Label: METHADONE HYDROCHLORIDE injection, solution
- NDC Code(s): 67457-217-20
- Packager: Mylan Institutional LLC
- Category: HUMAN PRESCRIPTION DRUG LABEL
- DEA Schedule: CII
- Marketing Status: New Drug Application
Drug Label Information
Updated December 1, 2023
If you are a consumer or patient please visit this version.
- Download DRUG LABEL INFO: PDF XML
- Official Label (Printer Friendly)
-
BOXED WARNING
(What is this?)
WARNING: SERIOUS AND LIFE-THREATENING RISKS FROM USE OF METHADONE HYDROCHLORIDE INJECTION
Addiction, Abuse, and Misuse
Because the use of Methadone Hydrochloride Injection exposes patients and other users to the risks of opioid addiction, abuse, and misuse, which can lead to overdose and death, assess each patient’s risk prior to prescribing and reassess all patients regularly for the development of these behaviors and conditions (see WARNINGS).
Life-Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression may occur with use of Methadone Hydrochloride Injection, especially during initiation or following a dosage increase. To reduce the risk of respiratory depression, proper dosing and titration of Methadone Hydrochloride Injection are essential (see WARNINGS).
Neonatal Opioid Withdrawal Syndrome (NOWS)
If opioid use is required for an extended period of time in a pregnant woman, advise the patient of the risk of NOWS, which may be life-threatening if not recognized and treated. Ensure that management by neonatology experts will be available at delivery (see WARNINGS).
Risks From Concomitant Use With Benzodiazepines Or Other CNS Depressants
Concomitant use of opioids with benzodiazepines or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Reserve concomitant prescribing of Methadone Hydrochloride Injection and benzodiazepines or other CNS depressants for use in patients for whom alternative treatment options are inadequate (see WARNINGS, PRECAUTIONS).
Life-Threatening QT Prolongation
QT interval prolongation and serious arrhythmia (torsades de pointes) have occurred during treatment with methadone. Most cases involve patients being treated for pain with large, multiple daily doses of methadone, although cases have been reported in patients receiving doses commonly used for maintenance treatment of opioid addiction. Closely monitor patients with risk factors for development of prolonged QT interval, a history of cardiac conduction abnormalities, and those taking medications affecting cardiac conduction for changes in cardiac rhythm during initiation and titration of Methadone Hydrochloride Injection (see WARNINGS).
Interactions with Drugs Affecting Cytochrome P450 Isoenzymes
The concomitant use of Methadone Hydrochloride Injection with all cytochrome P450 3A4, 2B6, 2C19, 2C9 or 2D6 inhibitors may result in an increase in methadone plasma concentrations, which could cause potentially fatal respiratory depression. In addition, discontinuation of concomitantly used cytochrome P450 3A4 2B6, 2C19, or 2C9 inducers may also result in an increase in methadone plasma concentration. Follow patients closely for respiratory depression and sedation and consider dosage reduction with any changes of concomitant medications that result in an increase in methadone levels (see WARNINGS, PRECAUTIONS: Drug Interactions).
Conditions for Distribution and Use of Methadone Products for the Treatment of Opioid Addiction
For detoxification and maintenance of opioid dependence, methadone should be administered in accordance with the treatment standards cited in 42 CFR Section 8, including limitations on unsupervised administration (see INDICATIONS AND USAGE).
-
DESCRIPTION
Methadone Hydrochloride Injection USP, 10 mg/mL is an opioid analgesic for parenteral use (intravenous, intramuscular or subcutaneous use). Methadone Hydrochloride Injection USP, 10 mg/mL contains methadone hydrochloride as the active pharmaceutical ingredient.
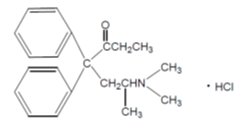
Methadone hydrochloride is a white, crystalline material that is water-soluble. Methadone hydrochloride is chemically described as 6-(dimethylamino)-4,4-diphenyl-3-hepatanone hydrochloride. Its molecular formula is C21H27NO•HCl and it has a molecular weight of 345.91. Methadone hydrochloride has a melting point of 235°C, and a pKa of 8.25 in water at 20°C. Its octanol/water partition coefficient at pH 7.4 is 117. A solution (1:100) in water has a pH between 4.5 and 6.5.
Methadone hydrochloride has the following structural formula:
Methadone Hydrochloride Injection is a sterile injectable solution available in 20 mL multiple-dose vials. Each mL of the Methadone Hydrochloride Injection contains: 10 mg of methadone hydrochloride (equivalent to 8.95 mg of methadone free base), 5 mg of chlorobutanol, as a preservative, 9 mg of sodium chloride, as tonicity agent, and hydrochloric acid and sodium hydroxide as pH adjusters, in water for injection. The pH of the sterile injectable solution is between 3.0 to 6.5.
-
CLINICAL PHARMACOLOGY
Mechanism of Action
Methadone hydrochloride is a mu-agonist; a synthetic opioid analgesic with multiple actions qualitatively similar to those of morphine, the most prominent of which involve the central nervous system and organs composed of smooth muscle. The principal therapeutic uses for methadone are for analgesia and for detoxification or maintenance in opioid addiction. The methadone abstinence syndrome, although qualitatively similar to that of morphine, differs in that the onset is slower, the course is more prolonged, and the symptoms are less severe.
Some data also indicate that methadone acts as an antagonist at the N-methyl-D-aspartate (NMDA) receptor. The contribution of NMDA receptor antagonism to methadone’s efficacy is unknown.
Pharmacodynamics
Effects on the Central Nervous System
Methadone produces respiratory depression by direct action on brain stem respiratory centers. The respiratory depression involves a reduction in the responsiveness of the brain stem respiratory centers to both increases in carbon dioxide tension and electrical stimulation.
Methadone causes miosis, even in total darkness. Pinpoint pupils are a sign of opioid overdose but are not pathognomonic (e.g., pontine lesions of hemorrhagic or ischemic origins may produce similar findings). Marked mydriasis rather than miosis may be seen due to hypoxia in overdose situations.
Some NMDA receptor antagonists have been shown to produce neurotoxic effects in animals.
Effects on the Gastrointestinal Tract and Other Smooth Muscle
Methadone causes a reduction in motility associated with an increase in smooth muscle tone in the antrum of the stomach and duodenum. Digestion of food in the small intestine is delayed and propulsive contractions are decreased. Propulsive peristaltic waves in the colon are decreased, while tone is increased to the point of spasm, resulting in constipation. Other opioid-induced effects may include a reduction in biliary and pancreatic secretions, spasm of sphincter of Oddi, and transient elevations in serum amylase.
Effects on the Cardiovascular System
Methadone produces peripheral vasodilation, which may result in orthostatic hypotension or syncope. Manifestations of histamine release and/or peripheral vasodilation may include pruritus, flushing, red eyes, sweating, and/or orthostatic hypotension.
Effects on the Endocrine System
Opioids inhibit the secretion of adrenocorticotropic hormone (ACTH), cortisol, and luteinizing hormone (LH) in humans. They also stimulate prolactin, growth hormone (GH) secretion, and pancreatic secretion of insulin and glucagon.
Chronic use of opioids for an extended period of time may influence the hypothalamic-pituitary-gonadal axis, leading to androgen deficiency that may manifest as low libido, impotence, erectile dysfunction, amenorrhea, or infertility. The causal role of opioids in the clinical syndrome of hypogonadism is unknown because the various medical, physical, lifestyle, and psychological stressors that may influence gonadal hormone levels have not been adequately controlled for in studies conducted to date.
Effects on the Immune System
Opioids have been shown to have a variety of effects on components of the immune system in in vitro and animal models. The clinical significance of these findings is unknown. Overall, the effects of opioids appear to be modestly immunosuppressive.
Concentration–Efficacy Relationships
The minimum effective analgesic concentration will vary widely among patients, especially among patients who have been previously treated with opioid agonists. The minimum effective analgesic concentration of methadone for any individual patient may increase over time due to an increase in pain, the development of a new pain syndrome, and/or the development of analgesic tolerance.
Concentration–Adverse Reaction Relationships
There is a relationship between increasing methadone plasma concentration and increasing frequency of dose-related opioid adverse reactions such as nausea, vomiting, CNS effects, and respiratory depression. In opioid-tolerant patients, the situation may be altered by the development of tolerance to opioid-related adverse reactions.
Pharmacokinetics
Absorption
Methadone Hydrochloride Injection is intended for parenteral (intravenous, subcutaneous and intramuscular) administration. Methadone pharmacokinetics following subcutaneous and intramuscular administration have not been systematically studied and differences among the various parenteral routes have not been well characterized. As with many drugs, absorption into the systemic circulation may vary with subcutaneous and intramuscular administration.
Distribution
Methadone is a lipophilic drug and the steady state volume of distribution ranges between 2 L/kg to 6 L/kg. In plasma, methadone is predominantly bound to α1-acid glycoprotein (85% to 90%). Methadone is secreted in saliva, breast milk, amniotic fluid and umbilical cord plasma.
Elimination
Metabolism
Methadone is primarily metabolized by N-demethylation to an inactive metabolite, 2-ethylidene-1,5-dimethyl-3,3-diphenylpyrrolidene (EDDP). Cytochrome P450 enzymes, primarily CYP3A4, CYP2B6, CYP2C19, CYP2C9 and CYP2D6, are responsible for conversion of methadone to EDDP and other inactive metabolites, which are excreted mainly in urine.
Excretion
Elimination of methadone is mediated by extensive biotransformation, followed by renal and fecal excretion. After single intravenous dose administration the plasma clearance of methadone ranged between 3 L/h to 10 L/h and the terminal half-life (t½) ranged between 8 to 59 hours. Methadone has been known to persist in the liver and other tissues. Slow release from the liver and other tissues may prolong the duration of methadone action despite low plasma concentrations.
Specific Populations
Use During Pregnancy
There are no pharmacokinetic studies of parenteral methadone in pregnancy. The disposition of oral methadone has been studied in approximately 30 pregnant patients in 2nd and 3rd trimesters. Elimination of methadone was significantly changed in pregnancy. Total body clearance of methadone was increased in pregnant patients compared to the same patients postpartum or to non-pregnant opioid-dependent women. The terminal half-life of methadone is decreased during second and third trimesters. The decrease in plasma half-life and increased clearance of methadone resulting in lower methadone trough levels during pregnancy can lead to withdrawal symptoms in some pregnant patients. The dosage may need to be increased or the dosing interval decreased in pregnant patients receiving methadone (see DOSAGE AND ADMINISTRATION).
