|
|
|||||||||||||||||||||||
FULL PRESCRIBING INFORMATION
1 INDICATIONS AND USAGE
Morphine sulfate is an opioid analgesic indicated for the relief of moderate to severe acute and chronic pain where use of an opioid analgesic is appropriate.
2 DOSAGE AND ADMINISTRATION
Selection of patients for treatment with morphine sulfate should be governed by the same principles that apply to the use of similar opioid analgesics. Physicians should individualize treatment in every case, using non-opioid analgesics, opioids on an as needed basis and/or combination products, and chronic opioid therapy in a progressive plan of pain management such as outlined by the World Health Organization, the Agency for Healthcare Research and Quality, and the American Pain Society.
2.1 Individualization of Dosage
As with any opioid drug product adjust the dosing regimen for each patient individually, taking into account the patient’s prior analgesic treatment experience. In the selection of the initial dose of morphine sulfate, attention should be given to the following:
- the total daily dose, potency and specific characteristics of the opioid the patient has been taking previously;
- the reliability of the relative potency estimate used to calculate the equivalent morphine sulfate dose needed;
- the patient’s degree of opioid tolerance;
- the general condition and medical status of the patient;
- concurrent medications;
- the type and severity of the patient’s pain;
- risk factors for abuse, addiction or diversion, including a prior history of abuse, addiction or diversion.
The following dosing recommendations, therefore, can only be considered suggested approaches to what is actually a series of clinical decisions over time in the management of the pain of each individual patient.
Continual re-evaluation of the patient receiving morphine sulfate is important, with special attention to the maintenance of pain control and the relative incidence of side effects associated with therapy. During chronic therapy, especially for non-cancer-related pain, the continued need for the use of opioid analgesics should be re-assessed as appropriate.
During periods of changing analgesic requirements, including initial titration, frequent contact is recommended between physician, other members of the healthcare team, the patient, and the caregiver/family.
2.2 Initiation of Therapy in Opioid-Naïve Patients
Patients who have not been receiving opioid analgesics should be started on morphine sulfate in the following dosing range:
- Morphine Sulfate Oral Solution: 10 to 20 mg every 4 hours as needed for pain.
- Morphine Sulfate Tablets: 15 to 30 mg every 4 hours as needed for pain.
The dose should be titrated based upon the individual patient’s response to their initial dose of morphine sulfate. This dose can then be adjusted to an acceptable level of analgesia taking into account the improvement in pain intensity and the tolerability of the morphine by the patient.
2.3 Conversion to Oral Morphine Sulfate
There is inter-patient variability in the potency of opioid drugs and opioid formulations. Therefore, a conservative approach is advised when determining the total daily dose of morphine sulfate. It is better to underestimate a patient’s 24-hour oral morphine sulfate dose and make available rescue medication than to overestimate the 24-hour oral morphine sulfate dose and manage an adverse experience of overdose.
The following general points should be considered regarding opioid conversions.
Conversion From Parenteral Morphine to Oral Morphine Sulfate
For conversion from parenteral to oral morphine sulfate, anywhere from 3 to 6 mg of oral morphine sulfate may be required to provide pain relief equivalent to 1 mg of parenteral morphine.
Conversion From Parenteral Oral Non-Morphine Opioids to Oral Morphine Sulfate
In converting patients from other opioids to morphine sulfate, close observation and adjustment of dosage based upon the patient’s response to morphine sulfate is imperative. Administration of supplemental analgesia for breakthrough or incident pain and titration of the total daily dose of morphine sulfate may be necessary, especially in patients who have disease states that are changing rapidly.
Physicians and other healthcare professionals are advised to refer to published relative potency information, keeping in mind that conversion ratios are only approximate.
Conversion From Controlled-Release Oral Morphine to Oral Morphine Sulfate
For a given dose, the same total amount of morphine sulfate is available from Morphine Sulfate Oral Solution and Morphine Sulfate Tablets, and controlled-release and extended-release morphine capsules. The extended duration of release of morphine sulfate from controlled-release tablets or extended-release tablets results in reduced maximum and increased minimum plasma morphine sulfate concentrations than with shorter acting morphine sulfate products. Conversion from oral solution or immediate-release tablets to the same total daily dose of controlled-release tablets or extended-release tablets could lead to excessive sedation at peak serum levels. Dosage adjustment with close observation is recommended.
2.4 Maintenance of Therapy
Continual re-evaluation of the patient receiving morphine sulfate is important, with special attention to the maintenance of pain control and the relative incidence of side effects associated with therapy. If the level of pain increases, effort should be made to identify the source of increased pain, while adjusting the dose as described above to decrease the level of pain. During chronic therapy, especially for non-cancer-related pain (or pain associated with other terminal illnesses), the continued need for the use of opioid analgesics should be re-assessed as appropriate.
