EPOPROSTENOL
-
epoprostenol powder, for solution
Actelion Pharmaceuticals US, Inc.
----------
|
|||||||||||||||||||||
FULL PRESCRIBING INFORMATION
1 INDICATIONS AND USAGE
Epoprostenol is indicated for:
- the long-term intravenous treatment of primary pulmonary hypertension
- and pulmonary hypertension associated with the scleroderma spectrum of disease in NYHA Class III and Class IV patients who do not respond adequately to conventional therapy
- [see CLINICAL STUDIES: Clinical Trials in Pulmonary Hypertension (14.1)].
2 DOSAGE AND ADMINISTRATION
Important Note: Epoprostenol for Injection must be reconstituted only as directed with Sterile Water for Injection, USP, or Sodium Chloride 0.9% Injection, USP. Reconstituted solutions of Epoprostenol for Injection must not be diluted or administered with other parenteral solutions or medications [see WARNINGS AND PRECAUTIONS: General (5.1)].
2.1 Dosage
Continuous chronic infusion of epoprostenol should be prepared as directed [see Reconstitution (2.4)], and administered through a central venous catheter. Temporary peripheral intravenous infusion may be used until central access is established. Chronic infusion of epoprostenol should be initiated at 2 ng/kg/min and increased in increments of 2 ng/kg/min every 15 minutes or longer until dose-limiting pharmacologic effects are elicited or until a tolerance limit to the drug is established or further increases in the infusion rate are not clinically warranted [see Dosage Adjustments (2.2)]. If dose-limiting pharmacologic effects occur, then the infusion rate should be decreased to the point that the pharmacologic effects of epoprostenol are tolerated. In clinical trials, the most common dose-limiting adverse events were nausea, vomiting, hypotension, sepsis, headache, abdominal pain, or respiratory disorder (most treatment-limiting adverse events were not serious). If the initial infusion rate of 2 ng/kg/min is not tolerated, use a lower dose.
In the controlled 12-week trial in PH/SSD, for example, the dose increased from a mean starting dose of 2.2 ng/kg/min. During the first 7 days of treatment, the dose was increased daily to a mean dose of 4.1 ng/kg/min on day 7 of treatment. At the end of week 12, the mean dose was 11.2 ng/kg/min. The mean incremental increase was 2 to 3 ng/kg/min every 3 weeks.
2.2 Dosage Adjustments
Changes in the chronic infusion rate should be based on persistence, recurrence, or worsening of the patient's symptoms of pulmonary hypertension and the occurrence of adverse events due to excessive doses of epoprostenol. In general, increases in dose from the initial chronic dose should be expected.
Increments in dose should be considered if symptoms of pulmonary hypertension persist or recur after improving. The infusion should be increased by 1- to 2-ng/kg/min increments at intervals sufficient to allow assessment of clinical response; these intervals should be at least 15 minutes. In clinical trials, incremental increases in dose occurred at intervals of 24 to 48 hours or longer. Following establishment of a new chronic infusion rate, the patient should be observed, and standing and supine blood pressure and heart rate monitored for several hours to ensure that the new dose is tolerated.
During chronic infusion, the occurrence of dose-limiting pharmacological events may necessitate a decrease in infusion rate, but the adverse event may occasionally resolve without dosage adjustment. Dosage decreases should be made gradually in 2-ng/kg/min decrements every 15 minutes or longer until the dose-limiting effects resolve. Abrupt withdrawal of epoprostenol or sudden large reductions in infusion rates should be avoided. Except in life-threatening situations (e.g., unconsciousness, collapse, etc.), infusion rates of epoprostenol should be adjusted only under the direction of a physician.
In patients receiving lung transplants, doses of epoprostenol were tapered after the initiation of cardiopulmonary bypass.
2.3 Administration
Epoprostenol for Injection, once prepared as directed [see Reconstitution (2.4)], is administered by continuous intravenous infusion via a central venous catheter using an ambulatory infusion pump. During initiation of treatment, epoprostenol may be administered peripherally.
The ambulatory infusion pump used to administer epoprostenol should: (1) be small and lightweight, (2) be able to adjust infusion rates in 2-ng/kg/min increments, (3) have occlusion, end-of-infusion, and low-battery alarms, (4) be accurate to ±6% of the programmed rate, and (5) be positive pressure-driven (continuous or pulsatile) with intervals between pulses not exceeding 3 minutes at infusion rates used to deliver epoprostenol. The reservoir should be made of polyvinyl chloride, polypropylene, or glass. The infusion pump used in the most recent clinical trials was the CADD-1 HFX 5100 (SIMS Deltec). A 60-inch microbore non-DEHP extension set with proximal antisyphon valve, low priming volume (0.9 mL), and in-line 0.22 micron filter was used during clinical trials.
To avoid potential interruptions in drug delivery, the patient should have access to a backup infusion pump and intravenous infusion sets. A multi-lumen catheter should be considered if other intravenous therapies are routinely administered.
2.4 Reconstitution
Epoprostenol for Injection is stable only when reconstituted as directed using Sterile Water for Injection, USP, or Sodium Chloride 0.9% Injection, USP. Epoprostenol for Injection must not be reconstituted or mixed with any other parenteral medications or solutions prior to or during administration.
