MEDROXYPROGESTERONE ACETATE
-
medroxyprogesterone acetate tablet
Rebel Distributors Corp.
----------
MEDROXYPROGESTERONE ACETATE TABLETS, USPRx only
WARNINGS
CARDIOVASCULAR AND OTHER RISKS
Estrogens with progestins should not be used for the prevention of cardiovascular disease or dementia. (See CLINICAL STUDIES and WARNINGS, Cardiovascular Disorders and Dementia.)
The Women’s Health Initiative (WHI) estrogen plus progestin substudy reported increased risks of myocardial infarction, stroke, invasive breast cancer, pulmonary emboli, and deep vein thrombosis (DVT) in postmenopausal women (50 to 79 years of age) during 5.6 years of treatment with daily oral conjugated estrogens (CE 0.625 mg) combined with medroxyprogesterone acetate (MPA 2.5 mg) relative to placebo. (See CLINICAL STUDIES and WARNINGS, Cardiovascular Disorders and Malignant Neoplasms, Breast Cancer.)
The Women’s Health Initiative Memory Study (WHIMS), a substudy of the WHI study, reported increased risk of developing probable dementia in postmenopausal women 65 years of age or older during 4 years of treatment with daily CE 0.625 mg combined with MPA 2.5 mg, relative to placebo. It is unknown whether this finding applies to younger postmenopausal women. (See CLINICAL STUDIES and WARNINGS, Dementia, and PRECAUTIONS, Geriatric Use.)
In the absence of comparable data, these risks should be assumed to be similar for other doses of CE and MPA and other combinations and dosage forms of estrogens and progestins. Because of these risks, estrogens with or without progestins should be prescribed at the lowest effective doses and for the shortest duration consistent with treatment goals and risks for the individual woman.
DESCRIPTION
Medroxyprogesterone acetate tablets contain medroxyprogesterone acetate, which is a derivative of progesterone. It is a white to off-white, odorless crystalline powder, stable in air, melting between 200 and 210°C. It is freely soluble in chloroform, soluble in acetone and in dioxane, sparingly soluble in alcohol and in methanol, slightly soluble in ether, and insoluble in water.
The chemical name for medroxyprogesterone acetate is pregn-4-ene-3, 20-dione, 17-(acetyloxy)-6-methyl-, (6α)-. The structural formula is:
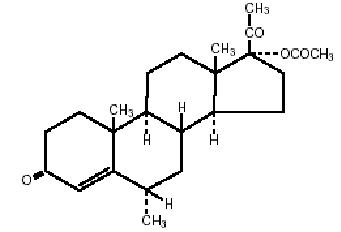
C24H34O4 Molecular Weight: 386.53
Each tablet, for oral administration, contains 2.5 mg, 5 mg or 10 mg of medroxyprogesterone acetate. In addition, each tablet contains the following inactive ingredients: crospovidone, lactose monohydrate, magnesium stearate, methylcellulose, pregelatinized starch, and sodium lauryl sulfate.
CLINICAL PHARMACOLOGY
Medroxyprogesterone acetate (MPA) administered orally or parenterally in the recommended doses to women with adequate endogenous estrogen, transforms proliferative into secretory endometrium. Androgenic and anabolic effects have been noted, but the drug is apparently devoid of significant estrogenic activity. While parenterally administered MPA inhibits gonadotropin production, which in turn prevents follicular maturation and ovulation, available data indicate that this does not occur when the usually recommended oral dosage is given as single daily doses.
Pharmacokinetics
The pharmacokinetics of MPA were determined in 20 postmenopausal women following a single-dose administration of eight medroxyprogesterone acetate 2.5 mg tablets or a single administration of two medroxyprogesterone acetate 10 mg tablets under fasting conditions. In another study, the steady-state pharmacokinetics of MPA were determined under fasting conditions in 30 postmenopausal women following daily administration of one medroxyprogesterone acetate 10 mg tablet for 7 days. In both studies, MPA was quantified in serum using a validated gas chromatography-mass spectrometry (GC-MS) method. Estimates of the pharmacokinetic parameters of MPA after single and multiple doses of medroxyprogesterone acetate tablets were highly variable and are summarized in Table 1.
|
|||||||
|
Tablet Strength |
Cmax (ng/mL) |
Tmax (h) |
Auc0-(∞) (ng·h/mL) |
t½ (h) |
Vd/f (L) |
CL/f (mL/min) |
|
| Single Dose | |||||||
| 2 x 10 mg | 1.01 (0.599) | 2.65 (1.41) | 6.95 (3.39) | 12.1 (3.49) |
78024 (47220) |
64110 (42662) |
|
| 8 x 2.5 mg | 0.805 (0.413) | 2.22 (1.39) | 5.62 (2.79) | 11.6 (2.81) |
62748 (40146) |
74123 (35126) |
|
| Multiple Dose | |||||||
| 10 mg* | 0.71 (0.35) | 2.83 (1.83) | 6.01 (3.16) | 16.6 (15) |
40564 (38256) |
41963 (38402) |
|
A. Absorption
No specific investigation on the absolute bioavailability of MPA in humans has been conducted. MPA is rapidly absorbed from the gastrointestinal tract, and maximum MPA concentrations are obtained between 2 to 4 hours after oral administration.
Administration of medroxyprogesterone acetate with food increases the bioavailability of MPA. A 10 mg dose of medroxyprogesterone acetate, taken immediately before or after a meal, increased MPA Cmax (50 to 70%) and AUC (18 to 33%). The half-life of MPA was not changed with food.
