FULL PRESCRIBING INFORMATION
1 INDICATIONS AND USAGE
Skyla® is indicated to prevent pregnancy for up to 3 years.
Replace the system after 3 years if continued use is desired.
2 DOSAGE AND ADMINISTRATION
2.1 Dosing Over Time
Skyla contains 13.5 mg of levonorgestrel (LNG) released in vivo at a rate of approximately 14 mcg/day after 24 days. This rate decreases progressively to approximately 6 mcg/day after 1 year and to 5 mcg/day after 3 years. The average in vivo release rate of LNG is approximately 8 mcg/day over the first year of use and 6 mcg/day over a period of 3 years. [See Clinical Pharmacology (12.3).]
Skyla must be removed by the end of the third year and can be replaced at the time of removal with a new Skyla if continued contraceptive protection is desired.
Skyla can be physically distinguished from other intrauterine systems (IUSs) by the combination of the visibility of the silver ring on ultrasound and the brown color of the removal threads.
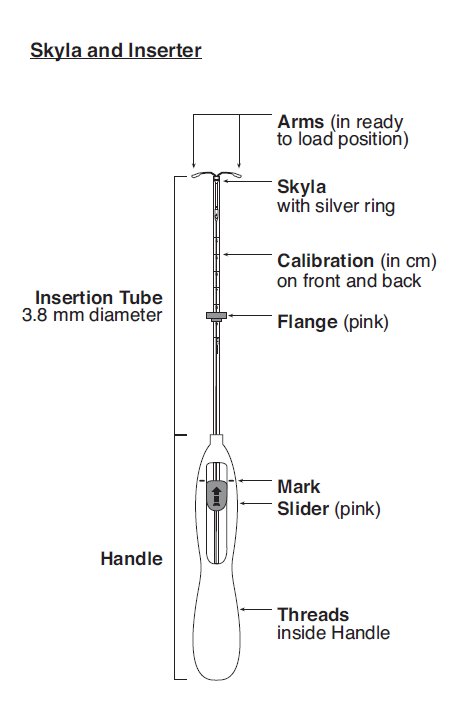
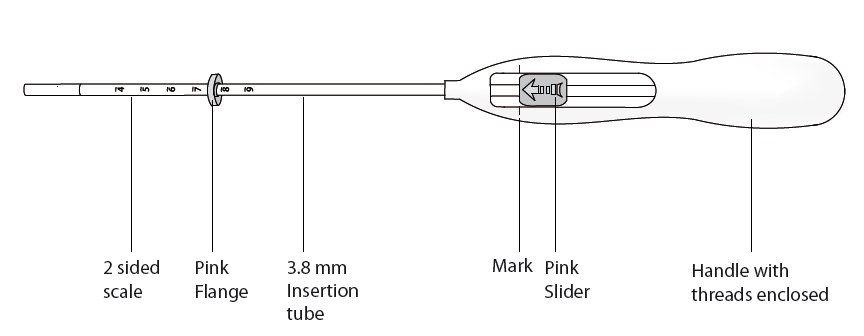
Skyla is supplied in a sterile package within an inserter that enables single-handed loading (see Figure 1). Do not open the package until required for insertion [see Description (11.2)]. Do not use if the seal of the sterile package is broken or appears compromised. Use strict aseptic techniques throughout the insertion procedure [see Warnings and Precautions (5.3)].
2.2. Insertion Instructions
- •
- Obtain a complete medical and social history to determine conditions that might influence the selection of a levonorgestrel-releasing intrauterine system (LNG IUS) for contraception. If indicated, perform a physical examination, and appropriate tests for any forms of genital or other sexually transmitted infections. [See Contraindications (4) and Warnings and Precautions (5.10).] Because irregular bleeding/spotting is common during the first months of Skyla use, exclude endometrial pathology (polyps or cancer) prior to the insertion of Skyla in women with persistent or uncharacteristic bleeding [see Warnings and Precautions (5.8)].
- •
- Follow the insertion instructions exactly as described to ensure proper placement and avoid premature release of Skyla from the inserter. Once released, Skyla cannot be re-loaded.
- •
- Skyla should be inserted by a trained healthcare provider. Healthcare providers should become thoroughly familiar with the insertion instructions before attempting insertion of Skyla.
- •
- Insertion may be associated with some pain and/or bleeding or vasovagal reactions (for example, syncope, bradycardia) or with seizure, especially in patients with a predisposition to these conditions. Consider administering analgesics prior to insertion.
Timing of Insertion
|
Starting Skyla in women not currently using hormonal or intrauterine contraception |
|
|
Switching to Skyla from an oral, transdermal or vaginal hormonal contraceptive |
|
|
Switching to Skyla from an injectable progestin contraceptive |
|
|
Switching to Skyla from a contraceptive implant or another IUS |
|
|
Inserting Skyla after first trimester abortion or miscarriage |
|
|
Inserting Skyla after childbirth or second-trimester abortion or miscarriage | |
|
|
|
Interval insertion following complete involution of the uterus |
|
Tools for Insertion
Note: The inserter provided with Skyla (see Figure 1) and the Insertion Procedure described in this section are not applicable for immediate insertion after childbirth or second-trimester abortion or miscarriage. For immediate insertion, remove Skyla from the inserter by first loading (see Figure 2) and then releasing (see Figure 7) Skyla from the inserter, and insert according to accepted practice.
Preparation for insertion
- •
- Exclude pregnancy and confirm that there are no other contraindications to the use of Skyla.
- •
- Check expiration date of Skyla prior to initiating insertion.
- •
- With the patient comfortably in lithotomy position, do a bimanual exam to establish the size, shape and position of the uterus.
- •
- Gently insert a speculum to visualize the cervix.
- •
- Thoroughly cleanse the cervix and vagina with a suitable antiseptic solution.
- •
- Prepare to sound the uterine cavity. Grasp the upper lip of the cervix with a tenaculum forceps and gently apply traction to stabilize and align the cervical canal with the uterine cavity. Perform a paracervical block if needed. If the uterus is retroverted, it may be more appropriate to grasp the lower lip of the cervix. The tenaculum should remain in position and gentle traction on the cervix should be maintained throughout the insertion procedure.
- •
- Gently insert a uterine sound to check the patency of the cervix, measure the depth of the uterine cavity in centimeters, confirm cavity direction, and detect the presence of any uterine anomaly. If you encounter difficulty or cervical stenosis, use dilatation, and not force, to overcome resistance. If cervical dilatation is required, consider using a paracervical block.
Insertion Procedure
Proceed with insertion only after completing the above steps and ascertaining that the patient is appropriate for Skyla. Ensure use of aseptic technique throughout the entire procedure.