Prior to use, Epoprostenol for Injection solutions reconstituted with 5 mL diluent must be protected from light and can be refrigerated at 2° to 8°C (36° to 46°F) for as long as 5 days or held at up to 25°C (77°F) for up to 48 hours prior to use. Do not freeze reconstituted solutions of Epoprostenol for Injection. Discard any reconstituted solution that has been frozen. Discard any reconstituted solution if it has been refrigerated for more than 5 days, or if held at room temperature for more than 48 hours.
During use, a single reservoir of diluted solution of Epoprostenol for Injection prepared as directed can be administered at room temperature for up to 24 hours. (If lower concentrations are chosen, pump reservoirs should be changed every 12 hours when administered at room temperature.) Do not expose this solution to direct sunlight.
A concentration for the solution of epoprostenol should be selected that is compatible with the infusion pump being used with respect to minimum and maximum flow rates, reservoir capacity, and the infusion pump criteria listed above. Epoprostenol, when administered chronically, should be prepared in a drug delivery reservoir appropriate for the infusion pump. Outlined in Table 1 are directions for preparing different concentrations of epoprostenol for up to a 24-hour period.
| To make 100 mL of solution with Final Concentration (ng/mL) of: | Directions: |
|---|---|
|
|
| 15,000 ng/mL* | Dissolve contents of one 1.5 mg vial with 5 mL of Sterile Water for Injection, USP, or Sodium Chloride 0.9% Injection, USP. Withdraw entire vial contents and add to a sufficient volume of the identical diluent to make a total of 100 mL. |
| 30,000 ng/mL* | Dissolve contents of two 1.5 mg vials each with 5 mL of Sterile Water for Injection, USP, or Sodium Chloride 0.9% Injection, USP. Withdraw entire vial contents and add to a sufficient volume of the identical diluent to make a total of 100 mL. |
Infusion rates may be calculated using the following formula:
| Infusion Rate (mL/hr) = | [Dose (ng/kg/min) × Weight (kg) × 60 min/hr] |
| Final Concentration (ng/mL) |
Tables 2 and 3 provide infusion delivery rates for doses up to 16 ng/kg/min based upon patient weight, drug delivery rate, and concentration of the solution of epoprostenol to be used. These tables may be used to select the most appropriate concentration of epoprostenol that will result in an infusion rate between the minimum and maximum flow rates of the infusion pump and that will allow the desired duration of infusion from a given reservoir volume. For infusion/dose rates lower than those listed in Tables 2 and 3, it is recommended that the pump rate be set by a healthcare professional such that steady state is achieved in the patient, keeping in mind the half life of epoprostenol is no more than six minutes. Higher infusion rates, and therefore, more concentrated solutions may be necessary with long-term administration of epoprostenol. If lower concentrations are chosen, pump reservoirs should be changed every 12 hours when administered at room temperature.
| Dose or Drug Delivery Rate (ng/kg/min) | |||||||
|---|---|---|---|---|---|---|---|
| Patient weight (kg) | 4 | 6 | 8 | 10 | 12 | 14 | 16 |
| Infusion Delivery Rate (mL/hr) | |||||||
| 20 | --- | --- | --- | --- | 1.0 | 1.1 | 1.3 |
| 30 | --- | --- | 1.0 | 1.2 | 1.4 | 1.7 | 1.9 |
| 40 | --- | 1.0 | 1.3 | 1.6 | 1.9 | 2.2 | 2.6 |
| 50 | --- | 1.2 | 1.6 | 2.0 | 2.4 | 2.8 | 3.2 |
| 60 | 1.0 | 1.4 | 1.9 | 2.4 | 2.9 | 3.4 | 3.8 |
| 70 | 1.1 | 1.7 | 2.2 | 2.8 | 3.4 | 3.9 | 4.5 |
| 80 | 1.3 | 1.9 | 2.6 | 3.2 | 3.8 | 4.5 | 5.1 |
| 90 | 1.4 | 2.2 | 2.9 | 3.6 | 4.3 | 5.0 | 5.8 |
| 100 | 1.6 | 2.4 | 3.2 | 4.0 | 4.8 | 5.6 | 6.4 |
| Dose or Drug Delivery Rate (ng/kg/min) | ||||||
|---|---|---|---|---|---|---|
| Patient weight (kg) | 6 | 8 | 10 | 12 | 14 | 16 |
| 30 | --- | --- | --- | --- | --- | 1.0 |
| 40 | --- | --- | --- | 1.0 | 1.1 | 1.3 |
| 50 | --- | --- | 1.0 | 1.2 | 1.4 | 1.6 |
| 60 | --- | 1.0 | 1.2 | 1.4 | 1.7 | 1.9 |
| 70 | --- | 1.1 | 1.4 | 1.7 | 2.0 | 2.2 |
| 80 | 1.0 | 1.3 | 1.6 | 1.9 | 2.2 | 2.6 |
| 90 | 1.1 | 1.4 | 1.8 | 2.2 | 2.5 | 2.9 |
| 100 | 1.2 | 1.6 | 2.0 | 2.4 | 2.8 | 3.2 |
3 DOSAGE FORMS AND STRENGTHS
Epoprostenol for Injection contains epoprostenol sodium equivalent to 1.5 mg (1,500,000 ng) epoprostenol and is supplied as a sterile lyophilized material in a 10 mL vial with a red flip-off seal.
