DESCRIPTION
Each tablet of promethazine hydrochloride contains 12.5 mg, 25 mg, or 50 mg promethazine hydrochloride. The inactive ingredients present are hydroxypropyl cellulose, lactose monohydrate, low-substituted hydroxypropyl cellulose and magnesium stearate.
Promethazine hydrochloride is a racemic compound; the molecular formula is C 17H 20N 2S HCl and its molecular weight is 320.88.
Promethazine hydrochloride, a phenothiazine derivative, is designated chemically as 10 H-Phenothiazine-10-ethanamine, N, N,α-trimethyl-, monohydrochloride, (±)- with the following structural formula.
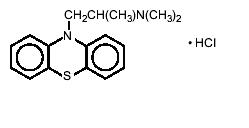
Promethazine hydrochloride occurs as a white to faint yellow, practically odorless, crystalline powder which slowly oxidizes and turns blue on prolonged exposure to air. It is freely soluble in water, in hot dehydrated alcohol, and in chloroform; practically insoluble in ether, in acetone and in ethyl acetate.
CLINICAL PHARMACOLOGY
Promethazine is a phenothiazine derivative which differs structurally from the antipsychotic phenothiazines by the presence of a branched side chain and no ring substitution. It is thought that this configuration is responsible for its relative lack (1/10 that of chlorpromazine) of dopamine antagonist properties.
Promethazine is an H 1receptor blocking agent. In addition to its antihistaminic action, it provides clinically useful sedative and antiemetic effects.
Promethazine is well absorbed from the gastrointestinal tract. Clinical effects are apparent within 20 minutes after oral administration and generally last four to six hours, although they may persist as long as 12 hours. Promethazine is metabolized by the liver to a variety of compounds; the sulfoxides of promethazine and N-demethylpromethazine are the predominant metabolites appearing in the urine.
INDICATIONS AND USAGE
Promethazine Hydrochloride, is useful orally for.
Perennial and seasonal allergic rhinitis.
Vasomotor rhinitis.
Allergic conjunctivitis due to inhalant allergens and foods.
Mild, uncomplicated allergic skin manifestations of urticaria and angioedema.
Amelioration of allergic reactions to blood or plasma.
Dermographism.
Anaphylactic reactions, as adjunctive therapy to epinephrine and other standard measures, after the acute manifestations have been controlled.
Preoperative, postoperative, or obstetric sedation.
Prevention and control of nausea and vomiting associated with certain types of anesthesia and surgery.
Therapy adjunctive to meperidine or other analgesics for control of post-operative pain.
Sedation in both children and adults, as well as relief of apprehension and production of light sleep from which the patient can be easily aroused.
Active and prophylactic treatment of motion sickness.
Antiemetic therapy in postoperative patients.
CONTRAINDICATIONS
Promethazine hydrochloride tablets, USP are contraindicated for use in pediatric patients less than two years of age.
Promethazine hydrochloride tablets, USP are contraindicated in comatose states, and in individuals known to be hypersensitive or to have had an idiosyncratic reaction to promethazine or to other phenothiazines.
Antihistamines are contraindicated for use in the treatment of lower respiratory tract symptoms including asthma.
WARNINGS
PROMETHAZINE HYDROCHLORIDE TABLETS, USP SHOULD NOT BE USED IN PEDIATRIC PATIENTS LESS THAN 2 YEARS OF AGE BECAUSE OF THE POTENTIAL FOR FATAL RESPIRATORY DEPRESSION.
POSTMARKETING CASES OF RESPIRATORY DEPRESSION, INCLUDING FATALITIES, HAVE BEEN REPORTED WITH USE OF PROMETHAZINE HYDROCHLORIDE TABLETS, USP IN PEDIATRIC PATIENTS LESS THAN 2 YEARS OF AGE. A WIDE RANGE OF WEIGHT-BASED DOSES OF PROMETHAZINE HYDROCHLORIDE TABLETS, USP HAVE RESULTED IN RESPIRATORY DEPRESSION IN THESE PATIENTS.
CAUTION SHOULD BE EXERCISED WHEN ADMINISTERING PROMETHAZINE HYDROCHLORIDE TABLETS, USP TO PEDIATRIC PATIENTS 2 YEARS OF AGE AND OLDER. IT IS RECOMMENDED THAT THE LOWEST EFFECTIVE DOSE OF PROMETHAZINE HYDROCHLORIDE BE USED IN PEDIATRIC PATIENTS 2 YEARS OF AGE AND OLDER AND CONCOMITANT ADMINISTRATION OF OTHER DRUGS WITH RESPIRATORY DEPRESSANT EFFECTS BE AVOIDED.
