VANCOMYCIN HYDROCHLORIDE
-
vancomycin hydrochloride injection, powder, lyophilized, for solution
Pfizer Laboratories Div Pfizer Inc
----------
Rx only
To reduce the development of drug-resistant bacteria and maintain the effectiveness of Vancomycin Hydrochloride for Injection, USP and other antibacterial drugs, Vancomycin Hydrochloride for Injection, USP should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria.
DESCRIPTION
Vancomycin Hydrochloride for Injection, USP is a lyophilized powder, for preparing intravenous (IV) infusions. Each Vancomycin Hydrochloride for Injection, USP 10 g Pharmacy Bulk Package bottle contains vancomycin hydrochloride equivalent to 10 g vancomycin base. 500 mg of the base are equivalent to 0.34 mmol. When reconstituted with Sterile Water for Injection to a concentration of 100 mg/mL for the 10 g Pharmacy Bulk Package bottle, the pH of the solution is between 2.5 to 4.5. Vancomycin Hydrochloride for Injection, USP should be administered intravenously in diluted solution (see DOSAGE AND ADMINISTRATION).
Vancomycin Hydrochloride for Injection, USP is a tricyclic glycopeptide antibiotic derived from Amycolatopasis orientalis (formerly Nocardia orientalis). The chemical name for vancomycin hydrochloride is (Sa)-(3S, 6R, 7R, 22R, 23S, 26S, 36R, 38aR)-44- [[2-O-(3-Amino-2, 3, 6-trideoxy-3-C-methyl-α-L-lyxo-hexopyranosyl)-β-D-glucopyranosyl]oxy]- 3-(carbamoylmethyl)-10, 19-dichloro-2, 3, 4, 5, 6, 7, 23, 24, 25, 26, 36, 37, 38, 38a-tetradecahydro-7, 22, 28, 30, 32-pentahydroxy-6- [(2R)-4-methyl-2-(methylamino)valeramido]- 2, 5, 24, 38, 39-pentaoxo-22H-8, 11 : 18, 21-dietheno-23, 36-(iminomethano)-13, 16 : 31, 35-dimetheno-1H, 16H- [1,6,9]oxadiazacyclohexadecino[4, 5-m][10, 2, 16]- benzoxadiazacyclotetracosine-26-carboxylic acid, monohydrochloride. Vancomycin hydrochloride has the following structural formula:
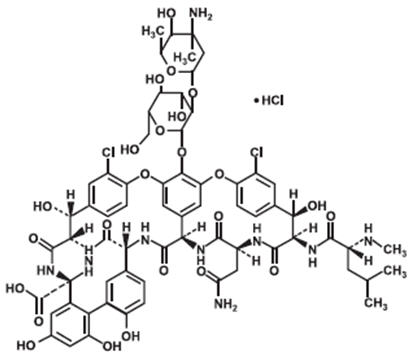
C66H75Cl2N9O24• HCl 1485.71
A Pharmacy Bulk Package is a sterile dosage form containing many single doses. The contents are intended for use in a pharmacy admixture program and are restricted to the preparation of admixtures for IV infusion. AFTER RECONSTITUTION FURTHER DILUTION IS REQUIRED BEFORE USE.
CLINICAL PHARMACOLOGY
Vancomycin is poorly absorbed after oral administration.
In subjects with normal kidney function, multiple intravenous dosing of 1 g of vancomycin (15 mg/kg) infused over 60 minutes produces mean plasma concentrations of approximately 63 mcg/mL immediately after the completion of infusion, mean plasma concentrations of approximately 23 mcg/mL 2 hours after infusion, and mean plasma concentrations of approximately 8 mcg/mL 11 hours after the end of the infusion. Multiple dosing of 500 mg infused over 30 minutes produces mean plasma concentrations of about 49 mcg/mL at the completion of infusion, mean plasma concentrations of about 19 mcg/mL 2 hours after infusion, and mean plasma concentrations of about 10 mcg/mL 6 hours after infusion. The plasma concentrations during multiple dosing are similar to those after a single dose.
