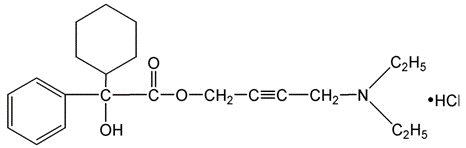OXYBUTYNIN CHLORIDE- oxybutynin chloride tablet, film coated, extended release
Cardinal Health
Reference Label Set Id: 6df70145-9f60-4177-b28f-dd0bc28f2f1f
----------
DESCRIPTION
Oxybutynin chloride is an antispasmodic, anticholinergic agent. Each oxybutynin chloride extended-release tablet, USP contains 5 mg or 10 mg of oxybutynin chloride USP, formulated as a once-a-day controlled-release tablet for oral administration. Oxybutynin chloride is administered as a racemate of R- and S- enantiomers.
Chemically, oxybutynin chloride is d,l (racemic) 4-diethylamino-2-butynyl phenyl-cyclohexylglycolate hydrochloride. The molecular formula of oxybutynin chloride is C22H31NO3 • HCl.
Its structural formula is:
Oxybutynin chloride, USP is a white crystalline solid with a molecular weight of 393.9. It is readily soluble in water and acids, but relatively insoluble in alkalis.
Oxybutynin chloride extended-release tablets contain the following inactive ingredients: colloidal silicon dioxide, dibasic calcium phosphate (anhydrous), hypromellose, magnesium stearate, methacrylic acid copolymer dispersion, polydextrose, polyethylene glycol, polysorbate 80, povidone, sodium hydroxide, talc, titanium dioxide, triacetin and triethyl citrate. The 5 mg strength also contains D&C Yellow No. 10 Aluminum Lake, FD&C Blue No. 1 Aluminum Lake and FD&C Red No. 40 Aluminum Lake; and the 10 mg strength also contains FD&C Yellow No. 6 Aluminum Lake.
In addition, the imprinting ink contains black iron oxide, hypromellose and propylene glycol.
Meets USP Dissolution Test 2.
System Components and Performance
Oxybutynin chloride extended-release tablets are formulated to deliver oxybutynin chloride at a controlled rate over approximately 24 hours. The dosage form is comprised of a hydrophilic cellulose polymer matrix tablet surrounded by an enteric coating system. The enteric coat is insoluble in the low pH environment of the stomach. As the tablet passes through the stomach and enters the higher pH environment of the small intestine, the enteric coating dissolves and/or erodes to expose the polymer matrix tablet which swells and releases drug at a controlled rate via diffusion and/or erosion.
CLINICAL PHARMACOLOGY
Oxybutynin chloride exerts a direct antispasmodic effect on smooth muscle and inhibits the muscarinic action of acetylcholine on smooth muscle. Oxybutynin chloride exhibits only one-fifth of the anticholinergic activity of atropine on the rabbit detrusor muscle, but 4 to 10 times the antispasmodic activity. No blocking effects occur at skeletal neuromuscular junctions or autonomic ganglia (antinicotinic effects).
Oxybutynin chloride relaxes bladder smooth muscle. In patients with conditions characterized by involuntary bladder contractions, cystometric studies have demonstrated that oxybutynin increases bladder (vesical) capacity, diminishes the frequency of uninhibited contractions of the detrusor muscle, and delays the initial desire to void. Oxybutynin thus decreases urgency and the frequency of both incontinent episodes and voluntary urination.
Antimuscarinic activity resides predominantly in the R-isomer. A metabolite, desethyloxybutynin, has pharmacological activity similar to that of oxybutynin in in vitro studies.
Pharmacokinetics
Absorption
Following the first dose of oxybutynin chloride extended-release tablets, oxybutynin plasma concentrations rise for 4 to 6 hours; thereafter steady concentrations are maintained for up to 24 hours, minimizing fluctuations between peak and trough concentrations associated with oxybutynin.
