HELIDAC THERAPY
-
bismuth subsalicylate/metronidazole/tetracycline hydrochloride
Prometheus Laboratories Inc.
----------
HELIDAC® Therapy[Prometheus Laboratories Inc.]
To reduce the development of drug-resistant bacteria and maintain the effectiveness of HELIDAC Therapy and other antibacterial drugs, HELIDAC Therapy should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria.
PHARMACIST INFORMATION & COUNSELING AID
Not intended for distribution to Patient
- This Counseling Aid contains concise information for the Pharmacist and is meant to aid in counseling; please refer to the attached Package Insert for complete prescribing information.
- There is a detailed PATIENT INFORMATION BOOKLET contained in this package which should be read by the patient prior to initiating therapy.
- Instructions for opening the enclosed dosing blister cards can be found on the top of this package.
For Your Information
- Helicobacter pylori (H. pylori) infection has been found to play a primary role in the pathogenesis of duodenal ulcers, and is considered the causative organism in 80% to 95% of patients with duodenal ulcers.
- The components of HELIDAC Therapy [bismuth subsalicylate (BSS), metronidazole (MTZ), and tetracycline hydrochloride (TCN)] are indicated for the treatment of patients with an active duodenal ulcer associated with H. pylori infection. The eradication of H. pylori has been demonstrated to reduce the risk of duodenal ulcer recurrence. Appropriate doses of an H2 antagonist indicated for the treatment of active duodenal ulcer should be prescribed for ulcer healing.
- HELIDAC Therapy is a combination of three antimicrobial agents: bismuth subsalicylate, metronidazole, and tetracycline hydrochloride. Clinical trials using this combination have demonstrated H. pylori eradication in up to 82% of patients with a duodenal ulcer. Please note: bismuth subsalicylate is used in this combination for its antimicrobial properties and not for symptomatic relief of upset stomach.
- Clinical data show that eradication of H. pylori is directly related to compliance. This therapy has been designed to enhance compliance and contains 14 blister cards, one for each day of the 14-day treatment plan, with each card divided into the 4 daily doses. The therapy also contains a patient-oriented information booklet and patient reminders.
Information To Share With Your Patient
- Scientists have discovered that most ulcers are caused by an infection from a specific germ called H. pylori.
- The medicines in this therapy have been demonstrated to treat the infection in the majority of cases when taken correctly. Treating the infection is important to reduce the risk of the ulcer coming back.
- Each pill of every dose is important. Studies have shown that taking all this medicine is very important to eradicate all the ulcer-causing germs. If doses are skipped or treatment is stopped early, some of these germs may not be eradicated and another ulcer can develop.
Dosing and Administration
It may be useful to open the therapy and explain dosing while showing the patient one of the dosing blister cards.
- Each dose includes 4 pills: 2 pink round chewable tablets (bismuth subsalicylate), 1 white round tablet (metronidazole), and 1 black and yellow capsule (tetracycline hydrochloride).
- Take 1 dose (all 4 pills) 4 times a day – at mealtimes and bedtime.
- Chew and swallow the 2 pink tablets.
Then swallow the white tablet and black and yellow capsule whole with a full glass of water (8 ounces).
Remember: Chew-Chew-Swallow-Swallow = 1 dose. - All 4 daily doses are contained on an individual blister card.
- This therapy contains 14 blister cards, one card for each day of the 14-day treatment plan.
- If you miss a dose, do not take a double dose. Instead, make up any missed doses by continuing your normal dosing schedule until the medication is gone. (Please contact prescriber if more than 4 doses are missed.)
- Each dose should be taken with a full glass of water (8 ounces), especially the bedtime dose.*
- Concomitantly prescribed H2 antagonist therapy should be taken as directed.
*To reduce risk of esophageal irritation and ulceration due to tetracycline
OTHER IMPORTANT INFORMATION TO GUIDE YOUR DISCUSSION WITH THE PATIENT
Contraindications:
HELIDAC Therapy is contraindicated in the following patient populations:
- Pregnant or nursing women
- Pediatric patients
- Patients with renal or hepatic impairment
- Patients with known hypersensitivity to bismuth subsalicylate, metronidazole or other nitroimidazole derivatives, or any of the tetracyclines; this product does not contain aspirin, but should not be administered to those patients who have a known allergy to aspirin or salicylates.
Warnings and Precautions (also see Contraindications): The following is a partial list. Please refer to the Package Insert for more complete information.
- Patients should avoid:
- -
- Alcohol during therapy and at least 1 day after completion of all doses due to potential metronidazole effects
- -
- Sun lamps or sun because of possible photosensitivity secondary to tetracycline
- -
- Other medications without first consulting with your pharmacist or prescriber (See Drug Interactions.)
- Administer with caution in patients with central nervous system diseases.
- Administer with caution in elderly patients who may suffer from asymptomatic renal and hepatic dysfunction.
- Bismuth subsalicylate may cause a temporary and harmless darkening of the tongue and/or black stool. This should not be confused with melena (blood in the stool).
Adverse Reactions:
Adverse reactions associated with the individual components of HELIDAC Therapy have been well described and are included in the Package Insert. The most common adverse reactions (≥1.5%) reported in clinical trials where all three components were given concomitantly are as follows: nausea (12.0%), diarrhea (6.8%), abdominal pain (6.8%), melena (3.0%), upper respiratory infection (2.3%), constipation (1.9%), anorexia (1.5%), asthenia (1.5%), vomiting (1.5%), discolored tongue (1.5%), headache (1.5%), dyspepsia (1.5%), and dizziness (1.5%). The majority of the events were related to the gastrointestinal tract, were reversible, and usually did not lead to discontinuation of therapy.
Some other possible adverse reactions include:
- Temporary and harmless darkening of the tongue and/or black stool
- Metallic taste in the mouth
- Temporary darkening of the urine (rare)
- Sore mouth
- Yeast infections in women
As with most medications, rare but serious side effects have been reported with the use of the components contained in HELIDAC Therapy. (See Package Insert.) Patients should be instructed to report any unusual symptoms to their pharmacist or prescriber.
Drug Interactions: See Package Insert for more complete information.
Alcohol: There is a potential for a disulfiram-like interaction with metronidazole. Patients should be warned not to drink alcoholic beverages or alcohol-containing products during therapy and for at least 1 day after the therapy is completed.
Antacids containing aluminum, calcium, or magnesium, and preparations containing iron, zinc, or sodium bicarbonate; or milk or dairy products: Absorption of tetracycline may be impaired when co-administered.