The mean elimination half-life of vancomycin from plasma is 4 to 6 hours in subjects with normal renal function. In the first 24 hours, about 75% of an administered dose of vancomycin is excreted in urine by glomerular filtration. Mean plasma clearance is about 0.058 L/kg/h, and mean renal clearance is about 0.048 L/kg/h. Renal dysfunction slows excretion of vancomycin. In anephric patients, the average half-life of elimination is 7.5 days. The distribution coefficient is from 0.3 to 0.43 L/kg. There is no apparent metabolism of the drug. About 60% of an intraperitoneal dose of vancomycin administered during peritoneal dialysis is absorbed systemically in 6 hours. Serum concentrations of about 10 mcg/mL are achieved by intraperitoneal injection of 30 mg/kg of vancomycin. However, the safety and efficacy of the intraperitoneal use of vancomycin has not been established in adequate and well-controlled trials (see PRECAUTIONS).
Total systemic and renal clearance of vancomycin may be reduced in the elderly.
Vancomycin is approximately 55% serum protein bound as measured by ultrafiltration at vancomycin serum concentrations of 10 to 100 mcg/mL. After IV administration of vancomycin, inhibitory concentrations are present in pleural, pericardial, ascitic, and synovial fluids; in urine; in peritoneal dialysis fluid; and in atrial appendage tissue. Vancomycin does not readily diffuse across normal meninges into the spinal fluid; but, when the meninges are inflamed, penetration into the spinal fluid occurs.
Microbiology
The bactericidal action of vancomycin results primarily from inhibition of cell-wall biosynthesis. In addition, vancomycin alters bacterial-cell-membrane permeability and RNA synthesis. There is no cross-resistance between vancomycin and other antibiotics.
Vancomycin is not active in vitro against gram-negative bacilli, mycobacteria, or fungi.
Synergy
The combination of vancomycin and an aminoglycoside acts synergistically in vitro against many strains of Staphylococcus aureus, Streptococcus bovis, enterococci, and the viridans group streptococci.
Vancomycin has been shown to be active against most strains of the following microorganisms, both in vitro and in clinical infections as described in the INDICATION AND USAGE section.
Aerobic gram-positive microorganisms
Diphtheroids
Enterococci (e.g., Enterococcus faecalis)
Staphylococci, including Staphylococcus aureus and Staphylococcus epidermis (including heterogeneous methicillin-resistant strains)
Streptococcus bovis
Viridans group streptococci
The following in vitro data are available, but their clinical significance is unknown.
Vancomycin exhibits in vitro MIC's of 1 mcg/mL or less against most (≥90%) strains of streptococci listed below and MIC's of 4 mcg/mL or less against most (≥90%) strains of other listed microorganisms; however, the safety and effectiveness of vancomycin in treating clinical infections due to these microorganisms have not been established in adequate and well-controlled clinical trials.
Aerobic gram-positive microorganisms
Listeria monocytogenes
Streptococcus pyogenes
Streptococcus pneumoniae (including penicillin-resistant strains)
Streptococcus agalactiae
Susceptibility Test Methods
When available, the clinical microbiology laboratory should provide the results of in-vitro susceptibility test results for antimicrobial drugs used in local hospitals and practice areas to the physician as periodic reports that describe the susceptibility profile of nosocomial and community acquired pathogens. These reports should aid the physician in selecting the most effective antimicrobial.
Dilution Techniques
Quantitative methods are used to determine antimicrobial minimum inhibitory concentrations (MICs). These MICs provide estimates of the susceptibility of bacteria to antimicrobial compound. The MICs should be determined using a standardized procedure. Standardized procedures are based on dilution method1,2 (broth, agar or microdilution) or equivalent using standardized inoculum and concentrations of vancomycin powder. The MIC values should be interpreted according to the criteria in Table 1.
