PENICILLIN G PROCAINE
-
penicillin g procaine injection
Monarch Pharmaceuticals,Inc.
----------
Prior to administration of the drug, carefully read the WARNINGS, ADVERSE REACTIONS, and DOSAGE and ADMINISTRATION sections of the labeling.
DESCRIPTION
This product is designed to provide a stable aqueous suspension of penicillin G procaine, ready for immediate use. This eliminates the necessity for addition of any diluent, required for the usual dry formulation of injectable penicillin.
Penicillin G procaine is chemically designated as (2S, 5R, 6R)-3,3-Dimethyl-7-oxo-6-(2-phenylacetamido)-4-thia-1-azabicyclo[3.2.0]heptane-2-carboxylic acid compound with 2-(diethylamino)ethyl p-aminobenzoate (1:1) monohydrate.
Its molecular formula is C16H18N2O4S•C13H20N2O2•H2O with a molecular weight of 588.72. Its structural formula is as follows:
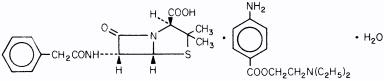
Each TUBEX®; Sterile Cartridge-Needle Unit, 1,200,000 units (2 mL size) or 600,000 units (1 mL size), contains penicillin G procaine in a stabilized aqueous suspension with sodium citrate buffer; and as w/v, approximately 0.5% lecithin, 0.5% carboxymethylcellulose, 0.5% povidone, 0.1% methylparaben, and 0.01% propylparaben.
Penicillin G Procaine Injectable Suspension in the TUBEX formulation is viscous and opaque. Read CONTRAINDICATIONS, WARNINGS, PRECAUTIONS, and DOSAGE AND ADMINISTRATION sections prior to use.
CLINICAL PHARMACOLOGY
Penicillin G procaine is an equimolecular compound of procaine and penicillin G, administered intramuscularly as a suspension. It dissolves slowly at the site of injection, giving a plateau type of blood level at about 4 hours which falls slowly over a period of the next 15 to 20 hours.
Approximately 60% of penicillin G is bound to serum protein. The drug is distributed throughout the body tissues in widely varying amounts. Highest levels are found in the kidneys with lesser amounts in the liver, skin, and intestines. Penicillin G penetrates into all other tissues to a lesser degree with a very small level found in the cerebrospinal fluid. With normal kidney function, the drug is excreted rapidly by tubular excretion. In neonates and young infants and in individuals with impaired kidney functions, excretion is considerably delayed. Approximately 60 to 90 percent of a dose of parenteral penicillin G is excreted in the urine within 24 to 36 hours.
Microbiology: Penicillin G exerts a bactericidal action against penicillin-susceptible microorganisms during the stage of active multiplication. It acts through the inhibition of biosynthesis of cell-wall mucopeptide. It is not active against the penicillinase-producing bacteria, which include many strains of staphylococci. While in vitro studies have demonstrated the susceptibility of most strains of the following organisms, clinical efficacy for infections other than those included in the INDICATIONS AND USAGE section has not been documented. Penicillin G exerts high in vitro activity against staphylococci (except penicillinase-producing strains), streptococci (Groups A, C, G, H, L, and M), and pneumococci. Other organisms susceptible to penicillin G are Corynebacterium diphtheriae, Bacillus anthracis, Clostridium species, Actinomyces bovis, Streptobacillus moniliformis, Listeria monocytogenes , and Leptospira species. Treponema pallidum is extremely susceptible to the bactericidal action of penicillin G.
