDs, is not completely understood but inhibition of cyclooxygenase (COX-1 and COX-2).
VIMOVO has analgesic, anti-inflammatory, and antipyretic properties contributed by the naproxen component. Naproxen is a potent inhibitor of prostaglandin synthesis in vitro. Naproxen concentrations reached during therapy have produced in vivo effects. Prostaglandins sensitize afferent nerves and potentiate the action of bradykinin in inducing pain in animal models. Prostaglandins are mediators of inflammation. Because naproxen is an inhibitor of prostaglandin synthesis, its mode of action may be due to an increase of prostaglandins in peripheral tissues.
Esomeprazole is a proton pump inhibitor that suppresses gastric acid secretion by specific inhibition of the H+/K+-ATPase in the gastric parietal cell. Esomeprazole is protonated and converted in the acidic compartment of the parietal cell forming the active inhibitor, the achiral sulphenamide. By acting specifically on the proton pump, esomeprazole blocks the final step in acid production, thus reducing gastric acidity. This effect is dose-related up to a daily dose of 20 to 40 mg and leads to inhibition of gastric acid secretion.
12.2 Pharmacodynamics
Interaction with Aspirin
In a healthy volunteer study, 10 days of concomitant administration of naproxen 220 mg once-daily with low-dose immediate-release aspirin (81 mg) showed an interaction with the antiplatelet activity of aspirin as measured by % serum thromboxane B2 inhibition at 24 hours following the day 10 dose [98.7% (aspirin alone) vs 93.1% (naproxen and aspirin)]. The interaction was observed even following discontinuation of naproxen on day 11 (while aspirin dose was continued) but normalized by day 13. In the same study, the interaction was greater when naproxen was administered 30 minutes prior to aspirin [98.7% vs 87.7%] and minimal when aspirin was administered 30 minutes prior to naproxen [98.7% vs 95.4%].
Following administration of naproxen 220 mg twice-daily with low-dose immediate-release aspirin (first naproxen dose given 30 minutes prior to aspirin), the interaction was minimal at 24 h following day 10 dose [98.7% vs 95.7%]. However, the interaction was more prominent after discontinuation of naproxen (washout) on day 11 [98.7% vs 84.3%] and did not normalize completely by day 13 [98.5% vs 90.7%] [see Drug Interactions (7)].
Antisecretory Activity
The effect of VIMOVO on intragastric pH was determined in 25 healthy volunteers in one study. Three VIMOVO combinations (naproxen 500 mg combined with either esomeprazole 10, 20, or 30 mg) were administered twice daily over 9 days. The results are shown in the following table:
| Naproxen 500 mg combined with esomeprazole | |||
|---|---|---|---|
| 10 mg | 20 mg | 30 mg | |
| LS Mean (SE) | |||
|
|||
| % Time Gastric pH >4* | 41.1 (3.0) | 71.5 (3.0) | 76.8 (3.0) |
| Coefficient of variation | 55% | 18% | 16% |
Serum Gastrin Effects
The effect of esomeprazole on serum gastrin concentrations was evaluated in approximately 2,700 patients in clinical trials up to 8 weeks and in over 1,300 patients for up to 6-12 months.
The mean fasting gastrin level increased in a dose-related manner. This increase reached a plateau within two to three months of therapy and returned to baseline levels within four weeks after discontinuation of therapy.
Increased gastrin causes enterochromaffin-like cell hyperplasia and increased serum Chromogranin A (CgA) levels. The increased CgA levels may cause false positive results in diagnostic investigations for neuroendocrine tumors. Healthcare providers should temporarily stop esomeprazole treatment at least 14 days before assessing CgA levels and consider repeating the test if initial CgA levels are high.
Enterochromaffin-like (ECL) Cell Effects
In over 1,000 patients treated with esomeprazole (10, 20 or 40 mg/day) up to 6-12 months, the prevalence of ECL cell hyperplasia increased with time and dose. No patient developed ECL cell carcinoids, dysplasia, or neoplasia in the gastric mucosa.
Endocrine Effects
Esomeprazole had no effect on thyroid function when given in oral doses of 20 or 40 mg for 4 weeks. Other effects of esomeprazole on the endocrine system were assessed using omeprazole studies. Omeprazole given in oral doses of 30 or 40 mg for 2 to 4 weeks had no effect on carbohydrate metabolism, circulating levels of parathyroid hormone, cortisol, estradiol, testosterone, prolactin, cholecystokinin or secretin.