Anticoagulants: Individual components of HELIDAC Therapy have the potential to interact with anticoagulants. Monitoring anticoagulant therapy with appropriate adjustment of the anticoagulant dosage may be warranted if concurrent therapy is instituted. (See Package Insert.)
Antidiabetics: There is a possible enhanced hypoglycemic effect when given with salicylates.
Cimetidine: The simultaneous administration of drugs that decrease microsomal liver enzyme activity, such as cimetidine, may prolong the half-life and decrease plasma clearance of metronidazole.
Oral Contraceptives: As with many antibacterial preparations, concomitant use of HELIDAC Therapy may reduce the effectiveness of estrogen-containing oral contraceptives; breakthrough bleeding may occur. Patients should be advised to use an additional or different form of contraception. Women who become pregnant while taking HELIDAC therapy should be advised to notify their prescriber immediately.
See the Package Insert regarding the following possible, suspected, or confirmed interactions: aspirin, probenecid, sulfinpyrazone, methoxyflurane, penicillin, disulfiram (within 2 weeks), lithium, and microsomal liver enzyme inducers, such as phenytoin or phenobarbital.
In patients stabilized on relatively high doses of lithium, short-term metronidazole therapy has been associated with elevation of serum lithium and, in a few cases, signs of lithium toxicity. Serum lithium and serum creatinine should be obtained several days after beginning metronidazole to detect any increase that may precede clinical symptoms of lithium toxicity.
Although there is an anticipated reduction in tetracycline systemic absorption due to an interaction with bismuth and/or bismuth subsalicylate tablet excipients (calcium carbonate), the relative contribution of systemic versus local antimicrobial activity against H. pylori for these agents has not been established.
PACKAGE INSERT
THESE PRODUCTS ARE INTENDED ONLY FOR USE AS DESCRIBED. The individual products contained in this package should not be used alone or in combination for other purposes. The information described in this labeling concerns only the use of these products as indicated in this combination package. For information on use of the individual components when dispensed as individual medications outside this combined use for treating Helicobacter pylori, please see the package inserts for each individual product.
WARNING
Metronidazole has been shown to be carcinogenic in mice and rats. (See PRECAUTIONS.) Unnecessary use of the drug should be avoided. Its use should be reserved for the conditions described in the INDICATIONS AND USAGE section below.
DESCRIPTION:
HELIDAC Therapy consists of 112 bismuth subsalicylate 262.4-mg chewable tablets, 56 metronidazole 250-mg tablets, USP, and 56 tetracycline hydrochloride 500-mg capsules, USP, for oral administration.
Bismuth subsalicylate chewable tablets: Each pink round tablet contains 262.4 mg bismuth subsalicylate (102 mg salicylate) for oral administration.
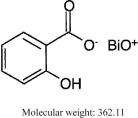
Bismuth subsalicylate is a fine, white, odorless, and tasteless powder that is stable and non-hygroscopic. It is a highly insoluble salt of trivalent bismuth and salicylic acid.
Bismuth subsalicylate is 2-Hydroxybenzoic acid bismuth (3+) salt with the following structural formula:
Inactive Ingredients: Each bismuth subsalicylate chewable tablet contains calcium carbonate, D&C Red No. 27 aluminum lake, flavor, magnesium stearate, mannitol, povidone, saccharin sodium, and talc.
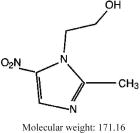
Metronidazole tablets, USP: Each, round, white tablet contains 250 mg metronidazole. Metronidazole is 2-Methyl-5-nitroimidazole-1-ethanol, with the following structural formula:
Inactive Ingredients: Each metronidazole tablet contains colloidal silicon dioxide, crospovidone, stearic acid, magnesium stearate and microcrystalline cellulose.
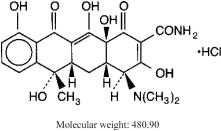
Tetracycline hydrochloride capsules, USP: Each black and yellow capsule contains 500 mg tetracycline hydrochloride. Tetracycline is a yellow, odorless, crystalline powder. Tetracycline is stable in air but exposure to strong sunlight causes it to darken. Its potency is affected in solutions of pH below 2 and is rapidly destroyed by alkali hydroxide solutions. Tetracycline is very slightly soluble in water, freely soluble in dilute acid and in alkali hydroxide solutions, sparingly soluble in alcohol, and practically insoluble in chloroform and ether.
Tetracycline hydrochloride is (4S,4aS,5aS,6S,12aS)-4-(Dimethylamino)-1,4,4a,5,5a,6,11,12a-octahydro-3,6,10,12,12a-pentahydroxy-6-methyl-1,11-dioxo-2-naphthacenecarboxamide monohydrochloride, with the following structural formula:
Inactive Ingredients: Each tetracycline hydrochloride capsule contains lactose, magnesium stearate and sodium lauryl sulfate; D & C yellow no.10, FD & C blue No 1, FD & C red no. 40, gelatin and titanium dioxide. It may also contain benzyl alcohol, butylparaben, edetate calcium disodium, FD & C yellow no. 6, methylparaben, propylparaben, silicon dioxide and sodium propionate.
CLINICAL PHARMACOLOGY
Pharmacokinetics: Pharmacokinetics for the HELIDAC Therapy components (bismuth subsalicylate chewable tablets, metronidazole tablets, and tetracycline hydrochloride capsules) when coadministered has not been studied. There is no information about the gastric mucosal concentrations of bismuth, metronidazole, and tetracycline after administration of these agents concomitantly or in combination with an acid suppressive agent. The systemic pharmacokinetic information presented below is based on studies in which each product was administered alone.
Bismuth Subsalicylate: Upon oral administration, bismuth subsalicylate is almost completely hydrolyzed in the gastrointestinal tract to bismuth and salicylic acid. Thus, the pharmacokinetics of bismuth subsalicylate following oral administration can be described by the individual pharmacokinetics of bismuth and salicylic acid.
Bismuth: Less than 1% of bismuth from oral doses of bismuth subsalicylate is absorbed from the gastrointestinal tract into the systemic circulation. Absorbed bismuth is distributed throughout the body. Bismuth is highly bound to plasma proteins (> 90%). Bismuth has multiple disposition half-lives with an intermediate half-life of 5 to 11 days and a terminal half-life of 21 to 72 days. Elimination of bismuth is primarily through urinary and biliary routes with a renal clearance of 50 ± 18 mL/min. The mean trough blood bismuth concentration after 2 weeks oral administration of 787 mg bismuth subsalicylate (3 chewable tablets) four times daily under fasted condition was 5.1 ± 3.1 ng/mL. In another study, the mean trough blood bismuth concentration after 2 weeks oral administration of 525 mg bismuth subsalicylate (as PEPTO-BISMOL® liquid suspension) four times daily was 5 ng/mL with the highest value being 32 ng/mL.