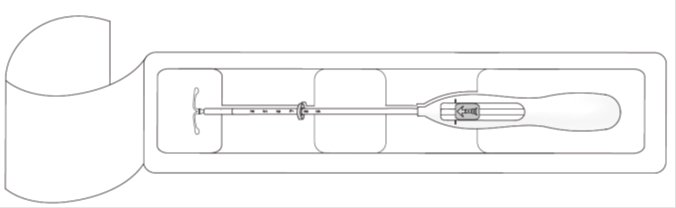
Step 1–Opening of the package
- •
- Open the package (Figure 1). The contents of the package are sterile.
- •
- Using sterile gloves, lift the handle of the sterile inserter and remove from the sterile package.
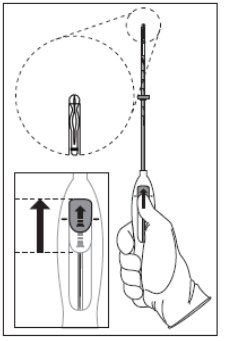
Step 2–Load Skyla into the insertion tube
- •
- Push the slider forward as far as possible in the direction of the arrow thereby moving the insertion tube over the Skyla T-body to load Skyla into the insertion tube (Figure 2). The tips of the arms will meet to form a rounded end that extends slightly beyond the insertion tube.
- •
- Maintain forward pressure with your thumb or forefinger on the slider. DO NOT move the slider downward at this time as this may prematurely release the threads of Skyla. Once the slider is moved below the mark, Skyla cannot be re-loaded.
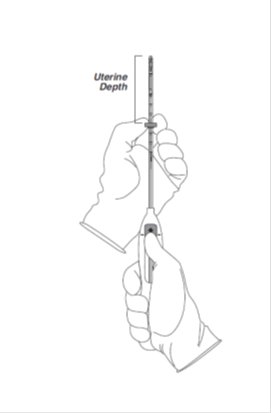
Step 3–Setting the Flange
- •
- Holding the slider in this forward position, set the upper edge of the flange to correspond to the uterine depth (in centimeters) measured during sounding (Figure 3).
Step 4–Skyla is now ready to be inserted
- •
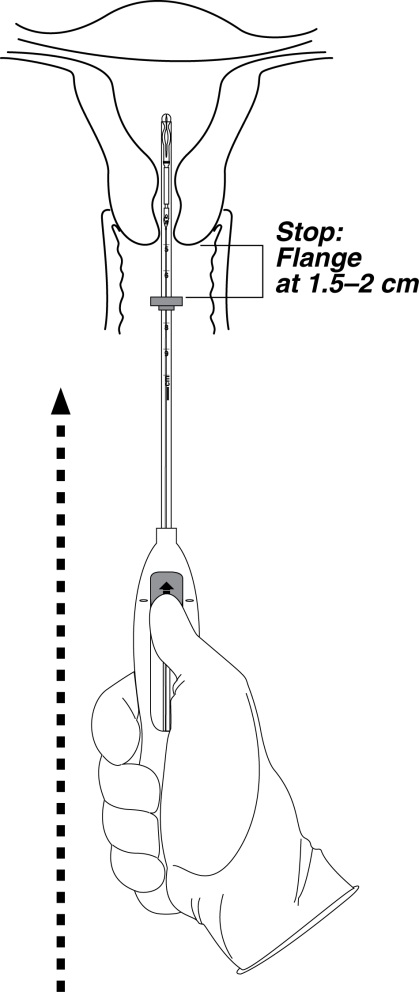
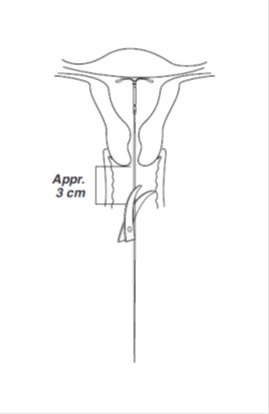
- Continue holding the slider in this forward position. Advance the inserter through the cervix until the flange is approximately 1.5–2 cm from the cervix and then pause (Figure 4).
Do not force the inserter. If necessary, dilate the cervical canal.
Step 5–Open the arms
- •
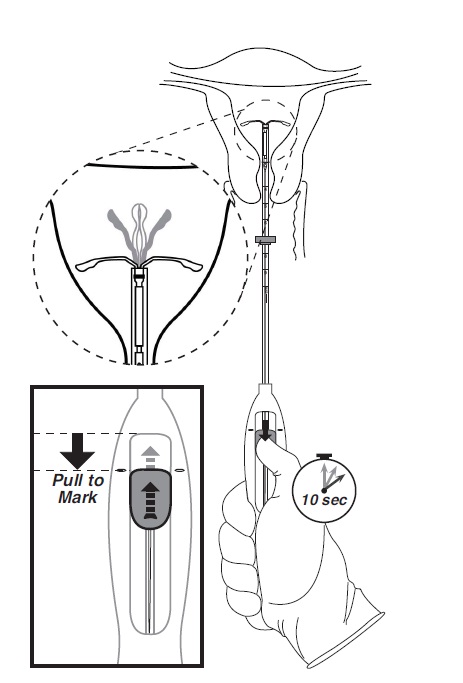
- While holding the inserter steady, move the slider down to the mark to release the arms of Skyla (Figure 5). Wait 10 seconds for the horizontal arms to open completely.
Step 6–Advance to fundal position
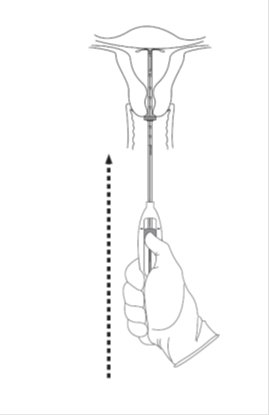
Advance the inserter gently towards the fundus of the uterus until the flange touches the cervix. If you encounter fundal resistance do not continue to advance. Skyla is now in the fundal position (Figure 6). Fundal positioning of Skyla is important to prevent expulsion.
Step 7–Release Skyla and withdraw the inserter
- •
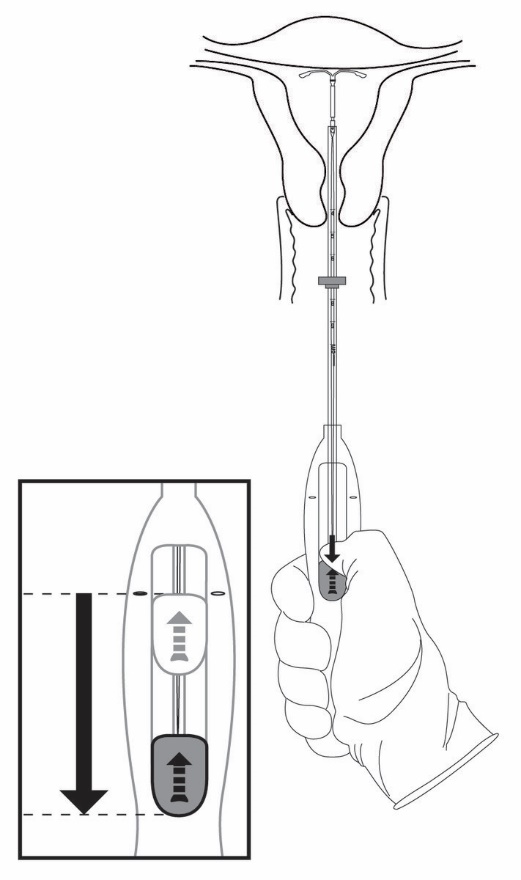
- Holding the entire inserter firmly in place, release Skyla by moving the slider all the way down (Figure 7).
