Rx only
WARNING: ABUSE, MISUSE, AND ADDICTION
Methamphetamine has a high potential for abuse and misuse, which can lead to the development of a substance use disorder, including addiction. Misuse and abuse of CNS stimulants, including methamphetamine hydrochloride tablets, can result in overdose and death (see OVERDOSAGE), and this risk is increased with higher doses or unapproved methods of administration, such as snorting or injection.
Before prescribing methamphetamine hydrochloride tablets, assess each patient’s risk for abuse, misuse, and addiction. Educate patients and their families about these risks, proper storage of the drug, and proper disposal of any unused drug. Throughout methamphetamine treatment, reassess each patient’s risk of abuse, misuse, and addiction and frequently monitor for signs and symptoms of abuse, misuse, and addiction (see WARNINGS and DRUG Abuse AND DEPENDENCE).
DESCRIPTION
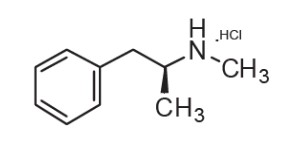
Methamphetamine hydrochloride, USP, chemically known as (αS)-α-Methylbenzeneethan-(N-methyl)-amine Hydrochloride, is a member of the amphetamine group of sympathomimetic amines. It has the following structural formula:
Methamphetamine hydrochloride tablets, USP contain 5 mg of methamphetamine hydrochloride, USP for oral administration. In addition, each tablet contains the following inactive ingredients: crospovidone, magnesium stearate, microcrystalline cellulose, povidone and purified water.
CLINICAL PHARMACOLOGY
Methamphetamine is a sympathomimetic amine with CNS stimulant activity. Peripheral actions include elevation of systolic and diastolic blood pressures and weak bronchodilator and respiratory stimulant action. Other central nervous system actions, or metabolic effects, may be involved, for example.
The mechanism of action involved in producing the beneficial behavioral changes seen in hyperkinetic children receiving methamphetamine is unknown.
In humans, methamphetamine is rapidly absorbed from the gastrointestinal tract. The primary site of metabolism is in the liver by aromatic hydroxylation, N-dealkylation and deamination. At least seven metabolites have been identified in the urine. The biological half-life has been reported in the range of 4 to 5 hours. Excretion occurs primarily in the urine and is dependent on urine pH. Alkaline urine will significantly increase the drug halflife. Approximately 62% of an oral dose is eliminated in the urine within the first 24 hours with about one-third as intact drug and the remainder as metabolites.
INDICATIONS AND USAGE
Attention Deficit Disorder with Hyperactivity: Methamphetamine hydrochloride tablets are indicated as an integral part of a total treatment program which typically includes other remedial measures (psychological, educational, social) for a stabilizing effect in children over 6 years of age with a behavioral syndrome characterized by the following group of developmentally inappropriate symptoms: moderate to severe distractibility, short attention span, hyperactivity, emotional lability, and impulsivity. The diagnosis of this syndrome should not be made with finality when these symptoms are only of comparatively recent origin. Nonlocalizing (soft) neurological signs, learning disability, and abnormal EEG may or may not be present, and a diagnosis of central nervous system dysfunction may or may not be warranted.
CONTRAINDICATIONS
In patients known to be hypersensitive to amphetamine, or other components of methamphetamine hydrochloride tablets, hypersensitivity reactions such as angioedema and anaphylactic reactions have been reported in patients treated with other amphetamine products (see ADVERSE REACTIONS).
Patients taking monoamine oxidase inhibitors (MAOIs), or within 14 days of stopping MAOIs (including MAOIs such as linezolid or intravenous methylene blue), because of an increased risk of hypertensive crisis (see WARNINGS and DRUG INTERACTIONS).
WARNINGS
Abuse, Misuse, and Addiction
Methamphetamine hydrochloride tablets havea high potential for abuse and misuse. The use of methamphetamine hydrochloride tablets exposes individuals to the risks of abuse and misuse, which can lead to the development of a substance use disorder, including addiction. Methamphetamine hydrochloride tablets can be diverted for non-medical use into illicit channels or distribution (see DRUG ABUSEand DEPENDENCE: Abuse). Misuse and abuse of CNS stimulants, including methamphetamine hydrochloride tablets can result in overdose and death (see OVERDOSAGE), and this risk is increased with higher doses or unapproved methods of administration, such as snorting or injection.
