MEFENAMIC ACID- mefenamic acid capsule
Paddock Laboratories, LLC
----------
Mefenamic Acid Capsules, USP 250 mg
Rx Only
Cardiovascular Risk
- •
- NSAIDs may cause an increased risk of serious cardiovascular thrombotic events, myocardial infarction, and stroke, which can be fatal. This risk may increase with duration of use. Patients with cardiovascular disease or risk factors for cardiovascular disease may be at greater risk (See WARNINGS).
- •
- Mefenamic acid is contraindicated for the treatment of peri-operative pain in the setting of coronary artery bypass graft (CABG) surgery (See WARNINGS).
Gastrointestinal Risk
- •
- NSAIDs cause an increased risk of serious gastrointestinal adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients are at greater risk for serious gastrointestinal events (See WARNINGS).
DESCRIPTION
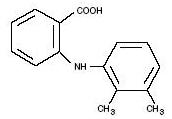
Mefenamic acid is a member of the fenamate group of nonsteroidal anti-inflammatory drugs (NSAIDs). Each Size ‘1’ Yellow-Yellow capsule, with ‘PAD’ imprinted on the cap & ‘195’ imprinted on the body, contains 250 mg of mefenamic acid for oral administration. Mefenamic acid is a white to greyish-white, odorless, microcrystalline powder with a melting point of 230° to 231°C and water solubility of 0.004% at pH 7.1. The chemical name is N-2,3-xylylanthranilic acid. The molecular weight is 241.29. Its molecular formula is C15H15N02 and the structural formula of mefenamic acid is:
Each capsule also contains lactose monohydrate. The capsule shell contains D&C yellow No. 10; FD&C blue No. 1; FD&C red No. 3; FD&C yellow No. 6; gelatin, sodium lauryl sulfate, titanium dioxide, black iron oxide, propylene glycol & shellac.
CLINICAL PHARMACOLOGY
Pharmacodynamics
Mefenamic acid is a non-steroidal anti-inflammatory drug (NSAID) that exhibits anti-inflammatory, analgesic, and antipyretic activities in animal models. The mechanism of action of mefenamic acid, like that of other NSAIDs, is not completely understood but may be related to prostaglandin synthetase inhibition.
Pharmacokinetics
Absorption: Mefenamic acid is rapidly absorbed after oral administration. In two 500 mg single oral dose studies, the mean extent of absorption was 30.5 mcg/hr/mL (17% CV).1,2 The bioavailability of the capsule relative to an IV dose or an oral solution has not been studied.
Following a single 1 gram oral dose, mean peak plasma levels ranging from 10 to 20 mcg/mL3 have been reported. Peak plasma levels are attained in 2 to 4 hours and the elimination half-life approximates 2 hours. Following multiple doses, plasma levels are proportional to dose with no evidence of drug accumulation. In a multiple dose trial of normal adult subjects (n=6) receiving 1 gram doses of mefenamic acid four times daily, steady-state concentrations of 20 mcg/mL were reached on the second day of administration, consistent with the short half-life.
The effect of food on the rate and extent of absorption of mefenamic acid has not been studied. Concomitant ingestion of antacids containing magnesium hydroxide has been shown to significantly increase the rate and extent of mefenamic acid absorption (see PRECAUTIONS, Drug Interactions).1
Distribution: Mefenamic acid has been reported as being greater than 90% bound to albumin.9 The relationship of unbound fraction to drug concentration has not been studied. The apparent volume of distribution (Vzss/F) estimated following a 500 mg oral dose of mefenamic acid was 1.06 L/kg.2
Based on its physical and chemical properties, mefenamic acid is expected to be excreted in human breast milk.
Metabolism: Mefenamic acid is metabolized by cytochrome P450 enzyme CYP2C9 to 3-hydroxymethyl mefenamic acid (Metabolite I). Further oxidation to a 3-carboxymefenamic acid (Metabolite II) may occur.10 The activity of these metabolites has not been studied. The metabolites may undergo glucuronidation and mefenamic acid is also glucuronidated directly. A peak plasma level approximating 20 mcg/mL was observed at 3 hours for the hydroxy metabolite and its glucuronide (n=6) after a single 1 gram dose. Similarly, a peak plasma level of 8 mcg/mL was observed at 6 to 8 hours for the carboxy metabolite and its glucuronide.3
Excretion: Approximately fifty-two percent of a mefenamic acid dose is excreted into the urine primarily as glucuronides of mefenamic acid (6%), 3-hydroxymefenamic acid (25%) and 3-carboxymefenamic acid (21%). The fecal route of elimination accounts for up to 20% of the dose, mainly in the form of unconjugated 3-carboxymefenamic acid.3
The elimination half-life of mefenamic acid is approximately two hours. Half-lives of metabolites I and II have not been precisely reported, but appear to be longer than the parent compound.3 The metabolites may accumulate in patients with renal or hepatic failure. The mefenamic acid glucuronide may bind irreversibly to plasma proteins. Because both renal and hepatic excretion are significant pathways of elimination, dosage adjustments in patients with renal or hepatic dysfunction may be necessary. Mefenamic acid should not be administered to patients with preexisting renal disease or in patients with significantly impaired renal function.