Diffusion Techniques
Quantitative methods that require measurement of zone diameters also provide reproducible estimates of the susceptibility of bacteria to antimicrobial compounds. One such standardized procedure2,3 requires the use of standardized inoculum concentrations. This procedure uses paper disks impregnated with 30 mcg of vancomycin to test the susceptibility of microorganisms to vancomycin. Interpretation involves correlation of the diameter obtained in the disk test with the MIC for vancomycin. Reports from the laboratory providing results of the standard single-disk susceptibility test with a 30 mcg vancomycin disk should be interpreted according to the following criteria in Table 1.
| Minimum Inhibitory Concentrations (mcg/mL) | Disk Diffusion Diameters (mm) | |||||
|---|---|---|---|---|---|---|
| Pathogen | Susceptible (S) | Intermediate (I) | Resistant (R) | Susceptible (S) | Intermediate (I) | Resistant (R) |
|
||||||
| Enterococci * | ≤4 | 8–16 | ≥32 | ≥17† | 15 – 16† | ≥14† |
| Staphylococcus aureus | ≤2 | 4–8 | ≥16 | ≥15‡ | - | - |
| Coagulase-negative staphylococci | ≤4 | 8–16 | ≥32 | ≥15‡ | - | - |
| Streptococci other than S.pneumoniae | ≤1‡,§ | - | - | ≥17 ‡,¶ | - | - |
A report of "Susceptible" indicates that the pathogen is likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable. A report of "Intermediate" indicates that the result should be considered equivocal, and, if the microorganism is not fully susceptible to alternative, clinically feasible drugs the test should be repeated. This category implies possible clinical applicability in body sites where the drug is physiologically concentrated or in situations where high dosage of drug can be used. This category also provides a buffer zone which prevents small uncontrolled technical factors from causing major discrepancies in interpretation. A report of "Resistant" indicates that the pathogen is not likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable; other therapy should be selected.
Quality Control
Standardized susceptibility test procedures require the use of laboratory control microorganisms to monitor and ensure the accuracy and precision of the supplies and reagents used in the assay, and the techniques of the individuals performing the test. Standard vancomycin powder should provide MIC values provided below. For the diffusion technique, the 30 mcg vancomycin disk should provide the following zone diameters with the quality control strains:
| Organism (ATCC #) | MIC range (mcg/mL) | Disk diffusion range (mm) |
|---|---|---|
|
||
| Enterococcus faecalis (29212) | 1–4 | Not applicable |
| Staphylococcus aureus (29213) | 0.5–2 | Not applicable |
| Staphylococcus aureus (25923) | Not applicable | 17 – 21 |
| Streptococcus pneumoniae (49619)* | 0.12–0.5 | 20 – 27 |
INDICATIONS AND USAGE
To reduce the development of drug-resistant bacteria and maintain the effectiveness of Vancomycin Hydrochloride for Injection, USP and other antibacterial drugs, Vancomycin Hydrochloride for Injection, USP should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Vancomycin Hydrochloride for Injection, USP is indicated for the treatment of serious or severe infections caused by susceptible strains of methicillin-resistant (β-lactam-resistant) staphylococci. It is indicated for penicillin-allergic patients, for patients who cannot receive or who have failed to respond to other drugs, including the penicillins or cephalosporins, and for infections caused by vancomycin-susceptible organisms that are resistant to other antimicrobial drugs. Vancomycin Hydrochloride for Injection, USP is indicated for initial therapy when methicillin-resistant staphylococci are suspected, but after susceptibility data are available, therapy should be adjusted accordingly.
Vancomycin Hydrochloride for Injection, USP is effective in the treatment of staphylococcal endocarditis. Its effectiveness has been documented in other infections due to staphylococci, including septicemia, bone infections, lower respiratory tract infections, and skin and skin-structure infections. When staphylococcal infections are localized and purulent, antibiotics are used as adjuncts to appropriate surgical measures.
Vancomycin Hydrochloride for Injection, USP has been reported to be effective alone or in combination with an aminoglycoside for endocarditis caused by Streptococcus viridans or S. bovis. For endocarditis caused by enterococci (e.g., E. faecalis), Vancomycin Hydrochloride for Injection, USP has been reported to be effective only in combination with an aminoglycoside.
