EMEND
-
fosaprepitant dimeglumine injection, powder, lyophilized, for solution
Merck & Co., Inc.
----------
EMEND®
(fosaprepitant dimeglumine)
for Injection
DESCRIPTION
EMEND1 (fosaprepitant dimeglumine) for Injection is a sterile, lyophilized prodrug of aprepitant and is chemically described as 1-Deoxy-1-(methylamino)-D-glucitol[3-[[(2R,3S)-2-[(1R)-1-[3,5-bis(trifluoromethyl)phenyl]ethoxy]-3-(4-fluorophenyl)-4-morpholinyl]methyl]-2,5-dihydro-5-oxo-1H-1,2,4-triazol-1-yl]phosphonate (2:1) (salt).
Its empirical formula is C23H22F7N4O6P · 2(C7H17NO5) and its structural formula is:
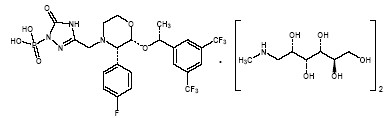
Fosaprepitant dimeglumine is a white to off-white amorphous powder with a molecular weight of 1004.83. It is freely soluble in water.
EMEND for Injection is a lyophilized prodrug of aprepitant containing polysorbate 80 (PS80), to be administered intravenously as an infusion.
Each vial of EMEND for Injection for intravenous administration contains 188 mg of fosaprepitant dimeglumine equivalent to 115 mg of fosaprepitant and the following inactive ingredients: edetate disodium (14.4 mg), polysorbate 80 (57.5 mg), lactose anhydrous (287.5 mg), sodium hydroxide and/or hydrochloric acid (for pH adjustment). Fosaprepitant dimeglumine hereafter will be referred to as fosaprepitant.
Aprepitant is a substance P/neurokinin 1 (NK1) receptor antagonist, chemically described as 5-[[(2R,3S )-2-[(1R)-1-[3,5-bis(trifluoromethyl)phenyl]ethoxy]-3-(4-fluorophenyl)-4-morpholinyl]methyl]-1,2-dihydro-3H-1,2,4-triazol-3-one.
Its empirical formula is C23H21F7N4O3, and its structural formula is:
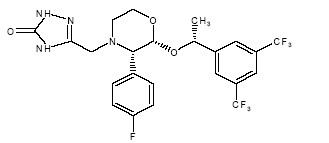
- 1
-
Trademark of MERCK & CO., Inc.
COPYRIGHT © 2008, MERCK & CO., Inc.
All rights reserved
CLINICAL PHARMACOLOGY
Fosaprepitant, a prodrug of aprepitant, when administered intravenously is rapidly converted to aprepitant, a substance P/neurokinin 1 (NK1) receptor antagonist. Plasma concentrations of fosaprepitant are below the limits of quantification (10 ng/mL) within 30 minutes of the completion of infusion (see CLINICAL PHARMACOLOGY, Pharmacokinetics). Upon conversion of 115 mg of fosaprepitant to aprepitant, 18.3 mg of phosphate and 73 mg of meglumine are liberated from fosaprepitant.
Mechanism of Action
Fosaprepitant is a prodrug of aprepitant and accordingly, its antiemetic effects are attributable to aprepitant.
Aprepitant is a selective high-affinity antagonist of human substance P/neurokinin 1 (NK1) receptors. Aprepitant has little or no affinity for serotonin (5-HT3), dopamine, and corticosteroid receptors, the targets of existing therapies for chemotherapy-induced nausea and vomiting (CINV). Aprepitant has been shown in animal models to inhibit emesis induced by cytotoxic chemotherapeutic agents, such as cisplatin, via central actions. Animal and human Positron Emission Tomography (PET) studies with aprepitant have shown that it crosses the blood brain barrier and occupies brain NK1 receptors. Animal and human studies show that aprepitant augments the antiemetic activity of the 5-HT3-receptor antagonist ondansetron and the corticosteroid dexamethasone and inhibits both the acute and delayed phases of cisplatin-induced emesis.
Pharmacokinetics
Aprepitant after Fosaprepitant Administration
Following a single intravenous dose of fosaprepitant administered as a 15-minute infusion to healthy volunteers the mean AUC0-∞ of aprepitant was 31.7 (± 14.3) mcg•hr/mL and the mean maximal aprepitant concentration (Cmax) was 3.27 (± 1.16) mcg/mL. The mean aprepitant plasma concentration at 24 hours postdose was similar between the 125-mg oral aprepitant dose and the 115-mg intravenous fosaprepitant dose (See Figure 1).
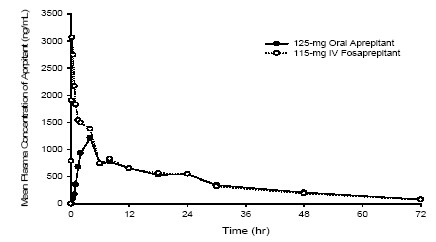
Figure 1: Mean Plasma Concentration of Aprepitant Following 125-mg Oral Aprepitant and 115-mg I.V. Fosaprepitant
Distribution
Fosaprepitant is rapidly converted to aprepitant. Aprepitant is greater than 95% bound to plasma proteins. The mean apparent volume of distribution at steady state (Vdss) is approximately 70 L in humans.
Aprepitant crosses the placenta in rats and rabbits and crosses the blood brain barrier in humans (see CLINICAL PHARMACOLOGY, Mechanism of Action).
Metabolism
Fosaprepitant was rapidly converted to aprepitant in in vitro incubations with liver preparations from nonclinical species (rat and dog) and humans. Furthermore, fosaprepitant underwent rapid and nearly complete conversion to aprepitant in S9 preparations from multiple other human tissues including kidney, lung and ileum. Thus, it appears that the conversion of fosaprepitant to aprepitant can occur in multiple extrahepatic tissues in addition to the liver. In humans, fosaprepitant administered intravenously was rapidly converted to aprepitant within 30 minutes following the end of infusion.
Aprepitant undergoes extensive metabolism. In vitro studies using human liver microsomes indicate that aprepitant is metabolized primarily by CYP3A4 with minor metabolism by CYP1A2 and CYP2C19. Metabolism is largely via oxidation at the morpholine ring and its side chains. No metabolism by CYP2D6, CYP2C9, or CYP2E1 was detected. In healthy young adults, aprepitant accounts for approximately 24% of the radioactivity in plasma over 72 hours following a single oral 300-mg dose of [14C]-aprepitant, indicating a substantial presence of metabolites in the plasma. Seven metabolites of aprepitant, which are only weakly active, have been identified in human plasma.
Excretion
Following administration of a single I.V. 100-mg dose of [14C]-fosaprepitant to healthy subjects, 57% of the radioactivity was recovered in urine and 45% in feces.
Aprepitant is eliminated primarily by metabolism; aprepitant is not renally excreted. The apparent terminal half-life of aprepitant ranged from approximately 9 to 13 hours.
Special Populations
Fosaprepitant, a prodrug of aprepitant, when administered intravenously is rapidly converted to aprepitant.
Gender
Following oral administration of a single 125-mg dose of aprepitant, no difference in AUC0-24hr was observed between males and females. The Cmax for aprepitant is 16% higher in females as compared with males. The half-life of aprepitant is 25% lower in females as compared with males and Tmax occurs at approximately the same time. These differences are not considered clinically meaningful. No dosage adjustment is necessary based on gender.
Geriatric
Following oral administration of a single 125-mg dose of aprepitant on Day 1 and 80 mg once daily on Days 2 through 5, the AUC0-24hr of aprepitant was 21% higher on Day 1 and 36% higher on Day 5 in elderly (≥65 years) relative to younger adults. The Cmax was 10% higher on Day 1 and 24% higher on Day 5 in elderly relative to younger adults. These differences are not considered clinically meaningful. No dosage adjustment is necessary in elderly patients.
