PHENYLEPHRINE HYDROCHLORIDE- phenylephrine hydrochloride solution
Sandoz Inc
Disclaimer: This drug has not been found by FDA to be safe and effective, and this labeling has not been approved by FDA. For further information about unapproved drugs, click here.
----------
Phenylephrine Hydrochloride Ophthalmic Solution, 2.5%
Vasoconstrictor and Mydriatic
For Use in Ophthalmology
WARNING:
PHYSICIANS SHOULD COMPLETELY FAMILIARIZE THEMSELVES WITH THE COMPLETE CONTENTS OF THIS LEAFLET BEFORE PRESCRIBING PHENYLEPHRINE HYDROCHLORIDE.
DESCRIPTION
Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% is a sterile topical ophthalmic solution. The active ingredient is represented by the chemical structure:
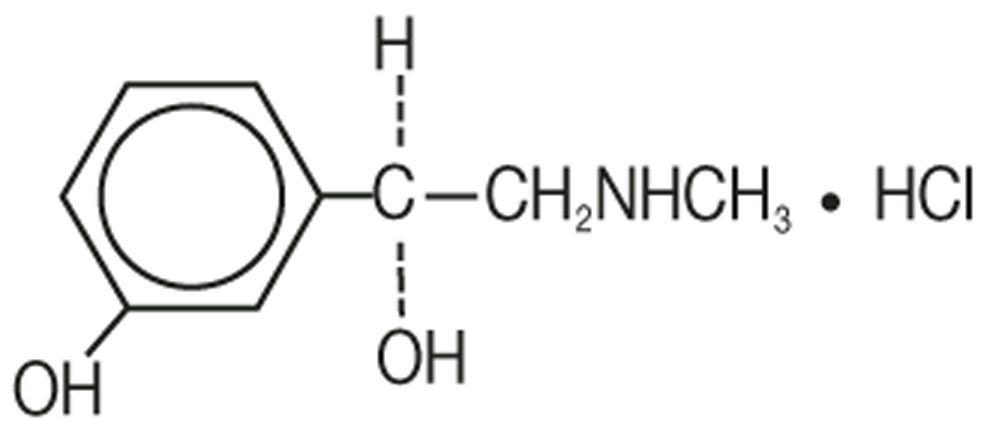
Chemical name: Benzenemethanol,3-hydroxy-α-[(methylamino)methyl]-,hydrochloride (R)-.
Established name: Phenylephrine Hydrochloride
Each mL contains: Active: Phenylephrine HCl 2.5%. Preservative: Benzalkonium Chloride 0.01%. Inactive: Boric Acid, Sodium Bisulfite, Edetate Disodium, Sodium Hydroxide and/or Hydrochloric Acid (to adjust pH), Purified Water.
CLINICAL PHARMACOLOGY
Phenylephrine HCl is an alpha receptor sympathetic agonist used in local ocular disorders because of its vasoconstrictor and mydriatic action. It exhibits rapid and moderately prolonged action, and it produces little rebound vasodilation. Systemic side effects are uncommon.
INDICATIONS & USAGE
Phenylephrine HCl is recommended as a vasoconstrictor, decongestant, and mydriatic in a variety of ophthalmic conditions and procedures. Some of its uses are for pupillary dilation in uveitis (to prevent or aid in the disruption of posterior synechiae formation), for many ophthalmic surgical procedures and for refraction without cycloplegia. Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may also be used for funduscopy and other diagnostic procedures.
CONTRAINDICATIONS
Ophthalmic solutions of phenylephrine HCl are contraindicated in patients with anatomically narrow angles or narrow angle glaucoma. Phenylephrine HCl may be contraindicated in low birth weight infants and in some elderly adults with severe arteriosclerotic cardiovascular or cerebrovascular disease. Phenylephrine HCl may be contraindicated during intraocular operative procedures when the corneal epithelial barrier has been disturbed. This preparation is also contraindicated in persons with a known sensitivity to phenylephrine HCl or any of its components.