Before prescribing methamphetamine hydrochloride tablets, assess each patient’s risk for abuse, misuse, and addiction. Educate patients and their families about these risks and proper disposal of any unused drug. Advise patients to store amphetamine sulfate in a safe place, preferably locked, and instruct patients to not give methamphetamine hydrochloride tablets to anyone else. Throughout methamphetamine treatment, reassess each patient’s risk of abuse, misuse, and addiction and frequently monitor for signs and symptoms of abuse, misuse, and addiction.
Risks to Patients with Serious Cardiac Disease
Sudden death has been reported in patients with structural cardiac abnormalities or other serious cardiac disease who are treated with CNS stimulants at the recommended ADHD dosages.
Avoid methamphetamine use in patients with known structural cardiac abnormalities, cardiomyopathy, serious cardiac arrhythmia, coronary artery disease, or other serious cardiac disease.
Increased Blood Pressure and Heart Rate
CNS stimulants cause an increase in blood pressure (mean increase about 2 to 4 mm Hg) and heart rate (mean increase about 3 to 6 bpm). Monitor all patients for potential tachycardia and hypertension.
Psychiatric Adverse Reactions
Exacerbation of Pre-existing Psychosis
CNS stimulants may exacerbate symptoms of behavior disturbance and thought disorder in patients with a pre-existing psychotic disorder.
Induction of a Manic Episode in Patients with Bipolar Disease
CNS stimulants may induce a manic or mixed episode in patients. Prior to initiating treatment, screen patients for risk factors for developing a manic episode (e.g., comorbid or history of depressive symptoms or a family history of suicide, bipolar disorder, or depression).
New Psychotic or Manic Symptoms
CNS stimulants, at recommended doses, may cause psychotic or manic symptoms (e.g., hallucinations, delusional thinking, or mania) in patients without a prior history of psychotic illness or mania. In a pooled analysis of multiple short-term, placebo-controlled studies of CNS stimulants, psychotic or manic symptoms occurred in approximately 0.1% of CNS stimulant-treated patients, compared with 0% of placebo-treated patients. If such symptoms occur, consideration discontinuing methamphetamine hydrochloride tablets.
Long-Term Suppression of Growth in Pediatric Patients
CNS stimulants have been associated with weight loss and slowing of growth rate in pediatric patients, including methamphetamine hydrochloride tablets. Closely monitor growth (weight and height) in methamphetamine-treated pediatric patients treated with CNS stimulants.
Pediatric patients who are not growing or gaining height or weight as expected may need to have their treatment interrupted (see PRECAUTIONS, Pediatric Use).
Seizures
There is some clinical evidence that stimulants may lower the convulsive threshold in patients with prior history of seizures, in patients with prior EEG abnormalities in absence of seizures, and, very rarely, in patients without a history of seizures and no prior EEG evidence of seizures. In the presence of seizures, the drug should be discontinued.
Peripheral Vasculopathy, Including Raynaud’s Phenomenon
Stimulants, including methamphetamine hydrochloride tablets, used to treat ADHD are associated with peripheral vasculopathy, including Raynaud’s phenomenon. Signs and symptoms are usually intermittent and mild; however, sequelae have included digital ulceration and/or soft tissue breakdown. Effects of peripheral vasculopathy, including Raynaud’s phenomenon, were observed in postmarketing reports and at therapeutic dosages in all age groups throughout the course of treatment. Signs and symptoms generally improve after dosage reduction in dose- or discontinuation of the CNS stimulant. Careful observation for digital changes is necessary during methamphetamine treatment. Further clinical evaluation (e.g., rheumatology referral) may be appropriate for methamphetamine-treated patients who develop signs or symptoms of peripheral vasculopathy.
Serotonin Syndrome
Serotonin syndrome, a potentially life-threatening reaction, may occur when amphetamines are used in combination with other drugs that affect the serotonergic neurotransmitter systems such as monoamine oxidase inhibitors (MAOIs), selective serotonin reuptake inhibitors (SSRIs), serotonin norepinephrine reuptake inhibitors (SNRIs), triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, tryptophan, buspirone, and St. John’s Wort (see DRUG INTERACTIONS).