Pediatric
Fosaprepitant has not been evaluated in patients below 18 years of age.
Race
Following oral administration of a single 125-mg dose of aprepitant, the AUC0-24hr is approximately 25% and 29% higher in Hispanics as compared with Whites and Blacks, respectively. The Cmax is 22% and 31% higher in Hispanics as compared with Whites and Blacks, respectively. These differences are not considered clinically meaningful. There was no difference in AUC0-24hr or Cmax between Whites and Blacks. No dosage adjustment is necessary based on race.
Hepatic Insufficiency
Fosaprepitant is metabolized in various extrahepatic tissues; therefore hepatic insufficiency is not expected to alter the conversion of fosaprepitant to aprepitant.
Oral aprepitant was well tolerated in patients with mild to moderate hepatic insufficiency. Following administration of a single 125-mg dose of oral aprepitant on Day 1 and 80 mg once daily on Days 2 and 3 to patients with mild hepatic insufficiency (Child-Pugh score 5 to 6), the AUC0-24hr of aprepitant was 11% lower on Day 1 and 36% lower on Day 3, as compared with healthy subjects given the same regimen. In patients with moderate hepatic insufficiency (Child-Pugh score 7 to 9), the AUC0-24hr of aprepitant was 10% higher on Day 1 and 18% higher on Day 3, as compared with healthy subjects given the same regimen. These differences in AUC0-24hr are not considered clinically meaningful; therefore, no dosage adjustment is necessary in patients with mild to moderate hepatic insufficiency.
There are no clinical or pharmacokinetic data in patients with severe hepatic insufficiency (Child-Pugh score >9) (see PRECAUTIONS).
Renal Insufficiency
A single 240-mg dose of oral aprepitant was administered to patients with severe renal insufficiency (CrCl<30 mL/min) and to patients with end stage renal disease (ESRD) requiring hemodialysis.
In patients with severe renal insufficiency, the AUC0-∞ of total aprepitant (unbound and protein bound) decreased by 21% and Cmax decreased by 32%, relative to healthy subjects. In patients with ESRD undergoing hemodialysis, the AUC0-∞ of total aprepitant decreased by 42% and Cmax decreased by 32%. Due to modest decreases in protein binding of aprepitant in patients with renal disease, the AUC of pharmacologically active unbound drug was not significantly affected in patients with renal insufficiency compared with healthy subjects. Hemodialysis conducted 4 or 48 hours after dosing had no significant effect on the pharmacokinetics of aprepitant; less than 0.2% of the dose was recovered in the dialysate.
No dosage adjustment is necessary for patients with renal insufficiency or for patients with ESRD undergoing hemodialysis.
Pharmacodynamics
Cardiac Electrophysiology
In a randomized, double-blind, positive-controlled, thorough QTc study, a single 200-mg dose of fosaprepitant had no effect on the QTc interval.
Clinical Studies
Fosaprepitant, a prodrug of aprepitant, when administered intravenously is rapidly converted to aprepitant. Fosaprepitant 115 mg I.V. infused over 15 minutes can be substituted for 125 mg oral aprepitant on Day 1 (see DOSAGE AND ADMINISTRATION). Pivotal efficacy studies were conducted with oral aprepitant.
Oral administration of aprepitant in combination with ondansetron and dexamethasone (aprepitant regimen) has been shown to prevent acute and delayed nausea and vomiting associated with highly emetogenic chemotherapy including high-dose cisplatin, and nausea and vomiting associated with moderately emetogenic chemotherapy.
Highly Emetogenic Chemotherapy
In 2 multicenter, randomized, parallel, double-blind, controlled clinical studies, the aprepitant regimen (see table below) was compared with standard therapy in patients receiving a chemotherapy regimen that included cisplatin >50 mg/m2 (mean cisplatin dose = 80.2 mg/m2). Of the 550 patients who were randomized to receive the aprepitant regimen, 42% were women, 58% men, 59% White, 3% Asian, 5% Black, 12% Hispanic American, and 21% Multi-Racial. The aprepitant-treated patients in these clinical studies ranged from 14 to 84 years of age, with a mean age of 56 years. 170 patients were 65 years or older, with 29 patients being 75 years or older.
Patients (N = 1105) were randomized to either the aprepitant regimen (N = 550) or standard therapy (N = 555). The treatment regimens are defined in the table below.
| Treatment Regimen | Day 1 | Days 2 to 4 |
| Aprepitant | Aprepitant 125 mg PO Dexamethasone 12 mg PO Ondansetron 32 mg I.V. | Aprepitant 80 mg PO Daily (Days 2 and 3 only) Dexamethasone 8 mg PO Daily (morning) |
| Standard Therapy | Dexamethasone 20 mg PO Ondansetron 32 mg I.V. | Dexamethasone 8 mg PO Daily (morning) Dexamethasone 8 mg PO Daily (evening) |
| Aprepitant placebo and dexamethasone placebo were used to maintain blinding. | ||
During these studies 95% of the patients in the aprepitant group received a concomitant chemotherapeutic agent in addition to protocol-mandated cisplatin. The most common chemotherapeutic agents and the number of aprepitant patients exposed follow: etoposide (106), fluorouracil (100), gemcitabine (89), vinorelbine (82), paclitaxel (52), cyclophosphamide (50), doxorubicin (38), docetaxel (11).
The antiemetic activity of oral aprepitant was evaluated during the acute phase (0 to 24 hours post-cisplatin treatment), the delayed phase (25 to 120 hours post-cisplatin treatment) and overall (0 to 120 hours post-cisplatin treatment) in Cycle 1. Efficacy was based on evaluation of the following endpoints:
Primary endpoint:
- complete response (defined as no emetic episodes and no use of rescue therapy)
Other prespecified endpoints:
- complete protection (defined as no emetic episodes, no use of rescue therapy, and a maximum nausea visual analogue scale [VAS] score <25 mm on a 0 to 100 mm scale)
- no emesis (defined as no emetic episodes regardless of use of rescue therapy)
- no nausea (maximum VAS <5 mm on a 0 to 100 mm scale)
- no significant nausea (maximum VAS <25 mm on a 0 to 100 mm scale)
A summary of the key study results from each individual study analysis is shown in Table 1 and in Table 2.
| ENDPOINTS | Aprepitant Regimen (N = 260)* % | Standard Therapy (N = 261)* % | p-Value |
|
|||
| PRIMARY ENDPOINT | |||
| Complete Response | |||
| Overall† | 73 | 52 | <0.001 |
| OTHER PRESPECIFIED ENDPOINTS | |||
| Complete Response | |||
| Acute phase‡
Delayed phase§ | 89 75 | 78 56 | <0.001 <0.001 |
| Complete Protection | |||
| Overall Acute phase Delayed phase | 63 85 66 | 49 75 52 | 0.001 NS¶ <0.001 |
| No Emesis | |||
| Overall Acute phase Delayed phase | 78 90 81 | 55 79 59 | <0.001 0.001 <0.001 |
| No Nausea | |||
| Overall Delayed phase | 48 51 | 44 48 | NS#
NS# |
| No Significant Nausea | |||
| Overall Delayed phase | 73 75 | 66 69 | NS#
NS# |
| Visual analogue scale (VAS) score range: 0 mm = no nausea; 100 mm = nausea as bad as it could be. | |||
|
|||
| ENDPOINTS | Aprepitant Regimen (N = 261)* % | Standard Therapy (N = 263)* % | p-Value |
| PRIMARY ENDPOINT | |||
| Complete Response | |||
| Overall† | 63 | 43 | <0.001 |
| OTHER PRESPECIFIED ENDPOINTS | |||
| Complete Response | |||
| Acute phase‡
Delayed phase§ | 83 68 | 68 47 | <0.001 <0.001 |
| Complete Protection | |||
| Overall Acute phase Delayed phase | 56 80 61 | 41 65 44 | <0.001 <0.001 <0.001 |
| No Emesis | |||
| Overall Acute phase Delayed phase | 66 84 72 | 44 69 48 | <0.001 <0.001 <0.001 |
| No Nausea | |||
| Overall Delayed phase | 49 53 | 39 40 | NS¶
NS¶ |
| No Significant Nausea | |||
| Overall Delayed phase | 71 73 | 64 65 | NS#
NS# |
| Visual analogue scale (VAS) score range: 0 mm = no nausea; 100 mm = nausea as bad as it could be. | |||
In both studies, a statistically significantly higher proportion of patients receiving the aprepitant regimen in Cycle 1 had a complete response (primary endpoint), compared with patients receiving standard therapy. A statistically significant difference in complete response in favor of the aprepitant regimen was also observed when the acute phase and the delayed phase were analyzed separately.