B. Distribution
MPA is approximately 90% protein bound, primarily to albumin; no MPA binding occurs with sex hormone binding globulin.
C. Metabolism
Following oral dosing, MPA is extensively metabolized in the liver via hydroxylation, with subsequent conjugation and elimination in the urine.
D. Excretion
Most MPA metabolites are excreted in the urine as glucuronide conjugates with only minor amounts excreted as sulfates.
E. Special Populations
Renal Insufficiency
The pharmacokinetics of MPA in patients with varying degrees of renal insufficiency have not been investigated.
Hepatic Insufficiency
MPA is almost exclusively eliminated via hepatic metabolism. In 14 patients with advanced liver disease, MPA disposition was significantly altered (reduced elimination). In patients with fatty liver, the mean percent dose excreted in the 24-hour urine as intact MPA after a 10 mg or 100 mg dose was 7.3% and 6.4%, respectively.
F. Drug Interactions
No formal pharmacokinetic drug interaction studies have been conducted with medroxyprogesterone acetate.
CLINICAL STUDIES
Effects on the Endometrium
In a 3-year, double-blind, placebo-controlled study of 356 nonhysterectomized, postmenopausal women between 45 and 64 years of age randomized to receive placebo (n=119), 0.625 mg conjugated estrogen only (n=119), or 0.625 mg conjugated estrogen plus cyclic medroxyprogesterone acetate (n=118), results showed a reduced risk of endometrial hyperplasia in the treatment group receiving 10 mg medroxyprogesterone acetate plus 0.625 mg conjugated estrogens compared to the group receiving 0.625 mg conjugated estrogens only. See Table 2.
| * Includes most extreme abnormal result | |||
|
Histological Results |
Placebo (n=119) |
CEE* (n=119) |
Medroxyprogesterone |
|
Normal/No hyperplasia (%) | 116 (97) | 45 (38) | 112 (95) |
|
Simple (cystic) hyperplasia (%) | 1 (1) | 33 (28) | 4 (3) |
|
Complex (adenomatous) hyperplasia (%) | 1 (1) | 27 (22) | 2 (2) |
| Atypia (%) | 0 | 14 (12) | 0 |
| Adenocarcinoma (%) | 1 (1) | 0 | 0 |
In a second 1-year study, 832 postmenopausal women between 45 and 65 years of age were treated with daily 0.625 mg conjugated estrogen (days 1-28), plus either 5 mg cyclic medroxyprogesterone acetate or 10 mg cyclic medroxyprogesterone acetate (days 15-28), or daily 0.625 mg conjugated estrogen only. The treatment groups receiving 5 or 10 mg cyclic medroxyprogesterone acetate (days 15-28) plus daily conjugated estrogens showed a significantly lower rate of hyperplasia as compared to the conjugated estrogens only group. See Table 3.
| CEE* | MPA† + CEE* | ||
|
(n=283) |
MPA 5 mg (n=277) |
MPA 10 mg (n=272) |
|
|
Cystic hyperplasia (%) | 55 (19) | 3 (1) | 0 |
|
Adenomatous hyperplasia without atypia | 2 (1) | 0 | 0 |
Women’s Health Initiative Studies
The Women’s Health Initiative (WHI) enrolled approximately 27,000 predominantly healthy postmenopausal women in two substudies to assess the risks and benefits of either the use of daily oral conjugated estrogens (CE 0.625 mg) alone or in combination with medroxyprogesterone acetate (MPA 2.5 mg) compared to placebo in the prevention of certain chronic diseases. The primary endpoint was the incidence of coronary heart disease (CHD) (nonfatal myocardial infarction (MI), silent MI and CHD death), with invasive breast cancer as the primary adverse outcome studied. A “global index” included the earliest occurrence of CHD, invasive breast cancer, stroke, pulmonary embolism (PE), endometrial cancer (only in the CE/MPA substudy), colorectal cancer, hip fracture, or death due to other cause. The study did not evaluate the effects of CE or CE/MPA on menopausal symptoms.
The estrogen plus progestin substudy was stopped early. According to the predefined stopping rule, after an average follow-up of 5.2 years of treatment, the increased risk of breast cancer and cardiovascular events exceeded the specified benefits included in the “global index.” The absolute excess risk of events included in the “global index” was 19 per 10,000 women-years (relative risk [RR] 1.15, 95 percent, nominal confidence interval [nCI], 1.03-1.28).
For those outcomes included in the WHI “global index,” that reached statistical significance after 5.6 years of follow-up, the absolute excess risks per 10,000 women-years in the group treated with CE/MPA were 6 more CHD events, 7 more strokes, 10 more PEs, and 8 more invasive breast cancers, while the absolute risk reduction per 10,000 women-years were 7 fewer colorectal cancers and 5 fewer hip fractures. (See BOXED WARNINGS, WARNINGS and PRECAUTIONS.)