- •
- Continue to hold the slider all the way down while you slowly and gently withdraw the inserter from the uterus.
- •
- Using a sharp, curved scissor, cut the threads perpendicular, leaving about 3 cm visible outside of the cervix [cutting threads at an angle may leave sharp ends (Figure 8)]. Do not apply tension or pull on the threads when cutting to prevent displacing Skyla.
.
- Skyla insertion is now complete. Prescribe analgesics, if indicated. Record the Skyla lot number in the patient records.
Important information to consider during or after insertion
- •
- If you suspect that Skyla is not in the correct position, check placement (for example, using transvaginal ultrasound). Remove Skyla if it is not positioned completely within the uterus. Do not reinsert a removed Skyla.
If there is clinical concern, exceptional pain or bleeding during or after insertion, take appropriate steps (such as physical examination and ultrasound) immediately to exclude perforation.
2.3 Patient Follow-up
Reexamine and evaluate patients 4 to 6 weeks after insertion and once a year thereafter, or more frequently if clinically indicated.
2.4 Removal of Skyla
Timing of Removal
- •
- Skyla should not remain in the uterus after 3 years.
- •
- If pregnancy is not desired, remove Skyla during the first 7 days of the menstrual cycle, provided the woman is still experiencing regular menses. If removal will occur at other times during the cycle or the woman does not experience regular menses, she is at risk of pregnancy, start a new contraceptive method a week prior to removal for these women. [See Dosage and Administration (2.5).]
Removal Procedure
- •
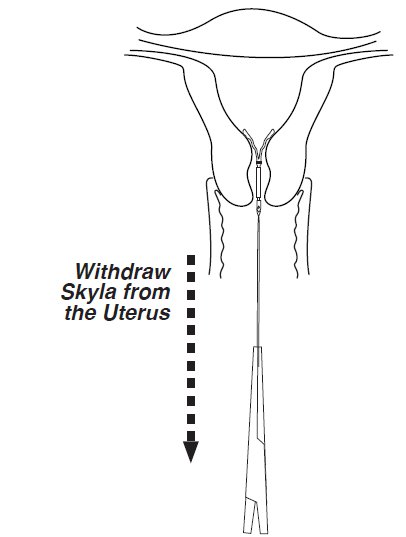
- Remove Skyla by applying gentle traction on the threads with forceps (Figure 9).
- •
- If the threads are not visible, determine location of Skyla by ultrasound [see Warnings and Precautions (5.10)].
- •
- If Skyla is found to be in the uterine cavity on ultrasound exam, it may be removed using a narrow forceps, such as an alligator forceps. This may require dilation of the cervical canal. After removal of Skyla, examine the system to ensure that it is intact.
Removal may be associated with some pain and/or bleeding or vasovagal reactions (for example, syncope, bradycardia) or seizure, especially in patients with a predisposition to these conditions.
2.5 Continuation of Contraception after Removal
- •
- If pregnancy is not desired and if a woman wishes to continue using Skyla, a new system can be inserted immediately after removal any time during the cycle.
- •
- If a patient with regular cycles wants to start a different contraceptive method, time removal and initiation of the new method to ensure continuous contraception. Either remove Skyla during the first 7 days of the menstrual cycle and start the new method immediately thereafter or start the new method at least 7 days prior to removing Skyla if removal is to occur at other times during the cycle.
If a patient with irregular cycles or amenorrhea wants to start a different contraceptive method, start the new method at least 7 days before removal.
3 DOSAGE FORMS AND STRENGTHS
Skyla is a LNG-releasing IUS (a type of intrauterine device, or IUD) consisting of a T-shaped polyethylene frame with a steroid reservoir containing a total of 13.5 mg LNG.
4 CONTRAINDICATIONS
The use of Skyla is contraindicated when one or more of the following conditions exist:
- •
- Pregnancy or suspicion of pregnancy [see Warnings and Precautions (5.2), Use in Specific Populations (8.1)]
- •
- For use as post-coital contraception (emergency contraception)
- •
- Congenital or acquired uterine anomaly including fibroids, that distorts the uterine cavity
- •
- Acute pelvic inflammatory disease (PID) or a history of PID unless there has been a subsequent intrauterine pregnancy [see Warnings and Precautions (5.4)]
- •
- Postpartum endometritis or infected abortion in the past 3 months
- •
- Known or suspected uterine or cervical malignancy
- •
- Known or suspected breast cancer or other progestin-sensitive cancer, now or in the past
- •
- Uterine bleeding of unknown etiology
- •
- Untreated acute cervicitis or vaginitis, including bacterial vaginosis or other lower genital tract infections until infection is controlled
- •
- Acute liver disease or liver tumor (benign or malignant)
- •
- Conditions associated with increased susceptibility to pelvic infections [see Warnings and Precautions (5.4)]
- •
- A previously inserted intrauterine device (IUD) that has not been removed
- •
- Hypersensitivity to any component of this product [see Adverse Reactions (6.2) and Description (11.1)]
5 WARNINGS AND PRECAUTIONS
5.1 Risk of Ectopic Pregnancy
- Evaluate women for ectopic pregnancy if they become pregnant with Skyla in place because the likelihood of a pregnancy being ectopic is increased with Skyla. Approximately one-half of pregnancies that occur with Skyla in place are likely to be ectopic. Also consider the possibility of ectopic pregnancy in the case of lower abdominal pain, especially in association with missed menses or if an amenorrheic woman starts bleeding.
The incidence of ectopic pregnancy in clinical trials with Skyla, which excluded women with a history of ectopic pregnancy, was approximately 0.1% per year. The risk of ectopic pregnancy in women who have a history of ectopic pregnancy and use Skyla is unknown. Women with a previous history of ectopic pregnancy, tubal surgery or pelvic infection carry a higher risk of ectopic pregnancy. Ectopic pregnancy may result in loss of fertility.
5.2 Risks with Intrauterine Pregnancy
If pregnancy occurs while using Skyla, remove Skyla because leaving it in place may increase the risk of spontaneous abortion and preterm labor. Removal of Skyla or probing of the uterus may also result in spontaneous abortion. In the event of an intrauterine pregnancy with Skyla, consider the following:
Septic abortion
In patients becoming pregnant with an IUS in place, septic abortion—with septicemia, septic shock, and death—may occur.
Continuation of pregnancy
If a woman becomes pregnant with Skyla in place and if Skyla cannot be removed or the woman chooses not to have it removed, warn her that failure to remove Skyla increases the risk of miscarriage, sepsis, premature labor and premature delivery. Advise her of isolated reports of virilization of the female fetus following local exposure to LNG during pregnancy with an LNG IUS in place [see Use in Specific Populations (8.1)]. Follow her pregnancy closely and advise her to report immediately any symptom that suggests complications of the pregnancy.