Hepatic Impairment
Methadone pharmacokinetics have not been extensively evaluated in patients with hepatic insufficiency. Methadone is metabolized in the liver and patients with liver impairment may be at risk of accumulating methadone after multiple dosing.
Renal Impairment
Methadone pharmacokinetics have not been extensively evaluated in patients with renal insufficiency. Unchanged methadone and its metabolites are excreted in urine to a variable degree. Methadone is a basic (pKa = 9.2) compound and the luminal pH of the urinary tract can affect its extraction from plasma. Urine acidification has been shown to increase renal elimination of methadone. Forced diuresis, peritoneal dialysis, hemodialysis, or charcoal hemoperfusion have not been established as beneficial for increasing methadone or metabolite elimination.
Drug Interaction Studies
Cytochrome P450 Interactions
Methadone undergoes hepatic N-demethylation by cytochrome P450 (CYP) isoforms, principally CYP3A4, CYP2B6, CYP2C19, CYP2C9 and CYP2D6. Co-administration of methadone with CYP inducers may result in more rapid metabolism and potential for decreased effects of methadone, whereas administration with CYP inhibitors may reduce metabolism and potentiate methadone’s effects. Although antiretroviral drugs such as efavirenz, nelfinavir, nevirapine, ritonavir, lopinavir+ritonavir combination are known to inhibit some CYPs, they are shown to reduce the plasma levels of methadone, possibly due to CYP induction activity (see PRECAUTIONS: Drug Interactions).
Cytochrome P450 Inducers
The following drug interactions were reported following co-administration of methadone with known inducers of cytochrome P450 enzymes:
Rifampin
In patients well-stabilized on methadone, concomitant administration of rifampin resulted in a marked reduction in serum methadone levels and a concurrent appearance of withdrawal symptoms.
Phenytoin
In a pharmacokinetic study with patients on methadone maintenance therapy, phenytoin administration (250 mg twice daily initially for 1 day followed by 300 mg daily for 3 to 4 days) resulted in an approximately 50% reduction in methadone exposure and withdrawal symptoms occurred concurrently. Upon discontinuation of phenytoin, the incidence of withdrawal symptoms decreased and methadone exposure increased to a level comparable to that prior to phenytoin administration.
Cytochrome P450 Inhibitors
Voriconazole
Voriconazole can inhibit the activity of CYP3A4, CYP2C9, and CYP2C19. Repeat dose administration of oral voriconazole (400 mg every 12 hours for 1 day, then 200 mg every 12 hours for 4 days) increased the peak plasma concentration (Cmax) and AUC of (R)-methadone by 31% and 47%, respectively, in subjects receiving a methadone maintenance dose (30 mg to 100 mg daily. The Cmax and AUC of (S)-methadone increased by 65% and 103%, respectively. Increased plasma concentrations of methadone have been associated with toxicity including QT prolongation. Frequent monitoring for adverse events and toxicity related to methadone is recommended during co-administration. Dose reduction of methadone may be needed (see PRECAUTIONS: Drug Interactions).
Antiretroviral Drugs
Although antiretroviral drugs such as efavirenz, nelfinavir, nevirapine, ritonavir, telaprevir, lopinavir+ritonavir combination are known to inhibit some CYPs, they are shown to reduce the plasma levels of methadone, possibly due to CYP induction activity.
Abacavir, amprenavir, darunavir+ritonavir, efavirenz, nelfinavir, nevirapine, ritonavir, telaprevir, lopinavir+ritonavir, saquinavir+ritonavir, tipranvir+ritonavir combination
Co-administration of these anti-retroviral agents resulted in increased clearance or decreased plasma levels of methadone (see PRECAUTIONS: Drug Interactions).
Didanosine and Stavudine
Methadone decreased the AUC and peak levels for didanosine and stavudine, with a more significant decrease for didanosine. Methadone disposition was not substantially altered (see PRECAUTIONS: Drug Interactions).
Zidovudine
Methadone increased the AUC of zidovudine which could result in toxic effects (see PRECAUTIONS: Drug Interactions).
Pharmacokinetics in Special Populations
Pregnancy
There are no pharmacokinetic studies of parenteral methadone in pregnancy. The disposition of oral methadone has been studied in approximately 30 pregnant patients in 2nd and 3rd trimesters. Elimination of methadone was significantly changed in pregnancy. Total body clearance of methadone was increased in pregnant patients compared to the same patients postpartum or to non-pregnant opioid-dependent women. The terminal half-life of methadone is decreased during second and third trimesters. The decrease in plasma half-life and increased clearance of methadone resulting in lower methadone trough levels during pregnancy can lead to withdrawal symptoms in some pregnant patients. The dosage may need to be increased or the dosing interval decreased in pregnant patients receiving methadone (see DOSAGE AND ADMINISTRATION).
-
INDICATIONS AND USAGE
- 1.
- Methadone Hydrochloride Injection is indicated for the management of severe and persistent pain that requires an extended treatment period with a daily opioid analgesic and for which alternative treatment options are inadequate.
Limitations of Use- •
- Because of the risks of addiction, abuse, and misuse with opioids, which can occur at any dosage or duration, and because of the greater risks of overdose and death with extended-release/long-acting opioid formulations, (see WARNINGS) reserve Methadone Hydrochloride Injection for use in patients for whom alternative treatment options (e.g., nonopioid analgesics or immediate-release opioids) are ineffective, not tolerated, or would be otherwise inadequate to provide sufficient management of pain.
- •
- Methadone Hydrochloride Injection is not indicated as an as-needed (prn) analgesic.
- 2.
- For use in temporary treatment of opioid dependence in patients unable to take oral medication.
Limitations of Use- •
- Injectable methadone products are not approved for the outpatient treatment of opioid dependence. In this patient population, parenteral methadone is to be used only for patients unable to take oral medication, such as hospitalized patients.
Conditions for Distribution and Use of Methadone Products for the Treatment of Opioid Addiction
Code of Federal Regulations, Title 42, Sec 8.
Methadone products when used for the treatment of opioid addiction in detoxification or maintenance programs, shall be dispensed only by opioid treatment programs (and agencies, practitioners or institutions by formal agreement with the program sponsor) certified by the Substance Abuse and Mental Health Services Administration and approved by the designated state authority. Certified treatment programs shall dispense and use methadone in oral form only and according to the treatment requirements stipulated in the Federal Opioid Treatment Standards (42 CFR 8.12). See below for important regulatory exceptions to the general requirement for certification to provide opioid agonist treatment.
Failure to abide by the requirements in these regulations may result in criminal prosecution, seizure of the drug supply, revocation of the program approval, and injunction precluding operation of the program.
Regulatory Exceptions to the General Requirement for Certification to Provide Opioid Agonist Treatment: During inpatient care, when the patient was admitted for any condition other than concurrent opioid addiction (pursuant to 21CFR 1306.07(c)), to facilitate the treatment of the primary admitting diagnosis.
During an emergency period of no longer than 3 days while definitive care for the addiction is being sought in an appropriately licensed facility (pursuant to 21CFR 1306.07(b)).
-
CONTRAINDICATIONS
Methadone Hydrochloride Injection is contraindicated in patients with:
-
- •
- Significant respiratory depression
- •
- Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment
- •
- Known or suspected gastrointestinal obstruction, including paralytic ileus
- •
- Hypersensitivity to methadone hydrochloride (e.g. anaphylaxis) or any other ingredient in Methadone Hydrochloride Injection.
-
WARNINGS
Addiction, Abuse and Misuse
Methadone Hydrochloride Injection contains methadone, a Schedule II controlled substance. As an opioid, Methadone Hydrochloride Injection exposes users to the risks of addiction, abuse, and misuse.
Although the risk of addiction in any individual is unknown, it can occur in patients appropriately prescribed Methadone Hydrochloride Injection. Addiction can occur at recommended doses and if the drug is misused or abused.
Assess each patient’s risk for opioid addiction, abuse, or misuse prior to prescribing Methadone Hydrochloride Injection, and reassess all patients receiving Methadone Hydrochloride Injection for the development of these behaviors and conditions. Risks are increased in patients with a personal or family history of substance abuse (including drug or alcohol addiction or abuse) or mental illness (e.g., major depression). The potential for these risks should not, however, prevent the prescribing of Methadone Hydrochloride Injection for the proper management of pain in any given patient.
Opioids are sought for nonmedical use and are subject to diversion from legitimate prescribed use. Consider these risks when prescribing or dispensing Methadone Hydrochloride Injection. Strategies to reduce these risks include proper product storage and control practices for a C-II drug. Contact local state professional licensing board or state-controlled substances authority for information on how to prevent and detect abuse or diversion of this product.
Life-Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression has been reported with the use of opioids, even when used as recommended. Respiratory depression, if not immediately recognized and treated, may lead to respiratory depression and death. Management of respiratory depression may include close observation, supportive measures, and use of opioid antagonists, depending on the patient’s clinical status. Carbon dioxide (CO2) retention from opioid-induced respiratory depression can exacerbate the sedating effects of opioids.
While serious, life-threatening, or fatal respiratory depression can occur at any time during the use of Methadone Hydrochloride Injection, the risk is greatest during the initiation of therapy or following a dosage increase.
To reduce the risk of respiratory depression, proper dosing and titration of Methadone Hydrochloride Injection are essential. Overestimating the Methadone Hydrochloride Injection dosage when converting patients from another opioid product can result in a fatal overdose with the first dose.
Methadone Hydrochloride Injection should be administered with extreme caution to patients with conditions accompanied by hypoxia, hypercapnia, or decreased respiratory reserve such as; asthma, chronic obstructive pulmonary disease or cor pulmonale, severe obesity, sleep apnea syndrome, myxedema, kyphoscoliosis, CNS depression or coma. In these patients even usual therapeutic doses of methadone may decrease respiratory drive while simultaneously increasing airway resistance to the point of apnea. Alternative non-opioid analgesics should be considered, and methadone should be employed only under careful medical supervision at the lowest effective dose.