2.5 Cessation of Therapy
When the patient no longer requires therapy with morphine sulfate, doses should be tapered gradually to prevent signs and symptoms of withdrawal in the physically dependent patient.
3 DOSAGE FORMS AND STRENGTHS
Each 5 mL of green Morphine Sulfate Oral Solution contains: morphine sulfate 10 mg or 20 mg.
Each 15 mg tablet for oral administration contains: morphine sulfate 15 mg and is a white, biconvex tablet scored on one side and product identification "54 733" debossed on the other side.
Each 30 mg tablet for oral administration contains: morphine sulfate 30 mg and is a white, biconvex tablet scored on one side and product identification "54 262" debossed on the other side.
4 CONTRAINDICATIONS
Morphine sulfate is contraindicated in patients with known hypersensitivity to morphine, morphine salts, or any components of the product.
Morphine sulfate is contraindicated in patients with respiratory depression in the absence of resuscitative equipment.
Morphine sulfate is contraindicated in patients with acute or severe bronchial asthma or hypercarbia.
Morphine sulfate is contraindicated in any patient who has or is suspected of having paralytic ileus.
5 WARNINGS AND PRECAUTIONS
5.1 Respiratory Depression
Respiratory depression is the primary risk of morphine sulfate. Respiratory depression occurs more frequently in elderly or debilitated patients and in those suffering from conditions accompanied by hypoxia, hypercapnia, or upper airway obstruction, in whom even moderate therapeutic doses may significantly decrease pulmonary ventilation.
Morphine sulfate should be used with extreme caution in patients with chronic obstructive pulmonary disease or cor pulmonale and in patients having a substantially decreased respiratory reserve (e.g., severe kyphoscoliosis), hypoxia, hypercapnia, or pre-existing respiratory depression. In such patients, even usual therapeutic doses of morphine sulfate may increase airway resistance and decrease respiratory drive to the point of apnea. Alternative non-opioid analgesics should be considered, and morphine sulfate should be employed only under careful medical supervision at the lowest effective dose in such patients.
5.2 Misuse, Abuse and Diversion of Opioids
Morphine sulfate is an opioid agonist and a Schedule II controlled substance. Such drugs are sought by drug abusers and people with addiction disorders. Diversion of Schedule II products is an act subject to criminal penalty.
Morphine sulfate can be abused in a manner similar to other opioid agonists, legal or illicit. This should be considered when prescribing or dispensing morphine sulfate in situations where the physician or pharmacist is concerned about an increased risk of misuse, abuse, or diversion.
Morphine sulfate may be abused by crushing, chewing, snorting or injecting the product. These practices pose a significant risk to the abuser that could result in overdose and death. [See DRUG ABUSE AND DEPENDENCE (9)]
Concerns about abuse, addiction, and diversion should not prevent the proper management of pain. Healthcare professionals should contact their State Professional Licensing Board or State Controlled Substances Authority for information on how to prevent and detect abuse or diversion of this product.
5.3 Interactions with Alcohol and Drugs of Abuse
Morphine sulfate may be expected to have additive effects when used in conjunction with alcohol, other opioids, or illicit drugs that cause central nervous system depression because respiratory depression, hypotension, profound sedation, coma or death may result.
5.4 Use In Head Injury and Increased Intracranial Pressure
In the presence of head injury, intracranial lesions or a preexisting increase in intracranial pressure, the possible respiratory depressant effects of morphine sulfate and its potential to elevate cerebrospinal fluid pressure (resulting from vasodilation following CO2 retention) may be markedly exaggerated. Furthermore, morphine sulfate can produce effects on pupillary response and consciousness, which may obscure neurologic signs of further increases in intracranial pressure in patients with head injuries.
5.5 Hypotensive Effect
Morphine sulfate may cause severe hypotension in an individual whose ability to maintain blood pressure has already been compromised by a depleted blood volume or concurrent administration of drugs such as phenothiazines or general anesthetics. Morphine sulfate may produce orthostatic hypotension and syncope in ambulatory patients.
Morphine sulfate should be administered with caution to patients in circulatory shock, as vasodilation produced by the drug may further reduce cardiac output and blood pressure.
5.6 Gastrointestinal Effects
Morphine sulfate should not be administered to patients with gastrointestinal obstruction, especially paralytic ileus because morphine sulfate diminishes propulsive peristaltic waves in the gastrointestinal tract and may prolong the obstruction.
The administration of morphine sulfate may obscure the diagnosis or clinical course in patients with acute abdominal condition.
5.7 Use in Pancreatic/Biliary Tract Disease
Morphine sulfate should be used in caution in patients with biliary tract disease, including acute pancreatitis, as morphine sulfate may cause spasm of the sphincter of Oddi and diminish biliary and pancreatic secretions.