5.3 Sepsis
Severe infection or sepsis, including Group A streptococcal sepsis (GAS), have been reported following insertion of a LNG-releasing IUS. In some cases, severe pain occurred within hours of insertion followed by sepsis within days. Because death from GAS is more likely if treatment is delayed, it is important to be aware of these rare but serious infections. Aseptic technique during insertion of Skyla is essential in order to minimize serious infections such as GAS.
5.4 Pelvic Infection
Pelvic Inflammatory Disease (PID)
Skyla is contraindicated in the presence of known or suspected PID or in women with a history of PID unless there has been a subsequent intrauterine pregnancy [see Contraindications (4)]. IUDs have been associated with an increased risk of PID, most likely due to organisms being introduced into the uterus during insertion. In clinical trials, PID was observed in 0.4% of women overall and occurred more frequently within the first year and most often within the first month after insertion of Skyla.
Promptly examine users with complaints of lower abdominal or pelvic pain, odorous discharge, unexplained bleeding, fever, genital lesions or sores. Remove Skyla in cases of recurrent endometritis or pelvic inflammatory disease, or if an acute pelvic infection is severe or does not respond to treatment.
Women at increased risk for PID
PID is often associated with a sexually transmitted infection (STI), and Skyla does not protect against STI. The risk of PID is greater for women who have multiple sexual partners, and also for women whose sexual partner(s) have multiple sexual partners. Women who have had PID are at increased risk for a recurrence or re-infection. In particular, ascertain whether the woman is at increased risk of infection (for example, leukemia, acquired immune deficiency syndrome [AIDS], intravenous drug abuse).
Actinomycosis
Actinomycosis has been associated with IUDs. Remove Skyla from symptomatic women and treat with antibiotics. The significance of actinomyces-like organisms on Pap smear in an asymptomatic IUD user is unknown, and so this finding alone does not always require Skyla removal and treatment. When possible, confirm a Pap smear diagnosis with cultures.
5.5 Perforation
Perforation (total or partial, including penetration/embedment of Skyla in the uterine wall or cervix) may occur most often during insertion, although the perforation may not be detected until sometime later. The incidence of perforation during clinical trials was < 0.1%.
The risk of uterine perforation is increased in women who have recently given birth, and in women who are breastfeeding at the time of insertion. In a large postmarketing safety study conducted in the US, the risk of uterine perforation was highest when insertion occurred within ≤ 6 weeks postpartum, and also higher with breastfeeding at the time of insertion [see Adverse Reactions (6.2)].
The risk of perforation may be increased if Skyla is inserted when the uterus is fixed, retroverted or not completely involuted.
If perforation occurs, locate and remove Skyla. Surgery may be required. Delayed detection or removal of Skyla in case of perforation may result in migration outside the uterine cavity, adhesions, peritonitis, intestinal perforations, intestinal obstruction, abscesses and erosion of adjacent viscera. In addition, perforation may reduce contraceptive efficacy and result in pregnancy.
5.6 Expulsion
Partial or complete expulsion of Skyla may occur resulting in the loss of efficacy. Expulsion may be associated with symptoms of bleeding or pain, or it may be asymptomatic and go unnoticed. Skyla typically decreases menstrual bleeding over time; therefore, an increase of menstrual bleeding may be indicative of an expulsion. Consider further diagnostic imaging, such as x-ray, if expulsion is suspected based on ultrasound [see Warnings and Precautions (5.10)]. In clinical trials, a 5-year expulsion rate of 3.5% (59 out of 1,690 subjects) was reported.
The risk of expulsion is increased with insertions immediately after delivery and appears to be increased with insertion after second-trimester abortion based on limited data. In a large postmarketing safety study conducted in the US, the risk of expulsion was lower with breastfeeding status [see Adverse Reactions (6.2)].
Remove a partially expelled Skyla. If expulsion has occurred, a new Skyla can be inserted any time the provider can be reasonably certain the woman is not pregnant.
5.7 Ovarian Cysts
Because the contraceptive effect of Skyla is mainly due to its local effects within the uterus, ovulatory cycles with follicular rupture usually occur in women of fertile age using Skyla. Ovarian cysts (reported as adverse reactions if they were abnormal, non-functional cysts and/or had a diameter >3 cm on ultrasound examination) were reported at least once over the course of clinical trials in 13.2% of women using Skyla, and 0.3% of subjects discontinued because of an ovarian cyst. Most ovarian cysts are asymptomatic, although some may be accompanied by pelvic pain or dyspareunia. In most cases the ovarian cysts disappear spontaneously during two to three months observation. Evaluate persistent ovarian cysts. Surgical intervention is not usually required.
5.8 Bleeding Pattern Alterations
Skyla can alter the bleeding pattern and result in spotting, irregular bleeding, heavy bleeding, oligomenorrhea and amenorrhea. During the first 3–6 months of Skyla use, the number of bleeding and spotting days may be higher and bleeding patterns may be irregular. Thereafter, the number of bleeding and spotting days usually decreases but bleeding may remain irregular.
In Skyla clinical trials, amenorrhea developed by the end of the first year of use in approximately 6% of Skyla users. A total of 77 subjects out of 1,672 (4.6%) discontinued due to uterine bleeding complaints. Table 2 shows the bleeding patterns as documented in the Skyla clinical trials based on 90-day reference periods. Table 3 shows the number of bleeding and spotting days based on 28-day cycle equivalents.
|
Skyla |
First 90 days
|
Second 90 days
|
End of year 1
|
End of year 3
|
|
Amenorrhea1 |
<1% |
3% |
6% |
12% |
|
Infrequent bleeding2 |
8% |
19% |
20% |
22% |
|
Frequent bleeding3 |
31% |
12% |
8% |
4% |
|
Prolonged bleeding4 |
55% |
14% |
6% |
2% |
|
Irregular bleeding5 |
39% |
25% |
18% |
15% |
1Defined as subjects with no bleeding/spotting throughout the 90-day reference period
2Defined as subjects with 1 or 2 bleeding/spotting episodes in the 90-day reference period
3Defined as subjects with more than 5 bleeding/spotting episodes in the 90-day reference period
4Defined as subjects with bleeding/spotting episodes lasting more than 14 days in the 90-day reference period. Subjects with prolonged bleeding may also be included in one of the other categories (excluding amenorrhea)
5Defined as subjects with 3 to 5 bleeding/spotting episodes and less than 3 bleeding/spotting-free intervals of 14 or more days.
|
28-day Cycle Equivalent |
Cycle 1 N=1,588 |
Cycle 4 N=1,535 |
Cycle 7 N=1,468 |
Cycle 13 N=1,345 |
Cycle 39 N=781 |
|
Days on treatment |
1–28 |
85–112 |
169–196 |
337–364 |
1065–1092 |
|
Mean (SD) |
Mean (SD) |
Mean (SD) |
Mean (SD) |
Mean (SD) |
|
|
Number of bleeding days |
7.3 (5.6) |
3.5 (3.4) |
2.8 (3.1) |
2.1 (2.7) |
1.4 (2.1) |
|
Number of spotting days |
9.2 (6.1) |
4.8 (4.4) |
3.8 (3.6) |
3.3 (3.1) |
2.7 (2.7) |
If a significant change in bleeding develops during prolonged use, take appropriate diagnostic measures to rule out endometrial pathology. Consider the possibility of pregnancy if menstruation does not occur within six weeks of the onset of a previous menstruation. Once pregnancy has been excluded, repeated pregnancy tests are generally not necessary in amenorrheic women unless indicated, for example, by other signs of pregnancy or by pelvic pain.