TABLE 1. Pharmacokinetic Parameter Estimates for Mefenamic Acid
|
PK Parameters
|
Normal Healthy Adults (18 to 45 yr)
|
|
|
|
Value |
CV |
|
Tmax (hr) |
2 |
66 |
|
Oral clearance (L/hr) |
21.23 |
38 |
|
Apparent volume of distribution; Vz/F (L/kg) |
1.06 |
60 |
|
Half-life; t1/2 (hrs) |
2 to 4 |
N/A |
Special Populations
Pediatric: Mefenamic acid has not been adequately investigated in pediatric patients less than 14 years of age. A study in 17 preterm infants administered 2 mg/kg indicated that the half life was about five times as long as adults, consistent with the low activity of metabolic enzymes in newborn infants. The mean Cmax in this study was 4 mcg/mL (range 2.9 to 6.1). The mean time to maximum concentration (Tmax) was 8 hours (range 2 to 18 hrs).11
Race: Pharmacokinetic differences due to race have not been identified.
Hepatic Insufficiency: Mefenamic acid pharmacokinetics have not been studied in patients with hepatic dysfunction. As hepatic metabolism is a significant pathway of mefenamic acid elimination, patients with acute and chronic hepatic disease may require reduced doses of mefenamic acid compared to patients with normal hepatic function.
Renal Insufficiency: Mefenamic acid pharmacokinetics have not been investigated in subjects with renal insufficiency. Given that mefenamic acid, its metabolites and conjugates are primarily excreted by the kidneys, the potential exists for mefenamic acid metabolites to accumulate. Mefenamic acid should not be administered to patients with preexisting renal disease or in patients with significantly impaired renal function.
Clinical Studies
In controlled, double-blind, clinical trials, mefenamic acid was evaluated for the treatment of primary spasmodic dysmenorrhea. The parameters used in determining efficacy included pain assessment by both patient and investigator; the need for concurrent analgesic medication; and evaluation of change in frequency and severity of symptoms characteristic of spasmodic dysmenorrhea. Patients received either mefenamic acid, 500 mg (2 capsules) as an initial dose of 250 mg every 6 hours, or placebo at onset of bleeding or of pain, whichever began first. After three menstrual cycles, patients were crossed over to the alternate treatment for an additional three cycles. Mefenamic acid was significantly superior to placebo in all parameters, and both treatments (drug and placebo) were equally tolerated.
INDICATIONS AND USAGE
Carefully consider the potential benefits and risks of mefenamic acid and other treatment options before deciding to use mefenamic acid . Use the lowest effective dose for the shortest duration consistent with individual patient treatment goals (see WARNINGS).
Mefenamic acid is indicated:
- •
- For relief of mild to moderate pain in patients ≥14 years of age, when therapy will not exceed one week (7 days).
- •
- For treatment of primary dysmenorrhea.
CONTRAINDICATIONS
Mefenamic acid is contraindicated in patients with known hypersensitivity to mefenamic acid.
Mefenamic acid should not be given to patients who have experienced asthma, urticaria, or allergic-type reactions after taking aspirin or other NSAIDs. Severe, rarely fatal, anaphylactic-like reactions to NSAIDs have been reported in such patients (see WARNINGS-Anaphylactoid Reactions, and PRECAUTIONS-Preexisting Asthma).
Mefenamic acid is contraindicated for the treatment of peri-operative pain in the setting of coronary artery bypass graft (CABG) surgery (see WARNINGS).
Mefenamic acid is contraindicated in patients with acute active ulceration or chronic inflammation of either the upper or lower gastrointestinal tract.
Mefenamic acid should not be used in patients with preexisting renal disease.
