SULFAMETHOXAZOLE AND TRIMETHOPRIM- sulfamethoxazole and trimethoprim injection, solution
Teva Parenteral Medicines, Inc.
----------
Rx only
9503
9514
9526
To reduce the development of drug-resistant bacteria and maintain the effectiveness of sulfamethoxazole and trimethoprim injection and other antibacterial drugs, sulfamethoxazole and trimethoprim injection should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria.
DESCRIPTION
Sulfamethoxazole and trimethoprim injection USP, a sterile solution for intravenous infusion only, is a synthetic antibacterial combination product. Each mL contains: sulfamethoxazole USP 80 mg; trimethoprim USP 16 mg; alcohol 12.3% (v/v); propylene glycol 400 mg; benzyl alcohol 10 mg as a preservative; diethanolamine 3 mg; sodium metabisulfite 1 mg as an antioxidant; water for injection q.s.; air replaced with nitrogen; pH adjusted with sodium hydroxide and/or hydrochloric acid if necessary. pH: 9.5 to 10.5.
Sulfamethoxazole USP is N 1-(5-methyl-3-isoxazolyl)sulfanilamide. It is an almost white, odorless, tasteless compound with the following structural formula:
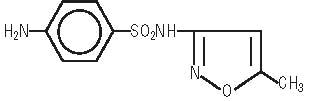
C10H11N3O3S M.W. 253.28
Trimethoprim USP is 2,4-diamino-5-(3,4,5-trimethoxybenzyl) pyrimidine. It is a white to light yellow, odorless, bitter compound with the following structural formula:
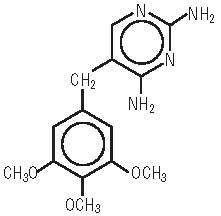
C14H18N4O3 M.W. 290.3
CLINICAL PHARMACOLOGY
Following a 1 hour intravenous infusion of a single dose of 800 mg sulfamethoxazole and 160 mg trimethoprim to 11 patients whose weight ranged from 105 lbs to 165 lbs (mean, 143 lbs) the peak plasma concentrations of sulfamethoxazole and trimethoprim were 46.3 ± 2.7 mcg/mL and 3.4 ± 0.3 mcg/mL, respectively. Following repeated intravenous administration of the same dose at 8 hour intervals, the mean plasma concentrations just prior to and immediately after each infusion at steady state were 70.6 ± 7.3 mcg/mL and 105.6 ± 10.9 mcg/mL for sulfamethoxazole and 5.6 ± 0.6 mcg/mL and 8.8 ± 0.9 mcg/mL for trimethoprim. The mean plasma half-life was 12.8 ± 1.8 hours for sulfamethoxazole and 11.3 ± 0.7 hours for trimethoprim. All of these 11 patients had normal renal function, and their ages ranged from 17 to 78 years (median, 60 years).1
Pharmacokinetic studies in children and adults suggest an age-dependent half-life of trimethoprim, as indicated in the following table.2
|
Age (years) |
No. of Patients |
Mean TMP Half-life (hours) |
| <1 | 2 | 7.67 |
| 1 to 10 | 9 | 5.49 |
| 10 to 20 | 5 | 8.19 |
| 20 to 63 | 6 | 12.82 |
Patients with severely impaired renal function exhibit an increase in the half-lives of both components, requiring dosage regimen adjustment (see DOSAGE AND ADMINISTRATION section).
Both sulfamethoxazole and trimethoprim exist in the blood as unbound, protein-bound and metabolized forms; sulfamethoxazole also exists as the conjugated form. The metabolism of sulfamethoxazole occurs predominately by N4-acetylation, although the glucuronide conjugate has been identified. The principal metabolites of trimethoprim are the 1- and 3-oxides and the 3’- and 4’-hydroxy derivatives. The free forms of sulfamethoxazole and trimethoprim are considered to be the therapeutically active forms. Approximately 70% of sulfamethoxazole and 44% of trimethoprim are bound to plasma proteins. The presence of 10 mg percent sulfamethoxazole in plasma decreases the protein binding of trimethoprim by an insignificant degree; trimethoprim does not influence the protein binding of sulfamethoxazole.
Excretion of sulfamethoxazole and trimethoprim is primarily by the kidneys through both glomerular filtration and tubular secretion. Urine concentrations of both sulfamethoxazole and trimethoprim are considerably higher than are the concentrations in the blood. The percent of dose excreted in urine over a 12 hour period following the intravenous administration of the first dose of 1200 mg of sulfamethoxazole and 240 mg of trimethoprim on day 1 ranged from 7% to 12.7% as free sulfamethoxazole and 17% to 42.4% as free trimethoprim; and 36.7% to 56% as total (free plus the N4-acetylated metabolite) sulfamethoxazole. When administered together, neither sulfamethoxazole nor trimethoprim affects the urinary excretion pattern of the other. Both sulfamethoxazole and trimethoprim distribute to sputum and vaginal fluid; trimethoprim also distributes to bronchial secretions, and both pass the placental barrier and are excreted in breast milk.
