aldoril (methyldopa and hydrochlorothiazide) tablet, film coated
[MERCK and CO., Inc.]
WARNING
This fixed combination drug is not indicated for initial therapy of hypertension. Hypertension requires therapy titrated to the individual patient. If the fixed combination represents the dosage so determined, its use may be more convenient in patient management. The treatment of hypertension is not static, but must be re-evaluated as conditions in each patient warrant.
DESCRIPTION
ALDORIL1 (Methyldopa-Hydrochlorothiazide) combines two antihypertensives: methyldopa and hydrochlorothiazide.
- 1
- Registered trademark of MERCK & CO., Inc. COPYRIGHT © MERCK & CO., Inc., 1986 All rights reserved
Methyldopa
Methyldopa is an antihypertensive and is the L-isomer of alphamethyldopa. It is levo-3-(3,4-dihydroxyphenyl)-2-methylalanine. Its empirical formula is C10H13NO4, with a molecular weight of 211.22, and its structural formula is:
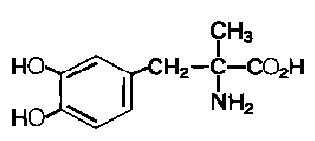
Methyldopa is a white to yellowish white, odorless fine powder, and is soluble in water.
Hydrochlorothiazide
Hydrochlorothiazide is a diuretic and antihypertensive. It is the 3,4-dihydro derivative of chlorothiazide. Its chemical name is 6-chloro-3,4-dihydro-2H- 1,2,4-benzothiadiazine-7-sulfonamide 1,1-dioxide. Its empirical formula is C7H8ClN3O4S2 and its structural formula is:
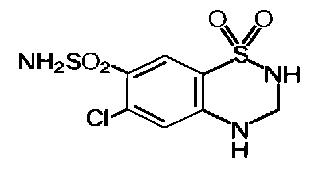
Hydrochlorothiazide is a white, or practically white, crystalline powder with a molecular weight of 297.74, which is slightly soluble in water, but freely soluble in sodium hydroxide solution.
ALDORIL is supplied as tablets in four strengths for oral use:
ALDORIL 15, contains 250 mg of methyldopa and 15 mg of hydrochlorothiazide.
ALDORIL 25, contains 250 mg of methyldopa and 25 mg of hydrochlorothiazide.
ALDORIL D30, contains 500 mg of methyldopa and 30 mg of hydrochlorothiazide.
ALDORIL D50, contains 500 mg of methyldopa and 50 mg of hydrochlorothiazide.
Each tablet contains the following inactive ingredients: calcium disodium edetate, calcium phosphate, cellulose, citric acid, colloidal silicon dioxide, ethylcellulose, guar gum, hydroxypropyl methylcellulose, magnesium stearate, propylene glycol, talc, and titanium dioxide. ALDORIL 15 and ALDORIL D30 also contain iron oxide.
CLINICAL PHARMACOLOGY
Methyldopa
Methyldopa is an aromatic-amino-acid decarboxylase inhibitor in animals and in man. Although the mechanism of action has yet to be conclusively demonstrated, the antihypertensive effect of methyldopa probably is due to its metabolism to alpha-methylnorepinephrine, which then lowers arterial pressure by stimulation of central inhibitory alpha-adrenergic receptors, false neurotransmission, and/or reduction of plasma renin activity. Methyldopa has been shown to cause a net reduction in the tissue concentration of serotonin, dopamine, norepinephrine, and epinephrine.
Only methyldopa, the L-isomer of alpha-methyldopa, has the ability to inhibit dopa decarboxylase and to deplete animal tissues of norepinephrine. In man, the antihypertensive activity appears to be due solely to the L-isomer. About twice the dose of the racemate (DL-alpha-methyldopa) is required for equal antihypertensive effect.
Methyldopa has no direct effect on cardiac function and usually does not reduce glomerular filtration rate, renal blood flow, or filtration fraction. Cardiac output usually is maintained without cardiac acceleration. In some patients the heart rate is slowed.