WARNINGS
CARDIOVASCULAR EFFECTS
Cardiovascular Thrombotic Events
Clinical trials of several COX-2 selective and nonselective NSAIDs of up to three years duration have shown an increased risk of serious cardiovascular (CV) thrombotic events, myocardial infarction, and stroke, which can be fatal. All NSAIDs, both COX-2 selective and nonselective, may have a similar risk. Patients with known CV disease or risk factors for CV disease may be at greater risk. To minimize the potential risk for an adverse CV event in patients treated with an NSAID, the lowest effective dose should be used for the shortest duration possible. Physicians and patients should remain alert for the development of such events, even in the absence of previous CV symptoms. Patients should be informed about the signs and/or symptoms of serious CV events and the steps to take if they occur.
There is no consistent evidence that concurrent use of aspirin mitigates the increased risk of serious CV thrombotic events associated with NSAID use. The concurrent use of aspirin and an NSAID does increase the risk of serious GI events (see GI WARNINGS).
Two large, controlled, clinical trials of a COX-2 selective NSAID for the treatment of pain in the first 10 to 14 days following CABG surgery found an increased incidence of myocardial infarction and stroke (see CONTRAINDICATIONS).
Hypertension
NSAIDs, including mefenamic acid, can lead to onset of new hypertension or worsening of preexisting hypertension, either of which may contribute to the increased incidence of CV events. Patients taking thiazides or loop diuretics may have impaired response to these therapies when taking NSAIDs. NSAIDS, including mefenamic acid, should be used with caution in patients with hypertension. Blood pressure (BP) should be monitored closely during the initiation of NSAID treatment and throughout the course of therapy.
Congestive Heart Failure and Edema
Fluid retention and edema have been observed in some patients taking NSAIDs. Mefenamic acid should be used with caution in patients with fluid retention or heart failure.
Gastrointestinal Effects - Risk of Ulceration, Bleeding, and Perforation
NSAIDs, including mefenamic acid, can cause serious gastrointestinal (GI) adverse events including inflammation, bleeding, ulceration, and perforation of the stomach, small intestine, or large intestine, which can be fatal. These serious adverse events can occur at any time, with or without warning symptoms, in patients treated with NSAIDs. Only one in five patients, who develop a serious upper GI adverse event on NSAID therapy, is symptomatic. Upper GI ulcers, gross bleeding, or perforation caused by NSAIDs occur in approximately 1% of patients treated for 3 to 6 months, and in about 2 to 4% of patients treated for one year. These trends continue with longer duration of use, increasing the likelihood of developing a serious GI event at some time during the course of therapy. However, even short-term therapy is not without risk.
NSAIDs should be prescribed with extreme caution in those with a prior history of ulcer disease or gastrointestinal bleeding. Patients with a prior history of peptic ulcer disease and/or gastrointestinal bleeding who use NSAIDs have a greater than 10-fold increased risk for developing a GI bleed compared to patients with neither of these risk factors. Other factors that increase the risk for GI bleeding in patients treated with NSAIDs include concomitant use of oral corticosteroids or anticoagulants, longer duration of NSAID therapy, smoking, use of alcohol, older age, and poor general health status. Most spontaneous reports of fatal GI events are in elderly or debilitated patients and therefore, special care should be taken in treating this population.
To minimize the potential risk for an adverse GI event in patients treated with an NSAID, the lowest effective dose should be used for the shortest possible duration. Patients and physicians should remain alert for signs and symptoms of GI ulceration and bleeding during NSAID therapy and promptly initiate additional evaluation and treatment if a serious GI adverse event is suspected. This should include discontinuation of the NSAID until a serious GI adverse event is ruled out. For high risk patients, alternate therapies that do not involve NSAIDs should be considered.
Renal Effects
Long-term administration of NSAIDs have resulted in renal papillary necrosis and other renal injury. Renal toxicity has also been seen in patients in whom renal prostaglandins have a compensatory role in the maintenance of renal perfusion. In these patients, administration of a nonsteroidal anti-inflammatory drug may cause a dose-dependent reduction in prostaglandin formation and, secondarily, in renal blood flow, which may precipitate overt renal decompensation. Patients at greatest risk of this reaction are those with impaired renal function, heart failure, liver dysfunction, those taking diuretics and ACE inhibitors, and the elderly. Discontinuation of NSAID therapy is usually followed by recovery to the pretreatment state.