Amphetamines and amphetamine derivatives are known to be metabolized, to some degree, by cytochrome P450 2D6 (CYP2D6) and display minor inhibition of CYP2D6 metabolism (see CLINICAL PHARMACOLOGY). The potential for a pharmacokinetic interaction exists with the coadministration of CYP2D6 inhibitors which may increase the risk with increased exposure to methamphetamine hydrochloride tablets. In these situations, consider an alternative nonserotonergic drug or an alternative drug that does not inhibit CYP2D6 (see DRUG INTERACTIONS).
Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, delirium, and coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia), neuromuscular symptoms (e.g., tremor, rigidity, myoclonus, hyperreflexia, incoordination), seizures, and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea).
Concomitant use of methamphetamine hydrochloride tablets with MAOI drugs is contraindicated (see CONTRAINDICATIONS).
Discontinue treatment with methamphetamine hydrochloride tablets and any concomitant serotonergic agents immediately if the above symptoms occur, and initiate supportive symptomatic treatment. If concomitant use of methamphetamine hydrochloride tablets with other serotonergic drugs or CYP2D6 inhibitors is clinically warranted, initiate methamphetamine hydrochloride tablets with lower doses, monitor patients for the emergence of serotonin syndrome during drug initiation or titration, and inform patients of the increased risk for serotonin syndrome.
Motor and Verbal Tics, and Worsening of Tourette’s Syndrome
CNS stimulants, including amphetamine sulfate, have been associated with the onset or exacerbation of motor and verbal tics. Worsening of Tourette’s syndrome has also been reported. Before initiating methamphetamine hydrochloride tablets, assess the family history and clinically evaluate patients for tics or Tourette’s syndrome. Regularly monitor patients for the emergence or worsening of tics or Tourette’s syndrome with methamphetamine hydrochloride tablets, and discontinue treatment if clinically appropriate.
PRECAUTIONS
General
Methamphetamine hydrochloride tablets should be used with caution in patients with even mild hypertension. Methamphetamine should not be used to combat fatigue or to replace rest in normal persons.
Prescribing and dispensing of methamphetamine should be limited to the smallest amount that is feasible at one time in order to minimize the possibility of overdosage.
Information for Patients
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Abuse, Misuse, and Addiction
Educate patients and their families about the risks of abuse, misuse, and addiction of methamphetamine hydrochloride tablets, which can lead to overdose and death, and proper disposal of any unused drug (see WARNINGS,DRUG ABUSE AND DEPENDENCE, and OVERDOSAGE). Advise patients to store methamphetamine hydrochloride tablets in a safe place, preferably locked, and instruct patients to not give methamphetamine hydrochloride tablets to anyone else.
The patient should be informed that methamphetamine may impair the ability to engage in potentially hazardous activities, such as, operating machinery or driving a motor vehicle.
Circulation Problems in Fingers and Toes [Peripheral Vasculopathy, Including Raynaud’s Phenomenon]
- •
- Instruct patients beginning treatment with methamphetamine hydrochloride tablets about the risk of peripheral vasculopathy, including Raynaud’s Phenomenon, and associated signs and symptoms: fingers or toes may feel numb, cool, painful, and/or may change color from pale, to blue, to red.
- •
- Instruct patients to report to their physician any new numbness, pain, skin color change, or sensitivity to temperature in fingers or toes.
- •
- Instruct patients to call their physician immediately with any signs of unexplained wounds appearing on fingers or toes while taking methamphetamine hydrochloride tablets.
- •
- Further clinical evaluation (e.g., rheumatology referral) may be appropriate for certain patients.
Motor and Verbal Tics, and Worsening of Tourette’s Syndrome
- •
- Advise patients that motor and verbal tics and worsening of Tourette’s Syndrome may occur during treatment with methamphetamine hydrochloride tablets. Instruct the patients to notify their healthcare provider if emergence or worsening of tics or Tourette’s syndrome occurs (see WARNINGS).
The patient should be cautioned not to increase dosage, except on advice of the physician.
Drug Interactions
Insulin requirements in diabetes mellitus may be altered in association with the use of methamphetamine and the concomitant dietary regimen.
Methamphetamine may decrease the hypotensive effect of guanethidine.