Normal or elevated plasma renin activity may decrease in the course of methyldopa therapy.
Methyldopa reduces both supine and standing blood pressure. It usually produces highly effective lowering of the supine pressure with infrequent symptomatic postural hypotension. Exercise hypotension and diurnal blood pressure variations rarely occur.
Hydrochlorothiazide
The mechanism of the antihypertensive effect of thiazides is unknown. Hydrochlorothiazide does not usually affect normal blood pressure.
Hydrochlorothiazide affects the distal renal tubular mechanism of electrolyte reabsorption. At maximal therapeutic dosage all thiazides are approximately equal in their diuretic efficacy.
Hydrochlorothiazide increases excretion of sodium and chloride in approximately equivalent amounts. Natriuresis may be accompanied by some loss of potassium and bicarbonate.
After oral use diuresis begins within 2 hours, peaks in about 4 hours and lasts about 6 to 12 hours.
Pharmacokinetics and Metabolism
Methyldopa
The maximum decrease in blood pressure occurs four to six hours after oral dosage. Once an effective dosage level is attained, a smooth blood pressure response occurs in most patients in 12 to 24 hours. After withdrawal, blood pressure usually returns to pretreatment levels within 24-48 hours.
Methyldopa is extensively metabolized. The known urinary metabolites are: α-methyldopa mono-0-sulfate; 3-0-methyl-α-methyldopa; 3,4-dihydroxyphenylacetone;α-methyldopamine; 3-0-methyl-α-methyldopamine and their conjugates.
Approximately 70 percent of the drug which is absorbed is excreted in the urine as methyldopa and its mono-0-sulfate conjugate. The renal clearance is about 130 mL/min in normal subjects and is diminished in renal insufficiency. The plasma half-life of methyldopa is 105 minutes. After oral doses, excretion is essentially complete in 36 hours.
Methyldopa crosses the placental barrier, appears in cord blood, and appears in breast milk.
Hydrochlorothiazide
Hydrochlorothiazide is not metabolized but is eliminated rapidly by the kidney. When plasma levels have been followed for at least 24 hours, the plasma half-life has been observed to vary between 5.6 and 14.8 hours. At least 61 percent of the oral dose is eliminated unchanged within 24 hours. Hydrochlorothiazide crosses the placental but not the blood-brain barrier and is excreted in breast milk.
INDICATION AND USAGE
Hypertension ( see box warning).
CONTRAINDICATIONS
ALDORIL is contraindicated in patients:
- with active hepatic disease, such as acute hepatitis and active cirrhosis
- with liver disorders previously associated with methyldopa therapy (see WARNINGS)
- with anuria
- with hypersensitivity to methyldopa, or to hydrochlorothiazide or other sulfonamide-derived drugs
- on therapy with monoamine oxidase (MAO) inhibitors.
WARNINGS
Methyldopa
It is important to recognize that a positive Coombs test, hemolytic anemia, and liver disorders may occur with methyldopa therapy. The rare occurrences of hemolytic anemia or liver disorders could lead to potentially fatal complications unless properly recognized and managed. Read this section carefully to understand these reactions.
With prolonged methyldopa therapy, 10 to 20 percent of patients develop a positive direct Coombs test which usually occurs between 6 and 12 months of methyldopa therapy. Lowest incidence is at daily dosage of 1 g or less. This on rare occasions may be associated with hemolytic anemia, which could lead to potentially fatal complications. One cannot predict which patients with a positive direct Coombs test may develop hemolytic anemia.
Prior existence or development of a positive direct Coombs test is not in itself a contraindication to use of methyldopa. If a positive Coombs test develops during methyldopa therapy, the physician should determine whether hemolytic anemia exists and whether the positive Coombs test may be a problem. For example, in addition to a positive direct Coombs test there is less often a positive indirect Coombs test which may interfere with cross matching of blood.
Before treatment is started it is desirable to do a blood count (hematocrit, hemoglobin, or red cell count) for a baseline or to establish whether there is anemia. Periodic blood counts should be done during therapy to detect hemolytic anemia. It may be useful to do a direct Coombs test before therapy and at 6 and 12 months after the start of therapy.