4 CONTRAINDICATIONS
A large study evaluating the effect of epoprostenol on survival in NYHA Class III and IV patients with congestive heart failure due to severe left ventricular systolic dysfunction was terminated after an interim analysis of 471 patients revealed a higher mortality in patients receiving epoprostenol plus conventional therapy than in those receiving conventional therapy alone. The chronic use of epoprostenol in patients with congestive heart failure due to severe left ventricular systolic dysfunction is therefore contraindicated.
Some patients with pulmonary hypertension have developed pulmonary edema during dose initiation, which may be associated with pulmonary veno-occlusive disease. Epoprostenol should not be used chronically in patients who develop pulmonary edema during dose initiation.
Epoprostenol is also contraindicated in patients with known hypersensitivity to the drug or to structurally related compounds.
5 WARNINGS AND PRECAUTIONS
5.1 General
Epoprostenol for Injection must be reconstituted only as directed using Sterile Water for Injection, USP, or Sodium Chloride 0.9% Injection, USP. Epoprostenol for Injection must not be reconstituted or mixed with any other parenteral medications or solutions prior to or during administration. [See Reconstitution (2.4)]
Epoprostenol should be used only by clinicians experienced in the diagnosis and treatment of pulmonary hypertension. The diagnosis of pulmonary hypertension should be carefully established.
5.2 Dose Initiation
Epoprostenol is a potent pulmonary and systemic vasodilator. Dose initiation with epoprostenol must be performed in a setting with adequate personnel and equipment for physiologic monitoring and emergency care. Dose initiation in controlled PPH clinical trials was performed during right heart catheterization. In clinical trials, dose initiation was performed without cardiac catheterization. The risk of cardiac catheterization in patients with pulmonary hypertension should be carefully weighed against the potential benefits. During dose initiation, asymptomatic increases in pulmonary artery pressure coincident with increases in cardiac output occurred rarely. In such cases, dose reduction should be considered, but such an increase does not imply that chronic treatment is contraindicated.
5.3 Chronic Use and Dose Adjustment
During chronic use, epoprostenol is delivered continuously on an ambulatory basis through a permanent indwelling central venous catheter. Unless contraindicated, anticoagulant therapy should be administered to PPH and PH/SSD patients receiving epoprostenol to reduce the risk of pulmonary thromboembolism or systemic embolism through a patent foramen ovale. In order to reduce the risk of infection, aseptic technique must be used in the reconstitution and administration of epoprostenol as well as in routine catheter care. Because epoprostenol is metabolized rapidly, even brief interruptions in the delivery of epoprostenol may result in symptoms associated with rebound pulmonary hypertension including dyspnea, dizziness, and asthenia. The decision to initiate therapy with epoprostenol should be based upon the understanding that there is a high likelihood that intravenous therapy with epoprostenol will be needed indefinitely, and the patient's ability to accept and care for a permanent intravenous catheter and infusion pump should be carefully considered.
Based on clinical trials, the acute hemodynamic response (reduction in pulmonary artery resistance) to epoprostenol did not correlate well with improvement in exercise tolerance or survival during chronic use of epoprostenol. Dosage of epoprostenol during chronic use should be adjusted at the first sign of recurrence or worsening of symptoms attributable to pulmonary hypertension or the occurrence of adverse events associated with epoprostenol [see DOSAGE AND ADMINISTRATION (2)]. Following dosage adjustments, standing and supine blood pressure and heart rate should be monitored closely for several hours.
5.4 Withdrawal Effects
Abrupt withdrawal (including interruptions in drug delivery) or sudden large reductions in dosage of epoprostenol may result in symptoms associated with rebound pulmonary hypertension, including dyspnea, dizziness, and asthenia. In clinical trials, one Class III primary pulmonary hypertension patient's death was judged attributable to the interruption of epoprostenol. Abrupt withdrawal should be avoided.
5.5 Sepsis
See ADVERSE REACTIONS, Adverse Events Attributable to the Drug Delivery System (6.1).
6 ADVERSE REACTIONS
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
During clinical trials, adverse events were classified as follows: (1) adverse events during dose initiation and escalation, (2) adverse events during chronic dosing, and (3) adverse events associated with the drug delivery system.
Adverse Events During Dose Initiation and Escalation
During early clinical trials, epoprostenol was increased in 2-ng/kg/min increments until the patients developed symptomatic intolerance. The most common adverse events and the adverse events that limited further increases in dose were generally related to vasodilation, the major pharmacologic effect of epoprostenol. The most common dose-limiting adverse events (occurring in ≥1% of patients) were nausea, vomiting, headache, hypotension, and flushing, but also include chest pain, anxiety, dizziness, bradycardia, dyspnea, abdominal pain, musculoskeletal pain, and tachycardia. Table 4 lists the adverse events reported during dose initiation and escalation in decreasing order of frequency.
| Adverse Events Occurring in ≥1% of Patients | Epoprostenol (n = 391) |
|---|---|
| Flushing | 58% |
| Headache | 49% |
| Nausea/vomiting | 32% |
| Hypotension | 16% |
| Anxiety, nervousness, agitation | 11% |
| Chest pain | 11% |
| Dizziness | 8% |
| Bradycardia | 5% |
| Abdominal pain | 5% |
| Musculoskeletal pain | 3% |
| Dyspnea | 2% |
| Back pain | 2% |
| Sweating | 1% |
| Dyspepsia | 1% |
| Hypesthesia/paresthesia | 1% |
| Tachycardia | 1% |
Adverse Events During Chronic Administration for PPH
Interpretation of adverse events is complicated by the clinical features of PPH and PH/SSD, which are similar to some of the pharmacologic effects of epoprostenol (e.g., dizziness, syncope). Adverse events probably related to the underlying disease include dyspnea, fatigue, chest pain, edema, hypoxia, right ventricular failure, and pallor. Several adverse events, on the other hand, can clearly be attributed to epoprostenol. These include headache, jaw pain, flushing, diarrhea, nausea and vomiting, flu-like symptoms, and anxiety/nervousness.