Methadone's peak respiratory depressant effects typically occur later, and persist longer than its peak analgesic effects, in the short-term use setting. These characteristics can contribute to cases of iatrogenic overdose, particularly during treatment initiation and dose titration.
Opioids can cause sleep-related breathing disorders including central sleep apnea (CSA) and sleep-related hypoxemia. Opioid use increases the risk of CSA in a dose-dependent fashion. In patients who present with CSA, consider decreasing the opioid dosage using best practices for opioid taper (see DOSAGE AND ADMINISTRATION).
Life-Threatening QT Prolongation
Cases of QT interval prolongation and serious arrhythmia (torsades de pointes) have been observed during treatment with methadone. These cases appear to be more commonly associated with, but not limited to, higher dose treatment (> 200 mg/day). Most cases involve patients being treated for pain with large, multiple daily doses of methadone, although cases have been reported in patients receiving doses commonly used for maintenance treatment of opioid addiction. In most patients on the lower doses typically used for maintenance, concomitant medications and/or clinical conditions such as hypokalemia were noted as contributing factors. However, the evidence strongly suggests that methadone possesses the potential for adverse cardiac conduction effects in some patients. The effects of methadone on the QT interval have been confirmed in in vivo laboratory studies, and methadone has been shown to inhibit cardiac potassium channels in in vitro studies.
Closely monitor patients with risk factors for development of prolonged QT interval (e.g., cardiac hypertrophy, concomitant diuretic use, hypokalemia and hypomagnesemia), a history of cardiac conduction abnormalities, and those taking medications affecting cardiac conduction. QT prolongation has also been reported in patients with no prior cardiac history who have received high doses of methadone.
Evaluate patients developing QT prolongation while on methadone treatment for the presence of modifiable risk factors, such as concomitant medications with cardiac effects, drugs that might cause electrolyte abnormalities, and drugs that might act as inhibitors of methadone metabolism.
Only initiate methadone hydrochloride tablets therapy for pain in patients for whom the anticipated benefit outweighs the risk of QT prolongation and development of dysrhythmias that have been reported with high doses of methadone.
The use of methadone in patients already known to have a prolonged QT interval has not been systematically studied.
Risks from Concomitant Use with Benzodiazepines or Other CNS Depressants
Profound sedation, respiratory depression, coma, and death may result from the concomitant use of Methadone Hydrochloride Injection with benzodiazepines or other CNS depressants, including alcohol (e.g., non-benzodiazepine sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, other opioids). Because of these risks, reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate.
Observational studies have demonstrated that concomitant use of opioid analgesics and benzodiazepines increases the risk of drug-related mortality compared to use of opioid analgesics alone. Because of similar pharmacological properties, it is reasonable to expect similar risk with the concomitant use of other CNS depressant drugs with opioid analgesics (see PRECAUTIONS: Drug Interactions).
If the decision is made to prescribe a benzodiazepine or other CNS depressant concomitantly with an opioid analgesic, prescribe the lowest effective dosages and minimum durations of concomitant use. In patients already receiving an opioid analgesic, prescribe a lower initial dose of the benzodiazepine or other CNS depressant than indicated in the absence of an opioid, and titrate based on clinical response. If an opioid analgesic is initiated in a patient already taking a benzodiazepine or other CNS depressant, prescribe a lower initial dose of the opioid analgesic, and titrate based on clinical response. Follow patients closely for signs and symptoms of respiratory depression and sedation.
Neonatal Opioid Withdrawal Syndrome
Neonatal opioid withdrawal syndrome (NOWS) is an expected and treatable outcome of prolonged use of opioids during pregnancy, whether that use is medically-authorized or illicit. Unlike opioid withdrawal syndrome in adults, NOWS may be life-threatening if not recognized and treated in the neonate. Advise the patient of the risk of NOWS so that appropriate planning for management of the neonate can occur. Healthcare professionals should observe newborns for signs of NOWS and manage accordingly (see PRECAUTIONS: Pregnancy).
The balance between the risks of NOWS and the benefits of maternal Methadone Hydrochloride Injection use may differ based on the risks associated with the mother’s underlying condition, pain or addiction, and the risks of the alternative treatments.
- •
- For management of pain, prescribers should discuss all available treatment options with females of reproductive potential, including non-opioid and non-pharmacologic options.
- •
- Untreated opioid addiction often results in continued or relapsing illicit opioid use and is associated with poor pregnancy outcomes. NOWS can result from in utero exposure to opioids regardless of the source. Therefore, prescribers should discuss the importance and benefits of management of opioid addiction throughout pregnancy.
Risks of Concomitant Use of Cytochrome P450 3A4, 2B6, 2C19, 2C9, or 2D6 Inhibitors or Discontinuation P450 3A4, 2B6, 2C19, or 2C9 Inducers
Concomitant use of Methadone Hydrochloride Injection with CYP3A4, CYP2B6, CYP2C19, CYP2C9, or CYP2D6 inhibitors, may increase plasma concentrations of methadone, prolong opioid adverse reactions, and may cause potentially fatal respiratory depression, particularly when an inhibitor is added after a stable dose of Methadone Hydrochloride Injection is achieved. Similarly, discontinuation of concomitant CYP3A4, CYP2B6, CYP2C19, or CYP2C9 inducers in Methadone Hydrochloride Injection-treated patients may increase methadone plasma concentrations resulting in fatal respiratory depression. Consider dosage reduction of Methadone Hydrochloride Injection when using concomitant CYP3A4, CYP2B6, CYP2C19, CYP2C9 or CYP2D6 inhibitors or discontinuing CYP3A4, CYP2B6, CYP2C19, or CYP2C9 inducers in methadone-treated patients, and follow patients closely at frequent intervals for signs and symptoms of respiratory depression and sedation.
Addition of CYP3A4, CYP2B6, CYP2C19, or CYP2C9 inducers or discontinuation of a CYP3A4, CYP2B6, CYP2C19, CYP2C9, or CYP2D6 inhibitors in patients treated with Methadone Hydrochloride Injection may decrease methadone plasma concentrations, reducing efficacy and may lead to opioid withdrawal symptoms in patients physically dependent on methadone. When using Methadone Hydrochloride Injection with CYP3A4, CYP2B6, CYP2C19, or CYP2C9 inducers or discontinuing CYP3A4, CYP2B6, CYP2C19, CYP2C9, or CYP2D6 inhibitors, follow patients for signs or symptoms of opioid withdrawal and consider increasing the Methadone Hydrochloride Injection dosage as needed.
Opioid-Induced Hyperalgesia and Allodynia
Opioid-Induced Hyperalgesia (OIH) occurs when an opioid analgesic paradoxically causes an increase in pain, or an increase in sensitivity to pain. This condition differs from tolerance, which is the need for increasing doses of opioids to maintain a defined effect (see Dependence). Symptoms of OIH include (but may not be limited to) increased levels of pain upon opioid dosage increase, decreased levels of pain upon opioid dosage decrease, or pain from ordinarily non-painful stimuli (allodynia). These symptoms may suggest OIH only if there is no evidence of underlying disease progression, opioid tolerance, opioid withdrawal, or addictive behavior.
Cases of OIH have been reported, both with short-term and longer-term use of opioid analgesics. Though the mechanism of OIH is not fully understood, multiple biochemical pathways have been implicated. Medical literature suggests a strong biologic plausibility between opioid analgesics and OIH and allodynia. If a patient is suspected to be experiencing OIH, carefully consider appropriately decreasing the dose of the current opioid analgesic, or opioid rotation (safely switching the patient to a different opioid moiety) (see WARNINGS; DOSAGE AND ADMINISTRATION).
Serotonin Syndrome with Concomitant Use of Serotonergic Drugs
Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of methadone with serotonergic drugs. Serotonergic drugs include selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that affect the serotonergic neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), and drugs that impair metabolism of serotonin (including MAO inhibitors, both those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue) (see PRECAUTIONS: Drug Interactions). This may occur within the recommended dosage range.
Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, coma), autonomic instability (e.g., tachycardia, labile blood pressure, hyperthermia), neuromuscular aberrations (e.g., hyperreflexia, incoordination, rigidity), and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea) and can be fatal. The onset of symptoms generally occurs within several hours to a few days of concomitant use, but may occur later than that. Discontinue Methadone Hydrochloride Injection if serotonin syndrome is suspected.
Adrenal Insufficiency
Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Presentation of adrenal insufficiency may include non-specific symptoms and signs including nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. If adrenal insufficiency is suspected, confirm the diagnosis with diagnostic testing as soon as possible. If adrenal insufficiency is diagnosed, treat with physiologic replacement doses of corticosteroids. Wean the patient off of the opioid to allow adrenal function to recover and continue corticosteroid treatment until adrenal function recovers. Other opioids may be tried as some cases reported use of a different opioid without recurrence of adrenal insufficiency. The information available does not identify any particular opioids as being more likely to be associated with adrenal insufficiency.
Severe Hypotension
Methadone Hydrochloride Injection may cause severe hypotension including orthostatic hypotension and syncope in ambulatory patients. There is increased risk in patients whose ability to maintain blood pressure has already been compromised by a reduced blood volume, or concurrent administration of certain CNS depressant drugs (e.g., phenothiazines or general anesthetics). Monitor these patients for signs of hypotension after initiating or titrating the dosage of Methadone Hydrochloride Injection. In patients with circulatory shock, Methadone Hydrochloride Injection may cause vasodilation that can further reduce cardiac output and blood pressure. Avoid the use of Methadone Hydrochloride Injection in patients with circulatory shock.
Risks of Use in Patients with Increased Intracranial Pressure, Brain Tumors, Head Injury, or Impaired Consciousness
In patients who may be susceptible to the intracranial effects of CO2 retention (e.g., those with evidence of increased intracranial pressure or brain tumors), Methadone Hydrochloride Injection may reduce respiratory drive, and the resultant CO2 retention can further increase intracranial pressure. Monitor such patients for signs of sedation and respiratory depression, particularly when initiating therapy with Methadone Hydrochloride Injection.
Opioids may also obscure the clinical course in a patient with a head injury.
Avoid the use of Methadone Hydrochloride Injection in patients with impaired consciousness or coma.
Risks of Use in Patients with Gastrointestinal Conditions
Methadone Hydrochloride Injection is contraindicated in patients with known or suspected gastrointestinal obstruction, including paralytic ileus.