The relative bioavailabilities of R- and S-oxybutynin from oxybutynin chloride extended-release are 156% and 187%, respectively, compared with oxybutynin. The mean pharmacokinetic parameters for R- and S-oxybutynin are summarized in Table 1. The plasma concentration-time profiles for R- and S-oxybutynin are similar in shape; Figure 1 shows the profile for R-oxybutynin.
|
Parameters (units) |
R-Oxybutynin |
S-Oxybutynin |
||
|
Cmax (ng/mL) |
1 |
(0.6) |
1.8 |
(1) |
|
Tmax (h) |
12.7 |
(5.4) |
11.8 |
(5.3) |
|
t½ (h) |
13.2 |
(6.2) |
12.4 |
(6.1) |
|
AUC(0-48) (ng•h/mL) |
18.4 |
(10.3) |
34.2 |
(16.9) |
|
AUCinf (ng•h/mL) |
21.3 |
(12.2) |
39.5 |
(21.2) |
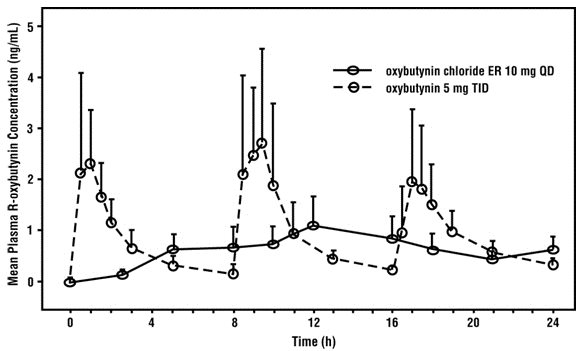
Figure 1. Mean R-oxybutynin plasma concentrations following a single dose of oxybutynin chloride ER 10 mg and oxybutynin 5 mg administered every 8 hours (n = 23 for each treatment).
Figure 1. Mean R-oxybutynin plasma concentrations following a single dose of oxybutynin chloride ER 10 mg and oxybutynin 5 mg administered every 8 hours (n = 23 for each treatment).
Steady-state oxybutynin plasma concentrations are achieved by Day 3 of repeated oxybutynin chloride extended-release dosing, with no observed drug accumulation or change in oxybutynin and desethyloxybutynin pharmacokinetic parameters.
Oxybutynin chloride extended-release steady-state pharmacokinetics were studied in 19 children aged 5 to 15 years with detrusor overactivity associated with a neurological condition (e.g. spina bifida). The children were on oxybutynin chloride extended-release total daily dose ranging from 5 mg to 20 mg (0.10 to 0.77 mg/kg). Sparse sampling technique was used to obtain serum samples. When all available data are normalized to an equivalent of 5 mg per day oxybutynin chloride extended-release, the mean pharmacokinetic parameters derived for R- and S-oxybutynin and R- and S-desethyloxybutynin are summarized in Table 2. The plasma-time concentration profiles for R- and S-oxybutynin are similar in shape; Figure 2 shows the profile for R-oxybutynin when all available data are normalized to an equivalent of 5 mg per day.
|
R-Oxybutynin |
S-Oxybutynin |
R-Desethyloxybutynin |
S-Desethyloxybutynin |
|
|
Cmax (ng/mL) |
0.7 ± 0.4 |
1.3 ± 0.8 |
7.8 ± 3.7 |
4.2 ± 2.3 |
|
Tmax (hr) |
5 |
5 |
5 |
5 |
|
AUC (ng•hr/mL) |
12.8 ± 7 |
23.7 ± 14.4 |
125.1 ± 66.7 |
73.6 ± 47.7 |
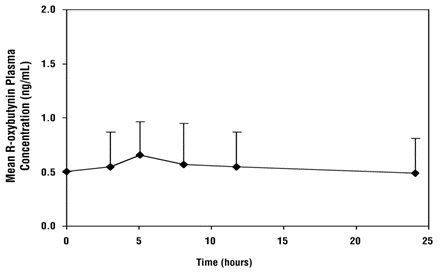
Figure 2. Mean steady-state (±SD) R-oxybutynin plasma concentrations following administration of 5 mg to 20 mg oxybutynin chloride extended-release tablets once daily in children aged 5 to 15. Plot represents all available data normalized to an equivalent of oxybutynin chloride extended-release tablets 5 mg once daily.