Results of the CE/MPA substudy which included 16,608 women (average age of 63 years, range 50 to 79; 83.9 percent White, 6.8 percent Black, 5.4 percent Hispanic, 3.9 percent Other) are presented in Table 4. These results reflect centrally adjudicated data after an average follow-up of 5.6 years.
|
|||||
|
Event† |
Relative Risk CE/MPA vs placebo (95% nCI‡) |
|
|
||
| Absolute Risk per 10,000 Women-Years | |||||
| CHD events Non-fatal MI CHD death | 1.24 (1.00-1.54) 1.28 (1.00-1.63) 1.10 (0.70-1.75) | 33 25 8 | 39 31 8 |
||
| All strokes | 1.31 (1.02-1.68) | 24 | 31 | ||
| Ischemic stroke | 1.44 (1.09-1.90) | 18 | 26 | ||
| Deep vein thrombosis | 1.95 (1.43-2.67) | 13 | 26 | ||
| Pulmonary embolism | 2.13 (1.45-3.11) | 8 | 18 | ||
| Invasive breast cancer† | 1.24 (1.01-1.54) | 33 | 41 | ||
| Invasive colorectal cancer | 0.56 (0.38-0.81) | 16 | 9 | ||
| Endometrial cancer | 0.81 (0.48-1.36) | 7 | 6 | ||
| Cervical Cancer | 1.44 (0.47-4.42) | 1 | 2 | ||
| Hip fracture | 0.67 (0.47-0.96) | 16 | 11 | ||
| Vertebral fractures | 0.65 (0.46-0.92) | 17 | 11 | ||
| Lower arm/wrist fractures | 0.71 (0.59-0.85) | 62 | 44 | ||
| Total fractures | 0.76 (0.69-0.83) | 199 | 152 | ||
Women's Health Initiative Memory Study
The estrogen plus progestin Women’s Health Initiative Memory Study (WHIMS), a substudy of WHI, enrolled 4,532 predominantly healthy postmenopausal women 65 years of age and older (47 percent were aged 65 to 69 years, 35 percent were 70 to 74 years, and 18 percent were 75 years of age and older) to evaluate the effects of daily conjugated estrogens (CE 0.625 mg) plus medroxyprogesterone acetate (MPA 2.5 mg) on the incidence of probable dementia (primary outcome) compared with placebo.
After an average follow-up of 4 years, 40 women in the estrogen plus progestin group (45 per 10,000 women-years) and 21 in the placebo group (22 per 10,000 women-years) were diagnosed with probable dementia. The relative risk of probable dementia in the hormone therapy group was 2.05 (95 percent CI, 1.21-3.48) compared to placebo.
INDICATIONS AND USAGE
Medroxyprogesterone Acetate Tablets are a progestin indicated for the treatment of secondary amenorrhea and abnormal uterine bleeding due to hormonal imbalance in the absence of organic pathology, such as fibroids or uterine cancer. Medroxyprogesterone Acetate Tablets are also indicated to reduce the incidence of endometrial hyperplasia in nonhysterectomized postmenopausal women receiving daily oral conjugated estrogens 0.625 mg tablets.
CONTRAINDICATIONS
Medroxyprogesterone Acetate should not be used in women with any of the following conditions:
- Undiagnosed abnormal genital bleeding.
- Known, suspected, or history of cancer of the breast.
- Known or suspected estrogen- or progesterone-dependent neoplasia.
- Active deep vein thrombosis, pulmonary embolism or a history of these conditions.
- Active or recent (within the past year) arterial thromboembolic disease (for example, stroke and myocardial infarction).
- Known liver dysfunction or disease.
- Missed abortion.
- As a diagnostic test for pregnancy.
- Known hypersensitivity to the ingredients in medroxyprogesterone acetate tablets.
- Known or suspected pregnancy.
WARNINGS
See BOXED WARNINGS.
1. Cardiovascular Disorders.
An increased risk of stroke, deep vein thrombosis (DVT), pulmonary embolism, and myocardial infarction has been reported with estrogen plus progestin therapy. Should any of these events occur or be suspected, estrogen plus progestin therapy should be discontinued immediately.
Risk factors for arterial vascular disease (for example, hypertension, diabetes mellitus, tobacco use, hypercholesterolemia, and obesity) and/or venous thromboembolism (for example, personal history or family history of venous thromboembolism [VTE]), obesity, and systemic lupus erythematosus should be managed appropriately.
a. Stroke
In the estrogen plus progestin substudy of the Women’s Health Initiative (WHI) a statistically significant increased risk of stroke was reported in women receiving daily conjugated estrogens (CE 0.625 mg) plus medroxyprogesterone acetate (MPA 2.5 mg) compared to women receiving placebo (31 versus 24 per 10,000 women-years). The increase in risk was demonstrated after the first year and persisted. (See CLINICAL STUDIES.)
b. Coronary heart disease
In the estrogen plus progestin substudy of WHI, no statistically significant increase of CHD events (defined as non-fatal myocardial infarction [MI], silent MI or CHD death was reported in women receiving CE/MPA compared to women receiving placebo (39 versus 33 per 10,000 women-years). An increase in relative risk was demonstrated in year one, and a trend toward decreasing relative risk was reported in years 2 through 5. (See CLINICAL STUDIES.)
In postmenopausal women with documented heart disease (n = 2,763, average age 66.7 years), in a controlled clinical trial of secondary prevention of cardiovascular disease (Heart and Estrogen/Progestin Replacement Study [HERS]), treatment with daily CE 0.625 mg/ MPA 2.5 mg per day demonstrated no cardiovascular benefit. During an average follow-up of 4.1 years, treatment with CE/MPA did not reduce the overall rate of CHD events in postmenopausal women with established coronary heart disease. There were more CHD events in the CE/MPA-treated group than in the placebo group in year 1, but not during the subsequent years. Two thousand three hundred and twenty one (2,321) women from the original HERS trial agreed to participate in an open label extension of HERS, HERS II. Average follow-up in HERS II was an additional 2.7 years, for a total of 6.8 years overall. Rates of CHD events were comparable among women in the CE/MPA group and the placebo group in HERS, HERS II, and overall.
c. Venous thromboembolism (VTE)
In the estrogen plus progestin substudy of WHI, a statistically significant two-fold greater rate of VTE, (DVT and pulmonary embolism [PE]), was reported in women receiving daily CE/MPA compared to women receiving placebo (35 versus 17 per 10,000 women-years). Statistically significant increases in risk for both DVT (26 versus 13 per 10,000 women-years) and PE (18 versus 8 per 10,000 women-years) were also demonstrated. The increase in VTE risk was observed during the first year and persisted. (See CLINICAL STUDIES.)
