lialda (mesalamine) tablet, delayed release
[Shire US Inc.]
DESCRIPTION
Each LIALDA delayed release tablet for oral administration contains 1.2g 5-aminosalicylic acid (5-ASA; mesalamine), an anti-inflammatory agent. Mesalamine also has the chemical name 5-amino-2-hydroxybenzoic acid and its structural formula is:
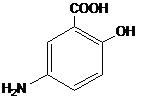
Molecular formula: C7H7NO3Molecular weight: 153.14
The tablet is coated with a gastro-resistant pH dependent polymer film, which breaks down at or above pH 7, normally in the terminal ileum where mesalamine then begins to be released from the tablet core. The tablet core contains mesalamine with hydrophilic and lipophilic excipients.
The inactive ingredients of LIALDA tablets are sodium carboxymethylcellulose, carnauba wax, stearic acid, silica (colloidal hydrated), sodium starch glycolate (type A), talc, magnesium stearate, methacrylic acid copolymer types A and B, triethylcitrate, titanium dioxide, red ferric oxide and polyethyleneglycol 6000.
CLINICAL PHARMACOLOGY
The mechanism of action of mesalamine is not fully understood, but appears to be topical. Mucosal production of arachidonic acid metabolites, both through the cyclooxygenase and lipoxygenase pathways, is increased in patients with chronic inflammatory bowel disease, and it is possible that mesalamine diminishes inflammation by blocking cyclooxygenase and inhibiting prostaglandin production in the colon. Recent data also suggest that mesalamine can inhibit the activation of NFkB, a nuclear transcription factor that regulates the transcription of many genes for pro-inflammatory proteins.
Pharmacokinetics
Absorption: The total absorption of mesalamine from LIALDA 2.4g or 4.8g given once daily for 14 days to healthy volunteers was found to be approximately 21-22% of the administered dose.
Gamma-scintigraphy studies have shown that a single dose of LIALDA 1.2g (one tablet) passed intact through the upper gastrointestinal tract of fasted healthy volunteers. Scintigraphic images showed a trail of radio-labeled tracer in the colon, suggesting that mesalamine had distributed throughout this region of the gastrointestinal tract.
In a single dose study, LIALDA 1.2g, 2.4g and 4.8g were administered in the fasted state to healthy subjects. Plasma concentrations of mesalamine were detectable after 2 hours and reached a maximum by 9-12 hours on average for the doses studied. The pharmacokinetic parameters are highly variable among subjects (Table 1). Mesalamine systemic exposure in terms of area under the plasma concentration-time curve (AUC) was slightly more than dose proportional between 1.2g and 4.8g LIALDA. Maximum plasma concentrations (Cmax) of mesalamine increased approximately dose proportionately between 1.2g and 2.4g and sub-proportionately between 2.4g and 4.8g LIALDA, with the dose normalized value at 4.8g representing, on average, 74% of that at 2.4g based on geometric means.
| Parameter1 of Mesalamine | LIALDA 1.2g
(N=47) | LIALDA 2.4g
(N=48) | LIALDA 4.8g
(N=48) |
|---|---|---|---|
| AUC0-t (ng.h/mL) | 9039+ (5054) | 20538 (12980) | 41434 (26640) |
| AUC0-∞ (ng.h/mL) | 9578*** (5214) | 21084 (13185) | 44775# (30302) |
| Cmax (ng/mL) | 857 (638) | 1595 (1484) | 2154 (1140) |
| Tmax* (h) | 9.0**(4.0-32.1) | 12.0 (4.0-34.1) | 12.0 (4.0-34.0) |
| Tlag* (h) | 2.0** (0-8.0) | 2.0 (1.0-4.0) | 2.0 (1.0-4.0) |
| T1/2 (h) (Terminal Phase) | 8.56 (6.38) | 7.05§ (5.54) | 7.25# (8.32) |
| 1 Arithmetic mean of parameter values are presented except for Tmax and Tlag. * Median (min, max); +N=43, ***N=27, §N=33, #N=36, **N=46 |
|||
Administration of a single dose of LIALDA 4.8g with a high fat meal resulted in further delay in absorption and plasma concentrations of mesalamine were detectable 4 hours following dosing. However, high fat meal increased systemic exposure of mesalamine (mean Cmax increased 91%; mean AUC increased 16%) compared to results in the fasted state. LIALDA was administered with food in the Phase 3 trials.