Figure 2. Mean steady-state (±SD) R-oxybutynin plasma concentrations following administration of 5 mg to 20 mg oxybutynin chloride extended-release tablets once daily in children aged 5 to 15. Plot represents all available data normalized to an equivalent of oxybutynin chloride extended-release tablets 5 mg once daily.
Distribution
Oxybutynin is widely distributed in body tissues following systemic absorption.The volume of distribution is 193 L after intravenous administration of 5 mg oxybutynin chloride. Both enantiomers of oxybutynin are highly bound (> 99%) to plasma proteins. Both enantiomers of N-desethyloxybutynin are also highly bound (> 97%) to plasma proteins. The major binding protein is alpha-1 acid glycoprotein.
Metabolism
Oxybutynin is metabolized primarily by the cytochrome P450 enzyme systems, particularly CYP3A4 found mostly in the liver and gut wall. Its metabolic products include phenylcyclohexylglycolic acid, which is pharmacologically inactive, and desethyloxybutynin, which is pharmacologically active. Following oxybutynin chloride extended-release administration, plasma concentrations of R- and S-desethyloxybutynin are 73% and 92%, respectively, of concentrations observed with oxybutynin.
Excretion
Oxybutynin is extensively metabolized by the liver, with less than 0.1% of the administered dose excreted unchanged in the urine. Also, less than 0.1% of the administered dose is excreted as the metabolite desethyloxybutynin.
Dose Proportionality
Pharmacokinetic parameters of oxybutynin and desethyloxybutynin (Cmax and AUC) following administration of 5 mg to 20 mg of oxybutynin chloride extended-release tablets are dose proportional.
Special Populations
Geriatric
The pharmacokinetics of oxybutynin chloride extended-release were similar in all patients studied (up to 78 years of age).
Pediatric
The pharmacokinetics of oxybutynin chloride extended-release were evaluated in 19 children aged 5 to 15 years with detrusor overactivity associated with a neurological condition (e.g., spina bifida). The pharmacokinetics of oxybutynin chloride extended-release in these pediatric patients were consistent with those reported for adults (see Tables 1 and 2, and Figures 1 and 2 above).
Gender
There are no significant differences in the pharmacokinetics of oxybutynin in healthy male and female volunteers following administration of oxybutynin chloride extended-release.
Race
Available data suggest that there are no significant differences in the pharmacokinetics of oxybutynin based on race in healthy volunteers following administration of oxybutynin chloride extended-release.
CLINICAL STUDIES
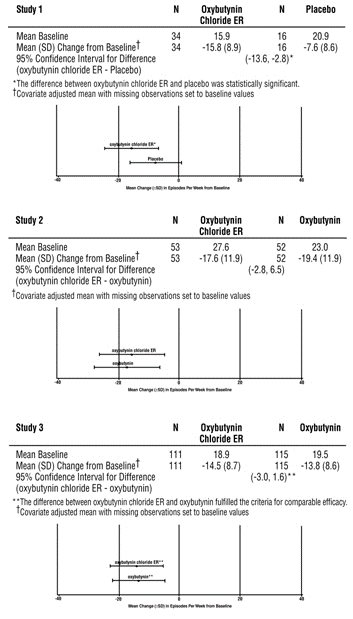
Oxybutynin chloride extended-release was evaluated for the treatment of patients with overactive bladder with symptoms of urge urinary incontinence, urgency, and frequency in three controlled studies and one open-label study. The majority of patients were Caucasian (89%) and female (91.9%) with a mean age of 59 years (range, 18 to 98 years). Entry criteria required that patients have urge or mixed incontinence (with a predominance of urge) as evidenced by ≥ 6 urge incontinence episodes per week and ≥ 10 micturitions per day. Study 1 was a fixed dose escalation design, whereas the other studies used a dose adjustment design in which each patient’s final dose was adjusted to a balance between improvement of incontinence symptoms and tolerability of side effects. Controlled studies included patients known to be responsive to oxybutynin or other anticholinergic medications, and these patients were maintained on a final dose for up to 2 weeks.