Advanced Renal Disease
No information is available for controlled studies regarding the use of mefenamic acid in patients with advanced renal disease. Therefore, treatment with mefenamic acid is not recommended in these patients with advanced renal disease (see CONTRAINDICATIONS).
Anaphylactoid Reactions
As with other NSAIDs, anaphylactoid reactions may occur in patients without known prior exposure to mefenamic acid. Mefenamic acid should not be given to patients with the aspirin triad. This symptom complex typically occurs in asthmatic patients who experience rhinitis with or without nasal polyps, or who exhibit severe, potentially fatal bronchospasm after taking aspirin or other NSAIDs (see CONTRAINDICATIONS and PRECAUTIONS-Preexisting Asthma). Emergency help should be sought in cases where an anaphylactoid reaction occurs.
Skin Reactions
NSAIDs, including mefenamic acid, can cause serious skin adverse events such as exfoliative dermatitis, Stevens-Johnson Syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal. These serious events may occur without warning. Patients should be informed about the signs and symptoms of serious skin manifestations and use of the drug should be discontinued at the first appearance of skin rash or any other sign of hypersensitivity.
PRECAUTIONS
General
Mefenamic acid cannot be expected to substitute for corticosteroids or to treat corticosteroid insufficiency. Abrupt discontinuation of corticosteroids may lead to disease exacerbation. Patients on prolonged corticosteroid therapy should have their therapy tapered slowly if a decision is made to discontinue corticosteroids.
The pharmacological activity of mefenamic acid in reducing fever and inflammation may diminish the utility of these diagnostic signs in detecting complications of presumed noninfectious, painful conditions.
Hepatic Effects
Borderline elevations of one or more liver tests may occur in up to 15% of patients taking NSAIDs including mefenamic acid. These laboratory abnormalities may progress, may remain unchanged, or may be transient with continuing therapy. Notable elevations of ALT or AST (approximately three or more times the upper limit of normal) have been reported in approximately 1% of patients in clinical trials with NSAIDs. In addition, rare cases of severe hepatic reactions, including jaundice and fatal fulminant hepatitis, liver necrosis and hepatic failure, some of them with fatal outcomes have been reported.
A patient with symptoms and/or signs suggesting liver dysfunction, or in whom an abnormal liver test has occurred, should be evaluated for evidence of the development of a more severe hepatic reaction while on therapy with mefenamic acid. If clinical signs and symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g., eosinophilia, rash, etc.), mefenamic acid should be discontinued.
Hematological Effects
Anemia is sometimes seen in patients receiving NSAIDs, including mefenamic acid. This may be due to fluid retention, GI blood loss, or an incompletely described effect upon erythropoiesis. Patients on long-term treatment with NSAIDs, including mefenamic acid, should have their hemoglobin or hematocrit checked if they exhibit any signs or symptoms of anemia. NSAIDs inhibit platelet aggregation and have been shown to prolong bleeding time in some patients. Unlike aspirin, their effect on platelet function is quantitatively less, of shorter duration, and reversible. Patients receiving mefenamic acid who may be adversely affected by alterations in platelet function, such as those with coagulation disorders or patients receiving anticoagulants, should be carefully monitored.
Preexisting Asthma
Patients with asthma may have aspirin-sensitive asthma. The use of aspirin in patients with aspirin-sensitive asthma has been associated with severe bronchospasm which can be fatal. Since cross reactivity, including bronchospasm, between aspirin and other nonsteroidal anti-inflammatory drugs has been reported in such aspirin-sensitive patients, mefenamic acid should not be administered to patients with this form of aspirin sensitivity and should be used with caution in patients with preexisting asthma.
Information for Patients
Patients should be informed of the following information before initiating therapy with an NSAID and periodically during the course of ongoing therapy. Patients should also be encouraged to read the NSAID Medication Guide that accompanies each prescription dispensed.
- 1.
- Mefenamic acid, like other NSAIDs, may cause serious CV side effects, such as MI or stroke, which may result in hospitalization and even death. Although serious CV events can occur without warning symptoms, patients should be alert for the signs and symptoms of chest pain, shortness of breath, weakness, slurring of speech, and should ask for medical advice when observing any indicative sign or symptoms. Patients should be apprised of the importance of this follow-up (see WARNINGS, Cardiovascular Effects).
- 2.
