FULL PRESCRIBING INFORMATION
WARNING: CONGESTIVE HEART FAILURE
- Thiazolidinediones, including pioglitazone, which is a component of alogliptin and pioglitazone tablets, cause or exacerbate congestive heart failure in some patients [see Warnings and Precautions (5.1)].
- After initiation of alogliptin and pioglitazone tablets and after dose increases, monitor patients carefully for signs and symptoms of heart failure (e.g., excessive, rapid weight gain, dyspnea and/or edema). If heart failure develops, it should be managed according to current standards of care and discontinuation or dose reduction of pioglitazone in alogliptin and pioglitazone tablets must be considered [see Warnings and Precautions (5.1)].
- Alogliptin and pioglitazone tablets are not recommended in patients with symptomatic heart failure [see Warnings and Precautions (5.1)].
- Initiation of alogliptin and pioglitazone tablets in patients with established New York Heart Association (NYHA) Class III or IV heart failure is contraindicated [see Contraindications (4) and Warnings and Precautions (5.1)].
1 INDICATIONS AND USAGE
Alogliptin and pioglitazone tablets are indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
2 DOSAGE AND ADMINISTRATION
2.1 Recommendations for All Patients
Alogliptin and pioglitazone tablets should be taken once daily and can be taken with or without food. Do not split tablets.
The recommended starting dose for alogliptin and pioglitazone tablets:
- for patients inadequately controlled on diet and exercise is 25 mg/15 mg or 25 mg/30 mg,
- for patients inadequately controlled on metformin monotherapy is 25 mg/15 mg or 25 mg/30 mg,
- for patients on alogliptin who require additional glycemic control is 25 mg/15 mg or 25 mg/30 mg,
- for patients on pioglitazone who require additional glycemic control is 25 mg/15 mg, 25 mg/30 mg or 25 mg/45 mg as appropriate based upon current therapy,
- for patients switching from alogliptin coadministered with pioglitazone, alogliptin and pioglitazone tablets may be initiated at the dose of alogliptin and pioglitazone based upon current therapy,
- for patients with congestive heart failure (NYHA Class I or II) is 25 mg/15 mg.
The alogliptin and pioglitazone tablets dose can be titrated up to a maximum of 25 mg/45 mg once daily based on glycemic response as determined by hemoglobin A1c (A1C).
After initiation of alogliptin and pioglitazone tablets or with dose increase, monitor patients carefully for adverse reactions related to fluid retention as has been seen with pioglitazone (e.g., weight gain, edema and signs and symptoms of congestive heart failure) [see Boxed Warning and Warnings and Precautions (5.1)].
2.2 Patients with Renal Impairment
No dose adjustment of alogliptin and pioglitazone tablets is necessary for patients with mild renal impairment (creatinine clearance [CrCl] ≥60 mL/min).
The dose of alogliptin and pioglitazone tablets is 12.5 mg/15 mg, 12.5 mg/30 mg or 12.5 mg/45 mg once daily for patients with moderate renal impairment (CrCl ≥30 to <60 mL/min).
Alogliptin and pioglitazone tablets are not recommended for patients with severe renal impairment or ESRD [see Use in Specific Populations (8.6) and Clinical Pharmacology (12.3)]. Coadministration of pioglitazone and alogliptin 6.25 mg once daily based on individual requirements may be considered in these patients.
Because there is a need for dose adjustment based upon renal function, assessment of renal function is recommended prior to initiation of alogliptin and pioglitazone tablets therapy and periodically thereafter.
2.3 Coadministration with Strong CYP2C8 Inhibitors
Coadministration of pioglitazone and gemfibrozil, a strong CYP2C8 inhibitor, increases pioglitazone exposure approximately three-fold. Therefore, the maximum recommended dose of alogliptin and pioglitazone tablets is 25 mg/15 mg daily when used in combination with gemfibrozil or other strong CYP2C8 inhibitors [see Drug Interactions (7.1) and Clinical Pharmacology (12.3)].
3 DOSAGE FORMS AND STRENGTHS
| Pharmaceutical form | Strength (alogliptin/ pioglitazone) | Color | Shape | Markings (on one side) |
|---|---|---|---|---|
| film-coated tablets | 12.5 mg/15 mg | Pale yellow | Round biconvex | "A/P" and 12.5/15" |
| film-coated tablets | 12.5 mg/30 mg | Pale peach | Round biconvex | "A/P and "12.5/30" |
| film-coated tablets | 12.5 mg/45 mg | Pale red | Round biconvex | "A/P" and 12.5/45" |
| film-coated tablets | 25 mg/15 mg | Yellow | Round biconvex | "A/P" and "25/15" |
| film-coated tablets | 25 mg/30 mg | Peach | Round biconvex | "A/P" and "25/30" |
| film-coated tablets | 25 mg/45 mg | Red | Round biconvex | "A/P" and "25/45" |
4 CONTRAINDICATIONS
Serious hypersensitivity reaction to alogliptin or pioglitazone or any of the excipients in alogliptin and pioglitazone tablets, such as anaphylaxis, angioedema and severe cutaneous adverse reactions have been reported [see Warnings and Precautions (5.3), Adverse reactions (6.2)].
Do not initiate in patients with NYHA Class III or IV heart failure [see Boxed Warning].
5 WARNINGS AND PRECAUTIONS
5.1 Congestive Heart Failure
Consider the risks and benefits of alogliptin and pioglitazone tablets prior to initiating treatment in patients at risk for heart failure, such as those with a prior history of heart failure and a history of renal impairment, and observe these patients for signs and symptoms of congestive heart failure. Patients should be advised of the characteristic symptoms of congestive heart failure and should be instructed to immediately report such symptoms. If congestive heart failure develops, it should be managed according to current standards of care and consider discontinuation of alogliptin and pioglitazone tablets.
Alogliptin
In the EXAMINE trial which enrolled patients with type 2 diabetes and recent acute coronary syndrome, 106 (3.9%) of patients treated with alogliptin and 89 (3.3%) of patients treated with placebo were hospitalized for congestive heart failure.
Pioglitazone
Pioglitazone, like other thiazolidinediones, can cause dose-related fluid retention when used alone or in combination with other antidiabetic medications and is most common when pioglitazone is used in combination with insulin. Fluid retention may lead to or exacerbate congestive heart failure [see Boxed Warning, Contraindications (4) and Adverse Reactions (6.1)].
5.2 Pancreatitis
Acute pancreatitis has been reported in the postmarketing setting and in randomized clinical trials. In glycemic control trials in patients with type 2 diabetes, acute pancreatitis was reported in six (0.2%) patients treated with alogliptin 25 mg and two (<0.1%) patients treated with active comparators or placebo. In the EXAMINE trial (a cardiovascular outcomes trial of patients with type 2 diabetes and high cardiovascular (CV) risk), acute pancreatitis was reported in ten (0.4%) patients treated with alogliptin and in seven (0.3%) patients treated with placebo.
It is unknown whether patients with a history of pancreatitis are at increased risk for pancreatitis while using alogliptin and pioglitazone tablets.
After initiation of alogliptin and pioglitazone tablets, patients should be observed for signs and symptoms of pancreatitis. If pancreatitis is suspected, alogliptin and pioglitazone tablets should promptly be discontinued and appropriate management should be initiated.
5.3 Hypersensitivity Reactions
There have been postmarketing reports of serious hypersensitivity reactions in patients treated with alogliptin. These reactions include anaphylaxis, angioedema and severe cutaneous adverse reactions, including Stevens-Johnson syndrome. If a serious hypersensitivity reaction is suspected, discontinue alogliptin and pioglitazone tablets, assess for other potential causes for the event and institute alternative treatment for diabetes [see Adverse Reactions (6.2)]. Use caution in patients with a history of angioedema with another dipeptidyl peptidase-4 (DPP-4) inhibitor because it is unknown whether such patients will be predisposed to angioedema with alogliptin and pioglitazone tablets.
5.4 Hepatic Effects
There have been postmarketing reports of fatal and nonfatal hepatic failure in patients taking pioglitazone or alogliptin, although some of the reports contain insufficient information necessary to establish the probable cause [see Adverse Reactions (6.2)].
In glycemic control trials of alogliptin in patients with type 2 diabetes, serum alanine aminotransferase (ALT) elevations greater than three times the upper limit of normal (ULN) were reported in 1.3% of patients treated with alogliptin 25 mg and 1.7% of patients treated with active comparators or placebo. In the EXAMINE trial (a cardiovascular outcomes trial of patients with type 2 diabetes and high cardiovascular (CV) risk), increases in serum alanine aminotransferase three times the upper limit of the reference range occurred in 2.4% of patients treated with alogliptin and in 1.8% of patients treated with placebo.
Patients with type 2 diabetes may have fatty liver disease or cardiac disease with episodic congestive heart failure, both of which may cause liver test abnormalities, and they may also have other forms of liver disease, many of which can be treated or managed. Therefore, obtaining a liver test panel (ALT, aspartate aminotransferase [AST], alkaline phosphatase and total bilirubin) and assessing the patient is recommended before initiating alogliptin and pioglitazone tablets therapy. In patients with abnormal liver tests, alogliptin and pioglitazone tablets should be initiated with caution.
Measure liver tests promptly in patients who report symptoms that may indicate liver injury, including fatigue, anorexia, right upper abdominal discomfort, dark urine or jaundice. In this clinical context, if the patient is found to have abnormal liver tests (ALT greater than three times the upper limit of the reference range), alogliptin and pioglitazone tablets treatment should be interrupted and an investigation done to establish the probable cause. Alogliptin and pioglitazone tablets should not be restarted in these patients without another explanation for the liver test abnormalities.
5.5 Edema
Pioglitazone
In controlled clinical trials, edema was reported more frequently in patients treated with pioglitazone than in placebo-treated patients and is dose-related [see Adverse Reactions (6.1)]. In postmarketing experience, reports of new onset or worsening of edema have been received.
Alogliptin and pioglitazone tablets should be used with caution in patients with edema. Because thiazolidinediones, including pioglitazone, can cause fluid retention, which can exacerbate or lead to congestive heart failure, alogliptin and pioglitazone tablets should be used with caution in patients at risk for congestive heart failure. Patients treated with alogliptin and pioglitazone tablets should be monitored for signs and symptoms of congestive heart failure [see Boxed Warning, Warnings and Precautions (5.1) and Patient Counseling Information (17)].
5.6 Fractures
Pioglitazone
In PROactive (the Prospective Pioglitazone Clinical Trial in Macrovascular Events), 5238 patients with type 2 diabetes and a history of macrovascular disease were randomized to pioglitazone (N=2605), force-titrated up to 45 mg daily or placebo (N=2633) in addition to standard of care. During a mean follow-up of 34.5 months, the incidence of bone fracture in females was 5.1% (44/870) for pioglitazone versus 2.5% (23/905) for placebo. This difference was noted after the first year of treatment and persisted during the course of the study. The majority of fractures observed in female patients were nonvertebral fractures including lower limb and distal upper limb. No increase in the incidence of fracture was observed in men treated with pioglitazone (1.7%) versus placebo (2.1%). The risk of fracture should be considered in the care of patients, especially female patients, treated with pioglitazone and attention should be given to assessing and maintaining bone health according to current standards of care.
5.7 Urinary Bladder Tumors
Pioglitazone
Tumors were observed in the urinary bladder of male rats in the two-year carcinogenicity study [see Nonclinical Toxicology (13.1)]. In addition, during the three year PROactive clinical trial, 14 patients out of 2605 (0.54%) randomized to pioglitazone and 5 out of 2633 (0.19%) randomized to placebo were diagnosed with bladder cancer. After excluding patients in whom exposure to study drug was less than one year at the time of diagnosis of bladder cancer, there were six (0.23%) cases on pioglitazone and two (0.08%) cases on placebo. After completion of the trial, a large subset of patients was observed for up to ten additional years, with little additional exposure to pioglitazone. During the 13 years of both PROactive and observational follow-up, the occurrence of bladder cancer did not differ between patients randomized to pioglitazone or placebo (HR =1.00; [95% CI: 0.59–1.72]).
Findings regarding the risk of bladder cancer in patients exposed to pioglitazone vary among observational studies; some did not find an increased risk of bladder cancer associated with pioglitazone, while others did.
A large prospective ten year observational cohort study conducted in the United States found no statistically significant increase in the risk of bladder cancer in diabetic patients ever exposed to pioglitazone, compared to those never exposed to pioglitazone (HR =1.06 [95% CI 0.89–1.26]).
A retrospective cohort study conducted with data from the United Kingdom found a statistically significant association between ever exposure to pioglitazone and bladder cancer (HR: 1.63; [95% CI: 1.22–2.19]).
