COLCHICINE
-
colchicine tablet
West-ward Pharmaceutical Corp
----------
|
|||||||||||||||||||||
FULL PRESCRIBING INFORMATION
1. INDICATION AND USAGE
Colchicine is indicated for prophylaxis of gout flares in adults.
2. DOSAGE AND ADMINISTRATION
The dosage for adults and adolescents older than 16 years of age is 0.6 mg (one tablet) once or twice daily. Maximum dose 1.2 mg/day.
Dosage reduction should be carefully considered in patients with impaired hepatic or renal function and in patients who are receiving concomitant treatment with P-gp and CYP3A4 inhibitors.
Colchicine tablets are administered orally, without regard to meals.
Colchicine is not an analgesic medication and should not be used to treat pain from other causes.
The safety and efficacy of colchicine in children to reduce the incidence of acute gout flares has not been evaluated.
3. DOSAGE FORMS AND STRENGTHS
0.6 mg tablets ― white, round, unscored, shallow concave compressed tablets with WEST-WARD 201 debossed on tablet.
4. CONTRAINDICATIONS
Colchicine should not be prescribed to patients with a hypersensitivity to colchicine. Colchicine should not be prescribed to patients with impaired renal or hepatic function who are taking P-gp or strong CYP3A4 inhibitors..
5. WARNINGS AND PRECAUTIONS
5.1 General
In rare instances severe allergic reactions and anaphylaxis have been reported with the use of colchicine. Most of these rare allergic reactions have been reported to occur within several hours after readministration following prior usage of the drug. The appearance of hypersensitivity reactions requires cessation of therapy with colchicine.
Both accidental and intentional overdoses with colchicine in children and adults have been reported [See OVERDOSE (10)]. Keep Colchicine Tablets out of the reach of children.
5.2 Renal Impairment
Colchicine is significantly excreted in urine in healthy subjects. Clearance of Colchicine is decreased in patients with impaired renal function. Consideration should be given to the reduction of the dosage in patients with renal impairment. Patients with any degree of renal dysfunction, who are treated with Colchicine, should be monitored closely for adverse effects of Colchicine.
5.3 Hepatic Impairment
The clearance of Colchicine may be significantly reduced and plasma half-life prolonged in patients with chronic hepatic impairment, compared to healthy subjects. Consideration should be given to the reduction of the dosage in patients with hepatic impairment. All patients with hepatic impairment should be monitored closely for adverse effects of Colchicine.
5.4 Drug Interactions
[see DRUG INTERACTIONS in section 7]
6. ADVERSE REACTIONS
The most frequent adverse effects of oral colchicine in therapeutic doses are those involving the gastrointestinal tract with diarrhea, nausea, vomiting, and abdominal pain often being the first signs of toxicity and the first indication that the colchicine dose may need to be reduced or therapy stopped. Larger doses may cause profuse diarrhea, gastrointestinal hemorrhage, skin rashes, renal and hepatic damage. Bone marrow suppression with agranulocytosis, thrombocytopenia, and aplastic anemia have rarely occurred with prolonged treatment, as have peripheral neuropathy, myopathy, rashes, and alopecia.
Side effects due to Colchicine appear to be a function of dosage. The possibility of increased colchicine toxicity in the presence of renal or hepatic dysfunction should be considered.
7 DRUG INTERACTIONS
Since colchicine is metabolized by cytochrome P (CYP) 3A4 demethylation in the liver, it may interact with substrates of this enzyme system, including estrogen, steroids, dapsone, diltiazem, erythromycin, lidocaine, lovastatin (and most other statins), midazolam, quinidine, terfenadine, testosterone, nifedipine, and verapamil. It may also be affected by inhibitors of this enzyme system, such as diltiazem, gestodene, grapefruit juice, ketoconazole, toleadomycin, and erythromycin. (Ben-Chetrit & Levy, 2003)(Hsu, Chen, Chang, & Chiu, 2002) (Holtzman, Wiggins, & Spinler, 2006)P-glycoprotein modulators or substrates that may interact with colchicine include morphine, doxorubicin, vinblastine, vincristine, paclitaxel, digoxin, quinidine, amprenavir, indinavir, nelfinavir, ritonavir, saquinavir, loperamide, josamycin, erythromycin, clarithromycin, cyclosporine, aldosterone, dexamethasone, prednisolone, progesterone, verapamil, talinolol, fexofenadine, cimetidine, amitriptyline, nortriptyline, phenytoin, and simvastatin. (Niel & Scherrmann, 2006)
Administration of colchicine with macrolide antibiotics such as clarithromycin impairs colchicine elimination, resulting in excess drug accumulation and toxicity, (Akdag, Erosy, Kahvecioglu, Gullulu, & Dilek, 2006) (Rollot, Pajot, Chauvelot-Moachon, Nazal, Kelaidi, & Blanche, 2004)Acute myopathy has been reported when colchicine is used with pravastatin. (Alayli, Cengiz, Canturk, Durmus, Akyol, & Menkse, 2005) (Hung, et al., 2005) Rhabdomylosis has been reported when colchicine was used with atorvastatin. (Tufan, Cavus, Altintas, Iskit, & Topeli, 2006)
When used for long periods of time, such as in the treatment of familial Meditarranean fever, colchicine can alter drug absorption and cause gastrointestinal effects such as lactose intolerance. (Ben-Chetrit & Levy, 2003)The available data suggest a dosage adjustment is necessary with strong CYP3A4 and P-gp inhibitors.