Microbiology
Sulfamethoxazole inhibits bacterial synthesis of dihydrofolic acid by competing with para-aminobenzoic acid (PABA). Trimethoprim blocks the production of tetrahydrofolic acid from dihydrofolic acid by binding to and reversibly inhibiting the required enzyme, dihydrofolate reductase. Thus, this combination blocks two consecutive steps in the biosynthesis of nucleic acids and proteins essential to many bacteria.
In vitro studies have shown that bacterial resistance develops more slowly with this combination than with either sulfamethoxazole or trimethoprim alone.
In vitro serial dilution tests have shown that the spectrum of antibacterial activity of sulfamethoxazole and trimethoprim injection includes common bacterial pathogens with the exception of Pseudomonas aeruginosa. The following organisms are usually susceptible: Escherichia coli, Klebsiella species, Enterobacter species, Morganella morganii, Proteus mirabilis, indole-positive Proteus species including Proteus vulgaris, Haemophilus influenzae (including ampicillin-resistant strains), Streptococcus pneumoniae, Shigella flexneri and Shigella sonnei. It should be noted, however, that there are little clinical data on the use of sulfamethoxazole and trimethoprim injection in serious systemic infections due to Haemophilus influenzae and Streptococcus pneumoniae.
| SMX = sulfamethoxazole TMP = trimethoprim *Rudoy RC, Nelson JD, Haltalin KC. Antimicrob Agents Chemother. May 1974; 5:439-443. |
||||
| Bacteria |
TMP alone |
SMX alone |
TMP/SMX TMP |
(1:20) SMX |
| Escherichia coli | 0.05 to 1.5 | 1 to 245 | 0.05 to 0.5 | 0.95 to 9.5 |
| Proteus species
(indole positive) | 0.5 to 5 | 7.35 to 300 | 0.05 to 1.5 | 0.95 to 28.5 |
| Morganella morganii | 0.5 to 5 | 7.35 to 300 | 0.05 to 1.5 | 0.95 to 28.5 |
| Proteus mirabilis | 0.5 to 1.5 | 7.35 to 30 | 0.05 to 0.15 | 0.95 to 2.85 |
| Klebsiella species | 0.15 to 5 | 2.45 to 245 | 0.05 to 1.5 | 0.95 to 28.5 |
| Enterobacter species | 0.15 to 5 | 2.45 to 245 | 0.05 to 1.5 | 0.95 to 28.5 |
| Haemophilus influenzae | 0.15 to 1.5 | 2.85 to 95 | 0.015 to 0.15 | 0.285 to 2.85 |
| Streptococcus pneumoniae | 0.15 to 1.5 | 7.35 to 24.5 | 0.05 to 0.15 | 0.95 to 2.85 |
| Shigella flexneri* | <0.01 to 0.04 | <0.16 to >320 | <0.002 to 0.03 | 0.04 to 0.625 |
| Shigella sonnei* | 0.02 to 0.08 | 0.625 to >320 | 0.004 to 0.06 | 0.08 to 1.25 |
The recommended quantitative disc susceptibility method may be used for estimating the susceptibility of bacteria to sulfamethoxazole and trimethoprim.3, 4 With this procedure, a report from the laboratory of “Susceptible to sulfamethoxazole and trimethoprim” indicates that the infection is likely to respond to therapy with this product. If the infection is confined to the urine, a report of “Intermediate susceptibility to sulfamethoxazole and trimethoprim” also indicates that the infection is likely to respond. A report of “Resistant to sulfamethoxazole and trimethoprim” indicates that the infection is unlikely to respond to therapy with this product.
INDICATIONS AND USAGE
To reduce the development of drug-resistant bacteria and maintain the effectiveness of sulfamethoxazole and trimethoprim injection USP and other antibacterial drugs, sulfamethoxazole and trimethoprim injection USP should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to empiric selection of therapy.
Urinary Tract Infections
For the treatment of urinary tract infections due to susceptible strains of the following organisms: Escherichia coli, Klebsiella species, Enterobacter species, Morganella morganii, Proteus mirabilis and Proteus vulgaris. It is recommended that initial episodes of uncomplicated urinary tract infections be treated with a single effective antibacterial agent rather than the combination.