The efficacy results for the three controlled trials are presented in the following tables and figures.
Number of Urge Urinary Incontinence Episodes per Week
INDICATIONS AND USAGE
Oxybutynin chloride extended-release tablets are once daily controlled-release tablets indicated for the treatment of overactive bladder with symptoms of urge urinary incontinence, urgency, and frequency.
Oxybutynin chloride extended-release tablets are also indicated in the treatment of pediatric patients aged 6 years and older with symptoms of detrusor overactivity associated with a neurological condition (e.g., spina bifida).
CONTRAINDICATIONS
Oxybutynin chloride extended-release tablets are contraindicated in patients with urinary retention, gastric retention and other severe decreased gastrointestinal motility conditions, uncontrolled narrow angle glaucoma and in patients who are at risk for these conditions.
Oxybutynin chloride extended-release is also contraindicated in patients who have demonstrated hypersensitivity to the drug substance or other components of the product.
WARNINGS
Angioedema of the face, lips, tongue and/or larynx has been reported with oxybutynin. In some cases, angioedema occurred after the first dose. Angioedema associated with upper airway swelling may be life threatening. If involvement of the tongue, hypopharynx or larynx occurs, oxybutynin should be promptly discontinued and appropriate therapy and/or measures necessary to ensure a patent airway should be promptly provided.
PRECAUTIONS
Central Nervous System Effects
Oxybutynin is associated with anticholinergic central nervous system (CNS) effects (see ADVERSE REACTIONS). A variety of CNS anticholinergic effects have been reported, including hallucinations, agitation, confusion and somnolence. Patients should be monitored for signs of anticholinergic CNS effects, particularly in the first few months after beginning treatment or increasing the dose. If a patient experiences anticholinergic CNS effects, dose reduction or drug discontinuation should be considered.
Oxybutynin chloride extended-release should be used with caution in patients with preexisting dementia treated with cholinesterase inhibitors due to the risk of aggravation of symptoms.
General
Oxybutynin chloride extended-release should be used with caution in patients with hepatic or renal impairment and in patients with myasthenia gravis due to the risk of symptom aggravation.
Urinary Retention
Oxybutynin chloride extended-release should be administered with caution to patients with clinically significant bladder outflow obstruction because of the risk of urinary retention (see CONTRAINDICATIONS).
Gastrointestinal Disorders
Oxybutynin chloride extended-release should be administered with caution to patients with gastrointestinal obstructive disorders because of the risk of gastric retention (see CONTRAINDICATIONS).
Oxybutynin chloride extended-release, like other anticholinergic drugs, may decrease gastrointestinal motility and should be used with caution in patients with conditions such as ulcerative colitis and intestinal atony.
Oxybutynin chloride extended-release should be used with caution in patients who have gastroesophageal reflux and/or who are concurrently taking drugs (such as bisphosphonates) that can cause or exacerbate esophagitis.
As with any other nondeformable material, caution should be used when administering oxybutynin chloride extended-release to patients with preexisting severe gastrointestinal narrowing (pathologic or iatrogenic). There have been rare reports of obstructive symptoms in patients with known strictures in association with the ingestion of other drugs in nondeformable controlled-release formulations.