8. USE IN SPECIFIC POPULATIONS
8.1 Use in Pregnancy
Colchicine is an FDA Pregnancy Category C Drug. There are no adequate and well-controlled studies with colchicine in pregnant women. Colchicine crosses the human placenta. Published animal reproduction and development studies indicate that colchicine causes embryofetal toxicity, teratogenicity, and altered postnatal development at exposures within or above the clinical therapeutic range. Colchicine Tablets should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
8.2 Labor and Delivery
The effect of colchicine on labor and delivery is not known.
8.3 Use in Nursing Mothers
Colchicine is excreted into human milk. Limited information suggests that exclusively breastfed infants receive less than 10 percent of the maternal weight-adjusted dose. While there are no published reports of adverse effects in breast-feeding infants of mothers taking colchicine, colchicine can affect gastrointestinal cell renewal and permeability. Caution should be exercised and breastfeeding infants should be observed for adverse effects when colchicine is administered to a nursing woman.
8.4 Pediatric Use
Gout is rare in pediatric patients,. Safety and effectiveness of colchicine in pediatric patients has not been established.
8.4 Geriatric Use
Because of the increased incidence of decreased renal function in the elderly population, and the higher incidence, in the elderly population, of other co-morbid conditions, which often require the use of other medications, it is essential to carefully consider the need for a reduction in the dosage of Colchicine, when elderly patients are treated with Colchicine.
8.5 Use in Patients with Renal Dysfunction
Please see WARNINGS AND PRECAUTIONS for discussion of usage in patients with Renal or Hepatic Dysfunction.
8.6 Use in Patients with Hepatic Dysfunction
Please see WARNINGS AND PRECAUTIONS for discussion of usage in patients with Renal or Hepatic Dysfunction.
9. DRUG ABUSE AND DEPENDENCE
Tolerance, abuse, or dependence from colchicine has not been reported.
10. OVERDOSAGE
The dose of colchicine that induces significant toxicity isnot known. Fatalities have been reported in patients after ingesting a dose as low as 7 mg over a 4-day period, while other patients have reportedly survived after ingesting more than 60 mg. A review of 150 patients who overdosed on colchicine found that those who ingested less than 0.5 mg/kg survived and tended to have milder adverse reactions, such as gastrointestinal symptoms, whereas those who ingested from 0.5 to 0.8 mg/kg had more severe adverse reactions, including myelosuppression. There was 100% mortality among patients who ingested more than 0.8 mg/kg.
- The first stage of acute colchicine toxicity typically begins within 24 hours of ingestion and includes gastrointestinal symptoms, such as abdominal pain, nausea, vomiting, diarrhea, and significant fluid loss, leading to volume depletion. Peripheral leukocytosis may also be seen.
- Life-threatening complications occur during the second stage, which occurs 24 to 72 hours after drug administration, attributed to multi-organ failure and its associated consequences. Death usually results from respiratory depression and cardiovascular collapse. If the patient survives, recovery of multi-organ injury may be accompanied by rebound leukocytosis and alopecia starting about 1 week after the initial ingestion.
- Treatment of colchicine overdose should begin with gastric lavage and measures to prevent shock. Otherwise, treatment is symptomatic and supportive. No specific antidote is known. Colchicine is not effectively removed by dialysis.
11. DESCRIPTION
Colchicine is an alkaloid obtained from the plant Colchicum autumnale.
The chemical name for colchicine is (S)-N-(5,6,7,9- tetrahydro-1,2,3,10-tetramethoxy-9-oxobenzol[α]heptalen-7-yl) acetamide. The structural formula is represented below:
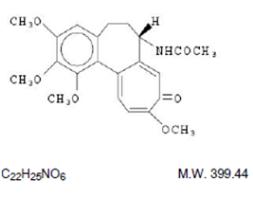
Colchicine consists of pale yellow scales or powder; it darkens on exposure to light. Colchicine is soluble in water, freely soluble in alcohol and in chloroform, and slightly soluble in ether.
