velcade (bortezomib) injection, powder, lyophilized, for solution
[Millennium Pharmaceuticals, Inc.]
PRESCRIBING INFORMATION
DESCRIPTION
VELCADE® (bortezomib) for Injection is an antineoplastic agent available for intravenous injection (IV) use only. Each single dose vial contains 3.5 mg of bortezomib as a sterile lyophilized powder. Inactive ingredient: 35 mg mannitol, USP.
Bortezomib is a modified dipeptidyl boronic acid. The product is provided as a mannitol boronic ester which, in reconstituted form, consists of the mannitol ester in equilibrium with its hydrolysis product, the monomeric boronic acid. The drug substance exists in its cyclic anhydride form as a trimeric boroxine.
The chemical name for bortezomib, the monomeric boronic acid, is [(1R)-3-methyl-1-[[(2S)-1-oxo-3-phenyl-2-[(pyrazinylcarbonyl) amino]propyl]amino]butyl] boronic acid.
Bortezomib has the following chemical structure:
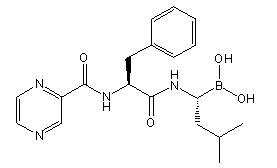
The molecular weight is 384.24. The molecular formula is C19H25BN4O4. The solubility of bortezomib, as the monomeric boronic acid, in water is 3.3 to 3.8 mg/mL in a pH range of 2 to 6.5.
CLINICAL PHARMACOLOGY
Mechanism of Action
Bortezomib is a reversible inhibitor of the chymotrypsin-like activity of the 26S proteasome in mammalian cells. The 26S proteasome is a large protein complex that degrades ubiquitinated proteins. The ubiquitin-proteasome pathway plays an essential role in regulating the intracellular concentration of specific proteins, thereby maintaining homeostasis within cells. Inhibition of the 26S proteasome prevents this targeted proteolysis, which can affect multiple signaling cascades within the cell. This disruption of normal homeostatic mechanisms can lead to cell death. Experiments have demonstrated that bortezomib is cytotoxic to a variety of cancer cell types in vitro. Bortezomib causes a delay in tumor growth in vivo in nonclinical tumor models, including multiple myeloma.
Pharmacokinetics
Following intravenous administration of 1.0 mg/m2 and 1.3 mg/m2 doses to 24 patients with multiple myeloma (n=12, per each dose level), the mean maximum plasma concentrations of bortezomib (Cmax) after the first dose (Day 1) were 57 and 112 ng/mL, respectively. In subsequent doses, when administered twice weekly, the mean maximum observed plasma concentrations ranged from 67 to 106 ng/mL for the 1.0 mg/m2 dose and 89 to 120 ng/mL for the 1.3 mg/m2 dose. The mean elimination half-life of bortezomib upon multiple dosing ranged from 40 to 193 hours after the 1.0 mg/m2 dose and 76 to 108 hours after the 1.3mg/m2 dose. The mean total body clearances was 102 and 112 L/h following the first dose for doses of 1.0 mg/m2 and 1.3 mg/m2, respectively, and ranged from 15 to 32 L/h following subsequent doses for doses of 1.0 and 1.3 mg/m2, respectively.
Distribution
The mean distribution volume of bortezomib ranged from approximately 498 to 1884 L/m2 following single- or repeat-dose administration of 1.0mg/m2 or 1.3mg/m2 to patients with multiple myeloma. This suggests bortezomib distributes widely to peripheral tissues. The binding of bortezomib to human plasma proteins averaged 83% over the concentration range of 100 to 1000 ng/mL.
Metabolism
In vitro studies with human liver microsomes and human cDNA-expressed cytochrome P450 isozymes indicate that bortezomib is primarily oxidatively metabolized via cytochrome P450 enzymes 3A4, 2C19, and 1A2. Bortezomib metabolism by CYP 2D6 and 2C9 enzymes is minor. The major metabolic pathway is deboronation to form 2 deboronated metabolites that subsequently undergo hydroxylation to several metabolites. Deboronated bortezomib metabolites are inactive as 26S proteasome inhibitors. Pooled plasma data from 8 patients at 10 min and 30 min after dosing indicate that the plasma levels of metabolites are low compared to the parent drug.
Elimination
The pathways of elimination of bortezomib have not been characterized in humans.
Special Populations
Age: Analyses of data after the first dose of Cycle 1 (Day 1) in 39 multiple myeloma patients who had received intravenous doses of 1.0 mg/m2 and 1.3 mg/m2 showed that both dose-normalized AUC and Cmax tend to be less in younger patients. Patients < 65 years of age (n=26) had about 25% lower mean dose-normalized AUC and Cmax than those ≥ 65 years of age (n=13).
Gender: Mean dose-normalized AUC and Cmax values were comparable between male (n=22) and female (n=17) patients after the first dose of Cycle 1 for the 1.0 and 1.3 mg/m2 doses.
Race: The effect of race on exposure to bortezomib could not be assessed as most of the patients were Caucasian.
Hepatic Impairment: No pharmacokinetic studies were conducted with bortezomib in patients with hepatic impairment (see PRECAUTIONS).
Renal Impairment: Clinical studies included patients with creatinine clearance values as low as 13.8 mL/min (see PRECAUTIONS).
Pediatric: There are no pharmacokinetic data in pediatric patients.
Drug Interactions
No formal drug interaction studies have been conducted with bortezomib.
In vitro studies with human liver microsomes indicate that bortezomib is primarily a substrate of cytochrome P450 3A4, 2C19, and 1A2 (see PRECAUTIONS).
Bortezomib is a poor inhibitor of human liver microsome cytochrome P450 1A2, 2C9, 2D6, and 3A4, with IC50 values of >30µM (>11.5µg/mL). Bortezomib may inhibit 2C19 activity (IC50 = 18 µM, 6.9 µg/mL) and increase exposure to drugs that are substrates for this enzyme.
Bortezomib did not induce the activities of cytochrome P450 3A4 and 1A2 in primary cultured human hepatocytes.
Pharmacodynamics
Following twice weekly administration of 1.0 mg/m2 and 1.3 mg/m2 bortezomib doses (n=12 per each dose level), the maximum inhibition of 20S proteasome activity (relative to baseline) in whole blood was observed 5 minutes after drug administration. Comparable maximum inhibition of 20S proteasome activity was observed between 1.0 and 1.3 mg/m2 doses. Maximal inhibition ranged from 70% to 84% and from 73% to 83% for the 1.0 mg/m2 and 1.3 mg/m2 dose regimens, respectively.
CLINICAL STUDIES
Randomized, Open-Label, Phase 3 Clinical Study in Relapsed Multiple Myeloma
A prospective phase 3, international, randomized (1:1), stratified, open-label clinical study enrolling 669 patients was designed to determine whether VELCADE resulted in improvement in time to progression (TTP) compared to high-dose dexamethasone in patients with progressive multiple myeloma following 1 to 3 prior therapies. Patients considered to be refractory to prior high-dose dexamethasone were excluded as were those with baseline grade ≥2 peripheral neuropathy or platelet counts <50,000/µL. A total of 627 patients were evaluable for response.
Stratification factors were based on the number of lines of prior therapy the patient had previously received (1 previous line versus more than 1 line of therapy), time of progression relative to prior treatment (progression during or within 6 months of stopping their most recent therapy versus relapse >6 months after receiving their most recent therapy), and screening β2-microglobulin levels (≤2.5 mg/L versus >2.5 mg/L).
Baseline patient and disease characteristics are summarized in Table 1.
| Patient Characteristics | VELCADE N=333 |
Dexamethasone N=336 |
|---|---|---|
| Median age in years (range) | 62.0 (33, 84) | 61.0 (27, 86) |
| Gender: Male/female | 56% / 44% | 60% / 40% |
| Race: Caucasian/black/other | 90% / 6% / 4% | 88% / 7% / 5% |
| Karnofsky performance status score ≤70 | 13% | 17% |
| Hemoglobin <100 g/L | 32% | 28% |
| Platelet count <75 x 109/L | 6% | 4% |
| Disease Characteristics | ||
| Type of myeloma (%): IgG/IgA/Light chain | 60% / 23% / 12% | 59% / 24% / 13% |
| Median β2-microglobulin (mg/L) | 3.7 | 3.6 |
| Median albumin (g/L) | 39.0 | 39.0 |
| Creatinine clearance ≤30 mL/min [n (%)] | 17 (5%) | 11 (3%) |
| Median Duration of Multiple Myeloma Since Diagnosis (Years) | 3.5 | 3.1 |
| Number of Prior Therapeutic Lines of Treatment | ||
| Median | 2 | 2 |
| 1 prior line | 40% | 35% |
| >1 prior line | 60% | 65% |
| Previous Therapy | ||
| Any prior steroids, e.g., dexamethasone, VAD | 98% | 99% |
| Any prior anthracyclines, e.g., VAD, mitoxantrone | 77% | 76% |
| Any prior alkylating agents, e.g., MP, VBMCP | 91% | 92% |
| Any prior thalidomide therapy | 48% | 50% |
| Vinca alkaloids | 74% | 72% |
| Prior stem cell transplant/other high-dose therapy | 67% | 68% |
| Prior experimental or other types of therapy | 3% | 2% |
Patients in the VELCADE treatment group were to receive eight 3-week treatment cycles followed by three 5-week treatment cycles of VELCADE. Within each 3-week treatment cycle, VELCADE 1.3 mg/m2/dose alone was administered by IV bolus twice weekly for 2 weeks on Days 1, 4, 8, and 11 followed by a 10-day rest period (Days 12 to 21). Within each 5-week treatment cycle, VELCADE 1.3 mg/m2/dose alone was administered by IV bolus once weekly for 4 weeks on Days 1, 8, 15, and 22 followed by a 13-day rest period (Days 23 to 35) (see DOSAGE AND ADMINISTRATION).