WARNINGS
Not for intraocular use. As with other adrenergic drugs, when Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% is administered simultaneously with, or up to 21 days after, administration of monoamine oxidase (MAO) inhibitors, careful supervision and adjustment of dosages are required since exaggerated adrenergic effects may result. The pressor response of adrenergic agents may also be potentiated by tricyclic antidepressants. Systemic side effects are more common in patients taking beta adrenergic blocking agents such as propanolol. Concomitant use of phenylephrine and atropine may enhance the pressor effects and induce tachycardia in some patients, especially infants.1 Contains sodium bisulfite, a sulfite that may cause allergic-type reactions including anaphylactic symptoms and life-threatening or less severe asthmatic episodes in certain susceptible people. The overall prevalence of sulfite sensitivity in the general population is unknown and probably low. Sulfite sensitivity is seen more frequently in asthmatic than in nonasthmatic people.
PRECAUTIONS
Ordinarily, any mydriatic, including phenylephrine HCl, is contraindicated in patients with glaucoma, since it may occasionally raise intraocular pressure. However, when temporary dilation of the pupil may free adhesions, this advantage may temporarily outweigh the danger from coincident dilation of the pupil. Rebound miosis has been reported in older persons one day after receiving phenylephrine HCl ophthalmic solutions, and reinstillation of the drug may produce less mydriasis than previously. This may be of clinical importance in dilating the pupils of older subjects prior to retinal detachment or cataract surgery. The lacrimal sac should be compressed by digital pressure for two to three minutes after instillation to avoid excessive systemic absorption. Due to a strong action of the drug on the dilator muscle, older individuals may also develop transient pigment floaters in the aqueous humor 40 to 45 minutes following the administration of phenylephrine HCl ophthalmic solution. The appearance may be similar to anterior uveitis or to a microscopic hyphema. To prevent pain, a drop of suitable topical anesthetic may be applied before using Phenylephrine Hydrochloride Ophthalmic Solution, 2.5%. Prolonged exposure to air or strong light may cause oxidation and discoloration. Do not use if solution is brown or contains a precipitate. Monitor blood pressure in geriatric patients with known cardiac disease. Use caution in infants with known cardiac anomalies. Exceeding recommended dosages or applying Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% to the instrumented, traumatized, diseased or postsurgical eye or adnexa, or to patients with suppressed lacrimation, as during anesthesia, may result in the absorption of sufficient quantities of phenylephrine to produce a systemic vasopressor response.
Information For Patients
Do not touch dropper tip to any surface, as this may contaminate the solution.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies with phenylephrine HCl have been completed in mice at doses up to 2500 ppm in feed and in rats at doses up to 1250 ppm in feed. Phenylephrine HCl demonstrated no carcinogenic effect in male or female mice and rats.
Pregnancy
Pregnancy Category C. Animal reproduction studies have not been conducted with phenylephrine HCl. It is also not known whether phenylephrine HCl can cause fetal harm when administered to a pregnant woman or can affect reproduction capacity. Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% should be given to a pregnant woman only if clearly needed.
ADVERSE REACTIONS
A marked increase in blood pressure has been reported in low-weight premature neonates, infants, and adult patients with idiopathic orthostatic hypotension. Cardiovascular reactions which have occurred primarily in elderly patients include marked increase in blood pressure, syncope, myocardial infarction, tachycardia, arrhythmia, and fatal subarachnoid hemorrhage.2
DOSAGE & ADMINISTRATION
Vasoconstriction and Pupil Dilation: Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% is especially useful when rapid and powerful dilation of the pupil without cycloplegia and reduction of congestion in the capillary bed are desired. A drop of a suitable topical anesthetic may be applied, followed in a few minutes by 1 drop of Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% on the upper limbus. The anesthetic prevents stinging and consequent dilution of the solution by lacrimination. It may occasionally be necessary to repeat the instillation after one hour, again preceded by the use of the topical anesthetic.