5.8 Special Risk Groups
Morphine sulfate should be administered cautiously and in reduced dosages in patients with severe renal or hepatic impairment, Addison’s disease, hypothyroidism, prostatic hypertrophy, or urethral stricture, and in elderly or debilitated patients. [See USE IN SPECIFIC POPULATIONS (8.5)]
Caution should be exercised in the administration of morphine sulfate to patients with CNS depression, toxic psychosis, acute alcoholism and delirium tremens.
All opioids may aggravate convulsions in patients with convulsive disorders, and all opioids may induce or aggravate seizures in some clinical settings.
5.9 Driving and Operating Machinery
Patients should be cautioned that morphine sulfate could impair the mental and/or physical abilities needed to perform potentially hazardous activities such as driving a car or operating machinery.
Patients should also be cautioned about the potential combined effects of morphine sulfate with other CNS depressants, including other opioids, phenothiazines, sedative/hypnotics and alcohol. [See DRUG INTERACTIONS (7)]
6 ADVERSE REACTIONS
Serious adverse reactions associated with morphine sulfate use include: respiratory depression, apnea, and to a lesser degree, circulatory depression, respiratory arrest, shock and cardiac arrest.
The common adverse reactions seen on initiation of therapy with morphine sulfate are dose-dependent and are typical opioid-related side effects. The most frequent of these include constipation, nausea, and somnolence. Other commonly observed adverse reactions include: lightheadedness, dizziness, sedation, vomiting, and sweating. The frequency of these events depends upon several factors including clinical setting, the patient’s level of opioid tolerance, and host factors specific to the individual. These events should be anticipated and managed as part of opioid analgesia therapy.
Other less frequently observed adverse reactions expected from opioid analgesics, including morphine sulfate include:
Body as a Whole: malaise, withdrawal syndrome
Cardiovascular System: bradycardia, hypertension, hypotension, palpitations, syncope, tachycardia
Digestive System: biliary pain, dyspepsia, dysphagia, gastroenteritis, abnormal liver function tests, rectal disorder, thirst
Hemic and Lymphatic System: anemia, thrombocytopenia
Metabolic and Nutritional Disorders: edema, weight loss
Musculoskeletal: skeletal muscle rigidity
Nervous System: abnormal dreams, abnormal gait, agitation, amnesia, anxiety, ataxia, confusion, convulsions, coma, delirium, hallucinations, lethargy, nervousness, abnormal thinking, tremor, vasodilation, vertigo, headache
Respiratory System: hiccup, hypoventilation, voice alteration
Skin and Appendages: dry skin, urticaria, pruritus
Special Senses: amblyopia, eye pain, taste perversion
Urogenital System: abnormal ejaculation, dysuria, impotence, decreased libido, oliguria, urinary retention, anti-diuretic effect
7 DRUG INTERACTIONS
7.1 CNS Depressants
Other central nervous system (CNS) depressants including sedatives, hypnotics, general anesthetics, antiemetics, phenothiazines, or other tranquilizers or alcohol increases the risk of respiratory depression, hypotension, profound sedation, or coma. Use morphine sulfate with caution and in reduced dosages in patients taking these agents.
7.2 Muscle Relaxants
Morphine sulfate may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression.
7.3 Mixed Agonist/Antagonist Opioid Analgesics
Mixed agonist/antagonist analgesics (i.e., pentazocine, nalbuphine, and butorphanol) should NOT be administered to patients who have received or are receiving a course of therapy with a pure opioid agonist analgesic such as morphine sulfate. In these patients, mixed agonist/antagonist analgesics may reduce the analgesic effect and/or may precipitate withdrawal symptoms.
7.4 Cimetidine
Concomitant administration of morphine sulfate and cimetidine has been reported to precipitate apnea, confusion, and muscle twitching in an isolated report. Patients should be monitored for increased respiratory and CNS depression when receiving cimetidine concomitantly with morphine sulfate.
7.5 Monoamine Oxidase Inhibitors (MAOIs)
MAOIs markedly potentiate the action of morphine sulfate. Morphine sulfate should not be used in patients taking MAOIs or within 14 days of stopping such treatment.
7.6 Anticholinergics
Anticholinergics or other medications with anticholinergic activity when used concurrently with opioid analgesics may result in increased risk of urinary retention and/or severe constipation, which may lead to paralytic ileus.
