GLUMETZA
-
metformin hydrochloride tablet, film coated, extended release
Depomed, Inc.
----------
GLUMETZA(metformin hydrochloride extended release tablets)
Rx Only
DESCRIPTION
GLUMETZA (metformin hydrochloride) extended release tablet is an oral antihyperglycemic drug used in the management of type 2 diabetes. Metformin hydrochloride (N,N-dimethylimidodicarbonimidic diamide hydrochloride) is not chemically or pharmacologically related to any other classes of oral antihyperglycemic agents. The structural formula of metformin hydrochloride (metformin HCl) is as shown:
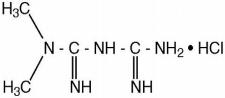
Metformin HCl is a white to off-white crystalline compound with a molecular formula of C4H11N5•HCl and a molecular weight of 165.63. Metformin HCl is freely soluble in water and is practically insoluble in acetone, ether, and chloroform. The pKa of metformin is 12.4. The pH of a 1% aqueous solution of metformin hydrochloride is 6.68. GLUMETZA tablets are modified release dosage forms that contain 500 mg or 1000 mg of metformin HCl. Each 500 mg tablet contains coloring, hypromellose, magnesium stearate, microcrystalline cellulose and polyethylene oxide. Each 1000 mg tablet contains colloidal silicon dioxide, polyvinyl alcohol, crospovidone, glyceryl behenate, polyacrylate dispersion, hypromellose, talc, polyethylene glycol, eudragit, titanium dioxide, simethicone emulsion, polysorbate and coloring. GLUMETZA 500 and 1000 mg tablets both utilize polymer-based, oral drug delivery systems, which allow delivery of metformin HCl to the upper gastrointestinal (GI) tract.
CLINICAL PHARMACOLOGY
Mechanism of Action
Metformin is an antihyperglycemic agent, which improves glucose tolerance in patients with type 2 diabetes, lowering both basal and postprandial plasma glucose. Its pharmacologic mechanisms of action are different from other classes of oral antihyperglycemic agents. Metformin decreases hepatic glucose production, decreases intestinal absorption of glucose, and improves insulin sensitivity by increasing peripheral glucose uptake and utilization. Unlike sulfonylureas, metformin does not produce hypoglycemia in either patients with type 2 diabetes or normal subjects (except in special circumstances, see PRECAUTIONS) and does not cause hyperinsulinemia. With metformin therapy, insulin secretion remains unchanged while fasting insulin levels and daylong plasma insulin response may actually decrease.
Pharmacokinetics
Absorption and Bioavailability
The following pharmacokinetic studies were performed with the 500 mg dosage form. Following a single oral dose of 1000 mg (2x500 mg tablets) GLUMETZA after a meal, the time to reach maximum plasma metformin concentration (Tmax) is achieved at approximately 7-8 hours. In both single and multiple-dose studies in healthy subjects, once daily 1000 mg (2x500 mg tablets) dosing provides equivalent systemic exposure, as measured by area-under-the-curve (AUC), and up to 35% higher Cmax, of metformin relative to the immediate release given as 500 mg twice daily. GLUMETZA tablets must be administered immediately after a meal to maximize therapeutic benefit.
| PK Parameter | Glumetza
2x500 mg | Glumetza
1x500 mg BID | Glucophage
1x500 mg BID |
| AUC0-36 (ng.hr/mL) | 14182 ± 2415 | 15260 ± 3496 | 15342 ± 3398 |
| Cmax (ng/mL) | 1301.4 ± 285.7 | 811.9 ± 173.7 | 959.1 ± 204.0 |
| Tmax (hr) | 7.5 ± 1.2 | 7.1 ± 1.2 | 4.2 ± 1.6 |
Single oral doses of GLUMETZA from 500 mg to 2500 mg resulted in less than proportional increase in both AUC and Cmax. The mean Cmax values were 473 ± 145, 868 ± 223, 1171 ± 297, and 1630 ± 399 ng/mL for single doses of 500, 1000, 1500, and 2500 mg, respectively. For AUC, the mean values were 3501 ± 796, 6705 ± 1918, 9299 ± 2833, and 14161 ± 4432 ng·hr/mL for single doses of 500, 1000, 1500, and 2500 mg, respectively.
Low-fat and high-fat meals increased the systemic exposure (as measured by AUC) from GLUMETZA tablets by about 38% and 73%, respectively, relative to fasting. Both meals prolonged metformin Tmax by approximately 3 hours but Cmax was not affected.
In a two-way, single-dose crossover study in healthy volunteers, the 1000 mg tablet was found to be bioequivalent to two 500 mg tablets under fed conditions based on equivalent Cmax and AUCs for the two formulations (Table 2).
| PK Parameters | Glumetza
1000 mg Tablet | Glumetza
2x500 mg Tablets |
| AUC0-t (ng.hr/mL) | 11706 ± 2520 | 12408 ± 2581 |
| AUC0-∞ (ng.hr/mL) | 11907 ± 2521 | 12599 ± 2616 |
| Cmax (ng/mL) | 1238 ± 271 | 1116 ± 254 |
Distribution
The apparent volume of distribution (V/F) of metformin following single oral doses of 850 mg immediate release metformin hydrochloride averaged 654 ± 358 L. Metformin is negligibly bound to plasma proteins. Metformin partitions into erythrocytes, most likely as a function of time. At usual clinical doses and dosing schedules of metformin, steady state plasma concentrations of metformin are reached within 24-48 hours and are generally < 1 µg/mL. During controlled clinical trials, which served as the basis of approval for metformin, maximum metformin plasma levels did not exceed 5 µg/mL, even at maximum doses.
Metabolism and Excretion
Intravenous single-dose studies in normal subjects demonstrate that metformin is excreted unchanged in the urine and does not undergo hepatic metabolism (no metabolites have been identified in humans), nor biliary excretion. Renal clearance is approximately 3.5 times greater than creatinine clearance, which indicates that tubular secretion is the major route of metformin elimination. Following oral administration, approximately 90% of the absorbed drug is eliminated via the renal route within the first 24 hours, with a plasma elimination half-life of approximately 6.2 hours. In blood, the elimination half-life is approximately 17.6 hours, suggesting that the erythrocyte mass may be a compartment of distribution.
Special Populations
Renal Impairment: In patients with mild and moderate renal failure (based on measured creatinine clearance) the oral and renal clearance of metformin were decreased by 33% and 50% and 16% and 53%, respectively (see WARNINGS). Metformin peak and systemic exposure were significantly greater in patients with renal failure relative to healthy volunteers with normal renal function. There was a rank-order correlation of metformin AUC and Cmax with degree of renal failure. Since metformin can accumulate to toxic levels in patients with renal impairment, administration of GLUMETZA is contraindicated in these patients.
Hepatic Impairment: No pharmacokinetic studies of GLUMETZA have been conducted in subjects with hepatic insufficiency.