5.9 Breast Cancer
Women who currently have or have had breast cancer, or have a suspicion of breast cancer, should not use hormonal contraception, including Skyla because some breast cancers are hormone-sensitive [see Contraindications (4)].
Spontaneous reports of breast cancer have been received during postmarketing experience with a LNG-releasing IUS. Observational studies of the risk of breast cancer with use of a LNG-releasing IUS do not provide conclusive evidence of increased risk.
5.10 Clinical Considerations for Use and Removal
Use Skyla with caution after careful assessment if any of the following conditions exist, and consider removal of the system if any of them arise during use:
- •
- Coagulopathy or use of anticoagulants
- •
- Migraine, focal migraine with asymmetrical visual loss or other symptoms indicating transient cerebral ischemia
- •
- Exceptionally severe headache
- •
- Marked increase of blood pressure
- •
- Severe arterial disease such as stroke or myocardial infarction
In addition, consider removing Skyla if any of the following conditions arise during use:
- •
- Uterine or cervical malignancy
- •
- Jaundice
- •
- If the threads are not visible or are significantly shortened they may have broken or retracted into the cervical canal or uterus. Consider the possibility that the system may have been displaced, (for example, expelled or perforated the uterus) [see Warnings and Precautions (5.5, 5.6)]. Exclude pregnancy and verify the location of Skyla, for example, by sonography, X-ray, or by gentle exploration of the cervical canal with a suitable instrument. If Skyla is displaced, remove it. A new Skyla may be inserted at that time or during the next menses if it is certain that conception has not occurred. If Skyla is in place with no evidence of perforation, no intervention is indicated.
5.11 Magnetic Resonance Imaging (MRI) Safety Information
Non-clinical testing has demonstrated that Skyla is MR Conditional. A patient with Skyla can be safely scanned in an MR system meeting the following conditions:
- •
- Static magnetic field of 3.0 T or less
- •
- Maximum spatial field gradient of 36,000 gauss/cm (360 T/m)
- •
- Maximum MR system reported, whole body averaged specific absorption rate (SAR) of 4W/kg (First Level Controlled Operating Mode)
Under the scan conditions defined above, the Skyla IUS is expected to produce a maximum temperature rise of less than 2°C after 15 minutes of continuous scanning.
In non-clinical testing, the image artifact caused by the IUS extended up to 5 mm from the IUS when imaged with a gradient echo pulse sequence and a 3.0 T MRI system.
6 ADVERSE REACTIONS
The following serious or otherwise important adverse reactions are discussed elsewhere in the labeling:
- •
- Ectopic Pregnancy [see Warnings and Precautions (5.1)]
- •
- Intrauterine Pregnancy [see Warnings and Precautions (5.2)]
- •
- Group A Streptococcal Sepsis (GAS) [see Warnings and Precautions (5.3)]
- •
- Pelvic Inflammatory Disease [see Warnings and Precautions (5.4)]
- •
- Perforation [see Warnings and Precautions (5.5)]
- •
- Expulsion [see Warnings and Precautions (5.6)]
- •
- Ovarian Cysts [see Warnings and Precautions (5.7)]
- •
- Bleeding Pattern Alterations [see Warnings and Precautions (5.8)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The data described below reflect exposure to Skyla in 1,672 patients in two contraception studies, including 1,383 exposed for one year and 993 who completed the three year studies. The population was generally healthy, 18 to 40-year old females requesting contraception and predominately Caucasian (82.6%). The data cover more than 40,000 cycles of exposure. The frequencies of reported adverse drug reactions represent crude incidences.
Most common adverse reactions (occurring in ≥ 5% users) were increased bleeding (7.8%), vulvovaginitis (20.2%), abdominal/pelvic pain (18.9%), acne/seborrhea (15.0%), ovarian cyst (13.2%), headache (12.4%), dysmenorrhea (8.6%), breast pain/discomfort (8.6%) and nausea (5.5%).
In the contraception studies, 18% discontinued prematurely due to an adverse reaction. The most common adverse reactions leading to discontinuation (in >1% of users) were uterine bleeding complaints (4.6%), device expulsion (3.2%), acne/seborrhea (2.9%), abdominal pain (2.5%) dysmenorrhea/uterine spasms (2.0%) and pelvic pain (1.8%).
Other common adverse reactions (occurring in ≥ 1% users) by System Organ Class (SOC): The frequencies of adverse reactions observed in clinical trials are summarized in Table 4 by SOC (presented as crude incidences).
|
System Organ Class |
Adverse Reaction |
Incidence (%)
|
|
Reproductive System and Breast Disorders |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Gastrointestinal Disorders |
|
|
|
|
|
|
Skin and Subcutaneous |
|
|
|
|
|
|
Nervous System Disorders |
|
|
|
|
|
|
Psychiatric Disorders |
|
|
6.2 Postmarketing Experience
The following adverse reactions have been identified during post approval use of LNG-releasing IUSs. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- •
- Arterial thrombotic and venous thromboembolic events, including cases of pulmonary embolism, deep vein thrombosis and stroke
- •
- Device breakage
- •
- Hypersensitivity (including rash, urticaria, and angioedema)
- •
- Increased blood pressure
Adverse Reactions from Postmarketing Spontaneous Reports
The following adverse reactions have been identified during post-approval use of LNG-releasing IUSs. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- •
- Arterial thrombotic and venous thromboembolic events, including cases of pulmonary embolism, deep vein thrombosis and stroke
- •
- Device breakage
- •
- Hypersensitivity (including rash, urticaria, and angioedema)
- •
- Increased blood pressure
Reported Adverse Reactions from Postmarketing Studies
Assessment of Perforation and Expulsion of Intrauterine Devices (APEX IUD) Study
APEX IUD was a large US retrospective cohort study to assess the impact of breastfeeding and timing of postpartum IUD insertion on uterine perforation and IUD expulsion. The analyses included a total of 326,658 insertions, 30% (97,824 insertions) of which were performed in women with a delivery in the previous 12 months. For insertions performed in women who had delivered ≤ 52 weeks before IUD insertion, the majority of postpartum insertions, 57.3% (56,047 insertions) occurred between 6 and 14 weeks postpartum. Breastfeeding data were available in 94,817 insertions performed in women 52 weeks or less after delivery.