7.7 P-Glycoprotein (PGP) Inhibitors
Based on published reports, PGP inhibitors (e.g. quinidine) may increase the absorption/exposure of morphine sulfate by about two fold. Therefore, caution should be exercised when morphine sulfate is co-administered with PGP inhibitors.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Teratogenic Effects (Pregnancy Category C)
Animal reproduction studies have not been conducted with morphine sulfate. It is also not known whether morphine sulfate can cause fetal harm when administered to a pregnant woman or can affect reproduction capacity. Morphine sulfate should be given to a pregnant woman only if clearly needed.
In humans, the frequency of congenital anomalies has been reported to be no greater than expected among the children of 70 women who were treated with morphine sulfate during the first four months of pregnancy or in 448 women treated with this drug anytime during pregnancy. Furthermore, no malformations were observed in the infant of a woman who attempted suicide by taking an overdose of morphine sulfate and other medication during the first trimester of pregnancy.
Several literature reports indicate that morphine sulfate administered subcutaneously during the early gestational period in mice and hamsters produced neurological, soft tissue and skeletal abnormalities. With one exception, the effects that have been reported were following doses that were maternally toxic and the abnormalities noted were characteristic to those observed when maternal toxicity is present. In one study, following subcutaneous infusion of doses greater than or equal to 0.15 mg/kg to mice, exencephaly, hydronephrosis, intestinal hemorrhage, split supraoccipital, malformed sternebrae, and malformed xiphoid were noted in the absence of maternal toxicity. In the hamster, morphine sulfate given subcutaneously on gestation day 8 produced exencephaly and cranioschisis. Morphine sulfate was not a significant teratogen in the rat at exposure levels significantly beyond that normally encountered in clinical practice. In one study however, decreased litter size and viability were observed in the offspring of male rats administered morphine at doses approximately 3-fold the maximum recommended human daily dose (MRHDD) for 10 days prior to mating. In two studies performed in the rabbit, no evidence of teratogenicity was reported at subcutaneous doses up to 100 mg/kg.
Nonteratogenic Effects
Controlled studies of chronic in utero morphine exposure in pregnant women have not been conducted. Infants born to mothers who have taken opioids chronically may exhibit withdrawal symptoms, following birth, reversible reduction in brain volume, small size, decreased ventilatory response to CO2 and increased risk of sudden infant death syndrome.
Manifestations of the neonatal withdrawal syndrome include irritability, hyperactivity, abnormal sleep pattern, high-pitched cry, tremor, vomiting, diarrhea, weight loss, and failure to gain weight. The time and amount of the mother’s last dose and the rate of elimination of the drug from the newborn may affect the onset, duration, and severity of the disorder. When severe symptoms occur, pharmacologic intervention may be required.
Published literature has reported that exposure to morphine sulfate during pregnancy is associated with reduction in growth and a host of behavioral abnormalities in the offspring of animals. Morphine sulfate treatment during gestational periods of organogenesis in rats, hamsters, guinea pigs and rabbits resulted in the following treatment-related embryotoxicity and neonatal toxicity in one or more studies: decreased litter size, embryo-fetal viability, fetal and neonatal body weights, absolute brain and cerebellar weights, lengths or widths at birth and during the neonatal period, delayed motor and sexual maturation, and increased neonatal mortality, cyanosis and hypothermia. Decreased fertility in female offspring, and decreased plasma and testicular levels of luteinizing hormone and testosterone, decreased testes weights, seminiferous tubule shrinkage, germinal cell aplasia, and decreased spermatogenesis in male offspring were also observed. Behavioral abnormalities resulting from chronic morphine sulfate exposure of fetal animals included altered reflex and motor skill development, mild withdrawal, and altered responsiveness to morphine sulfate persisting into adulthood.
8.2 Labor And Delivery
Opioids cross the placenta and may produce respiratory depression and psycho-physiologic effects in neonates. Morphine sulfate is not recommended for use in women during and immediately prior to labor. Occasionally, opioid analgesics may prolong labor through actions which temporarily reduce the strength, duration and frequency of uterine contractions. However this effect is not consistent and may be offset by an increased rate of cervical dilatation, which tends to shorten labor. Neonates whose mothers received opioid analgesics during labor should be observed closely for signs of respiratory depression. A specific opioid antagonist, such as naloxone or nalmefene, should be available for reversal of opioid-induced respiratory depression in the neonate.
8.3 Nursing Mothers
Low levels of morphine sulfate have been detected in maternal milk. The milk:plasma morphine AUC ratio is about 2.5:1. The amount of morphine sulfate delivered to the infant depends on the plasma concentration of the mother, the amount of milk ingested by the infant, and the extent of first-pass metabolism. Because of the potential for serious adverse reactions in nursing infants from morphine sulfate including respiratory depression, sedation and possibly withdrawal symptoms upon cessation of morphine sulfate administration to the mother, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
8.4 Pediatric Use
The safety and effectiveness and the pharmacokinetics of Morphine Sulfate Oral Solution and Morphine Sulfate Tablets in pediatric patients below the age of 18 have not been established.