Salicylic Acid: More than 80% of the salicylic acid is absorbed from oral doses of bismuth subsalicylate chewable tablets. Salicylic acid is about 90% plasma protein bound. The volume of distribution is about 170 mL/kg of body weight. Salicylic acid is extensively metabolized and about 10% is excreted unchanged in the urine. The metabolic clearance of salicylic acid is saturable; accordingly, nonlinear pharmacokinetics is observed at bismuth subsalicylate doses above 525 mg. Salicylic acid metabolic clearance is lower in females than in males. The terminal half-life of salicylic acid upon a single oral dose of 525 mg bismuth subsalicylate is between 2 to 5 hours. After a single oral dose of 525 mg bismuth subsalicylate (2 chewable tablets), the mean peak plasma salicylic acid concentration was 13.1 ± 3.4 μg/mL under fasted condition. The mean steady-state serum total salicylate concentration after 2 weeks oral administration of 525 mg bismuth subsalicylate (as PEPTO-BISMOL liquid suspension) four times daily was 24 μg/mL with the highest value being 70 μg/mL.
Metronidazole: Following oral administration, metronidazole is well absorbed, with peak plasma concentrations occurring between 1 and 2 hours after administration. Plasma concentrations of metronidazole are proportional to the administered dose, with oral administration of 250 mg producing a peak plasma concentration of 6 μg/mL. Studies reveal no significant bioavailability differences between males and females; however because of weight differences, the resulting plasma levels in males are generally lower.
Metronidazole is the major component appearing in the plasma, with lesser quantities of the 2-hydroxymethyl metabolite also being present. Less than 20% of the circulating metronidazole is bound to plasma proteins. Metronidazole also appears in cerebrospinal fluid, saliva, and human milk in concentrations similar to those found in plasma.
The average elimination half-life in normal volunteers is 8 hours. The major route of elimination of metronidazole and its metabolites is via the urine (60% to 80% of the dose), with fecal excretion accounting for 6% to 15% of the dose. The metabolites that appear in the urine result primarily from side-chain oxidation [1-(ß-hydroxyethyl)-2-hydroxymethyl-5-nitroimidazole and 2-methyl-5-nitroimidazole-1-yl-acetic acid] and glucuronide conjugation, with unchanged metronidazole accounting for approximately 20% of the total. Renal clearance of metronidazole is approximately 10 mL/min/1.73 m2.
Decreased renal function does not alter the single-dose pharmacokinetics of metronidazole. In patients with decreased liver function, plasma clearance of metronidazole is decreased.
Tetracycline Hydrochloride: Tetracyclines are readily absorbed and are bound to plasma proteins in varying degrees. They are concentrated by the liver in the bile and excreted in the urine and feces at high concentrations in a biologically active form.
The relative contribution of systemic versus local antimicrobial activity against H. pylori for agents used in eradication therapy has not been established.
Microbiology: Bismuth subsalicylate, metronidazole, and tetracycline administered individually as combination therapy have been shown to be active against most strains of Helicobacter pylori in vitro, and in clinical infections as described in the CLINICAL STUDIES and INDICATIONS AND USAGE sections.
Helicobacter: Helicobacter pylori: In the Graham and Cutler studies, susceptibility testing was not performed for bismuth subsalicylate, metronidazole, or tetracycline. No adequate data were collected during the clinical studies to indicate that bismuth subsalicylate can either decrease or increase metronidazole MICs. (See CLINICAL STUDIES.)
Susceptibility testing of Helicobacter pylori isolates was performed in the P&GP study for metronidazole using agar dilution methodology1 and minimum inhibitory concentrations (MICs) were determined.
Susceptibility Testing of Helicobacter pylori: Susceptibility testing of Helicobacter pylori for metronidazole has not been standardized. No interpretive criteria have been established for testing metronidazole against H. pylori. The clinical significance of metronidazole MIC values against H. pylori is unknown.
INDICATIONS AND USAGE
The components of the HELIDAC Therapy (bismuth subsalicylate, metronidazole, and tetracycline hydrochloride), in combination with an H2 antagonist, are indicated for the eradication of H. pylori for treatment of patients with H. pylori infection and duodenal ulcer disease (active or a history of duodenal ulcer). Appropriate doses of H2 antagonists for the treatment of active duodenal ulcers should be prescribed in all patients. The eradication of H. pylori has been demonstrated to reduce the risk of duodenal ulcer recurrence in patients with active duodenal ulcer disease. (See CLINICAL STUDIES and DOSAGE AND ADMINISTRATION.)
To reduce the development of drug-resistant bacteria and maintain the effectiveness of HELIDAC Therapy and other antibacterial drugs, HELIDAC Therapy should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
CLINICAL STUDIES
Eradication of H. pylori in Patients with Active Duodenal Ulcer Disease: Investigators in the U.S. (Graham et al., 1991, 1992, and Cutler et al., 1993) and Germany (Labenz et al., 1993) studied the effect of therapy on the eradication of H. pylori using bismuth subsalicylate, metronidazole, and tetracycline hydrochloride. The patient population in these studies consisted predominantly of duodenal ulcer patients with active disease. In addition to bismuth subsalicylate, metronidazole, tetracycline hydrochloride triple therapy, most patients were also prescribed antisecretory therapy at doses recommended for ulcer healing, with the majority receiving ranitidine. The primary efficacy variable used in these studies to determine effectiveness of therapy was H. pylori eradication, or cure of infection. Use of cure of infection as a surrogate for reduced ulcer recurrence is based on an extensive review of the literature. Eradication rates are derived from results of the randomized, controlled study of Graham et al. and the uncontrolled, nonrandomized study of Cutler et al. H. pylori eradication was defined as no positive test (culture, histology, rapid urease, or 13C breath test) at least 4 weeks following the end of treatment. In the analysis performed, dropouts and patients with missing H. pylori tests post-treatment were excluded. HELIDAC Therapy (bismuth subsalicylate, metronidazole, and tetracycline hydrochloride) was effective in eradicating H. pylori.