Methamphetamine should not be used concurrently with monoamine oxidase inhibitors(see CONTRAINDICATIONS).
Methamphetamine hydrochloride tablets should not be used concurrently with monoamine oxidase inhibitors (see CONTRAINDICATIONS).
Concurrent administration of tricyclic antidepressants and indirect-acting sympathomimetic amines such as the amphetamines, should be closely supervised and dosage carefully adjusted. Phenothiazines are reported in the literature to antagonize the CNS stimulant action of the amphetamines.
Drug/Laboratory Test Interactions
Literature reports suggest that amphetamines may be associated with significant elevation of plasma corticosteroids. This should be considered if determination of plasma corticosteroid levels is desired in a person receiving amphetamines.
Acidifying Agents
Lower blood levels and efficacy of amphetamines. Increase dose based on clinical response. Examples of acidifying agents include gastrointestinal acidifying agents (e.g., guanethidine, reserpine, glutamic acid HCl, ascorbic acid) and urinary acidifying agents (e.g., ammonium chloride, sodium acid phosphate, methenamine salts).
Alkalinizing Agents
Increase blood levels and potentiate the action of amphetamine. Co-administration of methamphetamine and gastrointestinal alkalinizing agents should be avoided. Examples of alkalinizing agents include gastrointestinal alkalinizing agents (e.g., sodium bicarbonate) and urinary alkalinizing agents (e.g., acetazolamide, some thiazides).
Tricyclic Antidepressants
May enhance the activity of tricyclic or sympathomimetic agents causing striking and sustained increases in the concentration of d-amphetamine in the brain; cardiovascular effects can be potentiated. Monitor frequently and adjust or use alternative therapy based on clinical response. Examples of tricyclic antidepressants include desipramine, Protriptyline.
CYP2D6 Inhibitors
The concomitant use of methamphetamine and CYP2D6 inhibitors may increase the exposure of methamphetamine compared to the use of the drug alone and increase the risk of serotonin syndrome. Initiate with lower doses and monitor patients for signs and symptoms of serotonin syndrome particularly during methamphetamine initiation and after a dosage increase. If serotonin syndrome occurs, discontinue methamphetamine and the CYP2D6 inhibitor (see WARNINGS, OVERDOSAGE). Examples of CYP2D6 Inhibitors include paroxetine and fluoxetine (also serotonergic drugs), quinidine, ritonavir.
Serotonergic Drugs
The concomitant use of methamphetamine and serotonergic drugs increases the risk of serotonin syndrome. Initiate with lower doses and monitor patients for signs and symptoms of serotonin syndrome, particularly during methamphetamine initiation or dosage increase. If serotonin syndrome occurs, discontinue methamphetamine and the concomitant serotonergic drug(s) (see WARNINGS and PRECAUTIONS). Examples of serotonergic drugs include selective serotonin reuptake inhibitors (SSRI), serotonin norepinephrine reuptake inhibitors (SNRI), triptans, tricyclic antidepressants, fentanyl, lithium, tramadol, tryptophan, buspirone, St. John’s Wort.
MAO Inhibitors
Concomitant use of MAOIs and CNS stimulants can cause hypertensive crisis. Potential outcomes include death, stroke, myocardial infarction, aortic dissection, ophthalmological complications, eclampsia, pulmonary edema, and renal failure. Do not administer methamphetamine concomitantly or within 14 days after discontinuing MAOI (see CONTRAINDICATIONS and WARNINGS). Examples of MAOIs include selegiline, tranylcypromine, isocarboxazid, phenelzine, linezolid, methylene blue.
Proton Pump Inhibitors
Time to maximum concentration (Tmax) of amphetamine is decreased compared to when administered alone. Monitor patients for changes in clinical effect and adjust therapy based on clinical response. An example of a proton pump inhibitor is omeprazole.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Data are not available on longterm potential for carcinogenicity, mutagenicity, or impairment of fertility.
Pregnancy
Teratogenic Effects
Methamphetamine has been shown to have teratogenic and embryocidal effects in mammals given high multiples of the human dose. There are no adequate and well-controlled studies in pregnant women. Methamphetamine hydrochloride tablets should not be used during pregnancy unless the potential benefit justifies the potential risk to the fetus.