CNS Depression
Promethazine hydrochloride tablets, USP may impair the mental and/or physical abilities required for the performance of potentially hazardous tasks, such as driving a vehicle or operating machinery. The impairment may be amplified by concomitant use of other central-nervous-system depressants such as alcohol, sedatives/hypnotics (including barbiturates), narcotics, narcotic analgesics, general anesthetics, tricyclic antidepressants, and tranquilizers; therefore such agents should either be eliminated or given in reduced dosage in the presence of promethazine hydrochloride (see PRECAUTIONS Information for Patientsand Drug Interactions)
Respiratory Depression
Promethazine hydrochloride tablets, USP may lead to potentially fatal respiratory depression.
Use of promethazine hydrochloride tablets, USP in patients with compromised respiratory function (e.g., COPD, sleep apnea) should be avoided.
Lower Seizure Threshold
Promethazine hydrochloride tablets, USP may lower seizure threshold. It should be used with caution in persons with seizure disorders or in persons who are using concomitant medications, such as narcotics or local anesthetics, which may also affect seizure threshold.
Bone-Marrow Depression
Promethazine hydrochloride tablets, USP should be used with caution in patients with bone-marrow depression. Leukopenia and agranulocytosis have been reported, usually when promethazine hydrochloride has been used in association with other known marrow-toxic agents.
Neuroleptic Malignant Syndrome
A potentially fatal symptom complex sometimes referred to as Neuroleptic Malignant Syndrome (NMS) has been reported in association with promethazine hydrochloride alone or in combination with antipsychotic drugs. Clinical manifestations of NMS are hyperpyrexia, muscle rigidity, altered mental status and evidence of autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis and cardiac dysrhythmias).
The diagnostic evaluation of patients with this syndrome is complicated. In arriving at a diagnosis, it is important to identify cases where the clinical presentation includes both serious medical illness (e.g., pneumonia, systemic infection, etc.) and untreated or inadequately treated extrapyramidal signs and symptoms (EPS). Other important considerations in the differential diagnosis include central anticholinergic toxicity, heat stroke, drug fever and primary central nervous system (CNS) pathology.
The management of NMS should include 1) immediate discontinuation of promethazine hydrochloride, antipsychotic drugs, if any, and other drugs not essential to concurrent therapy, 2) intensive symptomatic treatment and medical monitoring, and 3) treatment of any concomitant serious medical problems for which specific treatments are available. There is no general agreement about specific pharmacological treatment regimens for uncomplicated NMS.
Since recurrences of NMS have been reported with phenothiazines, the reintroduction of promethazine hydrochloride should be carefully considered.
Use in Pediatric Patients
PROMETHAZINE HYDROCHLORIDE TABLETS, USP ARE CONTRAINDICATED FOR USE IN PEDIATRIC PATIENTS LESS THAN TWO YEARS OF AGE.
CAUTION SHOULD BE EXERCISED WHEN ADMINISTERING PROMETHAZINE HYDROCHLORIDE TABLETS, USP TO PEDIATRIC PATIENTS 2 YEARS OF AGE AND OLDER BECAUSE OF THE POTENTIAL FOR FATAL RESPIRATORY DEPRESSION. RESPIRATORY DEPRESSION AND APNEA, SOMETIMES ASSOCIATED WITH DEATH, ARE STRONGLY ASSOCIATED WITH PROMETHAZINE PRODUCTS AND ARE NOT DIRECTLY RELATED TO INDIVIDUALIZED WEIGHT-BASED DOSING, WHICH MIGHT OTHERWISE PERMIT SAFE ADMINISTRATION. CONCOMITANT ADMINISTRATION OF PROMETHAZINE PRODUCTS WITH OTHER RESPIRATORY DEPRESSANTS HAS AN ASSOCIATION WITH RESPIRATORY DESPRESSION, AND SOMETIMES DEATH, IN PEDIATRIC PATIENTS.