If Coombs-positive hemolytic anemia occurs, the cause may be methyldopa and the drug should be discontinued. Usually the anemia remits promptly. If not, corticosteroids may be given and other causes of anemia should be considered. If the hemolytic anemia is related to methyldopa, the drug should not be reinstituted.
When methyldopa causes Coombs positivity alone or with hemolytic anemia, the red cell is usually coated with gamma globulin of the IgG (gamma G) class only. The positive Coombs test may not revert to normal until weeks to months after methyldopa is stopped.
Should the need for transfusion arise in a patient receiving methyldopa, both a direct and an indirect Coombs test should be performed. In the absence of hemolytic anemia, usually only the direct Coombs test will be positive. A positive direct Coombs test alone will not interfere with typing or cross matching. If the indirect Coombs test is also positive, problems may arise in the major cross match and the assistance of a hematologist or transfusion expert will be needed.
Occasionally, fever has occurred within the first three weeks of methyldopa therapy, associated in some cases with eosinophilia or abnormalities in one or more liver function tests, such as serum alkaline phosphatase, serum transaminases (SGOT, SGPT), bilirubin, and prothrombin time. Jaundice, with or without fever, may occur with onset usually within the first two to three months of therapy. In some patients the findings are consistent with those of cholestasis. In others the findings are consistent with hepatitis and hepatocellular injury.
Rarely, fatal hepatic necrosis has been reported after use of methyldopa. These hepatic changes may represent hypersensitivity reactions. Periodic determination of hepatic function should be done particularly during the first 6 to 12 weeks of therapy or whenever an unexplained fever occurs. If fever, abnormalities in liver function tests, or jaundice appear, stop therapy with methyldopa. If caused by methyldopa, the temperature and abnormalities in liver function characteristically have reverted to normal when the drug was discontinued. Methyldopa should not be reinstituted in such patients.
Rarely, a reversible reduction of the white blood cell count with a primary effect on the granulocytes has been seen. The granulocyte count returned promptly to normal on discontinuance of the drug. Rare cases of granulocytopenia have been reported. In each instance, upon stopping the drug, the white cell count returned to normal. Reversible thrombocytopenia has occurred rarely.
Hydrochlorothiazide
Use with caution in severe renal disease. In patients with renal disease, thiazides may precipitate azotemia. Cumulative effects of the drug may develop in patients with impaired renal function.
Thiazides should be used with caution in patients with impaired hepatic function or progressive liver disease, since minor alterations of fluid and electrolyte balance may precipitate hepatic coma.
Thiazides may add to or potentiate the action of other antihypertensive drugs.
Sensitivity reactions may occur in patients with or without a history of allergy or bronchial asthma.
The possibility of exacerbation or activation of systemic lupus erythematosus has been reported.
Lithium generally should not be given with diuretics (see PRECAUTIONS, Drug Interactions).
PRECAUTIONS
General
Methyldopa
Methyldopa should be used with caution in patients with a history of previous liver disease or dysfunction (see WARNINGS).
Some patients taking methyldopa experience clinical edema or weight gain which may be controlled by use of a diuretic. Methyldopa should not be continued if edema progresses or signs of heart failure appear.
Hypertension has recurred occasionally after dialysis in patients given methyldopa because the drug is removed by this procedure.
Rarely, involuntary choreoathetotic movements have been observed during therapy with methyldopa in patients with severe bilateral cerebrovascular disease. Should these movements occur, stop therapy.
Hydrochlorothiazide
All patients receiving diuretic therapy should be observed for evidence of fluid or electrolyte imbalance: namely; hyponatremia, hypochloremic alkalosis, and hypokalemia. Serum and urine electrolyte determinations are particularly important when the patient is vomiting excessively or receiving parenteral fluids. Warning signs or symptoms of fluid and electrolyte imbalance, irrespective of cause, include dryness of mouth, thirst, weakness, lethargy, drowsiness, restlessness, confusion, seizures, muscle pains or cramps, muscular fatigue, hypotension, oliguria, tachycardia, and gastrointestinal disturbances such as nausea and vomiting.