The methadone in Methadone Hydrochloride Injection may cause spasm of the sphincter of Oddi. Opioids may cause increases in the serum amylase. Monitor patients with biliary tract disease, including acute pancreatitis, for worsening symptoms.
Increased Risk of Seizures in Patients with Seizure Disorders
The methadone in Methadone Hydrochloride Injection may increase the frequency of seizures in patients with seizure disorders, and may increase the risk of seizures in other clinical settings associated with seizures. Monitor patients with a history of seizure disorders for worsened seizure control during Methadone Hydrochloride Injection therapy.
Withdrawal
Avoid the use of mixed agonist/antagonist (i.e., pentazocine, nalbuphine, and butorphanol) or partial agonist (e.g., buprenorphine) analgesics in patients who are receiving a full opioid agonist, including Methadone Hydrochloride Injection. In these patients, mixed agonists/antagonist and partial agonist analgesics may reduce the analgesic effect and/or may precipitate withdrawal symptoms (see PRECAUTIONS: Drug Interactions).
When discontinuing Methadone Hydrochloride Injection, gradually taper the dosage (see DOSAGE AND ADMINISTRATION). Do not abruptly discontinue Methadone Hydrochloride Injection (see DRUG ABUSE AND DEPENDENCE).
Risks Driving and Operating Machinery
Methadone Hydrochloride Injection may impair the mental or physical abilities needed to perform potentially hazardous activities such as driving a car or operating machinery. Warn patients not to drive or operate dangerous machinery unless they are tolerant to the effects of Methadone Hydrochloride Injection and know how they will react to the medication (see PRECAUTIONS: Information for Patients).
Hypoglycemia
Cases of methadone-associated hypoglycemia have been reported, some resulting in hospitalization. In many cases, patients had predisposing risk factors (e.g., diabetes). The relationship between methadone and hypoglycemia is not fully understood but may be dose dependent. If hypoglycemia is suspected, monitor blood glucose levels, and manage the patient as clinically appropriate.
-
PRECAUTIONS
General
Methadone given on a fixed-dose schedule may have a narrow therapeutic index in certain patient populations, especially when combined with other drugs, and should be reserved for cases where the benefits of opioid analgesia outweigh the known potential risks of cardiac conduction abnormalities, respiratory depression, altered mental states and postural hypotension. Methadone Hydrochloride Injection should be used with caution in elderly and debilitated patients; patients who are known to be sensitive to central nervous system depressants, such as those with cardiovascular, pulmonary, renal, or hepatic disease; and in patients with comorbid conditions or concomitant medications which may predispose to dysrhythmia.
Selection of patients for treatment with methadone should be governed by the same principles that apply to the use of other parenteral opioids (see INDICATIONS AND USAGE). Physicians should individualize treatment in every case (see DOSAGE AND ADMINISTRATION), taking into account the high degree of interpatient variability in response to and metabolism of methadone.
Information for Patients
Addiction, Abuse, and Misuse
Inform patients that the use of Methadone Hydrochloride Injection, even when taken as recommended, can result in addiction, abuse, and misuse, which can lead to overdose or death (see WARNINGS).
Life-Threatening Respiratory Depression
Inform patients of the risk of life-threatening respiratory depression, including information that the risk is greatest when starting Methadone Hydrochloride Injection or when the dosage is increased, and that it can occur even at recommended dosages (see WARNINGS). Advise patients how to recognize respiratory depression and to seek medical attention if breathing difficulties develop.
Symptoms of Arrhythmia
Instruct patients to seek medical attention immediately if they experience symptoms suggestive of an arrhythmia (such as palpitations, near syncope, or syncope) when taking methadone (see WARNINGS).
Interactions with Benzodiazepines and Other CNS Depressants
Inform patients and caregivers that potentially fatal additive effects may occur if Methadone Hydrochloride Injection are used with benzodiazepines or other CNS depressants, including alcohol, and not to use these concomitantly unless supervised by a health care provider (see WARNINGS, PRECAUTIONS: Drug Interactions).
Hyperalgesia and Allodynia
Advise patients to inform their healthcare provider if they experience symptoms of hyperalgesia, including worsening pain, increased sensitivity to pain, or new pain (see WARNINGS; ADVERSE REACTIONS).
Serotonin Syndrome
Inform patients that opioids could cause a rare but potentially life-threatening condition called serotonin syndrome resulting from concomitant administration of serotonergic drugs. Warn patients of the symptoms of serotonin syndrome and to seek medical attention right away if symptoms develop. Instruct patients to inform their physicians if they are taking, or plan to take serotonergic medications (see WARNINGS, PRECAUTIONS: Drug Interactions).
MAOI Interaction
Inform patients to avoid taking Methadone Hydrochloride Injection while using any drugs that inhibit monoamine oxidase. Patients should not start MAOIs while taking Methadone Hydrochloride Injection (see PRECAUTIONS: Drug Interactions).
Adrenal Insufficiency
Inform patients that opioids could cause adrenal insufficiency, a potentially life-threatening condition. Adrenal insufficiency may present with non-specific symptoms and signs such as nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. Advise patients to seek medical attention if they experience a constellation of these symptoms (see WARNINGS).
Hypotension
Inform patients that Methadone Hydrochloride Injection may cause orthostatic hypotension and syncope. Instruct patients how to recognize symptoms of low blood pressure and how to reduce the risk of serious consequences should hypotension occur (e.g., sit or lie down, carefully rise from a sitting or lying position) (see WARNINGS).
Anaphylaxis
Inform patients that anaphylaxis has been reported with ingredients contained Methadone Hydrochloride Injection. Advise patients how to recognize such a reaction and when to seek medical attention (see CONTRAINDICATIONS, ADVERSE REACTIONS).
Pregnancy
Neonatal Opioid Withdrawal Syndrome
Advise women that if they are pregnant while being treated with Methadone Hydrochloride Injection, the baby may have signs of withdrawal at birth and that withdrawal is treatable (see BOXED WARNING, WARNINGS: Neonatal Opioid Withdrawal Syndrome, PRECAUTIONS: Pregnancy)
Embryo-Fetal Toxicity
Inform female patients of reproductive potential that Methadone Hydrochloride Injection can cause fetal harm and to inform their healthcare provider of a known or suspected pregnancy (see PRECAUTIONS: Pregnancy).
Lactation
Advise women who are breastfeeding to monitor the infant for increased sleepiness (more than usual), difficulty breathing or limpness. Instruct nursing mothers using Methadone Hydrochloride Injection to watch for signs of methadone toxicity in their infants, which include increased sleepiness (more than usual), difficulty breastfeeding, breathing difficulties, or limpness. Instruct nursing mothers to talk to the baby’s healthcare provider immediately if they notice these signs. If they cannot reach the healthcare provider right away, instruct them to take the baby to the emergency room or call 911 (or local emergency services) (see PRECAUTIONS: Lactation).
Infertility
Advise patients that chronic use of opioids, such as Methadone Hydrochloride Injection, may cause reduced fertility. It is not known whether these effects on fertility are reversible (see PRECAUTIONS: Females and Males of Reproductive Potential).
Driving or Operating Heavy Machinery
Inform patients that Methadone Hydrochloride Injection may impair the ability to perform potentially hazardous activities such as driving a car or operating heavy machinery. Advise patients not to perform such tasks until they know how they will react to the medication (see WARNINGS).
Constipation
Advise patients of the potential for severe constipation, including management instructions and when to seek medical attention (see CLINICAL PHARMACOLOGY: Pharmacodynamics, ADVERSE REACTIONS).
Hypoglycemia
Inform patients that methadone may cause hypoglycemia. Instruct patients how to recognize the symptoms of low blood glucose and to contact their health care provider if these symptoms occur (see WARNINGS).
Drug Interactions
Inhibitors of CYP3A4, CYP2B6, CYP2C19, CYP2C9, or CYP2D6
Clinical Impact:
Methadone undergoes hepatic N-demethylation by several cytochrome P450 (CYP) isoforms, including CYP3A4, CYP2B6, CYP2C19, CYP2C9, and CYP2D6. The concomitant use of Methadone Hydrochloride Injection and CYP3A4, CYP2B6, CYP2C19, CYP2C9, or CYP2D6 inhibitors can increase the plasma concentration of methadone, resulting in increased or prolonged opioid effects, and may result in a fatal overdose, particularly when an inhibitor is added after a stable dose of Methadone Hydrochloride Injection is achieved. These effects may be more pronounced with concomitant use of drugs that inhibit more than one of the CYP enzymes listed above.
After stopping a CYP3A4, CYP2B6, CYP2C19, CYP2C9, or CYP2D6 inhibitor, as the effects of the inhibitor decline, the methadone plasma concentration can decrease (see CLINICAL PHARMACOLOGY), resulting in decreased opioid efficacy or withdrawal symptoms in patients physically dependent on methadone.
Intervention:
If concomitant use is necessary, consider dosage reduction of Methadone Hydrochloride Injection until stable drug effects are achieved. Monitor patients for respiratory depression and sedation at frequent intervals.
If a CYP3A4, CYP2B6, CYP2C19, CYP2C9, or CYP2D6 inhibitor is discontinued, follow patients for signs of opioid withdrawal and consider increasing the Methadone Hydrochloride Injection dosage until stable drug effects are achieved.
Examples:
Macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), protease inhibitors (e.g., ritonavir), fluconazole, fluvoxamine, Some selective serotonin reuptake inhibitors (SSRIs) (e.g., sertraline, fluvoxamine)
Inducers of CYP3A4, CYP2B6, CYP2C19, or CYP2C9
Clinical Impact:
The concomitant use of Methadone Hydrochloride Injection and CYP3A4, CYP2B6, CYP2C19, or CYP2C9 inducers can decrease the plasma concentration of methadone (see CLINICAL PHARMACOLOGY), resulting in decreased efficacy or onset of withdrawal symptoms in patients physically dependent on methadone. These effects could be more pronounced with concomitant use of drugs that can induce multiple CYP enzymes.
After stopping a CYP3A4, CYP2B6, CYP2C19, or CYP2C9 inducer, as the effects of the inducer decline, the methadone plasma concentration can increase (see CLINICAL PHARMACOLOGY), which could increase or prolong both the therapeutic effects and adverse reactions, and may cause serious respiratory depression, sedation, or death.