Acute Otitis Media
For the treatment of acute otitis media in pediatric patients due to susceptible strains of Streptococcus pneumoniae or Haemophilus influenzae when in the judgment of the physician sulfamethoxazole USP and trimethoprim USP offers some advantage over the use of other antimicrobial agents. To date, there are limited data on the safety of repeated use of sulfamethoxazole and trimethoprim injection USP in pediatric patients under two years of age. Sulfamethoxazole and trimethoprim injection USP is not indicated for prophylactic or prolonged administration in otitis media at any age.
Acute Exacerbations of Chronic Bronchitis in Adults
For the treatment of acute exacerbations of chronic bronchitis due to susceptible strains of Streptococcus pneumoniae or Haemophilus influenzae when in the judgment of the physician sulfamethoxazole and trimethoprim injection USP offers some advantage over the use of a single antimicrobial agent.
Shigellosis
For the treatment of enteritis caused by susceptible strains of Shigella flexneri and Shigella sonnei when antibacterial therapy is indicated.
CONTRAINDICATIONS
Sulfamethoxazole and trimethoprim injection is contraindicated in patients with a known hypersensitivity to trimethoprim or sulfonamides, in patients with a history of drug-induced immune thrombocytopenia with use of trimethoprim and/or sulfonamides, and in patients with documented megaloblastic anemia due to folate deficiency. Sulfamethoxazole and trimethoprim injection is also contraindicated in pregnant patients and nursing mothers, because sulfonamides pass the placenta and are excreted in the milk and may cause kernicterus. Sulfamethoxazole and trimethoprim injection is contraindicated in pediatric patients less than 2 months of age. Sulfamethoxazole and trimethoprim injection is also contraindicated in patients with marked hepatic damage or with severe renal insufficiency when renal function status cannot be monitored.
WARNINGS
FATALITIES ASSOCIATED WITH THE ADMINISTRATION OF SULFONAMIDES, ALTHOUGH RARE, HAVE OCCURRED DUE TO SEVERE REACTIONS, INCLUDING STEVENS-JOHNSON SYNDROME, TOXIC EPIDERMAL NECROLYSIS, FULMINANT HEPATIC NECROSIS, AGRANULOCYTOSIS, APLASTIC ANEMIA AND OTHER BLOOD DYSCRASIAS.
SULFONAMIDES, INCLUDING SULFONAMIDE-CONTAINING PRODUCTS SUCH AS SULFAMETHOXAZOLE/TRIMETHOPRIM, SHOULD BE DISCONTINUED AT THE FIRST APPEARANCE OF SKIN RASH OR ANY SIGN OF ADVERSE REACTION. In rare instances, a skin rash may be followed by a more severe reaction, such as Stevens-Johnson syndrome, toxic epidermal necrolysis, hepatic necrosis, and serious blood disorders (see PRECAUTIONS). Clinical signs, such as rash, sore throat, fever, arthralgia, pallor, purpura or jaundice may be early indications of serious reactions.
Cough, shortness of breath, and pulmonary infiltrates are hypersensitivity reactions of the respiratory tract that have been reported in association with sulfonamide treatment.
Thrombocytopenia
Sulfamethoxazole/trimethoprim-induced thrombocytopenia may be an immune-mediated disorder. Severe cases of thrombocytopenia that are fatal or life threatening have been reported. Thrombocytopenia usually resolves within a week upon discontinuation of sulfamethoxazole/trimethoprim.
The sulfonamides should not be used for treatment of group A β-hemolytic streptococcal infections. In an established infection, they will not eradicate the streptococcus and, therefore, will not prevent sequelae such as rheumatic fever.
Clostridium difficile associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including sulfamethoxazole and trimethoprim injection, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibiotic use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibiotic use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibiotic treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
Sulfamethoxazole and trimethoprim injection contains sodium metabisulfite, a sulfite that may cause allergic-type reactions, including anaphylactic symptoms and life-threatening or less severe asthmatic episodes in certain susceptible people. The overall prevalence of sulfite sensitivity in the general population is unknown and probably low. Sulfite sensitivity is seen more frequently in asthmatic than in nonasthmatic people.
Contains benzyl alcohol. In newborn infants, benzyl alcohol has been associated with an increased incidence of neurological and other complications which are sometimes fatal.