Hypokalemia may develop, especially after prolonged therapy or when severe cirrhosis is present (see CONTRAINDICATIONS and WARNINGS).
Interference with adequate oral electrolyte intake will also contribute to hypokalemia. Hypokalemia may cause cardiac arrhythmia and may also sensitize or exaggerate the response of the heart to the toxic effects of digitalis (e.g., increased ventricular irritability). Hypokalemia may be avoided or treated by use of potassium sparing diuretics or potassium supplements such as foods with a high potassium content.
Although any chloride deficit is generally mild and usually does not require specific treatment except under extraordinary circumstances (as in liver disease or renal disease), chloride replacement may be required in the treatment of metabolic alkalosis.
Dilutional hyponatremia may occur in edematous patients in hot weather; appropriate therapy is water restriction, rather than administration of salt, except in rare instances when the hyponatremia is life-threatening. In actual salt depletion appropriate replacement is the therapy of choice.
Hyperuricemia may occur or acute gout may be precipitated in certain patients receiving thiazides.
In diabetic patients dosage adjustment of insulin or oral hypoglycemic agents may be required. Hyperglycemia may occur with thiazide diuretics. Thus latent diabetes mellitus may become manifest during thiazide therapy.
The antihypertensive effects of the drug may be enhanced in the postsympathectomy patient.
If progressive renal impairment becomes evident, consider withholding or discontinuing diuretic therapy.
Thiazides have been shown to increase the urinary excretion of magnesium; this may result in hypomagnesemia.
Thiazides may decrease urinary calcium excretion. Thiazides may cause intermittent and slight elevation of serum calcium in the absence of known disorders of calcium metabolism. Marked hypercalcemia may be evidence of hidden hyperparathyroidism. Thiazides should be discontinued before carrying out tests for parathyroid function.
Increases in cholesterol and triglyceride levels may be associated with thiazide diuretic therapy.
Laboratory Tests
Methyldopa
Blood count, Coombs test and liver function test, are recommended before initiating therapy and at periodic intervals (see WARNINGS).
Hydrochlorothiazide
Periodic determination of serum electrolytes to detect possible electrolyte imbalance should be done at appropriate intervals.
Drug Interactions
Methyldopa
When methyldopa is used with other antihypertensive drugs, potentiation of antihypertensive effect may occur. Patients should be followed carefully to detect side reactions or unusual manifestations of drug idiosyncrasy.
Patients may require reduced doses of anesthetics when on methyldopa. If hypotension does occur during anesthesia, it usually can be controlled by vasopressors. The adrenergic receptors remain sensitive during treatment with methyldopa.
When methyldopa and lithium are given concomitantly the patient should be carefully monitored for symptoms of lithium toxicity. Read the prescribing information for lithium preparations.
Several studies demonstrate a decrease in the bioavailability of methyldopa when it is ingested with ferrous sulfate or ferrous gluconate. This may adversely affect blood pressure control in patients treated with methyldopa. Coadministration of methyldopa with ferrous sulfate or ferrous gluconate is not recommended.
Monoamine oxidase (MAO) inhibitors: See CONTRAINDICATIONS.
Hydrochlorothiazide
When given concurrently the following drugs may interact with thiazide diuretics.
Alcohol, barbiturates, or narcotics — potentiation of orthostatic hypotension may occur.
Antidiabetic drugs (oral agents and insulin) — dosage adjustment of the antidiabetic drug may be required.
Other antihypertensive drugs — additive effect or potentiation.
Cholestyramine and colestipol resins — Absorption of hydrochlorothiazide is impaired in the presence of anionic exchange resins. Single doses of either cholestyramine or colestipol resins bind the hydrochlorothiazide and reduce its absorption from the gastrointestinal tract by up to 85 and 43 percent, respectively.