Information for Patients
Patients should be informed that oxybutynin may produce angioedema that could result in life threatening airway obstruction. Patients should be advised to promptly discontinue oxybutynin therapy and seek immediate medical attention if they experience edema of the tongue, edema of the laryngopharynx or difficulty breathing.
Patients should be informed that heat prostration (fever and heat stroke due to decreased sweating) can occur when anticholinergics such as oxybutynin chloride are administered in the presence of high environmental temperature.
Because anticholinergic agents such as oxybutynin may produce drowsiness (somnolence) or blurred vision, patients should be advised to exercise caution.
Patients should be informed that alcohol may enhance the drowsiness caused by anticholinergic agents such as oxybutynin.
Patients should be informed that oxybutynin chloride extended-release tablets should be swallowed whole with the aid of liquids. Patients should not chew, divide, or crush tablets.
Oxybutynin chloride extended-release tablets should be taken at approximately the same time each day.
Drug Interactions
The concomitant use of oxybutynin with other anticholinergic drugs or with other agents which produce dry mouth, constipation, somnolence (drowsiness), and/or other anticholinergic-like effects may increase the frequency and/or severity of such effects.
Anticholinergic agents may potentially alter the absorption of some concomitantly administered drugs due to anticholinergic effects on gastrointestinal motility. This may be of concern for drugs with a narrow therapeutic index.
Mean oxybutynin chloride plasma concentrations were approximately 2-fold higher when oxybutynin chloride extended-release tablets were administered with ketoconazole, a potent CYP3A4 inhibitor. Other inhibitors of the cytochrome P450 3A4 enzyme system, such as antimycotic agents (e.g., itraconazole and miconazole) or macrolide antibiotics (e.g., erythromycin and clarithromycin), may alter oxybutynin mean pharmacokinetic parameters (i.e., Cmax and AUC). The clinical relevance of such potential interactions is not known. Caution should be used when such drugs are coadministered.
Carcinogenesis, Mutagenesis, Impairment of Fertility
A 24-month study in rats at dosages of oxybutynin chloride of 20, 80 and 160 mg/kg/day showed no evidence of carcinogenicity. These doses are approximately 6, 25 and 50 times the maximum human exposure, based on surface area.
Oxybutynin chloride showed no increase of mutagenic activity when tested in Schizosaccharomyces pompholiciformis, Saccharomyces cerevisiae, and Salmonella typhimurium test systems.
Reproduction studies with oxybutynin chloride in the mouse, rat, hamster, and rabbit showed no definite evidence of impaired fertility.
Pregnancy
Teratogenic Effects. Pregnancy Category B
Reproduction studies with oxybutynin chloride in the mouse, rat, hamster, and rabbit showed no definite evidence of impaired fertility or harm to the animal fetus. The safety of oxybutynin chloride extended-release administration to women who are or who may become pregnant has not been established. Therefore, oxybutynin chloride extended-release should not be given to pregnant women unless, in the judgment of the physician, the probable clinical benefits outweigh the possible hazards.
Nursing Mothers
It is not known whether oxybutynin is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when oxybutynin chloride extended-release is administered to a nursing woman.
Pediatric Use
The safety and efficacy of oxybutynin chloride was studied in 60 children in a 24-week, open-label trial. Patients were aged 6 to 15 years, all had symptoms of detrusor overactivity in association with a neurological condition (e.g., spina bifida), all used clean intermittent catheterization, and all were current users of oxybutynin chloride. Study results demonstrated that administration of oxybutynin chloride extended-release 5 to 20 mg/day was associated with an increase from baseline in mean urine volume per catheterization from 108 mL to 136 mL, an increase from baseline in mean urine volume after morning awakening from 148 mL to 189 mL, and an increase from baseline in the mean percentage of catheterizations without a leaking episode from 34% to 51%.