Geriatrics: Limited data from controlled pharmacokinetic studies of metformin hydrochloride in healthy elderly subjects suggest that total plasma clearance of metformin is decreased, the half-life is prolonged and Cmax is increased, compared to healthy young subjects. From these data, it appears that the change in metformin pharmacokinetics with aging is primarily accounted for by a change in renal function (see CLINICAL PHARMACOLOGY, Pharmacokinetics). Metformin treatment should not be initiated in patients 80 years of age unless measurement of creatinine clearance demonstrates that renal function is not reduced (see WARNINGS and DOSAGE AND ADMINISTRATION).
Gender: In the pharmacokinetic studies in healthy volunteers, there were no important differences between male and female subjects with respect to metformin AUC (males = 268, females = 293) and t1/2 (males = 229, females = 260). However, Cmax for metformin were somewhat higher in female subjects (Female/Male Cmax Ratio = 1.4). The gender differences for Cmax are unlikely to be clinically important. Similarly, in controlled clinical studies in patients with type 2 diabetes, the antihyperglycemic effect of metformin hydrochloride tablets was comparable in males and females.
Race: There were no definitive conclusions on the differences between the races with respect to the pharmacokinetics of metformin because of the imbalance in the respective sizes of the racial groups. However, the data suggest a trend towards higher metformin Cmax and AUC values for metformin are obtained in Asian subjects when compared to Caucasian, Hispanic and Black subjects. The differences between the Asian and Caucasian groups are unlikely to be clinically important. In controlled clinical studies of metformin hydrochloride in patients with type 2 diabetes, the antihyperglycemic effect was comparable in whites (n = 249), blacks (n = 51) and Hispanics (n = 24).
Pediatrics: No pharmacokinetic data from studies of GLUMETZA in pediatric subjects are available.
CLINICAL STUDIES
GLUMETZA has been studied as monotherapy and in combination with a sulfonylurea and insulin.
In a multicenter, randomized, double-blind, active-controlled, dose-ranging, parallel group study GLUMETZA 1500 mg once a day, GLUMETZA 1500 per day in divided doses (500 mg in the morning and 1000 mg in the evening), and GLUMETZA 2000 mg once a day were compared to immediate release metformin 1500 mg per day in divided doses (500 mg in the morning and 1000 mg in the evening). (See Table 3.) Newly diagnosed patients, diet-and-exercise-treated (diet/exercise) patients, patients who received combination therapy consisting of metformin up to 1500 mg/day plus a sulfonylurea at a dose equal to or less than one-half the maximum dose allowed (following a 6-week washout), or patients on monotherapy with an antihyperglycemic agent (following a 6-week washout) were randomized to treatment and began titration from 1000 mg/day up to their assigned treatment dose over 3 weeks. Metformin IR treatment was initiated as 500 mg BID for 1 week followed by 500 mg with breakfast and 1000 mg with dinner for the second week. The 3-week treatment period was followed by an additional 21-week period at the randomized dose. Each of the GLUMETZA regimens, were at least as effective as immediate release metformin in all measures of glycemic control. Additionally, once daily dosing was as effective as the commonly prescribed twice daily dosing of the immediate release metformin formulation.
| Parameter | GLUMETZA | Metformin IR 1500 mg AM/PM
(n = 174) |
||
| 1500 mg QD
(n = 178) | 1500 mg AM/PM
(n = 182) | 2000 mg QD
(n = 172) | ||
| HbA1c (%) | ||||
| n | 169 | 175 | 159 | 170 |
| Baseline | 8.22 ± 0.25 | 8.50 ± 0.24 | 8.26 ± 0.24 | 8.70 ± 0.25 |
| Mean Change ± SE at Final Visit | -0.73 ± 0.12 | -0.74 ± 0.12 | -1.06 ± 0.12 | -0.70 ± 0.12 |
| Mean Difference ± SE from Metformin IR | -0.03 ± 0.12 | -0.04 ± 0.12 | -0.36 ± 0.12 | N/A |
| 98.4% CI for Difference | (-0.32, 0.26) | (-0.33, 0.25) | (-0.65, -0.06) | |
| Fasting Plasma Glucose (mg/dL) | ||||
| n | 175 | 179 | 170 | 172 |
| Baseline | 190.0 ± 9.9 | 192.5 ± 9.9 | 183.9 ± 9.9 | 196.5 ± 11.2 |
| Mean Change ± SE at Final Visit | -38.5 ± 4.4 | -31.8 ± 4.4 | -42.0 ± 4.5 | -32.1 ± 4.5 |
| Mean Difference ± SE from Metformin IR | -6.4 ± 4.4 | 0.2 ± 4.3 | -9.9 ± 4.4 | N/A |
| 95% CI for Difference | (-15.0, 2.1) | (-8.3, 8.7) | (-18.5, -1.3) | |
| Body Weight (kg) | ||||
| n | 176 | 180 | 171 | 173 |
| Baseline | 88.17 ± 3.66 | 90.50 ± 3.66 | 87.73 ± 3.66 | 88.72 ± 3.87 |
| Mean Change ± SE at Final Visit | -0.93 ± 0.40 | -0.68 ± 0.40 | -1.10 ± 0.40 | -0.85 ± 0.41 |
| Mean Difference ± SE from Metformin IR | -0.09 ± 0.40 | 0.17 ± 0.39 | -0.26 ± 0.40 | N/A |
| 95% CI for Difference | (-0.86, 0.69) | (-0.61, 0.94) | (-1.04, 0.52) | |
In a double-blind, randomized, placebo-controlled (glyburide add-on) multicenter study, patients with type 2 diabetes mellitus who were newly diagnosed or treated with diet and exercise, or who were receiving monotherapy with metformin, sulfonylureas, alpha-glucosidase inhibitors, thiazolidinediones, or meglinitides, or treated with combination therapy consisting of metformin/glyburide at doses up to 1000 mg metformin + 10 mg glyburide per day (or equivalent doses of glipizide or glimepiride up to half the maximum therapeutic dose) were enrolled. They were stabilized on glyburide for a 6-week period, and then randomized to 1 of 4 treatments: placebo + glyburide (glyburide alone); GLUMETZA 1500 mg once a day + glyburide, GLUMETZA 2000 mg once a day + glyburide, or GLUMETZA 1000 mg twice a day + glyburide. A 3-week GLUMETZA titration phase was followed by a 21-week maintenance treatment phase. The difference in the change from Baseline in HbA1c levels between the combined M-ER+ SU (sulfonylurea) groups and the SU only group was statistically significant (p<0.001). The changes in glycemic control across the three GLUMETZA+glyburide groups were comparable. (See Table 4.)