Nonteratogenic Effects
Infants born to mothers dependent on amphetamines have an increased risk of premature delivery and low birth weight. Also, these infants may experience symptoms of withdrawal as demonstrated by dysphoria, including agitation and significant lassitude.
Usage in Nursing Mothers
Amphetamines are excreted in human milk. Mothers taking amphetamines should be advised to refrain from nursing.
Pediatric Use
Long-term effects of methamphetamine in children have not been established (see WARNINGS).
Drug treatment is not indicated in all cases of the behavioral syndrome characterized by moderate to severe distractibility, short attention span, hyperactivity, emotional lability and impulsivity. It should be considered only in light of the complete history and evaluation of the child. The decision to prescribe methamphetamine hydrochloride tablets should depend on the physician's assessment of the chronicity and severity of the child's symptoms and their appropriateness for his/her age. Prescription should not depend solely on the presence of one or more of the behavioral characteristics.
When these symptoms are associated with acute stress reactions, treatment with methamphetamine hydrochloride tablets is usually not indicated.
Clinical experience suggests that in psychotic children, administration of methamphetamine hydrochloride tablets may exacerbate symptoms of behavior disturbance and thought disorder.
Amphetamines have been reported to exacerbate motor and phonic tics and Tourette's syndrome. Therefore, clinical evaluation for tics and Tourette's syndrome in children and their families should precede use of stimulant medications.
Geriatric Use
Clinical Studies of methamphetamine did not include sufficient numbers of subjects age 65 years and over to determine whether elderly subjects respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal or cardiac function, and of concomitant disease or other drug therapy observed in this population.
ADVERSE REACTIONS
The following are adverse reactions in decreasing order of severity within each category that have been reported:
Cardiovascular: Elevation of blood pressure, tachycardia and palpitation. Fatal cardiorespiratory arrest has been reported, mostly in the context of abuse/misuse.
Central Nervous System: Psychotic episodes have been rarely reported at recommended doses. Dizziness, dysphoria, overstimulation, euphoria, insomnia, tremor, restlessness and headache. Exacerbation of motor and verbal tics and Tourette's syndrome.
Gastrointestinal: Diarrhea, constipation, dryness of mouth, unpleasant taste, intestinal ischemia, and other gastrointestinal disturbances.
Hypersensitivity: Urticaria.
Endocrine: Impotence and changes in libido; frequent or prolonged erections.
Musculoskeletal: Rhabdomyolysis.
Miscellaneous: Suppression of growth has been reported with the long-term use of stimulants in children (see WARNINGS).
Skin and Subcutaneous Tissue Disorders: Alopecia.
To report SUSPECTED ADVERSE REACTIONS, contact Hikma Pharmaceuticals USA Inc. at 1-800-962-8364 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
DRUG ABUSE AND DEPENDENCE
Abuse
Methamphetamine hydrochloride tablets have a high potential for abuse and misuse which can lead to the development of a substance use disorder, including addiction [see WARNINGS and PRECAUTIONS]. Methamphetamine hydrochloride tablets can be diverted for non-medical use into illicit channels or distribution.
Abuse is the intentional non-therapeutic use of a drug, even once, to achieve a desired psychological or physiological effect. Misuse is the intentional use, for therapeutic purposes, of a drug by an individual in a way other than prescribed by a health care provider or for whom it was not prescribed. Drug addiction is a cluster of behavioral, cognitive, and physiological phenomena that may include a strong desire to take the drug, difficulties in controlling drug use (e.g., continuing drug use despite harmful consequences, giving a higher priority to drug use than other activities and obligations), and possible tolerance or physical dependence.
Misuse and abuse of methamphetamine may cause increased heart rate, respiratory rate, or blood pressure; sweating; dilated pupils; hyperactivity; restlessness; insomnia; decreased appetite; loss of coordination; tremors; flushed skin; vomiting; and/or abdominal pain. Anxiety, psychosis, hostility, aggression, and suicidal or homicidal ideation have also been observed with CNS stimulants abuse and/or misuse. Misuse and abuse of CNS stimulants, including methamphetamine hydrochloride tablets, can result in overdose and death (see OVERDOSAGE), and this risk is increased with higher doses or unapproved methods of administration, such as snorting or injection.