Each tablet contains 0.6 mg (1/100 grain) colchicine USP and the following inactive ingredients: colloidal silicon dioxide, lactose anhydrous, magnesium stearate, microcrystalline cellulose, and sodium starch glycolate.
12. CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Colchicine’s effectiveness as a treatment for gout has been postulated to be due to its ability to block neutrophil-mediated inflammatory responses induced by monosodium urate crystals in synovial fluid by disrupting the function of the neutrophil’s cytoskeleton and interfering with microtubule assembly. This results in the prevention of activation, degranulation, and migration of neutrophils to sites of inflammation. New evidence suggests that colchicine may interfere with the intracellular assembly of the inflammasome complex found in neutrophils and monocytes that mediate IL-1b activation.
Colchicine is predominantly eliminated by biliary excretion and through the stool; gastrointestinal tract lining cell turnover has a variable role in colchicine elimination. Colchicine is extruded from cells, including the enteric lining cells, into the gastrointestinal tract, mediated by the multidrug resistance transporter molecule ABCB1 (full name: ATP-binding cassette subfamily B member, 1, MDRI, PGYI; also known as P-glycoprotein [P-gp] or CD243). Normally, a lesser but significant role in colchicine metabolism (-5 to 20%) is played by enteric and hepatic cytochrome P450 3E4 (CYP3A4), which catalyzes demethylation of colchicine to inactive metabolites. Hepatic demethylation of colchicine dependent on CYP3A4 occurs before hepatobiliary excretion of colchicine.
Renal elimination has been estimated to be responsible for 10 to 20% of drug disposition in normal subjects. CYP3A4 and renal disposition of colchicine become more critical with certain drug-drug interactions that affect ABCB 1, with hepatobiliary dysfunction and with aging.
Colchicine is not removed by hemodialysis.
12.2 Pharmacokinetics
Absorption
In healthy adults, colchicine appears to be readily absorbed when orally administered. When Colchicine Tablets 0.6 mg were administered to 18 healthy volunteers, a Cmax of about 2 ng/Ml at a tmax of 1 hou was observed.
Distribution
Colchicine is lipid-soluble and has a mean apparent volume of distribution in healthy young volunteers of approximately 5 to 8 L/kg. Colchicine binding to serum protein is 39% (plus or minus 5%), and binds primarily to albumin; it crosses the placenta and distributes into breast milk.
Metabolism
There are two primary metabolites, 2-O-demethylcolchicine and 3-O-demethylcolchicine (known as 2- and 3-DMC, respectively), and one minor metabolite, 10-O-demethylcolchicine (also known as 10-DMC or colchiceine). Human liver microsomes studies have shown that CYP3A4 is involved in the metabolism of colchicine to 2- and 3-DMC. In vivo, exposure to 2-DMC and 3-DMC metabolites is less than 5% of parent drug.
13. NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Carcinogenicity studies of colchicine have not been evaluated. Due to the potential for colchicine to produce aneuploid cells (cells with an unequal number of chromosomes), colchicine presents a theoretical increased risk of malignancy.
Mutagenesis
Colchicine was negative for mutagenicity in the bacterial reverse mutation assay. In a chromosomal aberration assay in cultured human white blood cells, colchicine treatment resulted in the formation of micronuclei. Since published studies demonstrated that colchicine induces aneuploidy from the process of mitotic nondisjunction without structural DNA changes, colchicine is not considered clastogenic, although micronuclei are formed.
Impairment of Fertility
Published nonclinical studies demonstrated that colchicine-induced disruption of microtubule formation affects meiosis and mitosis. Reproductive studies also reported abnormal sperm morphology and reduced sperm counts in males, and interference with sperm penetration, second meiotic division, and normal cleavage in females when exposed to colchicine. Colchicine administered to pregnant animals resulted in fetal death and teratogenicity. These effects were dose dependent, with the timing of exposure critical for the effects on embryofetal development. The nonclinical doses evaluated were generally higher than an equivalent human therapeutic dose, but safety margins for reproductive and developmental toxicity could not be determined. There are published studies that show that men and women taking colchicine can safely have children.
Case reports and epidemiology studies in human male subjects on colchicine therapy indicated that infertility from colchicine is rare. A case report indicated that azoospermia was reversed when therapy was stopped. Case reports and epidemiology studies in female subjects on colchicine therapy have not established a clear relationship between colchicine use and female infertility.