- Mefenamic acid, like other NSAIDs, can cause GI discomfort and, rarely, serious GI side effects, such as ulcers and bleeding, which may result in hospitalizations and even death. Although serious GI tract ulcerations and bleeding can occur without warning symptoms, patients should be alert for the signs and symptoms of ulceration and bleeding, and should ask for medical advice when observing any indicative sign or symptoms including epigastric pain, dyspepsia, melena, and hematemesis. Patients should be apprised of the importance of this follow-up (see WARNINGS, Gastrointestinal Effects: Risk of Ulceration, Bleeding, and Perforation).
- 3.
- Mefenamic acid, like other NSAIDs, can cause serious skin side effects such as exfoliative dermatitis, SJS, and TEN, which may result in hospitalizations and even death. Although serious skin reactions may occur without warning, patients should be alert for the signs and symptoms of skin rash and blisters, fever, or other signs of hypersensitivity such as itching, and should ask for medical advice when observing any indicative signs or symptoms. Patients should be advised to stop the drug immediately if they develop any type of rash and contact their physicians as soon as possible.
- 4.
- Patients should promptly report signs or symptoms of unexplained weight gain or edema to their physicians.
- 5.
- Patients should be informed of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, pruritus, jaundice, right upper quadrant tenderness, and “flu-like” symptoms). If these occur, patients should be instructed to stop therapy and seek immediate medical therapy.
- 6.
- Patients should be informed of the signs of an anaphylactoid reaction (e.g., difficulty breathing, swelling of the face or throat). If these occur, patients should be instructed to seek immediate emergency help (see WARNINGSWARNINGS).
- 7.
- In late pregnancy, as with other NSAIDs, mefenamic acid should be avoided because it may cause premature closure of the ductus arteriosus.
Laboratory Tests
Because serious GI tract ulcerations and bleeding can occur without warning symptoms, physicians should monitor for signs or symptoms of GI bleeding. Patients on long-term treatment with NSAIDs should have their CBC and a chemistry profile checked periodically. If clinical signs and symptoms consistent with liver or renal disease develop, systemic manifestations occur (e.g., eosinophilia, rash, etc.) or if abnormal liver tests persist or worsen, mefenamic acid should be discontinued.
Drug Interactions
A number of compounds are inhibitors of CYP2C9. Drug interactions studies of mefenamic acid and these compounds have not been conducted. The possibility of altered safety and efficacy should be considered when mefenamic acid is used concomitantly with these drugs.
ACE-inhibitors
Reports suggest that NSAIDs may diminish the antihypertensive effect of ACE-inhibitors. This interaction should be given consideration in patients taking NSAIDs concomitantly with ACE-inhibitors.
Aspirin
When mefenamic acid is administered with aspirin, its protein binding is reduced, although the clearance of free mefenamic acid is not altered. The clinical significance of this interaction is not known; however, as with other NSAIDs, concomitant administration of mefenamic acid and aspirin is not generally recommended because of the potential of increased adverse effects.
Diuretics
Clinical studies, as well as postmarketing observations, have shown that mefenamic acid can reduce the natriuretic effect of furosemide and thiazides in some patients. This response has been attributed to inhibition of renal prostaglandin synthesis. During concomitant therapy of NSAIDs, the patient should be observed closely for signs of renal failure (see PRECAUTIONS, Renal Effects), as well as to assure diuretic efficacy.
Lithium
NSAIDs have produced an elevation of plasma lithium levels and a reduction in renal lithium clearance. The mean minimum lithium concentration increased 15% and the renal clearance decreased by approximately 20%. These effects have been attributed to inhibition of renal prostaglandin synthesis by the NSAID. Thus, when NSAIDs and lithium are administered concurrently, subjects should be observed carefully for signs of lithium toxicity.
Methotrexate
NSAIDs have been reported to competitively inhibit methotrexate accumulation in rabbit kidney slices. This may indicate that they could enhance the toxicity of methotrexate. Caution should be used when NSAIDs are administered concomitantly with methotrexate.
Warfarin
The effects of warfarin and NSAIDs on GI bleeding are synergistic, such that users of both drugs together have a risk of serious GI bleeding higher than users of either drug alone.
Antacids
In a single dose study (n=6), ingestion of an antacid containing 1.7 grams of magnesium hydroxide with 500 mg of mefenamic acid increased the Cmax and AUC of mefenamic acid by 125% and 36%, respectively.1
Drug/Laboratory Test Interactions
Mefenamic acid may prolong prothrombin time.4 Therefore, when the drug is administered to patients receiving oral anticoagulant drugs, frequent monitoring of prothrombin time is necessary.