2. Malignant Neoplasms
a. Breast cancer
The use of estrogens and progestins by postmenopausal women has been reported to increase the risk of breast cancer in some studies. Observational studies have also reported an increased risk of breast cancer for estrogen plus progestin therapy, and a smaller increased risk for estrogen alone therapy, after several years of use. The risk increased with duration of use and appeared to return to baseline in about 5 years after stopping treatment (only the observational studies have substantial data on risk after stopping). Observational studies also suggest that the risk of breast cancer was greater, and became apparent earlier, with estrogen plus progestin therapy as compared to estrogen alone therapy. However, these studies have not found significant variation in the risk of breast cancer among different estrogens or among different estrogen plus progestin combinations, doses, or routes of administration.
The most important randomized clinical trial providing information about this issue is the Women’s Health Initiative (WHI) substudy of daily conjugated estrogens (CE 0.625 mg) plus medroxyprogesterone acetate (MPA 2.5 mg) (See CLINICAL STUDIES.)
In the estrogen plus progestin substudy of WHI, after a mean follow-up of 5.6 years, the WHI substudy reported an increased risk of breast cancer in women who took daily CE/MPA. In this substudy, prior use of estrogen alone or estrogen plus progestin therapy was reported by 26 percent of the women. The relative risk of invasive breast cancer was 1.24 (95 percent nominal confidence interval [nCI], 1.01-1.54), and the absolute risk was 41 versus 33 cases per 10,000 women-years, for estrogen plus progestin compared with placebo, respectively. Among women who reported prior use of hormone therapy, the relative risk of invasive breast cancer was 1.86, and the absolute risk was 46 versus 25 cases per 10,000 women-years, for CE/MPA compared with placebo. Among women who reported no prior use of hormone therapy, the relative risk of invasive breast cancer was 1.09, and the absolute risk was 40 versus 36 cases per 10,000 women-years, for estrogen plus progestin compared with placebo. In the same substudy, invasive breast cancers were larger and diagnosed at a more advanced stage in the CE/MPA group compared with the placebo group. Metastatic disease was rare with no apparent difference between the two groups. Other prognostic factors such as histologic subtype, grade, and hormone receptor status did not differ between the groups.
The use of estrogen plus progestin has been reported to result in an increase in abnormal mammograms requiring further evaluation. All women should receive yearly breast examinations by a health care provider and perform monthly breast self-examinations. In addition, mammography examinations should be scheduled based on patient age, risk factors, and prior mammogram results.
b. Endometrial cancer
An increased risk of endometrial cancer has been reported with the use of unopposed estrogen therapy in women with a uterus. The reported endometrial cancer risk among unopposed estrogen users is about 2- to 12 times greater than in nonusers, and appears dependent on duration of treatment and on estrogen dose. Most studies show no significant increased risk associated with the use of estrogens for less than 1 year. The greatest risk appears associated with prolonged use, with increased risks of 15- to 24-fold for 5 to 10 years or more. This risk has been shown to persist for at least 8 to 15 years after estrogen therapy is discontinued.
Clinical surveillance of all women using estrogen plus progestin therapy is important. Adequate diagnostic measures, including endometrial sampling when indicated, should be undertaken to rule out malignancy in all cases of undiagnosed persistent or recurring abnormal vaginal bleeding. There is no evidence that the use of natural estrogens results in a different endometrial risk profile than synthetic estrogens of equivalent estrogen dose. Adding a progestin to estrogen therapy has been shown to reduce the risk of endometrial hyperplasia, which may be a precursor to endometrial cancer.
c. Ovarian cancer
The estrogen plus progestin substudy of WHI reported that daily CE/MPA increased the risk of ovarian cancer. After an average follow-up of 5.6 years, the relative risk for ovarian cancer for CE/MPA versus placebo was 1.58 (95 percent nCI, 0.77-3.24) but was not statistically significant. The absolute risk for CE/MPA was 4.2 versus 2.7 cases per 10,000 women-years.
3. Dementia
In the estrogen plus progestin Women’s Health Initiative Memory Study (WHIMS), a substudy of WHI, a population of 4,532 postmenopausal women aged 65 to 79 years was randomized to daily conjugated estrogens (CE 0.625 mg) plus medroxyprogesterone acetate (MPA 2.5 mg) or placebo.
After an average follow-up of 4 years, 40 women in the CE/MPA group and 21 women in the placebo group were diagnosed with probable dementia. The relative risk of probable dementia for CE/MPA versus placebo was 2.05 (95 percent CI, 1.21-3.48). The absolute risk of probable dementia for CE/MPA versus placebo was 45 versus 22 cases per 10,000 women-years. It is unknown whether these findings apply to younger postmenopausal women. (See BOXED WARNINGS and PRECAUTIONS, Geriatric Use.)
4. Visual Abnormalities
Discontinue medication pending examination if there is sudden partial or complete loss of vision, or a sudden onset of proptosis, diplopia or migraine. If examination reveals papilledema or retinal vascular lesions, medication should be permanently discontinued.