Associations between cumulative dose or cumulative duration of exposure to pioglitazone and bladder cancer were not detected in some studies including the ten year observational study in the U.S., but were in others. Inconsistent findings and limitations inherent in these and other studies preclude conclusive interpretations of the observational data.
Pioglitazone may be associated with an increase in the risk of urinary bladder tumors. There are insufficient data to determine whether pioglitazone is a tumor promoter for urinary bladder tumors.
Consequently, alogliptin and pioglitazone tablets should not be used in patients with active bladder cancer and the benefits of glycemic control versus unknown risks for cancer recurrence with alogliptin and pioglitazone tablets should be considered in patients with a prior history of bladder cancer.
5.8 Hypoglycemia with Concomitant Use with Insulin or Insulin Secretagogues
Insulin and insulin secretagogues, such as sulfonylureas, are known to cause hypoglycemia. Therefore, a lower dose of insulin or insulin secretagogue may be required to minimize the risk of hypoglycemia when used in combination with alogliptin and pioglitazone tablets.
5.9 Macular Edema
Pioglitazone
Macular edema has been reported in postmarketing experience in diabetic patients who were taking pioglitazone or another thiazolidinedione. Some patients presented with blurred vision or decreased visual acuity, but others were diagnosed on routine ophthalmologic examination.
Most patients had peripheral edema at the time macular edema was diagnosed. Some patients had improvement in their macular edema after discontinuation of their thiazolidinedione.
Patients with diabetes should have regular eye exams by an ophthalmologist according to current standards of care. Patients with diabetes who report any visual symptoms should be promptly referred to an ophthalmologist, regardless of the patient's underlying medications or other physical findings [see Adverse Reactions (6.1)].
5.10 Severe and Disabling Arthralgia
There have been postmarketing reports of severe and disabling arthralgia in patients taking DPP-4 inhibitors. The time to onset of symptoms following initiation of drug therapy varied from one day to years. Patients experienced relief of symptoms upon discontinuation of the medication. A subset of patients experienced a recurrence of symptoms when restarting the same drug or a different DPP-4 inhibitor. Consider DPP-4 inhibitors as a possible cause for severe joint pain and discontinue drug if appropriate.
5.11 Bullous Pemphigoid
Postmarketing cases of bullous pemphigoid requiring hospitalization have been reported with DPP-4 inhibitor use. In reported cases, patients typically recovered with topical or systemic immunosuppressive treatment and discontinuation of the DPP-4 inhibitor. Tell patients to report development of blisters or erosions while receiving alogliptin and pioglitazone tablets. If bullous pemphigoid is suspected, alogliptin and pioglitazone tablets should be discontinued and referral to a dermatologist should be considered for diagnosis and appropriate treatment.
6 ADVERSE REACTIONS
The following serious adverse reactions are described below or elsewhere in the prescribing information:
- Congestive Heart Failure [see Warnings and Precautions (5.1)]
- Pancreatitis [see Warnings and Precautions (5.2)]
- Hypersensitivity Reactions [see Warnings and Precautions (5.3)]
- Hepatic Effects [see Warnings and Precautions (5.4)]
- Severe and Disabling Arthralgia [see Warnings and Precautions (5.10)]
- Bullous Pemphigoid [see Warnings and Precautions (5.11)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Alogliptin and Pioglitazone
Over 1500 patients with type 2 diabetes have received alogliptin coadministered with pioglitazone in four large, randomized, double-blind, controlled clinical trials. The mean exposure to alogliptin and pioglitazone tablets was 29 weeks with more than 100 subjects treated for more than one year. The studies consisted of two placebo-controlled studies of 16 to 26 weeks in duration and two active-controlled studies of 26 weeks and 52 weeks in duration. In the alogliptin and pioglitazone tablets arm, the mean duration of diabetes was approximately six years, the mean body mass index (BMI) was 31 kg/m2 (54% of patients had a BMI ≥30 kg/m2), and the mean age was 54 years (16% of patients ≥65 years of age).
In a pooled analysis of these four controlled clinical studies, the overall incidence of adverse reactions was 65% in patients treated with alogliptin and pioglitazone tablets compared to 57% treated with placebo. Overall discontinuation of therapy due to adverse reactions was 2.5% with alogliptin and pioglitazone tablets compared to 2.0% with placebo, 3.7% with pioglitazone or 1.3% with alogliptin.
Adverse reactions reported in ≥4% of patients treated with alogliptin and pioglitazone tablets and more frequently than in patients who received alogliptin, pioglitazone or placebo are summarized in Table 1.
| Number of Patients (%) | ||||
|---|---|---|---|---|
|
||||
| Alogliptin and Pioglitazone Tablets* | Alogliptin† | Pioglitazone‡ | Placebo | |
| N=1533 | N=446 | N=949 | N=153 | |
| Nasopharyngitis | 75 (4.9) | 21 (4.7) | 37 (3.9) | 6 (3.9) |
| Back Pain | 64 (4.2) | 9 (2.0) | 32 (3.4) | 5 (3.3) |
| Upper Respiratory Tract Infection | 63 (4.1) | 19 (4.3) | 26 (2.7) | 5 (3.3) |
Alogliptin Add-On Therapy to a Thiazolidinedione
In addition, in a 26 week, placebo-controlled, double-blind study, patients inadequately controlled on a thiazolidinedione alone or in combination with metformin or a sulfonylurea were treated with add-on alogliptin therapy or placebo; the adverse reactions reported in ≥5% of patients and more frequently than in patients who received placebo was influenza (alogliptin, 5.5%; placebo, 4.1%).
Hypoglycemia
In a 26 week, placebo-controlled factorial study with alogliptin in combination with pioglitazone on background therapy with metformin, the incidence of subjects reporting hypoglycemia was 0.8%, 0% and 3.8% for alogliptin 25 mg with pioglitazone 15 mg, 30 mg or 45 mg, respectively; 2.3% for alogliptin 25 mg; 4.7%, 0.8% and 0.8% for pioglitazone 15 mg, 30 mg or 45 mg, respectively; and 0.8% for placebo.
In a 26 week, active-controlled, double-blind study with alogliptin alone, pioglitazone alone or alogliptin coadministered with pioglitazone in patients inadequately controlled on diet and exercise, the incidence of hypoglycemia was 3% on alogliptin 25 mg with pioglitazone 30 mg, 0.6% on alogliptin 25 mg and 1.8% on pioglitazone 30 mg.
In a 52 week, active-controlled, double-blind study of alogliptin as add-on therapy to the combination of pioglitazone 30 mg and metformin compared to the titration of pioglitazone 30 mg to 45 mg and metformin, the incidence of subjects reporting hypoglycemia was 4.5% in the alogliptin 25 mg with pioglitazone 30 mg and metformin group versus 1.5% in the pioglitazone 45 mg and metformin group.
Alogliptin
A total of 14,778 patients with type 2 diabetes participated in 14 randomized, double-blind, controlled clinical trials of whom 9052 subjects were treated with alogliptin, 3469 subjects were treated with placebo and 2257 were treated with an active comparator. The mean duration of diabetes was seven years, the mean body mass index (BMI) was 31 kg/m2 (49% of patients had a BMI ≥30 kg/m2) and the mean age was 58 years (26% of patients ≥65 years of age).
The mean exposure to alogliptin was 49 weeks with 3348 subjects treated for more than one year.
In a pooled analysis of these 14 controlled clinical trials, the overall incidence of adverse reactions was 73% in patients treated with alogliptin 25 mg compared to 75% with placebo and 70% with active comparator. Overall discontinuation of therapy due to adverse reactions was 6.8% with alogliptin 25 mg compared to 8.4% with placebo or 6.2% with active comparator.
Adverse reactions reported in ≥4% of patients treated with alogliptin 25 mg and more frequently than in patients who received placebo are summarized in Table 2.
| Number of Patients (%) | |||
| Alogliptin 25 mg | Placebo | Active Comparator | |
| N=6447 | N=3469 | N=2257 | |
| Nasopharyngitis | 309 (4.8) | 152 (4.4) | 113 (5.0) |
| Upper Respiratory Tract Infection | 287 (4.5) | 121 (3.5) | 113 (5.0) |
| Headache | 278 (4.3) | 101 (2.9) | 121 (5.4) |
Hypoglycemia
Hypoglycemic events were documented based upon a blood glucose value and/or clinical signs and symptoms of hypoglycemia.
In the monotherapy study, the incidence of hypoglycemia was 1.5% in patients treated with alogliptin compared to 1.6% with placebo. The use of alogliptin as add-on therapy to glyburide or insulin did not increase the incidence of hypoglycemia compared to placebo. In a monotherapy study comparing alogliptin to a sulfonylurea in elderly patients, the incidence of hypoglycemia was 5.4% with alogliptin compared to 26% with glipizide.
In the EXAMINE trial, the incidence of investigator reported hypoglycemia was 6.7% in patients receiving alogliptin and 6.5% in patients receiving placebo. Serious adverse reactions of hypoglycemia were reported in 0.8% of patients treated with alogliptin and in 0.6% of patients treated with placebo.
Renal Impairment
In glycemic control trials in patients with type 2 diabetes, 3.4% of patients treated with alogliptin and 1.3% of patients treated with placebo had renal function adverse reactions. The most commonly reported adverse reactions were renal impairment (0.5% for alogliptin and 0.1% for active comparators or placebo), decreased creatinine clearance (1.6% for alogliptin and 0.5% for active comparators or placebo) and increased blood creatinine (0.5% for alogliptin and 0.3% for active comparators or placebo) [see Use in Specific Populations (8.6)].
In the EXAMINE trial of high CV risk type 2 diabetes patients, 23% of patients treated with alogliptin and 21% of patients treated with placebo had an investigator reported renal impairment adverse reaction. The most commonly reported adverse reactions were renal impairment (7.7% for alogliptin and 6.7% for placebo), decreased glomerular filtration rate (4.9% for alogliptin and 4.3% for placebo) and decreased renal clearance (2.2% for alogliptin and 1.8% for placebo). Laboratory measures of renal function were also assessed. Estimated glomerular filtration rate decreased by 25% or more in 21.1% of patients treated with alogliptin and 18.7% of patients treated with placebo. Worsening of chronic kidney disease stage was seen in 16.8% of patients treated with alogliptin and in 15.5% of patients treated with placebo.
Pioglitazone
Over 8500 patients with type 2 diabetes have been treated with pioglitazone in randomized, double-blind, controlled clinical trials, including 2605 patients with type 2 diabetes and macrovascular disease treated with pioglitazone in the PROactive clinical trial. In these trials, over 6000 patients have been treated with pioglitazone for six months or longer, over 4500 patients have been treated with pioglitazone for one year or longer, and over 3000 patients have been treated with pioglitazone for at least two years.
Common Adverse Reactions: 16 to 26 Week Monotherapy Trials
A summary of the incidence and type of common adverse reactions reported in three pooled 16 to 26 week placebo-controlled monotherapy trials of pioglitazone is provided in Table 3. Terms that are reported represent those that occurred at an incidence of >5% and more commonly in patients treated with pioglitazone than in patients who received placebo. None of these adverse reactions were related to pioglitazone dose.
| % of Patients | ||
|---|---|---|
| Placebo | Pioglitazone | |
| N=259 | N=606 | |
| Upper Respiratory Tract Infection | 8.5 | 13.2 |
| Headache | 6.9 | 9.1 |
| Sinusitis | 4.6 | 6.3 |
| Myalgia | 2.7 | 5.4 |
| Pharyngitis | 0.8 | 5.1 |
Congestive Heart Failure
A summary of the incidence of adverse reactions related to congestive heart failure for the 16 to 24 week add-on to sulfonylurea trials, for the 16 to 24 week add-on to insulin trials, and for the 16 to 24 week add-on to metformin trials were (at least one congestive heart failure, 0.2% to 1.7%; hospitalized due to congestive heart failure, 0.2% to 0.9%). None of the reactions were fatal.