Patients in the dexamethasone treatment group were to receive four 5-week treatment cycles followed by five 4-week treatment cycles. Within each 5-week treatment cycle, dexamethasone 40 mg/day PO was administered once daily on Days 1 to 4, 9 to 12, and 17 to 20 followed by a 15-day rest period (Days 21-35). Within each 4-week treatment cycle, dexamethasone 40 mg/day PO was administered once daily on Days 1 to 4 followed by a 24-day rest period (Days 5 to 28). Patients with documented progressive disease on dexamethasone were offered VELCADE at a standard dose and schedule on a companion study.
Following a preplanned interim analysis of time to progression, the dexamethasone arm was halted and all patients randomized to dexamethasone were offered VELCADE, regardless of disease status. At this time of study termination, a final statistical analysis was performed. Due to this early termination of the study, the median duration of follow-up for surviving patients (n=534) is limited to 8.3 months.
In the VELCADE arm, 34% of patients received at least one VELCADE dose in all 8 of the 3-week cycles of therapy, and 13% received at least one dose in all 11 cycles. The average number of VELCADE doses during the study was 22, with a range of 1 to 44. In the dexamethasone arm, 40% of patients received at least one dose in all 4 of the 5-week treatment cycles of therapy, and 6% received at least one dose in all 9 cycles.
The time to event analyses and response rates from the phase 3 multiple myeloma study are presented in Table 2. Response and progression were assessed using the European Group for Blood and Marrow Transplantation (EBMT) criteria.1 Complete response (CR) required <5% plasma cells in the marrow, 100% reduction in M-protein, and a negative immunofixation test (IF-). Partial Response (PR) requires ≥50% reduction in serum myeloma protein and ≥90% reduction of urine myeloma protein on at least 2 occasions for a minimum of at least 6 weeks along with stable bone disease and normal calcium. Near complete response (nCR) was defined as meeting all the criteria for complete response including 100% reduction in M-protein by protein electrophoresis, however M-protein was still detectable by immunofixation (IF+).
| Efficacy Endpoint | All Patients | 1 Prior Line of Therapy | > 1 Prior Line of Therapy | |||
|---|---|---|---|---|---|---|
| VELCADE | Dex | VELCADE | Dex | VELCADE | Dex | |
| n=333 | n=336 | n=132 | n=119 | n=200 | n=217 | |
| a Kaplan-Meier estimate. | ||||||
| b Hazard ratio is based on Cox proportional-hazard model with the treatment as single independent variable. A hazard ratio less than 1 indicates an advantage for VELCADE. | ||||||
| c p-value based on the stratified log-rank test including randomization stratification factors. | ||||||
| d Precise p-value cannot be rendered. | ||||||
| e Response population includes patients who had measurable disease at baseline and received at least 1 dose of study drug. | ||||||
| f EBMT criteria1; nCR meets all EBMT criteria for CR but has positive IF. Under EBMT criteria. nCR is in the PR category. | ||||||
| g In 2 patients, the IF was unknown. | ||||||
| h p-value for Response Rate (CR + PR) from the Cochran-Mantel-Haenszel chi-square test adjusted for the stratification factors; | ||||||
| i Not Estimable. | ||||||
| j Not Applicable, no patients in category. | ||||||
| Time to Progression Events n (%) |
147 (44) | 196 (58) | 55 (42) | 64 (54) | 92 (46) | 132 (61) |
| Median a (95% CI) |
6.2 mo (4.9, 6.9) |
3.5 mo (2.9, 4.2) |
7.0 mo (6.2, 8.8) |
5.6 mo (3.4, 6.3) |
4.9 mo (4.2, 6.3) |
2.9 mo (2.8, 3.5) |
| Hazard ratio b (95% CI) |
0.55 (0.44, 0.69) |
0.55 (0.38, 0.81) |
0.54 (0.41, 0.72) |
|||
| p-value c | <0.0001 | 0.0019 | <0.0001 | |||
| Overall Survival Events (deaths) n (%) |
51 (15) | 84 (25) | 12 (9) | 24 (20) | 39 (20) | 60 (28) |
| Hazard ratio b (95% CI) |
0.57 (0.40, 0.81) |
0.39 (0.19, 0.81) |
0.65 (0.43, 0.97) |
|||
| p-value c,d | <0.05 | <0.05 | <0.05 | |||
| Response Rate Population e n = 627 |
n=315 | n=312 | n=128 | n=110 | n=187 | n=202 |
| CR f n (%) | 20 (6) | 2 (<1) | 8 (6) | 2 (2) | 12 (6) | 0 (0) |
| PR f n(%) | 101 (32) | 54 (17) | 49 (38) | 27 (25) | 52 (28) | 27 (13) |
| nCR f,g n(%) | 21 (7) | 3 (<1) | 8 (6) | 2 (2) | 13 (7) | 1 (<1) |
| CR + PR f n (%) | 121 (38) | 56 (18) | 57 (45) | 29 (26) | 64 (34) | 27 (13) |
| p-value h | <0.0001 | 0.0035 | <0.0001 | |||
| Median Response Duration | ||||||
| CR f | 9.9 mo | NE i | 9.9 mo | NE | 6.3 mo | NA j |
| nCR f | 11.5 mo | 9.2 mo | NE | NE | 11.5 mo | 9.2 mo |
| CR + PR f | 8.0 mo | 5.6 mo | 8.1 mo | 6.2 mo | 7.8 mo | 4.1 mo |
TTP was statistically significantly longer on the VELCADE arm (see Figure 1).
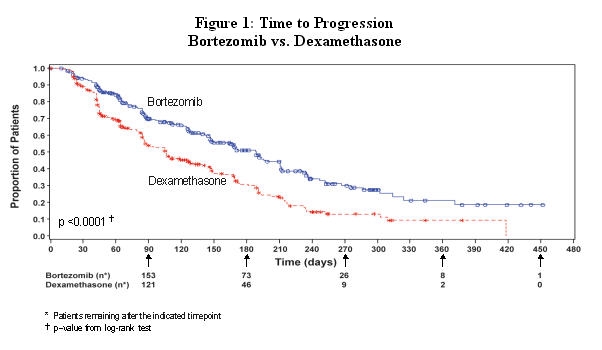
As shown in Figure 2, VELCADE had a significant survival advantage relative to dexamethasone (p<0.05). The median follow-up was 8.3 months.
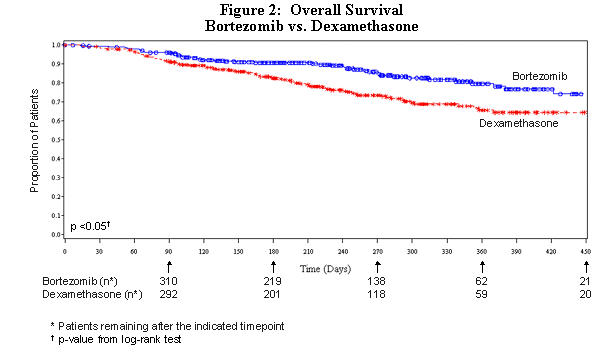
For the 121 patients achieving a response (CR or PR) on the VELCADE arm, the median duration was 8.0 months (95% CI: 6.9, 11.5 months) compared to 5.6 months (95% CI: 4.8, 9.2 months) for the 56 responders on the dexamethasone arm. The response rate was significantly higher on the VELCADE arm regardless of β2-microglobulin levels at baseline.
Phase 2 Single-arm Clinical Study in Relapsed Multiple Myeloma
The safety and efficacy of VELCADE in relapsed multiple myeloma were evaluated in an open-label, single-arm, multicenter study of 202 patients who had received at least 2 prior therapies and demonstrated disease progression on their most recent therapy. The median number of prior therapies was 6. Baseline patient and disease characteristics are summarized in Table 3.
