BRAVELLE- urofollitropin
Ferring Pharmaceuticals Inc.
Reference Label Set Id: 46f7740f-c879-4a77-9a16-2821fd772641
----------
HIGHLIGHTS OF PRESCRIBING INFORMATIONThese highlights do not include all the information needed to use BRAVELLE
® safely and effectively. See full prescribing information for BRAVELLE
®
BRAVELLE ® (urofollitropin for injection, purified) for subcutaneous or intramuscular injection Initial U.S. Approval: 2002 INDICATIONS AND USAGEBRAVELLE ® (urofollitropin for injection, purified) is a gonadotropin indicated for:
DOSAGE AND ADMINISTRATIONOvulation Induction ( 2.2)
Assisted Reproductive Technology (ART) ( 2.3)
DOSAGE FORMS AND STRENGTHSLyophilized powder for injection: containing 82.5 International Units of FSH, to deliver 75 International Units FSH after reconstituting, supplied as lyophilized powder in sterile vials with diluent vials. ( 3) CONTRAINDICATIONSBRAVELLE ® is contraindicated in women who exhibit:
WARNINGS AND PRECAUTIONSADVERSE REACTIONS
To report SUSPECTED ADVERSE REACTIONS, contact Ferring Pharmaceuticals Inc. at 1-888-FERRING (1-888-337-7464) or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch. DRUG INTERACTIONSNo drug/drug interaction studies have been conducted for BRAVELLE ® in humans ( 7) USE IN SPECIFIC POPULATIONS
See 17 for PATIENT COUNSELING INFORMATION and FDA-approved patient labeling. Revised: 7/2015 |
FULL PRESCRIBING INFORMATION
1 INDICATIONS AND USAGE
1.1 Induction of Ovulation in Women who have Previously Received Pituitary Suppression
Prior to initiation of treatment with BRAVELLE ®:
- Perform a complete gynecologic and endocrinologic evaluation
- Exclude a diagnosis of primary ovarian failure
- Exclude the possibility of pregnancy
- Demonstrate tubal patency
- Evaluate the fertility status of the male partner
1.2 Development of Multiple Follicles as Part of an Assisted Reproductive Technology (ART) Cycle in Ovulatory Women Who Have Previously Received Pituitary Suppression
Prior to initiation of treatment with BRAVELLE ®:
- Perform a complete gynecologic and endocrinologic evaluation, and diagnose the cause of infertility
- Exclude the possibility of pregnancy
- Evaluate the fertility status of the male partner
- Exclude women with primary ovarian failure
2 DOSAGE AND ADMINISTRATION
2.1 General Dosing Information
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
- Administer BRAVELLE ® subcutaneously in the abdomen or intramuscularly as described in Instructions for Use.
- A healthcare provider should administer BRAVELLE ® intramuscularly.
2.2 Recommended Dosing for Induction of Ovulation
The dosing scheme is stepwise and is individualized for each woman [see Clinical Studies (14.1)].
- For women who have received GnRH agonist or antagonist pituitary suppression, a starting dose of 150 International Units per day of BRAVELLE ® is administered subcutaneously or intramuscularly for 5 days in the first cycle of treatment.
- In subsequent cycles of treatment, the starting dose (and dosage adjustments) of BRAVELLE ® should be determined based on the history of the ovarian response to BRAVELLE ®.
- The following should be considered when planning the woman's individualized dose of BRAVELLE
®:
- Appropriate BRAVELLE ® dose adjustment(s), based on clinical monitoring (including serum estradiol levels and vaginal ultrasound results), should be used to prevent multiple follicular growth and cycle cancellation.
- Do not make adjustments in dose more frequently than once every 2 days and do not exceed more than 75 to 150 International Units per adjustment.
- Use the lowest dose of BRAVELLE ® that will achieve desired results.
- The maximum, individualized, daily dose of BRAVELLE ® is 450 International Units per day.
- In general, do not exceed 12 days of treatment.
- When pre-ovulatory conditions are reached, administer human chorionic gonadotropin (hCG) to induce final oocyte maturation and ovulation.
- Withhold hCG in cases where the ovarian monitoring on the last day of BRAVELLE ® treatment suggests an increased risk of ovarian hyperstimulation syndrome (OHSS) [see Warnings and Precautions (5.2, 5.3, 5.11)].
- Encourage the woman and her partner to have intercourse daily, beginning on the day prior to the administration of hCG and until ovulation becomes apparent.
Discourage intercourse when the risk for OHSS is increased [see Warnings and Precautions (5.2, 5.3)] .
2.3 Recommended Dosing for Assisted Reproduction Technology (ART)
The recommended dosing scheme for patients undergoing IVF follows a stepwise approach and is individualized for each woman. The recommended initial dose of BRAVELLE ® for women who have received a GnRH agonist for pituitary suppression is 225 International Units. BRAVELLE ® may be administered together with MENOPUR ® (menotropins for injection, USP), and the total initial dose when the products are combined should not exceed 225 International Units (150 International Units of BRAVELLE ® and 75 International Units of MENOPUR ® or 75 International Units of BRAVELLE ® and 150 International Units of MENOPUR ®).
- Beginning on cycle day 2 or 3, a starting dose of 225 International Units of BRAVELLE ® is administered subcutaneously daily until sufficient follicular development, as determined by ultrasound in combination with measurement of serum estradiol levels, is attained. In most cases, therapy should not exceed 12 days.
- Adjust the dose after 5 days based on the woman's ovarian response, as determined by ultrasound evaluation of follicular growth and serum estradiol levels.
- Do not make additional dosage adjustments more frequently than every 2 days or by more than 75 - 150 International Units at each adjustment.
- Continue treatment until adequate follicular development is evident, and then administer hCG.
- Withhold the administration of hCG in cases where the ovarian monitoring suggests an increased risk of OHSS on the last day of BRAVELLE ® therapy [see Warnings and Precautions (5.2, 5.3, 5.11)] .
- Do not administer daily doses of BRAVELLE ® or BRAVELLE ® in combination with MENOPUR ® that exceed 450 International Units .
3 DOSAGE FORMS AND STRENGTHS
Lyophilized powder for Injection containing 82.5 International Units of FSH, to deliver 75 International Units of FSH after reconstituting with the diluent, supplied in sterile vials with diluent vials and Q•Cap ® vial adapters.
4 CONTRAINDICATIONS
BRAVELLE ® is contraindicated in women who exhibit:
- Prior hypersensitivity to BRAVELLE ® or urofollitropins
- High levels of FSH indicating primary ovarian failure [see Indications and Usage (1.1, 1.2)]
- Pregnancy
BRAVELLE ® may cause fetal harm when administered to a pregnant woman [see Use in Specific Populations (8.1)] . BRAVELLE ® is contraindicated in women who are pregnant. If this drug is used during pregnancy, or if the woman becomes pregnant while taking this drug, the woman should be apprised of the potential hazard to a fetus. - Presence of uncontrolled non-gonadal endocrinopathies (e.g., thyroid, adrenal, or pituitary disorders) [see Indications and Usage (1.1, 1.2)]
- Sex hormone dependent tumors of the reproductive tract and accessory organ
- Tumors of pituitary gland or hypothalamus
- Abnormal uterine bleeding of undetermined origin
- Ovarian cysts or enlargement of undetermined origin, not due to polycystic ovary syndrome
5 WARNINGS AND PRECAUTIONS
BRAVELLE ® should only be used by physicians who are experienced in infertility treatment. BRAVELLE ® contains gonadotropic substances capable of causing in women, Ovarian Hyperstimulation Syndrome [OHSS] with or without pulmonary or vascular complications [see Warnings and Precautions (5.3, 5.4)] and multiple births [see Warnings and Precautions (5.6)] . Gonadotropin therapy requires the availability of appropriate monitoring facilities [see Warnings and Precautions (5.11)] . Use the lowest effective dose.