In an effort to separate the adverse effects of the drug from the adverse effects of the underlying disease, Table 5 lists adverse events that occurred at a rate at least 10% different in the 2 groups in controlled trials for PPH.
| Adverse Event | Epoprostenol (n = 52) | Conventional Therapy (n = 54) |
|---|---|---|
| Occurrence More Common With Epoprostenol | ||
| General | ||
| Chills/fever/sepsis/flu-like symptoms | 25% | 11% |
| Cardiovascular | ||
| Tachycardia | 35% | 24% |
| Flushing | 42% | 2% |
| Gastrointestinal | ||
| Diarrhea | 37% | 6% |
| Nausea/vomiting | 67% | 48% |
| Musculoskeletal | ||
| Jaw pain | 54% | 0% |
| Myalgia | 44% | 31% |
| Nonspecific musculoskeletal pain | 35% | 15% |
| Neurological | ||
| Anxiety/nervousness/tremor | 21% | 9% |
| Dizziness | 83% | 70% |
| Headache | 83% | 33% |
| Hypesthesia, hyperesthesia, paresthesia | 12% | 2% |
| Occurrence More Common With Standard Therapy | ||
| Cardiovascular | ||
| Heart failure | 31% | 52% |
| Syncope | 13% | 24% |
| Shock | 0% | 13% |
| Respiratory | ||
| Hypoxia | 25% | 37% |
Thrombocytopenia has been reported during uncontrolled clinical trials in patients receiving epoprostenol.
Table 6 lists additional adverse events reported in PPH patients receiving epoprostenol plus conventional therapy or conventional therapy alone during controlled clinical trials.
| Adverse Event | Epoprostenol (n = 52) | Conventional Therapy (n = 54) |
|---|---|---|
| General | ||
| Asthenia | 87% | 81% |
| Cardiovascular | ||
| Angina pectoris | 19% | 20% |
| Arrhythmia | 27% | 20% |
| Bradycardia | 15% | 9% |
| Supraventricular tachycardia | 8% | 0% |
| Pallor | 21% | 30% |
| Cyanosis | 31% | 39% |
| Palpitation | 63% | 61% |
| Cerebrovascular accident | 4% | 0% |
| Hemorrhage | 19% | 11% |
| Hypotension | 27% | 31% |
| Myocardial ischemia | 2% | 6% |
| Gastrointestinal | ||
| Abdominal Pain | 27% | 31% |
| Anorexia | 25% | 30% |
| Ascites | 12% | 17% |
| Constipation | 6% | 2% |
| Metabolic | ||
| Edema | 60% | 63% |
| Hypokalemia | 6% | 4% |
| Weight reduction | 27% | 24% |
| Weight gain | 6% | 4% |
| Musculoskeletal | ||
| Arthralgia | 6% | 0% |
| Bone pain | 0% | 4% |
| Chest pain | 67% | 65% |
| Neurological | ||
| Confusion | 6% | 11% |
| Convulsion | 4% | 0% |
| Depression | 37% | 44% |
| Insomnia | 4% | 4% |
| Respiratory | ||
| Cough increase | 38% | 46% |
| Dyspnea | 90% | 85% |
| Epistaxis | 4% | 2% |
| Pleural effusion | 4% | 2% |
| Skin and Appendages | ||
| Pruritus | 4% | 0% |
| Rash | 10% | 13% |
| Sweating | 15% | 20% |
| Special Senses | ||
| Amblyopia | 8% | 4% |
| Vision abnormality | 4% | 0% |
Adverse Events During Chronic Administration for PH/SSD
In an effort to separate the adverse effects of the drug from the adverse effects of the underlying disease, Table 7 lists adverse events that occurred at a rate at least 10% different in the 2 groups in the controlled trial for patients with PH/SSD.
| Adverse Event | Epoprostenol (n = 56) | Conventional Therapy (n = 55) |
|---|---|---|
| Occurrence More Common With Epoprostenol | ||
| Cardiovascular | ||
| Flushing | 23% | 0% |
| Hypotension | 13% | 0% |
| Gastrointestinal | ||
| Anorexia | 66% | 47% |
| Nausea/vomiting | 41% | 16% |
| Diarrhea | 50% | 5% |
| Musculoskeletal | ||
| Jaw pain | 75% | 0% |
| Pain/neck pain/arthralgia | 84% | 65% |
| Neurological | ||
| Headache | 46% | 5% |
| Skin and Appendages | ||
| Skin ulcer | 39% | 24% |
| Eczema/rash/urticaria | 25% | 4% |
| Occurrence More Common With Conventional Therapy | ||
| Cardiovascular | ||
| Cyanosis | 54% | 80% |
| Pallor | 32% | 53% |
| Syncope | 7% | 20% |
| Gastrointestinal | ||
| Ascites | 23% | 33% |
| Esophageal reflux/gastritis | 61% | 73% |
| Metabolic | ||
| Weight decrease | 45% | 56% |
| Neurological | ||
| Dizziness | 59% | 76% |
| Respiratory | ||
| Hypoxia | 55% | 65% |
Table 8 lists additional adverse events reported in PH/SSD patients receiving epoprostenol plus conventional therapy or conventional therapy alone during controlled clinical trials.