An IV bolus injection of VELCADE 1.3 mg/m2/dose was administered twice weekly for 2 weeks on Days 1, 4, 8, and 11 followed by a 10-day rest period (Days 12 to 21) for a maximum of 8 treatment cycles. The study employed dose modifications for toxicity (see DOSAGE AND ADMINISTRATION). Patients who experienced a response to VELCADE were allowed to continue VELCADE treatment in an extension study.
| Patient Characteristics | N = 202 |
|---|---|
| * Based on number of patients with baseline data available | |
| Median age in years (range) | 59 (34, 84) |
| Gender: Male/female | 60% / 40% |
| Race: Caucasian/black/other | 81% / 10% /8% |
| Karnofsky Performance Status score ≤70 | 20% |
| Hemoglobin <100 g/L | 44% |
| Platelet count <75 x 109/L | 21% |
| Disease Characteristics | |
| Type of myeloma (%): IgG/IgA/Light chain | 60% / 24% / 14% |
| Median β2-microglobulin (mg/L) | 3.5 |
| Median creatinine clearance (mL/min) | 73.9 |
| Abnormal cytogenetics | 35% |
| Chromosome 13 deletion | 15% |
| Median Duration of Multiple Myeloma Since Diagnosis in Years | 4.0 |
| Previous Therapy | |
| Any prior steroids, e.g., dexamethasone, VAD | 99% |
| Any prior alkylating agents, e.g., MP, VBMCP | 92% |
| Any prior anthracyclines, e.g., VAD, mitoxantrone | 81% |
| Any prior thalidomide therapy | 83% |
| Received at least 2 of the above | 98% |
| Received at least 3 of the above | 92% |
| Received all 4 of the above | 66% |
| Any prior stem cell transplant/other high-dose therapy | 64% |
| Prior experimental or other types of therapy | 44% |
Responses to VELCADE alone are shown in Table 4. Response rates to VELCADE alone were determined by an independent review committee (IRC) based on EBMT criteria.1 Response rates using the Southwest Oncology Group (SWOG) criteria2 are also shown. SWOG response required a ≥75% reduction in serum myeloma protein and/or ≥90% urine protein. A total of 188 patients were evaluable for response; 9 patients with nonmeasurable disease could not be evaluated for response by the IRC, and 5 patients were excluded from the efficacy analyses because they had had minimal prior therapy. The mean number of cycles administered was 6. The median time to response was 38 days (range 30 to 127 days). The median survival of all patients enrolled was 17 months (range <1 to 36+ months).
| Response Analyses (VELCADE monotherapy) N = 188 | N (%) | (95% CI) |
|---|---|---|
| a Clinical Remission (SWOG) required ≥75% reduction in serum myeloma protein and/or ≥90% reduction of urine myeloma protein on at least 2 occasions for a minimum of at least 6 weeks, stable bone disease and normal calcium.2 | ||
| Overall Response Rate (EBMT) (CR + PR) | 52 (28%) | (21, 35) |
| Complete Response (CR) | 5 (3%) | (1, 6) |
| Partial Response (PR) | 47 (25%) | (19, 32) |
| Clinical Remission (SWOG)a | 33 (18%) | (12, 24) |
| Kaplan-Meier Estimated Median Duration of Response (95% CI) | 385 Days | (245, 538) |
Of the 202 patients enrolled, 35% were 65 years of age or older. Nineteen percent (19%) of patients aged 65 years or older experienced CR or PR.
In this study, the response rate to VELCADE, based on a univariate analysis, was independent of the number and types of prior therapies. There was a decreased likelihood of response in patients with either >50% plasma cells or abnormal cytogenetics in the bone marrow. Responses were seen in patients with chromosome 13 abnormalities.
A Randomized Phase 2 Dose-Response Study in Relapsed Multiple Myeloma
An open-label, multicenter study randomized 54 patients with multiple myeloma who had progressed or relapsed on or after front-line therapy to receive VELCADE 1.0 mg/m2 or 1.3 mg/m2 IV bolus twice weekly for 2 weeks on Days 1, 4, 8, and 11 followed by a 10-day rest period (Days 12 to 21). The median duration of time between diagnosis of multiple myeloma and first dose of VELCADE on this trial was 2.0 years, and patients had received a median of 1 prior line of treatment (median of 3 prior therapies). A single complete response was seen at each dose. The overall response rates (CR + PR) were 30% (8/27) at 1.0 mg/m2 and 38% (10/26) at 1.3 mg/m2.
A Phase 2 Open-Label Extension Study in Relapsed Multiple Myeloma
Patients from the two phase 2 studies who in the investigators’ opinion would experience additional clinical benefit continued to receive VELCADE beyond 8 cycles on an extension study. Sixty-three (63) patients from the phase 2 multiple myeloma studies were enrolled and received a median of 7 additional cycles of VELCADE therapy for a total median of 14 cycles (range 7 to 32). The overall median dosing intensity was the same in both the parent protocol and extension study. Sixty-seven percent (67%) of patients initiated the extension study at the same or higher dose intensity at which they completed the parent protocol, and 89% of patients maintained the standard 3-week dosing schedule during the extension study. No new cumulative or new long-term toxicities were observed with prolonged VELCADE treatment (see ADVERSE REACTIONS).
A Phase 2 Single-arm Clinical Study in Relapsed Mantle Cell Lymphoma After Prior Therapy
The safety and efficacy of VELCADE in relapsed or refractory mantle cell lymphoma were evaluated in an open-label, single-arm, multicenter study of 155 patients with progressive disease who had received at least 1 prior therapy. The median age of the patients was 65 years (42, 89), 81% were male, and 92% were caucasian. Of the total, 75% had one or more extra-nodal sites of disease, and 77% were stage 4. In 91% of the patients, prior therapy included all of the following: an anthracycline or mitoxantrone, cyclophosphamide, and rituximab. A total of thirty seven percent (37%) of patients were refractory to their last prior therapy. An IV bolus injection of VELCADE 1.3 mg/m2/dose was administered twice weekly for 2 weeks on Days 1, 4, 8, and 11 followed by a 10-day rest period (Days 12 to 21) for a maximum of 17 treatment cycles. The study employed dose modifications for toxicity (see DOSAGE AND ADMINISTRATION).
Responses to VELCADE are shown in Table 5. Response rates to VELCADE were determined according to the International Workshop Criteria (IWRC)3 based on independent radiologic review of CT scans. The median number of cycles administered across all patients was 4; in responding patients the median number of cycles was 8. The median time to response was 40 days (range 31 to 204 days). The median duration of follow-up was more than 13 months.
| Response Analyses (N = 155) | N (%) | 95% CI |
|---|---|---|
| Overall Response Rate (IWRC) (CR + CRu + PR) | 48 (31) | (24, 39) |
| Complete Response (CR + CRu) | 12 (8) | (4, 13) |
| CR | 10 (6) | (3, 12) |
| CRu | 2 (1) | (0, 5) |
| Partial Response (PR) | 36 (23) | (17, 31) |
| Duration of Response | Median | 95% CI |
| CR + CRu + PR (N = 48) | 9.3 months | (5.4, 13.8) |
| CR + CRu (N = 12) | 15.4 months | (13.4, 15.4) |
| PR (N=36) | 6.1 months | (4.2, 9.3) |
INDICATIONS AND USAGE
VELCADE® (bortezomib) for Injection is indicated for the treatment of patients with multiple myeloma who have received at least 1 prior therapy.
VELCADE® (bortezomib) for Injection is indicated for the treatment of patients with mantle cell lymphoma who have received at least 1 prior therapy.
CONTRAINDICATIONS
VELCADE is contraindicated in patients with hypersensitivity to bortezomib, boron, or mannitol.
WARNINGS
VELCADE should be administered under the supervision of a physician experienced in the use of antineoplastic therapy.
Pregnancy Category D
Women of childbearing potential should avoid becoming pregnant while being treated with VELCADE.
Bortezomib was not teratogenic in nonclinical developmental toxicity studies in rats and rabbits at the highest dose tested (0.075 mg/kg; 0.5 mg/m2 in the rat and 0.05 mg/kg; 0.6 mg/m2 in the rabbit) when administered during organogenesis. These dosages are approximately half the clinical dose of 1.3 mg/m2 based on body surface area.
Pregnant rabbits given bortezomib during organogenesis at a dose of 0.05mg/kg (0.6 mg/m2) experienced significant post-implantation loss and decreased number of live fetuses. Live fetuses from these litters also showed significant decreases in fetal weight. The dose is approximately 0.5 times the clinical dose of 1.3 mg/m2 based on body surface area.
No placental transfer studies have been conducted with bortezomib. There are no adequate and well-controlled studies in pregnant women. If VELCADE is used during pregnancy, or if the patient becomes pregnant while receiving this drug, the patient should be apprised of the potential hazard to the fetus.