Patients with type 2 diabetes and NYHA class II or early class III congestive heart failure were randomized to receive 24 weeks of double-blind treatment with either pioglitazone at daily doses of 30 mg to 45 mg (N=262) or glyburide at daily doses of 10 mg to 15 mg (N=256). A summary of the incidence of adverse reactions related to congestive heart failure reported in this study is provided in Table 4.
| Number (%) of Subjects | ||
| Pioglitazone | Glyburide | |
| N=262 | N=256 | |
| Death due to cardiovascular causes (adjudicated) | 5 (1.9%) | 6 (2.3%) |
| Overnight hospitalization for worsening CHF (adjudicated) | 26 (9.9%) | 12 (4.7%) |
| Emergency room visit for CHF (adjudicated) | 4 (1.5%) | 3 (1.2%) |
| Patients experiencing CHF progression during study | 35 (13.4%) | 21 (8.2%) |
Congestive heart failure events leading to hospitalization that occurred during the PROactive trial are summarized in Table 5.
| Number (%) of Patients | ||
| Placebo | Pioglitazone | |
| N=2633 | N=2605 | |
| At least one hospitalized congestive heart failure event | 108 (4.1%) | 149 (5.7%) |
| Fatal | 22 (0.8%) | 25 (1%) |
| Hospitalized, nonfatal | 86 (3.3%) | 124 (4.7%) |
Cardiovascular Safety
In the PROactive trial, 5238 patients with type 2 diabetes and a history of macrovascular disease were randomized to pioglitazone (N=2605), force-titrated up to 45 mg daily or placebo (N=2633) in addition to standard of care. Almost all patients (95%) were receiving cardiovascular medications (beta blockers, ACE inhibitors, angiotensin II receptor blockers, calcium channel blockers, nitrates, diuretics, aspirin, statins and fibrates). At baseline, patients had a mean age of 62 years, mean duration of diabetes of 9.5 years and mean A1C of 8.1%. Mean duration of follow-up was 34.5 months.
The primary objective of this trial was to examine the effect of pioglitazone on mortality and macrovascular morbidity in patients with type 2 diabetes mellitus who were at high risk for macrovascular events. The primary efficacy variable was the time to the first occurrence of any event in a cardiovascular composite endpoint that included all-cause mortality, nonfatal myocardial infarction (MI) including silent MI, stroke, acute coronary syndrome, cardiac intervention including coronary artery bypass grafting or percutaneous intervention, major leg amputation above the ankle and bypass surgery or revascularization in the leg. A total of 514 (19.7%) patients treated with pioglitazone and 572 (21.7%) placebo-treated patients experienced at least one event from the primary composite endpoint (hazard ratio 0.90; 95% Confidence Interval: 0.80, 1.02; p=0.10).
Although there was no statistically significant difference between pioglitazone and placebo for the three year incidence of a first event within this composite, there was no increase in mortality or in total macrovascular events with pioglitazone. The number of first occurrences and total individual events contributing to the primary composite endpoint is shown in Table 6.
| CABG=coronary artery bypass grafting; PCI=percutaneous intervention | ||||
| Placebo
N=2633 | Pioglitazone
N=2605 |
|||
| Cardiovascular Events | First Events n (%) | Total Events n | First Events n (%) | Total Events n |
| Any Event | 572 (21.7) | 900 | 514 (19.7) | 803 |
| All-Cause Mortality | 122 (4.6) | 186 | 110 (4.2) | 177 |
| Nonfatal Myocardial Infarction (MI) | 118 (4.5) | 157 | 105 (4) | 131 |
| Stroke | 96 (3.6) | 119 | 76 (2.9) | 92 |
| Acute Coronary Syndrome | 63 (2.4) | 78 | 42 (1.6) | 65 |
| Cardiac Intervention (CABG/PCI) | 101 (3.8) | 240 | 101 (3.9) | 195 |
| Major Leg Amputation | 15 (0.6) | 28 | 9 (0.3) | 28 |
| Leg Revascularization | 57 (2.2) | 92 | 71 (2.7) | 115 |
Weight Gain
Dose-related weight gain occurs when pioglitazone is used alone or in combination with other antidiabetic medications. The mechanism of weight gain is unclear but probably involves a combination of fluid retention and fat accumulation.
Edema
Edema induced from taking pioglitazone is reversible when pioglitazone is discontinued. The edema usually does not require hospitalization unless there is coexisting congestive heart failure.
Hepatic Effects
There has been no evidence of pioglitazone-induced hepatotoxicity in the pioglitazone controlled clinical trial database to date. One randomized, double-blind, three-year trial comparing pioglitazone to glyburide as add-on to metformin and insulin therapy was specifically designed to evaluate the incidence of serum ALT elevation to greater than three times the upper limit of the reference range, measured every eight weeks for the first 48 weeks of the trial then every 12 weeks thereafter. A total of 3/1051 (0.3%) patients treated with pioglitazone and 9/1046 (0.9%) patients treated with glyburide developed ALT values greater than three times the upper limit of the reference range. None of the patients treated with pioglitazone in the pioglitazone controlled clinical trial database to date have had a serum ALT greater than three times the upper limit of the reference range and a corresponding total bilirubin greater than two times the upper limit of the reference range, a combination predictive of the potential for severe drug-induced liver injury.
Hypoglycemia
In the pioglitazone clinical trials, adverse reactions of hypoglycemia were reported based on clinical judgment of the investigators and did not require confirmation with finger stick glucose testing. In the 16 week add-on to sulfonylurea trial, the incidence of reported hypoglycemia was 3.7% with pioglitazone 30 mg and 0.5% with placebo. In the 16 week add-on to insulin trial, the incidence of reported hypoglycemia was 7.9% with pioglitazone 15 mg, 15.4% with pioglitazone 30 mg and 4.8% with placebo. The incidence of reported hypoglycemia was higher with pioglitazone 45 mg compared to pioglitazone 30 mg in both the 24 week add-on to sulfonylurea trial (15.7% versus 13.4%) and in the 24 week add-on to insulin trial (47.8% versus 43.5%). Three patients in these four trials were hospitalized due to hypoglycemia. All three patients were receiving pioglitazone 30 mg (0.9%) in the 24 week add-on to insulin trial. An additional 14 patients reported severe hypoglycemia (defined as causing considerable interference with patient's usual activities) that did not require hospitalization. These patients were receiving pioglitazone 45 mg in combination with sulfonylurea (N=2) or pioglitazone 30 mg or 45 mg in combination with insulin (N=12).
Urinary Bladder Tumors
Tumors were observed in the urinary bladder of male rats in the two year carcinogenicity study [see Nonclinical Toxicology (13.1)]. During the three year PROactive clinical trial, 14 patients out of 2605 (0.54%) randomized to pioglitazone and 5 out of 2633 (0.19%) randomized to placebo were diagnosed with bladder cancer. After excluding patients in whom exposure to study drug was less than one year at the time of diagnosis of bladder cancer, there were six (0.23%) cases on pioglitazone and two (0.08%) cases on placebo. After completion of the trial, a large subset of patients was observed for up to ten additional years, with little additional exposure to pioglitazone. During the 13 years of both PROactive and observational follow-up, the occurrence of bladder cancer did not differ between patients randomized to pioglitazone or placebo (HR =1.00; 95% CI: 0.59-1.72) [see Warnings and Precautions (5.7)].
Laboratory Abnormalities
Pioglitazone
Hematologic Effects
Pioglitazone may cause decreases in hemoglobin and hematocrit. In placebo-controlled monotherapy trials, mean hemoglobin values declined by 2% to 4% in patients treated with pioglitazone compared with a mean change in hemoglobin of -1% to +1% in placebo-treated patients. These changes primarily occurred within the first four to 12 weeks of therapy and remained relatively constant thereafter. These changes may be related to increased plasma volume associated with pioglitazone therapy and are not likely to be associated with any clinically significant hematologic effects.
Creatine Phosphokinase
During protocol-specified measurement of serum creatine phosphokinase (CPK) in pioglitazone clinical trials, an isolated elevation in CPK to greater than ten times the upper limit of the reference range was noted in nine (0.2%) patients treated with pioglitazone (values of 2150 to 11400 IU/L) and in no comparator-treated patients. Six of these nine patients continued to receive pioglitazone, two patients were noted to have the CPK elevation on the last day of dosing and one patient discontinued pioglitazone due to the elevation. These elevations resolved without any apparent clinical sequelae. The relationship of these events to pioglitazone therapy is unknown.
6.2 Postmarketing Experience
Alogliptin
The following adverse reactions have been identified during the postmarketing use of alogliptin. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Gastrointestinal disorders: acute pancreatitis, diarrhea, constipation, nausea, ileus
Hepatobiliary disorders: fulminant hepatic failure
Immune system disorders: hypersensitivity reactions including anaphylaxis
Investigations: hepatic enzyme elevations
Musculoskeletal and Connective Tissue Disorders: severe and disabling arthralgia, rhabdomyolysis
Renal and urinary disorders: tubulointerstitial nephritis
Skin and subcutaneous tissue disorders: angioedema, rash, urticaria and severe cutaneous adverse reactions including Stevens-Johnson syndrome, bullous pemphigoid
Pioglitazone
The following adverse reactions have been identified during the postmarketing use of pioglitazone. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Cardiac disorders: rapid increases in weight and increases in excess of that generally observed in clinical trials, excessive edema, congestive heart failure both with and without previously known heart disease and both with and without concomitant insulin administration
Eye disorders: New onset or worsening diabetic macular edema with decreased visual
Hepatobiliary disorders: Fatal and nonfatal hepatic failure
7 DRUG INTERACTIONS
Alogliptin
Alogliptin is primarily renally excreted. Cytochrome (CYP) P450-related metabolism is negligible. No significant drug-drug interactions were observed with the CYP-substrates or inhibitors tested or with renally excreted drugs [see Clinical Pharmacology (12.3)].
7.1 Strong CYP2C8 Inhibitors
Pioglitazone
An inhibitor of CYP2C8 (e.g., gemfibrozil) significantly increases the exposure (area under the concentration-time curve [AUC]) and half-life of pioglitazone. Therefore, the maximum recommended dose of pioglitazone is 15 mg daily if used in combination with gemfibrozil or other strong CYP2C8 inhibitors [see Dosage and Administration (2.3) and Clinical Pharmacology (12.3)].
7.2 CYP2C8 Inducers
Pioglitazone
An inducer of CYP2C8 (e.g., rifampin) may significantly decrease the exposure (AUC) of pioglitazone. Therefore, if an inducer of CYP2C8 is started or stopped during treatment with alogliptin and pioglitazone tablets, changes in diabetes treatment may be needed based on clinical response without exceeding the maximum recommended daily dose of 45 mg for pioglitazone [see Clinical Pharmacology (12.3)].
7.3 Topiramate
Pioglitazone
A decrease in the exposure of pioglitazone and its active metabolites were noted with concomitant administration of pioglitazone and topiramate [see Clinical Pharmacology (12.3)]. The clinical relevance of this decrease is unknown; however, when pioglitazone and topiramate are used concomitantly, monitor patients for adequate glycemic control.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary
Limited data with alogliptin and pioglitazone tablets in pregnant women are not sufficient to inform a drug-associated risk for major birth defects or miscarriage. There are risks to the mother and fetus associated with poorly controlled diabetes in pregnancy [see Clinical Considerations].
In animal reproduction studies, no adverse developmental effects were observed when pioglitazone was administered to pregnant rats and rabbits during organogenesis at exposures up to 5 and 35 times the 45 mg clinical dose, respectively, based on body surface area. No adverse developmental effects were observed when alogliptin was administered to pregnant rats and rabbits during organogenesis at exposures 180 and 149 times the 25 mg clinical dose, respectively, based on plasma drug exposure (AUC) [see Data].
The estimated background risk of major birth defects is 6-10% in women with pre-gestational diabetes with a HbA1c >7 and has been reported to be as high as 20-25% in women with a HbA1c >10. The estimated background risk of miscarriage for the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Clinical Considerations
Disease-associated maternal and/or embryo/fetal risk
Poorly controlled diabetes in pregnancy increases the maternal risk for diabetic ketoacidosis, pre-eclampsia, spontaneous abortions, preterm delivery and delivery complications. Poorly controlled diabetes increases the fetal risk for major birth defects, still birth, and macrosomia related morbidity.
Data
Animal Data
Alogliptin and Pioglitazone
Co-administration of 100 mg/kg alogliptin and 40 mg/kg pioglitazone (39 and 10 times the 25 mg and 45 mg clinical doses, respectively, based on body surface area) to pregnant rats during organogenesis slightly augmented pioglitazone-related fetal effects of delayed development and reduced fetal weights but did not result in embryofetal mortality or teratogenicity.
Alogliptin
Alogliptin administered to pregnant rabbits and rats during the period of organogenesis did not cause adverse developmental effects at doses of up to 200 mg/kg and 500 mg/kg, or 149 times and 180 times, the 25 mg clinical dose, respectively, based on plasma drug exposure (AUC). Placental transfer of alogliptin into the fetus was observed following oral dosing to pregnant rats.
No adverse developmental outcomes were observed in offspring when alogliptin was administered to pregnant rats during gestation and lactation at doses up to 250 mg/kg (~95 times the 25 mg clinical dose, based on AUC).
