DIDANOSINE - didanosine powder, for solution
Aurobindo Pharma Limited
----------
HIGHLIGHTS OF PRESCRIBING INFORMATIONThese highlights do not include all the information needed to use didanosine safely and effectively. See full prescribing information for didanosine for oral solution.
Didanosine for Oral Solution, USP Initial U.S. Approval: 1991
WARNING: PANCREATITIS, LACTIC ACIDOSIS and HEPATOMEGALY with STEATOSIS
|
| at least 60 kg | less than 60 kg | |
|---|---|---|
| Preferred dosing | 200 mg twice daily | 125 mg twice daily |
| Dosing for patients whose management requires once-daily frequency | 400 mg once daily | 250 mg once daily |
- Pediatric patients (2 weeks old to 18 years old): Administered on an empty stomach at least 30 minutes before or 2 hours after eating.
- Between 2 weeks and 8 months old, dosing is 100 mg/m2 twice daily.
- For those greater than 8 months old, dosing is 120 mg/m2 twice daily but not to exceed the adult dosing recommendation. (2.1)
DOSAGE FORMS AND STRENGTHS
WARNINGS AND PRECAUTIONS
- Pancreatitis: Suspension or discontinuation of didanosine may be necessary. (5.1)
- Lactic acidosis and severe hepatomegaly with steatosis: Suspend didanosine in patients who develop clinical symptoms or signs with or without laboratory findings. (5.2)
- Hepatic toxicity: Interruption or discontinuation of didanosine must be considered upon worsening of liver disease. (5.3)
- Non-cirrhotic portal hypertension: Discontinue didanosine in patients with evidence of non-cirrhotic portal hypertension. (5.4)
- Patients may develop peripheral neuropathy (5.5), retinal changes and optic neuritis (5.6), immune reconstitution syndrome (5.7), and redistribution/accumulation of body fat. (5.8)
ADVERSE REACTIONS
- In adults, the most common adverse reactions (greater than 10%, all grades) are diarrhea, peripheral neurologic symptoms/neuropathy, abdominal pain, nausea, headache, rash, and vomiting. (6.1)
- Adverse reactions in pediatric patients were consistent with those in adults. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Aurobindo Pharma USA, Inc. at 1-866-850-2876 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
DRUG INTERACTIONS
USE IN SPECIFIC POPULATIONS
Pregnancy: Fatal lactic acidosis has been reported in pregnant women who received both didanosine and stavudine with other agents. This combination should be used with caution during pregnancy and only if the potential benefit clearly outweighs the potential risk. (5.2, 8.1) Physicians are encouraged to register patients in the Antiretroviral Pregnancy Registry by calling 1-800-258-4263.
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide.
Revised: 2/2012
FULL PRESCRIBING INFORMATION
WARNING: PANCREATITIS, LACTIC ACIDOSIS and HEPATOMEGALY with STEATOSIS
Fatal and nonfatal pancreatitis has occurred during therapy with didanosine used alone or in combination regimens in both treatment-naive and treatment-experienced patients, regardless of degree of immunosuppression. Didanosine should be suspended in patients with suspected pancreatitis and discontinued in patients with confirmed pancreatitis [see Warnings and Precautions (5.1)].
Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogues alone or in combination, including didanosine and other antiretrovirals. Fatal lactic acidosis has been reported in pregnant women who received the combination of didanosine and stavudine with other antiretroviral agents. The combination of didanosine and stavudine should be used with caution during pregnancy and is recommended only if the potential benefit clearly outweighs the potential risk [see Warnings and Precautions (5.2)].
1 INDICATIONS AND USAGE
Didanosine also known as ddI, in combination with other antiretroviral agents is indicated for the treatment of human immunodeficiency virus (HIV)-1 infection [see Clinical Studies (14)].
2 DOSAGE AND ADMINISTRATION
Didanosine for oral solution should be administered on an empty stomach, at least 30 minutes before or 2 hours after eating.
2.1 Recommended Dosage (Adult and Pediatric Patients)
The preferred dosing frequency of didanosine for oral solution is twice daily because there is more evidence to support the effectiveness of this dosing regimen. Once-daily dosing should be considered only for patients whose management requires once-daily dosing of didanosine for oral solution [see Clinical Studies (14)].
The recommended adult total daily dose is based on body weight (kg) (see Table 1).
| at least 60 kg | less than 60 kg | |
|---|---|---|
| Preferred dosing | 200 mg twice daily | 125 mg twice daily |
| Dosing for patients whose management requires once-daily frequency | 400 mg once daily | 250 mg once daily |
Pediatric Patients (2 weeks old to 18 years old): The recommended dose of didanosine for oral solution in pediatric patients between 2 weeks old and 8 months old is 100 mg/m2 twice daily, and the recommended didanosine for oral solution dose for pediatric patients greater than 8 months old is 120 mg/m2 twice daily but not to exceed the adult dosing recommendation.
Dosing recommendations in patients less than 2 weeks of age cannot be made because the pharmacokinetics of didanosine in these children are too variable to determine an appropriate dose. There are no data on once-daily dosing of didanosine for oral solution in pediatric patients.
2.2 Renal Impairment
Adult Patients
In adult patients with impaired renal function, the dose of didanosine for oral solution should be adjusted to compensate for the slower rate of elimination. The recommended doses and dosing intervals of didanosine for oral solution in adult patients with renal insufficiency are presented in Table 2.
| Creatinine Clearance (mL/min) | Recommended Didanosine for Oral Solution Dose by Patient Weight |
|
|---|---|---|
| at least 60 kg | less than 60 kg | |
| a 400 mg once daily (at least 60 kg) or 250 mg once daily (less than 60 kg) for patients whose management requires once-daily frequency of administration. |
||
| at least 60 | 200 mg twice dailya
| 125 mg twice dailya
|
| 30-59 | 200 mg once daily or 100 mg twice daily | 150 mg once daily or 75 mg twice daily |
| 10-29 | 150 mg once daily | 100 mg once daily |
| less than 10 | 100 mg once daily | 75 mg once daily |
Pediatric Patients
Urinary excretion is also a major route of elimination of didanosine in pediatric patients, therefore the clearance of didanosine may be altered in pediatric patients with renal impairment. Although there are insufficient data to recommend a specific dose adjustment of didanosine for oral solution in this patient population, a reduction in the dose should be considered (see Table 2).
Patients Requiring Continuous Ambulatory Peritoneal Dialysis (CAPD) or Hemodialysis
For patients requiring CAPD or hemodialysis, follow dosing recommendations for patients with creatinine clearance of less than 10 mL/min, shown in Table 2. It is not necessary to administer a supplemental dose of didanosine for oral solution following hemodialysis.
2.3 Dosage Adjustment
Concomitant Therapy with Tenofovir Disoproxil Fumarate
In patients who are also taking tenofovir disoproxil fumarate, a dose reduction of didanosine for oral solution to 250 mg (adults weighing at least 60 kg with creatinine clearance of at least 60 mL/min) or 200 mg (adults weighing less than 60 kg with creatinine clearance of at least 60 mL/min) once daily is recommended. Didanosine for oral solution and tenofovir disoproxil fumarate may be taken together in the fasted state. Alternatively, if tenofovir disoproxil fumarate is taken with food, didanosine for oral solution should be taken on an empty stomach (at least 30 minutes before food or 2 hours after food). The appropriate dose of didanosine for oral solution coadministered with tenofovir disoproxil fumarate in patients with creatinine clearance of less than 60 mL/min has not been established. ([See Drug Interactions (7) and Clinical Pharmacology (12.3)]; see the complete prescribing information for didanosine delayed-release capsules (enteric-coated formulation of didanosine) for results of drug interaction studies of tenofovir disoproxil fumarate with reduced doses of the enteric-coated formulation of didanosine.)
Hepatic Impairment
No dose adjustment is required in patients with hepatic impairment [see Warnings and Precautions (5.3) and Clinical Pharmacology (12.3)].
3 DOSAGE FORMS AND STRENGTHS
Didanosine for Oral Solution is white to almost white, crystalline powder and is supplied in 2 g/bottle per carton and 4 g/bottle per carton.
4 CONTRAINDICATIONS
These recommendations are based on either drug interaction studies or observed clinical toxicities.
4.1 Allopurinol
Coadministration of didanosine and allopurinol is contraindicated because systemic exposures of didanosine are increased, which may increase didanosine-associated toxicity [see Clinical Pharmacology (12.3)].