Vancomycin Hydrochloride for Injection, USP has been reported to be effective for the treatment of diphtheroid endocarditis. Vancomycin Hydrochloride for Injection, USP has been used successfully in combination with either rifampin, an aminoglycoside, or both in early-onset prosthetic valve endocarditis caused by S. epidermidis or diphtheroids.
Specimens for bacteriologic cultures should be obtained in order to isolate and identify causative organisms and to determine their susceptibilities to Vancomycin Hydrochloride for Injection, USP.
The parenteral form of Vancomycin Hydrochloride for Injection, USP may be administered orally for treatment of antibiotic-associated pseudomembranous colitis produced by C. difficile and for staphylococcal enterocolitis. Parenteral administration of vancomycin hydrochloride alone is of unproven benefit for these indications. Vancomycin is not effective by the oral route for other types of infection.
CONTRAINDICATIONS
Vancomycin Hydrochloride for Injection, USP is contraindicated in patients with known hypersensitivity to this antibiotic.
WARNINGS
Rapid bolus administration (e.g., over several minutes) may be associated with exaggerated hypotension including shock, and rarely, cardiac arrest.
Vancomycin Hydrochloride for Injection, USP should be administered in a diluted solution over a period of not less than 60 minutes to avoid rapid-infusion-related reactions. Stopping the infusion usually results in a prompt cessation of these reactions.
Ototoxicity has occurred in patients receiving vancomycin. It may be transient or permanent. It has been reported mostly in patients who have been given excessive doses, who have an underlying hearing loss, or who are receiving concomitant therapy with another ototoxic agent such as an aminoglycoside. Vancomycin should be used with caution in patients with renal insufficiency because the risk of toxicity is appreciably increased by high, prolonged blood concentrations.
Dosage of vancomycin must be adjusted for patients with renal dysfunction (see PRECAUTIONS and DOSAGE AND ADMINISTRATION).
Clostridium difficile associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including Vancomycin Hydrochloride for Injection, USP, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibiotic use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibiotic use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibiotic treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
PRECAUTIONS
General
Prescribing Vancomycin Hydrochloride for Injection, USP in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
Clinically significant serum concentrations have been reported in some patients being treated for active C. difficile-induced pseudomembranous colitis after multiple oral doses of vancomycin.
Prolonged use of vancomycin may result in the overgrowth of non-susceptible organisms. Careful observation of the patient is essential. If superinfection occurs during therapy, appropriate measures should be taken. In rare instances, there have been reports of pseudomembranous colitis due to C. difficile developing in patients who received IV vancomycin.
In order to minimize the risk of nephrotoxicity when treating patients with underlying renal dysfunction or patients receiving concomitant therapy with an aminoglycoside, serial monitoring of renal function should be performed and particular care should be taken in following appropriate dosing schedules (see DOSAGE AND ADMINISTRATION).
Serial tests of auditory function may be helpful in order to minimize the risk of ototoxicity.
Reversible neutropenia has been reported in patients receiving vancomycin (see ADVERSE REACTIONS). Patients who will undergo prolonged therapy with vancomycin or those who are receiving concomitant drugs which may cause neutropenia should have periodic monitoring of the leukocyte count.
Vancomycin is irritating to tissue and must be given by a secure intravenous route of administration. Pain, tenderness, and necrosis occur with intramuscular (IM) injection of vancomycin or with inadvertent extravasation. Thrombophlebitis may occur, the frequency and severity of which can be minimized by administering the drug slowly as a dilute solution (2.5 to 5 g/L) and by rotation of venous access sites.
There have been reports that the frequency of infusion-related events (including hypotension, flushing, erythema, urticaria, and pruritus) increases with the concomitant administration of anesthetic agents. Infusion-related events may be minimized by the administration of vancomycin as a 60-minute infusion prior to anesthetic induction.
The safety and efficacy of vancomycin administration by the intrathecal (intralumbar or intraventricular) route or by the intraperitoneal route have not been established by adequate and well-controlled trials.