Corticosteroids, ACTH — intensified electrolyte depletion, particularly hypokalemia.
Pressor amines (e.g., norepinephrine) — possible decreased response to pressor amines but not sufficient to preclude their use.
Skeletal muscle relaxants, nondepolarizing (e.g., tubocurarine) — possible increased responsiveness to the muscle relaxant.
Lithium — generally should not be given with diuretics. Diuretic agents reduce the renal clearance of lithium and add a high risk of lithium toxicity. Refer to the package insert for lithium preparations before use of such preparations with ALDORIL.
Non-steroidal Anti-inflammatory Drugs — In some patients, the administration of a non-steroidal anti-inflammatory agent can reduce the diuretic, natriuretic, and antihypertensive effects of loop, potassium-sparing and thiazide diuretics. Therefore, when ALDORIL and non-steroidal anti-inflammatory agents are used concomitantly, the patient should be observed closely to determine if the desired effect of the diuretic is obtained.
Drug/Laboratory Test Interactions
Methyldopa
Methyldopa may interfere with measurement of: urinary uric acid by the phosphotungstate method, serum creatinine by the alkaline picrate method, and SGOT by colorimetric methods. Interference with spectrophotometric methods for SGOT analysis has not been reported.
Since methyldopa causes fluorescence in urine samples at the same wave lengths as catecholamines, falsely high levels of urinary catecholamines may be reported. This will interfere with the diagnosis of pheochromocytoma. It is important to recognize this phenomenon before a patient with a possible pheochromocytoma is subjected to surgery. Methyldopa does not interfere with measurement of VMA (vanillylmandelic acid), a test for pheochromocytoma, by those methods which convert VMA to vanillin. Methyldopa is not recommended for the treatment of patients with pheochromocytoma. Rarely, when urine is exposed to air after voiding, it may darken because of breakdown of methyldopa or its metabolites.
Hydrochlorothiazide
Thiazides should be discontinued before carrying out tests for parathyroid function (see PRECAUTIONS, General).
Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term studies in animals have not been performed to evaluate the effects upon fertility, mutagenic or carcinogenic potential of the combination.
Methyldopa
No evidence of a tumorigenic effect was seen when methyldopa was given for two years to mice at doses up to 1800 mg/kg/day or to rats at doses up to 240 mg/kg/day (30 and 4 times the maximum recommended human dose in mice and rats, respectively, when compared on the basis of body weight; 2.5 and 0.6 times the maximum recommended human dose in mice and rats, respectively, when compared on the basis of body surface area; calculations assume a patient weight of 50 kg).
Methyldopa was not mutagenic in the Ames Test and did not increase chromosomal aberration or sister chromatid exchanges in Chinese hamster ovary cells. These in vitro studies were carried out both with and without exogenous metabolic activation.
Fertility was unaffected when methyldopa was given to male and female rats at 100 mg/kg/day (1.7 times the maximum daily human dose when compared on the basis of body weight; 0.2 times the maximum daily human dose when compared on the basis of body surface area). Methyldopa decreased sperm count, sperm motility, the number of late spermatids and the male fertility index when given to male rats at 200 and 400 mg/kg/day (3.3 and 6.7 times the maximum daily human dose when compared on the basis of body weight; 0.5 and 1 times the maximum daily human dose when compared on the basis of body surface area).
Hydrochlorothiazide
Two-year feeding studies in mice and rats conducted under the auspices of the National Toxicology Program (NTP) uncovered no evidence of a carcinogenic potential of hydrochlorothiazide in female mice (at doses of up to approximately 600 mg/kg/day) or in male and female rats (at doses of up to approximately 100 mg/kg/day). The NTP, however, found equivocal evidence for hepatocarcinogenicity in male mice.