ANTIEMETICS ARE NOT RECOMMENDED FOR TREATMENT OF UNCOMPLICATED VOMITING IN PEDIATRIC PATIENTS, AND THEIR USE SHOULD BE LIMITED TO PROLONGED VOMITING OF KNOWN ETIOLOGY. THE EXTRAPYRAMIDAL SYMPTOMS WHICH CAN OCCUR SECONDARY TO PROMETHAZINE HYDROCHLORIDE TABLETS, USP ADMINISTRATION MAY BE CONFUSED WITH THE CNS SIGNS OF UNDIAGNOSED PRIMARY DISEASE, e.g., ENCEPHALOPATHY OR REYE'S SYNDROME. THE USE OF PROMETHAZINE HYDROCHLORIDE TABLETS, USP SHOULD BE AVOIDED IN PEDIATRIC PATIENTS WHOSE SIGNS AND SYMPTOMS MAY SUGGEST REYE'S SYNDROME OR OTHER HEPATIC DISEASES.
Excessively large dosages of antihistamines, including promethazine hydrochloride tablets, USP in pediatric patients may cause sudden death (see OVERDOSAGE).Hallucinations and convulsions have occurred with therapeutic doses and overdoses of promethazine hydrochloride in pediatric patients. In pediatric patients who are acutely ill associated with dehydration, there is an increased susceptibility to dystonias with the use of promethazine hydrochloride.
PRECAUTIONS
General
Drugs having anticholinergic properties should be used with caution in patients with narrow-angle glaucoma, prostatic hypertrophy, stenosing peptic ulcer, pyloroduodenal obstruction, and bladder-neck obstruction.
Promethazine hydrochloride tablets, USP should be used cautiously in persons with cardiovascular disease or with impairment of liver function.
Information for Patients
Promethazine hydrochloride tablets, USP may cause marked drowsiness or impair the mental and/or physical abilities required for the performance of potentially hazardous tasks, such as driving a vehicle or operating machinery. The use of alcohol or other central-nervous-system depressants such as sedatives/hypnotics (including barbiturates), narcotics, narcotic analgesics, general anesthetics, tricyclic antidepressants, and tranquilizers, may enhance impairment ( see WARNINGS-CNS Depressionand PRECAUTIONS-Drug Interactions). Pediatric patients should be supervised to avoid potential harm in bike riding or in other hazardous activities.
Patients should be advised to report any involuntary muscle movements.
Avoid prolonged exposure to the sun.
Repackaged By / Distributed By: RemedyRepack Inc.
625 Kolter Drive, Indiana, PA 15701
(724) 465-8762
Drug Interactions
CNS Depressants- Promethazine hydrochloride tablets, USP may increase, prolong, or intensify the sedative action of other central-nervous-system depressants, such as alcohol, sedatives/hypnotics (including barbiturates), narcotics, narcotic analgesics, general anesthetics, tricyclic antidepressants, and tranquilizers; therefore, such agents should be avoided or administered in reduced dosage to patients receiving promethazine hydrochloride. When given concomitantly with promethazine hydrochloride tablets, USP the dose of barbiturates should be reduced by at least one-half, and the dose of narcotics should be reduced by one-quarter to one-half. Dosage must be individualized. Excessive amounts of promethazine hydrochloride relative to a narcotic may lead to restlessness and motor hyperactivity in the patient with pain; these symptoms usually disappear with adequate control of the pain.
Epinephrine- Because of the potential for promethazine hydrochloride to reverse epinephrine's vasopressor effect, epinephrine should NOT be used to treat hypotension associated with promethazine hydrochloride tablets, USP overdose.
Anticholinergics- Concomitant use of other agents with anticholinergic properties should be undertaken with caution.
Monoamine Oxidase Inhibitors (MAOI)- Drug interactions, including an increased incidence of extrapyramidal effects, have been reported when some MAOI and phenothiazines are used concomitantly. This possibility should be considered with promethazine hydrochloride tablets, USP.
Drug/Laboratory Test Interactions
The following laboratory tests may be affected in patients who are receiving therapy with promethazine hydrochloride:
Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term animal studies have not been performed to assess the carcinogenic potential of promethazine, nor are there other animal or human data concerning carcinogenicity, mutagenicity, or impairment of fertility with this drug. Promethazine was nonmutagenic in the Salmonellatest system of Ames.
Pregnancy
Teratogenic Effects - Pregnancy Category C
Teratogenic effects have not been demonstrated in rat-feeding studies at doses of 6.25 and 12.5 mg/kg of promethazine hydrochloride. These doses are from approximately 2.1 to 4.2 times the maximum recommended total daily dose of promethazine for a 50-kg subject, depending upon the indication for which the drug is prescribed. Daily doses of 25 mg/kg intraperitoneally have been found to produce fetal mortality in rats.
