Label: DESOXIMETASONE ointment
- NDC Code(s): 0168-0151-15, 0168-0151-60
- Packager: E. Fougera & Co. a division of Fougera Pharmaceuticals Inc.
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: None
- Marketing Status: Abbreviated New Drug Application
Drug Label Information
Updated November 7, 2019
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
- SPL UNCLASSIFIED SECTION
-
DESCRIPTION
Desoximetasone Ointment USP, 0.25% contains the active synthetic corticosteroid desoximetasone. The topical corticosteroids constitute a class of primarily synthetic steroids used as anti-inflammatory and antipruritic agents.
Each gram of Desoximetasone Ointment USP, 0.25% contains 2.5 mg of desoximetasone in a base consisting of white petrolatum and medium chain triglycerides.
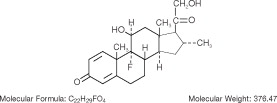
The chemical name of desoximetasone is: Pregna-1,4-diene-3,20-dione, 9-fluoro-11,21-dihydroxy-16-methyl-, (11β,16α)-. Desoximetasone has the following structural formula:
-
CLINICAL PHARMACOLOGY
Topical corticosteroids share anti-inflammatory, antipruritic and vasoconstrictive actions.
The mechanism of anti-inflammatory activity of the topical corticosteroids is unclear. Various laboratory methods, including vasoconstrictor assays, are used to compare and predict potencies and/or clinical efficacies of the topical corticosteroids. There is some evidence to suggest that a recognizable correlation exists between vasoconstrictor potency and therapeutic efficacy in man.
Pharmacokinetics: The extent of percutaneous absorption of topical corticosteroids is determined by many factors including the vehicle, the integrity of the epidermal barrier, and the use of occlusive dressings.
Topical corticosteroids can be absorbed from normal intact skin. Inflammation and/or other disease processes in the skin may increase percutaneous absorption. Occlusive dressings substantially increase the percutaneous absorption of topical corticosteroids. Thus, occlusive dressings may be a valuable therapeutic adjunct for treatment of resistant dermatoses.
Once absorbed through the skin, topical corticosteroids are handled through pharmacokinetic pathways similar to systemically administered corticosteroids. Corticosteroids are bound to plasma proteins in varying degrees. Corticosteroids are metabolized primarily in the liver and are then excreted by the kidneys. Some of the topical corticosteroids and their metabolites are also excreted into the bile.
Pharmacokinetic studies in men with Desoximetasone Ointment, USP 0.25% with tagged desoximetasone showed no detectable level (limit of sensitivity: 0.003 μg/mL) in 1 subject and 0.004 and 0.006 μg/mL in the remaining 2 subjects in the blood when it was applied topically on the back followed by occlusion for 24 hours. The extent of absorption for the ointment was 7% based on radioactivity recovered from urine and feces. Seven days after application, no further radioactivity was detected in urine or feces. Studies with other similarly structured steroids have shown that predominant metabolite reaction occurs through conjugation to form the glucuronide and sulfate ester.
- INDICATIONS AND USAGE
- CONTRAINDICATIONS
- WARNINGS
-
PRECAUTIONS
General: Systemic absorption of topical corticosteroids has produced reversible hypothalamic-pituitary-adrenal (HPA) axis suppression, manifestations of Cushing's syndrome, hyperglycemia, and glucosuria in some patients.
Conditions that augment systemic absorption include the application of the more potent steroids, use over large surface areas, prolonged use, and the addition of occlusive dressings.
Therefore, patients receiving a large dose of a potent topical steroid applied to a large surface area or under an occlusive dressing should be evaluated periodically for evidence of HPA axis suppression by using the urinary free cortisol and ACTH stimulation tests. If HPA axis suppression is noted, an attempt should be made to withdraw the drug, to reduce the frequency of application, or to substitute a less potent steroid.
Recovery of HPA axis function is generally prompt and complete upon discontinuation of the drug. Infrequently, signs and symptoms of steroid withdrawal may occur, requiring supplemental systemic corticosteroids.
Children may absorb proportionally larger amounts of topical corticosteroids and thus be more susceptible to systemic toxicity (See PRECAUTIONS: Pediatric Use).
If irritation develops, topical corticosteroids should be discontinued and appropriate therapy instituted.
In the presence of dermatologic infections, the use of an appropriate antifungal or antibacterial agent should be instituted. If a favorable response does not occur promptly, the corticosteroid should be discontinued until the infection has been adequately controlled.
Information for Patients: Patients using topical corticosteroids should receive the following information and instructions:
- 1.