|
† Evaluable patients were defined as having a confirmed duodenal ulcer within 2 years prior to treatment and having taken 14 days of bismuth subsalicylate, metronidazole, and tetracycline (range 11 to 17 days). Eradication was defined as no evidence of H. pylori infection by culture, histology, rapid urease test and/or urea breath test from at least 4 weeks post-treatment up to 1 year post-treatment. |
||
| Investigator | Eradication Rate in Duodenal Ulcer Patients† | 95% Confidence Intervals |
| Graham 2,3 | 77% | 61% - 89% |
| (N = 39) | ||
| Cutler4 | 82% | 70% - 92% |
| (N = 51) | ||
Graham et al. 19923 studied long-term outcome in patients treated for active duodenal ulcer by frequently monitoring for ulcer recurrence for up to 1 year after therapy. This study compared patients who received bismuth subsalicylate (BSS), metronidazole (MTZ), and tetracycline hydrochloride (TCN) for 2 weeks with ranitidine to those who received ranitidine alone. The ulcer recurrence rates at 6 months and 1 year regardless of post-treatment eradication status are summarized below for duodenal ulcer patients who were H. pylori positive at baseline.
| Therapy | All Patients | H. pylori Negative Patients Post-Treatment |
| BSS/MTZ/TCN + Ranitidine | 4% (1/25) | 6% (1/18) |
| Ranitidine | 85% (17/20) | 100% (1/1) |
|
† Includes all patients randomized to therapy who were H. pylori positive at baseline (by culture, histology, and/or urea breath test) who had ulcer healing and 24 or 48 weeks of endoscopic follow-up data. |
||
| Therapy | All Patients | H. pylori Negative Patients Post-Treatment |
| BSS/MTZ/TCN + Ranitidine | 9% (2/22) | 13% (2/16) |
| Ranitidine | 95% (18/19) | 100% (1/1) |
Eradication of H. pylori in Patients with a History of Duodenal Ulcer Disease: A controlled, multicenter trial conducted by P&GP in the U.S. compared the rates of eradication of H. pylori following 14 days of treatment with HELIDAC Therapy (bismuth subsalicylate, metronidazole, and tetracycline hydrochloride) or control (bismuth subsalicylate, metronidazole placebo, and tetracycline placebo) in 103 patients infected with H. pylori who had a history of duodenal ulcer disease. No H2-receptor antagonist was used. The primary efficacy measurement was H. pylori eradication assessed by rapid urease testing, histology, and culture at least 4 weeks after the last dose. HELIDAC Therapy was effective in eradicating H. pylori. The eradication rates are noted in the table below:
|
a The lower limit for this calculation was -2.2 but was truncated to 0 for reporting purposes. |
||||
|
† Evaluable patients were defined as having a history of a confirmed duodenal ulcer prior to treatment and having taken ≥ 70% of each component of HELIDAC Therapy (bismuth subsalicylate, metronidazole, tetracycline hydrochloride) during the 14-day dosing period. Eradication was defined as no evidence of H. pylori infection by two or three diagnostic tests (culture, histology, and rapid urease test) from at least 4 weeks to 6 weeks post-treatment. Excluded from the evaluable population were patients who were non-compliant with medication, patients who were not infected with H. pylori at baseline, and patients without ulcer documentation. Three patients in the HELIDAC Therapy group and one patient in the Control group were included as eradication failures because they withdrew from the study due to treatment-related adverse events. |
||||
|
‡ Patients were included in the analysis if they had documented H. pylori infection at baseline and had confirmed duodenal ulcer disease. All dropouts were included as failures of therapy. Eradication was defined as no evidence of H. pylori infection by culture, histology, or rapid urease test. |
||||
| Population | Evaluable Population† | Intent-To-Treat Population‡ | ||
| Therapy | HELIDAC Therapy | Control | HELIDAC Therapy | Control |
| Eradication Rate | 71% | 7% | 72% | 6% |
| (Number of Patients) | (40/56) | (2/30) | (41/57) | (2/32) |
| 95% confidence interval | 60, 83 | 0a, 16 | 60, 84 | 0a, 15 |
Compliance with the triple therapy regimen was also evaluated in the clinical study. In the intent-to-treat population, 93% of the HELIDAC Therapy group took at least 75% of their medication.
CONTRAINDICATIONS
This therapy is contraindicated in pregnant or nursing women, pediatric patients, in patients with renal or hepatic impairment, and in those with known hypersensitivity to bismuth subsalicylate, metronidazole or other nitroimidazole derivatives, or any of the tetracyclines. (See WARNINGS and PRECAUTIONS.) This product does not contain aspirin but should not be administered to those patients who have a known allergy to aspirin or salicylates.
WARNINGS
Bismuth Subsalicylate
Children and teenagers who have or who are recovering from chicken pox or flu should NOT use this medicine to treat nausea or vomiting. If nausea or vomiting is present, patients are advised to consult a doctor because this could be an early sign of Reye's syndrome, a rare but serious illness.
There have been rare reports of neurotoxicity associated with excessive doses of bismuth subsalicylate. Effects have been reversible with discontinuation of therapy.
Metronidazole
Central Nervous System Effects: Convulsive seizures and peripheral neuropathy, the latter characterized mainly by numbness or paresthesia of an extremity, have been reported in patients treated with metronidazole. The prevalence and severity of the neuropathy are directly related to the cumulative dose and duration of therapy, being most prevalent in patients taking high doses for prolonged treatment periods. The appearance of abnormal neurologic signs demands the prompt discontinuation of metronidazole therapy. Metronidazole should be administered with caution to patients with central nervous system diseases.
Pregnancy: Teratogenic Effects. Metronidazole crosses the placental barrier and its effects on the human fetal organogenesis are not known. No fetotoxicity was observed when metronidazole was administered orally to pregnant mice at 20 mg/kg/day approximately one and a half times the most frequently recommended human dose (750 mg/day) based on mg/kg body weight; however, in a single small study where the drug was administered intraperitoneally, some intrauterine deaths were observed. The relationship of these findings to the drug is unknown.
Tetracycline
THE USE OF DRUGS OF THE TETRACYCLINE CLASS DURING TOOTH DEVELOPMENT (LAST HALF OF PREGNANCY, INFANCY, AND CHILDHOOD TO THE AGE OF 8 YEARS) MAY CAUSE PERMANENT DISCOLORATION OF THE TEETH (YELLOW-GRAY-BROWN). This adverse reaction is more common during long-term use of the drugs but has been observed following repeated short-term courses. Enamel hypoplasia has also been reported. TETRACYCLINE HYDROCHLORIDE IS A COMPONENT OF THE HELIDAC THERAPY, THEREFORE, HELIDAC THERAPY SHOULD NOT BE USED IN THESE PATIENT POPULATIONS. (See CONTRAINDICATIONS.)
Tetracycline hydrochloride, as a component of the HELIDAC Therapy, should not be used during pregnancy. Results of animal studies indicate that tetracyclines cross the placenta, are found in fetal tissues, and can have toxic effects on the developing fetus (often related to retardation of skeletal development). Evidence of embryotoxicity has also been noted in animals treated early in pregnancy. If this drug is used during pregnancy or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to the fetus.