15. REFERENCES
Akdag, I., Erosy, A., Kahvecioglu, S., Gullulu, M., & Dilek, K. (2006). Acute colchicine intoxication during clarithromycin administration in patients with chronic renal failure. Journal of Nephrology , 19, 515-517.
Alayli, G., Cengiz, K., Canturk, F., Durmus, D., Akyol, Y., & Menkse, E. (2005). Acute Myopathy in a Patient with Concomitant Use of Pravastatin and Colchicine. The Annals of Pharmacology , 39, 1358-1361.
Ben-Chetrit, D., & Levy, M. (2003). Reproductive system in familial Mediterranean fever: an overview. Annals of Rheumatic Diseases , 62, 916-919.
Holtzman, C., Wiggins, B., & Spinler, S. (2006). Role of P-glycoprotein in Statin Drug Interactions. Pharmacotherapy , 26 (11), 1601-1607.
Hsu, W.-C., Chen, W.-H., Chang, M.-T., & Chiu, H.-C. (2002). Colchicine-Induced Acute Myopathy in a Patient with Concomitant Use of Simvastatin. Clinical Neuropharmacology , 25 (5), 266-268.
Hung, I., Wu, A. C., Tang, B., To, K., Yeung, C., Woo, P., et al. (2005). Fatal Interaction between Clarithromycin and Colchicine in Patients with Renal Insufficiency; A Retrospective Study. Clinical Infectious Diseases , 41, 291-300.
Niel, E., & Scherrmann, J.-M. (2006). Colchicine today. Joint Bone Spine , 73, 672-678.
Rollot, F., Pajot, O., Chauvelot-Moachon, L., Nazal, E., Kelaidi, C., & Blanche, P. (2004). Acute Colchicine Intoxication During Clarithromycin Administration. The Annals of Pharmacotherapy , 38, 2074-2077.
Tufan, A. D., Cavus, S., Altintas, N., Iskit, A., & Topeli, A. (2006). Rhabdomyolysis in a Patient Treated with Colchicine and Atorvastatin. The Annals of Pharmacotherapy , 40, 1466-1469.
16. HOW SUPPLIED STORAGE AND HANDLING
16.1 How Supplied
Colchicine Tablets, USP 0.6 mg are white, round, unscored, shallow concave compressed tablets with WEST-WARD 201on the tablets.
Bottles of 100 tablets
Bottles of 1000 tablets
16.2 Storage
Store at 20° to 25° C (68° to 77° F).
[See USP Controlled Room Temperature]
Protect from light.
17. PATIENT COUNSELING
See Colchicine Medication Guide
17.1 Dosing Instructions
1 Patients should be counseled to continue to take Colchicine Tablets, even if they are no longer in pain. They should be told to consult their health care professional before stopping use of Colchicine Tablets. If a dose is missed patients may take it within 6 hours of their normal dose, or skip the dose and return to their normal schedule if more than 6 hours have passed. Emphasize to patients not to double the next dose if they skip a dose, as gastrointestinal symptoms may occur.
17.2 Blood Dyscrasias
Patients should be told that colchicine can cause bone marrow suppression with anemia and low platelets, as well as agranulocytosis.
17.3 Drug and Food Interactions
Patients should be made aware that many drugs and other substances can interact with colchicine; sometimes these interactions might be fatal. They should be told to check make sure their health care professional knows every drug and supplement they are taking, and to check with him or her before starting any new medications or supplements, including over-the-counter products. They should be told not to drink grapefruit juice or eat grapefruit.
17.4 Neuromuscular Toxicity
Patients should be told that muscle weakness or pain, tingling or numbness in fingers or toes are signs of problems with colchicine. They should be instructed that if this occurs, they discontinue colchicine therapy and seek immediate medical evaluation.
Manufactured and Distributed by:
West-Ward Pharmaceutical Corp.
Tel: +1 732 542 1191
Fax: +1 732 542 0940
Prepared September 2010
Colchicine Medication Guide
This Medication Guide provides some important general information about Colchicine. However, it is very important for you to see your physician on a regular basis while taking Colchicine and to discuss any concerns or questions that you have with your physician.
What is Colchicine?
- Colchicine is a prescription medication that is used to reduce the incidence of Acute Gout Flares in patients with an established diagnosis of Gout
What is the most important information I should know about Colchicine?
- Colchicine can cause serious side effects or even death if Colchicine levels are too high in your body.
- You must keep Colchicine out of the reach of children at all times.
- Colchicine is not a pain medicine and it should not be taken to treat pain related to conditions other than the condition for which your physician prescribed it.
Who should not take Colchicine?
- You should not take Colchicine if you have had an allergic reaction to Colchicine in the past.