Pioglitazone
Pioglitazone administered to pregnant rats during organogenesis did not cause adverse developmental effects at a dose of 20 mg/kg (~5 times the 45 mg clinical dose), but delayed parturition and reduced embryofetal viability at 40 and 80 mg/kg, or ≥9 times the 45 mg clinical dose, by body surface area. In pregnant rabbits administered pioglitazone during organogenesis, no adverse developmental effects were observed at 80 mg/kg (~35 times the 45 mg clinical dose), but reduced embryofetal viability at 160 mg/kg, or ~69 times the 45 mg clinical dose, by body surface area. When pregnant rats received pioglitazone during late gestation and lactation, delayed postnatal development, attributed to decreased body weight, occurred in offspring at maternal doses of 10 mg/kg and above or ≥2 times the 45 mg clinical dose, by body surface area.
8.2 Lactation
Risk Summary
There is no information regarding the presence of pioglitazone or alogliptin in human milk, the effects on the breastfed infant, or the effects on milk production. Pioglitazone and alogliptin are present in rat milk; however, due to species-specific differences in lactation physiology, animal data may not reliably predict drug levels in human milk. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for alogliptin and pioglitazone tablets and any potential adverse effects on the breastfed infant from alogliptin and pioglitazone tablets or from the underlying maternal condition.
8.3 Females and Males of Reproductive Potential
Discuss the potential for unintended pregnancy with premenopausal women as therapy with pioglitazone, like other thiazolidinediones, may result in ovulation in some anovulatory women.
8.4 Pediatric Use
Safety and effectiveness of alogliptin and pioglitazone tablets in pediatric patients have not been established.
Alogliptin and pioglitazone tablets are not recommended for use in pediatric patients based on adverse effects observed in adults, including fluid retention and congestive heart failure, fractures and urinary bladder tumors [see Warnings and Precautions (5.1, 5.5, 5.6, 5.7)].
8.5 Geriatric Use
Alogliptin and Pioglitazone
Of the total number of patients (N=1533) in clinical safety and efficacy studies treated with alogliptin and pioglitazone, 248 (16.2%) patients were 65 years and older and 15 (1%) patients were 75 years and older. No overall differences in safety or effectiveness were observed between these patients and younger patients. While this and other reported clinical experiences have not identified differences in responses between the elderly and younger patients, greater sensitivity of some older individuals cannot be excluded.
Alogliptin
Of the total number of patients (N=9052) in clinical safety and efficacy studies treated with alogliptin, 2257 (24.9%) patients were ≥65 years old and 386 (4.3%) patients were ≥75 years old. No overall differences in safety or effectiveness were observed between patients ≥65 years old and younger patients.
Pioglitazone
A total of 92 patients (15.2%) treated with pioglitazone in the three pooled, 16 to 26 week, double-blind, placebo-controlled, monotherapy trials were ≥65 years old and two patients (0.3%) were ≥75 years old. In the two pooled 16 to 24 week add-on to sulfonylurea trials, 201 patients (18.7%) treated with pioglitazone were ≥65 years old and 19 (1.8%) were ≥75 years old. In the two pooled 16 to 24 week add-on to metformin trials, 155 patients (15.5%) treated with pioglitazone were ≥65 years old and 19 (1.9%) were ≥75 years old. In the two pooled 16 to 24 week add-on to insulin trials, 272 patients (25.4%) treated with pioglitazone were ≥65 years old and 22 (2.1%) were ≥75 years old.
In PROactive, 1068 patients (41%) treated with pioglitazone were ≥65 years old and 42 (1.6%) were ≥75 years old.
In pharmacokinetic studies with pioglitazone, no significant differences were observed in pharmacokinetic parameters between elderly and younger patients. These clinical experiences have not identified differences in effectiveness and safety between the elderly (≥65 years) and younger patients although small sample sizes for patients ≥75 years old limit conclusions [see Clinical Pharmacology (12.3)].
8.6 Renal Impairment
Alogliptin
A total of 602 patients with moderate renal impairment (eGFR ≥30 and <60 mL/min/1.73 m2) and four patients with severe renal impairment/end-stage renal disease (eGFR <30 mL/min/1.73 m2 or <15 mL/min/1.73 m2, respectively) at baseline were treated with alogliptin in clinical trials in patients with type 2 diabetes. Reductions in HbA1c were generally similar in this subgroup of patients. The overall incidence of adverse reactions was generally balanced between alogliptin and placebo treatments in this subgroup of patients.
In the EXAMINE trial of high CV risk type 2 diabetes patients, 694 patients had moderate renal impairment and 78 patients had severe renal impairment or end-stage renal disease at baseline. The overall incidences of adverse reactions, serious adverse reactions and adverse reactions leading to study drug discontinuation were generally similar between the treatment groups.
8.7 Hepatic Impairment
Alogliptin
No dose adjustments are required in patients with mild to moderate hepatic impairment (Child-Pugh Grade A and B) based on insignificant change in systemic exposures (e.g., AUC) compared to subjects with normal hepatic function in a pharmacokinetic study. Alogliptin has not been studied in patients with severe hepatic impairment (Child-Pugh Grade C). Use caution when administering alogliptin to patients with liver disease [see Warnings and Precautions (5.4)].
Pioglitazone
No dose adjustments are required in patients with hepatic impairment (Child-Pugh Grade B and C) based on insignificant change in systemic exposures (e.g., AUC) compared to subjects with normal hepatic function in a pharmacokinetic study. However, use with caution in patients with liver disease [see Warnings and Precautions (5.4)].
10 OVERDOSAGE
In the event of an overdose, it is reasonable to institute the necessary clinical monitoring and supportive therapy as dictated by the patient's clinical status. Per clinical judgment, it may be reasonable to initiate removal of unabsorbed material from the gastrointestinal tract.
Alogliptin is minimally dialyzable; over a three-hour hemodialysis session, approximately 7% of the drug was removed. Therefore, hemodialysis is unlikely to be beneficial in an overdose situation. It is not known if alogliptin is dialyzable by peritoneal dialysis.
To contact the poison control center, call 1-800-222-1222.
11 DESCRIPTION
Alogliptin and pioglitazone tablets contain two oral antihyperglycemic drugs used in the management of type 2 diabetes: alogliptin and pioglitazone.
Alogliptin
Alogliptin is a selective, orally bioavailable inhibitor of the enzymatic activity of dipeptidyl peptidase-4 (DPP-4). Chemically, alogliptin is prepared as a benzoate salt, which is identified as 2-({6-[(3R)-3-aminopiperidin-1-yl]-3-methyl-2,4-dioxo-3,4-dihydropyrimidin-1(2H)-yl}methyl)benzonitrile monobenzoate. It has a molecular formula of C18H21N5O2∙C7H6O2 and a molecular weight of 461.51 daltons. The structural formula is:
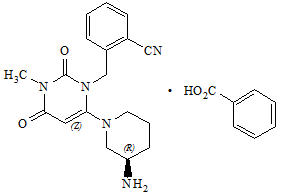
Alogliptin benzoate is a white to off-white crystalline powder containing one asymmetric carbon in the aminopiperidine moiety. It is soluble in dimethylsulfoxide, sparingly soluble in water and methanol, slightly soluble in ethanol and very slightly soluble in octanol and isopropyl acetate.
Pioglitazone
Pioglitazone is an oral antihyperglycemic agent that acts primarily by decreasing insulin resistance. Chemically, pioglitazone is prepared as hydrochloride salt, which is identified as (±)-5-[[4-[2-(5-ethyl-2-pyridinyl)ethoxy]phenyl]methyl]-2,4-thiazolidinedione monohydrochloride. It has a molecular formula of C19H20N2O3S∙HCl and a molecular weight of 392.90 daltons. The structural formula is:
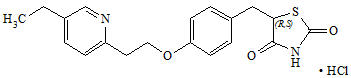
Pioglitazone hydrochloride is an odorless white crystalline powder that contains one asymmetric carbon in the thiazolidinedione moiety. The synthetic compound is a racemate and the two enantiomers of pioglitazone interconvert in vivo. It is soluble in N,N dimethylformamide, slightly soluble in anhydrous ethanol, very slightly soluble in acetone and acetonitrile, practically insoluble in water and insoluble in ether.
Alogliptin and pioglitazone tablets are available as a fixed-dose combination tablet for oral administration containing 34 mg alogliptin benzoate equivalent to 25 mg alogliptin and any of the following strengths of pioglitazone hydrochloride:
- 16.53 mg pioglitazone hydrochloride equivalent to 15 mg pioglitazone (25 mg/15 mg)
- 33.06 mg pioglitazone hydrochloride equivalent to 30 mg pioglitazone (25 mg/30 mg)
- 49.59 mg pioglitazone hydrochloride equivalent to 45 mg pioglitazone (25 mg/45 mg)
Alogliptin and pioglitazone tablets are also available as a fixed-dose combination tablet for oral administration containing 17 mg alogliptin benzoate equivalent to 12.5 mg alogliptin and any of the following strengths of pioglitazone hydrochloride:
- 16.53 mg pioglitazone hydrochloride equivalent to 15 mg pioglitazone (12.5 mg/15 mg)
- 33.06 mg pioglitazone hydrochloride equivalent to 30 mg pioglitazone (12.5 mg/30 mg)
- 49.59 mg pioglitazone hydrochloride equivalent to 45 mg pioglitazone (12.5 mg/45 mg)
Alogliptin and pioglitazone tablets contain the following inactive ingredients: mannitol, microcrystalline cellulose, hydroxypropyl cellulose, croscarmellose sodium, magnesium stearate and lactose monohydrate; the tablets are film-coated with hypromellose, polyethylene glycol, titanium dioxide, talc and ferric oxide (yellow and/or red) and are marked with printing ink (Red A1 or Gray F1).
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Alogliptin and pioglitazone tablets combine two antihyperglycemic agents with complementary and distinct mechanisms of action to improve glycemic control in patients with type 2 diabetes: alogliptin, a selective inhibitor of DPP-4, and pioglitazone, a member of the TZD class.
Alogliptin
Increased concentrations of the incretin hormones such as glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP) are released into the bloodstream from the small intestine in response to meals. These hormones cause insulin release from the pancreatic beta cells in a glucose-dependent manner but are inactivated by the dipeptidyl peptidase-4 (DPP-4) enzyme within minutes. GLP-1 also lowers glucagon secretion from pancreatic alpha cells, reducing hepatic glucose production. In patients with type 2 diabetes, concentrations of GLP-1 are reduced but the insulin response to GLP-1 is preserved. Alogliptin is a DPP-4 inhibitor that slows the inactivation of the incretin hormones, thereby increasing their bloodstream concentrations and reducing fasting and postprandial glucose concentrations in a glucose-dependent manner in patients with type 2 diabetes mellitus. Alogliptin selectively binds to and inhibits DPP-4 but not DPP-8 or DPP-9 activity in vitro at concentrations approximating therapeutic exposures.
Pioglitazone
Pharmacologic studies indicate that pioglitazone improves insulin sensitivity in muscle and adipose tissue while inhibiting hepatic gluconeogenesis. Unlike sulfonylureas, pioglitazone is not an insulin secretagogue. Pioglitazone is an agonist for peroxisome proliferator-activated receptor-gamma (PPARγ). PPAR receptors are found in tissues important for insulin action such as adipose tissue, skeletal muscle and liver. Activation of PPARγ nuclear receptors modulates the transcription of a number of insulin- responsive genes involved in the control of glucose and lipid metabolism.
In animal models of diabetes, pioglitazone reduces the hyperglycemia, hyperinsulinemia and hypertriglyceridemia characteristic of insulin-resistant states such as type 2 diabetes. The metabolic changes produced by pioglitazone result in increased responsiveness of insulin-dependent tissues and are observed in numerous animal models of insulin resistance.
Because pioglitazone enhances the effects of circulating insulin (by decreasing insulin resistance), it does not lower blood glucose in animal models that lack endogenous insulin.
12.2 Pharmacodynamics
Alogliptin and Pioglitazone
In a 26 week, randomized, active-controlled study, patients with type 2 diabetes received alogliptin 25 mg coadministered with pioglitazone 30 mg, alogliptin 12.5 mg coadministered with pioglitazone 30 mg, alogliptin 25 mg alone or pioglitazone 30 mg alone. Patients who were randomized to alogliptin 25 mg with pioglitazone 30 mg achieved a 26.2% decrease in triglyceride levels from a mean baseline of 214.2 mg/dL compared to an 11.5% decrease for alogliptin alone and a 21.8% decrease for pioglitazone alone. In addition, a 14.4% increase in HDL cholesterol levels from a mean baseline of 43.2 mg/dL was also observed for alogliptin 25 mg with pioglitazone 30 mg compared to a 1.9% increase for alogliptin alone and a 13.2% increase for pioglitazone alone. The changes in measures of LDL cholesterol and total cholesterol were similar between alogliptin 25 mg with pioglitazone 30 mg versus alogliptin alone and pioglitazone alone. A similar pattern of lipid effects was observed in a 26 week, placebo-controlled factorial study.