Intervention:
If concomitant use is necessary, consider increasing the Methadone Hydrochloride Injection dosage until stable drug effects are achieved. Monitor for signs of opioid withdrawal. If a CYP3A4, CYP2B6, CYP2C19, or CYP2C9 inducer is discontinued, consider Methadone Hydrochloride Injection dosage reduction and monitor for signs of respiratory depression and sedation.
Examples:
Rifampin, carbamazepine, phenytoin, St. John’s Wort, Phenobarbital
Benzodiazepines and other Central Nervous System (CNS) Depressants
Clinical Impact:
Due to additive pharmacologic effect, the concomitant use of benzodiazepines or other CNS depressants including alcohol, increases the risk of respiratory depression, profound sedation, coma, and death.
Intervention:
Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Follow patients closely for signs of respiratory depression and sedation (see WARNINGS, PRECAUTIONS).
Examples:
Benzodiazepines and other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, other opioids, alcohol.
Potentially Arrhythmogenic Agents
Clinical Impact:
Pharmacodynamic interactions may occur with concomitant use of methadone and potentially arrhythmogenic agents or drugs capable of inducing electrolyte disturbances (hypomagnesemia, hypokalemia).
Intervention:
Monitor patients closely for cardiac conduction changes.
Examples:
Drugs known to have potential to prolong QT interval: Class I and III antiarrhythmics, some neuroleptics and tricyclic antidepressants, and calcium channel blockers. Drugs capable of inducing electrolyte disturbances: Diuretics, laxatives, and, in rare cases, mineralocortocoid hormones.
Serotonergic Drugs
Clinical Impact:
The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome (see WARNINGS, PRECAUTIONS).
Intervention:
If concomitant use is warranted, carefully observe the patient, particularly during treatment initiation and dose adjustment. Discontinue Methadone Hydrochloride Injection if serotonin syndrome is suspected.
Examples:
Selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that effect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), monoamine oxidase (MAO) inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue).
Monoamine Oxidase Inhibitors (MAOIs)
Clinical Impact:
MAOI interactions with opioids may manifest as serotonin syndrome (see PRECAUTIONS) or opioid toxicity (e.g., respiratory depression, coma) (see PRECAUTIONS).
Intervention:
The use of Methadone Hydrochloride Injection is not recommended for patients taking MAOIs or within 14 days of stopping such treatment.
Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics
Clinical Impact:
May reduce the analgesic effect of Methadone Hydrochloride Injection and/or precipitate withdrawal symptoms.
Intervention:
Avoid concomitant use.
Examples:
butorphanol, nalbuphine, pentazocine, buprenorphine
Muscle Relaxants
Clinical Impact:
Methadone may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression.
Intervention:
Monitor patients for signs of respiratory depression that may be greater than otherwise expected and decrease the dosage of Methadone Hydrochloride Injection and/or the muscle relaxant as necessary.
Diuretics
Clinical Impact:
Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone.
Intervention:
Monitor patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed.
Anticholinergic Drugs
Clinical Impact:
The concomitant use of anticholinergic drugs may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus.
Intervention:
Monitor patients for signs of urinary retention or reduced gastric motility when Methadone Hydrochloride Injection is used concomitantly with anticholinergic drugs.
Anti-Retroviral Agents
Nevirapine
Based on the known metabolism of methadone, nevirapine may decrease plasma concentrations of methadone by increasing its hepatic metabolism. Opioid withdrawal syndrome has been reported in patients treated with nevirapine and methadone concomitantly. Methadone-maintained patients beginning nevirapine therapy should be monitored for evidence of withdrawal and methadone dose should be adjusted accordingly.
Efavirenz
Coadministration of efavirenz in HIV-infected methadone-maintenance patients has resulted in decreased methadone plasma concentrations of methadone associated with signs of opioid withdrawal, and necessitating increases in methadone dose.
Ritonavir and Ritonavir/Lopinavir
Reduced plasma methadone levels have been observed after administration of ritonavir alone or ritonavir/lopinavir combination. Withdrawal symptoms were however, inconsistently observed. Caution is warranted when administering methadone to patients receiving ritonavir-containing regimens in addition to other drugs known to decrease methadone plasma levels.
Zidovudine
Experimental evidence suggests that methadone increases the area under the concentration-time curve (AUC) of zidovudine with possible toxic effects.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Data from published reports of carcinogenicity studies indicate that there was a significant increase in pituitary adenomas in female B6C2F1 mice consuming 15 mg/kg/day methadone for two years. This dose was approximately 0.6 times a human daily oral dose of 120 mg/day, on a body surface area basis (HDD). However, this finding was not seen in mice consuming 60 mg/kg/day (approximately 2.5 times the HDD). Furthermore, in a two-year study of dietary administration of methadone to Fischer 344 rats, there was no clear evidence for treatment related increase in the incidence of neoplasms, at doses as high as 28 mg/kg/day in males and 88 mg/kg/day in females (approximately 2.3 times and 7.1 times, respectively, the HDD).
Mutagenesis
In published reports, methadone tested negative in tests for chromosome breakage and disjunction and sex-linked recessive lethal gene mutations in germ cells of Drosophila using feeding and injection procedures. Methadone treatment of male mice increased sex chromosome and autosome univalent chromosomes and translocations in multivalent chromosomes. Methadone tested positive in the E.coli DNA repair system and Neurospora crassa and mouse lymphoma forward mutation assays.
Impairment of Fertility
Published animal studies show that methadone treatment of males can alter reproductive function. Methadone produces decreased sexual activity (mating) of male rats at 10 mg/kg/day (corresponding to 0.3 times the human daily oral dose of 120 mg/day based on body surface area). Methadone also produces a significant regression of sex accessory organs and testes of male mice and rats at 0.2 and 0.8 times the HDD, respectively. Decreased serum levels of testosterone were observed in male rats that were treated with methadone (1.3 mg/kg/day to 3.3 mg/kg/day for 14 days, corresponding to 0.1 to 0.3 times the HDD) or 10 mg/kg/day to 15 mg/kg/day for 10 days (0.8 to 1.2 times the HDD).
Pregnancy
Risk Summary
The majority of available data from clinical trials, observational studies, case series, and case reports on methadone use in pregnancy do not indicate an increased risk of major malformations specifically due to methadone.
Pregnant women involved in methadone maintenance programs have been reported to have improved prenatal care leading to reduced incidence of obstetric and fetal complications and neonatal morbidity and mortality when compared to women using illicit drugs. Several factors, including maternal use of illicit drugs, nutrition, infection and psychosocial circumstances, complicate the interpretation of investigations of the children of women who take methadone during pregnancy. Information is limited regarding dose and duration of methadone use during pregnancy, and most maternal exposure in these studies appears to occur after the first trimester of pregnancy (see Data).
Neonatal opioid withdrawal syndrome (NOWS) is an expected and treatable outcome of prolonged use of opioids during pregnancy (see WARNINGS, PRECAUTIONS).
In published animal reproduction studies, methadone administered subcutaneously during the early gestational period produced neural tube defects (i.e., exencephaly and cranioschisis) in the hamster at doses 2 times the human daily oral dose of 120 mg/day on a mg/m2 basis (HDD) and in mice at doses equivalent to the HDD. Administration of methadone to pregnant animals during organogenesis and through lactation resulted decreased litter size, increased pup mortality, decreased pup body weights, developmental delays, and long-term neurochemical changes in the brain of offspring which correlate with altered behavioral responses that persist through adulthood at exposures comparable to and less than the HDD. Administration of methadone to male rodents prior to mating with untreated females resulted in increased neonatal mortality and significant differences in behavioral tests in the offspring at exposures comparable to and less than the HDD (see Data). Based on animal data, advise pregnant women of the potential risk to a fetus.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations
Disease-associated Maternal and Embryo-fetal risk
Untreated opioid addiction in pregnancy is associated with adverse obstetrical outcomes such as low birth weight, preterm birth, and fetal death. In addition, untreated opioid addiction often results in continued or relapsing illicit opioid use.
Dosage Adjustment During Pregnancy
Dosage adjustment using higher doses or administering the daily dose in divided doses may be necessary in pregnant women treated with Methadone Hydrochloride Injection. Pregnant women appear to have significantly lower trough plasma methadone concentrations, increased plasma methadone clearance, and shorter methadone half-life than after delivery (see DOSAGE AND ADMINISTRATION and CLINICAL PHARMACOLOGY). Withdrawal signs and symptoms should be closely monitored and the dose adjusted as necessary.
Fetal/Neonatal Adverse Reactions
Neonatal opioid withdrawal syndrome may occur in newborn infants of mothers who are receiving treatment with Methadone Hydrochloride Injection.
Neonatal opioid withdrawal syndrome presents as irritability, hyperactivity and abnormal sleep pattern, high pitched cry, tremor, vomiting, diarrhea, and/or failure to gain weight. Signs of neonatal withdrawal usually occur in the first days after birth. The duration and severity of neonatal opioid withdrawal syndrome may vary. Observe newborns for signs of neonatal opioid withdrawal syndrome and manage accordingly (see BOXED WARNING, WARNINGS: Neonatal Opioid Withdrawal Syndrome).
Data
Human Data
The majority of available data from clinical trials, observational studies, case series, and case reports on methadone use in pregnancy do not indicate an increased risk of major malformations specifically due to methadone. Findings regarding specific major malformations, decreased fetal growth, premature birth and Sudden Infant Death Syndrome have been inconsistent. Children prenatally exposed to methadone have been reported to demonstrate mild but persistent deficits in performance on psychometric and behavioral tests and visual abnormalities.
In a multicenter, double-blind, randomized, controlled trial [Maternal Opioid Treatment: Human Experimental Research (MOTHER)] designed primarily to assess neonatal opioid withdrawal effects, opioid-dependent pregnant women were randomized to buprenorphine (n = 86) or methadone (n = 89) treatment, with enrollment at an average gestational age of 18.7 weeks in both groups. A total of 28 of the 86 women in the buprenorphine group (33%) and 16 of the 89 women in the methadone group (18%) discontinued treatment before the end of pregnancy.