In both studies, the estimated time to first emesis after initiation of cisplatin treatment was longer with the aprepitant regimen, and the incidence of first emesis was reduced in the aprepitant regimen group compared with standard therapy group as depicted in the Kaplan-Meier curves in Figure 2.
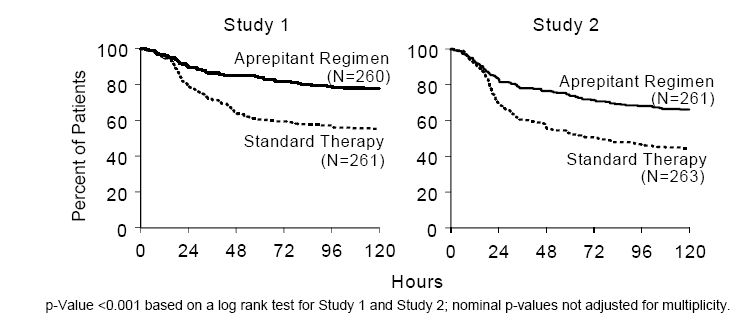
Figure 2: Percent of Patients Receiving Highly Emetogenic Chemotherapy Who Remain Emesis Free Over Time – Cycle 1
Patient-Reported Outcomes: The impact of nausea and vomiting on patients’ daily lives was assessed in Cycle 1 of both Phase III studies using the Functional Living Index–Emesis (FLIE), a validated nausea- and vomiting-specific patient-reported outcome measure. Minimal or no impact of nausea and vomiting on patients’ daily lives is defined as a FLIE total score >108. In each of the 2 studies, a higher proportion of patients receiving the aprepitant regimen reported minimal or no impact of nausea and vomiting on daily life (Study 1: 74% versus 64%; Study 2: 75% versus 64%).
Multiple-Cycle Extension: In the same 2 clinical studies, patients continued into the Multiple-Cycle extension for up to 5 additional cycles of chemotherapy. The proportion of patients with no emesis and no significant nausea by treatment group at each cycle is depicted in Figure 3. Antiemetic effectiveness for the patients receiving the aprepitant regimen is maintained throughout repeat cycles for those patients continuing in each of the multiple cycles.
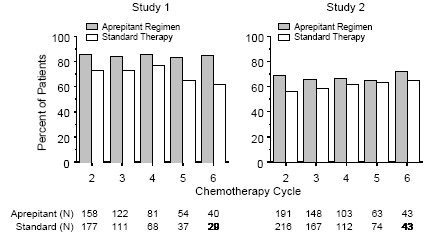
Figure 3: Proportion of Patients Receiving Highly Emetogenic Chemotherapy With No Emesis and No Significant Nausea by Treatment Group and Cycle
Moderately Emetogenic Chemotherapy
In a multicenter, randomized, double-blind, parallel-group, clinical study in breast cancer patients, the aprepitant regimen (see table that follows) was compared with a standard of care therapy in patients receiving a moderately emetogenic chemotherapy regimen that included cyclophosphamide 750-1500 mg/m2; or cyclophosphamide 500-1500 mg/m2 and doxorubicin (≤60 mg/m2) or epirubicin (≤100 mg/m2).
In this study, the most common combinations were cyclophosphamide + doxorubicin (60.6%); and cyclophosphamide + epirubicin + fluorouracil (21.6%).
Of the 438 patients who were randomized to receive the aprepitant regimen, 99.5% were women. Of these, approximately 80% were White, 8% Black, 8% Asian, 4% Hispanic, and <1% Other. The aprepitant-treated patients in this clinical study ranged from 25 to 78 years of age, with a mean age of 53 years; 70 patients were 65 years or older, with 12 patients being over 74 years.
Patients (N = 866) were randomized to either the aprepitant regimen (N = 438) or standard therapy (N = 428). The treatment regimens are defined in the table that follows.
| Treatment Regimen | Day 1 | Days 2 to 3 |
| Aprepitant | Aprepitant 125 mg PO*
Dexamethasone 12 mg PO† Ondansetron 8 mg PO x 2 doses‡ | Aprepitant 80 mg PO Daily |
| Standard Therapy | Dexamethasone 20 mg PO Ondansetron 8 mg PO x 2 doses | Ondansetron 8 mg PO Daily (every 12 hours) |
| Aprepitant placebo and dexamethasone placebo were used to maintain blinding. | ||
The antiemetic activity of oral aprepitant was evaluated based on the following endpoints:
Primary endpoint:
Complete response (defined as no emetic episodes and no use of rescue therapy) in the overall phase (0 to 120 hours post-chemotherapy)
Other prespecified endpoints:
- no emesis (defined as no emetic episodes regardless of use of rescue therapy)
- no nausea (maximum VAS <5 mm on a 0 to 100 mm scale)
- no significant nausea (maximum VAS <25 mm on a 0 to 100 mm scale)
- complete protection (defined as no emetic episodes, no use of rescue therapy, and a maximum nausea visual analogue scale [VAS] score <25 mm on a 0 to 100 mm scale)
- complete response during the acute and delayed phases.
A summary of the key results from this study is shown in Table 3.
| ENDPOINTS | Aprepitant Regimen (N = 433)* % | Standard Therapy (N = 424)* % | p-Value |
| PRIMARY ENDPOINT | |||
| Complete Response † | 51 | 42 | 0.015 |
| OTHER PRESPECIFIED ENDPOINTS | |||
| No Emesis | 76 | 59 | NS‡ |
| No Nausea | 33 | 33 | NS |
| No Significant Nausea | 61 | 56 | NS |
| No Rescue Therapy | 59 | 56 | NS |
| Complete Protection | 43 | 37 | NS |
In this study, a statistically significantly (p=0.015) higher proportion of patients receiving the aprepitant regimen (51%) in Cycle 1 had a complete response (primary endpoint) during the overall phase compared with patients receiving standard therapy (42%). The difference between treatment groups was primarily driven by the “No Emesis Endpoint”, a principal component of this composite primary endpoint. In addition, a higher proportion of patients receiving the aprepitant regimen in Cycle 1 had a complete response during the acute (0-24 hours) and delayed (25-120 hours) phases compared with patients receiving standard therapy; however, the treatment group differences failed to reach statistical significance, after multiplicity adjustments.
Patient-Reported Outcomes: In a phase III study in patients receiving moderately emetogenic chemotherapy, the impact of nausea and vomiting on patients’ daily lives was assessed in Cycle 1 using the FLIE. A higher proportion of patients receiving the aprepitant regimen reported minimal or no impact on daily life (64% versus 56%). This difference between treatment groups was primarily driven by the “No Vomiting Domain” of this composite endpoint.
Multiple-Cycle Extension: Patients receiving moderately emetogenic chemotherapy were permitted to continue into the Multiple-Cycle extension of the study for up to 3 additional cycles of chemotherapy. Antiemetic effect for patients receiving the aprepitant regimen is maintained during all cycles.