Alogliptin
Single-dose administration of alogliptin to healthy subjects resulted in a peak inhibition of DPP-4 within two to three hours after dosing. The peak inhibition of DPP-4 exceeded 93% across doses of 12.5 mg to 800 mg. Inhibition of DPP-4 remained above 80% at 24 hours for doses greater than or equal to 25 mg. Peak and total exposure over 24 hours to active GLP-1 were three- to four-fold greater with alogliptin (at doses of 25 to 200 mg) than placebo. In a 16 week, double-blind, placebo-controlled study alogliptin 25 mg demonstrated decreases in postprandial glucagon while increasing postprandial active GLP-1 levels compared to placebo over an eight-hour period following a standardized meal. It is unclear how these findings relate to changes in overall glycemic control in patients with type 2 diabetes mellitus. In this study, alogliptin 25 mg demonstrated decreases in two-hour postprandial glucose compared to placebo (-30 mg/dL versus 17 mg/dL respectively).
Multiple-dose administration of alogliptin to patients with type 2 diabetes also resulted in a peak inhibition of DPP-4 within one to two hours and exceeded 93% across all doses (25 mg, 100 mg and 400 mg) after a single dose and after 14 days of once-daily dosing. At these doses of alogliptin, inhibition of DPP-4 remained above 81% at 24 hours after 14 days of dosing.
Pioglitazone
Clinical studies demonstrate that pioglitazone improves insulin sensitivity in insulin-resistant patients. Pioglitazone enhances cellular responsiveness to insulin, increases insulin-dependent glucose disposal, and improves hepatic sensitivity to insulin. In patients with type 2 diabetes, the decreased insulin resistance produced by pioglitazone results in lower plasma glucose concentrations, lower plasma insulin concentrations and lower A1C values. In controlled clinical trials, pioglitazone had an additive effect on glycemic control when used in combination with a sulfonylurea, metformin or insulin [see Clinical Studies (14)]. Patients with lipid abnormalities were included in clinical trials with pioglitazone. Overall, patients treated with pioglitazone had mean decreases in serum triglycerides, mean increases in HDL cholesterol and no consistent mean changes in LDL and total cholesterol. There is no conclusive evidence of macrovascular benefit with pioglitazone [see Warnings and Precautions (5.12) and Adverse Reactions (6.1)].
In a 26 week, placebo-controlled, dose-ranging monotherapy study, mean serum triglycerides decreased in the pioglitazone 15 mg, 30 mg and 45 mg dose groups compared to a mean increase in the placebo group. Mean HDL cholesterol increased to a greater extent in patients treated with pioglitazone than in the placebo-treated patients. There were no consistent differences for LDL and total cholesterol in patients treated with pioglitazone compared to placebo (Table 7).
| Placebo | Pioglitazone 15 mg Once Daily | Pioglitazone 30 mg Once Daily | Pioglitazone 45 mg Once Daily |
|
|---|---|---|---|---|
| Triglycerides (mg/dL) | N=79 | N=79 | N=84 | N=77 |
| Baseline (mean) | 263 | 284 | 261 | 260 |
| Percent change from baseline (adjusted mean*) | 4.8% | -9%† | -9.6%† | -9.3%† |
| HDL Cholesterol (mg/dL) | N=79 | N=79 | N=83 | N=77 |
| Baseline (mean) | 42 | 40 | 41 | 41 |
| Percent change from baseline (adjusted mean*) | 8.1% | 14.1%† | 12.2% | 19.1%† |
| LDL Cholesterol (mg/dL) | N=65 | N=63 | N=74 | N=62 |
| Baseline (mean) | 139 | 132 | 136 | 127 |
| Percent change from baseline (adjusted mean*) | 4.8% | 7.2% | 5.2% | 6% |
| Total Cholesterol (mg/dL) | N=79 | N=79 | N=84 | N=77 |
| Baseline (mean) | 225 | 220 | 223 | 214 |
| Percent change from baseline (adjusted mean*) | 4.4% | 4.6% | 3.3% | 6.4% |
In the two other monotherapy studies (16 weeks and 24 weeks) and in combination therapy studies with sulfonylurea (16 weeks and 24 weeks), metformin (16 weeks and 24 weeks) or insulin (16 weeks and 24 weeks), the lipid results were generally consistent with the data above.
12.3 Pharmacokinetics
Absorption and Bioavailability
Alogliptin and Pioglitazone
In bioequivalence studies of alogliptin and pioglitazone tablets, the area under the plasma concentration curve (AUC) and maximum concentration (Cmax) of both the alogliptin and the pioglitazone component following a single dose of the combination tablet (12.5 mg/15 mg or 25 mg/45 mg) were bioequivalent to alogliptin (12.5 mg or 25 mg) concomitantly administered with pioglitazone (15 mg or 45 mg respectively) tablets under fasted conditions in healthy subjects.
Administration of alogliptin and pioglitazone tablets 25 mg/45 mg with food resulted in no significant change in overall exposure of alogliptin or pioglitazone. Alogliptin and pioglitazone tablets may therefore be administered with or without food.
Distribution
Alogliptin
Following a single, 12.5 mg intravenous infusion of alogliptin to healthy subjects, the volume of distribution during the terminal phase was 417 L, indicating that the drug is well distributed into tissues.
Alogliptin is 20% bound to plasma proteins.
Pioglitazone
The mean apparent Vd/F of pioglitazone following single-dose administration is 0.63 ± 0.41 (mean ± SD) L/kg of body weight. Pioglitazone is extensively protein bound (>99%) in human serum, principally to serum albumin. Pioglitazone also binds to other serum proteins, but with lower affinity. Metabolites M-III and M-IV also are extensively bound (>98%) to serum albumin.
Metabolism
Alogliptin
Alogliptin does not undergo extensive metabolism and 60% to 71% of the dose is excreted as unchanged drug in the urine.
Two minor metabolites were detected following administration of an oral dose of [14C] alogliptin, N-demethylated, M-I (less than 1% of the parent compound), and N-acetylated alogliptin, M-II (less than 6% of the parent compound). M-I is an active metabolite and is an inhibitor of DPP-4 similar to the parent molecule; M-II does not display any inhibitory activity toward DPP-4 or other DPP-related enzymes. In vitro data indicate that CYP2D6 and CYP3A4 contribute to the limited metabolism of alogliptin.
Alogliptin exists predominantly as the (R)-enantiomer (more than 99%) and undergoes little or no chiral conversion in vivo to the (S)-enantiomer. The (S)-enantiomer is not detectable at the 25 mg dose.
Pioglitazone
Pioglitazone is extensively metabolized by hydroxylation and oxidation; the metabolites also partly convert to glucuronide or sulfate conjugates. Metabolites M-III and M-IV are the major circulating active metabolites in humans. Following once-daily administration of pioglitazone, steady-state serum concentrations of both pioglitazone and its major active metabolites, M-III (keto derivative of pioglitazone) and M-IV (hydroxyl derivative of pioglitazone), are achieved within seven days. At steady-state, M-III and M-IV reach serum concentrations equal to or greater than that of pioglitazone. At steady-state, in both healthy volunteers and patients with type 2 diabetes, pioglitazone comprises approximately 30% to 50% of the peak total pioglitazone serum concentrations (pioglitazone plus active metabolites) and 20% to 25% of the total AUC.
Maximum serum concentration (Cmax), AUC and trough serum concentrations (Cmin) for pioglitazone and M-III and M-IV, increased proportionally with administered doses of 15 mg and 30 mg per day.
In vitro data demonstrate that multiple CYP isoforms are involved in the metabolism of pioglitazone. The cytochrome P450 isoforms involved are CYP2C8 and, to a lesser degree, CYP3A4 with additional contributions from a variety of other isoforms, including the mainly extrahepatic CYP1A1. In vivo studies of pioglitazone in combination with gemfibrozil, a strong CYP2C8 inhibitor, showed that pioglitazone is a CYP2C8 substrate [see Dosage and Administration (2.3) and Drug Interactions (7)]. Urinary 6β-hydroxycortisol/cortisol ratios measured in patients treated with pioglitazone showed that pioglitazone is not a strong CYP3A4 enzyme inducer.
Excretion and Elimination
Alogliptin
The primary route of elimination of [14C] alogliptin derived radioactivity occurs via renal excretion (76%) with 13% recovered in the feces, achieving a total recovery of 89% of the administered radioactive dose. The renal clearance of alogliptin (9.6 L/hr) indicates some active renal tubular secretion and systemic clearance was 14.0 L/hr.
Pioglitazone
Following oral administration, approximately 15% to 30% of the pioglitazone dose is recovered in the urine. Renal elimination of pioglitazone is negligible, and the drug is excreted primarily as metabolites and their conjugates. It is presumed that most of the oral dose is excreted into the bile either unchanged or as metabolites and eliminated in the feces.
The mean serum half-life of pioglitazone and its metabolites (M-III and M-IV) range from three to seven hours and 16 to 24 hours, respectively. Pioglitazone has an apparent clearance, CL/F, calculated to be 5 to 7 L/hr.
Special Populations
Renal Impairment
Alogliptin
A single-dose, open-label study was conducted to evaluate the pharmacokinetics of alogliptin 50 mg in patients with chronic renal impairment compared with healthy subjects.
In patients with mild renal impairment (creatinine clearance [CrCl] ≥60 to <90 mL/min), an approximate 1.2 fold increase in plasma AUC of alogliptin was observed. Because increases of this magnitude are not considered clinically relevant, dose adjustment for patients with mild renal impairment is not recommended.
In patients with moderate renal impairment (CrCl ≥30 to <60 mL/min), an approximate two fold increase in plasma AUC of alogliptin was observed. To maintain similar systemic exposures of alogliptin and pioglitazone tablets to those with normal renal function, the recommended dose of alogliptin and pioglitazone tablets is 12.5 mg/15 mg, 12.5 mg/30 mg or 12.5 mg/45 mg once daily in patients with moderate renal impairment.
In patients with severe renal impairment (CrCl ≥15 to <30 mL/min) and end-stage renal disease (ESRD) (CrCl <15 mL/min or requiring dialysis), an approximate three and four fold increase in plasma AUC of alogliptin were observed, respectively. Dialysis removed approximately 7% of the drug during a three hour dialysis session. Alogliptin and pioglitazone tablets are not recommended for patients with severe renal impairment or ESRD. Coadministration of pioglitazone and alogliptin 6.25 mg once daily based on individual requirements may be considered in these patients.
Pioglitazone
The serum elimination half-life of pioglitazone, M-III and M-IV remains unchanged in patients with moderate (creatinine clearance 30 to 50 mL/min) to severe (creatinine clearance <30 mL/min) renal impairment when compared to subjects with normal renal function. Therefore no dose adjustment in patients with renal impairment is required.
Hepatic Impairment
Alogliptin
Total exposure to alogliptin was approximately 10% lower and peak exposure was approximately 8% lower in patients with moderate hepatic impairment (Child-Pugh Grade B) compared to healthy subjects. The magnitude of these reductions is not considered to be clinically meaningful. Patients with severe hepatic impairment (Child-Pugh Grade C) have not been studied. Use caution when administering alogliptin and pioglitazone tablets to patients with liver disease [see Use in Specific Populations (8.7) and Warnings and Precautions (5.4)].
Pioglitazone
Compared with healthy controls, subjects with impaired hepatic function (Child-Pugh Grade B and C) have an approximate 45% reduction in pioglitazone and total pioglitazone (pioglitazone, M-III and M-IV) mean peak concentrations but no change in the mean AUC values. Therefore, no dose adjustment in patients with hepatic impairment is required.
There are postmarketing reports of liver failure with pioglitazone and clinical trials have generally excluded patients with serum ALT >2.5 times the upper limit of the reference range. Use caution in patients with liver disease [see Warnings and Precautions (5.4)].
Gender
Alogliptin
No dose adjustment of alogliptin is necessary based on gender. Gender did not have any clinically meaningful effect on the pharmacokinetics of alogliptin.
Pioglitazone
The mean Cmax and AUC values of pioglitazone were increased 20% to 60% in women compared to men. In controlled clinical trials, A1C decreases from baseline were generally greater for females than for males (average mean difference in A1C 0.5%). Because therapy should be individualized for each patient to achieve glycemic control, no dose adjustment is recommended based on gender alone.