|
||||
| Parameter | GLUMETZA + Glyburide* | Placebo/
Glyburide* |
||
| 1500 mg QD
(n = 144) | 1000 mg
BID (n = 141) | 2000 mg QD
(n = 146) | (n= 144) | |
| HbA1c (%) | ||||
| n | 136 | 136 | 144 | 141 |
| Baseline | 7.93 ± 0.13 | 7.75 ± 0.13 | 7.68 ± 0.13 | 8.08 ± 0.13 |
| Mean Change ± SE at Final Visit | -0.72 ± 0.09 | -0.82 ± 0.09 | -0.71 ± 0.08 | -0.07 ± 0.08 |
| Mean Difference ± SE from Glyburide Alone | -0.79 ± 0.11 | -0.89 ± 0.11 | -0.77 ± 0.11 | N/A |
| 95% CI for Difference | (-1.01, -0.57) | (-1.11, -0.67) | (-0.99, -0.56) | |
| p-value for pairwise comparison | < 0.001 | < 0.001 | < 0.001 | |
| Fasting Plasma Glucose (mg/dL) | ||||
| n | 143 | 141 | 145 | 144 |
| Baseline | 163.4 ± 4.6 | 163.2 ± 4.7 | 158.8 ± 4.7 | 164.0 ± 4.7 |
| Mean Change ± SE at Final Visit | -13.7 ± 3.7 | -15.7 ± 3.7 | -9.4 ± 3.7 | 15.5 ± 3.7 |
| Mean Difference ± SE from Glyburide Alone | -29.2 ± 4.9 | -31.2 ± 40.9 | -24.9 ± 4.9 | N/A |
| 95% CI for Difference | (-38.8, -19.6) | (-40.9, -21.6) | (-34.5, -15.4) | |
| p-value for pairwise comparison | < 0.001 | < 0.001 | < 0.001 | |
| Body Weight (kg) | ||||
| n | 143 | 141 | 146 | 144 |
| Baseline | 89.38 ± 11.21 | 103.70 ± 11.21 | 102.90 ± 11.21 | 95.56 ± 7.96 |
| Mean Change ± SE at Final Visit | 0.28 ± 1.05 | 0.08 ± 1.05 | -0.03 ± 1.05 | 0.71 ± 1.04 |
| Mean Difference ± SE from Glyburide Alone | -0.43 ± 0.52 | -0.63 ± 0.53 | -0.74 ± 0.52 | N/A |
| 95% CI for Difference | (-1.46, 0.60) | (-1.67, 0.40) | (-1.77, 0.28) | |
| p-value for pairwise comparison | 0.410 | 0.230 | 0.156 | |
A 24-week, double-blind, placebo-controlled study of immediate release metformin plus insulin versus insulin plus placebo was conducted in patients with type 2 diabetes who failed to achieve adequate glycemic control on insulin alone. Patients randomized to receive metformin plus insulin achieved a reduction in HbA1c of 2.10%, compared to a 1.56% reduction in HbA1c achieved by insulin plus placebo. The improvement in glycemic control was achieved at the final study visit with 16% less insulin, 93.0 U/day vs. 110.6 U/day, metformin plus insulin versus insulin plus placebo, respectively, p=0.04. A second double-blind, placebo-controlled study (n=51), with 16 weeks of randomized treatment, demonstrated that in patients with type 2 diabetes controlled on insulin for 8 weeks with an average HbA1c of 7.46 ± 0.97%, the addition of metformin maintained similar glycemic control (HbA1c 7.15 ± 0.61 versus 6.97 ± 0.62 for metformin plus insulin and placebo plus insulin, respectively) with 19% less insulin versus baseline (reduction of 23.68 ± 30.22 versus an increase of 0.43 ± 25.20 units for metformin plus insulin and placebo plus insulin, p<0.01). In addition, this study demonstrated that the combination of metformin plus insulin resulted in reduction in body weight of 3.11 ± 4.30 lbs, compared to an increase of 1.30 ± 6.08 lbs for placebo plus insulin, p=0.01.
INDICATIONS AND USE
GLUMETZA is indicated as an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus.
CONTRAINDICATIONS
GLUMETZA is contraindicated in patients with:
- Renal disease or renal dysfunction (e.g., as suggested by serum creatinine levels ≥ 1.5 mg/dL [males], ≥ 1.4 mg/dL [females] or abnormal creatinine clearance), which may also result from conditions such as cardiovascular collapse (shock), acute myocardial infarction, and septicemia (see WARNINGS and PRECAUTIONS).
- Known hypersensitivity to metformin hydrochloride.
- Acute or chronic metabolic acidosis, including diabetic ketoacidosis, with or without coma. Diabetic ketoacidosis should be treated with insulin.
GLUMETZA should be temporarily discontinued in patients undergoing radiologic studies involving intravascular administration of iodinated contrast materials, because use of such products may result in acute alteration of renal function. (See also PRECAUTIONS.)
WARNINGS
Lactic Acidosis:
Lactic acidosis is a rare, but serious, metabolic complication that can occur due to metformin accumulation during treatment with GLUMETZA; when it occurs, it is fatal in approximately 50% of cases. Lactic acidosis may also occur in association with a number of pathophysiologic conditions, including diabetes mellitus, and whenever there is significant tissue hypoperfusion and hypoxemia. Lactic acidosis is characterized by elevated blood lactate levels (>5 mmol/L), decreased blood pH, electrolyte disturbances with an increased anion gap, and an increased lactate/pyruvate ratio. When metformin is implicated as the cause of lactic acidosis, metformin plasma levels >5 µg/mL are generally found. The reported incidence of lactic acidosis in patients receiving metformin hydrochloride is very low (approximately 0.03 cases/1000 patient-years, with approximately 0.015 fatal cases/1000 patient-years). In more than 20,000 patient-years exposure to metformin in clinical trials, there were no reports of lactic acidosis. Reported cases have occurred primarily in diabetic patients with significant renal insufficiency, including both intrinsic renal disease and renal hypoperfusion, often in the setting of multiple concomitant medical/surgical problems and multiple concomitant medications. Patients with congestive heart failure requiring pharmacologic management, in particular those with unstable or acute congestive heart failure who are at risk of hypoperfusion and hypoxemia, are at increased risk of lactic acidosis. The risk of lactic acidosis increases with the degree of renal dysfunction and the patient’s age. The risk of lactic acidosis may, therefore, be significantly decreased by regular monitoring of renal function in patients taking GLUMETZA and by use of the minimum effective dose of GLUMETZA. In particular, treatment of the elderly should be accompanied by careful monitoring of renal function. GLUMETZA treatment should not be initiated in patients ≥ 80 years of age unless measurement of creatinine clearance demonstrates that renal function is not reduced, as these patients are more susceptible to developing lactic acidosis. In addition, GLUMETZA should be promptly withheld in the presence of any condition associated with hypoxemia, dehydration, or sepsis. Because impaired hepatic function may significantly limit the ability to clear lactate, GLUMETZA should generally be avoided in patients with clinical or laboratory evidence of hepatic disease. Patients should be cautioned against excessive alcohol intake, either acute or chronic, when taking GLUMETZA , since alcohol potentiates the effects of metformin hydrochloride on lactate metabolism. In addition, GLUMETZA should be temporarily discontinued prior to any intravascular radiocontrast study and for any surgical procedure (see also PRECAUTIONS). The onset of lactic acidosis often is subtle, and accompanied only by nonspecific symptoms such as malaise, myalgias, respiratory distress, increasing somnolence, and nonspecific abdominal distress. These may be associated hypothermia, hypotension, and resistant bradyarrhythmias with more marked acidosis.