| Adverse Event* | Epoprostenol (n = 56) | Conventional Therapy (n = 55) |
|---|---|---|
|
||
| General | ||
| Asthenia | 100% | 98% |
| Hemorrhage/hemorrhage injection site/hemorrhage rectal | 11% | 2% |
| Infection/rhinitis | 21% | 20% |
| Chills/fever/sepsis/flu-like symptoms | 13% | 11% |
| Blood and Lymphatic | ||
| Thrombocytopenia | 4% | 0% |
| Cardiovascular | ||
| Heart failure/heart failure right | 11% | 13% |
| Myocardial Infarction | 4% | 0% |
| Palpitation | 63% | 71% |
| Shock | 5% | 5% |
| Tachycardia | 43% | 42% |
| Vascular disorder peripheral | 96% | 100% |
| Vascular disorder | 95% | 89% |
| Gastrointestinal | ||
| Abdominal enlargement | 4% | 0% |
| Abdominal pain | 14% | 7% |
| Constipation | 4% | 2% |
| Flatulence | 5% | 4% |
| Metabolic | ||
| Edema/edema peripheral/edema genital | 79% | 87% |
| Hypercalcemia | 48% | 51% |
| Hyperkalemia | 4% | 0% |
| Thirst | 0% | 4% |
| Musculoskeletal | ||
| Arthritis | 52% | 45% |
| Back pain | 13% | 5% |
| Chest pain | 52% | 45% |
| Cramps leg | 5% | 7% |
| Respiratory | ||
| Cough increase | 82% | 82% |
| Dyspnea | 100% | 100% |
| Epistaxis | 9% | 7% |
| Pharyngitis | 5% | 2% |
| Pleural effusion | 7% | 0% |
| Pneumonia | 5% | 0% |
| Pneumothorax | 4% | 0% |
| Pulmonary edema | 4% | 2% |
| Respiratory disorder | 7% | 4% |
| Neurological | ||
| Anxiety/hyperkinesia/nervousness/tremor | 7% | 5% |
| Depression/depression psychotic | 13% | 4% |
| Hyperesthesia/hypesthesia/paresthesia | 5% | 0% |
| Insomnia | 9% | 0% |
| Somnolence | 4% | 2% |
| Skin and Appendages | ||
| Collagen disease | 82% | 84% |
| Pruritus | 4% | 2% |
| Sweat | 41% | 36% |
| Urogenital | ||
| Hematuria | 5% | 0% |
| Urinary tract infection | 7% | 0% |
Although the relationship to epoprostenol administration has not been established, pulmonary embolism has been reported in several patients taking epoprostenol and there have been reports of hepatic failure.
Adverse Events Attributable to the Drug Delivery System
Chronic infusions of epoprostenol are delivered using a small, portable infusion pump through an indwelling central venous catheter. During controlled PPH trials of up to 12 weeks' duration, up to 21% of patients reported a local infection and up to 13% of patients reported pain at the injection site. During a controlled PH/SSD trial of 12 weeks' duration, 14% of patients reported a local infection and 9% of patients reported pain at the injection site. During long-term follow-up in the clinical trial of PPH, sepsis was reported at least once in 14% of patients and occurred at a rate of 0.32 infections/patient per year in patients treated with epoprostenol. This rate was higher than reported in patients using chronic indwelling central venous catheters to administer parenteral nutrition, but lower than reported in oncology patients using these catheters. Malfunctions in the delivery system resulting in an inadvertent bolus of or a reduction in epoprostenol were associated with symptoms related to excess or insufficient epoprostenol, respectively [see ADVERSE REACTIONS, Clinical Trials Experience, Adverse Events During Chronic Administration for PPH (6.1)].
6.2 Post-Marketing Experience
In addition to adverse reactions reported from clinical trials, the following events have been identified during post-approval use of epoprostenol. Because they are reported voluntarily from a population of unknown size, estimates of frequency cannot be made. These events have been chosen for inclusion due to a combination of their seriousness, frequency of reporting, or potential causal connection to epoprostenol.
Blood and Lymphatic: Anemia, hypersplenism, pancytopenia, splenomegaly.
Endocrine and Metabolic: Hyperthyroidism
7 DRUG INTERACTIONS
Additional reductions in blood pressure may occur when epoprostenol is administered with diuretics, antihypertensive agents, or other vasodilators. When other antiplatelet agents or anticoagulants are used concomitantly, there is the potential for epoprostenol to increase the risk of bleeding. However, patients receiving infusions of epoprostenol in clinical trials were maintained on anticoagulants without evidence of increased bleeding. In clinical trials, epoprostenol was used with digoxin, diuretics, anticoagulants, oral vasodilators, and supplemental oxygen.