Susceptibility Testing
Ten unit Penicillin G Susceptibility Discs may be used to determine microbial susceptibility to penicillin G using one of the following standard methods recommended by the National Committee for Laboratory Standards:
M2-T4, “Performance Standards for Antimicrobial Disc Susceptibility Tests”
M7-T2, “Methods for Dilution Antimicrobial Susceptibility Tests for Bacteria that Grow Aerobically”
Tests should be interpreted by the following criteria:
| Susceptible | Moderately Susceptible | Resistant | |
| Staphylococci | ≥29 | - | ≤28 |
| Enterococci | - | ≥15 | ≤14 |
| L. monocytogenes | ≥20 | - | ≤19 |
| Non-enterococcal streptococci | ≥28 | 20–27 | ≤19 |
| Susceptible | Resistant | |
| Staphylococci | ≤0.1 μg/mL | β-lactamase |
| Enterococci | - | ≥16 μg/mL |
| L. monocytogenes | ≤2 μg/mL | ≥4 μg/mL |
| Non-enterococcal streptococci | ≤0.12 μg/mL | ≥4 μg/mL |
Interpretations of susceptible, intermediate, and resistant correlate zone size diameters with MIC values. A laboratory report of “susceptible” indicates that the suspected causative microorganism most likely will respond to therapy with penicillin G. A laboratory report of “resistant” indicates that the infecting microorganism most likely will not respond to therapy. A laboratory report of “moderately susceptible” indicates that the microorganism is most likely susceptible if a high dosage of penicillin G is used, or if the infection is such that high levels of penicillin G may be attained as in urine. A report of “intermediate” using the disc diffusion method may be considered an equivocal result, and dilution tests may be indicated.
Control organisms are recommended for susceptibility testing. Each time the test is performed the following organism should be included. The range for zones of inhibition is shown below:
| Control Organism | Zone of Inhibition Range |
| Staphylococcus aureus | 26–37 |
| (ATCC 25923) |
INDICATIONS AND USAGE
Penicillin G procaine is indicated in the treatment of moderately severe infections in both adults and pediatric patients due to penicillin-G-susceptible microorganisms that are susceptible to the low and persistent serum levels common to this particular dosage form in the indications listed below. Therapy should be guided by bacteriological studies (including susceptibility tests) and by clinical response.
NOTE: When high, sustained serum levels are required, aqueous penicillin G, either IM or IV, should be used.
The following infections will usually respond to adequate dosages of intramuscular penicillin G procaine: Moderately severe to severe infections of the upper respiratory tract, skin and soft-tissue infections, scarlet fever, and erysipelas due to susceptible streptococci (Group A-without bacteremia).
NOTE: Streptococci in Groups A, C, G, H, L, and M are very sensitive to penicillin G. Other groups, including Group D (enterococcus), are resistant. Aqueous penicillin is recommended for streptococcal infections with bacteremia.
Moderately severe infections of the respiratory tract due to susceptible pneumococci.
NOTE: Severe pneumonia, empyema, bacteremia, pericarditis, meningitis, peritonitis, and arthritis of pneumococcal etiology are better treated with aqueous penicillin G during the acute stage.
Moderately severe infections of the skin and soft tissues due to susceptible staphylococci (penicillin G-susceptible).
NOTE: Reports indicate an increasing number of strains of staphylococci resistant to penicillin G, emphasizing the need for culture and sensitivity studies in treating suspected staphylococcal infections. Indicated surgical procedures should be performed.
Fusospirochetosis (Vincent's gingivitis and pharyngitis). Moderately severe infections of the oropharynx due to susceptible fusiform bacilli and spirochetes.
NOTE: Necessary dental care should be accomplished in infections involving the gum tissue.
Syphilis (all stages) due to susceptible Treponema pallidum.
NOTE: This drug should not be used in the treatment of beta-lactamase producing organisms which include most strains of Neisseria gonorrhea.
Yaws, Bejel, Pinta due to susceptible organisms.
Penicillin G procaine is an adjunct to antitoxin for prevention of the carrier stage of diphtheria due to susceptible C. diphtheriae.
Anthrax due to Bacillus anthracis, including inhalational anthrax (post-exposure): to reduce the incidence or progression of the disease following exposure to aerosolized Bacillus anthracis.
Rat-bite fever due to susceptible Streptobacillus moniliformis and Spirillum minus organisms.
Erysipeloid due to susceptible Erysipelothrix rhusiopathiae.
Subacute bacterial endocarditis, only in extremely sensitive infections, due to susceptible Group A streptococci.
WARNINGS
Penicillin G procaine should only be prescribed for the indications listed in this insert.
NOTE: This drug is no longer indicated in the treatment of gonorrhea.