Specific studies to test the action of the drug on parturition, lactation, and development of the animal neonate were not done, but a general preliminary study in rats indicated no effect on these parameters. Although antihistamines have been found to produce fetal mortality in rodents, the pharmacological effects of histamine in the rodent do not parallel those in man. There are no adequate and well-controlled studies of promethazine hydrochloride tablets, USP in pregnant women.
Promethazine hydrochloride tablets, USP should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Labor and Delivery
Promethazine hydrochloride may be used alone or as an adjunct to narcotic analgesics during labor ( DOSAGE AND ADMINISTRATION). Limited data suggest that use of promethazine hydrochloride during labor and delivery does not have an appreciable effect on the duration of labor or delivery and does not increase the risk of need for intervention in the newborn. The effect on later growth and development of the newborn is unknown (see also Nonteratogenic Effects).
Nursing Mothers
It is not known whether promethazine hydrochloride is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from promethazine hydrochloride tablets, USP a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
PROMETHAZINE HYDROCHLORIDE TABLETS, USP ARE CONTRAINDICATED FOR USE IN PEDIATRIC PATIENTS LESS THAN TWO YEARS OF AGE(see WARNINGS-BLACK BOX Warningand Use in Pediatric Patients).
Promethazine hydrochloride tablets, USP should be used with caution in pediatric patients 2 years of age and older (see WARNINGS-Use in Pediatric Patients).
Geriatric Use
Clinical studies of promethazine hydrochloride formulations did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal or cardiac function, and of concomitant disease or other drug therapy.
Sedating drugs may cause confusion and over-sedation in the elderly; elderly patients generally should be started on low doses of promethazine hydrochloride tablets, USP and observed closely.
ADVERSE REACTIONS
Central Nervous System
Drowsiness is the most prominent CNS effect of this drug. Sedation, somnolence, blurred vision, dizziness; confusion, disorientation, and extrapyramidal symptoms such as oculogyric crisis, torticollis, and tongue protrusion; lassitude, tinnitus, incoordination, fatigue, euphoria, nervousness, diplopia, insomnia, tremors, convulsive seizures, excitation, catatonic-like states, hysteria. Hallucinations have also been reported.
Cardiovascular-Increased or decreased blood pressure, tachycardia, bradycardia, faintness.
Dermatologic- Dermatitis, photosensitivity, urticaria.
Hematologic-Leukopenia, thrombocytopenia, thrombocytopenic purpura, agranulocytosis.
Gastrointestinal-Dry mouth, nausea, vomiting, jaundice.
Respiratory-Asthma, nasal stuffiness, respiratory depression (potentially fatal) and apnea (potentially fatal) (see WARNINGS-Respiratory Depression).
Other-Angioneurotic edema. Neuroleptic malignant syndrome (potentially fatal) has also been reported (see WARNINGS-Neuroleptic Malignant Syndrome).
Paradoxical Reactions
Hyperexcitability and abnormal movements have been reported in patients following a single administration of promethazine hydrochloride. Consideration should be given to the discontinuation of promethazine hydrochloride and to the use of other drugs if these reactions occur. Respiratory depression, nightmares, delirium, and agitated behavior have also been reported in some of these patients.
OVERDOSAGE
Signs and symptoms of overdosage with promethazine hydrochloride range from mild depression of the central nervous system and cardiovascular system to profound hypotension, respiratory depression, unconsciousness, and sudden death. Other reported reactions include hyperreflexia, hypertonia, ataxia, athetosis, and extensor-plantar reflexes (Babinski reflex).
Stimulation may be evident, especially in children and geriatric patients. Convulsions may rarely occur. A paradoxical-type reaction has been reported in children receiving single doses of 75 mg to 125 mg orally, characterized by hyperexcitability and nightmares.
Atropine-like signs and symptoms-dry mouth, fixed, dilated pupils, flushing, as well as gastrointestinal symptoms-may occur.
Treatment
Treatment of overdosage is essentially symptomatic and supportive. Only in cases of extreme overdosage or individual sensitivity do vital signs, including respiration, pulse, blood pressure, temperature, and EKG, need to be monitored. Activated charcoal orally or by lavage may be given, or sodium or magnesium sulfate orally as a cathartic. Attention should be given to the reestablishment of adequate respiratory exchange through provision of a patent airway and institution of assisted or controlled ventilation. Diazepam may be used to control convulsions. Acidosis and electrolyte losses should be corrected. Note that any depressant effects of promethazine hydrochloride are not reversed by naloxone. Avoid analeptics which may cause convulsions.