In a single and multiple dose pharmacokinetic study of LIALDA 2.4g or 4.8g was administered once daily with standard meals to 28 healthy volunteers per dose group. Plasma concentrations of mesalamine were detectable after 4 hours and were maximal by 8 hours after the single dose. Steady state was achieved generally by 2 days after dosing. Mean AUC at steady state was only modestly greater (1.1- to 1.4-fold) than predictable from single dose pharmacokinetics.
Distribution: Mesalamine is approximately 43% bound to plasma proteins at the concentration of 2.5 μg/mL.
Metabolism: The major metabolite of mesalamine (5-aminosalicylic acid) is N-acetyl-5-aminosalicylic acid. Its formation is brought about by N-acetyltransferase activity in the liver and intestinal mucosa.
Elimination: Elimination of mesalamine is mainly via the renal route following metabolism to N-acetyl-5-aminosalicylic acid (acetylation). However, there is also limited excretion of the parent drug in urine. Of the approximately 21-22% of the dose absorbed, less than 8% of the dose was excreted unchanged in the urine, compared with greater than 13% for N-acetyl-5-aminosalicylic acid. The apparent terminal half-lives for mesalamine and its major metabolite after administration of LIALDA 2.4g and 4.8g were, on average, 7-9 hours and 8-12 hours, respectively.
Special Populations
Geriatrics: No pharmacokinetic information is available in patients who are 65 years or older ( see PRECAUTIONS).
Pediatrics: No pharmacokinetic information is available in patients who are less than 18 years of age ( see PRECAUTIONS).
Gender: No consistent trend on gender effect was observed in the clinical trials.
Renal Insufficiency: No information is available in patients with mild, moderate, and severe renal impairment ( see PRECAUTIONS).
Hepatic Insufficiency: No information is available for patients with hepatic impairment ( see PRECAUTIONS).
Race: No pharmacokinetic information is available which examines LIALDA in different races.
Drug-Drug Interaction
There are no data available on interactions between LIALDA and other drugs. However, there have been reports of interaction between other mesalamine medications and other drugs ( see PRECAUTIONS).
CLINICAL TRIALS
Active, Mild to Moderate Ulcerative Colitis
Two similarly designed, randomized, double blind, placebo-controlled trials were conducted in 517 adult patients with active, mild to moderate ulcerative colitis. The study population was primarily Caucasian (80%), had a mean age of 42 years (6% age 65 years or older), and was approximately 50% male. Both studies used LIALDA doses of 2.4g/day and 4.8g/day administered once daily for 8 weeks except for the 2.4g/day group in Study 1, which was given in two divided doses (1.2g BID). The primary efficacy end-point in both trials was to compare the percentage of patients in remission after 8 weeks of treatment for the LIALDA treatment groups vs placebo. Remission was defined as an Ulcerative Colitis Disease Activity Index (UC-DAI) of ≤ 1, with scores of zero for rectal bleeding and for stool frequency, and a sigmoidoscopy score reduction of 1 point or more from baseline.
In both studies, the LIALDA doses of 2.4g/day and 4.8g/day demonstrated superiority over placebo in the primary efficacy endpoint (Table 2). Both LIALDA doses also provided consistent benefit in secondary efficacy parameters, including clinical improvement, treatment failure, clinical remission, and sigmoidoscopic improvement. LIALDA 2.4g/day and 4.8g/day had similar efficacy profiles.
| Dose | Study 1 | Study 2 |
|---|---|---|
| (n=262) | (n=255) | |
| n/N (%) | n/N (%) | |
| LIALDA 2.4g/day | 30/88 (34.1) | 34/84 (40.5) |
| LIALDA 4.8g/day | 26/89 (29.2) | 35/85 (41.2) |
| Placebo | 11/85 (12.9) | 19/86 (22.1) |
INDICATIONS AND USAGE
LIALDA tablets are indicated for the induction of remission in patients with active, mild to moderate ulcerative colitis. Safety and effectiveness of LIALDA beyond 8 weeks has not been established.
CONTRAINDICATIONS
LIALDA is contraindicated in patients with hypersensitivity to salicylates (including mesalamine) or to any of the components of LIALDA.
PRECAUTIONS
General:
Patients with pyloric stenosis may have prolonged gastric retention of LIALDA, which could delay mesalamine release in the colon.
The majority of patients who are intolerant or hypersensitive to sulfasalazine can take mesalamine medications without risk of similar reactions. However, caution should be exercised when treating patients allergic to sulfasalazine.
Mesalamine has been associated with an acute intolerance syndrome that may be difficult to distinguish from a flare of inflammatory bowel disease. Although the exact frequency of occurrence has not been determined, it has occurred in 3% of patients in controlled clinical trials of mesalamine or sulfasalazine. Symptoms include cramping, acute abdominal pain and bloody diarrhea, sometimes fever, headache and rash. If acute intolerance syndrome is suspected, prompt withdrawal is required.