Uveitis: Posterior Synechiae: Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may be used in patients with uveitis when synechiae are present or may develop. The formation of synechiae may be prevented by the use of this solution and atropine or other cycloplegics to produce wide dilation of the pupil. For recently formed posterior synechiae one drop of Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may be applied to the upper surface of the cornea and be repeated as necessary, not to exceed three times. Treatment may be continued the following day, if necessary. Atropine sulfate and the application of hot compresses should also be used if indicated.
Glaucoma: Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may be used with miotics in patients with open angle glaucoma. It reduces the difficulties experienced by the patient because of the small field produced by miosis, and still it permits and often supports the effect of the miotic in lowering the intraocular pressure in open angle glaucoma. Hence, there may be marked improvement in visual acuity after using Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% in conjunction with miotic drugs.
Surgery: When a short-acting mydriatic is needed for wide dilation of the pupil before intraocular surgery, Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may be applied topically from 30 to 60 minutes before the operation.
Refraction: Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may be used effectively to increase mydriasis with homatropine hydrobromide, cyclopentolate hydrochloride, tropicamide hydrochloride and atropine sulfate.
FOR ADULTS: One drop of the preferred cycloplegic is placed in each eye, followed in 5 minutes by one drop of Phenylephrine Hydrochloride Ophthalmic Solution, 2.5%. Since adequate cycloplegia is achieved at different time intervals after the instillation of the necessary number of drops, different cycloplegics will require different waiting periods to achieve adequate cycloplegia.
FOR CHILDREN: For a “one application method,” Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may be combined with one of the preferred rapid acting cycloplegics to produce adequate cycloplegia.
Ophthalmoscopic Examination: One drop of Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% is placed in each eye. Sufficient mydriasis to permit examination is produced in 15 to 30 minutes. Dilation lasts from one to three hours.
Diagnostic Procedures: Provocative Test for Angle Closure Glaucoma: Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may be used cautiously as a provocative test when interval narrow angle closure glaucoma is suspected. Intraocular tension and gonioscopy are performed prior to and after dilation of the pupil with phenylephrine HCl. A “significant” intraocular pressure (IOP) rise combined with gonioscopic evidence of angle closure indicates an anterior segment anatomy capable of angle closure. A negative test does not rule this out. This pharmacologically induced angle closure glaucoma may not simulate real life conditions and other causes for transient elevations of IOP should be excluded.
Retinoscopy (Shadow Test): When dilation of the pupil without cycloplegic action is desired for retinoscopy, Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% may be used.
NOTE: Heavily pigmented irides may require larger doses in all of the above procedures.
Blanching Test: One or two drops of Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% should be applied to the injected eye. After five minutes, examine for perilimbal blanching. If blanching occurs, the congestion is superficial and probably does not indicate iridocyclitis.
HOW SUPPLIED
Phenylephrine Hydrochloride Ophthalmic Solution, 2.5% in plastic DROP-TAINER* dispensers:
3mL NDC 61314-342-01
5mL NDC 61314-342-02
REFERENCES
1. Fraunfelder, F.T., and Meyer, S.M.: Possible Cardiovascular Effects Secondary to Topical Ophthalmic 2.5% Phenylephrine, Am. J. Ophthalmol, 99:3:362, 1985.
2. Ibid.
Rx Only
*DROP-TAINER is a registered trademark of Alcon Manufacturing, Ltd.
345309-0804
Dist. by:
FALCON Pharmaceuticals, Ltd
Ft. Worth, TX 76134
Mfd. by:
ALCON LABORATORIES, INC.
Fort Worth, TX 76134 USA
Printed in USA
| PHENYLEPHRINE HYDROCHLORIDE
phenylephrine hydrochloride solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Sandoz Inc (005387188) |