Anaphylaxis
SERIOUS AND OCCASIONALLY FATAL HYPERSENSITIVITY (ANAPHYLACTIC) REACTIONS HAVE BEEN REPORTED IN PATIENTS ON PENICILLIN THERAPY. THESE REACTIONS ARE MORE LIKELY TO OCCUR IN INDIVIDUALS WITH A HISTORY OF PENICILLIN HYPERSENSITIVITY AND/OR A HISTORY OF SENSITIVITY TO MULTIPLE ALLERGENS. THERE HAVE BEEN REPORTS OF INDIVIDUALS WITH A HISTORY OF PENICILLIN HYPERSENSITIVITY WHO HAVE EXPERIENCED SEVERE REACTIONS WHEN TREATED WITH CEPHALOSPORINS. BEFORE INITIATING THERAPY WITH ANY PENICILLIN, CAREFUL INQUIRY SHOULD BE MADE CONCERNING PREVIOUS HYPERSENSITIVITY REACTIONS TO PENICILLINS, CEPHALOSPORINS, OR OTHER ALLERGENS. IF AN ALLERGIC REACTION OCCURS, THE DRUG SHOULD BE DISCONTINUED AND APPROPRIATE THERAPY INSTITUTED. SERIOUS ANAPHYLACTIC REACTIONS REQUIRE IMMEDIATE EMERGENCY TREATMENT WITH EPINEPHRINE. OXYGEN, INTRAVENOUS STEROIDS, AND AIRWAY MANAGEMENT, INCLUDING INTUBATION, SHOULD ALSO BE ADMINISTERED AS INDICATED.
Pseudomembranous Colitis
Pseudomembranous colitis has been reported with nearly all antibacterial agents, including penicillin G, and may range in severity from mild to life-threatening. Therefore, it is important to consider this diagnosis in patients who present with diarrhea subsequent to the administration of antibacterial agents.
Treatment with antibacterial agents alters the normal flora of the colon and may permit overgrowth of clostridium. Studies indicate that a toxin produced by Clostridium difficile is one primary cause of “antibiotic-associated colitis.”
After the diagnosis of pseudomembranous colitis has been established, therapeutic measures should be initiated. Mild cases of pseudomembranous colitis usually respond to drug discontinuation alone. In moderate to severe cases, consideration should be given to management of fluids and electrolytes, protein supplementation and treatment with an antibacterial drug clinically effective against C. difficile colitis.
Procaine Reactions
Immediate toxic reactions to procaine may occur in some individuals, particularly when a large single dose is administered (4.8 million units). These reactions may be manifested by mental disturbances, including anxiety, confusion, agitation, depression, weakness, seizures, hallucinations, combativeness, and expressed “fear of impending death.” The reactions noted in carefully controlled studies occurred in approximately one in 500 patients who received large doses of penicillin G procaine. Reactions are transient, lasting from 15 to 30 minutes.
Method of Administration
Do not inject into or near an artery or nerve.
Injection into or near a nerve may result in permanent neurological damage.
Inadvertent intravascular administration, including inadvertent direct intra-arterial injection or injection immediately adjacent to arteries, of Penicillin G Procaine Injectable Suspension and other penicillin preparations has resulted in severe neurovascular damage, including transverse myelitis with permanent paralysis, gangrene requiring amputation of digits and more proximal portions of extremities, and necrosis and sloughing at and surrounding the injection site. Such severe effects have been reported following injections into the buttock, thigh, and deltoid areas. Other serious complications of suspected intravascular administration which have been reported include immediate pallor, mottling, or cyanosis of the extremity, both distal and proximal to the injection site, followed by bleb formation; severe edema requiring anterior and/or posterior compartment fasciotomy in the lower extremity. The above-described severe effects and complications have most often occurred in infants and small children. Prompt consultation with an appropriate specialist is indicated if any evidence of compromise of the blood supply occurs at, proximal to, or distal to the site of injection.1-9 (See PRECAUTIONS, and DOSAGE AND ADMINISTRATION.)
Quadriceps femoris fibrosis and atrophy have been reported following repeated intramuscular injections of penicillin preparations into the anterolateral thigh.
PRECAUTIONS
General
Penicillin should be used with caution in individuals with histories of significant allergies and/or asthma.
Care should be taken to avoid intravenous or intra-arterial administration, or injection into or near major peripheral nerves or blood vessels, since such injections may produce neurovascular damage. (See WARNINGS, and DOSAGE AND ADMINISTRATION.)