Effects on Gastrointestinal Microbial Ecology
Decreased gastric acidity due to any means including proton pump inhibitors, increases gastric counts of bacteria normally present in the gastrointestinal tract. Treatment with proton pump inhibitors may lead to slightly increased risk of gastrointestinal infections such as Salmonella and Campylobacter and, in hospitalized patients, possibly also Clostridium difficile.
12.3 Pharmacokinetics
Absorption
Naproxen
At steady state following administration of VIMOVO twice daily, peak plasma concentrations of naproxen are reached on average 3 hours following both the morning and the evening dose.
Bioequivalence between VIMOVO and enteric-coated naproxen, based on both area under the plasma concentration-time curve (AUC) and maximum plasma concentration (Cmax) of naproxen, has been demonstrated for both the 375 mg and 500 mg doses.
Naproxen is absorbed from the gastrointestinal tract with an in vivo bioavailability of 95%.
Steady-state levels of naproxen are reached in 4 to 5 days.
Esomeprazole
Following administration of VIMOVO twice daily, esomeprazole is rapidly absorbed with peak plasma concentration reached within on average, 0.43 to 1.2 hours, following the morning and evening dose on both the first day of administration and at steady state. The peak plasma concentrations of esomeprazole are higher at steady state compared to on first day of dosing of VIMOVO.
Figure 1 represents the pharmacokinetics of naproxen and esomeprazole following administration of VIMOVO 500 mg/20 mg.
Figure 1: Mean plasma concentrations of naproxen and esomeprazole following single dose administration of VIMOVO (500mg/20 mg)
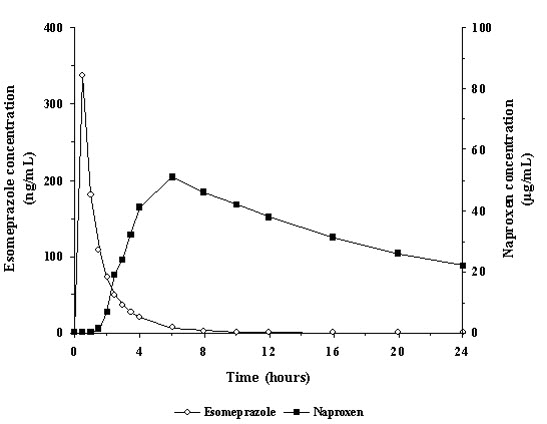
Food Effect
Administration of VIMOVO together with high-fat food in healthy volunteers does not affect the extent of absorption of naproxen but significantly prolongs tmax by 10 hours and decreases peak plasma concentration (Cmax) by about 12%.
Administration of VIMOVO together with high-fat food in healthy volunteers delays tmax of esomeprazole by 1 hour and significantly reduces the extent of absorption, resulting in 52% and 75% reductions of area under the plasma concentration versus time curve (AUC) and peak plasma concentration (Cmax), respectively.
Administration of VIMOVO 30 minutes before high-fat food intake in healthy volunteers does not affect the extent of absorption of naproxen but delays the absorption by about 4 hours and decreases peak plasma concentration (Cmax) by about 17%, but has no significant effect on the rate or extent of esomeprazole absorption compared to administration under fasted conditions [see Dosage and Administration (2)].
Administration of VIMOVO 60 minutes before high-fat food intake in healthy volunteers has no effect on the rate and extent of naproxen absorption; however, increases the esomeprazole AUC by 25% and Cmax by 50% compared to administration under fasted conditions. This increase in esomeprazole Cmax does not raise a safety issue since the approved dosing regimen of esomeprazole at 40 mg QD would result in higher Cmax [see Dosage and Administration (2)].
Therefore, VIMOVO should be taken at least 30 minutes before the meal.
Distribution
Naproxen
Naproxen has a volume of distribution of 0.16 L/kg. At therapeutic levels naproxen is greater than 99% albumin-bound. At doses of naproxen greater than 500 mg/day there is less than proportional increase in plasma levels due to an increase in clearance caused by saturation of plasma protein binding at higher doses (average trough Css 36.5, 49.2 and 56.4 mg/L with 500, 1000 and 1500 mg daily doses of naproxen, respectively). The naproxen anion has been found in the milk of lactating women at a concentration equivalent to approximately 1% of maximum naproxen concentration in plasma [see Use in Specific Populations (8.2)].
Elimination
Metabolism
Naproxen
Naproxen is extensively metabolized in the liver by the cytochrome P450 system (CYP), CYP2C9 and CYP1A2, to 6-0-desmethyl naproxen. Neither the parent drug nor the metabolites induce metabolizing enzymes. Both naproxen and 6-0-desmethyl naproxen are further metabolized to their respective acylglucuronide conjugated metabolites. Consistent with the half- life of naproxen, the area under the plasma concentration time curve increases with repeated dosing of VIMOVO twice daily.