Reports have revealed that administration of sterile vancomycin by the intraperitoneal route during continuous ambulatory peritoneal dialysis (CAPD) has resulted in a syndrome of chemical peritonitis. To date, this syndrome has ranged from a cloudy dialysate alone to a cloudy dialysate accompanied by variable degrees of abdominal pain and fever. This syndrome appears to be short-lived after discontinuation of intraperitoneal vancomycin.
Information for Patients
Patients should be counseled that antibacterial drugs including vancomycin should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When vancomycin is prescribed to treat a bacterial infection, patients should be told that although it is common to feel better early in the course of therapy, the medication should be taken exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by vancomycin or other antibacterial drugs in the future.
Diarrhea is a common problem caused by antibiotics which usually ends when the antibiotic is discontinued. Sometimes after starting treatment with antibiotics, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as two or more months after having taken the last dose of the antibiotic. If this occurs, patients should contact their physician as soon as possible.
Drug interactions
Concomitant administration of vancomycin and anesthetic agents has been associated with erythema and histamine-like flushing (see Pediatric Use under PRECAUTIONS) and anaphylactoid reactions (see ADVERSE REACTIONS).
Concurrent and/or sequential systemic or topical use of other potentially, neurotoxic and/or nephrotoxic drugs, such as amphotericin B, aminoglycosides, bacitracin, polymyxin B, colistin, viomycin, or cisplatin, when indicated requires careful monitoring.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Although no long-term studies in animals have been performed to evaluate carcinogenic potential, no mutagenic potential of vancomycin was found in standard laboratory tests. No definitive fertility studies have been performed.
Pregnancy
Teratogenic Effects
Pregnancy Category C
Animal reproduction studies have not been conducted with vancomycin. It is not known whether vancomycin can affect reproduction capacity. In a controlled clinical study, vancomycin was administered to pregnant women for serious staphylococcal infections that were complications of their IV drug abuse to evaluate potential ototoxic and nephrotoxic effects on the infant. Vancomycin was found in cord blood. No sensorineural hearing loss or nephrotoxicity attributable to vancomycin was noted. One infant experienced conductive hearing loss that was not attributed to the administration of vancomycin. Because the number of patients treated in this study was limited and vancomycin was administered only in the second and third trimesters, it is not known whether vancomycin causes fetal harm. Vancomycin should be given to a pregnant woman only if clearly needed.
Nursing Mothers
Vancomycin is excreted in human milk. Caution should be exercised when vancomycin is administered to a nursing woman. Because of the potential for adverse events, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
In pediatric patients, it may be appropriate to confirm desired vancomycin serum concentrations. Concomitant administration of vancomycin and anesthetic agents has been associated with erythema and histamine-like flushing in pediatric patients (see ADVERSE REACTIONS).
Geriatric Use
The natural decrement of glomerular filtration with increasing age may lead to elevated vancomycin serum concentrations if dosage is not adjusted. Vancomycin dosage schedules should be adjusted in elderly patients (see DOSAGE AND ADMINISTRATION).
ADVERSE REACTIONS
Infusion-Related Events
During or soon after rapid infusion of vancomycin patients may develop anaphylactoid reactions, including hypotension (see ANIMAL PHARMACOLOGY), wheezing, dyspnea, urticaria, or pruritus. Rapid infusion may also cause flushing of the upper body ("red neck") or pain and muscle spasm of the chest and back. These reactions usually resolve within 20 minutes but may persist for several hours. Such events are infrequent if vancomycin is given by a slow infusion over 60 minutes. In studies of normal volunteers, infusion-related events did not occur when vancomycin was administered at a rate of 10 mg/min or less.
Nephrotoxicity
Renal failure, principally manifested by increased serum creatinine or BUN concentrations, especially in patients administered large doses of vancomycin, has been reported rarely. Cases of interstitial nephritis have also been reported rarely. Most of these have occurred in patients who were given aminoglycosides concomitantly or who had preexisting kidney dysfunction. When vancomycin was discontinued, azotemia resolved in most patients.