8.5 Geriatric Use
Elderly patients (aged 65 years or older) may have increased sensitivity to morphine sulfate. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
8.6 Gender
While evidence of greater post-operative morphine sulfate consumption in men compared to women is present in the literature, clinically significant differences in analgesic outcomes and pharmacokinetic parameters have not been consistently demonstrated. Some studies have shown an increased sensitivity to the adverse effects of morphine sulfate, including respiratory depression, in women compared to men.
8.7 Hepatic Impairment
Morphine sulfate pharmacokinetics have been reported to be significantly altered in patients with cirrhosis. Clearance was found to decrease with a corresponding increase in half-life. The M3G and M6G to morphine AUC ratios also decreased in these subjects, indicating diminished metabolic activity. These patients should be started cautiously with lower doses of morphine sulfate and titrated slowly while carefully monitoring for side effects.
8.8 Renal Impairment
Morphine sulfate pharmacokinetics are altered in patients with renal failure. Clearance is decreased and the metabolites, M3G and M6G, may accumulate to much higher plasma levels in patients with renal failure as compared to patients with normal renal function. These patients should be started cautiously with lower doses of morphine sulfate and titrated slowly while carefully monitoring for side effects.
9 DRUG ABUSE AND DEPENDENCE
9.1 Controlled Substance
Morphine sulfate is a mu-agonist opioid and is a Schedule II controlled substance. Morphine sulfate, like other opioids used in analgesia, can be abused and is subject to criminal diversion.
9.2 Abuse
Drug addiction is characterized by compulsive use, use for non-medical purposes, and continued use despite harm or risk of harm. Drug addiction is a treatable disease, utilizing a multi-disciplinary approach, but relapse is common.
“Drug-seeking” behavior is very common in addicts and drug abusers. Drug-seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing or referral, repeated “loss” of prescriptions, tampering with prescriptions and reluctance to provide prior medical records or contact information for other treating physician(s). “Doctor shopping” to obtain additional prescriptions is common among drug abusers and people suffering from untreated addiction.
Abuse and addiction are separate and distinct from physical dependence and tolerance. Physicians should be aware that addiction may not be accompanied by concurrent tolerance and symptoms of physical dependence. The converse is also true. In addition, abuse of opioids can occur in the absence of true addiction and is characterized by misuse for non-medical purposes, often in combination with other psychoactive substances. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests is strongly advised.
Morphine sulfate is intended for oral use only. Abuse of morphine sulfate poses a risk of overdose and death. The risk is increased with concurrent abuse of alcohol and other substances. Parenteral drug abuse is commonly associated with transmission of infectious diseases such as hepatitis and HIV.
Proper assessment of the patient, proper prescribing practices, periodic re-evaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal symptoms. [See USE IN SPECIFIC POPULATIONS (8.2) ]
9.3 Dependence
Tolerance is the need for increasing doses of opioids to maintain a defined effect such as analgesia (in the absence of disease progression or other external factors). Physical dependence is manifested by withdrawal symptoms after abrupt discontinuation of a drug or upon administration of an antagonist. Physical dependence and tolerance are not unusual during chronic opioid therapy.
The opioid abstinence or withdrawal syndrome is characterized by some or all of the following: restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate.
In general, opioids should not be abruptly discontinued. [See DOSAGE AND ADMINISTRATION (2.5)]
10 OVERDOSAGE
10.1 Symptoms
Acute overdosage with morphine sulfate is manifested by respiratory depression (a decrease in respiratory rate and/or tidal volume, Cheyne-Stokes respiration, cyanosis), extreme somnolence progressing to stupor or coma, skeletal muscle flaccidity, cold and clammy skin, constricted pupils, and, in some cases, pulmonary edema, bradycardia, hypotension, cardiac arrest and death.
Morphine sulfate may cause miosis, even in total darkness. Pinpoint pupils are a sign of opioid overdose but are not pathognomonic (e.g., pontine lesions of hemorrhagic or ischemic origin may produce similar findings). Marked mydriasis rather than miosis may be seen with hypoxia in overdose situations. [See CLINICAL PHARMACOLOGY (12) ]
10.2 Treatment
Primary attention should be given to re-establishment of a patent airway and institution of assisted or controlled ventilation. Supportive measures (including oxygen and vasopressors) should be employed in the management of circulatory shock and pulmonary edema accompanying overdose as indicated. Cardiac arrest or arrhythmias may require cardiac massage or defibrillation. Elimination or evacuation of gastric contents may be necessary in order to eliminate unabsorbed drug. Before attempting treatment by gastric emptying or activated charcoal, care should be taken to secure the airway.