Geriatric
Alogliptin
No dose adjustment of alogliptin is necessary based on age. Age did not have any clinically meaningful effect on the pharmacokinetics of alogliptin.
Pioglitazone
In healthy elderly subjects, peak serum concentrations of pioglitazone and total pioglitazone are not significantly different, but AUC values are approximately 21% higher than those achieved in younger subjects. The mean terminal half-life values of pioglitazone were also longer in elderly subjects (about ten hours) as compared to younger subjects (about seven hours). These changes were not of a magnitude that would be considered clinically relevant.
Pediatrics
Alogliptin
Studies characterizing the pharmacokinetics of alogliptin in pediatric patients have not been performed.
Pioglitazone
Safety and efficacy of pioglitazone in pediatric patients have not been established. Pioglitazone is not recommended for use in pediatric patients [see Use in Specific Populations (8.4)].
Drug Interactions
Coadministration of alogliptin 25 mg once daily with a CYP2C8 substrate, pioglitazone 45 mg once daily for 12 days had no clinically meaningful effects on the pharmacokinetics of pioglitazone and its active metabolites.
Specific pharmacokinetic drug interaction studies with alogliptin and pioglitazone tablets have not been performed, although such studies have been conducted with the individual components of alogliptin and pioglitazone tablets (alogliptin and pioglitazone).
Alogliptin
In Vitro Assessment of Drug Interactions
In vitro studies indicate that alogliptin is neither an inducer of CYP1A2, CYP2B6, CYP2C9, CYP2C19 and CYP3A4, nor an inhibitor of CYP1A2, CYP2C8, CYP2C9, CYP2C19, CYP3A4 and CYP2D6 at clinically relevant concentrations.
In Vivo Assessment of Drug Interactions
Effects of Alogliptin on the Pharmacokinetics of Other Drugs
In clinical studies, alogliptin did not meaningfully increase the systemic exposure to the following drugs that are metabolized by CYP isozymes or excreted unchanged in urine (Figure 1). No dose adjustment of alogliptin is recommended based on results of the described pharmacokinetic studies.
Figure 1. Effect of Alogliptin on the Pharmacokinetic Exposure to Other Drugs
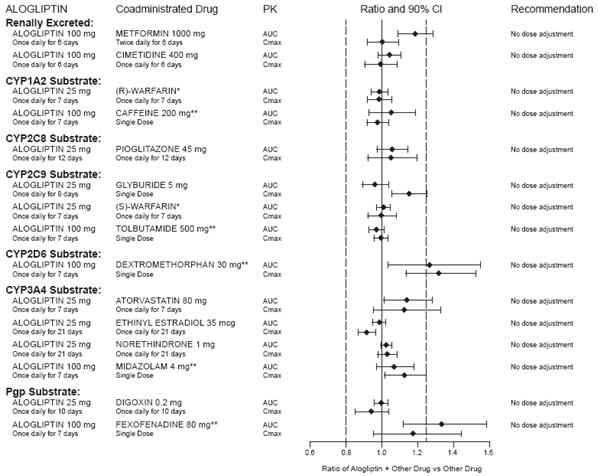
* Warfarin was given once daily at a stable dose in the range of 1 mg to 10 mg. Alogliptin had no significant effect on the prothrombin time (PT) or International Normalized Ratio (INR).
** Caffeine (1A2 substrate), tolbutamide (2C9 substrate), dextromethorphan (2D6 substrate), midazolam (3A4 substrate) and fexofenadine (P-gp substrate) were administered as a cocktail.
Effects of Other Drugs on the Pharmacokinetics of Alogliptin
There are no clinically meaningful changes in the pharmacokinetics of alogliptin when alogliptin is administered concomitantly with the drugs described below (Figure 2).
Figure 2. Effect of Other Drugs on the Pharmacokinetic Exposure of Alogliptin
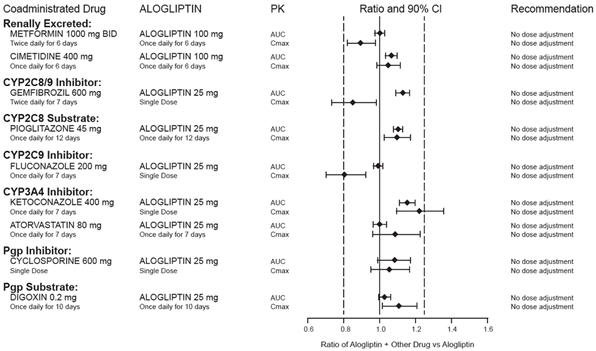
Pioglitazone
| Coadministered Drug | |||||
|---|---|---|---|---|---|
| Pioglitazone Dosage Regimen (mg)* | Name and Dose Regimens | Change in AUC† | Change in Cmax† | ||
| 45 mg (N=12) | Warfarin‡ | ||||
| Daily loading then maintenance doses based PT and INR values Quick's Value=35 ± 5% | R-Warfarin | ↓3% | R-Warfarin | ↓2% | |
| S-Warfarin | ↓1% | S-Warfarin | ↑1% | ||
| 45 mg (N=12) | Digoxin | ||||
| 0.200 mg twice daily (loading dose) then 0.250 mg daily (maintenance dose, 7 days) | ↑15% | ↑17% | |||
| 45 mg daily for 21 days (N=35) | Oral Contraceptive | ||||
| [Ethinyl Estradiol (EE) 0.035 mg plus Norethindrone (NE) 1 mg] for 21 days | EE | ↓11% | EE | ↓13% | |
| NE | ↑3% | NE | ↓7% | ||
| 45 mg (N=23) | Fexofenadine | ||||
| 60 mg twice daily for 7 days | ↑30% | ↑37% | |||
| 45 mg (N=14) | Glipizide | ||||
| 5 mg daily for 7 days | ↓3% | ↓8% | |||
| 45 mg daily for 8 days (N=16) | Metformin | ||||
| 1000 mg single dose on 8 days | ↓3% | ↓5% | |||
| 45 mg (N=21) | Midazolam | ||||
| 7.5 mg single dose on Day 15 | ↓26% | ↓26% | |||
| 45 mg (N=24) | Ranitidine | ||||
| 150 mg twice daily for 7 days | ↑1% | ↓1% | |||
| 45 mg daily for 4 days (N=24) | Nifedipine ER | ||||
| 30 mg daily for 4 days | ↓13% | ↓17% | |||
| 45 mg (N=25) | Atorvastatin Ca | ||||
| 80 mg daily for 7 days | ↓14% | ↓23% | |||
| 45 mg (N=22) | Theophylline | ||||
| 400 mg twice daily for 7 days | ↑2% | ↑5% | |||
| Coadministered Drug and Dosage Regimen | Pioglitazone | ||
|---|---|---|---|
| Dose Regimen (mg)* | Change in AUC† | Change in Cmax† | |
|
|||
| Gemfibrozil 600 mg twice daily for 2 days (N=12) | 30 mg single dose | ↑3.4-fold‡ | ↑6% |
| Ketoconazole 200 mg twice daily for 7 days (N=28) | 45 mg | ↑34% | ↑14% |
| Rifampin 600 mg daily for 5 days (N=10) | 30 mg single dose | ↓54% | ↓5% |
| Fexofenadine 60 mg twice daily for 7 days (N=23) | 45 mg | ↑1% | 0% |
| Ranitidine 150 mg twice daily for 4 days (N=23) | 45 mg | ↓13% | ↓16% |
| Nifedipine ER 30 mg daily for 7 days (N=23) | 45 mg | ↑5% | ↑4% |
| Atorvastatin Ca 80 mg daily for 7 days (N=24) | 45 mg | ↓24% | ↓31% |
| Theophylline 400 mg twice daily for 7 days (N=22) | 45 mg | ↓4% | ↓2% |
| Topiramate 96 mg twice daily for 7 days§
(N=26) | 30 mg§ | ↓15%¶ | 0% |
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Alogliptin and Pioglitazone
No carcinogenicity, mutagenicity or impairment of fertility studies have been conducted with alogliptin and pioglitazone tablets. The following data are based on findings in studies performed with alogliptin or pioglitazone individually.
Alogliptin
Rats were administered oral doses of 75, 400 and 800 mg/kg alogliptin for two years. No drug-related tumors were observed up to 75 mg/kg or approximately 32 times the maximum recommended clinical dose of 25 mg, based on area under the plasma concentration curve (AUC) exposure. At higher doses (approximately 308 times the maximum recommended clinical dose of 25 mg), a combination of thyroid C-cell adenomas and carcinomas increased in male but not female rats. No drug-related tumors were observed in mice after administration of 50, 150 or 300 mg/kg alogliptin for two years, or up to approximately 51 times the maximum recommended clinical dose of 25 mg, based on AUC exposure.
Alogliptin was not mutagenic or clastogenic, with and without metabolic activation, in the Ames test with S. typhimurium and E. coli or the cytogenetic assay in mouse lymphoma cells. Alogliptin was negative in the in vivo mouse micronucleus study.
In a fertility study in rats, alogliptin had no adverse effects on early embryonic development, mating or fertility at doses up to 500 mg/kg, or approximately 172 times the clinical dose based on plasma drug exposure (AUC).
Pioglitazone
A two year carcinogenicity study was conducted in male and female rats at oral doses up to 63 mg/kg (approximately 14 times the MRHD of 45 mg based on mg/m2). Drug-induced tumors were not observed in any organ except for the urinary bladder. Benign and/or malignant transitional cell neoplasms were observed in male rats at 4 mg/kg and above (approximately equal to the MRHD based on mg/m2). A two year carcinogenicity study was conducted in male and female mice at oral doses up to 100 mg/kg (approximately 11 times the MRHD based on mg/m2). No drug-induced tumors were observed in any organ.
Pioglitazone was not mutagenic in a battery of genetic toxicology studies, including the Ames bacterial assay, a mammalian cell forward gene mutation assay (CHO/HPRT and AS52/XPRT), an in vitro cytogenetics assay using CHL cells, an unscheduled DNA synthesis assay and an in vivo micronucleus assay.
No adverse effects upon fertility were observed in male and female rats at oral doses up to 40 mg/kg pioglitazone daily prior to and throughout mating and gestation (approximately nine times the MRHD based on mg/m2).
13.2 Animal Toxicology and/or Pharmacology
Pioglitazone
Heart enlargement has been observed in mice (100 mg/kg), rats (4 mg/kg and above) and dogs (3 mg/kg) treated orally with pioglitazone (approximately 11, one, and two times the MRHD for mice, rats and dogs, respectively, based on mg/m2). In a one year rat study, drug-related early death due to apparent heart dysfunction occurred at an oral dose of 160 mg/kg (approximately 35 times the MRHD based on mg/m2). Heart enlargement was seen in a 13 week study in monkeys at oral doses of 8.9 mg/kg and above (approximately four times the MRHD based on mg/m2), but not in a 52 week study at oral doses up to 32 mg/kg (approximately 13 times the MRHD based on mg/m2).
14 CLINICAL STUDIES
The coadministration of alogliptin and pioglitazone has been studied in patients with type 2 diabetes inadequately controlled on either diet and exercise alone or on metformin alone.
There have been no clinical efficacy studies conducted with alogliptin and pioglitazone tablets; however, bioequivalence of alogliptin and pioglitazone tablets with coadministered alogliptin and pioglitazone tablets was demonstrated, and efficacy of the combination of alogliptin and pioglitazone has been demonstrated in four Phase 3 efficacy studies.
In patients with type 2 diabetes, treatment with alogliptin and pioglitazone tablets produced clinically meaningful and statistically significant improvements in A1C compared to either alogliptin or pioglitazone alone. As is typical for trials of agents to treat type 2 diabetes, the mean reduction in A1C with alogliptin and pioglitazone tablets appears to be related to the degree of A1C elevation at baseline.
Alogliptin and Pioglitazone Coadministration in Patients with Type 2 Diabetes Inadequately Controlled on Diet and Exercise
In a 26 week, double-blind, active-controlled study, a total of 655 patients inadequately controlled on diet and exercise alone (mean baseline A1C=8.8%) were randomized to receive alogliptin 25 mg alone, pioglitazone 30 mg alone, alogliptin 12.5 mg with pioglitazone 30 mg or alogliptin 25 mg with pioglitazone 30 mg once daily. Coadministration of alogliptin 25 mg with pioglitazone 30 mg resulted in statistically significant improvements from baseline in A1C and FPG compared to either alogliptin 25 mg alone or to pioglitazone 30 mg alone (Table 10). Coadministration of alogliptin 25 mg with pioglitazone 30 mg once daily resulted in statistically significant reductions in fasting plasma glucose (FPG) starting from Week 2 through Week 26 compared to either alogliptin 25 mg or pioglitazone 30 mg alone. A total of 3% of patients receiving alogliptin 25 mg coadministered with pioglitazone 30 mg, 11% of those receiving alogliptin 25 mg alone, and 6% of those receiving pioglitazone 30 mg alone required glycemic rescue.