PRECAUTIONS
A. General
- Addition of a progestin when a woman has not had a hysterectomy
Studies of the addition of a progestin for 10 or more days of a cycle of estrogen administration, or daily with estrogen in a continuous regimen, have reported a lowered incidence of endometrial hyperplasia than would be induced by estrogen treatment alone. Endometrial hyperplasia may be a precursor to endometrial cancer.
There are, however, possible risks that may be associated with the use of progestins with estrogens compared to estrogen-alone regimens. These include a possible increased risk of breast cancer, adverse effects on lipoprotein metabolism (lowering HDL, raising LDL) and impairment of glucose tolerance. - Undiagnosed abnormal vaginal bleeding
In cases of undiagnosed abnormal vaginal bleeding, adequate diagnostic measures are indicated. - Elevated blood pressure
Blood pressure should be monitored at regular intervals with estrogen plus progestin therapy. - Hypertriglyceridemia
In patients with pre-existing hypertriglyceridemia, estrogen plus progestin therapy may be associated with elevations of plasma triglycerides leading to pancreatitis and other complications. - Impaired liver function and past history of cholestatic jaundice
Estrogens plus progestins may be poorly metabolized in patients with impaired liver function. For patients with a history of cholestatic jaundice associated with past estrogen use or with pregnancy, caution should be exercised, and in the case of recurrence, medication should be discontinued. - Fluid Retention
Progestins may cause some degree of fluid retention. Patients who have conditions which might be influenced by this factor, such as cardiac or renal dysfunction, warrant careful observation when estrogen plus progestin are prescribed. - Hypocalcemia
Estrogen plus progestin therapy should be used with caution in individuals with severe hypocalcemia. - Exacerbation of other conditions
Estrogen plus progestin therapy may cause an exacerbation of asthma, diabetes mellitus, epilepsy, migraine, porphyria, systemic lupus erythematosus, and hepatic hemangiomas and should be used with caution in women with these conditions.
B. Patient Information
Physicians are advised to discuss the Patient Information leaflet with patients for whom they prescribe medroxyprogesterone acetate.
There may be an increased risk of minor birth defects in children whose mothers are exposed to progestins during the first trimester of pregnancy. The possible risk to the male baby is hypospadias, a condition in which the opening of the penis is on the underside rather than the tip of the penis. This condition occurs naturally in approximately 5 to 8 per 1,000 male births. The risk may be increased with exposure to medroxyprogesterone acetate. Enlargement of the clitoris and fusion of the labia may occur in female babies. However, a clear association between hypospadias, clitoral enlargement and labial fusion with use of medroxyprogesterone acetate has not been established.
Inform the patient of the importance of reporting exposure to medroxyprogesterone acetate in early pregnancy.
C. Drug/Laboratory Test Interactions
The following laboratory results may be altered by the use of estrogen plus progestin therapy:
- Accelerated prothrombin time, partial thromboplastin time, and platelet aggregation time; increased platelet count; increased factors II, VII antigen, VIII antigen, VIII coagulant activity, IX, X, XII, VII-X complex, II-VII-X complex, and beta-thromboglobulin; decreased levels of anti-factor Xa and antithrombin III, decreased antithrombin III activity; increased levels of fibrinogen and fibrinogen activity; increased plasminogen antigen and activity.
- Increased thyroid-binding globulin (TBG) levels leading to increased circulating total thyroid hormone levels as measured by protein-bound iodine (PBI), T4 levels (by column or by radioimmunoassay) or T3 levels by radioimmunoassay, T3 resin uptake is decreased, reflecting the elevated TBG. Free T4 and free T3 concentrations are unaltered. Patients on thyroid replacement therapy may require higher doses of thyroid hormone.
- Other binding proteins may be elevated in serum (i.e., corticosteroid binding globulin (CBG), sex hormone binding globulin (SHBG) leading to increased circulating corticosteroid and sex steroids, respectively. Free or biologically active hormone concentrations are unchanged. Other plasma proteins may be increased (angiotensinogen/renin substrate, alpha-1-antitrypsin, ceruloplasmin).
- Increased plasma HDL and HDL2 cholesterol subfraction concentrations, reduced LDL cholesterol concentration, increased triglycerides levels.
- Impaired glucose metabolism.
D. Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term intramuscular administration of medroxyprogesterone acetate has been shown to produce mammary tumors in beagle dogs. There was no evidence of a carcinogenic effect associated with the oral administration of medroxyprogesterone acetate to rats and mice. Medroxyprogesterone acetate was not mutagenic in a battery of in vitro or in vivo genetic toxicity assays.
Medroxyprogesterone acetate at high doses is an antifertility drug and high doses would be expected to impair fertility until the cessation of treatment.
Long-term continuous administration of estrogen plus progestin therapy, has shown an increased risk of breast cancer and ovarian cancer. (See WARNINGS and PRECAUTIONS.)
E. Pregnancy
Pregnancy Category X
Medroxyprogesterone acetate should not be used during pregnancy. (See CONTRAINDICATIONS.)
There may be increased risks for hypospadias, clitoral enlargement and labial fusion in children whose mothers are exposed to medroxyprogesterone acetate during the first trimester of pregnancy. However, a clear association between these conditions with use of medroxyprogesterone acetate has not been established.
F. Nursing Mothers
Medroxyprogesterone acetate should not be used during lactation. Detectable amounts of progestin have been identified in the milk of nursing mothers receiving progestins.
G. Pediatric Use
Medroxyprogesterone acetate is not intended for pediatric use and no clinical data has been collected in children.