Ototoxicity
A few dozen cases of hearing loss associated with vancomycin have been reported. Most of these patients had kidney dysfunction or a preexisting hearing loss, or were receiving concomitant treatment with an ototoxic drug. Vertigo, dizziness, and tinnitus have been reported rarely.
Hematopoietic
Reversible neutropenia, usually starting one week or more after onset of therapy with vancomycin or after a total dosage of more than 25 g, has been reported for several dozen patients. Neutropenia appears to be promptly reversible when vancomycin is discontinued. Thrombocytopenia has rarely been reported. Although a causal relationship has not been established, reversible agranulocytosis (granulocytes <500/mm3) has been reported rarely.
Gastrointestinal
Onset of pseudomembranous colitis symptoms may occur during or after antibiotic treatment (see WARNINGS).
Miscellaneous
Infrequently, patients have been reported to have had anaphylaxis, drug fever, nausea, chills, eosinophilia, rashes including exfoliative dermatitis, linear IgA bullous dermatosis, Stevens-Johnson syndrome, toxic epidermal necrolysis, and vasculitis in association with the administration of vancomycin.
Chemical peritonitis has been reported following intraperitoneal administration (see PRECAUTIONS).
Post Marketing Reports
The following adverse reactions have been identified during post-approval use of vancomycin. Because these reactions are reported voluntarily from a population of uncertain size, it is not possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Skin and Subcutaneous Tissue Disorders
Drug Rash with Eosinophilia and Systemic Symptoms (DRESS)
To report SUSPECTED ADVERSE EVENTS, contact FDA at 1-800-FDA-1088 or www.fda.gov.
OVERDOSAGE
Supportive care is advised, with maintenance of glomerular filtration. Vancomycin is poorly removed by dialysis.
Hemofiltration and hemoperfusion with polysulfone resin have been reported to result in increased vancomycin clearance. The median lethal intravenous dose is 319 mg/kg in rats and 400 mg/kg in mice.
To obtain up-to-date information about the treatment of overdose, a good resource is your certified Regional Poison Control Center. Telephone numbers of certified poison control centers are listed in the Physicians' Desk Reference (PDR). In managing overdosage, consider the possibility of multiple drug overdoses, interaction among drugs, and unusual drug kinetics in your patient.
DOSAGE AND ADMINISTRATION
Infusion-related events are related to both the concentration and the rate of administration of vancomycin. Concentrations of no more than 5 mg/mL and rates of no more than 10 mg/min are recommended in adults (see also age-specific recommendations). In selected patients in need of fluid restriction, a concentration up to 10 mg/mL may be used; use of such higher concentrations may increase the risk of infusion-related events. An infusion rate of 10 mg/min or less is associated with fewer infusion-related events (see ADVERSE REACTIONS). Infusion-related events may occur, however, at any rate or concentration.
Patients with Normal Renal Function
Adults
The usual daily intravenous dose is 2 g divided either as 500 mg every six hours or 1 g every 12 hours. Each dose should be administered at no more than 10 mg/min, or over a period of at least 60 minutes, whichever is longer. Other patient factors, such as age or obesity, may call for modification of the usual intravenous daily dose.
Pediatric Patients
The usual intravenous dosage of vancomycin is 10 mg/kg per dose given every 6 hours. Each dose should be administered over a period of at least 60 minutes. Close monitoring of serum concentrations of vancomycin may be warranted in these patients.
Neonates
In pediatric patients up to the age of of 1 month, the total daily intravenous dosage may be lower. In neonates, an initial dose of 15 mg/kg is suggested, followed by 10 mg/kg every 12 hours for neonates in the 1st week of life and every 8 hours thereafter up to the age of 1 month. Each dose should be administered over 60 minutes. In premature infants, vancomycin clearance decreases as postconceptional age decreases. Therefore, longer dosing intervals may be necessary in premature infants. Close monitoring of serum concentrations of vancomycin is recommended in these patients.