INDICATIONS AND USAGE
EMEND for Injection, in combination with other antiemetic agents, is indicated for the:
- prevention of acute and delayed nausea and vomiting associated with initial and repeat courses of highly emetogenic cancer chemotherapy including high-dose cisplatin.
- prevention of nausea and vomiting associated with initial and repeat courses of moderately emetogenic cancer chemotherapy (see DOSAGE AND ADMINISTRATION).
CONTRAINDICATIONS
EMEND for Injection is contraindicated in patients who are hypersensitive to EMEND for Injection, aprepitant, polysorbate 80 or any other components of the product.
Aprepitant, when administered orally, is a moderate cytochrome P450 isoenzyme 3A4 (CYP3A4) inhibitor following the 3-day antiemetic dosing regimen for CINV. Since fosaprepitant is rapidly converted to aprepitant, fosaprepitant should not be used concurrently with pimozide, terfenadine, astemizole, or cisapride. Inhibition of CYP3A4 by aprepitant could result in elevated plasma concentrations of these drugs, potentially causing serious or life-threatening reactions (see PRECAUTIONS, Drug Interactions).
PRECAUTIONS
General
Fosaprepitant is rapidly converted to aprepitant, which is a moderate inhibitor of CYP3A4 when administered as a 3-day antiemetic dosing regimen for CINV. Fosaprepitant should be used with caution in patients receiving concomitant medications that are primarily metabolized through CYP3A4. Inhibition of CYP3A4 by aprepitant could result in elevated plasma concentrations of these concomitant medications. When fosaprepitant is used concomitantly with another CYP3A4 inhibitor, aprepitant plasma concentrations could be elevated. (See PRECAUTIONS; Drug Interactions.)
Chemotherapy agents that are known to be metabolized by CYP3A4 include docetaxel, paclitaxel, etoposide, irinotecan, ifosfamide, imatinib, vinorelbine, vinblastine and vincristine. In clinical studies, the oral aprepitant regimen was administered commonly with etoposide, vinorelbine, or paclitaxel. The doses of these agents were not adjusted to account for potential drug interactions.
In separate pharmacokinetic studies no clinically significant change in docetaxel or vinorelbine pharmacokinetics was observed when the oral aprepitant regimen was co-administered.
Due to the small number of patients in clinical studies who received the CYP3A4 substrates vinblastine, vincristine, or ifosfamide, particular caution and careful monitoring are advised in patients receiving these agents or other chemotherapy agents metabolized primarily by CYP3A4 that were not studied (see PRECAUTIONS, Drug Interactions).
Chronic continuous use of EMEND for Injection for prevention of nausea and vomiting is not recommended because it has not been studied and because the drug interaction profile may change during chronic continuous use.
Coadministration of aprepitant with warfarin may result in a clinically significant decrease in International Normalized Ratio (INR) of prothrombin time. In patients on chronic warfarin therapy, the INR should be closely monitored in the 2-week period, particularly at 7 to 10 days, following initiation of the 3-day regimen of fosaprepitant followed by oral aprepitant with each chemotherapy cycle (see PRECAUTIONS, Drug Interactions).
Upon coadministration with aprepitant, the efficacy of hormonal contraceptives during and for 28 days following the last dose of aprepitant may be reduced. Alternative or back-up methods of contraception should be used during treatment with aprepitant and for 1 month following the last dose of aprepitant (see PRECAUTIONS, Drug Interactions).
There are no clinical or pharmacokinetic data in patients with severe hepatic insufficiency (Child-Pugh score >9). Therefore, caution should be exercised when fosaprepitant or aprepitant is administered in these patients (see CLINICAL PHARMACOLOGY, Special Populations, Hepatic Insufficiency and DOSAGE AND ADMINISTRATION).
Information for Patients
Physicians should instruct their patients to read the patient package insert before starting therapy with EMEND for Injection and to reread it each time the prescription is renewed.
Patients should follow the physician’s instructions for the EMEND for Injection regimen.
For the prevention of CINV, patients should be given their dose of EMEND for Injection as an infusion over 15 minutes, 30 minutes prior to chemotherapy on Day 1.
Allergic reactions, which may be serious, and may include hives, rash and itching and cause difficulty in breathing or swallowing, have been reported in general use with EMEND. Patients should be instructed to stop using EMEND and report to their doctor right away if they experience an allergic reaction.
EMEND for Injection may interact with some drugs including chemotherapy; therefore, patients should be advised to report to their doctor the use of any other prescription, non-prescription medication or herbal products.
Patients on chronic warfarin therapy should be instructed to have their clotting status closely monitored in the 2-week period, particularly at 7 to 10 days, following initiation of the 3-day regimen of fosaprepitant followed by aprepitant, with each chemotherapy cycle.
Administration of EMEND for Injection may reduce the efficacy of hormonal contraceptives. Patients should be advised to use alternative or back-up methods of contraception during treatment with EMEND for Injection and for 1 month following the last dose of the 3-day aprepitant regimen.
Drug Interactions
Drug interactions following administration of fosaprepitant are likely to occur with drugs that interact with oral aprepitant. The following information was derived from data with oral aprepitant and one study conducted with fosaprepitant and oral midazolam.
Aprepitant is a substrate, a moderate inhibitor, and an inducer of CYP3A4 when administered as a 3-day antiemetic dosing regimen for CINV. Aprepitant is also an inducer of CYP2C9.
Effect of aprepitant on the pharmacokinetics of other agents
As a moderate inhibitor of CYP3A4, aprepitant can increase plasma concentrations of orally coadministered medicinal products that are metabolized through CYP3A4 (see CONTRAINDICATIONS).
Aprepitant has been shown to induce the metabolism of S(-) warfarin and tolbutamide, which are metabolized through CYP2C9. Coadministration of fosaprepitant or oral aprepitant with these drugs or other drugs that are known to be metabolized by CYP2C9, such as phenytoin, may result in lower plasma concentrations of these drugs.
Fosaprepitant or aprepitant is unlikely to interact with drugs that are substrates for the P-glycoprotein transporter, as demonstrated by the lack of interaction of oral aprepitant with digoxin in a clinical drug interaction study.
5-HT3 antagonists: In clinical drug interaction studies, aprepitant did not have clinically important effects on the pharmacokinetics of ondansetron, granisetron or hydrodolasetron (the active metabolite of dolasetron).
Corticosteroids:
Dexamethasone: Oral aprepitant, when given as a regimen of 125 mg with dexamethasone coadministered orally as 20 mg on Day 1, and oral aprepitant when given as 80 mg/day with dexamethasone coadministered orally as 8 mg on Days 2 through 5, increased the AUC of dexamethasone, a CYP3A4 substrate, by 2.2-fold on Days 1 and 5. The oral dexamethasone doses should be reduced by approximately 50% when coadministered with a regimen of fosaprepitant followed by aprepitant, to achieve exposures of dexamethasone similar to those obtained when dexamethasone is given without aprepitant. The daily dose of dexamethasone administered in clinical CINV studies with oral aprepitant reflects an approximate 50% reduction of the dose of dexamethasone (see DOSAGE AND ADMINISTRATION).
Methylprednisolone: Oral aprepitant, when given as a regimen of 125 mg on Day 1 and 80 mg/day on Days 2 and 3, increased the AUC of methylprednisolone, a CYP3A4 substrate, by 1.34-fold on Day 1 and by 2.5-fold on Day 3, when methylprednisolone was coadministered intravenously as 125 mg on Day 1 and orally as 40 mg on Days 2 and 3. The I.V. methylprednisolone dose should be reduced by approximately 25%, and the oral methylprednisolone dose should be reduced by approximately 50% when coadministered with a regimen of fosaprepitant followed by aprepitant to achieve exposures of methylprednisolone similar to those obtained when it is given without aprepitant.
Chemotherapeutic agents: See PRECAUTIONS, General.