Improvements in A1C were not affected by gender, age or baseline BMI.
The mean increase in body weight was similar between pioglitazone alone and alogliptin when coadministered with pioglitazone.
| Alogliptin 25 mg | Pioglitazone 30 mg | Alogliptin 25 mg + Pioglitazone 30 mg | |
|---|---|---|---|
| A1C (%) | N=160 | N=153 | N=158 |
| Baseline (mean) | 8.8 | 8.8 | 8.8 |
| Change from Baseline (adjusted mean†) | -1 | -1.2 | -1.7 |
| Difference from alogliptin 25 mg (adjusted mean† with 95% confidence interval) | -0.8‡ (-1, -0.5) | ||
| Difference from pioglitazone 30 mg (adjusted mean† with 95% confidence interval) | -0.6‡ (-0.8, -0.3) | ||
| % of Patients (n/N) achieving A1C ≤ 7% | 24% (40/164) | 34% (55/163) | 63% (103/164)‡ |
| FPG (mg/dL) | N=162 | N=157 | N=162 |
| Baseline (mean) | 189 | 189 | 185 |
| Change from Baseline (adjusted mean†) | -26 | -37 | -50 |
| Difference from alogliptin 25 mg (adjusted mean† with 95% confidence interval) | -25‡ (-34, -15) | ||
| Difference from pioglitazone 30 mg (adjusted mean† with 95% confidence interval) | -13‡ (-22, -4) | ||
Alogliptin and Pioglitazone Coadministration in Patients with Type 2 Diabetes Inadequately Controlled on Metformin Alone
In the second 26 week, double-blind, placebo-controlled study, a total of 1554 patients already on metformin (mean baseline A1C=8.5%) were randomized to one of 12 double-blind treatment groups: placebo; 12.5 mg or 25 mg of alogliptin alone; 15 mg, 30 mg or 45 mg of pioglitazone alone; or 12.5 mg or 25 mg of alogliptin in combination with 15 mg, 30 mg or 45 mg of pioglitazone. Patients were maintained on a stable dose of metformin (median dose=1700 mg) during the treatment period. Coadministration of alogliptin and pioglitazone provided statistically significant improvements in A1C and FPG compared to placebo, to alogliptin alone, or to pioglitazone alone when added to background metformin therapy (Table 11, Figure 3). A total of 4%, 5% or 2% of patients receiving alogliptin 25 mg with 15 mg, 30 mg or 45 mg pioglitazone, 33% of patients receiving placebo, 13% of patients receiving alogliptin 25 mg, and 10%, 15% or 9% of patients receiving pioglitazone 15 mg, 30 mg or 45 mg alone required glycemic rescue.
Improvements in A1C were not affected by gender, age or baseline BMI.
The mean increase in body weight was similar between pioglitazone alone and alogliptin when coadministered with pioglitazone.
| Placebo | Alogliptin 25 mg | Pioglitazone 15 mg | Pioglitazone 30 mg | Pioglitazone 45 mg | Alogliptin 25 mg + Pioglitazone 15 mg | Alogliptin 25 mg + Pioglitazone 30 mg | Alogliptin 25 mg + Pioglitazone 45 mg | |
|---|---|---|---|---|---|---|---|---|
| A1C (%) | N=126 | N=123 | N=127 | N=123 | N=126 | N=127 | N=124 | N=126 |
| Baseline (mean) | 8.5 | 8.6 | 8.5 | 8.5 | 8.5 | 8.5 | 8.5 | 8.6 |
| Change from baseline (adjusted mean† with 95% confidence interval) | -0.1 | -0.9 | -0.8 | -0.9 | -1 | -1.3‡ | -1.4‡ | -1.6‡ |
| Difference from pioglitazone (adjusted mean† with 95% confidence interval) | - | - | - | - | - | -0.5‡ (-0.7, -0.3) | -0.5‡ (-0.7, -0.3) | -0.6‡ (-0.8, -0.4) |
| Difference from alogliptin (adjusted mean† with 95% confidence interval) | - | - | - | - | - | -0.4‡ (-0.6, -0.1) | -0.5‡ (-0.7, -0.3) | -0.7‡ (-0.9, -0.5) |
| Patients (%) achieving A1C ≤7% | 6% (8/129) | 27% (35/129) | 26% (33/129) | 30% (38/129) | 36% (47/129) | 55% (71/130)‡ | 53% (69/130)‡ | 60% (78/130)‡ |
| FPG (mg/dL) | N=129 | N=126 | N=127 | N=125 | N=129 | N=130 | N=126 | N=127 |
| Baseline (mean) | 177 | 184 | 177 | 175 | 181 | 179 | 179 | 178 |
| Change from baseline (adjusted mean† with 95% confidence interval) | 7 | -19 | -24 | -29 | -32 | -38‡ | -42‡ | -53‡ |
| Difference from pioglitazone (adjusted mean† with 95% confidence interval) | - | - | - | - | - | -14‡ (-24, -5) | -13‡ (-23, -3) | -20‡ (-30, -11) |
| Difference from alogliptin (adjusted mean† with 95% confidence interval) | - | - | - | - | - | -19‡ (-29, -10) | -23‡ (-33, -13) | -34‡ (-44, -24) |
Figure 3. Change from Baseline in A1C at Week 26 with Alogliptin and Pioglitazone Alone and Alogliptin in Combination with Pioglitazone when Added to Metformin
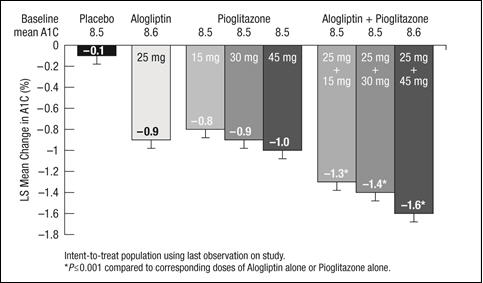
Alogliptin Add-On Therapy in Patients with Type 2 Diabetes Inadequately Controlled on Metformin in Combination with Pioglitazone
In a 52 week, active-comparator study, a total of 803 patients inadequately controlled (mean baseline A1C = 8.2%) on a current regimen of pioglitazone 30 mg and metformin at least 1500 mg per day or at the maximum tolerated dose were randomized to either receive the addition of alogliptin 25 mg or the titration of pioglitazone 30 mg to 45 mg following a four week, single-blind, placebo run-in period. Patients were maintained on a stable dose of metformin (median dose=1700 mg). Patients who failed to meet prespecified hyperglycemic goals during the 52 week treatment period received glycemic rescue therapy.
In combination with pioglitazone and metformin, alogliptin 25 mg was shown to be statistically superior in lowering A1C and FPG compared with the titration of pioglitazone from 30 mg to 45 mg at Week 26 and Week 52 (Table 12, results shown only for Week 52). A total of 11% of patients who were receiving alogliptin 25 mg in combination with pioglitazone 30 mg and metformin and 22% of patients receiving a dose titration of pioglitazone from 30 mg to 45 mg in combination with metformin required glycemic rescue.
Improvements in A1C were not affected by gender, age, race or baseline BMI. The mean increase in body weight was similar in both treatment arms. Lipid effects were neutral.
| Alogliptin 25 mg + Pioglitazone 30 mg + Metformin | Pioglitazone 45 mg + Metformin | |
|---|---|---|
|
||
| A1C (%) | N=397 | N=394 |
| Baseline (mean) | 8.2 | 8.1 |
| Change from Baseline (adjusted mean†) | -0.7 | -0.3 |
| Difference from Pioglitazone 45 mg + Metformin (adjusted mean† with 95% confidence interval) | -0.4‡ (-0.5, -0.3) | - |
| % of Patients (n/N) achieving A1C ≤7% | 33% (134/404)§ | 21% (85/399) |
| FPG (mg/dL) | N=399 | N=396 |
| Baseline (mean) | 162 | 162 |
| Change from Baseline (adjusted mean†) | -15 | -4 |
| Difference from Pioglitazone 45 mg + Metformin (adjusted mean† with 95% confidence interval) | -11§ (-16, -6) | ˗ |
Alogliptin Add-On Therapy to a Thiazolidinedione
A 26 week, placebo-controlled study, was conducted to evaluate the efficacy and safety of alogliptin as add-on therapy to pioglitazone in patients with type 2 diabetes. A total of 493 patients inadequately controlled on a thiazolidinedione alone or in combination with metformin or a sulfonylurea (mean baseline A1C=8%) were randomized to receive alogliptin 12.5 mg, alogliptin 25 mg or placebo. Patients were maintained on a stable dose of pioglitazone (median dose=30 mg) during the treatment period and those who were also previously treated on metformin (median dose=2000 mg) or sulfonylurea (median dose=10 mg) prior to randomization were maintained on the combination therapy during the treatment period. All patients entered into a four week, single-blind, placebo run-in period prior to randomization. Following randomization, all patients continued to receive instruction on diet and exercise. Patients who failed to meet prespecified hyperglycemic goals during the 26 week treatment period received glycemic rescue.
The addition of alogliptin 25 mg once daily to pioglitazone therapy resulted in significant improvements from baseline in A1C and FPG at Week 26 when compared to the addition of placebo (Table 13). A total of 9% of patients who were receiving alogliptin 25 mg and 12% of patients receiving placebo required glycemic rescue.
The improvement in A1C was not affected by gender, age, baseline BMI or baseline pioglitazone dose. The mean increase in body weight was similar between alogliptin and placebo when given in combination with pioglitazone. Lipid effects were neutral.
| Alogliptin 25 mg + Pioglitazone ± Metformin ± Sulfonylurea | Placebo + Pioglitazone ± Metformin ± Sulfonylurea | |
|---|---|---|
|
||
| A1C (%) | N=195 | N=95 |
| Baseline (mean) | 8 | 8 |
| Change from baseline (adjusted mean†) | -0.8 | -0.2 |
| Difference from placebo (adjusted mean† with 95% confidence interval) | -0.6‡ (-0.8, -0.4) | - |
| % of patients (n/N) achieving A1C ≤7% | 49% (98/199)‡ | 34% (33/97) |
| FPG (mg/dL) | N=197 | N=97 |
| Baseline (mean) | 170 | 172 |
| Change from baseline (adjusted mean†) | -20 | -6 |
| Difference from placebo (adjusted mean† with 95% confidence interval) | -14‡ (-23, -5) | - |
Cardiovascular Safety Trial
A randomized, double-blind, placebo-controlled cardiovascular outcomes trial (EXAMINE) was conducted to evaluate the cardiovascular risk of alogliptin. The trial compared the risk of major adverse cardiovascular events (MACE) between alogliptin (N=2701) and placebo (N=2679) when added to standard of care therapies for diabetes and atherosclerotic vascular disease (ASCVD). The trial was event driven and patients were followed until a sufficient number of primary outcome events accrued.
Eligible patients were adults with type 2 diabetes who had inadequate glycemic control at baseline (e.g., HbA1c >6.5%) and had been hospitalized for an acute coronary syndrome event (e.g., acute myocardial infarction or unstable angina requiring hospitalization) 15 to 90 days prior to randomization. The dose of alogliptin was based on estimated renal function at baseline per dosage and administration recommendations [see Dosage and Administration (2.2)]. The average time between an acute coronary syndrome event and randomization was approximately 48 days.
The mean age of the population was 61 years. Most patients were male (68%), Caucasian (73%), and were recruited from outside of the United States (86%). Asian and Black patients contributed 20% and 4% of the total population, respectively. At the time of randomization patients had a diagnosis of type 2 diabetes mellitus for approximately 9 years, 87% had a prior myocardial infarction and 14% were current smokers. Hypertension (83%) and renal impairment (27% with an eGFR ≤60 ml/min/1.73 m2) were prevalent co-morbid conditions. Use of medications to treat diabetes (e.g., metformin 73%, sulfonylurea 54%, insulin 41%), and ASCVD (e.g., statin 94%, aspirin 93%, renin-angiotensin system blocker 88%, beta-blocker 87%) was similar between patients randomized to alogliptin and placebo at baseline. During the trial, medications to treat diabetes and ASCVD could be adjusted to ensure care for these conditions adhered to standard of care recommendations set by local practice guidelines.