H. Geriatric Use
Of the total number of subjects in the estrogen plus progestin substudy of the Women’s Health Initiative (WHI), 44 percent (n = 7,320) were 65 years and older, while 6.6 percent (n = 1,095) were 75 years and older. In women 75 and older compared to women less than 75 years of age, there was a higher relative risk of non-fatal stroke and invasive breast cancer in the estrogen plus progestin group versus placebo. In women greater than 75 years of age, the increased risk of non-fatal stroke and invasive breast cancer observed in the estrogen plus progestin group compared to placebo was 75 versus 24 per 10,000 women-years and 52 versus 12 per 10,000 women-years, respectively.
In the estrogen plus progestin Women’s Health Initiative Memory Study (WHIMS), a substudy of WHI, a population of 4,532 postmenopausal women, aged 65 to 70 years, was randomized to receive daily CE 0.625 mg/MPA 2.5 mg or placebo. In the estrogen plus progestin group, after an average follow-up of 4 years, the relative risk (CE/MPA versus placebo) of probable dementia was 2.05 (95 percent CI, 1.21-3.48). The absolute risk of developing probable dementia with CE/MPA was 45 versus 22 cases per 10,000 women-years compared with placebo.
Eighty-two percent of the cases of probable dementia occurred in women that were older than 70 in the CE/MPA group. The most common classification of probable dementia in the estrogen plus progestin and placebo groups was Alzheimer’s disease.
When data from the estrogen alone and estrogen plus progestin WHIMS substudies were pooled as planned in the WHIMS protocol, the reported overall relative risk for probable dementia was 1.76 (95 percent CI, 1.19-2.60). Since both substudies were conducted in women aged 65 to 79 years, it is unknown whether these findings apply to younger postmenopausal women. (See BOXED WARNINGS and WARNINGS, Dementia.)
ADVERSE REACTIONS
See BOXED WARNINGS, WARNINGS, and PRECAUTIONS.
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The following adverse reactions have been reported in women taking progestins, including medroxyprogesterone acetate tablets, without concomitant estrogens treatment:
1. Genitourinary System
Abnormal uterine bleeding (irregular, increase, decrease), change in menstrual flow, breakthrough bleeding, spotting, amenorrhea, changes in cervical erosion and cervical secretions.
2. Breasts
Breast tenderness, mastodynia or galactorrhea has been reported.
3. Cardiovascular
Thromboembolic disorders including thrombophlebitis and pulmonary embolism have been reported.
4. Gastrointestinal
Nausea, cholestatic jaundice.
5. Skin
Sensitivity reactions consisting of urticaria, pruritus, edema and generalized rash have occurred. Acne, alopecia and hirsutism have been reported.
6. Eyes
Neuro-ocular lesions, for example, retinal thrombosis, and optic neuritis.
7. Central Nervous System
Mental depression, insomnia, somnolence, dizziness, headache, nervousness.
8. Miscellaneous
Hypersensitivity reactions (for example, anaphylaxis and anaphylactoid reactions, angioedema), rash (allergic) with and without pruritus, change in weight (increase or decrease), pyrexia, edema/fluid retention, fatigue, decreased glucose tolerance.
The following additional adverse reactions have been reported with estrogen and/or progestin therapy.
1. Genitourinary System
Abnormal uterine bleeding/spotting, or flow; breakthrough bleeding; spotting; dysmenorrheal/pelvic pain; increase in size of uterine leiomyomata; vaginitis, including vaginal candidiasis; change in amount of cervical secretion; changes in cervical ectropion; ovarian cancer; endometrial hyperplasia; endometrial cancer.
2. Breasts
Tenderness, enlargement, pain, nipple discharge, galactorrhea; fibrocystic breast changes; breast cancer.
3. Cardiovascular
Deep and superficial venous thrombosis; pulmonary embolism; thrombophlebitis; myocardial infarction; stroke; increase in blood pressure.
4. Gastrointestinal
Nausea, vomiting; abdominal cramps, bloating; cholestatic jaundice; increased incidence of gallbladder disease; pancreatitis; enlargement of hepatic hemangiomas.
5. Skin
Chloasma or melasma that may persist when drug is discontinued; erythema multiforme; erythema nodosum; hemorrhagic eruption; loss of scalp hair; hirsutism; pruritus, rash.
6. Eyes
Retinal vascular thrombosis, intolerance to contact lenses.
7. Central Nervous System
Headache; migraine; dizziness; mental depression; chorea; nervousness; mood disturbances; irritability; exacerbation of epilepsy, dementia.
8. Miscellaneous
Increase or decrease in weight; reduced carbohydrate tolerance; aggravation of porphyria; edema; arthalgias; leg cramps; changes in libido; urticaria, angioedema, anaphylactoid/anaplylactic reactions; hypocalcemia; exacerbation of asthma; increased triglycerides.
OVERDOSAGE
Overdosage of estrogen plus progestin therapy may cause nausea and vomiting, breast tenderness, dizziness, abdominal pain, drowsiness/fatigue and withdrawal bleeding may occur in women. Treatment of overdose consists of discontinuation of CE/MPA together with institution of appropriate symptomatic care.
DOSAGE AND ADMINISTRATION
Secondary Amenorrhea
Medroxyprogesterone acetate tablets may be given in dosages of 5 or 10 mg daily for 5 to 10 days. A dose for inducing an optimum secretory transformation of an endometrium that has been adequately primed with either endogenous or exogenous estrogen is 10 mg of medroxyprogesterone acetate daily for 10 days. In cases of secondary amenorrhea, therapy may be started at any time. Progestin withdrawal bleeding usually occurs within three to seven days after discontinuing medroxyprogesterone acetate therapy.