The patient and the patient’s physician must be aware of the possible importance of such symptoms and the patient should be withdrawn until the situation is clarified. Serum electrolytes, ketones, blood glucose and, if indicated, blood pH, lactate levels, and even blood metformin levels may be useful. Once a patient is stabilized on any dose level of GLUMETZA, gastrointestinal symptoms, which are common during initiation of therapy, are unlikely to be drug related. Later occurrence of gastrointestinal symptoms could be due to lactic acidosis or other serious disease. Levels of fasting venous plasma lactate above the upper limit of normal but less than 5 mmol/L in patients taking GLUMETZA do not necessarily indicate impending lactic acidosis and may be explainable by other mechanisms, such as poorly controlled diabetes or obesity, vigorous physical activity, or technical problems in sample handling. (See also PRECAUTIONS.) Lactic acidosis should be suspected in any diabetic patient with metabolic acidosis lacking evidence of ketoacidosis (ketonuria and ketonemia). Lactic acidosis is a medical emergency that must be treated in a hospital setting. In a patient with lactic acidosis who is taking GLUMETZA, the drug should be discontinued immediately and general supportive measures promptly instituted. Because metformin hydrochloride is dialyzable (with a clearance of up to 170 mL/min under good hemodynamic conditions), prompt hemodialysis is recommended to correct the acidosis and remove the accumulated metformin. Such management often results in prompt reversal of symptoms and recovery. (See also CONTRAINDICATIONS and PRECAUTIONS.)
PRECAUTIONS
General
There have been no clinical studies establishing conclusive evidence of macrovascular risk reduction with GLUMETZA or any other oral anti-diabetic drug.
Monitoring of renal function — Metformin is substantially excreted by the kidney, and the risk of metformin accumulation and lactic acidosis increases with the degree of impairment of renal function. Thus, patients with serum creatinine levels above the upper limit of normal for their age should not receive GLUMETZA. In patients with advanced age, GLUMETZA should be carefully titrated to establish the minimum dose for adequate glycemic effect, because aging is associated with reduced renal function. In elderly patients, particularly those ≥80 years of age, renal function should be monitored regularly and GLUMETZA should generally not be titrated to the maximum dose (see WARNINGS and DOSAGE AND ADMINISTRATION). Before initiation of GLUMETZA therapy and at least annually thereafter, renal function should be assessed and verified as normal. In patients in whom development of renal dysfunction is anticipated, renal function should be assessed more frequently and GLUMETZA discontinued if evidence of renal impairment is present.
Use of concomitant medications that may affect renal function or metformin disposition —
Concomitant medication(s) that may affect renal function or result in significant hemodynamic change or may interfere with the disposition of metformin, such as cationic drugs that are eliminated by renal tubular secretion (see PRECAUTIONS: Drug Interactions), should be used with caution. Radiologic studies involving the use of intravascular iodinated contrast materials (for example, intravenous urogram, intravenous cholangiography, angiography, and computed tomography (CT) scans with intravascular contrast materials) — Intravascular contrast studies with iodinated materials can lead to acute alteration of renal function and have been associated with lactic acidosis in patients receiving metformin (see CONTRAINDICATIONS). Therefore, in patients in whom any such study is planned, GLUMETZA should be temporarily discontinued at the time of or prior to the procedure, and withheld for 48 hours subsequent to the procedure and reinstituted only after renal function has been re-evaluated and found to be normal.
Hypoxic states — Cardiovascular collapse (shock) from whatever cause, acute congestive heart failure, acute myocardial infarction and other conditions characterized by hypoxemia have been associated with lactic acidosis and may also cause prerenal azotemia. When such events occur in patients on GLUMETZA therapy, the drug should be promptly discontinued.
Surgical procedures — GLUMETZA therapy should be temporarily suspended for any surgical procedure (except minor procedures not associated with restricted intake of food and fluids) and should not be restarted until the patient’s oral intake has resumed and renal function has been evaluated as normal.
Alcohol intake — Alcohol is known to potentiate the effect of metformin on lactate metabolism. Patients, therefore, should be warned against excessive alcohol intake, acute or chronic, while receiving GLUMETZA.
Impaired hepatic function — Since impaired hepatic function has been associated with some cases of lactic acidosis GLUMETZA should generally be avoided in patients with clinical or laboratory evidence of hepatic disease.
Vitamin B12 levels — In controlled, 29-week clinical trials of immediate release metformin, a decrease to subnormal levels of previously normal serum Vitamin B12 levels, without clinical manifestations, was observed in approximately 7% of patients. Such decrease, possibly due to interference with B12 absorption from the B12-intrinsic factor complex, is, however, very rarely associated with anemia and appears to be rapidly reversible with discontinuation of GLUMETZA or Vitamin B12 supplementation. Measurement of hematologic parameters on an annual basis is advised in patients on GLUMETZA and any apparent abnormalities should be appropriately investigated and managed (see PRECAUTIONS: Laboratory Tests). Certain individuals (those with inadequate Vitamin B12 or calcium intake or absorption) appear to be predisposed to developing subnormal Vitamin B12 levels. In these patients, routine serum Vitamin B12 measurements at two- to three-year intervals may be useful.
Change in clinical status of patients with previously controlled type 2 diabetes — A patient with type 2 diabetes previously well controlled on GLUMETZA who develops laboratory abnormalities or clinical illness (especially vague and poorly defined illness) should be evaluated promptly for evidence of ketoacidosis or lactic acidosis. Evaluation should include serum electrolytes and ketones, blood glucose and, if indicated, blood pH, lactate, pyruvate, and metformin levels. If acidosis of either form occurs, GLUMETZA must be stopped immediately and other appropriate corrective measures initiated (see also WARNINGS).
Hypoglycemia — Hypoglycemia does not occur in patients receiving metformin alone under usual circumstances of use, but could occur when caloric intake is deficient, when strenuous exercise is not compensated by caloric supplementation, or during concomitant use with other glucose-lowering agents (such as sulfonylureas and insulin) or ethanol. Elderly, debilitated, or malnourished patients, and those with adrenal or pituitary insufficiency or alcohol intoxication are particularly susceptible to hypoglycemic effects. Hypoglycemia may be difficult to recognize in the elderly, and in people who are taking beta-adrenergic blocking drugs.