The primary endpoint in EXAMINE was the time to first occurrence of a MACE defined as the composite of cardiovascular death, nonfatal myocardial infarction (MI), or nonfatal stroke. The study was designed to exclude a pre-specified risk margin of 1.3 for the hazard ratio of MACE. The median exposure to study drug was 526 days and 95% of the patients were followed to study completion or death.
Table 14 shows the study results for the primary MACE composite endpoint and the contribution of each component to the primary MACE endpoint. The upper bound of the confidence interval was 1.16 and excluded a risk margin larger than 1.3.
| Composite of first event of CV death, nonfatal MI or nonfatal stroke (MACE) | Alogliptin | Placebo | Hazard Ratio | ||
|---|---|---|---|---|---|
| Number of Patients (%) | Rate per 100 PY* | Number of Patients (%) | Rate per 100 PY* | (98% CI) | |
| N=2701 | N=2679 | ||||
| 305 (11.3) | 7.6 | 316 (11.8) | 7.9 | 0.96 (0.80, 1.16) | |
|
|||||
| CV Death | 89 (3.3) | 2.2 | 111 (4.1) | 2.8 | |
| Nonfatal MI | 187 (6.9) | 4.6 | 173 (6.5) | 4.3 | |
| Nonfatal stroke | 29 (1.1) | 0.7 | 32 (1.2) | 0.8 | |
The Kaplan-Meier based cumulative event probability is presented in Figure 4 for the time to first occurrence of the primary MACE composite endpoint by treatment arm. The curves for placebo and alogliptin overlap throughout the duration of the study. The observed incidence of MACE was highest within the first 60 days after randomization in both treatment arms (14.8 MACE per 100 PY), decreased from day 60 to the end of the first year (8.4 per 100 PY) and was lowest after one year of follow-up (5.2 per 100 PY).
| Figure 4. Observed Cumulative Rate of MACE in EXAMINE |
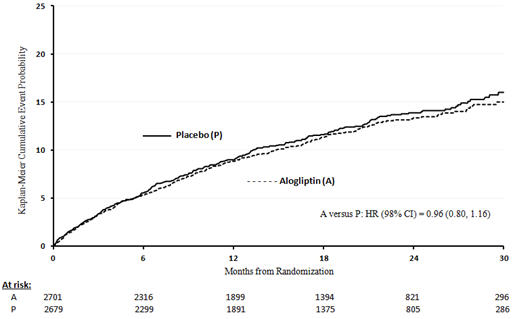 |
The rate of all cause death was similar between treatment arms with 153 (3.6 per 100 PY) recorded among patients randomized to alogliptin and 173 (4.1 per 100 PY) among patients randomized to placebo. A total of 112 deaths (2.9 per 100 PY) among patients on alogliptin and 130 among patients on placebo (3.5 per 100 PY) were adjudicated as cardiovascular deaths.
16 HOW SUPPLIED/STORAGE AND HANDLING
Alogliptin and pioglitazone tablets are available in the following strengths and packages:
25 mg/15 mg tablet: yellow, round, biconvex and film-coated with both "A/P" and "25/15" printed on one side, available in:
| NDC 45802-351-65 | Bottles of 30 tablets |
25 mg/30 mg tablet: peach, round, biconvex and film-coated with both "A/P" and "25/30" printed on one side, available in:
| NDC 45802-402-65 | Bottles of 30 tablets |
25 mg/45 mg tablet: red, round, biconvex, film-coated and with both "A/P" and "25/45" printed on one side, available in:
| NDC 45802-499-65 | Bottles of 30 tablets |
12.5 mg/15 mg tablet: pale yellow, round, biconvex and film-coated with both "A/P" and "12.5/15" printed on one side, available in:
| NDC 45802-238-65 | Bottles of 30 tablets |
12.5 mg/30 mg tablet: pale peach, round, biconvex and film-coated with both "A/P" and "12.5/30" printed on one side, available in:
| NDC 45802-260-65 | Bottles of 30 tablets |
12.5 mg/45 mg tablet: pale red, round, biconvex and film-coated with both "A/P" and "12.5/45" printed on one side, available in:
| NDC 45802-304-65 | Bottles of 30 tablets |
17 PATIENT COUNSELING INFORMATION
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Heart Failure
Inform patients of the signs and symptoms of heart failure. Before initiating alogliptin and pioglitazone tablets, patients should be asked about a history of heart failure or other risk factors for heart failure including moderate to severe renal impairment. Instruct patients who experience an unusually rapid increase in weight or edema or who develop shortness of breath or other symptoms of heart failure while on alogliptin and pioglitazone tablets should immediately report these symptoms to their physician.
Pancreatitis
Inform patients that acute pancreatitis has been reported during use of alogliptin. Educate patients that persistent, severe abdominal pain, sometimes radiating to the back, which may or may not be accompanied by vomiting, is the hallmark symptom of acute pancreatitis. Instruct patients to promptly discontinue alogliptin and pioglitazone tablets and contact their physician if persistent severe abdominal pain occurs.
Hypersensitivity Reactions
Inform patients that allergic reactions have been reported during use of alogliptin and pioglitazone. Instruct patients if symptoms of allergic reactions (including skin rash, hives and swelling of the face, lips, tongue and throat that may cause difficulty in breathing or swallowing) occur, patients should discontinue alogliptin and pioglitazone tablets and seek medical advice promptly.
Hepatic Effects
Inform patients that postmarketing reports of liver injury, sometimes fatal, have been reported during use of alogliptin and pioglitazone. Instruct patients if signs or symptoms of liver injury occur (e.g., unexplained nausea, vomiting, abdominal pain, fatigue, anorexia or dark urine), patients should discontinue alogliptin and pioglitazone tablets and seek medical advice promptly.
Urinary Bladder Tumours
Instruct patients to promptly report any sign of macroscopic hematuria or other symptoms such as dysuria or urinary urgency that develop or increase during treatment, as these may be due to bladder cancer.
Hypoglycemia with Concomitant Use with Insulin or Insulin Secretagogues
Inform patients that hypoglycemia can occur, particularly when an insulin secretagogue or insulin is used in combination with alogliptin and pioglitazone tablets. Explain the risks, symptoms and appropriate management of hypoglycemia.
Females of Reproductive Age
Inform female patients that treatment with pioglitazone, like other thiazolidinediones, may result in an unintended pregnancy in some premenopausal anovulatory females due to its effect on ovulation [see Use in Specific Populations (8.3)].
Severe and Disabling Arthralgia
Inform patients that severe and disabling joint pain may occur with this class of drugs. The time to onset of symptoms can range from one day to years. Instruct patients to seek medical advice if severe joint pain occurs.
Bullous Pemphigoid
Inform patients that bullous pemphigoid may occur with this class of drugs. Instruct patients to seek medical advice if blisters or erosions occur [see Warnings and Precautions (5.11)].
| MEDICATION GUIDE Alogliptin and Pioglitazone Tablets |
|||||
|---|---|---|---|---|---|
| ALS333 R6 | |||||
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | 03/2022 | ||||
| Read this Medication Guide carefully before you start taking alogliptin and pioglitazone tablets and each time you get a refill. There may be new information. This information does not take the place of talking with your doctor about your medical condition or your treatment. If you have any questions about alogliptin and pioglitazone tablets, ask your doctor or pharmacist. | |||||
|
What is the most important information I should know about alogliptin and pioglitazone tablets? |
|||||
| Alogliptin and pioglitazone tablets can cause serious side effects, including: | |||||
|
|||||
| Before you start taking alogliptin and pioglitazone tablets:
Tell your doctor if you have ever had: |
|||||
|
|
|
|||
| Stop taking alogliptin and pioglitazone tablets and call your doctor right away if you have pain in your stomach area (abdomen) that is severe and will not go away. The pain may be felt going from your abdomen through to your back. The pain may happen with or without vomiting. These may be symptoms of pancreatitis. | |||||
| What are alogliptin and pioglitazone tablets? | |||||
|
|||||
| It is not known if alogliptin and pioglitazone tablets are safe and effective in children under the age of 18. Alogliptin and pioglitazone tablets are not recommended for use in children. | |||||
| Who should not take alogliptin and pioglitazone tablets? | |||||
| Do not take alogliptin and pioglitazone tablets if you: | |||||
|
|||||
| Symptoms of a serious allergic reaction to alogliptin and pioglitazone tablets may include: | |||||
|
|
||||
| If you have these symptoms, stop taking alogliptin and pioglitazone tablets and contact your doctor or go to the nearest hospital emergency room right away. | |||||
| What should I tell my doctor before and during treatment with alogliptin and pioglitazone tablets? | |||||
| Before you start taking alogliptin and pioglitazone tablets, tell your doctor if you: | |||||
|
|||||
| Tell your doctor about all the medicines you take, including prescription and over-the-counter medicines, vitamins and herbal supplements. Know the medicines you take. Keep a list of them and show it to your doctor and pharmacist before you start a new medicine. Alogliptin and pioglitazone tablets may affect the way other medicines work, and other medicines may affect how alogliptin and pioglitazone tablets works. Contact your doctor before you start or stop other types of medicines. |
|||||
| How should I take alogliptin and pioglitazone tablets? | |||||
|
|||||
| What are the possible side effects of alogliptin and pioglitazone tablets? | |||||
| Alogliptin and pioglitazone tablets can cause serious side effects, including: | |||||
|
|||||
|
|
||||
| If you have these symptoms, stop taking alogliptin and pioglitazone tablets and contact your doctor right away or go to the nearest hospital emergency room | |||||
|
|||||
|
|
|
|||
|
|||||
|
|
|
|||
|
|||||
|
|
|
|
|
|
|
|||||
| The most common side effects of alogliptin and pioglitazone tablets include stuffy or runny nose and sore throat, back pain, cold-like symptoms (upper respiratory tract infection). Tell your doctor if you have any side effect that bothers you or that does not go away. These are not all the possible side effects of alogliptin and pioglitazone tablets. For more information, ask your doctor or pharmacist. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
|||||
| How should I store alogliptin and pioglitazone tablets? | |||||
|
|||||
| Keep alogliptin and pioglitazone tablets and all medicines out of the reach of children. | |||||
| General information about the safe and effective use of alogliptin and pioglitazone tablets
Medicines are sometimes prescribed for purposes other than those listed in the Medication Guide. Do not take alogliptin and pioglitazone tablets for a condition for which it was not prescribed. Do not give alogliptin and pioglitazone tablets to other people, even if they have the same symptoms you have. It may harm them. This Medication Guide summarizes the most important information about alogliptin and pioglitazone tablets. If you would like to know more information, talk with your doctor. You can ask your doctor or pharmacist for information about alogliptin and pioglitazone tablets that is written for health professionals. For more information, go to www.padagis.com or call 1-877-TAKEDA-7 (1-877-825-3327). |
|||||
| What are the ingredients in alogliptin and pioglitazone tablets?
Active ingredients: alogliptin and pioglitazone. Inactive ingredients: mannitol, microcrystalline cellulose, hydroxypropyl cellulose, croscarmellose sodium, magnesium stearate, and lactose monohydrate; the tablets are film-coated with hypromellose, polyethylene glycol, titanium dioxide, talc and ferric oxide (yellow and/or red) and are marked with red A1 or gray F1 printing ink. Distributed by: Padagis™ Allegan, MI 49010 • www.padagis.com All trademarks are the property of their respective owners |
|||||
PRINCIPAL DISPLAY PANEL - 12.5 mg/15 mg Tablet Bottle Label
Rx Only
NDC 45802-238-65
Alogliptin
and Pioglitazone
Tablets
12.5 mg/15 mg
Dispense with
Medication Guide
30 Tablets
Perrigo®
PRINCIPAL DISPLAY PANEL - 12.5 mg/30 mg Tablet Bottle Label
NDC 45802-260-65
Rx Only
Alogliptin
and Pioglitazone
Tablets
12.5 mg/30 mg
DISPENSE WITH
MEDICATION GUIDE
30 Tablets
Padagis™
PRINCIPAL DISPLAY PANEL - 12.5 mg/45 mg Tablet Bottle Label
Rx Only
NDC 45802-304-65
Alogliptin
and Pioglitazone
Tablets
12.5 mg/45 mg
Dispense with
Medication Guide
30 Tablets
Perrigo®
PRINCIPAL DISPLAY PANEL - 25 mg/15 mg Tablet Bottle Label
NDC 45802-351-65
Rx Only
Alogliptin
and Pioglitazone
Tablets
25 mg/15 mg
DISPENSE WITH
MEDICATION GUIDE
30 Tablets
Padagis™