A small percentage of patients are sensitive to procaine. If there is a history of sensitivity, make the usual test: Inject intradermally 0.1 mL of a 1 to 2 percent procaine solution. Development of an erythema, wheal, flare, or eruption indicates procaine sensitivity. Sensitivity should be treated by the usual methods, including barbiturates, and procaine penicillin preparations should not be used. Antihistaminics appear beneficial in treatment of procaine reactions.
The use of antibiotics may result in overgrowth of nonsusceptible organisms. Constant observation of the patient is essential. If new infections due to bacteria or fungi appear during therapy, the drug should be discontinued and appropriate measures taken.
Whenever allergic reactions occur, penicillin should be withdrawn unless, in the opinion of the physician, the condition being treated is life-threatening and amenable only to penicillin therapy.
Laboratory Tests
In suspected staphylococcal infections, proper laboratory studies, including susceptibility tests, should be performed.
In prolonged therapy with penicillin, and particularly with high-dosage schedules, periodic evaluation of the renal and hematopoietic systems is recommended. In such situations, use of penicillin for more than 2 weeks may be associated with an increased risk of neutropenia and an increased incidence of serum sickness-like reactions.
When treating gonococcal infections in which primary or secondary syphilis may be suspected, proper diagnostic procedures, including dark-field examinations, should be done. In all cases in which concomitant syphilis is suspected, monthly serological tests should be made for at least four months.
Drug Interactions
Tetracycline, a bacteriostatic antibiotic, may antagonize the bactericidal effect of penicillin and concurrent use of these drugs should be avoided.
Concurrent administration of penicillin and probenecid increases and prolongs serum penicillin levels by decreasing the apparent volume of distribution and slowing the rate of excretion by competitively inhibiting renal tubular secretion of penicillin.
Carcinogenesis, Mutagenesis, Impairment of Fertility
No long-term animal studies have been conducted with these drugs.
Pregnancy
Teratogenic effects—Pregnancy Category B: Reproduction studies performed in the mouse, rat, and rabbit have revealed no evidence of impaired fertility or harm to the fetus due to penicillin G. Human experience with the penicillins during pregnancy has not shown any positive evidence of adverse effects on the fetus. There are, however, no adequate and well-controlled studies in pregnant women showing conclusively that harmful effects of these drugs on the fetus can be excluded. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
Nursing Mothers
Penicillins are excreted in human milk. Caution should be exercised when penicillins are administered to a nursing woman.
Pediatric Use
Because of incompletely developed renal function in newborns, penicillin elimination may be delayed. Guidelines for administration of this drug to pediatric patients are presented in DOSAGE AND ADMINISTRATION.
ADVERSE REACTIONS
Allergic Reactions
Penicillin is a substance of low toxicity but does possess a significant index of sensitization. The following hypersensitivity reactions associated with use of penicillin have been reported: Skin rashes, ranging from maculopapular eruptions to exfoliative dermatitis; urticaria; serum-sicknesslike reactions, including chills, fever, edema, arthralgia, and prostration. Severe and often fatal anaphylaxis has been reported (see WARNINGS). As with other treatments for syphilis, the Jarisch-Herxheimer reaction has been reported.
Procaine toxicity manifestations and hypersensitivity reactions have been reported (see WARNINGS and PRECAUTIONS).
Gastrointestinal
Pseudomembranous colitis has been reported with the use of penicillin G. Onset of pseudomembranous colitis symptoms may occur during or after antibiotic treatment (see WARNINGS).
DOSAGE AND ADMINISTRATION
Do not inject into or near an artery or nerve. Injection into or near a nerve may result in permanent neurologic damage (see WARNINGS).
Penicillin G procaine (aqueous) is for intramuscular injection only.
Administer by DEEP INTRAMUSCULAR INJECTION in the upper, outer quadrant of the buttock. In neonates, infants and small children, the midlateral aspect of the thigh may be preferable. When doses are repeated, vary the injection site.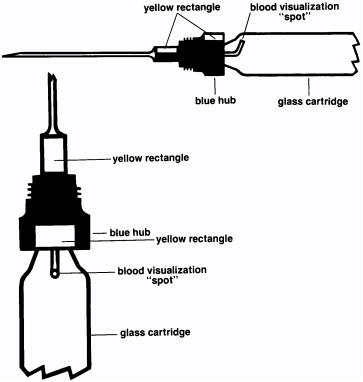
The TUBEX® cartridge for this product incorporates several features that are designed to facilitate the visualization of blood on aspiration if a blood vessel is inadvertently entered.