Among women who remained in treatment until delivery, there was no difference between methadone-treated and buprenorphine-treated groups in the number of neonates requiring NOWS treatment or in the peak severity of NOWS. Buprenorphine-exposed neonates required less morphine (mean total dose, 1.1 mg vs. 10.4 mg), had shorter hospital stays (10.0 days vs. 17.5 days), and shorter duration of treatment for NOWS (4.1 days vs. 9.9 days) compared to the methadone-exposed group. There were no differences between groups in other primary outcomes (neonatal head circumference) or secondary outcomes (weight and length at birth, preterm birth, gestational age at delivery, and 1-minute and 5-minute Apgar scores), or in the rates of maternal or neonatal adverse events. The outcomes among mothers who discontinued treatment before delivery and may have relapsed to illicit opioid use are not known. Because of the imbalance in discontinuation rates between the methadone and buprenorphine groups, the study findings are difficult to interpret.
Animal Data
Formal reproductive and developmental toxicology studies for methadone have not been conducted. Exposure margins for the following published study reports are based on a human daily dose (HDD) of 120 mg methadone using a body surface area comparison.
In a published study in pregnant hamsters, a single subcutaneous dose of methadone ranging from 31 mg/kg (2 times the HDD) to 185 mg/kg on Gestation Day 8 resulted in a decrease in the number of fetuses per litter and an increase in the percentage of fetuses exhibiting neural tube defects including exencephaly, cranioschisis, and “various other lesions.” The majority of the doses tested also resulted in maternal death. In a study in pregnant JBT/Jd mice, a single subcutaneous dose of 22 to 24 mg/kg methadone (approximately equivalent to the HDD) administered on Gestation Day 9 produced exencephaly in 11% of the embryos. In another study in pregnant mice, subcutaneous doses up to 28 mg/kg/day methadone (equivalent to the HDD) administered from Gestation Day 6 to 15 resulted in no malformations, but there were increased post-implantation loss and decreased live fetuses at 10 mg/kg/day or greater (0.4 times the HDD) and decreased ossification and fetal body weight at 20 mg/kg/day or greater (0.8 times the HDD). In a second study of pregnant mice dosed with subcutaneous doses up to 28 mg/kg/day methadone from Gestation Day 6 to 15, there was decreased pup viability, delayed onset of development of negative phototaxis and eye opening, increased righting reflexes at 5 mg/kg/day or greater (0.2 times the HDD), and decreased number of live pups at birth and decreased pup weight gain at 20 mg/kg/day or greater (0.8 times the HDD).
No effects were reported in a study of pregnant rats and rabbits at oral doses up to 40 mg/kg (3 and 6 times, respectively, the HDD) administered from Gestation Days 6 to 15 and 6 to 18, respectively.
When pregnant rats were treated with intraperitoneal doses of 2.5, 5, or 7.5 mg/kg methadone from one week prior to mating, through gestation until the end of lactation period, 5 mg/kg or greater (0.4 times the HDD) methadone resulted in decreases in litter size and live pups born and 7.5 mg/kg (0.6 times the HDD) resulted in decreased birth weights. Furthermore, decreased pup viability and pup body weight gain at 2.5 mg/kg or greater (0.2 times the HDD) were noted during the preweaning period.
Additional animal data demonstrate evidence for neurochemical changes in the brains of offspring from methadone-treated pregnant rats, including changes to the cholinergic, dopaminergic, noradrenergic and serotonergic systems at doses below the HDD. Other animal studies have reported that prenatal and/or postnatal exposure to opioids including methadone alters neuronal development and behavior in the offspring including alterations in learning ability, motor activity, thermal regulation, nociceptive responses, and sensitivity to drugs at doses below the HDD. Treatment of pregnant rats subcutaneously with 5 mg/kg methadone from Gestation Day 14 to 19 (0.4 times the HDD) reduced fetal blood testosterone and androstenedione in males.
Published animal data have reported increased neonatal mortality in the offspring of male rodents that were treated with methadone at doses comparable to and less than the HDD for 1 to 12 days before and/or during mating (with more pronounced effects in the first 4 days). In these studies, the female rodents were not treated with methadone, indicating paternally-mediated developmental toxicity. Specifically, methadone administered to the male rat prior to mating with methadone-naïve females resulted in decreased weight gain in progeny after weaning. The male progeny demonstrated reduced thymus weights, whereas the female progeny demonstrated increased adrenal weights. Behavioral testing of these male and female progeny revealed significant differences in behavioral tests compared to control animals, suggesting that paternal methadone exposure can produce physiological and behavioral changes in progeny in this model. Examination of uterine contents of methadone-naïve female mice bred to methadone-treated male mice (once a day for three consecutive days) indicated that methadone treatment produced an increase in the rate of preimplantation deaths in all post-meiotic states at 1 mg/kg/day or greater (0.04 times the HDD). Chromosome analysis revealed a dose-dependent increase in the frequency of chromosomal abnormalities at 1 mg/kg/day or greater.
Studies demonstrated that methadone treatment of male rats for 21 to 32 days prior to mating with methadone-naïve females did not produce any adverse effects, suggesting that prolonged methadone treatment of the male rat resulted in tolerance to the developmental toxicities noted in the progeny. Mechanistic studies in this rat model suggest that the developmental effects of “paternal” methadone on the progeny appear to be due to decreased testosterone production. These animal data mirror the reported clinical findings of decreased testosterone levels in human males on methadone maintenance therapy for opioid addiction and in males receiving chronic intraspinal opioids.
Lactation
Risk Summary
Based on two small clinical studies, methadone was present in low levels in human milk, but the exposed infants in these studies did not show adverse reactions. Based on an average milk consumption of 150 mL/kg/day, an infant would consume approximately 17.4 mcg/kg/day which is approximately 2 to 3% of the oral maternal dose. There have been rare case reports of sedation and respiratory depression in infants exposed to methadone through breast milk (see Data). Monitor infants exposed to Methadone Hydrochloride Injection through breast milk for excess sedation and respiratory depression. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for methadone and any potential adverse effects on the breastfed child from the drug or from the underlying maternal condition.
Data
In a study of ten breastfeeding women maintained on oral methadone doses of 10 to 80 mg/day, methadone concentrations from 50 to 570 mcg/L in milk were reported, which, in the majority of samples, were lower than maternal serum drug concentrations at steady state. Peak methadone levels in milk occur approximately 4 to 5 hours after an oral dose.
In a study of twelve breastfeeding women maintained on oral methadone doses of 20 to 80 mg/day, methadone concentrations from 39 to 232 mcg/L in milk were reported. Based on an average milk consumption of 150 mL/kg/day, an infant would consume approximately 17.4 mcg/kg/day, which is approximately 2 to 3% of the oral maternal dose. Methadone has been detected in very low plasma concentrations in some infants whose mothers were taking methadone.
Females and Males of Reproductive Potential
Infertility
The effect of Methadone Hydrochloride Injection on fertility is unknown. Use of opioids for an extended period of time may cause reduced fertility in females and males of reproductive potential. It is not known whether these effects on fertility are reversible (see ADVERSE REACTIONS, CLINICAL PHARMACOLOGY). Reproductive function in human males may be decreased by methadone treatment. Reductions in ejaculate volume and seminal vesicle and prostate secretions have been reported in methadone-treated individuals. In addition, reductions in serum testosterone levels and sperm motility, and abnormalities in sperm morphology have been reported.
In published animal studies, methadone produces a significant regression of sex accessory organs and testes of male mice and rats and administration of methadone to pregnant rats reduced fetal blood testosterone and androstenedione in male offspring (see PRECAUTIONS: Carcinogenesis, Mutagenesis, Impairment of Fertility).
Pediatric Use
Safety and effectiveness in pediatric patients below the age of 18 years have not been established.
Geriatric Use
Clinical studies of Methadone Hydrochloride Injection did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients.
Elderly patients (aged 65 years or older) may have increased sensitivity to methadone. In general, use caution when selecting a dosage for an elderly patient, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
Respiratory depression is the chief risk for elderly patients treated with opioids, and has occurred after large initial doses were administered to patients who were not opioid-tolerant or when opioids were co-administered with other agents that depress respiration. Titrate the dosage of Methadone Hydrochloride Injection slowly in geriatric patients and monitor closely for signs of respiratory depression (see WARNINGS, PRECAUTIONS).
Methadone is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to regularly evaluate renal function.
Hepatic Impairment
Methadone has not been extensively evaluated in patients with hepatic insufficiency. Methadone is metabolized by hepatic pathways; therefore patients with liver impairment may be at risk of increased systemic exposure to methadone after multiple dosing. Start these patients on lower doses and titrate slowly while regularly evaluating for signs of respiratory and central nervous system depression.
Renal Impairment
The use of methadone has not been extensively evaluated in patients with renal insufficiency. Since unmetabolized methadone and its metabolites are excreted in urine to a variable degree, start these patients on lower doses and with longer dosing intervals and titrate slowly while regularly evaluating for signs of respiratory and central nervous system depression.
-
ADVERSE REACTIONS
The following serious adverse reactions are described, or described in greater detail, in other sections:
- •
- Addiction, Abuse, and Misuse (see WARNINGS)
- •
- Life Threatening Respiratory Depression (see WARNINGS)
- •
- QT Prolongation (see WARNINGS)
- •
- Neonatal Opioid Withdrawal Syndrome (see WARNINGS)
- •
- Interactions with CNS Depressants (see WARNINGS)
- •
- Serotonin Syndrome (see WARNINGS)
- •
- Adrenal Insufficiency (see WARNINGS)
- •
- Severe Hypotension (see WARNINGS)
- •
- Gastrointestinal Adverse Reactions (see WARNINGS)
- •
- Seizures (see WARNINGS)
- •
- Withdrawal (see WARNINGS)
- •
- Hypoglycemia (see WARNINGS)
The following adverse reactions associated with the use of methadone were identified in clinical studies or post-marketing reports. Because some of these reactions were reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
The major hazards of methadone are respiratory depression and, to a lesser degree, systemic hypotension. Respiratory arrest, shock, cardiac arrest, and death have occurred.