The study results indicated that the risk of uterine perforation was highest in women with IUD insertion ≤ 6 weeks postpartum. Immediate postpartum insertion (0–3 days) findings are limited due to the relatively small number of insertions occurring within this time interval. Women who were breastfeeding at the time of insertion were at 33% higher risk of perforation (adjusted hazard ratio [HR]=1.33, 95% confidence interval [CI]: 1.07–1.64) compared to women who were not breastfeeding at the time of insertion. Progressively lower risk of uterine perforation was observed in postpartum time windows beyond 6 weeks, in both breastfeeding and not breastfeeding women. Table 5 presents the uterine perforation rates for LNG IUS stratified by breastfeeding status and postpartum interval.
|
Breastfeeding at time of insertion |
Not breastfeeding at time of insertion |
|||
|
Postpartum interval at time of insertion |
Number of events/ insertions |
Uterine perforation rate per 1,000 insertions |
Number of events/ insertions |
Uterine perforation rate |
|
0 to 3 days |
8/1,896 |
4.22 |
0/277 |
0.00 |
|
4 days to ≤ 6 weeks |
120/10,735 |
11.18 |
28/2,377 |
11.78 |
|
> 6 to ≤ 14 weeks |
268/29,677 |
9.03 |
30/12,011 |
6.66 |
|
> 14 to ≤ 52 weeks |
43/6,139 |
7.00 |
22/9,089 |
2.42 |
|
> 52 weeks or no delivery |
no data available |
243/184,733 |
1.32 |
|
1Uterine perforation includes both complete and partialperforation
Risk of expulsion was variable over the postpartum intervals through 52 weeks. Women who were breastfeeding were at 28% lower risk of IUD expulsion (adjusted HR=0.72, 95% CI: 0.64-0.80) compared to women who were not breastfeeding at time of insertion. Table 6 presents the IUD expulsion rates for LNG IUS stratified by breastfeeding status and postpartum interval.
|
Breastfeeding at time of insertion |
Not breastfeeding at time of insertion |
|||
|
Postpartum interval at time of insertion |
Number of events/ insertions |
Expulsion rate |
Number of events/ insertions |
Expulsion rate |
|
0 to 3 days |
187/1,896 |
98.63 |
12/277 |
43.32 |
|
4 days to ≤ 6 weeks |
185/10,735 |
17.23 |
52/2,377 |
21.88 |
|
> 6 to ≤ 14 weeks |
421/29,677 |
14.19 |
306/12,011 |
25.48 |
|
> 14 to ≤ 52 weeks |
120/6,139 |
19.55 |
273/9,089 |
30.04 |
|
> 52 weeks or no delivery |
no data available |
5,481/184,733 |
29.67 |
|
1Expulsion includes both complete and partial expulsion
7 DRUG INTERACTIONS
No drug-drug interaction studies have been conducted with Skyla.
Drugs or herbal products that induce or inhibit LNG metabolizing enzymes, including CYP3A4, may decrease or increase, respectively, the serum concentrations of LNG during the use of Skyla. However, the contraceptive effect of Skyla is mediated via the direct release of LNG into the uterine cavity and is unlikely to be affected by drug interactions via enzyme induction or inhibition.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
The use of Skyla is contraindicated in pregnancy or with a suspected pregnancy and Skyla may cause adverse pregnancy outcomes [see Contraindications (4), Warnings and Precautions (5.1, 5.2)]. If a woman becomes pregnant with Skyla in place, the likelihood of ectopic pregnancy is increased and there is an increased risk of miscarriage, sepsis, premature labor, and premature delivery. Remove Skyla, if possible, if pregnancy occurs in a woman using Skyla. If Skyla cannot be removed, follow the pregnancy closely [see Warnings and Precautions (5.1, 5.2)].
There have been isolated cases of virilization of the external genitalia of the female fetus following local exposure to LNG during pregnancy with an LNG IUS in place. Animal reproduction studies have not been conducted with Skyla.
8.2 Lactation
Risk Summary
Published studies report the presence of LNG in human milk. Small amounts of progestins (approximately 0.1% of the total maternal doses) were detected in the breast milk of nursing mothers who used other LNG-releasing IUSs, resulting in exposure of LNG to the breastfed infants. There are no reports of adverse effects in breastfed infants with maternal use of progestin-only contraceptives. Isolated cases of decreased milk production have been reported with a LNG-releasing IUS. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for Skyla and any potential adverse effects on the breastfed child from Skyla or from the underlying maternal condition.
11 DESCRIPTION
Skyla (levonorgestrel-releasing intrauterine system) contains 13.5 mg of LNG, a progestin, and is intended to provide an initial release rate of approximately14 mcg/day of LNG after 24 days.
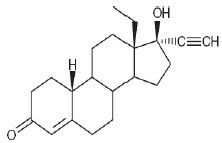
Levonorgestrel USP, (-)-13-Ethyl-17-hydroxy-18,19-dinor-17α-pregn-4-en-20-yn-3-one, the active ingredient in Skyla, has a molecular weight of 312.4, a molecular formula of C21H28O2, and the following structural formula:
11.1 Skyla
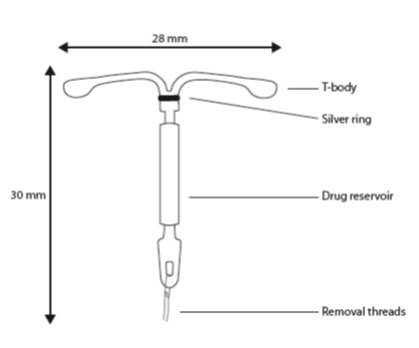
Skyla consists of a T-shaped polyethylene frame (T-body) with a steroid reservoir (hormone elastomer core) around the vertical stem. The white T-body has a loop at one end of the vertical stem and two horizontal arms at the other end. The reservoir consists of a whitish or pale yellow cylinder, made of a mixture of LNG and silicone (polydimethylsiloxane), containing a total of 13.5 mg LNG. The reservoir is covered by a semi-opaque silicone membrane, composed of polydimethylsiloxane and colloidal silica. A ring composed of 99.95% pure silver is located at the top of the vertical stem close to the horizontal arms and is visible by ultrasound. The polyethylene of the T-body is compounded with barium sulfate, which makes it radiopaque. A monofilament brown polyethylene removal thread is attached to a loop at the end of the vertical stem of the T-body. The polyethylene of the removal thread contains iron oxide as a colorant (see Figure 10).
The components of Skyla, including its packaging, are not manufactured using natural rubber latex.
