testosterone enanthate (Testosterone Enanthate) injection, solution
[Paddock Laboratories, Inc]
CIII
Multiple Dose Vial
DESCRIPTION
Testosterone enanthate injection, USP provides testosterone enanthate, a derivative of the primary endogenous androgen testosterone, for intramuscular administration. In their active form, androgens have a 17-beta-hydroxy group. Esterification of the 17-beta-hydroxy group increases the duration of action of testosterone; hydrolysis to free testosterone occurs in vivo. Each mL of sterile, colorless to pale yellow solution provides 200 mg testosterone enanthate in sesame oil with 5 mg chlorobutanol (chloral derivative) as a preservative.
Testosterone enanthate is designated chemically as androst-4-en-3-one, 17-[(1-oxoheptyl)-oxy]-, (17β)-. Structural formula:
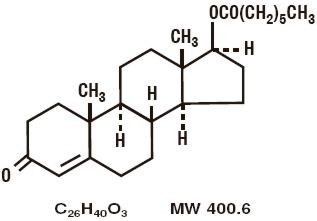
CLINICAL PHARMACOLOGY
Endogenous androgens are responsible for the normal growth and development of the male sex organs and for maintenance of secondary sex characteristics. These effects include growth and maturation of prostate, seminal vesicles, penis, and scrotum; development of male hair distribution, such as beard, pubic, chest, and axillary hair; laryngeal enlargement; vocal chord thickening; alterations in body musculature; and fat distribution.
Androgens also cause retention of nitrogen, sodium, potassium, and phosphorus, and decreased urinary excretion of calcium. Androgens have been reported to increase protein anabolism and decrease protein catabolism. Nitrogen balance is improved only when there is sufficient intake of calories and protein.
Androgens are responsible for the growth spurt of adolescence and for the eventual termination of linear growth which is brought about by fusion of the epiphyseal growth centers. In children, exogenous androgens accelerate linear growth rates but may cause a disproportionate advancement in bone maturation. Use over long periods may result in fusion of the epiphyseal growth centers and termination of the growth process. Androgens have been reported to stimulate the production of red blood cells by enhancing the production of erythropoietic stimulating factor.
During exogenous administration of androgens, endogenous testosterone release is inhibited through feedback inhibition of pituitary luteinizing hormone (LH). At large doses of exogenous androgens, spermatogenesis may also be suppressed through feedback inhibition of pituitary follicle stimulating hormone (FSH).
There is a lack of substantial evidence that androgens are effective in fractures, surgery, convalescence, and functional uterine bleeding.
PHARMACOKINETICS
Testosterone esters are less polar than free testosterone. Testosterone esters in oil injected intramuscularly are absorbed slowly from the lipid phase; thus testosterone enanthate can be given at intervals of two to four weeks.
Testosterone in plasma is 98 percent bound to a specific testosterone-estradiol binding globulin, and about two percent is free. Generally, the amount of this sex-hormone binding globulin (SHBG) in the plasma will determine the distribution of testosterone between free and bound forms, and the free testosterone concentration will determine its half-life.
About 90 percent of a dose of testosterone is excreted in the urine as glucuronic and sulfuric acid conjugates of testosterone and its metabolites; about six percent of a dose is excreted in the feces, mostly in the unconjugated form. Inactivation of testosterone occurs primarily in the liver. Testosterone is metabolized to various 17-keto steroids through two different pathways. There are considerable variations of the half-life of testosterone as reported in the literature, ranging from 10 to 100 minutes.
In responsive tissues, the activity of testosterone appears to depend on reduction to dihydrotestosterone (DHT), which binds to cytosol receptor proteins. The steroid-receptor complex is transported to the nucleus where it initiates transcription events and cellular changes related to androgen action.
INDICATIONS AND USAGE
Males
Testosterone enanthate injection, USP is indicated for replacement therapy in conditions associated with a deficiency or absence of endogenous testosterone.
Primary hypogonadism (congenital or acquired) - Testicular failure due to cryptorchidism, bilateral torsion, orchitis, vanishing testis syndrome, or orchidectomy.