Esomeprazole
Esomeprazole is extensively metabolized in the liver by the CYP enzyme system. The major part of the metabolism of esomeprazole is dependent on the polymorphic CYP2C19, responsible for the formation of the hydroxyl- and desmethyl metabolites of esomeprazole. The remaining part is dependent on another specific isoform CYP3A4, responsible for the formation of esomeprazole sulphone, the main metabolite in plasma. The major metabolites of esomeprazole have no effect on gastric acid secretion.
The area under the plasma esomeprazole concentration-time curve increases with repeated administration of VIMOVO. This increase is dose-dependent and results in a non-linear dose- AUC relationship after repeated administration. An increased absorption of esomeprazole with repeated administration of VIMOVO probably also contributes to the time-and dose-dependency.
Excretion
Naproxen
Following administration of VIMOVO twice daily, the mean elimination half-life for naproxen is approximately 15 hours following the evening dose, with no change with repeated dosing.
The clearance of naproxen is 0.13 mL/min/kg. Approximately 95% of the naproxen from any dose is excreted in the urine, primarily as naproxen (<1%), 6-0-desmethyl naproxen (<1%) or their conjugates (66% to 92%). Small amounts, 3% or less of the administered dose, are excreted in the feces. In patients with renal failure, metabolites may accumulate [see Warnings and Precautions (5.6)].
Esomeprazole
Following administration of VIMOVO twice daily, the mean elimination half-life of esomeprazole is approximately 1 hour following both the morning and evening dose on day 1, with a slightly longer elimination half-life at steady state (1.2-1.5 hours).
Almost 80% of an oral dose of esomeprazole is excreted as metabolites in the urine, the remainder in the feces. Less than 1% of the parent drug is found in the urine.
Specific Populations
Geriatric Patients
There is no specific data on the pharmacokinetics of VIMOVO in patients over age 65.
Studies indicate that although total plasma concentration of naproxen is unchanged, the unbound plasma fraction of naproxen is increased in the elderly, although the unbound fraction is <1% of the total naproxen concentration. Unbound trough naproxen concentrations in elderly subjects have been reported to range from 0.12% to 0.19% of total naproxen concentration, compared with 0.05% to 0.075% in younger subjects. The clinical significance of this finding is unclear, although it is possible that the increase in free naproxen concentration could be associated with an increase in the rate of adverse events per a given dosage in some elderly patients [see Adverse Reactions (6) and Use in Specific Populations (8.5)].
The AUC and Cmax values of esomeprazole were slightly higher (25% and 18%, respectively) in the elderly as compared to younger subjects at steady state. Dosage adjustment for the esomeprazole component based on age is not necessary.
Male and Female Patients
The AUC and Cmax values of esomeprazole were slightly higher (13%) in females than in males at steady state. Dosage adjustment for the esomeprazole component based on gender is not necessary.
Racial or Ethnic Groups
Pharmacokinetic differences due to race have not been studied for naproxen.
Approximately 3% of Caucasians and 15 to 20% of Asians lack a functional CYP2C19 enzyme and are called poor metabolizers. In these individuals the metabolism of esomeprazole is probably mainly catalyzed by CYP3A4. After repeated once-daily administration of 40 mg esomeprazole, the mean area under the plasma concentration-time curve was approximately 100% higher in poor metabolizers than in subjects having a functional CYP2C19 enzyme (extensive metabolizers).
Patients with Renal Impairment
The pharmacokinetics of VIMOVO or naproxen have not been determined in subjects with renal impairment.
Given that naproxen, its metabolites and conjugates are primarily excreted by the kidney, the potential exists for naproxen metabolites to accumulate in the presence of renal impairment. Elimination of naproxen is decreased in patients with severe renal impairment. Naproxen- containing products, including VIMOVO, is not recommended for use in patients with moderate to severe and severe renal impairment (creatinine clearance <30 ml/min) [see Dosage and Administration (2), Warnings and Precautions (5.6), Use in Specific Populations (8.7)].
No studies have been performed with esomeprazole in patients with decreased renal function. Since the kidney is responsible for the excretion of the metabolites of esomeprazole but not for the elimination of the parent compound, the metabolism of esomeprazole is not expected to be changed in patients with impaired renal function.
Patients with Hepatic Impairment
The pharmacokinetics of VIMOVO or naproxen have not been determined in subjects with hepatic impairment.