Loss of control of blood glucose — When a patient stabilized on any diabetic regimen is exposed to stress such as fever, trauma, infection, or surgery, a temporary loss of glycemic control may occur. At such times, it may be necessary to withhold GLUMETZA and temporarily administer insulin. GLUMETZA may be reinstituted after the acute episode is resolved. The effectiveness of oral antidiabetic drugs in lowering blood glucose to a targeted level decreases in many patients over a period of time. This phenomenon, which may be due to progression of the underlying disease or to diminished responsiveness to the drug, is known as secondary failure, to distinguish it from primary failure in which the drug is ineffective during initial therapy. Should secondary failure occur with either GLUMETZA or sulfonylurea monotherapy, combined therapy with GLUMETZA and sulfonylurea may result in a response. Should secondary failure occur with combined GLUMETZA/sulfonylurea therapy, it may be necessary to consider therapeutic alternatives including initiation of insulin therapy.
Information for Patients
Patients should be informed of the potential risks and benefits of GLUMETZA and of alternative modes of therapy. They should also be informed about the importance of adherence to dietary instructions, of a regular exercise program, and of regular testing of blood glucose, glycosylated hemoglobin, renal function, and hematologic parameters.
The risks of lactic acidosis, its symptoms, and conditions that predispose to its development, as noted in the GLUMETZA sections, should be explained to patients. Patients should be advised to discontinue GLUMETZA immediately and to promptly notify their health practitioner if unexplained hyperventilation, myalgia, malaise, unusual somnolence, or other nonspecific symptoms occur. Once a patient is stabilized on any dose level of GLUMETZA, gastrointestinal symptoms, which are common during initiation of metformin therapy, are unlikely to be drug related. Later occurrence of gastrointestinal symptoms could be due to lactic acidosis or other serious disease. Patients should be counseled against excessive alcohol intake, either acute or chronic, while receiving GLUMETZA. GLUMETZA (metformin hydrochloride extended-release tablets) alone does not usually cause hypoglycemia, although it may occur when GLUMETZA is used in conjunction with oral sulfonylureas and insulin. When initiating combination therapy, the risks of hypoglycemia, its symptoms and treatment, and conditions that predispose to its development should be explained to patients and responsible family members. Patients should be informed that GLUMETZA must be swallowed whole and not crushed or chewed, and that the inactive ingredients may occasionally be eliminated in the feces as a soft mass that may resemble the original tablet. (See Patient Information.)
Laboratory Tests
Response to all diabetic therapies should be monitored by periodic measurements of fasting blood glucose and glycosylated hemoglobin levels, with a goal of decreasing these levels toward the normal range. During initial dose titration, fasting glucose can be used to determine the therapeutic response. Thereafter, both glucose and glycosylated hemoglobin should be monitored. Measurements of glycosylated hemoglobin may be especially useful for evaluating long-term control (see also DOSAGE AND ADMINISTRATION). Initial and periodic monitoring of hematologic parameters (e.g., hemoglobin/hematocrit and red blood cell indices) and renal function (serum creatinine) should be performed, at least on an annual basis. While megaloblastic anemia has rarely been seen with metformin therapy, if this is suspected, Vitamin B12 deficiency should be excluded.
Drug Interactions (Clinical Evaluation of Drug Interactions Conducted with metformin)
Glyburide — The influence of glyburide on GLUMETZA pharmacokinetics was assessed in a single-dose interaction study in healthy subjects. Co-administration of a single dose of 500 mg GLUMETZA and 5 mg glyburide did not result in any changes in metformin pharmacokinetics as AUC; Cmax as well as Tmax were unchanged. Changes in pharmacodynamics were not evaluated in this study (see DOSAGE AND ADMINISTRATION: Concomitant GLUMETZA and Oral Sulfonylurea Therapy).
Furosemide — A single-dose, metformin-furosemide drug interaction study in healthy subjects demonstrated that pharmacokinetic parameters of both compounds were affected by co-administration. Furosemide increased the metformin plasma and blood Cmax by 22% and blood AUC by 15%, without any significant change in metformin renal clearance. When administered with metformin, the Cmax and AUC of furosemide were 31% and 12% smaller, respectively, than when administered alone, and the terminal half-life was decreased by 32%, without any significant change in furosemide renal clearance. No information is available about the interaction of metformin and furosemide when co-administered chronically.
Nifedipine — A single-dose, metformin-nifedipine drug interaction study in normal healthy volunteers demonstrated that co-administration of nifedipine increased plasma metformin Cmax and AUC by 20% and 9%, respectively, and increased the amount excreted in the urine. Tmax and half-life were unaffected. Nifedipine appears to enhance the absorption of metformin. Metformin had minimal effects on nifedipine.
Cationic drugs — Cationic drugs (e.g., amiloride, digoxin, morphine, procainamide, quinidine, quinine, ranitidine, triamterene, trimethoprim, or vancomycin) that are eliminated by renal tubular secretion theoretically have the potential for interaction with metformin by competing for common renal tubular transport systems. Such interaction between metformin and oral cimetidine has been observed in normal healthy volunteers in both single- and multiple-dose, metformin-cimetidine drug interaction studies, with a 60% increase in peak metformin plasma and whole blood concentrations and a 40% increase in plasma and whole blood metformin AUC. There was no change in elimination half-life in the single-dose study. Metformin had no effect on cimetidine pharmacokinetics.
Although such interactions remain theoretical (except for cimetidine), careful patient monitoring and dose adjustment of GLUMETZA and/or the interfering drug is recommended in patients who are taking cationic medications that are excreted via the proximal renal tubular secretory system.
Other — Certain drugs tend to produce hyperglycemia and may lead to loss of glycemic control. These drugs include the thiazides and other diuretics, corticosteroids, phenothiazines, thyroid products, estrogens, oral contraceptives, phenytoin, nicotinic acid, sympathomimetics, calcium channel blocking drugs, and isoniazid. When such drugs are administered to a patient receiving GLUMETZA, the patient should be closely observed for loss of blood glucose control. When such drugs are withdrawn from a patient receiving GLUMETZA, the patient should be observed closely for hypoglycemia. In healthy volunteers, the pharmacokinetics of metformin and propranolol, and metformin and ibuprofen were not affected when co-administered in single-dose interaction studies. Metformin is negligibly bound to plasma proteins and is, therefore, less likely to interact with highly protein-bound drugs such as salicylates, sulfonamides, chloramphenicol, and probenecid, as compared to the sulfonylureas, which are extensively bound to serum proteins.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Long-term carcinogenicity studies have been performed in Sprague Dawley rats at doses of 150, 300, and 450 mg/kg/day in males and 150, 450, 900, and 1200 mg/kg/day in females. These doses are approximately 2, 4, and 8 times in males, and 3, 7, 12, and 16 times in females of the maximum recommended human daily dose of 2000 mg based on body surface area comparisons. No evidence of carcinogenicity with metformin was found in either male or female rats. A carcinogenicity study was also performed in Tg.AC transgenic mice at doses up to 2000 mg applied dermally. No evidence of carcinogenicity was observed in male or female mice.