Patients with Impaired Renal Function and Elderly Patients
Dosage adjustment must be made in patients with impaired renal function. In premature infants and the elderly, greater dosage reductions than expected may be necessary because of decreased renal function. Measurement of vancomycin serum concentrations can be helpful in optimizing therapy, especially in seriously ill patients with changing renal function. Vancomycin serum concentrations can be determined by use of microbiologic assay, radioimmunoassay, fluorescence polarization immunoassay, fluorescence immunoassay, or high-pressure liquid chromatography.
If creatinine clearance can be measured or estimated accurately, the dosage for most patients with renal impairment can be calculated using the following table. The dosage of vancomycin per day in mg is about 15 times the glomerular filtration rate in mL/min (see following table).
| Creatinine Clearance mL/min | Vancomycin Dose mg/24 hr |
|---|---|
| 100 | 1,545 |
| 90 | 1,390 |
| 80 | 1,235 |
| 70 | 1,080 |
| 60 | 925 |
| 50 | 770 |
| 40 | 620 |
| 30 | 465 |
| 20 | 310 |
| 10 | 155 |
The initial dose should be no less than 15 mg/kg, even in patients with mild to moderate renal insufficiency.
The table is not valid for functionally anephric patients. For such patients, an initial dose of 15 mg/kg of body weight should be given to achieve prompt therapeutic serum concentrations. The dose required to maintain stable concentrations is 1.9 mg/kg/24 hr. In patients with marked renal impairment, it may be more convenient to give maintenance doses of 250 to 1000 mg once every several days rather than administering the drug on a daily basis. In anuria, a dose of 1000 mg every 7 to 10 days has been recommended.
When only serum creatinine concentration is known, the following formula (based on sex, weight, and age of the patient) may be used to calculate creatinine clearance. Calculated creatinine clearances (mL/min) are only estimates. The creatinine clearance should be measured promptly.
| Men: | Weight (kg) × (140 - age in years) |
| 72 × serum creatinine concentration (mg/dL) | |
| Women: | 0.85 × above value |
The serum creatinine must represent a steady state of renal function. Otherwise, the estimated value for creatinine clearance is not valid. Such a calculated clearance is an overestimate of actual clearance in patients with conditions: (1) characterized by decreasing renal function, such as shock, severe heart failure, or oliguria; (2) in which a normal relationship between muscle mass and total body weight is not present, such as in obese patients or those with liver disease, edema, or ascites; and (3) accompanied by debilitation, malnutrition, or inactivity.
The safety and efficacy of vancomycin administration by the intrathecal (intralumbar or intraventricular) route have not been established.
Intermittent infusion is the recommended method of administration.
COMPATIBILITY WITH OTHER DRUGS AND IV FLUIDS
The following diluents are physically and chemically compatible (with 4g/L vancomycin hydrochloride):
- 5% Dextrose Injection, USP
- 5% Dextrose Injection and 0.9% Sodium Chloride Injection, USP
- Lactated Ringer's Injection, USP
- 5% Dextrose and Lactated Ringer's Injection
- Normosol®-M and 5% Dextrose
- 0.9% Sodium Chloride Injection, USP
- Isolyte® E
Good professional practice suggests that compounded admixtures should be administered as soon after preparation as is feasible.
Vancomycin solution has a low pH and may cause physical instability of other compounds.
DIRECTIONS FOR PROPER USE OF PHARMACY BULK PACKAGE-NOT FOR DIRECT INFUSION
Pharmacy bulk packages are for use in pharmacy admixture service only in a suitable work area, such as a laminar flow hood. They should be hung by the integral hanger provided and suspended as a unit in the laminar flow hood. Using aseptic technique the container closure should be penetrated only one time after reconstitution utilizing a suitable sterile dispensing set which allows measured distribution of the contents. Use of a syringe and needle is not recommended as it may cause leakage. Swab vial stopper with an antiseptic solution.
Once the sterile dispensing set has been inserted into the container, withdrawal of the contents should be accomplished without delay. However, if this is not possible, a maximum time of 4 hours from the initial closure entry may be permitted to complete fluid transfer operations. Discard the container no later than 4 hours after initial closure puncture. This time limit should begin with introduction of solvent or diluent into the Pharmacy Bulk Package bottle.