PRECAUTIONS
General
Prescribing sulfamethoxazole and trimethoprim injection in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
Sulfamethoxazole and trimethoprim injection should be given with caution to patients with impaired renal or hepatic function, to those with possible folate deficiency (e.g., the elderly, chronic alcoholics, patients receiving anticonvulsant therapy, patients with malabsorption syndrome, and patients in malnutrition states) and to those with severe allergies or bronchial asthma. In glucose-6-phosphate dehydrogenase deficient individuals, hemolysis may occur. This reaction is frequently dose-related (seeCLINICAL PHARMACOLOGY and DOSAGE AND ADMINISTRATION).
Cases of hypoglycemia in non-diabetic patients treated with sulfamethoxazole and trimethoprim injection are seen rarely, usually occurring after a few days of therapy. Patients with renal dysfunction, liver disease, malnutrition or those receiving high doses of sulfamethoxazole and trimethoprim injection are particularly at risk.
Hematological changes indicative of folic acid deficiency may occur in elderly patients or in patients with preexisting folic acid deficiency or kidney failure. These effects are reversible by folinic acid therapy.
Trimethoprim has been noted to impair phenylalanine metabolism, but this is of no significance in phenylketonuric patients on appropriate dietary restriction.
As with all drugs containing sulfonamides, caution is advisable in patients with porphyria or thyroid dysfunction.
Use in the Treatment of and Prophylaxis for Pneumocystis Carinii Pneumonia in Patients with Acquired Immunodeficiency Syndrome (AIDS)
AIDS patients may not tolerate or respond to sulfamethoxazole and trimethoprim injection in the same manner as non-AIDS patients. The incidence of side effects, particularly rash, fever, leukopenia and elevated aminotransferase (transaminase) values, with sulfamethoxazole and trimethoprim injection therapy in AIDS patients who are being treated for Pneumocystis carinii pneumonia has been reported to be greatly increased compared with the incidence normally associated with the use of sulfamethoxazole and trimethoprim injection in non-AIDS patients. The incidence of hyperkalemia appears to be increased in AIDS patients receiving sulfamethoxazole and trimethoprim injection. Adverse effects are generally less severe in patients receiving sulfamethoxazole and trimethoprim injection for prophylaxis. A history of mild intolerance to sulfamethoxazole and trimethoprim injection in AIDS patients does not appear to predict intolerance of subsequent secondary prophylaxis.5 However, if a patient develops skin rash or any sign of adverse reaction, therapy with sulfamethoxazole and trimethoprim injection should be reevaluated (see WARNINGS).
High dosage of trimethoprim, as used in patients with Pneumocystis carinii pneumonia, induces a progressive but reversible increase of serum potassium concentrations in a substantial number of patients. Even treatment with recommended doses may cause hyperkalemia when trimethoprim is administered to patients with underlying disorders of potassium metabolism, with renal insufficiency, or if drugs known to induce hyperkalemia are given concomitantly. Close monitoring of serum potassium is warranted in these patients.
During treatment, adequate fluid intake and urinary output should be ensured to prevent crystalluria. Patients who are "slow acetylators" may be more prone to idiosyncratic reactions to sulfonamides.
Information for Patients
Patients should be counseled that antibacterial drugs including sulfamethoxazole and trimethoprim injection should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When sulfamethoxazole and trimethoprim injection is prescribed to treat a bacterial infection, patients should be told that although it is common to feel better early in the course of therapy, the medication should be taken exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by sulfamethoxazole and trimethoprim injection or other antibacterial drugs in the future.
Patients should be instructed to maintain an adequate fluid intake in order to prevent crystalluria and stone formation.
Diarrhea is a common problem caused by antibiotics which usually ends when the antibiotic is discontinued. Sometimes after starting treatment with antibiotics, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as two or more months after having taken the last dose of the antibiotic. If this occurs, patients should contact their physician as soon as possible.
Laboratory Tests
Complete blood counts should be done frequently in patients receiving sulfamethoxazole and trimethoprim injection; if a significant reduction in the count of any formed blood element is noted, sulfamethoxazole and trimethoprim injection should be discontinued. Urinalyses with careful microscopic examination and renal function tests should be performed during therapy, particularly for those patients with impaired renal function.
Drug Interactions
In elderly patients concurrently receiving certain diuretics, primarily thiazides, an increased incidence of thrombocytopenia with purpura has been reported.
It has been reported that sulfamethoxazole and trimethoprim injection may prolong the prothrombin time in patients who are receiving the anticoagulant warfarin. This interaction should be kept in mind when sulfamethoxazole and trimethoprim injection is given to patients already on anticoagulant therapy, and the coagulation time should be reassessed.
Sulfamethoxazole and trimethoprim injection may inhibit the hepatic metabolism of phenytoin. Sulfamethoxazole and trimethoprim injection, given at a common clinical dosage, increased the phenytoin half-life by 39% and decreased the phenytoin metabolic clearance rate by 27%. When administering these drugs concurrently, one should be alert for possible excessive phenytoin effect.