In a pharmacokinetic substudy in patients with congestive heart failure receiving furosemide or digoxin in whom therapy with epoprostenol was initiated, apparent oral clearance values for furosemide (n = 23) and digoxin (n = 30) were decreased by 13% and 15%, respectively, on the second day of therapy and had returned to baseline values by day 87. The change in furosemide clearance value is not likely to be clinically significant. However, patients on digoxin may show elevations of digoxin concentrations after initiation of therapy with epoprostenol, which may be clinically significant in patients prone to digoxin toxicity.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category B. Reproductive studies have been performed in pregnant rats and rabbits at doses up to 100 mcg/kg/day (600 mcg/m2/day in rats, 2.5 times the recommended human dose, and 1,180 mcg/ m2/day in rabbits, 4.8 times the recommended human dose based on body surface area) and have revealed no evidence of impaired fertility or harm to the fetus due to epoprostenol. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
8.2 Labor and Delivery
The use of epoprostenol during labor, vaginal delivery, or cesarean section has not been adequately studied in humans.
8.3 Nursing Mothers
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when epoprostenol is administered to a nursing woman.
8.4 Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
8.5 Geriatric Use
Clinical studies of epoprostenol in pulmonary hypertension did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger patients. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
10 OVERDOSAGE
Signs and symptoms of excessive doses of epoprostenol during clinical trials are the expected dose-limiting pharmacologic effects of epoprostenol, including flushing, headache, hypotension, tachycardia, nausea, vomiting, and diarrhea. Treatment will ordinarily require dose reduction of epoprostenol.
One patient with secondary pulmonary hypertension accidentally received 50 mL of an unspecified concentration of epoprostenol. The patient vomited and became unconscious with an initially unrecordable blood pressure. Epoprostenol was discontinued and the patient regained consciousness within seconds. In clinical practice, fatal occurrences of hypoxemia, hypotension, and respiratory arrest have been reported following overdosage of epoprostenol.
Single intravenous doses of epoprostenol at 10 and 50 mg/kg (2,703 and 27,027 times the recommended acute phase human dose based on body surface area) were lethal to mice and rats, respectively. Symptoms of acute toxicity were hypoactivity, ataxia, loss of righting reflex, deep slow breathing, and hypothermia.
11 DESCRIPTION
Epoprostenol for Injection is a sterile sodium salt formulated for intravenous (IV) administration. Each vial of Epoprostenol for Injection contains epoprostenol sodium equivalent to 1.5 mg (1,500,000 ng) epoprostenol, 50 mg arginine, and 50 mg mannitol. Sodium hydroxide is added to adjust pH.
Epoprostenol (PGI2, PGX, prostacyclin), a metabolite of arachidonic acid, is a naturally occurring prostaglandin with potent vasodilatory activity and inhibitory activity of platelet aggregation.
Epoprostenol is (5Z,9a,lla,13E,15S)-6,9-epoxy-11,15-dihydroxyprosta-5,13-dien-l-oic acid. Epoprostenol sodium has a molecular weight of 374.45 and a molecular formula of C20H31NaO5. The structural formula is:
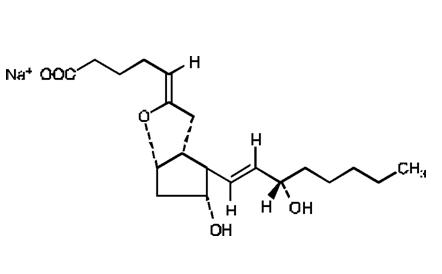
Epoprostenol for Injection is a white to off-white lyophilized material that may be translucent. It is reconstituted with Sterile Water for Injection, USP, or Sodium Chloride 0.9% Injection, USP.
The reconstituted solution of Epoprostenol for Injection has a pH of >11.0 and is increasingly unstable at a lower pH.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Epoprostenol has 2 major pharmacological actions: (1) direct vasodilation of pulmonary and systemic arterial vascular beds, and (2) inhibition of platelet aggregation.
12.2 Pharmacodynamics
In animals, the vasodilatory effects reduce right- and left-ventricular afterload and increase cardiac output and stroke volume. The effect of epoprostenol on heart rate in animals varies with dose. At low doses, there is vagally mediated bradycardia, but at higher doses, epoprostenol causes reflex tachycardia in response to direct vasodilation and hypotension. No major effects on cardiac conduction have been observed. Additional pharmacologic effects of epoprostenol in animals include bronchodilation, inhibition of gastric acid secretion, and decreased gastric emptying.
12.3 Pharmacokinetics
Epoprostenol is rapidly hydrolyzed at neutral pH in blood and is also subject to enzymatic degradation. Animal studies using tritium-labeled epoprostenol have indicated a high clearance (93 mL/kg/min), small volume of distribution (357 mL/kg), and a short half-life (2.7 minutes). During infusions in animals, steady-state plasma concentrations of tritium-labeled epoprostenol were reached within 15 minutes and were proportional to infusion rates.
No available chemical assay is sufficiently sensitive and specific to assess the in vivo human pharmacokinetics of epoprostenol. The in vitro half-life of epoprostenol in human blood at 37°C and pH 7.4 is approximately 6 minutes; therefore, the in vivo half-life of epoprostenol in humans is expected to be no greater than 6 minutes. The in vitro pharmacologic half-life of epoprostenol in human plasma, based on inhibition of platelet aggregation, was similar for males (n = 954) and females (n = 1,024).
Tritium-labeled epoprostenol has been administered to humans in order to identify the metabolic products of epoprostenol. Epoprostenol is metabolized to 2 primary metabolites: 6-keto-PGF1α (formed by spontaneous degradation) and 6,15-diketo-13,14-dihydro-PGF1α (enzymatically formed), both of which have pharmacological activity orders of magnitude less than epoprostenol in animal test systems. The recovery of radioactivity in urine and feces over a 1-week period was 82% and 4% of the administered dose, respectively. Fourteen additional minor metabolites have been isolated from urine, indicating that epoprostenol is extensively metabolized in humans.