PREPARATION AND STABILITY
10 g Pharmacy Bulk Package bottle
At the time of use, reconstitute by adding 95 mL of Sterile Water for Injection, USP to the 10 g of Pharmacy Bulk Package bottle of dry, vancomycin powder. The resultant solution will contain vancomycin equivalent to 500 mg/5 mL (1 g/10 mL). AFTER RECONSTITUTION FURTHER DILUTION IS REQUIRED.
Reconstituted solutions of vancomycin (500 mg/5 mL) must be further diluted in at least 100 mL of a suitable infusion solution. For doses of 1 gram (10 mL), at least 200 mL of solution must be used. The desired dose diluted in this manner should be administered by intermittent IV infusion over a period of at least 60 minutes.
Parenteral drug products should be visually inspected for particulate matter and discoloration prior to administration, whenever solution and container permit.
For Oral Administration
Oral vancomycin is used in treating antibiotic-associated pseudomembranous colitis caused by C. difficile and for staphylococcal enterocolitis. Vancomycin is not effective by the oral route for other types of infections. The usual adult total daily dose is 500 mg to 2 g given in 3 or 4 divided doses for 7 to 10 days. The total daily dose in children is 40 mg/kg of body weight in 3 or 4 divided doses for 7 to 10 days. The total daily dosage should not exceed 2 g. The appropriate dose may be diluted in 1 oz of water and given to the patient to drink. Common flavoring syrups may be added to the solution to improve the taste for oral administration. The diluted solution may be administered via a nasogastric tube.
HOW SUPPLIED
NDC 0069-2599-99 - Vancomycin Hydrochloride for Injection, USP is supplied as a Pharmacy Bulk Package bottle equivalent to 10 grams of vancomycin, individually packaged in a carton.
ANIMAL PHARMACOLOGY
In animal studies, hypotension and bradycardia occurred in dogs receiving an intravenous infusion of vancomycin hydrochloride, 25 mg/kg, at a concentration of 25 mg/mL and an infusion rate of 13.3 mL/min.
REFERENCES
- Methods for Dilution Antimicrobial Susceptibility Tests for Bacteria That Grow Aerobically; Approved Standard - 7th ed., CLSI document M7-A7. Clinical and Laboratory Standards Institute. Wayne, PA. January, 2006.
- Performance Standards for Antimicrobial Susceptibility Testing; 18th Informational Supplement, CLSI document M100-S18. Clinical and Laboratory Standards Institute. Wayne, PA. January, 2008.
- Performance Standards for Antimicrobial Disk Susceptibility Tests; Approved Standard - 9th ed., CLSI document M2-A9. Clinical and Laboratory Standards Institute. Wayne, PA. January, 2006.
- Moellering RC, Krogstad DJ, Greenblatt DJ: Vancomycin therapy in patients with impaired renal function: A nomogram for dosage. Ann Inter Med 1981;94:343.
PRINCIPAL DISPLAY PANEL - 10 g Carton
NDC 0069-2599-99
Rx only
VANCOMYCIN
HYDROCHLORIDE
FOR INJECTION, USP
(Formerly: Sterile Vancomycin
Hydrochloride)
PHARMACY BULK PACKAGE
NOT FOR DIRECT INFUSION
10 grams* per
Pharmacy Bulk Package
Sterile
LYOPHILIZED
For IV Infusion After Dilution
AFTER RECONSTITUTION MUST BE FURTHER
DILUTED. NOT TO BE DISPENSED AS A UNIT.
One Pharmacy Bulk Package bottle
Pfizer Injectables

| VANCOMYCIN HYDROCHLORIDE
vancomycin hydrochloride injection, powder, lyophilized, for solution |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| ANDA | ANDA091469 | 05/10/2011 | |
| Labeler - Pfizer Laboratories Div Pfizer Inc (134489525) |
| Establishment | |||
| Name | Address | ID/FEI | Operations |
| Strides Arcolab Limited SPD | 676199117 | ANALYSIS, MANUFACTURE | |
Revised: 07/2011 Pfizer Laboratories Div Pfizer Inc