Abnormal Uterine Bleeding Due to Hormonal Imbalance in the Absence of Organic Pathology
Beginning on the calculated 16th or 21st day of the menstrual cycle, 5 or 10 mg of medroxyprogesterone acetate may be given daily for 5 to 10 days. To produce an optimum secretory transformation of an endometrium that has been adequately primed with either endogenous or exogenous estrogen, 10 mg of medroxyprogesterone acetate daily for 10 days beginning on the 16th day of the cycle is suggested. Progestin withdrawal bleeding usually occurs within three to seven days after discontinuing therapy with medroxyprogesterone acetate. Patients with a past history of recurrent episodes of abnormal uterine bleeding may benefit from planned menstrual cycling with medroxyprogesterone acetate.
Reduction of Endometrial Hyperplasia in Postmenopausal Women Receiving Daily 0.625 mg Conjugated Estrogens
When estrogen is prescribed for a postmenopausal woman with a uterus, a progestin should also be initiated to reduce the risk of endometrial cancer. A woman without a uterus does not need progestin. Use of estrogen, alone or in combination with a progestin, should be with the lowest effective dose and for the shortest duration consistent with treatment goals and risks for the individual woman. Patients should be re-evaluated periodically as clinically appropriate (for example, 3-month to 6-month intervals) to determine if treatment is still necessary (see WARNINGS). For women who have a uterus, adequate diagnostic measures, such as endometrial sampling, when indicated, should be undertaken to rule out malignancy in cases of undiagnosed persistent or recurring abnormal vaginal bleeding.
Medroxyprogesterone acetate tablets may be given in dosages of 5 or 10 mg daily for 12 to 14 consecutive days per month, in postmenopausal women receiving daily 0.625 mg conjugated estrogens, either beginning on the 1st day of the cycle or the 16th day of the cycle.
Patients should be started at the lowest dose.
The lowest effective dose of medroxyprogesterone acetate has not been determined.
HOW SUPPLIED
Medroxyprogesterone Acetate Tablets, USP are available as:
| 10 mg: | White, round, scored, biconvex tablet. Debossed with 555/779 on the scored side and stylized b on the other side. | |
| Available in bottles of: | ||
| 10 Tablets | NDC 21695-896-10 | |
Dispense with a child-resistant closure in a tight container.
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature].
PATIENT INFORMATION
Read this PATIENT INFORMATION before you start taking medroxyprogesterone acetate and read the patient information each time you refill your medroxyprogesterone acetate prescription. There may be new information. This information does not take the place of talking to your health care provider about your medical condition or your treatment.
WHAT IS THE MOST IMPORTANT INFORMATION I SHOULD KNOW ABOUT MEDROXYPROGESTERONE ACETATE (A PROGESTIN HORMONE)?
* Vaginal bleeding after menopause may be a warning sign of cancer of the uterus (womb). Your health care provider should check any unusual vaginal bleeding to find out the cause.
* Do not use estrogens with or without progestins to prevent heart disease, heart attacks, or strokes. Using estrogens with or without progestins may increase your chance of getting heart attacks, strokes, breast cancer, and blood clots.
* Using estrogens with or without progestins may increase your risk of dementia, based on a study of women age 65 years or older.
You and your health care provider should talk regularly about whether you still need treatment with medroxyprogesterone acetate.
What is Medroxyprogesterone Acetate?
Medroxyprogesterone Acetate is a medicine that contains medroxyprogesterone acetate, a progestin hormone.
What is Medroxyprogesterone Acetate used for?
Medroxyprogesterone Acetate is used to:
- Treat menstrual periods that have stopped or to treat abnormal uterine bleeding. Women with a uterus who are not pregnant, who stop having regular menstrual periods or who begin to have irregular menstrual periods may have a drop in their progesterone level. Talk with your health care provider about whether Medroxyprogesterone Acetate is right for you.
- Reduce your chances of getting cancer of the uterus. In postmenopausal women with a uterus who use estrogens, taking progestin in combination with estrogen will reduce your chances of getting cancer of the uterus.
Who should not take Medroxyprogesterone Acetate?
Do not start taking Medroxyprogesterone Acetate if you:
- Have undiagnosed vaginal bleeding
- Currently have or have had certain cancers
Estrogen plus progestin may increase your chance of getting certain cancers, including cancer of the breast. If you have or have had cancer, talk with your health care provider about whether you should use medroxyprogesterone acetate.
- Had a stroke or heart attack in the past year
- Currently have or have had blood clots
- Currently have or have had liver problems
- Think you may be pregnant
Tell your health care provider if you think that you may be pregnant or having a miscarriage. There may be an increased risk of minor birth defects in children whose mothers take this drug during the first 4 months of pregnancy. If you take medroxyprogesterone acetate and later find out you were pregnant when you took it, be sure to discuss this with your doctor as soon as possible.
Medroxyprogesterone Acetate should not be used as a test for pregnancy.
- Are allergic to any of the ingredients in medroxyprogesterone acetate.
See the list of ingredients in medroxyprogesterone acetate at the end of this leaflet.
Tell your health care provider:
- If you are breastfeeding. The hormone in medroxyprogesterone acetate can pass into your breast milk.
- About all of your medical problems. Your health care provider may need to check you more carefully if you have certain conditions, such as asthma (wheezing); epilepsy (seizures); migraine headaches; endometriosis (severe pelvic pain); lupus; problems with your heart, liver, thyroid, or kidneys; or if you have high calcium levels in your blood.
- About all the medicines you take. This includes prescription and nonprescription medicines, vitamins, and herbal supplements. Some medicines may affect how medroxyprogesterone acetate works. Medroxyprogesterone Acetate may also affect how other medicines work.