Dependence
Physical Dependence
Methamphetamine hydrochloride tablets may produce physical dependence. Physical dependence is a state that develops as a result of physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
Withdrawal signs and symptoms after abrupt discontinuation or dose reduction following prolonged use of CNS stimulants including methamphetamine hydrochloride tablets include dysphoric mood; depression; fatigue; vivid, unpleasant dreams; insomnia or hypersomnia; increased appetite; and psychomotor retardation or agitation.
Tolerance
Methamphetamine hydrochloride tablets may produce tolerance. Tolerance is a physiological state characterized by a reduced response to a drug after repeated administration (i.e., a higher dose of a drug is required to produce the same effect that was once obtained at a lower dose).
OVERDOSAGE
Clinical Effects of Overdose
Overdose of CNS stimulants is characterized by the following sympathomimetic effects:
- •
- Cardiovascular effects including tachyarrhythmias, and hypertension or hypotension. Vasospasm, myocardial infarction, or aortic dissection may precipitate sudden cardiac death. Takotsubo cardiomyopathy may develop.
- •
- CNS effects including psychomotor agitation, confusion, and hallucinations. Serotonin syndrome, seizures, cerebral vascular accidents, and coma may occur.
- •
- Life-threatening hyperthermia (temperatures greater than 104oF) and rhabdomyolysis may develop.
DOSAGE AND ADMINISTRATION
Methamphetamine hydrochloride tablets are given orally.
Methamphetamine should be administered at the lowest effective dosage, and dosage should be individually adjusted. Late evening medication should be avoided because of the resulting insomnia.
Prior to treating patients with methamphetamine hydrochloride tablets, assess:
- •
- for the presence of cardiac disease (i.e., perform a careful history, family history of sudden death or ventricular arrhythmia, and physical exam) (see WARNINGS).
- •
- the family history and clinically evaluate patients for motor or verbal tics or Tourette’s syndrome (see WARNINGS).
Attention Deficit Disorder with Hyperactivity
For treatment of children 6 years or older with a behavioral syndrome characterized by moderate to severe distractibility, short attention span, hyperactivity, emotional lability and impulsivity: an initial dose of
5 mg methamphetamine once or twice a day is recommended. Daily dosage may be raised in increments of 5 mg at weekly intervals until an optimum clinical response is achieved. The usual effective dose is
20 to 25 mg daily. The total daily dose may be given in two divided doses daily.
HOW SUPPLIED
Methamphetamine Hydrochloride Tablets, USP
5 mg tablets are supplied as a round, white to off-white, biconvex, debossed tablet with "54" on one side and "681" on the other side.
NDC 0054-0389-25: Bottle of 100 tablets
Recommended Storage:Store at 20ºC to 25ºC (68ºF to 77ºF). [See USP Controlled Room Temperature.]
Dispense in a tight, light resistant, child-resistant container as defined in the USP/NF.
Distributed by: Hikma
Pharmaceuticals USA Inc.
Berkeley Heights, NJ 07922
C50000760/03
Revised October 2023
Medication Guide
Methamphetamine Hydrochloride Tablets USP, CII
(meth″ am fet′ a meen hye″ droe klor′ ide)
Rx only
|
What is the most important information I should know about methamphetamine hydrochloride tablets? Methamphetamine hydrochloride tablets may cause serious side effects, including:
Your child’s healthcare provider should check your child carefully for heart problems before starting treatment with methamphetamine hydrochloride tablets. Tell your child’s healthcare provider if your child has any heart problems, heart disease, or heart defects. Call your child’s healthcare provider or go to the nearest hospital emergency room right away if your child has any signs of heart problems such as chest pain, shortness of breath, or fainting during treatment with methamphetamine hydrochloride tablets.
Tell your child’s healthcare provider about any mental problems your child has, or about a family history of suicide, bipolar illness, or depression. Call your child’s healthcare provider right away if your child has any new or worsening mental symptoms or problems during treatment with methamphetamine hydrochloride tablets, especially hearing voices, seeing or believing things that are not real, or new manic symptoms. |
What are methamphetamine hydrochloride tablets?
Methamphetamine hydrochloride tablets are a central nervous system (CNS) stimulant prescription medicine used for the treatment of Attention Deficit Hyperactivity Disorder (ADHD) in children 6 years to 17 years of age. Methamphetamine hydrochloride tablets may help increase attention and decrease impulsiveness and hyperactivity in people with ADHD.