Mesalamine-induced cardiac hypersensitivity reactions (myocarditis and pericarditis) have been reported with other mesalamine medications. Caution should be taken in prescribing this medication to patients with conditions predisposing to the development of myocarditis or pericarditis.
Renal:
Reports of renal impairment, including minimal change nephropathy, and acute or chronic interstitial nephritis have been associated with mesalamine medications and pro-drugs of mesalamine. For any patient with known renal dysfunction, caution should be exercised and LIALDA should be used only if the benefits outweigh the risks. It is recommended that all patients have an evaluation of renal function prior to initiation of therapy and periodically while on treatment. In animal studies with mesalamine, a 13-week oral toxicity study in mice and 13-week and 52-week oral toxicity studies in rats and cynomolgus monkeys have shown the kidney to be the major target organ of mesalamine toxicity. Oral daily doses of 2400 mg/kg in mice and 1150 mg/kg in rats produced renal lesions including granular and hyaline casts, tubular degeneration, tubular dilation, renal infarct, papillary necrosis, tubular necrosis, and interstitial nephritis. In cynomolgus monkeys, oral daily doses of 250 mg/kg or higher produced nephrosis, papillary edema, and interstitial fibrosis.
Hepatic Impairment:
No information is available on patients with hepatic impairment, and therefore, caution is recommended in these patients.
Information for Patients:
Patients should be instructed to swallow LIALDA tablets whole, taking care not to break the outer coating. The outer coating is designed to remain intact to protect the active ingredient, mesalamine, and ensure its availability throughout the colon.
Drug Interaction:
No investigations have been performed between LIALDA and other drugs. However, the following are reports of interactions between mesalamine medications and other drugs. The concurrent use of mesalamine with known nephrotoxic agents, including non-steroidal anti-inflammatory drugs (NSAIDs) may increase the risk of renal reactions. In patients receiving azathioprine or 6-mercaptopurine, concurrent use of mesalamine can increase the potential for blood disorders.
Carcinogenesis, Mutagenesis, Impairment of Fertility:
In a 104-week dietary carcinogenicity study in CD-1 mice, mesalamine at doses up to 2500 mg/kg/day was not tumorigenic. This dose is 2.2 times the maximum recommended human dose (based on a body surface area comparison) of LIALDA. Furthermore, in a 104-week dietary carcinogenicity study in Wistar rats, mesalamine up to a dose of 800 mg/kg/day was not tumorigenic. This dose is 1.4 times the recommended human dose (based on a body surface area comparison) of LIALDA.
No evidence of mutagenicity was observed in an in vitro Ames test or an in vivo mouse micronucleus test.
No effects on fertility or reproductive performance were observed in male or female rats at oral doses of mesalamine up to 400 mg/kg/day (0.7 times the maximum recommended human dose based on a body surface area comparison). Semen abnormalities and infertility in men, which have been reported in association with sulfasalazine, have not been seen with other mesalamine products during controlled clinical trials.
Pregnancy:
Teratogenic Effects: Pregnancy Category B
Reproduction studies with mesalamine have been performed in rats at doses up to 1000 mg/kg/day (1.8 times the maximum recommended human dose based on a body surface area comparison) and rabbits at doses up to 800 mg/kg/day (2.9 times the maximum recommended human dose based on a body surface area comparison) and have revealed no evidence of impaired fertility or harm to the fetus due to mesalamine. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed. Mesalamine is known to cross the placental barrier.
Nursing Mothers:
Low concentrations of mesalamine and higher concentrations of its N-acetyl metabolite have been detected in human breast milk. While there is limited experience of lactating women using mesalamine, caution should be exercised if LIALDA is administered to a nursing mother, and used only if the benefits outweigh the risks.
Pediatric Use:
Safety and effectiveness of LIALDA tablets in pediatric patients who are less than 18 years of age have not been studied.
Geriatric Use:
Clinical trials of LIALDA did not include sufficient numbers of patients aged 65 and over to determine whether they respond differently from younger patients. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concurrent disease or other drug therapy.
ADVERSE REACTIONS
LIALDA tablets have been evaluated in 655 ulcerative colitis patients in controlled and open-label trials.