The treatment of choice for resulting hypotension is administration of intravenous fluids, accompanied by repositioning if indicated. In the event that vasopressors are considered for the management of severe hypotension which does not respond to intravenous fluids and repositioning, the administration of norepinephrine or phenylephrine should be considered. EPINEPHRINE SHOULD NOT BE USED, since its use in patients with partial adrenergic blockade may further lower the blood pressure. Extrapyramidal reactions may be treated with anticholinergic antiparkinsonian agents, diphenhydramine, or barbiturates. Oxygen may also be administered.
Limited experience with dialysis indicates that it is not helpful.
DOSAGE AND ADMINISTRATION
Promethazine hydrochloride tablets, USP are contraindicated for children under 2 years of age(see WARNINGS-Black Box Warningand Use in Pediatric Patients).
Allergy
The average oral dose is 25 mg taken before retiring; however, 12.5 mg may be taken before meals and on retiring, if necessary. Single 25-mg doses at bedtime or 6.25 to 12.5 mg taken three times daily will usually suffice. After initiation of treatment in children or adults, dosage should be adjusted to the smallest amount adequate to relieve symptoms. The administration of promethazine hydrochloride in 25-mg doses will control minor transfusion reactions of an allergic nature.
Motion Sickness
The average adult dose is 25 mg taken twice daily. The initial dose should be taken one-half to one hour before anticipated travel and be repeated 8 to 12 hours later, if necessary. On succeeding days of travel, it is recommended that 25 mg be given on arising and again before the evening meal. For children, promethazine hydrochloride tablets, USP, 12.5 to 25 mg, twice daily, may be administered.
Nausea and Vomiting
Antiemetics should not be used in vomiting of unknown etiology in children and adolescents (see WARNINGS-Use in Pediatric Patients).
The average effective dose of promethazine hydrochloride for the active therapy of nausea and vomiting in children or adults is 25 mg. When oral medication cannot be tolerated, the dose should be given parenterally (cf. Promethazine hydrochloride Injection). 12.5- to 25-mg doses may be repeated, as necessary, at 4- to 6-hour intervals.
For nausea and vomiting in children, the usual dose is 0.5 mg per pound of body weight, and the dose should be adjusted to the age and weight of the patient and the severity of the condition being treated.
For prophylaxis of nausea and vomiting, as during surgery and the postoperative period, the average dose is 25 mg repeated at 4- to 6-hour intervals, as necessary.
Sedation
This product relieves apprehension and induces a quiet sleep from which the patient can be easily aroused. Administration of 12.5 to 25 mg promethazine hydrochloride by the oral route or by rectal suppository at bedtime will provide sedation in children. Adults usually require 25 to 50 mg for nighttime, presurgical, or obstetrical sedation.
Pre- and Postoperative Use
Promethazine hydrochloride in 12.5- to 25-mg doses for children and 50-mg doses for adults the night before surgery relieves apprehension and produces a quiet sleep.
For preoperative medication, children require doses of 0.5 mg per pound of body weight in combination with an appropriately reduced dose of narcotic or barbiturate and the appropriate dose of an atropine-like drug. Usual adult dosage is 50 mg promethazine hydrochloride with an appropriately reduced dose of narcotic or barbiturate and the required amount of a belladonna alkaloid.
Postoperative sedation and adjunctive use with analgesics may be obtained by the administration of 12.5 to 25 mg in children and 25- to 50-mg doses in adults.
Promethazine hydrochloride tablets, USP are contraindicated for children under 2 years of age.
HOW SUPPLIED
Promethazine hydrochloride tablets USP, 12.5 mg are white to off-white, round shape, biconvex, uncoated tablets debossed with the logo of "ZC", "01" and bisect on one side and plain on the other side and are supplied as follows:
NDC: 70518-2488-00
PACKAGING: 30 in 1 BLISTER PACK
Keep tightly closed.
Store at 20°C to 25°C (68°F to 77°F) [See USP Controlled Room Temperature].
Protect from light.
Dispense in light-resistant, tight container.
Repackaged and Distributed By:
Remedy Repack, Inc.
625 Kolter Dr. Suite #4 Indiana, PA 1-724-465-8762
Promethazine Hydrochloride Tablets, USP
(proe meth′ a zeen hye″ droe klor′ ide)
This is a summary of the most important information about promethazine. For details, talk to your healthcare professional.
Repackaged By / Distributed By: RemedyRepack Inc.