The design of this cartridge is such that blood which enters its needle will be quickly visualized as a red or dark-colored “spot.” This “spot” will appear on the barrel of the glass cartridge immediately proximal to the blue hub. The TUBEX is designed with two orientation marks, in order to determine where this “spot” can be seen. First insert and secure the cartridge in the TUBEX injector in the usual fashion. Locate the yellow rectangle at the base of the blue hub. This yellow rectangle is aligned with the blood visualization “spot.” An imaginary straight line, drawn from this yellow rectangle to the shoulder of the glass cartridge, will point to the area on the cartridge where the “spot” can be visualized. When the needle cover is removed, a second yellow rectangle will be visible. The second yellow rectangle is also aligned with the blood visualization “spot” to assist the operator in locating this “spot.” If the 2 mL metal or plastic syringe is used, the glass cartridge should be rotated by turning the plunger of the syringe clockwise until the yellow rectangle is visualized. If the 1 mL metal syringe is used, it will not be possible to continue to rotate the glass cartridge clockwise once it is properly engaged and fully threaded; it can, however, then be rotated counterclockwise as far as necessary to properly orient the yellow rectangles and locate the observation area. (In this same area in some cartridges, a dark spot may sometimes be visualized prior to injection. This is the proximal end of the needle and does not represent a foreign body in, or other abnormality of, the suspension.)
Thus, before the needle is inserted into the selected muscle, it is important for the operator to orient the yellow rectangles so that any blood which may enter after needle insertion and during aspiration can be visualized in the area on the cartridge where it will appear and not be obscured by any obstructions.
After selection of the proper site and insertion of the needle into the selected muscle, aspirate by pulling back on the plunger. While maintaining negative pressure for 2 to 3 seconds, carefully observe the barrel of the cartridge in the area previously identified (see above) for the appearance of a red or dark-colored “spot.”
Blood or “typical blood color” may not be seen if a blood vessel has been entered-only a mixture of blood and Penicillin G Procaine Injectable Suspension. The appearance of any discoloration is reason to withdraw the needle and discard the glass TUBEX cartridge. If it is elected to inject at another site, a new cartridge should be used. If no blood or discoloration appears, inject the contents of the cartridge slowly. Discontinue delivery of the dose if the subject complains of severe immediate pain at the injection site or if, especially in neonates, infants and young children, symptoms or signs occur suggesting onset of severe pain.
Some TUBEX cartridges may contain a small air bubble which should be disregarded, since it does not affect administration of the product. DO NOT clear any air bubbles from the cartridge or needle as this may interfere with the visualization of any blood or discoloration during aspiration.
Because of the high concentration of suspended material in this product, the needle may be blocked if the injection is not made at a slow, steady rate.
Pneumonia (pneumococcal), moderately severe (uncomplicated): 600,000 to 1,000,000 units daily.
Streptococcal infections (Group A), moderately severe to severe tonsillitis, erysipelas, scarlet fever, upper respiratory tract, skin and soft tissue: 600,000 to 1,000,000 units daily for 10-day minimum.
Staphylococcal infections, moderately severe to severe: 600,000 to 1,000,000 units daily.
In pneumonia, streptococcal (Group A) and staphylococcal infections in pediatric patients under 60 pounds: 300,000 units daily.
Bacterial endocarditis (Group A streptococci) only in extremely sensitive infections: 600,000 to 1,000,000 units daily.
Penicillin G procaine is not recommended for prophylaxis against bacterial endocarditis. For prophylaxis against bacterial endocarditis in patients with congenital heart disease or rheumatic or other acquired valvular heart disease when undergoing dental procedures or surgical procedures of the upper respiratory tract, use penicillin V. For patients unable to take oral medications, aqueous penicillin G is recommended.
Syphilis
Primary, secondary, and latent with a negative spinal fluid in adults and pediatric patients over 12 years of age: 600,000 units daily for 8 days-total 4,800,000 units.
Late (tertiary, neurosyphilis, and latent syphilis with positive spinal-fluid examination or no spinal-fluid examination): 600,000 units daily for 10 to 15 days-total 6 to 9 million units.