In patients with severe hepatic impairment, VIMOVO should be avoided due to increase of risk of NSAID associated bleeding and/or renal failure associated with naproxen.
Chronic alcoholic liver disease and probably also other forms of cirrhosis reduce the total plasma concentration of naproxen, but the plasma concentration of unbound naproxen is increased. The implication of this finding for the naproxen component of VIMOVO dosing is unknown but it is prudent to use the lowest effective dose.
The AUCs of esomeprazole in patients with severe hepatic impairment (Child Pugh Class C) have been shown to be 2-3 times higher than in patients with normal liver function. For this reason, it has been recommended that esomeprazole doses not exceed 20 mg daily in patients with severe hepatic impairment. However, there is no dose adjustment necessary for patients with Child Pugh Class A and B for the esomeprazole component of VIMOVO. There is no VIMOVO dosage form that contains less than 20 mg esomeprazole for twice daily dosing [see Dosage and Administration (2), Warnings and Precautions (5.3)].
Drug Interaction Studies
Effect of Naproxen on Other Drugs
Aspirin: When NSAIDs were administered with aspirin, the protein binding of NSAIDs were reduced, although the clearance of free NSAID was not altered. The clinical significance of this interaction is not known. See Table 3 for clinically significant drug interactions of NSAIDs with aspirin [see Drug Interactions (7)].
Effect of Esomeprazole on Other Drugs
Cytochrome P 450 Interactions
Esomeprazole is extensively metabolized in the liver by CYP2C19 and CYP3A4. In vitro and in vivo studies have shown that esomeprazole is not likely to inhibit CYPs 1A2, 2A6, 2C9, 2D6, 2E1 and 3A4. No clinically relevant interactions with drugs metabolized by these CYP enzymes would be expected. Drug interaction studies have shown that esomeprazole does not have any clinically significant interactions with phenytoin, warfarin, quinidine, clarithromycin or amoxicillin.
Clopidogrel: Results from a crossover study in healthy subjects have shown a pharmacokinetic interaction between clopidogrel (300 mg loading dose/75 mg daily maintenance dose) and esomeprazole (40 mg p.o. once daily) when co-administered for 30 days. Exposure to the active metabolite of clopidogrel was reduced by 35% to 40% over this time period. Pharmacodynamic parameters were also measured and demonstrated that the change in inhibition of platelet aggregation was related to the change in the exposure to clopidogrel active metabolite [see Warnings and Precautions (5.22), Drug Interactions (7)].
Mycophenolate Mofetil: Administration of omeprazole 20 mg twice daily for 4 days and a single 1000 mg dose of MMF approximately one hour after the last dose of omeprazole to 12 healthy subjects in a cross-over study resulted in a 52% reduction in the Cmax and 23% reduction in the AUC of MPA [see Drug Interactions (7)].
Cilostazol: Omeprazole acts as an inhibitor of CYP2C19. Omeprazole, given in doses of 40 mg daily for one week to 20 healthy subjects in cross-over study, increased Cmax and AUC of cilostazol by 18% and 26% respectively. Cmax and AUC of one of its active metabolites, 3,4- dihydrocilostazol, which has 4-7 times the activity of cilostazol, were increased by 29% and 69% respectively [see Drug Interactions (7)].
Nelfinavir: Following multiple doses of nelfinavir (1250 mg, twice daily) and omeprazole (40 mg once a day), AUC was decreased by 36% and 92%, Cmax by 37% and 89% and Cmin by 39% and 75% respectively for nelfinavir and main oxidative metabolite, hydroxy-t-butylamide (M8) [see Drug Interactions (7)].
Atazanavir: Following multiple doses of atazanavir (400 mg, once a day) and omeprazole (40 mg, once a day, 2 hr before atazanavir), AUC was decreased by 94%, Cmax by 96%, and Cmin by 95% [see Drug Interactions (7)].
Saquinavir: Elevated serum levels have been reported with an increase in AUC by 82% in Cmax by 75% and in Cmin by 106% following multiple dosing of saquinavir/ritonavir (1000/100 mg) twice a day for 15 days with omeprazole 40 mg once a day co-administered on days 11 to 15 [see Drug Interactions (7)].
Diazepam: Co-administration of esomeprazole 30 mg and diazepam, a CYP2C19 substrate, resulted in a 45% decrease in clearance of diazepam [see Drug Interactions (7)].
Digoxin: Concomitant administration of omeprazole 20 mg once daily and digoxin in healthy subjects increased the bioavailability of digoxin by 10% (30% in two subjects) [see Drug Interactions (7)].