4.2 Ribavirin
Coadministration of didanosine and ribavirin is contraindicated because exposures of the active metabolite of didanosine (dideoxyadenosine 5’-triphosphate) are increased. Fatal hepatic failure, as well as peripheral neuropathy, pancreatitis, and symptomatic hyperlactatemia/lactic acidosis have been reported in patients receiving both didanosine and ribavirin.
5 WARNINGS AND PRECAUTIONS
5.1 Pancreatitis
Fatal and nonfatal pancreatitis has occurred during therapy with didanosine used alone or in combination regimens in both treatment-naive and treatment-experienced patients, regardless of degree of immunosuppression. Didanosine should be suspended in patients with signs or symptoms of pancreatitis and discontinued in patients with confirmed pancreatitis. Patients treated with didanosine in combination with stavudine may be at increased risk for pancreatitis.
When treatment with life-sustaining drugs known to cause pancreatic toxicity is required, suspension of didanosine therapy is recommended. In patients with risk factors for pancreatitis, didanosine should be used with extreme caution and only if clearly indicated. Patients with advanced HIV-1 infection, especially the elderly, are at increased risk of pancreatitis and should be followed closely. Patients with renal impairment may be at greater risk for pancreatitis if treated without dose adjustment. The frequency of pancreatitis is dose related. [See Adverse Reactions (6).]
5.2 Lactic Acidosis/Severe Hepatomegaly with Steatosis
Lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogues alone or in combination, including didanosine and other antiretrovirals. A majority of these cases have been in women. Obesity and prolonged nucleoside exposure may be risk factors. Fatal lactic acidosis has been reported in pregnant women who received the combination of didanosine and stavudine with other antiretroviral agents. The combination of didanosine and stavudine should be used with caution during pregnancy and is recommended only if the potential benefit clearly outweighs the potential risk [see Use in Specific Populations (8.1)]. Particular caution should be exercised when administering didanosine to any patient with known risk factors for liver disease; however, cases have also been reported in patients with no known risk factors. Treatment with didanosine should be suspended in any patient who develops clinical signs or symptoms with or without laboratory findings consistent with symptomatic hyperlactatemia, lactic acidosis, or pronounced hepatotoxicity (which may include hepatomegaly and steatosis even in the absence of marked transaminase elevations).
5.3 Hepatic Toxicity
The safety and efficacy of didanosine have not been established in HIV-infected patients with significant underlying liver disease. During combination antiretroviral therapy, patients with preexisting liver dysfunction, including chronic active hepatitis, have an increased frequency of liver function abnormalities, including severe and potentially fatal hepatic adverse events, and should be monitored according to standard practice. If there is evidence of worsening liver disease in such patients, interruption or discontinuation of treatment must be considered.
Hepatotoxicity and hepatic failure resulting in death were reported during postmarketing surveillance in HIV-infected patients treated with hydroxyurea and other antiretroviral agents. Fatal hepatic events were reported most often in patients treated with the combination of hydroxyurea, didanosine, and stavudine. This combination should be avoided. [See Adverse Reactions (6).]
5.4 Non-cirrhotic Portal Hypertension
Postmarketing cases of non-cirrhotic portal hypertension have been reported, including cases leading to liver transplantation or death. Cases of didanosine-associated non-cirrhotic portal hypertension were confirmed by liver biopsy in patients with no evidence of viral hepatitis. Onset of signs and symptoms ranged from months to years after start of didanosine therapy. Common presenting features included elevated liver enzymes, esophageal varices, hematemesis, ascites, and splenomegaly.
Patients receiving didanosine should be monitored for early signs of portal hypertension (e.g., thrombocytopenia and splenomegaly) during routine medical visits. Appropriate laboratory testing including liver enzymes, serum bilirubin, albumin, complete blood count, and international normalized ratio (INR) and ultrasonography should be considered. Didanosine should be discontinued in patients with evidence of non-cirrhotic portal hypertension.
5.5 Peripheral Neuropathy
Peripheral neuropathy, manifested by numbness, tingling, or pain in the hands or feet, has been reported in patients receiving didanosine therapy. Peripheral neuropathy has occurred more frequently in patients with advanced HIV disease, in patients with a history of neuropathy, or in patients being treated with neurotoxic drug therapy, including stavudine. Discontinuation of didanosine should be considered in patients who develop peripheral neuropathy. [See Adverse Reactions (6).]
5.6 Retinal Changes and Optic Neuritis
Retinal changes and optic neuritis have been reported in adult and pediatric patients. Periodic retinal examinations should be considered for patients receiving didanosine [see Adverse Reactions (6)].
5.7 Immune Reconstitution Syndrome
Immune reconstitution syndrome has been reported in patients treated with combination antiretroviral therapy, including didanosine. During the initial phase of combination antiretroviral treatment, patients whose immune system responds may develop an inflammatory response to indolent or residual opportunistic infections (such as Mycobacterium avium infection, cytomegalovirus, Pneumocystis jiroveci pneumonia [PCP], or tuberculosis), which may necessitate further evaluation and treatment.
Autoimmune disorders (such as Graves’ disease, polymyositis, and Guillain-Barré syndrome) have also been reported to occur in the setting of immune reconstitution; however, the time to onset is more variable, and can occur many months after initiation of treatment.
5.8 Fat Redistribution
Redistribution/accumulation of body fat including central obesity, dorsocervical fat enlargement (buffalo hump), peripheral wasting, facial wasting, breast enlargement, and “cushingoid appearance” have been observed in patients receiving antiretroviral therapy. The mechanism and long-term consequences of these events are currently unknown. A causal relationship has not been established.
6 ADVERSE REACTIONS
The following adverse reactions are discussed in greater detail in other sections:
- Pancreatitis [see Boxed Warning, Warnings and Precautions (5.1)]
- Lactic acidosis/severe hepatomegaly with steatosis [see Boxed Warning, Warnings and Precautions (5.2)]
- Hepatic toxicity [see Warnings and Precautions (5.3)]
- Non-cirrhotic portal hypertension [see Warnings and Precautions (5.4)]
- Peripheral neuropathy [see Warnings and Precautions (5.5)]
- Retinal changes and optic neuritis [see Warnings and Precautions (5.6)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Adults
Selected clinical adverse reactions that occurred in adult patients in clinical studies with didanosine are provided in Tables 3 and 4.
| Adverse Reactions | Percent of Patients* | |||
|---|---|---|---|---|
| ACTG 116A | ACTG 116B/117 | |||
| didanosine n=197 | zidovudine n=212 | didanosine n=298 | zidovudine n=304 |
|
| * The incidences reported included all severity grades and all reactions regardless of causality. |
||||
| Diarrhea Peripheral Neurologic Symptoms/Neuropathy Abdominal Pain Rash/Pruritus Pancreatitis | 19 17 13 7 7 | 15 14 8 8 3 | 28 20 7 9 6 | 21 12 8 5 2 |
| Adverse Reactions | Percent of Patientsa,c | |||
|---|---|---|---|---|
| AI454-148b | START 2b | |||
| didanosine + stavudine + nelfinavir n=482 | zidovudine + lamivudine + nelfinavir n=248 | didanosine + stavudine + indinavir n=102 | zidovudine + lamivudine + indinavir n=103 |
|
| a Percentages based on treated subjects. b Median duration of treatment 48 weeks. c The incidences reported included all severity grades and all reactions regardless of causality. * This event was not observed in this study arm. |
||||
| Diarrhea Nausea Peripheral Neurologic Symptoms/Neuropathy Headache Rash Vomiting Pancreatitis (see below) | 70 28 26 21 13 12 1 | 60 40 6 30 16 14 * | 45 53 21 46 30 30 less than 1 | 39 67 10 37 18 35 * |
Pancreatitis resulting in death was observed in one patient who received didanosine plus stavudine plus nelfinavir in Study AI454-148 and in one patient who received didanosine plus stavudine plus indinavir in the START 2 study. In addition, pancreatitis resulting in death was observed in 2 of 68 patients who received didanosine plus stavudine plus indinavir plus hydroxyurea in an ACTG clinical trial [see Warnings and Precautions (5)].
The frequency of pancreatitis is dose related. In phase 3 studies, incidence ranged from 1% to 10% with doses higher than are currently recommended and from 1% to 7% with recommended dose.