PRECAUTIONS
Peripheral Neuropathy: VELCADE treatment causes a peripheral neuropathy that is predominantly sensory. However, cases of severe sensory and motor peripheral neuropathy have been reported. Patients with pre-existing symptoms (numbness, pain or a burning feeling in the feet or hands) and/or signs of peripheral neuropathy may experience worsening peripheral neuropathy (including ≥Grade 3) during treatment with VELCADE. Patients should be monitored for symptoms of neuropathy, such as a burning sensation, hyperesthesia, hypoesthesia, paresthesia, discomfort, neuropathic pain or weakness. Patients experiencing new or worsening peripheral neuropathy may require change in the dose and schedule of VELCADE (see DOSAGE AND ADMINISTRATION). Following dose adjustments, improvement in or resolution of peripheral neuropathy was reported in 51% of patients with ≥Grade 2 peripheral neuropathy in the phase 3 multiple myeloma study. Improvement in or resolution of peripheral neuropathy was reported in 73% of patients who discontinued due to Grade 2 neuropathy or who had ≥Grade 3 peripheral neuropathy in the phase 2 multiple myeloma studies (also see ADVERSE REACTIONS). The long-term outcome of peripheral neuropathy has not been studied in mantle cell lymphoma.
Hypotension: The incidence of hypotension (postural, orthostatic, and hypotension NOS) was 13%. These events are observed throughout therapy. Caution should be used when treating patients with a history of syncope, patients receiving medications known to be associated with hypotension, and patients who are dehydrated. Management of orthostatic/postural hypotension may include adjustment of antihypertensive medications, hydration, and administration of mineralocorticoids and/or sympathomimetics (see ADVERSE REACTIONS).
Cardiac Disorders: Acute development or exacerbation of congestive heart failure, and/or new onset of decreased left ventricular ejection fraction has been reported, including reports in patients with few or no risk factors for decreased left ventricular ejection fraction. Patients with risk factors for, or existing heart disease should be closely monitored. In the phase 3 multiple myeloma study, the incidence of any treatment-emergent cardiac disorder was 15% and 13% in the VELCADE and dexamethasone groups, respectively. The incidence of heart failure events (acute pulmonary edema, cardiac failure, congestive cardiac failure, cardiogenic shock, pulmonary edema) was similar in the VELCADE and dexamethasone groups, 5% and 4%, respectively. There have been isolated cases of QT-interval prolongation in clinical studies; causality has not been established.
Pulmonary Disorders: There have been rare reports of acute diffuse infiltrative pulmonary disease of unknown etiology such as pneumonitis, interstitial pneumonia, lung infiltration and Acute Respiratory Distress Syndrome (ARDS) in patients receiving VELCADE. Some of these events have been fatal. A higher proportion of these events have been reported in Japan.
In a clinical trial, the first two patients given high-dose cytarabine (2 g/m2 per day) by continuous infusion with daunorubicin and VELCADE for relapsed acute myelogenous leukemia died of ARDS early in the course of therapy.
There have been rare reports of pulmonary hypertension associated with VELCADE administration in the absence of left heart failure or significant pulmonary disease.
In the event of new or worsening cardiopulmonary symptoms, a prompt comprehensive diagnostic evaluation should be conducted.
Reversible Posterior Leukoencephalopathy Syndrome (RPLS): There have been rare reports of RPLS in patients receiving VELCADE. RPLS is a rare, reversible, neurological disorder which can present with seizure, hypertension, headache, lethargy, confusion, blindness, and other visual and neurological disturbances. Brain imaging, preferably MRI (Magnetic Resonance Imaging), is used to confirm the diagnosis. In patients developing RPLS, discontinue VELCADE. The safety of reinitiating VELCADE therapy in patients previously experiencing RPLS is not known.
Laboratory Tests: Complete blood counts (CBC) should be frequently monitored during treatment with VELCADE.
Gastrointestinal Adverse Events: VELCADE treatment can cause nausea, diarrhea, constipation, and vomiting (see ADVERSE REACTIONS) sometimes requiring use of antiemetic and antidiarrheal medications. Fluid and electrolyte replacement should be administered to prevent dehydration.
Thrombocytopenia/Neutropenia: VELCADE is associated with thrombocytopenia and neutropenia (see ADVERSE REACTIONS). Platelets and neutrophils were lowest at Day 11 of each cycle of VELCADE treatment and typically recovered to baseline by the next cycle. The cyclical pattern of platelet and neutrophil decreases and recovery remained consistent over the 8 cycles of twice weekly dosing, and there was no evidence of cumulative thrombocytopenia or neutropenia. The mean platelet count nadir measured was approximately 40% of baseline. The severity of thrombocytopenia related to pretreatment platelet count is shown in Table 6. In the phase 3 multiple myeloma study, the incidence of significant bleeding events (≥Grade 3) was similar on both the VELCADE (4%) and dexamethasone (5%) arms. Platelet counts should be monitored prior to each dose of VELCADE. VELCADE therapy should be held when the platelet count is <25,000/µL and reinitiated at a reduced dose (see DOSAGE AND ADMINISTRATION and ADVERSE REACTIONS). There have been reports of gastrointestinal and intracerebral hemorrhage in association with VELCADE. Transfusions may be considered. The incidence of febrile neutropenia was <1%.
| Pretreatment Platelet Count* |
Number of Patients (N=331)** |
Number (%) of Patients with Platelet Count <10,000/µL |
Number (%) of Patients with Platelet Count 10,000-25,000/µL |
|---|---|---|---|
| * A baseline platelet count of 50,000/µL was required for study eligibility. | |||
| ** Data were missing at baseline for 1 patient | |||
| ≥75,000/µL | 309 | 8 (3%) | 36 (12%) |
| ≥ 50,000/µL-<75,000/µL | 14 | 2 (14%) | 11 (79%) |
| ≥10,000/µL-<50,000/µL | 7 | 1 (14%) | 5 (71%) |
Tumor Lysis Syndrome: Because VELCADE is a cytotoxic agent and can rapidly kill malignant cells, the complications of tumor lysis syndrome may occur. Patients at risk of tumor lysis syndrome are those with high tumor burden prior to treatment. These patients should be monitored closely and appropriate precautions taken.
Hepatic Events
Rare cases of acute liver failure have been reported in patients receiving multiple concomitant medications and with serious underlying medical conditions. Other reported hepatic events include increases in liver enzymes, hyperbilirubinemia, and hepatitis. Such changes may be reversible upon discontinuation of VELCADE. There is limited re-challenge information in these patients.
Patients with Hepatic Impairment: Bortezomib is metabolized by liver enzymes and bortezomib’s clearance may decrease in patients with hepatic impairment. These patients should be closely monitored for toxicities when treated with VELCADE (see CLINICAL PHARMACOLOGY/Pharmacokinetics-Special Populations).
Patients with Renal Impairment: Patients with renal impairment should be closely monitored for toxicities when treated with VELCADE (see CLINICAL PHARMACOLOGY/Pharmacokinetics-Special Populations).
Animal Toxicity Findings
Cardiovascular Toxicity
Studies in monkeys showed that administration of dosages approximately twice the recommended clinical dose resulted in heart rate elevations, followed by profound progressive hypotension, bradycardia, and death 12 to 14 hours post dose. Doses ≥1.2 mg/m2 induced dose-proportional changes in cardiac parameters. Bortezomib has been shown to distribute to most tissues in the body, including the myocardium. In a repeated dosing toxicity study in the monkey, myocardial hemorrhage, inflammation, and necrosis were also observed.
Chronic Administration
In animal studies at a dose and schedule similar to that recommended for patients (twice weekly dosing for 2 weeks followed by 1-week rest), toxicities observed included severe anemia and thrombocytopenia, and gastrointestinal, neurological and lymphoid system toxicities. Neurotoxic effects of bortezomib in animal studies included axonal swelling and degeneration in peripheral nerves, dorsal spinal roots, and tracts of the spinal cord. Additionally, multifocal hemorrhage and necrosis in the brain, eye, and heart were observed.
Information for Patients
Physicians are advised to discuss the PATIENT INFORMATION section with patients prior to treatment with VELCADE (see PATIENT INFORMATION).
Ability to Drive or Operate Machinery or Impairment of Mental Ability: VELCADE may cause fatigue, dizziness, syncope, orthostatic/postural hypotension. Patients should be advised not to drive or operate machinery if they experience these symptoms.
Dehydration/Hypotension: Since patients receiving VELCADE therapy may experience vomiting and/or diarrhea, patients should be advised regarding appropriate measures to avoid dehydration. Patients should be instructed to seek medical advice if they experience symptoms of dizziness, light headedness or fainting spells.
Drug Interactions
No formal drug interaction studies have been conducted with VELCADE.