Hypogonadotropic hypogonadism (congenital or acquired) - Idiopathic gonadotropin or luteinizing hormone-releasing hormone (LHRH) deficiency, or pituitary-hypothalamic injury from tumors, trauma, or radiation. (Appropriate adrenal cortical and thyroid hormone replacement therapy are still necessary, however, and are actually of primary importance.)
If the above conditions occur prior to puberty, androgen replacement therapy will be needed during the adolescent years for development of secondary sexual characteristics. Prolonged androgen treatment will be required to maintain sexual characteristics in these and other males who develop testosterone deficiency after puberty.
Delayed puberty - Testosterone enanthate injection, USP may be used to stimulate puberty in carefully selected males with clearly delayed puberty. These patients usually have a familial pattern of delayed puberty that is not secondary to a pathological disorder; puberty is expected to occur spontaneously at a relatively late date. Brief treatment with conservative doses may occasionally be justified in these patients if they do not respond to psychological support. The potential adverse effect on bone maturation should be discussed with the patient and parents prior to androgen administration. An X-ray of the hand and wrist to determine bone age should be obtained every six months to assess the effect of treatment on the epiphyseal centers (see WARNINGS).
Females
Metastatic mammary cancer - Testosterone enanthate injection, USP may be used secondarily in women with advancing inoperable metastatic (skeletal) mammary cancer who are one to five years postmenopausal. Primary goals of therapy in these women include ablation of the ovaries. Other methods of counteracting estrogen activity are adrenalectomy, hypophysectomy, and/or antiestrogen therapy. This treatment has also been used in premenopausal women with breast cancer who have benefited from oophorectomy and are considered to have a hormone-responsive tumor. Judgment concerning androgen therapy should be made by an oncologist with expertise in this field.
CONTRAINDICATIONS
Androgens are contraindicated in men with carcinomas of the breast or with known or suspected carcinomas of the prostate and in women who are or may become pregnant. When administered to pregnant women, androgens cause virilization of the external genitalia of the female fetus. This virilization includes clitoromegaly, abnormal vaginal development and fusion of genital folds to form a scrotal-like structure. The degree of masculinization is related to the amount of drug given and the age of the fetus and is most likely to occur in the female fetus when the drugs are given in the first trimester. If the patient becomes pregnant while taking androgens, she should be apprised of the potential hazard to the fetus.
This preparation is also contraindicated in patients with a history of hypersensitivity to any of its components.
WARNINGS
In patients with breast cancer and in immobilized patients, androgen therapy may cause hypercalcemia by stimulating osteolysis. In patients with cancer, hypercalcemia may indicate progression of bony metastasis. If hypercalcemia occurs, the drug should be discontinued and appropriate measures instituted.
Prolonged use of high doses of androgens has been associated with the development of peliosis hepatis and hepatic neoplasms including hepatocellular carcinoma (see PRECAUTIONS, Carcinogenesis). Peliosis hepatis can be a life-threatening or fatal complication.
If cholestatic hepatitis with jaundice appears or if liver function tests become abnormal, the androgen should be discontinued and the etiology should be determined. Drug-induced jaundice is reversible when the medication is discontinued.
Geriatric patients treated with androgens may be at an increased risk for the development of prostatic hypertrophy and prostatic carcinoma.
Due to sodium and water retention, edema with or without congestive heart failure may be a serious complication in patients with preexisting cardiac, renal, or hepatic disease. In addition to discontinuation of the drug, diuretic therapy may be required. If the administration of testosterone enanthate is restarted, a lower dose should be used.
Gynecomastia frequently develops and occasionally persists in patients being treated for hypogonadism.
Androgen therapy should be used cautiously in healthy males with delayed puberty. The effect on bone maturation should be monitored by assessing bone age of the wrist and hand every six months. In children, androgen treatment may accelerate bone maturation without producing compensatory gain in linear growth. This adverse effect may result in compromised adult stature. The younger the child the greater the risk of compromising final mature height.