Photosensitivity manifested by an exaggerated sunburn reaction has been observed in some individuals taking tetracyclines. Patients apt to be exposed to direct sunlight or ultraviolet light should be advised that this reaction can occur with tetracycline drugs. Treatment should be discontinued at the first evidence of skin erythema.
The antianabolic action of the tetracyclines may cause an increase in blood urea nitrogen (BUN). While this is not a problem in those with normal renal function, in patients with significantly impaired renal function, higher serum levels of tetracycline may lead to azotemia, hyperphosphatemia, and acidosis.
PRECAUTIONS
General
Prescribing HELIDAC Therapy in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
Bismuth Subsalicylate
Bismuth subsalicylate may cause a temporary and harmless darkening of the tongue and/or black stool. Stool darkening should not be confused with melena.
Metronidazole
Patients with severe hepatic disease metabolize metronidazole slowly, with resultant accumulation of metronidazole and its metabolites in plasma. (See CONTRAINDICATIONS.) Metronidazole is a nitroimidazole and should be used with caution in patients with evidence of, or history of, blood dyscrasia. A mild leukopenia has been observed; however, no persistent hematologic abnormalities attributable to metronidazole have been observed.
Known or previously unrecognized candidiasis may present more prominent symptoms during therapy with metronidazole and requires treatment with a candicidal agent.
Tetracycline
As with other antibiotics, use of tetracycline hydrochloride may result in overgrowth of nonsusceptible organisms, including fungi. If superinfection occurs, tetracycline should be discontinued and appropriate therapy should be instituted.
Pseudotumor cerebri (benign intracranial hypertension) in adults has been associated with the use of tetracyclines. The usual clinical manifestations are headache and blurred vision. While this condition and related symptoms usually resolve soon after discontinuation of the tetracycline, the possibility for permanent sequelae exists.
Information for Patients: Each dose includes 4 pills: 2 pink round chewable tablets (bismuth subsalicylate), 1 white round tablet (metronidazole), and 1 black and yellow capsule (tetracycline hydrochloride). Each dose (all 4 pills) should be taken 4 times a day, at mealtimes and bedtime. Patients should be instructed to chew and swallow the pink round tablets (bismuth subsalicylate tablets) and to swallow the white round tablet (metronidazole tablet) and the black and yellow capsule (tetracycline hydrochloride capsule) whole with a full glass of water (8 ounces). Concomitantly prescribed H2 antagonist therapy should be taken as directed.
Administration of adequate amounts of fluid, particularly with the bedtime dose of tetracycline hydrochloride, is recommended to reduce the risk of esophageal irritation and ulceration. (See ADVERSE REACTIONS.)
Missed doses can be made up by continuing the normal dosing schedule until the medication is gone. Patients should not take double doses. (If more than 4 doses are missed, the prescriber should be contacted.)
This treatment regimen includes salicylates. If taken with aspirin and ringing in the ears occurs, the prescriber should be consulted concerning discontinuation of the aspirin therapy until the HELIDAC Therapy is completed.
Concurrent use of tetracyclines may render oral contraceptives less effective. Patients should be advised to use a different or additional form of contraception. Breakthrough bleeding has been reported. Women who become pregnant while taking components of the HELIDAC Therapy should be advised to notify their prescriber immediately. (See CONTRAINDICATIONS and WARNINGS.)
Alcoholic beverages should be avoided while taking metronidazole and for at least 1 day afterward. (See Drug Interactions.)
Patients taking tetracycline hydrochloride should be cautioned to avoid exposure to sun or sun lamps. (See WARNINGS.)
Bismuth subsalicylate may cause temporary and harmless darkening of the tongue and/or black stool. Stool darkening should not be confused with melena (blood in the stool).
Patients should be counseled that antibacterial drugs, including HELIDAC Therapy, should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When HELIDAC Therapy is prescribed to treat a bacterial infection, patients should be told that although it is common to feel better early in the course of therapy, the medication should be taken exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by HELIDAC Therapy or other antibacterial drugs in the future.
Drug Interactions: Individual components of the HELIDAC Therapy have a potential interaction with anticoagulants. Tetracycline has been shown to depress plasma prothrombin activity. Metronidazole has been reported to potentiate the anticoagulant effect of warfarin and other oral coumarin anticoagulants, resulting in a prolongation of prothrombin time. Salicylates may cause an increased risk of bleeding when administered with anticoagulant therapy. Therefore, monitoring anticoagulant therapy with appropriate adjustment of the anticoagulant dosage may be warranted if concurrent therapy is instituted.
Caution is advised in the administration of bismuth subsalicylate to patients taking medication for diabetes (possible enhanced hypoglycemic effect when given with salicylates) or patients taking aspirin, probenecid, or sulfinpyrazone.
Absorption of tetracyclines is impaired by antacids containing aluminum, calcium, or magnesium; preparations containing iron, zinc, or sodium bicarbonate; or milk or dairy products.
There is an anticipated reduction in tetracycline systemic absorption due to an interaction with bismuth and/or calcium carbonate, an excipient of bismuth subsalicylate tablets. The clinical significance of this is unknown as the relative contribution of systemic versus local antimicrobial activity against H. pylori for these agents has not been established.
Since bacteriostatic drugs, such as the tetracycline class of antibiotics, may interfere with the bactericidal action of penicillin, it is not advisable to administer these drugs concomitantly.
The concurrent use of tetracycline and methoxyflurane has been reported to result in fatal renal toxicity.
Concurrent use of tetracycline may render oral contraceptives less effective. Patients should be advised to use a different or additional form of contraception. Breakthrough bleeding has been reported. Women who become pregnant while on the HELIDAC Therapy should be advised to notify their prescriber immediately.
The simultaneous administration of drugs that decrease microsomal liver enzyme activity, such as cimetidine, may prolong the half-life and decrease plasma clearance of metronidazole. The simultaneous administration of drugs that induce microsomal liver enzymes, such as phenytoin or phenobarbital, may accelerate the elimination of metronidazole, resulting in reduced plasma levels; impaired clearance of phenytoin has also been reported.
In patients stabilized on relatively high doses of lithium, short-term metronidazole therapy has been associated with elevation of serum lithium and, in a few cases, signs of lithium toxicity. Serum lithium and serum creatinine should be obtained several days after beginning metronidazole to detect any increase that may precede clinical symptoms of lithium intoxication.
Alcoholic beverages should not be consumed during metronidazole therapy and for at least 1 day afterward because abdominal cramps, nausea, vomiting, headaches, and flushing may occur.