5.1 Hypersensitivity and Anaphylactic Reactions
Hypersensitivity/anaphylactic reactions associated with urofollitropins for injection, purified administration have been reported in some patients. These reactions presented as generalized urticaria, facial edema, angioneurotic edema, and/or dyspnea suggestive of laryngeal edema. The relationship of these symptoms to uncharacterized urinary proteins is uncertain.
5.2 Abnormal Ovarian Enlargement
In order to minimize the hazard associated with abnormal ovarian enlargement that may occur with BRAVELLE ® therapy, the lowest effective dose should be used [see Dosage and Administration (2.2, 2.3)]. Use of ultrasound monitoring of ovarian response and/or measurement of serum estradiol levels is important to minimize the risk of ovarian stimulation [see Warnings and Precautions (5.11)] .
If the ovaries are abnormally enlarged on the last day of BRAVELLE ® therapy, hCG should not be administered in order to reduce the chances of development of the Ovarian Hyperstimulation Syndrome [see Warnings and Precautions (5.3)] . Prohibit intercourse in women with significant ovarian enlargement because of the danger of hemoperitoneum resulting from rupture of ovarian cysts [see Warnings and Precautions (5.3)] .
5.3 Ovarian Hyperstimulation Syndrome (OHSS)
OHSS: OHSS is a medical event distinct from uncomplicated ovarian enlargement. OHSS may progress rapidly to become a serious medical event. It is characterized by an apparent dramatic increase in vascular permeability, which can result in a rapid accumulation of fluid in the peritoneal cavity, thorax, and potentially, the pericardium. The early warning signs of development of OHSS are severe pelvic pain, nausea, vomiting, and weight gain. Abdominal pain, abdominal distension, gastrointestinal symptoms including nausea, vomiting and diarrhea, severe ovarian enlargement, weight gain, dyspnea, and oliguria have been reported with OHSS. Clinical evaluation may reveal hypovolemia, hemoconcentration, electrolyte imbalances, ascites, hemoperitoneum, pleural effusions, hydrothorax, acute pulmonary distress, and thromboembolic events [see Warnings and Precautions (5.4)]. Transient liver function test abnormalities suggestive of hepatic dysfunction, which may be accompanied by morphologic changes on liver biopsy, have been reported in association with OHSS.
OHSS occurs after treatment has been discontinued and reaches its maximum at about 7 to 10 days after treatment. Usually, OHSS resolves spontaneously with the onset of menses. If there is evidence that OHSS may be developing prior to hCG administration [see Warnings and Precautions (5.2)] , the hCG must be withheld.
Cases of OHSS are more common, more severe and more protracted if pregnancy occurs. OHSS develops rapidly; therefore patients should be followed for at least two weeks after hCG administration.
If severe OHSS occurs, gonadotropins, including hCG, must be stopped and consideration should be given as to whether the woman needs be hospitalized. Treatment is primarily symptomatic and overall should consist of bed rest, fluid and electrolyte management, and analgesics (if needed). Because the use of diuretics can accentuate the diminished intravascular volume, diuretics should be avoided except in the late phase of resolution as described below. The management of OHSS may be divided into three phases as follows:
- Acute Phase:
Management should be directed at preventing hemoconcentration due to loss of intravascular volume to the third space and minimizing the risk of thromboembolic phenomena and kidney damage. Fluid intake and output, weight, hematocrit, serum and urinary electrolytes, urine specific gravity, BUN and creatinine, total proteins with albumin: globulin ratio, coagulation studies, electrocardiogram to monitor for hyperkalemia, and abdominal girth should be thoroughly assessed daily or more often based on the clinical need. Treatment, consisting of limited intravenous fluids, electrolytes, human serum albumin, is intended to normalize electrolytes while maintaining an acceptable but somewhat reduced intravascular volume. Full correction of the intravascular volume deficit may lead to an unacceptable increase in the amount of third space fluid accumulation. - Chronic Phase:
After the acute phase is successfully managed as above, excessive fluid accumulation in the third space should be limited by instituting severe potassium, sodium, and fluid restriction. - Resolution Phase:
As third space fluid returns to the intravascular compartment, a fall in hematocrit and increasing urinary output are observed in the absence of any increase in intake. Peripheral and/or pulmonary edema may result if the kidneys are unable to excrete third space fluid as rapidly as it is mobilized. Diuretics may be indicated during the resolution phase, if necessary, to combat pulmonary edema.
Do not remove ascitic, pleural, and pericardial fluid unless there is the necessity to relieve symptoms such as pulmonary distress or cardiac tamponade.
OHSS increases the risk of injury to the ovary. Pelvic examination or intercourse may cause rupture of an ovarian cyst, which may result in hemoperitoneum, and should be avoided.
If bleeding occurs and requires surgical intervention, the clinical objective should be to control the bleeding and retain as much ovarian tissue as possible. A physician experienced in the management of this syndrome, or who is experienced in the management of fluid and electrolyte imbalances, should be consulted.
In a clinical study of induction of ovulation indication, 6 of 72 (8.33%) BRAVELLE ® treated women developed OHSS and 2 were classified as severe. In a clinical study for the development of multiple follicles as part of an IVF cycle, 3 of 60 women treated with BRAVELLE ® developed OHSS and 1 was classified as severe.
5.4 Pulmonary and Vascular Complications
Serious pulmonary conditions (e.g., atelectasis, acute respiratory distress syndrome) have been reported in women treated with gonadotropins. In addition, thromboembolic events both in association with, and separate from, the Ovarian Hyperstimulation Syndrome have been reported in women treated with gonadotropins. Intravascular thrombosis and embolism, which may originate in venous or arterial vessels, can result in reduced blood flow to critical organs or the extremities. Women with generally recognized risk factors for thrombosis, such as personal or family history, severe obesity, or thrombophilia, may have an increased risk of venous or arterial thromboembolic events during or following treatment with gonadotropins. Sequelae of such reactions have included venous thrombophlebitis, pulmonary embolism, pulmonary infarction, cerebral vascular occlusion (stroke), and arterial occlusion resulting in loss of limb and rarely in myocardial infarctions. In rare cases, pulmonary complications and/or thromboembolic events have resulted in death. In women with recognized risk factors, the benefits of ovulation induction and assisted reproductive technology need to be weighed against the risks. Pregnancy also carries an increased risk of thrombosis.