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis and Mutagenesis and Impairment of Fertility
Long-term studies in animals have not been performed to evaluate carcinogenic potential. A micronucleus test in rats revealed no evidence of mutagenicity. The Ames test and DNA elution tests were also negative, although the instability of epoprostenol makes the significance of these tests uncertain. Fertility was not impaired in rats given epoprostenol by subcutaneous injection at doses up to 100 mcg/kg/day (600 mcg/m2/day, 2.5 times the recommended human dose [4.6 ng/kg/min or 245.1 mcg/m2/day, IV] based on body surface area).
14 CLINICAL STUDIES
14.1 Clinical Trials in Pulmonary Hypertension
Acute Hemodynamic Effects: Acute intravenous infusions of epoprostenol for up to 15 minutes in patients with secondary and primary pulmonary hypertension produce dose-related increases in cardiac index (CI) and stroke volume (SV) and dose-related decreases in pulmonary vascular resistance (PVR), total pulmonary resistance (TPR), and mean systemic arterial pressure (SAPm). The effects of epoprostenol on mean pulmonary arterial pressure (PAPm) were variable and minor.
Chronic Infusion in Primary Pulmonary Hypertension (PPH):
Hemodynamic Effects: Chronic continuous infusions of epoprostenol in patients with PPH were studied in 2 prospective, open, randomized trials of 8 and 12 weeks' duration comparing epoprostenol plus conventional therapy to conventional therapy alone. Dosage of epoprostenol was determined as described in DOSAGE AND ADMINISTRATION (2) and averaged 9.2 ng/kg/min at study's end. Conventional therapy varied among patients and included some or all of the following: anticoagulants in essentially all patients; oral vasodilators, diuretics, and digoxin in one half to two thirds of patients; and supplemental oxygen in about half the patients. Except for 2 New York Heart Association (NYHA) functional Class II patients, all patients were either functional Class III or Class IV. As results were similar in the 2 studies, the pooled results are described.
Chronic hemodynamic effects were generally similar to acute effects. Increases in CI, SV, and arterial oxygen saturation and decreases in PAPm, mean right atrial pressure (RAPm), TPR, and systemic vascular resistance (SVR) were observed in patients who received epoprostenol chronically compared to those who did not. Table 9 illustrates the treatment-related hemodynamic changes in these patients after 8 or 12 weeks of treatment.
| Baseline | Mean Change from Baseline at End of Treatment Period* | |||
|---|---|---|---|---|
| Hemodynamic Parameter | Epoprostenol (N = 52) | Standard Therapy (N = 54) | Epoprostenol (N = 48) | Standard Therapy (N = 41) |
|
||||
| CI (L/min/m2) | 2.0 | 2.0 | 0.3† | -0.1 |
| PAPm (mm Hg) | 60 | 60 | -5† | 1 |
| PVR (Wood U) | 16 | 17 | -4† | 1 |
| SAPm (mm Hg) | 89 | 91 | -4 | -3 |
| SV (mL/beat) | 44 | 43 | 6† | -1 |
| TPR (Wood U) | 20 | 21 | -5† | 1 |
These hemodynamic improvements appeared to persist when epoprostenol was administered for at least 36 months in an open, nonrandomized study.
Clinical Effects: Statistically significant improvement was observed in exercise capacity, as measured by the 6-minute walk test in patients receiving continuous intravenous epoprostenol plus conventional therapy (N = 52) for 8 or 12 weeks compared to those receiving conventional therapy alone (N = 54). Improvements were apparent as early as the first week of therapy. Increases in exercise capacity were accompanied by statistically significant improvement in dyspnea and fatigue, as measured by the Chronic Heart Failure Questionnaire and the Dyspnea Fatigue Index.
Survival was improved in NYHA functional Class III and Class IV PPH patients treated with epoprostenol for 12 weeks in a multicenter, open, randomized, parallel study. At the end of the treatment period, 8 of 40 (20%) patients receiving conventional therapy alone died, whereas none of the 41 patients receiving epoprostenol died (p = 0.003).
Chronic Infusion in Pulmonary Hypertension Associated with the Scleroderma Spectrum of Diseases (PH/SSD):
Hemodynamic Effects: Chronic continuous infusions of epoprostenol in patients with PH/SSD were studied in a prospective, open, randomized trial of 12 weeks' duration comparing epoprostenol plus conventional therapy (N = 56) to conventional therapy alone (N = 55). Except for 5 NYHA functional Class II patients, all patients were either functional Class III or Class IV. Dosage of epoprostenol was determined as described in DOSAGE AND ADMINISTRATION (2) and averaged 11.2 ng/kg/min at study's end. Conventional therapy varied among patients and included some or all of the following: anticoagulants in essentially all patients, supplemental oxygen and diuretics in two thirds of the patients, oral vasodilators in 40% of the patients, and digoxin in a third of the patients. A statistically significant increase in CI, and statistically significant decreases in PAPm, RAPm, PVR, and SAPm after 12 weeks of treatment were observed in patients who received epoprostenol chronically compared to those who did not. Table 10 illustrates the treatment-related hemodynamic changes in these patients after 12 weeks of treatment.