PRECAUTIONS
General
Women should be observed for signs of virilization (deepening of the voice, hirsutism, acne, clitoromegaly, and menstrual irregularities). Discontinuation of drug therapy at the time of evidence of mild virilism is necessary to prevent irreversible virilization. Such virilization is usual following androgen use at high doses and is not prevented by concomitant use of estrogens. A decision may be made by the patient and the physician that some virilization will be tolerated during treatment for breast carcinoma.
Because androgens may alter serum cholesterol concentration, caution should be used when administering these drugs to patients with a history of myocardial infarction or coronary artery disease. Serial determinations of serum cholesterol should be made and therapy adjusted accordingly. A causal relationship between myocardial infarction and hypercholesterolemia has not been established.
Information for Patients
Male adolescent patients receiving androgens for delayed puberty should have bone development checked every six months.
The physician should instruct patients to report any of the following side effects of androgens:
Adult or adolescent males - too frequent or persistent erections of the penis.
Women - hoarseness, acne, changes in menstrual periods, or more facial hair.
All patients - any nausea, vomiting, changes in skin color, or ankle swelling.
Geriatric Use
Clinical studies of testosterone enanthate injection, USP did not include sufficient numbers of subjects, aged 65 and older, to determine whether they respond differently from younger subjects. Testosterone replacement is not indicated in geriatric patients who have age-related hypogonadism only ("andropause"), because there is insufficient safety and efficacy information to support such use. Current studies do not assess whether testosterone use increases risks of prostate cancer, prostate hyperplasia, and cardiovascular disease in the geriatric population.
Laboratory Tests
Women with disseminated breast carcinoma should have frequent determination of urine and serum calcium levels during the course of androgen therapy (see WARNINGS).
Periodic (every six months) X-ray examinations of bone age should be made during treatment of prepubertal males to determine the rate of bone maturation and the effects of androgen therapy on the epiphyseal centers.
Hemoglobin and hematocrit should be checked periodically for polycythemia in patients who are receiving high doses of androgens.
Drug Interactions
When administered concurrently, the following drugs may interact with androgens:
Anticoagulants, oral - C-17 substituted derivatives of testosterone, such as methandrostenolone, have been reported to decrease the anticoagulant requirement. Patients receiving oral anticoagulant therapy require close monitoring especially when androgens are started or stopped.
Antidiabetic drugs and insulin - In diabetic patients, the metabolic effects of androgens may decrease blood glucose and insulin requirements.
ACTH and corticosteroids - Enhanced tendency toward edema. Use caution when giving these drugs together, especially in patients with hepatic or cardiac disease.
Oxphenbutazone - Elevated serum levels of oxyphenbutazone may result.
Drug/Laboratory Test Interferences
Androgens may decrease levels of thyroxine-binding globulin, resulting in decreased total T4 serum levels and increased resin uptake of T3 and T4. Free thyroid hormone levels remain unchanged, however, and there is no clinical evidence of thyroid dysfunction.
Carcinogenesis
Testosterone has been tested by subcutaneous injection and implantation in mice and rats. The implant induced cervical-uterine tumors in mice, which metastasized in some cases. There is suggestive evidence that injection of testosterone into some strains of female mice increases their susceptibility to hepatoma. Testosterone is also known to increase the number of tumors and decrease the degree of differentiation of chemically induced carcinomas of the liver in rats.
There are rare reports of hepatocellular carcinoma in patients receiving long-term therapy with androgens in high doses. Withdrawal of the drugs did not lead to regression of the tumors in all cases.
Geriatric patients treated with androgens may be at an increased risk for the development of prostatic hypertrophy and prostatic carcinoma.
Pregnancy:
Teratogenic Effects
Category X (see CONTRAINDICATIONS).
Nursing Mothers
It is not known whether androgens are excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from androgens, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
Androgen therapy should be used very cautiously in pediatric patients and only by specialists who are aware of the adverse effects on bone maturation. Skeletal maturation must be monitored every six months by an X-ray of the hand and wrist (see INDICATIONS AND USAGE, and WARNINGS).