5.5 Ovarian Torsion
Ovarian torsion has been reported after treatment with gonadotropins. This may be related to OHSS, pregnancy, previous abdominal surgery, past history of ovarian torsion, previous or current ovarian cyst and polycystic ovaries. Damage to the ovary due to reduced blood supply can be limited by early diagnosis and immediate detorsion.
5.6 Multi-fetal Gestation and Birth
Multi-fetal gestation and births have been reported with all gonadotropin therapy including therapy with BRAVELLE ®.
In a controlled study of 72 patients undergoing induction of ovulation, 66.7% of pregnancies of women treated with subcutaneous BRAVELLE ® were multiples, while 28.6% of pregnancies in women treated with intramuscular BRAVELLE ® were multiples.
In a controlled study of 60 patients undergoing IVF, 34.8% of pregnancies of women treated with subcutaneous BRAVELLE ® were multiples.
Before beginning treatment with BRAVELLE ®, advise the woman and her partner of the potential risk of multi-fetal gestation and birth.
5.7 Congenital Malformations
The incidence of congenital malformations after some ART [specifically in vitro fertilization (IVF) or intracytoplasmic sperm injection (ICSI)] may be slightly higher than after spontaneous conception. This slightly higher incidence is thought to be related to differences in parental characteristics (e.g., maternal age, maternal and paternal genetic background, sperm characteristics) and to the higher incidence of multi-fetal gestations after IVF or ICSI. There are no indications that the use of gonadotropins during IVF or ICSI is associated with an increased risk of congenital malformations.
5.8 Ectopic Pregnancy
Since infertile women undergoing ART often have tubal abnormalities, the incidence of ectopic pregnancy may be increased. Early confirmation of intrauterine pregnancy should be determined by β-hCG testing and transvaginal ultrasound.
5.9 Spontaneous Abortion
The risk of spontaneous abortion (miscarriage) is increased with gonadotropin products. However, causality has not been established. The increased risk may be a factor of the underlying infertility .
5.10 Ovarian Neoplasms
There have been infrequent reports of ovarian neoplasms, both benign and malignant, in women who have had multiple drug therapy for controlled ovarian stimulation; however, a causal relationship has not been established.
5.11 Laboratory Tests
In most instances, treatment of women with BRAVELLE ® will result only in follicular growth and maturation. In the absence of an endogenous LH surge, hCG is given when monitoring of the woman indicates that sufficient follicular development has occurred. This may be estimated by ultrasound alone or in combination with measurement of serum estradiol levels. The combination of both ultrasound and serum estradiol measurement are useful for monitoring follicular growth and maturation, timing of the ovulatory trigger, detecting ovarian enlargement and minimizing the risk of the Ovarian Hyperstimulation Syndrome and multiple gestation.
The clinical confirmation of ovulation is obtained by direct or indirect indices of progesterone production as well as sonographic evidence of ovulation.
Direct or indirect indices of progesterone production:
- Urinary or serum luteinizing hormone (LH) rise
- A rise in basal body temperature
- Increase in serum progesterone
- Menstruation following the shift in basal body temperature
Sonographic evidence of ovulation:
- Collapsed follicle
- Fluid in the cul-de-sac
- Features consistent with corpus luteum formation
- Secretory endometrium
6 ADVERSE REACTIONS
The following serious adverse reactions are discussed elsewhere in the labeling:
- Hypersensitivity and Anaphylactic Reactions [see Warnings and Precautions (5.1)]
- Abnormal Ovarian Enlargement [see Warnings and Precautions (5.2)]
- Ovarian Hyperstimulation Syndrome [see Warnings and Precautions (5.3)]
- Thromboembolic events [see Warnings and Precautions (5.4)]
- Ovarian Torsion [see Warnings and Precautions (5.5)]
- Multi-fetal Gestation and Birth [see Warnings and Precautions (5.6)]
- Congenital Malformations [see Warnings and Precautions (5.7)]
- Ectopic Pregnancy [see Warnings and Precautions (5.8)]
- Spontaneous Abortion [see Warnings and Precautions (5.9)]
- Ovarian Neoplasms [see Warnings and Precautions (5.10)]
6.1 Clinical Trial Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trial of another drug and may not reflect the rates observed in practice.
The safety of BRAVELLE ® was examined in four clinical studies that enrolled a total of 222 women who received BRAVELLE ®.
Ovulation Induction
In a randomized, multi-center, active controlled study, a total of 72 women received BRAVELLE ® (35 in a subcutaneous administration arm and 37 in an intramuscular administration arm) for induction of ovulation. Adverse reactions occurring at an incidence of ≥2% incidence in women receiving BRAVELLE ® are shown in Table 1.
| All Patients with Adverse Events ≥ 2% | ||
|---|---|---|
| Adverse Events (%) | BRAVELLE ® subcutaneous | BRAVELLE ® intramuscular |
| N=35 | N=37 | |
| Genitourinary/Reproductive | ||
| OHSS | 4 (11.4) | 2 (5.4) |
| Vaginal Hemorrhage | 3 (8.6) | 0 (0.0) |
| Ovarian Disorder (Pain, Cyst) | 1 (2.9) | 3 (8.1) |
| Urinary tract infection | 0 | 1 (2.7) |
| Cervix disorder | 1 (2.9) | 0 |
| Gastrointestinal | ||
| Nausea | 2 (5.7) | 0 (0.0) |
| Enlarged Abdomen | 1 (2.9) | 1 (2.7) |
| Abdominal Pain | 1 (2.9) | 2 (5.4) |
| Vomiting | 0 | 1 (2.7) |
| Constipation | 0 | 1 (2.7) |
| Diarrhea | 0 | 1 (2.7) |
| Metabolic/Nutritional | ||
| Dehydration | 0 | 1 (2.7) |
| Weight gain | 1 (2.9) | 0 |
| Skin/Appendages | ||
| Acne | 1 (2.9) | 0 |
| Exfoliative dermatitis | 0 | 1 (2.7) |
| Other Body Systems | ||
| Headache | 4 (11.4) | 3 (8.1) |
| Pain | 2 (5.7) | 0 (0.0) |
| Neck pain | 0 | 1 (2.7) |
| Respiratory Disorder | 2 (5.7) | 0 (0.0) |
| Hot Flashes | 2 (5.7) | 0 (0.0) |
| Fever | 0 | 1 (2.7) |
| Hypertension | 0 | 1 (2.7) |
| Emotional lability | 0 | 1 (2.7) |
| Depression | 0 | 1 (2.7) |
| Accidental injury | 0 | 1 (2.7) |
Assisted Reproductive Technology
Three studies examined the safety profile of BRAVELLE ® in ART. A total of 150 women received treatment with BRAVELLE ® in these studies. Adverse reactions occurring at an incidence of ≥2% incidence for this integrative assessment are presented in Table 2.