Sulfonamides can also displace methotrexate from plasma protein binding sites and can compete with the renal transport of methotrexate, thus increasing free methotrexate concentrations.
There have been reports of marked but reversible nephrotoxicity with coadministration of sulfamethoxazole and trimethoprim injection and cyclosporine in renal transplant recipients.
Increased digoxin blood levels can occur with concomitant sulfamethoxazole and trimethoprim injection therapy, especially in elderly patients. Serum digoxin levels should be monitored.
Increased sulfamethoxazole blood levels may occur in patients who are also receiving indomethacin.
Occasional reports suggest that patients receiving pyrimethamine as malaria prophylaxis in doses exceeding 25 mg weekly may develop megaloblastic anemia if sulfamethoxazole and trimethoprim injection is prescribed.
The efficacy of tricyclic antidepressants can decrease when coadministered with sulfamethoxazole and trimethoprim injection.
Like other sulfonamide-containing drugs, sulfamethoxazole and trimethoprim injection potentiates the effect of oral hypoglycemics.
In the literature, a single case of toxic delirium has been reported after concomitant intake of sulfamethoxazole/trimethoprim and amantadine.
In the literature, three cases of hyperkalemia in elderly patients have been reported after concomitant intake of sulfamethoxazole/trimethoprim and an angiotensin converting enzyme inhibitor.6,7
Drug/Laboratory Test Interactions
Sulfamethoxazole and trimethoprim injection, specifically the trimethoprim component, can interfere with a serum methotrexate assay as determined by the competitive binding protein technique (CBPA) when a bacterial dihydrofolate reductase is used as the binding protein. No interference occurs, however, if methotrexate is measured by a radioimmunoassay (RIA).
The presence of sulfamethoxazole and trimethoprim may also interfere with the Jaffé alkaline picrate reaction assay for creatinine, resulting in overestimations of about 10% in the range of normal values.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Long-term studies in animals to evaluate carcinogenic potential have not been conducted with sulfamethoxazole and trimethoprim injection.
Mutagenesis
Bacterial mutagenic studies have not been performed with sulfamethoxazole and trimethoprim in combination. Trimethoprim was demonstrated to be nonmutagenic in the Ames assay. No chromosomal damage was observed in human leukocytes cultured in vitro with sulfamethoxazole and trimethoprim alone or in combination; the concentrations used exceeded blood levels of these compounds following therapy with sulfamethoxazole and trimethoprim. Observations of leukocytes obtained from patients treated with sulfamethoxazole and trimethoprim revealed no chromosomal abnormalities.
Pregnancy
Teratogenic Effects
Pregnancy Category C
In rats, oral doses of 533 mg/kg or 200 mg/kg produced teratologic effects manifested mainly as cleft palates.
The highest dose which did not cause cleft palates in rats was 512 mg/kg sulfamethoxazole or 192 mg/kg trimethoprim when administered separately. In two studies in rats, no teratology was observed when 512 mg/kg of sulfamethoxazole was used in combination with 128 mg/kg of trimethoprim. In one study, however, cleft palates were observed in one litter out of 9 when 355 mg/kg of sulfamethoxazole was used in combination with 88 mg/kg of trimethoprim.
In some rabbit studies, an overall increase in fetal loss (dead and resorbed and malformed conceptuses) was associated with doses of trimethoprim 6 times the human therapeutic dose.
While there are no large, well-controlled studies on the use of sulfamethoxazole and trimethoprim in pregnant women, Brumfitt and Pursell,8 in a retrospective study, reported the outcome of 186 pregnancies during which the mother received either placebo or sulfamethoxazole and trimethoprim. The incidence of congenital abnormalities was 4.5% (3 of 66) in those who received placebo and 3.3% (4 of 120) in those receiving sulfamethoxazole and trimethoprim. There were no abnormalities in the 10 children whose mothers received the drug during the first trimester. In a separate survey, Brumfitt and Pursell also found no congenital abnormalities in 35 children whose mothers had received oral sulfamethoxazole and trimethoprim at the time of conception or shortly thereafter.
Because sulfamethoxazole and trimethoprim may interfere with folic acid metabolism, sulfamethoxazole and trimethoprim injection should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Pediatric Use
Sulfamethoxazole and trimethoprim injection is not recommended for infants younger than 2 months of age (seeINDICATIONSandCONTRAINDICATIONS sections).
Geriatric Use
Clinical studies of sulfamethoxazole and trimethoprim injection did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects.