Docetaxel: In a pharmacokinetic study, oral aprepitant (CINV regimen) did not influence the pharmacokinetics of docetaxel.
Vinorelbine: In a pharmacokinetic study, oral aprepitant (CINV regimen) did not influence the pharmacokinetics of vinorelbine to a clinically significant degree.
Warfarin: A single 125-mg dose of oral aprepitant was administered on Day 1 and 80 mg/day on Days 2 and 3 to healthy subjects who were stabilized on chronic warfarin therapy. Although there was no effect of oral aprepitant on the plasma AUC of R(+) or S(-) warfarin determined on Day 3, there was a 34% decrease in S(-) warfarin (a CYP2C9 substrate) trough concentration accompanied by a 14% decrease in the prothrombin time (reported as International Normalized Ratio or INR) 5 days after completion of dosing with oral aprepitant. In patients on chronic warfarin therapy, the prothrombin time (INR) should be closely monitored in the 2-week period, particularly at 7 to 10 days, following initiation of the 3-day regimen of fosaprepitant followed by aprepitant with each chemotherapy cycle.
Tolbutamide: Oral aprepitant, when given as 125 mg on Day 1 and 80 mg/day on Days 2 and 3, decreased the AUC of tolbutamide (a CYP2C9 substrate) by 23% on Day 4, 28% on Day 8, and 15% on Day 15, when a single dose of tolbutamide 500 mg was administered orally prior to the administration of the 3-day regimen of oral aprepitant and on Days 4, 8, and 15.
Oral contraceptives: Aprepitant, when given once daily for 14 days as a 100-mg capsule with an oral contraceptive containing 35 mcg of ethinyl estradiol and 1 mg of norethindrone, decreased the AUC of ethinyl estradiol by 43%, and decreased the AUC of norethindrone by 8%.
In another study, a daily dose of an oral contraceptive containing ethinyl estradiol and norethindrone was administered on Days 1 through 21, and oral aprepitant was given as a 3-day regimen of 125 mg on Day 8 and 80 mg/day on Days 9 and 10 with ondansetron 32 mg I.V. on Day 8 and oral dexamethasone given as 12 mg on Day 8 and 8 mg/day on Days 9, 10, and 11. In the study, the AUC of ethinyl estradiol decreased by 19% on Day 10 and there was as much as a 64% decrease in ethinyl estradiol trough concentrations during Days 9 through 21. While there was no effect of oral aprepitant on the AUC of norethindrone on Day 10, there was as much as a 60% decrease in norethindrone trough concentrations during Days 9 through 21. The coadministration of fosaprepitant or aprepitant may reduce the efficacy of hormonal contraceptives during and for 28 days after administration of the last dose of either. Alternative or back-up methods of contraception should be used during treatment with fosaprepitant and aprepitant and for 1 month following the last dose.
Midazolam: A study was completed with fosaprepitant and oral midazolam. Fosaprepitant was given at a dose of 100 mg over 15 minutes along with a single dose of midazolam 2 mg. The plasma AUC of midazolam was increased by 1.6-fold. This effect was not considered clinically important.
Oral aprepitant increased the AUC of midazolam by 2.3-fold on Day 1 and 3.3-fold on Day 5, when a single oral dose of midazolam 2 mg was coadministered on Day 1 and Day 5 of a regimen of oral aprepitant 125 mg on Day 1 and 80 mg/day on Days 2 through 5. The potential effects of increased plasma concentrations of midazolam or other benzodiazepines metabolized via CYP3A4 (alprazolam, triazolam) should be considered when coadministering these agents with a 3-day regimen of fosaprepitant followed by aprepitant. In another study with intravenous administration of midazolam, oral aprepitant was given as 125 mg on Day 1 and 80 mg/day on Days 2 and 3, and midazolam 2 mg I.V. was given prior to the administration of the 3-day regimen of oral aprepitant and on Days 4, 8, and 15. Oral aprepitant increased the AUC of midazolam by 25% on Day 4 and decreased the AUC of midazolam by 19% on Day 8 relative to the dosing of oral aprepitant on Days 1 through 3. These effects were not considered clinically important. The AUC of midazolam on Day 15 was similar to that observed at baseline.
An additional study was completed with intravenous administration of midazolam and oral aprepitant. Intravenous midazolam 2 mg was given 1 hour after oral administration of a single dose of oral aprepitant 125 mg. The plasma AUC of midazolam was increased by 1.5-fold.
Effect of other agents on the pharmacokinetics of aprepitant
Aprepitant is a substrate for CYP3A4; therefore, coadministration of fosaprepitant or aprepitant with drugs that inhibit CYP3A4 activity may result in increased plasma concentrations of aprepitant. Consequently, concomitant administration of fosaprepitant or aprepitant with strong CYP3A4 inhibitors (e.g., ketoconazole, itraconazole, nefazodone, troleandomycin, clarithromycin, ritonavir, nelfinavir) should be approached with caution. Because moderate CYP3A4 inhibitors (e.g., diltiazem) result in a 2-fold increase in plasma concentrations of aprepitant, concomitant administration should also be approached with caution.
Aprepitant is a substrate for CYP3A4; therefore, coadministration of fosaprepitant or aprepitant with drugs that strongly induce CYP3A4 activity (e.g., rifampin, carbamazepine, phenytoin) may result in reduced plasma concentrations and decreased efficacy.
Ketoconazole: When a single 125-mg dose of oral aprepitant was administered on Day 5 of a 10-day regimen of 400 mg/day of ketoconazole, a strong CYP3A4 inhibitor, the AUC of aprepitant increased approximately 5-fold and the mean terminal half-life of aprepitant increased approximately 3-fold. Concomitant administration of fosaprepitant or aprepitant with strong CYP3A4 inhibitors should be approached cautiously.
Rifampin: When a single 375-mg dose of oral aprepitant was administered on Day 9 of a 14-day regimen of 600 mg/day of rifampin, a strong CYP3A4 inducer, the AUC of aprepitant decreased approximately 11-fold and the mean terminal half-life decreased approximately 3-fold.
Coadministration of fosaprepitant or aprepitant with drugs that induce CYP3A4 activity may result in reduced plasma concentrations and decreased efficacy.
Additional interactions
Diltiazem: In a study in 10 patients with mild to moderate hypertension, intravenous infusion of 100 mg fosaprepitant over 15 minutes with diltiazem 120 mg 3 times daily, resulted in a 1.5-fold increase of aprepitant AUC and a 1.4-fold increase in diltiazem AUC. It also resulted in a small but clinically meaningful further maximum decrease in diastolic blood pressure [mean (SD) of 24.3 (± 10.2) mm Hg with fosaprepitant versus 15.6 (± 4.1) mm Hg without fosaprepitant] and resulted in a small further maximum decrease in systolic blood pressure [mean (SD) of 29.5 (± 7.9) mm Hg with fosaprepitant versus 23.8 (± 4.8) mm Hg without fosaprepitant], which may be clinically meaningful, but did not result in a clinically meaningful further change in heart rate or PR interval, beyond those changes induced by diltiazem alone.
In the same study, administration of aprepitant once daily, as a tablet formulation comparable to 230 mg of the capsule formulation, with diltiazem 120 mg 3 times daily for 5 days, resulted in a 2-fold increase of aprepitant AUC and a simultaneous 1.7-fold increase of diltiazem AUC. These pharmacokinetic effects did not result in clinically meaningful changes in ECG, heart rate or blood pressure beyond those changes induced by diltiazem alone.