| All Patients with Adverse Events ≥ 2% | |
|---|---|
| Adverse Events (%) | BRAVELLE ® subcutaneous |
| N=150 | |
| Genitourinary/Reproductive | |
| Vaginal hemorrhage | 7 (4.7) |
| Post retrieval pain | 12 (8.0) |
| Pelvic pain/cramps | 10 (6.7) |
| OHSS | 9 (6.0) |
| Uterine spasms | 4 (2.7) |
| Vaginal spotting | 4 (2.7) |
| Urinary tract infection | 5 (3.3) |
| Ovarian disorder | 3 (2.0) |
| Breast tenderness | 3 (2.0) |
| Vaginal Discharge | 4 (2.7) |
| Infection fungal | 3 (2.0) |
| Gastrointestinal | |
| Abdominal cramps | 21 (14.0) |
| Nausea | 13 (8.7) |
| Abdominal pain | 7 (4.7) |
| Abdominal fullness/enlargement | 10 (6.7) |
| Constipation | 3 (2.0) |
| Other Body Systems | |
| Headache | 19 (12.7) |
| Pain | 8 (5.3) |
| Rash | 4 (2.7) |
| Respiratory disorder | 6 (4.0) |
| Sinusitis | 3 (2.0) |
| Injection site reaction | 6 (4.0) |
| Hot flash | 6 (4.0) |
| Emotional lability | 3 (2.0) |
6.2 Postmarketing Experience
The following adverse reactions have been reported during postmarketing use of gonadotropins. Because these reactions were reported voluntarily from a population of uncertain size, the frequency or a causal relationship to BRAVELLE ® cannot be reliably determined.
- Gastrointestinal disorders: Abdominal pain, Nausea, Vomiting, Abdominal distension, Abdominal discomfort, Diarrhea, Constipation
- General disorders and administration site conditions: Pain, Injection site reactions (redness, bruising, swelling and/or pruritus)
- Infections and infestations: Urinary tract infection, Nasopharyngitis
- Musculoskeletal and connective tissue disorders: Muscle spasm
- Nervous system disorders: Headache
- Reproductive system disorders: Vaginal hemorrhage, OHSS [see Warnings and Precautions (5.3)] , Pelvic pain, Breast tenderness, Vaginal discharge. Ovarian enlargement, Multiple pregnancies [see Warnings and Precautions (5.6)]
- Skin and subcutaneous tissue disorders: Rash
- Vascular disorders: Hot flushes
8 USE IN SPECIFIC POPULATIONS
8.3 Nursing Mothers
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in the nursing infant from BRAVELLE ®, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
10 OVERDOSAGE
Aside from possible ovarian hyperstimulation [see Warnings and Precautions (5.3)] and multiple gestations [see Warnings and Precautions (5.6)] , little is known concerning the consequences of acute overdosage with BRAVELLE ®.
11 DESCRIPTION
BRAVELLE ® is a product containing a highly purified preparation of human follicle stimulating hormone (hFSH) extracted from the urine of postmenopausal women. Human FSH is a gonadotropin and consists of two non-covalently linked glycoproteins designated as the α and β subunits. The α subunit has 92 amino acids of which two are modified by attachment of carbohydrates. The β subunit has 111 amino acids of which two are modified by attachment of carbohydrates.
BRAVELLE ® is a sterile, lyophilized powder intended for subcutaneous or intramuscular injection after reconstitution with sterile 0.9% Sodium Chloride Injection, USP. Each vial of BRAVELLE ® contains 82.5 International Units (IU) of Follicle Stimulating Hormone (FSH) activity, 23 mg Lactose Monohydrate, 0.005 mg Polysorbate 20, and Sodium Phosphate buffer (Sodium Phosphate dibasic, Heptahydrate and Phosphoric acid) for pH adjustments, which, when reconstituted with diluent, will deliver 75 International Units of FSH. BRAVELLE ® contains up to 2% luteinizing hormone (LH) activity based on bioassay. Human Chorionic Gonadotropin (hCG) is not detected in BRAVELLE ®. When stored at 3° to 25°C, up to 40% of the α-subunits may be oxidized.
The in vivo biological activity of urofollitropin for injection, purified is determined by using reference standards calibrated against the First International Standard for follicle-stimulating hormone, (FSH, Urofollitropin), Urinary, Human for Bioassay, National Institute for Biological Standards and Control (NIBSC) at its 46th meeting in 1995.
FSH is a glycoprotein that is acidic and water-soluble.
BRAVELLE ® has been mixed in vitro with MENOPUR ® with no evidence of aggregation.
Therapeutic class: Infertility
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
BRAVELLE ® administered for 7 to 12 days produces ovarian follicular growth in women who do not have primary ovarian failure. Treatment with BRAVELLE ® in most instances results only in follicular growth and maturation. When sufficient follicular maturation has occurred, hCG must be given to induce ovulation.
12.3 Pharmacokinetics
Single doses of 225 International Units and multiple daily doses (7 days) of 150 International Units of BRAVELLE ® were administered to healthy volunteer female subjects while their endogenous FSH was suppressed. Sixteen subjects received BRAVELLE ® subcutaneously and 12 received the drug intramuscularly. Serum FSH concentrations were determined. Based on the steady state ratio of FSH C max and AUC, subcutaneous and intramuscular administration of BRAVELLE ® were not bioequivalent. Multiple doses of BRAVELLE ® intramuscular resulted in C max and AUC of 77.7% and 81.8% compared to multiple doses of BRAVELLE ® subcutaneous. The FSH pharmacokinetic parameters for single and multiple dose BRAVELLE ®, administered subcutaneously and intramuscularly are in Table 3.
| Single Dose (225 IU) | Multiple Dose × 7 (150 IU) | |||
|---|---|---|---|---|
| PK Parameters | Subcutaneous | Intramuscular | Subcutaneous | Intramuscular |
| C max (mIU/mL) | 6.0 (1.7) | 8.8 (4.5) | 14.8 (2.9) | 11.5 (2.9) |
| T max (hrs) | 20.5 (7.7) | 17.4 (12.2) | 9.6 (2.1) | 11.3 (8.4) |
| AUC obs (mIU∙hr/mL) | 379 (111) | 331 (179) | 234.7 (77.0) | 192.1 (52.3) |
| t 1/2 (hrs) | 31.8 | 37 | 20.6 | 15.2 |
14 CLINICAL STUDIES
The efficacy of BRAVELLE ® was examined in two clinical studies, one for in-vitro fertilization (IVF) and one for ovulation induction (OI).