ADVERSE REACTIONS
Endocrine and Urogenital, Female - The most common side effects of androgen therapy are amenorrhea and other menstrual irregularities, inhibition of gonadotropin secretion, and virilization, including deepening of the voice and clitoral enlargement. The latter usually is not reversible after androgens are discontinued. When administered to a pregnant woman, androgens cause virilization of the external genitalia of the female fetus. Male - Gynecomastia, and excessive frequency and duration of penile erections. Oligospermia may occur at high dosages (see CLINICAL PHARMACOLOGY).
Skin and Appendages - Hirsutism, male pattern baldness, and acne.
Fluid and Electrolyte Disturbances - Retention of sodium, chloride, water, potassium, calcium (see WARNINGS), and inorganic phosphates.
Gastrointestinal - Nausea, cholestatic jaundice, alterations in liver function tests; rarely, hepatocellular neoplasms, peliosis hepatis (see WARNINGS).
Hematologic - Suppression of clotting factors II, V, VII, and X; bleeding in patients on concomitant anticoagulant therapy; polycythemia.
Nervous System - Increased or decreased libido, headache, anxiety, depression, and generalized paresthesia.
Metabolic - Increased serum cholesterol.
Miscellaneous - Rarely, anaphylactoid reactions; inflammation and pain at injection site.
DRUG ABUSE AND DEPENDENCE
Testosterone enanthate injection, USP is classified as a controlled substance under the Anabolic Steroids Control Act of 1990 and has been assigned to Schedule III.
OVERDOSAGE
There have been no reports of acute overdosage with androgens.
DOSAGE AND ADMINISTRATION
Dosage and duration of therapy with testosterone enanthate injection, USP will depend on age, sex, diagnosis, patient's response to treatment, and appearance of adverse effects. When properly given, injections of testosterone enanthate injection, USP are well tolerated. Care should be taken to inject the preparation deeply into the gluteal muscle following the usual precautions for intramuscular administration. In general, total doses above 400 mg per month are not required because of the prolonged action of the preparation. Injections more frequently than every two weeks are rarely indicated. NOTE: Use of a wet needle or wet syringe may cause the solution to become cloudy; however this does not affect the potency of the material. Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. Testosterone enanthate injection, USP is a clear, colorless to pale yellow solution.
Male hypogonadism:
As replacement therapy, i.e., for eunuchism, the suggested dosage is 50 to 400 mg every 2 to 4 weeks.
In males with delayed puberty:
Various dosage regimens have been used; some call for lower dosages initially with gradual increases as puberty progresses, with or without a decrease to maintenance levels. Other regimens call for higher dosage to induce pubertal changes and lower dosage for maintenance after puberty. The chronological and skeletal ages must be taken into consideration, both in determining the initial dose and in adjusting the dose. Dosage is within the range of 50 to 200 mg every 2 to 4 weeks for a limited duration, for example, 4 to 6 months. X-rays should be taken at appropriate intervals to determine the amount of bone maturation and skeletal development (see INDICATIONS AND USAGE, and WARNINGS).
Palliation of inoperable mammary cancer in women:
A dosage of 200 to 400 mg every 2 to 4 weeks is recommended. Women with metastatic breast carcinoma must be followed closely because androgen therapy occasionally appears to accelerate the disease.
HOW SUPPLIED
Testosterone enanthate injection, USP is available in 5 mL (200 mg/mL) multiple dose vials.
NDC 0574-0821-05
STORAGE
Testosterone enanthate injection, USP should be stored at controlled room temperature 20°C to 25°C (68°F to 77°F) [see USP].
Warming and rotating the vial between the palms of the hands will redissolve any crystals that may have formed during storage at low temperatures.
For Prescription Use Only
Manufactured by:
PharmaForce, Inc.
Hilliard, OH 43026
Manufactured for:
Paddock Laboratories, Inc.
Minneapolis, MN 55427
March 2007
| Testosterone Enanthate (Testosterone Enanthate) | ||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
Revised: 08/2007Paddock Laboratories, Inc