There may be an increased risk of severe adverse reactions in elderly patients, particularly when complicating conditions exist, e.g., impaired kidney and/or liver function, possible folate deficiency, or concomitant use of other drugs. Severe skin reactions, generalized bone marrow suppression (see WARNINGSand ADVERSE REACTIONSsections), a specific decrease in platelets (with or without purpura), and hyperkalemia are the most frequently reported severe adverse reactions in elderly patients. In those concurrently receiving certain diuretics, primarily thiazides, an increased incidence of thrombocytopenia with purpura has been reported. Increased digoxin blood levels can occur with concomitant sulfamethoxazole and trimethoprim injection therapy, especially in elderly patients. Serum digoxin levels should be monitored. Hematological changes indicative of folic acid deficiency may occur in elderly patients. These effects are reversible by folinic acid therapy. Appropriate dosage adjustments should be made for patients with impaired kidney function and duration of use should be as short as possible to minimize risks of undesired reactions (see DOSAGE AND ADMINISTRATIONsection). The trimethoprim component of sulfamethoxazole and trimethoprim injection may cause hyperkalemia when administered to patients with underlying disorders of potassium metabolism, with renal insufficiency or when given concomitantly with drugs known to induce hyperkalemia, such as angiotensin converting enzyme inhibitors. Close monitoring of serum potassium is warranted in these patients. Discontinuation of sulfamethoxazole and trimethoprim injection treatment is recommended to help lower potassium serum levels.
Pharmacokinetics parameters for sulfamethoxazole were similar for geriatric subjects and younger adult subjects. The mean maximum serum trimethoprim concentration was higher and mean renal clearance of trimethoprim was lower in geriatric subjects compared with younger subjects (see CLINICAL PHARMACOLOGY: Geriatric Pharmacokinetics).
ADVERSE REACTIONS
The most common adverse effects are gastrointestinal disturbances (nausea, vomiting, anorexia) and allergic skin reactions (such as rash and urticaria). FATALITIES ASSOCIATED WITH THE ADMINISTRATION OF SULFONAMIDES, ALTHOUGH RARE, HAVE OCCURRED DUE TO SEVERE REACTIONS, INCLUDING STEVENS-JOHNSON SYNDROME, TOXIC EPIDERMAL NECROLYSIS, FULMINANT HEPATIC NECROSIS, AGRANULOCYTOSIS, APLASTIC ANEMIA AND OTHER BLOOD DYSCRASIAS (SEE WARNINGS SECTION). Local reaction, pain and slight irritation on IV administration are infrequent. Thrombophlebitis has rarely been observed.
Hematologic
Agranulocytosis, aplastic anemia, thrombocytopenia, leukopenia, neutropenia, hemolytic anemia, megaloblastic anemia, hypoprothrombinemia, methemoglobinemia, eosinophilia.
Allergic Reactions
Stevens-Johnson syndrome, toxic epidermal necrolysis, anaphylaxis, allergic myocarditis, erythema multiforme, exfoliative dermatitis, angioedema, drug fever, chills, Henoch-Schoenlein purpura, serum sickness-like syndrome, generalized allergic reactions, generalized skin eruptions, photosensitivity, conjunctival and scleral injection, pruritus, urticaria and rash. In addition, periarteritis nodosa and systemic lupus erythematosus have been reported.
Gastrointestinal
Hepatitis (including cholestatic jaundice and hepatic necrosis), elevation of serum transaminase and bilirubin, pseudomembranous enterocolitis, pancreatitis, stomatitis, glossitis, nausea, emesis, abdominal pain, diarrhea, anorexia.
Genitourinary
Renal failure, interstitial nephritis, BUN and serum creatinine elevation, toxic nephrosis with oliguria and anuria, crystalluria and nephrotoxicity in association with cyclosporine.
Metabolic and Nutritional
Hyperkalemia (see PRECAUTIONS: Use in the Treatment of and Prophylaxis for Pneumocystis Carinii Pneumonia in Patients with Acquired Immunodeficiency Syndrome (AIDS)).
Neurologic
Aseptic meningitis, convulsions, peripheral neuritis, ataxia, vertigo, tinnitus, headache.
Endocrine
The sulfonamides bear certain chemical similarities to some goitrogens, diuretics (acetazolamide and the thiazides) and oral hypoglycemic agents. Cross-sensitivity may exist with these agents. Diuresis and hypoglycemia have occurred rarely in patients receiving sulfonamides.
Musculoskeletal
Arthralgia and myalgia. Isolated cases of rhabdomyolysis have been reported with sulfamethoxazole and trimethoprim injection, mainly in AIDS patients.