The pure opioid antagonists, naloxone or nalmefene, are specific antidotes to respiratory depression resulting from opioid overdose. Since the duration of reversal is expected to be less than the duration of action of morphine sulfate, the patient must be carefully monitored until spontaneous respiration is reliably re-established. If the response to opioid antagonists is sub-optimal or only brief in nature, additional antagonist should be administered as directed by the manufacturer of the product.
Opioid antagonists should not be administered in the absence of clinically significant respiratory or circulatory depression secondary to morphine sulfate overdose. Such agents should be administered cautiously to persons who are known, or suspected to be physically dependent on morphine sulfate. In such cases, an abrupt or complete reversal of opioid effects may precipitate an acute abstinence syndrome.
In an individual physically dependent on opioids, administration of the usual dose of the antagonist will precipitate an acute withdrawal syndrome. The severity of the withdrawal symptoms experienced will depend on the degree of physical dependence and the dose of the antagonist administered. Use of an opioid antagonist should be reserved for cases where such treatment is clearly needed. If it is necessary to treat serious respiratory depression in the physically dependent patient, administration of the antagonist should be initiated with care and titrated with smaller than usual doses.
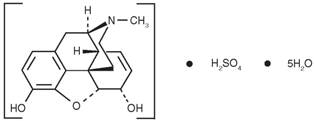
11 DESCRIPTION
Chemically, morphine sulfate is 7,8-didehydro-4,5 alpha-epoxy-17 methyl-morphinan-3,6 alpha-diol sulfate (2:1) (salt) pentahydrate with a molecular mass of 758. Morphine sulfate occurs as white, feathery, silky crystals; cubical masses of crystal; or white crystalline powder. It is soluble in water and slightly soluble in alcohol, but is practically insoluble in chloroform or ether. The octanol:water partition coefficient of morphine is 1.42 at physiologic pH and the pKa is 7.9 for the tertiary nitrogen (the majority is ionized at pH 7.4).
Each 5 mL of oral solution contains 10 or 20 mg of morphine sulfate, USP and the following inactive ingredients: citric acid, edetate disodium, FD&C Green No. 3 (fast green), glycerin, methylparaben (only in 20 mg/5mL concentration), propylparaben (only in 20 mg/5mL concentration), sodium benzoate, sorbitol and water.
Each tablet contains 15 or 30 mg of morphine sulfate, USP and the following inactive ingredients: colloidal silicon dioxide, corn starch, microcrystalline cellulose, pregelatinized starch, and stearic acid.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism Of Action
Morphine sulfate, a pure opioid agonist, is relatively selective for the mu receptor, although it can interact with other opioid receptors at higher doses. In addition to analgesia, the widely diverse effects of morphine sulfate include drowsiness, changes in mood, respiratory depression, decreased gastrointestinal motility, nausea, vomiting, and alterations of the endocrine and autonomic nervous system.
Effects on the Central Nervous System (CNS)
The principal therapeutic action of morphine sulfate is analgesia. Other therapeutic effects of morphine sulfate include anxiolysis, euphoria and feelings of relaxation. Although the precise mechanism of the analgesic action is unknown, specific CNS opiate receptors and endogenous compounds with morphine sulfate-like activity have been identified throughout the brain and spinal cord and are likely to play a role in the expression and perception of analgesic effects. In common with other opioids, morphine sulfate causes respiratory depression, in part by a direct effect on the brainstem respiratory centers. Morphine sulfate and related opioids depress the cough reflex by direct effect on the cough center in the medulla. Antitussive effects may occur with doses lower than those usually required for analgesia.
Morphine sulfate causes miosis, even in total darkness.
Effects on the Gastrointestinal Tract and on Other Smooth Muscle
Gastric, biliary and pancreatic secretions are decreased by morphine sulfate. Morphine sulfate causes a reduction in motility and is associated with an increase in tone in the antrum of the stomach and duodenum. Digestion of food in the small intestine is delayed and propulsive contractions are decreased. Propulsive peristaltic waves in the colon are decreased, while tone is increased to the point of spasm. The end result may be constipation. Morphine sulfate can cause a marked increase in biliary tract pressure as a result of spasm of the sphincter of Oddi. Morphine sulfate may also cause spasm of the sphincter of the urinary bladder.
Effects on the Cardiovascular System
In therapeutic doses, morphine sulfate does not usually exert major effects on the cardiovascular system. Morphine sulfate produces peripheral vasodilation which may result in orthostatic hypotension and fainting. Release of histamine can occur, which may play a role in opioid-induced hypotension. Manifestations of histamine release and/or peripheral vasodilation may include pruritus, flushing, red eyes and sweating.