The most frequently observed adverse reactions include lightheadedness, dizziness, sedation, nausea, vomiting, and sweating. These effects seem to be more prominent in ambulatory patients and in those who are not suffering severe pain. In such individuals, lower doses of methadone are advisable. Other adverse reactions that have been reported in patients (including opioid addicts taking methadone for detoxification or maintenance) receiving methadone include the following:
Body as a Whole: asthenia (weakness), edema, headache
Cardiovascular: Arrhythmias, bigeminal rhythms, bradycardia, extrasystoles, tachycardia, Torsade de Pointes, ventricular fibrillation, ventricular tachycardia. ECG abnormalities, prolonged QT interval, T-wave inversion, cardiomyopathy, flushing, heart failure, hypotension, palpitations, phlebitis, syncope
Digestive: Abdominal pain, anorexia, biliary tract spasm, constipation, dry mouth, glossitis
Hematologic and Lymphatic: Reversible thrombocytopenia has been described in opioid addicts with chronic hepatitis.
Metabolic and Nutritional: Hypokalemia, hypomagnesemia, weight gain
Central Nervous System: Agitation, confusion, seizures, disorientation, dysphoria, euphoria, insomnia, hallucinations, seizures, visual disturbances, congenital oculomotor disorders (nystagmus, strabismus)
Respiratory: Pulmonary edema
Skin and Appendages: Intramuscular and Subcutaneous: Local tissue reactions (pain, erythema, swelling), particularly with continuous subcutaneous infusion
Intravenous: Pruritis, urticaria, other skin rashes, and rarely, hemorrhagic urticaria
Special Senses: Visual disturbances
Urogenital: Antidiuretic effect, amenorrhea, urinary retention or hesitancy, reduced libido and/or potency
Serotonin Syndrome: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs.
Adrenal Insufficiency: Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use.
Anaphylaxis: Anaphylaxis has been reported with ingredients contained in Methadone Hydrochloride Injection.
Androgen Deficiency: Cases of androgen deficiency have occurred with use of opioids for an extended period of time.
Hyperalgesia and Allodynia: Cases of hyperalgesia and allodynia have been reported with opioid therapy of any duration (see WARNINGS).
Hypoglycemia: Cases of hypoglycemia have been reported in patients taking methadone (see WARNINGS).
-
DRUG ABUSE AND DEPENDENCE
Controlled Substance
Methadone Hydrochloride Injection contains methadone, a Schedule II controlled substance.
Abuse
Methadone Hydrochloride Injection contains methadone, a substance with high potential for misuse and abuse, which can lead to the development of substance use disorder, including addiction (see WARNINGS).
Misuse is the intentional use, for therapeutic purposes, of a drug by an individual in a way other than prescribed by a healthcare provider or for whom it was not prescribed.
Abuse is the intentional, non-therapeutic use of a drug, even once, for its desirable psychological or physiological effects.
Drug addiction is a cluster of behavioral, cognitive, and physiological phenomena that may include a strong desire to take the drug, difficulties in controlling drug use (e.g., continuing drug use despite harmful consequences, giving a higher priority to drug use than other activities and obligations), and possible tolerance or physical dependence.
Misuse and abuse of Methadone Hydrochloride Injection increases risk of overdose, which may lead to central nervous system and respiratory depression, hypotension, seizures, and death. The risk is increased with concurrent abuse of Methadone Hydrochloride Injection with alcohol and/or other central nervous system depressants. Abuse of and addiction to opioids in some individuals may not be accompanied by concurrent tolerance and symptoms of physical dependence. In addition, abuse of opioids can occur in the absence of addiction.
All patients treated with opioids require careful and frequent reevaluation for signs of misuse, abuse, and addiction, because use of opioid analgesic products carries the risk of addiction even under appropriate medical use. Patients at high risk of Methadone Hydrochloride Injection abuse include those with a history of prolonged use of any opioid, including products containing methadone, those with a history of drug or alcohol abuse, or those who use Methadone Hydrochloride Injection in combination with other abused drugs.
“Drug-seeking” behavior is very common in persons with substance use disorders. Drug-seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing, or referral, repeated “loss” of prescriptions, tampering with prescriptions, and reluctance to provide prior medical records or contact information for other treating healthcare provider(s). “Doctor shopping” (visiting multiple prescribers to obtain additional prescriptions) is common among people who abuse drugs and people with substance use disorder. Preoccupation with achieving adequate pain relief can be appropriate behavior in a patient with inadequate pain control.
Methadone Hydrochloride Injection, like other opioids, can be diverted for nonmedical use into illicit channels of distribution. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests, as required by state and federal law, is strongly advised.
Proper assessment of the patient, proper prescribing practices, periodic reevaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
Risks Specific to Abuse of Methadone Hydrochloride Injection
Abuse of Methadone Hydrochloride Injection poses a risk of overdose and death. The risk is increased with concurrent use of Methadone Hydrochloride Injection with alcohol and/or other CNS depressants.
Parenteral drug abuse is commonly associated with transmission of infectious diseases such as hepatitis and HIV.
Dependence
Both tolerance and physical dependence can develop during use of opioid therapy.
Tolerance is a physiological state characterized by a reduced response to a drug after repeated administration (i.e., a higher dose of a drug is required to produce the same effect that was once obtained at a lower dose).
Physical dependence is a state that develops as a result of a physiological adaptation in response to repeated drug use, manifested by withdrawal signs and symptoms after abrupt discontinuation or a significant dose reduction of a drug.
Withdrawal may be precipitated through the administration of drugs with opioid antagonist activity (e.g., naloxone), mixed agonist/antagonist analgesics (e.g., pentazocine, butorphanol, nalbuphine), or partial agonists (e.g., buprenorphine). Physical dependence may not occur to a clinically significant degree until after several days to weeks of continued use.
Do not abruptly discontinue Methadone Hydrochloride Injection in a patient physically dependent on opioids. Rapid tapering of Methadone Hydrochloride Injection in a patient physically dependent on opioids may lead to serious withdrawal symptoms, uncontrolled pain, and suicide. Rapid discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse.
When discontinuing Methadone Hydrochloride Injection, gradually taper the dosage using a patient-specific plan that considers the following: the dose of Methadone Hydrochloride Injection the patient has been taking, the duration of treatment, and the physical and psychological attributes of the patient. To improve the likelihood of a successful taper and minimize withdrawal symptoms, it is important that the opioid tapering schedule is agreed upon by the patient. In patients taking opioids for an extended period of time at high doses, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper (see DOSAGE AND ADMINISTRATION, and WARNINGS).
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal signs (see PRECAUTIONS: Pregnancy).
-
OVERDOSAGE
Clinical Presentation
Acute overdosage with methadone can be manifested by respiratory depression, somnolence progressing to stupor or coma, skeletal-muscle flaccidity, cold and clammy skin, constricted pupils, and, in some cases, pulmonary edema, bradycardia, hypotension, hypoglycemia, partial or complete airway obstruction, atypical snoring, and death. Marked mydriasis rather than miosis may be seen with hypoxia in overdose situations (see CLINICAL PHARMACOLOGY). In severe overdosage, particularly by the intravenous route, apnea, circulatory collapse, cardiac arrest, and death may occur.
Methadone overdosage is associated with rhabdomyolysis. Seek medical attention, especially if abuse/misuse results in prolonged immobilization. Acute toxic leukoencephalopathy has been reported after methadone overdose, often weeks after apparent recovery from the initial intoxication. Hearing loss has been reported after methadone overdose, in some cases permanent.
Treatment of Overdose
In the case of overdose, priorities are the reestablishment of a patent and protected airway and institution of assisted or controlled ventilation, if needed. Employ other supportive measures (including oxygen and vasopressors) in the management of circulatory shock and pulmonary edema as indicated. Cardiac arrest or arrhythmias will require advanced life-support measures.
Opioid antagonists, such as naloxone, are specific antidotes to respiratory depression resulting from opioid overdose. For clinically significant respiratory or circulatory depression secondary to methadone overdose, administer an opioid antagonist.
The physician must remember that methadone is a long-acting depressant (36 to 48 hours), whereas the antagonists act for much shorter periods (one to three hours). Because the duration of opioid reversal is expected to be less than the duration of action of methadone in Methadone Hydrochloride Injection, carefully monitor the patient until spontaneous respiration is reliably reestablished. If the response to an opioid antagonist is suboptimal or only brief in nature, administer additional antagonist as directed by the product’s prescribing information.
In an individual physically dependent on opioids, the administration of the usual dose of an opioid antagonist will precipitate an acute withdrawal syndrome. The severity of the withdrawal symptoms experienced will depend on the degree of physical dependence and the dose of the antagonist administered. If a decision is made to treat serious respiratory depression in the physically dependent patient, administration of the antagonist should be initiated with care and by titration with smaller than usual doses of the antagonist.
-
DOSAGE AND ADMINISTRATION
Important General Information
Consider the following important factors that differentiate methadone from other opioids:
- •
- The peak respiratory depressant effect of methadone occurs later and persists longer than its peak pharmacologic effect.
- •
- A high degree of opioid tolerance does not eliminate the possibility of methadone overdose, iatrogenic or otherwise. Deaths have been reported during conversion to methadone from chronic, high-dose treatment with other opioid agonists and during initiation of methadone treatment of addiction in subjects previously abusing high doses of other opioid agonists.
- •
- There is high interpatient variability in absorption, metabolism, and relative analgesic potency. Population-based conversion ratios between methadone and other opioids are not accurate when applied to individuals.
- •
- With repeated dosing, methadone is retained in the liver and then slowly released, prolonging the duration of potential toxicity.
- •
- Steady-state plasma concentrations are not attained until 3 to 5 days after initiation of dosing.
- •
- Methadone has a narrow therapeutic index, especially when combined with other drugs.
Methadone Hydrochloride Injection for Management of Pain
Methadone Hydrochloride Injection should be prescribed only by healthcare professionals who are knowledgeable in the use of potent opioids for the management of chronic pain.
Consider the following important factors that differentiate methadone from other opioid analgesics:
- •
- There is high interpatient variability in absorption, metabolism, and relative analgesic potency. Population-based equianalgesic conversion ratios between methadone and other opioids are not accurate when applied to individuals.
- •
- The duration of analgesic action of methadone is 4 to 8 hours (based on single-dose studies) but the plasma elimination half-life is 8 to 59 hours.
- •
- With repeated dosing, the potency of methadone increases due to systemic accumulation.
- •
- Steady-state plasma concentrations, and full analgesic effects, are not attained until at least 3 to 5 days on a dose and may take longer in some patients.