Genotoxicity assessments in the Ames test, gene mutation test (mouse lymphoma cells), chromosomal aberrations test (human lyhpocytes) and in vivo mouse micronucleus tests were negative. Fertility of male or female rats was not affected by metformin when administered at dose up to 600 mg/kg/day, which is approximately 3 times the maximum recommended human daily dose based on body surface area comparisons.
Pregnancy
Teratogenic Effects: Pregnancy Category B.
Metformin was not teratogenic in rats and rabbits at doses up to 600 mg/kg/day, which represent 3 and 6 times the maximum recommended human daily dose of 2000 mg based on body surface area comparison for rats and rabbits, respectively. However, because animal reproduction studies are not always predictive of human response, Metformin HCl should not be used during pregnancy unless clearly needed.
Nursing Mothers
Studies in lactating rats show that metformin is excreted into milk and reaches levels comparable to those in plasma. Similar studies have not been conducted in nursing mothers. Thus, the potential for hypoglycemia in nursing infants after Metformin HCl Oral Solution may exist.
Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
Geriatric Use
Clinical studies of GLUMETZA did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
This drug may be known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function. (See WARNINGS: Lactic Acidosis.)
ADVERSE REACTIONS
In clinical trials conducted in the U.S., over 1000 patients with type 2 diabetes mellitus have been treated with GLUMETZA 1500–2000 mg/day in active-controlled and placebo-controlled studies with the 500 mg dosage form.
In the 24-week active-controlled monotherapy trial, serious adverse events were reported in 3.6% (19/528) of the GLUMETZA-treated patients compared to 2.9% (5/174) of the patients treated with immediate-release metformin. During the 6-month open-label, uncontrolled, extension trial, an additional 10 (4.0%) GLUMETZA-treated patients reported a serious adverse event. In the add-on to sulfonylurea study, a serious adverse event was reported in 2.1% (9/431) of the GLUMETZA+glyburide treated patients compared to 1.4% (2/144) of the placebo+glyburide treated patients. When the data from all clinical trials were combined, the most frequently (incidence ≥0.5 %) reported serious adverse events classified by system organ class were gastrointestinal disorders (1.0% of GLUMETZA-treated patients compared to 0% of patients not treated with GLUMETZA) and cardiac disorders (0.4% of GLUMETZA-treated patients compared to 0.5% of patients not treated with GLUMETZA). Only 2 serious adverse events (unstable angina [n=2] and pancreatitis [n=2]) were reported in more than one GLUMETZA-treated patient.
In the placebo-controlled study, patients receiving background glyburide (SU; sulfonylurea) therapy were randomized to receive add-on treatment of either one of three different regimens of GLUMETZA or placebo. In total, 431 patients received GLUMETZA + SU and 144 patients placebo + SU. Adverse events reported in greater than 5% of patients treated with GLUMETZA that were more common in the combined GLUMETZA + SU group than in the placebo + SU group are shown in Table 5.
In 0.7% of patients treated with GLUMETZA + SU, diarrhea was responsible for discontinuation of study medication compared to zero in the placebo + SU group.
|
||
| Adverse Event (MedDRA Preferred Term) | Glumetza + SU (n = 431) | Placebo + SU (n = 144) |
| Hypoglycemia NOS | 13.7% | 4.9% |
| Diarrhea | 12.5% | 5.6% |
| Nausea | 6.7% | 4.2% |
In the same study, the following adverse events were reported by 1-5% of patients for the combined GLUMETZA + SU group and these events occurred more commonly in the GLUMETZA-treated than in the placebo-treated patients:
Ear and labyrinth disorders: ear pain
Gastrointestinal disorders: vomiting NOS, dyspepsia, flatulence, abdominal pain upper, abdominal distension, abdominal pain NOS, toothache, loose stools
General disorders and administration site conditions: asthenia, chest pain
Immune system disorders: seasonal allergy
Infections and infestations: gastroenteritis viral NOS, tooth abscess, tonsillitis, fungal infection NOS
Injury, poisoning and procedural complications: muscle strain
Musculoskeletal and connective tissue disorders: pain in limb, myalgia, muscle cramp
Nervous system disorders: dizziness, tremor, sinus headache, hypoaesthesia
Respiratory, thoracic and mediastinal disorders: nasal congestion
Skin and subcutaneous tissue disorders: contusion
Vascular disorders: hypertension NOS
No cases of overdose were reported during GLUMETZA clinical trials. It would be expected that adverse reactions of a more intense character including epigastric discomfort, nausea, and vomiting followed by diarrhea, drowsiness, weakness, dizziness, malaise and headache might be seen. Should those symptoms persist, lactic acidosis should be excluded. The drug should be discontinued and proper supportive therapy instituted. In other metformin clinical trials, hypoglycemia has not been seen even with ingestion of up to 85 grams of metformin, although lactic acidosis has occurred in such circumstances (see WARNINGS). Metformin is dialyzable with a clearance of up to 170 mL/min under good hemodynamic conditions. Therefore, hemodialysis may be useful for removal of accumulated drug from patients in whom metformin overdosage is suspected.
DOSAGE AND ADMINISTRATION
GLUMETZA should be taken once daily. However, there is no fixed dosage regimen for the management of hyperglycemia in patients with type 2 diabetes with GLUMETZA or any other pharmacologic agent. Dosage of GLUMETZA must be individualized on the basis of both effectiveness and tolerance, while not exceeding the maximum recommended daily dose. The maximum recommended daily dose of GLUMETZA is 2000 mg. GLUMETZA therapy should generally be initiated with 1000 mg daily which should be taken with food preferably in the evening. Gradual dose escalation from this low dose is recommended both to reduce gastrointestinal side effects and to permit identification of the minimum dose required for adequate glycemic control. During treatment initiation and dose titration (see Recommended Dosing Schedule), fasting plasma glucose should be used to determine the therapeutic response to GLUMETZA and identify the minimum effective dose. Thereafter, glycosylated hemoglobin should be measured at intervals of approximately three months. The therapeutic goal should be to decrease both fasting plasma glucose and glycosylated hemoglobin levels to normal or near normal by using the lowest effective dose of GLUMETZA, either when used as monotherapy or in combination with sulfonylurea or insulin.