Selected laboratory abnormalities in clinical studies with didanosine are shown in Tables 5 to 7.
| Parameter | Percent of Patients | |||
|---|---|---|---|---|
| ACTG 116A | ACTG 116B/117 | |||
| didanosine n=197 | zidovudine n=212 | didanosine n=298 | zidovudine n=304 |
|
| ULN = upper limit of normal. |
||||
| SGOT (AST) (greater than 5 x ULN) SGPT (ALT) (greater than 5 x ULN) Alkaline phosphatase (greater than 5 x ULN) Amylase (at least 1.4 x ULN) Uric acid (greater than 12 mg/dL) | 9 9 4 17 3 | 4 6 1 12 1 | 7 6 1 15 2 | 6 6 1 5 1 |
| Parameter | Percent of Patientsa | |||
|---|---|---|---|---|
| AI454-148b | START 2b | |||
| didanosine + stavudine + nelfinavir n=482 | zidovudine + lamivudine + nelfinavir n=248 | didanosine + stavudine + indinavir n=102 | zidovudine + lamivudine + indinavir n=103 |
|
| ULN = upper limit of normal. NC = Not Collected. a Percentages based on treated subjects. b Median duration of treatment 48 weeks. |
||||
| Bilirubin (greater than 2.6 x ULN) SGOT (AST) (greater than 5 x ULN) SGPT (ALT) (greater than 5 x ULN) GGT (greater than 5 x ULN) Lipase (greater than 2 x ULN) Amylase (greater than 2 x ULN) | less than 1 3 3 NC 7 NC | less than 1 2 3 NC 2 NC | 16 7 8 5 5 8 | 8 7 5 2 5 2 |
| Parameter | Percent of Patientsa | |||
|---|---|---|---|---|
| AI454-148b | START 2b | |||
| didanosine + stavudine + nelfinavir n=482 | zidovudine + lamivudine + nelfinavir n=248 | didanosine + stavudine + indinavir n=102 | zidovudine + lamivudine + indinavir n=103 |
|
| NC = Not Collected. a Percentages based on treated subjects. b Median duration of treatment 48 weeks. |
||||
| Bilirubin SGOT (AST) SGPT (ALT) GGT Lipase Amylase | 7 42 37 NC 17 NC | 3 23 24 NC 11 NC | 68 53 50 28 26 31 | 55 20 18 12 19 17 |
Pediatric Patients
In clinical trials, 743 pediatric patients between 2 weeks and 18 years of age have been treated with didanosine. Adverse reactions and laboratory abnormalities reported to occur in these patients were generally consistent with the safety profile of didanosine in adults.
In pediatric phase 1 studies, pancreatitis occurred in 2 of 60 (3%) patients treated at entry doses below 300 mg/m2/day and in 5 of 38 (13%) patients treated at higher doses. In study ACTG 152, pancreatitis occurred in none of the 281 pediatric patients who received didanosine 120 mg/m2 every 12 hours and in less than 1% of the 274 pediatric patients who received didanosine 90 mg/m2 every 12 hours in combination with zidovudine [see Clinical Studies (14)].
Retinal changes and optic neuritis have been reported in pediatric patients.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of didanosine. Because they are reported voluntarily from a population of unknown size, estimates of frequency cannot be made. These reactions have been chosen for inclusion due to their seriousness, frequency of reporting, causal connection to didanosine, or a combination of these factors.
Blood and Lymphatic System Disorders – anemia, leukopenia, and thrombocytopenia.
Body as a Whole – alopecia, anaphylactoid reaction, asthenia, chills/fever, pain, and redistribution/accumulation of body fat [see Warnings and Precautions (5.8)].
Digestive Disorders – anorexia, dyspepsia, and flatulence.
Exocrine Gland Disorders – pancreatitis (including fatal cases) [see Boxed Warning, Warnings and Precautions (5.1)], sialoadenitis, parotid gland enlargement, dry mouth, and dry eyes.
Hepatobiliary Disorders – symptomatic hyperlactatemia/lactic acidosis and hepatic steatosis [see Boxed Warning, Warnings and Precautions (5.2)]; non-cirrhotic portal hypertension [see Warnings and Precautions (5.4)]; hepatitis and liver failure.
Metabolic Disorders – diabetes mellitus, hypoglycemia, and hyperglycemia.
Musculoskeletal Disorders – myalgia (with or without increases in creatine kinase), rhabdomyolysis including acute renal failure and hemodialysis, arthralgia, and myopathy.
Ophthalmologic Disorders – retinal depigmentation and optic neuritis [see Warnings and Precautions (5.6)].
Use with Stavudine- and Hydroxyurea-Based Regimens
When didanosine is used in combination with other agents with similar toxicities, the incidence of these toxicities may be higher than when didanosine is used alone. Thus, patients treated with didanosine in combination with stavudine, with or without hydroxyurea, may be at increased risk for pancreatitis and hepatotoxicity, which may be fatal, and severe peripheral neuropathy [see Warnings and Precautions (5)]. The combination of didanosine and hydroxyurea, with or without stavudine, should be avoided.
7 DRUG INTERACTIONS
7.1 Established Drug Interactions
Clinical recommendations based on the results of drug interaction studies are listed in Table 8. Pharmacokinetic results of drug interaction studies are shown in Tables 12 and 13 [see Contraindications (4.1 and 4.2), Clinical Pharmacology (12.3)].
| Drug | Effect | Clinical Comment |
|---|---|---|
| ↑ Indicates increase. ↓ Indicates decrease. a The dosing recommendation for coadministration of didanosine delayed-release capsules and tenofovir disoproxil fumarate with respect to meal consumption differs from that of didanosine. See the complete prescribing information for didanosine delayed-release capsules. |
||
| ciprofloxacin | ↓ ciprofloxacin concentration | Administer didanosine at least 2 hours after or 6 hours before ciprofloxacin. |
| delavirdine | ↓ delavirdine concentration | Administer didanosine 1 hour after delavirdine. |
| ganciclovir | ↓ didanosine concentration | If there is no suitable alternative to ganciclovir, then use in combination with didanosine with caution. Monitor for didanosine-associated toxicity. |
| indinavir | ↓ indinavir concentration | Administer didanosine 1 hour after indinavir. |
| methadone | ↓ didanosine concentration | Do not coadminister methadone with didanosine pediatric powder due to significant decreases in didanosine concentrations. If coadministration of methadone and didanosine is necessary, the recommended formulation of didanosine is didanosine delayed-release capsules. Patients should be closely monitored for adequate clinical response when didanosine delayed-release capsules are coadministered with methadone, including monitoring for changes in HIV RNA viral load. |
| nelfinavir | ↓ No interacion 1 hour after didanosine | Administer nelfinavir 1 hour after didanosine. |
| tenofovir disoproxil fumarate | ↓ didanosine concentration | A dose reduction of didanosine to the following dosage once daily is recommended.a
|
Exposure to didanosine is increased when coadministered with tenofovir disoproxil fumarate [Table 8 and see Clinical Pharmacology (12.3, Table 12)]. Increased exposure may cause or worsen didanosine-related clinical toxicities, including pancreatitis, symptomatic hyperlactatemia/lactic acidosis, and peripheral neuropathy. Coadministration of tenofovir disoproxil fumarate with didanosine should be undertaken with caution, and patients should be monitored closely for didanosine-related toxicities and clinical response. Didanosine should be suspended if signs or symptoms of pancreatitis, symptomatic hyperlactatemia, or lactic acidosis develop [see Dosage and Administration (2.3), Warnings and Precautions (5)]. Suppression of CD4 cell counts has been observed in patients receiving tenofovir disoproxil fumarate with didanosine at a dose of 400 mg daily.
7.2 Predicted Drug Interactions
Predicted drug interactions with didanosine are listed in Table 9.
| Drug or Drug Class | Effect | Clinical Comment |
|---|---|---|
| ↑ Indicates increase. ↓ Indicates decrease. a Only if other drugs are not available and if clearly indicated. If treatment with life-sustaining drugs that cause pancreatic toxicity is required, suspension of didanosine is recommended [see Warnings and Precautions (5.1)]. b[See Warnings and Precautions (5.6).] |
||
| Drugs that may cause pancreatic toxicity | ↑ risk of pancreatitis | Use only with extreme cautiona
|
| Neurotoxic drugs | ↑ risk of neuropathy | Use with cautionb
|
| Antacids containing magnesium or aluminum | ↑ side effects associated with antacid components | Use caution with Didanosine Pediatric Powder for Oral Solution |
| Azole antifungals | ↓ ketoconazole or Itraconazole concentration | Administer drugs such as ketoconazole or itraconazole at least 2 hours before didanosine. |
| Quinolone antibiotics (see also ciprofloxacin in Table 8) | ↓ quinolone concentration | Consult package insert of the quinolone. |
| Tetracycline antibiotics | ↓ antibiotic concentration | Consult package insert of the tetracycline. |
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Teratogenic Effects
Pregnancy Category B
Reproduction studies have been performed in rats and rabbits at doses up to 12 and 14.2 times the estimated human exposure (based upon plasma levels), respectively, and have revealed no evidence of impaired fertility or harm to the fetus due to didanosine. At approximately 12 times the estimated human exposure, didanosine was slightly toxic to female rats and their pups during mid and late lactation. These rats showed reduced food intake and body weight gains but the physical and functional development of the offspring was not impaired and there were no major changes in the F2 generation. A study in rats showed that didanosine and/or its metabolites are transferred to the fetus through the placenta. Animal reproduction studies are not always predictive of human response.