Effect of Other Drugs on Esomeprazole
Because esomeprazole is metabolized by CYP2C19 and CYP3A4, inducers and inhibitors of these enzymes may potentially alter exposure of esomeprazole.
St. John's Wort: In a cross-over study in 12 healthy male subjects, St. John's Wort (300 mg three times daily for 14 days) significantly decreased the systemic exposure of omeprazole in CYP2C19 poor metabolizers (Cmax and AUC decreased by 37.5% and 37.9%, respectively) and extensive metabolizers (Cmax and AUC decreased by 49.6% and 43.9%, respectively) [see Warnings and Precautions (5.25), Drug Interactions (7)].
Voriconazole: Concomitant administration of omeprazole and voriconazole (a combined inhibitor of CYP2C19 and CYP3A4) resulted in more than doubling of the omeprazole exposure. When voriconazole (400 mg every 12 hours for one day, followed by 200 mg once daily for 6 days) was given with omeprazole (40 mg once daily for 7 days) to healthy subjects, the steady-state Cmax and AUC0-24 of omeprazole significantly increased: an average of 2 times (90% CI: 1.8, 2.6) and 4 times (90% CI: 3.3, 4.4), respectively, as compared to when omeprazole was given without voriconazole [see Drug Interactions (7)].
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, and Impairment of Fertility
Carcinogenesis
Naproxen
A 2-year study was performed in rats to evaluate the carcinogenic potential of naproxen at rat doses of 8, 16, and 24 mg/kg/day (0.05, 0.1, and 0.16 times the maximum recommended human daily dose of 1500 mg/day based on a body surface area comparison). The maximum dose used was 0.28 times the highest recommended human dose. No evidence of tumorigenicity was found.
Esomeprazole
The carcinogenic potential of esomeprazole was assessed using omeprazole studies, of which esomeprazole is an enantiomer. In two 24-month oral carcinogenicity studies in rats, omeprazole at daily doses of 1.7, 3.4, 13.8, 44 and 140.8 mg/kg/day (about 0.41 to 34.2 times the human dose of 40 mg/day expressed on a body surface area basis) produced gastric ECL cell carcinoids in a dose-related manner in both male and female rats; the incidence of this effect was markedly higher in female rats, which had higher blood levels of omeprazole. Gastric carcinoids seldom occur in the untreated rat. In addition, ECL cell hyperplasia was present in all treated groups of both sexes. In one of these studies, female rats were treated with 13.8 mg omeprazole/kg/day (about 3.36 times the human dose of 40 mg/day on a body surface area basis) for 1 year, then followed for an additional year without the drug. No carcinoids were seen in these rats. An increased incidence of treatment-related ECL cell hyperplasia was observed at the end of 1 year (94% treated vs 10% controls). By the second year the difference between treated and control rats was much smaller (46% vs 26%) but still showed more hyperplasia in the treated group. Gastric adenocarcinoma was seen in one rat (2%). No similar tumor was seen in male or female rats treated for 2 years. For this strain of rat, no similar tumor has been noted historically, but a finding involving only one tumor is difficult to interpret. A 78-week mouse carcinogenicity study of omeprazole did not show increased tumor occurrence, but the study was not conclusive.
Mutagenesis
Esomeprazole was negative in the Ames mutation test, in the in vivo rat bone marrow cell chromosome aberration test, and the in vivo mouse micronucleus test. Esomeprazole, however, was positive in the in vitro human lymphocyte chromosome aberration test. Omeprazole was positive in the in vitro human lymphocyte chromosome aberration test, the in vivo mouse bone marrow cell chromosome aberration test, and the in vivo mouse micronucleus test.
Impairment of Fertility
The potential effects of esomeprazole on fertility and reproductive performance were assessed using omeprazole studies. Omeprazole at oral doses up to 138 mg/kg/day in rats (about 33.6 times the human dose of 40 mg/day on a body surface area basis) was found to have no effect on reproductive performance of parental animals.
Studies to evaluate the impact of naproxen on male or female fertility have not been completed.
13.2 Animal Toxicology and/or Pharmacology
Naproxen
Reproduction studies have been performed in rats at 20 mg/kg/day (125 mg/m2/day, 0.23 times the maximum recommended human dose), rabbits at 20 mg/kg/day (220 mg/m2/day, 0.27 times the maximum recommended human dose), and mice at 170 mg/kg/day (510 mg/m2/day, 0.28 times the maximum recommended human dose) with no evidence of impaired fertility or harm to the fetus due to the drug. However, animal reproduction studies are not always predictive of human response.