Paroxetine: Coadministration of once daily doses of aprepitant, as a tablet formulation comparable to 85 mg or 170 mg of the capsule formulation, with paroxetine 20 mg once daily, resulted in a decrease in AUC by approximately 25% and Cmax by approximately 20% of both aprepitant and paroxetine.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies were conducted in Sprague-Dawley rats and in CD-1 mice for 2 years. In the rat carcinogenicity studies, animals were treated with oral doses ranging from 0.05 to 1000 mg/kg twice daily. The highest dose produced a systemic exposure to aprepitant (plasma AUC0-24hr) of 0.7 to 1.6 times the human exposure (AUC0-24hr = 19.6 mcg•hr/mL) at the recommended dose of 125 mg/day. Treatment with aprepitant at doses of 5 to 1000 mg/kg twice daily caused an increase in the incidences of thyroid follicular cell adenomas and carcinomas in male rats. In female rats, it produced hepatocellular adenomas at 5 to 1000 mg/kg twice daily and hepatocellular carcinomas and thyroid follicular cell adenomas at 125 to 1000 mg/kg twice daily. In the mouse carcinogenicity studies, the animals were treated with oral doses ranging from 2.5 to 2000 mg/kg/day. The highest dose produced a systemic exposure of about 2.8 to 3.6 times the human exposure at the recommended dose. Treatment with aprepitant produced skin fibrosarcomas at 125 and 500 mg/kg/day doses in male mice. Carcinogenicity studies were not conducted with fosaprepitant.
Aprepitant and fosaprepitant were not genotoxic in the Ames test, the human lymphoblastoid cell (TK6) mutagenesis test, the rat hepatocyte DNA strand break test, the Chinese hamster ovary (CHO) cell chromosome aberration test and the mouse micronucleus test.
Fosaprepitant, when administered intravenously, is rapidly converted to aprepitant. In the fertility studies conducted with fosaprepitant and aprepitant, the highest systemic exposures to aprepitant were obtained following oral administration of aprepitant. Oral aprepitant did not affect the fertility or general reproductive performance of male or female rats at doses up to the maximum feasible dose of 1000 mg/kg twice daily (providing exposure in male rats lower than the exposure at the recommended human dose and exposure in female rats at about 1.6 times the human exposure).
Pregnancy
Teratogenic Effects: Category B.
In the teratology studies conducted with fosaprepitant and aprepitant, the highest systemic exposures to aprepitant were obtained following oral administration of aprepitant. Teratology studies performed in rats at oral doses of aprepitant up to 1000 mg/kg twice daily (plasma AUC0-24hr of 31.3 mcg•hr/mL, about 1.6 times the human exposure at the recommended dose) and in rabbits at oral doses up to 25 mg/kg/day (plasma AUC0-24hr of 26.9 mcg•hr/mL, about 1.4 times the human exposure at the recommended dose) revealed no evidence of impaired fertility or harm to the fetus due to aprepitant. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
Nursing Mothers
Aprepitant is excreted in the milk of rats. It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk and because of the potential for possible serious adverse reactions in nursing infants from aprepitant and because of the potential for tumorigenicity shown for aprepitant in rodent carcinogenicity studies, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
Geriatric Use
In 2 well-controlled chemotherapy-induced nausea and vomiting clinical studies, of the total number of patients (N=544) treated with oral aprepitant, 31% were 65 and over, while 5% were 75 and over. No overall differences in safety or effectiveness were observed between these subjects and younger subjects. Greater sensitivity of some older individuals cannot be ruled out. Dosage adjustment in the elderly is not necessary.
ADVERSE REACTIONS
The overall safety of aprepitant was evaluated in approximately 4900 individuals.
Since EMEND for Injection is converted to aprepitant, those adverse experiences associated with aprepitant might also be expected to occur with EMEND for Injection.
Fosaprepitant (intravenous formulation)
In a randomized, open-label, incomplete crossover, bioequivalence study, 66 subjects were dosed with 115 mg of EMEND for Injection intravenously and 72 subjects received 125 mg of aprepitant orally. Systemic exposure of 115 mg of intravenous EMEND for Injection is equivalent to 125 mg oral aprepitant. The following clinical adverse experiences, regardless of causality, were reported in subjects dosed with EMEND for Injection: infusion site pain, 5 (7.6%); infusion site induration, 1 (1.5%); headache, 2 (3%).
Oral Aprepitant
Highly Emetogenic Chemotherapy
In 2 well-controlled clinical trials in patients receiving highly emetogenic cancer chemotherapy, 544 patients were treated with aprepitant during Cycle 1 of chemotherapy and 413 of these patients continued into the Multiple-Cycle extension for up to 6 cycles of chemotherapy. Oral aprepitant was given in combination with ondansetron and dexamethasone and was generally well tolerated. Most adverse experiences reported in these clinical studies were described as mild to moderate in intensity.
In Cycle 1, clinical adverse experiences were reported in approximately 69% of patients treated with the aprepitant regimen compared with approximately 68% of patients treated with standard therapy. Table 4 shows the percent of patients with clinical adverse experiences reported at an incidence ≥3%.
| Aprepitant Regimen (N=544) | Standard Therapy (N=550) |
|
| Body as a Whole/ Site Unspecified | ||
|
Abdominal Pain |
4.6 |
3.3 |
| Digestive System | ||
|
Constipation |
10.3 |
12.2 |
| Eyes, Ears, Nose, and Throat | ||
|
Tinnitus |
3.7 |
3.8 |
| Hemic and Lymphatic System | ||
|
Neutropenia |
3.1 |
2.9 |
| Metabolism and Nutrition | ||
|
Anorexia |
10.1 |
9.5 |
| Nervous System | ||
|
Headache |
8.5 |
8.7 |
| Respiratory System | ||
|
Hiccups |
10.8 |
5.6 |
In addition, isolated cases of serious adverse experiences, regardless of causality, of bradycardia, disorientation, and perforating duodenal ulcer were reported in highly emetogenic CINV clinical studies.
Moderately Emetogenic Chemotherapy
During Cycle 1 of a moderately emetogenic chemotherapy study, 438 patients were treated with the aprepitant regimen and 385 of these patients continued into the Multiple-Cycle extension for up to 4 cycles of chemotherapy. In Cycle 1, clinical adverse experiences were reported in approximately 73% of patients treated with the aprepitant regimen compared with approximately 75% of patients treated with standard therapy.
The adverse experience profile in the moderately emetogenic chemotherapy study was generally comparable to the highly emetogenic chemotherapy studies. Table 5 shows the percent of patients with clinical adverse experiences reported at an incidence ≥3%.
| Aprepitant Regimen (N=438) | Standard Therapy (N=428) |
|
| Blood and Lymphatic System Disorders | ||
|
Neutropenia |
8.9 |
8.4 |
| Metabolism and Nutrition Disorders | ||
|
Anorexia |
4.3 |
5.8 |
| Psychiatric Disorders | ||
|
Insomnia |
4.1 |
5.6 |
| Nervous System Disorders | ||
|
Dizziness |
3.4 |
4.2 |
| Vascular Disorders | ||
|
Hot Flush |
3.0 |
1.4 |
| Respiratory, Thoracic and Mediastinal Disorders | ||
|
Pharyngolaryngeal pain |
3.0 |
2.3 |
| Gastrointestinal Disorders | ||
|
Constipation |
12.3 |
18.0 |
| Skin and Subcutaneous Tissue Disorders | ||
|
Alopecia |
24.0 |
22.2 |
| General Disorders and General Administration Site Conditions | ||
|
Asthenia |
3.4 |
3.7 |
Isolated cases of serious adverse experiences, regardless of causality, of dehydration, enterocolitis, febrile neutropenia, hypertension, hypoesthesia, neutropenic sepsis, pneumonia, and sinus tachycardia were reported in the moderately emetogenic CINV clinical study.
Highly and Moderately Emetogenic Chemotherapy
The following additional clinical adverse experiences (incidence >0.5% and greater than standard therapy), regardless of causality, were reported in patients treated with aprepitant regimen:
Infections and infestations: candidiasis, herpes simplex, lower respiratory infection, pharyngitis, septic shock, upper respiratory infection, urinary tract infection.