In vitro studies with human liver microsomes indicate that bortezomib is primarily a substrate for cytochrome P450 3A4, 2C19, and 1A2. Patients who are concomitantly receiving VELCADE and drugs that are inhibitors or inducers of cytochrome P450 3A4 should be closely monitored for either toxicities or reduced efficacy (see CLINICAL PHARMACOLOGY/ Pharmacokinetics-Drug Interactions).
During clinical trials, hypoglycemia and hyperglycemia were reported in diabetic patients receiving oral hypoglycemics. Patients on oral antidiabetic agents receiving VELCADE treatment may require close monitoring of their blood glucose levels and adjustment of the dose of their antidiabetic medication.
Drug Laboratory Test Interactions
None known.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies have not been conducted with bortezomib.
Bortezomib showed clastogenic activity (structural chromosomal aberrations) in the in vitro chromosomal aberration assay using Chinese hamster ovary cells. Bortezomib was not genotoxic when tested in the in vitro mutagenicity assay (Ames test) and in vivo micronucleus assay in mice.
Fertility studies with bortezomib were not performed but evaluation of reproductive tissues has been performed in the general toxicity studies. In the 6-month rat toxicity study, degenerative effects in the ovary were observed at doses ≥0.3 mg/m2 (one-fourth of the recommended clinical dose), and degenerative changes in the testes occurred at 1.2 mg/m2. VELCADE could have a potential effect on either male or female fertility.
Pregnancy Category D (see WARNINGS)
Pregnancy
Patients should be advised to use effective contraceptive measures to prevent pregnancy.
Nursing Mothers
It is not known whether bortezomib is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from VELCADE, women should be advised against breast feeding while being treated with VELCADE.
Pediatric Use
The safety and effectiveness of VELCADE in children has not been established.
Geriatric Use
Of the 669 patients enrolled in the phase 3 multiple myeloma study, 245 (37%) were 65 years of age or older: 125 (38%) on the VELCADE arm and 120 (36%) on dexamethasone arm. Median time to progression and median duration of response for patients ≥65 were longer on VELCADE compared to dexamethasone [5.5 mo versus 4.3 mo, and 8.0 mo versus 4.9 mo, respectively]. On the VELCADE arm, 40% (n=46) of evaluable patients aged ≥65 experienced response (CR+PR) versus 18% (n=21) on the dexamethasone arm. The incidence of Grade 3 and 4 events was 64%, 78% and 75% for VELCADE patients ≤50, 51-64 and ≥65 years old, respectively (see CLINICAL STUDIES).
In the phase 2 clinical study of 202 patients with relapsed multiple myeloma, 35% of patients were 65 years of age or older, the incidence of Grade ≥3 events was 74%, 80%, and 85% for VELCADE patients ≤50, 51 to 65, and >65 years old, respectively (see CLINICAL STUDIES).
No overall differences in safety or effectiveness were observed between patients ≥ age 65 and younger patients receiving VELCADE; but greater sensitivity of some older individuals cannot be ruled out.
ADVERSE REACTIONS
Randomized Open-Label Phase 3 Multiple Myeloma Study
Among the 331 VELCADE treated patients, the most commonly reported events overall were asthenic conditions (61%), diarrhea and nausea (each 57%), constipation (42%), peripheral neuropathy NEC (36%), vomiting, pyrexia, thrombocytopenia, and psychiatric disorders (each 35%), anorexia and appetite decreased (34%), paresthesia and dysesthesia (27%), anemia and headache (each 26%), and cough (21%). The most commonly reported adverse events reported among the 332 patients in the dexamethasone group were psychiatric disorders (49%), asthenic conditions (45%), insomnia (27%), anemia (22%), and diarrhea and lower respiratory/lung infections (each 21%). Fourteen percent (14%) of patients in the VELCADE treated arm experienced a Grade 4 adverse event; the most common toxicities were thrombocytopenia (4%), neutropenia (2%) and hypercalcemia (2%). Sixteen percent (16%) of dexamethasone treated patients experienced a Grade 4 adverse event; the most common toxicity was hyperglycemia (2%).
Serious Adverse Events (SAEs) and Events Leading to Treatment Discontinuation in the Phase 3 Multiple Myeloma Study
Serious adverse events are defined as any event, regardless of causality, that results in death, is life-threatening, requires hospitalization or prolongs a current hospitalization, results in a significant disability, or is deemed to be an important medical event. A total of 144 (44%) patients from the VELCADE treatment arm experienced an SAE during the study, as did 144 (43%) dexamethasone-treated patients. The most commonly reported SAEs in the VELCADE treatment arm were pyrexia (6%), diarrhea (5%), dyspnea and pneumonia (4%), and vomiting (3%). In the dexamethasone treatment group, the most commonly reported SAEs were pneumonia (7%), pyrexia (4%), and hyperglycemia (3%).
A total of 145 patients, including 84 (25%) of 331 patients in the VELCADE treatment group and 61 (18%) of 332 patients in the dexamethasone treatment group were discontinued from treatment due to adverse events assessed as drug-related by the investigators. Among the 331 VELCADE treated patients, the most commonly reported drug-related event leading to discontinuation was peripheral neuropathy (8%). Among the 332 patients in the dexamethasone group, the most commonly reported drug-related events leading to treatment discontinuation were psychotic disorder and hyperglycemia (2% each).
Four deaths were considered to be VELCADE related in the phase 3 multiple myeloma study: 1 case each of cardiogenic shock, respiratory insufficiency, congestive heart failure and cardiac arrest. Four deaths were considered dexamethasone-related: 2 cases of sepsis, 1 case of bacterial meningitis, and 1 case of sudden death at home.
Most Commonly Reported Adverse Events in the Phase 3 Multiple Myeloma Study
The most common adverse events from the phase 3 multiple myeloma study are shown in Table 7. All adverse events with incidence ≥10% in the VELCADE arm are included.
| Treatment Group | ||||||
|---|---|---|---|---|---|---|
| VELCADE (n=331) [n (%)] | Dexamethasone (n=332) [n (%)] | |||||
| All Events | Grade 3 Events |
Grade 4 Events |
All Events | Grade 3 Events |
Grade 4 Events |
|
| a Peripheral neuropathy includes all terms under peripheral neuropathy NEC, (peripheral neuropathy NOS, peripheral neuropathy aggravated, peripheral sensory neuropathy, and peripheral motor neuropathy, and neuropathy NOS). | ||||||
| Adverse Event | 331 (100) | 203 (61) | 45 (14) | 327 (98) | 146 (44) | 52 (16) |
| Asthenic conditions | 201 (61) | 39 (12) | 1 (<1) | 148 (45) | 20 (6) | 0 |
| Diarrhea | 190 (57) | 24 (7) | 0 | 69 (21) | 6 (2) | 0 |
| Nausea | 190 (57) | 8 (2) | 0 | 46 (14) | 0 | 0 |
| Constipation | 140 (42) | 7 (2) | 0 | 49 (15) | 4 (1) | 0 |
| Peripheral neuropathya | 120 (36) | 24 (7) | 2 (<1) | 29 (9) | 1 (<1) | 1 (<1) |
| Vomiting | 117 (35) | 11 (3) | 0 | 20 (6) | 4 (1) | 0 |
| Pyrexia | 116 (35) | 6 (2) | 0 | 54 (16) | 4 (1) | 1 (<1) |
| Thrombocytopenia | 115 (35) | 85 (26) | 12 (4) | 36 (11) | 18 (5) | 4 (1) |
| Psychiatric disorders | 117 (35) | 9 (3) | 2 (<1) | 163 (49) | 26 (8) | 3 (<1) |
| Anorexia and appetite decreased | 112 (34) | 9 (3) | 0 | 31 (9) | 1 (<1) | 0 |
| Paresthesia and dysesthesia | 91 (27) | 6 (2) | 0 | 38 (11) | 1 (<1) | 0 |
| Anemia | 87 (26) | 31 (9) | 2 (<1) | 74 (22) | 32 (10) | 3 (<1) |
| Headache | 85 (26) | 3 (<1) | 0 | 43 (13) | 2 (<1) | 0 |
| Cough | 70 (21) | 2 (<1) | 0 | 35 (11) | 1 (<1) | 0 |
| Dyspnea | 65 (20) | 16 (5) | 1 (<1) | 58 (17) | 9 (3) | 2 (<1) |
| Neutropenia | 62 (19) | 40 (12) | 8 (2) | 5 (2) | 4 (1) | 0 |
| Rash | 61 (18) | 4 (1) | 0 | 20 (6) | 0 | 0 |
| Insomnia | 60 (18) | 1 (<1) | 0 | 90 (27) | 5 (2) | 0 |
| Abdominal pain | 53 (16) | 6 (2) | 0 | 12 (4) | 1 (<1) | 0 |
| Bone pain | 52 (16) | 12 (4) | 0 | 50 (15) | 9 (3) | 0 |
| Lower respiratory/lung infections | 48 (15) | 12 (4) | 2 (<1) | 69 (21) | 24 (7) | 1 (<1) |
| Pain in limb | 50 (15) | 5 (2) | 0 | 24 (7) | 2 (<1) | 0 |
| Back pain | 46 (14) | 10 (3) | 0 | 33 (10) | 4 (1) | 0 |
| Arthralgia | 45 (14) | 3 (<1) | 0 | 35 (11) | 5 (2) | 0 |
| Dizziness (excl. vertigo) | 45 (14) | 3 (<1) | 0 | 34 (10) | 0 | 0 |
| Nasopharyngitis | 45 (14) | 1 (<1) | 0 | 22 (7) | 0 | 0 |
| Herpes zoster | 42 (13) | 6 (2) | 0 | 15 (5) | 4 (1) | 1 (<1) |
| Muscle cramps | 41 (12) | 0 | 0 | 50 (15) | 3 (<1) | 0 |
| Myalgia | 39 (12) | 1 (<1) | 0 | 18 (5) | 1 (<1) | 0 |
| Rigors | 37 (11) | 0 | 0 | 8 (2) | 0 | 0 |
| Edema lower limb | 35 (11) | 0 | 0 | 43 (13) | 1 (<1) | 0 |
The Phase 2 Open-Label Extension Study in Relapsed Multiple Myeloma
In the phase 2 extension study of 63 patients noted above (see CLINICAL STUDIES) no new cumulative or new long-term toxicities were observed with prolonged VELCADE treatment.