Endocrine System
Opioid agonists have been shown to have a variety of effects on the secretion of hormones. Opioids inhibit the secretion of ACTH, cortisol, and luteinizing hormone (LH) in humans. They also stimulate prolactin, growth hormone (GH) secretion, and pancreatic secretion of insulin and glucagon in humans and other species, rats and dogs. Thyroid stimulating hormone (TSH) has been shown to be both inhibited and stimulated by opioids.
Immune System
Opioids have been shown to have a variety of effects on components of the immune system in in vitro and animal models. The clinical significance of these findings is unknown.
12.2 Pharmacodynamics
Morphine sulfate concentrations are not predictive of analgesic response, especially in patients previously treated with opioids. The minimum effective concentration varies widely and is influenced by a variety of factors, including the extent of previous opioid use, age and general medical condition. Effective doses in tolerant patients may be significantly higher than in opioid-naïve patients.
12.3 Pharmacokinetics
Absorption
Morphine sulfate is about two-thirds absorbed from the gastrointestinal tract with the maximum analgesic effect occurring 60 minutes post-administration. The oral bioavailability of morphine sulfate is less than 40% and shows large inter-individual variability due to extensive pre-systemic metabolism.
Food Effects
When morphine sulfate 30 mg tablet was administered 30 minutes after ingesting a high fat/high calorie meal, there was no change in the extent of absorption (AUC) of morphine sulfate. There was, however, an increase in the median Tmax from 0.5 to 0.75 hours and an 11% decrease in Cmax. Although the presence of a food effect was not assessed with morphine sulfate oral solution, significant food effect is not expected with a solution formulation. Both, the tablet and solution can be administered without regard to meals.
Steady-State
Administration of the 30 mg Morphine Sulfate Tablet and 30 mg of Morphine Sulfate Oral Solution every six hours for 5 days resulted in a comparable 24-hour exposure (AUC). The steady-state levels were achieved within 48 hours for both tablets and solution. The mean steady state Cmax values were about 78 and 58 ng/mL for tablet and solution, respectively.
Distribution
Once absorbed, morphine sulfate is distributed to skeletal muscle, kidneys, liver, intestinal tract, lungs, spleen and brain. Although the primary site of action is the CNS, only small quantities cross the blood-brain barrier. Morphine sulfate also crosses the placental membranes and has been found in breast milk. The volume of distribution of morphine sulfate is approximately 1 to 6 L/kg, and morphine sulfate is 20 to 35% reversibly bound to plasma proteins.
Metabolism
The major pathway of morphine sulfate detoxification is conjunction, either with D-glucuronic acid to produce glucuronides or with sulfuric acid to produce morphine-3-etheral sulfate. While a small fraction (less than 5%) of morphine sulfate is demethylated, virtually all morphine sulfate is converted by hepatic metabolism to the 3- and 6-glucuronide metabolites (M3G and M6G; about 50% and 15%, respectively). M6G has been shown to have analgesic activity but crosses the blood-brain barrier poorly, while M3G has no significant analgesic activity.
Excretion
Most of a dose of morphine sulfate is excreted in urine as M3G and M6G, with elimination of morphine sulfate occurring primarily as renal excretion of M3G. Approximately 10% of the dose is excreted unchanged in urine. A small amount of glucuronide conjugates are excreted in bile, with minor enterohepatic recycling. Seven to 10% of administered morphine sulfate is excreted in the feces.
The mean adult plasma clearance is approximately 20 to 30 mL/min/kg. The effective terminal half-life of morphine sulfate after IV administration is reported to be approximately 2 hours. In some studies involving longer periods of plasma sampling, a longer terminal half-life of morphine sulfate of about 15 hours was reported.
Race
There may be some pharmacokinetic differences associated with race. In one published study, Chinese subjects given intravenous morphine sulfate had a higher clearance when compared to Caucasian subjects (1852 +/- 116 mL/min compared to 1495 +/- 80 mL/min).
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment Of Fertility
Studies in animals to evaluate the carcinogenic potential of morphine sulfate have not been conducted. No formal studies to assess the mutagenic potential of morphine sulfate have been conducted. In the published literature, the results of in vitro studies showed that morphine sulfate is non-mutagenic in the Drosophila melanogaster lethal mutation assay and produced no evidence of chromosomal aberrations when incubated with murine splenocytes. Contrary to these results, morphine sulfate was found to increase DNA fragmentation when incubated in vitro with a human lymphoma line. In vivo, morphine sulfate has been reported to produce an increase in the frequency of micronuclei in bone marrow cells and immature red blood cells in the mouse micronucleus test and to induce chromosomal aberrations in murine lymphocytes and spermatids. Some of the in vivo clastogenic effects reported with morphine sulfate in mice may be directly related to increases in glucocorticoid levels produced by morphine sulfate in this species.