14.1 Ovulation Induction
In the randomized, multi-center, active-controlled, ovulation induction study, women underwent pituitary suppression with a GnRH agonist before being randomized to subcutaneously administered BRAVELLE ® , intramuscularly-administered BRAVELLE ®, or a subcutaneously administered commercial recombinant FSH product. A total of 111 oligo-anovulatory women were randomized to both treatment arms, of which 72 received BRAVELLE ®, starting at a dose of 150 International Units daily for 5 days. Subsequently each woman received individual titration of the BRAVELLE ® dose from 75 to 450 International Units daily based on ultrasound and estradiol (E 2) levels. The total duration of dosing did not exceed 12 days. Results for the Intent-To-Treat Population are summarized in Table 4.
| BRAVELLE ® Subcutaneous | BRAVELLE ® Intramuscular | |
|---|---|---|
| Parameter | N=35 | N=37 |
| Ovulation (%) | 24 (68.6) | 26 (70.3) |
| Received hCG (%) | 25 (71.4) | 28 (75.7) |
| Mean Peak Serum E2 (pg/mL) (SD) | 976.5 (680.6) | 893.2 (815.2) |
| Chemical Pregnancy (%) | 11 (31.4) | 8 (21.6) |
| Clinical Pregnancy (%) | 9 (25.7) | 7 (18.9) |
| Continuing Pregnancy (%) | 9 (25.7) | 7 (18.9) |
| Pts. w/Live Births (%) | 9 (25.7) | 6 (16.2) |
14.2 Assisted Reproductive Technologies [ART]
In the randomized, multi-center, active-controlled, IVF study, women underwent pituitary suppression with a GnRH agonist before being randomized to subcutaneously administered BRAVELLE ® or a subcutaneously administered commercial recombinant FSH product. A total of 120 patients were randomized to both treatment arms, of which 60 received BRAVELLE ®, starting at a dose of 225 International Units daily for 5 days. Subsequently each woman received individual titration of the dose from 75 to 450 International Units daily based on ultrasound and estradiol (E 2) levels. The total duration of dosing did not exceed 12 days. Results are summarized in Table 5 for the Intent-To-Treat population.
| BRAVELLE ® subcutaneous | |
|---|---|
| Parameter | n=60 |
| Mean Total Oocytes Retrieved Per Patient (SD) | 11.8 (6.3) |
| Mean Mature Oocytes Retrieved Per Patient (SD) | 9.0 (5.7) |
| Patients with Oocyte Retrieval (%) | 57 (95.0) |
| Patients with Embryo Transfer (%) | 57 (95.0) |
| Patients with Chemical Pregnancy (%) | 28 (46.6) |
| Patients with Clinical Pregnancy (%) | 25 (41.7) |
| Patients with Continuing Pregnancy (%) | 23 (38.3) |
16 HOW SUPPLIED/STORAGE AND HANDLING
16.1 How Supplied
BRAVELLE ® (urofollitropin for injection, purified) is supplied in a sterile, lyophilized, single dose vial containing 82.5 International Units of FSH, to deliver 75 International Units FSH after reconstituting with the diluent.
Each vial is available with an accompanying vial of sterile diluent containing 2 mL of 0.9% Sodium Chloride Injection, USP.
75 International Units FSH activity, supplied as:
NDC 55566-8505-6: Box of 5 vials + 5 vials diluent + 5 Q•Cap
® vial adaptors.
17 PATIENT COUNSELING INFORMATION
See FDA-approved patient labeling (Patient Information and Instructions for Use)
17.1 Dosing and Use
Instruct women on the correct usage and dosing of MENOPUR ® [see Dosage and Administration (2.2)] . Caution women not to change the dosage or the schedule of administration unless she is told to do so by her healthcare provider.
17.2 Duration and Monitoring Required
Prior to beginning therapy with BRAVELLE ®, inform women about the time commitment and monitoring procedures necessary for treatment.
17.3 Instructions Regarding a Missed Dose
Inform the woman that if she misses or forgets to take a dose of BRAVELLE ®, the next dose should not be doubled and she should call her healthcare provider for further dosing instructions.
17.4 Ovarian Hyperstimulation Syndrome (OHSS)
Inform women regarding the risks of OHSS [see Warnings and Precautions (5.3)] and OHSS-associated symptoms including lung and blood vessel problems [see Warnings and Precautions (5.4)] and ovarian torsion [see Warnings and Precautions (5.5)] with the use of BRAVELLE ®.
17.5 Multi-fetal Gestation and Birth
Inform women regarding the risk of multi-fetal gestation and birth with the use of BRAVELLE ® [see Warnings and Precautions (5.6)] .
Vials of sterile diluent of 0.9% Sodium Chloride Injection, USP, manufactured for Ferring Pharmaceuticals Inc.
Patient Information
BRAVELLE
® (brä-vel)
(urofollitropin for injection, purified)
for subcutaneous use
Read this Patient Information before you start using BRAVELLE ® and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or your treatment.
What is BRAVELLE ®?
BRAVELLE ® is a prescription medicine that contains follicle stimulating hormone (FSH). BRAVELLE ® is used to treat women:
- who need help developing and releasing eggs (ovulating) and have already received a medicine to control their pituitary gland
- with healthy ovaries so they can make multiple (more than 1) eggs as part of an Assisted Reproductive Technology (ART) Cycle
Who should not use BRAVELLE ®?
Do not use BRAVELLE ® if you:
- are allergic to urofollitropin or any of the ingredients in BRAVELLE ®. See the end of this leaflet for a complete list of ingredients in BRAVELLE ®.
- have ovaries that no longer make eggs (primary ovarian failure)
- are pregnant or think you may be pregnant. If BRAVELLE ® is taken while you are pregnant, it may harm your baby,
- have problems with your thyroid gland or adrenal gland or pituitary gland that are not controlled by taking medicine
- have a tumor in your female organs, including your ovaries, breast, or uterus that may get worse with high levels of estrogen
- have a tumor of your pituitary gland or hypothalamus
- have abnormal bleeding from your uterus or vagina and the cause is not known
- have ovarian cysts or enlarged ovaries, not due to a problem called polycystic ovary syndrome (PCOS)
What should I tell my healthcare provider before using BRAVELLE ®?
Before using BRAVELLE ®, tell your healthcare provider if you:
- have been told by a healthcare provider that you are at an increased risk for blood clots (thrombosis)
- have ever had a blood clot (thrombosis), or anyone in your family has ever had a blood clot
- had stomach (abdominal) surgery
- had twisting of your ovary (ovarian torsion)
- had or have a cyst in your ovary
- have any other medical conditions
- are breast feeding or plan to breast feed. It is not known if BRAVELLE ® passes into your breast milk. You and your healthcare provider should decide if you will use BRAVELLE ® or breastfeed. You should not do both.
Tell your healthcare provider all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine.
How should I use BRAVELLE ®?
- Read the Instructions for Use at the end of this Patient Information about the right way to use BRAVELLE ® or BRAVELLE ® mixed with MENOPUR ®.
- Use BRAVELLE ® exactly as your healthcare provider tells you to use it.
- Your healthcare provider will tell you how much BRAVELLE ® to use and when to use it.
- Your healthcare provider may change your dose of BRAVELLE ® if needed.
- If you miss a dose of BRAVELLE ®, call your healthcare provider right away. Do not double the amount of BRAVELLE ® you are taking.
- You may need more than 1 vial of BRAVELLE ® for your dose.
- BRAVELLE ® may be given under your skin (subcutaneously) or into your muscle (intramuscularly). Your healthcare provider will tell you where and how to give your BRAVELLE ®.
- Your healthcare provider will give you BRAVELLE ® intramuscularly.
- BRAVELLE ® may be mixed with MENOPUR ® in the same syringe when you give it subcutaneously.
What are possible side effects of BRAVELLE ®?