Integrated Summary of Safety (Multiple Myeloma and Mantle Cell Lymphoma)
Safety data from phase 2 and 3 studies of VELCADE 1.3 mg/m2/dose twice weekly for 2 weeks followed by a 10-day rest period in 1163 patients with multiple myeloma (N=1008) and mantle cell lymphoma (N=155) were integrated and tabulated. In these studies, the safety profile of VELCADE was similar in patients with multiple myeloma and mantle cell lymphoma.
In the integrated analysis, the most commonly reported adverse events were asthenic conditions (including fatigue, malaise, and weakness) (64%), nausea (55%), diarrhea (52%), constipation (41%), peripheral neuropathy NEC (including peripheral sensory neuropathy and peripheral neuropathy aggravated) (39%), thrombocytopenia and appetite decreased (including anorexia) (each 36%), pyrexia (34%), vomiting (33%), and anemia (29%). Twenty percent (20%) of patients experienced at least 1 episode of ≥Grade 4 toxicity, most commonly thrombocytopenia (5%) and neutropenia (3%).
Serious Adverse Events (SAEs) and Events Leading to Treatment Discontinuation in the Integrated Summary of Safety
A total of 50% of patients experienced SAEs during the studies. The most commonly reported SAEs included pneumonia (7%), pyrexia (6%), diarrhea (5%), vomiting (4%), and nausea, dehydration, dyspnea and thrombocytopenia (each 3%).
Adverse events thought by the investigator to be drug-related and leading to discontinuation occurred in 22% of patients. The reasons for discontinuation included peripheral neuropathy (8%), asthenic conditions (3%) and thrombocytopenia and diarrhea (each 2%).
In total, 2% of the patients died and the cause of death was considered by the investigator to be possibly related to study drug: including reports of cardiac arrest, congestive heart failure, respiratory failure, renal failure, pneumonia and sepsis.
Most Commonly Reported Adverse Events in the Integrated Summary of Safety
The most common adverse events are shown in Table 8. All adverse events occurring at ≥10% are included. In the absence of a randomized comparator arm, it is often not possible to distinguish between adverse events that are drug-caused and those that reflect the patient’s underlying disease. Please see the discussion of specific adverse reactions that follows.
| All Patients (N=1163) |
Multiple Myeloma (N=1008) |
Mantle Cell Lymphoma (N=155) |
||||
|---|---|---|---|---|---|---|
| Adverse Events | All Events | ≥Grade 3 | All Events | ≥Grade 3 | All Events | ≥Grade 3 |
| a Peripheral neuropathy includes all terms under peripheral neuropathy NEC (peripheral neuropathy NOS, peripheral neuropathy aggravated, peripheral sensory neuropathy, and peripheral motor neuropathy, and neuropathy NOS). | ||||||
| Asthenic conditions | 740 (64) | 189 (16) | 628 (62) | 160 (16) | 112 (72) | 29 (19) |
| Nausea | 640 (55) | 43 (4) | 572 (57) | 39 (4) | 68 (44) | 4 (3) |
| Diarrhea | 604 (52) | 96 (8) | 531 (53) | 85 (8) | 73 (47) | 11 (7) |
| Constipation | 481 (41) | 26 (2) | 404 (40) | 22 (2) | 77 (50) | 4 (3) |
| Peripheral neuropathya | 457 (39) | 134 (12) | 372 (37) | 114 (11) | 85 (55) | 20 (13) |
| Thrombocytopenia | 421 (36) | 337 (29) | 388 (38) | 320 (32) | 33 (21) | 17 (11) |
| Appetite decreased | 417 (36) | 30 (3) | 357 (35) | 25 (2) | 60 (39) | 5 (3) |
| Pyrexia | 401 (34) | 36 (3) | 371 (37) | 34 (3) | 30 (19) | 2 (1) |
| Vomiting | 385 (33) | 57 (5) | 343 (34) | 53 (5) | 42 (27) | 4 (3) |
| Anemia | 333 (29) | 124 (11) | 306 (30) | 120 (12) | 27 (17) | 4 (3) |
| Edema | 262 (23) | 10 (<1) | 218 (22) | 6 (<1) | 44 (28) | 4 (3) |
| Paresthesia and dysesthesia | 254 (22) | 16 (1) | 240 (24) | 14 (1) | 14 ( 9) | 2 (1) |
| Headache | 253 (22) | 17 (1) | 227 (23) | 17 (2) | 26 (17) | 0 |
| Dyspnea | 244 (21) | 59 (5) | 209 (21) | 52 (5) | 35 (23) | 7 (5) |
| Cough | 232 (20) | 5 (<1) | 202 (20) | 5 (<1) | 30 (19) | 0 |
| Insomnia | 232 (20) | 7 (<1) | 199 (20) | 6 (<1) | 33 (21) | 1 (<1) |
| Rash | 213 (18) | 10 (<1) | 170 (17) | 6 (<1) | 43 (28) | 4 (3) |
| Arthralgia | 199 (17) | 27 (2) | 179 (18) | 25 (2) | 20 (13) | 2 (1) |
| Neutropenia | 195 (17) | 143 (12) | 185 (18) | 137 (14) | 10 (6) | 6 (4) |
| Dizziness (excluding vertigo) | 195 (17) | 18 (2) | 159 (16) | 13 (1) | 36 (23) | 5 (3) |
| Pain in limb | 179 (15) | 36 (3) | 172 (17) | 36 (4) | 7 (5) | 0 |
| Abdominal pain | 170 (15) | 30 (3) | 146 (14) | 22 (2) | 24 (15) | 8 (5) |
| Bone pain | 166 (14) | 37 (3) | 163 (16) | 37 (4) | 3 (2) | 0 |
| Back pain | 151 (13) | 39 (3) | 150 (15) | 39 (4) | 1 (<1) | 0 |
| Hypotension | 147 (13) | 37 (3) | 124 (12) | 32 (3) | 23 (15) | 5 (3) |
| Herpes zoster | 145 (12) | 22 (2) | 131 (13) | 21 (2) | 14 (9) | 1 (<1) |
| Nasopharyngitis | 139 (12) | 2 (<1) | 126 (13) | 2 (<1) | 13 (8) | 0 |
| Upper respiratory tract infection | 138 (12) | 2 (<1) | 114 (11) | 1 (<1) | 24 (15) | 1 (<1) |
| Myalgia | 136 (12) | 9 (<1) | 121 (12) | 9 (<1) | 15 (10) | 0 |
| Pneumonia | 134 (12) | 72 (6) | 120 (12) | 65 (6) | 14 (9) | 7 (5) |
| Muscle cramps | 125 (11) | 1 (<1) | 118 (12) | 1 (<1) | 7 (5) | 0 |
| Dehydration | 120 (10) | 40 (3) | 109 (11) | 33 (3) | 11 (7) | 7 (5) |
| Anxiety | 118 (10) | 6 (<1) | 111 (11) | 6 (<1) | 7 (5) | 0 |
Description of Selected Adverse Events from the Phase 2 and 3 Multiple Myeloma and Phase 2 Mantle Cell Lymphoma Studies
Gastrointestinal Events
A total of 87% of patients experienced at least one GI disorder. The most common GI disorders included nausea, diarrhea, constipation, vomiting, and appetite decreased. Other GI disorders included dyspepsia and dysgeusia. Grade 3 GI events occurred in 18% of patients; Grade 4 events were rare (1%). GI events were considered serious in 11% of patients. Five percent (5%) of patients discontinued due to a GI event. Nausea was reported more often in patients with multiple myeloma (57%) compared to patients with mantle cell lymphoma (44%) (see PRECAUTIONS).