It is not known if methamphetamine hydrochloride tablets are safe and effective in children under 6 years of age.
Methamphetamine hydrochloride tablets are a federally controlled substance (CII) because it contains methamphetamine that can be a target for people who abuse prescription medicines or street drugs. Keep methamphetamine hydrochloride tablets in a safe place to protect it from theft. Never give your methamphetamine hydrochloride tablets to anyone else because it may cause death or harm them. Selling or giving away methamphetamine hydrochloride tablets may harm others and is against the law.
Do not take methamphetamine hydrochloride tablets if your child is:
- •
- allergic to amphetamine or any of the ingredients in methamphetamine hydrochloride tablets. See the end of this Medication Guide for a complete list of ingredients in methamphetamine hydrochloride tablets.
- •
- taking, or has stopped taking within the past 14 days, a medicine used to treat depression called a monoamine oxidase inhibitor (MAOI).
Before taking methamphetamine hydrochloride tablets, tell your child’s healthcare provider about all your child’s medical conditions, including if your child:
- •
- has heart problems, heart disease, heart defects, or high blood pressure
- •
- has mental problems including psychosis, mania, bipolar illness or depression, or a family history of suicide bipolar illness, or depression
- •
- has circulation problems in fingers and toes
- •
- has kidney problems
- •
- have or had repeated movements or sounds (tics) or Tourette’s syndrome, or have a family history of tics or Tourette’s syndrome
- •
- is pregnant or plans to become pregnant. Methamphetamine hydrochloride tablets may harm the unborn baby.
- o
- Pregnancy Exposure Registry: There is a pregnancy registry for women who are exposed to methamphetamine hydrochloride tablets during pregnancy. The purpose of the registry is to collect information about the health of women exposed to methamphetamine hydrochloride tablets and their baby. If your child becomes pregnant during treatment with methamphetamine hydrochloride tablets, talk to your child’s healthcare provider about registering with the National Pregnancy Registry for Psychostimulants at 1-866-961-2388 or by visiting online at https://womensmentalhealth.org/clinical-and-researchprograms/ pregnancyregistry/othermedications/
- •
- is breastfeeding or plans to breastfeed. Methamphetamine hydrochloride tablets pass into breast milk. Your child should not breastfeed during treatment with methamphetamine hydrochloride tablets. Talk to your child’s healthcare provider about the best way to feed the baby during treatment with methamphetamine hydrochloride tablets.
Tell your child’s healthcare provider about all of the medicines that your child takes including prescription and over-the-counter medicines, vitamins, and herbal supplements.
Methamphetamine hydrochloride tablets and some medicines may interact with each other and cause serious side effects. Sometimes the doses of other medicines will need to be changed during treatment with methamphetamine hydrochloride tablets. Your child’s healthcare provider will decide whether methamphetamine hydrochloride tablets can be taken with other medicines.
Especially tell your child’s healthcare provider if your child takes:
- •
- medicines used to treat migraine headaches known as triptans
- •
- tricyclic antidepressants
- •
- fentanyl
- •
- lithium
- •
- tramadol
- •
- tryptophan
- •
- buspirone
- •
- St. John’s Wort
- •
- medicines used to treat mood, anxiety, psychotic or thought disorders, including selective serotonin reuptake inhibitors (SSRIs) and serotonin norepinephrine reuptake inhibitors (SNRIs)
Ask your child’s healthcare provider if you are not sure if your child takes any of these medicines. Know the medicines your child takes. Keep a list of your child’s medicines with you to show your child’s healthcare provider and pharmacist. Do not start any new medicine during treatment with methamphetamine hydrochloride tablets without talking to your child’s healthcare provider first.
How should methamphetamine hydrochloride tablets be taken?
- •
- Take methamphetamine hydrochloride tablets exactly as prescribed.
- •
- Your child’s healthcare provider may change the dose or have your child stop taking methamphetamine hydrochloride tablets if needed.
- •
- Methamphetamine hydrochloride tablets are usually taken 1 or 2 times each day. Avoid taking methamphetamine hydrochloride tablets late in the evening because it may cause sleep problems.