A false-positive reaction for urinary bile, using the diazo tablet test, may result after mefenamic acid administration. If biliuria is suspected, other diagnostic procedures, such as the Harrison spot test, should be performed.
Pregnancy
Teratogenic Effects. Pregnancy Category C
Reproductive studies conducted in rats and rabbits have not demonstrated evidence of developmental abnormalities. However, animal reproduction studies are not always predictive of human response. There are no adequate or well controlled studies in pregnant women. Mefenamic acid should be used in pregnancy only if the potential benefit justifies the potential risk to the fetus.
Labor and Delivery
In rat studies with NSAIDs, as with other drugs known to inhibit prostaglandin synthesis, an increased incidence of dystocia, delayed parturition, and decreased pup survival occurred. The effects of mefenamic acid on labor and delivery in pregnant women are unknown.
Nursing Mothers
Trace amounts of mefenamic acid may be present in breast milk and transmitted to the nursing infant.7 Because of the potential for serious adverse reactions in nursing infants from mefenamic acid, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
Safety and effectiveness in pediatric patients below the age of 14 have not been established.
Geriatric Use
Clinical studies of mefenamic acid did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. As with any NSAIDs, caution should be exercised in treating the elderly (65 years and older).
This drug is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function (see CLINICAL PHARMACOLOGY and ADVERSE REACTIONS).
ADVERSE REACTIONS
In patients taking mefenamic acid or other NSAIDs, the most frequently reported adverse experiences occurring in approximately 1 to 10% of patients are:
Gastrointestinal experiences including - abdominal pain, constipation, diarrhea, dyspepsia, flatulence, gross bleeding/perforation, heartburn, nausea, GI ulcers (gastric/duodenal), vomiting, abnormal renal function, anemia, dizziness, edema, elevated liver enzymes, headaches, increased bleeding time, pruritus, rashes, tinnitus
Additional adverse experiences reported occasionally and listed here by body system include:
Body as a whole - fever, infection, sepsis.
Cardiovascular system - congestive heart failure, hypertension, tachycardia, syncope.
Digestive system - dry mouth, esophagitis, gastric/peptic ulcers, gastritis, gastrointestinal bleeding, glossitis, hematemesis, hepatitis, jaundice.
Hemic and lymphatic system - ecchymosis, eosinophilia, leukopenia, melena, purpura, rectal bleeding, stomatitis, thrombocytopenia.
Metabolic and nutritional - weight changes.
Nervous system - anxiety, asthenia, confusion, depression, dream abnormalities, drowsiness; insomnia, malaise, nervousness, paresthesia, somnolence, tremors, vertigo.
Respiratory system - asthma, dyspnea.
Skin and appendages - alopecia, photosensitivity, pruritus, sweat.
Special senses - blurred vision.
Urogenital system - cystitis, dysuria, hematuria, interstitial nephritis, oliguria/polyuria, proteinuria, renal failure.
Other adverse reactions, which occur rarely are:
Body as a whole - anaphylactoid reactions, appetite changes, death.
Cardiovascular system - arrhythmia, hypotension, myocardial infarction, palpitations, vasculitis
Digestive system - eructation, liver failure, pancreatitis.
Hemic and lymphatic system - agranulocytosis, hemolytic anemia, aplastic anemia, lymphadenopathy, pancytopenia.
Metabolic and nutritional – hyperglycemia.
Nervous system - convulsions, coma, hallucinations, meningitis.
Respiratory - respiratory depression, pneumonia.
Skin and appendages - angioedema, toxic epidermal necrosis, erythema multiforme, exfoliative dermatitis, Stevens-Johnson syndrome, urticaria.
Special senses - conjunctivitis, hearing impairment.
OVERDOSAGE
Symptoms following acute NSAIDs overdoses are usually limited to lethargy, drowsiness, nausea, vomiting, and epigastric pain, which are generally reversible with supportive care. Gastrointestinal bleeding can occur. Hypertension, acute renal failure, respiratory depression and coma may occur, but are rare. Anaphylactoid reactions have been reported with therapeutic ingestion of NSAIDs, and may occur following an overdose.
Patients should be managed by symptomatic and supportive care following an NSAID overdose. There are no specific antidotes. Emesis and/or activated charcoal (60 to 100 g in adults, 1 to 2 g/kg in children) and/or osmotic cathartic may be indicated in patients seen within 4 hours of ingestion with symptoms or following a large overdose (5 to 10 times the usual dose). Forced diuresis, alkalinization of urine, hemodialysis, or hemoperfusion may not be useful due to high protein binding.