Thrombocytopenia
Across the studies, VELCADE associated thrombocytopenia was characterized by a decrease in platelet count during the dosing period (days 1 to 11) and a return toward baseline during the 10-day rest period during each treatment cycle. Overall, thrombocytopenia was reported in 36% of patients. Thrombocytopenia was Grade 3 in 24%, ≥Grade 4 in 5%, and serious in 3% of patients, and the event resulted in VELCADE discontinuation in 2% of patients (see PRECAUTIONS). Thrombocytopenia was reported more often in patients with multiple myeloma (38%) compared to patients with mantle cell lymphoma (21%). The incidence of ≥Grade 3 thrombocytopenia also was higher in patients with multiple myeloma (32%) compared to patients with mantle cell lymphoma (11%).
Peripheral Neuropathy
Overall, peripheral neuropathy NEC occurred in 39% of patients. Peripheral neuropathy was Grade 3 for 11% of patients and Grade 4 for <1% of patients. Eight percent (8%) of patients discontinued VELCADE due to peripheral neuropathy. The incidence of peripheral neuropathy was higher among patients with mantle cell lymphoma (55%) compared to patients with multiple myeloma (37%).
In the phase 3 multiple myeloma study, among the 87 patients who experienced ≥ Grade 2 peripheral neuropathy, 51% had improved or resolved with a median of 3.5 months from first onset.
Among the patients with peripheral neuropathy in the phase 2 multiple myeloma studies that was Grade 2 and led to discontinuation or was ≥Grade 3, 73% (24 of 33) reported improvement or resolution following VELCADE dose adjustment, with a median time to improvement of one Grade or more from the last dose of VELCADE of 33 days (see PRECAUTIONS).
Hypotension
The incidence of hypotension (postural hypotension, orthostatic hypotension and hypotension NOS) was 13% in patients treated with VELCADE. Hypotension was Grade 1 or 2 in the majority of patients and Grade 3 in 3% and ≥Grade 4 in <1%. Three percent (3%) of patients had hypotension reported as an SAE, and 1% discontinued due to hypotension. The incidence of hypotension was similar in patients with multiple myeloma (12%) and those with mantle cell lymphoma (15%). In addition, 2% of patients experienced hypotension and had a syncopal event. Doses of antihypertensive medications may need to be adjusted in patients receiving VELCADE (see PRECAUTIONS).
Neutropenia
Neutrophil counts decreased during the VELCADE dosing period (days 1 to 11) and returned toward baseline during the 10-day rest period during each treatment cycle. Overall, neutropenia occurred in 17% of patients and was Grade 3 in 9% of patients and ≥Grade 4 in 3%. Neutropenia was reported as a serious event in <1% of patients and <1% of patients discontinued due to neutropenia. The incidence of neutropenia was higher in patients with multiple myeloma (18%) compared to patients with mantle cell lymphoma (6%). The incidence of ≥Grade 3 neutropenia also was higher in patients with multiple myeloma (14%) compared to patients with mantle cell lymphoma (4%) (see PRECAUTIONS).
Asthenic conditions (Fatigue, Malaise, Weakness)
Asthenic conditions were reported in 64% of patients. Asthenia was Grade 3 for 16% and ≥Grade 4 in <1% of patients. Four percent (4%) of patients discontinued treatment due to asthenia. Asthenic conditions were reported in 62% of patients with multiple myeloma and 72% of patients with mantle cell lymphoma.
Pyrexia
Pyrexia (>38ºC) was reported as an adverse event for 34% of patients. The event was Grade 3 in 3% and ≥Grade 4 in <1%. Pyrexia was reported as a serious adverse event in 6% of patients and led to VELCADE discontinuation in <1% of patients. The incidence of pyrexia was higher among patients with multiple myeloma (37%) compared to patients with mantle cell lymphoma (19%). The incidence of ≥Grade 3 pyrexia was 3% in patients with multiple myeloma and 1% in patients with mantle cell lymphoma.
Reactivation of Herpes Virus Infection
Reactivation of herpes virus infections, including herpes zoster and herpes simplex was reported in 13% and 7% of patients, respectively. This included ophthalmic herpes zoster and ophthalmic herpes simplex each in <1% of patients. Multidermatomal herpes zoster also has been reported. Herpes reactivation was reported as a serious event in 2% of patients and led to discontinuation of VELCADE in <1% of patients. In the phase 3 multiple myeloma study, herpes reactivation was more common in patients treated with VELCADE (13% herpes zoster, 8% herpes simplex) than in patients treated with dexamethasone (5% herpes zoster, 5% herpes simplex). In the postmarketing experience, rare cases of herpes meningoencephalitis and ophthalmic herpes have been reported.
Additional Adverse Events from Clinical Studies and Post-Marketing
The following clinically important SAEs that are not described above have been reported in clinical trials in patients treated with VELCADE administered as monotherapy or in combination with other chemotherapeutics. These studies were conducted in patients with hematological malignancies and in solid tumors.
Blood and lymphatic system disorders: Disseminated intravascular coagulation, lymphopenia, leukopenia
Cardiac disorders: Angina pectoris, atrial fibrillation aggravated, atrial flutter, bradycardia, sinus arrest, cardiac amyloidosis, complete atrioventricular block, myocardial ischemia, myocardial infarction, pericarditis, pericardial effusion, Torsades de pointes, ventricular tachycardia
Ear and labyrinth disorders: Hearing impaired, vertigo
Eye disorders: Diplopia and blurred vision, conjunctival infection, irritation
Gastrointestinal disorders: Ascites, dysphagia, fecal impaction, gastroenteritis, gastritis hemorrhagic, hematemesis, hemorrhagic duodenitis, ileus paralytic, large intestinal obstruction, paralytic intestinal obstruction, peritonitis, small intestinal obstruction, large intestinal perforation, stomatitis, melena, pancreatitis acute, oral mucosal petechiae, gastroesophageal reflux
General disorders and administration site conditions: Injection site erythema, neuralgia, injection site pain, irritation, phlebitis
Hepatobiliary disorders: Cholestasis, hepatic hemorrhage, hyperbilirubinemia, portal vein thrombosis, hepatitis, liver failure
Immune system disorders: Anaphylactic reaction, drug hypersensitivity, immune complex mediated hypersensitivity, angioedema, laryngeal edema
Infections and infestations: Aspergillosis, bacteremia, urinary tract infection, herpes viral infection, listeriosis, septic shock, toxoplasmosis, oral candidiasis, sinusitis, catheter related infection
Injury, poisoning and procedural complications: Catheter related complication, skeletal fracture, subdural hematoma
Metabolism and nutrition disorders: Hypocalcemia, hyperuricemia, hypokalemia, hyperkalemia, hyponatremia, hypernatremia
Nervous system disorders: Ataxia, coma, dysarthria, dysautonomia, encephalopathy, cranial palsy, grand mal convulsion, hemorrhagic stroke, motor dysfunction, spinal cord compression, paralysis, postherpetic neuralgia, transient ischemic attack, reversible posterior leukoencephalopathy syndrome
Psychiatric disorders: Agitation, confusion, mental status change, psychotic disorder, suicidal ideation
Renal and urinary disorders: Calculus renal, bilateral hydronephrosis, bladder spasm, hematuria, hemorrhagic cystitis, urinary incontinence, urinary retention, renal failure (acute and chronic), glomerular nephritis proliferative
Respiratory, thoracic and mediastinal disorders: Acute respiratory distress syndrome, aspiration pneumonia, atelectasis, chronic obstructive airways disease exacerbated, dysphagia, dyspnea, dyspnea exertional, epistaxis, hemoptysis, hypoxia, lung infiltration, pleural effusion, pneumonitis, respiratory distress, pulmonary hypertension
Skin and subcutaneous tissue disorders: Urticaria, face edema, rash (which may be pruritic), leukocytoclastic vasculitis
Vascular disorders: Cerebrovascular accident, cerebral hemorrhage, deep venous thrombosis, peripheral embolism, pulmonary embolism, pulmonary hypertension
Post-Marketing Experience
Clinically significant adverse events are listed here if they have been reported during post-approval use of VELCADE and either they have not been reported in clinical trials, or they have been reported in clinical trials, but their occurrence in the post-approval setting is considered meaningful:
Atrioventricular block complete, cardiac tamponade, ischemic colitis,
encephalopathy, dysautonomia, deafness bilateral, disseminated
intravascular coagulation, hepatitis, acute pancreatitis, acute diffuse
infiltrative pulmonary disease and toxic epidermal necrolysis.