Neoplasms benign, malignant and unspecified (including cysts and polyps): malignant neoplasm, non-small cell lung carcinoma.
Blood and lymphatic system disorders: anemia, febrile neutropenia, thrombocytopenia.
Metabolism and nutrition disorders: appetite decreased, diabetes mellitus, hypokalemia.
Psychiatric disorders: anxiety disorder, confusion, depression.
Nervous system: peripheral neuropathy, sensory neuropathy, taste disturbance, tremor.
Eye disorders: conjunctivitis.
Cardiac disorders: myocardial infarction, palpitations, tachycardia.
Vascular disorders: deep venous thrombosis, flushing, hypertension, hypotension.
Respiratory, thoracic and mediastinal disorders: cough, dyspnea, nasal secretion, pneumonitis, pulmonary embolism, respiratory insufficiency, vocal disturbance.
Gastrointestinal disorders: acid reflux, deglutition disorder, dry mouth, dysgeusia, dysphagia, eructation, flatulence, obstipation, salivation increased.
Skin and subcutaneous tissue disorders: acne, diaphoresis, rash.
Musculoskeletal and connective tissue disorders: arthralgia, back pain, muscular weakness, musculoskeletal pain, myalgia.
Renal and urinary disorders: dysuria, renal insufficiency.
Reproductive system and breast disorders: pelvic pain.
General disorders and administrative site conditions: edema, malaise, rigors.
Investigations: weight loss.
Laboratory Adverse Experiences
Table 6 shows the percent of patients with laboratory adverse experiences reported at an incidence ≥3% in patients receiving highly emetogenic chemotherapy.
| Aprepitant Regimen (N=544) | Standard Therapy (N=550) |
|
|
ALT Increased AST Increased Blood Urea Nitrogen Increased Serum Creatinine Increased Proteinuria |
6.0 3.0 4.7 3.7 6.8 |
4.3 1.3 3.5 4.3 5.3 |
The following additional laboratory adverse experiences (incidence >0.5% and greater than standard therapy), regardless of causality, were reported in patients treated with aprepitant regimen: alkaline phosphatase increased, hyperglycemia, hyponatremia, leukocytes increased, erythrocyturia, leukocyturia.
The adverse experiences of increased AST and ALT were generally mild and transient.
The following laboratory adverse experiences were reported at an incidence ≥3% during Cycle 1 of the moderately emetogenic chemotherapy study in patients treated with the aprepitant regimen or standard therapy, respectively: decreased hemoglobin (2.3%, 4.7%) and decreased white blood cell count (9.3%, 9.0%).
The adverse experience profiles in the Multiple-Cycle extensions for up to 6 cycles of chemotherapy were generally similar to that observed in Cycle 1.
Stevens-Johnson syndrome was reported as a serious adverse experience in a patient receiving aprepitant with cancer chemotherapy in another CINV study.
Other Studies with Postoperative Nausea and Vomiting
In well-controlled clinical studies in patients receiving general anesthesia, 564 patients were administered 40 mg aprepitant orally and 538 patients were administered 4 mg ondansetron I.V. EMEND was generally well tolerated. Most adverse experiences reported in these clinical studies were described as mild to moderate in intensity. Clinical adverse experiences were reported in approximately 60% of patients treated with 40 mg aprepitant compared with approximately 64% of patients treated with 4 mg ondansetron I.V.
Additional adverse experiences were observed in patients receiving general anesthesia. In the patients treated with aprepitant (40 mg) for postoperative nausea and vomiting, the following additional adverse experiences were reported, regardless of causality, at an incidence ≥3%: anemia, bradycardia, flatulence, hypotension, pruritus, pyrexia.
The following adverse experiences were reported, regardless of causality, in patients treated with aprepitant for postoperative nausea and vomiting at an incidence of >0.5% and greater than with ondansetron: abdominal pain, abdominal pain upper, blood pressure decreased, dizziness, dyspepsia, hematoma, hypoesthesia, hypothermia, hypovolemia, hypoxia, operative hemorrhage, pain, postoperative infection, respiratory depression, syncope, urticaria, wound dehiscence.
Other adverse experiences (incidence ≤0.5%) reported, regardless of causality, in patients treated with aprepitant 40 mg for postoperative nausea and vomiting included: bowel sounds abnormal, dysarthria, miosis, sensory disturbance, stomach discomfort, visual acuity reduced, wheezing.
Laboratory Adverse Experiences with Postoperative Nausea and Vomiting
One laboratory adverse experience, hemoglobin decreased (40 mg aprepitant), was reported, regardless of causality, at an incidence ≥3% in a patient receiving general anesthesia.
The following additional laboratory adverse experiences (incidence >0.5% and greater than ondansetron), regardless of causality, were reported in patients treated with aprepitant 40 mg: blood albumin decreased, blood bilirubin increased, blood glucose increased, blood potassium decreased, glucose urine present.
The adverse experience of ALT increased occurred with similar incidence in patients treated with aprepitant as in patients treated with ondansetron.
Other Studies
In addition, two serious adverse experiences were reported in postoperative nausea and vomiting (PONV) clinical studies in patients taking a higher dose of aprepitant: one case of constipation, and one case of sub-ileus.
Angioedema and urticaria were reported as serious adverse experiences in a patient receiving aprepitant in a non-CINV/non-PONV study.
Post-Marketing Experience:
The following adverse reactions have been identified during post-marketing use of aprepitant. Because these reactions are reported voluntarily from a population of uncertain size, it is generally not possible to reliably estimate their frequency or establish a causal relationship to the drug.
Skin and subcutaneous tissue disorders: pruritus, rash, urticaria
Immune system disorders: hypersensitivity reactions including anaphylactic reactions
OVERDOSAGE
No specific information is available on the treatment of overdosage. Single doses up to 200 mg of fosaprepitant I.V. and 600 mg of oral aprepitant were generally well tolerated in healthy subjects.
Three out of 33 subjects receiving 200 mg of fosaprepitant experienced mild injection site thrombosis. Aprepitant was generally well tolerated when administered as 375 mg once daily for up to 42 days to patients in non-CINV studies. In 33 cancer patients, administration of a single 375-mg dose of aprepitant on Day 1 and 250 mg once daily on Days 2 to 5 was generally well tolerated.
Drowsiness and headache were reported in one patient who ingested 1440 mg of aprepitant.
In the event of overdose, oral aprepitant should be discontinued and general supportive treatment and monitoring should be provided. Because of the antiemetic activity of aprepitant, drug-induced emesis may not be effective.
Aprepitant cannot be removed by hemodialysis.
DOSAGE AND ADMINISTRATION
EMEND for Injection is a sterile, lyophilized prodrug of aprepitant containing polysorbate 80 (PS80), to be administered intravenously as an infusion. Aprepitant is available as capsules (EMEND2) for oral administration.
EMEND for Injection (115 mg) may be substituted for EMEND (125 mg) 30 minutes prior to chemotherapy, on Day 1 only of the CINV regimen as an infusion administered over 15 minutes.
EMEND for Injection should not be mixed or reconstituted with solutions for which physical and chemical compatibility have not been established. EMEND for Injection is incompatible with any solutions containing divalent cations (e.g., Ca2+, Mg2+), including Lactated Ringer’s Solution and Hartmann's Solution.
The 3-day CINV regimen includes EMEND for Injection (115 mg) or EMEND (125 mg orally) on Day 1; EMEND (80 mg orally) on Days 2 and 3; in addition to a corticosteroid and a 5-HT3 antagonist as specified in the tables below.