DOSAGE AND ADMINISTRATION
Carefully consider the potential benefits and risks of mefenamic acid and other treatment options before deciding to use mefenamic acid. Use the lowest effective dose for the shortest duration consistent with individual patient treatment goals (see WARNINGS).
After observing the response to initial therapy with mefenamic acid, the dose and frequency should be adjusted to suit an individual patient's needs.
For the relief of acute pain in adults and adolescents ≥ 14 years of age, the recommended dose is 500 mg as an initial dose followed by 250 mg every 6 hours as needed, usually not to exceed one week.4
For the treatment of primary dysmenorrhea, the recommended dose is 500 mg as an initial dose followed by 250 mg every 6 hours, given orally, starting with the onset of bleeding and associated symptoms. Clinical studies indicate that effective treatment can be initiated with the start of menses and should not be necessary for more than 2 to 3 days.5
HOW SUPPLIED
Mefenamic Acid Capsules USP 250 mg are Size ‘1’ yellow-yellow capsules with ‘PAD’ imprinted on the cap & ‘195’ imprinted on the body. They are supplied as follows:
Bottles of 30 NDC 0574-0195-30
Bottles of 100 NDC 0574-0195-01
Storage
Store at 20-25°C (68-77°F); excursions permitted to 15-30°C (59-86°F) [See USP Controlled Room Temperature].
REFERENCES
- 1.
- Neuvonen PJ, Kivisto KT: Enhancement of drug absorption by antacids. An unrecognized drug interaction. Clin Pharmacokinet. 27:120-8, Aug 1994.
- 2.
- Tall AR, Mistilits SP: Studies on Ponstan (mefenamic acid): I. Gastro-intestinal blood loss; II. Absorption and excretion of a new formulation. J Int Med Res (UK). 1975, 3 (3) p176-82.
- 3.
- Winder CV, Kaump DH, Glazko et al: Experimental observations of flufenamic, mefenamic, and meclofenamic acids. AnnPhys Med (Eng), Suppl p7-49.1967.
- 4.
- Glazko AJ: Experimental observations of flufenamic, mefenamic, and meclofenamic acids. Part III. Metabolic disposition, in Fenamates in Medicine. A Symposium, London, 1966. Annals of Physical Medicine, Supplement, pp 23-36, 1967.
- 5.
- Data on file, First Horizon (Protocol 356).
- 6.
- Budoff PW: Use of mefenamic acid in the treatment of primary dysmenorrhea. JAMA. 241: 2713-2716, 1979.
- 7.
- Buchanan RA, et al. The breast milk excretion of mefenamic acid. Curr Ther Res. 10:592, 1968.
- 8.
- Corby DG, Decker WJ: Management of acute poisoning with activated charcoal. Pediatrics. 54:324, 1974.
- 9.
- Champion GD, Graham GG: Pharmacokinetics of non-steroidal anti-inflammatory agents. Aust NZ J Med. 8 (Supp 1): 94-100, Jun 1978
- 10.
- McGurk KA, Remmel RP, Hosagrahara VP, Tosh D, Burchell B: Reactivity of mefenamic acid 1-o-acyl glucuronide with proteins in vitro and ex vivo. Drug Metab Dispos. Aug 1996, 24 (8) p842-9.
- 11.
- Ito K, Niida Y, Sato J et al: Pharmacokinetics of mefenamic acid in preterm infants with patent ductus arteriosus. Acta Paediatr JPN. 36 (4): 387-91, 1994.
Manufactured in India by:
MICRO LABS LIMITED
Plot No. S-155-159,
Verna Industrial Estate
Phase-III, Verna GOA 403722, INDIA.
Manufactured For:
Perrigo
Minneapolis, MN 55427
Revised: 09/2014
Medication Guide for Nonsteroidal Anti-Inflammatory Drugs (NSAIDs) (See the end of this Medication Guide for a list of prescription NSAID medicines.)
What is the most important information I should know about medicines called Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)?
NSAID medicines may increase the chance of a heart attack or stroke that can lead to death. This chance increases:
- •
- with increasing doses of NSAID medicines
- •
- with longer use of NSAID medicines
- •
- in people who have heart disease
NSAID medicines should never be used right before or after a heart surgery called a “coronary artery bypass graft (CABG).”