| Baseline | Mean Change from Baseline at 12 Weeks | |||
|---|---|---|---|---|
| Hemodynamic Parameter | Epoprostenol (N = 56) | Conventional Therapy (N = 55) | Epoprostenol (N = 50) | Conventional Therapy (N = 48) |
|
||||
| CI (L/min/m2) | 1.9 | 2.2 | 0.5* | -0.1 |
| PAPm (mm Hg) | 51 | 49 | -5* | 1 |
| RAPm (mm Hg) | 13 | 11 | -1* | 1 |
| PVR (Wood U) | 14 | 11 | -5* | 1 |
| SAPm (mm Hg) | 93 | 89 | -8* | -1 |
Clinical Effects: Statistically significant improvement was observed in exercise capacity, as measured by the 6-minute walk, in patients receiving continuous intravenous epoprostenol plus conventional therapy for 12 weeks compared to those receiving conventional therapy alone. Improvements were apparent in some patients at the end of the first week of therapy. Increases in exercise capacity were accompanied by statistically significant improvements in dyspnea and fatigue, as measured by the Borg Dyspnea Index and Dyspnea Fatigue Index. At week 12, NYHA functional class improved in 21 of 51 (41%) patients treated with epoprostenol compared to none of the 48 patients treated with conventional therapy alone. However, more patients in both treatment groups (28/51 [55%] with epoprostenol and 35/48 [73%] with conventional therapy alone) showed no change in functional class, and 2/51 (4%) with epoprostenol and 13/48 (27%) with conventional therapy alone worsened. Of the patients randomized, NYHA functional class data at 12 weeks were not available for 5 patients treated with epoprostenol and 7 patients treated with conventional therapy alone.
No statistical difference in survival over 12 weeks was observed in PH/SSD patients treated with epoprostenol as compared to those receiving conventional therapy alone. At the end of the treatment period, 4 of 56 (7%) patients receiving epoprostenol died, whereas 5 of 55 (9%) patients receiving conventional therapy alone died.
No controlled clinical trials with epoprostenol have been performed in patients with pulmonary hypertension associated with other diseases.
16 HOW SUPPLIED / STORAGE AND HANDLING
16.1 How Supplied
Epoprostenol for Injection is supplied as a sterile lyophilized material in 10 mL vials each with a red flip-off seal.
Each 10 mL vial containing epoprostenol sodium equivalent to 1.5 mg (1,500,000 ng) epoprostenol, is packaged in carton of 1 vial (NDC 66215-401-01).
Store the vials of Epoprostenol for Injection at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. Protect from light.
16.2 Storage and Stability
Unopened vials of Epoprostenol for Injection are stable until the date indicated on the package when stored at 20° to 25°C (68° to 77°F) and protected from light in the carton.
Prior to use, Epoprostenol for Injection solutions reconstituted with 5 mL diluent must be protected from light and can be refrigerated at 2° to 8°C (36° to 46°F) for as long as 5 days or held at up to 25°C (77°F) for up to 48 hours prior to use. Do not freeze reconstituted solutions of Epoprostenol for Injection. Discard any reconstituted solution that has been frozen. Discard any reconstituted solution if it has been refrigerated for more than 5 days, or if held at room temperature for more than 48 hours.
When the patient is then ready for the administration at room temperature, the dosing solutions may be prepared from the 5 mL solution as directed, by dilution with the same appropriate diluent to the needed concentration. This fully diluted solution can then be administered at room temperature for periods up to 24 hours. (If lower concentrations are chosen, the pump reservoirs should be changed every 12 hours when administered at room temperature.) Do not expose this solution to direct sunlight. [See Reconstitution (2.4)].
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration whenever solution and container permit. If either occurs, Epoprostenol for Injection should not be administered.
17 PATIENT COUNSELING INFORMATION
Patients receiving Epoprostenol for Injection should receive the following information.
Epoprostenol for Injection must be reconstituted as directed using only Sterile Water for Injection, USP, or Sodium Chloride 0.9% Injection, USP. Epoprostenol is infused continuously through a permanent indwelling central venous catheter via a small, portable infusion pump. Thus, therapy with epoprostenol requires commitment by the patient to drug reconstitution, drug administration, and care of the permanent central venous catheter. Sterile technique must be adhered to in preparing the drug and in the care of the catheter, and even brief interruptions in the delivery of epoprostenol may result in rapid symptomatic deterioration. A patient's decision to receive epoprostenol should be based upon the understanding that there is a high likelihood that therapy with epoprostenol will be needed for prolonged periods, possibly years. The patient's ability to accept and care for a permanent intravenous catheter and infusion pump should also be carefully considered.
Manufactured for:
Actelion Pharmaceuticals US, Inc.
5000 Shoreline Court, Ste. 200
South San Francisco, CA 94080
Manufactured by:
Hollister-Stier Laboratories, LLC
3525 N. Regal
Spokane, WA 99207
ACT20100312
March 2010
PRINCIPAL DISPLAY PANEL - 1.5 mg Vial Carton
NDC 66215-401-01
Single Dose Vial
EPOPROSTENOL
for
Injection
1.5 mg (1,500,000 ng)/vial
Sterile, Lyophilized Product
FOR INTRAVENOUS
INFUSION ONLY
Rx Only
ACTELION
| EPOPROSTENOL
epoprostenol powder, for solution |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| NDA | NDA022260 | 04/22/2010 | |
| Labeler - Actelion Pharmaceuticals US, Inc. (002641228) |