Methadone Hydrochloride Injection should be prescribed only by healthcare professionals who are knowledgeable about the use of extended-release/long-acting opioids and how to mitigate the associated risks.
Use the lowest effective dosage for the shortest duration of time consistent with individual patient treatment goals (see WARNINGS). Because the risk of overdose increases as opioid doses increase, reserve titration to higher doses of Methadone Hydrochloride Injection for patients in whom lower doses are insufficiently effective and in whom the expected benefits of using a higher dose opioid clearly outweigh the substantial risks.
Initiate the dosing regimen for each patient individually, taking into account the patient’s underlying cause and severity of pain, prior analgesic treatment and response, and risk factors for addiction, abuse, and misuse (see WARNINGS).
Respiratory depression can occur at any time during opioid therapy, especially when initiating and following dosage increases with Methadone Hydrochloride Injection. Consider this risk when selecting an initial dose and when making dose adjustments (see WARNINGS).
Methadone Hydrochloride Injection multiple-dose vials may be administered intravenously, subcutaneously or intramuscularly. The absorption of subcutaneous and intramuscular methadone has not been well characterized and appears to be unpredictable. Local tissue reactions may occur.
Parenteral products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
Initiation of Therapy in Opioid Non-Tolerant Patients
When parenteral methadone is used as the first analgesic in patients who are not already being treated with, and tolerant to, opioids, the usual intravenous methadone starting dose is 2.5 mg to 10 mg every 8 to 12 hours, slowly titrated to effect. More frequent administration may be required during methadone initiation in order to maintain adequate analgesia, and extreme caution is necessary to avoid overdosage, taking into account methadone's long elimination half-life.
Conversion from Oral Methadone to Parenteral Methadone
Conversion from oral methadone to parenteral methadone should initially use a 2:1 dose ratio (e.g., 10 mg oral methadone to 5 mg parenteral methadone).
Switching Patients to Parenteral Methadone from Other Chronic Opioids
Switching a patient from another chronically administered opioid to methadone requires caution due to the uncertainty of dose conversion ratios and incomplete cross-tolerance. Deaths have occurred in opioid tolerant patients during conversion to methadone.
The potency of methadone relative to other opioid analgesics is nonlinear and increases with increasing dose. Table 1 provides an estimated conversion factor for use when converting patients from another opioid to methadone. Because of the high inter-patient variability in absorption, metabolism, and relative potency, it is critical to avoid overestimating the methadone dose which can lead to fatal respiratory depression. It is safer to underestimate a patient’s 24-hour methadone dosage and provide rescue medication (e.g., immediate-release opioid) than to overestimate the 24-hour methadone dosage and manage an adverse reaction due to an overdose. The dose conversion scheme below is derived from various consensus guidelines for converting chronic pain patients to methadone from morphine. The guidelines used to construct this table, however, were all designed for converting patients from oral morphine to oral methadone. The third column assumes a 2:1 ratio for converting from oral to intravenous methadone. Clinicians should consult published conversion guidelines to determine the equivalent morphine dose for patients converting from other opioids.
Consider the following when using the information in Table 1:
- •
- This is not a table of equianalgesic doses.
- •
- The conversion factors in this table are only for the conversion from another oral opioid analgesic to methadone hydrochloride tablets.
- •
- The table cannot be used to convert from methadone hydrochloride tablets to another opioid. Doing so will result in an overestimation of the dose of the new opioid and may result in fatal overdose.
Table 1. Oral Morphine to Intravenous Methadone Conversion for Chronic Administration - *
- The total daily methadone dose derived from the table above may then be divided to reflect the intended dosing schedule (i.e., for administration every 8 hours, divide total daily methadone dose by 3).
Total Daily Baseline Oral Morphine Dose
Estimated Daily Oral Methadone Requirement as Percent of Total Daily Morphine Dose
Estimated Daily Intravenous Methadone as Percent of Total Daily Oral Morphine Dose*
Less than 100 mg
20% to 30%
10% to 15%
100 mg to 300 mg
10% to 20%
5% to 10%
300 mg to 600 mg
8% to 12%
4% to 6%
600 mg to 1000 mg
5% to 10%
3% to 5%
Greater than 1000 mg
Less than 5%
Less than 3%
Table 2. Parenteral Morphine to Intravenous Methadone Conversion for Chronic Administration (Derived from Table 1, Assuming a 3:1 Oral:Parenteral Morphine Ratio) - *
- The total daily methadone dose derived from the table above may then be divided to reflect the intended dosing schedule (i.e., for administration every 8 hours, divide total daily methadone dose by 3).
Total Daily Baseline Parenteral Morphine Dose
Estimated Daily Parenteral Methadone Requirement as Percent of Total Daily Morphine Dose*
10 mg to 30 mg
40% to 66%
30 mg to 50 mg
27% to 66%
50 mg to 100 mg
22% to 50%
100 mg to 200 mg
15% to 34%
200 mg to 500 mg
10% to 20%
Note: Equianalgesic methadone dosing varies not only between patients, but also within the same patient, depending on baseline morphine (or other opioid) dose. Tables 1 and 2 have been included in order to illustrate this concept and to provide a safe starting point for opioid conversion. Methadone dosing should not be based solely on these tables. Methadone conversion and dose titration methods should always be individualized to account for the patient's prior opioid exposure, general medical condition, concomitant medication, and anticipated breakthrough medication use. The endpoint of titration is achievement of adequate pain relief, balanced against tolerability of opioid side effects. If a patient develops intolerable opioid related side effects, the methadone dose, or dosing interval, may need to be decreased.
Methadone Hydrochloride Injection for Treatment of Opioid Dependence
Detoxification and Maintenance Treatment of Opioid Dependence
For detoxification and maintenance of opiate dependence, methadone should be administered in accordance with the treatment standards cited in 42CFR Section 8.12, including limitations on unsupervised administration. Injectable methadone products are not approved for the outpatient treatment of opioid dependence. Parenteral methadone should be used only for patients who are unable to take oral medication, such as during hospitalization. The patient's oral methadone dose should be converted to an equivalent parenteral dose using the considerations above.
Risk of Relapse in Patients on Methadone Maintenance Treatment of Opioid Addiction
Abrupt opioid discontinuation can lead to development of opioid withdrawal symptoms (see PRECAUTIONS). Presentation of these symptoms has been associated with an increased risk of susceptible patients to relapse to illicit drug use and should be considered when assessing the risks and benefit of methadone use.
Considerations for Management of Acute Pain During Methadone Maintenance Treatment
Maintenance patients on a stable dose of methadone who experience physical trauma, postoperative pain or other causes of acute pain cannot be expected to derive analgesia from their stable dose of methadone regimens. Such patients should be given analgesics, including opioids, that would be indicated in other patients experiencing similar nociceptive stimulation. Due to the opioid tolerance induced by methadone, when opioids are required for management of acute pain in methadone patients, somewhat higher and/or more frequent doses will often be required than would be the case for other, non-tolerant patients.
Dosage Adjustment During Pregnancy
Methadone clearance may be increased during pregnancy. During pregnancy, a woman's methadone dose may need to be increased, or the dosing interval decreased (see PRECAUTIONS: Pregnancy).
-
HOW SUPPLIED
Methadone Hydrochloride Injection USP, 200 mg/20 mL (10 mg/mL) is a clear, colorless solution and is available in:
NDC 67457-217-20
20 mL Multiple-Dose Vials: One vial per cartonStore at 20°C to 25°C (68°F to 77°F), with excursions permitted between 15°C to 30°C (59°F to 86°F). [See USP Controlled Room Temperature.]
Protect from light. Store in carton until contents have been used.
Manufactured for:
Mylan Institutional LLC
Morgantown, WV 26505 U.S.A.Manufactured by:
Alcami Corporation
Charleston, SC 29405 U.S.A.Revised: 12/2023
MI:MTHDIJ:RX10
-
PRINCIPAL DISPLAY PANEL – 20 mL
NDC 67457-217-20
20 mLMethadone
Hydrochloride
Injection, USP
CII200 mg/20 mL
(10mg/mL)For Intravenous,
Intramuscular or
Subcutaneous UseRx only Multiple-Dose Vial
Each mL contains:
Active: 10 mg of methadone
hydrochloride (equivalent
to 8.95 mg methadone free
base). [WARNING: May
be habit forming.]
Inactives: 5 mg of
chlorobutanol, as a
preservative, 9 mg of sodium
chloride, as tonicity agent,
and hydrochloric acid and
sodium hydroxide as pH
adjusters, in water for
injection. The pH of the
sterile injectable solution
is between 3.0 to 6.5.
Usual Dosage: See
accompanying prescribing
information.Store at 20°C to 25°C
(68°F to 77°F), with
excursions permitted
between 15°C to 30°C
(59°F to 86°F). [See USP
Controlled Room
Temperature.]Protect from light.
Store in carton until
contents have been
used.Manufactured for:
Mylan Institutional LLC
Morgantown, WV 26505 U.S.A.Made in U.S.A.
MI:217:1C:R7
Mylan.com
-
INGREDIENTS AND APPEARANCE
METHADONE HYDROCHLORIDE
methadone hydrochloride injection, solutionProduct Information Product Type HUMAN PRESCRIPTION DRUG Item Code (Source) NDC:67457-217 Route of Administration INTRAVENOUS, INTRAMUSCULAR, SUBCUTANEOUS DEA Schedule CII Active Ingredient/Active Moiety Ingredient Name Basis of Strength Strength Methadone Hydrochloride (UNII: 229809935B) (Methadone - UNII:UC6VBE7V1Z) Methadone Hydrochloride 10 mg in 1 mL Inactive Ingredients Ingredient Name Strength Sodium chloride (UNII: 451W47IQ8X) 9 mg in 1 mL Chlorobutanol (UNII: HM4YQM8WRC) Sodium Hydroxide (UNII: 55X04QC32I) Hydrochloric Acid (UNII: QTT17582CB) Packaging # Item Code Package Description Marketing Start Date Marketing End Date 1 NDC:67457-217-20 1 in 1 CARTON 12/20/2012 1 20 mL in 1 VIAL, MULTI-DOSE; Type 0: Not a Combination Product Marketing Information Marketing Category Application Number or Monograph Citation Marketing Start Date Marketing End Date NDA NDA021624 12/20/2012 Labeler - Mylan Institutional LLC (790384502)