Congenital syphilis under 70-lb. body weight: 50,000 units/kg/day for 10 days.
Yaws, Bejel, and Pinta: Treatment as for syphilis in corresponding stage of disease.
Diphtheria-adjunctive therapy with antitoxin: 300,000 to 600,000 units daily.
Diphtheria carrier state: 300,000 units daily for 10 days.
Anthrax-cutaneous: 600,000 to 1,000,000 units/day.
Anthrax-inhalational (post-exposure): 1,200,000 units every 12 hours in adults, 25,000 units per kilogram of body weight (maximum 1,200,000 unit) every 12 hours in children. The available safety data for penicillin G procaine at this dose would best support a duration of therapy of 2 weeks or less. Treatment for inhalational anthrax (post-exposure) must be continued for a total of 60 days. Physicians must consider the risks and benefits of continuing administration of penicillin G procaine for more than 2 weeks or switching to an effective alternative treatment.
Vincent's infection (fusospirochetosis): 600,000 to 1,000,000 units/day.
Erysipeloid: 600,000 to 1,000,000 units/day.
Streptobacillus moniliformis and Spirillum minus (rat-bite fever): 600,000 to 1,000,000 units/day.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
HOW SUPPLIED
Penicillin G Procaine Injectable Suspension is supplied in packages of 10 TUBEX® Sterile Cartridge-Needle Units as follows:
1 mL size, containing 600,000 units per TUBEX® (21 gauge, thin-wall 1-1/4 inch needle), NDC 61570-085-10.
2 mL size, containing 1,200,000 units per TUBEX® (21 gauge, thin-wall 1-1/4 inch needle), NDC 61570-086-10.
Store in a refrigerator, 2° to 8°C (36° to 46°F).
Keep from freezing.
TUBEX® Injector
PLEASE NOTE: THE METAL TUBEX HYPODERMIC SYRINGE AND TUBEX FAST-TRAK SYRINGE HAVE BEEN DISCONTINUED AND REPLACED BY THE TUBEX INJECTOR. EXCHANGE OF THESE DISCONTINUED SYRINGES IS AVAILABLE, FREE OF CHARGE, FROM WYETH-AYERST DIRECTLY. FOR LOADING AND UNLOADING INFORMATION ON THESE DISCONTINUED SYRINGES, CONTACT THE MEDICAL AFFAIRS DEPARTMENT AT WYETH-AYERST LABORATORIES, P.O. BOX 8299, PHILADELPHIA, PA 19101.
NOTE: The TUBEX Injector is reusable: do not discard.
DIRECTIONS FOR USE:
BEFORE PROCEEDING, SEE IMPORTANT INFORMATION UNDERDOSAGE AND ADMINISTRATION SECTION.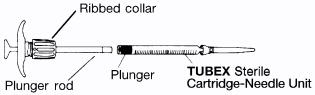
NOTE: USE ASEPTIC TECHNIQUE FOR ALL MANIPULATIONS OF STERILE PARTS.
To load a TUBEX Sterile Cartridge-Needle Unit into the TUBEX Injector
- Turn the ribbed collar to the “OPEN” position until it stops.
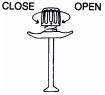
- Hold the Injector with the open end up and fully insert the TUBEX Sterile Cartridge-Needle Unit. Firmly tighten the ribbed collar in the direction of the “CLOSE” arrow.
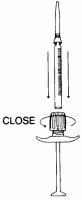
- Thread the plunger rod into the plunger of the TUBEX Sterile Cartridge-Needle Unit until slight resistance is felt.

The Injector is now ready for use in the usual manner.
-
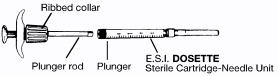
To load an E.S.I. DOSETTE® Sterile Cartridge-Needle Unit into the TUBEX Injector
- Turn the ribbed collar to the “OPEN” position until it stops.
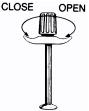
- Hold the Injector with the open end up and fully insert the E.S.I. DOSETTE Sterile Cartridge-Needle Unit. Firmly tighten the ribbed collar in the direction of the “CLOSE” arrow.
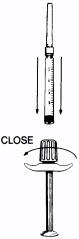
- Thread the plunger rod into the plunger of the E.S.I. DOSETTE Sterile Cartridge-Needle Unit until slight resistance is felt.