NSAID medicines can cause ulcers and bleeding in the stomach and intestines at any time during treatment. Ulcers and bleeding:
- •
- can happen without warning symptoms
- •
- may cause death
The chance of a person getting an ulcer or bleeding increases with:
- •
- increasing doses of NSAID medicines
- •
- taking medicines called "corticosteroids" and "anticoagulants"
- •
- longer use
- •
- smoking
- •
- drinking alcohol
- •
- older age
- •
- having poor health
NSAID medicines should only be used:
- •
- exactly as prescribed
- •
- at the lowest dose possible for your treatment
- •
- for the shortest time needed
What are Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)?
NSAID medicines are used to treat pain and redness, swelling, and heat (inflammation) from medical conditions such as:
- •
- different types of arthritis
- •
- menstrual cramps and other types of short-term pain
Who should not take a Nonsteroidal Anti-Inflammatory Drug (NSAID)?
Do not take an NSAID medicine:
- •
- if you had an asthma attack, hives, or other allergic reaction with aspirin or any other NSAID medicine
- •
- for pain right before or after heart bypass surgery
Tell your healthcare provider:
- •
- about all of your medical conditions.
- •
- about all of the medicines you take. NSAIDs and some other medicines can interact with each other and cause serious side effects. Keep a list of your medicines to show to your healthcare provider and pharmacist.
- •
- if you are pregnant, NSAID medicines should not be used past 30 weeks of pregnancy.
- •
- if you are breastfeeding, talk to your doctor.
What are the possible side effects of Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)?
|
Serious side effects include:
|
Other side effects include:
|
|
|
Get emergency help right away if you have any of the following symptoms:
|
|
|
|
|
|
Stop your NSAID medicine and call your healthcare provider right away if you have any of the following symptoms:
|
|
|
|
|
|
|
|
|
|
|
|
These are not all the side effects with NSAID medicines. Talk to your healthcare provider or pharmacist for more information about NSAID medicines.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Other information about Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
- •
- Aspirin is an NSAID medicine but it does not increase the chance of a heart attack. Aspirin can cause bleeding in the brain, stomach, and intestines. Aspirin can also cause ulcers in the stomach and intestines.
- •
- Some of these NSAID medicines are sold in lower doses without a prescription (over-the-counter). Talk to your healthcare provider before using over-the-counter NSAIDs for more than 10 days.
NSAID medicines requiring a prescription
|
Generic Name
|
Tradename
|
|
Celecoxib |
Celebrex |
|
Diclofenac |
Zorvolex, Cataflam, Cambia, Voltaren, Voltaren gel, Arthrotec (combined with misoprostol), Flector, Zipsor, Pennsaid |
|
Diflunisal |
Dolobid |
|
Etodolac |
Lodine, Lodine XL |
|
Fenoprofen |
Nalfon, Nalfon 200 |
|
Flurbiprofen |
Ansaid |
|
Ibuprofen |
Motrin, Tab-Profen, *Vicoprofen (combined with hydrocodone), Combunox (combined with oxycodone), Duexis (combined with famotidine) |
|
Indomethacin |
Tivorbex, Indocin, Indocin SR, Indo-Lemmon, Indomethagan |
|
Ketoprofen |
Oruvail, Nexcede |
|
Ketorolac |
Toradol, Sprix |
|
Mefenamic Acid |
Ponstel |
|
Meloxicam |
Mobic |
|
Nabumetone |
Relafen |
|
Naproxen |
Naprosyn, Anaprox, Anaprox DS, EC-Naprosyn, Naprelan, Naprapac (copackaged with lansoprazole), Treximet (combined with sumatriptan succinate) and Vimovo (combined with esomeprazole magnesium) |
|
Oxaprozin |
Daypro |
|
Piroxicam |
Feldene |
|
Sulindac |
Clinoril |
|
Tolmetin |
Tolectin, Tolectin DS, Tolectin 600 |
*Vicoprofen contains the same dose of ibuprofen as over-the-counter (OTC) NSAIDs, and is usually used for less than 10 days to treat pain. The OTC NSAID label warns that long term continuous use may increase the risk of heart attack or stroke.
The brands listed are the trademarks or register marks of their respective owners and are not trademarks or register marks of Micro labs.
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Manufactured in India by:
MICRO LABS LIMITED
Plot No. S-155 to S-159,
Verna Industrial Estate Phase-III,
Verna, Goa-403722. INDIA.
Revised: 09/2014
| MEFENAMIC ACID
mefenamic acid capsule |
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
|
||||||||||||||||||||||||||
| Labeler - Paddock Laboratories, LLC (967694121) |