If your child takes too many methamphetamine hydrochloride tablets, call your child’s healthcare provider or Poison Help line at 1-800-222-1222 or go to the nearest hospital emergency room right away.
What are possible side effects of methamphetamine hydrochloride tablets?
Methamphetamine hydrochloride tablets may cause serious side effects, including:
- •
- See “What is the most important information I should know about methamphetamine hydrochloride tablets?”
- •
- Slowing of growth (height and weight) in children. Children should have their height and weight checked often during treatment with methamphetamine hydrochloride tablets. Methamphetamine hydrochloride tablets treatment may be stopped if your child is not growing or gaining weight.
- •
- Circulation problems in fingers and toes (peripheral vasculopathy, including Raynaud’s phenomenon). Signs and symptoms may include:
- o
- fingers or toes may feel numb, cool, painful
- o
- fingers or toes may change color from pale, to blue, to red
Tell your child’s healthcare provider if your child has numbness, pain, skin color change, or sensitivity to temperature in your fingers or toes or if your child has any signs of unexplained wounds appearing on fingers or toes during treatment with methamphetamine hydrochloride tablets.
- •
- Serotonin syndrome. This problem may happen when methamphetamine hydrochloride tablets are taken with certain other medicines and may be life-threatening. Call your healthcare provider or go to the nearest hospital emergency room if you have any of the following symptoms of serotonin syndrome:
- o
- agitation, hallucinations, coma
- o
- changes in blood pressure
- o
- high body temperature
- o
- dizziness
- o
- sweating or fever
- o
- muscle stiffness or tightness
- o
- fast heartbeat
- o
- flushing
- o
- seizures
- o
- nausea, vomiting, diarrhea
- o
- loss of coordination
- o
- confusion
- •
- New or worsening tics or worsening Tourette’s syndrome. Tell your healthcare provider if you or your child get any new or worsening tics or worsening Tourette’s syndrome during treatment with methamphetamine hydrochloride tablets.
The most common side effects with methamphetamine hydrochloride tablets include:
- •
- fast heartbeat or heart beating harder than normal
- •
- dizziness
- •
- trouble sleeping
- •
- shaking
- •
- headache
- •
- diarrhea
- •
- dry mouth
These are not all the possible side effects of methamphetamine hydrochloride tablets.
Call your child’s doctor for medical advice about side effects. You may report side effects to FDA at
1-800-FDA-1088.
How should I store methamphetamine hydrochloride tablets?
- •
- Store methamphetamine hydrochloride tablets at room temperature between 68°F to 77°F
(20°C to 25°C). [See USP Controlled Room Temperature.] - •
- Store methamphetamine hydrochloride tablets in a safe place like a locked cabinet.
Protect from light. - •
- Dispose of remaining, unused, or expired methamphetamine hydrochloride tablets by a medicine take-back program at a U.S. Drug Enforcement Administration (DEA) authorized collection site.
If no take-back program or DEA authorized collector is available, mix methamphetamine hydrochloride tablets with an undesirable, nontoxic substance such as dirt, cat litter, or used coffee grounds to make it less appealing to children and pets. Place the mixture in a container such as a sealed plastic bag and throw away methamphetamine hydrochloride tablets in the household trash. Visit www.fda.gov/drugdisposal for additional information on disposal of unused medicines.
Keep methamphetamine hydrochloride tablets and all medicines out of the reach of children.
General information about the safe and effective use of methamphetamine hydrochloride tablets.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide.
Do not use methamphetamine hydrochloride tablets for a condition for which it was not prescribed.
Do not give methamphetamine hydrochloride tablets to other people, even if they have the same symptoms that your child has. It may harm them and it is against the law.
You can ask your child’s pharmacist or healthcare provider for information about methamphetamine hydrochloride tablets that is written for healthcare professionals.
What are the ingredients in methamphetamine hydrochloride tablets?
Active Ingredient: methamphetamine hydrochloride, USP
Inactive Ingredients: crospovidone, magnesium stearate, microcrystalline cellulose, povidone, and purified water.
For more information about methamphetamine hydrochloride tablets, go to www.hikma.com or call Hikma Pharmaceuticals USA Inc. at 1-800-962-8364.
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Distributed by: Hikma
Pharmaceuticals USA Inc.
Berkeley Heights, NJ 07992
C50000760/03
Revised October 2023