There are no adequate and well-controlled studies of didanosine in pregnant women. Didanosine should be used during pregnancy only if the potential benefit justifies the potential risk.
Fatal lactic acidosis has been reported in pregnant women who received the combination of didanosine and stavudine with other antiretroviral agents. It is unclear if pregnancy augments the risk of lactic acidosis/hepatic steatosis syndrome reported in nonpregnant individuals receiving nucleoside analogues [see Warnings and Precautions (5.2)]. The combination of didanosine and stavudine should be used with caution during pregnancy and is recommended only if the potential benefit clearly outweighs the potential risk. Healthcare providers caring for HIV-infected pregnant women receiving didanosine should be alert for early diagnosis of lactic acidosis/hepatic steatosis syndrome.
Antiretroviral Pregnancy Registry
To monitor maternal-fetal outcomes of pregnant women exposed to didanosine and other antiretroviral agents, an Antiretroviral Pregnancy Registry has been established. Physicians are encouraged to register patients by calling 1-800-258-4263.
8.3 Nursing Mothers
The Centers for Disease Control and Prevention recommend that HIV-infected mothers not breastfeed their infants to avoid risking postnatal transmission of HIV. A study in rats showed that following oral administration, didanosine and/or its metabolites were excreted into the milk of lactating rats. It is not known if didanosine is excreted in human milk. Because of both the potential for HIV transmission and the potential for serious adverse reactions in nursing infants, mothers should be instructed not to breastfeed if they are receiving didanosine.
8.4 Pediatric Use
Use of didanosine in pediatric patients from 2 weeks of age through adolescence is supported by evidence from adequate and well-controlled studies of didanosine in adult and pediatric patients [see Dosage and Administration (2), Adverse Reactions (6.1), Clinical Pharmacology (12.3), and Clinical Studies (14)].
8.5 Geriatric Use
In an Expanded Access Program for patients with advanced HIV infection, patients aged 65 years and older had a higher frequency of pancreatitis (10%) than younger patients (5%) [see Warnings and Precautions (5.1)]. Clinical studies of didanosine did not include sufficient numbers of subjects aged 65 years and over to determine whether they respond differently than younger subjects. Didanosine is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection. In addition, renal function should be monitored and dosage adjustments should be made accordingly [see Dosage and Administration (2.2)].
8.6 Renal Impairment
Patients with renal impairment (creatinine clearance of less than 60 mL/min) may be at greater risk of toxicity from didanosine due to decreased drug clearance [see Clinical Pharmacology (12.3)]. A dose reduction is recommended for these patients [see Dosage and Administration (2)].
10 OVERDOSAGE
There is no known antidote for didanosine overdosage. In phase 1 studies, in which didanosine was initially administered at doses ten times the currently recommended dose, toxicities included: pancreatitis, peripheral neuropathy, diarrhea, hyperuricemia, and hepatic dysfunction. Didanosine is not dialyzable by peritoneal dialysis, although there is some clearance by hemodialysis [see Clinical Pharmacology (12.3)].
11 DESCRIPTION
Didanosine a synthetic purine nucleoside analogue active against HIV-1.
Didanosine is available as a pediatric powder for oral solution [see How Supplied/Storage and Handling (16)] and as didanosine delayed-release capsules, containing enteric-coated beadlets [consult prescribing information for didanosine delayed-release capsules].
The chemical name for didanosine is 2’,3’-dideoxyinosine. The structural formula is:
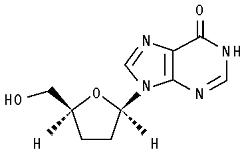
Didanosine USP is a white crystalline powder with the molecular formula C10H12N4O3 and a molecular weight of 236.2. The aqueous solubility of didanosine at 25°C and pH of approximately 6 is 27.3 mg/mL. Didanosine is unstable in acidic solutions. For example, at pH less than 3 and 37° C, 10% of didanosine decomposes to hypoxanthine in less than 2 minutes.
12 CLINICAL PHARMACOLOGY
12.3 Pharmacokinetics
The pharmacokinetic parameters of didanosine are summarized in Table 10. Didanosine is rapidly absorbed, with peak plasma concentrations generally observed from 0.25 to 1.5 hours following oral dosing. Increases in plasma didanosine concentrations were dose proportional over the range of 50 to 400 mg. Steady-state pharmacokinetic parameters did not differ significantly from values obtained after a single dose. Binding of didanosine to plasma proteins in vitro was low (less than 5%). Based on data from in vitro and animal studies, it is presumed that the metabolism of didanosine in man occurs by the same pathways responsible for the elimination of endogenous purines.
| Parameter | Adult Patientsa | n | Pediatric Patientsb | |||
|---|---|---|---|---|---|---|
| 8 months to 19 years | n | 2 weeks to 4 months | n | |||
| CSF = cerebrospinal fluid, ND = not determined. a Parameter units for adults were converted to the same units in pediatric patients to facilitate comparisons among populations: mean adult body weight = 70 kg and mean adult body surface area = 1.73 m2. b In 1-day old infants (n=10), the mean ± SD apparent oral clearance was 1523 ± 1176 mL/min/m2 and half-life was 2 ± 0.7 h. c Following IV administration. d Following IV administration in adults and IV or oral administration in pediatric patients. e Mean ± SE. f Following oral administration. g Apparent oral clearance estimate was determined as the ratio of the mean systemic clearance and the mean oral bioavailability estimate. |
||||||
| Oral bioavailability (%) | 42 ± 12 | 6 | 25 ± 20 | 46 | ND | |
| Apparent volume of distributionc (L/m2) | 43.7 ± 8.9 | 6 | 28 ± 15 | 49 | ND | |
| CSF-plasma ratiod
| 21 ± 0.03%e
| 5 | 46% (range 12 to 85%) | 7 | ND | |
| Systemic clearancec (mL/min/m2) | 526 ± 64.7 | 6 | 516 ± 184 | 49 | ND | |
| Renal clearancef (mL/min/m2) | 223 ± 85 | 6 | 240 ± 90 | 15 | ND | |
| Apparent oral clearanceg (mL/min/m2) | 1252 ± 154 | 6 | 2064 ± 736 | 48 | 1353 ± 759 | 41 |
| Elimination half-lifef (h) | 1.5 ± 0.4 | 6 | 0.8 ± 0.3 | 60 | 1.2 ± 0.3 | 21 |
| Urinary recovery of didanosinef (%) | 18 ± 8 | 6 | 18 ± 10 | 15 | ND | |
Effect of Food
Didanosine peak plasma concentrations (Cmax) and area under the plasma concentration time curve (AUC) were decreased by approximately 55% when didanosine tablets were administered up to 2 hours after a meal. Administration of didanosine tablets up to 30 minutes before a meal did not result in any significant changes in bioavailability [see Dosage and Administration (2)]. Didanosine should be taken on an empty stomach.
Special Populations
Renal Insufficiency: Data from two studies in adults indicated that the apparent oral clearance of didanosine decreased and the terminal elimination half-life increased as creatinine clearance decreased (see Table 11). Following oral administration, didanosine was not detectable in peritoneal dialysate fluid (n=6); recovery in hemodialysate (n=5) ranged from 0.6% to 7.4% of the dose over a 3 to 4 hour dialysis period. The absolute bioavailability of didanosine was not affected in patients requiring dialysis. [See Dosage and Administration (2.2).]
| ND = not determined due to anuria. CLcr = creatinine clearance. CL/F = apparent oral clearance. CLR = renal clearance. |
|||||
| Parameter
| Creatinine Clearance (mL/min)
| ||||
| at least 90
n=12 | 60-90
n=6 | 30-59
n=6 | 10-29
n=3 | Dialysis Patients
n=11 |
|
| CLcr (mL/min) | 112 ± 22 | 68 ± 8 | 46 ± 8 | 13 ± 5 | ND |
| CL/F (mL/min) | 2164 ± 638 | 1566 ± 833 | 1023 ± 378 | 628 ± 104 | 543 ± 174 |
| CLR (mL/min) | 458 ± 164 | 247 ± 153 | 100 ± 44 | 20 ± 8 | less than 10 |
| T½ (h) | 1.42 ± 0.33 | 1.59 ± 0.13 | 1.75 ± 0.43 | 2 ± 0.3 | 4.1 ± 1.2 |
Hepatic Impairment: The pharmacokinetics of didanosine have been studied in 12 non-HIV-infected subjects with moderate (n=8) to severe (n=4) hepatic impairment (Child-Pugh Class B or C). Mean AUC and Cmax values following a single 400 mg dose of didanosine were approximately 13% and 19% higher, respectively, in patients with hepatic impairment compared to matched healthy subjects. No dose adjustment is needed, because a similar range and distribution of AUC and Cmax values was observed for subjects with hepatic impairment and matched healthy controls. [See Dosage and Administration (2.3).]