- This medication is to be used as directed by the physician. It is for external use only. Avoid contact with the eyes.
- 2.
- Patients should be advised not to use this medication for any disorder other than that for which it was prescribed.
- 3.
- The treated skin area should not be bandaged or otherwise covered or wrapped so as to be occlusive unless directed by the physician.
- 4.
- Patients should report any signs of local adverse reactions, especially under occlusive dressing, to the physician.
- 5.
- Parents of pediatric patients should be advised not to use tight-fitting diapers or plastic pants on a child being treated in the diaper area, as these garments may constitute occlusive dressings.
Laboratory Tests: The following tests may be helpful in evaluating HPA axis suppression:
Urinary free cortisol test
ACTH stimulation test
Carcinogenesis, Mutagenesis, Impairment of Fertility: Long-term animal studies have not been performed to evaluate the carcinogenic potential or the effect on fertility of desoximetasone. Desoximetasone was nonmutagenic in the Ames test.
Pregnancy: Teratogenic Effects–Pregnancy Category C. Corticosteroids are generally teratogenic in laboratory animals when administered systemically at relatively low dosage levels. The more potent corticosteroids have been shown to be teratogenic after dermal application in laboratory animals.
Desoximetasone has been shown to be teratogenic and embryotoxic in mice, rats, and rabbits when given by subcutaneous or dermal routes of administration in doses 3 to 30 times the human dose of Desoximetasone Ointment, 0.25%.
There are no adequate and well-controlled studies in pregnant women on teratogenic effects from topically applied corticosteroids. Therefore, Desoximetasone Ointment, 0.25% should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. Drugs of this class should not be used extensively on pregnant patients, in large amounts, or for prolonged periods of time.
Nursing Mothers: It is not known whether topical administration of corticosteroids could result in sufficient systemic absorption to produce detectable quantities in breast milk. Systemically administered corticosteroids are secreted into breast milk in quantities not likely to have a deleterious effect on the infant. Nevertheless, caution should be exercised when topical corticosteroids are administered to a nursing woman.
Pediatric Use: Pediatric patients may demonstrate greater susceptibility to topical corticosteroid-induced HPA axis suppression and Cushing's syndrome than mature patients because of a larger skin surface area to body weight ratio.
Hypothalamic-pituitary-adrenal (HPA) axis suppression, Cushing's syndrome, and intracranial hypertension have been reported in children receiving topical corticosteroids. Manifestations of adrenal suppression in children include linear growth retardation, delayed weight gain, low plasma cortisol levels, and absence of response to ACTH stimulation. Manifestations of intracranial hypertension include bulging fontanelles, headaches, and bilateral papilledema.
Administration of topical corticosteroids to children should be limited to the least amount compatible with an effective therapeutic regimen. Chronic corticosteroid therapy may interfere with the growth and development of children. Safety and effectiveness of Desoximetasone Ointment, 0.25% in children below the age of 10 have not been established.
-
ADVERSE REACTIONS
The following local adverse reactions are reported infrequently with topical corticosteroids, but may occur more frequently with the use of occlusive dressings. These reactions are listed in an approximate decreasing order of occurrence: burning, itching, irritation, dryness, folliculitis, hypertrichosis, acneiform eruptions, hypopigmentation, perioral dermatitis, allergic contact dermatitis, maceration of the skin, secondary infection, skin atrophy, striae, and miliaria.
-
OVERDOSAGE
Topically applied corticosteroids can be absorbed in sufficient amounts to produce systemic effects (see PRECAUTIONS).
- DOSAGE AND ADMINISTRATION
- HOW SUPPLIED
- PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – 60 gram TUBE
- PACKAGE LABEL – PRINCIPAL DISPLAY PANEL – 60 gram CARTON
-
INGREDIENTS AND APPEARANCE
DESOXIMETASONE
desoximetasone ointmentProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:0168-0151 Route of Administration TOPICAL Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength desoximetasone (UNII: 4E07GXB7AU) (desoximetasone - UNII:4E07GXB7AU) desoximetasone 2.5 mg in 1 g Inactive Ingredients Ingredient Name Strength petrolatum (UNII: 4T6H12BN9U) medium-chain triglycerides (UNII: C9H2L21V7U) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:0168-0151-15 1 in 1 CARTON 09/28/2012 1 15 g in 1 TUBE; Type 0: Not a Combination Product 2 NDC:0168-0151-60 1 in 1 CARTON 09/28/2012 2 60 g in 1 TUBE; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date ANDA ANDA078657 09/28/2012 Labeler - E. Fougera & Co. a division of Fougera Pharmaceuticals Inc. (043838424)