- You should not take Colchicine if you have liver or kidney problems and you take certain other medicines (See Below).
What should I discuss with my healthcare provider before taking Colchicine?
- Before taking Colchicine it is essential to tell your healthcare provider about all of your medical problems and health conditions. It is especially important to tell your physician about the following:
• Any history of kidney or liver problems.
• If you are pregnant or plan to become pregnant, because Colchicine is in the FDA pregnancy category C, and this means that it is not known whether Colchicine will harm an unborn baby. Therefore, do not take Colchicine if you are pregnant, without first consulting with your physician.
• If you are breast feeding, because Colchicine passes into breast milk. Therefore, do not take Colchicine without first consulting with your doctor if you are breast-feeding a baby.
• Every medication (including vitamins, herbal products, etc.) that you currently take or have recently taken, because certain medicines when taken with Colchicine can cause a buildup of abnormally high levels of Colchicine in your body. Keep in mind that:
• Colchicine and other medicines may affect each other causing serious side effects or even death, so it is important that you consult with your physician before taking any new medication.
• Even medications (e.g., antibiotics) that you take for short periods may interact with Colchicine and cause serious side effects or death.
• Medications that can cause particularly serious problems when taken with Colchicine include the following:
○ Clarithromycin
○ Telithromycin
○ Cyclosporin
○ Ketoconazole
○ Itraconazole
○ HIV Protease Inhibitors
○ Nefazodone
○ Cholesterol Lowering Medications
○ Digoxin
How should I take Colchicine?
- Take Colchicine exactly as directed by your doctor. If you do not understand these directions, ask your physician or pharmacist to explain them to you.
- Colchicine can be taken with or without food.
- Do not stop taking Colchicine even if you start to feel better, unless you are told to do so by your doctor.
What happens if I miss a dose?
- Take the missed dose as soon as you remember. However, if it is almost time for your next dose, skip the dose that you missed and take only your next regularly scheduled dose. Do not take a double dose of this medication.
What should I do if I overdose?
- If you take too much Colchicine go to the nearest hospital emergency room immediately.
What should I avoid while taking Colchicine?
- Avoid eating grapefruit or drinking grapefruit juice while taking Colchicine. It can increase your chances of getting serious side effects.
What are the possible side effects of Colchicine?
- The most common side effects of Colchicine are diarrhea, nausea, vomiting, and abdominal pain. Other less common side effects include:
○ Muscle weakness or pain
○ Numbness or tingling in your fingers or toes
○ Unusual bleeding or bruising
○ Increased infections
○ Weakness or fatigue
○ Pale or gray color to your lips, tongue, or palms of your hands
- These are not all of the possible side effects of Colchicine, and it is important to consult with your physician if you develop any side effect that that does not resolve quickly.
- You may report side effects to FDA at 1-800-FDA-1088.
How should I store Colchicine?
- Store Colchicine at room temperature between 68° and 77° F (20° to 25°C).
- Keep Colchicine in a tightly closed container.
- Keep Colchicine out of the light.
- Keep Colchicine and all medicines out of the reach of children.
General Information about Colchicine:
Physicians sometimes prescribe medications for conditions other than those listed in a Medication Guide. You should only use Colchicine for the condition for which it was prescribed for you. You should never give your Cholchicine to other people, although their symptoms may appear to be similar to yours, because this could be harmful to the other person. While this Medication Guide provides a summary of important information about Colchicine, you should consult with your physician or pharmacist if you need more detailed information.
What are the active ingredients in Colchicine?
Active Ingredient: Colchicine 0.6 mg, USP
Inactive Ingredients: colloidal silicon dioxide, lactose anhydrous, magnesium stearate, microcrystalline cellulose and sodium starch glycolate.
Manufacturer: West-Ward Pharmaceutical Corp.
PRINCIPAL DISPLAY PANEL
NDC 0143-1201-01
Colchicine
Tablets, USP
0.6 mg
Rx Only
6505-01-083-5984
100 TABLETS
Manufactured by:
West-ward Pharmaceutical Corp.
Eatontown, NJ 07724

| COLCHICINE
colchicine tablet |
|||||||||||||||||||||
|
|||||||||||||||||||||
|
|||||||||||||||||||||
|
|||||||||||||||||||||
|
|||||||||||||||||||||
|
|||||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| UNAPPROVED DRUG OTHER | 10/08/1990 | 12/28/2010 | |
| Labeler - West-ward Pharmaceutical Corp (001230762) |
| Establishment | |||
| Name | Address | ID/FEI | Operations |
| West-ward Pharmaceutical Corp | 001230762 | MANUFACTURE | |