625 Kolter Drive, Indiana, PA 15701
(724) 465-8762
What Is Promethazine?
Promethazine is an antihistamine which can be taken by mouth as a tablet or syrup, rectally as a suppository, or by injection. It can be used for:
- "hay fever," or, a stuffy runny nose from allergy
- watery, itchy eyes due to inhaled allergies and foods
- mild allergic skin reactions with itching and swelling
- allergic reactions to blood or plasma
- dermographism, a form of hives known as "skin writing"
- serious allergic reactions along with epinephrine and other treatments
- sedation before or after surgery, or during childbirth
- prevention and control of nausea and vomiting after surgery
- along with meperidine (demerol) or other pain medicines
- sedation, relief of anxiety, and production of light sleep
- from which the patient can be easily aroused
- treatment and prevention of motion sickness
Who Should Not Use Promethazine?
Promethazine should not be given to:
- children under two years of age
- patients who are unconscious
- patients who are allergic to promethazine, any of the ingredients in promethazine, or to other phenothiazines
- patients with lung symptoms including asthma
- children who are vomiting unless the vomiting is prolonged and there is a known cause
What Are The Risks?
The following are the major potential risks and side effects of promethazine therapy. However, this list is not complete.
Severe drowsiness and reduced mental alertness.Promethazine may cause drowsiness which may impair your ability to ride a bike, drive a car, or operate machinery. This may be worsened if taken with alcohol or other drugs that also cause central nervous system (CNS) slowing such as sedatives, pain medicines, tranquilizers or certain drugs for depression.
Serious breathing problems.Promethazine should not be used in patients with poor lung function such as chronic obstructive lung disease or breathing problems while sleeping (sleep apnea).
Increased risk of seizures.Promethazine should be used with caution in patients with seizures or who are on other medicines which may also increase the risk of seizures.
Bone-marrow problems and blood cell production.Promethazine should not be used in patients with bone-marrow problems or used with other drugs that affect the bone marrow's production of blood cells.
Neuroleptic malignant syndrome.This potentially deadly syndrome includes symptoms such as fever, muscle rigidity mental changes, changes in pulse or blood pressure, fast heartbeat, increased sweating or irregular heart rhythm.
- The most common side effects aredrowsiness, changes in blood pressure, skin reactions, blood cell changes and breathing problems. Increased excitability or abnormal movements may occur after one dose of promethazine. If they do, consult your doctor about using another medicine.
What Should I Tell My Healthcare Professional?
Before you start taking promethazine,tell your healthcare professional if you:
- have narrow-angle glaucoma
- have an enlarged prostate
- have a stomach ulcer
- have an intestinal blockage
- have a bladder blockage
- have heart problems
- have liver problems
- have breathing or lung problems
- have sleep apnea (breathing problems when sleeping)
- have seizures
- drink alcohol
- are trying to become pregnant, are already pregnant, or are breast-feeding
Can Other Medicines Or Food Affect Promethazine?
Promethazine and certain other medicines can interact with each other. Tell your healthcare professional about all the medicines you take including prescription and non-prescription medicines, vitamins, and herbal supplements. Some medicines may affect how promethazine works or promethazine may affect how your other medicines work. Know the medicines you take. Keep a list of them with you to show your healthcare professional.
Especially tell your healthcare professional if you take:
- medicines that affect your brain such as anti-anxiety medicine, sleeping pills, pain medicines, sedatives, narcotics, antidepressants or tranquilizers
- epinephrine
- a monoamine oxidase inhibitor (MAOI) which is used to treat depression or other mental disorders
- medicines called anticholinergics
Repackaged and Distributed By:
Remedy Repack, Inc.
625 Kolter Dr. Suite #4 Indiana, PA 1-724-465-8762
DRUG: Promethazine Hydrochloride
GENERIC: Promethazine Hydrochloride
DOSAGE: TABLET
ADMINSTRATION: ORAL
NDC: 70518-2488-0
COLOR: white
SHAPE: ROUND
SCORE: Two even pieces
SIZE: 6 mm
IMPRINT: ZC;01
PACKAGING: 30 in 1 BLISTER PACK
ACTIVE INGREDIENT(S):
- PROMETHAZINE HYDROCHLORIDE 12.5mg in 1
INACTIVE INGREDIENT(S):
- LACTOSE MONOHYDRATE
- MAGNESIUM STEARATE
- HYDROXYPROPYL CELLULOSE, UNSPECIFIED
- HYDROXYPROPYL CELLULOSE, LOW SUBSTITUTED