Hydrochlorothiazide was not genotoxic in vitro in the Ames mutagenicity assay of Salmonella typhimurium strains TA 98, TA 100, TA 1535, TA 1537, and TA 1538 and in the Chinese Hamster Ovary (CHO) test for chromosomal aberrations, or in vivo in assays using mouse germinal cell chromosomes, Chinese hamster bone marrow chromosomes, and the Drosophila sex-linked recessive lethal trait gene. Positive test results were obtained only in the in vitro CHO Sister Chromatid Exchange (clastogenicity) and in the Mouse Lymphoma Cell (mutagenicity) assays, using concentrations of hydrochlorothiazide from 43 to 1300 µg/mL, and in the Aspergillus nidulans non-disjunction assay at an unspecified concentration.
Hydrochlorothiazide had no adverse effects on the fertility of mice and rats of either sex in studies wherein these species were exposed, via their diet, to doses of up to 100 and 4 mg/kg, respectively, prior to conception and throughout gestation.
Pregnancy
Use of diuretics during normal pregnancy is inappropriate and exposes mother and fetus to unnecessary hazard. Diuretics do not prevent development of toxemia of pregnancy and there is no satisfactory evidence that they are useful in the treatment of toxemia.
Teratogenic Effects
Pregnancy Category C: Animal reproduction studies have not been conducted with ALDORIL. It is also not known whether ALDORIL can affect reproduction capacity or can cause fetal harm when given to a pregnant woman. ALDORIL should be given to a pregnant woman only if clearly needed.
Hydrochlorothiazide: Studies in which hydrochlorothiazide was orally administered to pregnant mice and rats during their respective periods of major organogenesis at doses up to 3000 and 1000 mg hydrochlorothiazide/kg, respectively, provided no evidence of harm to the fetus. There are, however, no adequate and well-controlled studies in pregnant women.
Methyldopa: Reproduction studies performed with methyldopa at oral doses up to 1000 mg/kg in mice, 200 mg/kg in rabbits and 100 mg/kg in rats revealed no evidence of harm to the fetus. These doses are 16.6 times, 3.3 times and 1.7 times, respectively, the maximum daily human dose when compared on the basis of body weight; 1.4 times, 1.1 times and 0.2 times, respectively, when compared on the basis of body surface area; calculations assume a patient weight of 50 kg. There are, however, no adequate and well-controlled studies in pregnant women in the first trimester of pregnancy. Because animal reproduction studies are not always predictive of human response, methyldopa should be used during pregnancy only if clearly needed.
Published reports of the use of methyldopa during all trimesters indicate that if this drug is used during pregnancy the possibility of fetal harm appears remote. In five studies, three of which were controlled, involving 332 pregnant hypertensive women, treatment with methyldopa was associated with an improved fetal outcome. The majority of these women were in the third trimester when methyldopa therapy was begun.
In one study, women who had begun methyldopa treatment between weeks 16 and 20 of pregnancy gave birth to infants whose average head circumference was reduced by a small amount (34.2 ± 1.7 cm vs. 34.6 ± 1.3 cm [mean ± 1 S.D.]). Long term follow-up of 195 (97.5%) of the children born to methyldopa-treated pregnant women (including those who began treatment between weeks 16 and 20) failed to uncover any significant adverse effect on the children. At four years of age, the developmental delay commonly seen in children born to hypertensive mothers was less evident in those whose mothers were treated with methyldopa during pregnancy than those whose mothers were untreated. The children of the treated group scored consistently higher than the children of the untreated group on five major indices of intellectual and motor development. At age 7 and one-half developmental scores and intelligence indices showed no significant differences in children of treated or untreated hypertensive women.
Nonteratogenic Effects
Thiazides cross the placental barrier and appear in cord blood. There is a risk of fetal or neonatal jaundice, thrombocytopenia, and possibly other adverse reactions that have occurred in adults.
Nursing Mothers
Methyldopa and thiazides appear in breast milk. Therefore, because of the potential for serious adverse reactions in nursing infants from hydrochlorothiazide, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Geriatric Use
Clinical studies of ALDORIL did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
This drug is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function.
Pediatric Use
Safety and effectiveness of ALDORIL in pediatric patients have not been established.
ADVERSE REACTIONS
The following adverse reactions have been reported and, within each category, are listed in order of decreasing severity.