In two 8-week placebo-controlled clinical trials involving 535 ulcerative colitis patients, 356 received 2.4g/day or 4.8g/day LIALDA tablets and 179 received placebo. More treatment emergent adverse events occurred in the placebo group (119) than in each of the LIALDA treatment groups (109 in 2.4g/day, 92 in 4.8g/day). A lower percentage of LIALDA patients discontinued therapy due to adverse events compared to placebo (2.2% vs 7.3%). The most frequent adverse event leading to discontinuation from LIALDA therapy was exacerbation of ulcerative colitis (0.8%).
The majority of adverse events in the double blind, placebo-controlled trials were mild or moderate in severity. The percentage of patients with severe adverse events was higher in the placebo group (6.1% in placebo; 1.1% in 2.4g/day; 2.2% in 4.8g/day). The most common severe adverse events were gastrointestinal disorders which were mainly symptoms associated with ulcerative colitis. Pancreatitis occurred in less than 1% of patients during clinical trials and resulted in discontinuation of therapy with LIALDA in patients experiencing this event.
Overall, the percentage of patients who experienced any adverse event was similar across treatment groups. Treatment related adverse events occurring in LIALDA or placebo groups at a frequency of at least 1% in two Phase 3, 8-week, double blind, placebo-controlled trials are listed in Table 3. The most common treatment related adverse events with LIALDA 2.4g/day and 4.8g/day were headache (5.6% and 3.4%, respectively) and flatulence (4% and 2.8%, respectively).
|
Event | LIALDA
2.4g/day (n = 177) | LIALDA
4.8g/day (n = 179) | Placebo
(n = 179) |
|---|---|---|---|
| Headache | 10 (5.6%) | 6 (3.4%) | 1 (0.6%) |
| Flatulence | 7 (4%) | 5 (2.8%) | 5 (2.8%) |
| Increased alanine aminotransferase | 1 (0.6%) | 2 (1.1%) | 0 |
| Alopecia | 0 | 2 (1.1%) | 0 |
| Pruritis | 1 (0.6%) | 2 (1.1%) | 0 |
The following treatment-related adverse events, presented by body system, were reported infrequently (less than 1%) by LIALDA-treated ulcerative colitis patients in controlled trials.
Cardiovascular and Vascular: tachycardia, hypertension, hypotension
Dermatological: acne, prurigo, rash, urticaria
Gastrointestinal Disorders: abdominal distention, diarrhea, pancreatitis, rectal polyp, vomiting
Hematologic: decreased platelet count
Hepatobiliary Disorders: elevated total bilirubin
Musculoskeletal and Connective Tissue Disorders: arthralgia, back pain
Nervous System Disorders: somnolence, tremor
Respiratory, Thoracic and Mediastinal Disorders: pharyngolaryngeal pain
General Disorders and Administrative Site Disorders: asthenia, face edema, fatigue, pyrexia
Special Senses: ear pain
DRUG ABUSE AND DEPENDENCY
Abuse:
None reported.
Dependency:
Drug dependence has not been reported with chronic administration of mesalamine.
OVERDOSAGE
There have been no reports of overdosage with LIALDA. LIALDA is an aminosalicylate, and symptoms of salicylate toxicity may include tinnitus, vertigo, headache, confusion, drowsiness, sweating, hyperventilation, vomiting, and diarrhea. Severe intoxication may lead to disruption of electrolyte balance and blood-pH, hyperthermia, and dehydration.
Although there has been no direct experience with LIALDA, conventional therapy for salicylate toxicity may be beneficial in the event of acute overdosage. This includes prevention of further gastrointestinal tract absorption by emesis and, if necessary, by gastric lavage. Fluid and electrolyte imbalance should be corrected by the administration of appropriate intravenous therapy. Adequate renal function should be maintained.
DOSAGE AND ADMINISTRATION
The recommended dosage for the induction of remission in adult patients with active, mild to moderate ulcerative colitis is two to four 1.2g tablets to be taken once daily with meal for a total daily dose of 2.4g or 4.8g. Treatment duration in controlled clinical trials was up to 8 weeks.
HOW SUPPLIED
LIALDA tablets are available as red-brown ellipsoidal film coated tablets containing 1.2g mesalamine, and debossed on one side with S476.
NDC 54092-476-12 Bottle of 120 tablets
Store at room temperature 15°C to 25°C (59°F to 77°F); excursions permitted to 30°C (86°F). See USP Controlled Room Temperature.
Manufactured for Shire US Inc., 725 Chesterbrook Blvd., Wayne, PA 19087, USA. 476 1207 002B
© 2007 Shire US Inc. N7600A
U.S. Patent No. 6,773,720. by license of Giuliani S.p.A., Milan, Italy. Rev. 1/07
| LIALDA (mesalamine) | ||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||
Revised: 02/2007