11.2 Inserter
Skyla is packaged sterile within an inserter. The inserter (Figure 11), which is used for insertion of Skyla into the uterine cavity, consists of a symmetric two-sided body and slider that are integrated with flange, lock, pre-bent insertion tube and plunger. The outer diameter of the insertion tube is 3.8 mm. The vertical stem of Skyla is loaded in the insertion tube at the tip of the inserter. The arms are pre-aligned in the horizontal position. The removal threads are contained within the insertion tube and handle. Once Skyla has been placed, the inserter is discarded.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
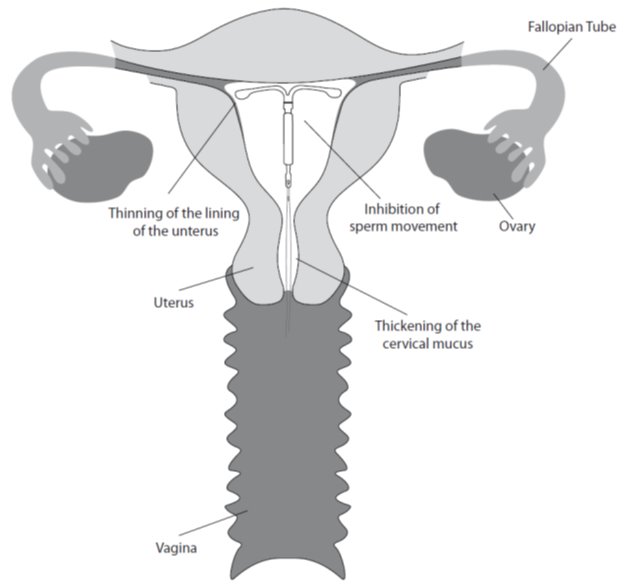
The local mechanism by which continuously released LNG contributes to the contraceptive effectiveness of Skyla has not been conclusively demonstrated. Studies of Skyla and similar LNG IUS prototypes have suggested several mechanisms that prevent pregnancy: thickening of cervical mucus preventing passage of sperm into the uterus, inhibition of sperm capacitation or survival, and alteration of the endometrium.
12.2 Pharmacodynamics
Skyla has mainly local progestogenic effects in the uterine cavity. The local concentrations of LNG lead to morphological changes including stromal pseudodecidualization, glandular atrophy, a leukocytic infiltration and a decrease in glandular and stromal mitoses.
In clinical trials with Skyla, ovulation was assessed based on serum progesterone values >2.5 ng/mL in one study and serum progesterone values >2.5 ng/mL together with serum estradiol levels <27.24 pg/mL in another study. Evidence of ovulation by these criteria was seen in 34 out of 35 women in the first year, in 26 out of 27 women in the second year, and in all 26 women in the third year.
12.3 Pharmacokinetics
Absorption
Low doses of LNG are administered into the uterine cavity with the Skyla intrauterine delivery system. The in vivo release rate is approximately 14 mcg/day after 24 days and is reduced to approximately 10 mcg/day after 60 days and then declines progressively to approximately 6 mcg/day after 1 year and 5 mcg/day after 3 years. The average LNG in vivo release rate is approximately 8 mcg/day over the first year of use and 6 mcg/day over the period of 3 years.
In a subset of 7 subjects, the maximum observed serum LNG concentration (mean ±SD) was 192 ± 105 pg/mL, reached after 2 days (median) of Skyla insertion. Thereafter, the LNG serum concentrations (mean ±SD) at year 1, 2, and 3 were 77 ± 21 pg/mL, 62 ± 38 pg/mL, and 72 ± 29 pg/mL, respectively. A population pharmacokinetic evaluation based on a broader database (>1000 patients) showed similar concentration data of 168 ± 46 pg/mL at 7 days after placement. Thereafter, LNG serum concentrations decline slowly to a value 61 ± 19 pg/mL after 3 years.
Distribution
The apparent volume of distribution of LNG is reported to be approximately 1.8 L/kg. LNG is bound non-specifically to serum albumin and specifically to sex hormone binding globulin (SHBG). Accordingly, changes in the concentration of SHBG in serum result in an increase (at higher SHBG concentration) or a decrease (at lower SHBG concentration) of the total LNG concentration in serum. In a subset of 7 subjects, the concentration of SHBG declined by a mean value of 18% within 2 weeks after insertion of Skyla and remained relatively stable over the 3 year period of use. Less than 2% of the circulating LNG is present as free steroid.
Elimination
Following intravenous administration of 0.09 mg LNG to healthy volunteers, the total clearance of LNG is approximately 1 mL/min/kg and the elimination half-life is approximately 20 hours. Metabolic clearance rates may differ among individuals by several-fold, and this may account in part for wide individual variations in LNG concentrations seen in individuals using LNG–containing contraceptive products.
Metabolism
- Following absorption, LNG is extensively metabolized. The most important metabolic pathways are the reduction of the Δ4-3-oxo group and hydroxylations at positions 2α, 1β and 16β, followed by conjugation. Significant amounts of conjugated and unconjugated 3α, 5β- are also present in serum, along with much smaller amounts of 3α, 5α-tetrahydrolevonorgestrel and 16β-hydroxylevonorgestrel. CYP3A4 is the main enzyme involved in the oxidative metabolism of LNG.
Specific Populations
Pediatric: Safety and efficacy of Skyla have been established in women of reproductive age. Use of this product before menarche is not indicated.
In a one-year phase 3 study in post-menarcheal female adolescents (mean age 16.2, range 12 to 18 years) using Skyla, the population pharmacokinetic analysis of 278 adolescents showed mean estimated LNG serum concentrations slightly higher (approximately 10%) in adolescents compared to prior data in adults. This correlates to the generally lower body weight in adolescents. The ranges estimated for adolescents lie within the ranges estimated for adults.
Geriatric: Skyla has not been studied in women over age 65 and is not approved for use in this population.
Race: A three-year phase 3 study in the Asian-Pacific region (93% Asian women, the majority of whom were Chinese, 7% other ethnicities) using Skyla was performed. The population pharmacokinetic analysis of the Asian (Chinese) population in this study showed that estimated LNG serum concentrations in Asian women were slightly higher (approximately 4 to 16%) than those in another phase 3 study which was performed in mainly Caucasian women (79.7%). This slightly higher exposure might be explained by the lower body weight of Asian women.
Hepatic Impairment: No studies were conducted to evaluate the effect of hepatic disease on the disposition of Skyla.
Renal Impairment: No formal studies were conducted to evaluate the effect of renal disease on the disposition of Skyla.
Drug-Drug Interactions
No drug-drug interaction studies were conducted with Skyla [see Drug Interactions (7)].