Methyldopa
Sedation, usually transient, may occur during the initial period of therapy or whenever the dose is increased. Headache, asthenia, or weakness may be noted as early and transient symptoms. However, significant adverse effects due to methyldopa have been infrequent and this agent usually is well tolerated.
Cardiovascular: Aggravation of angina pectoris, congestive heart failure, prolonged carotid sinus hypersensitivity, orthostatic hypotension (decrease daily dosage), edema or weight gain, bradycardia.
Digestive: Pancreatitis, colitis, vomiting, diarrhea, sialadenitis, sore or “black” tongue, nausea, constipation, distention, flatus, dryness of mouth.
Endocrine: Hyperprolactinemia.
Hematologic: Bone marrow depression, leukopenia, granulocytopenia, thrombocytopenia, hemolytic anemia; positive tests for antinuclear antibody, LE cells, and rheumatoid factor, positive Coombs test.
Hepatic: Liver disorders including hepatitis, jaundice, abnormal liver function tests (see WARNINGS).
Hypersensitivity: Myocarditis, pericarditis, vasculitis, lupus-like syndrome, drug-related fever, eosinophilia.
Nervous System/Psychiatric: Parkinsonism, Bell's palsy, decreased mental acuity, involuntary choreoathetotic movements, symptoms of cerebrovascular insufficiency, psychic disturbances including nightmares and reversible mild psychoses or depression, headache, sedation, asthenia or weakness, dizziness, lightheadedness, paresthesias.
Metabolic: Rise in BUN.
Musculoskeletal: Arthralgia, with or without joint swelling; myalgia.
Respiratory: Nasal stuffiness.
Skin: Toxic epidermal necrolysis, rash.
Urogenital: Amenorrhea, breast enlargement, gynecomastia, lactation, impotence, decreased libido.
Hydrochlorothiazide
Body as a Whole: Weakness.
Cardiovascular: Hypotension including orthostatic hypotension (may be aggravated by alcohol, barbiturates, narcotics or antihypertensive drugs).
Digestive: Pancreatitis, jaundice (intrahepatic cholestatic jaundice), diarrhea, vomiting, sialadenitis, cramping, constipation, gastric irritation, nausea, anorexia.
Hematologic: Aplastic anemia, agranulocytosis, leukopenia, hemolytic anemia, thrombocytopenia.
Hypersensitivity: Anaphylactic reactions, necrotizing angiitis (vasculitis and cutaneous vasculitis), respiratory distress including pneumonitis and pulmonary edema, photosensitivity, fever, urticaria, rash, purpura.
Metabolic: Electrolyte imbalance (see PRECAUTIONS), hyperglycemia, glycosuria, hyperuricemia.
Musculoskeletal: Muscle spasm.
Nervous System/Psychiatric: Vertigo, paresthesias, dizziness, headache, restlessness.
Renal: Renal failure, renal dysfunction, interstitial nephritis. (See WARNINGS.)
Skin: Erythema multiforme including Stevens-Johnson syndrome, exfoliative dermatitis including toxic epidermal necrolysis, alopecia.
Special Senses: Transient blurred vision, xanthopsia.
Urogenital: Impotence.
OVERDOSAGE
Acute overdosage may produce acute hypotension with other responses attributable to brain and gastrointestinal malfunction (excessive sedation, weakness, bradycardia, dizziness, lightheadedness, constipation, distention, flatus, diarrhea, nausea, vomiting).
In the event of overdosage, symptomatic and supportive measures should be employed. When ingestion is recent, gastric lavage or emesis may reduce absorption. When ingestion has been earlier, infusions may be helpful to promote urinary excretion. Otherwise, management includes special attention to cardiac rate and output, blood volume, electrolyte balance, paralytic ileus, urinary function and cerebral activity.
Sympathomimetic drugs [e.g., levarterenol, epinephrine, ARAMINE1 (Metaraminol Bitartrate)] may be indicated. Methyldopa is dialyzable. The degree to which hydrochlorothiazide is removed by hemodialysis has not been established.