Esomeprazole – Reproduction Studies
Reproduction studies have been performed in rats at oral doses up to 280 mg/kg/day (about 68 times an oral human dose of 40 mg on a body surface area basis) and in rabbits at oral doses up to 86 mg/kg/day (about 42 times an oral human dose of 40 mg on a body surface area basis) and have revealed no evidence of impaired fertility or harm to the fetus due to esomeprazole [see Use in Specific Populations (8.1)].
Esomeprazole – Juvenile Animal Data
A 28-day toxicity study with a 14-day recovery phase was conducted in juvenile rats with esomeprazole magnesium at doses of 70 to 280 mg /kg/day (about 17 to 68 times a daily oral human dose of 40 mg on a body surface area basis). An increase in the number of deaths at the high dose of 280 mg /kg/day was observed when juvenile rats were administered esomeprazole magnesium from postnatal day 7 through postnatal day 35. In addition, doses equal to or greater than 140 mg/kg/day (about 34 times a daily oral human dose of 40 mg on a body surface area basis), produced treatment-related decreases in body weight (approximately 14%) and body weight gain, decreases in femur weight and femur length, and affected overall growth.
Comparable findings described above have also been observed in this study with another esomeprazole salt, esomeprazole strontium, at equimolar doses of esomeprazole.
14 CLINICAL STUDIES
Two randomized, multi-center, double-blind trials (Study 1 and Study 2) compared the incidence of gastric ulcer formation in 428 patients taking VIMOVO and 426 patients taking enteric-coated naproxen. Subjects were at least 18 years of age with a medical condition expected to require daily NSAID therapy for at least 6 months, and, if less than 50 years old, with a documented history of gastric or duodenal ulcer within the past 5 years. The majority of patients were female (67%), white (86%). The majority of patients were 50-69 years of age (83%). Approximately one quarter were on low-dose aspirin.
Studies 1 and 2 showed that VIMOVO given as 500 mg/20 mg twice daily statistically significantly reduced the 6-month cumulative incidence of gastric ulcers compared to enteric- coated naproxen 500 mg twice daily (see Table 6).
Approximately a quarter of the patients in Studies 1 and 2 were taking concurrent low-dose aspirin (≤ 325 mg daily). The results for this subgroup analysis in patients who used aspirin were consistent with the overall findings of the study.
The results at one month, three months, and six months are presented in Table 6.
| Study 1 | Study 2 | |||
|---|---|---|---|---|
| VIMOVO N=218 number (%) | EC-naproxen N=216 number (%) | VIMOVO N=210 number (%) | EC-naproxen N=210 number (%) |
|
|
||||
| 0-1 Month | 3 (1.4) | 28 (13.0) | 4 (1.9) | 21 (10.0) |
| 0-3 Months | 4 (1.8) | 42 (19.4) | 10 (4.8) | 37 (17.6) |
| 0-6 Months* | 9 (4.1) | 50 (23.1) | 15 (7.1) | 51 (24.3) |
In these trials, patients receiving VIMOVO had a mean duration of therapy of 152 days compared to 124 days in patients receiving enteric-coated naproxen alone. A higher proportion of patients taking EC-naproxen (12%) discontinued the study due to upper GI adverse events (including duodenal ulcers) compared to VIMOVO (4%) in both trials [see Adverse Reactions (6)].
The efficacy of VIMOVO in treating the signs and symptoms of osteoarthritis was established in two 12-week randomized, double-blind, placebo-controlled trials in patients with osteoarthritis (OA) of the knee. In these two trials, patients were allowed to remain on low-dose aspirin for cardioprophylaxis. VIMOVO was given as 500 mg/20 mg twice daily. In each trial, patients receiving VIMOVO had significantly better results compared to patients receiving placebo as measured by change from baseline of the WOMAC pain subscale and the WOMAC physical function subscale and a Patient Global Assessment Score.
Based on studies with enteric-coated naproxen, improvement in patients treated for rheumatoid arthritis was demonstrated by a reduction in joint swelling, a reduction in duration of morning stiffness, a reduction in disease activity as assessed by both the investigator and patient, and by increased mobility as demonstrated by a reduction in walking time. In patients with osteoarthritis, the therapeutic action of naproxen has been shown by a reduction in joint pain or tenderness, an increase in range of motion in knee joints, increased mobility as demonstrated by a reduction in walking time, and improvement in capacity to perform activities of daily living impaired by the disease. In patients with ankylosing spondylitis, naproxen has been shown to decrease night pain, morning stiffness and pain at rest.