Pediatric Patients: The pharmacokinetics of didanosine have been evaluated in HIV-exposed and HIV-infected pediatric patients from birth to adulthood. Overall, the pharmacokinetics of didanosine in pediatric patients are similar to those of didanosine in adults. Didanosine plasma concentrations appear to increase in proportion to oral doses ranging from 25 to 120 mg/m2 in pediatric patients less than 5 months old and from 80 to 180 mg/m2 in children above 8 months old. For information on controlled clinical studies in pediatric patients [see Clinical Studies (14.2) and Use in Specific Populations (8.4)].
Geriatric Patients: Didanosine pharmacokinetics have not been studied in patients over 65 years of age [see Use in Specific Populations (8.5)].
Gender: The effects of gender on didanosine pharmacokinetics have not been studied.
Drug Interactions
Tables 12 and 13 summarize the effects on AUC and Cmax, with a 95% confidence interval (CI) when available, following coadministration of didanosine with a variety of drugs. Drug-drug interactions for didanosine buffered tablets are applicable to the didanosine pediatric powder formulation and are noted in Tables 12 and 13. For clinical recommendations based on drug interaction studies for drugs in bold font [see Dosage and Administration (2.3 for Concomitant Therapy with Tenofovir Disoproxil Fumarate), Contraindications (4.1), and Drug Interactions (7.1 and 7.2)].
| % Change of Didanosine Pharmacokinetic Parametersa | ||||
|---|---|---|---|---|
| Drug | Didanosine Dosage | n | AUC of Didanosine (95% CI) | Cmax of Didanosine (95% CI) |
| ↑ Indicates increase. ↓ Indicates decrease. ↔ Indicates no change, or mean increase or decrease of less than 10%. a The 95% confidence intervals for the percent change in the pharmacokinetic parameter are displayed. b HIV-infected patients. c 90% CI. d Comparisons are made to a parallel control group not receiving methadone (n=10) eComparisons are made to historical controls (n=68, pooled from 3 studies) conducted in healthy subjects. The number of subjects evaluated for AUC and Cmax is 15 and 16, respectively. f For results of drug interaction studies between the enteric-coated formulation of didanosine (didanosine delayed-release capsules) and methadone, see the complete prescribing information for didanosine delayed-release capsules. g Tenofovir disoproxil fumarate. h For results of drug interaction studies between the enteric-coated formulation of didanosine (didanosine delayed-release capsules) and tenofovir disoproxil fumarate, see the complete prescribing information for didanosine delayed-release capsules. i Patients less than 60 kg with creatinine clearance of at least 60 mL/min. NA = Not available. |
||||
| allopurinol,
| | |||
| renally impaired, 300 mg/day
| 200 mg single dose | 2 | ↑ 312% | ↑ 232% |
| healthy volunteer, 300 mg/day for 7 days
| 400 mg single dose | 14 | ↑ 113% | ↑ 69% |
| ciprofloxacin, 750 mg every 12 hours for 3 days, 2 hours before didanosine
| 200 mg every 12 hours for 3 days | 8b
| ↓ 16% | ↓ 28% |
| ganciclovir, 1000 mg every 8 hours, 2 hours after didanosine indinavir, 800 mg single dose, | 200 mg every 12 hours | 12 | ↑ 111% | NA |
| simultaneous | 200 mg single dose | 16 | ↔ | ↔ |
| 1 hour before didanosine
| 200 mg single dose | 16 | ↓ 17% (-27, -7%)c | ↓ 13% (-28, 5%)c |
| ketoconazole, 200 mg/day for 4 days, 2 hours before didanosine
| 375 mg every 12 hours for 4 days | 12b
| ↔ | ↓ 12% |
| methadone, chronic maintenance dosef
| 200 mg single dose | 16d
| ↓ 57% | ↓ 66% |
| 400 mg single dose | 15, 16e
| ↓ 29% (-40, -16%)c | ↓ 41% (-54, -26%)c |
|
| tenofovir,g,h 300 mg once daily, 1 hour after didanosine
| 250i mg or 400 mg once daily for 7 days | 14 | ↑ 44% (31, 59%)c | ↑ 28% (11, 48%)c |
| loperamide, 4 mg every 6 hours for 1 day
| 300 mg single dose | 12b
| ↔ | ↓ 23% |
| metoclopramide, 10 mg single dose
| 300 mg single dose | 12b
| ↔ | ↑ 13% |
| ranitidine, 150 mg single dose, 2 hours before didanosine | 375 mg single dose | 12b
| ↑ 14% | ↑ 13% |
| rifabutin, 300 or 600 mg/day for 12 days | 167 mg or 250 mg every 12 hours for 12 days | 11 | ↑ 13% (-1, 27%) | ↑ 17% (-4, 38%) |
| ritonavir, 600 mg every 12 hours for 4 days | 200 mg every 12 hours for 4 days | 12 | ↓ 13% (0, 23%) | ↓ 16% (5, 26%) |
| stavudine, 40 mg every 12 hours for 4 days | 100 mg every 12 hours for 4 days | 10 | ↔ | ↔ |
| sulfamethoxazole, 1000 mg single dose | 200 mg single dose | 8b
| ↔ | ↔ |
| trimethoprim, 200 mg single dose | 200 mg single dose | 8b
| ↔ | ↑ 17% (-23, 77%) |
| zidovudine, 200 mg every 8 hours for 3 days | 200 mg every 12 hours for 3 days | 6b
| ↔ | ↔ |
| % Change of Coadministered Drug Pharmacokinetic Parametersa |
||||
|---|---|---|---|---|
| Drug | Didanosine Dosage | n | AUC of Coadministered Drug (95% CI) | Cmax of Coadministered Drug (95% CI) |
| ↑ Indicates increase. ↓ Indicates decrease. ↔ Indicates no change, or mean increase or decrease of less than 10%. a The 95% confidence intervals for the percent change in the pharmacokinetic parameter are displayed. b HIV-infected patients. c Tenofovir disoproxil fumarate. d Patients less than 60 kg with creatinine clearance of at least 60 mL/min. NA = Not available. |
||||
| ciprofloxacin
| | |||
| 750 mg every 12 hours for 3 days, 2 hours before didanosine | 200 mg every 12 hours for 3 days | 8b
| ↓ 26% | ↓ 16% |
| 750 mg single dose | buffered placebo tablet | 12 | ↓ 98% | ↓ 93% |
| delavirdine, 400 mg single dose simultaneous | 125 mg or 200 mg every 12 hours | 12b
| ↓ 32% | ↓ 53% |
| 1 hour before didanosine | 125 mg or 200 mg every 12 hours | 12b
| ↑ 20% | ↑ 18% |
| ganciclovir, 1000 mg every 8 hours, 2 hours after didanosine | 200 mg every 12 hours | 12b
| ↓ 21% | NA |
| indinavir, 800 mg single dose simultaneous | 200 mg single dose | 16 | ↓ 84% | ↓ 82% |
| 1 hour before didanosine | 200 mg single dose | 16 | ↓ 11% | ↓ 4% |
| ketoconazole, 200 mg/day for 4 days, 2 hours before didanosine | 375 mg every 12 hours for 4 days | 12b
| ↓ 14% | ↓ 20% |
| nelfinavir, 750 mg single dose, 1 hour after didanosine | 200 mg single dose | 10b
| ↑ 12% | ↔ |
| dapsone, 100 mg single dose | 200 mg every 12 hours for 14 days | 6b
| ↔ | ↔ |
| ranitidine, 150 mg single dose, 2 hours before didanosine | 375 mg single dose | 12b
| ↓ 16% | ↔ |
| ritonavir, 600 mg every 12 hours for 4 days | 200 mg every 12 hours for 4 days | 12 | ↔ | ↔ |
| stavudine, 40 mg every 12 hours for 4 days | 100 mg every 12 hours for 4 days | 10b
| ↔ | ↑ 17% |
| sulfamethoxazole, 1000 mg single dose | 200 mg single dose | 8b
| ↓ 11% (-17, -4%) | ↓ 12% (-28, 8%) |
| tenofovir,c 300 mg once daily 1 hour after didanosine | 250d mg or 400 mg once daily for 7 days | 14 | ↔ | ↔ |
| trimethoprim, 200 mg single dose | 200 mg single dose | 8b
| ↑ 10% (-9, 34%) | ↓ 22% (-59, 49%) |
| zidovudine, 200 mg every 8 hours for 3 days | 200 mg every 12 hours for 3 days | 6b
| ↓ 10% (-27, 11%) | ↓ 16.5% (-53, 47%) |
12.4 Microbiology
Mechanism of Action
Didanosine is a synthetic nucleoside analogue of the naturally occurring nucleoside deoxyadenosine in which the 3’-hydroxyl group is replaced by hydrogen. Intracellularly, didanosine is converted by cellular enzymes to the active metabolite, dideoxyadenosine 5’-triphosphate. Dideoxyadenosine 5’-triphosphate inhibits the activity of HIV-1 reverse transcriptase both by competing with the natural substrate, deoxyadenosine 5’-triphosphate, and by its incorporation into viral DNA causing termination of viral DNA chain elongation.