Urodynamic results were consistent with clinical results. Administration of oxybutynin chloride extended-release resulted in an increase from baseline in mean maximum cystometric capacity from 185 mL to 254 mL, a decrease from baseline in mean detrusor pressure at maximum cystometric capacity from 44 cm H2O to 33 cm H2O, and a reduction in the percentage of patients demonstrating uninhibited detrusor contractions (of at least 15 cm H2O) from 60% to 28%.
Oxybutynin chloride extended-release tablets are not recommended in pediatric patients who cannot swallow the tablet whole without chewing, dividing or crushing, or in children under the age of 6 years (see DOSAGE AND ADMINISTRATION).
Geriatric Use
The rate and severity of anticholinergic effects reported by patients less than 65 years old and those 65 years and older were similar (see CLINICAL PHARMACOLOGY: Pharmacokinetics: Special Populations: Geriatric).
ADVERSE REACTIONS
Clinical Trials
Because clinical trials are conducted under widely varying conditions, the adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The safety and efficacy of oxybutynin chloride were evaluated in a total of 580 participants who received oxybutynin chloride extended-release tablets in four clinical trials (429 patients) and four pharmacokinetic studies (151 healthy volunteers). The 429 patients were treated with 5 to 30 mg/day for up to 4.5 months. Three of the four clinical trials allowed dose adjustments based on efficacy and adverse events and one was a fixed dose escalation design. Safety information is provided for 429 patients from these three controlled clinical studies and one open-label study in the first column of Table 3 below.
Adverse reactions from two additional fixed dose, active controlled, 12-week treatment duration, post-marketing studies, in which 576 patients were treated with oxybutynin chloride extended-release tablets 10 mg/day, are also listed in Table 3 (second column).
|
Body System |
Adverse Reactions |
Oxybutynin Chloride ER
|
Oxybutynin Chloride ER
|
|
General |
headache |
10 |
6 |
|
Digestive |
dry mouth |
61 |
29 |
|
constipation |
13 |
7 |
|
|
diarrhea |
9 |
7 |
|
|
nausea |
9 |
2 |
|
|
dyspepsia |
7 |
5 |
|
|
Nervous |
somnolence |
12 |
2 |
|
dizziness |
6 |
4 |
|
|
Special senses |
blurred vision |
8 |
1 |
|
dry eyes |
6 |
3 |
|
|
Urogenital |
urinary tract infection |
5 |
5 |
The most common adverse reactions reported by the 429 patients receiving 5 to 30 mg/day oxybutynin chloride extended-release tablets were the expected side effects of anticholinergic agents. The incidence of dry mouth was dose related.
The discontinuation rate for all adverse reactions was 6.8% in the 429 patients from the four studies of efficacy and safety who received 5 to 30 mg/day. The most frequent adverse reactions causing early discontinuation of study medication was nausea (1.9%), while discontinuation due to dry mouth was 1.2%.
In addition, the following adverse reactions were reported by ≥ 1 to < 5% of all patients who received oxybutynin chloride extended-release tablets in the six adjustable and fixed dose efficacy and safety studies. Psychiatric Disorders: depression, nervousness, insomnia, confusional state; Nervous System Disorders: dysgeusia; Cardiac Disorders: palpitations; Vascular Disorders: hypertension; Respiratory, Thoracic and Mediastinal Disorders: nasal dryness, cough, oropharyngeal pain, dry throat; Gastrointestinal Disorders: gastroesophageal reflux disease, abdominal pain, flatulence, vomiting; Skin and Subcutaneous Tissue Disorders: dry skin, pruritus; Renal and Urinary Disorders: urinary retention, urinary hesitation, dysuria; General Disorders and Administration Site Conditions: fatigue, edema peripheral, chest pain.
The following adverse reactions were reported by < 1% of oxybutynin chloride extended-release tablet-treated patients and at a higher incidence than placebo in clinical trials: Metabolism and Nutrition Disorders: anorexia, fluid retention; Vascular Disorders: hot flush; Respiratory, Thoracic and Mediastinal Disorders: dysphonia; Gastrointestinal Disorders: dysphagia, frequent bowel movements; General Disorders and Administration Site Conditions: chest discomfort, thirst.