BRAVELLE ® may cause serious side effects, including:
-
serious allergic reactions. Symptoms of allergic reactions include:
- rash
- swelling of your face and throat
- rapid swelling all over your body
- trouble breathing
If you have a serious allergic reaction, stop using BRAVELLE ® and call your healthcare provider or go to the nearest hospital emergency room right away.
- ovaries that are too large. BRAVELLE ® may cause your ovaries to be abnormally large. Symptoms of large ovaries include bloating or pain in your lower stomach (pelvic) area. If your ovaries become too large your healthcare provider may tell you that you should not have intercourse (sex) so you do not rupture an ovarian cyst.
-
ovarian hyperstimulation syndrome (OHSS). Using BRAVELLE
® may cause OHSS. OHSS is a serious medical condition that can happen when your ovaries produce too many eggs (overstimulated). OHSS can cause fluid to suddenly build up in the area of your stomach, chest, and heart, and cause blood clots to form. OHSS may also happen after you stop using BRAVELLE
®. Stop using BRAVELLE
® and call your healthcare provider or go to the nearest hospital emergency room right away if you have any of the following symptoms of OHSS:
- severe pelvic or stomach pain
- nausea
- vomiting
- sudden weight gain
- swollen stomach
- diarrhea
- trouble breathing
- decreased or no urine
- lung problems. BRAVELLE ® may cause serious lung problems that can sometimes lead to death including fluid in the lungs, trouble breathing, and worsening of asthma.
-
blood clots. BRAVELLE
® may increase your chance of having blood clots in your blood vessels. Blood clots can cause:
- blood vessel problems (thrombophlebitis)
- stroke
- loss of your arm or leg
- blood clot in your lung (pulmonary embolus)
- twisting (torsion) of your ovaries. BRAVELLE ® may increase the chance of your ovary twisting, if you already have certain conditions such as OHSS, pregnancy and previous abdominal surgery. Twisting of your ovary may lead to blood flow being cut off to your ovary.
- pregnancy with and birth of multiple babies. BRAVELLE ® may increase your chance of having a pregnancy with more than 1 baby. Having a pregnancy and giving birth to more than 1 baby at a time increases the health risk for you and your babies. Your healthcare provider should talk to you about your chances of multiple births before you start using BRAVELLE ®.
- birth defects in your unborn baby. Babies born after ART may have an increased chance of birth defects. Your age, certain sperm problems, your genetic background and that of your partner, and a pregnancy with more than 1 baby at a time may increase the chance that your baby may have birth defects.
- ectopic pregnancy (pregnancy outside your womb). BRAVELLE ® may increase your chance of having a pregnancy that is abnormally outside of your womb. Your chance of having a pregnancy outside of your womb is increased if you also have fallopian tube problems.
- miscarriage. Your chance of loss of an early pregnancy may be increased if you had difficulty becoming pregnant.
- tumors of the ovary. If you have used medicines like BRAVELLE ® more than 1 time to get pregnant, you may have an increased chance of having tumors in your ovaries, including cancer.
The most common side effects of BRAVELLE ® include:
- stomach cramps
- stomach fullness and bloating
- headache
- nausea
- pain
- pelvic pain
- hot flashes
- trouble breathing
- pain after egg removal (retrieval)
These are not all the possible side effects of BRAVELLE ®. For more information, ask your healthcare provider or pharmacist.
Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
How should I store BRAVELLE ®?
- Before mixing, store BRAVELLE ® powder in the refrigerator or at room temperature between 37ºF to 77ºF (3ºC to 25ºC).
- Protect BRAVELLE ® from light.
- BRAVELLE ® should be used right after mixing.
- Throw away any unused BRAVELLE ®.
Keep BRAVELLE ® and all medicines out of the reach of children.
General information about the safe and effective use of BRAVELLE ®.
Medicines are sometimes prescribed for purposes other than those listed in a Patient Information leaflet. Do not use BRAVELLE ® for a condition for which it was not prescribed. Do not give BRAVELLE ® to other people, even if they have the same condition you have. It may harm them.
This Patient Information summarizes the most important information about BRAVELLE ®. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about BRAVELLE ® that is written for health professionals.
For more information go to www.bravelle.com, or call 1-888-FERRING (1-888-337-7464).
What are the ingredients in BRAVELLE®?
Active ingredient: urofollitropin
Inactive ingredients: lactose monohydrate, polysorbate, sodium phosphate dibasic, heptahydrate and phosphoric acid
Instructions for Use
BRAVELLE® (brä-vel)
(urofollitropin for injection, purified)
for subcutaneous use
Your healthcare provider should show you how to mix and inject BRAVELLE ® or BRAVELLE ® mixed with MENOPUR ® before you do it for the first time. Before using BRAVELLE ® or BRAVELLE ® mixed with MENOPUR ® for the first time, read this Instructions for Use carefully. Keep this leaflet in a safe place and read it when you have questions.
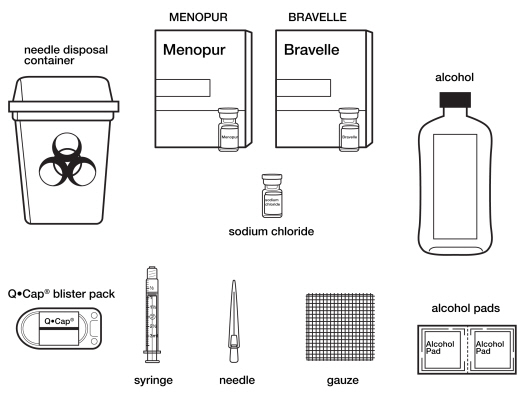
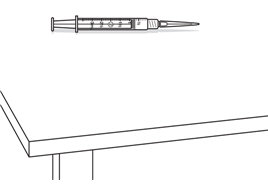
Supplies you will need to give your injection of BRAVELLE ® or BRAVELLE ® mixed with MENOPUR ®. See Figure A.
- a clean, flat surface to work on, like a table
- vials of BRAVELLE ® powder (and MENOPUR ® powder if you are going to mix the 2 medicines)
- 1 vial of 0.9% Sodium Chloride, USP used for mixing the medicine
- alcohol pads
- rubbing alcohol
- gauze pads
- 1 sterile syringe and 1 sterile needle with cap. Your healthcare provider should tell you which syringe and needle to use.
- the Q•Cap ® (vial adapter) that comes with your medicine
- a sharps disposal container for throwing away your used needles and syringes. See "
Disposing of your used needles and syringes" at the end of these instructions.
Step 1. Preparing your BRAVELLE ® or BRAVELLE ® mixed with MENOPUR ®.
- Wash your hands well with soap and water and dry them with a clean towel.
- Place all the supplies you need on the clean surface you already prepared.
- Check the vial(s) of BRAVELLE (and ® MENOPUR ® if needed) to make sure there is powder or a pellet in the vial(s). If you do not see any powder in the vial(s) do not use the vial and call your pharmacist or healthcare provider.
- Check the 0.9% Sodium Chloride, USP vial to make sure that the liquid is clear and does not contain any particles. If you see any particles in the liquid or the liquid is discolored, do not use the vial and call your pharmacist or healthcare provider.