A literature report indicated that morphine sulfate impairs fertility in rats. In a fertility study in which male rats were administered morphine sulfate subcutaneous prior to mating (up to 30 mg/kg twice daily) and during mating (20 mg/kg twice daily) with untreated females, a number of adverse reproductive effects were observed. These included reduction in total pregnancies, higher incidence of pseudopregnancies, and reduction in implantation sites.
16 HOW SUPPLIED/STORAGE AND HANDLING
Morphine Sulfate Oral Solution
Morphine Sulfate Oral Solution is a green solution available in two strengths as follows:
10 mg per 5 mL Oral Solution
NDC 0054-0237-55: Four shelf packs per shipper: Unit dose Patient Cup™ filled to deliver 5 mL (10 mg Morphine Sulfate), ten 5 mL Patient Cups™ per shelf pack
NDC 0054-0237-49: Bottles of 100 mL
NDC 0054-0237-63: Bottles of 500 mL
20 mg per 5 mL Oral Solution
NDC 0054-0238-49: Bottles of 100 mL
NDC 0054-0238-63: Bottles of 500 mL
Morphine Sulfate Tablets
15 mg Tablet: white, biconvex tablets scored on one side and product identification "54 733" debossed on the other side.
Unit dose, 25 tablets per card
NDC 0054-0235-24: 4 Cards Per Carton
NDC 0054-0235-25: Bottle of 100 Tablets
30 mg Tablet: white, biconvex tablets scored on one side and product identification "54 262" debossed on the other side.
Unit dose, 25 tablets per card
NDC 0054-0236-24: 4 Cards Per Carton
NDC 0054-0236-25: Bottle of 100 Tablets
Storage
Store at Controlled Room Temperature, 15° to 30°C (59° to 86°F).
PROTECT FROM MOISTURE.
All opioids are liable to diversion and misuse both by the general public and healthcare workers and should be handled accordingly.
17 PATIENT COUNSELING INFORMATION
Patients receiving morphine sulfate should be given the following instructions by the physician:
- Patients should be advised that morphine sulfate is a narcotic pain reliever, and should be taken only as directed.
- The dose of morphine sulfate should not be adjusted without consulting with a physician or other healthcare professional.
- Patients should be advised that morphine sulfate may cause drowsiness, dizziness, or lighheadedness and may impair mental and/or physical ability required for the performance of potentially hazardous tasks (e.g., driving, operating machinery). Patients started on morphine sulfate or patients whose dose has been adjusted should refrain from any potentially dangerous activity until it is established that they are not adversely affected.
- Morphine sulfate will add to the effect of alcohol and other CNS depressants (such as antihistamines, sedatives, hypnotics, tranquilizers, general anesthetics, phenothiazines, other opioids, and monoamine oxidase [MAO] inhibitors).
- Patients should not combine morphine sulfate with alcohol or other central nervous system depressants (sleep aids, tranquilizers) except by the orders of the prescribing physician, because dangerous additive effects may occur, resulting in serious injury or death.
- Women of childbearing potential who become or are planning to become pregnant should consult a physician prior to initiating or continuing therapy with morphine sulfate.
- Safe use in pregnancy has not been established. Prolonged use of opioid analgesics during pregnancy may cause fetal-neonatal physical dependence, and neonatal withdrawal may occur.
- If patients have been receiving treatment with morphine sulfate for more than a few weeks and cessation of therapy is indicated, they should be counseled on the importance of safely tapering the dose and that abruptly discontinuing the medication could precipitate withdrawal symptoms. The physician should provide a dose schedule to accomplish a gradual discontinuation of the medication.
- Patients should be advised that morphine sulfate is a potential drug of abuse. They should protect it from theft. It should never be given to anyone other than the individual for whom it was prescribed.
- Patients should be instructed to keep morphine sulfate in a secure place out of the reach of children. When morphine sulfate is no longer needed, the unused capsules should be destroyed by flushing down the toilet.
- As with other opioids, patients taking morphine sulfate should be advised of the potential for severe constipation; appropriate laxatives and/or stool softeners as well as other appropriate treatments should be initiated from the onset of opioid therapy.
- Patients should be advised of the most common adverse events that may occur while taking morphine sulfate: constipation, nausea, somnolence, lightheadedness, dizziness, sedation, vomiting, and sweating.
©RLI, 2008

| Morphine Sulfate (Morphine Sulfate) | |||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||||||||
| Morphine Sulfate (Morphine Sulfate) | |||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||
|
|||||||||||||||||||||||||||||||
| Morphine Sulfate (Morphine Sulfate) | |||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
| Morphine Sulfate (Morphine Sulfate) | |||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
Revised: 04/2008Roxane Laboratories, Inc.