Psychotic reactions have been reported in alcoholic patients who are using metronidazole and disulfiram concurrently. Metronidazole should not be given to patients who have taken disulfiram within the last 2 weeks.
Drug/Laboratory Test Interactions: Bismuth absorbs x-rays and may interfere with x-ray diagnostic procedures of the gastrointestinal tract.
Bismuth subsalicylate may cause a temporary and harmless darkening of the stool. However, this does not interfere with standard tests for occult blood.
Metronidazole may interfere with certain types of determinations of serum chemistry values, such as aspartate aminotransferase (AST, SGOT), alanine aminotransferase (ALT, SGPT), lactate dehydrogenase (LDH), triglycerides, and hexokinase glucose. Values of zero may be observed. All of the assays in which interference has been reported involve enzymatic coupling of the assay to oxidation-reduction of nicotinamide (NAD+ ⇔ NADH). Interference is due to the similarity in absorbance peaks of NADH (340 nm) and metronidazole (322 nm) at pH 7.
Carcinogenesis, Mutagenesis, Impairment of Fertility: Metronidazole has shown evidence of carcinogenic activity in a number of studies involving chronic, oral administration in mice and rats. Prominent among the effects in the mouse was an increased incidence of pulmonary tumorigenesis. This has been observed in all six reported studies in that species, including one study in which the animals were dosed on an intermittent schedule (administration during every fourth week only). At very high dose levels, (approximately 500 mg/kg/day, which is approximately 33 times the most frequently recommended human dose for a 50 kg adult based on mg/kg body weight), there was a statistically significant increase in the incidence of malignant liver tumors in male mice. Also, the published results of one of the mouse studies indicate an increase in the incidence of malignant lymphomas as well as pulmonary neoplasms associated with lifetime feeding of the drug. All these effects are statistically significant. Long-term, oral-dosing studies in the rat showed statistically significant increases in the incidence of various neoplasms, particularly in mammary and hepatic tumors, among female rats administered metronidazole over those noted in the concurrent female control groups. Two lifetime tumorigenicity studies in hamsters have been performed and reported to be negative.
There has been no evidence of carcinogenicity for tetracycline hydrochloride in studies conducted with rats and mice. Some related antibiotics (oxytetracycline, minocycline) have shown evidence of oncogenic activity in rats.
No long-term toxicity studies have been conducted with bismuth subsalicylate.
No long-term studies have been performed to evaluate the effect of the combined use of bismuth subsalicylate, metronidazole, and tetracycline on carcinogenesis, mutagenesis, or impairment of fertility.
Although metronidazole has shown mutagenic activity in a number of in vitro assay systems, studies in mammals (in vivo) have failed to demonstrate a potential for genetic damage.
In two in vitro mammalian cell assay systems (L51784y mouse lymphoma and Chinese hamster lung cells), there was evidence of mutagenicity by tetracycline hydrochloride at concentrations of 60 and 10 μg/mL, respectively.
Bismuth did not show mutagenic potential in the NTP salmonella plate assay.
No reproductive toxicity studies have been conducted with bismuth subsalicylate.
Tetracycline hydrochloride had no effect on fertility when administered in the diet to male and female rats at a daily intake of 25 times the human dose.
Metronidazole, at doses up to 400 mg/kg/day (approximately 3.5 times the recommended maximum human dose based on mg/m2) for 28 days, failed to produce any adverse effects on fertility and testicular function in male rats. Fertility studies have been performed in mice at doses up to six times the maximum recommended human dose based on mg/m2 and have revealed no evidence of impaired fertility.
Pregnancy
Teratogenic Effects. Pregnancy Category D: Category D is based on the pregnancy category for tetracycline hydrochloride. (See CONTRAINDICATIONS and WARNINGS, Tetracycline and Metronidazole subsections.)
Non-teratogenic Effects: (See WARNINGS.)
Pregnant women with renal disease may be more prone to develop tetracycline-associated liver failure.
Labor and Delivery: The effect of this therapy on labor and delivery is unknown.
Nursing Mothers: Metronidazole and tetracycline are both secreted into human milk. Because of the potential for tumorigenicity shown for metronidazole in mouse and rat studies, and because of the potential for serious adverse reactions in nursing infants from tetracyclines, a decision should be made whether to discontinue nursing or to discontinue therapy, taking into account the importance of the therapy to the mother. Metronidazole is secreted in human milk in concentrations similar to those found in plasma. (See CONTRAINDICATIONS.)
Pediatric Use: Safety and effectiveness in pediatric patients infected with H. pylori have not been established. (See CONTRAINDICATIONS and WARNINGS.)
Geriatric Use: Clinical studies of HELIDAC Therapy did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy in elderly patients should be considered when prescribing HELIDAC Therapy. As stated in the CONTRAINDICATIONS section, this therapy is contraindicated in patients with renal or hepatic impairment.
ADVERSE REACTIONS
The most common adverse reactions (≥ 1%) reported in clinical trials when all three components of this therapy were given concomitantly are listed in the table below. The majority of the adverse reactions were related to the gastrointestinal tract, were reversible, and infrequently led to discontinuation of therapy.
Incidence of Adverse Reactions Reported
in Clinical Trials (≥ 1%)†
|
† Includes reactions reported at ≥1% in patients taking BSS/MTZ/TCN in Graham, Cutler, and P&GP studies. |
|
|
‡ In the Graham and Cutler studies (N = 197), most patients were on concomitant acid suppression therapy. |
|
| BSS/MTZ/TCN‡
(N = 266) |
|
| Adverse Reactions | % Patients |
| Nausea | 12.0 |
| Diarrhea | 6.8 |
| Abdominal Pain | 6.8 |
| Melena | 3.0 |
| Upper Respiratory Infection | 2.3 |
| Constipation | 1.9 |
| Anorexia | 1.5 |
| Asthenia | 1.5 |
| Vomiting | 1.5 |
| Discolored Tongue | 1.5 |
| Headache | 1.5 |
| Dyspepsia | 1.5 |
| Dizziness | 1.5 |
| Stool Abnormality | 1.1 |
| Duodenal Ulcer | 1.1 |
| Sinusitis | 1.1 |
| Taste Perversion | 1.1 |
| Flatulence | 1.1 |
| GI Hemorrhage | 1.1 |
| Pain | 1.1 |
| Insomnia | 1.1 |
| Anal Discomfort | 1.1 |
| Paresthesia | 1.1 |
The additional adverse reactions (< 1%) reported in clinical trials when all three components of this therapy were given concomitantly are listed below and divided by body system:
Gastrointestinal: dry mouth, dysphagia, eructation, GI monilia, glossitis, intestinal obstruction, rectal hemorrhage, stomatitis
Skin: acne, ecchymosis, photosensitivity reaction (see WARNINGS), pruritus, rash
Cardiovascular: cerebral ischemia, chest pain, hypertension, myocardial infarction
CNS: nervousness, somnolence
Musculoskeletal: arthritis, rheumatoid arthritis, tendonitis
Metabolic: SGOT increase, SGPT increase
Urogenital: urinary tract infection
Other: conjunctivitis, flu syndrome, infection, malaise, neoplasm, rhinitis, syncope, tooth disorder
The following adverse reactions from the labeling for bismuth subsalicylate are provided for information.