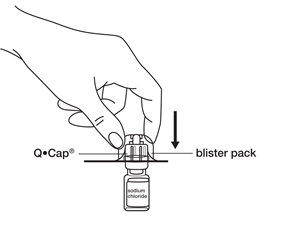
- Check the Q•Cap ® blister pack package to make sure it is intact. Do not use if the package is damaged.
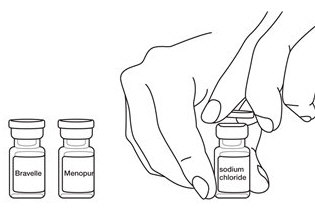
- Remove the plastic cap(s) from the vial(s) of BRAVELLE
® (and MENOPUR
® if needed) and 0.9% Sodium Chloride, USP vial.
See
Figure B.
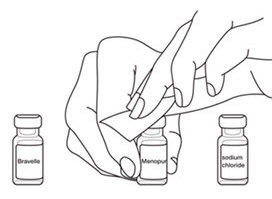
- Wipe the tops of the vials with alcohol and allow them to dry. Do not touch the tops of the vials after you have wiped them.
See
Figure C.
- Place the vial of 0.9% Sodium Chloride, USP on the table.
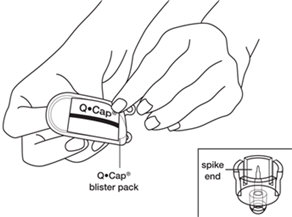
- Open the Q•Cap
® blister pack by peeling back the lidding.
See
Figure D. Do not take the Q•Cap
® out of the blister pack at this time.
Do not touch the spike or connector (luer) ends of the Q•Cap
®.
- Hold the 0.9% Sodium Chloride, USP vial in 1 hand. With your other hand, hold the sides of the Q•Cap
® blister pack, turn the Q•Cap
® blister pack over, and place it on top of the vial. Push the Q•Cap
® straight down into the rubber stopper of the vial until it stops.
See
Figure E.
- Do not use the Q•Cap ® if it falls out of the blister pack. Throw it away and get a new one.
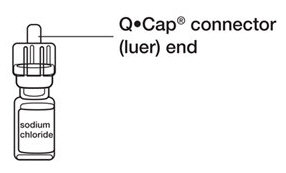
- Remove the blister pack and throw it away in your household trash. Do not touch the connector end (luer) of the Q•Cap
®.
See
Figure F.
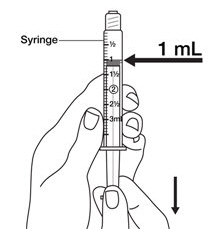
- Take the syringe and pull down on the syringe plunger rod until you have withdrawn the amount of 0.9% Sodium Chloride, USP from the vial that your healthcare provider told you to use.
- The usual amount of 0.9% Sodium Chloride, USP used to mix your BRAVELLE
® is 1 mL, but you should use the amount that your healthcare provider tells you to use.
See
Figure G.
- Be very careful not to touch the syringe plunger during this step.
- The usual amount of 0.9% Sodium Chloride, USP used to mix your BRAVELLE
® is 1 mL, but you should use the amount that your healthcare provider tells you to use.
See
Figure G.
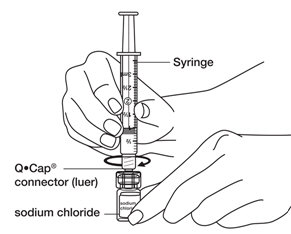
- Place the tip of the syringe into the connector end (luer) of the Q•Cap
® then twist the syringe clockwise until it is tight. Be careful not to overtighten the syringe.
See
Figure H.
- Slowly push down on the syringe plunger to push the air from the syringe into the vial.
See
Figure I.
- Keeping the syringe and Q•Cap
® together, turn the vial upside down and pull down on the syringe plunger to withdraw the right amount of 0.9% Sodium Chloride, USP from the vial. Your healthcare provider should tell you the right amount of 0.9% Sodium Chloride, USP to use.
See
Figure J.
- Separate the Q•Cap
® and syringe from the vial by pulling up on the syringe barrel. Do not pull the plunger to remove the Q•Cap
®. Throw away 0.9% Sodium Chloride, USP vial in your household trash.
See
Figure K.
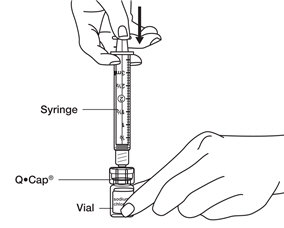
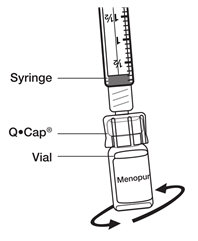
- Hold the vial of BRAVELLE
® powder in 1 hand. With your other hand, hold the sides of the syringe with the Q•Cap
® attached and place the tip of the Q•Cap
® over the top of the vial. Push the tip of the Q•Cap
® into the rubber stopper on the top of the vial until it stops and snaps into place. Be careful not to push down on the syringe plunger during this step.
See
Figure L.
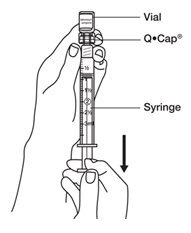
- Slowly push down on the syringe plunger to push the 0.9% Sodium Chloride, USP into the vial with the BRAVELLE
® powder in it. Gently swirl the vial until the BRAVELLE
® powder is completely dissolved.
Do not shake the vial as this will cause bubbles.
See
Figure M.
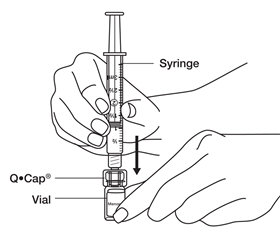
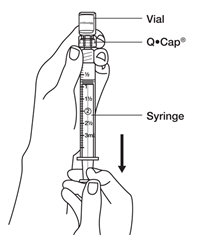
- As soon as the powdered medicine has completely dissolved, push the plunger down to empty any remaining air from the syringe, then turn the vial upside down and slowly pull down on the plunger to withdraw all of the BRAVELLE
® into the syringe.
See
Figure N.
- Be careful not to pull the plunger stopper all the way out of the syringe barrel.
If your healthcare provider tells you to use more than 1 vial of BRAVELLE ® or tells you to mix your BRAVELLE ® with MENOPUR ® in the same syringe:
- Mix your first vial of BRAVELLE ® powder or MENOPUR ® powder with 0.9% Sodium Chloride, USP. Do not inject your dose yet.
- Use the liquid in the syringe you have just mixed to mix the next vial of BRAVELLE ® or MENOPUR ®. See Figures L through N.
- You can use the liquid in the syringe to mix up to 5 more vials of medicine.
- Your healthcare provider will tell you how many vials of BRAVELLE ® and MENOPUR ® to use.
Step 2. Removing the Q•Cap ® and adding your needle for injection.