Postmarketing Experience
The following adverse reactions have been identified during post-approval use of trimethoprim-sulfamethoxazole. Because these reactions were reported voluntarily from a population of uncertain size, it is not possible to reliably estimate their frequency or establish a causal relationship to drug exposure:
Σ Thrombotic thrombocytopenia purpura
Σ Idiopathic thrombocytopenic purpura
OVERDOSAGE
Acute
The amount of a single dose of sulfamethoxazole and trimethoprim injection that is either associated with symptoms of overdosage or is likely to be life-threatening has not been reported. Signs and symptoms of overdosage reported with sulfonamides include anorexia, colic, nausea, vomiting, dizziness, headache, drowsiness and unconsciousness. Pyrexia, hematuria and crystalluria may be noted. Blood dyscrasias and jaundice are potential late manifestations of overdosage.
Signs of acute overdosage with trimethoprim include nausea, vomiting, dizziness, headache, mental depression, confusion and bone marrow depression.
General principles of treatment include the institution of gastric lavage or emesis, forcing oral fluids, and the administration of intravenous fluids if urine output is low and renal function is normal. Acidification of the urine will increase renal elimination of trimethoprim. The patient should be monitored with blood counts and appropriate blood chemistries, including electrolytes. If a significant blood dyscrasia or jaundice occurs, specific therapy should be instituted for these complications. Peritoneal dialysis is not effective and hemodialysis is only moderately effective in eliminating sulfamethoxazole and trimethoprim.
Chronic
Use of sulfamethoxazole and trimethoprim injection at high doses and/or for extended periods of time may cause bone marrow depression manifested as thrombocytopenia, leukopenia and/or megaloblastic anemia. If signs of bone marrow depression occur, the patient should be given leucovorin 5 to 15 mg daily until normal hematopoiesis is restored.
Animal Toxicity
The LD50 of sulfamethoxazole and trimethoprim injection in mice is 700 mg/kg or 7.3 mL/kg; in rats and rabbits the LD50 is >500 mg/kg or >5.2 mL/kg. The vehicle produced the same LD50 in each of these species as the active drug.
The signs and symptoms noted in mice, rats and rabbits with sulfamethoxazole and trimethoprim or its vehicle at the high IV doses used in acute toxicity studies included ataxia, decreased motor activity, loss of righting reflex, tremors or convulsions, and/or respiratory depression.
DOSAGE AND ADMINISTRATION
CONTRAINDICATED IN INFANTS LESS THAN 2 MONTHS OF AGE. CAUTION—SULFAMETHOXAZOLE AND TRIMETHOPRIM INJECTION MUST BE DILUTED IN 5% DEXTROSE IN WATER SOLUTION PRIOR TO ADMINISTRATION. DO NOT MIX SULFAMETHOXAZOLE AND TRIMETHOPRIM INJECTION WITH OTHER DRUGS OR SOLUTIONS. RAPID INFUSION OR BOLUS INJECTION MUST BE AVOIDED.
Children and Adults
Pneumocystis Carinii Pneumonia
Total daily dose is 15 to 20 mg/kg (based on the trimethoprim component) given in 3 or 4 equally divided doses every 6 to 8 hours for up to 14 days. One investigator noted that a total daily dose of 10 to 15 mg/kg was sufficient in 10 adult patients with normal renal function.9
Severe Urinary Tract Infections And Shigellosis
Total daily dose is 8 to 10 mg/kg (based on the trimethoprim component) given in 2 or 4 equally divided doses every 6, 8 or 12 hours for up to 14 days for severe urinary tract infections and 5 days for shigellosis. The maximum recommended daily dose is 60 mL per day.
For Patients With Impaired Renal Function:
When renal function is impaired, a reduced dosage should be employed using the following table:
|
Creatinine Clearance (mL/min) |
Recommended Dosage Regimen |
| Above 30 | Usual standard regimen |
| 15 to 30 | 1⁄2 the usual regimen |
| Below 15 | Use not recommended |
Method Of Preparation
Sulfamethoxazole and trimethoprim injection must be diluted. EACH 5 ML SHOULD BE ADDED TO 125 ML OF 5% DEXTROSE IN WATER. After diluting with 5% dextrose in water the solution should not be refrigerated and should be used within 6 hours. If a dilution of 5 mL per 100 mL of 5% dextrose in water is desired, it should be used within 4 hours. If upon visual inspection there is cloudiness or evidence of crystallization after mixing, the solution should be discarded and a fresh solution prepared.
Multidose Vials
After initial entry into the vial, the remaining contents must be used within 48 hours.