In clinical studies with EMEND, the following regimen was used for the prevention of nausea and vomiting associated with highly emetogenic cancer chemotherapy:
| Day 1 | Day 2 | Day 3 | Day 4 | |
|
||||
| EMEND* | 125 mg orally | 80 mg orally | 80 mg orally | none |
| Dexamethasone† | 12 mg orally | 8 mg orally | 8 mg orally | 8 mg orally |
| Ondansetron‡ | 32 mg I.V. | none | none | none |
In a clinical study with EMEND, the following regimen was used for the prevention of nausea and vomiting associated with moderately emetogenic cancer chemotherapy:
| Day 1 | Day 2 | Day 3 | |
|
|||
| EMEND* | 125 mg orally | 80 mg orally | 80 mg orally |
| Dexamethasone† | 12 mg orally | none | none |
| Ondansetron‡ | 2 x 8 mg orally | none | none |
- 2
-
Registered trademark of MERCK & CO., Inc.
Preparation of EMEND for Injection
- Aseptically inject 5 mL 0.9% Sodium Chloride for Injection (saline) into the vial. Assure that saline is added to the vial along the vial wall in order to prevent foaming. Swirl the vial gently. Avoid shaking and jetting saline into the vial.
- Aseptically prepare an infusion bag filled with 110 mL of saline.
- Aseptically withdraw the entire volume from the vial and transfer it into the infusion bag containing 110 mL of saline to yield a total volume of 115 mL and a final concentration of 1 mg/1 mL.
- Gently invert the bag 2-3 times.
The reconstituted final drug solution is stable for 24 hours at ambient room temperature (at or below 25°C).
Parenteral drug products should be inspected visually for particulate matter and discoloration before administration whenever solution and container permit.
Caution: EMEND for Injection should not be mixed or reconstituted with solutions for which physical and chemical compatibility have not been established. EMEND for Injection is incompatible with any solutions containing divalent cations (e.g., Ca2+, Mg2+), including Lactated Ringer’s Solution and Hartmann's Solution.
General Information
EMEND for Injection has not been studied for the treatment of established nausea and vomiting.
Chronic continuous administration is not recommended (see PRECAUTIONS).
See PRECAUTIONS, Drug Interactions for additional information on dose adjustment for corticosteroids when coadministered with EMEND for Injection.
Refer to the full prescribing information for coadministered antiemetic agents.
EMEND for Injection may be administered with or without food.
No dosage adjustment is necessary for the elderly.
No dosage adjustment is necessary for patients with renal insufficiency or for patients with end stage renal disease undergoing hemodialysis.
No dosage adjustment is necessary for patients with mild to moderate hepatic insufficiency (Child-Pugh score 5 to 9). There are no clinical data in patients with severe hepatic insufficiency (Child-Pugh score >9).
HOW SUPPLIED
No. 3884 — One 115 mg single dose per 10 mL glass vial: White to off-white lyophilized solid. Supplied as follows:
NDC 0006-3884-32 1 vial per carton.
Storage
Vials: Store at 2-8°C (36-46°F).
Sterile lyophilized powder for intravenous use only after reconstitution and dilution.
Rx only
Manufactured for:
MERCK & CO., INC., Whitehouse Station, NJ 08889, USA
Manufactured by:
DSM Pharmaceuticals, Inc., 5900 Martin Luther King Jr. Highway, Greenville, NC 27834
U.S. Patent Nos.: 5,512,570; 5,691,336
Issued February 2009
Printed in USA
9840002
PATIENT PACKAGE INSERT
Patient Information
EMEND®
(fosaprepitant dimeglumine)
for Injection
You should read this information before you start taking EMEND1 (fosaprepitant dimeglumine) for Injection. Also, read the leaflet each time you refill your prescription, in case any information has changed. This leaflet provides only a summary of certain information about EMEND for Injection. Your doctor or pharmacist can give you an additional leaflet that is written for health professionals that contains more complete information. This leaflet does not take the place of careful discussions with your doctor. You and your doctor should discuss EMEND for Injection when you start taking your medicine.
What is EMEND for Injection?
EMEND for Injection is an antiemetic medicine for use in adult patients, to be given intravenously by your doctor. An antiemetic is a medicine used to prevent and control nausea and vomiting. EMEND for Injection is always used WITH OTHER MEDICINES to prevent and control nausea and vomiting caused by your chemotherapy treatment. EMEND for Injection is not used to treat nausea and vomiting that you already have.
Who should not take EMEND for Injection?
Do not take EMEND for Injection if you:
- are taking any of the following medicines3:
- ORAP® (pimozide)
- SELDANE® (terfenadine)
- HISMANAL® (astemizole)
- PROPULSID® (cisapride)
Taking EMEND for Injection with these medicines could cause serious or life-threatening problems.
- are allergic to fosaprepitant or any of the ingredients in EMEND for Injection. The active ingredient is fosaprepitant. See the end of this leaflet for a list of all the ingredients in EMEND for Injection.
- 3
-
The brands listed are the registered trademarks of their respective owners and are not trademarks of Merck & Co., Inc.
What should I tell my doctor before and during treatment with EMEND for Injection?
Tell your doctor:
- if you are pregnant or plan to become pregnant. It is not known if EMEND for Injection can harm your unborn baby.
- if you are breast-feeding. It is not known if EMEND for Injection passes into your milk and if it can harm your baby.
- if you have liver problems.
- about all your medical problems.
- about all the medicines that you are taking or plan to take, prescription and nonprescription medicines, vitamins, and herbal supplements. EMEND for Injection may cause serious life-threatening reactions if used with certain medicines (see the section Who should not take EMEND for Injection?). Some medicines can affect EMEND for Injection. EMEND for Injection may also affect some medicines, including chemotherapy, causing them to work differently in your body.
Your doctor may check to make sure your other medicines are working, while you are taking EMEND for Injection. Patients who take COUMADIN® (warfarin) may need to have blood tests after each 3-day treatment to check their blood clotting.
Women who use birth control medicines during treatment with EMEND for Injection and for up to 1 month after using EMEND for Injection should also use a back-up method of contraception to avoid pregnancy.
How should I take EMEND for Injection?
- EMEND for Injection is given intravenously on Day 1 only of a 3-day regimen.
The recommended dose of EMEND for Injection is:
- 115 mg given intravenously 30 minutes before you start your chemotherapy treatment;
AND - One 80-mg capsule of EMEND2 (aprepitant) each morning for the 2 days following your chemotherapy treatment.
- EMEND for Injection may be administered with or without food.
- Tell your doctor if you already have nausea and vomiting before you are given EMEND for Injection.
What are the possible side effects of EMEND for Injection?
The most common side effects of EMEND for Injection are:
- tiredness
- nausea
- hiccups
- constipation
- diarrhea
- loss of appetite
- headache
- hair loss
- injection site pain
- hardening of site of injection
The following side effects have been reported in general use with EMEND (aprepitant):
- Allergic reactions, which may be serious, and may include hives, rash and itching and cause difficulty in breathing or swallowing. If you have an allergic reaction, stop taking EMEND and call your doctor right away.
These are not all of the possible side effects of EMEND for Injection. For further information ask your doctor or pharmacist. Talk to your doctor about any side effect that bothers you.
General information about the use of EMEND for Injection
This leaflet summarizes the most important information about EMEND for Injection. If you would like to know more information, talk with your doctor. You can ask your doctor or pharmacist for information about EMEND for Injection that is written for health professionals.
What are the ingredients in EMEND for Injection?
Active ingredient: fosaprepitant
Inactive ingredients: edetate disodium, polysorbate 80, lactose anhydrous, sodium hydroxide and/or hydrochloric acid (for pH adjustment).
U.S. Patent Nos.: 5,512,570; 5,691,336
Issued February 2009
Manufactured for:
MERCK & CO., INC., Whitehouse Staton, NJ 08889, USA
Manufactured by:
DSM Pharmaceuticals, Inc., 5900 Martin Luther King Jr. Highway, Greenville, NC 27834
9840002
| EMEND
fosaprepitant dimeglumine injection, powder, lyophilized, for solution |
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
|
|||||||||||||||||||||||||
Revised: 02/2009Merck & Co., Inc.