The oral LD50 of methyldopa is greater than 1.5 g/kg in both the mouse and the rat. The oral LD50 of hydrochlorothiazide is greater than 10 g/kg in the mouse and rat.
DOSAGE AND ADMINISTRATION
DOSAGE MUST BE INDIVIDUALIZED, AS DETERMINED BY TITRATION OF THE INDIVIDUAL COMPONENTS ( see box warning). Once the patient has been successfully titrated, ALDORIL may be substituted if the previously determined titrated doses are the same as in the combination. The usual starting dosage is one tablet of ALDORIL 15 two or three times a day or one tablet of ALDORIL 25 two times a day. Alternatively, one tablet of ALDORIL D30 or ALDORIL D50 once daily may be used. Hydrochlorothiazide doses greater than 50 mg daily should be avoided.
Hydrochlorothiazide can be given at doses of 12.5 to 50 mg per day when used alone. The usual daily dosage of methyldopa is 500 mg to 2 g. To minimize the sedation associated with methyldopa, start dosage increases in the evening. The maximum recommended daily dose of methyldopa is 3 g.
Occasionally tolerance to methyldopa may occur, usually between the second and third month of therapy. Additional separate doses of methyldopa or replacement of ALDORIL with single entity agents is necessary until the new effective dose ratio is re-established by titration. If ALDORIL does not adequately control blood pressure, additional doses of other agents may be given. When ALDORIL is given with antihypertensives other than thiazides, the initial dosage of methyldopa should be limited to 500 mg daily in divided doses and the dose of these other agents may need to be adjusted to effect a smooth transition.
Since both components of ALDORIL have a relatively short duration of action, withdrawal is followed by return of hypertension usually within 48 hours. This is not complicated by an overshoot of blood pressure.
Since methyldopa is largely excreted by the kidney, patients with impaired renal function may respond to smaller doses. Syncope in older patients may be related to an increased sensitivity and advanced arteriosclerotic vascular disease. This may be avoided by lower doses. ( See PRECAUTIONS, Geriatric Use.)
HOW SUPPLIED
No. 3294 — Tablets ALDORIL 15 are salmon, round, film coated tablets, coded MSD 423 on one side and ALDORIL on the other. Each tablet contains 250 mg of methyldopa and 15 mg of hydrochlorothiazide. They are supplied as follows:
NDC 0006-0423-68 bottles of 100.
No. 3295 — Tablets ALDORIL 25 are white, round, film coated tablets, coded MSD 456 on one side and ALDORIL on the other. Each tablet contains 250 mg of methyldopa and 25 mg of hydrochlorothiazide. They are supplied as follows:
NDC 0006-0456-68 bottles of 100
NDC 0006-0456-82 bottles of 1000.
No. 3362 — Tablets ALDORIL D30 are salmon, oval, film coated tablets, coded MSD 694 on one side and ALDORIL on the other. Each tablet contains 500 mg of methyldopa and 30 mg of hydrochlorothiazide. They are supplied as follows:
NDC 0006-0694-68 bottles of 100.
No. 3363 — Tablets ALDORIL D50 are white, oval, film coated tablets, coded MSD 935 on one side and ALDORIL on the other. Each tablet contains 500 mg of methyldopa and 50 mg of hydrochlorothiazide. They are supplied as follows:
NDC 0006-0935-68 bottles of 100.
Storage
Keep container tightly closed. Protect from light, moisture, freezing, –20°C (–4°F) and store at controlled room temperature, 15-30°C (59-86°F).
MERCK& CO., Inc., Whitehouse Station, NJ 08889, USA
Issued February 2004
Printed in USA
7843556
| ALDORIL (methyldopa and hydrochlorothiazide) | ||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
| ALDORIL (methyldopa and hydrochlorothiazide) | |||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||
| ALDORIL (methyldopa and hydrochlorothiazide) | ||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
| ALDORIL (methyldopa and hydrochlorothiazide) | |||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||||||||||||||
Revised: 03/2006