Gastrointestinal: black stools
Mouth: temporary and harmless darkening of the tongue
The following adverse reactions from the labeling for metronidazole are provided for information.
Gastrointestinal: The most common adverse reactions reported have been referable to the gastrointestinal tract, particularly nausea reported by about 12% of patients, sometimes accompanied by headache, anorexia, and occasionally vomiting, diarrhea, epigastric distress, and abdominal cramping. Constipation has also been reported.
Mouth: A sharp, unpleasant metallic taste is not unusual. Furry tongue, glossitis, stomatitis have occurred; these may be associated with a sudden overgrowth of Candida which may occur during therapy.
Blood: Reversible neutropenia (leukopenia); rarely, reversible thrombocytopenia.
Cardiovascular: Flattening of the T-wave may be seen in electrocardiographic tracings.
CNS: Convulsive seizures, peripheral neuropathy, dizziness, vertigo, incoordination, ataxia, confusion, irritability, depression, weakness, and insomnia. Two serious adverse reactions reported in patients treated with metronidazole have been convulsive seizures and peripheral neuropathy, the latter characterized mainly by numbness or paresthesia of an extremity. Since persistent peripheral neuropathy has been reported in some patients receiving prolonged administration of metronidazole, patients should be specifically warned about these reactions and should be told to stop the drug and report immediately to their physicians if any neurologic symptoms occur.
Hypersensitivity: urticaria, erythematous rash, flushing, nasal congestion, dryness of mouth (or vagina or vulva), and fever.
Renal: Dysuria, cystitis, polyuria, incontinence, and a sense of pelvic pressure. Instances of darkened urine have been reported by approximately one patient in 100,000. Although the pigment which is probably responsible for this phenomenon has not been positively identified, it is almost certainly a metabolite of metronidazole and seems to have no clinical significance.
Other: Proliferation of Candida in the vagina, dyspareunia, decrease of libido, proctitis, and fleeting joint pains sometimes resembling “serum sickness.” If patients receiving metronidazole drink alcoholic beverages, they may experience abdominal distress, nausea, vomiting, flushing, or headache. A modification of the taste of alcoholic beverages has also been reported. Crohn's disease patients are known to have an increased incidence of gastrointestinal and certain extraintestinal cancers. There have been some reports in the medical literature of breast and colon cancer in Crohn's disease patients who have been treated with metronidazole at high doses for extended periods of time. A cause and effect relationship has not been established. Rare cases of pancreatitis, which abated on withdrawal of the drug, have been reported.
The following adverse reactions from the labeling for tetracycline hydrochloride are provided for information.
Gastrointestinal: Anorexia, nausea, epigastric distress, vomiting, diarrhea, glossitis, black hairy tongue, dysphagia, enterocolitis, and inflammatory lesions (with monilial overgrowth) in the anogenital region. Rare instances of esophagitis and esophageal ulceration have been reported in patients taking the tetracycline-class antibiotics in capsule and tablet form. Most of the patients who experienced esophageal irritation took the medication immediately before going to bed. (See DOSAGE AND ADMINISTRATION.)
Liver: Hepatotoxicity and liver failure have been observed in patients receiving large doses of tetracycline and in tetracycline-treated patients with renal impairment. Increases in liver enzymes and hepatic toxicity have been reported rarely.
Teeth: Permanent discoloration of teeth may be caused during tooth development. Enamel hypoplasia has also been reported. (See WARNINGS.)
Blood: hemolytic anemia, thrombocytopenia, thrombocytopenic purpura, neutropenia, and eosinophilia.
CNS: Pseudotumor cerebri (benign intracranial hypertension) in adults and bulging fontanels in infants. (See PRECAUTIONS: Tetracycline.) Dizziness, tinnitus, and visual disturbances have been reported. Myasthenic syndrome has been reported rarely.
Hypersensitivity: urticaria, angioneurotic edema, anaphylaxis, anaphylactoid purpura, pericarditis, exacerbation of systemic lupus erythematosus and serum sickness-like reactions, as fever, rash, and arthralgia.
Renal: Rise in BUN has been reported and is apparently dose related. (See WARNINGS).
Skin: Maculopapular and erythematous rashes have been reported. Exfoliative dermatitis has been rarely reported. Photosensitivity (see WARNINGS), onycholysis, and discoloration of the nails have been reported rarely.
Other: When given over prolonged periods, tetracyclines have been reported to produce brown-black microscopic discoloration of thyroid glands. No abnormalities of thyroid function studies are known to occur.
OVERDOSAGE
In case of an overdose, patients should contact a physician, poison control center, or emergency room. If all three components of this therapy are involved in an overdose, acute treatment should focus on the salicylate intoxication. There is neither a pharmacologic basis nor data suggesting an increased toxicity of the combination compared to individual components.
Bismuth Subsalicylate: The main concern of an acute bismuth subsalicylate (BSS) overdose focuses on the salicylate burden and not on bismuth, since less than 1% of the bismuth is normally absorbed. Each 262.4-mg tablet of BSS contains an amount of salicylate comparable to approximately 130 mg aspirin. Acute ingestion of less than 150 mg/kg of aspirin (i.e., less than one tablet of bismuth subsalicylate per kilogram of body weight) is not expected to lead to toxicity. Mild to moderate toxicity may result from the ingestion of 150 to 300 mg/kg, while severe toxicity may occur from ingestions over 300 mg/kg. Salicylate intoxication is well described in the literature and presents a complex clinical picture. Multiple respiratory and metabolic effects result in fluid, electrolyte, glucose, and acid-base disturbances. Initial symptoms of salicylate toxicity include hyperpnea, nausea, vomiting, tinnitus, hyperpyrexia, lethargy, tachycardia, and confusion. In severe cases, these symptoms may progress to severe hyperpnea, convulsions, pulmonary or cerebral edema, respiratory failure, cardiovascular collapse, coma, and death.