16 HOW SUPPLIED/STORAGE AND HANDLING
VIMOVO (375 mg naproxen /20 mg esomeprazole magnesium) delayed-release tablets are oval, yellow film-coated tablets printed with 375/20 in black ink, supplied as:
| NDC 75987-031-04 | Bottles of 60 tablets |
VIMOVO (500 mg naproxen /20 mg esomeprazole magnesium) delayed-release tablets are oval, yellow film-coated tablets printed with 500/20 in black ink, supplied as:
| NDC 75987-030-04 | Bottles of 60 tablets |
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Inform patients, families, or caregivers of the following before initiating therapy with VIMOVO and periodically during the course of ongoing therapy.
Cardiovascular Thrombotic Events
Advise patients to be alert for the symptoms of cardiovascular thrombotic events, including chest pain, shortness of breath, weakness, or slurring of speech, and to report any of these symptoms to their health care provider immediately [see Warnings and Precautions (5.1)].
Gastrointestinal Bleeding, Ulceration, and Perforation
Advise patients to report symptoms of ulcerations and bleeding, including epigastric pain, dyspepsia, melena, and hematemesis to their health care provider. In the setting of concomitant use of low-dose aspirin for cardiac prophylaxis, inform patients of the increased risk for and the signs and symptoms of GI bleeding [see Warnings and Precautions (5.2)].
Hepatotoxicity
Inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If these occur, instruct patients to stop VIMOVO and seek immediate medical therapy [see Warnings and Precautions (5.3)].
Heart Failure and Edema
Advise patients to be alert for the symptoms of congestive heart failure including shortness of breath, unexplained weight gain, or edema and to contact their health care provider if such symptoms occur [see Warnings and Precautions (5.5)].
Anaphylactic Reactions
Inform patients of the signs of an anaphylactic reaction (e.g., difficulty breathing, swelling of the face or throat). If these occur, patients should be instructed to seek immediate emergency help [see Contraindications (4), Warnings and Precautions (5.7)].
Serious Skin Reactions, Including DRESS
Advise patients to stop taking VIMOVO immediately if they develop any type of rash or fever and contact their health care provider as soon as possible [see Warnings and Precautions (5.9, 5.10)].
Fetal Toxicity
Inform pregnant women to avoid use of VIMOVO and other NSAIDs starting at 30 weeks gestation because of the risk of the premature closure of the fetal ductus arteriosus. If treatment with VIMOVO is needed for a pregnant woman between about 20 to 30 weeks gestation, advise her that she may need to be monitored for oligohydramnios [see Warnings and Precautions (5.11), Use in Specific Populations (8.1)].
Infertility
Advise females of reproductive potential that NSAIDs, including VIMOVO, may be associated with reversible infertility [see Use in Specific Populations (8.3)].
Gastric Malignancy
To return to their healthcare provider if they have gastric symptoms while taking VIMOVO or after completing treatment [see Warnings and Precautions (5.17)].
Acute Tubulointerstitial Nephritis
Advise patients to report to their health care provider immediately if they experience a decrease in the amount they urinate or have blood in their urine [see Warnings and Precautions (5.18)].
Clostridium difficile-Associated Diarrhea
Advise patients to immediately report and seek care for diarrhea that does not improve. This may be a sign of Clostridium difficile associated diarrhea [see Warnings and Precautions (5.19)].
Bone Fracture
Advise patients to report any sign or symptom of osteoporosis (e.g., recent bone fracture, low bone density) to their health care provider [see Warnings and Precautions (5.20)].
Cutaneous and Systemic Lupus Erythematosus
Advise patients to immediately call their healthcare provider any new or worsening of symptoms associated with cutaneous or systemic lupus erythematosus [see Warnings and Precautions (5.21)].
Cyanocobalamin (Vitamin B-12) Deficiency
Advise patients taking VIMOVO for long periods of time, to report to their healthcare provider if they experience weakness, tiredness, or light-headedness or rapid heartbeat and breathing or pale skin [see Warnings and Precautions (5.23)].
Hypomagnesemia and Mineral Metabolism
Advise patients to report any clinical symptoms that may be associated with hypomagnesemia, hypocalcemia, and/or hypokalemia to their healthcare provider, if they have been receiving VIMOVO for at least 3 months [see Warnings and Precautions (5.24)].
Drug Interactions
- Inform patients that the concomitant use of VIMOVO with other NSAIDs or salicylates (e.g., diflunisal, salsalate) it is not recommended due to the increased risk of gastrointestinal toxicity, and little or no increase in efficacy [see Warnings and Precautions (5.16), Drug Interactions (7)]. Alert patients that NSAIDs may be present in the "over the counter" medications for treatment of colds, fever or insomnia.