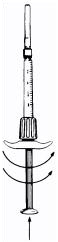
- Engage the needle-cap assembly by pulling the cap down over the silver cartridge hub. The needle is fully engaged when the silver hub is completely covered.

The Injector is now ready for use in the usual manner.
To administer TUBEX/DOSETTE Sterile Cartridge-Needle Units
Method of administration is the same as with conventional syringe. Remove needle cover by grasping it securely; twist and pull. Introduce needle into patient, aspirate by pulling back slightly on the plunger, and inject.
To remove the empty TUBEX/DOSETTE Cartridge-Needle Unit and dispose into a vertical needle disposal container
- Do not recap the needle. Disengage the plunger rod.

- Hold the Injector, needle down, over a vertical needle disposal container and loosen the ribbed collar. TUBEX/DOSETTE Cartridge-Needle Unit will drop into the container.
- Discard the needle cover.
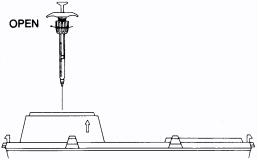
To remove the empty TUBEX/DOSETTE Cartridge-Needle Unit and dispose into a horizontal (mailbox) needle disposal container
- Do not recap the needle. Disengage the plunger rod.
- Open the horizontal (mailbox) needle disposal container. Insert TUBEX/DOSETTE Cartridge-Needle Unit, needle pointing down, halfway into container. Close the container lid on cartridge. Loosen ribbed collar; TUBEX/DOSETTE Cartridge-Needle Unit will drop into the container.
- Discard the needle cover.
The TUBEX Injector is reusable and should not be discarded.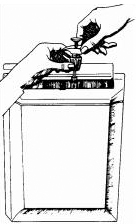
Used TUBEX/ DOSETTE Cartridge-Needle Units should not be employed for successive injections or as multiple-dose containers. They are intended to be used only once and discarded.
NOTE: Any graduated markings on TUBEX/DOSETTE Sterile Cartridge-Needle Units are to be used only as a guide in administering doses.
Wyeth-Ayerst does not recommend and will not accept responsibility for the use of any cartridge-needle units or needle-less units other than TUBEX or E.S.I. DOSETTE Cartridge-Needle Units in the TUBEX Injector.
TUBEX is a registered trademark of Wyeth-Ayerst Laboratories.
REFERENCES
- SHAW, E.: Transverse myelitis from injection of penicillin. Am. J. Dis. Child., 111:548, 1966.
- KNOWLES, J.: Accidental intra-arterial injection of penicillin. Am. J. Dis. Child., 111:552, 1966.
- DARBY, C. et al: Ischemia following an intragluteal injection of benzathine-procaine penicillin G mixture in a one-year-old boy. Clin. Pediatrics,12:485, 1973.
- BROWN, L. & NELSON, A.: Postinfectious intravascular thrombosis with gangrene. Arch. Surg., 94:652, 1967.
- BORENSTINE, J.: Transverse myelitis and penicillin (Correspondence). Am. J. Dis. Child., 112:166, 1966.
- ATKINSON, J.: Transverse myelopathy secondary to penicillin injection. J. Pediatrics, 75:867, 1969.
- TALBERT, J. et al: Gangrene of the foot following intramuscular injection in the lateral thigh: A case report with recommendations for prevention. J. Pediatrics, 70:110, 1967.
- FISHER, T.: Medicolegal affairs. Canad. Med. Assoc. J., 112:395, 1975.
- SCHANZER, H. et al: Accidental intra-arterial injection of penicillin G. JAMA, 242 :1289, 1979.
Prescribing Information as of March 2002.
Distributed by: Monarch Pharmaceuticals, Inc., Bristol, TN 37620
Manufactured by: Wyeth Laboratories, Philadelphia, PA 19101
| PENICILLIN G PROCAINE
penicillin g procaine injection |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| ANDA | ANDA060101 | 04/26/1948 | 09/14/2007 |
| PENICILLIN G PROCAINE
penicillin g procaine injection |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| ANDA | ANDA060101 | 04/26/1948 | 09/14/2007 |
| Labeler - Monarch Pharmaceuticals,Inc. (809587413) |
Revised: 09/2011 Monarch Pharmaceuticals,Inc.