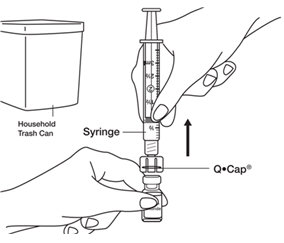
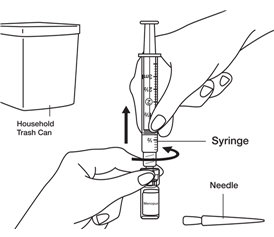
- When you have finished mixing the last vial needed for your injection and have withdrawn all the medicine into the syringe, remove the syringe from the Q•Cap
® by twisting the syringe counter-clockwise while holding the Q•Cap
® steady.
See
Figure O.
Throw away the Q•Cap
® with the attached vial into your household trash.
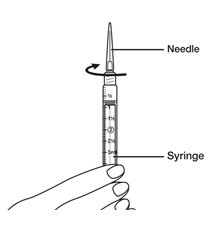
- You are now ready to attach the needle to the syringe for your injection.
Your healthcare provider will tell you what needle you should use for your injection. - While holding the syringe with the syringe tip pointing up, place the needle on the top of the syringe. Gently push down on the needle and twist the needle onto the syringe in a clockwise direction until it is tight.
See
Figure P.
-
Do not remove the needle cap until you are ready for your injection.(
See
Step 4)
- Carefully set the syringe with the needle down on the table.
See
Figure Q.
- Carefully set the syringe with the needle down on the table.
See
Figure Q.
Step 3. Prepare Injection site for BRAVELLE ® or with BRAVELLE ® mixed with MENOPUR ®.
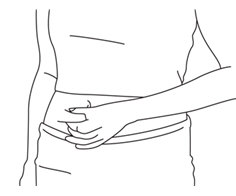
- Select a site to inject BRAVELLE
® or with BRAVELLE
® mixed with MENOPUR
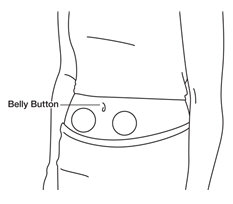
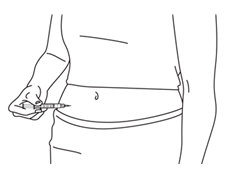
® on your stomach area (abdomen).
- Pick a site on your lower abdomen, 1-2 inches below the navel, alternating between left and right sides.
- Each day, inject in a different site to help reduce soreness and skin problems. For example, on day 1, inject yourself on the right side of your abdomen. The next day, inject yourself on the left side of your abdomen. Changing your injection sites every day will help reduce soreness and skin problems.
See
Figure R.
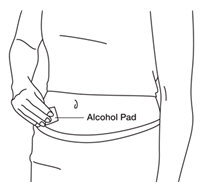
- Clean your injection site with an alcohol pad. Let the alcohol dry.
See
Figure S.
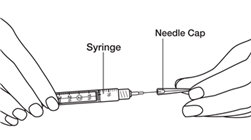
- Carefully remove the needle cap from the syringe.
See
Figure T.
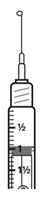
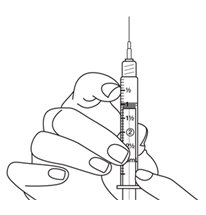
- Hold the syringe with the needle pointing straight up. Pull down slightly on the plunger and tap the barrel of the syringe so that any air bubbles rise to the top. Slowly press the plunger up until all the air is out of the syringe and a small drop of liquid is seen at the tip of the needle.
See
Figure U.
- Tap the syringe to remove the small drop of liquid at the tip of the needle.
Do not let the needle touch anything to keep it sterile.
See
Figure V.
- The medicine is now ready for you to inject. See Figure V.
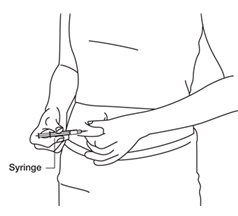
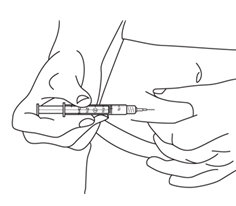
- Hold the syringe in 1 hand. Use your other hand to gently pinch a fold of cleaned skin where you will insert your needle. Hold the skin between your thumb and index finger.
See
Figure W.
- Hold your syringe at a right angle to your skin. Quickly insert the needle all the way into your skin fold.
See
Figure X.
- Push down the plunger of the syringe with a steady motion. Keep pushing until all the fluid is injected into your skin.
See
Figure Y.
- Let go of your skin fold and pull the needle straight out of your skin.
See
Figure Z.
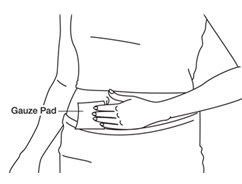
- If there is any bleeding at your injection site, place a gauze pad over your injection site. Apply gentle pressure to stop the bleeding. Do not rub the site.
See
Figure AA.
- If your injection site becomes sore or red, you may put ice on your injection site for 1 minute and then take it off for 3 minutes. If needed, you may repeat this 3 or 4 times.
Step 6. Disposing of your used needles and syringes.
- Put your used needles and syringes in a FDA-cleared sharps disposal container right away after use. Do not throw away loose needles and syringes in your household trash.
- If you do not have a FDA-cleared sharps disposal container, you may use a household container that:
- is made of a heavy-duty plastic,
- can be closed with a tight-fitting, puncture-resistant lid, without sharps being able to come out,
- remains upright and stable during use,
- is leak-resistant, and
- is properly labeled to warn of hazardous waste inside the container.
- When your sharps disposal container is almost full, you will need to follow your community guidelines for the right way to dispose of your sharps disposal container. There may be state or local laws about how you should throw away used needles and syringes. For more information about safe sharps disposal, and for specific information about sharps disposal in the state that you live in, go to the FDA's website at: http://www.fda.gov/safesharpsdisposal.
Do not dispose of your used sharps disposal container in your household trash unless your community guidelines permit this. Do not recycle your used sharps disposal container.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
MANUFACTURED FOR:

FERRING PHARMACEUTICALS INC.
PARSIPPANY, NJ 07054
Revised: July 2015
PRINCIPAL DISPLAY PANEL - Kit Carton
NDC 55566-8505-2
Bravelle® 75 IU
(urofollitropin for injection, purified)
5 single dose vials of urofollitropin for injection, purified
5 single dose vials of 0.9% Sodium Chloride Injection, USP, 2 mL
FOR SUBCUTANEOUS OR
INTRAMUSCULAR INJECTION ONLY
Rx only
Reconstitute with 1 mL 0.9% Sodium Chloride Injection, USP.
Administer SC or IM immediately after reconstitution.
Discard unused portion.
Usual Dosage: See package insert for dosage and complete
Prescribing Information.
Lyophilized powder may be stored refrigerated or at room
temperature (3° to 25° C / 37° to 77° F). Protect from light.
FERRING
PHARMACEUTICALS

| BRAVELLE
urofollitropin kit |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Ferring Pharmaceuticals Inc. (103722955) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Ferring Production Inc. | 079510999 | label(55566-8505) , pack(55566-8505) | |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Jubilant HollisterStier General Partnership | 246762764 | manufacture(55566-8505) , pack(55566-8505) | |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Ferring GmbH | 328609615 | manufacture(55566-8505) | |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| F. M. Howell & Company | 962888116 | pack(55566-8505) | |