Antiviral Activity in Cell Culture
The anti-HIV-1 activity of didanosine was evaluated in a variety of HIV-1 infected lymphoblastic cell lines and monocyte/macrophage cell cultures. The concentration of drug necessary to inhibit viral replication by 50% (EC50) ranged from 2.5 to 10 µM (1 µM = 0.24 mcg/mL) in lymphoblastic cell lines and 0.01 to 0.1 µM in monocyte/macrophage cell cultures.
Resistance
HIV-1 isolates with reduced sensitivity to didanosine have been selected in cell culture and were also obtained from patients treated with didanosine. Genetic analysis of isolates from didanosine-treated patients showed mutations in the reverse transcriptase gene that resulted in the amino acid substitutions K65R, L74V, and M184V. The L74V substitution was most frequently observed in clinical isolates. Phenotypic analysis of HIV-1 isolates from 60 patients (some with prior zidovudine treatment) receiving 6 to 24 months of didanosine monotherapy showed that isolates from 10 of 60 patients exhibited an average of a 10-fold decrease in susceptibility to didanosine in cell culture compared to baseline isolates. Clinical isolates that exhibited a decrease in didanosine susceptibility harbored one or more didanosine resistance-associated substitutions.
Cross-resistance
HIV-1 isolates from 2 of 39 patients receiving combination therapy for up to 2 years with didanosine and zidovudine exhibited decreased susceptibility to didanosine, lamivudine, stavudine, zalcitabine, and zidovudine in cell culture. These isolates harbored five substitutions (A62V, V75I, F77L, F116Y, and Q151M) in the reverse transcriptase gene. In data from clinical studies, the presence of thymidine analogue mutations (M41L, D67N, L210W, T215Y, K219Q) has been shown to decrease the response to didanosine.
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Lifetime carcinogenicity studies were conducted in mice and rats for 22 and 24 months, respectively. In the mouse study, initial doses of 120, 800, and 1200 mg/kg/day for each sex were lowered after 8 months to 120, 210, and 210 mg/kg/day for females and 120, 300, and 600 mg/kg/day for males. The two higher doses exceeded the maximally tolerated dose in females and the high dose exceeded the maximally tolerated dose in males. The low dose in females represented 0.68-fold maximum human exposure and the intermediate dose in males represented 1.7-fold maximum human exposure based on relative AUC comparisons. In the rat study, initial doses were 100, 250, and 1000 mg/kg/day, and the high dose was lowered to 500 mg/kg/day after 18 months. The upper dose in male and female rats represented 3-fold maximum human exposure.
Didanosine induced no significant increase in neoplastic lesions in mice or rats at maximally tolerated doses.
Didanosine was positive in the following genetic toxicology assays: 1) the Escherichia coli tester strain WP2 uvrA bacterial mutagenicity assay; 2) the L5178Y/TK+/- mouse lymphoma mammalian cell gene mutation assay; 3) the in vitro chromosomal aberrations assay in cultured human peripheral lymphocytes; 4) the in vitro chromosomal aberrations assay in Chinese Hamster Lung cells; and 5) the BALB/c 3T3 in vitro transformation assay. No evidence of mutagenicity was observed in an Ames Salmonella bacterial mutagenicity assay or in rat and mouse in vivo micronucleus assays.
13.2 Animal Toxicology and/or Pharmacology
Evidence of a dose-limiting skeletal muscle toxicity has been observed in mice and rats (but not in dogs) following long-term (greater than 90 days) dosing with didanosine at doses that were approximately 1.2 to 12 times the estimated human exposure. The relationship of this finding to the potential of didanosine to cause myopathy in humans is unclear. However, human myopathy has been associated with administration of didanosine and other nucleoside analogues.
14 CLINICAL STUDIES
14.1 Adult Patients
Combination Therapy
START 2 was a multicenter, randomized, open-label study comparing didanosine (200 mg twice daily)/stavudine/indinavir to zidovudine/lamivudine/indinavir in 205 treatment-naive patients. Both regimens resulted in a similar magnitude of suppression of HIV-1 RNA levels and increases in CD4 cell counts through 48 weeks.
Study AI454-148 was a randomized, open-label, multicenter study comparing treatment with didanosine (400 mg once daily) plus stavudine (40 mg twice daily) and nelfinavir (750 mg three times daily) versus zidovudine (300 mg twice daily) plus lamivudine (150 mg twice daily) and nelfinavir (750 mg three times daily) in 756 treatment-naive patients, with a median CD4 cell count of 340 cells/mm3 (range 80 to 1568 cells/mm3) and a median plasma HIV-1 RNA of 4.69 log10 copies/mL (range 2.6 to 5.9 log10 copies/mL) at baseline. Median CD4 cell count increases at 48 weeks were 188 cells/mm3 in both treatment groups. Treatment response and outcomes through 48 weeks are shown in Figure 1 and Table 14.
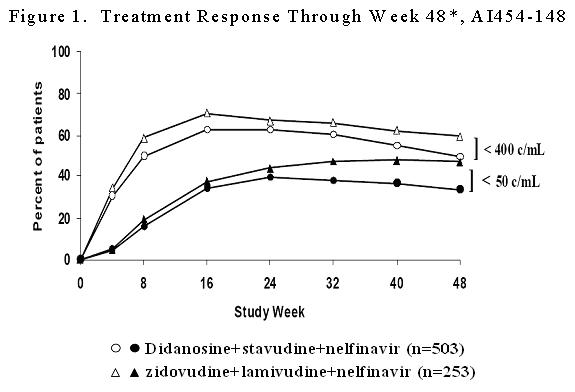
* Percent of patients at each time point who have HIV RNA <400 or <50 copies/mL, are on their original study medication (except stavudine-zidovudine switches), and have not experienced an AIDS-defining event.
| Week 48 Status | Percent of Patients with HIV-1 RNA less than 400 copies/mL (less than 50 copies/mL) |
|
|---|---|---|
| didanosine/stavudine/nelfinavir n=503 | lamivudine/zidovudine/ nelfinavir n=253 |
|
| * p less than 0.05 for the differences between treatment groups, by Cochran-Mantel-Haenszel test. a Patients achieved virologic response [two consecutive viral loads less than 400 (less than 50) copies/mL] and maintained it to Week 48. b Includes viral rebound and failing to achieve confirmed less than 400 (less than 50) copies/mL by Week 48. c Includes lost to follow-up, noncompliance, withdrawal, and pregnancy. |
||
| Respondera
| 50* (34*) | 59 (47) |
| Virologic failureb
| 36 (57) | 32 (48) |
| Death or disease progression | less than 1 (less than 1) | 1 (less than 1) |
| Discontinued due to adverse events | 4 (2) | 2 (less than 1) |
| Discontinued due to other reasonsc
| 6 (3) | 4 (2) |
| Never initiated treatment | 4 (4) | 2 (2) |
Monotherapy
The efficacy of didanosine was demonstrated in two randomized, double-blind studies comparing didanosine, given on a twice-daily schedule, to zidovudine, given three times daily, in 617 (ACTG 116A, conducted 1989 to 1992) and 913 (ACTG 116B/117, conducted 1989 to 1991) patients with symptomatic HIV infection or AIDS who were treated for more than one year. In treatment-naive patients (ACTG 116A), the rate of HIV disease progression or death was similar between the treatment groups; mortality rates were 26% for patients receiving didanosine and 21% for patients receiving zidovudine. Of the patients who had received previous zidovudine treatment (ACTG 116B/117), those treated with didanosine had a lower rate of HIV disease progression or death (32%) compared to those treated with zidovudine (41%); however, survival rates were similar between the treatment groups.