Post-Marketing Experience
The following additional adverse drug reactions have been reported from worldwide post-marketing experience with oxybutynin chloride extended-release tablets. Because post-marketing reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Psychiatric Disorders: psychotic disorder, agitation, hallucinations, memory impairment; Nervous System Disorders: convulsions; Eye Disorders: glaucoma; Cardiac Disorders: arrhythmia, tachycardia, QT interval prolongation; Vascular Disorders: flushing; Skin and Subcutaneous Tissue Disorders: rash; Renal and Urinary Disorders: impotence; General Disorders and Administration Site Conditions: hypersensitivity reactions, including angioedema with airway obstruction, urticaria, and face edema; rare anaphylactic reactions requiring hospitalization for emergency treatment; Injury, Poisoning and Procedural Complications: fall.
Additional adverse events reported with some other oxybutynin chloride formulations include: cycloplegia, mydriasis, and suppression of lactation.
OVERDOSAGE
The continuous release of oxybutynin from oxybutynin chloride extended-release tablets should be considered in the treatment of overdosage. Patients should be monitored for at least 24 hours. Treatment should be symptomatic and supportive. Activated charcoal as well as a cathartic may be administered.
Overdosage with oxybutynin chloride has been associated with anticholinergic effects including central nervous system excitation, flushing, fever, dehydration, cardiac arrhythmia, vomiting, and urinary retention.
Ingestion of 100 mg oxybutynin chloride in association with alcohol has been reported in a 13 year old boy who experienced memory loss, and a 34 year old woman who developed stupor, followed by disorientation and agitation on awakening, dilated pupils, dry skin, cardiac arrhythmia, and retention of urine. Both patients fully recovered with symptomatic treatment.
DOSAGE AND ADMINISTRATION
Oxybutynin chloride extended-release tablets must be swallowed whole with the aid of liquids, and must not be chewed, divided, or crushed.
Oxybutynin chloride extended-release tablets may be administered with or without food.
Adults
The recommended starting dose of oxybutynin chloride extended-release tablets is 5 mg or 10 mg once daily at approximately the same time each day. Dosage may be adjusted in 5 mg increments to achieve a balance of efficacy and tolerability (up to a maximum of 30 mg/day). In general, dosage adjustment may proceed at approximately weekly intervals.
Pediatric Patients Aged 6 Years of Age and Older
The recommended starting dose of oxybutynin chloride extended-release tablets is 5 mg once daily at approximately the same time each day. Dosage may be adjusted in 5 mg increments to achieve a balance of efficacy and tolerability (up to a maximum of 20 mg/day).
HOW SUPPLIED
Oxybutynin Chloride Extended-release Tablets, USP are available containing 5 mg or 10 mg of oxybutynin chloride, USP.
The 5 mg tablets are light green film-coated, round, unscored tablets with M over O 5 imprinted in black ink on one side of the tablet and blank on the other side. They are available as follows:
NDC 0378-6605-01
bottles of 100 tablets
NDC 0378-6605-05
bottles of 500 tablets
The 10 mg tablets are peach film-coated, round, unscored tablets with M over O 10 imprinted in black ink on one side of the tablet and blank on the other side. They are available as follows:
NDC 0378-6610-01
bottles of 100 tablets
NDC 0378-6610-05
bottles of 500 tablets
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature.]
Protect from moisture and humidity.
Dispense in a tight, light-resistant container as defined in the USP using a child-resistant closure.
Mylan Pharmaceuticals Inc.
Morgantown, WV 26505 U.S.A.
REVISED MAY 2013
OXBN:R6
| OXYBUTYNIN CHLORIDE
oxybutynin chloride tablet, film coated, extended release |
||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||
| Labeler - Cardinal Health (603638201) |