OVERDOSAGE
There is no known specific antidote for VELCADE overdosage (see PRECAUTIONS and DOSAGE AND ADMINISTRATION). In humans, fatal outcomes following the administration of more than twice the recommended therapeutic dose have been reported, which were associated with the acute onset of symptomatic hypotension and thrombocytopenia. In the event of an overdosage, the patient’s vital signs should be monitored and appropriate supportive care given.
Studies in monkeys and dogs showed that IV bortezomib doses as low as 2 times the recommended clinical dose on a mg/m2 basis were associated with increases in heart rate, decreases in contractility, hypotension, and death. In dog studies, a slight increase in the corrected QT interval was observed at doses resulting in death. In monkeys, doses of 3.0 mg/m2 and greater (approximately twice the recommended clinical dose) resulted in hypotension starting at 1 hour post-administration, with progression to death in 12 to 14 hours following drug administration.
DOSAGE AND ADMINISTRATION
The recommended dose of VELCADE is 1.3 mg/m2/dose administered as a 3 to 5 second bolus intravenous injection twice weekly for 2 weeks (Days 1, 4, 8, and 11) followed by a 10-day rest period (Days 12-21). For extended therapy of more than 8 cycles, VELCADE may be administered on the standard schedule or on a maintenance schedule of once weekly for 4 weeks (Days 1, 8, 15, and 22) followed by a 13-day rest period (Days 23 to 35) (see CLINICAL STUDIES section for a description of dose administration during the trials). At least 72 hours should elapse between consecutive doses of VELCADE.
Dose Modification and Re-initiation of Therapy
VELCADE therapy should be withheld at the onset of any Grade 3 non-hematological or Grade 4 hematological toxicities excluding neuropathy as discussed below (see PRECAUTIONS). Once the symptoms of the toxicity have resolved, VELCADE therapy may be reinitiated at a 25% reduced dose (1.3 mg/m2/dose reduced to 1.0 mg/m2/dose; 1.0 mg/m2/dose reduced to 0.7 mg/m2/dose).
Table 9 contains the recommended dose modification for the management of patients who experience VELCADE related neuropathic pain and/or peripheral neuropathy. Patients with preexisting severe neuropathy should be treated with VELCADE only after careful risk-benefit assessment.
| Severity of Peripheral Neuropathy Signs and Symptoms | Modification of Dose and Regimen | |
|---|---|---|
| Grading based on NCI Common Toxicity Criteria CTCAE v3.0 | ||
| Grade 1 (paresthesias, weakness and/or loss of reflexes) without pain or loss of function | No action | |
| Grade 1 with pain or Grade 2 (interfering with function but not with activities of daily living) | Reduce VELCADE to 1.0 mg/m2 | |
| Grade 2 with pain or Grade 3 (interfering with activities of daily living) | Withhold VELCADE therapy until toxicity resolves. When toxicity resolves reinitiate with a reduced dose of VELCADE at 0.7 mg/m2 and change treatment schedule to once per week. | |
| Grade 4 (Sensory neuropathy which is disabling or motor neuropathy that is life threatening or leads to paralysis) | Discontinue VELCADE | |
Administration Precautions: VELCADE is an antineoplastic. Caution should be used during handling and preparation including careful dose calculation to prevent overdose. The drug quantity contained in one vial (3.5 mg) may exceed the usual single dose required. Proper aseptic technique should be used. Use of gloves and other protective clothing to prevent skin contact is recommended. In clinical trials, local skin irritation was reported in 5% of patients, but extravasation of VELCADE was not associated with tissue damage.
Reconstitution/Preparation for Intravenous Administration: Prior to use, the contents of each vial must be reconstituted with 3.5 mL of normal (0.9%) saline, Sodium Chloride Injection, USP. The reconstituted product should be a clear and colorless solution.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration whenever solution and container permit. If any discoloration or particulate matter is observed, the reconstituted product should not be used.
Stability: Unopened vials of VELCADE are stable until the date indicated on the package when stored in the original package protected from light.
VELCADE contains no antimicrobial preservative. When reconstituted as directed, VELCADE may be stored at 25°C (77°F). Reconstituted VELCADE should be administered within 8 hours of preparation. The reconstituted material may be stored in the original vial and/or the syringe prior to administration. The product may be stored for up to 8 hours in a syringe; however total storage time for the reconstituted material must not exceed 8 hours when exposed to normal indoor lighting.
HOW SUPPLIED
VELCADE® (bortezomib) for Injection is supplied as individually cartoned 10 mL vials containing 3.5 mg of bortezomib as a white to off-white cake or powder.
NDC 63020-049-01
3.5 mg single dose vial
STORAGE
Unopened vials may be stored at controlled room temperature 25°C (77°F); excursions permitted from 15 to 30°C (59 to 86°F) [see USP Controlled Room Temperature]. Retain in original package to protect from light.
Caution: Rx only
U.S. Patents: 5,780,454; 6,083,903; 6,297,217; 6,617,317; 6,713, 446; 6,747,150 B2
Distributed and Marketed by:
Millennium Pharmaceuticals, Inc.
40 Landsdowne Street
Cambridge, MA 02139
VELCADE, and MILLENNIUM are registered trademarks of Millennium Pharmaceuticals, Inc.
©2006 Millennium Pharmaceuticals, Inc. All rights reserved. Printed in USA.
Issued December 2006
Rev 6: December 2006
References:
- Bladé J, Samson D, Reece D, Apperley J, Bjorkstrand B, Gahrton G et al. Criteria for evaluating disease response and progression in patients with multiple myeloma treated by high- dose therapy and haematopoietic stem cell transplantation. Myeloma Subcommittee of the EBMT. European Group for Blood and Marrow Transplant. British Journal of Haematology 1998;102(5):1115-1123.
- Salmon SE, Haut A, Bonnet JD, Amare M, Weick JK, Durie BG et al. Alternating combination chemotherapy and levamisole improves survival in multiple myeloma: a Southwest Oncology Group Study. Journal of Clinical Oncology 1983;1(8): 453-461.
- Cheson BD, Horning SJ, Coiffier B, Shipp MA, Fisher RI, Connors JM et al. Report of an international workshop to standardize response criteria for non-Hodgkin's lymphomas. NCI Sponsored International Working Group. Journal of Clinical Oncology 1999; 17 (4):1244.
VELCADE® (bortezomib) for Injection
PATIENT INFORMATION
VELCADE is intended for use under the guidance and supervision of a healthcare professional. Please discuss the possibility of the following side effects with your doctor:
Effects on Ability to Drive or Operate Machinery or Impairment of Mental Ability:
VELCADE may cause tiredness, dizziness, fainting, or blurred vision. Do not drive any vehicle or operate any dangerous tools or machinery if you experience these side effects. Even if you have not felt these effects previously, you must still be cautious.
Pregnancy/Nursing:
Please use effective contraceptive measures to prevent pregnancy during treatment with VELCADE. It is advised that you are not given VELCADE if you are pregnant. You must make sure that you do not become pregnant while receiving VELCADE, but if you do, inform your doctor immediately. It is advised that you do not breast feed while you are receiving VELCADE. If you wish to restart breast feeding after your VELCADE treatment, you must discuss this with your doctor or nurse, who will tell you when it is safe to do so.
Dehydration/Hypotension:
Following the use of VELCADE therapy, you may experience vomiting and/or diarrhea. Drink plenty of fluids. Speak with your doctor if these symptoms occur about what you should do to control or manage these symptoms. If you experience symptoms of dizziness or light-headedness, consult a healthcare professional. Seek immediate medical attention if you experience fainting spells.
Concomitant Medications:
Please speak with your doctor about any other medication you are currently taking. Your doctor will want to be aware of any other medications.
Diabetic Patients:
If you are a patient on oral antidiabetic medication while receiving VELCADE treatment, please check your blood sugar level frequently. Please call your doctor if you notice an unusual change.
Peripheral Neuropathy:
Contact your doctor if you experience new or worsening symptoms of peripheral neuropathy such as tingling, numbness, pain, a burning feeling in the feet or hands, or weakness in your arms or legs.
Herpes zoster (Shingles):
Contact your doctor if you develop a rash.
Heart Failure and Lung Disease:
Contact your doctor if you experience shortness of breath, cough, or swelling of the feet, ankles, or legs.
Millennium Pharmaceuticals, Inc.
40 Landsdowne Street
Cambridge, MA 02139
VELCADE, and MILLENNIUM are registered trademarks of Millennium Pharmaceuticals, Inc.
©2006 Millennium Pharmaceuticals, Inc. All rights reserved. Printed in USA.
Issued December 2006
Rev 6
| VELCADE (bortezomib) | ||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
|
||||||||||||||||||||||||
Revised: 12/2006Millennium Pharmaceuticals, Inc.