Studies have demonstrated that the clinical benefit of monotherapy with antiretrovirals, including didanosine, was time limited.
14.2 Pediatric Patients
Efficacy in pediatric patients was demonstrated in a randomized, double-blind, controlled study (ACTG 152, conducted 1991 to 1995) involving 831 patients 3 months to 18 years of age treated for more than 1.5 years with zidovudine (180 mg/m2 every 6 hours), didanosine (120 mg/m2 every 12 hours), or zidovudine (120 mg/m2 every 6 hours) plus didanosine (90 mg/m2 every 12 hours). Patients treated with didanosine or didanosine plus zidovudine had lower rates of HIV-1 disease progression or death compared with those treated with zidovudine alone.
16 HOW SUPPLIED/STORAGE AND HANDLING
Didanosine for Oral Solution, USP is white to almost white, crystalline powder and is supplied as follows:
2 g/bottle per carton NDC 65862-109-02
4 g/bottle per carton NDC 65862-110-04
Prior to dispensing, the pharmacist must reconstitute dry powder with Purified Water, USP, to an initial concentration of 20 mg/mL and immediately mix the resulting solution with antacid to a final concentration of 10 mg/mL as follows:
20 mg/mL Initial Solution
Reconstitute the product to 20 mg/mL by adding 100 mL or 200 mL of Purified Water, USP, to the 2 g or 4 g of didanosine powder, respectively, in the product bottle.
10 mg/mL Final Admixture
- Immediately mix one part of the 20 mg/mL initial solution with one part of Maximum Strength Mylanta® Liquid for a final dispensing concentration of 10 mg didanosine per mL. For patient home use, the admixture should be dispensed in appropriately sized, flint-glass or plastic (HDPE, PET, or PETG) bottles with child-resistant closures.
- Instruct the patient to shake the admixture thoroughly prior to use and to store the tightly closed container in the refrigerator.
Storage
Storedry powder at 20° to 25° C (68° to 77° F); excursions permitted to 15° to 30° C (59° to 86° F) [ see USP Controlled Room Temperature] .
The didanosine admixture may be stored up to 30 days in a refrigerator, 36° to 46°F (2° to 8°C). Discard any unused portion after 30 days.
Mylanta® is a registered trademark of Johnson & Johnson-Merck Consumer Pharmaceuticals Company.
17 PATIENT COUNSELING INFORMATION
See Medication Guide.
17.1 Pancreatitis
Patients should be informed that a serious toxicity of didanosine, used alone and in combination regimens, is pancreatitis, which may be fatal.
17.2 Peripheral Neuropathy
Patients should be informed that peripheral neuropathy, manifested by numbness, tingling, or pain in hands or feet, may develop during therapy with didanosine. Patients should be counseled that peripheral neuropathy occurs with greatest frequency in patients with advanced HIV-1 disease or a history of peripheral neuropathy, and that discontinuation of didanosine may be required if toxicity develops.
17.3 Lactic Acidosis and Severe Hepatomegaly with Steatosis
Patients should be informed that lactic acidosis and severe hepatomegaly with steatosis, including fatal cases, have been reported with the use of nucleoside analogues alone or in combination, including didanosine and other antiretrovirals.
17.4 Hepatic Toxicity
Patients should be informed that hepatotoxicity including fatal hepatic adverse events were reported in patients with preexisting liver dysfunction. The safety and efficacy of didanosine have not been established in HIV-infected patients with significant underlying liver disease.
17.5 Non-cirrhotic Portal Hypertension
Patients should be informed that non-cirrhotic portal hypertension has been reported in patients taking didanosine, including cases leading to liver transplantation or death.
17.6 Retinal Changes and Optic Neuritis
Patients should be informed that retinal changes and optic neuritis have been reported in adult and pediatric patients.
17.7 Fat Redistribution
Patients should be informed that redistribution or accumulation of body fat may occur in patients receiving antiretroviral therapy and that the cause and long-term health effects of these conditions are not known at this time.
17.8 Concomitant Therapy
Patients should be informed that when didanosine is used in combination with other agents with similar toxicities, the incidence of adverse events may be higher than when didanosine is used alone. These patients should be followed closely.
Patients should be cautioned about the use of medications or other substances, including alcohol, which may exacerbate didanosine toxicities.
17.9 General Information
Didanosine is not a cure for HIV-1 infection, and patients may continue to experience illnesses associated with HIV-1 infection, including opportunistic infections. Therefore, patients should remain under the care of a physician when using didanosine.
Patients should be advised to avoid doing things that can spread HIV-1 infection to others.
- Do not share needles or other injection equipment.
- Do not share personal items that can have blood or body fluids on them, like toothbrushes and razor blades.
- Do not have any kind of sex without protection. Always practice safe sex by using a latex or polyurethane condom or other barrier method to lower the chance of sexual contact with semen, vaginal secretions, or blood.
- Do not breastfeed. It is not known if didanosine can be passed to your baby in your breast milk and whether it could harm your baby. Also, mothers with HIV-1 should not breastfeed because HIV-1 can be passed to the baby in breast milk.
Patients should be informed that the preferred dosing frequency of didanosine is twice daily because there is more evidence to support the effectiveness of this dosing frequency. Once-daily dosing should be considered only for patients whose management requires once-daily dosing of didanosine.
Patients should be instructed to not miss a dose but if they do, patients should take didanosine as soon as possible. Patients should be told that if it is almost time for the next dose, they should skip the missed dose and continue with the regular dosing schedule.
Patients should be instructed to contact a poison control center or emergency room right away in case of an overdose.
Manufactured for:
Aurobindo Pharma USA, Inc.
2400 Route 130 North
Dayton, NJ 08810
Manufactured by:
Aurobindo Pharma Limited
Hyderabad-500 072, India
Revised: 02/2012
Medication Guide
Didanosine for Oral Solution, USP
(didanosine, also known as ddI)
Read this Medication Guide before you start taking didanosine for oral solution and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or your treatment. You and your healthcare provider should talk about your treatment with didanosine for oral solution before you start taking it and at regular check-ups. You should stay under your healthcare provider's care when taking didanosine for oral solution.
What is the most important information I should know about didanosine for oral solution?
Didanosine for oral solution may cause serious side effects, including:
1. Swelling of your pancreas (pancreatitis) that may cause death. Pancreatitis can happen at any time during your treatment with didanosine for oral solution. Before you start taking didanosine for oral solution, tell your healthcare provider if you:
- have had pancreatitis
- have advanced HIV (human immunodeficiency virus) infection
- have kidney problems
- drink alcoholic beverages
- take a medicine called ZERIT® (stavudine)
It is important to call your healthcare provider right away if you have:
- stomach pain
- swelling of your stomach
- nausea and vomiting
- fever
2. Build-up of acid in your blood (lactic acidosis). Lactic acidosis must be treated in the hospital as it may cause death. The risk for lactic acidosis may be higher if you:
- have liver problems
- are pregnant. There have been deaths reported in pregnant women who get lactic acidosis after taking didanosine for oral solution and ZERIT (stavudine).
- are overweight
- have been treated for a long time with other medicines to treat HIV
It is important to call your health care provider right away if you:
- feel weak or tired
- have unusual (not normal) muscle pain
- have trouble breathing
- have stomach pain with nausea and vomiting
- feel cold, especially in your arms and legs
- feel dizzy or light-headed
- have a fast or irregular heartbeat
3. Liver problems. Some people (including pregnant women) who have taken didanosine for oral solution have had serious liver problems. These problems include liver enlargement (hepatomegaly), fat in the liver (steatosis), liver failure, and high blood pressure in the large vein of the liver (portal hypertension). Severe liver problems can lead to liver transplantation or death in some people taking didanosine for oral solution. Your healthcare provider should check your liver function while you are taking didanosine for oral solution. You should be especially careful if you have a history of heavy alcohol use or liver problems.
It is important to call your healthcare provider right away if you have:
- yellowing of your skin or the white of your eyes (jaundice)
- dark urine
- pain on the right side of your stomach
- swelling of your stomach
- easy bruising or bleeding
- loss of appetite
- nausea or vomiting
- vomiting blood or dark colored stools (bowel movements)
What is didanosine for oral solution?