- Advise patients to report to their healthcare provider if they start treatment with clopidogrel, St. John's Wort or rifampin; or, if they take high-dose methotrexate [see Warnings and Precautions (5.22, 5.25, 5.27)].
- Inform patients not to use low-dose aspirin concomitantly with VIMOVO until they talk to their health care provider [see Drug Interactions (7)].
Administration
- Inform patients that VIMOVO tablets should be swallowed whole with liquid. Tablets should not be split, chewed, crushed or dissolved. VIMOVO tablets should be taken at least 30 minutes before meals [see Dosage and Administration (2)].
- Patients should be instructed that if a dose is missed, it should be taken as soon as possible. However, if the next scheduled dose is due, the patient should not take the missed dose, and should be instructed to take the next dose on time. Patients should be instructed not to take 2 doses at one time to make up for a missed dose.
- Inform patients that antacids may be used while taking VIMOVO.
VIMOVO is a trademark of the AstraZeneca group of companies.
The VIMOVO trademark has been licensed to Horizon for use in the US. Other trademarks are the property of AstraZeneca respective companies.
Distributed by:
Horizon Medicines, LLC.
Deerfield, IL 60015
VIM-US-PI-004
| Medication Guide VIMOVO (vi-moh-voh) (naproxen and esomeprazole magnesium) delayed-release tablets |
|||
|---|---|---|---|
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 3/2022 | ||
|
What is the most important information I should know about VIMOVO?
|
|||
|
|
||
|
|||
VIMOVO can have other serious side effects. See "What are the possible side effects of VIMOVO?" |
|||
| What is VIMOVO?
VIMOVO is a prescription medicine used in adults and adolescents, 12 years of age and older who weigh at least 84 pounds (38 kg), who need to take naproxen for relief of symptoms of arthritis and who also need to decrease the risk of developing stomach ulcers caused by naproxen. The naproxen in VIMOVO is used for the relief of signs and symptoms of:
Studies in people who take VIMOVO have not extended past 6 months. |
|||
Do not take VIMOVO:
|
|||
Before taking VIMOVO, tell your healthcare provider about all of your medical conditions, including if you:
Especially tell your healthcare provider if you take: |
|||
|
|
||
How should I take VIMOVO?
|
|||
|
What are the possible side effects of VIMOVO?
Get emergency help right away if you get any of the following symptoms: |
|||
|
|
||
| Stop taking VIMOVO and call your healthcare provider right away if you get any of the following symptoms: | |||
|
|
||
| If you take too much VIMOVO, call your healthcare provider or get medical help right away.
These are not all the possible side effects of VIMOVO. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||
How should I store VIMOVO?
|
|||
| What are the ingredients in VIMOVO? Active ingredients: naproxen and esomeprazole magnesium Inactive ingredients: carnauba wax, colloidal silicon dioxide, croscarmellose sodium, iron oxide yellow, glyceryl monostearate, hypromellose, iron oxide black, magnesium stearate, methacrylic acid copolymer dispersion, methylparaben, polysorbate 80, polydextrose, polyethylene glycol, povidone, propylene glycol, propylparaben, titanium dioxide, and triethyl citrate |
|||
| General information about the safe and effective use of VIMOVO.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use VIMOVO for a condition for which it was not prescribed. Do not give VIMOVO to other people, even if they have the same symptoms that you have. It may harm them. You can ask your healthcare provider or pharmacist for information about VIMOVO that is written for health professionals. Distributed by: Horizon Medicines, LLC., Deerfield, IL 60015 For more information, go to www.VIMOVO.com or call 1-866-479-6742. |
|||
VIM-US-MG-004
PRINCIPAL DISPLAY PANEL - 375 mg/20 mg Tablet Bottle Label
NDC 75987-031-04
60 tablets
VIMOVO®
(naproxen and esomeprazole
magnesium)
delayed release tablets
375 mg/20 mg*
*Each tablet contains 22.3 mg
esomeprazole magnesium, equivalent
to 20 mg of esomeprazole.
Dispense the enclosed Medication
Guide to each patient.
Rx only
HORIZON

PRINCIPAL DISPLAY PANEL - 500 mg/20 mg Tablet Bottle Label
NDC 75987-030-04
60 tablets
VIMOVO®
(naproxen and esomeprazole
magnesium)
delayed release tablets
500 mg/20 mg*
*Each tablet contains 22.3 mg
esomeprazole magnesium, equivalent
to 20 mg of esomeprazole.
Dispense the enclosed Medication
Guide to each patient.
Rx only
HORIZON