The following infusion systems have been tested and found satisfactory: unit-dose glass containers; unit-dose polyvinyl chloride and polyolefin containers. No other systems have been tested and therefore no others can be recommended.
Dilution
EACH 5 ML OF SULFAMETHOXAZOLE AND TRIMETHOPRIM INJECTION SHOULD BE ADDED TO 125 ML OF 5% DEXTROSE IN WATER.
Note: In those instances where fluid restriction is desirable, each 5 mL may be added to 75 mL of 5% dextrose in water. Under these circumstances the solution should be mixed just prior to use and should be administered within 2 hours. If upon visual inspection there is cloudiness or evidence of crystallization after mixing, the solution should be discarded and a fresh solution prepared.
DO NOT MIX SULFAMETHOXAZOLE AND TRIMETHOPRIM INJECTION 5% DEXTROSE IN WATER WITH DRUGS OR SOLUTIONS IN THE SAME CONTAINER.
Administration
The solution should be given by intravenous infusion over a period of 60 to 90 minutes. Rapid infusion or bolus injection must be avoided. Sulfamethoxazole and trimethoprim injection should not be given intramuscularly.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever the solution and container permit.
HOW SUPPLIED
| 5 mL single dose amber vials packaged 10 per shelf pack. 10 mL multiple dose amber vials packaged 10 per shelf pack. 30 mL multiple dose amber vials packaged individually. |
|||
| NDC Numbers | Sulfamethoxazole USP | Trimethoprim USP | Size |
| 0703-9503-03 | 80 mg/mL | 16 mg/mL |
5 mL Single dose vial |
| 0703-9514-03 | 80 mg/mL | 16 mg/mL |
10 mL Multiple dose vial |
| 0703-9526-01 | 80 mg/mL | 16 mg/mL |
30 mL Multiple dose vial |
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature].
DO NOT REFRIGERATE.
REFERENCES
- Grose WE, Bodey GP, Loo TL. Clinical Pharmacology of Intravenously Administered Trimethoprim-Sulfamethoxazole. Antimicrob Agents Chemother. Mar 1979;15:447-451.
- Siber GR, Gorham C, Durbin W, Lesko L, Levin MJ. Pharmacology of Intravenous Trimethoprim-Sulfamethoxazole in Children and Adults. Current Chemotherapy and Infectious Diseases, American Society for Microbiology, Washington, D.C., 1980, Vol. 1, pp. 691-692.
- Bauer AW, Kirby WMM, Sherris JC, Turck M. Antibiotic Susceptibility Testing by a Standardized Single Disk Method. Am J Clin Pathol. Apr 1966;45:493-496.
- National Committee for Clinical Laboratory Standards. Performance Standards For Antimicrobial Disc Susceptibility Test. 771 East Lancaster Avenue, Villanova, Pennsylvania 19085: Approved Standard ASM-2.
- Hardy DW, et al. A controlled trial of trimethoprim-sulfamethoxazole or aerosolized pentamidine for secondary prophylaxis of Pneumocystis carinii pneumonia in patients with the acquired immunodeficiency syndrome. N Engl J Med. 1992; 327: 1842–1848.
- Marinella Mark A. 1999. Trimethoprim-induced hyperkalemia: An analysis of reported cases. Gerontol. 45:209–212.
- Margassery, S. and B. Bastani. 2002. Life threatening hyperkalemia and acidosis secondary to trimethoprim-sulfamethoxazole treatment. J. Nephrol. 14:410–414.
- Brumfitt W, Pursell R. Trimethoprim/Sulfamethoxazole in the Treatment of Bacteriuria in Women. J Infect Dis. Nov 1973; 128 (Suppl):S657–S663.
- Winston DJ, Lau WK, Gale RP, Young LS. Trimethoprim- Sulfamethoxazole for the Treatment of Pneumocystis carinii pneumonia. Ann Intern Med. June 1980;92:762-769.
Teva Parenteral Medicines, Inc.
Irvine, CA 92618
Rev. B 10/2011
PRINCIPAL DISPLAY PANEL

Sulfamethoxazole and Trimethoprim Injection, USP 30 mL Multiple Dose Vial Label Text
NDC 0703-9526-01 Rx only
Sulfamethoxazole and
Trimethoprim
Injection, USP
Sulfamethoxazole 80 mg/mL
Trimethoprim 16 mg/mL
For IV Infusion Only
30 mL Multiple Dose Vial
Must be diluted with 5% dextrose
injection prior to administration.
TEVA
| SULFAMETHOXAZOLE AND TRIMETHOPRIM
sulfamethoxazole and trimethoprim injection, solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Teva Parenteral Medicines, Inc. (794362533) |