Didanosine for oral solution is a prescription medicine used with other antiretroviral medicines to treat human immunodeficiency virus (HIV) infection in children and adults. Didanosine for oral solution belongs to a class of drugs called nucleoside analogues.
Didanosine for oral solution will not cure your HIV infection. At present there is no cure for HIV infection. Even while taking didanosine for oral solution, you may continue to have HIV-related illnesses, including infections with other disease-producing organisms. Continue to see your healthcare provider regularly and report any medical problems that occur.
Who should not take didanosine for oral solution?
Do not take didanosine for oral solution if you take:
- ZYLOPRIM®, LOPURIN®, ALOPRIM® (allopurinol)
- COPEGUS®, REBETOL®, RIBASPHERE®, RIBAVIRIN®, VIRAZOLE® (ribavirin)
What should I tell my healthcare provider before taking didanosine for oral solution?
Before you take didanosine for oral solution, tell your healthcare provider if you:
- have or had kidney problems
- have or had liver problems (such as hepatitis)
- have or had persistent numbness, tingling, or pain in the hands or feet (neuropathy)
- have any other medical conditions
- are pregnant or plan to become pregnant. It is not known if didanosine for oral solution will harm your unborn baby. Tell your healthcare provider right away if you become pregnant while taking didanosine for oral solution. You and your healthcare provider will decide if you should take didanosine for oral solution while you are pregnant.
Pregnancy Registry: There is a pregnancy registry for women who take antiviral medicines during pregnancy. The purpose of the registry is to collect information about the health of you and your baby. Talk to your doctor about how you can take part in this registry.
- are breastfeeding or plan to breastfeed. Do not breastfeed. It is not known if didanosine can be passed to your baby in your breast milk and whether it could harm your baby. Also, mothers with HIV-1 should not breastfeed because HIV-1 can be passed to the baby in the breast milk.
Tell your healthcare provider about all the medicines you take, including prescription and non-prescription medicines, vitamins and herbal supplements. Didanosine for oral solution may affect the way other medicines work, and other medicines may affect how didanosine for oral solution works.
Especially tell your healthcare provider if you take:
- VIREAD® (tenofovir disoproxil fumarate)
- DROXIA®, HYDREA® (hydroxyurea)
- RESCRIPTOR® (delavirdine mesylate)
- CYTOVENE®, VALCYTE® (ganciclovir)
- CRIXIVAN® (indinavir)
- DOLOPHINE® HYDROCHLORIDE, METHADOSE® (methadone)
- VIRACEPT® (nelfinavir)
- antacids
- antifungal medicines such as NIZORAL® (ketoconazole) or SPORANOX® (itraconazole)
- quinolone antibiotics such as CIPRO®, PROQUIN® XR (ciprofloxacin)
- tetracycline antibiotics such as BRISTACYCLINE®, SUMYCIN® (tetracycline)
- alcoholic beverages
Know the medicines you take. Keep a list of your medicines and show it to your healthcare provider and pharmacist when you get a new medicine.
Ask your healthcare provider if you are not sure if you take one of the medicines listed above.
How should I take didanosine for oral solution?
- Take didanosine for oral solution exactly as your healthcare provider tells you to take it.
- Your healthcare provider will tell you how much didanosine for oral solution to take and when to take it.
- Your healthcare provider may change your dose. Do not change your dose of didanosine for oral solution without talking to your healthcare provider.
- Do not take didanosine for oral solution with food. Take didanosine for oral solution on an empty stomach at least 30 minutes before or 2 hours after you eat.
- Try not to miss a dose, but if you do, take it as soon as possible. If it is almost time for the next dose, skip the missed dose and continue your regular dosing schedule.
- Some medicines should not be taken at the same time of day that you take didanosine for oral solution. Check with your healthcare provider.
- If your kidneys are not working well, your healthcare provider will need to do regular blood and urine tests to check how they are working while you take didanosine for oral solution. Your healthcare provider may also lower your dosage of didanosine for oral solution if your kidneys are not working well.
- If you take too much didanosine for oral solution, contact a poison control center or emergency room right away.
What should I avoid while taking didanosine for oral solution?
- Alcohol. Do not drink alcohol while you take didanosine for oral solution. Alcohol may increase your risk of getting pain and swelling of your pancreas (pancreatitis) or may damage your liver.
What are the possible side effects of didanosine for oral solution?
Didanosine for oral solution can cause pancreatitis, lactic acidosis, and liver problems. See “What is the most important information I should know about didanosine for oral solution?” at the beginning of this Medication Guide.
- Vision changes. You should have regular eye exams while you take didanosine for oral solution.
- Peripheral neuropathy. Symptoms include: numbness, tingling, or pain in your hands or feet. This condition is more likely to happen in people who have had it before, in patients taking medicines that affect the nerves, and in people with advanced HIV disease. A child may not notice these symptoms. Ask your child's healthcare provider for the signs and symptoms of peripheral neuropathy in children.
- Changes in your immune system (immune reconstitution syndrome). Your immune system may get stronger and begin to fight infections that have been hidden in your body for a long time. Tell your healthcare provider if you start having new or worse symptoms of infection after you start taking HIV medicine.
- Changes in body fat (fat redistribution). Changes in body fat have been seen in people who take antiretroviral medicines. These changes may include:
- more fat in or around your
- upper back and neck (buffalo hump)
- breasts or chest
- trunk
- less fat in your
- legs
- arms
- face
Tell your healthcare provider if you have any of the symptoms listed above.
The most common side effects of didanosine for oral solution include:
- diarrhea
- stomach pain
- nausea
- vomiting
- headache
- rash
Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
These are not all the possible side effects of didanosine for oral solution. For more information, ask your healthcare provider or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at l-800-FDA-1088.
How should I store didanosine for oral solution?
Store the didanosine for oral solution mixture in a tightly closed container in the refrigerator between 36° to 46°F (2° to 8°C) for up to 30 days.
- Safely throw away any unused didanosine for oral solution after 30 days.
Keep didanosine for oral solution and all medicines out of the reach of children and pets.
General information about the safe and effective use of didanosine for oral solution
Avoid doing things that can spread HIV-1 infection to others.
- Do not share needles or other injection equipment.
- Do not share personal items that can have blood or body fluids on them, like toothbrushes and razor blades.
-
Do not have any kind of sex without protection. Always practice safe sex by using a latex or polyurethane condom or other barrier method to lower the chance of sexual contact with semen, vaginal secretions, or blood.
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use didanosine for oral solution for a condition for which it was not prescribed. Do not give didanosine for oral solution to other people, even if they have the same symptoms as you have. It may harm them. Do not keep medicine that is out of date or that you no longer need. Dispose of unused medicines through community take-back disposal programs when available or place didanosine for oral solution in an unrecognizable closed container in the household trash.
This Medication Guide summarizes the most important information about didanosine for oral solution. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about didanosine for oral solution that is written for health professionals. For more information, call 1-866-850-2876.
What are the ingredients in didanosine for oral solution?
Active Ingredient: didanosine
Inactive Ingredients:
Pediatric Oral Solution: Maximum Strength Mylanta® Liquid.
All brands listed are the trademarks of their respective owners and are not trademarks of Aurobindo Pharma Limited.
Manufactured for:
Aurobindo Pharma USA, Inc.
2400 Route 130 North
Dayton, NJ 08810
Manufactured by:
Aurobindo Pharma Limited
Hyderabad-500 072, India
Revised: 02/2012
This Medication Guide has been approved by the U.S. Food and Drug Administration.
PACKAGE LABEL-PRINCIPAL DISPLAY PANEL - 10 mg/mL (2 g Bottle)
NDC 65862-109-02
Didanosine for Oral Solution, USP
2 g
PHARMACIST: Dispense the Medication
Guide provided separately to each patient.
Rx only
AUROBINDO

PACKAGE LABEL-PRINCIPAL DISPLAY PANEL - 10 mg/mL Carton (2 g Bottle)
NDC 65862-109-02
Didanosine for Oral Solution, USP
2 g
PHARMACIST: Dispense the Medication Guide
provided separately to each patient.
Rx only
AUROBINDO

| DIDANOSINE
didanosine powder, for solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| DIDANOSINE
didanosine powder, for solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Aurobindo Pharma Limited (650082092) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Aurobindo Pharma Limited | 918917642 | ANALYSIS(65862-109, 65862-110), MANUFACTURE(65862-109, 65862-110) | |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| Aurobindo Pharma Limited | 918917662 | API MANUFACTURE(65862-109, 65862-110) | |