Monitoring of blood glucose and glycosylated hemoglobin will also permit detection of primary failure, i.e., inadequate lowering of blood glucose at the maximum recommended dose of medication, and secondary failure, i.e., loss of an adequate blood glucose lowering response after an initial period of effectiveness. Short-term administration of GLUMETZA may be sufficient during periods of transient loss of control in patients usually well-controlled on diet alone. GLUMETZA tablets must be swallowed whole and never split, crushed or chewed. Occasionally, the inactive ingredients of GLUMETZA 500 mg may be eliminated in the feces as a soft, hydrated mass, while the 1000 mg may leave an insoluble shell. (See Patient Information.)
Recommended Dosing Schedule
Adults — In general, clinically significant responses are not seen at doses below 1500 mg per day. However, a lower recommended starting dose and gradually increased dosage is advised to minimize gastrointestinal symptoms. The starting dose of GLUMETZA is 1000 mg once daily which in order to maximize therapeutic efficacy must be taken with food preferably in the evening. Dosage increases should be made in increments of 500 mg weekly, up to a maximum of 2000 mg once daily with the evening meal. If glycemic control is not achieved on GLUMETZA 2000 mg once daily, a trial of GLUMETZA 1000 mg twice daily should be considered. (See CLINICAL PHARMACOLOGY, Clinical Studies).
In one trial, patients treated with immediate release metformin were switched to GLUMETZA. Results of this trial suggest that patients receiving immediate release metformin treatment can be switched to GLUMETZA once daily at the same total daily dose, up to 2000 mg once daily. Following a switch from immediate release metformin to GLUMETZA, glycemic control should be closely monitored and dosage adjustments made accordingly. (See CLINICAL PHARMACOLOGY, Clinical Studies).
Pediatrics — GLUMETZA has been studied in adult patients only.
Transfer From Other Antidiabetic Therapy
When transferring patients from standard oral hypoglycemic agents other than chlorpropamide to GLUMETZA, no transition period is generally necessary.
When transferring patients from chlorpropamide, care should be exercised during the first two weeks because of the prolonged retention of chlorpropamide in the body, leading to overlapping drug effects and possible hypoglycemia.
Concomitant GLUMETZA and Oral Sulfonylurea Therapy in Adult Patients
If patients have not responded to four weeks of the maximum dose of GLUMETZA monotherapy, consideration should be given to gradual addition of an oral sulfonylurea while continuing GLUMETZA at the maximum dose, even if prior primary or secondary failure to a sulfonylurea has occurred. Clinical and pharmacokinetic drug-drug interaction data are currently available only for metformin plus glyburide (glibenclamide). With concomitant GLUMETZA and sulfonylurea therapy, the desired control of blood glucose may be obtained by adjusting the dose of each drug.
However, attempts should be made to identify the minimum effective dose. With concomitant GLUMETZA and sulfonylurea therapy, the risk of hypoglycemia associated with sulfonylurea therapy continues and may be increased. Appropriate precautions should be taken. (See Package Insert of the respective sulfonylurea.) If patients have not satisfactorily responded to one to three months of concomitant therapy with the maximum dose of GLUMETZA and the maximum dose of an oral sulfonylurea, consider therapeutic alternatives including switching to insulin with or without GLUMETZA.
Concomitant GLUMETZA and Insulin Therapy in Adult Patients
The current insulin dose should be continued upon initiation of GLUMETZA. GLUMETZA therapy should be initiated at 500 mg once daily in patients on insulin therapy. For patients not responding adequately, the dose of GLUMETZA should be increased by 500 mg after approximately 1 week and by 500 mg every week thereafter until adequate glycemic control is achieved. The maximum recommended daily dose of GLUMETZA is 2000 mg.
It is recommended that the insulin dose be decreased by 10% to 25% when fasting plasma glucose concentrations decrease to less than 120 mg/dL in patients receiving concomitant insulin and GLUMETZA. Further adjustment should be individualized based on glucose-lowering response.
Specific Patient Populations
GLUMETZA is not recommended for use in pregnancy. GLUMETZA is not recommended in pediatric patients (below the age of 18 years). The initial and maintenance dosing of GLUMETZA should be conservative in patients with advanced age, due to the potential for decreased renal function in this population.
Any dosage adjustment should be based on a careful assessment of renal function.
Generally, elderly, debilitated, and malnourished patients should not be titrated to the maximum dose of GLUMETZA. Monitoring of renal function is necessary to aid in prevention of lactic acidosis, particularly in the elderly. (See WARNINGS.)
HOW SUPPLIED
GLUMETZA tablets-500 mg are available as blue, film coated, oval-shaped tablets debossed with “GMZ” on one side and “500” on the other side.
GLUMETZA tablets 1000 mg are available as white, film coated, oval-shaped tablets with “M1000” on one side.
They are supplied as follows:
| Package | Strength | NDC Code |
| Bottles of 100 | 500 mg | 13913-002-13 |
| Bottles of 90 | 1000 mg | 13913-003-16 |
Storage
Store at 20°-25°C (68°-77°F); excursions permitted to 15°-30°C (59°-86°F); see [USP Controlled Room Temperature.]
Rx Only
Depomed, Inc.
Menlo Park, CA
(866) 458-6389
©2008 Depomed, Inc.
www.GlumetzaXR.com
Revised December 2008
GLU-001-C.1
PATIENT INFORMATION
Rx Only
GLUMETZA (Gloo-met-za) (metformin hydrochloride extended-release tablets)
Read this information carefully before you start taking this medicine and each time you refill your prescription. There may be new information. This information does not take the place of your doctor’s advice. Ask your doctor or pharmacist if you do not understand some of this information or if you want to know more about this medicine.
What is the most important information I should know about GLUMETZA?
Warning: GLUMETZA can cause a rare, but serious condition called lactic acidosis (a buildup of an acid in the blood) that can cause death. Lactic acidosis is a medical emergency and must be treated in the hospital. Stop taking GLUMETZA and call your doctor right away if you get the following symptoms of lactic acidosis.
-
You feel very weak or tired.
-
You have unusual (not normal) muscle pain.
-
You have trouble breathing.
-
You have stomach pain with nausea and vomiting, and diarrhea.
-
You feel cold, especially in your arms and legs.
-
You feel dizzy or lightheaded.
-
You have a slow or irregular heartbeat.
- Your medical condition suddenly changes.
You have a higher chance for getting lactic acidosis with GLUMETZA if you:
-
have kidney or liver problems.
-
have congestive heart failure that requires treatments with medicines.
-
drink a lot of alcohol (very often or short-term “binge” drinking).
-
get dehydrated (lose a large amount of body fluids). This can happen if you are sick with a fever, vomiting, or diarrhea. Dehydration can also happen when you sweat a lot with activity or exercise and don’t drink enough fluids.
-
have certain x-ray test with injectable dye used.
-
have surgery.
-
have a heart attack, severe infection, or a stroke.
- are 80 years of age or older and have not had your kidney function tested.
What is GLUMETZA?