Treatment: There is no specific antidote for salicylate poisoning. If there are no contraindications, vomiting should be induced as soon as possible with syrup of ipecac, or gastric lavage should be instituted, provided that no more than one hour has elapsed since ingestion. Activated charcoal and a cathartic may be administered as primary decontamination therapy in those cases where greater than one hour has elapsed since ingestion, or to further decontaminate the gastrointestinal tract in those who have already received ipecac or gastric lavage. Plasma salicylate levels may be useful; a common nomogram can be used to help predict the severity of intoxication. Supportive and symptomatic treatment should be provided, with emphasis on correcting fluid, electrolyte, blood glucose, and acid-base disturbances. (Note: An acidotic blood pH increases the un-ionized salicylate form, allowing more to reach the central nervous system.) Elimination may be enhanced by urinary alkalinization, hemodialysis, or hemoperfusion. Since hemodialysis aids in correcting acid-base disturbances, this method may be preferred over hemoperfusion.
Metronidazole: Single oral doses of metronidazole, up to 19.5 g in adults, have been reported without resultant serious toxicity in suicide attempts and accidental overdoses. Symptoms reported include nausea, vomiting, and ataxia.
Neurotoxic effects, including seizures and peripheral neuropathy, have been reported after 5 to 7 days of doses of 6 to 10.4 g every other day.
Treatment: There is no specific antidote for metronidazole overdose. Management of the patient should consist of symptomatic and supportive therapy. Metronidazole is dialyzable.
Tetracycline: The acute toxicity of tetracycline in overdose is not well established in the literature. Therapeutic and overdose quantities of tetracycline can cause gastrointestinal symptoms such as nausea, vomiting, and diarrhea.
Treatment: There is no specific antidote for tetracycline overdose. Management of the patient should consist of symptomatic and supportive therapy. Tetracycline is not dialyzable.
DOSAGE AND ADMINISTRATION
Adults: The recommended dosages are: bismuth subsalicylate, 525 mg (two 262.4 mg-chewable tablets), metronidazole, 250 mg (one 250-mg tablet), and tetracycline hydrochloride, 500 mg (one 500-mg capsule) taken four times daily (q.i.d.) for 14 days plus an H2 antagonist approved for the treatment of acute duodenal ulcer. Patients should be instructed to take the medicines at mealtimes and at bedtime. The bismuth subsalicylate tablets should be chewed and swallowed. The metronidazole tablet and tetracycline hydrochloride capsule should be swallowed whole with a full glass of water (8 ounces). Concomitantly prescribed H2 antagonist therapy should be taken as directed.
Ingestion of adequate amounts of fluid, particularly with the bedtime dose of tetracycline hydrochloride, is recommended to reduce the risk of esophageal irritation and ulceration. (See ADVERSE REACTIONS.)
Missed doses can be made up by continuing the normal dosing schedule until the medication is gone. Patients should not take double doses. If more than 4 doses are missed, the prescriber should be contacted.
HOW SUPPLIED
The HELIDAC Therapy is supplied in a carton containing patient instructions, patient reminders, and 14 blister cards, each card containing the following daily dosage:
- 8 bismuth subsalicylate 262.4-mg chewable tablets, each pink round tablet engraved “PG 11”.
- 4 metronidazole 250-mg tablets are unscored, round, white, debossed MP 45.
- 4 tetracycline hydrochloride 500-mg capsules, each black/yellow capsule imprinted with “barr 010”.
NDC 65483-495-14 carton containing 14 days of therapy
Store at controlled room temperature 20°-25°C (68°-77°F) [See USP].
REFERENCES
- Clinical and Laboratory Standards Institute. Methods for Dilution Antimicrobial susceptibility Tests for Bacteria that Grow Aerobically-Approved Standard Seventh Edition. Clinical and Laboratory Standards Institute document M7-A7, Vol. 26, No. 2, CLSI, Wayne, PA, January 2006.
- Graham DY, Lew GM, Evans DG, Evans DJ Jr, Klein PD. Effect of triple therapy (antibiotics plus bismuth) on duodenal ulcer healing. Ann Intern Med 1991; 115:266-69.
- Graham DY, Lew GM, Klein PD, Evans DG, Evans DJ Jr, Saeed ZA, Malaty HM. Effect of treatment of Helicobacter pylori infection on the long-term recurrence of gastric or duodenal ulcer. Ann Int Med 1992; 116:705-08.
- Cutler AF, Schubert TT. Long-term Helicobacter pylori recurrence after successful eradication with triple therapy. Am J Gastroenterol 1993; 88:1359-61.
Sold under U.S. Patents 5,256,684; 5,403,830; 5,407,688; and 5,601,848
PEPTO-BISMOL is the registered trademark of The Procter & Gamble Company.
Bismuth subsalicylate tablets are manufactured by Norwich Pharmaceuticals, Inc. Metronidazole 250-mg tablets, USP are manufactured by URL Pharma, Inc. and tetracycline hydrochloride 500-mg capsules, USP are manufactured by Watson Pharmaceuticals, Inc.
for
Prometheus Laboratories Inc.
San Diego, CA 92121
REVISED JANUARY 2009
HE006K09
Chew and swallow the 2 pink tablets
Swallow capsule and white tablet whole with a glass of water
HELIDAC® Therapy
(bismuth subsalicylate/metronidazole/tetracycline HCl)
NDC 65483-495-14
56 DOSAGE
UNITS
HELIDAC® Therapy
(bismuth subsalicylate/metronidazole/
tetracycline hydrochloride)
112 bismuth subsalicylate 262.4 mg tablets
56 metronidazole 250 mg tablets, USP
56 tetracycline hydrochloride 500 mg capsules, USP
Carton contains 14 blister cards, one for each day of therapy.
Each card contains 8 bismuth subsalicylate tablets, 4 metronidazole
tablets, and 4 tetracycline hydrochloride capsules.
Note: Change
in tetracycline
hydrochloride capsule
color to Black and Yellow
Rx Only
| HELIDAC THERAPY
bismuth subsalicylate/metronidazole/tetracycline hydrochloride kit |
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| NDA | NDA050719 | 08/15/1996 | |
| Labeler - Prometheus Laboratories Inc. (967000860) |
| Establishment | |||
| Name | Address | ID/FEI | Operations |
| Norwich Pharmaceuticals, Inc. | 132218731 | MANUFACTURE | |
| Establishment | |||
| Name | Address | ID/FEI | Operations |
| URL Pharma, Inc. | 002811818 | MANUFACTURE | |
| Establishment | |||
| Name | Address | ID/FEI | Operations |
| BARR Laboratories Inc. | 002931751 | MANUFACTURE | |
| Establishment | |||
| Name | Address | ID/FEI | Operations |
| Sharp Corporation | 002346625 | REPACK | |