14 CLINICAL STUDIES
The contraceptive efficacy of Skyla was evaluated in a clinical trial that enrolled generally healthy women aged 18–35, 1,432 of whom received Skyla. Of these, 38.8 % (556) were nulliparous women, and 819 women completed 3 years of use. The trial was a multicenter, multi-national, randomized open-label study conducted in 11 countries in Europe, Latin America, the US and Canada. Women less than six weeks postpartum, with a history of ectopic pregnancy, with clinically significant ovarian cysts or with HIV or otherwise at high risk for sexually transmitted infections were excluded. A total of 540 (37.7%) were treated at US sites and 892 (62.3%) were at non-US sites. The racial demographics of enrolled women who received Skyla was: Caucasian (79.7%), Hispanic (11.5%), Black/African Americans (5.2%), Other (2.7%) and Asian (0.8%). The weight range was 38 to 155 kg (mean weight: 68.7 kg) and mean BMI was 25.3 kg/m2 (range 16–55 kg/m2). The clinical trial had no upper or lower weight or BMI limit. Of Skyla-treated women, 21.9% discontinued the study treatment due to an adverse event, 4.4% were lost to follow up, 1.8% withdrew for unspecified reasons, 1.1% discontinued due to protocol deviation, 0.6% discontinued due to pregnancy, and 13.0% discontinued due to other reasons.
The pregnancy rate calculated as the Pearl Index (PI) in women aged 18–35 years was the primary efficacy endpoint used to assess contraceptive reliability. The PI was calculated based on 28-day equivalent exposure cycles; evaluable cycles excluded those in which back-up contraception was used unless a pregnancy occurred in that cycle. Skyla-treated women provided 15,763 evaluable 28-day cycle equivalents in the first year and 39,368 evaluable cycles over the three year treatment period. The PI estimate for the first year of use based on the 5 pregnancies that occurred after the onset of treatment and within 7 days after Skyla removal or expulsion was 0.41 with a 95% upper confidence limit of 0.96. The cumulative 3-year pregnancy rate, based on 10 pregnancies, estimated by the Kaplan-Meier method was 0.9 per 100 women or 0.9%, with a 95% upper confidence limit of 1.7%.
16 HOW SUPPLIED/STORAGE AND HANDLING
- Skyla (levonorgestrel-releasing intrauterine system), containing a total of 13.5 mg LNG, is available in a carton of one sterile unit. NDC# 50419-422-01
Skyla is supplied sterile. Skyla is sterilized with ethylene oxide. Do not resterilize. For single use only. Do not use if the inner package is damaged or open. Insert before the end of the month shown on the label.
Store at 25°C (77°F); with excursions permitted between 15–30°C (59–86°F) [see USP Controlled Room Temperature].
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Patient Information)
- •
- Sexually Transmitted Infections: Advise the patient that this product does not protect against HIV infection (AIDS) and other sexually transmitted infections (STIs).
- •
- Risk of Ectopic Pregnancy: Advise the patient about the risks of ectopic pregnancy, including the loss of fertility. Teach her to recognize and report to her healthcare provider promptly any symptoms of ectopic pregnancy. [See Warnings and Precautions (5.1).]
- •
- Risks of Intrauterine Pregnancy: Advise the patient to contact her healthcare provider if she thinks she might be pregnant. Inform the patient about the risks of intrauterine pregnancy while using Skyla, including the risks of leaving Skyla in place and the risks of removing Skyla or probing of the uterus. If Skyla cannot be removed in a pregnant patient, advise her to report immediately any symptom that suggests complications of the pregnancy. Advise her of isolated reports of virilization of the female fetus following local exposure to LNG during pregnancy with an LNG IUS in place. [See Warnings and Precautions (5.2) and Use in Special Populations (8.1).]
- •
- Sepsis: Advise the patient that severe infection or sepsis, including Group A streptococcal sepsis (GAS), can occur within the first few days after Skyla is inserted. Instruct her to contact a healthcare provider immediately if she develops severe pain or fever shortly after Skyla is inserted. [See Warnings and Precautions (5.3).]
- •
- Pelvic Infection: Advise the patient about the possibility of pelvic infections including PID and that these infections can cause tubal damage leading to ectopic pregnancy or infertility, or infrequently can necessitate hysterectomy, or cause death. Teach patients to recognize and report to their healthcare provider promptly any symptoms of pelvic infection. These symptoms include development of menstrual disorders (prolonged or heavy bleeding), unusual vaginal discharge, abdominal or pelvic pain or tenderness, dyspareunia, chills, and fever. [See Warnings and Precautions (5.4).]
- •
- Perforation and Expulsion: Advise the patient that the IUS may be expelled from or perforate the uterus and instruct her on how she can check that the threads still protrude from the cervix. Inform her that excessive pain or vaginal bleeding during Skyla placement, worsening pain or bleeding after placement, or the inability to feel Skyla strings may occur with Skyla perforation and expulsion. Caution her not to pull on the threads and displace Skyla. Inform her that there is no contraceptive protection if Skyla is displaced or expelled. Instruct the patient to contact her healthcare provider if she cannot feel the threads and to avoid intercourse or use a non-hormonal back-up birth control (such as condoms or spermicide) until the location of Skyla has been confirmed. Advise her that if perforation occurs, Skyla will have to be located and removed; surgery may be required. [See Warnings and Precautions (5.5, 5.6, 5.10).]
- •
- Ovarian Cysts: Advise the patient regarding the risk of ovarian cysts and that cysts can cause clinical symptoms including pelvic pain, abdominal pain or dyspareunia. Advise the patient to contact her healthcare provider if she experiences these symptoms. [See Warnings and Precautions (5.7).]
- •
- Bleeding Pattern Alterations: Advise the patient that irregular or prolonged bleeding and spotting, and/or cramps may occur during the first few weeks after insertion. Inform the patient that, during the first 3–6 months of Skyla use, the number of bleeding and spotting days may be higher and bleeding patterns may be irregular. If her symptoms continue or are severe she should report them to her healthcare provider. [See Warnings and Precautions (5.8).]
- •
- Clinical Considerations for Use and Removal: Advise the patient to contact her healthcare provider if she experiences any of the following:
- •
- A stroke or heart attack
- •
- Very severe or migraine headaches
- •
- Unexplained fever
- •
- Yellowing of the skin or whites of the eyes, as these may be signs of serious liver problems
- •
- Pregnancy or suspected pregnancy
- •
- Pelvic pain, abdominal pain, or pain during sex
- •
- HIV positive seroconversion in herself or her partner
- •
- Possible exposure to STIs
- •
- Unusual vaginal discharge or genital sores
- •
- Severe vaginal bleeding or bleeding that lasts a long time, or if she misses a menstrual period
- •
- Inability to feel Skyla's threads
- •
- Magnetic Resonance Imaging (MRI) Safety Information: Inform the patient that Skyla can be safely scanned with MRI only under specific conditions [see Warnings and Precautions (5.11)]. Instruct patients who will have an MRI to tell their doctor that they have Skyla.
- This Patient Information has been approved by the U.S. Food and Drug Administration. 5/2021
Skyla (levonorgestrel-releasing intrauterine system) Carton
NDC 50419-422-01
1 Sterile Unit
IMPORTANT: To be inserted in the uterus by or under the supervision of a licensed clinician. See physician insert for detailed instructions for use.
Skyla
(levonorgestrel-releasing intrauterine system)
Rx only
— 13.5 mg levonorgestrel
— 1 sterile unit
— intrauterine use