- If you are going to have surgery or will be on bed rest. If you are taking estrogen in addition to medroxyprogesterone acetate, you may need to stop taking estrogen and medroxyprogesterone acetate.
How should I take Medroxyprogesterone Acetate?
Start at the lowest dose and talk to your health care provider about how well that dose is working for you. The lowest effective dose of medroxyprogesterone acetate has not been determined.
You and your health care provider should talk regularly (every 3-6 months) about the dose you are taking and whether you still need treatment with medroxyprogesterone acetate.
- Absence of menstrual period: Medroxyprogesterone acetate may be given in doses ranging from 5 to 10 mg daily for 5 to 10 days.
- Abnormal Uterine Bleeding: Medroxyprogesterone acetate may be given in doses ranging from 5 to 10 mg daily for 5 to 10 days.
- Overgrowth of the lining of the uterus: When used in combination with oral conjugated estrogens in postmenopausal women with a uterus, medroxyprogesterone acetate may be given in doses ranging from 5 or 10 mg daily for 12 to 14 straight days per month.
What are the possible side effects of Medroxyprogesterone Acetate?
The following side effects have been reported with the use of Medroxyprogesterone Acetate alone:
- Breast tenderness
- Breast milk secretion
- Breakthrough bleeding
- Spotting (minor vaginal bleeding)
- Irregular periods
- Amenorrhea (absence of menstrual periods)
- Vaginal secretions
- Headaches
- Nervousness
- Dizziness
- Depression
- Insomnia, sleepiness, fatigue
- Premenstrual syndrome-like symptoms
- Thrombophlebitis (inflamed veins)
- Blood clot
- Itching, hives, skin rash
- Acne
- Hair loss, hair growth
- Abdominal discomfort
- Nausea
- Bloating
- Fever
- Increase in weight
- Swelling
- Changes in vision and sensitivity to contact lenses
The following side effects have been reported with the use of Medroxyprogesterone Acetate with an estrogen.
Side effects are grouped by how serious they are and how often they happen when you are treated:
Serious but less common side effects of estrogen include:
- Breast cancer
- Cancer of the uterus
- Stroke
- Heart attack
- Blood clots
- Dementia
- Gallbladder disease
- Ovarian cancer
- High blood pressure
- Liver problems
- High blood sugar
- Enlargement of benign tumors of the uterus (“fibroids”)
Some of the warning signs of these serious side effects include:
- Breast lumps
- Unusual vaginal bleeding
- Dizziness and faintness
- Changes in speech
- Severe headaches
- Chest pain
- Shortness of breath
- Pains in your legs
- Changes in vision
- Vomiting
- Yellowing of the skin, eyes or nail beds
Call your health care provider right away if you get any of these warning signs, or any other unusual symptom that concerns you.
Less serious but common side effects include:
- Headache
- Breast pain
- Irregular vaginal bleeding or spotting
- Stomach/abdominal cramps, bloating
- Nausea and vomiting
- Hair loss
- Fluid retention
- Vaginal yeast infection
These are not all the possible side effects of medroxyprogesterone acetate with or without estrogen. For more information, ask your health care provider or pharmacist.
What can I do to lower my chances of a serious side effect with Medroxyprogesterone Acetate?
- Talk with your health care provider regularly about whether you should continue taking medroxyprogesterone acetate. The addition of a progestin is generally recommended for women with a uterus to reduce the chance of getting cancer of the uterus.
- See your health care provider right away if you get vaginal bleeding while taking medroxyprogesterone acetate.
- Have a pelvic exam, breast exam and mammogram (breast X-ray) every year unless your health care provider tells you otherwise. If members of your family have had breast cancer or if you have ever had breast lumps or an abnormal mammogram, you may need to have breast exams more often.
- If you have high blood pressure, high cholesterol (fat in the blood), diabetes, are overweight, or if you use tobacco, you may have a higher chance of getting heart disease. Ask your health care provider for ways to lower your chance of getting heart disease.
General information about safe and effective use of Medroxyprogesterone Acetate
- Medicines are sometimes prescribed for conditions that are not mentioned in patient information leaflets.
- Do not take Medroxyprogesterone Acetate for conditions for which it was not prescribed.
- Do not give Medroxyprogesterone Acetate to other people, even if they have the same symptoms you have. It may harm them.
Keep Medroxyprogesterone Acetate out of the reach of children.
This leaflet provides a summary of the most important information about Medroxyprogesterone Acetate. If you would like more information, talk with your health care provider or pharmacist. You can ask for information about Medroxyprogesterone Acetate that is written for health professionals.
What are the ingredients in Medroxyprogesterone Acetate?
Each Medroxyprogesterone Acetate tablet for oral administration contains 2.5 mg, 5 mg or 10 mg of medroxyprogesterone acetate.
Inactive ingredients: crospovidone, lactose monohydrate, magnesium stearate, methylcellulose, corn starch, and sodium lauryl sulfate.
BARR LABORATORIES, INC.
POMONA, NY 10970
Repackaged by:
REBEL DISTRIBUTORS CORP
Thousand Oaks, CA 91320
Principal Display Panel
| MEDROXYPROGESTERONE ACETATE
medroxyprogesterone acetate tablet |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| ANDA | ANDA040159 | 08/09/1996 | |
| Labeler - Rebel Distributors Corp. (118802834) |
| Establishment | |||
| Name | Address | ID/FEI | Operations |
| Rebel Distributors Corp. | 118802834 | RELABEL, REPACK | |