LEVOCARNITINE- levocarnitine injection
Teva Parenteral Medicines, Inc.
----------
Levocarnitine Injection, USP
DESCRIPTION
Levocarnitine is a carrier molecule in the transport of long-chain fatty acids across the inner mitochondrial membrane.
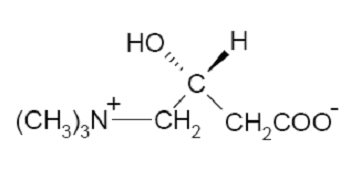
The chemical name of levocarnitine is 3-carboxy-2(R)-hydroxy-N,N,N-trimethyl-1-propanaminium, inner salt. Levocarnitine is a white crystalline, hygroscopic powder. It is readily soluble in water, hot alcohol, and insoluble in acetone. The specific rotation of levocarnitine is between -29° and -32°. Its chemical structure is:
Empirical Formula: C7H15NO3 Molecular Weight: 161.20
Levocarnitine injection is a sterile aqueous solution containing 200 mg of levocarnitine per mL. The pH is adjusted to 6.0–6.5 with hydrochloric acid.
CLINICAL PHARMACOLOGY
Levocarnitine is a naturally occurring substance required in mammalian energy metabolism. It has been shown to facilitate long-chain fatty acid entry into cellular mitochondria, therefore delivering substrate for oxidation and subsequent energy production. Fatty acids are utilized as an energy substrate in all tissues except the brain. In skeletal and cardiac muscle, fatty acids are the main substrate for energy production.
Primary systemic carnitine deficiency is characterized by low concentrations of levocarnitine in plasma, RBC, and/or tissues. It has not been possible to determine which symptoms are due to carnitine deficiency and which are due to the underlying organic acidemia, as symptoms of both abnormalities may be expected to improve with levocarnitine. The literature reports that carnitine can promote the excretion of excess organic or fatty acids in patients with defects in fatty acid metabolism and/or specific organic acidopathies that bioaccumulate acylCoA esters.1–6
Secondary carnitine deficiency can be a consequence of inborn errors of metabolism. Levocarnitine may alleviate the metabolic abnormalities of patients with inborn errors that result in accumulation of toxic organic acids. Conditions for which this effect was demonstrated are: glutaric aciduria II, methyl malonic aciduria, propionic acidemia, and medium chain fatty acylCoA dehydrogenase deficiency.7,8 Autointoxication occurs in these patients due to the accumulations of acylCoA compounds that disrupt intermediary metabolism. The subsequent hydrolysis of the acylCoA compound to its free acid results in acidosis that can be life-threatening. Levocarnitine clears the acylCoA compound by formation of acylcarnitine, which is quickly excreted. Carnitine deficiency is defined biochemically as abnormally low plasma concentrations of free carnitine, less than 20 µmol/L at one week post term and may be associated with low tissue and/or urine concentrations. Further, this condition may be associated with a plasma concentration ratio of acylcarnitine/levocarnitine greater than 0.4 or abnormally elevated concentrations of acylcarnitine in the urine. In premature infants and newborns, secondary deficiency is defined as plasma levocarnitine concentrations below age related normal concentrations.
PHARMACOKINETICS
In a relative bioavailability study in 15 healthy adult male volunteers, levocarnitine tablets were found to be bio-equivalent to levocarnitine oral solution. Following 4 days of dosing with 6 tablets of levocarnitine 330 mg b.i.d. or 2 g of levocarnitine oral solution b.i.d., the maximum plasma concentration (Cmax) was about 80 µmol/L and the time to maximum plasma concentration (Tmax) occurred at 3.3 hours.
The plasma concentration profiles of levocarnitine after a slow 3 minute intravenous bolus dose of 20 mg/kg of levocarnitine were described by a two-compartment model. Following a single i.v. administration, approximately 76% of the levocarnitine dose was excreted in the urine during the 0-24h interval. Using plasma concentrations uncorrected for endogenous levocarnitine, the mean distribution half life was 0.585 hours and the mean apparent terminal elimination half life was 17.4 hours.
The absolute bioavailability of levocarnitine from the two oral formulations of levocarnitine, calculated after correction for circulating endogenous plasma concentrations of levocarnitine, was 15.1 ± 5.3% for levocarnitine tablets and 15.9 ± 4.9% for levocarnitine oral solution.
Total body clearance of levocarnitine (Dose/AUC including endogenous baseline concentrations) was a mean of 4.00 L/h.
Levocarnitine was not bound to plasma protein or albumin when tested at any concentration or with any species including the human.9
METABOLISM AND EXCRETION
In a pharmacokinetic study where five normal adult male volunteers received an oral dose of [3H-methyl]-L-carnitine following 15 days of a high carnitine diet and additional carnitine supplement, 58 to 65% of the administered radioactive dose was recovered in the urine and feces in 5 to 11 days. Maximum concentration of [3H-methyl]-L-carnitine in serum occurred from 2.0 to 4.5 hr after drug administration. Major metabolites found were trimethylamine N-oxide, primarily in urine (8% to 49% of the administered dose) and [3H]-γ-butyrobetaine, primarily in feces (0.44% to 45% of the administered dose). Urinary excretion of levocarnitine was about 4 to 8% of the dose. Fecal excretion of total carnitine was less than 1% of the administered dose.10
After attainment of steady state following 4 days of oral administration of levocarnitine tablets (1980 mg q12h) or Oral Solution (2000 mg q12h) to 15 healthy male volunteers, the mean urinary excretion of levocarnitine during single dosing interval (12h) was about 9% of the orally administered dose (uncorrected for endogenous urinary excretion).
INDICATIONS AND USAGE
For the acute and chronic treatment of patients with an inborn error of metabolism that results in secondary carnitine deficiency.