GLUMETZA is used along with diet and exercise to improve blood sugar control in adults with type 2 diabetes. GLUMETZA may also be used with another anti-diabetes medicine called a sulfonylurea or with insulin to improve blood sugar levels in adults. GLUMETZA helps control your blood sugar in a number of ways. These include helping your body respond better to the insulin it makes naturally, decreasing the amount of sugar your liver makes, and decreasing the amount of sugar your intestines absorb. GLUMETZA has not been studied in children under 18 years of age.
Who should not take GLUMETZA?
Do not take GLUMETZA if you:
- have kidney problems.
- have heart failure that is treated with medicines.
- have a condition called metabolic acidosis, including diabetic ketoacidosis. Diabetic ketoacidosis should be treated with insulin.
- are allergic to GLUMETZA or to any of its ingredients. See the end of this leaflet for a list of ingredients in GLUMETZA.
What should I tell my doctor before taking GLUMETZA?
Tell your doctor about all of your medical conditions including if you:
- have kidney problems.
- have liver problems.
- have heart problems.
- drink a lot of alcohol.
-
are pregnant or planning to become pregnant. It is not known if GLUMETZA can harm your unborn baby. Talk to your doctor about the best way to control your blood sugar levels while pregnant.
- are breastfeeding. It is not known if GLUMETZA passes into your milk and if it can harm your baby. Talk to your doctor about the best way to feed your baby while taking GLUMETZA.
Tell your doctor about all the medicines you take including prescription and nonprescription medicines, vitamins and herbal supplements. GLUMETZA and some of your other medicines can interact. You may need to have the dose of GLUMETZA or certain other medicines adjusted. Certain other medicines can affect your blood sugar control.
Know the medicines you take. Keep a list of them to show your doctor and pharmacist. Talk to your doctor before you start any new medicine.
How should I take GLUMETZA?
- Take GLUMETZA exactly as prescribed. Your doctor will usually start you on a low dose and increase your dose slowly to control your blood sugar levels. Do not change your dose unless told to do so by your doctor.
- Take GLUMETZA once a day in the evening with food.
-
Swallow GLUMETZA tablets whole. Never crush, split or chew GLUMETZA tablets. Tell your doctor if you cannot swallow tablets whole. Your doctor will prescribe a different medicine for you.
-
You may see the GLUMETZA tablet shell in your stool. You may also see a soft mass of the GLUMETZA inactive ingredients in your stool. Both of these are normal to see in your stool.
- Stay on your exercise and diet program and test your blood sugar regularly while taking GLUMETZA.
- Your doctor should monitor your diabetes and do blood tests on you from time to time to check your kidneys and your liver.
- If you miss a dose of GLUMETZA resume dosing according to schedule.
- If you take too much GLUMETZA or overdose, call your doctor or poison control center right away.
- You may need to stop GLUMETZA for a short period of time if you:
- are sick with severe vomiting, diarrhea or fever, or if you drink a much lower amount of liquid than normal.
- plan to have surgery.
- are having an x-ray procedure with an injection of dye.
- are sick with severe vomiting, diarrhea or fever, or if you drink a much lower amount of liquid than normal.
Call your doctor right away for instructions.
What should I avoid while taking GLUMETZA?
Do not drink a lot of alcoholic drinks while taking GLUMETZA. This means you should not binge drink for short periods, and you should not drink a lot of alcohol on a regular basis. Alcohol can increase the chance of getting lactic acidosis.
What are the side effects of GLUMETZA?
GLUMETZA can cause a rare, but serious side effect called lactic acidosis (a buildup of an acid in your blood) that can cause death. See “What is the most important information I should know about GLUMETZA?”
The most common side effects of GLUMETZA include diarrhea, nausea, and upset stomach. These side effects usually go away after you take the medicine for a while. Taking your medicine with the evening meal can help reduce these side effects.
GLUMETZA rarely causes low blood sugar (hypoglycemia) by itself. However, low blood sugar can happen if you do not eat enough, if you drink alcohol, or if you take other medicines to lower blood sugar.
Tell your doctor if you have side effects that bother you, last for more than a few weeks, come back after they have gone away, or start later in therapy. You may need a lower dose or need to stop taking GLUMETZA.
These are not all the side effects with GLUMETZA. For more information, ask your doctor or pharmacist.
How should I store GLUMETZA?
- Store GLUMETZA at room temperature, 59° to 86° F (15° to 30° C).
- Keep GLUMETZA and all medicines out of the reach of children.
General information about GLUMETZA.
Medicines are sometimes prescribed for conditions that are not mentioned in patient information leaflets. Do not use GLUMETZA for a condition for which it was not prescribed. Do not give GLUMETZA to other people, even if they have the same symptoms you have. It may harm them.
This leaflet summarizes the most important information about GLUMETZA. If you would like more information, talk with your doctor. You can ask your doctor or pharmacist for information about GLUMETZA that is written for health professionals or contact 1-866-458-6389.
What are the ingredients in GLUMETZA?
Active Ingredient: 500 mg or 1000 mg of metformin HCl
Inactive Ingredient: Each 500 mg tablet contains coloring, hypromellose, magnesium stearate, microcrystalline cellulose and polyethylene oxide. Each 1000 mg tablet contains contains colloidal silicon dioxide, polyvinyl alcohol, crospovidone, glyceryl behenate, polyacrylate dispersion, hypromellose, talc, polyethylene glycol, titanium dioxide, simethicone emulsion, polysorbate and coloring. GLUMETZA 500 mg and 1000 mg tablets both utilize advanced, polymer-based, oral drug delivery systems, which allow delivery of metformin HCl to the upper GI tract.
Rx Only
Depomed, Inc.
Menlo Park, CA
(866) 458-6389
©2008 Depomed, Inc.
www.GlumetzaXR.com
PRINCIPAL DISPLAY PANEL
Package Label – 100-count Bottle, 500 mg Tablets
100 Tablets
NDC 13913-002-13
Glumetza® (metformin hydrochloride extended-release tablets)
500 mg
ONCE
DAILY
Rx
ONLY
DepomedTM

PRINCIPAL DISPLAY PANEL
Package Label – 90-count Bottle, 1000 mg Tablets
90 Tablets
NDC 13913-003-16
Glumetza® (metformin hydrochloride extended-release tablets)
1000 mg
ONCE
DAILY
Rx
ONLY
DepomedTM

| GLUMETZA
metformin hydrochloride tablet, film coated, extended release |
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
|
||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| NDA | NDA021748 | 08/01/2006 | |
| GLUMETZA
metformin hydrochloride tablet, film coated, extended release |
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
| Marketing Information | |||
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| NDA | NDA021748 | 06/17/2008 | |
| Labeler - Depomed, Inc. (937562890) |
| Establishment | |||
| Name | Address | ID/FEI | Operations |
| Patheon Puerto Rico, Inc. | 174050377 | MANUFACTURE | |