PRECAUTIONS
Carcinogenesis, mutagenesis, impairment of fertility
Mutagenicity tests performed in Salmonella typhimurium, Saccharomyces cerevisiae, and Schizosaccharomyces pombe indicate that levocarnitine is not mutagenic. No long-term animal studies have been performed to evaluate the carcinogenic potential of levocarnitine.
Pregnancy
Teratogenic Effects
Pregnancy Category B
Reproductive studies have been performed in rats and rabbits at doses up to 3.8 times the human dose on the basis of surface area and have revealed no evidence of impaired fertility or harm to the fetus due to levocarnitine. There are, however, no adequate and well controlled studies in pregnant women.
Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
Nursing Mothers
Levocarnitine supplementation in nursing mothers has not been specifically studied.
Studies in dairy cows indicate that the concentration of levocarnitine in milk is increased following exogenous administrations of levocarnitine. In nursing mothers receiving levocarnitine, any risks to the child of excess carnitine intake need to be weighed against the benefits of levocarnitine supplementation to the mother. Consideration may be given to discontinuation of nursing or of levocarnitine treatment.
ADVERSE REACTIONS
Transient nausea and vomiting have been observed. Less frequent adverse reactions are body odor, nausea, and gastritis. An incidence for these reactions is difficult to estimate due to the confounding effects of the underlying pathology.
Seizures have been reported to occur in patients, with or without pre-existing seizure activity, receiving either oral or intravenous levocarnitine. In patients with pre-existing seizure activity, an increase in seizure frequency and/or severity has been reported.
OVERDOSAGE
There have been no reports of toxicity from levocarnitine overdosage. Levocarnitine is easily removed from plasma by dialysis. The intravenous LD50 of levocarnitine in rats is 5.4 g/kg and the oral LD50 of levocarnitine in mice is 19.2 g/kg.
DOSAGE AND ADMINISTRATION
Levocarnitine injection is administered intravenously.
Metabolic Disorders
The recommended dose is 50 mg/kg given as a slow 2–3 minute bolus injection or by infusion. Often a loading dose is given in patients with severe metabolic crisis, followed by an equivalent dose over the following 24 hours. It should be administered q3h or q4h, and never less than q6h either by infusion or by intravenous injection. All subsequent daily doses are recommended to be in the range of 50 mg/kg or as therapy may require. The highest dose administered has been 300 mg/kg.
It is recommended that a plasma carnitine concentration be obtained prior to beginning this parenteral therapy. Weekly and monthly monitoring is recommended as well. This monitoring should include blood chemistries, vital signs, plasma carnitine concentrations (the plasma free carnitine concentration should be between 35 and 60 μmol/L) and overall clinical condition.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
COMPATIBILITY AND STABILITY
Levocarnitine injection is compatible and stable when mixed in parenteral solutions of sodium chloride 0.9% or lactated Ringer's in concentrations ranging from 250 mg/500 mL (0.5 mg/mL) to 4200 mg/500 mL (8.0 mg/mL) and stored at room temperature (25°C) for up to 24 hours in PVC plastic bags.
HOW SUPPLIED
Levocarnitine Injection, 200 mg/mL, is available as follows:
| NDC Number | Total Strength |
|---|---|
|
0703-0404-02 |
1 g/5 mL |
|
0703-0405-02 |
2.5 g/12.5 mL |
Packaged 5 vials per shelf carton.
Store at controlled room temperature (25°C/77°F). See USP.
Store in carton until time of use to protect from light.
Discard unused portion of an opened container, as they contain no preservative.
REFERENCES
- 1.
- Bohmer, T., Rynding, A. and Solberg, H.E. 1974. Carnitine levels in human serum in health and disease. Clin. Chim. Acta 57:55-61.
- 2.
- Brooks, H., Goldberg, L., Holland, R. et al. 1977. Carnitine-induced effects on cardiac and peripheral hemodynamics. J. Clin. Pharmacol. 17:561-578.
- 3.
- Christiansen, R., Bremer, J. 1976. Active transport of butyrobetaine and carnitine into isolated liver cells. Biochem. Biophys. Acta 448:562-577.
- 4.
- Lindstedt, S. and Lindstedt, G. 1961. Distribution and excretion of carnitine in the rat. Acta. Chem. Scand. 15:701-702.
- 5.
- Rebouche, C.J. and Engel, A.G. 1983. Carnitine metabolism and deficiency syndromes. Mayo Clin. Proc. 58:533-540.
- 6.
- Rebouche, C.J. and Paulson, D.J. 1986. Carnitine metabolism and function in humans. Ann. Rev. Nutr. 6:41-66.
- 7.
- Scriver, C.R., Beaudet, A.L., Sly, W.S. and Valle, D. 1989. The Metabolic Basis of Inherited Disease. New York: McGraw-Hill.
- 8.
- Schaub, J., Van Hoof, F. and Vis, H.L. 1991. Inborn Errors of Metabolism. New York:Raven Press.
- 9.
- Marzo, A., Arrigoni Martelli, E., Mancinelli, A., Cardace, G., Corbelletta, C., Bassani, E. and Solbiati, M. 1991. Protein binding of L-carnitine family components. Eur. J. Drug. Met. Pharmacokin., Special Issue III: 364-368.
- 10.
- Rebouche, C.J. 1991. Quantitative estimation of absorption and degradation of a carnitine supplement by human adults. Metabolism 40:1305-1310.
Rev. A 10/2011
TEVA PHARMACEUTICALS USA
Sellersville, PA 18960
| LEVOCARNITINE
levocarnitine injection |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| LEVOCARNITINE
levocarnitine injection |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Teva Parenteral Medicines, Inc. (794362533) |